Evaluation of Aqueous Maceration and Ultrasound-Assisted Extracts of Physalis philadelphica Lam. Solanaceae Husk on Hyperglycemia, Insulin Resistance, Hepatic Steatosis, and Oxidative Stress Markers in Obese Rats
Abstract
1. Introduction
2. Results
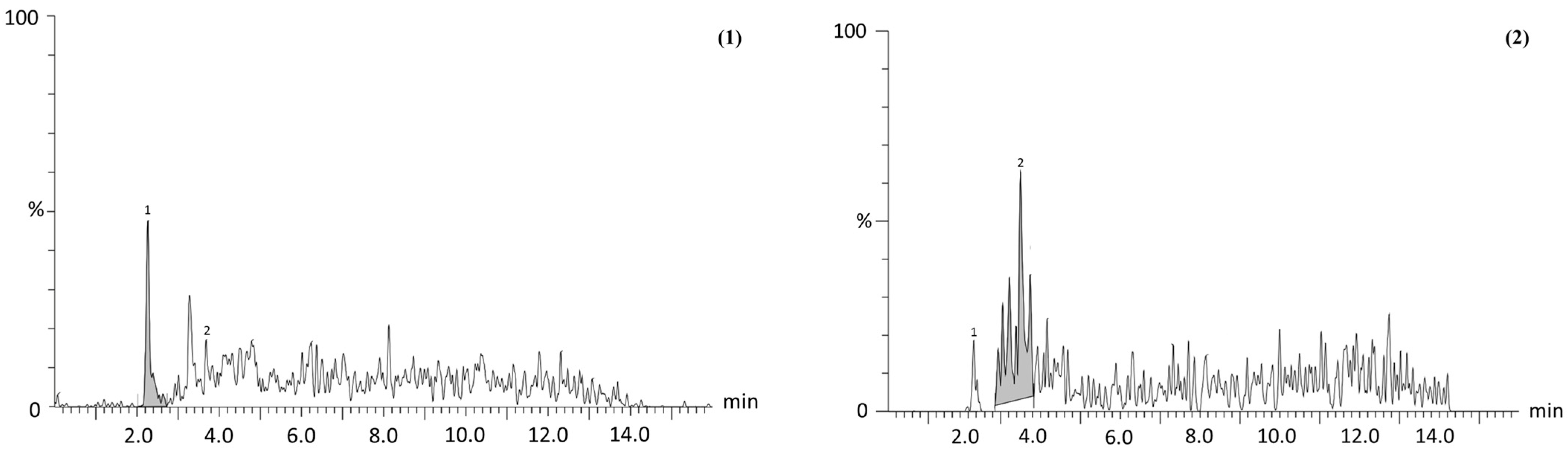
2.1. PH Values, Yields, and Chemical Characterization
2.2. Carbohydrate and Lipid Absorption Assessment
2.3. Effects of P. philadelphica Husk Extracts on Body Weight Gain, Lipid Profile, Fasting Glucose, Insulin Levels, and Insulin Resistance in Obese Rats
2.4. Effects of Physalis philadelphica Husk Extracts on Steatosis and Hepatic Triglyceride Content in Obese Rats
2.5. Effects of Physalis philadelphica Husk Extracts on Oxidative Stress Markers in Obese Rats
2.5.1. Nitric Oxide End Products (NOend-PD) and Lipid Peroxidation
2.5.2. Antioxidant Enzyme Activity
3. Discussion
4. Materials and Methods
4.1. Plant Material and Extracts
4.2. Physalis Philadelphica Husk Extract Extraction
4.3. Solid Yields and Chemical Characterization
4.4. Experimental Animals
4.5. Carbohydrate and Lipid Absorption Assessment
4.6. Obesity Induction
4.7. Blood Sampling and Liver Dissection
4.8. Serum Measurements
4.9. Serum Insulin Concentration and Insulin Resistance Assessment
4.10. Tissue Homogenate
4.11. Hepatic TG Content
4.12. Hepatic Steatosis Evaluation
4.13. Oxidative Stress Assessment
4.13.1. Lipid Peroxidation
4.13.2. End Products of Nitric Oxide (NOend-PD)
4.13.3. Catalase (CAT) Activity
4.13.4. Superoxide Dismutase (SOD) Activity
4.14. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| He-M | Husk extract obtained after maceration |
| He-US | Husk extract obtained by ultrasound |
| OSTT | Oral starch tolerance test |
| OLTT | Oral lipid tolerance test |
| FFAs | Free fatty acids |
| CAT | Catalase |
| SOD | Superoxide dismutase |
| NO | Nitric oxide |
| NOend-PD | Nitric oxide end products |
| IR | Insulin resistance |
| HOMA-IR | Homeostatic Model Assessment |
| MDA | Malondialdehyde |
| TC | Total cholesterol |
| TG | Triglyceride |
References
- Čolak, E.; Pap, D. The role of oxidative stress in the development of obesity and obesity-related metabolic disorders. J. Med. Biochem. 2021, 40, 1–9. [Google Scholar] [CrossRef]
