Does TENS Reduce the Intensity of Acute and Chronic Pain? A Comprehensive Appraisal of the Characteristics and Outcomes of 169 Reviews and 49 Meta-Analyses
Abstract
1. Introduction
Aim
2. Methods
2.1. Literature Search Methods
2.2. Eligibility Criteria
- that did not undertake an evaluation of TENS using systematic methodology in the broadest sense (e.g., comprehensive reviews, opinion pieces, commentaries);
- That evaluated invasive nerve stimulation techniques (e.g., percutaneous electrical nerve stimulation and electro-acupuncture);
- where TENS was not a primary treatment (i.e., where TENS was a possible comparator);
- where the primary intention of TENS was not to stimulate peripheral nerves to alleviate pain (e.g., TENS for bladder dysfunction, constipation, dementia);
- focused on ‘TENS-like’ currents that considered output specifications of a standard TENS device (e.g., interferential current, microcurrent).
2.3. Selection of Reviews
- report was not a review;
- report did not evaluate ‘standard TENS’;
- report did not evaluate TENS as a primary comparator i.e., TENS was a comparator rather than the primary treatment;
- report did not systematically search for RCTs;
- report did not evaluate pain intensity;
- report did not evaluate clinical pain, i.e., evaluation of healthy human participants.
2.4. Extraction and Management of Information
- clinical condition;
- type and scope of review;
- number of TENS studies, and/or reviews used in the evaluation;
- whether a meta-analysis was undertaken;
- effect size estimates for pain intensity, if calculated;
- conclusion stated by authors as a direct quote from their manuscript.
2.5. Data Analysis
Analysis of Characteristics of Reviews
- sufficient evidence in favour of TENS (+)—pooled analysis of ≥500 events or at least one RCT with ≥200 participants in each arm of the trial
- sufficient evidence in favour of control/placebo (−)—pooled analysis of ≥500 events or at least one RCT with ≥200 participants in each arm of the trial
- sufficient evidence that is conflicting/inconclusive (=)—no analysis of pooled data and at least two RCTs with ≥200 participants in each arm of the trial that are conflicting
- insufficient evidence to make a judgement (?)—pooled analysis of <500 events or no RCTs with ≥200 participants in each arm of the trial
3. Results
3.1. Search Findings
3.2. Description of Excluded Records
- the earlier review was more comprehensive and included more studies that the later review. For example, we included a Cochrane review on TENS for labour pain published in 2009 by Dowswell et al. [22] rather than a later journal report of the Cochrane report published in 2011 by the same team (Bedwell et al. [23]).
3.3. Characteristics of Included Reviews
3.3.1. Overviews of Systematic Reviews
3.3.2. Hybrid Reviews
3.3.3. Systematic Reviews
3.3.4. Meta-Analyses
Characteristics of the Analysis of Pain Intensity: Continuous Data
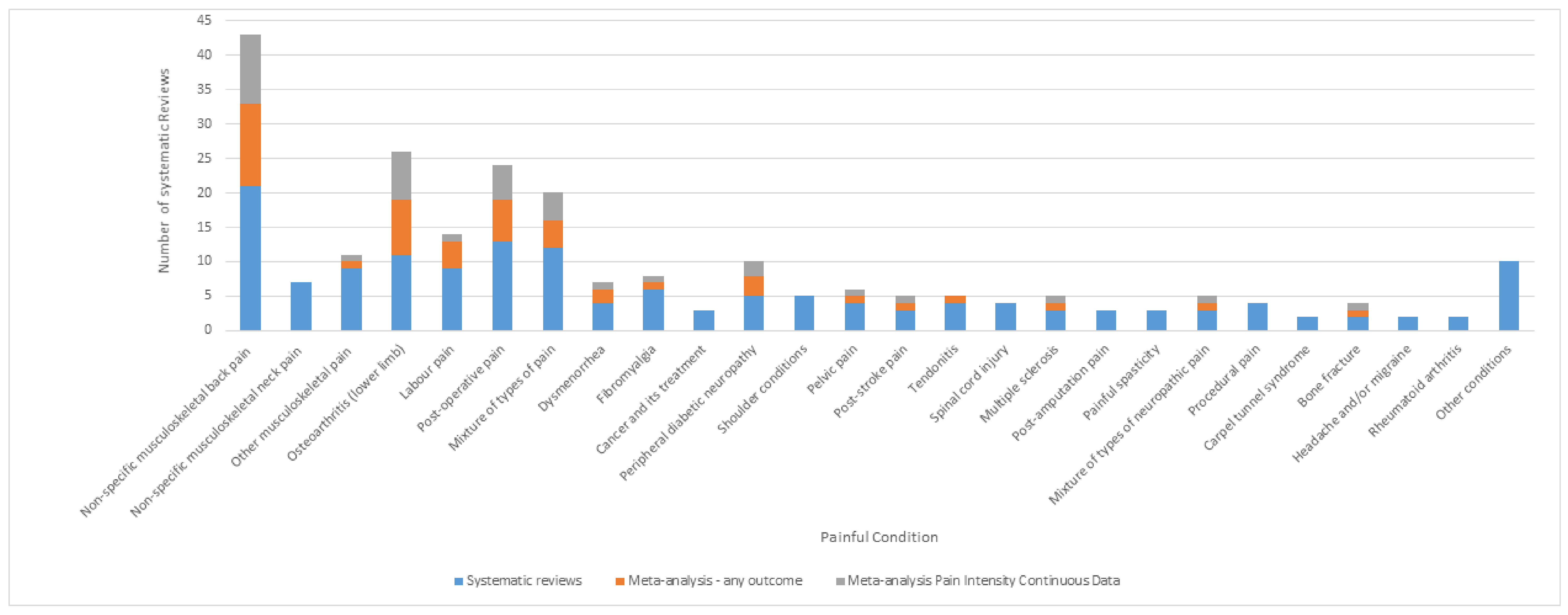
3.4. Analysis of Outcomes Irrespective of Condition
3.4.1. All Included Reviews
3.4.2. Overviews of Systematic Reviews
3.4.3. Hybrid Reviews
3.4.4. Systematic Reviews
3.4.5. Meta-Analyses TENS versus Control for Pain Intensity (Continuous Data)

3.5. Analysis of Outcomes Specific for Specific Pain Conditions
3.5.1. Mixtures of Painful Conditions (15 Reviews)
| Reference | Title | Condition | Comparison | No. Pooled Studies | Number of Participants Pooled TENS | Number of Participants Pooled Comparison | SMD | Lower CI | Upper CI | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Standardised Mean Difference during or post TENS relative to baseline | ||||||||||
| Wu et al., 2018 [14] | Literature Review and Meta-Analysis of Transcutaneous Electrical Nerve Stimulation in Treating Chronic Back Pain | Chronic low back pain | Control | 9 | TENS = 238 | Control = 159 | −0.2 | −0.58 | 0.18 | NOTE: Data also presented for SMD TENS vs. other nerve stimulation therapies = 0.86 (95%CI 0.15, 1.57), TENS = 122 NST = 105, 5 trials |
| Keller et al., 2007 [63] | Effect sizes of non-surgical treatments of non-specific low-back pain | Chronic low back pain | Placebo | 2 | Not reported Total sample = 114 | Not reported Total sample = 114 | −0.19 | −0.51 | 0.13 | NOTE: of the 2 studies one recorded improvement of pain on a 6 point Likert scale and the other pain intensity VAS |
| Philadelphia Panel 2001 [64] | Philadelphia Panel Evidence-Based Clinical Practice Guidelines on Selected Rehabilitation Interventions for Low Back Pain | Chronic low back pain | Unclear | 3 | Not reported | Not Reported | −0,2 | −0,4 | 0.1 | NOTE: MA for chronic back pain only. SMD reported but not trial arm sample sizes |
| Brosseau et al., 2002 [62] | Efficacy of the transcutaneous electrical nerve stimulation for the treatment of chronic low back pain—A meta-analysis. | Chronic low back pain | Placebo | 3 | TENS = 89 | Placebo = 82 | −4.32 | −10.36 | −1.72 | NOTE: We used data from Figure 1 of the report at 1 month |
| Stein et al., 2013 [65] | Electrical stimulation and electromagnetic field use in patients with diabetic neuropathy: systematic review and meta-analysis | Diabetic neuropathy | Sham | 5 | TENS = 76 | Sham TENS = 57 | −0.44 | −0.79 | −0.09 | |
| Jin et al., 2010 [66] | Effect of transcutaneous electrical nerve stimulation on symptomatic diabetic peripheral neuropathy: A meta-analysis of randomized controlled trials | Diabetic neuropathy | Sham | 2 | TENS = 26 | Sham TENS = 16 | −1.65 | −4.02 | 0.73 | NOTE: Forest plot has multiple counts from the same study. Figure within the report calculated an overall SMD with data extracted from different time points from the same study. We have extracted data at 12 weeks because other SMDs represented 1 study e.g., at 4 weeks SMD TENS vs. sham = −5.37 (95%CI −6.97, −3.77) pain intensity TENS = 18 sham = 13 |
| Almeida et al., 2018 [67] | Transcutaneous electrical nerve stimulation and interferential current demonstrate similar effects in relieving acute and chronic pain: a systematic review with meta-analysis | Acute and chronic pain—various | IFT | 8 | TENS = 249 | IFT = 243 | 0.36 | −0.56 | 1.27 | NOTE: Pain intensity VAS relative to baseline VAS, values pre-and post-intervention and results |
| Johnson and Martinson 2007 [10] | Efficacy of electrical nerve stimulation for chronic musculoskeletal pain: A meta-analysis of randomized controlled trials | Chronic musculoskeletal pain | Placebo | 28 | TENS/ES = 869 | Placebo = 823 | −0.99 | −1.25 | −0.74 | NOTE: Forest plot has multiple counts from the same study. Figure 2 within the report estimated overall SMD using data extracted from different time points from the same study. Also includes PENS interventions and data duplicates in analysis |
| Corbett et al., 2013 [68] | Acupuncture and other physical treatments for the relief of pain due to osteoarthritis of the knee: network meta-analysis | Osteoarthritis—knee pain | Standard care | 12 | Nor reported | Not reported | −0.65 | −1.06 | −0.25 | |
| Philadelphia Panel 2001 [69] | Clinical practice guidelines on selected rehabilitation interventions for knee pain | Osteoarthritis—knee pain | Placebo | 5 | TENS = 113 | Placebo = 111 | Not reported | Not reported | Not reported | NOTE: There is a forest plot but SMD not reported |
| Arik et al., 2021 [70] | The effect of TENS for pain relief in women with primary dysmenorrhea: A systematic review and meta-analysis | Dysmenorrhoea | Sham | 2 | TENS = 143 | Sham TENS = 156 | −1.38 | −2.26 | −0.5 | |
| Cottrell et al., 2014 [71] | Benefits and Harms of Electrical Neuromodulation for Chronic Pelvic Pain: A Systematic Review | Chronic pelvic pain | Control |
| Not reported
| Not reported
| Not reported | Not reported | Not reported | NOTE: Figure 2a from the report is a forest plot that provides pain scores in RCTs and (c) and Forest plot provides pain scores in non-RCTs. Neither states overall effect size for the TENS trials as overall effect size calculated from data pooled with other neuromodulation techniques |
| Price and Pandyan 2000 [72] | Electrical stimulation for preventing and treating post-stroke shoulder pain | Post-stroke—shoulder | Control | 2 | TENS = 46 | Control = 38 | −0.1 | −0.54 | 0.34 | NOTE: Extracted Electrical Stimulation (Functional electrical stimulation or TENS) vs. sham. There was only 1 SMD TENS vs. control = −0.44 (CI −1.05, −0.16), TENS = 26, control = 18 |
| Standardised Mean Difference during or post TENS (absolute difference) | ||||||||||
| Zimpel et al., 2020 [73] | Complementary and alternative therapies for post-caesarean pain | Postoperative pain—caesarean | Placebo | 3 | TENS = 119 | Control = 119 | −1.1 | −1.37 | −0.82 | SMD TENS (+ analgesia) vs. placebo (+ analgesia) = −1.10 (CI −1.37, −0.82) |
| Li and Song 2021 [74] | Transcutaneous electrical nerve stimulation for postoperative pain control after total knee arthroplasty: A meta-analysis of randomized controlled trials | Postoperative pain—knee arthroplasty | Control | 5 | TENS = 136 | Control = 131 | −0.26 | −0.44 | −0.08 | |
| Zhu et al., 2017 [75] | Effect of Transcutaneous Electrical Nerve Stimulation for Pain Control after Total Knee Arthroplasty: A Systematic Review and Meta-Analysis | Postoperative pain—knee arthroplasty | Control | 2 | TENS = 51 | Control = 51 | −0.47 | −0.87 | −0.08 | |
| Zeng et al., 2015 [76] | Electrical stimulation for pain relief in knee osteoarthritis systematic review and network meta-analysis | Osteoarthritis—knee pain | Control | 9 | Not reported Total sample = 329 | Not reported Total sample = 329 | −0.78 | −1.34 | −0.22 | NOTE: Used data for SMD h-TENS vs. control; Also reported: h-TENS vs. IFC = −0.14 (CI −1, 0.74), total sample = 56, 1 trial; h-TENS vs. l-TENS = −0.64 (CI −1.53, 0.32), total sample = 75. 2 trials; l-TENS vs. control = −0.14 (CI −1.03, 0.78), total sample = 123, 3 trials. This was a network meta-analysis. |
| Dowswell et al., 2009 [22] | Transcutaneous electrical nerve stimulation (TENS) for pain management in labour (Review) | Labour pain | Placebo/routine care | 2 | TENS = 143 | Placebo/routine care = 156 | −1.01 | −3.0 | 0.97 | NOTE: This is using the same study data as (Bedwell et al., 2011) but gets a different SMD. This used a random effects model |
| Standardised Mean Difference—Unclear whether absolute difference or difference relative to baseline | ||||||||||
| Chen et al., 2016 [77] | Transcutaneous Electrical Nerve Stimulation in Patients with Knee Osteoarthritis Evidence from Randomized-controlled Trials | Osteoarthritis—knee pain | Control | 12 | Not reported | Not reported | −0.79 | −1.31 | −0.27 | NOTE: Needed to manually calculate sample sizes. Exact time points for data extracted was unclear |
| Rutjes et al., 2009 [78] | Transcutaneous electrostimulation for osteoarthritis of the knee (Review) | Osteoarthritis—knee pain | Sham or no treatment | 11 | TENS = 275 | Control = 190 | −0.85 | −1.36 | −0.34 | NOTE: Post, but when post was not available, they pooled DRB |
| Sawant et al., 2015 [79] | Systematic review of efficacy of TENS for management of central pain in people with multiple sclerosis | Multiple sclerosis—central pain | Control | 4 | TENS = 109 | Control = 110 | −0.35 | −0.61 | −0.09 | |
| Standardised Mean Difference—No comparator (i.e., pre-post only) | ||||||||||
| Jauregui et al., 2016 [52] | A Meta-Analysis of Transcutaneous Electrical Nerve Stimulation for Chronic Low Back Pain | Chronic low back pain | None | 12 | Not reported | No control | 0.84 | 0.44 | 1.24 | |
| Cherian et al., 2016 [80] | The effects of various physical non-operative modalities on the pain in osteoarthritis of the knee | Osteoarthritis—knee pain | None | 7 | TENS = 107 | No control | 1.702 | 1.17 | 2.23 | |
| Reference | Title | Condition | Comparison | No. Pooled Studies | Number of Participants Pooled TENS | Number of Participants Pooled Comparison | Measure | MD | Lower CI | Upper CI | Comment |
|---|---|---|---|---|---|---|---|---|---|---|---|
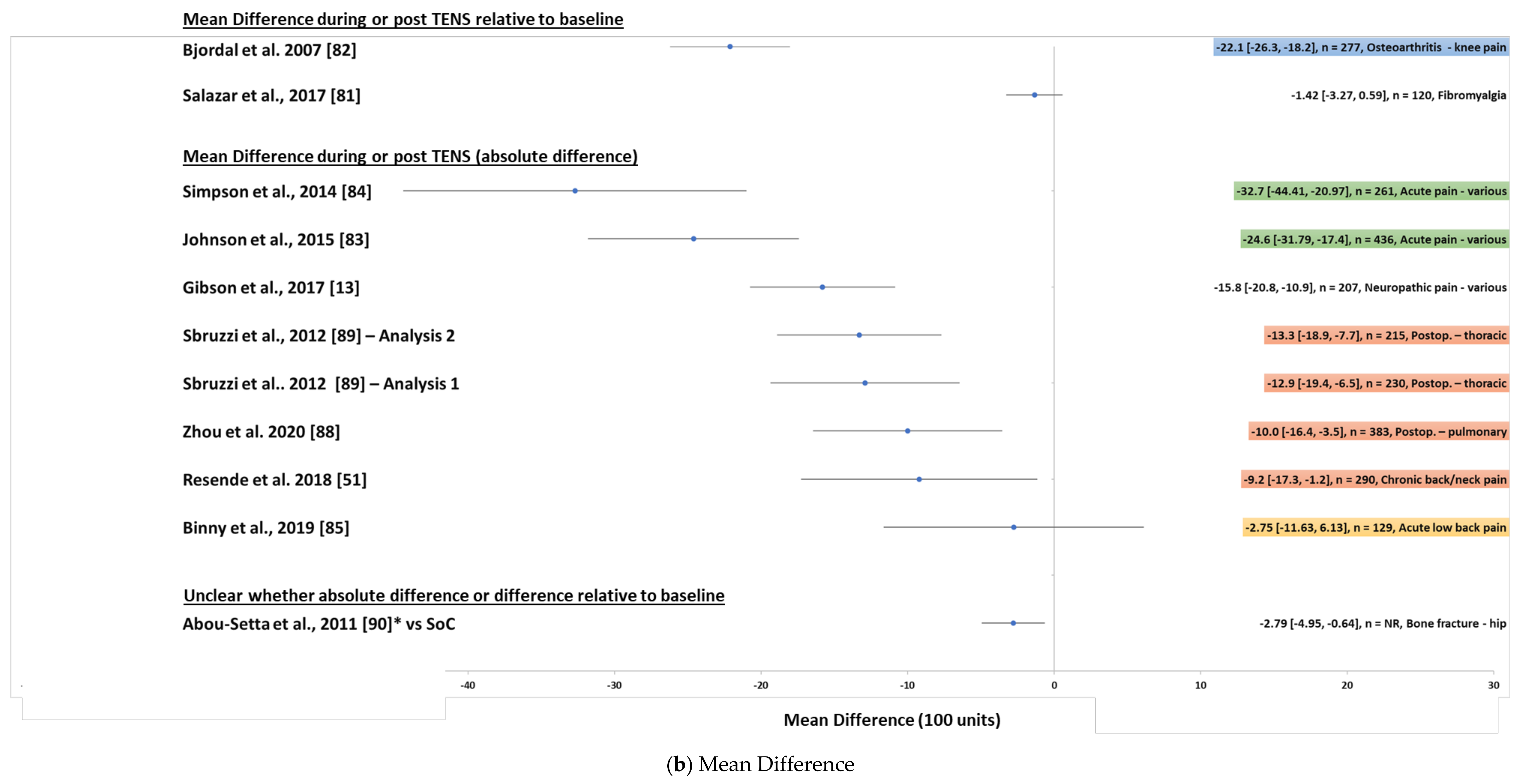
| Mean Difference during or post TENS relative to baseline | |||||||||||
| Salazar et al., 2017 [81] | Electric Stimulation for Pain Relief in Patients with Fibromyalgia: A Systematic Review and Meta-analysis of Randomized Controlled Trials | Fibromyalgia | Non-TENS | 5 | TENS = 63 | Non-TENS = 57 | Difference during/post TENS relative to baseline | −1.34 | −3.27 | 0.59 | Appears to be inconsistency in reporting of whether this is a mean difference or a standardised mean difference |
| Bjordal et al., 2007 [82] | Short-term efficacy of physical interventions in osteoarthritic knee pain. A systematic review and meta-analysis of randomised placebo-controlled trials. | Osteoarthritis—knee pain | Placebo | 7 | TENS (IFT) = 163 | Placebo = 114 | Difference during/post TENS relative to baseline | −22.1 | −26.3 | −18.12 | |
| Mean Difference during or post TENS (absolute difference) | |||||||||||
| Johnson et al., 2015 [83] | Transcutaneous electrical nerve stimulation for acute pain | Acute pain—various | Placebo | 6 | TENS = 218 | Placebo 218 | Absolute Difference during/post TENS | −24.6 | −31.79 | −17.4 | |
| Simpson et al., 2014 [84] | Transcutaneous electrical nerve stimulation for relieving acute pain in the prehospital setting | Acute pain—various in prehospital setting | Sham | 4 | TENS = 128 | Sham TENS = 133 | Absolute Difference during/post TENS | −32.7 | −44.41 | −20.97 | |
| Binny et al., 2019 [85] | Transcutaneous electric nerve stimulation (TENS) for acute low back pain: systematic review | Acute low back pain | Control | 2 | TENS = 64 | Control = 65 | Absolute Difference during/post TENS | −2.75 | −11.63 | 6.13 | |
| Resende et al., 2018 [51] | Meta-analysis of transcutaneous electrical nerve stimulation for relief of spinal pain | Chronic back and/or neck pain | Control | 6 | TENS/IFT 148 | Control = 142 | Absolute Difference during/post TENS | −9.2 | −17.3 | −1.2 | |
| Machado et al., 2009 [86] | Analgesic effects of treatments for non-specific low back pain: a meta-analysis of placebo-controlled randomized trials | Chronic low back pain | Placebo | 4 | Not reported Total sample 178 | Not reported Total sample 178 | Absolute Difference during/post TENS | Not reported | Not reported | Not reported | NOTE: Data was pooled and forest plot presented without numbers. Effect size not reported |
| Poitras and Brosseau 2008 [87] | Evidence-informed management of chronic low back pain with transcutaneous electrical nerve stimulation, interferential current, electrical muscle stimulation, ultrasound, and thermotherapy | Chronic low back pain | Control | 2 | Not reported | Not reported | Absolute Difference during/post TENS | Not reported | Not reported | Not reported | NOTE: There is a forest plot but MD data not reported—Figure 1 from the report—we used HF TENS (n = 2 studies) rather than LF TENSA (n = 3 studies) MD for High frequency = 2 studies but MD data not given on figure |
| van Middelkoop et al., 2011 [53] | A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain | Chronic low back pain | Control | 4 | Not reported | Not reported | Absolute Difference during/post TENS | Not possible to isolate TENS effects | Not possible to isolate TENS effects | Not possible to isolate TENS effects | NOTE: Not possible to isolate effects due to TENS alone as TENS as part of a combination therapy of therapeutic ultrasound, low level laser and massage. |
| Gibson et al., 2017 [13] | Transcutaneous electrical nerve stimulation (TENS) for neuropathic pain in adults (Review) | Neuropathic pain—various | Sham | 5 | TENS = 111 | Sham TENS = 96 | Absolute Difference during/post TENS | −15.8 | −20.8 | −10.9 | |
| Zhou et al., 2020 [88] | Efficacy of Transcutaneous Electronic Nerve Stimulation in Postoperative Analgesia After Pulmonary Surgery: A Systematic Review and Meta-Analysis | Postoperative pain—pulmonary surgery | Control | 7 | TENS = 193 | Control = 190 | Absolute Difference during/post TENS | −10 | −16.4 | −3.5 | |
| Sbruzzi et al., 2012 [89]—Analysis 1 surgery with posterolateral thoracotomy approach | Transcutaneous electrical nerve stimulation after thoracic surgery: systematic review and meta-analysis of randomized trials | Postoperative pain—thoracic surgery | Sham | 4 | TENS = 117 | Sham TENS = 113 | Absolute Difference during/post TENS | −12.9 | −19.4 | −6.5 | |
| Sbruzzi et al., 2012 [89]—Analysis 2 surgery with posterolateral thoracotomy approach | Transcutaneous electrical nerve stimulation after thoracic surgery: systematic review and meta-analysis of randomized trials | Postoperative pain—thoracic surgery | Control | 6 | TENS = 108 | Control = 107 | Absolute Difference during/post TENS | −13.3 | −18.9 | −7.7 | |
| Mean Difference—unclear whether absolute difference or difference relative to baseline | |||||||||||
| Abou-Setta et al., 2011 [90] | Comparative Effectiveness of Pain Management Interventions for Hip Fracture: A Systematic Review | Bone fracture—hip | Standard of care | 2 | Not reported | Not reported | Unclear | −2.79 | −4.95 | −0.64 | |
| Malone and Strube 1988 [91] | Meta-analysis of non-medical treatments for chronic pain | Chronic pain—various | No treatment | 2 | Not reported | Not reported | Unclear | 0.46 | Not reported | Not reported | MD TENS vs. no treatment control = 0.46 (SD = 0.07) |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Mixtures of different types of Chronic Pain | ||||||||||
| Gibson et al. [6] | Transcutaneous electrical nerve stimulation (TENS) for chronic pain—an overview of Cochrane Reviews (Review) | Chronic pain—various | Chronic | OCR | 51 | N | We were therefore unable to conclude with any confidence that, in people with chronic pain, TENS is harmful, or beneficial for pain control, disability, health-related quality of life, use of pain-relieving medicines, or global impression of change | ? | +/− | The most comprehensive review without meta-analysis to date |
| Axon et al. [92] | Use of multidomain management strategies by community dwelling adults with chronic pain: evidence from a systematic review | Chronic pain—various | Chronic | SR | 6 | N | No statement of conclusion for TENS | ? | ? | |
| Baird et al. [93] | Interventions for treating persistent pain in survivors of torture | Chronic pain—various | Chronic | CR | 1 | N | No statement of conclusion for TENS | ? | ? | Only 1 RCT—TENS as part of combination therapy |
| Crawford et al. [94] | Physically Oriented Therapies for the Self-Management of Chronic Pain Symptoms | Chronic pain—various | Chronic | SR | 2 | N | …no recommendation could be made for or against the usage of TENS as a self-management technique for chronic pain symptoms without more research | ? | ? | |
| Park et al. [95] | Nonpharmacological Approaches to the Management of Chronic Pain in Community-Dwelling Older Adults: A Review of Empirical Evidence | Chronic pain—various | Chronic | SR | 3 | N | Although the findings of the effectiveness of TENS are inconsistent in the reviewed studies, there was a trend toward greater pain reduction with active TENS than with placebo or the combination of TENS and acupuncture | ? | ? | |
| Nnoham et al. [96] | TENS for chronic pain | Chronic pain—various | Chronic | CR | 25 | N | Despite the widespread use of TENS machines, the analgesic effectiveness of TENS still remains uncertain | ? | ? | Update of Carroll et al. [97] by different team so included |
| Claydon et al. [24] | Does transcutaneous electrical nerve stimulation (TENS) produce ‘dose-responses’? A review of systematic reviews on chronic pain | Chronic pain—various | Chronic | OSR | 28 | N | Data from chronic pain trials that use these outcome measures show that any dose related responses of TENS cannot be conclusively demonstrated as a result of the number of confounding variables (e.g., inadequate design, low statistical power and differences in TENS protocols) | ? | ? | [28 RCTs described in 6 SRs] |
| Carroll et al. [97] | Transcutaneous electrical nerve stimulation (TENS) for chronic pain | Chronic pain—various | Chronic | CR | 19 | N | There is insufficient evidence to draw any conclusions about the effectiveness of TENS for the treatment of chronic pain in adults | ? | ? | Updated in 2008 (Nnoaham and Kumbang, 2008) [19 RCTs from 18 reports] |
| Reeve et al. [98] | Transcutaneous electrical nerve stimulation (TENS): a technology assessment | Chronic pain—various | Chronic | SR | 10 | N | …there is little evidence of the effectiveness of TENS in treating chronic pain | ? | ? | One report containing 3 separate SRs |
| Malone et al. [91] | Meta-analysis of non-medical treatments for chronic pain | Chronic pain—various | Chronic | SR | 7 | Y | Effect sizes for operant training and TENS were no larger than the estimated effect size for control conditions | − | ? | |
| Acute Pain (Various) 3 reviews | ||||||||||
| Johnson et al. [83] | Transcutaneous electrical nerve stimulation for acute pain | Acute pain—various | Acute | CR | 26 | Y | The analysis provides tentative evidence that TENS reduces pain intensity over and above that seen with placebo (no current) TENS when administered as a stand-alone treatment for acute pain in adults | + | ? | Comprehensive review—only assessed TENS as a stand-alone treatment |
| Simpson et al. [84] | Transcutaneous electrical nerve stimulation for relieving acute pain in the prehospital setting | Acute pain—various in prehospital setting | Acute | SR | 4 | Y | When administered by medics in the prehospital setting to patients with acute pain, TENS appears to be an effective and safe nonpharmacological analgesic modality that should be considered by emergency medical services organizations in which pharmacological pain management is restricted or unavailable | + | ? | |
| Reeve et al. [98] | Transcutaneous electrical nerve stimulation (TENS): a technology assessment | Acute—various | Acute | SR | 24 | N | …published evidence is equivocal in acute pain treatment | ? | ? | One report containing 3 separate SRs |
| Mixed Chronic/Acute Pain (Various) 2 reviews | ||||||||||
| Almeida et al. [67] | Transcutaneous electrical nerve stimulation and interferential current demonstrate similar effects in relieving acute and chronic pain: a systematic review with meta-analysis | Various—acute and chronic | Both | SR | 8 | Y | Transcutaneous electrical nerve stimulation and interferential current have similar effects on pain outcome | + | ? | There was no comparison with control/placebo |
| Samuel et al. [99] | Application of Low Frequency and Medium Frequency Currents in the Management of Acute and Chronic Pain—A Narrative Review | Various—acute and chronic | Both | MR | 3 9 SRs | N | We found through this review that even though TENS and IFT are used in management of pain, there is limited amount of high-quality research available… | ? | ? | |

Mixtures of Chronic Pain Conditions
Mixtures of Acute Pain Conditions
3.5.2. Musculoskeletal Pain (40 Reviews)
Non-Specific Back Pain (21 Reviews on Chronic, Two Reviews on Acute)
Non-Specific Neck Pain (Eight Reviews)
3.5.3. Osteoarthritis (13 Reviews)
3.5.4. Post-Operative Pain (13 Reviews)
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| OA Knee 10 reviews | ||||||||||
| Ferronato et al. [134] | Physical modalities on the functional performance in knee osteoarthritis: a systematic review | Osteoarthritis—knee | Chronic | SR | 13 | N | The use of TENS seems to be as or more effective than other analgesic therapies. From 11 articles included in this review, 10 articles evaluated the beneficial effects of TENS and 1 article didn’t notice increases in comparison with the placebo group | + | ? | |
| Chen et al. [77] | Transcutaneous Electrical Nerve Stimulation in Patients with Knee Osteoarthritis Evidence from Randomized-controlled Trials | Osteoarthritis—knee | Chronic | SR | 23 | Y | TENS might relieve pain due to knee osteoarthritis. Further randomized-controlled trials should focus on large-scale studies and a longer duration of follow-up. | ? | ? | |
| Cherian et al. [80] | The effects of various physical non-operative modalities on the pain in osteoarthritis of the knee | Osteoarthritis—knee | Chronic | SR | 7 | Y | In conclusion, all four non-operative modalities reduced the pain of OA of the knee: neuromuscular electrical stimulation and TENS were the most effective. | + | ? | |
| Zeng et al. [76] | Electrical stimulation for pain relief in knee osteoarthritis systematic review and network meta-analysis | Osteoarthritis—knee | Chronic | SR | 12 | Y | …the recommendation level of the other electrical stimulation therapies is either uncertain (h-TENS) or not appropriate (l-TENS…) for pain relief…Interferential currents seems to be the most promising pain relief treatment for the management of knee OA | ? | ? | |
