Synthesis of Saponite Based Nanocomposites to Improve the Controlled Oral Drug Release of Model Drug Quinine Hydrochloride Dihydrate
Abstract
1. Introduction
2. Material and Methods
2.1. Materials
2.2. Synthesis of Saponite
2.3. Synthesis of Clay Drug Nanocomposite
2.4. Characterization
2.5. In Vitro Drug Release Test
3. Results and Discussion
3.1. Powder X-Ray Diffraction Analysis (PXRD)
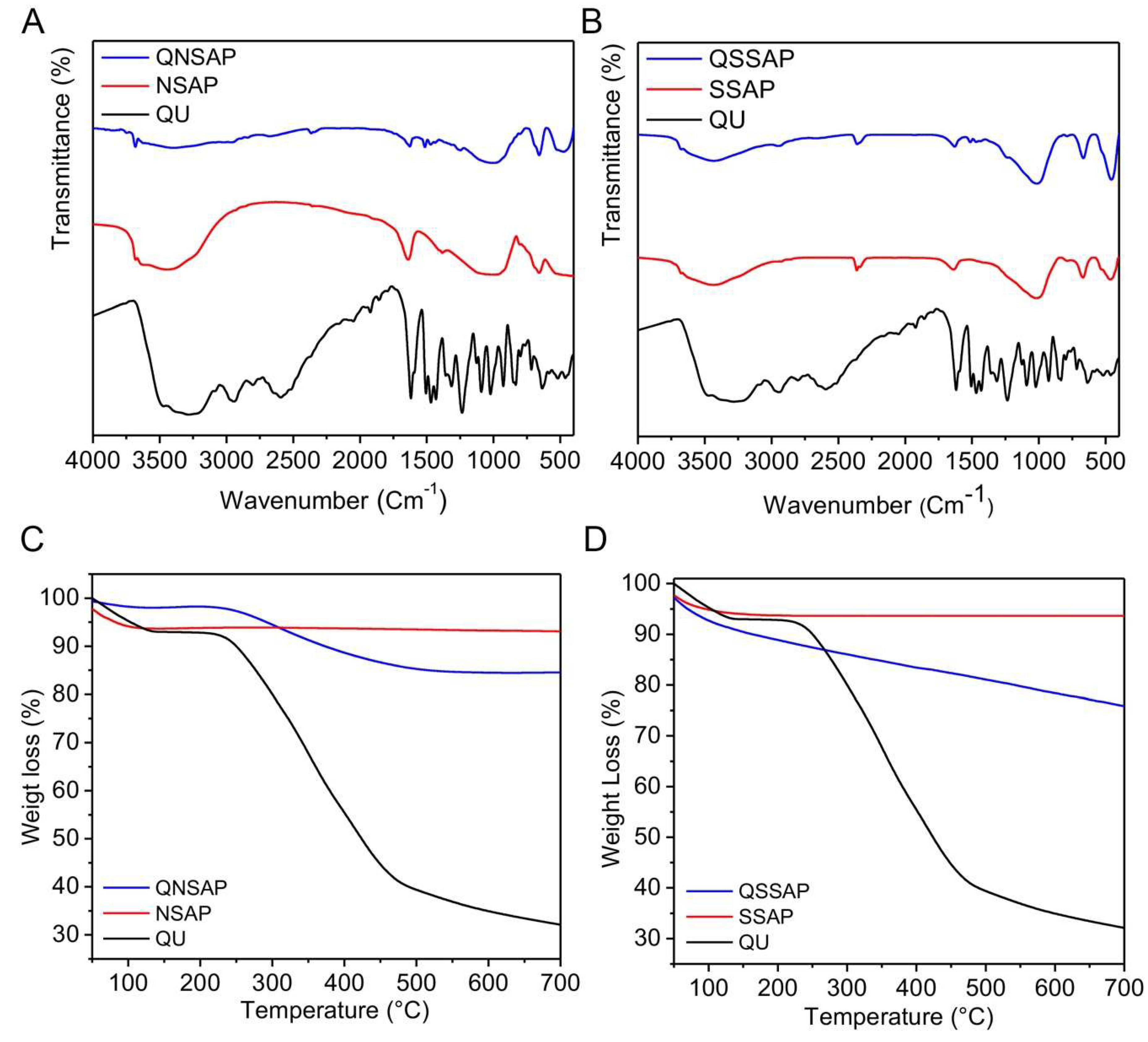
3.2. Fourier Transform Infrared Spectroscopy (FTIR)
3.3. Thermal Gravimetric Analysis (TGA)
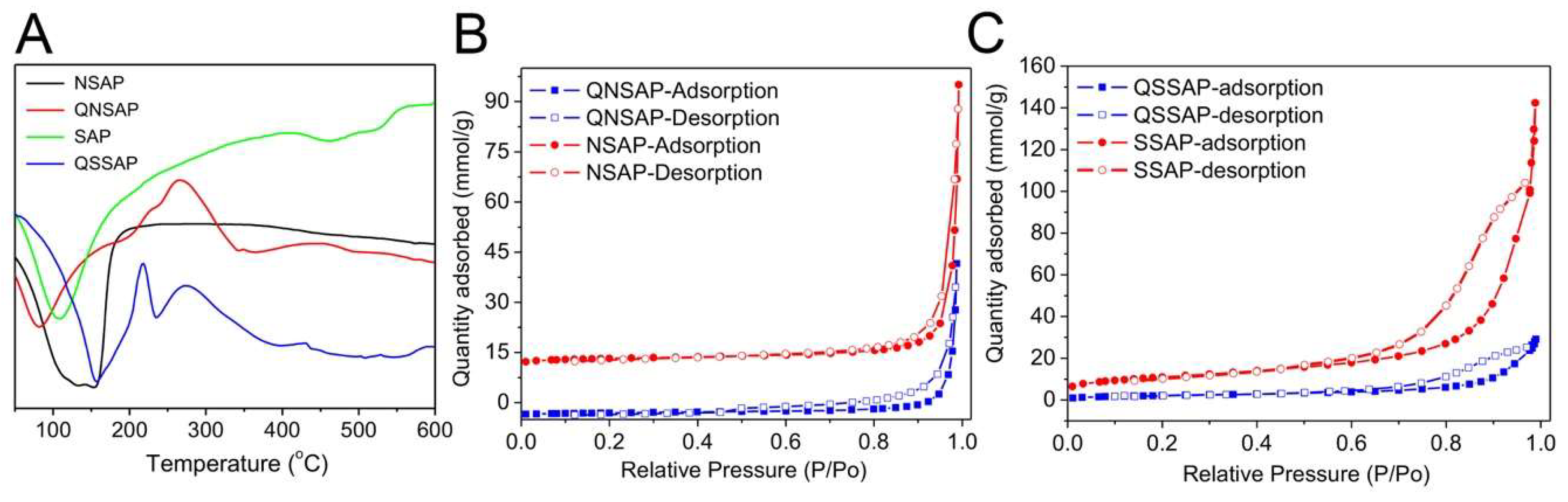
3.4. Differential Scanning Calorimetry Analysis (DSC)
3.5. BET Surface Area analysis
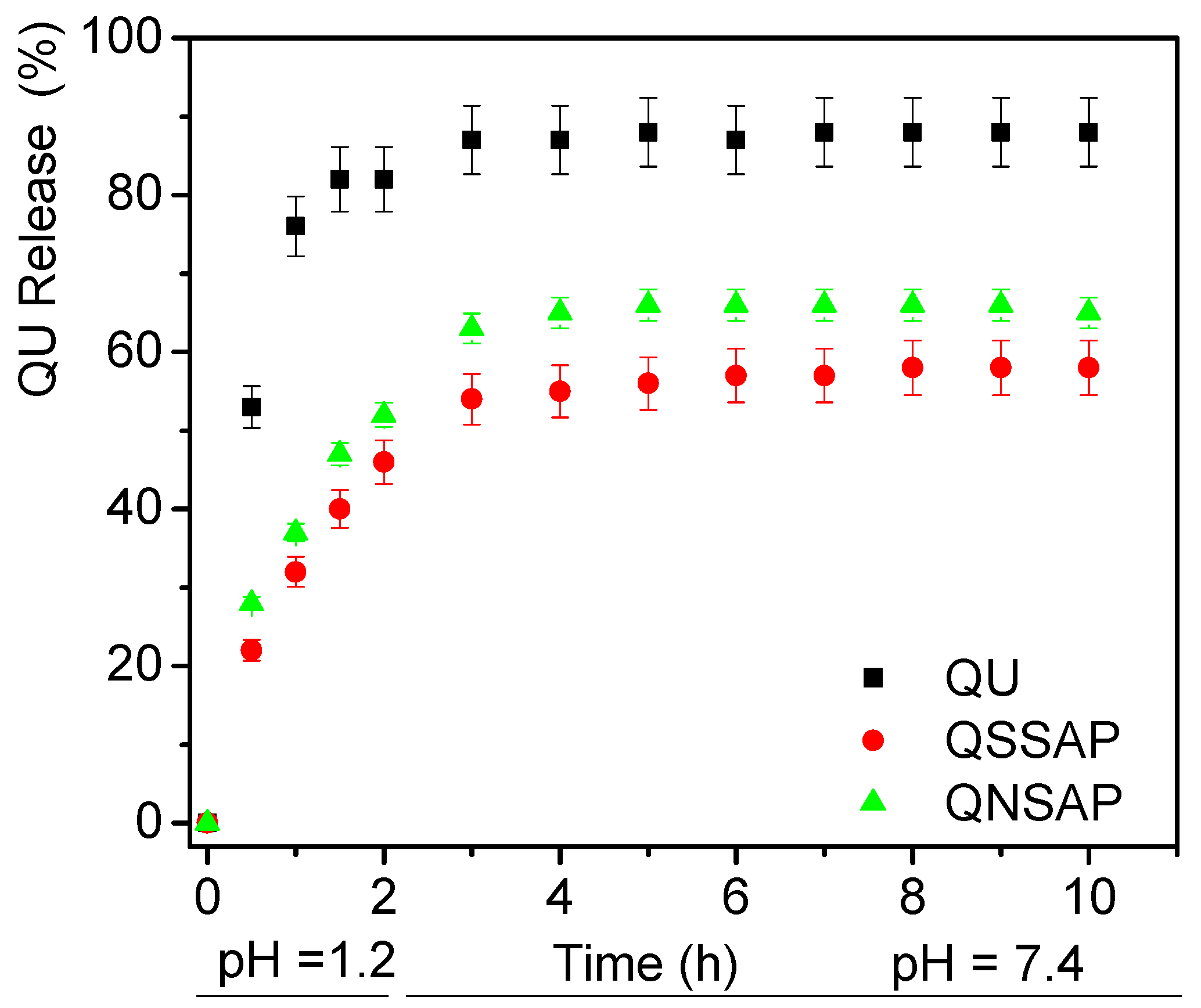
3.6. In Vitro Drug Release Study of Clay and Nanocomposite
4. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Reinholz, J.; Landfester, K.; Mailänder, V. The challenges of oral drug delivery via nanocarriers. Drug Deliv. 2018, 25, 1694–1705. [Google Scholar] [CrossRef] [PubMed]
- Webber, M.J.; Langer, R. Drug delivery by supramolecular design. Chem. Soc. Rev. 2017, 46, 6600–6620. [Google Scholar] [CrossRef] [PubMed]
- Bergaya, F.; Lagaly, G. Chapter 1 General Introduction: Clays, Clay Minerals, and Clay Science. In Developments in Clay Science; Bergaya, F., Theng, B.K.G., Lagaly, G., Eds.; Elsevier: Amsterdam, The Netherlands, 2006; Volume 1, pp. 1–18. [Google Scholar]
