Clinical Predictors Influencing the Length of Stay in Emergency Department Patients Presenting with Acute Heart Failure
Abstract
1. Introduction
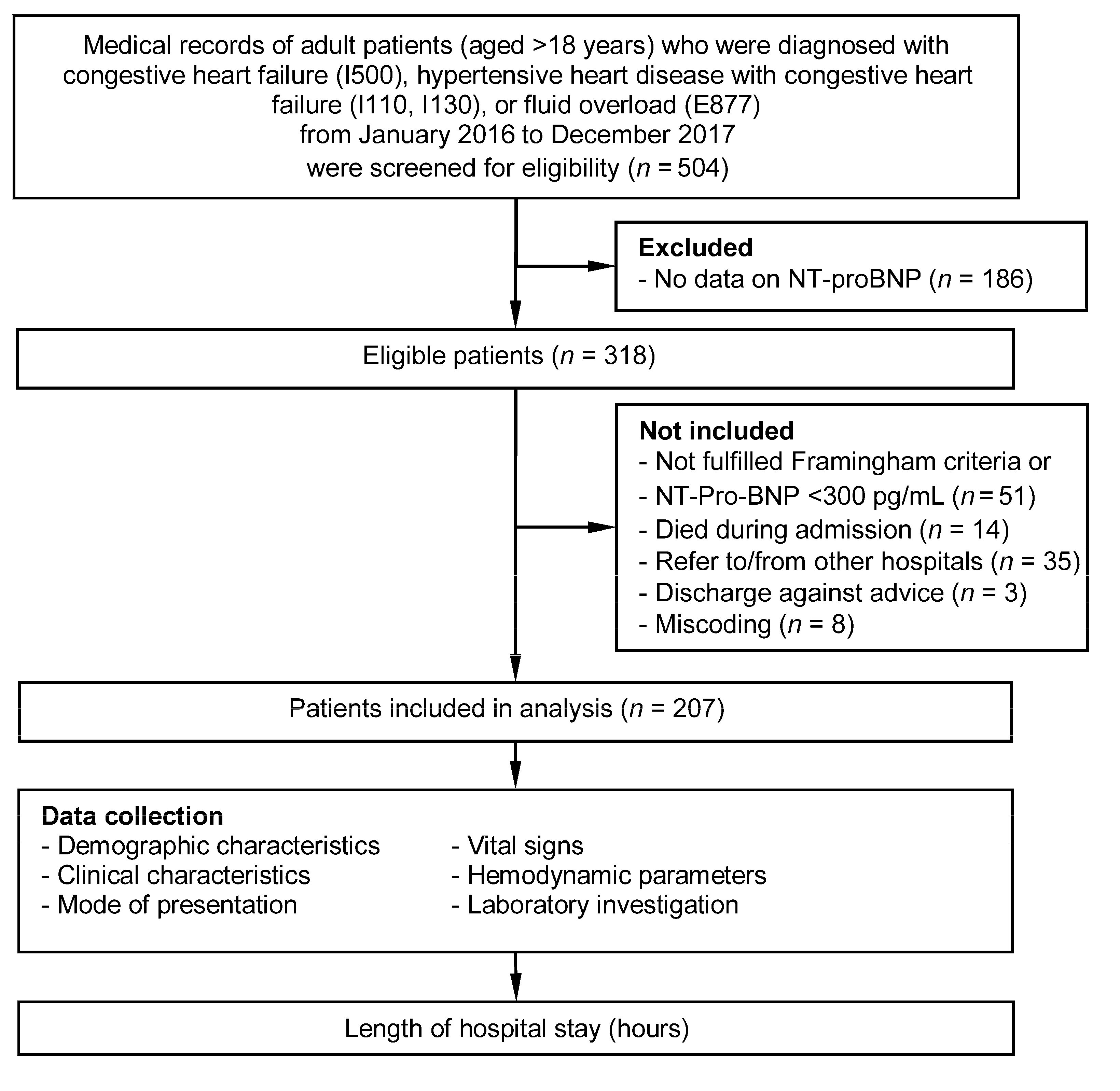
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Savarese, G.; Lund, L.H. Global Public Health Burden of Heart Failure. Card. Fail. Rev. 2017, 3, 7–11. [Google Scholar] [CrossRef]
- Lam, C.S.P. Heart failure in Southeast Asia: Facts and numbers. ESC Heart Fail 2015, 2, 46–49. [Google Scholar] [CrossRef] [PubMed]
- Ariyachaipanich, A.; Krittayaphong, R.; Kunjara Na Ayudhya, R.; Yingchoncharoen, T.; Buakhamsri, A.; Suvachittanont, N. Heart Failure Council of Thailand (HFCT) 2019 Heart Failure Guideline: Introduction and Diagnosis. J. Med Assoc. Thail. 2019, 102, 231–239. [Google Scholar]
- Weintraub, N.L.; Collins, S.P.; Pang, P.S.; Levy, P.D.; Anderson, A.S.; Arslanian-Engoren, C.; Gibler, W.B.; McCord, J.K.; Parshall, M.B.; Francis, G.S.; et al. Acute heart failure syndromes: Emergency department presentation, treatment, and disposition: Current approaches and future aims: A scientific statement from the American Heart Association. Circulation 2010, 122, 1975–1996. [Google Scholar] [CrossRef] [PubMed]
- Storrow, A.B.; Jenkins, C.A.; Self, W.H.; Alexander, P.T.; Barrett, T.W.; Han, J.H.; McNaughton, C.D.; Heavrin, B.S.; Gheorghiade, M.; Collins, S.P. The Burden of Acute Heart Failure on U.S. Emergency Departments. JACC Heart Fail. 2014, 2, 269–277. [Google Scholar] [CrossRef] [PubMed]
- Heidenreich, P.A.; Albert, N.M.; Allen, L.A.; Bluemke, D.A.; Butler, J.; Fonarow, G.C.; Ikonomidis, J.S.; Khavjou, O.; Konstam, M.A.; Maddox, T.M.; et al. Forecasting the impact of heart failure in the United States: A policy statement from the American Heart Association. Circ. Heart Fail. 2013, 6, 606–619. [Google Scholar] [CrossRef]
- Ho, E.C.; Schull, M.J.; Lee, D.S. The Challenge of Heart Failure Discharge from the Emergency Department. Curr. Heart Fail. Rep. 2012, 9, 252–259. [Google Scholar] [CrossRef][Green Version]
- Formiga, F.; Chivite, D.; Manito, N.; Mestre, A.R.; Llopis, F.; Pujol, R. Admission characteristics predicting longer length of stay among elderly patients hospitalized for decompensated heart failure. Eur. J. Intern. Med. 2008, 19, 198–202. [Google Scholar] [CrossRef]
- Whellan, D.J.; Zhao, X.; Hernandez, A.F.; Liang, L.; Peterson, E.D.; Bhatt, D.L.; Heidenreich, P.A.; Schwamm, L.H.; Fonarow, G.C. Predictors of Hospital Length of Stay in Heart Failure: Findings from Get With the Guidelines. J. Card. Fail. 2011, 17, 649–656. [Google Scholar] [CrossRef]
- Frigola-Capell, E.; Comin-Colet, J.; Davins-Miralles, J.; Gich-Saladich, I.; Wensing, M.; Verdú-Rotellar, J.M. Trends and predictors of hospitalization, readmissions and length of stay in ambulatory patients with heart failure. Rev. Clin. Esp. 2013, 213, 1–7. [Google Scholar] [CrossRef]