| Corbett et al. [68] | Acupuncture and other physical treatments for the relief of pain due to osteoarthritis of the knee: network meta-analysis | Osteoarthritis—knee | Chronic | SR | 18 | Y | End of treatment results showed that eight interventions: interferential therapy, acupuncture, TENS, pulsed electrical stimulation, balneotherapy, aerobic exercise, sham acupuncture, and muscle-strengthening exercise produced a statistically significant reduction in pain when compared with standard care…Our analyses found little evidence (of significant differences from standard care, let alone clinically-relevant differences) to support such guidance with respect to treating pain, other than for TENS, where the evidence was of poor quality and likely to be unreliable. | + | ? | |
| Rutjes et al. [78] | Transcutaneous electrostimulation for osteoarthritis of the knee (Review) | Osteoarthritis—knee | Chronic | CR | 12 | Y | …we could not confirm that TENS is effective for pain relief. The current systematic review is inconclusive, hampered by the inclusion of only small trials of questionable quality | ? | ? | Update of Osiri et al. [133]. We included both reviews because conducted by different teams. There were 4 studies on interferential therapy included in the analysis |
| Jamtvedt et al. [54] | Physical therapy interventions for patients with osteoarthritis of the knee: an overview of systematic reviews. | osteoarthritis—knee | Chronic | OSR | 0 1 SR | N | There is moderate-quality evidence that acupuncture, TENS, and low-level laser therapy reduce pain…. | + | ? | |
| Bjordal et al. [82] | Short-term efficacy of physical interventions in osteoarthritic knee pain. A systematic review and meta-analysis of randomised placebo-controlled trials. | osteoarthritic knee pain | Chronic | SR | 11 | Y | TENS, electroacupuncture and low level laser therapy administered with optimal doses in an intensive 2–4 week treatment regimen, seem to offer clinically relevant short-term pain relief for OAK | + | ? | |
| Philadelphia Panel [69] | Clinical practice guidelines on selected rehabilitation interventions for knee pain | Knee pain—various | Both | SR | 6 | Y | TENS and therapeutic exercises were beneficial for knee osteoarthritis…TENS for Post-surgery Rehabilitation, Level I (RCT), Grade C for Pain (No Evidence of Clinically Important Benefit) | + | ? | |
| Osiri et al. [133] | Transcutaneous electrical nerve stimulation for knee osteoarthritis (Review) | Osteoarthritis—knee | Chronic | CR | 9 | Y | TENS and AL-TENS are shown to be effective in pain control over placebo in this review. | + | ? | Subsequently updated by Rutjes et al.,(Rutjes et al., 2009) |
| OA knee and hip 3 reviews | ||||||||||
| Zhang et al. [55] | OARSI recommendations for the management of hip and knee osteoarthritis, Part I: Critical appraisal of existing treatment guidelines and systematic review of current research evidence | Osteoarthritis—knee and hip | Chronic | OSR | 0 | N | TENS can help with short-term pain control in some patients with hip or knee OA | + | ? | Conclusion based on expert consensus rather than systematic review evidence |
| Brosseau et al. [136] | Efficacy of transcutaneous electrical nerve stimulation for osteoarthritis of the lower extremities: A meta-analysis | Osteoarthritis—Knee and hip | Chronic | SR | 6 | N | All modes of TENS (CTENS, ALTENS, BTENS, and MIX TENS) showed a significant benefit for pain relief in the treatment of osteoarthritis involving the knee and/or hip. This was true regardless of duration and repetition of intervention. | + | ? | |
| Puett et al. [137] | Published trials of nonmedicinal and non-invasive therapies for hip and knee osteoarthritis | Osteoarthritis—knee and hip | Chronic | SR | 3 | N | More data are needed to…evaluate the role of topical capsaicin, laser therapy, acupuncture, TENS, and pulsed electromagnetic fields. | ? | ? | |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Zimpel et al. [73] | Complementary and alternative therapies for post-caesarean pain | Postoperative pain—caesarean | Acute | CR | 10 | Y | TENS plus analgesia, compared with placebo plus analgesia, may reduce pain, heart rate and respiratory rate… | + | ? | |
| Zhou et al. [88] | Efficacy of Transcutaneous Electronic Nerve Stimulation in Postoperative Analgesia After Pulmonary Surgery: A Systematic Review and Meta-Analysis | Postoperative pain—pulmonary | Acute | SR | 10 | Y | Transcutaneous electronic nerve stimulation might be an effective supplementary analgesic regimen in multimodal analgesia to decrease pain intensity after pulmonary surgery | + | ? | |
| Terracina et al. [138] | Prevention and Treatment of Postoperative Pain after Lumbar Spine Procedures: A Systematic Review | Postoperative—lumbar | Acute | SR | 2 | N | No statement of conclusion for TENS | ? | ? | |
| Yue et al. [139] | Systematic Review of Three Electrical Stimulation Techniques for Rehabilitation After Total Knee Arthroplasty | Postoperative pain—knee arthroplasty | Acute | SR | 7 | N | As adjunct modalities, neuromuscular electrical stimulation and TENS can effectively improve rehabilitation after total knee arthroplasty | + | ? | Analysis of post-operative and short-term rehabilitation to 12 weeks |
| Zhu et al. [75] | Effect of TENS for pain control after post op knee arthroplasty | Postoperative pain—knee arthroplasty | Acute | SR | 6 | Y | Compared with control intervention, TENS supplementation intervention was found to significantly reduce pain and morphine requirement over a period of 24 h and to promote functional recovery in patients who have undergone total knee arthroplasty | + | ? | |
| Li et al. [74] | Transcutaneous electrical nerve stimulation for postoperative pain control after total knee arthroplasty: A meta-analysis of randomized controlled trials. | Postoperative pain—knee arthroplasty | Acute | SR | 5 | Y | TENS could significantly reduce pain and opioid consumption after total knee arthroplasty. In addition, there were fewer adverse effects in the TENS groups | + | ? | |
| Kerai et al. [140] | Role of transcutaneous electrical nerve stimulation in post-operative analgesia | Postoperative pain | Acute | SR | 8 | N | Most of the studies have demonstrated clinically significant reduction in pain intensity and supplemental analgesic requirement. However, these trials vary in TENS parameters used that is, duration, intensity, frequency of stimulation and location of electrodes. | + | ? | |
| Caley et al. [141] | The effects of transcutaneous electrical nerve stimulation (TENS) in postoperative cardiothoracic pain: a systematic review. | Postoperative cardio-thoracic pain cardiothoracic | Acute | SR | 4 | N | All studies concluded TENS to have no adverse effects and to be beneficial in post-operative pain…firm conclusions on the use of TENS in this setting cannot be made from this systematic review | ? | ? | |
| Sbruzzi et al. [89] | Transcutaneous electrical nerve stimulation after thoracic surgery: systematic review and meta-analysis of randomized trials | Postoperative pain—thoracic | Acute | SR | 11 | Y | TENS associated with pharmacological analgesia provides pain relief compared to the placebo TENS in postoperative thoracic surgery patients both approached by thoracotomy and sternotomy. In sternotomy it also provides more effective pain relief compared to pharmacological analgesia alone, but it has no significant effect on pulmonary function | + | ? | Includes two meta-analyses for different surgeries but does not combine as one |
| Freynet et al. [142] | Is transcutaneous electrical nerve stimulation effective in relieving postoperative pain after thoracotomy? | Postoperative pain—thoracotomy | Acute | SR | 9 | N | Hence, current evidence shows TENS associated with postoperative medications to be safe and effective in alleviating postoperative pain and in improving patient recovery, thus enhancing the choice of available medical care and bettering outcome after thoracic surgery | + | ? | |
| Sabino et al. [143] | Transcutaneous Electrical Nerve Stimulation in Thoracic or Abdominal Postoperative Conditions | Postoperative pain—thoracic and abdominal | Acute | SR | 6 | N | TENS demonstrated specific effectiveness for different outcomes. The results of this systematic review presented no evidences to recommend or reject the use of TENS for functional recovery in the postoperative period. The use of distinct TENS parameters, chosen in a random and unjustified form, made it impossible to determine optimal stimulation patterns | + | ? | |
| Bjordal et al. [11] | Transcutaneous electrical nerve stimulation (TENS) can reduce postoperative analgesic consumption A meta-analysis with assessment of optimal treatment parameters for postoperative pain. | Postoperative pain—various | Acute | SR | 21 | Y | TENS, administered with a strong, subnoxious intensity at an adequate frequency in the wound area, can significantly reduce analgesic consumption for postoperative pain | + | + | |
| Carroll et al. [5] | Randomization is important in studies with pain outcomes: systematic review of transcutaneous electrical nerve stimulation in acute postoperative pain | Postoperative pain—various | Acute | SR | 17 | N | Fourteen of the 17 included RCTs compared TENS with sham TENS; no differences were found. In 17 of these 19 [non-randomised] TENS studies, the authors concluded that TENS had appositive analgesic effect. | − | ? | Non-randomized studies overestimated treatment effects. Some of this data also reported by McQuay et al. [3] |
3.5.5. Labour Pain (10 Reviews)
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Thuvarakan et al. [26] | Transcutaneous electrical nerve stimulation as a pain-relieving approach in labor pain: A systematic review and Meta-Analysis of randomized controlled trials | Labour pain | Acute | SR | 26 | Y | The forest plot showed a small, but statistically significant efficacy of TENS on the reduction of pain intensity. However, it is not clear if the results were affected by the poor quality of the studies. This systematic review is the first that shows the application of TENS has significant efficacy in lowering labor pain | + | + | |
| Melo et al. [146] | Non-pharmacological resources: performance of physiotherapy in labor, a systematic review | Labour pain | Acute | SR | 3 | N | The studies suggest that the physiotherapy techniques investigated, for the most part, contributed in a beneficial way to relieving the pain of parturients…However, some findings have demonstrated inconclusive results about the effectiveness of techniques such as TENS, acupuncture, walking and breathing exercises | ? | ? | |
| Liddle et al. [147] | Interventions for preventing and treating low-back and pelvic pain during pregnancy. | Labour pain—low-back and pelvic pain | Acute | CR | 1 | N | There was low-quality evidence from one study by Keskin et al. [148]; n = 79 analysed) that TENS improved pain and functional disability significantly more than usual prenatal care | ? | ? | |
| Mafetoni et al. [149] | Non-pharmacological methods for pain releife during labour: Integrative review. Revista Mineira de Enfermagem, 18, 513–520. | Labour pain | Acute | SR | 4 | N | The use of TENS, for example, took place in the beginning of the first phase of labor, increasing pain tolerance; walking and/or the practice of keep the parturient in vertical position, showed to be an important strategy for pain relief, although it has been described that pain scores are higher according to the evolution of cervical dilation. | + | ? | |
| Jones et al. [25] | Pain management for women in labour: an overview of systematic reviews. | Labour pain | Acute | OSR | 22 1 CR | N | There is insufficient evidence to make judgements on whether or not hypnosis, biofeedback, sterile water injection, aromatherapy, TENS, or parenteral opioids are more effective than placebo or other interventions for pain management in labour] | ? | ? | A Cochrane overview of SRs not focussed on TENS |
| Mello et al. [150] | Transcutaneous electrical stimulation for pain relief during labor: a systematic review and meta-analysis | Labour pain | Acute | SR | 9 | Y | The use of TENS had no impact on mother or child and no influence on labor. According to the results of this review, there is no evidence that TENS reduces the use of additional analgesia. | − | ? | |
| Dowswell et al. [22] | Transcutaneous electrical nerve stimulation (TENS) for pain management in labour (Review) | Labour pain | Acute | CR | 18 | Y | There is only limited evidence that TENS reduces pain in labour and it does not seem to have any impact (either positive or negative) on other outcomes for mothers or babies | ? | ? | This review was discussed in a subsequent report by Bedwell et al. [23] in which effect size estimates differed but did not affect the outcome |
| Simkin et al. [151] | Update on nonpharmacologic approaches to relieve labor pain and prevent suffering | Labour pain | Acute | SR | 3 | N | TENS provides modest pain relief benefits and is a satisfying option for most women who use it. Its efficacy in relieving back pain deserves further study | + | ? | |
| Carroll et al. [144] | Transcutaneous electrical nerve stimulation does not relieve labor pain: updated systematic review | Labour pain | Acute | SR | 10 | Y | The findings of this review suggest that TENS has no significant effect on pain in labour | − | ? | Update of Carroll et al. [152] and data also reported in McQuay et al. [3] |
| Reeve et al. [98] | Transcutaneous electrical nerve stimulation (TENS): a technology assessment. | Labour pain | Acute | SR | 12 | N | The bulk of evidence in labour and delivery indicates that TENS is not effective | − | ? | One report containing 3 separate SRs |
3.5.6. Dysmenorrhea (Seven Reviews) and Pelvic Pain (Four Reviews)
3.5.7. Fibromyalgia (Six Reviews)
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Pelvic pain | ||||||||||
| Cottrell et al. [71] | Benefits and Harms of Electrical Neuromodulation for Chronic Pelvic Pain: A Systematic Review | Pelvic pain | Chronic | SR | 12 | Y | TENS has been shown to be an effective treatment for women with chronic pelvic pain secondary to dysmenorrhea and is free from adverse events, with the advantage that it can be self-applied and cost effective | + | ? | Review included studies on dysmenorrhoea |
| Franco et al. [154] | Non-pharmacological interventions for treating chronic prostatitis/chronic pelvic pain syndrome | Pelvic pain | Chronic | CR | 2 | Y | We were uncertain about the effects of…TENS,… | ? | ? | |
| Cheong et al. [158] | Non-surgical interventions for the management of chronic pelvic pain | Pelvic pain | Chronic | CR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Cohen et al. [159] | Therapeutic intervention for chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS): a systematic review and meta-analysis. | Pelvic pain | Chronic | SR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Dysmenorrhea | ||||||||||
| Arik et al. [70] | The effect of TENS for pain relief in women with primary dysmenorrhea: A systematic review and meta-analysis | Dysmenorrhea | Acute | SR | 4 | Y | TENS is a safe and well tolerated electrophysical therapy that may be effective for relieving pain in primary dysmenorrhea | + | ? | |
| Burnett et al. [58] | No. 345-Primary Dysmenorrhea Consensus Guideline. | Dysmenorrhea | Acute | MR | 1 1 SR | N | High-frequency TENS should be considered as a complementary treatment or in women unable or unwilling to use conventional therapy (II-1B)… | + | ? | |
| Igwea et al. [160] | TENS and heat therapy for pain relief and quality of life improvement in individuals with primary dysmenorrhea: A systematic review | Dysmenorrhea | Acute | SR | 6 | N | TENS and heat therapy show potential as adjunct remedies in the management of primary dysmenorrhea, but rigorous high-quality trials are still needed to make conclusive recommendation | ? | ? | |
| Kannan et al. [161] | Some physiotherapy treatments may relieve menstrual pain in women with primary dysmenorrhea: a systematic review | Dysmenorrhea | Acute | SR | 1 | N | Physiotherapists could consider using heat, TENS, and yoga in the management of primary dysmenorrhea | + | ? | |
| Latthe et al. [59] | Dysmenorrhea | Dysmenorrhea | Acute | MR | 1 | N | High-frequency TENS may reduce pain compared with sham TENS but seems to be less effective than ibuprofen | + | ? | |
| Proctor and Farquhar [60] | Dysmenorrhea | Dysmenorrhea | Acute | MR | 2 SRs | N | High-frequency TENS reduces pain compared with placebo TENS (moderate-quality evidence). We don’t know whether low-frequency TENS reduces pain compared with placebo TENS (low-quality evidence). The effectiveness of TENS is unclear compared with NSAIDs…(very low-quality evidence). | + | ? | |
| Proctor et al. [153] | Transcutaneous electrical nerve stimulation for primary dysmenorrhoea (Review) | Dysmenorrhoea | Acute | CR | 7 | Y | High-frequency TENS was found to be effective for the treatment of dysmenorrhoea by a number of small trials. The minor adverse effects reported in one trial require further investigation. There is insufficient evidence to determine the effectiveness of low-frequency TENS in reducing dysmenorrhoea | + | ? | Subsequently updated as a MR by Proctor and Farquhar [60] |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Megia Garcia et al. [155] | Analgesic effects of transcutaneous electrical nerve stimulation (TENS) in patients with fibromyalgia A systematic review | Fibromyalgia | Chronic | SR | 8 | N | Treatment with TENS is effective for reducing pain in people with fibromyalgia. In addition, the inclusion of TENS in therapeutic exercise programs seems to have a greater effect than practicing therapeutic exercise in isolation. Further studies are needed to investigate the optimization of the parameters of the TENS and a greater consensus among the variables used. | + | ? | |
| Honda et al. [162] | Effects of Physical-Agent Pain Relief Modalities for Fibromyalgia Patients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials | Fibromyalgia | Chronic | SR | 1 | N | TENS significantly reduced visual analogue scale scores.…Effect of electromagnetic therapy and TENS for the treatment of fibromyalgia on pain intensity was observed. | + | ? | |
| Ibanez-Vera et al. [163] | Passive physiotherapy for the treatment of the syndrome of fibromyalgia. A systematic review | Fibromyalgia | Chronic | SR | 4 | N | The quality of their subjects with fibromyalgia seems to be improving with…TENS,…with a limited number of studies | + | ? | |
| Johnson et al. [156] | Transcutaneous electrical nerve stimulation (TENS) for fibromyalgia in adults (Review) | Fibromyalgia | Chronic | CR | 8 | N | There was insufficient high-quality evidence to support or refute the use of TENS for fibromyalgia | ? | ? | |
| Salazar et al. [81] | Electric Stimulation for Pain Relief in Patients with Fibromyalgia: A Systematic Review and Meta-analysis of Randomized Controlled Trials | Fibromyalgia | Chronic | SR | 6 | Y | Our meta-analyses showed that electrical stimulation (electroacupuncture + TENS) in comparison with a control group seems be effective for pain relief in patients with fibromyalgia. Additionally, when we performed sensitivity analysis of the type of intervention, electroacupuncture presented favorable results toward the experimental group regarding pain relief, while TENS showed no effect. | ? | ? | Not sure whether MD relative to baseline in MA was in cm or mm |
| Ricci et al. [164] | The use of electrothermal and phototherapeutic methods for the treatment of fibromyalgia syndrome: a systematic review | Fibromyalgia | Chronic | SR | 1 | N | [One study] had positive outcomes after applying TENS for pain control, depression and quality of life in FMS patients, despite the fact that the sample of this study was not representative | ? | ? |
3.5.8. Specific Shoulder Conditions (Five Reviews)
3.5.9. Cancer and Its Treatment (Five Reviews)
3.5.10. Peripheral Diabetic Neuropathy (Five Reviews)
3.5.11. Tendinitis/Tendinopathy (Four Reviews)
3.5.12. Post-Stroke Pain (4 Reviews)
3.5.13. Spinal Cord Injury (Four Reviews)
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Hawk et al. [174] | Systematic Review of Nondrug, Nonsurgical Treatment of Shoulder Conditions | Shoulder Impingement | ? | SR | 1 | N | Evidence was inconclusive because of the scarcity of studies | ? | ? | |
| Haik et al. [175] | Effectiveness of physical therapy treatment of clearly defined subacromial pain: a systematic review of randomised controlled trials | Subacromial pain | Both | SR | 1 | N | Microwave diathermy and TENS do not seem to be beneficial in SAPS [subacromial pain] treatment. The evidence is still low due to the low number of participants and studies available in the literature | − | ? | |
| Page et al. [176] | Electrotherapy modalities for rotator cuff disease (Review) | Rotator cuff disease | Both | CR | 8 | N | We are uncertain whether TENS is superior to placebo, and whether any electrotherapy modality provides benefits over other active interventions (e.g., glucocorticoid injection) because of the very low quality of the evidence. due to the high risk of performance and detection bias (downgraded by two points) and imprecision (downgraded by one point) | ? | ? | |
| Page et al. [177] | Electrotherapy modalities for adhesive capsulitis (frozen shoulder) | Adhesive capsulitis | Both | CR | 1 | N | Overall, based on very low-quality evidence, we are uncertain whether a combination of therapeutic ultrasound, TENS and hot packs is an effective adjunct to exercise | ? | ? | |
| Johansson et al. [178] | A combination of systematic review and clinicians’ beliefs in interventions for subacromial pain | Subacromial pain | UC | SR | 1 | N | …there is no available evidence for efficacy of TENS for patients with subacromial pain | ? | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | No. TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Wu et al. [166] | Effectiveness of acupuncture and related therapies for palliative care of cancer: overview of systematic reviews | Cancer | Both | OSR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Bao et al. [167] | Complementary and Alternative Medicine for Cancer Pain: An Overview of Systematic Reviews. | Cancer pain | Chronic | OSR | 1 CR | N | Based on available evidence, we could find that…TENS,…might have beneficial effects on adult cancer pain…results were inconsistent for…TENS…plus cancer treatment | ? | ? | |
| Hökkä et al. [179] | A systematic review: non-pharmacological interventions in treating pain in patients with advanced cancer | Cancer | Chronic | SR | 1 | N | With just one limited study, it is not possible to draw conclusions about the safety and potential of TENS to reduce pain | ? | ? | |
| Hurlow et al. [168] | Transcutaneous electric nerve stimulation (TENS) for cancer pain in adults (Review) | Cancer pain | Chronic | CR | 2 | N | …the results of this updated systematic review remain inconclusive due to a lack of suitable RCTs | ? | ? | Updated review of Robb et al. [180] |
| Pan et al. [181] | Complementary and Alternative Medicine in the Management of Pain, Dyspnea, and Nausea and Vomiting Near the End of Life: A Systematic Review | Cancer pain | Chronic | SR | 1 | N | Case series and a small RCT suggest that TENS may provide short-term pain relief in dying patients or in patients with intractable cancer pain. TENS may provide short-term pain relief in patients with intractable or advanced cancer pain | + | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Zeng et al. [169] | Non-invasive neuromodulation effects on painful diabetic peripheral neuropathy: a systematic review and meta-analysis | Diabetic peripheral neuropathy | Chronic | SR | 7 | Y | We found a consistent medium to large effect size on pain reduction by central techniques, but no significant effects for the overall peripheral techniques, although we found a large effect for one of its subgroups (electrical peripheral techniques, predominantly TENS) | + | ? | |
| Stein et al. [65] | Electrical stimulation and electromagnetic field use in patients with diabetic neuropathy: systematic review and meta-analysis | Diabetic peripheral neuropathy | Both | SR | 5 | Y | We found that TENS improved pain relief in patients with diabetic neuropathy, while no such improvement was observed with the use of electromagnetic field treatment. The limited number of studies…demonstrate the need for further randomized clinical trials. | + | ? | |