- Klein, S.; Gastaldelli, A.; Yki-Järvinen, H.; Scherer, P.E. Why does obesity cause diabetes? Cell Metab. 2022, 34, 11–20. [Google Scholar] [CrossRef]
- Neeland, I.J.; Ross, R.; Després, J.P.; Matsuzawa, Y.; Yamashita, S.; Shai, I.; Seidell, J.; Magni, P.; Santos, R.D.; Arsenault, B.; et al. Visceral and ectopic fat, atherosclerosis, and cardiometabolic disease: A position statement. Lancet Diabetes Endocrinol. 2019, 7, 715–725. [Google Scholar] [CrossRef]
- Kojta, I.; Chacińska, M.; Błachnio-Zabielska, A. Obesity, bioactive lipids, and adipose tissue inflammation in insulin resistance. Nutrients 2020, 12, 1305. [Google Scholar] [CrossRef] [PubMed]
- Vatner, D.F.; Majumdar, S.K.; Kumashiro, N.; Petersen, M.C.; Rahimi, Y.; Gattu, A.K.; Bears, M.; Camporez, J.P.G.; Cline, G.W.; Jurczak, M.J.; et al. Insulin-independent regulation of hepatic triglyceride synthesis by fatty acids. Proc. Natl. Acad. Sci. USA 2015, 112, 1143–1148. [Google Scholar] [CrossRef] [PubMed]
- Nielsen, S.; Jensen, M.D. Insulin regulation of regional lipolysis in upper-body obese and lean humans. JCI Insight 2024, 9, e175629. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, H.; Kanuri, B.N.; Dikshit, M. Role of iNOS in insulin resistance and endothelial dysfunction. In Oxidative Stress in Heart Diseases; Springer: Singapore, 2019; pp. 461–482. [Google Scholar]
- Pacher, P.; Beckman, J.S.; Liaudet, L. Nitric oxide and peroxynitrite in health and disease. Physiol. Rev. 2007, 87, 315–424. [Google Scholar] [CrossRef]
- Friedman, S.L.; Neuschwander-Tetri, B.A.; Rinella, M.; Sanyal, A.J. Mechanisms of NAFLD development and therapeutic strategies. Nat. Med. 2018, 24, 908–922. [Google Scholar] [CrossRef]
- Fernández-Ramos, D.; Lopitz-Otsoa, F.; Delacruz-Villar, L.; Bilbao, J.; Pagano, M.; Mosca, L.; Bizkarguenaga, M.; Serrano-Macia, M.; Azkargorta, M.; Iruarrizaga-Lejarreta, M.; et al. Arachidyl amido cholanoic acid improves liver glucose and lipid homeostasis in nonalcoholic steatohepatitis via AMPK and mTOR regulation. WJG 2020, 26, 5101. [Google Scholar] [CrossRef]
- Tchang, B.G.; Aras, M.; Kumar, R.B.; Aronne, L.J. Pharmacologic Treatment of Overweight and Obesity in Adults. Endotext; 2024. Available online: https://www.ncbi.nlm.nih.gov/sites/books/NBK279038/ (accessed on 1 August 2025).
