Ocular Co-Delivery of Timolol and Brimonidine from a Self-Assembling Peptide Hydrogel for the Treatment of Glaucoma: In Vitro and Ex Vivo Evaluation
Abstract
1. Introduction
2. Results and Discussion
2.1. Rheological Studies
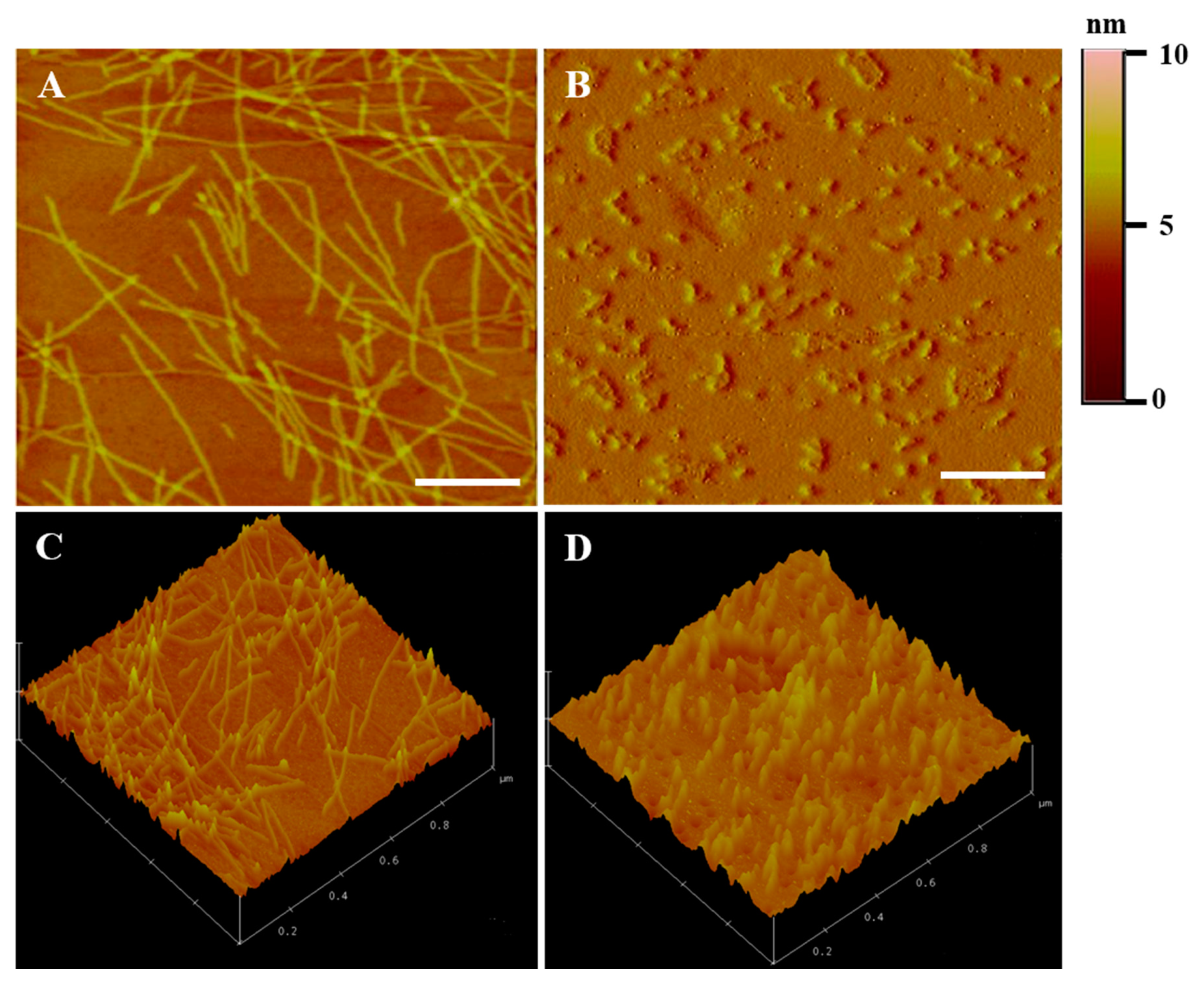
2.2. Atomic Force Microscopy (AFM) Characterization
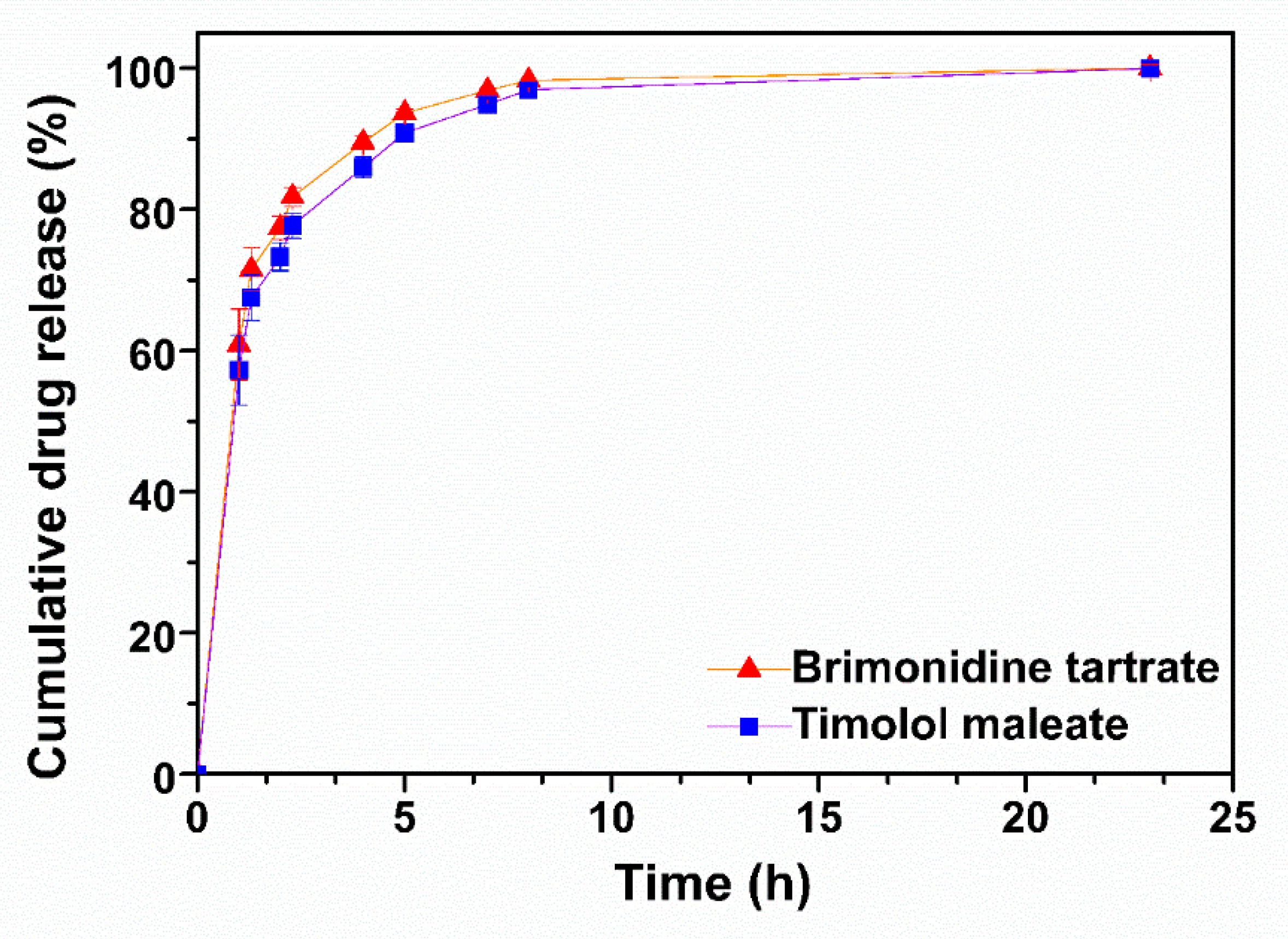
2.3. In Vitro Release Study of TM and BR from the Self-Assembling Peptide ac-(RADA)4-CONH2 in Simulated Tear Fluid (STF)
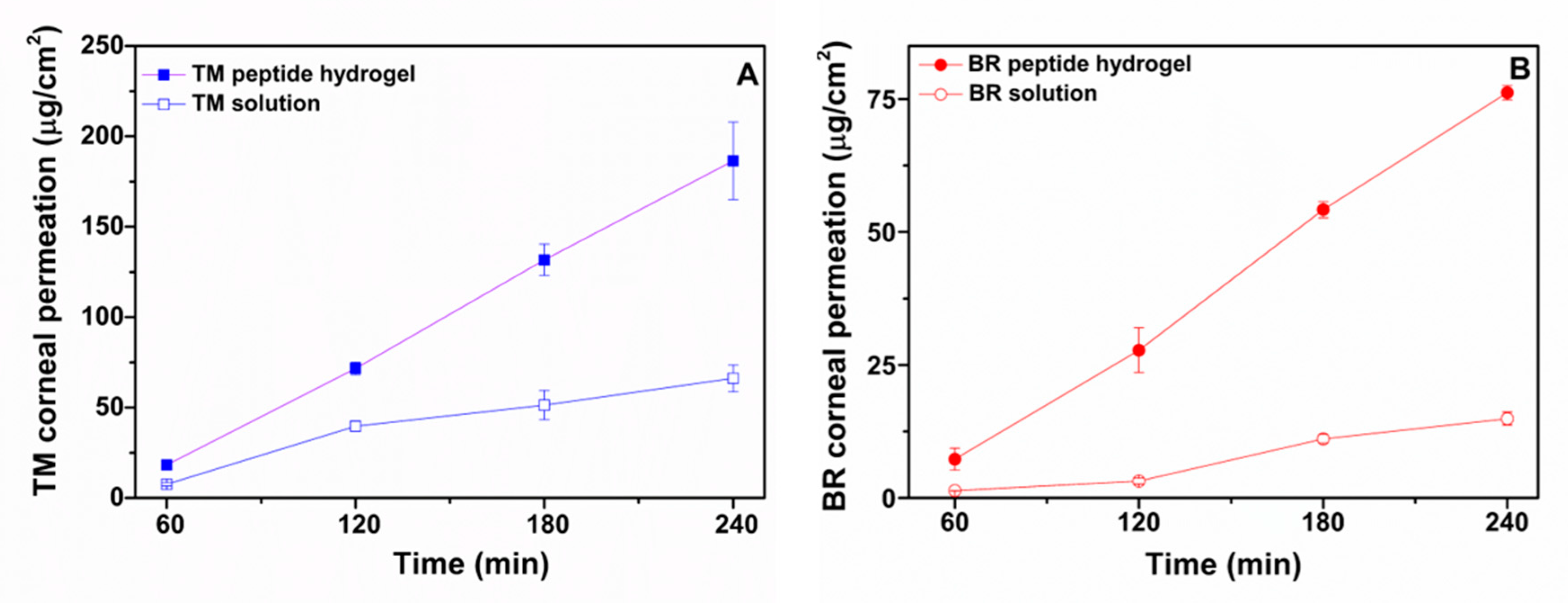
2.4. Ex Vivo Corneal Permeability Studies
2.5. Corneal Tissue Characterization Studies
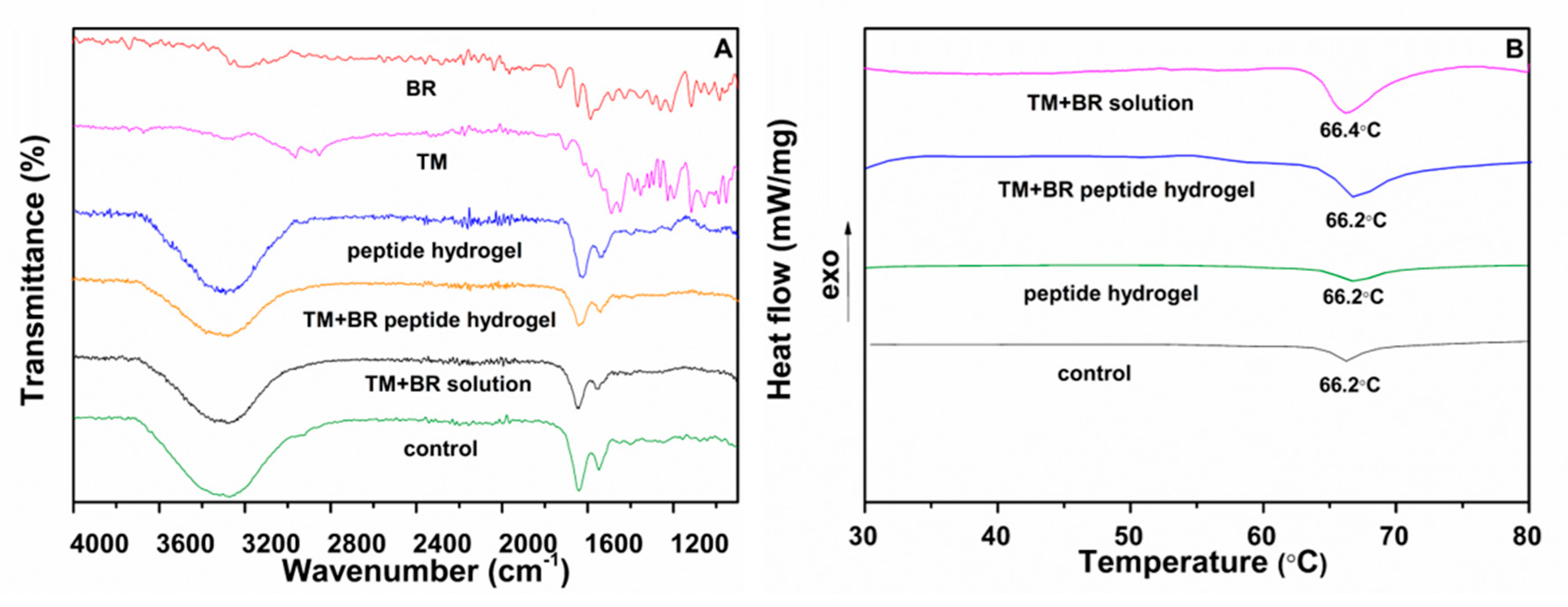
2.5.1. Fourier Transform Infrared Spectroscopy (FTIR) and Differential Scanning Calorimetry Analysis (DSC)
2.5.2. Hydration Content
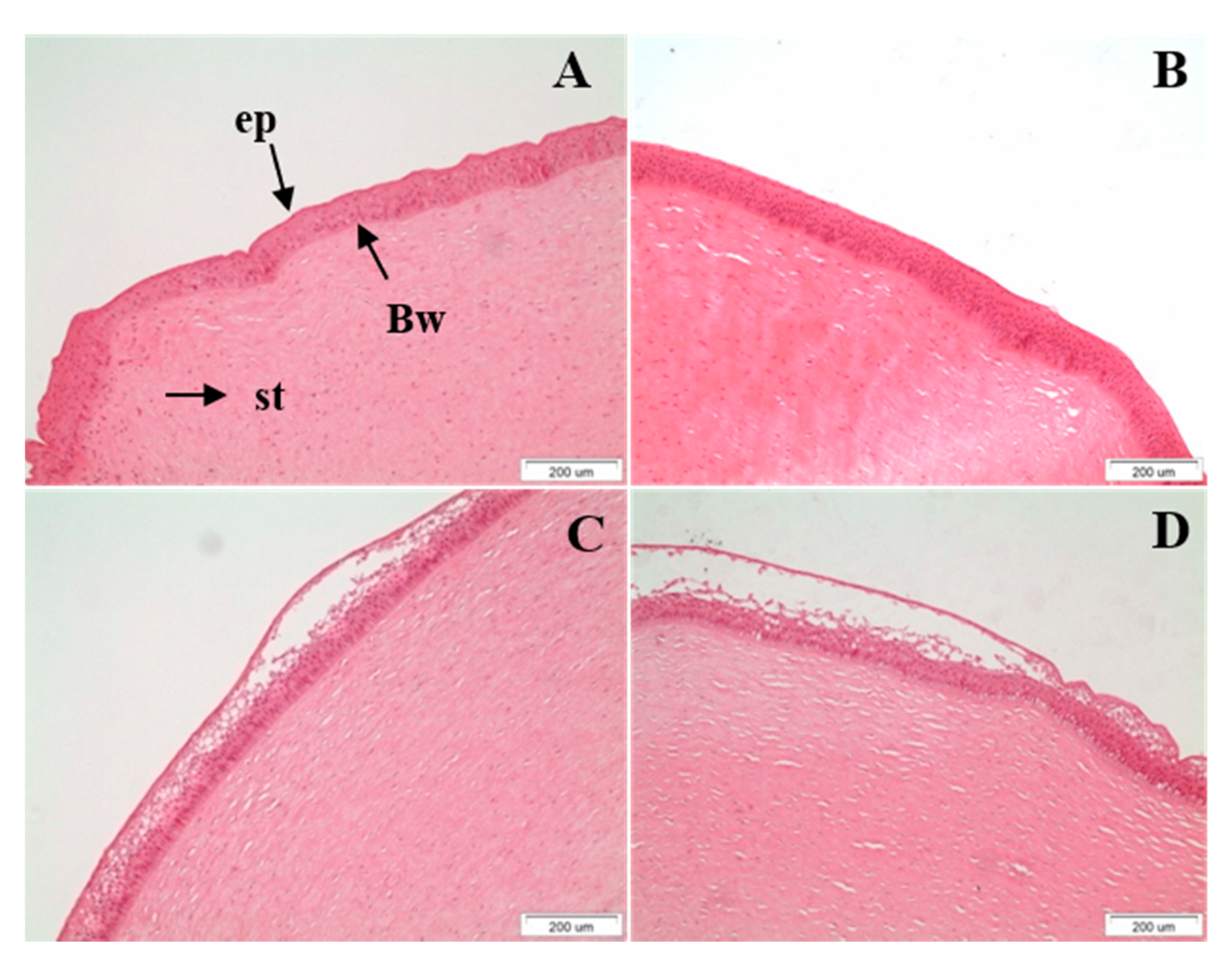
2.6. Histological Studies
3. Materials and Methods
3.1. Materials
3.2. Preparation of the Drug Loaded Peptide Hydrogel
3.3. Rheological Studies
3.4. Atomic Force Microscopy (AFM) Studies
3.5. In Vitro Release of TM and BR from the Self-Assembling Peptide Hydrogel in STF
3.6. Ex Vivo Corneal Permeability Studies
3.7. Data Processing
3.8. HPLC Analysis
3.9. Corneal Tissue Characterization
3.9.1. Fourier Transform Infrared (FTIR) Spectroscopy
3.9.2. Differential Scanning Calorimetry (DSC) Analysis
3.9.3. Hydration Content
3.10. Histological Studies