- Krantz, M.J.; Tanner, J.; Horwich, T.B.; Yancy, C.; Albert, N.M.; Hernandez, A.F.; Dai, D.; Fonarow, G.C. Get With the Guidelines Steering Committee and Hospitals Influence of hospital length of stay for heart failure on quality of care. Am. J. Cardiol. 2008, 102, 1693–1697. [Google Scholar] [CrossRef] [PubMed]
- Krumholz, H.M.; Chen, Y.T.; Bradford, W.D.; Cerese, J. Variations in and correlates of length of stay in academic hospitals among patients with heart failure resulting from systolic dysfunction. Am. J. Manag. Care 1999, 5, 715–723. [Google Scholar] [PubMed]
- Laothavorn, P.; Hengrussamee, K.; Kanjanavanit, R.; Moleerergpoom, W.; Laorakpongse, D.; Pachirat, O.; Boonyaratavej, S.; Sritara, P. Thai Acute Decompensated Heart Failure Registry (Thai ADHERE). CVD Prev. Control 2010, 5, 89–95. [Google Scholar] [CrossRef]
- Pongsuthana, S.; Chopchai, K. In-Hospital Mortality Predictors of Heart Failure Patients in Rajavithi Hospital. J. Med Assoc. Thail. 2017, 100, 96. [Google Scholar]
- McKee, P.A.; Castelli, W.P.; McNamara, P.M.; Kannel, W.B. The Natural History of Congestive Heart Failure: The Framingham Study. N. Engl. J. Med. 1971, 285, 1441–1446. [Google Scholar] [CrossRef]
- Maisel, A.; Mueller, C.; Adams, K.; Anker, S.D.; Aspromonte, N.; Cleland, J.G.F.; Cohen-Solal, A.; Dahlstrom, U.; DeMaria, A.; Di Somma, S.; et al. State of the art: Using natriuretic peptide levels in clinical practice. Eur. J. Heart Fail. 2008, 10, 824–839. [Google Scholar] [CrossRef]
- Januzzi, J.L. Natriuretic peptide testing: A window into the diagnosis and prognosis of heart failure. Cleve. Clin. J. Med. 2006, 73, 149–152, 155–157. [Google Scholar] [CrossRef]
- Gaggin, H.K.; Januzzi, J.L. The past, the present, and the future of natriuretic peptides in the diagnosis of heart failure. Eur. Heart J. Suppl. 2018, 20, G11–G20. [Google Scholar] [CrossRef]
- Ponikowski, P.; Voors, A.A.; Anker, S.D.; Bueno, H.; Cleland, J.G.F.; Coats, A.J.S.; Falk, V.; González-Juanatey, J.R.; Harjola, V.-P.; Jankowska, E.A.; et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC)Developed with the special contribution of the Heart Failure Association (HFA) of the ESC. Eur. Heart J. 2016, 37, 2129–2200. [Google Scholar] [CrossRef]
- Díez-Villanueva, P.; Alfonso, F. Heart failure in the elderly. J. Geriatr. Cardiol. 2016, 13, 115–117. [Google Scholar] [CrossRef]
- Nishino, M.; Matsuhiro, Y.; Nakamura, H.; Yasumoto, K.; Yasumura, K.; Tanaka, A.; Matsunaga-Lee, Y.; Nakamura, D.; Yano, M.; Yamato, M.; et al. Which factors are associated with length of stay in older patients with acute decompensated heart failure with preserved ejection fraction? AURORA study. Geriatr. Gerontol. Int. 2019, 19, 1084–1087. [Google Scholar] [CrossRef] [PubMed]