- Pino-de la Fuente, F.; Nocetti, D.; Sacristán, C.; Ruiz, P.; Guerrero, J.; Jorquera, G.; Uribe, E.; Bucarey, J.L.; Espinosa, A.; Puente, L. Physalis peruviana L. pulp prevents liver inflammation and insulin resistance in skeletal muscles of diet-induced obese mice. Nutrients 2020, 12, 700. [Google Scholar] [CrossRef]
- Lee, Y.Y.; Kim, M.; Irfan, M.; Kim, S.H.; Kim, S.D.; Rhee, M.H. Physalis alkekengi exhibits antiobesity effects in mice with potential of inducing white adipose tissue browning. J. Med. Food. 2020, 23, 312–318. [Google Scholar] [CrossRef]
- Moussa, S.A.A.; Ibrahim, F.A.; Abd-Elbaset, M.; Aziz, S.W.; Morsy, F.A.; Abdellatif, N.; Attia, A.; El-Toumy, S.A.; Salib, J.Y.; Bashandy, S.A. Goldenberry (Physalis peruviana) alleviates hepatic oxidative stress and metabolic syndrome in obese rats. J. Appl. Pharm. Sci. 2022, 12, 138–150. [Google Scholar]
- Guerrero-Romero, F.; Simental-Mendía, L.E.; Guerra Rosas, M.I.; Sayago-Monreal, V.I.; Morales Castro, J.; Gamboa-Gómez, C.I. Hypoglycemic and antioxidant effects of green tomato (Physalis ixocarpa Brot.) calyxes’ extracts. J. Food Biochem. 2021, 45, e13678. [Google Scholar] [CrossRef]
- Mazova, N.; Popova, V.; Stoyanova, A. Phytochemical composition and biological activity of Physalis spp.: A mini review. Food Sci. Appl. Biotechnol. 2020, 3, 56–70. [Google Scholar] [CrossRef]
- Mulato-Brito, J.; Peña-Lomelí, A. Germplasm evaluation of to- matillo (Physalis ixocarpa Brot.) cropped under Ontario, Canada and Chapingo, México environmental conditions. J. Veg. Crop. Prod. 2007, 66, 117–127. [Google Scholar]
- Svobodova, B.; Kuban, V. Solanaceae: A family well known and still surprising. In Phytochemicals in Vegetables: A Valuable Source of Bioactive Compounds; Bentham Science Publishers: Sharjah, United Arab Emirates, 2018; pp. 296–372. [Google Scholar]
- Lim, T.K. Physalis peruviana L. In Edible Medicinal and Nonmedicinal Plants: Fruits; SSBM: Geneva, Switzerland, 2013; pp. 300–309. [Google Scholar]
- Fischer, G.; Herrera, M. Cape gooseberry (Physalis peruviana L.). In Postharvest Biology and Technology of Tropical and Subtropical Fruits: Açai to Citrus; Woodhead: Cambridge, UK, 2011; Volume 2, pp. 374–396. [Google Scholar]
- Hu, H.X.; Xu, L.T.; Gao, H.; Lv, H.; Huang, M.; Fang, K.L.; Wang, S.Q.; Zhao, B.B.; Ren, D.M.; Wang, X.N.; et al. Chemical constituents from physalis calyx seu fructus and their inhibitory effects against oxidative stress and inflammatory response. Planta Med. 2020, 86, 1191–1203. [Google Scholar] [CrossRef] [PubMed]
- Khan, W.; Bakht, J.; Khan, B.M.; Naeem, I.; Uddin, M.N.; Padder, B.A. Morphometric and genetic characterization of medicinally important accessions of Physalis ixocarpa Brot. Bangladesh J. Bot. 2019, 48, 105–111. [Google Scholar] [CrossRef]
- González-Pérez, J.E.; Guerrero-Beltrán, J.Á. Tomatillo or husk tomato (Physalis philadelphica and Physalis ixocarpa): A review. Sci. Hortic. 2021, 288, 110306. [Google Scholar] [CrossRef]
- Kumar, K.; Yadav, A.N.; Kumar, V.; Vyas, P.; Dhaliwal, H.S. Food waste: A potential bioresource for extraction of nutraceuticals and bioactive compounds. Bioresour. Bioprocess. 2017, 4, 18. [Google Scholar] [CrossRef]
- Ameer, K.; Shahbaz, H.M.; Kwon, J.H. Green Extraction Methods for Polyphenols from Plant Matrices and Their Byproducts: A Review. Compr. Rev. Food Sci. Food Saf. 2017, 16, 295–315. [Google Scholar] [CrossRef]
- Hernández, I.; Alegre, L.; Van Breusegem, F.; Munné-Bosch, S. How relevant are flavonoids as antioxidants in plants? Trends Plant Sci. 2009, 14, 125–132. [Google Scholar] [CrossRef]
- Mathews, A.; Arbal, A.V.; Kaarunya, A.; Jha, P.K.; Le-Bail, A.; Rawson, A. Conventional vs Modern Extraction Techniques in the Food Industry. In Extraction Processes in the Food Industry; Woodhead: Cambridge, UK, 2024; pp. 97–146. [Google Scholar]