3.11. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Tatham, A.J.; Sarodia, U.; Gatrad, F.; Awan, A. Eye drop instillation technique in patients with glaucoma. Eye (Lond.) 2013, 27, 1293–1298. [Google Scholar] [CrossRef] [PubMed]
- Willoughby, C.E.; Ponzin, D.; Ferrari, S.; Lobo, A.; Landau, K.; Omidi, Y. Anatomy and physiology of the human eye: Effects of mucopolysaccharidoses disease on structure and function—A review. Clin. Experiment. Ophthalmol. 2010, 38, 2–11. [Google Scholar] [CrossRef]
- Gote, V.; Sikder, S.; Sicotte, J.; Pal, D. Ocular Drug Delivery: Present Innovations and Future Challenges. J. Pharmacol. Exp. Ther. 2019, 370, 602–624. [Google Scholar] [CrossRef] [PubMed]
- Patel, A.; Cholkar, K.; Agrahari, V.; Mitra, A.K. Ocular drug delivery systems: An overview. World J. Pharmacol. 2013, 2, 47–64. [Google Scholar] [CrossRef] [PubMed]
- Yu, Z.; Xu, Q.; Dong, C.; Lee, S.S.; Gao, L.; Li, Y.; D’Ortenzio, M.; Wu, J. Self-assembling peptide nanofibrous hydrogel as a versatile drug delivery platform. Curr. Pharm. Des. 2015, 21, 4342–4354. [Google Scholar] [CrossRef] [PubMed]
- Beniash, E.; Hartgerink, J.D.; Storrie, H.; Stendahl, J.C.; Stupp, S.I. Self-assembling peptide amphiphile nanofiber matrices for cell entrapment. Acta Biomater. 2005, 1, 387–397. [Google Scholar] [CrossRef] [PubMed]