- Carrado, K.A.; Decarreau, A.; Petit, S.; Bergaya, F.; Lagaly, G. Chapter 4 Synthetic Clay Minerals and Purification of Natural Clays. In Developments in Clay Science; Bergaya, F., Theng, B.K.G., Lagaly, G., Eds.; Elsevier: Amsterdam, The Netherlands, 2006; Volume 1, pp. 115–139. [Google Scholar]
- Murray, H.H. Overview — clay mineral applications. Appl. Clay Sci. 1991, 5, 379–395. [Google Scholar] [CrossRef]
- Ingole, P.G.; Pawar, R.R.; Baig, M.I.; Jeon, J.D.; Lee, H.K. Thin film nanocomposite (TFN) hollow fiber membranes incorporated with functionalized acid-activated bentonite (ABn-NH) clay: towards enhancement of water vapor permeance and selectivity. J. Mater. Chem. A 2017, 5, 20947–20958. [Google Scholar] [CrossRef]
- Chuaicham, C.; Pawar, R.; Sasaki, K. Dye-sensitized Photocatalyst of Sepiolite for Organic Dye Degradation. Catalysts 2019, 9, 235. [Google Scholar] [CrossRef]
- Pawar, R.R.; Lalhmunsiama; Bajaj, H.C.; Lee, S.-M. Activated bentonite as a low-cost adsorbent for the removal of Cu(II) and Pb(II) from aqueous solutions: Batch and column studies. J. Ind. Eng. Chem. 2016, 34, 213–223. [Google Scholar] [CrossRef]
- Pawar, R.R.; Gupta, P.; Lalhmunsiama; Bajaj, H.C.; Lee, S.-M. Al-intercalated acid activated bentonite beads for the removal of aqueous phosphate. Sci. Total Environ. 2016, 572, 1222–1230. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.; Jung, J.; Pawar, R.R.; Kim, M.; Lalhmunsiama; Lee, S.