- Alifakı, Ö.; Şakıyan, Ö.; Isci, A. Extraction of Phenolic Compounds from Cranberrybush (Viburnum opulus L.) Fruit using ultrasound, microwave, and ultrasound—Microwave combination methods. J. Food Meas. Charact. 2022, 16, 4009–4024. [Google Scholar] [CrossRef]
- Đurović, S.; Domínguez-Valencia, R.; Pateiro, M.; Teslić, N.; Lorenzo, J.M.; Pavlic, B. Industrial Hemp Nutraceutical Processing and Technology. J. Ind. Hemp. 2022, 191–218. [Google Scholar]
- Piecko, J.; Mieszczakowska-Frąc, M.; Celejewska, K.; Szwejda-Grzybowska, J. Impact of Ultrasound Pretreatment on Juice Yield and Bioactive Content in Juice Produced from Selected Berries Fruit. Foods 2024, 13, 1231. [Google Scholar] [CrossRef]
- Shen, Y.; Zhu, D.; Xi, P.; Cai, T.; Cao, X.; Liu, H.; Li, J. Effects of temperature-controlled ultrasound treatment on sensory properties, physical characteristics and antioxidant activity of cloudy apple juice. LWT 2021, 142, 111030. [Google Scholar] [CrossRef]
- Cho, A.S.; Jeon, S.M.; Kim, M.J.; Yeo, J.; Seo, K.I.; Choi, M.S.; Lee, M.K. Chlorogenic acid exhibits anti-obesity property and improves lipid metabolism in high-fat diet-induced-obese mice. Food Chem. Toxicol. 2010, 48, 937–943. [Google Scholar] [CrossRef]
- Varshney, R.; Mishra, R.; Das, N.; Sircar, D.; Roy, P. A comparative analysis of various flavonoids in the regulation of obesity and diabetes: An in vitro and in vivo study. J. Funct. Foods 2019, 59, 194–205. [Google Scholar] [CrossRef]
- Oboh, G.; Agunloye, O.M.; Adefegha, S.A.; Akinyemi, A.J.; Ademiluyi, A.O. Caffeic and chlorogenic acids inhibit key enzymes linked to type 2 diabetes (in vitro): A comparative study. J. Basic Clin. Physiol. Pharmacol. 2015, 26, 165–170. [Google Scholar] [CrossRef] [PubMed]
- Shishikura, Y.; Khokhar, S.; Murray, B.S. Effects of tea polyphenols on emulsification of olive oil in a small intestine model system. J. Agric. Food Chem. 2006, 54, 1906–1913. [Google Scholar] [CrossRef] [PubMed]
- Fisher, M. Acarbose and alpha glucosidase inhibitors. Diabetes Drug Notes 2022, 229–238. [Google Scholar]
- Ioannides-Demos, L.L.; Piccenna, L.; McNeil, J.J. Pharmacotherapies for obesity: Past, current, and future therapies. J. Obes. 2011, 1, 179674. [Google Scholar] [CrossRef]
- Xu, J.; Ge, J.; He, X.; Sheng, Y.; Zheng, S.; Zhang, C.; Xu, W.; Huang, K. Caffeic acid reduces body weight by regulating gut microbiota in diet-induced-obese mice. J. Funct. Foods 2020, 74, 104061. [Google Scholar] [CrossRef]
- Dong, J.; Zhang, X.; Zhang, L.; Bian, H.X.; Xu, N.; Bao, B.; Liu, J. Quercetin reduces obesity-associated ATM infiltration and inflammation in mice: A mechanism including AMPKα1/SIRT1. J. Lipid Res. 2014, 55, 363–374. [Google Scholar] [CrossRef] [PubMed]
- Tucci, S. The role of lipid and carbohydrate digestive enzyme inhibitors in the management of obesity: A review of current and emerging therapeutic agents. Diabetes Metab. Syndr. Obes. 2010, 3, 125. [Google Scholar] [CrossRef]
- Hsu, C.Y.; Shih, H.Y.; Chia, Y.C.; Lee, C.H.; Ashida, H.; Lai, Y.K.; Weng, C.F. Rutin potentiates insulin receptor kinase to enhance insulin-dependent glucose transporter 4 translocation. Mol. Nutr. Food Res. 2014, 58, 1168–1176. [Google Scholar] [CrossRef]
- Ihara, Y.; Asahara, S.I.; Inoue, H.; Seike, M.; Ando, M.; Kabutoya, H.; Kimura-Koyanagi, M.; Kido, Y. Chlorogenic acid and caffeine in coffee restore insulin signaling in pancreatic beta cells. Kobe J. Med. Sci. 2023, 69, E1. [Google Scholar]
- Odbayar, T.O.; Badamhand, D.; Kimura, T.; Takahashi, Y.; Tsushida, T.; Ide, T. Comparative studies of some phenolic compounds (quercetin, rutin, and ferulic acid) affecting hepatic fatty acid synthesis in mice. J. Agric. Food Chem. 2006, 54, 8261–8265. [Google Scholar] [CrossRef]
- Fukaya, M.; Sato, Y.; Kondo, S.; Adachi, S.I.; Yoshizawa, F.; Sato, Y. Quercetin enhances fatty acid β-oxidation by inducing lipophagy in AML12 hepatocytes. Heliyon 2021, 7, e07324. [Google Scholar] [CrossRef]