- Anderson, J.M.; Kushwaha, M.; Tambralli, A.; Bellis, S.L.; Camata, R.P.; Jun, H.-W. Osteogenic differentiation of human mesenchymal stem cells directed by extracellular matrix-mimicking ligands in a biomimetic self-assembled peptide amphiphile nanomatrix. Biomacromolecules 2009, 10, 2935–2944. [Google Scholar] [CrossRef] [PubMed]
- Zhang, S.; Lockshin, C.; Herbert, A.; Winter, E.; Rich, A. Zuotin, a putative Z-DNA binding protein in Saccharomyces cerevisiae. EMBO J. 1992, 11, 3787–3796. [Google Scholar] [CrossRef] [PubMed]
- Karavasili, C.; Panteris, E.; Vizirianakis, I.S.; Koutsopoulos, S.; Fatouros, D.G. Chemotherapeutic Delivery from a Self-Assembling Peptide Nanofiber Hydrogel for the Management of Glioblastoma. Pharm. Res. 2018, 35, 166. [Google Scholar] [CrossRef] [PubMed]
- Karavasili, C.; Andreadis, D.A.; Katsamenis, O.L.; Panteris, E.; Anastasiadou, P.; Kakazanis, Z.; Zoumpourlis, V.; Markopoulou, C.K.; Koutsopoulos, S.; Vizirianakis, I.S.; et al. Synergistic Antitumor Potency of a Self-Assembling Peptide Hydrogel for the Local Co-delivery of Doxorubicin and Curcumin in the Treatment of Head and Neck Cancer. Mol. Pharm. 2019, 16, 2326–2341. [Google Scholar] [CrossRef]
- Karavasili, C.; Komnenou, A.; Katsamenis, O.L.; Charalampidou, G.; Kofidou, E.; Andreadis, D.; Koutsopoulos, S.; Fatouros, D.G. Self-Assembling Peptide Nanofiber Hydrogels for Controlled Ocular Delivery of Timolol Maleate. ACS Biomater. Sci. Eng. 2017, 3, 3386–3394. [Google Scholar] [CrossRef]