-M. Arsenate and phosphate removal from water using Fe-sericite composite beads in batch and fixed-bed systems. J. Ind. Eng. Chem. 2017, 47, 375–383. [Google Scholar] [CrossRef]
- Pawar, R.R.; Lalhmunsiama; Kim, M.; Kim, J.-G.; Hong, S.-M.; Sawant, S.Y.; Lee, S.M. Efficient removal of hazardous lead, cadmium, and arsenic from aqueous environment by iron oxide modified clay-activated carbon composite beads. Appl. Clay Sci. 2018, 162, 339–350. [Google Scholar] [CrossRef]
- Yang, P.; Gai, S.; Lin, J. Functionalized mesoporous silica materials for controlled drug delivery. Chem. Soc. Rev. 2012, 41, 3679–3698. [Google Scholar] [CrossRef]
- Tibbitt, M.W.; Rodell, C.B.; Burdick, J.A.; Anseth, K.S. Progress in material design for biomedical applications. Proc. Natl. Acad. Sci. USA 2015, 112, 14444–14451. [Google Scholar] [CrossRef] [PubMed]
- Bhat, S.; Kumar, A. Biomaterials and bioengineering tomorrow’s healthcare. Biomatter 2013, 3, e24717. [Google Scholar] [CrossRef] [PubMed]
- Hun Kim, M.; Choi, G.; Elzatahry, A.; Vinu, A.; Bin Choy, Y.; Choy, J.-H. Review of Clay-drug Hybrid Materials for Biomedical Applications: Administration Routes. Clays Clay Miner. 2016, 64, 115–130. [Google Scholar] [CrossRef]
- Khurana, I.S.; Kaur, S.; Kaur, H.; Khurana, R.K. Multifaceted role of clay minerals in pharmaceuticals. Future Sci. OA 2015, 1, FSO6. [Google Scholar] [CrossRef] [PubMed]