| Dubinsky et al. [115] | Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review) | Diabetic peripheral neuropathy | Chronic | SR | 3 | N | TENS should be considered in the treatment of painful diabetic neuropathy (Level B) | + | ? | Conducted two analyses in same report—this is data for peripheral diabetic neuropathy |
| Jin et al. [66] | Effect of transcutaneous electrical nerve stimulation on symptomatic diabetic peripheral neuropathy: A meta-analysis of randomized controlled trials | Diabetic peripheral neuropathy | Chronic | SR | 3 | Y | TENS therapy may be an effective and safe strategy in treatment of symptomatic diabetic peripheral neuropathy | + | ? | |
| Pieber et al. [182] | Electrotherapy for the treatment of painful diabetic peripheral neuropathy: a review | Diabetic peripheral neuropathy | Chronic | SR | 5 | N | …the effects of TENS are consistent. The beneficial effects of prolonged use have been reported in three large studies and one small study.—TENS may be recommended for the treatment of PN. | + | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Dion et al. [183] | Are passive physical modalities effective for the management of common soft tissue injuries of the elbow? A systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) Collaboration | Tendinitis/Soft tissue injuries—elbow | UC | SR | 2 | N | …TENS provides no added benefit to patients with lateral epicondylitis. We found evidence from one low risk of bias RCT that TENS is not effective for the management of lateral epicondylitis | − | ? | |
| Wu et al. [184] | Comparative Effectiveness of Nonoperative Treatments for Chronic Calcific Tendinitis of the Shoulder: A Systematic Review and Network Meta-Analysis of Randomized Controlled Trials | Tendinitis—Shoulder, Chronic Calcific | Chronic | SR | 1 | Y | Compared with low-energy focused extracorporeal shockwave therapy, TENS, and ultrasound therapy, H-FSW is the best therapy for providing functional recovery | ? | ? | |
| Desmeules et al. [170] | Efficacy of transcutaneous electrical nerve stimulation for rotator cuff tendinopathy: a systematic review | Tendinopathy—rotator cuff | UC | SR | 6 | N | …no conclusions can be drawn on the efficacy of TENS for the treatment of rotator cuff tendinopathy | ? | ? | We categorised this study as tendinopathy rather than specific shoulder |
| Dingemanse et al. [185] | Evidence for the effectiveness of electrophysical modalities for treatment of medial and lateral epicondylitis: a systematic review | Lateral epicondylitis | Chronic | SR | 2 | N | …evidence of no difference in the effect of electrotherapy versus placebo was found | ? | ? | (Update of Dingemanse et al. [185]) |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Chen et al. [171] | The antalgic effects of non-invasive physical modalities on central post-stroke pain: a systematic review | Post-stroke pain | Chronic | SR | 1 | N | …the strength for its efficacy was poor and it was only effective for some of central post-stroke pain patients | ? | ? | |
| Ramos-Valero et al. [186] | Physiotherapy treatments for patients with shoulder pain after stroke. A systematic review | Post stroke pain—shoulder | Both | SR | 1 | N | These results indicate that this [TENS] technique does not only deal with the symptoms… | − | ? | |
| Barreca et al. [57] | Interventions for the paretic upper limb of stroke survivors: | Post stroke pain | Chronic | MR | 4 1 SR | N | …careful handling, electrical stimulation, movement with elevation, strapping, and the avoidance of overhead pulleys could effectively reduce or prevent pain in the paretic upper limb | + | ? | This systematic review focussed on motor impairment after stroke |
| Price and Pandyan [72] | Electrical stimulation for preventing and treating post-stroke shoulder pain | Post-stroke pain—shoulder | Both | CR | 4 | Y | The evidence…does not confirm or refute that electrical stimulation around the shoulder after stroke influences reports of pain, but there do appear to be benefits for passive humeral lateral rotation | ? | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Harvey et al. [172] | The effectiveness of 22 commonly administered physiotherapy interventions for people with spinal cord injury: a systematic review | Spinal cord injury | Chronic | SR | 2 | Y | …four interventions were clearly effective: fitness, hand and wheelchair training as well as TENS; however, the strength of evidence was not high | + | ? | |
| Boldt et al. [173] | Non-pharmacological interventions for chronic pain in people with spinal cord injury | Spinal cord injury—chronic | Chronic | CR | 1 | N | …Insufficient evidence…Trials using…TENS…provided no evidence that these interventions reduce chronic pain. | ? | ? | |
| Mehta et al. [187] | Neuropathic Pain Post Spinal Cord Injury Part 1: Systematic Review of Physical and Behavioral Treatment | Spinal cord injury—neuropathic pain | Chronic | SR | 2 | N | …there is conflicting evidence that TENS treatment reduces neuropathic pain post spinal cord injury | ? | ? | |
| Fattal et al. [188] | What is the efficacy of physical therapeutics for treating neuropathic pain in spinal cord injury patients? | Spinal cord injury—neuropathic | Unclear | SR | 2 | N | No statement of conclusion for TENS | ? | ? |
3.5.14. Procedural Pain (Four Reviews)
3.5.15. Neuropathic Pain (Three Reviews)
3.5.16. Multiple Sclerosis (Three Reviews)
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Kwan et al. [189] | Pain relief for women undergoing oocyte retrieval for assisted reproduction. | Procedural pain | Acute | CR | 0 | N | No statement of conclusion for TENS | ? | ? | Update of Kwan et al. [196] |
| Fleming et al. [197] | Non-pharmacological interventions for alleviating pain during orthodontic treatment | Orthodontic treatment—pain | Both | CR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Ngee-Ming et al. [191] | Complementary approaches to decreasing discomfort during shockwave lithotripsy (SWL) | Procedural pain | Acute | SR | 1 | N | …methods such as acupuncture, TENS and music offer an avenue to these benefits | + | ? | |
| Mujezinovic et al. [190] | Analgesia for amniocentesis or chorionic villus sampling | Procedural pain | Acute | CR | 0 | N | No statement of conclusion for TENS | ? | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | Meta-Analysis | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Gibson et al. [13] | Transcutaneous electrical nerve stimulation (TENS) for neuropathic pain in adults (Review) | Neuropathic pain—various | Chronic | CR | 15 | Y | …we were unable to confidently state whether TENS is effective for pain control in people with neuropathic pain. The very low quality of evidence means we have very limited confidence in the effect estimate reported; the true effect is likely to be substantially different | ? | ? | Robust review |
| Pittler et al. [198] | Complementary therapies for neuropathic and neuralgic pain: systematic review | Neuropathic pain—various | UC | SR | 3 | N | …evidence can be classified as encouraging and warrants further study for…electrostimulation | ? | ? | Included transcutaneous or percutaneous electrical nerve stimulation |
| Cruccu et al. [20] | EFNS guidelines on neurostimulation therapy for neuropathic pain | Neuropathic pain—various | UC | SR | 9 | N | High-frequency TENS may be better than placebo (level C) although worse than electroacupuncture (level B) | + | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Amatya et al. [192] | Non-pharmacological interventions for chronic pain in multiple sclerosis | Multiple sclerosis—chronic pain | Chronic | CR | 2 | N | There is very low-level evidence for the use of non-pharmacological interventions for chronic pain such as TENS,…in pain intensity of persons with multiple sclerosis | ? | ? | Update of Amatya et al. [199] |
| Sawant et al. [79] | Systematic review of efficacy of TENS for management of central pain in people with multiple sclerosis | Multiple sclerosis—central pain | Chronic | SR | 4 | Y | TENS is a safe and effective non-pharmacological alternative in the management of central pain in people living with multiple sclerosis. These findings are consistent with GRADE 2 level of evidence | + | ? | |
| Jawahar et al. [193] | Central neuropathic pain in multiple sclerosis | Multiple sclerosis—neuropathic pain | Chronic | SR | 2 | N | TENS may be effective in reducing central neuropathic pain… | + | ? |
3.5.17. Painful Spasticity (Three Reviews)
3.5.18. Post-Amputation Pain (Three Reviews)
3.5.19. Conditions with Two Reviews
3.5.20. Conditions with One Review
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Fernandez-Tenorio et al. [201] | Transcutaneous electrical nerve stimulation for spasticity: A systematic review | Spasticity—painful | Both | SR | 10 | N | We recommend TENS as a treatment for spasticity due to its low cost, ease of use, and absence of adverse reactions | + | ? | |
| Synnot et al. [202] | Interventions for managing skeletal muscle spasticity following traumatic brain injury (Review) | Muscle spasticity—traumatic brain injury | Acute | CR | 1 | N | No statement of conclusion for TENS | ? | ? | |
| Mills et al. [200] | Transcutaneous Electrical Nerve Stimulation for Management of Limb Spasticity: A Systematic Review | Spasticity | Both | SR | 14 | N | There was level 1 and 2 evidence for TENS improving spasticity-related outcome measures…Better responses in outcome measures…when TENS was used in combination with active therapy (e.g., exercise and task-related training) | + | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Johnson et al. [203] | Transcutaneous electrical nerve stimulation (TENS) for phantom pain and stump pain following amputation in adults (Review) | Amputation—phantom and stump pain | Chronic | CR | 2 | N | There were no RCTs to judge the effectiveness of TENS for the management of phantom pain and stump pain | ? | ? | There were two non RCTs |
| Hu et al. [209] | The effectiveness of acupuncture/TENS for phantom limb syndrome: A systematic review of controlled clinical trials | Amputation—phantom pain | Chronic | SR | 3 | N | There is some evidence for the use of acupuncture and TENS for the treatment of phantom limb pain, but insufficient high-quality evidence is available | ? | ? | |
| Halbert et al. [210] | Evidence for the Optimal Management of Acute and Chronic Phantom Pain: A Systematic Review | Amputation—phantom pain | Chronic | SR | 3 | N | No statement of conclusion for TENS | ? | ? |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Rheumatoid Arthritis | ||||||||||
| Brosseau et al. [205] | Transcutaneous electrical nerve stimulation (TENS) for the treatment of rheumatoid arthritis in the hand (Cochrane review) | Rheumatoid arthritis—hand | Chronic | CR | 3 | N | There are conflicting effects of TENS on pain outcomes in patients with RA. AL-TENS is beneficial for reducing pain intensity and improving muscle power scores over placebo while, conversely, C-TENS resulted in no clinical benefit on pain intensity compared with placebo. However, C-TENS resulted in a clinical benefit on patient assessment of change in disease over AL-TENS | ? | ? | Journal version also available in Brosseau et al. [62] |
| Ottawa Panel [204] | Ottawa Panel Evidence-Based Clinical Practice Guidelines for Electrotherapy and Thermotherapy Interventions in the Management of Rheumatoid Arthritis in Adults | Rheumatoid Arthritis | Chronic | SR | 3 | N | The Ottawa Panel recommends the use of…TENS…for the management of rheumatoid arthritis. Low-frequency TENS applied to the hand and wrist versus no stimulation, level I (RCT): grade A for pain at 3 weeks (clinically important benefit). High-frequency TENS applied to the hand and wrist versus placebo, level I (RCT): grade C for pain and joint tenderness, same day (no benefit). | + | ? | |
| Headache or migraine | ||||||||||
| Tao et al. [207] | Effectiveness of transcutaneous electrical nerve stimulation for the treatment of migraine: a meta-analysis of randomized controlled trials | Migraine | Chronic | SR | 4 | Y | This meta-analysis suggests that TENS may serve as an effective and well-tolerated alternative for migraineurs. However, low quality of evidence prevents us from reaching definitive conclusions RCTs | + | ? | Some interventions not standard TENS |
| Bronfort et al. [211] | Non-invasive physical treatments for chronic/recurrent headache | Headache | Chronic | CR | 2 | N | There is preliminary evidence that a combination of TENS and electrical neurotransmitter modulation is inferior to biofeedback and superior to relaxation for reduction of headache pain…evidence from one trial). There is limited evidence that a regimen of auto-massage, TENS, and stretching is superior to acupuncture for pain relief 4 to 9 weeks post-treatment. (evidence from one trial). | ? | ? | |
| Carpal tunnel syndrome | ||||||||||
| Huisstede et al. [212] | Carpal Tunnel Syndrome: Effectiveness of Physical Therapy and Electrophysical Modalities. An Updated Systematic Review of Randomized Controlled Trials | Carpal Tunnel | Chronic | SR | 2 | N | …there is moderate evidence that interferential current therapy is more effective than a night splint or TENS in the short term | − | ? | |
| Peters et al. [213] | Rehabilitation following carpal tunnel release | Carpal tunnel | Unclear | CR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Fracture Pain | ||||||||||
| Perillo et al. [214] | Pre-hospital femoral neck fracture management: A review of the literature | Bone fracture | Acute | SR | 1 | N | No statement of conclusion for TENS | ? | ? | One study found TENS effective in treating pain in the prehospital environment |
| Abou-Setta et al. [90] | Comparative Effectiveness of Pain Management Interventions for Hip Fracture: A Systematic Review | Hip fracture | Acute | SR | 2 | Y | …based on limited evidence, [TENS] seem to be safe and may result in clinically meaningful reductions in pain | ? | ? | |
3.6. Outcomes for Adverse Events
3.7. Synopsis of Characteristics and Outcomes
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Deussen et al. [215] | Relief of pain due to uterine cramping/involution after birth | Uterine cramping/involution after birth | Acute | CR | 3 | N | Very low-certainty evidence means we are uncertain if TENS is better than no TENS for adequate pain relief as reported by the women | ? | ? | Update of Deussen et al. [216] |
| Pal et al. [217] | Transcutaneous electrical nerve stimulation (TENS) for pain management in sickle cell disease (Review) | Sickle cell pain | Acute | CR | 1 | N | Since we have only included one small and very low-quality trial, with a high risk of bias across several domains, we are unable to conclude whether TENS is harmful or beneficial for managing pain in people with sickle cell disease | ? | ? | |
| De Andres et al. [218] | Vulvodynia—An Evidence-Based Literature Review and Proposed Treatment Algorithm | Vulvodynia | Chronic | SR | 3 | N | No statement of conclusion for TENS | ? | ? | |
| Liao et al. [219] | Efficacy of Non-invasive Stellate Ganglion Blockade Performed Using Physical Agent Modalities in Patients with Sympathetic Hyperactivity-Associated Disorders: A Systematic Review and Meta-Analysis. | Sympathetic Hyperactivity-Associated Disorders | Unclear | SR | 3 | N | Non-invasive Stellate Ganglion Blockade performed using PAMs [including TENS] effectively relieves pain of various etiologies, making it a valuable addition to the contemporary pain management armamentarium | ? | ? | |
| Oor et al. [220] | A systematic review of the treatment for abdominal cutaneous nerve entrapment syndrome | Nerve entrapment syndrome—abdominal cutaneous | Chronic | SR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Smart et al. [208] | Physiotherapy for pain and disability in adults with complex regional pain syndrome (CRPS) types I and II. | Complex regional pain syndrome | Both | CR | 6 | N | Evidence of the effectiveness of multimodal physiotherapy, electrotherapy and manual lymphatic drainage for treating people with CRPS types I and II is generally absent or unclear | + | ? | |
| Mansilla et al. [221] | Efficacy of transcutaneous electrical stimulation in trigeminal neuralgia. Eficacia de la estimulación eléctrica transcutánea en la neuralgia del trigémino. Rehabilitacion, 50, 81–86. | Trigeminal neuralgia | Chronic | SR | 2 | N | On the basis of published studies, TENS contributes positively to pain relief and functional improvement in patients affected by trigeminal pain. A larger number of studies are needed to…recommend its use | + | ? | In Portuguese |
| Kovacs et al. [222] | Surgery versus conservative treatment for symptomatic lumbar spinal stenosis: a systematic review of randomized controlled trials. | Spinal stenosis | Chronic | SR | 1 | N | One RCT on TENS as a comparator and uses TENS but is in combination with ultrasound and exercise. Not possible to isolate TENS | ? | ? | |
| McKneely et al. [223] | A systematic review of the effectiveness of physical therapy interventions for temporomandibular disorders. | temporomandibular disorders | Unclear | SR | 2 | N | …further research is warranted before dismissing any effect of TENS | ? | ? |
4. Discussion
4.1. Main Findings
4.2. Limitations of Our Appraisal
- Absence of an analysis of adverse events
- Absence of a quality assessment of included reviews
- Absence of an analysis of TENS technique, dose or timing of outcomes on judgements
4.2.1. Absence of an Analysis of Adverse Events
4.2.2. Absence of a Quality Assessment of Included Reviews
4.2.3. Absence of an Analysis of TENS Technique, Dose or Timing of Outcomes on Judgements
4.3. Challenges Encountered Conducting Our Descriptive Analysis
4.3.1. Screening Reports for Inclusion
4.3.2. Extracting, Categorising and Tallying Data
4.4. Strengths of Our Appraisal
4.5. Comments on the Body of Evidence
4.5.1. Unnecessary/Redundant Systematic Reviews
4.5.2. Variability in the Reporting and Execution of Reviews
4.5.3. Exaggeration of Process and Findings
4.5.4. Inadequacy of RCT Design
4.6. Stagnation of Knowledge over Three Decades
4.7. The Efficacy of TENS
4.8. Implications for Clinical Practice and Future Research
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Johnson, M. Transcutaneous Electrical Nerve Stimulation (TENS). Research to Support Clinical Practice; Oxford University Press: Oxford, UK, 2014. [Google Scholar]
- Long, D.M. Cutaneous afferent stimulation for relief of chronic pain. Clin. Neurosurg. 1974, 21, 257–268. [Google Scholar] [CrossRef]
- McQuay, H.J.; Moore, R.A.; Eccleston, C.; Morley, S.; Williams, A.C. Systematic review of outpatient services for chronic pain control. Health Technol. Assess. 1997, 1, 1–135. [Google Scholar] [CrossRef]
- McQuay, H.; Moore, A. TENS in acute postoperative pain. In An Evidence-Based Resource for Pain Relief; McQuay, H., Moore, A., Eds.; Oxford University Press: Oxford, UK, 1998; pp. 172–178. [Google Scholar]
- Carroll, D.; Tramer, M.; McQuay, H.; Nye, B.; Moore, A. Randomization is important in studies with pain outcomes: Systematic review of transcutaneous electrical nerve stimulation in acute postoperative pain. Br. J. Anaesth. 1996, 77, 798–803. [Google Scholar] [CrossRef] [PubMed]
- Gibson, W.; Wand, B.M.; Meads, C.; Catley, M.J.; O’Connell, N.E. Transcutaneous electrical nerve stimulation (TENS) for chronic pain—An overview of Cochrane Reviews. Cochrane Database Syst. Rev. 2019, 2, CD011890. [Google Scholar] [CrossRef] [PubMed]
- Travers, M.J.; O’Connell, N.E.; Tugwell, P.; Eccleston, C.; Gibson, W. Transcutaneous electrical nerve stimulation (TENS) for chronic pain: The opportunity to begin again. Cochrane Database Syst. Rev. 2020, 4, ED000139. [Google Scholar] [CrossRef] [PubMed]
- Moore, R.A.; Derry, S.; McQuay, H.J.; Straube, S.; Aldington, D.; Wiffen, P.; Bell, R.F.; Kalso, E.; Rowbotham, M.C. Clinical effectiveness: An approach to clinical trial design more relevant to clinical practice, acknowledging the importance of individual differences. Pain 2010, 149, 173–176. [Google Scholar] [CrossRef] [PubMed]
- Moore, R.A.; Gavaghan, D.; Tramer, M.R.; Collins, S.L.; McQuay, H.J. Size is everything-large amounts of information are needed to overcome random effects in estimating direction and magnitude of treatment effects. Pain 1998, 78, 209–216. [Google Scholar] [CrossRef]
- Johnson, M.; Martinson, M. Efficacy of electrical nerve stimulation for chronic musculoskeletal pain: A meta-analysis of randomized controlled trials. Pain 2007, 130, 157–165. [Google Scholar] [CrossRef]
- Bjordal, J.M.; Johnson, M.I.; Ljunggreen, A.E. Transcutaneous electrical nerve stimulation (TENS) can reduce postoperative analgesic consumption. A meta-analysis with assessment of optimal treatment parameters for postoperative pain. Eur. J. Pain 2003, 7, 181–188. [Google Scholar] [CrossRef]
- Knotkova, H.; Hamani, C.; Sivanesan, E.; Le Beuffe, M.F.E.; Moon, J.Y.; Cohen, S.P.; Huntoon, M.A. Neuromodulation for chronic pain. Lancet 2021, 397, 2111–2124. [Google Scholar] [CrossRef]
- Gibson, W.; Wand, B.M.; O’Connell, N.E. Transcutaneous electrical nerve stimulation (TENS) for neuropathic pain in adults. Cochrane Database Syst. Rev. 2017, 9, CD011976. [Google Scholar] [CrossRef]
- Wu, L.C.; Weng, P.W.; Chen, C.H.; Huang, Y.Y.; Tsuang, Y.H.; Chiang, C.J. Literature Review and Meta-Analysis of Transcutaneous Electrical Nerve Stimulation in Treating Chronic Back Pain. Reg. Anesth. Pain Med. 2018, 43, 425–433. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.I.; Jones, G.; Paley, C.A.; Wittkopf, P.G. The clinical efficacy of transcutaneous electrical nerve stimulation (TENS) for acute and chronic pain: A protocol for a meta-analysis of randomised controlled trials (RCTs). BMJ Open 2019, 9, e029999. [Google Scholar] [CrossRef]
- Dechartres, A.; Altman, D.G.; Trinquart, L.; Boutron, I.; Ravaud, P. Association between Analytic Strategy and Estimates of Treatment Outcomes in Meta-analysesAnalytic Strategy and Outcomes in Meta-analysesAnalytic Strategy and Outcomes in Meta-analyses. JAMA 2014, 312, 623–630. [Google Scholar] [CrossRef]
- Dechartres, A.; Trinquart, L.; Boutron, I.; Ravaud, P. Influence of trial sample size on treatment effect estimates: Meta-epidemiological study. BMJ 2013, 346, f2304. [Google Scholar] [CrossRef] [PubMed]
- Moore, A.R.; Eccleston, C.; Derry, S.; Wiffen, P.; Bell, R.F.; Straube, S.; McQuay, H. “Evidence” in chronic pain-establishing best practice in the reporting of systematic reviews. Pain 2010, 150, 386–389. [Google Scholar] [CrossRef] [PubMed]
- Moore, R.A.; Derry, S.; Wiffen, P.J. Challenges in design and interpretation of chronic pain trials. Br. J. Anaesth. 2013, 111, 38–45. [Google Scholar] [CrossRef] [PubMed]
- Cruccu, G.; Aziz, T.Z.; Garcia-Larrea, L.; Hansson, P.; Jensen, T.S.; Lefaucheur, J.P.; Simpson, B.A.; Taylor, R.S. EFNS guidelines on neurostimulation therapy for neuropathic pain. Eur. J. Neurol. 2007, 14, 952–970. [Google Scholar] [CrossRef] [PubMed]
- Cruccu, G.; Garcia-Larrea, L.; Hansson, P.; Keindl, M.; Lefaucheur, J.P.; Paulus, W.; Taylor, R.; Tronnier, V.; Truini, A.; Attal, N. EAN guidelines on central neurostimulation therapy in chronic pain conditions. Eur. J. Neurol. 2016, 23, 1489–1499. [Google Scholar] [CrossRef]
- Dowswell, T.; Bedwell, C.; Lavender, T.; Neilson, J.P. Transcutaneous electrical nerve stimulation (TENS) for pain relief in labour. Cochrane Database Syst. Rev. 2009, 2, CD007214. [Google Scholar] [CrossRef]
- Bedwell, C.; Dowswell, T.; Neilson, J.P.; Lavender, T. The use of transcutaneous electrical nerve stimulation (TENS) for pain relief in labour: A review of the evidence. Midwifery 2011, 27, e141–e148. [Google Scholar] [CrossRef]
- Claydon, L.; Chesterton, L. Does transcutaneous electrical nerve stimulation (TENS) produce ‘dose-responses’? A review of systematic reviews on chronic pain. Phys. Rev. 2008, 13, 450–463. [Google Scholar] [CrossRef]
- Jones, L.; Othman, M.; Dowswell, T.; Alfirevic, Z.; Gates, S.; Newburn, M.; Jordan, S.; Lavender, T.; Neilson, J.P. Pain management for women in labour: An overview of systematic reviews. Cochrane Database Syst. Rev. 2012, 3, CD009234. [Google Scholar] [CrossRef]
- Thuvarakan, K.; Zimmermann, H.; Mikkelsen, M.K.; Gazerani, P. Transcutaneous Electrical Nerve Stimulation as a Pain-Relieving Approach in Labor Pain: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Neuromodulation 2020, 23, 732–746. [Google Scholar] [CrossRef] [PubMed]
- Topuz, O.; Ozfidan, E.; Ozgen, M.; Ardic, F. Efficacy of transcutaneous electrical nerve stimulation and percutaneous neuromodulation therapy in chronic low back pain. J. Back Musculoskelet. Rehabil. 2004, 17, 127–133. [Google Scholar] [CrossRef]