- Liu, J.; Zhang, L.; Yang, Z.; Zhao, X. Controlled release of paclitaxel from a self-assembling peptide hydrogel formed in situ and antitumor study in vitro. Int. J. Nanomedicine. 2011, 6, 2143–2153. [Google Scholar] [CrossRef] [PubMed]
- Phipps, M.C.; Monte, F.; Mehta, M.; Kim, H.K.W. Intraosseous Delivery of Bone Morphogenic Protein-2 Using a Self-Assembling Peptide Hydrogel. Biomacromolecules 2016, 17, 2329–2336. [Google Scholar] [CrossRef] [PubMed]
- Zhou, A.; Chen, S.; He, B.; Zhao, W.; Chen, X.; Jiang, D. Controlled release of TGF-beta 1 from RADA self-assembling peptide hydrogel scaffolds. Drug Des. Devel. Ther. 2016, 10, 3043–3051. [Google Scholar] [CrossRef] [PubMed]
- Guo, H.; Cui, G.; Yang, J.; Wang, C.; Zhu, J.; Zhang, L.; Jiang, J.; Shao, S. Sustained delivery of VEGF from designer self-assembling peptides improves cardiac function after myocardial infarction. Biochem. Biophys. Res. Commun. 2012, 424, 105–111. [Google Scholar] [CrossRef]
- Weinreb, R.N.; Aung, T.; Medeiros, F.A. The pathophysiology and treatment of glaucoma: A review. JAMA 2014, 311, 1901–1911. [Google Scholar] [CrossRef]
- Yadav, K.S.; Rajpurohit, R.; Sharma, S. Glaucoma: Current treatment and impact of advanced drug delivery systems. Life Sci. 2019, 221, 362–376. [Google Scholar] [CrossRef]
- Spaeth, G.L.; Bernstein, P.; Caprioli, J.; Schiffman, R.M. Control of intraocular pressure and fluctuation with fixed-combination brimonidine-timolol versus brimonidine or timolol monotherapy. Am. J. Ophthalmol. 2011, 151, 93–99.e4. [Google Scholar] [CrossRef]