- Ziff, O.J.; Carter, P.R.; McGowan, J.; Uppal, H.; Chandran, S.; Russell, S.; Bainey, K.R.; Potluri, R. The interplay between atrial fibrillation and heart failure on long-term mortality and length of stay: Insights from the, United Kingdom ACALM registry. Int. J. Cardiol. 2018, 252, 117–121. [Google Scholar] [CrossRef] [PubMed]
- Sato, Y.; Yoshihisa, A.; Oikawa, M.; Nagai, T.; Yoshikawa, T.; Saito, Y.; Yamamoto, K.; Takeishi, Y.; Anzai, T. Relation of Systolic Blood Pressure on the Following Day with Post-Discharge Mortality in Hospitalized Heart Failure Patients with Preserved Ejection Fraction. Int. Heart J. 2019, 60, 876–885. [Google Scholar] [CrossRef]
- Shoaib, A.; Waleed, M.; Khan, S.; Raza, A.; Zuhair, M.; Kassianides, X.; Djahit, A.; Goode, K.; Wong, K.; Rigby, A.; et al. Breathlessness at rest is not the dominant presentation of patients admitted with heart failure. Eur. J. Heart Fail. 2014, 16, 1283–1291. [Google Scholar] [CrossRef] [PubMed]
- Ambrosy, A.P.; Fonarow, G.C.; Butler, J.; Chioncel, O.; Greene, S.J.; Vaduganathan, M.; Nodari, S.; Lam, C.S.P.; Sato, N.; Shah, A.N.; et al. The global health and economic burden of hospitalizations for heart failure: Lessons learned from hospitalized heart failure registries. J. Am. Coll. Cardiol. 2014, 63, 1123–1133. [Google Scholar] [CrossRef] [PubMed]
- Mwita, J.C.; Dewhurst, M.J.; Magafu, M.G.; Goepamang, M.; Omech, B.; Majuta, K.L.; Gaenamong, M.; Palai, T.B.; Mosepele, M.; Mashalla, Y. Presentation and mortality of patients hospitalised with acute heart failure in Botswana. Cardiovasc. J. Afr. 2017, 28, 112–117. [Google Scholar] [CrossRef][Green Version]
- Berra, G.; Garin, N.; Stirnemann, J.; Jannot, A.-S.; Martin, P.-Y.; Perrier, A.; Carballo, S. Outcome in Acute Heart Failure: Prognostic Value of Acute Kidney Injury and Worsening Renal Function. J. Card. Fail. 2015, 21, 382–390. [Google Scholar] [CrossRef]
- Adams, K.F.; Fonarow, G.C.; Emerman, C.L.; LeJemtel, T.H.; Costanzo, M.R.; Abraham, W.T.; Berkowitz, R.L.; Galvao, M.; Horton, D.P. ADHERE Scientific Advisory Committee and Investigators Characteristics and outcomes of patients hospitalized for heart failure in the United States: Rationale, design, and preliminary observations from the first 100,000 cases in the Acute Decompensated Heart Failure National Registry (ADHERE). Am. Heart J. 2005, 149, 209–216. [Google Scholar] [CrossRef]
- Cleland, J.G.F.; Swedberg, K.; Follath, F.; Komajda, M.; Cohen-Solal, A.; Aguilar, J.C.; Dietz, R.; Gavazzi, A.; Hobbs, R.; Korewicki, J.; et al. The EuroHeart Failure survey programme—A survey on the quality of care among patients with heart failure in EuropePart 1: Patient characteristics and diagnosis. Eur. Heart J. 2003, 24, 442–463. [Google Scholar] [CrossRef]