- Facci, L.M.; Nowotny, J.P.; Tormem, F.; Trevisani, V.F. Effects of transcutaneous electrical nerve stimulation (TENS) and interferential currents (IFC) in patients with nonspecific chronic low back pain: Randomized clinical trial. Sao Paulo Med. J. 2011, 129, 206–216. [Google Scholar] [CrossRef]
- Ratajczak, B.; Hawrylak, A.; Demidas, A.; Kuciel-Lewandowska, J.; Boerner, E. Effectiveness of diadynamic currents and transcutaneous electrical nerve stimulation in disc disease lumbar part of spine. J. Back Musculoskelet. Rehabil. 2011, 24, 155–159. [Google Scholar] [CrossRef]
- Sahin, N.; Albayrak, I.; Ugurlu, H. Effect of Different Transcutaneous Electrical Stimulation Modalities on Cervical Myofascial Pain Syndrome. J. Musculoskelet. Pain 2011, 19, 18–23. [Google Scholar] [CrossRef]
- Alizade, M.H.; Ahmadizad, S. A comparision of exercise therapy and transcutaneous electrical nerve stimulation for the treatment of chronic low back pain. World J. Sport Sci. 2009, 2, 43–47. [Google Scholar]
- Itoh, K.; Itoh, S.; Katsumi, Y.; Kitakoji, H. A pilot study on using acupuncture and transcutaneous electrical nerve stimulation to treat chronic non-specific low back pain. Complement. Clin. Pr. 2009, 15, 22–25. [Google Scholar] [CrossRef]
- Barker, K.L.; Elliott, C.J.; Sackley, C.M.; Fairbank, J.C. Treatment of chronic back pain by sensory discrimination training. A Phase I RCT of a novel device (FairMed) vs. TENS. BMC Musculoskelet. Disord. 2008, 9, 97. [Google Scholar] [CrossRef]
- Kofotolis, N.D.; Vlachopoulos, S.P.; Kellis, E. Sequentially allocated clinical trial of rhythmic stabilization exercises and TENS in women with chronic low back pain. Clin. Rehabil. 2008, 22, 99–111. [Google Scholar] [CrossRef]
- Thompson, J.W.; Bower, S.; Tyrer, S.P. A double blind randomised controlled clinical trial on the effect of transcutaneous spinal electroanalgesia (TSE) on low back pain. Eur. J. Pain 2008, 12, 371–377. [Google Scholar] [CrossRef]
- Shimoji, K.; Takahashi, N.; Nishio, Y.; Koyanagi, M.; Aida, S. Pain relief by transcutaneous electric nerve stimulation with bidirectional modulated sine waves in patients with chronic back pain: A randomized, double-blind, sham-controlled study. Neuromodulation 2007, 10, 42–51. [Google Scholar] [CrossRef]
- Warke, K.; Al-Smadi, J.; Baxter, D.; Walsh, D.; Lowe-Strong, A. Efficacy of transcutaneous electrical nerve stimulation (tens) for chronic low-back pain in a multiple sclerosis population: A randomized, placebo-controlled clinical trial. Clin. J. Pain 2006, 22, 812–819. [Google Scholar] [CrossRef]
- Jarzem, P.F.; Harvey, E.J.; Arcaro, N.; Kaczorowski, J. Transcutaneous electrical nerve stimulation TENS for chronic low back pain. J. Musculoskelet. Pain 2005, 13, 3–9. [Google Scholar] [CrossRef]
- Jarzem, P.F.; Harvey, E.J.; Arcaro, N.; Kaczorowski, J. Transcutaneous electrical nerve stimulation TENS for short-term treatment of low back pain-randomized double blind crossover study of sham versus conventional TENS. J. Musculoskelet. Pain 2005, 13, 11–17. [Google Scholar] [CrossRef]
- Yokoyama, M.; Sun, X.; Oku, S.; Taga, N.; Sato, K.; Mizobuchi, S.; Takahashi, T.; Morita, K. Comparison of percutaneous electrical nerve stimulation with transcutaneous electrical nerve stimulation for long-term pain relief in patients with chronic low back pain. Anesth. Analg. 2004, 98, 1552–1556. [Google Scholar] [CrossRef] [PubMed]
- Hsieh, R.L.; Lee, W.C. One-shot percutaneous electrical nerve stimulation vs. transcutaneous electrical nerve stimulation for low back pain: Comparison of therapeutic effects. Am. J. Phys. Med. Rehabil. 2002, 81, 838–843. [Google Scholar] [CrossRef]
- Tsukayama, H.; Yamashita, H.; Amagai, H.; Tanno, Y. Randomised controlled trial comparing the effectiveness of electroacupuncture and TENS for low back pain: A preliminary study for a pragmatic trial. Acupunct. Med. 2002, 20, 175–180. [Google Scholar] [CrossRef]
- Cheing, G.L.; Hui_Chan, C.W. Transcutaneous electrical nerve stimulation: Nonparallel antinociceptive effects on chronic clinical pain and acute experimental pain. Arch. Phys. Med. Rehabil. 1999, 80, 305–312. [Google Scholar] [CrossRef]
- Grant, D.J.; Bishop_Miller, J.; Winchester, D.M.; Anderson, M.; Faulkner, S. A randomized comparative trial of acupuncture versus transcutaneous electrical nerve stimulation for chronic back pain in the elderly. Pain 1999, 82, 9–13. [Google Scholar] [CrossRef]
- Ghoname, E.A.; Craig, W.F.; White, P.F.; Ahmed, H.E.; Hamza, M.A.; Henderson, B.N.; Gajraj, N.M.; Huber, P.J.; Gatchel, R.J. Percutaneous electrical nerve stimulation for low back pain: A randomized crossover study. JAMA 1999, 281, 818–823, Erratum in 1999, 281, 1795. [Google Scholar] [CrossRef]
- Moore, S.R.; Shurman, J. Combined neuromuscular electrical stimulation and transcutaneous electrical nerve stimulation for treatment of chronic back pain: A double-blind, repeated measures comparison. Arch. Phys. Med. Rehabil. 1997, 78, 55–60. [Google Scholar] [CrossRef]
- Marchand, S.; Charest, J.; Li, J.; Chenard, J.; Lavignolle, B.; Laurencelle, L. Is TENS purely a placebo effect? A controlled study on chronic low back pain. Pain 1993, 54, 99–106. [Google Scholar] [CrossRef]
- Gemignani, G.; Olivieri, I.; Ruju, G.; Pasero, G. Transcutaneous electrical nerve stimulation in ankylosing spondylitis: A double-blind study. Arthritis Rheum. 1991, 34, 788–789. [Google Scholar] [CrossRef]
- Deyo, R.A.; Walsh, N.E.; Martin, D.C.; Schoenfeld, L.S.; Ramamurthy, S. A controlled trial of transcutaneous electrical nerve stimulation (TENS) and exercise for chronic low back pain. N. Engl. J. Med. 1990, 322, 1627–1634. [Google Scholar] [CrossRef] [PubMed]
- Lehmann, T.; Russell, D.; Spratt, K.; Colby, H.; Liu, Y.; Fairchild, M.; Christensen, S. Efficacy of electroacupuncture and TENS in the rehabilitation of chronic low back pain patients. Pain 1986, 26, 277–290. [Google Scholar] [CrossRef]
- Resende, L.; Merriwether, E.; Rampazo, E.P.; Dailey, D.; Embree, J.; Deberg, J.; Liebano, R.E.; Sluka, K.A. Meta-analysis of transcutaneous electrical nerve stimulation for relief of spinal pain. Eur. J. Pain 2018, 22, 663–678. [Google Scholar] [CrossRef] [PubMed]
- Jauregui, J.J.; Cherian, J.J.; Gwam, C.U.; Chughtai, M.; Mistry, J.B.; Elmallah, R.K.; Harwin, S.F.; Bhave, A.; Mont, M.A. A Meta-Analysis of Transcutaneous Electrical Nerve Stimulation for Chronic Low Back Pain. Surg. Technol. Int. 2016, 28, 296–302. [Google Scholar]
- Van Middelkoop, M.; Rubinstein, S.M.; Kuijpers, T.; Verhagen, A.P.; Ostelo, R.; Koes, B.W.; van Tulder, M.W. A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain. Eur. Spine J. 2011, 20, 19–39. [Google Scholar] [CrossRef] [PubMed]
- Jamtvedt, G.; Dahm, K.T.; Christie, A.; Moe, R.H.; Haavardsholm, E.; Holm, I.; Hagen, K.B. Physical therapy interventions for patients with osteoarthritis of the knee: An overview of systematic reviews. Phys. Ther. 2008, 88, 123–136. [Google Scholar] [CrossRef] [PubMed]
- Zhang, W.; Moskowitz, R.W.; Nuki, G.; Abramson, S.; Altman, R.D.; Arden, N.; Bierma-Zeinstra, S.; Brandt, K.D.; Croft, P.; Doherty, M.; et al. OARSI recommendations for the management of hip and knee osteoarthritis, part I: Critical appraisal of existing treatment guidelines and systematic review of current research evidence. Osteoarthr. Cart. 2007, 15, 981–1000. [Google Scholar] [CrossRef]
- Jensen, I.; Harms-Ringdahl, K. Neck pain. Best Pr. Res. Clin. Rheumatol. 2007, 21, 93–108. [Google Scholar] [CrossRef]
- Barreca, S.; Wolf, S.L.; Fasoli, S.; Bohannon, R. Treatment interventions for the paretic upper limb of stroke survivors: A critical review. Neurorehabilit. Neural Repair 2003, 17, 220–226. [Google Scholar] [CrossRef] [PubMed]
- Burnett, M.; Lemyre, M. No. 345-Primary Dysmenorrhea Consensus Guideline. J. Obs. Gynaecol. Can. 2017, 39, 585–595. [Google Scholar] [CrossRef]
- Latthe, P.M.; Champaneria, R.; Khan, K.S. Dysmenorrhoea. BMJ Clin. Evid. 2011, 2011, 0813. [Google Scholar] [PubMed]
- Proctor, M.L.; Farquhar, C.M. Dysmenorrhoea. BMJ Clin. Evid. 2007, 2007, 0813. [Google Scholar]
- Chou, R.; Huffman, L.H. Nonpharmacologic therapies for acute and chronic low back pain: A review of the evidence for an American Pain Society/American College of Physicians clinical practice guideline. Ann. Intern. Med. 2007, 147, 492–504. [Google Scholar] [CrossRef] [PubMed]
- Brosseau, L.; Milne, S.; Robinson, V.; Marchand, S.; Shea, B.; Wells, G.; Tugwell, P. Efficacy of the transcutaneous electrical nerve stimulation for the treatment of chronic low back pain—A meta-analysis. Spine 2002, 27, 596–603. [Google Scholar] [CrossRef] [PubMed]
- Keller, A.; Hayden, J.; Bombardier, C.; van Tulder, M. Effect sizes of non-surgical treatments of non-specific low-back pain. Eur. Spine J. 2007, 16, 1776–1788. [Google Scholar] [CrossRef]
- Philadelphia, P. Philadelphia Panel evidence-based clinical practice guidelines on selected rehabilitation interventions for low back pain. Phys. Ther. 2001, 81, 1641–1674. [Google Scholar]
- Stein, C.; Eibel, B.; Sbruzzi, G.; Lago, P.D.; Plentz, R.D. Electrical stimulation and electromagnetic field use in patients with diabetic neuropathy: Systematic review and meta-analysis. Braz. J. Phys. 2013, 17, 93–104. [Google Scholar] [CrossRef] [PubMed]
- Jin, D.M.; Xu, Y.; Geng, D.F.; Yan, T.B. Effect of transcutaneous electrical nerve stimulation on symptomatic diabetic peripheral neuropathy: A meta-analysis of randomized controlled trials. Diabetes Res. Clin. Pr. 2010, 89, 10–15. [Google Scholar] [CrossRef] [PubMed]
- Almeida, C.C.; Maldaner da Silva, V.Z.M.; Cipriano Junior, G.; Liebano, R.E.; Quagliotti Durigan, J.L. Transcutaneous electrical nerve stimulation and interferential current demonstrate similar effects in relieving acute and chronic pain: A systematic review with meta-analysis [with consumer summary]. Braz. J. Phys. 2018, 22, 347–354. [Google Scholar] [CrossRef] [PubMed]
- Corbett, M.S.; Rice, S.J.; Madurasinghe, V.; Slack, R.; Fayter, D.A.; Harden, M.; Sutton, A.J.; Macpherson, H.; Woolacott, N.F. Acupuncture and other physical treatments for the relief of pain due to osteoarthritis of the knee: Network meta-analysis. Osteoarthr. Cart. 2013, 21, 1290–1298. [Google Scholar] [CrossRef]
- Philadelphia Panel. Philadelphia Panel evidence-based clinical practice guidelines on selected rehabilitation interventions for knee pain. Phys. Ther. 2001, 81, 1675–1700. [Google Scholar]
- Arik, M.I.; Kiloatar, H.; Aslan, B.; Icelli, M. The effect of tens for pain relief in women with primary dysmenorrhea: A systematic review and meta-analysis. Explore 2020, 29, 2541. [Google Scholar] [CrossRef]
- Cottrell, A.M.; Schneider, M.P.; Goonewardene, S.; Yuan, Y.; Baranowski, A.P.; Engeler, D.S.; Borovicka, J.; Dinis-Oliveira, P.; Elneil, S.; Hughes, J.; et al. Benefits and Harms of Electrical Neuromodulation for Chronic Pelvic Pain: A Systematic Review. Eur. Urol. Focus 2020, 6, 559–571. [Google Scholar] [CrossRef]
- Price, C.I.; Pandyan, A.D. Electrical stimulation for preventing and treating post-stroke shoulder pain. Cochrane Database Syst. Rev. 2000, 4, CD001698. [Google Scholar] [CrossRef]
- Zimpel, S.A.; Torloni, M.R.; Porfirio, G.J.; Flumignan, R.L.; da Silva, E.M. Complementary and alternative therapies for post-caesarean pain. Cochrane Database Syst. Rev. 2020, 9, CD011216. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Song, Y. Transcutaneous electrical nerve stimulation for postoperative pain control after total knee arthroplasty: A meta-analysis of randomized controlled trials. Medicine 2017, 96, e8036. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.; Feng, Y.; Peng, L. Effect of transcutaneous electrical nerve stimulation for pain control after total knee arthroplasty: A systematic review and meta-analysis. J. Rehabil. Med. 2017, 49, 700–704. [Google Scholar] [CrossRef] [PubMed]
- Zeng, C.; Li, H.; Yang, T.; Deng, Z.H.; Yang, Y.; Zhang, Y.; Lei, G.H. Electrical stimulation for pain relief in knee osteoarthritis: Systematic review and network meta-analysis. Osteoarthr. Cart. 2015, 23, 189–202. [Google Scholar] [CrossRef]
- Chen, L.-X.; Zhou, Z.-R.; Li, Y.-L.; Ning, G.-Z.; Li, Y.; Wang, X.-B.; Feng, S.-Q. Transcutaneous electrical nerve stimulation in patients with knee osteoarthritis: Evidence from randomized-controlled trials. Clin. J. Pain 2016, 32, 146–154. [Google Scholar] [CrossRef]
- Rutjes, A.W.; Nuesch, E.; Sterchi, R.; Kalichman, L.; Hendriks, E.; Osiri, M.; Brosseau, L.; Reichenbach, S.; Juni, P. Transcutaneous electrostimulation for osteoarthritis of the knee. Cochrane Database Syst. Rev. 2009, 4, CD002823. [Google Scholar] [CrossRef]
- Sawant, A.; Dadurka, K.; Overend, T.; Kremenchutzky, M. Systematic review of efficacy of TENS for management of central pain in people with multiple sclerosis. Mult. Scler. Relat. Disord. 2015, 4, 219–227. [Google Scholar] [CrossRef]
- Cherian, J.J.; Jauregui, J.J.; Leichliter, A.K.; Elmallah, R.K.; Bhave, A.; Mont, M.A. The effects of various physical non-operative modalities on the pain in osteoarthritis of the knee. Bone Jt. J. 2016, 98-B, 89–94. [Google Scholar] [CrossRef]
- Salazar, A.P.; Stein, C.; Marchese, R.R.; Plentz, R.D.; Pagnussat, A.S. Electric Stimulation for Pain Relief in Patients with Fibromyalgia: A Systematic Review and Meta-analysis of Randomized Controlled Trials. Pain Physician 2017, 20, 15–25. [Google Scholar] [CrossRef]
- Bjordal, J.M.; Johnson, M.I.; Ab Lopes-Martins, R.; Bogen, B.; Chow, R.; Ljunggren, A.E. Short-term efficacy of physical interventions in osteoarthritic knee pain. A systematic review and meta-analysis of randomised placebo-controlled trials. BMC Musculoskelet. Disord. 2007, 8, 51. [Google Scholar] [CrossRef]
- Johnson, M.I.; Paley, C.A.; Howe, T.E.; Sluka, K.A. Transcutaneous electrical nerve stimulation for acute pain. Cochrane Database Syst. Rev. 2015, 6, CD006142. [Google Scholar] [CrossRef] [PubMed]
- Simpson, P.M.; Fouche, P.F.; Thomas, R.E.; Bendall, J.C. Transcutaneous electrical nerve stimulation for relieving acute pain in the prehospital setting: A systematic review and meta-analysis of randomized-controlled trials. Eur. J. Emerg. Med. 2014, 21, 10–17. [Google Scholar] [CrossRef] [PubMed]
- Binny, J.; Joshua Wong, N.L.; Garga, S.; Lin, C.W.C.; Maher, C.G.; McLachlan, A.J.; Traeger, A.C.; Machado, G.C.; Shaheed, C.A. Transcutaneous electric nerve stimulation (TENS) for acute low back pain: Systematic review. Scand. J. Pain 2019, 19, 225–233. [Google Scholar] [CrossRef] [PubMed]
- Machado, L.A.; Kamper, S.J.; Herbert, R.D.; Maher, C.G.; McAuley, J.H. Analgesic effects of treatments for non-specific low back pain: A meta-analysis of placebo-controlled randomized trials. Rheumatology 2009, 48, 520–527. [Google Scholar] [CrossRef] [PubMed]
- Poitras, S.; Brosseau, L. Evidence-informed management of chronic low back pain with transcutaneous electrical nerve stimulation, interferential current, electrical muscle stimulation, ultrasound, and thermotherapy. Spine J. 2008, 8, 226–233. [Google Scholar] [CrossRef]
- Zhou, J.; Dan, Y.; Yixian, Y.; Lyu, M.; Zhong, J.; Wang, Z.; Zhu, Y.; Liu, L. Efficacy of Transcutaneous Electronic Nerve Stimulation in Postoperative Analgesia After Pulmonary Surgery: A Systematic Review and Meta-Analysis. Am. J. Phys. Med. Rehabil. 2020, 99, 241–249. [Google Scholar] [CrossRef] [PubMed]
- Sbruzzi, G.; Silveira, S.A.; Silva, D.V.; Coronel, C.C.; Plentz, R.D. Transcutaneous electrical nerve stimulation after thoracic surgery: Systematic review and meta-analysis of 11 randomized trials. Rev. Bras. Cir. Cardiovasc. 2012, 27, 75–87. [Google Scholar] [CrossRef]
- Abou-Setta, A.M.; Beaupre, L.A.; Rashiq, S.; Dryden, D.M.; Hamm, M.P.; Sadowski, C.A.; Menon, M.R.; Majumdar, S.R.; Wilson, D.M.; Karkhaneh, M.; et al. Comparative effectiveness of pain management interventions for hip fracture: A systematic review. Ann. Intern. Med. 2011, 155, 234–245. [Google Scholar] [CrossRef]
- Malone, M.D.; Strube, M.J. Meta-analysis of non-medical treatments for chronic pain. Pain 1988, 34, 231–244. [Google Scholar] [CrossRef]
- Axon, D.R.; Patel, M.J.; Martin, J.R.; Slack, M.K. Use of multidomain management strategies by community dwelling adults with chronic pain: Evidence from a systematic review. Scand. J. Pain 2019, 19, 9–23. [Google Scholar] [CrossRef]
- Baird, E.; Williams, A.; Hearn, L.; Amris, K. Interventions for treating persistent pain in survivors of torture. Cochrane Database Syst. Rev. 2017, 8, CD012051. [Google Scholar] [CrossRef]
- Crawford, C.; Lee, C.; May, T. Physically oriented therapies for the self-management of chronic pain symptoms. Pain Med. 2014, 15 (Suppl. 1), S54–S65. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Park, J.; Hughes, A.K. Nonpharmacological Approaches to the Management of Chronic Pain in Community-Dwelling Older Adults: A Review of Empirical Evidence. J. Am. Geriatr. Soc. 2012, 60, 555–568. [Google Scholar] [CrossRef] [PubMed]
- Nnoaham, K.E.; Kumbang, J. Transcutaneous electrical nerve stimulation (TENS) for chronic pain. Cochrane Database Syst. Rev. 2008, 3, CD003222. [Google Scholar]
- Carroll, D.; Moore, R.A.; McQuay, H.J.; Fairman, F.; Tramer, M.; Leijon, G. Transcutaneous electrical nerve stimulation (TENS) for chronic pain. Cochrane Database Syst. Rev. 2001, 4, CD003222. [Google Scholar]
- Reeve, J.; Menon, D.; Corabian, P. Transcutaneous electrical nerve stimulation (TENS): A technology assessment. Int. J. Technol. Assess. Health Care 1996, 12, 299–324. [Google Scholar] [CrossRef] [PubMed]
- Samuel, S.R.; Maiya, G.A. Application of Low Frequency and Medium Frequency Currents in the Management of Acute and Chronic Pain—A Narrative Review. Indian J. Palliat. Care 2015, 21, 116–120. [Google Scholar] [CrossRef]
- Khadilkar, A.; Odebiyi, D.O.; Brosseau, L.; Wells, G.A. Transcutaneous electrical nerve stimulation (TENS) versus placebo for chronic low-back pain. Cochrane Database Syst. Rev. 2008, 4, CD003008. [Google Scholar] [CrossRef]
- Ely, S.; Barlas, P. Transcutaneous electrical acupoint stimulation for people with chronic musculoskeletal pain: An exploratory review. Phys. Rev. 2019, 24, 377–388. [Google Scholar] [CrossRef]
- Ely, S. Transcutaneous electrical nerve stimulation (TENS) at acupuncture points for the management of chronic pain: A narrative review. Physiotherapy 2016, 102, e90. [Google Scholar] [CrossRef][Green Version]
- Nunes, A.M.P.; Moita, J. Effectiveness of physical and rehabilitation techniques in reducing pain in chronic trapezius myalgia: A systematic review and meta-analysis. Int. J. Osteopath. Med. 2015, 18, 189–206. [Google Scholar] [CrossRef]
- Almeida, M.O.; Silva, B.N.; Andriolo, R.B.; Atallah, A.N.; Peccin, M.S. Conservative interventions for treating exercise-related musculotendinous, ligamentous and osseous groin pain. Cochrane Database Syst. Rev. 2013, 6, CD009565. [Google Scholar] [CrossRef]
- Bellini, C.; Monti, S.; Pillastrini, P. Physical Therapy Applied to Pathologies of Rehabilitative Interest. Sci. Riabil. 2011, 13, 37–45. [Google Scholar]
- Vernon, H.; Schneider, M. Chiropractic management of myofascial trigger points and myofascial pain syndrome: A systematic review of the literature. J. Manip. Physiol. 2009, 32, 14–24. [Google Scholar] [CrossRef] [PubMed]
- Rickards, L.D. The effectiveness of non-invasive treatments for active myofascial trigger point pain: A systematic review of the literature. Int. J. Osteopath. Med. 2006, 9, 120–136. [Google Scholar] [CrossRef]
- O’Connor, R.; Hurley, D.A. The effectiveness of physiotherapeutic interventions in the management of delayed-onset muscle soreness: A systematic review. Phys. Rev. 2003, 8, 177–195. [Google Scholar] [CrossRef]
- Philadelphia, P. Philadelphia Panel evidence-based clinical practice guidelines on selected rehabilitation interventions for shoulder pain. Phys. Ther. 2001, 81, 1719–1730. [Google Scholar]
- Nascimento, P.R.C.D.; Costa, L.O.P.; Araujo, A.C.; Poitras, S.; Bilodeau, M. Effectiveness of interventions for non-specific low back pain in older adults. A systematic review and meta-analysis. Physiotherapy 2018, 105, 147–162. [Google Scholar] [CrossRef] [PubMed]
- Bredow, J.; Bloess, K.; Oppermann, J.; Boese, C.K.; Lohrer, L.; Eysel, P. Conservative treatment of nonspecific, chronic low back pain: Evidence of the efficacy—A systematic literature review. Orthopade 2016, 45, 573–578. [Google Scholar] [CrossRef]
- Ehrenbrusthoff, K.; Ryan, C.; Schofield, P.; Martin, D. Physical therapy management of older adults with chronic low back pain: A systematic review. J. Pain Manag. 2012, 5, 317–329. [Google Scholar]
- Chou, R. Low back pain (chronic). BMJ Clin. Evid. 2010, 2010, 1116. [Google Scholar]
- Hall, H.; McIntosh, G. Low back pain (chronic). BMJ Clin. Evid. 2008, 2008, 1116. [Google Scholar]
- Dubinsky, R.M.; Miyasaki, J. Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review): Report of the Therapeutics and Technology Assessment Subcommittee of the American Academy of Neurology. Neurology 2010, 74, 173–176. [Google Scholar] [CrossRef]
- Johnson, M.; Walsh, D. Continued uncertainty of TENS effectiveness for pain relief. Nat. Rev. Rheumatol. 2010, 6, 314–316. [Google Scholar] [CrossRef] [PubMed]
- Gaid, M.; Cozens, A. The role of transcutaneous electric nerve stimulation (TENS) for the management of chronic low back pain. Int. Musculoskelet. Med. 2009, 31, 19–23. [Google Scholar] [CrossRef]
- Gutiérrez, H.; Ortiz, L. Evidence of the analgesic effect of physiotherapy in the low back pain syndrome. Rev. Iberoam. Fisioter. Kinesiol. 2009, 12, 84–95. [Google Scholar] [CrossRef]
- Khadilkar, A.; Milne, S.; Brosseau, L.; Robinson, V.; Saginur, M.; Shea, B.; Tugwell, P.; Wells, G. Transcutaneous electrical nerve stimulation (TENS) for chronic low-back pain. Cochrane Database Syst. Rev. 2005, 3, CD003008. [Google Scholar]
- Milne, S.; Welch, V.; Brosseau, L.; Saginur, M.; Shea, B.; Tugwell, P.; Wells, G. Transcutaneous electrical nerve stimulation (TENS) for chronic low back pain. Cochrane Database Syst. Rev. 2001, 2, CD003008. [Google Scholar]
- Pengel, H.M.; Maher, C.G.; Refshauge, K.M. Systematic review of conservative interventions for subacute low back pain. Clin. Rehabil. 2002, 16, 811–820. [Google Scholar] [CrossRef]
- Flowerdew, M.; Gadsby, G. A review of the treatment of chronic low back pain with acupuncture-like transcuatenous electrical nerve stimulation and transcutaneous electrical nerve stimulation. Complement. Med. 1997, 5, 193–201. [Google Scholar] [CrossRef]
- Gadsby, G.; Flowerdew, M. Nerve stimulation for low back pain—A review. Nurs. Stand. 1997, 11, 32–33. [Google Scholar] [CrossRef]
- McIntosh, G.; Hall, H. Low back pain (acute). BMJ Clin. Evid. 2011, 2011, 1102. [Google Scholar]
- Martimbianco, A.L.C.; Porfirio, G.J.; Pacheco, R.L.; Torloni, M.R.; Riera, R. Transcutaneous electrical nerve stimulation (TENS) for chronic neck pain. Cochrane Database Syst. Rev. 2019, 12, CD011927. [Google Scholar] [CrossRef]
- Binder, A.I. Neck pain. BMJ Clin. Evid. 2008, 2008, 1103. [Google Scholar]
- Vernon, H.T.; Humphreys, B.K.; Hagino, C.A. A systematic review of conservative treatments for acute neck pain not due to whiplash. J. Manip. Physiol. 2005, 28, 443–448. [Google Scholar] [CrossRef] [PubMed]
- Philadelphia, P. Philadelphia Panel evidence-based clinical practice guidelines on selected rehabilitation interventions for neck pain. Phys. Ther. 2001, 81, 1701–1717. [Google Scholar]
- Kjellman, G.V.; Skargren, E.I.; Oberg, B.E. A critical analysis of randomised clinical trials on neck pain and treatment efficacy. A review of the literature. Scand. J. Rehabil. Med. 1999, 31, 139–152. [Google Scholar] [CrossRef]
- Aker, P.; Gross, A.; Goldsmith, C.; Peloso, P. Conservative management of mechanical neck pain: Systematic overview and meta-analysis. BMJ 1996, 313, 1291–1296. [Google Scholar] [CrossRef]
- Gross, A.R.; Aker, P.D.; Goldsmith, C.H.; Peloso, P. Conservative management of mechanical neck disorders. A systematic overview and meta-analysis. Online J. Curr. Clin. Trials 1996. [Google Scholar] [PubMed]
- Kroeling, P.; Gross, A.; Goldsmith, C.H.; Burnie, S.J.; Haines, T.; Graham, N.; Brant, A. Electrotherapy for neck pain. Cochrane Database Syst. Rev. 2013, 8, CD004251. [Google Scholar] [CrossRef]
- Osiri, M.; Welch, V.; Brosseau, L.; Shea, B.; McGowan, J.; Tugwell, P.; Wells, G. Transcutaneous electrical nerve stimulation for knee osteoarthritis. Cochrane Database Syst. Rev. 2000, 4, CD002823. [Google Scholar]
- Ferronato, L.; Cunha, H.M.; Machado, P.M.; dos Santos de Souza, G.; Limana, M.D.; Carelli Pereira de Avelar, N. Phisical modalities on the functional performance in knee osteoarthritis: A sytematic review. Fisioter. Mov. 2017, 30, 605–621. [Google Scholar] [CrossRef][Green Version]
- National Institute for Health and Care Excellence. Osteoarthritis: Care and Management. Available online: http://nice.org.uk/guidance/cg177 (accessed on 29 August 2019).