- Massaro, M.; Colletti, G.C.; Lazzara, G.; Riela, S. The Use of Some Clay Minerals as Natural Resources for Drug Carrier Applications. J. Funct. Biomater. 2018, 9. [Google Scholar] [CrossRef]
- Tiwari, G.; Tiwari, R.; Sriwastawa, B.; Bhati, L.; Pandey, S.; Pandey, P.; Bannerjee, S.K. Drug delivery systems: An updated review. Int. J. Pharm. Investig. 2012, 2, 2–11. [Google Scholar] [CrossRef]
- Senapati, S.; Mahanta, A.K.; Kumar, S.; Maiti, P. Controlled drug delivery vehicles for cancer treatment and their performance. Signal Trans. Target. Ther. 2018, 3, 7. [Google Scholar] [CrossRef]
- Joshi, G.V.; Kevadiya, B.D.; Patel, H.A.; Bajaj, H.C.; Jasra, R.V. Montmorillonite as a drug delivery system: Intercalation and in vitro release of timolol maleate. Int. J. Pharm. 2009, 374, 53–57. [Google Scholar] [CrossRef]
- Joshi, G.V.; Pawar, R.R.; Kevadiya, B.D.; Bajaj, H.C. Mesoporous synthetic hectorites: A versatile layered host with drug delivery application. Microporous Mesoporous Mater 2011, 142, 542–548. [Google Scholar] [CrossRef]
- Kevadiya, B.D.; Chettiar, S.S.; Rajkumar, S.; Bajaj, H.C.; Gosai, K.A.; Brahmbhatt, H. Evaluation of clay/poly (l-lactide) microcomposites as anticancer drug, 6-mercaptopurine reservoir through in vitro cytotoxicity, oxidative stress markers and in vivo pharmacokinetics. Colloids Surf. B Biointerfaces 2013, 112, 400–407. [Google Scholar] [CrossRef]