- Nieminen, M.S.; Brutsaert, D.; Dickstein, K.; Drexler, H.; Follath, F.; Harjola, V.-P.; Hochadel, M.; Komajda, M.; Lassus, J.; Lopez-Sendon, J.L.; et al. EuroHeart Failure Survey II (EHFS II): A survey on hospitalized acute heart failure patients: Description of population. Eur. Heart J. 2006, 27, 2725–2736. [Google Scholar] [CrossRef]
- Shiga, T.; Suzuki, A.; Haruta, S.; Mori, F.; Ota, Y.; Yagi, M.; Oka, T.; Tanaka, H.; Murasaki, S.; Yamauchi, T.; et al. Clinical characteristics of hospitalized heart failure patients with preserved, mid-range, and reduced ejection fractions in Japan. ESC Heart Fail. 2019, 6, 475–486. [Google Scholar] [CrossRef] [PubMed]
- Yancy, C.W.; Jessup, M.; Bozkurt, B.; Butler, J.; Casey, D.E.; Drazner, M.H.; Fonarow, G.C.; Geraci, S.A.; Horwich, T.; Januzzi, J.L.; et al. 2013 ACCF/AHA Guideline for the Management of Heart Failure. Circulation 2013, 128, e240–e327. [Google Scholar] [CrossRef] [PubMed]
- Arnold, J.M.O.; Liu, P.; Howlett, J.; Ignaszewski, A.; Leblanc, M.-H.; Kaan, A.; Pearce, C.; Sinclair, L.; Pearce, S.; Prentice, C. Ten year survival by NYHA functional class in heart failure outpatients referred to specialized multidisciplinary heart failure clinics 1999 to 2011. Eur. Heart J. 2013, 34. [Google Scholar] [CrossRef]
- Kajimoto, K.; Sato, N. Sex Differences in New York Heart Association Functional Classification and Survival in Acute Heart Failure Patients With Preserved or Reduced Ejection Fraction. Can. J. Cardiol. 2020, 36, 30–36. [Google Scholar] [CrossRef]
- Zaprutko, J.; Michalak, M.; Nowicka, A.; Dankowski, R.; Drożdż, J.; Ponikowski, P.; Opolski, G.; Nessler, J.; Nowalany-Kozielska, E.; Szyszka, A. Hospitalisation length and prognosis in heart failure patients. Kardiol. Pol. 2017, 75, 323–331. [Google Scholar] [CrossRef]
- Ahmed, A.; Aronow, W.S.; Fleg, J.L. Higher New York Heart Association classes and increased mortality and hospitalization in patients with heart failure and preserved left ventricular function. Am. Heart J. 2006, 151, 444–450. [Google Scholar] [CrossRef]
- Nafiu, O.O.; Gillespie, B.W.; Tsodikov, A. Continuous Variable Transformation in AnesthesiaUseful Clinical Shorthand, but Threat to Research. Anesthesiology 2015, 123, 504–506. [Google Scholar] [CrossRef]
- Dawson, N.V.; Weiss, R. Dichotomizing Continuous Variables in Statistical Analysis: A Practice to Avoid. Med. Decis. Mak. 2012, 32, 225–226. [Google Scholar] [CrossRef]
- Pascual-Figal, D.A.; Caballero, L.; Sanchez-Mas, J.; Lax, A. Prognostic markers for acute heart failure. Expert Opin. Med. Diagn. 2013, 7, 379–392. [Google Scholar] [CrossRef]