- Arcieri, E.S.; Arcieri, R.S.; Pereira, A.C.A.; Andreo, E.G.V.; Finotti, I.G.A.; Sá Filho, W.F. Comparing the fixed combination brimonidine-timolol versus fixed combination dorzolamide-timolol in patients with elevated intraocular pressure. Curr. Med. Res. Opin. 2007, 23, 683–689. [Google Scholar] [CrossRef]
- Samy, K.E.; Cao, Y.; Kim, J.; Konichi da Silva, N.R.; Phone, A.; Bloomer, M.M.; Bhisitkul, R.B.; Desai, T.A. Co-Delivery of Timolol and Brimonidine with a Polymer Thin-Film Intraocular Device. J. Ocul. Pharmacol. Ther. Off. 2019, 35, 124–131. [Google Scholar] [CrossRef]
- Dubey, A.; Prabhu, P. Formulation and evaluation of stimuli-sensitive hydrogels of timolol maleate and brimonidine tartrate for the treatment of glaucoma. Int. J. Pharm. Investig. 2014, 4, 112–118. [Google Scholar] [CrossRef] [PubMed]
- Yang, H.; Tyagi, P.; Kadam, R.S.; Holden, C.A.; Kompella, U.B. Hybrid Dendrimer Hydrogel/PLGA Nanoparticle Platform Sustains Drug Delivery for One Week and Antiglaucoma Effects for Four Days Following One-Time Topical Administration. ACS Nano 2012, 6, 7595–7606. [Google Scholar] [CrossRef]
- Wang, T.; Zhong, X.; Wang, S.; Lv, F.; Zhao, X. Molecular mechanisms of RADA16-1 peptide on fast stop bleeding in rat models. Int. J. Mol. Sci. 2012, 13, 15279–15290. [Google Scholar] [CrossRef]