- Brosseau, L.; Yonge, K.; Marchand, S.; Robinson, V.; Osiri, M.; Wells, G.; Tugwell, P. Efficacy of transcutaneous electrical nerve stimulation for osteoarthritis of the lower extremities: A meta-analysis. Phys. Rev. 2004, 9, 213–233. [Google Scholar] [CrossRef]
- Puett, D.; Griffin, M. Published trials of nonmedicinal and noninvasive therapies for hip and knee osteoarthritis. Ann. Intern. Med. 1994, 121, 133–140. [Google Scholar] [CrossRef]
- Terracina, S.; Robba, C.; Prete, A.; Sergi, P.G.; Bilotta, F. Prevention and Treatment of Postoperative Pain after Lumbar Spine Procedures: A Systematic Review. Pain Pr. 2018, 18, 925–945. [Google Scholar] [CrossRef]
- Yue, C.; Zhang, X.; Zhu, Y.; Jia, Y.; Wang, H.; Liu, Y. Systematic Review of Three Electrical Stimulation Techniques for Rehabilitation After Total Knee Arthroplasty. J. Arthroplast. 2018, 33, 2330–2337. [Google Scholar] [CrossRef]
- Kerai, S.; Saxena, K.N.; Taneja, B.; Sehrawat, L. Role of transcutaneous electrical nerve stimulation in post-operative analgesia. Indian J. Anaesth. 2014, 58, 388–393. [Google Scholar] [CrossRef]
- Caley, C. The effects of transcutaeous electrical nerve stimulation (TENS) in postoperative cardiothoracic pain: A systematic review. J. Physiother. Pain Assoc. 2012, 6–10. [Google Scholar]
- Freynet, A.; Falcoz, P.E. Is transcutaneous electrical nerve stimulation effective in relieving postoperative pain after thoracotomy? Interact. Cardiovasc. Thorac. Surg. 2010, 10, 283–288. [Google Scholar] [CrossRef]
- Sabino, G.S.; de Souza, M.V.S.; de Resende, M.A. Transcutaneous electrical nerve stimulation in thoracic or abdominal postoperative conditions. Fisioter. Mov. 2006, 19, 59–71. [Google Scholar]
- Carroll, D.; Moore, R.A.; Tramer, M.R.; McQuay, H.J. Transcutaneous electrical nerve stimulation does not relieve labor pain: Updated systematic review. Contemp. Rev. Obs. Gynaecol. 1997, 9, 195–205. [Google Scholar]
- National Institute for Health and Clinical Excellence. NICE Clinical Guideline 55 Intrapartum Care: Care of Healthy Women and Their Babies during Childbirth; National Institute for Health and Care Excellence: London, UK, 2007; pp. 1–65. [Google Scholar]
- Angelo, P.H.M.; Ribeiro, K.C.L.; Lins, L.G.; de Holanda Araújo Rosendo, A.M.P.; de Sousa, V.P.S.; Micussi, M.T.A.B.C. Recursos não farmacológicos: Atuação da fisioterapia no trabalho de parto, uma revisão sistemática. Fisioter. Bras. 2016, 17, 285–292. [Google Scholar] [CrossRef]
- Liddle, S.D.; Pennick, V. Interventions for preventing and treating low-back and pelvic pain during pregnancy. Cochrane Database Syst. Rev. 2015, 9, CD001139. [Google Scholar] [CrossRef] [PubMed]
- Keskin, E.A.; Onur, O.; Keskin, H.L.; Gumus, I.I.; Kafali, H.; Turhan, N. Transcutaneous electrical nerve stimulation improves low back pain during pregnancy. Gynecol. Obs. Investig. 2012, 74, 76–83. [Google Scholar] [CrossRef] [PubMed]
- Mafetoni, R.R.; Kakuda Shimo, A.K. Non-Pharmacological Methods of Pain Relief during Labor: Integrative review. Rev. Min. Enferm. 2014, 18, 513–520. [Google Scholar] [CrossRef][Green Version]
- Mello, L.F.; Nobrega, L.F.; Lemos, A. Transcutaneous electrical stimulation for pain relief during labor: A systematic review and meta-analysis. Rev. Bras. Fisioter. 2011, 15, 175–184. [Google Scholar] [CrossRef]
- Simkin, P.; Bolding, A. Update on nonpharmacologic approaches to relieve labor pain and prevent suffering. J. Midwifery Womens Health 2004, 49, 489–504. [Google Scholar] [CrossRef]
- Carroll, D.; Tramer, M.; McQuay, H.; Nye, B.; Moore, A. Transcutaneous electrical nerve stimulation in labour pain: A systematic review. Br. J. Obs. Gynaecol. 1997, 104, 169–175. [Google Scholar] [CrossRef]
- Proctor, M.; Farquhar, C.; Stones, W.; He, L.; Zhu, X.; Brown, J. Transcutaneous electrical nerve stimulation for primary dysmenorrhoea. Cochrane Database Syst. Rev. 2002, 1, CD002123. [Google Scholar] [CrossRef]
- Franco, J.V.A.; Turk, T.; Jung, J.H.; Xiao, Y.T.; Iakhno, S.; Garrote, V.; Vietto, V. Non-pharmacological interventions for treating chronic prostatitis/chronic pelvic pain syndrome. Cochrane Database Syst. Rev. 2018, 5, CD012551. [Google Scholar] [CrossRef]
- Megia Garcia, A.; Serrano-Munoz, D.; Bravo-Esteban, E.; Ando Lafuente, S.; Avendano-Coy, J.; Gomez-Soriano, J. Analgesic effects of transcutaneous electrical nerve stimulation (TENS) in patients with fibromyalgia: A systematic review. Aten. Prim. 2019, 51, 406–415. [Google Scholar] [CrossRef]
- Johnson, M.I.; Claydon, L.S.; Herbison, G.P.; Jones, G.; Paley, C.A. Transcutaneous electrical nerve stimulation (TENS) for fibromyalgia in adults. Cochrane Database Syst. Rev. 2017, 10, CD012172. [Google Scholar] [CrossRef]
- National Institute for Health and Care Excellence. Chronic Pain (Primary and Secondary) in over 16s: Assessment of All Chronic Pain and Management of Chronic Primary Pain (NG193); National Institute for Health and Care Excellence: London, UK, 2021; pp. 1–36. [Google Scholar]
- Cheong, Y.C.; Smotra, G.; Williams, A. Non-surgical interventions for the management of chronic pelvic pain. Cochrane Database Syst. Rev. 2014, 3, CD008797. [Google Scholar] [CrossRef] [PubMed]
- Cohen, J.M.; Fagin, A.P.; Hariton, E.; Niska, J.R.; Pierce, M.W.; Kuriyama, A.; Whelan, J.S.; Jackson, J.L.; Dimitrakoff, J.D. Therapeutic intervention for chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS): A systematic review and meta-analysis. PLoS ONE 2012, 7, e41941. [Google Scholar] [CrossRef] [PubMed]
- Igwea, S.E.; Tabansi-Ochuogu, C.S.; Abaraogu, U.O. TENS and heat therapy for pain relief and quality of life improvement in individuals with primary dysmenorrhea: A systematic review. Complement. Clin. Pr. 2016, 24, 86–91. [Google Scholar] [CrossRef] [PubMed]
- Kannan, P.; Claydon, L.S. Some physiotherapy treatments may relieve menstrual pain in women with primary dysmenorrhea: A systematic review. J. Physiother. 2014, 60, 13–21. [Google Scholar] [CrossRef] [PubMed]
- Honda, Y.; Sakamoto, J.; Hamaue, Y.; Kataoka, H.; Kondo, Y.; Sasabe, R.; Goto, K.; Fukushima, T.; Oga, S.; Sasaki, R.; et al. Effects of Physical-Agent Pain Relief Modalities for Fibromyalgia Patients: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Pain Res. Manag. 2018, 2018, 2930632. [Google Scholar] [CrossRef]
- Ibanez-Vera, A.J.; Garcia-Romero, J.C.; Alvero-Cruz, J.R. Fisioterapia pasiva para el tratamiento del sindrome de fibromialgia. Una revision sistematica (Passive physical therapy for the treatment of fibromyalgia syndrome. A systematic review). Fisioterapia 2017, 39, 216–222. [Google Scholar] [CrossRef]
- Ricci, N.A.; Dias, C.N.; Driusso, P. The use of electrothermal and phototherapeutic methods for the treatment of fibromyalgia syndrome: A systematic review. Rev. Bras. Fisioter. 2010, 14, 1–9. [Google Scholar] [CrossRef]
- Page, M.J.; Green, S.; McBain, B.; Surace, S.J.; Deitch, J.; Lyttle, N.; Mrocki, M.A.; Buchbinder, R. Manual therapy and exercise for rotator cuff disease. Cochrane Database Syst. Rev. 2016, 6, CD012224. [Google Scholar] [CrossRef]
- Wu, X.; Chung, V.C.; Hui, E.P.; Ziea, E.T.; Ng, B.F.; Ho, R.S.; Tsoi, K.K.; Wong, S.Y.; Wu, J.C. Effectiveness of acupuncture and related therapies for palliative care of cancer: Overview of systematic reviews. Sci. Rep. 2015, 5, 16776. [Google Scholar] [CrossRef]
- Bao, Y.J.; Kong, X.Y.; Yang, L.P.; Liu, R.; Shi, Z.; Li, W.D.; Hua, B.J.; Hou, W. Complementary and Alternative Medicine for Cancer Pain: An Overview of Systematic Reviews. Evid. Based Complement. Altern. Med. 2014, 2014, 170396. [Google Scholar] [CrossRef]
- Hurlow, A.; Bennett, M.I.; Robb, K.A.; Johnson, M.I.; Simpson, K.H.; Oxberry, S.G. Transcutaneous electric nerve stimulation (TENS) for cancer pain in adults. Cochrane Database Syst. Rev. 2012, 3, CD006276. [Google Scholar] [CrossRef]
- Zeng, H.; Pacheco-Barrios, K.; Cao, Y.; Li, Y.; Zhang, J.; Yang, C.; Fregni, F. Non-invasive neuromodulation effects on painful diabetic peripheral neuropathy: A systematic review and meta-analysis. Sci. Rep. 2020, 10, 19184. [Google Scholar] [CrossRef]
- Desmeules, F.; Boudreault, J.; Roy, J.S.; Dionne, C.E.; Fremont, P.; MacDermid, J.C. Efficacy of transcutaneous electrical nerve stimulation for rotator cuff tendinopathy: A systematic review. Physiotherapy 2016, 102, 41–49. [Google Scholar] [CrossRef] [PubMed]
- Chen, C.-C.; Chuang, Y.-F.; Huang, A.C.-W.; Chen, C.-K.; Chang, Y.-J. The antalgic effects of non-invasive physical modalities on central post-stroke pain: A systematic review. J. Phys. Sci. 2016, 28, 1369–1373. [Google Scholar] [CrossRef] [PubMed]
- Harvey, L.A.; Glinsky, J.V.; Bowden, J.L. The effectiveness of 22 commonly administered physiotherapy interventions for people with spinal cord injury: A systematic review. Spinal Cord 2016, 54, 914–923. [Google Scholar] [CrossRef] [PubMed]
- Boldt, I.; Eriks-Hoogland, I.; Brinkhof, M.W.; de Bie, R.; Joggi, D.; von Elm, E. Non-pharmacological interventions for chronic pain in people with spinal cord injury. Cochrane Database Syst. Rev. 2014, 11, CD009177. [Google Scholar] [CrossRef] [PubMed]
- Hawk, C.; Minkalis, A.L.; Khorsan, R.; Daniels, C.J.; Homack, D.; Gliedt, J.A.; Hartman, J.A.; Bhalerao, S. Systematic Review of Nondrug, Nonsurgical Treatment of Shoulder Conditions. J. Manip. Physiol. 2017, 40, 293–319. [Google Scholar] [CrossRef] [PubMed]
- Haik, M.N.; Alburquerque-Sendin, F.; Moreira, R.F.; Pires, E.D.; Camargo, P.R. Effectiveness of physical therapy treatment of clearly defined subacromial pain: A systematic review of randomised controlled trials. Br. J. Sports Med. 2016, 50, 1124–1134. [Google Scholar] [CrossRef]
- Page, M.J.; Green, S.; Mrocki, M.A.; Surace, S.J.; Deitch, J.; McBain, B.; Lyttle, N.; Buchbinder, R. Electrotherapy modalities for rotator cuff disease. Cochrane Database Syst. Rev. 2016, 6, CD012225. [Google Scholar] [CrossRef]
- Page, M.J.; Green, S.; Kramer, S.; Johnston, R.V.; McBain, B.; Buchbinder, R. Electrotherapy modalities for adhesive capsulitis (frozen shoulder). Cochrane Database Syst. Rev. 2014, 10, CD011324. [Google Scholar] [CrossRef]
- Johansson, K.; Oberg, B.; Adolfsson, L.; Foldevi, M. A combination of systematic review and clinicians’ beliefs in interventions for subacromial pain. Br. J. Gen. Pr. 2002, 52, 145–152. [Google Scholar]
- Hökkä, M.; Kaakinen, P.; Pölkki, T. A systematic review: Non-pharmacological interventions in treating pain in patients with advanced cancer. J. Adv. Nurs. 2012, 68, 1954–1969. [Google Scholar] [CrossRef]
- Robb, K.A.; Bennett, M.I.; Johnson, M.I.; Simpson, K.J.; Oxberry, S.G. Transcutaneous electric nerve stimulation (TENS) for cancer pain in adults. Cochrane Database Syst. Rev. 2008, 3, CD006276. [Google Scholar]
- Pan, C.X.; Morrison, R.S.; Ness, J.; Fugh-Berman, A.; Leipzig, R.M. Complementary and alternative medicine in the management of pain, dyspnea, and nausea and vomiting near the end of life. A systematic review. J. Pain Symptom Manag. 2000, 20, 374–387. [Google Scholar] [CrossRef]
- Pieber, K.; Herceg, M.; Paternostro-Sluga, T. Electrotherapy for the treatment of painful diabetic peripheral neuropathy: A review. J. Rehabil. Med. 2010, 42, 289–295. [Google Scholar] [CrossRef]
- Dion, S.; Wong, J.J.; Cote, P.; Yu, H.; Sutton, D.; Randhawa, K.; Southerst, D.; Varatharajan, S.; Stern, P.J.; Nordin, M.; et al. Are passive physical modalities effective for the management of common soft tissue injuries of the elbow? A systematic review by the Ontario Protocol for Traffic Injury Management (OPTIMa) collaboration. Clin. J. Pain 2017, 33, 71–86. [Google Scholar] [CrossRef]
- Wu, Y.-C.; Tsai, W.-C.; Tu, Y.-K.; Yu, T.-Y. Comparative Effectiveness of Nonoperative Treatments for Chronic Calcific Tendinitis of the Shoulder: A Systematic Review and Network Meta-Analysis of Randomized Controlled Trials. Arch. Phys. Med. Rehabil. 2017, 98, 1678–1692.e6. [Google Scholar] [CrossRef]
- Dingemanse, R.; Randsdorp, M.; Koes, B.W.; Huisstede, B.M. Evidence for the effectiveness of electrophysical modalities for treatment of medial and lateral epicondylitis: A systematic review. Br. J. Sports Med. 2014, 48, 957–965. [Google Scholar] [CrossRef]
- Ramos-Valero, L.; Meseguer-Henarejos, A.B. Physiotherapy treatments for patients with shoulder pain after stroke. A systematic review. Fisioterapia 2013, 35, 214–223. [Google Scholar] [CrossRef]
- Mehta, S.; Orenczuk, K.; McIntyre, A.; Willems, G.; Wolfe, D.L.; Hsieh, J.T.C.; Short, C.; Loh, E.; Teasell, R.W. Neuropathic Pain Post Spinal Cord Injury Part 1: Systematic Review of Physical and Behavioral Treatment. Top. Spinal Cord Inj. Rehabil. 2013, 19, 61–77. [Google Scholar] [CrossRef]
- Fattal, C.; Kong, A.S.D.; Gilbert, C.; Ventura, M.; Albert, T. What is the efficacy of physical therapeutics for treating neuropathic pain in spinal cord injury patients? Ann. Phys. Rehabil. Med. 2009, 52, 149–166. [Google Scholar] [CrossRef][Green Version]
- Kwan, I.; Wang, R.; Pearce, E.; Bhattacharya, S. Pain relief for women undergoing oocyte retrieval for assisted reproduction. Cochrane Database Syst. Rev. 2018, 5, CD004829. [Google Scholar] [CrossRef]
- Mujezinovic, F.; Alfirevic, Z. Analgesia for amniocentesis or chorionic villus sampling. Cochrane Database Syst. Rev. 2011, 11, CD008580. [Google Scholar] [CrossRef] [PubMed]
- Ngee-Ming, G.; Tamsin, D.; Rai, B.P.; Somani, B.K. Complementary approaches to decreasing discomfort during shockwave lithotripsy (SWL). Urolithiasis 2014, 42, 189–193. [Google Scholar] [CrossRef]
- Amatya, B.; Young, J.; Khan, F. Non-pharmacological interventions for chronic pain in multiple sclerosis. Cochrane Database Syst. Rev. 2018, 12, CD012622. [Google Scholar] [CrossRef] [PubMed]
- Jawahar, R.; Oh, U.; Yang, S.; Lapane, K.L. Alternative approach: A systematic review of non-pharmacological non-spastic and non-trigeminal pain management in multiple sclerosis. Eur. J. Phys. Rehabil. Med. 2014, 50, 567–577. [Google Scholar] [PubMed]
- Al-Smadi, J.; Warke, K.; Wilson, I.; Cramp, A.; Noble, G.; Walsh, D.; Lowe-Strong, A. A pilot investigation of the hypoalgesic effects of transcutaneous electrical nerve stimulation upon low back pain in people with multiple sclerosis. Clin. Rehabil. 2003, 17, 742–749. [Google Scholar] [CrossRef]
- Warke, K.; Al-Smadi, J.; Baxter, G.D.; Walsh, D.M.; Lowe-Strong, A.S. A double blind, placebo controlled, randomised, clinical trial investigating the efficacy of transcutaneous electrical nerve stimulation for low back pain in a multiple sclerosis population. Mult. Scler. 2004, 10, S107. [Google Scholar]
- Kwan, I.; Bhattacharya, S.; Knox, F.; McNeil, A. Pain relief for women undergoing oocyte retrieval for assisted reproduction. Cochrane Database Syst. Rev. 2013, 1, CD004829. [Google Scholar] [CrossRef]
- Fleming, P.S.; Strydom, H.; Katsaros, C.; MacDonald, L.C.I.; Curatolo, M.; Fudalej, P.; Pandis, N. Non-pharmacological interventions for alleviating pain during orthodontic treatment. Cochrane Database Syst. Rev. 2016, 12, CD010263. [Google Scholar] [CrossRef]
- Pittler, M.H.; Ernst, E. Complementary therapies for neuropathic and neuralgic pain: Systematic review. Clin. J. Pain 2008, 24, 731–733. [Google Scholar] [CrossRef]
- Amatya, B.; Khan, F.; La Mantia, L.; Demetrios, M.; Wade, D.T. Non pharmacological interventions for spasticity in multiple sclerosis. Cochrane Database Syst. Rev. 2013, 2, CD009974. [Google Scholar] [CrossRef]
- Mills, P.B.; Dossa, F. Transcutaneous Electrical Nerve Stimulation for Management of Limb Spasticity: A Systematic Review. Am. J. Phys. Med. Rehabil. 2016, 95, 309–318. [Google Scholar] [CrossRef]
- Fernandez-Tenorio, E.; Serrano-Munoz, D.; Avendano-Coy, J.; Gomez-Soriano, J. Transcutaneous electrical nerve stimulation for spasticity: A systematic review. Neurologia 2019, 34, 451–460. [Google Scholar] [CrossRef] [PubMed]
- Synnot, A.; Chau, M.; Pitt, V.; O’Connor, D.; Gruen, R.L.; Wasiak, J.; Clavisi, O.; Pattuwage, L.; Phillips, K. Interventions for managing skeletal muscle spasticity following traumatic brain injury. Cochrane Database Syst. Rev. 2017, 11, CD008929. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.I.; Mulvey, M.R.; Bagnall, A.M. Transcutaneous electrical nerve stimulation (TENS) for phantom pain and stump pain following amputation in adults. Cochrane Database Syst. Rev. 2015, 8, CD007264. [Google Scholar] [CrossRef] [PubMed]
- Ottawa, P. Ottawa Panel Evidence-Based Clinical Practice Guidelines for Electrotherapy and Thermotherapy Interventions in the Management of Rheumatoid Arthritis in Adults. Phys. Ther. 2004, 84, 1016–1043. [Google Scholar]
- Brosseau, L.; Judd, M.G.; Marchand, S.; Robinson, V.A.; Tugwell, P.; Wells, G.; Yonge, K. Transcutaneous electrical nerve stimulation (TENS) for the treatment of rheumatoid arthritis in the hand. Cochrane Database Syst. Rev. 2003, 2, CD004377. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Health and Care Excellence. Rheumatoid Arthritis in Adults. Available online: www.nice.org.uk/NG100 (accessed on 17 October 2019).