- Lee, D.S.; Austin, P.C.; Rouleau, J.L.; Liu, P.P.; Naimark, D.; Tu, J.V. Predicting mortality among patients hospitalized for heart failure: Derivation and validation of a clinical model. JAMA 2003, 290, 2581–2587. [Google Scholar] [CrossRef]
- Prekker, M.E.; Feemster, L.C.; Hough, C.L.; Carlbom, D.; Crothers, K.; Au, D.H.; Rea, T.D.; Seymour, C.W. The Epidemiology and Outcome of Prehospital Respiratory Distress. Acad. Emerg. Med. 2014, 21, 543–550. [Google Scholar] [CrossRef] [PubMed]
- Siniorakis, E.; Arvanitakis, S.; Tsitsimpikou, C.; Tsarouhas, K.; Tzevelekos, P.; Panta, S.; Aivalioti, F.; Zampelis, C.; Triposkiadis, F.; Limberi, S. Acute Heart Failure in the Emergency Department: Respiratory Rate as a Risk Predictor. In Vivo 2018, 32, 921–925. [Google Scholar] [CrossRef] [PubMed]
- Ebner, N.; Jankowska, E.A.; Ponikowski, P.; Lainscak, M.; Elsner, S.; Sliziuk, V.; Steinbeck, L.; Kube, J.; Bekfani, T.; Scherbakov, N.; et al. The impact of iron deficiency and anaemia on exercise capacity and outcomes in patients with chronic heart failure. Results from the Studies Investigating Co-morbidities Aggravating Heart Failure. Int. J. Cardiol. 2016, 205, 6–12. [Google Scholar] [CrossRef] [PubMed]
- Edelmann, F.; Stahrenberg, R.; Gelbrich, G.; Durstewitz, K.; Angermann, C.E.; Düngen, H.-D.; Scheffold, T.; Zugck, C.; Maisch, B.; Regitz-Zagrosek, V.; et al. Contribution of comorbidities to functional impairment is higher in heart failure with preserved than with reduced ejection fraction. Clin. Res. Cardiol. 2011, 100, 755–764. [Google Scholar] [CrossRef] [PubMed]
- Felker, G.M.; Gattis, W.A.; Leimberger, J.D.; Adams, K.F.; Cuffe, M.S.; Gheorghiade, M.; O’Connor, C.M. Usefulness of anemia as a predictor of death and rehospitalization in patients with decompensated heart failure. Am. J. Cardiol. 2003, 92, 625–628. [Google Scholar] [CrossRef]
- Ezekowitz, J.A.; McAlister, F.A.; Armstrong, P.W. Anemia is common in heart failure and is associated with poor outcomes: Insights from a cohort of 12 065 patients with new-onset heart failure. Circulation 2003, 107, 223–225. [Google Scholar] [CrossRef]
- Young, J.B.; Abraham, W.T.; Albert, N.M.; Gattis Stough, W.; Gheorghiade, M.; Greenberg, B.H.; O’Connor, C.M.; She, L.; Sun, J.L.; Yancy, C.W.; et al. Relation of low hemoglobin and anemia to morbidity and mortality in patients hospitalized with heart failure (insight from the OPTIMIZE-HF registry). Am. J. Cardiol. 2008, 101, 223–230. [Google Scholar] [CrossRef]
- Martín-Sánchez, F.J.; Carbajosa, V.; Llorens, P.; Herrero, P.; Jacob, J.; Miró, Ò.; Fernández, C.; Bueno, H.; Calvo, E.; Ribera Casado, J.M. Length of stay in patients admitted for acute heart failure. Gac. Sanit. 2016, 30, 191–200. [Google Scholar] [CrossRef]