- Kevadiya, B.D.; Joshi, G.V.; Bajaj, H.C. Layered bionanocomposites as carrier for procainamide. Int. J. Pharm. 2010, 388, 280–286. [Google Scholar] [CrossRef] [PubMed]
- Kevadiya, B.D.; Rajkumar, S.; Bajaj, H.C.; Chettiar, S.S.; Gosai, K.; Brahmbhatt, H.; Bhatt, A.S.; Barvaliya, Y.K.; Dave, G.S.; Kothari, R.K. Biodegradable gelatin–ciprofloxacin–montmorillonite composite hydrogels for controlled drug release and wound dressing application. Colloids Surf. B Biointerfaces 2014, 122, 175–183. [Google Scholar] [CrossRef] [PubMed]
- Patel, H.A.; Somani, R.S.; Bajaj, H.C.; Jasra, R.V. Preparation and characterization of phosphonium montmorillonite with enhanced thermal stability. Appl. Clay Sci. 2007, 35, 194–200. [Google Scholar] [CrossRef]
- Pawar, R.R.; Kevadiya, B.D.; Brahmbhatt, H.; Bajaj, H.C. Template free synthesis of mesoporous hectorites: Efficient host for pH responsive drug delivery. Int. J. Pharm. 2013, 446, 145–152. [Google Scholar] [CrossRef] [PubMed]
- Kevadiya, B.D.; Joshi, G.V.; Patel, H.A.; Ingole, P.G.; Mody, H.M.; Bajaj, H.C. Montmorillonite-Alginate Nanocomposites as a Drug Delivery System: Intercalation and In Vitro Release of Vitamin B1 and Vitamin B6. J. Biomater. Appl. 2010, 25, 161–177. [Google Scholar] [CrossRef]