- Boden, G. Fatty acid-induced inflammation and insulin resistance in skeletal muscle and liver. Curr. Diabetes Rev. 2006, 6, 177–181. [Google Scholar] [CrossRef]
- Lafay, S.; Gil-Izquierdo, A. Bioavailability of phenolic acids. Phytochem. Rev. 2008, 7, 301–311. [Google Scholar] [CrossRef]
- Zhao, Z.; Egashira, Y.; Sanada, H. Ferulic acid is quickly absorbed from rat stomach as the free form and then conjugated mainly in liver. J. Nutr. 2004, 134, 3083–3308. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez-Ramiro, I.; Vauzour, D.; Minihane, A.M. Polyphenols and non-alcoholic fatty liver disease: Impact and mechanisms. Proc. Nutr. Soc. 2016, 75, 47–60. [Google Scholar] [CrossRef]
- Xu, D.P.; Zheng, J.; Zhou, Y.; Li, Y.; Li, S.; Li, H.B. Ultrasound-assisted extraction of natural antioxidants from the flower of Limonium sinuatum: Optimization and comparison with conventional methods. Food Chem. 2017, 217, 552–559. [Google Scholar] [CrossRef]
- Toma, M.; Vinatoru, M.; Paniwnyk, L.; Mason, T.J. Investigation of the effects of ultrasound on vegetal tissues during solvent extraction. Ultrason. Sonochem. 2001, 8, 137–142. [Google Scholar] [CrossRef]
- Ji, M.; Gong, X.; Li, X.; Wang, C.; Li, M. Advanced research on the antioxidant activity and mechanism of polyphenols from Hippophae species—A review. Molecules 2020, 25, 917. [Google Scholar] [CrossRef]
- Cobaleda-Velasco, M.; Almaraz-Abarca, N.; Alanis-Bañuelos, R.E.; Uribe-Soto, J.N.; González-Valdez, L.S.; Muñoz-Hernández, G.; Rojas-López, M. Rapid determination of phenolics, flavonoids, and antioxidant properties of Physalis ixocarpa Brot. ex Hornem. and Physalis angulata L. by infrared spectroscopy and partial least squares. Anal. Lett. 2018, 51, 523–536. [Google Scholar] [CrossRef]
- Manach, C.; Scalbert, A.; Morand, C.; Rémésy, C.; Jiménez, L. Polyphenols: Food sources and bioavailability. Am. J. Clin. Nutr. 2004, 79, 727–747. [Google Scholar] [CrossRef]
- Del Rio, D.; Stalmach, A.; Calani, L.; Crozier, A. Bioavailability of coffee chlorogenic acids and green tea flavan-3-ols. Nutrients 2010, 2, 820–833. [Google Scholar] [CrossRef]
- Franco, L.A.; Ocampo, Y.C.; Gómez, H.A.; De la Puerta, R.; Espartero, J.L.; Ospina, L.F. Sucrose esters from Physalis peruviana calyces with anti-inflammatory activity. Planta Med. 2014, 80, 1605–1614. [Google Scholar] [CrossRef] [PubMed]
- Delcanale, P.; Hally, C.; Nonell, S.; Bonardi, S.; Viappiani, C.; Abbruzzetti, S. Photodynamic action of Hypericum perforatum hydrophilic extract against Staphylococcus aureus. Photochem. Photobiol. Sci. 2020, 19, 324–331. [Google Scholar] [CrossRef] [PubMed]
- Rivera-Mondragón, A.; Broeckx, G.; Bijttebier, S.; Naessens, T.; Fransen, E.; Kiekens, F.; Caballero-George, C.; Vander-Heyden, Y.; Apers, S.; Foubert, K. Ultrasound-assisted extraction optimization and validation of an HPLC-DAD method for the quantification of polyphenols in leaf extracts of Cecropia species. Sci. Rep. 2019, 9, 2028. [Google Scholar] [CrossRef] [PubMed]
- Ma, Y.Q.; Chen, J.C.; Liu, D.H.; Ye, X.Q. Simultaneous ex- traction of phenolic compounds of citrus peel extracts: Effect of ultrasound. Ultrason. Sonochem. 2009, 16, 57–62. [Google Scholar] [CrossRef]
- Safdar, M.N.; Kausar, T.; Jabbar, S.; Mumtaz, A.; Ahad, K.; Saddozai, A.A. Extraction and quantification of polyphenols from kinnow (Citrus reticulate L.) peel using ultrasound and maceration techniques. J. Food Drug Anal. 2017, 25, 488–500. [Google Scholar] [CrossRef] [PubMed]
- International Conference on Harmonization of Technical Requirements for Registration of Pharmaceuticals for Human Use: Validation of Analytical Procedures: Text and Methodology Q2 (ICH). 2005. Available online: http://www.ich.org/fileadmin/PublicWebSite/ICHProducts/Guidelines/Quality/Q2R1/Step4/Q2R1Guideline.pdf (accessed on 4 August 2024).