- Arnold, J.J.; Hansen, M.S.; Gorman, G.S.; Inoue, T.; Rao, V.; Spellen, S.; Hunsinger, R.N.; Chapleau, C.A.; Pozzo-Miller, L.; Daniel Stamer, W.; et al. The effect of Rho-associated kinase inhibition on the ocular penetration of timolol maleate. Investig. Ophthalmol. Vis. Sci. 2013, 54, 1118–1126. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Aksan, A. Fourier Transform Infrared Analysis of the Thermal Modification of Human Cornea Tissue during Conductive Keratoplasty. Appl. Spectrosc. 2010, 64, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Kampmeier, J.; Radt, B.; Birngruber, R.; Brinkmann, R. Thermal and Biomechanical Parameters of Porcine Cornea. Cornea 2000, 19, 355–363. [Google Scholar] [CrossRef]
- Miles, C.A.; Avery, N.C.; Rodin, V.V.; Bailey, A.J. The Increase in Denaturation Temperature Following Cross-linking of Collagen is Caused by Dehydration of the Fibres. J. Mol. Biol. 2005, 346, 551–556. [Google Scholar] [CrossRef]
- Lin, H.H.; Ko, S.M.; Hsu, L.R.; Tsai, Y.H. The preparation of norfloxacin-loaded liposomes and their in-vitro evaluation in pig’s eye. J. Pharm. Pharmacol. 1996, 48, 801–805. [Google Scholar] [CrossRef]
- Sionkowska, A. Thermal stability of UV-irradiated collagen in bovine lens capsules and in bovine cornea. J. Photochem. Photobiol. B Biol. 2005, 80, 87–92. [Google Scholar] [CrossRef]