- Kumaresan, S.; Pawar, R.R.; Lee, S.-M.; Bajaj, H. Quinine Intercalated Natural Hectorite Clay Layered Hybrid Nanocomposite for Controlled Drug Delivery Application. Sci. Technol. J. 2016, 1, 7–13. [Google Scholar]
- Pawar, R.R.; Lalhmunsiama; Gupta, P.; Sawant, S.Y.; Shahmoradi, B.; Lee, S.-M. Porous synthetic hectorite clay-alginate composite beads for effective adsorption of methylene blue dye from aqueous solution. Int. J. Biol. Macromol. 2018, 114, 1315–1324. [Google Scholar] [CrossRef]
- Sawant, S.Y.; Pawar, R.R.; Somani, R.S.; Bajaj, H.C. Facile hard template approach for synthetic hectorite hollow microspheres. Mater. Lett. 2014, 128, 121–124. [Google Scholar] [CrossRef]
- Sethia, G.; Patel, H.A.; Pawar, R.R.; Bajaj, H.C. Porous synthetic hectorites for selective adsorption of carbon dioxide over nitrogen, methane, carbon monoxide and oxygen. Appl. Clay Sci. 2014, 91–92, 63–69. [Google Scholar] [CrossRef]
- Pawar, R.R.; Patel, H.A.; Sethia, G.; Bajaj, H.C. Selective adsorption of carbon dioxide over nitrogen on calcined synthetic hectorites with tailor-made porosity. Appl. Clay Sci. 2009, 46, 109–113. [Google Scholar] [CrossRef]
- Vicente, M.A.; Suárez, M.; López-González, J.d.D.; Bañares-Muñoz, M.A. Characterization, Surface Area, and Porosity Analyses of the Solids Obtained by Acid Leaching of a Saponite. Langmuir 1996, 12, 566–572. [Google Scholar] [CrossRef]