- Office of Laboratory Animal Welfare, National Institutes of Health (US). Public Health Service Policy on Humane Care and Use of Laboratory Animals. U.S. Department of Health and Human Services, 2002. Available online: https://olaw.nih.gov/ (accessed on 4 August 2024).
- Secretaría de Agricultura, Ganadería, Desarrollo Rural, Pesca y Alimentación. NOM-062-ZOO-1999: Especificaciones Técnicas para la Producción, Cuidado y uso de los Animales de Laboratorio. Diario Oficial de la Federación. 1999. Available online: https://www.adopta.mx/wp-content/uploads/2011/07/NOM-062-ZOO-Uso-de-los-Animales-de-Laboratorio-22-de-Agosto-de-2001-DOF.pdf (accessed on 12 March 2022).
- Serafini, M.; Peluso, I. Functional foods for health: The interrelated antioxidant and anti-inflammatory role of fruits, vegetables, herbs, spices and cocoa in humans. Curr. Pharm. Des. 2016, 22, 6701–6715. [Google Scholar] [CrossRef]
- Reagan-Shaw, S.; Nihal, M.; Ahmad, N. Dose translation from animal to human studies revisited. FASEB J. 2008, 22, 659–661. [Google Scholar] [CrossRef]
- Gamboa-Gómez, C.I.; Simental-Mendía, L.E.; González-Laredo, R.F.; Alcantar-Orozco, E.J.; Monserrat-Juarez, V.H.; Ramírez-España, J.C.; Gallegos-Infante, J.A.; Moreno-Jiméneza, M.R.; Rocha-Guzmán, N.E. In vitro and in vivo assessment of anti-hyperglycemic and antioxidant effects of Oak leaves (Quercus convallata and Quercus arizonica) infusions and fermented beverages. Int. Food Res. J. 2017, 102, 690–699. [Google Scholar] [CrossRef] [PubMed]
- Falholt, K.; Lund, B.; Falholt, W. An easy colorimetric micromethod for routine determination of free fatty acids in plasma. Clin. Chim. Acta 1973, 46, 105–111. [Google Scholar] [CrossRef]
- Gamboa-Gómez, C.I.; Salgado, L.M.; González-Gallardo, A.; Ramos-Gómez, M.; Loarca-Piña, G.; Reynoso-Camacho, R. Consumption of Ocimum sanctum L. and Citrus paradisi infusions modulates lipid metabolism and insulin resistance in obese rats. Food Funct. 2014, 5, 927–935. [Google Scholar] [CrossRef]
- Bradford, M.M. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal. Biochem. 1976, 72, 248–254. [Google Scholar] [CrossRef]
- Folch, J.; Lees, M.; Sloane Stanley, G.H. A simple method for the isolation and purification of total lipids from animal tissues. J. Biol. Chem. 1957, 226, 497–509. [Google Scholar] [CrossRef]
- Rocha-Guzmán, N.E.; Simental-Mendía, L.E.; Barragán-Zúñiga, L.J.; Ramírez-España, J.C.; Gallegos-Infante, J.A.; Lujan-Mendoza, C.I.; Gamboa-Gómez, C.I. Effect of Buddleja scordioides K. leaves infusion on lipid peroxidation in mice with ultraviolet light-induced oxidative stress. Med. Chem. Res. 2018, 27, 2379–2385. [Google Scholar] [CrossRef]
- Rábago-Velasco, M.; Cortez-Valero, H.; Aguilar-Parada, E.; Arellano-Pérez, H.; Vázquez-Chávez, C.; Jiménez-Villarruel, M. Malondialdehído plasmático en pacientes con diabetes mellitus tipo 2 y en pacientes con enfermedad coronaria. Gac. Med. Mex. 2000, 136, 23–30. [Google Scholar] [PubMed]