- Pescina, S.; Govoni, P.; Potenza, A.; Padula, C.; Santi, P.; Nicoli, S. Development of a Convenient ex vivo Model for the Study of the Transcorneal Permeation of Drugs: Histological and Permeability Evaluation. J. Pharm. Sci. 2015, 104, 63–71. [Google Scholar] [CrossRef]
- Monti, D.; Chetoni, P.; Burgalassi, S.; Najarro, M.; Saettone, M. Increased corneal hydration induced by potential ocular penetration enhancers: Assessment by differential scanning calorimetry (DSC) and by desiccation. Int. J. Pharm. 2002, 232, 139–147. [Google Scholar] [CrossRef]
- Stewart, W.C.; Stewart, J.A.; Holmes, K.T.; Leech, J.N. Differences in ocular surface irritation between timolol hemihydrate and timolol maleate. Am. J. Ophthalmol. 2000, 130, 712–716. [Google Scholar] [CrossRef]
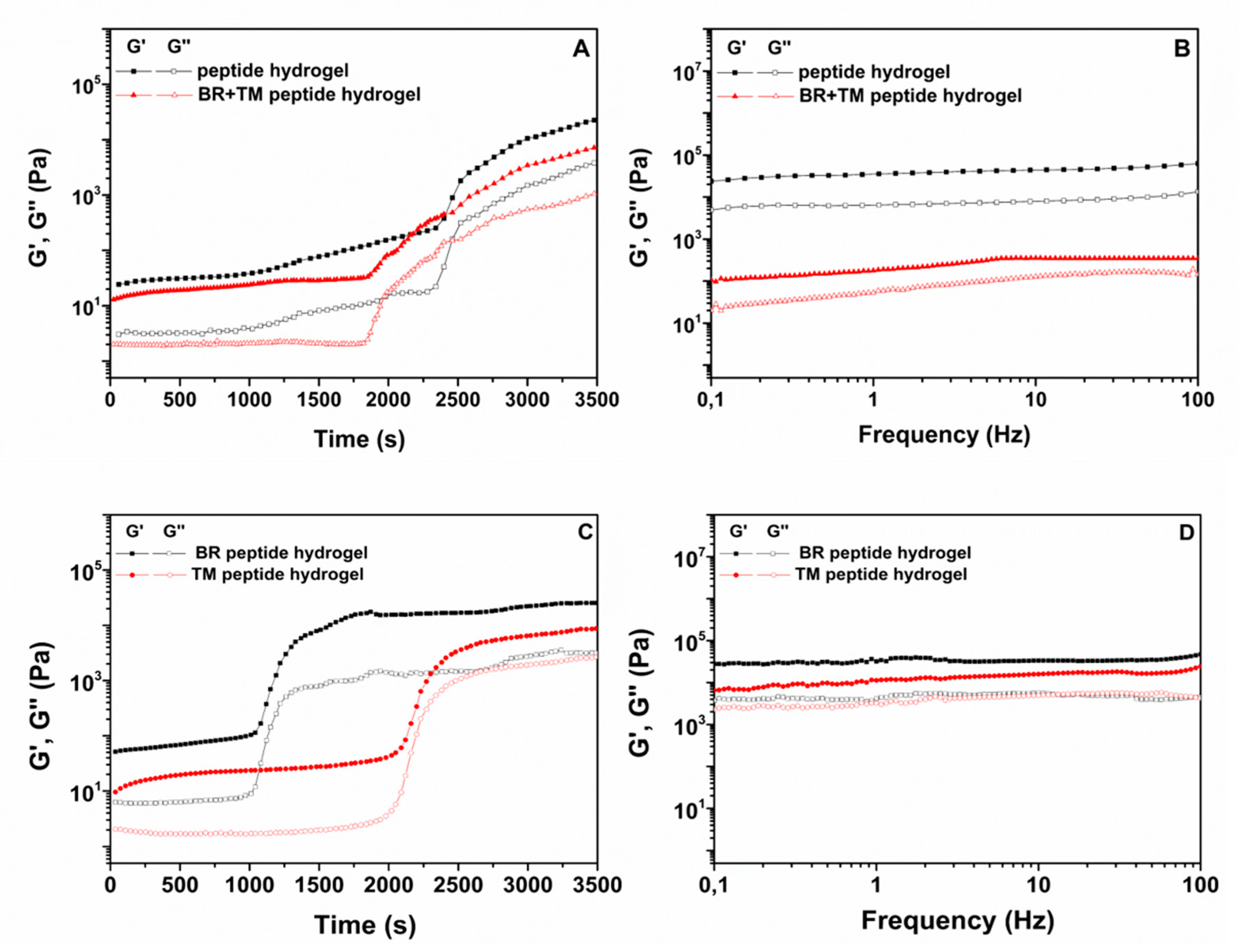
| Formulation | Gelation Onset (min) | G’max (kPa) | tan δ |
|---|---|---|---|
| Peptide hydrogel | 39 | 22.6 | 0.05 |
| BR + TM peptide hydrogel | 30 | 7.1 | 0.28 |
| BR peptide hydrogel | 18 | 25.3 | 0.13 |
| TM peptide hydrogel | 35 | 8.7 | 0.31 |
| Formulation | Jss (μg/cm2/min) | Papp (·10−6 cm/s) |
|---|---|---|
| TM peptide hydrogel | 0.94 ± 0.13 | 2.30 ± 0.30 |
| TM solution | 0.31 ± 0.02 | 0.75 ± 0.05 |
| BR peptide hydrogel | 0.40 ± 0.03 | 3.30 ± 0.30 |
| BR solution | 0.076 ± 0.007 | 0.63 ± 0.05 |
| Formulation | Hydration Content (%) |
|---|---|
| Control | 79.65 ± 3.40 |
| Peptide hydrogel | 80.15 ± 0.32 |
| TM + BR solution | 80.30 ± 0.47 |