- Tao, H.; Wang, T.; Dong, X.; Guo, Q.; Xu, H.; Wan, Q. Effectiveness of transcutaneous electrical nerve stimulation for the treatment of migraine: A meta-analysis of randomized controlled trials. J. Headache Pain 2018, 19, 42. [Google Scholar] [CrossRef]
- Smart, K.M.; Wand, B.M.; O’Connell, N.E. Physiotherapy for pain and disability in adults with complex regional pain syndrome (CRPS) types I and II. Cochrane Database Syst. Rev. 2016, 2, CD010853. [Google Scholar] [CrossRef]
- Hu, X.; Trevelyan, E.; Yang, G.; Lee, M.S.; Lorenc, A.; Liu, J.; Robinson, N. The effectiveness of acupuncture/TENS for phantom limb syndrome. I: A systematic review of controlled clinical trials. Eur. J. Integr. Med. 2014, 6, 355–364. [Google Scholar] [CrossRef]
- Halbert, J.; Crotty, M.; Cameron, I.D. Evidence for the optimal management of acute and chronic phantom pain: A systematic review. Clin. J. Pain 2002, 18, 84–92. [Google Scholar] [CrossRef]
- Bronfort, G.; Nilsson, N.; Haas, M.; Evans, R.; Goldsmith, C.H.; Assendelft, W.J.; Bouter, L.M. Non-invasive physical treatments for chronic/recurrent headache. Cochrane Database Syst. Rev. 2004, 3, CD001878. [Google Scholar]
- Huisstede, B.M.A.; Hoogvliet, P.; Franke, T.P.C.; Randsdorp, M.S.; Koes, B.W. Carpal tunnel syndrome: Effectiveness of physical therapy and electrophysical modalities. An updated systematic review of randomized controlled trials. Arch. Phys. Med. Rehabil. 2018, 99, 1623–1634.e23. [Google Scholar] [CrossRef] [PubMed]
- Peters, S.; Page, M.J.; Coppieters, M.W.; Ross, M.; Johnston, V. Rehabilitation following carpal tunnel release. Cochrane Database Syst. Rev. 2016, 2, CD004158. [Google Scholar] [CrossRef] [PubMed]
- Perillo, S.; Boyle, M.J. Pre-hospital femoral neck fracture management: A review of the literature. J. Paramed. Pr. 2013, 5, 99–103. [Google Scholar] [CrossRef]
- Deussen, A.R.; Ashwood, P.; Martis, R.; Stewart, F.; Grzeskowiak, L.E. Relief of pain due to uterine cramping/involution after birth. Cochrane Database Syst. Rev. 2020, 10, CD004908. [Google Scholar] [CrossRef] [PubMed]
- Deussen, A.R.; Ashwood, P.; Martis, R. Analgesia for relief of pain due to uterine cramping/involution after birth. Cochrane Database Syst. Rev. 2011, 5, CD004908. [Google Scholar] [CrossRef] [PubMed]
- Pal, S.; Dixit, R.; Moe, S.; Godinho, M.A.; Abas, A.B.; Ballas, S.K.; Ram, S.; Yousuf, U.A.M. Transcutaneous electrical nerve stimulation (TENS) for pain management in sickle cell disease. Cochrane Database Syst. Rev. 2020, 3, CD012762. [Google Scholar] [CrossRef]
- De Andres, J.; Sanchis-Lopez, N.; Asensio-Samper, J.M.; Fabregat-Cid, G.; Villanueva-Perez, V.L.; Monsalve Dolz, V.; Minguez, A. Vulvodynia--An Evidence-Based Literature Review and Proposed Treatment Algorithm. Pain Pr. 2016, 16, 204–236. [Google Scholar] [CrossRef]
- Liao, C.D.; Tsauo, J.Y.; Liou, T.H.; Chen, H.C.; Rau, C.L. Efficacy of Noninvasive Stellate Ganglion Blockade Performed Using Physical Agent Modalities in Patients with Sympathetic Hyperactivity-Associated Disorders: A Systematic Review and Meta-Analysis. PLoS ONE 2016, 11, e0167476. [Google Scholar] [CrossRef]
- Oor, J.E.; Unlu, C.; Hazebroek, E.J. A systematic review of the treatment for abdominal cutaneous nerve entrapment syndrome. Am. J. Surg. 2016, 212, 165–174. [Google Scholar] [CrossRef]
- Mansilla, J.R.; Sánchez, B.G.; de Toro Garcíac, A.; López-Arza, M.V.G. Eficacia de la estimulación eléctrica transcutánea en la neuralgia del trigémino. Rehabilitacion 2016, 50, 81–86. [Google Scholar] [CrossRef]
- Kovacs, F.M.; Urrutia, G.; Alarcon, J.D. Surgery versus conservative treatment for symptomatic lumbar spinal stenosis: A systematic review of randomized controlled trials. Spine 2011, 36, E1335–E1351. [Google Scholar] [CrossRef] [PubMed]
- McNeely, M.L.; Armijo Olivo, S.; Magee, D.J. A systematic review of the effectiveness of physical therapy interventions for temporomandibular disorders. Phys. Ther. 2006, 86, 710–725. [Google Scholar] [CrossRef]
- Dailey, D.L.; Vance, C.G.T.; Rakel, B.A.; Zimmerman, M.B.; Embree, J.; Merriwether, E.N.; Geasland, K.M.; Chimenti, R.; Williams, J.M.; Golchha, M.; et al. Transcutaneous Electrical Nerve Stimulation Reduces Movement-Evoked Pain and Fatigue: A Randomized, Controlled Trial. Arthritis Rheumatol. 2020, 72, 824–836. [Google Scholar] [CrossRef]
- Atamaz, F.C.; Durmaz, B.; Baydar, M.; Demircioglu, O.Y.; Iyiyapici, A.; Kuran, B.; Oncel, S.; Sendur, O.F. Comparison of the efficacy of transcutaneous electrical nerve stimulation, interferential currents, and shortwave diathermy in knee osteoarthritis: A double-blind, randomized, controlled, multicenter study. Arch. Phys. Med. Rehabil. 2012, 93, 748–756. [Google Scholar] [CrossRef] [PubMed]
- Palmer, S.; Domaille, M.; Cramp, F.; Walsh, N.; Pollock, J.; Kirwan, J.; Johnson, M.I. Transcutaneous electrical nerve stimulation as an adjunct to education and exercise for knee osteoarthritis: A randomised controlled trial. Arthritis Care Res. 2013, 66, 387–394. [Google Scholar] [CrossRef] [PubMed]
- Rakel, B.; Frantz, R. Effectiveness of transcutaneous electrical nerve stimulation on postoperative pain with movement. J. Pain 2003, 4, 455–464. [Google Scholar] [CrossRef]
- Baez-Suarez, A.; Martin-Castillo, E.; Garcia-Andujar, J.; Garcia-Hernandez, J.A.; Quintana-Montesdeoca, M.P.; Loro-Ferrer, J.F. Evaluation of different doses of transcutaneous nerve stimulation for pain relief during labour: A randomized controlled trial. Trials 2018, 19, 652. [Google Scholar] [CrossRef]
- Tsen, L.C.; Thomas, J.; Segal, S.; Datta, S.; Bader, A.M. Transcutaneous electrical nerve stimulation does not augment epidural labor analgesia. J. Clin. Anesth. 2001, 13, 571–575. [Google Scholar] [CrossRef]
- Thomas, I.L.; Tyle, V.; Webster, J.; Neilson, A. An evaluation of transcutaneous electrical nerve stimulation for pain relief in labour. Aust. N. Z. J. Obs. Gynaecol. 1988, 28, 182–189. [Google Scholar] [CrossRef] [PubMed]
- Bai, H.Y.; Bai, H.Y.; Yang, Z.Q. Effect of transcutaneous electrical nerve stimulation therapy for the treatment of primary dysmenorrheal. Medicine 2017, 96, e7959. [Google Scholar] [CrossRef] [PubMed]
- Başkurt, Z.; Başkurt, F.; Özcan, A.; Yilmaz, Ö. The immediate effects of heat and TENS on pressure pain threshold and pain intensity in patients with Stage I shoulder impingement syndrome. Pain Clin. 2006, 18, 81–85. [Google Scholar] [CrossRef]
- Bulut, M.; Özcan, A.; Çakan, T.; Mektas, M.; Çulha, C. The Comparison of Effectiveness of TENS and Placebo TENS in Peripheral Neuropathic Pain in Patients with Type II Diabetes Mellitus. Turk. Klin. J. Med. Sci. 2011, 31, 913–918. [Google Scholar] [CrossRef]
- Amer-Cuenca, J.J.; Goicoechea, C.; Girona-López, A.; Andreu-Plaza, J.L.; Palao-Román, R.; Martínez-Santa, G.; Lisón, J.F. Pain relief by applying transcutaneous electrical nerve stimulation (TENS) during unsedated colonoscopy: A randomized double-blind placebo-controlled trial. Eur. J. Pain 2011, 15, 29–35. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.I. Resolving Long-Standing Uncertainty about the Clinical Efficacy of Transcutaneous Electrical Nerve Stimulation (TENS) to Relieve Pain: A Comprehensive Review of Factors Influencing Outcome. Medicina 2021, 57, 378. [Google Scholar] [CrossRef]
- Nnoaham, K.E.; Kumbang, J. WITHDRAWN: Transcutaneous electrical nerve stimulation (TENS) for chronic pain. Cochrane Database Syst. Rev. 2014, 7, CD003222. [Google Scholar] [CrossRef]
- Treede, R.D.; Rief, W.; Barke, A.; Aziz, Q.; Bennett, M.I.; Benoliel, R.; Cohen, M.; Evers, S.; Finnerup, N.B.; First, M.B.; et al. A classification of chronic pain for ICD-11. Pain 2015, 156, 1003–1007. [Google Scholar] [CrossRef]
- Smith, B.H.; Fors, E.A.; Korwisi, B.; Barke, A.; Cameron, P.; Colvin, L.; Richardson, C.; Rief, W.; Treede, R.D.; The IASP Taskforce for the Classification of Chronic Pain. The IASP classification of chronic pain for ICD-11: Applicability in primary care. Pain 2019, 160, 83–87. [Google Scholar] [CrossRef]
- Ioannidis, J.P. The Mass Production of Redundant, Misleading, and Conflicted Systematic Reviews and Meta-analyses. Milbank Q. 2016, 94, 485–514. [Google Scholar] [CrossRef]
- Bennett, M.I.; Hughes, N.; Johnson, M.I. Methodological quality in randomised controlled trials of transcutaneous electric nerve stimulation for pain: Low fidelity may explain negative findings. Pain 2011, 152, 1226–1232. [Google Scholar] [CrossRef]
- Gladwell, P.W.; Badlan, K.; Cramp, F.; Palmer, S. Direct and Indirect Benefits Reported by Users of Transcutaneous Electrical Nerve Stimulation for Chronic Musculoskeletal Pain: Qualitative Exploration Using Patient Interviews. Phys. Ther. 2015, 95, 1518–1528. [Google Scholar] [CrossRef]
- Gladwell, P.W.; Cramp, F.; Palmer, S. Matching the perceived benefits of Transcutaneous Electrical Nerve Stimulation (TENS) for chronic musculoskeletal pain against Patient Reported Outcome Measures using the International Classification of Functioning, Disability and Health (ICF). Physiotherapy 2020, 106, 128–135. [Google Scholar] [CrossRef]
- Gladwell, P.W.; Badlan, K.; Cramp, F.; Palmer, S. Problems, Solutions, and Strategies Reported by Users of Transcutaneous Electrical Nerve Stimulation for Chronic Musculoskeletal Pain: Qualitative Exploration Using Patient Interviews. Phys. Ther. 2016, 96, 1039–1048. [Google Scholar] [CrossRef] [PubMed]
- National Institute for Health and Care Excellence. Low Back Pain and Sciatica in over 16s: Assessment and Management; Clinical guideline [NG59]; National Institute for Health and Care Excellence: London, UK, 2016; pp. 1–18. [Google Scholar]
- Almeida, T.; Figueiredo, F.; Barbosa Filho, V.C.; de Abreu, L.C.; Fonseca, F.L.A.; Adami, F. Effects of transcutaneous electrical nerve stimulation (TENS) on proinflammatory cytokines: Protocol for systematic review. Syst. Rev. 2017, 6, 139. [Google Scholar] [CrossRef] [PubMed]
- Anim-Somuah, M.; Smyth, R.M.D.; Cyna, A.M.; Cuthbert, A. Epidural versus non-epidural or no analgesia for pain management in labour. Cochrane Database Syst. Rev. 2018. [Google Scholar] [CrossRef]
- Arendt, K.W.; Tessmer-Tuck, J.A. Nonpharmacologic labor analgesia. Clin. Perinatol. 2013, 40, 351–371. [Google Scholar] [CrossRef] [PubMed]
- Barkatsa, V.; Iliadis, C.; Moraitis, V.; Syrmos, N.; Tzagarakis, M.; Tsipras, K. Physiotherapy interventions for the management of whiplash injuries. Bone 2011, 48, S271. [Google Scholar] [CrossRef]
- Binder, A.; Baron, R. Utility of transcutaneous electrical nerve stimulation in neurologic pain disorders. Neurology 2010, 74, 104–105. [Google Scholar] [CrossRef] [PubMed]
- Bjordal, J.M.; Baxter, D.; Leal, E., Jr.; Cheing, G.; Laakso, L. Evidence based use of electrophysical agents for managing musculoskeletal pain. Physiotherapy 2015, 101, eS8–eS9. [Google Scholar] [CrossRef][Green Version]
- Briones-Areán, Y.; Soto-González, M. Effectiveness of physiotherapy in shoulder impingement syndrome. Fisioterapia 2014, 36, 187–196. [Google Scholar] [CrossRef]
- Brosseau, L.; Yonge, K.; Marchand, S.; Robinson, V.; Wells, G.; Tugwell, P. Efficacy of transcutaneous electrical nerve stimulation (TENS) for rheumatoid arthritis: A systematic review. Phys. Ther. Rev. 2002, 7, 199–208. [Google Scholar] [CrossRef]
- Cadalso, R.T.; Daugherty, J.; Holmes, C.; Ram, S.; Enciso, R. Efficacy of Electrical Stimulation of the Occipital Nerve in Intractable Primary Headache Disorders: A Systematic Review with Meta-Analyses. J. Oral Facial Pain Headache 2018, 32, 40–52. [Google Scholar] [CrossRef] [PubMed]
- Cameron, M.; Lonergan, E.; Lee, H. Transcutaneous electrical nerve stimulation (TENS) for dementia. Cochrane Database Syst. Rev. 2003, CD004032. [Google Scholar] [CrossRef]
- Campo-Prieto, P.; Rodriguez-Fuentes, G. Effectiveness of mirror therapy in phantom limb pain: A literature review. Neurologia 2018. [Google Scholar] [CrossRef]
- Chan, P.S.L. Postherpetic neuralgia: Review of treatment modalities. Pain Res. Manag. 2000, 5, 69–74. [Google Scholar] [CrossRef]
- Chaparro, L.E.; Furlan, A.D.; Deshpande, A.; Mailis-Gagnon, A.; Atlas, S.; Turk, D.C. Opioids compared to placebo or other treatments for chronic low-back pain. Cochrane Database Syst. Rev. 2013, 8, CD004959. [Google Scholar] [CrossRef]
- Chen, C.; Tabasam, G.; Johnson, M. Does the pulse frequency of Transcutaneous Electrical Nerve Stimulation (TENS) influence hypoalgesia? A systematic review of studies using experimental pain and healthy human participants. Physiotherapy 2008, 94, 11–20. [Google Scholar] [CrossRef]
- Chesterton, L.S.; van der Windt, D.A.; Sim, J.; Lewis, M.; Mallen, C.D.; Mason, E.E.; Warlow, C.; Vohora, K.; Hay, E.M. Transcutaneous electrical nerve stimulation for the management of tennis elbow: A pragmatic randomized controlled trial: The TATE trial (ISRCTN 87141084). BMC Musculoskelet. Disord. 2009, 10, 156. [Google Scholar] [CrossRef]
- Choi, G.-H.; Wieland, L.S.; Lee, H.; Sim, H.; Lee, M.S.; Shin, B.-C. Acupuncture and related interventions for the treatment of symptoms associated with carpal tunnel syndrome. Cochrane Database Syst. Rev. 2018, 12, CD011215. [Google Scholar] [CrossRef]
- Claydon, L.S.; Chesterton, L.S.; Barlas, P.; Sim, J. Dose-specific effects of transcutaneous electrical nerve stimulation (TENS) on experimental pain: A systematic review. Clin. J. Pain 2011, 27, 635–647. [Google Scholar] [CrossRef]
- Claydon, L.S.; Chesterton, L.S.; Sim, J.; Barlas, P. The hypoalgesic efficacy of TENS parameters on experimental pain models in healthy humans: A systematic review. N. Z. J. Physiother. 2008, 36, 84–85. [Google Scholar]
- Dingemanse, R.; Randsdorp, M.; Koes, B.W.; Huisstede, B.M. Evidence for the effectiveness of electrophysical modalities for treatment of medial and lateral epicondylitis: A systematic review. Br. J. Sports Med. 2013, 48, 957–965. [Google Scholar] [CrossRef] [PubMed]
- Doyle, S.; Bennett, S.; Fasoli, S.E.; McKenna, K.T. Interventions for sensory impairment in the upper limb after stroke. Cochrane Database Syst. Rev. 2010. [Google Scholar] [CrossRef]
- Ducic, I.; Felder, J.M., 3rd; Fantus, S.A. A systematic review of peripheral nerve interventional treatments for chronic headaches. Ann. Plast. Surg. 2014, 72, 439–445. [Google Scholar] [CrossRef]
- Eberhart, L.H.; Morin, A.M.; Kranke, P.; Geldner, G.; Wulf, H. Transient neurologic symptoms after spinal anesthesia. A quantitative systematic review (meta-analysis) of randomized controlled studies. Anaesthesist 2002, 51, 539–546. [Google Scholar] [CrossRef] [PubMed]
- Eccleston, C.; Fisher, E.; Thomas, K.H.; Hearn, L.; Derry, S.; Stannard, C.; Knaggs, R.; Moore, R.A. Interventions for the reduction of prescribed opioid use in chronic non-cancer pain. Cochrane Database Syst. Rev. 2017, 11, Cd010323. [Google Scholar] [CrossRef] [PubMed]
- Ely, S. Transcutaneous electrical nerve stimulation (TENS) at acupuncture points for the management of chronic pain: A narrative review. In Proceedings of the 4th European Congress of the European Region of the World Confederation of Physical Therapy (ER-WCPT) Abstracts, Liverpool, UK, 11–12 November 2016. [Google Scholar] [CrossRef]
- Fargas-Babjak, A. Acupuncture, transcutaneous electrical nerve stimulation, and laser therapy in chronic pain. Clin. J. Pain 2001, 17, S105–S113. [Google Scholar] [CrossRef]
- Foletti, A.; Durrer, A.; Buchser, E. Neurostimulation technology for the treatment of chronic pain: A focus on spinal cord stimulation. Expert Rev. Med. Devices 2007, 4, 201–214. [Google Scholar] [CrossRef]
- Freynet, A.; Falcoz, P. Kinésithérapie basée sur les preuves en chirurgie thoracique après résection pulmonaire par thoracotomie: Evidence-based physiotherapy after lung resection via thoracotomy. Kinésithér. Rev. 2011, 11, 34–44. [Google Scholar] [CrossRef]
- Fu, X.; Wang, Y.; Wang, C.; Wu, H.; Li, J.; Li, M.; Ma, Q.; Yang, W. A mixed treatment comparison on efficacy and safety of treatments for spasticity caused by multiple sclerosis: A systematic review and network meta-analysis. Clin. Rehabil. 2018, 32, 713–721. [Google Scholar] [CrossRef] [PubMed]
- Gabler, C.M.; Lepley, A.S.; Uhl, T.L.; Mattacola, C.G. Comparison of Transcutaneous Electrical Nerve Stimulation and Cryotherapy for Increasing Quadriceps Activation in Patients With Knee Pathologies. J. Sport Rehabil. 2016, 25, 294–300. [Google Scholar] [CrossRef][Green Version]
- Gadsby, J.G.; Flowerdew, M.W. Transcutaneous electrical nerve stimulation and acupuncture-like transcutaneous electrical nerve stimulation for chronic low back pain. Cochrane Database Syst. Rev. 2000, CD000210. [Google Scholar]
- Gadsby, J.G.; Flowerdew, M.W. WITHDRAWN: Transcutaneous electrical nerve stimulation and acupuncture-like transcutaneous electrical nerve stimulation for chronic low back pain. Cochrane Database Syst. Rev. 2007, CD000210. [Google Scholar] [CrossRef]
- Gross, A.; Langevin, P.; Burnie, S.J.; Bedard-Brochu, M.S.; Empey, B.; Dugas, E.; Faber-Dobrescu, M.; Andres, C.; Graham, N.; Goldsmith, C.H.; et al. Manipulation and mobilisation for neck pain contrasted against an inactive control or another active treatment (Cochrane review) [with consumer summary]. Cochrane Database Syst. Rev. 2005. [Google Scholar]
- Hall, H.; McIntosh, G. Low back pain (acute). BMJ Clin. Evid. 2008, 2008, 1102. [Google Scholar]
- Handy, J.; Salinas, S.; Blanchard, S.A.; Aitken, M.J. Meta-analysis examining the effectiveness of electrical stimulation in improving functional use of the upper limb in stroke patients. Phys. Occup. Ther. Geriatr. 2003, 21, 67–78. [Google Scholar] [CrossRef]
- Hawker, G.A.; Mian, S.; Bednis, K.; Stanaitis, I. Osteoarthritis year 2010 in review: Non-pharmacologic therapy. Osteoarthr. Cartil. 2011, 19, 366–374. [Google Scholar] [CrossRef]
- Ho, K.W.D.; Przkora, R.; Kumar, S. Sphenopalatine ganglion: Block, radiofrequency ablation and neurostimulation—A systematic review. J. Headache Pain 2017, 18, 118. [Google Scholar] [CrossRef]
- Hoffman, R.M. Review: Transcutaneous electrical nerve stimulation is not effective for chronic low-back pain. ACP J. Club 2001, 135, 9999. [Google Scholar]