- Sastry, K.V.H.; Moudgal, R.P.; Mohan, J.; Tyagi, J.S.; Rao, G. Spectrophotometric determination of serum nitrite and nitrate by copper–cadmium alloy. Anal. Biochem. 2002, 306, 79–82. [Google Scholar] [CrossRef] [PubMed]
- Sinha, A.K. Colorimetric Assay of catalase. Anal. Biochem. 1972, 47, 389–394. [Google Scholar] [CrossRef] [PubMed]
- Ukeda, H.; Kawana, D.; Maeda, S.; Sawamura, M. Spectrofotometric assay for superoxide dismutase based on the reduction of highty water-soluble tetrazolium salts by xanthine-xanthine oxidase. Biosci. Biotechnol. Biochem. 1998, 63, 485–488. [Google Scholar] [CrossRef]




| No. | Compound | Transitions | RT (min) | LR (ng/mL) | CE (r2) | LOD (ng/mL) | LOQ (ng/mL) | He-M (ng/mg of Crude Extract) | He-US (ng/mg of Crude Extract) |
|---|---|---|---|---|---|---|---|---|---|
| 1 | Gallic acid | 169.15 > 125.05, 79.07 | 1.2 | 0–20 | 0.9973 | 0.03 | 0.09 | 0.33 ± 0.03 a | 0.45 ± 0.02 a |
| 2 | Protocatechuic acid | 153.1 >109.0, 91.04 | 2.1 | 0–24 | 0.9976 | 0.07 | 0.21 | 28.0 ± 0.60 a | 15.0 ± 1.20 b |
| 3 | Chlorogenic acid | 137.0 > 93.0 | 3.3 | 0–20 | 0.9983 | 0.3 | 0.9 | 3.00 ± 0.10 b | 24.0 ± 1.30 a |
| 4 | Vanillic acid | 167.1 > 123.0 | 3.7 | 0–20 | 0.9640 | 0.01 | 0.03 | 4.10 ± 0.40 a | 2.00 ± 0.30 b |
| 5 | Caffeic acid | 179.1 > 135.08, 89.09 | 3.9 | 0–32 | 0.9986 | 0.02 | 0.06 | 8.00 ± 0.05 b | 9.00 ± 0.50 a |
| 6 | Epicatechin | 289.1 > 245.1 | 4.3 | 0–20 | 0.9995 | 0.003 | 0.009 | 0.03 ± 0.00 a | 0.03 ± 0.00 a |
| 7 | Feruilic acid | 193.2 > 134.0, 178.07 | 5.7 | 0–32 | 0.9949 | 0.05 | 0.015 | 7.50 ± 0.30 a | 2.10 ± 0.1 b |
| 8 | Rutin | 609.2 > 300.2 | 5.8 | 0–20 | 0.9704 | 0.003 | 0.01 | 0.06 ± 0.00 b | 5.10 ± 0.20 a |
| 9 | Kaempferol-3-O-Glc | 447.3 > 255.1 | 6.7 | 0–20 | 0.9947 | 0.002 | 0.006 | 0.20 ± 0.00 b | 0.40 ± 0.00 a |
| 10 | Quercetin | 301.2 > 151.0 | 8.4 | 0–20 | 0.9898 | 0.001 | 0.003 | 4.00 ± 0.40 a | 1.50 ± 0.10 b |
| 11 | Luteolin | 285.2 > 133.0 | 8.5 | 0–20 | 0.9834 | 0.002 | 0.006 | 0.01 ± 0.00 a | 0.04 ± 0.00 a |
| 12 | Naringenin | 271.2 > 151.4, 119.06 | 9.2 | 0–20 | 0.9988 | 0.001 | 0.003 | Traces | 0.04 ± 0.00 a |
| * Standard Rodent Diet | Obesogenic Diet | ||
|---|---|---|---|
| Nutrients | % Per 100 g | Nutrients | % Per 100 g |
| Carbohydrates | 70.9 | Carbohydrates | 60.0 |
| Proteins | 13.9 | Proteins | 23.0 |
| Fat | 15.1 | Fat | 4.5 |
| Saturated fat | 3.9 | Saturated fat | -- |
| Polyunsaturated fat | 1.1 | Polyunsaturated fat | -- |
| Monosaturated fat | 4.5 | Monosaturated fat | -- |
| Ingredients | g per 100 g | ||
| Powdered standard rodent chow | 60 | ||
| Lard | 10 | ||
| Fructose | 30 | ||
| Total energy (kcal/100 g) | 372.5 | Total energy (kcal/100 g) | 511.1 |
| Healthy Control | Obese Control | He-M | He-US | |