- Szabó, T.s.; Mitea, R.; Leeman, H.; Premachandra, G.S.; Johnston, C.T.; Szekeres, M.R.; Dékány, I.; Schoonheydt, R.A. Adsorption of Protamine and Papain Proteins on Saponite. Clays Clay Miner. 2008, 56, 494–504. [Google Scholar] [CrossRef]
- Bisio, C.; Carniato, F.; Paul, G.; Gatti, G.; Boccaleri, E.; Marchese, L. One-Pot Synthesis and Physicochemical Properties of an Organo-Modified Saponite Clay. Langmuir 2011, 27, 7250–7257. [Google Scholar] [CrossRef] [PubMed]
- Okada, T.; Seki, Y.; Ogawa, M. Designed Nanostructures of Clay for Controlled Adsorption of Organic Compounds. J. Nanosci. Nanotechnol. 2014, 14, 2121–2134. [Google Scholar] [CrossRef] [PubMed]
- Vogels, R.J.M.J.; Kloprogge, J.T.; Geus, J.W. Synthesis and characterization of saponite clays. Am. Mineralogist 2005, 90, 931–944. [Google Scholar] [CrossRef]
- Post, J.L. Saponite from Near Ballarat, California. Clays Clay Miner. 1984, 32, 147–153. [Google Scholar] [CrossRef]
- Sing, K.S.W.; Everett, D.H.; Haul, R.A.W.; Moscou, L.; Pierotti, R.A.; Rouquérol, J.; Siemieniewska, T. Reporting Physisorption Data for Gas/Solid Systems With Special Reference to the Determination of Surface Area and Porosity. Pure Appl. Chem. 1985, 57, 603–619. [Google Scholar] [CrossRef]
- Shao, H.; Pinnavaia, T.J. Synthesis and Properties of Nanoparticle Forms Saponite Clay, Cancrinite Zeolite and Phase Mixtures Thereof. Microporous Mesoporous Mater 2010, 133, 10–17. [Google Scholar] [CrossRef]