- Hu, X.; Trevelyan, E.; Yang, G.; Lee, M.S.; Lorenc, A.; Liu, J.; Robinson, N. The effectiveness of acupuncture or TENS for phantom limb syndrome. II: A narrative review of case studies. Eur. J. Integr. Med. 2014, 6, 365–381. [Google Scholar] [CrossRef]
- Hunsinger, M.; Smith, S.M.; Rothstein, D.; McKeown, A.; Parkhurst, M.; Hertz, S.; Katz, N.P.; Lin, A.H.; McDermott, M.P.; Rappaport, B.A.; et al. Adverse event reporting in nonpharmacologic, noninterventional pain clinical trials: ACTTION systematic review. Pain 2014, 155, 2253–2262. [Google Scholar] [CrossRef]
- Jamtvedt, G.; Dahm, K.T.; Holm, I.; Odegaard-Jensen, J.; Flottorp, S. Choice of treatment modalities was not influenced by pain, severity or co-morbidity in patients with knee osteoarthritis. Physiother. Res. Int. 2010, 15, 16–23. [Google Scholar] [CrossRef] [PubMed]
- Jayasekara, R. Transcutaneous electrical nerve stimulation for acute pain. J. Pain Manag. 2011, 4, 437–438. [Google Scholar]
- Johnson, M.I. Transcutaneous electrical nerve stimulation: Review of effectiveness. Nurs. Stand. 2014, 28, 44–53. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.I. The clinical effectiveness of TENS in pain management. Crit. Rev. Phys. Ther. Rehabil. 2000, 12, 131–149. [Google Scholar] [CrossRef]
- Johnson, M.I. Transcutaneous Electrical Nerve Stimulation (TENS) and TENS-like devices. Do they provide pain relief? Pain Rev. 2001, 8, 121–128. [Google Scholar] [CrossRef]
- Johnson, M.I. Transcutaneous electrical nerve stimulation (TENS) as an adjunct for pain management in perioperative settings: A critical review. Expert Rev. Neurother. 2017, 17, 1013–1027. [Google Scholar] [CrossRef]
- Johnson, M.I.; Bjordal, J.M. Transcutaneous electrical nerve stimulation for the management of painful conditions: Focus on neuropathic pain. Expert Rev. Neurother. 2011, 11, 735–753. [Google Scholar] [CrossRef] [PubMed]
- Jordan, J.L.; Holden, M.A.; Mason, E.E.J.; Foster, N.E. Interventions to improve adherence to exercise for chronic musculoskeletal pain in adults. Cochrane Database Syst. Rev. 2010. [Google Scholar] [CrossRef]
- Kang, J.; Li, N.; Wu, B. Therapeutic methods for knee osteoarthritis: Randomized controlled trial and systemic evaluation. Chin. J. Clin. Rehabil. 2005, 9, 27–30. [Google Scholar]
- Khadilkar, A.; Milne, S.; Brosseau, L.; Wells, G.; Tugwell, P.; Robinson, V.; Shea, B.; Saginur, M. Transcutaneous electrical nerve stimulation for the treatment of chronic low back pain: A systematic review. Spine 2005, 30, 2657–2666. [Google Scholar] [CrossRef] [PubMed]
- Khalil, N.; Nicotra, A.; Rakowicz, W. Treatment for meralgia paraesthetica. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Khan, F.; Amatya, B.; Bensmail, D.; Yelnik, A. Non-pharmacological interventions for spasticity in adults: An overview of systematic reviews. Ann. Phys. Rehabil. Med. 2019, 62, 265–273. [Google Scholar] [CrossRef] [PubMed]
- Kirpalani, D.; Mitra, R. Cervical facet joint dysfunction: A review. Arch. Phys. Med. Rehabil. 2008, 89, 770–774. [Google Scholar] [CrossRef]
- Klomp, T. Inhaled analgesia for pain management in labour. J. Evid. Based Med. 2012, 5, 241. [Google Scholar] [CrossRef]
- Koes, B.W.; Assendelft, W.J.; van der Heijden, G.J.; Bouter, L.M.; Knipschild, P.G. Spinal manipulation and mobilisation for back and neck pain: A blinded review. BMJ 1991, 303, 1298–1303. [Google Scholar] [CrossRef]
- Koes, B.W.; Assendelft, W.J.; van der Heijden, G.J.; Bouter, L.M. Spinal manipulation for low back pain. An updated systematic review of randomized clinical trials. Spine 1996, 21, 2860–2871; discussion 2872–2873. [Google Scholar] [CrossRef]
- Koopman, F.S.; Beelen, A.; Gilhus, N.E.; de Visser, M.; Nollet, F. Treatment for postpolio syndrome. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef]
- Kosseim, M.; Rein, R.; McShane, C. Implementing evidence-based physiotherapy practice for treating children with low back pain: Are we there yet? Pediatr. Phys. Ther. 2008, 20, 179–184. [Google Scholar] [CrossRef]
- Kroeling, P.; Gross, A.; Goldsmith, C.H.; Houghton, P.E. Electrotherapy for neck disorders. Cochrane Database Syst. Rev. 2005. [Google Scholar] [CrossRef]
- Kus, G.; Yeldan, I. Strengthening the quadriceps femoris muscle versus other knee training programs for the treatment of knee osteoarthritis. Rheumatol. Int. 2019, 39, 203–218. [Google Scholar] [CrossRef] [PubMed]
- Lee, S.; Abd-Elsayed, A. Some Non-FDA Approved Uses for Neuromodulation: A Review of the Evidence. Pain Pract. 2016, 16, 935–947. [Google Scholar] [CrossRef] [PubMed]
- Lenza, M.; Buchbinder, R.; Johnston, R.V.; Ferrari, B.A.S.; Faloppa, F. Surgical versus conservative interventions for treating fractures of the middle third of the clavicle. Cochrane Database Syst. Rev. 2019. [Google Scholar] [CrossRef] [PubMed]
- Lin, C.W.C.; Donkers, N.A.J.; Refshauge, K.M.; Beckenkamp, P.R.; Khera, K.; Moseley, A.M. Rehabilitation for ankle fractures in adults. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Lindsley, K.; Nichols, J.J.; Dickersin, K. Non-surgical interventions for acute internal hordeolum. Cochrane Database Syst. Rev. 2017. [Google Scholar] [CrossRef] [PubMed]
- Mahmood, A.; Veluswamy, S.K.; Hombali, A.; Mullick, A.; Manikandan, N.; Solomon, J.M. Effect of Transcutaneous Electrical Nerve Stimulation on Spasticity in Adults With Stroke: A Systematic Review and Meta-analysis. Arch. Phys. Med. Rehabil. 2019, 100, 751–768. [Google Scholar] [CrossRef]
- Marcolino, M.A.Z.; Hauck, M.; Stein, C.; Schardong, J.; Pagnussat, A.S.; Plentz, R.D.M. Effects of transcutaneous electrical nerve stimulation alone or as additional therapy on chronic post-stroke spasticity: Systematic review and meta-analysis of randomized controlled trials. Disabil. Rehabil. 2020, 42, 623–635. [Google Scholar] [CrossRef] [PubMed]
- Martí-Carvajal, A.J.; Peña-Martí, G.E.; Comunián-Carrasco, G.; Martí-Peña, A.J. Interventions for treating painful sickle cell crisis during pregnancy. Cochrane Database Syst. Rev. 2009. [Google Scholar] [CrossRef] [PubMed]
- Miller, J.; Gross, A. Manual therapy and exercise for neck pain: Clinical treatment pocket notes. Physiotherapy 2011, 97, eS1554–eS1555. [Google Scholar] [CrossRef]
- Moisset, X.; Pereira, B.; Ciampi de Andrade, D.; Fontaine, D.; Lanteri-Minet, M.; Mawet, J. Neuromodulation techniques for acute and preventive migraine treatment: A systematic review and meta-analysis of randomized controlled trials. J. Headache Pain 2020, 21, 142. [Google Scholar] [CrossRef]
- Mollon, B.; da Silva, V.; Busse, J.W.; Einhorn, T.A.; Bhandari, M. Electrical stimulation for long-bone fracture-healing: A meta-analysis of randomized controlled trials. J. Bone Jt. Surg. Am. 2008, 90, 2322–2330. [Google Scholar] [CrossRef]
- Monaghan, B.; Caulfield, B.; O’Mathuna, D.P. Surface neuromuscular electrical stimulation for quadriceps strengthening pre and post total knee replacement. Cochrane Database Syst. Rev. 2010, CD007177. [Google Scholar] [CrossRef] [PubMed]
- Muller, A. Apropos the meta-analyses, randomization and postoperative pain relief with transcutaneous nerve stimulation. Ann. Fr. D Anesth. Reanim. 1997, 16, 459–460. [Google Scholar] [CrossRef]
- Mulvey, M.R.; Bagnall, A.; Johnson, M.I.; Marchant, P.R. Transcutaneous electrical nerve stimulation (TENS) for phantom pain and stump pain following amputation in adults. Cochrane Database Syst. Rev. 2010. [Google Scholar]
- Mulvey, M.R.; Radford, H.E.; Fawkner, H.J.; Hirst, L.; Neumann, V.; Johnson, M.I. Transcutaneous electrical nerve stimulation for phantom pain and stump pain in adult amputees. Pain Pract. 2013, 13, 289–296. [Google Scholar] [CrossRef]
- Mulvey, M.R.; Bagnall, A.-M.; Marchant, P.R.; Johnson, M.I. Transcutaneous electrical nerve stimulation (TENS) for phantom pain and stump pain following amputation in adults: An extended analysis of excluded studies from a Cochrane systematic review. Phys. Ther. Rev. 2014, 19, 234–244. [Google Scholar] [CrossRef]
- Munirama, S.; McLeod, G. A systematic review and meta-analysis of ultrasound versus electrical stimulation for peripheral nerve location and blockade. Anaesthesia 2015, 70, 1084–1091. [Google Scholar] [CrossRef]
- Novak, S.; Nemeth, W.C. How clinically relevant is a meta-analysis of electrical nerve stimulation when based on heterogeneous disease states? Pain 2007, 131, 228–229; author reply 229–230. [Google Scholar] [CrossRef]
- O’Connell, N.E.; Wand, B.M.; Marston, L.; Spencer, S.; Desouza, L.H. Non-invasive brain stimulation techniques for chronic pain. Cochrane Database Syst. Rev. 2014, CD008208. [Google Scholar] [CrossRef]
- O’Connell, N.E.; Marston, L.; Spencer, S.; DeSouza, L.H.; Wand, B.M. Non-invasive brain stimulation techniques for chronic pain. Cochrane Database Syst. Rev. 2018. [Google Scholar] [CrossRef] [PubMed]
- O’Gallagher, M.; Banteka, M.; Bunce, C.; Larkin, F.; Tuft, S.; Dahlmann-Noor, A. Systemic treatment for blepharokeratoconjunctivitis in children. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef] [PubMed]
- Pelland, L.; Brosseau, L.; Casimiro, L.; Welch, V.; Tugwell, P.; Wells, G.A. Electrical stimulation for the treatment of rheumatoid arthritis. Cochrane Database Syst. Rev. 2002. [Google Scholar] [CrossRef]
- Poropat, G.; Giljaca, V.; Hauser, G.; Štimac, D. Enteral nutrition formulations for acute pancreatitis. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef]
- Price, C.I.; Pandyan, A.D. Electrical stimulation for preventing and treating post-stroke shoulder pain: A systematic Cochrane review. Clin. Rehabil. 2001, 15, 5–19. [Google Scholar] [CrossRef]
- Proietti Cecchini, A.; Grazzi, L. Emerging therapies for chronic migraine. Curr. Pain Headache Rep. 2014, 18, 408. [Google Scholar] [CrossRef]
- Redgrave, J.; Day, D.; Leung, H.; Laud, P.J.; Ali, A.; Lindert, R.; Majid, A. Safety and tolerability of Transcutaneous Vagus Nerve stimulation in humans; a systematic review. Brain Stimul. 2018, 11, 1225–1238. [Google Scholar] [CrossRef]
- Reed, J.C. Review of acute and chronic pain published studies. J. Altern. Complement. Med. 1996, 2, 129–144; discussion 145–147. [Google Scholar] [CrossRef] [PubMed]
- Renner, R.M.; Jensen, J.T.; Nichols, M.D.; Edelman, A. Pain control in first trimester surgical abortion. Cochrane Database Syst. Rev. 2009. [Google Scholar] [CrossRef]
- Richards, B.L.; Whittle, S.L.; Buchbinder, R. Neuromodulators for pain management in rheumatoid arthritis. Cochrane Database Syst. Rev. 2012. [Google Scholar] [CrossRef]
- Robb, K.; Oxberry, S.G.; Bennett, M.I.; Johnson, M.I.; Simpson, K.H.; Searle, R.D. A Cochrane Systematic Review of Transcutaneous Electrical Nerve Stimulation for Cancer Pain. J. Pain Symptom. Manag. 2009, 37, 746–753. [Google Scholar] [CrossRef] [PubMed]
- Rojahn, R. Transcutaneous Electrostimulation for Osteoarthritis of the Knee. J. Pain Manag. 2011, 4, 447–449. [Google Scholar]
- Rome, K.; Handoll, H.H.G.; Ashford, R.L. Interventions for preventing and treating stress fractures and stress reactions of bone of the lower limbs in young adults. Cochrane Database Syst. Rev. 2005. [Google Scholar] [CrossRef] [PubMed]
- Rosted, P.; Andersen, C. Use of stimulation techniques in pain treatment. Ugeskr. Laeger. 2006, 168, 1982–1986. [Google Scholar]
- Saarto, T.; Wiffen, P.J. Antidepressants for neuropathic pain. Cochrane Database Syst. Rev. 2007. [Google Scholar] [CrossRef] [PubMed]
- Saulle, R.; Vecchi, S.; Gowing, L. Supervised dosing with a long-acting opioid medication in the management of opioid dependence. Cochrane Database Syst. Rev. 2017. [Google Scholar] [CrossRef] [PubMed]
- Scott, N.A.; Moga, C.; Harstall, C. Managing low back pain in the primary care setting: The know-do gap. Pain Res. Manag. 2010, 15, 392–400. [Google Scholar] [CrossRef]
- Singh, P.; Chaturvedi, A. Complementary and Alternative Medicine in Cancer Pain Management: A Systematic Review. Indian J. Palliat. Care 2015, 21, 105–115. [Google Scholar] [CrossRef]
- Sluka, K.A.; Bjordal, J.M.; Marchand, S.; Rakel, B.A. What Makes Transcutaneous Electrical Nerve Stimulation Work? Making Sense of the Mixed Results in the Clinical Literature. Phys. Ther. 2013, 93, 1397–1402. [Google Scholar] [CrossRef] [PubMed]
- Smith, C.A.; Levett, K.M.; Collins, C.T.; Dahlen, H.G.; Ee, C.C.; Suganuma, M. Massage, reflexology and other manual methods for pain management in labour. Cochrane Database Syst. Rev. 2018. [Google Scholar] [CrossRef] [PubMed]
- Stuiver, M.M.; ten Tusscher, M.R.; Agasi-Idenburg, C.S.; Lucas, C.; Aaronson, N.K.; Bossuyt, P.M.M. Conservative interventions for preventing clinically detectable upper-limb lymphoedema in patients who are at risk of developing lymphoedema after breast cancer therapy. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef]
- Tashani, O.; Johnson, M. Transcutaneous Electrical Nerve Stimulation (TENS) A Possible Aid for Pain Relief in Developing Countries? Libyan J. Med. 2009, 4, 62–65. [Google Scholar] [CrossRef]
- Tirlapur, S.A.; Vlismas, A.; Ball, E.; Khan, K.S. Nerve stimulation for chronic pelvic pain and bladder pain syndrome: A systematic review. Acta Obstet. Gynecol. Scand. 2013, 92, 881–887. [Google Scholar] [CrossRef]
- Twycross, A.; Forgeron, P.; Williams, A. Paediatric nurses’ postoperative pain management practices in hospital based non-critical care settings: A narrative review. Int. J. Nurs. Stud. 2015, 52, 836–863. [Google Scholar] [CrossRef] [PubMed]
- Tzortziou Brown, V.; Underwood, M.; Mohamed, N.; Westwood, O.; Morrissey, D. Professional interventions for general practitioners on the management of musculoskeletal conditions. Cochrane Database Syst. Rev. 2016. [Google Scholar] [CrossRef]
- Veves, A.; Backonja, M.; Malik, R.A. Painful diabetic neuropathy: Epidemiology, natural history, early diagnosis, and treatment options. Pain Med. 2008, 9, 660–674. [Google Scholar] [CrossRef] [PubMed]
- Walsh, D.M. The evolution of TENS. Hong Kong Physiother. J. 2003, 21, 1–4. [Google Scholar] [CrossRef]
- Walsh, D.M.; Howe, T.E.; Johnson, M.I.; Sluka, K.A. Transcutaneous electrical nerve stimulation for acute pain. Cochrane Database Syst. Rev. 2009, CD006142. [Google Scholar]
- Walsh, D.M.; Howe, T.E.; Johnson, M.I.; Moran, F.; Sluka, K.A. Transcutaneous electrical nerve stimulation for acute pain. Cochrane Database Syst. Rev. 2015. [Google Scholar] [CrossRef]
- Weiner, D.K.; Ernst, E. Complementary and alternative approaches to the treatment of persistent musculoskeletal pain. Clin. J. Pain 2004, 20, 244–255. [Google Scholar] [CrossRef] [PubMed]
- Wiffen, P.J. Pain and palliative care in the Issue Number 3, 2001 of The Cochrane Library. J. Pain Palliat. Care Pharmacother. 2002, 16, 81–86. [Google Scholar] [CrossRef] [PubMed]
- Wiffen, P.J. Evidence-based pain management and palliative care in issue three for 2004 of The Cochrane Library. J. Pain Palliat. Care Pharmacother. 2005, 19, 63–65. [Google Scholar] [CrossRef] [PubMed]
- Wiffen, P.J. Evidence-based pain management and palliative care systematic reviews in issue three for 2008 of The Cochrane Library. J. Pain Palliat. Care Pharmacother. 2009, 23, 69–71. [Google Scholar] [CrossRef] [PubMed]
- Wiffen, P.J. Evidence-based pain management and palliative care in Issue Two for 2009 of The Cochrane Library. J. Pain Palliat. Care Pharmacother. 2009, 23, 290–294. [Google Scholar] [CrossRef] [PubMed]
- Wiffen, P.J.; Derry, S.; Moore, R.A.; Kalso, E.A. Carbamazepine for chronic neuropathic pain and fibromyalgia in adults. Cochrane Database Syst. Rev. 2014. [Google Scholar] [CrossRef]
- Zhang, W.; Moskowitz, R.W.; Nuki, G.; Abramson, S.; Altman, R.D.; Arden, N.; Bierma-Zeinstra, S.; Brandt, K.D.; Croft, P.; Doherty, M.; et al. OARSI recommendations for the management of hip and knee osteoarthritis, Part II: OARSI evidence-based, expert consensus guidelines. Osteoarthr. Cartil. 2008, 16, 137–162. [Google Scholar] [CrossRef]
- Zakrzewska, J.M.; Akram, H. Neurosurgical interventions for the treatment of classical trigeminal neuralgia. Cochrane Database Syst. Rev. 2011. [Google Scholar] [CrossRef]

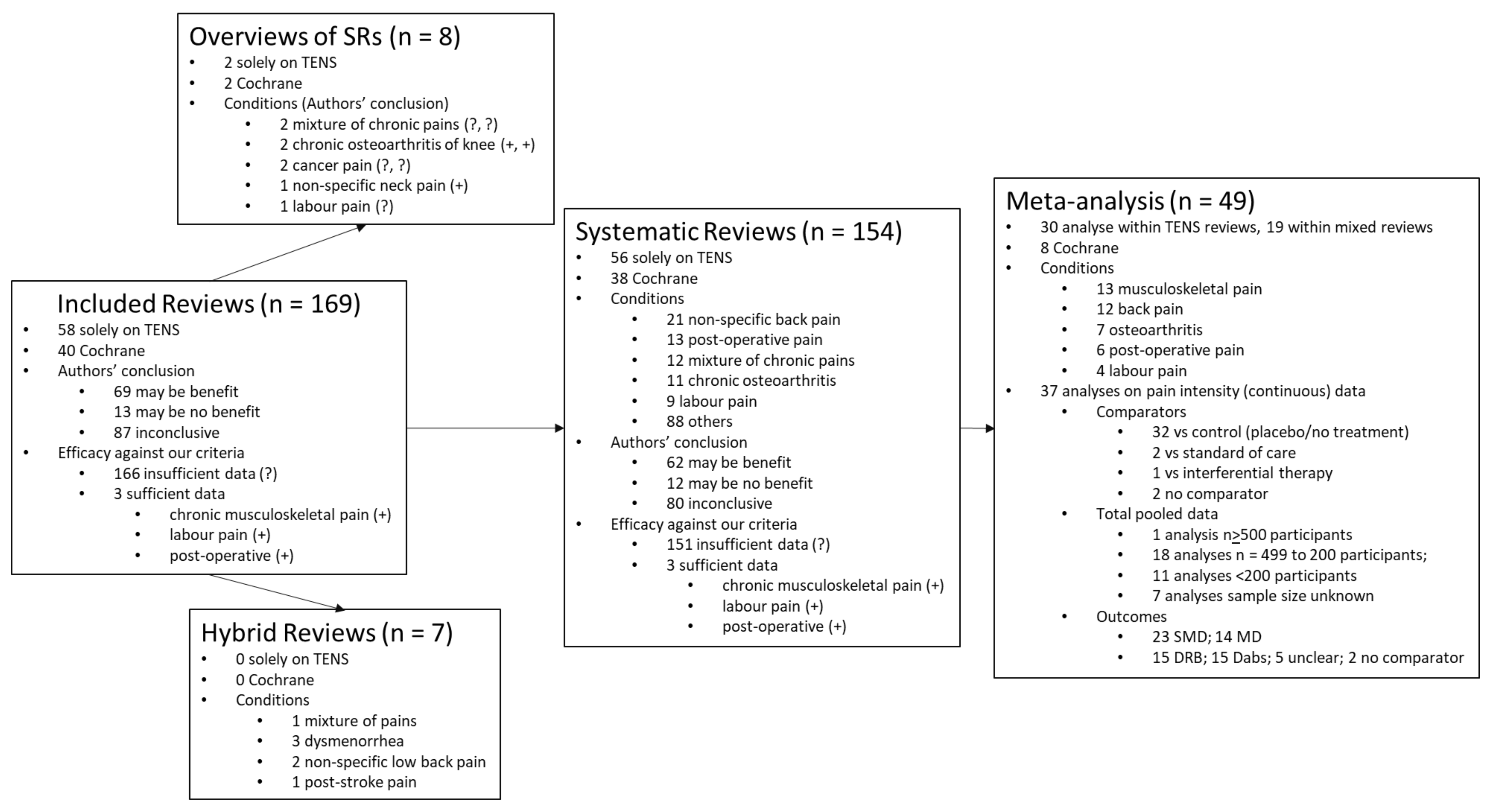

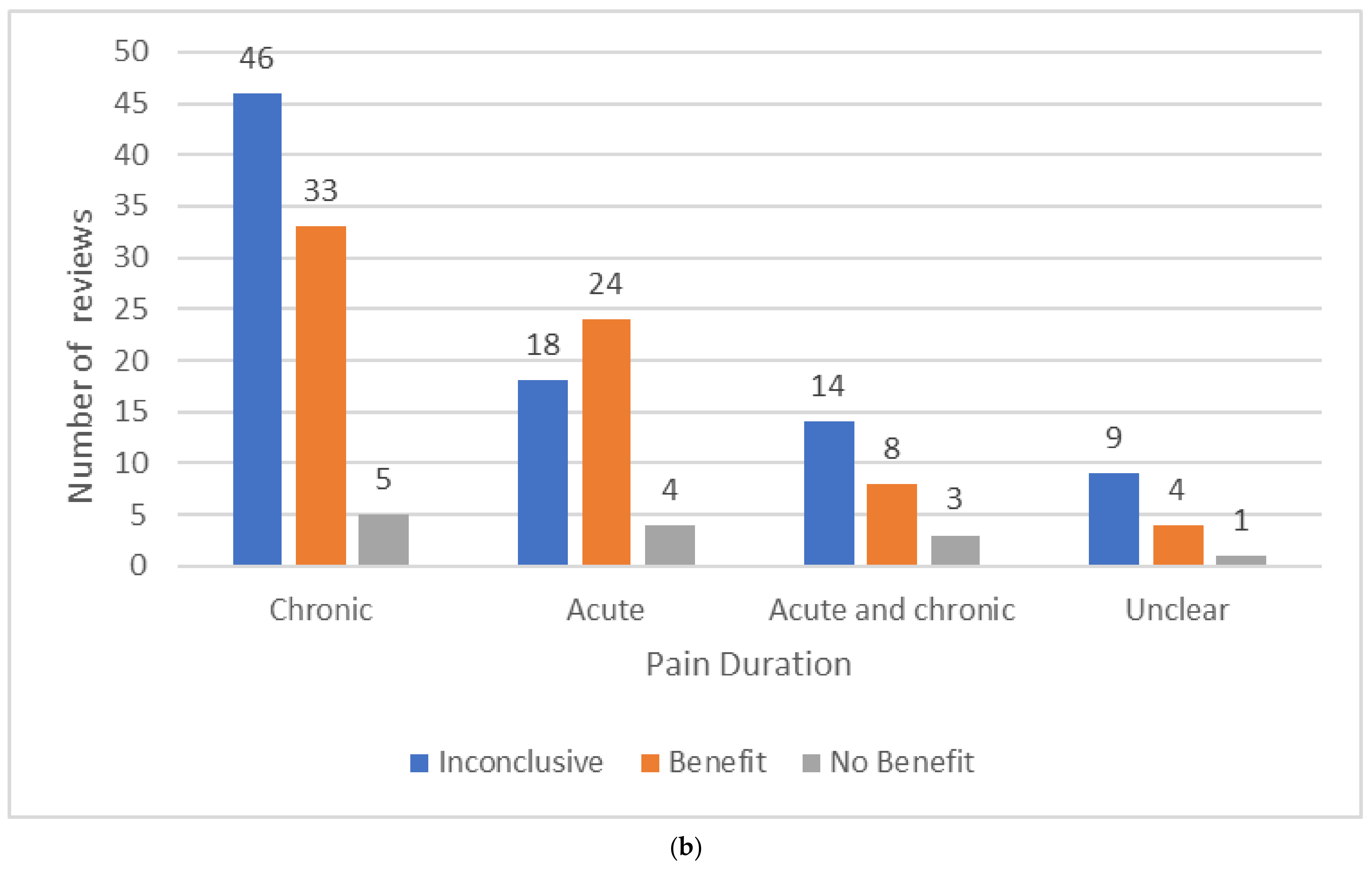
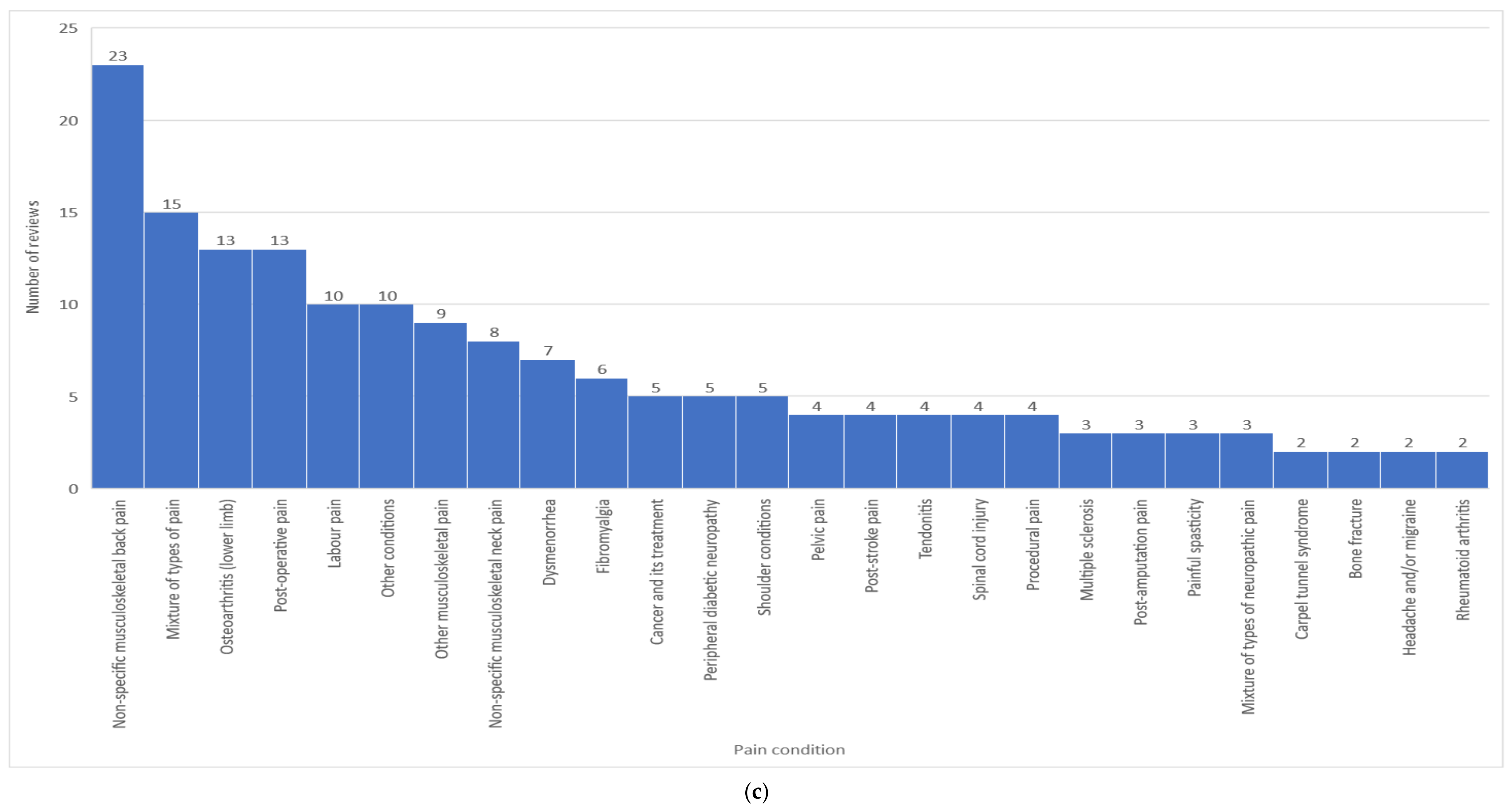

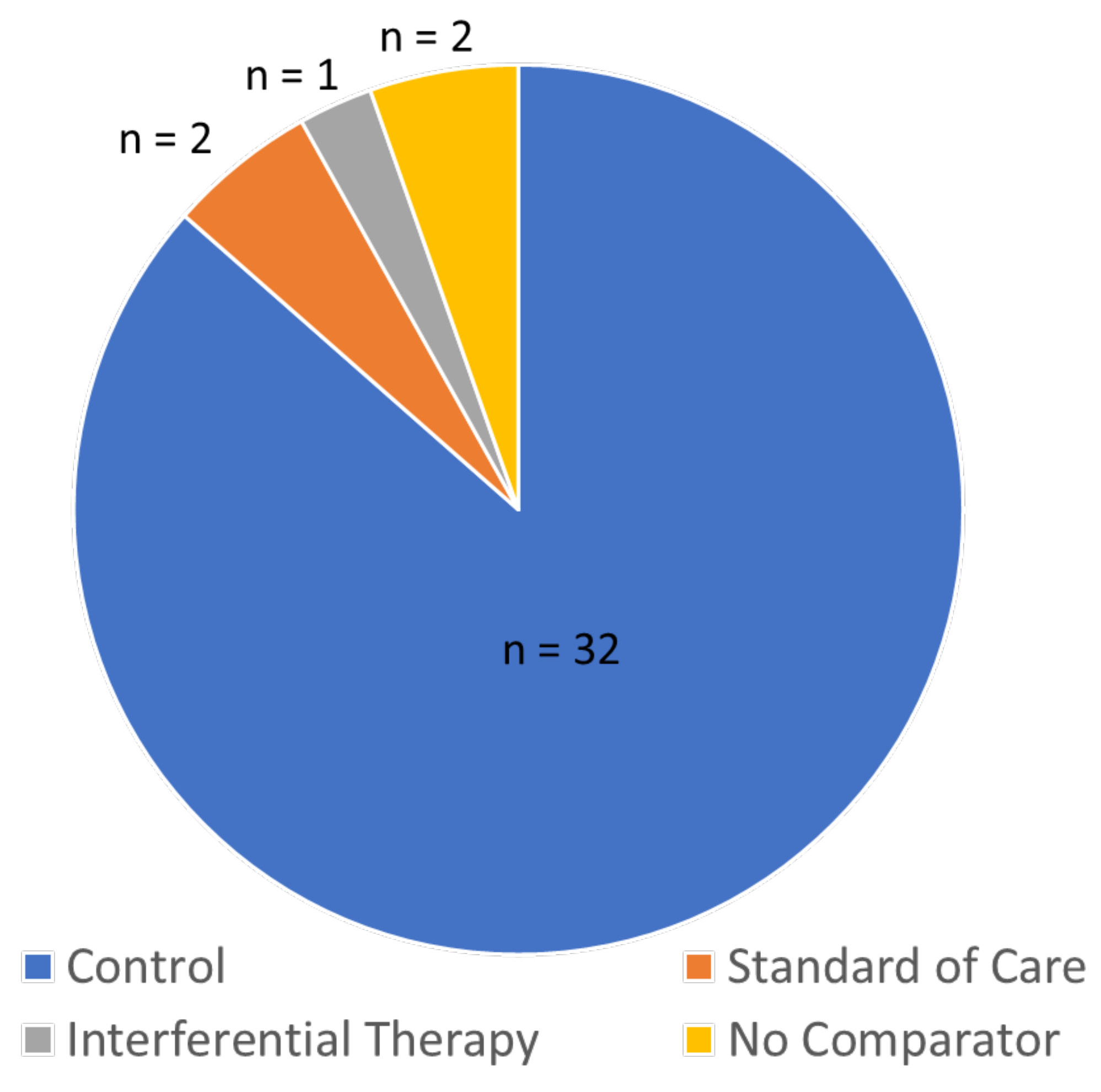
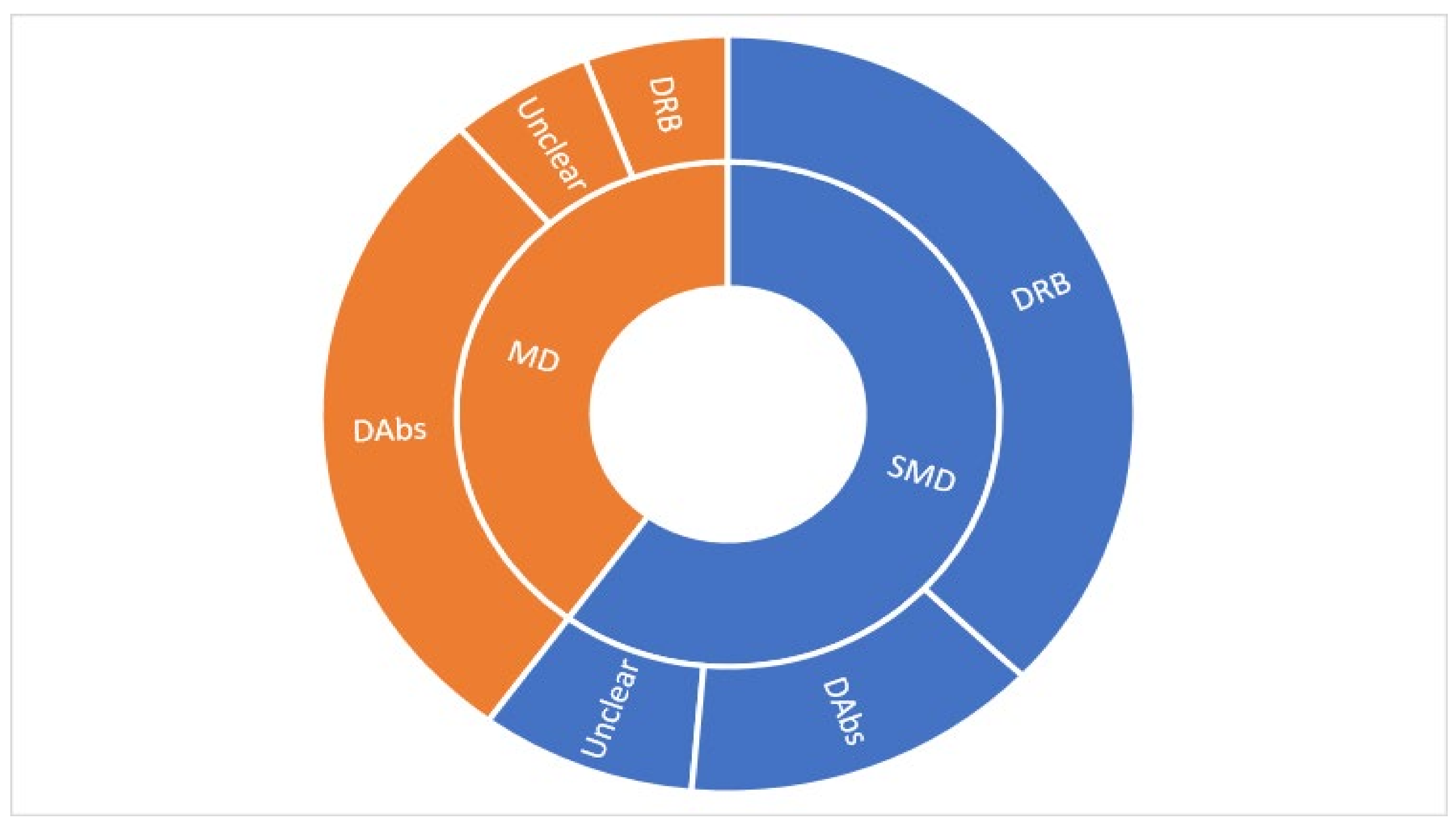
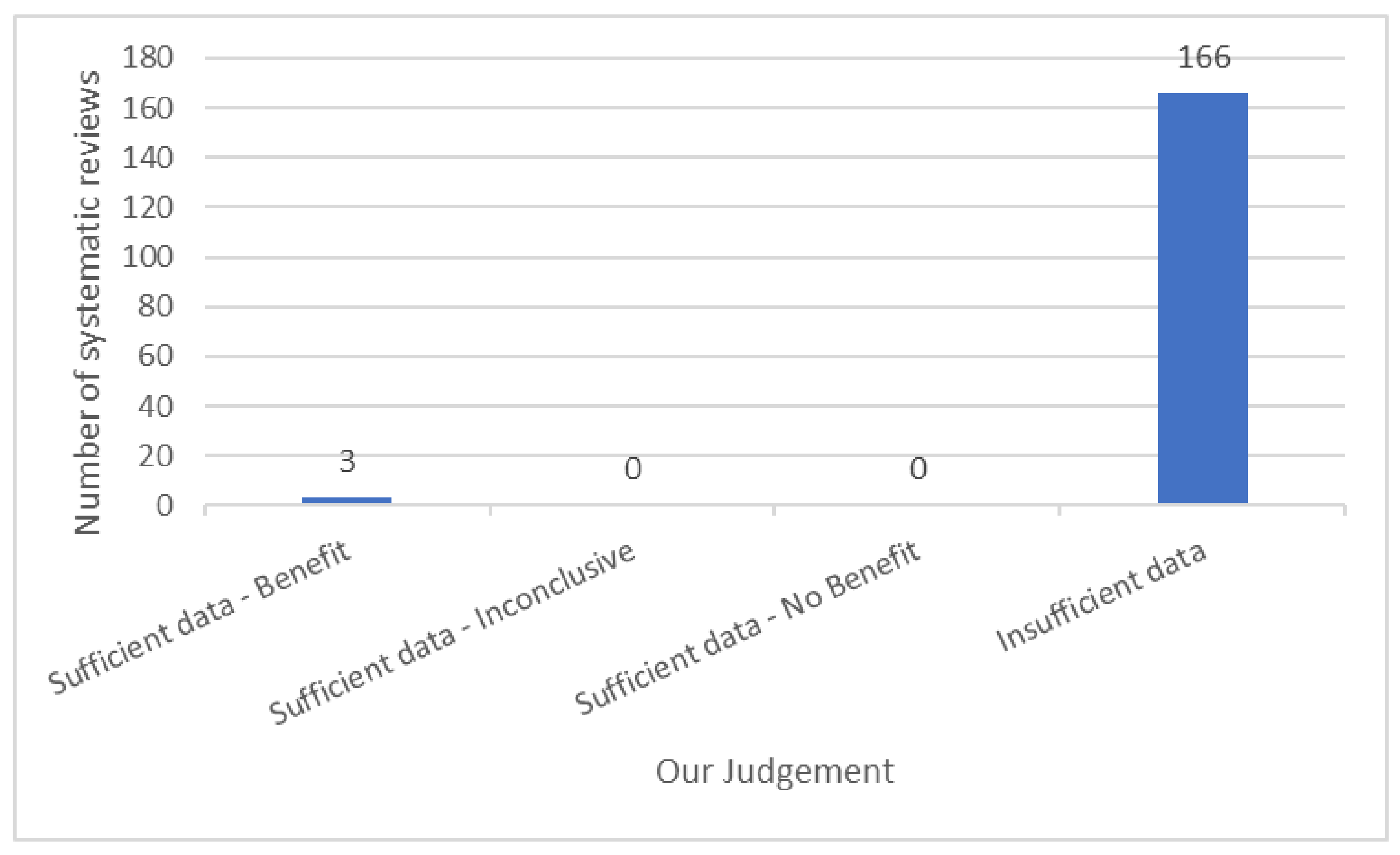
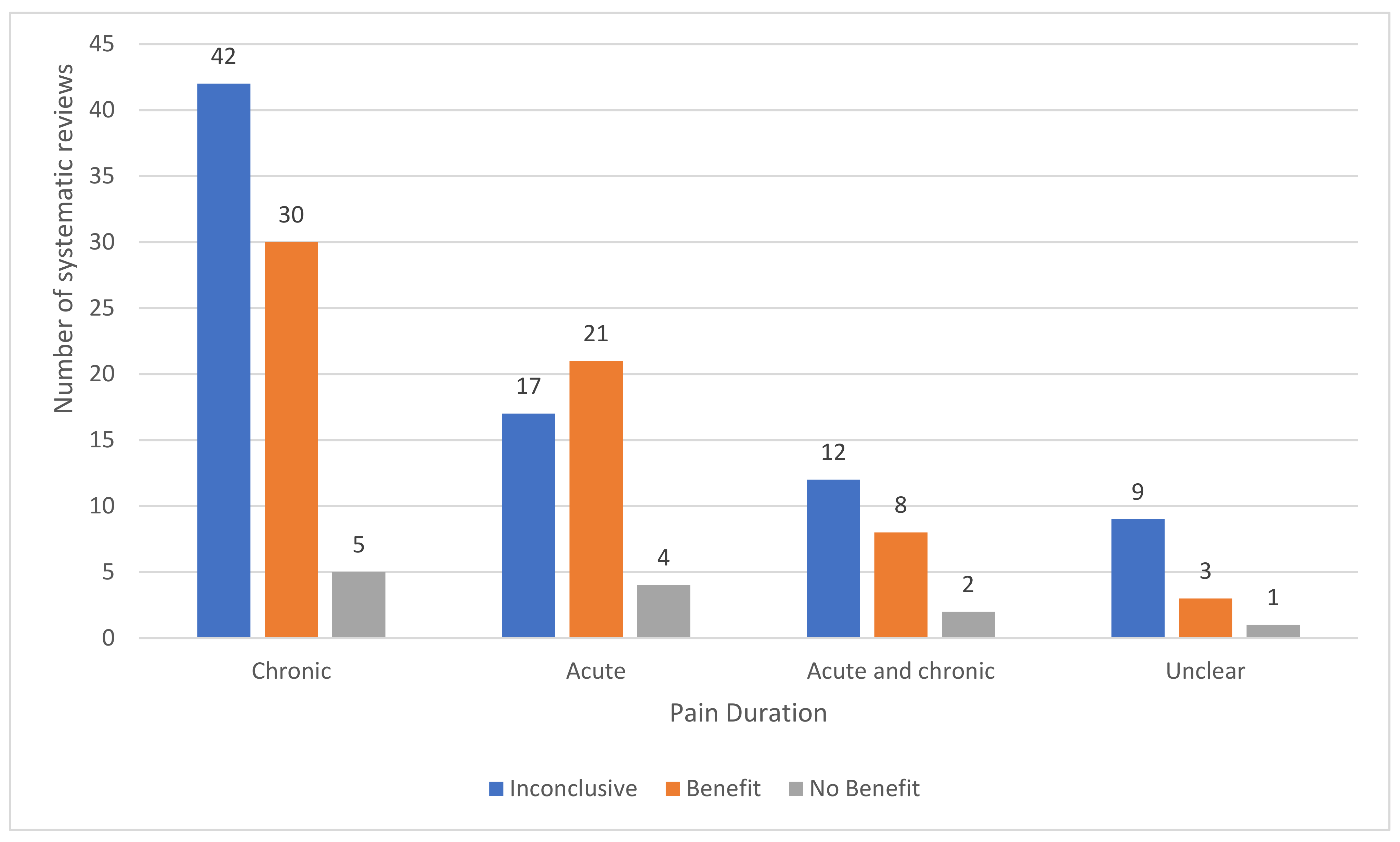
| Systematic Review. | Number of Studies Included in Review | Facci et al.,(2011) [28] | Ratajczak et al.,(2011) [29] | Sahin et al.,(2011) [30] | Alizadeh et al.,(2009) [31] | Itoh et al.,(2009) [32] | Barker et al.,(2008) [33] | Kofotolis et al.,(2008) [34] | Thompson et al.,(2008) [35] | Shimoji et al.,(2007) [36] | Warke et al.,(2006) [37] | Jarzem et al.,(2005) [38] | Jarzem et al.,(2005) [39] | Topuz et al.,(2004) [27] | Yokoyama et al.,(2004) [40] | Hsieh and Lee (2002) [41] | Tsukayama et al.,(2002) [42] | Cheing et al.,(1999) [43] | Grant et al.,(1999) [44] | Ghoname et al.,(1999) [45] | Moore and Shurman (1997) [46] | Marchand et al.,(1993) [47] | Gemignani et al.,(1991) [48] | Deyo et al.,(1990) [49] | Lehmann et al.,(1986) [50] |
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Resende et al. [51] | 9 | I | I | I | I DE | I DE | I DE | I DE | I DE | I DE | |||||||||||||||
| Wu et al. [14] | 12 | I DE | I DE | I DE | I DE | I DE | I | I DE | I DE | I DE | I DE | I DE | I DE | ||||||||||||
| Jauregui et al. [52] | 13 | I DE | I DE | I DE | I DE | I | I DE | I DE | I DE | I DE | I DE | I DE | I DE | I DE | |||||||||||
| Van Middelkoop et al. [53] | 7 | N/A | N/A | N/A | I DE | I DE | I DE | I DE | I DE | I DE | I DE |
| Ref. | Title | Condition | Acute/Chronic Pain | Review Type | Number of TENS Studies | MA | Authors’ Conclusion | Authors’ Judgement | Our Judgement | Comment |
|---|---|---|---|---|---|---|---|---|---|---|
| Various chronic musculoskeletal pain(9 reviews) | ||||||||||
| Ely et al. [101] | Transcutaneous electrical acupoint stimulation for people with chronic musculoskeletal pain: an exploratory review | Musculoskeletal pain—chronic | Chronic | SR | 20 | N | People with chronic musculoskeletal pain may achieve pain relief using transcutaneous electric acupoint stimulation but the existing evidence is limited, and high-quality clinical evidence is required to establish efficacy | ? | ? | We suspect that this is the full report of Ely et al. [102] |