- Halawa, A.; Burton, M.C.; Maniaci, M.J.; Shapiro, B.P.; Yip, D.S.; Hodge, D.O.; Vargas, E.R.; Dawson, N. Association of Anemia with Outcomes of Acute Heart Failure. South. Med. J. 2018, 111, 103–108. [Google Scholar] [CrossRef]
- Caughey, M.C.; Avery, C.L.; Ni, H.; Solomon, S.D.; Matsushita, K.; Wruck, L.M.; Rosamond, W.D.; Loehr, L.R. Outcomes of Patients with Anemia and Acute Decompensated Heart Failure with Preserved versus Reduced Ejection Fraction (From the ARIC Study Community Surveillance). Am. J. Cardiol. 2014, 114, 1850–1854. [Google Scholar] [CrossRef]
- Horwich, T.B.; Kalantar-Zadeh, K.; MacLellan, R.W.; Fonarow, G.C. Albumin levels predict survival in patients with systolic heart failure. Am. Heart J. 2008, 155, 883–889. [Google Scholar] [CrossRef] [PubMed]
- Liu, M.; Chan, C.-P.; Yan, B.P.; Zhang, Q.; Lam, Y.-Y.; Li, R.-J.; Sanderson, J.E.; Coats, A.J.S.; Sun, J.-P.; Yip, G.W.-K.; et al. Albumin levels predict survival in patients with heart failure and preserved ejection fraction. Eur. J. Heart Fail. 2012, 14, 39–44. [Google Scholar] [CrossRef] [PubMed]
- Bonilla-Palomas, J.L.; Gámez-López, A.L.; Moreno-Conde, M.; López-Ibáñez, M.C.; Anguita-Sánchez, M.; Gallego de la Sacristana, A.; García-Catalán, F.; Villar-Ráez, A. Hypoalbuminemia in acute heart failure patients: Causes and its impact on hospital and long-term mortality. J. Card. Fail. 2014, 20, 350–358. [Google Scholar] [CrossRef] [PubMed]
- Nohria, A.; Tsang, S.W.; Fang, J.C.; Lewis, E.F.; Jarcho, J.A.; Mudge, G.H.; Stevenson, L.W. Clinical assessment identifies hemodynamic profiles that predict outcomes in patients admitted with heart failure. J. Am. Coll. Cardiol. 2003, 41, 1797–1804. [Google Scholar] [CrossRef]
- Kinugasa, Y.; Kato, M.; Sugihara, S.; Hirai, M.; Yamada, K.; Yanagihara, K.; Yamamoto, K. Geriatric nutritional risk index predicts functional dependency and mortality in patients with heart failure with preserved ejection fraction. Circ. J. 2013, 77, 705–711. [Google Scholar] [CrossRef]
- Anand, I.S.; Latini, R.; Florea, V.G.; Kuskowski, M.A.; Rector, T.; Masson, S.; Signorini, S.; Mocarelli, P.; Hester, A.; Glazer, R.; et al. C-reactive protein in heart failure: Prognostic value and the effect of valsartan. Circulation 2005, 112, 1428–1434. [Google Scholar] [CrossRef]
- Bonilla-Palomas, J.L.; Gámez-López, A.L.; Anguita-Sánchez, M.P.; Castillo-Domínguez, J.C.; García-Fuertes, D.; Crespin-Crespin, M.; López-Granados, A.; Suárez de Lezo, J. Impact of Malnutrition on Long-Term Mortality in Hospitalized Patients With Heart Failure. Rev. Esp. Cardiol. 2011, 64, 752–758. [Google Scholar] [CrossRef]
- Cheng, Y.-L.; Sung, S.-H.; Cheng, H.-M.; Hsu, P.-F.; Guo, C.-Y.; Yu, W.-C.; Chen, C.-H. Prognostic Nutritional Index and the Risk of Mortality in Patients With Acute Heart Failure. J. Am. Heart Assoc. 2017, 6. [Google Scholar] [CrossRef]