|---|---|---|---|---|
| TG (mg/dL) | 140.0± 8.3 b | 154.6 ± 5.8 a | 158.1 ± 20.2 a | 150.8 ± 15.6 a |
| FFAs (µg/mL) | 24.83 ± 4.1 c | 59.3 ± 2.8 a | 36.5 ± 3.8 b | 28.3 ± 2.8 c |
| TC (mg/dL) | 68.1 ± 3.5 b | 180.6 ± 2.3 a | 65.8 ± 4.2 b | 68.1 ± 3.5 b |
| HDL-c (mg/dL) * | 28.8 (6.0–30.2) a | 30 (8.4–33.2) a | 24.4 (10.5–30.4) a | 23.4 (13–31.9) a |
| Sample | Serum (µM/mg protein) | Liver (µM/mg protein) | ||
|---|---|---|---|---|
| NOend-PD | MDA | NOend-PD | MDA | |
| Healthy control | 0. 21 ± 0.01 b | 1.26 ± 0.1 b | 0. 23 ± 0.00 c | 1.06 ± 0.1 c |
| Obese control | 0.52 ± 0.04 a | 1.74 ± 0.30 a | 0.45 ± 0.02 a | 2.83 ± 0.33 a |
| He-M | 0.45 ± 0.05 a | 1.61 ± 0.45 a | 0.36 ± 0.01 b | 1.92 ± 0.13 b |
| He-US | 0.48 ± 0.05 a | 2.10 ± 0.21 a | 0.30 ± 0.06 b | 2.63 ± 0.42 a |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Morales-Castro, J.; Barragán-Zúñiga, J.; Guerra-Rosas, M.I.; Sayago-Monreal, V.I.; Gónzalez, J.L.; Carlo-Ricartti, F.; Alvarado-Aguilar, A.; Guerrero-Romero, F.; Rodríguez-Morán, M.; Gamboa-Gómez, C.I. Evaluation of Aqueous Maceration and Ultrasound-Assisted Extracts of Physalis philadelphica Lam. Solanaceae Husk on Hyperglycemia, Insulin Resistance, Hepatic Steatosis, and Oxidative Stress Markers in Obese Rats. Pharmaceuticals 2025, 18, 1655. https://doi.org/10.3390/ph18111655
Morales-Castro J, Barragán-Zúñiga J, Guerra-Rosas MI, Sayago-Monreal VI, Gónzalez JL, Carlo-Ricartti F, Alvarado-Aguilar A, Guerrero-Romero F, Rodríguez-Morán M, Gamboa-Gómez CI. Evaluation of Aqueous Maceration and Ultrasound-Assisted Extracts of Physalis philadelphica Lam. Solanaceae Husk on Hyperglycemia, Insulin Resistance, Hepatic Steatosis, and Oxidative Stress Markers in Obese Rats. Pharmaceuticals. 2025; 18(11):1655. https://doi.org/10.3390/ph18111655
Chicago/Turabian StyleMorales-Castro, Juliana, Jazel Barragán-Zúñiga, María Inés Guerra-Rosas, Víctor Iván Sayago-Monreal, José Luis Gónzalez, Fabiola Carlo-Ricartti, Adrián Alvarado-Aguilar, Fernando Guerrero-Romero, Martha Rodríguez-Morán, and Claudia I. Gamboa-Gómez. 2025. "Evaluation of Aqueous Maceration and Ultrasound-Assisted Extracts of Physalis philadelphica Lam. Solanaceae Husk on Hyperglycemia, Insulin Resistance, Hepatic Steatosis, and Oxidative Stress Markers in Obese Rats" Pharmaceuticals 18, no. 11: 1655. https://doi.org/10.3390/ph18111655
APA StyleMorales-Castro, J., Barragán-Zúñiga, J., Guerra-Rosas, M. I., Sayago-Monreal, V. I., Gónzalez, J. L., Carlo-Ricartti, F., Alvarado-Aguilar, A., Guerrero-Romero, F., Rodríguez-Morán, M., & Gamboa-Gómez, C. I. (2025). Evaluation of Aqueous Maceration and Ultrasound-Assisted Extracts of Physalis philadelphica Lam. Solanaceae Husk on Hyperglycemia, Insulin Resistance, Hepatic Steatosis, and Oxidative Stress Markers in Obese Rats. Pharmaceuticals, 18(11), 1655. https://doi.org/10.3390/ph18111655