| Nunes et al. [103] | Effectiveness of physical and rehabilitation techniques in reducing pain in chronic trapezius myalgia: A systematic review and meta-analysis | Myalgia—chronic trapezius | Chronic | SR | 1 | N | There was very poor evidence that TENS therapy and manual therapy are effective in treating chronic trapezius myalgia | ? | ? | |
| Almeida et al. [104] | Conservative interventions for treating exercise-related musculotendinous, ligamentous and osseous groin pain | Exercise-related musculotendinous, ligamentous and osseous groin pain | UC | CR | 2 | N | The available evidence from the randomized trials is insufficient to advise on any specific conservative modality for treating exercise related groin pain. | ? | ? | The authors could not isolate effect of TENS because the included studies delivered TENS as part of multimodal physiotherapy treatment |
| Bellini et al. [105] | Physical therapy applied to pathologies of rehabilitative interest | Musculoskeletal pain | Chronic | SR | 5 | N | TENS is recommended for the treatment of tibio-femoral osteoarthritis, its effectiveness is questionable for carpal tunnel syndrome and not recommended for the treatment of chronic low-back pain | + | ? | |
| Vernon et al. [106] | Chiropractic management of myofascial trigger points and myofascial pain syndrome: a systematic review of the literature | Myofascial pain | Both | SR | 6 | N | There is moderately strong evidence that TENS may be effective in providing immediate relief at trigger point. The evidence level is B. | + | ? | Evaluated commonly used treatments |
| Johnson et al. [10] | Efficacy of electrical nerve stimulation for chronic musculoskeletal pain: A meta-analysis of randomized controlled trials | Musculoskeletal pain—chronic | Chronic | SR | 29 | Y | These results indicate that electrical nerve stimulation is an effective treatment modality for chronic musculoskeletal pain and that previous, equivocal results may have been due to underpowered studies. | + | + | There were 32 RCTS of which 29 were on TENS and the rest on peripheral nerve stimuation |
| Rickards et al. [107] | Myofascial trigger point pain | Myofascial | UC | SR | 7 | N | TENS appears to have an immediate effect in decreasing pain intensity in myofascial trigger point pain of the neck and upper back. However, there are insufficient data to provide the evidence of effectiveness for TENS beyond immediately after treatment. | + | ? | |
| O’Connor et al. [108] | The effectiveness of physiotherapeutic interventions in the management of delayed onset muscle soreness: A systematic review | Muscle soreness—post exercise | Acute | SR | 3 | N | The evidence did not support the use of static stretching, cryotherapy, acupuncture, pulsed ultrasound, TENS, interferential therapy, and microcurrent electrical stimulation | ? | ? | The authors stated that the evidence was conflicting |
| Philadelphia Panel [109] | Philadelphia Panel Evidence-Based Clinical Practice Guidelines on Selected Rehabilitation Interventions for Shoulder Pain | Shoulder pain—non-specific | Both | SR | 1 | N | …a lack of evidence regarding efficacy | ? | ? | |
| Non-specific back pain 21 reviews | ||||||||||
| Nascimento et al. [110] | Effectiveness of interventions for non-specific low back pain in older adults. A systematic review and meta-analysis | Back pain—chronic low | Chronic | SR | 1 | N | No statement of conclusion for TENS | ? | ? | The authors commented that a previous study showed a higher effectiveness of percutaneous electrical nerve stimulation (PENS) to decrease pain compared to TENS at short-term follow-up. |
| Resende et al. [51] | Meta-analysis of transcutaneous electrical nerve stimulation for relief of spinal pain | Back and/or neck pain—chronic | Chronic | SR | 9 | Y | …inconclusive evidence of TENS benefits in low back pain patients because the quality of the studies was low, and adequate parameters and timing of assessment were not uniformly used or reported. | ? | ? | Nine RCTs with seven data sets included for meta-analysis (655 participants) |
| Wu et al. [14] | Literature Review and Meta-Analysis of Transcutaneous Electrical Nerve Stimulation in Treating Chronic Back Pain | Back pain—Chronic | Chronic | SR | 12 | Y | These results suggest that TENS does not improve symptoms of lower back pain but may offer short-term improvement of functional disability. | − | ? | |
| Bredow et al. [111] | Non-specific chronic low back pain (NSCLBP): Which conservative therapy shows an evident effectiveness—A review of the current literature | Back pain—chronic non-specific (low) | Chronic | MR | 1 SR | N | In a Cochrane analysis by Khadilkar et al. [100] regarding the use of TENS there is no evidence regarding the treatment of Non-specific chronic low back pain | ? | ? | Article in German No RCTS were included |
| Jauregui et al. [52] | A Meta-Analysis of Transcutaneous Electrical Nerve Stimulation for Chronic Low Back Pain | Back—chronic low | Chronic | SR | 12 | Y | Treatment of chronic low back pain with TENS demonstrated significant pain reduction. The application of TENS may lead to less pain medication usage and should be incorporated into the treatment armamentarium for chronic low back pain | + | ? | |
| Ehrenbrusthoff et al. [112] | Physical therapy management of older adults with chronic low back pain: A systematic review | Back—chronic low | Chronic | SR | 0 | N | No statement of conclusion for TENS | ? | ? | Book chapter |
| van Middelkoop et al. [53] | A systematic review on the effectiveness of physical and rehabilitation interventions for chronic non-specific low back pain | Back pain—chronic low | Chronic | SR | 6 | Y | The data provided low quality evidence (serious limitations, heterogeneity) that there is no statistically significant difference on post-treatment pain intensity and disability between TENS and sham-TENS | − | ? | |
| Chou [113] | Low back pain (chronic) | Back pain—chronic low | Chronic | SR | 3 | N | Compared with placebo: We don’t know whether TENS is more effective at reducing pain in people with chronic low back pain (very low-quality evidence). Compared with sham TENS plus massage: TENS plus massage may be no more effective at reducing pain in people with chronic low back pain (low-quality evidence). | ? | ? | Update of Hall and McIntosh [114] |
| Dubinsky et al. [115] | Assessment: Efficacy of transcutaneous electric nerve stimulation in the treatment of pain in neurologic disorders (an evidence-based review) | Back—chronic low | Chronic | SR | 4 | N | TENS is not recommended for the treatment of chronic low back pain (Level A) | − | ? | Conducted two analyses in same report—this is data for back pain only. See rebuttal by Johnson and Walsh [116] |
| Gaid et al. [117] | The role of transcutaneous electric nerve stimulation (TENS) for the management of chronic low back pain | Back—chronic low | Chronic | SR | 3 | N | …evidence supporting the use TENS as a short-term effective treatment modality for chronic low back pain. Evidence of a longer-term effect is equivocal. | + | ? | |
| Gutiérrez et al. [118] | Evidence of the analgesic effect of physiotherapy in the low backpain syndrome | Low Back Pain | Both | SR | 4 | N | …controversial evidence regarding the use of laser and TENS in sub-acute and chronic low back pain | ? | ? | |
| Machado et al. [86] | Analgesic effects of treatments for non-specific low back pain: a meta-analysis of placebo-controlled randomized trials | Back pain—chronic low | Both | SR | 4 | Y | No statement of conclusion for TENS | ? | ? | No numerical data of effect size but the forest plot revealed the upper confidence interval was in favour of TENS and did not bisect the line of no difference |
| Khadilkar et al. [100] | Transcutaneous electrical nerve stimulation (TENS) versus placebo for chronic low-back pain (Review) | Back—chronic low | Chronic | CR | 5 | N | …evidence from the small number of placebo-controlled trials does not support the use of TENS in the routine management of chronic low back pain | − | ? | Updates of Khadilkar et al. [119] and Milne et al. [120] |
| Poitras et al. [87] | Evidence-informed management of chronic low back pain with transcutaneous electrical nerve stimulation, interferential current, electrical muscle stimulation, ultrasound, and thermotherapy | Back pain—chronic low | Chronic | SR | 4 | Y | Globally, high and low-frequency TENS appears to have an immediate impact on pain intensity, with results favoring high-frequency TENS | + | ? | The North American Spine Society sponsored this special focus issue. |
| Chou [61] | Nonpharmacologic Therapies for Acute and Chronic Low Back Pain: A Review of the Evidence for an American Pain Society/American College of Physicians Clinical Practice Guideline | Back pain—acute and chronic | Both | MR | 4 6 SRs | N | Other non-invasive therapies (back schools, interferential therapy, low-level laser therapy, lumbar supports, TENS, traction, and ultrasonography) have not been shown to be effective for either chronic or subacute or acute low back pain | − | ? | |
| Keller et al. [63] | Effect sizes of non-surgical treatments of non-specific low-back pain | Back pain—chronic low | Chronic | SR | 2 | Y | TENS and manipulation had small effect sizes | ? | ? | |
| Brosseau et al. [62] | Efficacy of the transcutaneous electrical nerve stimulation for the treatment of chronic low back pain—A meta-analysis. | Back pain—chronic low | Chronic | SR | 5 | Y | The results of the meta-analysis present no evidence to support the use or non-use of TENS alone in the treatment of chronic low back pain | ? | ? | |
| Pengel et al. [121] | Systematic review of conservative interventions for subacute low back pain | Back pain—subacute low | Both | SR | 3 | N | …there is evidence that…other treatments (e.g., manipulation, exercise, TENS) may be effective | + | ? | |
| Philadelphia Panel [64] | Philadelphia Panel Evidence-Based Clinical Practice Guidelines on Selected Rehabilitation Interventions for Low Back Pain | Back pain—low, non-specific | Both | SR | 5 | Y | …a lack of evidence regarding efficacy of TENS for Acute LBP (<4 Weeks), Level I (RCT), Grade C for Pain or Function (No Benefit Demonstrated) | ? | ? | Detailed analysis |
| Flowerdew and Gadsby [122] | A review of the treatment of chronic low back pain with acupuncture-like transcutaneous electrical nerve stimulation and transcutaneous electrical nerve stimulation | Back pain–chronic low | Chronic | SR | 6 | Y | There is limited statistical evidence that ALTENS and TENS reduce pain and improve function in patients with chronic low back pain, at least in the short term | + | ? | |
| Gadsby et al. [123] | Low back pain | Back pain—low | Chronic | SR | 6 | Y | …clear evidence that conventional TENS and acupuncture-like TENS reduce pain and increase range of motion of patients with chronic low back pain | + | ? | |
| Low Back Pain (Acute) 2 reviews | ||||||||||
| Binny et al. [85] | Transcutaneous electric nerve stimulation (TENS) for acute low back pain: systematic review | Back pain, low, acute | Acute | SR | 3 | Y | …is insufficient [evidence] to support or dismiss the use of TENS for acute low back pain | ? | ? | |
| McIntosh and Hall [124] | Low back pain (acute) | Back pain—low | Acute | SR | 0 | N | No statement of conclusion for TENS | ? | ? | |
| Non-specific neck pain 8 reviews | ||||||||||
| Martimbianco et al. [125] | Transcutaneous electrical nerve stimulation (TENS) for chronic neck pain | Neck pain—chronic | Chronic | SR | 7 | N | …there was very low-certainty evidence from two trials about the effects of conventional TENS when compared to sham TENS at short-term | ? | ? | This is described as a ‘split’ from Kroeling 2013’—we include because different team and over 5 years elapsed since original |
| (Kroeling et al., 2013) | Electrotherapy for neck pain (Review) | Neck Pain | UC | CR | 10 | N | TENS…might be more effective than placebo (very low quality evidence) | + | ? | |
| Binder et al. [126] | Clinical Evidence Neck pain | Neck pain—various… | Both | SR | 1 | N | We don’t know whether…TENS,…are better or worse than other treatments at reducing [various types of acute and chronic neck pain] | ? | ? | |
| Jensen et al. [56] | Neck pain | Neck pain—non-specific | UC | OSR | 0 | N | symptom relief this condition can be treated with TENS | + | ? | |
| Vernon et al. [127] | A systematic review of conservative treatment for acute neck pain not due to whiplash | Neck pain—not whiplash | Acute | SR | 1 | N | One trial 47 provides some evidence that TENS treatment is beneficial over a 3-week interval | ? | ? | |
| Philadelphia Panel [128] | Philadelphia Panel Evidence-Based Clinical Practice Guidelines on Selected Rehabilitation Interventions for Neck Pain | Neck pain—non-specific | Both | SR | 1 | N | …a lack of evidence regarding efficacy…TENS for acute neck pain | ? | ? | |
| Kjellman et al. [129] | A critical analysis of randomised clinical trials on neck pain and treatment efficacy. A review of the literature | Neck pain | Both | SR | 3 | N | [No statement of conclusion for TENS] | U | ? | No conclusion on TENS |
| Aker et al. [130] | Conservative management of mechanical neck pain: systematic overview and meta-analysis | Mechanical neck pain | Both | SR | 2 | No | …no treatments [including TENS] have been studied in enough detail to assess either efficacy or effectiveness | ? | ? | Article is a summary of Gross et al. [131] |
| Condition | Quantity of Included Reviews | Comment—Quality of Reviews | Comment—Quantity and Quality of RCT Data | Judgement—Analgesic Efficacy |
|---|---|---|---|---|
| Mixtures of painful conditions | 15 | One OCR, CRs and some SRs of high methodological quality Strongest review: Chronic pain—Gibson et al. [6]; Acute pain—Johnson et al. [83] | Well over 200 different studies on TENS for any type of pain cited in the included reviews. Majority of studies have small (inadequate) sized samples Strongest RCT: Dailey et al. [224] | + |
| Musculoskeletal pain including non-specific low back or neck pain | 40 reviews including 23 reviews on non-specific back pain | CRs and some SRs are high methodological quality Strongest review: Johnson and Martinsson [10] with Wu et al. [14] and Jauregui et al. [52] also notable | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes. More reviews than studies for back and for neck pain Majority of RCTs have small samples Strongest RCTs: Warke et al. [37], Deyo et al. [49] | ++ |
| Osteoarthritis | 11 reviews | CRs and some SRs are high methodological quality Strongest review: Chen et al. [77] and Rutjes et al. [78] | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Atamaz et al. [225] Palmer et al. [226] | + |
| Post-operative pain | 13 reviews | Some SRs are high methodological quality Strongest review: Zhou et al. [88] and Bjordal et al. [11] | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Rakel et al. [227] | ++ |
| Labour pain | 10 reviews | CRs and some SRs are high methodological quality Strongest reviews: Thuvarakan et al. [26] and Dowswell et al. [22] | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Baez-Suarez et al. [228], Tsen et al. [229], Thomas et al.,1988 [230] | + |
| Dysmenorrhea and Pelvic pain | 12 reviews | Some SRs are high methodological quality Strongest review: Cottrell et al. [71] and Arik et al. [70] | Few moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Bai et al. [231] | + |
| Fibromyalgia | 6 reviews | CRs and some SRs are high methodological quality Strongest review: Johnson et al. [156] and Megia Garcia et al. [155] | One very high quality moderately sized study Strongest RCT: Dailey et al. [224] | + |
| Cancer and its treatment | 5 reviews | CRs and some SRs are high methodological quality Strongest review: Hurlow et al. [168] | No suitable RCTs | ? |
| Specific shoulder conditions | 5 reviews | One CR of high methodological quality Strongest reviews: Page et al.—rotator cuff disease [176] | Few studies and most RCTs have small (inadequate) sample Strongest RCT: Baskurt et al. [232] | + |
| Peripheral diabetic neuropathy | 5 reviews | Some SRs are high methodological quality Strongest review: Zeng et al. [169] and Stein et al. [65] | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Bulut et al. [233] | + |
| Other painful conditions | 47 reviews | CRs and some SRs are high methodological quality Strongest reviews: Gibson et al.—neuropathic pain [13], Fernandez-Tenorio et al.—spasticity [201] | Some moderately sized studies well designed studies but most RCTs have small (inadequate) sample sizes Strongest RCT: Amer-Cuenca et al. [234]—procedural pain | ? |
| Overall | 169 reviews | CRs and some SRs are high methodological quality | Strongest RCT: Dailey et al. [224] | + |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Paley, C.A.; Wittkopf, P.G.; Jones, G.; Johnson, M.I. Does TENS Reduce the Intensity of Acute and Chronic Pain? A Comprehensive Appraisal of the Characteristics and Outcomes of 169 Reviews and 49 Meta-Analyses. Medicina 2021, 57, 1060. https://doi.org/10.3390/medicina57101060
Paley CA, Wittkopf PG, Jones G, Johnson MI. Does TENS Reduce the Intensity of Acute and Chronic Pain? A Comprehensive Appraisal of the Characteristics and Outcomes of 169 Reviews and 49 Meta-Analyses. Medicina. 2021; 57(10):1060. https://doi.org/10.3390/medicina57101060
Chicago/Turabian StylePaley, Carole A., Priscilla G. Wittkopf, Gareth Jones, and Mark I. Johnson. 2021. "Does TENS Reduce the Intensity of Acute and Chronic Pain? A Comprehensive Appraisal of the Characteristics and Outcomes of 169 Reviews and 49 Meta-Analyses" Medicina 57, no. 10: 1060. https://doi.org/10.3390/medicina57101060
APA StylePaley, C. A., Wittkopf, P. G., Jones, G., & Johnson, M. I. (2021). Does TENS Reduce the Intensity of Acute and Chronic Pain? A Comprehensive Appraisal of the Characteristics and Outcomes of 169 Reviews and 49 Meta-Analyses. Medicina, 57(10), 1060. https://doi.org/10.3390/medicina57101060