- Tevik, K.; Thürmer, H.; Husby, M.I.; de Soysa, A.K.; Helvik, A.-S. Nutritional risk screening in hospitalized patients with heart failure. Clin. Nutr. 2015, 34, 257–264. [Google Scholar] [CrossRef]
- Alnajashi, M.A.; Almasoud, M.A.; Aldaham, S.A.; Acuña, J.M.; Zevallos, J.C. Association of gender and length of stay among Puerto Ricans hospitalized with decompensated heart failure. Medicine 2016, 95. [Google Scholar] [CrossRef]
- Bo, M.; Fonte, G.; Pivaro, F.; Bonetto, M.; Comi, C.; Giorgis, V.; Marchese, L.; Isaia, G.; Maggiani, G.; Furno, E.; et al. Prevalence of and factors associated with prolonged length of stay in older hospitalized medical patients. Geriatr. Gerontol. Int. 2016, 16, 314–321. [Google Scholar] [CrossRef] [PubMed]
- Teixeira, A.; Arrigo, M.; Tolppanen, H.; Gayat, E.; Laribi, S.; Metra, M.; Seronde, M.F.; Cohen-Solal, A.; Mebazaa, A. Management of acute heart failure in elderly patients. Arch. Cardiovasc. Dis. 2016, 109, 422–430. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, N.E.; Burnett, J.C.; Butler, J.; Camacho, A.; Felker, G.M.; Fiuzat, M.; O’Connor, C.; Solomon, S.D.; Vaduganathan, M.; Zile, M.R.; et al. Natriuretic Peptides as Inclusion Criteria in Clinical Trials: A JACC: Heart Failure Position Paper. J. Am. Coll. Cardiol. HF 2020, 8, 347–358. [Google Scholar] [CrossRef]
| Characteristics | Mean ± SD or n (%) |
|---|---|
| Age (years) | 74.2 ± 12.5 |
| Gender | |
| Male | 128 (62%) |
| Female | 79 (38%) |
| Ethnicity | |
| Thai | 204 (99%) |
| Non-Thai | 3 (1%) |
| Underlying conditions | |
| Chronic kidney disease | 99 (48%) |
| Ischemic heart disease | 84 (41%) |
| Diabetic Mellitus | 105 (51%) |
| Atrial fibrillation | 84 (41%) |
| NYHA class | |
| 0-I | 36 (17%) |
| II | 54 (26%) |
| III | 92 (45%) |
| IV | 25 (12%) |
| Vital signs | |
| BT (Celsius) | 36.8 ± 0.6 |
| SBP (mmHg) | 152.4 ± 36.0 |
| HR (/min) | 90.6 ± 24.7 |
| RR (/min) | 25.5 ± 5.0 |
| Oxygen saturation (%) | 93.5 ± 5.4 |
| Biochemistry | |
| NT-ProBNP (pg/mL) | 14,240.1 ± 18,384.5 |
| Serum Na (mmol/L) | 136.8 ± 5.8 |
| Hb (g/dL) | 10.8 ± 2.1 |
| Alb (g/dL) | 3.0 ± 0.5 |
| Predictors | LOS (hours) Poisson Mean (SE) | Univariable Model | Multivariable Model | |||
|---|---|---|---|---|---|---|
| with Predictor | without Predictor | LOS Difference (hours) (95%CI) | p-Value | LOS Difference (hours) (95%CI) | p-Value | |
| Demographic | ||||||
| Age > 65 years | 148.7 (1.0) | 72.8 (1.2) | 75.9 (72.9,79.0) | <0.001 | 40.5 (−7.3, 88.3) | 0.097 |
| Male | 132.3 (1.3) | 130.4 (1.0) | 1.8 (−1.4, 5.1) | 0.259 | 21.8 (−37.3, 80.9) | 0.469 |
| Comorbidities | ||||||
| Chronic kidney disease | 151.9 (1.2) | 112.1 (1.0) | 39.8 (36.6, 42.9) | <0.001 | 2.4 (−50.3, 55.2) | 0.928 |