| TM + BR peptide hydrogel | 81.50 ± 0.60 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Taka, E.; Karavasili, C.; Bouropoulos, N.; Moschakis, T.; Andreadis, D.D.; Zacharis, C.K.; Fatouros, D.G. Ocular Co-Delivery of Timolol and Brimonidine from a Self-Assembling Peptide Hydrogel for the Treatment of Glaucoma: In Vitro and Ex Vivo Evaluation. Pharmaceuticals 2020, 13, 126. https://doi.org/10.3390/ph13060126
Taka E, Karavasili C, Bouropoulos N, Moschakis T, Andreadis DD, Zacharis CK, Fatouros DG. Ocular Co-Delivery of Timolol and Brimonidine from a Self-Assembling Peptide Hydrogel for the Treatment of Glaucoma: In Vitro and Ex Vivo Evaluation. Pharmaceuticals. 2020; 13(6):126. https://doi.org/10.3390/ph13060126
Chicago/Turabian StyleTaka, Elissavet, Christina Karavasili, Nikolaos Bouropoulos, Thomas Moschakis, Dimitrios D. Andreadis, Constantinos K. Zacharis, and Dimitrios G. Fatouros. 2020. "Ocular Co-Delivery of Timolol and Brimonidine from a Self-Assembling Peptide Hydrogel for the Treatment of Glaucoma: In Vitro and Ex Vivo Evaluation" Pharmaceuticals 13, no. 6: 126. https://doi.org/10.3390/ph13060126
APA StyleTaka, E., Karavasili, C., Bouropoulos, N., Moschakis, T., Andreadis, D. D., Zacharis, C. K., & Fatouros, D. G. (2020). Ocular Co-Delivery of Timolol and Brimonidine from a Self-Assembling Peptide Hydrogel for the Treatment of Glaucoma: In Vitro and Ex Vivo Evaluation. Pharmaceuticals, 13(6), 126. https://doi.org/10.3390/ph13060126