| Ischemic heart disease | 150.6 (1.3) | 117.8 (1.0) | 32.8 (29.5, 36.0) | <0.001 | 33.0 (−1.7, 81.7) | 0.185 |
| Diabetic mellitus | 145.7 (1.2) | 116.1 (1.1) | 29.6 (26.5, 32.7) | <0.001 | 8.8 (−47.6, 65.2) | 0.759 |
| Atrial fibrillation | 146.5 (1.3) | 120.7 (1.0) | 25.8 (22.6, 29.1) | <0.001 | 38.7 (−18.0, 95.4) | 0.181 |
| NYHA functional class | ||||||
| III/IV | 163.3 (1.2) | 89.3 (1.0) | 73.9 (70.9, 77.0) | <0.001 | 72.9 (23.9, 121.8) | 0.004 |
| Vital signs | ||||||
| SBP (mmHg) | ||||||
| <100 | 104.5 (3.9) | 146.8 (1.3) | −42.4 (−50.4, −34.4) | <0.001 | −48.0 (−130.7, 34.6) | 0.255 |
| 100–140 | Reference | Reference | Reference | |||
| >140 | 121.4 (1.0) | 146.8 (1.3) | −25.5 (−28.7, −22.2) | <0.001 | −14.9 (−67.4, 37.6) | 0.579 |
| RR > 24 (/minute) | 180.2 (1.4) | 94.1 (0.9) | 86.0 (82.7, 89.3) | <0.001 | 80.7 (28.0, 133.3) | 0.003 |
| Biochemistry | ||||||
| NT-ProBNP ≥ 1800 pg/mL | 138.1 (0.9) | 95.5 (1.7) | 42.6 (38.9, 46.3) | <0.001 | 16.1 (−1.4, 73.6) | 0.583 |
| Serum Na < 135 mmol/L | 154.0 (1.4) | 118.4 (0.9) | 35.6 (32.2, 39.0) | <0.001 | 7.7 (−50.1, 65.4) | 0.794 |
| Hb < 10 g/dL | 174.5 (1.4) | 98.5 (0.9) | 76.0 (72.7, 79.3) | <0.001 | 60.4 (8.6, 112.3) | 0.022 |
| Alb < 3.5 g/dL | 146.7 (0.9) | 59.5 (1.3) | 87.2 (84.1, 90.3) | <0.001 | 52.8 (3.6, 102.0) | 0.035 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Sricharoen, P.; Phinyo, P.; Patumanond, J.; Piyayotai, D.; Sittichanbuncha, Y.; Yuksen, C.; Likittanasombat, K.; Cheuathonghua, E. Clinical Predictors Influencing the Length of Stay in Emergency Department Patients Presenting with Acute Heart Failure. Medicina 2020, 56, 434. https://doi.org/10.3390/medicina56090434
Sricharoen P, Phinyo P, Patumanond J, Piyayotai D, Sittichanbuncha Y, Yuksen C, Likittanasombat K, Cheuathonghua E. Clinical Predictors Influencing the Length of Stay in Emergency Department Patients Presenting with Acute Heart Failure. Medicina. 2020; 56(9):434. https://doi.org/10.3390/medicina56090434
Chicago/Turabian StyleSricharoen, Pungkava, Phichayut Phinyo, Jayanton Patumanond, Dilok Piyayotai, Yuwares Sittichanbuncha, Chaiyaporn Yuksen, Khanchit Likittanasombat, and Ekpaiboon Cheuathonghua. 2020. "Clinical Predictors Influencing the Length of Stay in Emergency Department Patients Presenting with Acute Heart Failure" Medicina 56, no. 9: 434. https://doi.org/10.3390/medicina56090434
APA StyleSricharoen, P., Phinyo, P., Patumanond, J., Piyayotai, D., Sittichanbuncha, Y., Yuksen, C., Likittanasombat, K., & Cheuathonghua, E. (2020). Clinical Predictors Influencing the Length of Stay in Emergency Department Patients Presenting with Acute Heart Failure. Medicina, 56(9), 434. https://doi.org/10.3390/medicina56090434