- Dash, S.; Murthy, P.N.; Nath, L.; Chowdhury, P. Kinetic modeling on drug release from controlled drug delivery systems. Acta Poloniae Pharm. 2010, 67, 217–223. [Google Scholar]
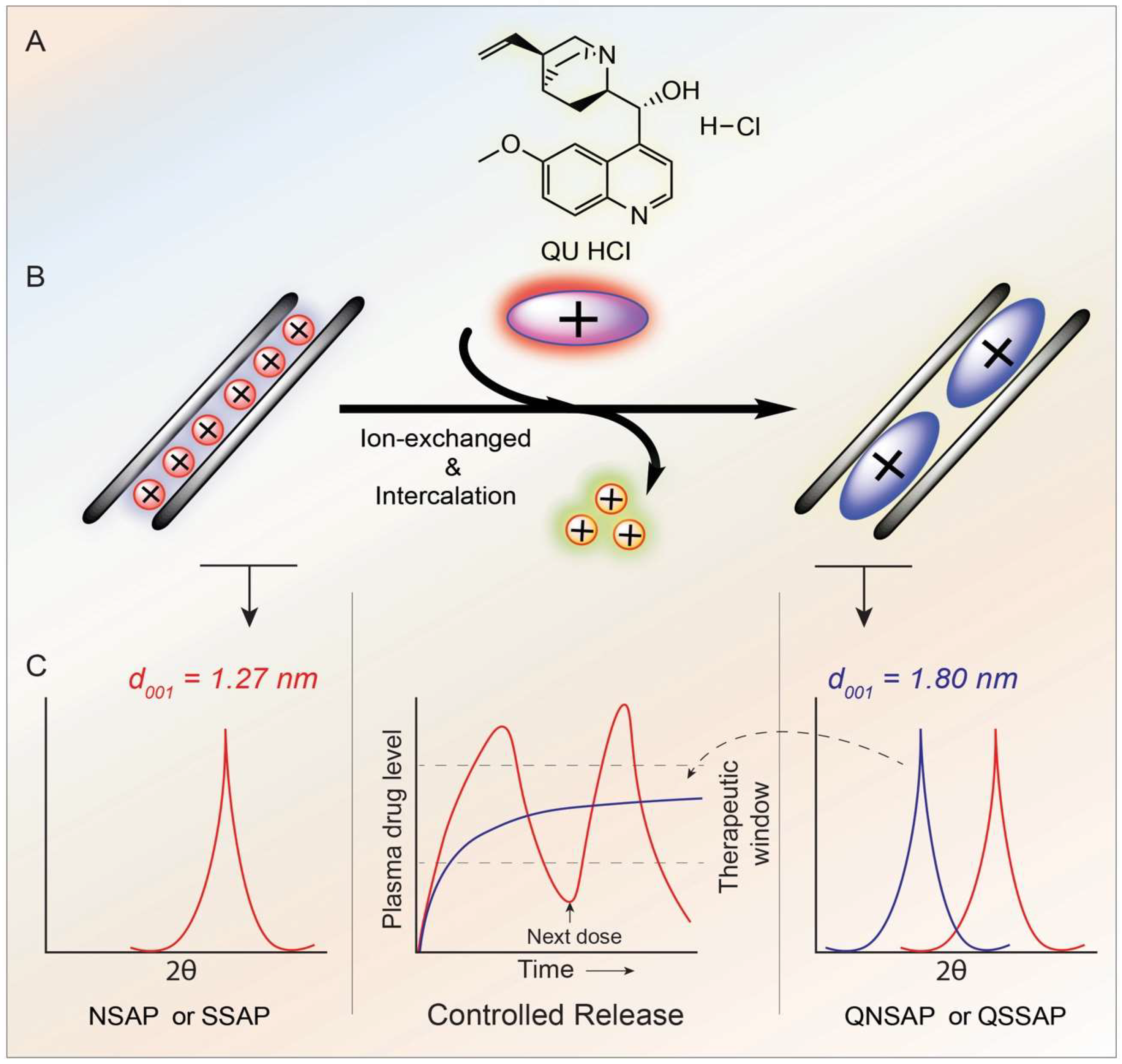
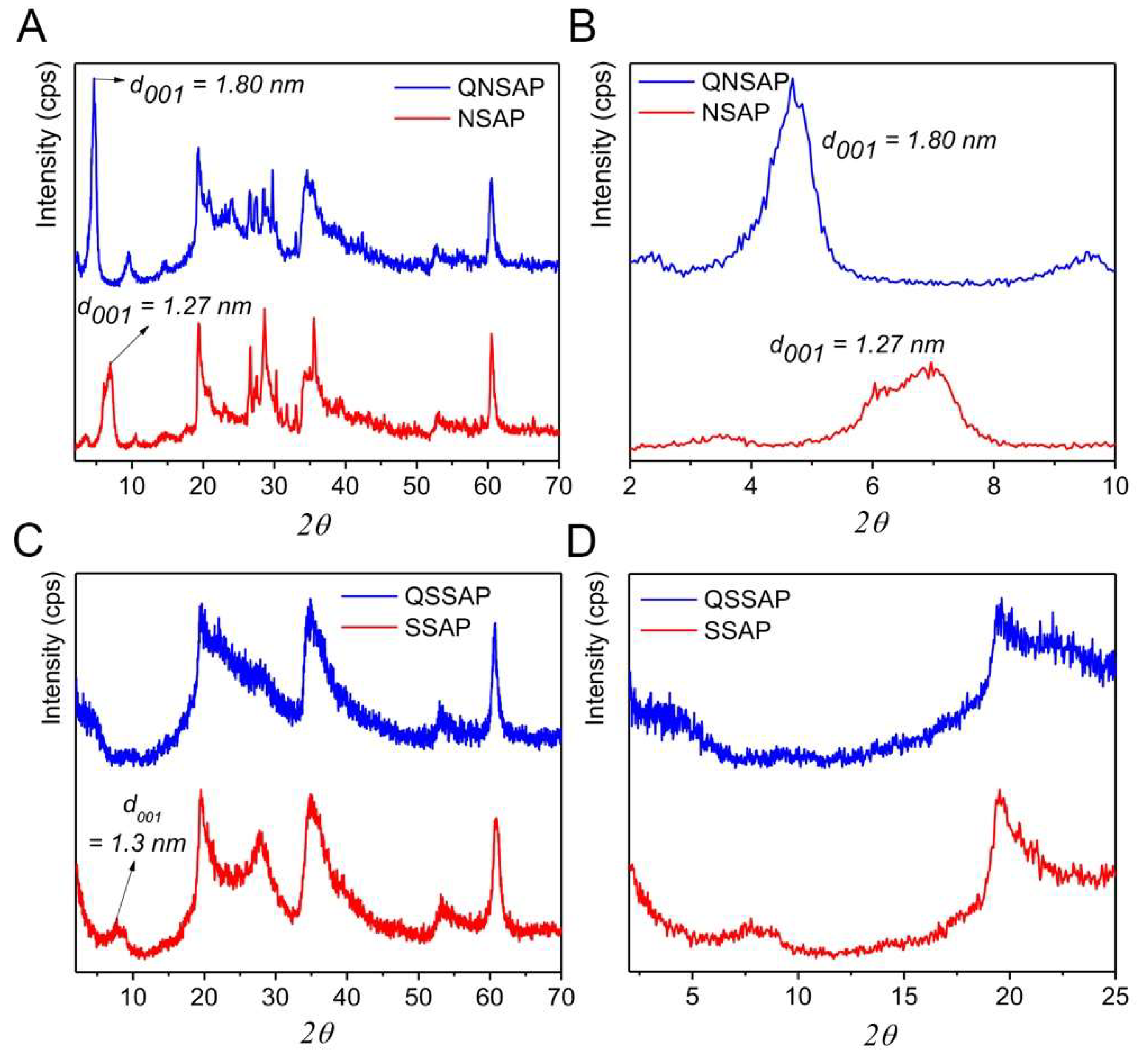

| Clay and Nano Composites | 2θ | 001 Basal Spacing (nm) |
|---|---|---|
| NSAP | 7.06 | 1.27 |
| QNSAP | 4.89 | 1.8 |
| SSAP | 6.93 | 1.3 |
| QSSAP | - | Exfoliation |
| Sample Type | Assignments | Absorption Bands of NSAP and SSAP, (cm−1) | QU (cm−1) | QNSAP and QSSAP, (cm−1) |
|---|---|---|---|---|
| Clay | Mg(OH)2 stretching -OH (for H2O) | 3686, 3685 3433, 1640 | - | 3678, 3675 3432, 1640 |
| Si-O | 1008, 1029 | - | 1023, 1014 | |
| Si-O-Al Si-O-Mg | 680, 669 528, 467 | - | 667 482, 456 | |
| QU | V(C-H) aliphatic | - | 2947 | 2949 |
| V(Qu-NH2 group): | - | 1618 | 1611, 1629 | |
| V(C=C), alkene V(Q ring) | - | 1505 | 1511, 1513 | |
| δ (CH3-methoxy) | - | 1468 1235 | 1451, 1467 1260, 1241 |
| Sample | BET Surface Area, (m2/g) | Pore Volume (cm3/g) | Pore Size (nm) |
|---|---|---|---|
| NSAP | 070.0 | 0.45 | 30.0 |
| QNSAP | 36.6 | 0.21 | 33.3 |
| SSAP | 881.0 | 3.44 | 15.6 |
| QSSAP | 181.0 | 0.82 | 18.05 |
| Composite | Drug Loading (mg/g) |
|---|---|
| QNSAP | 211 |
| QSSAP | 242 |
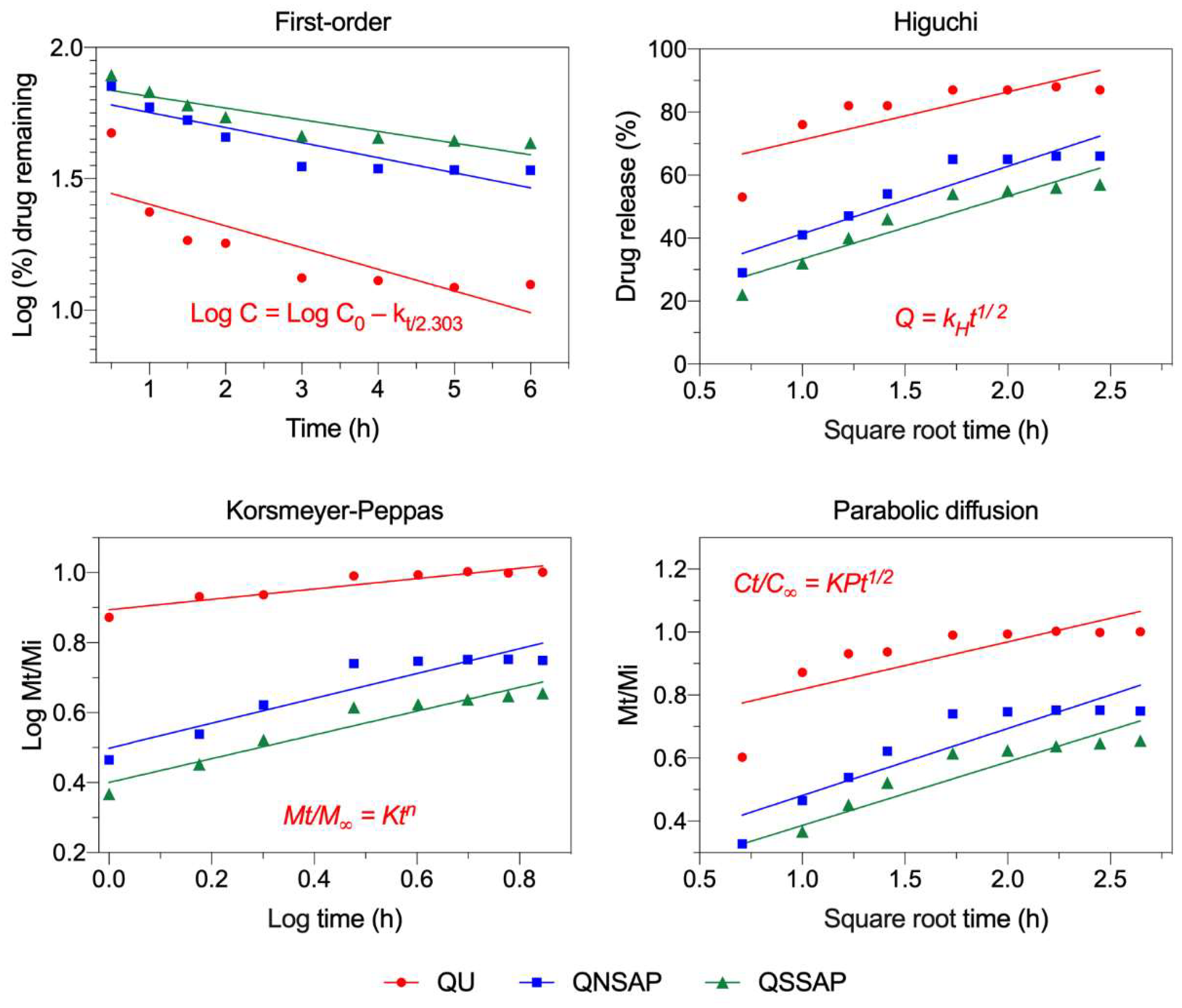
| Kinetic Models | Parameters | Formulations | ||
|---|---|---|---|---|
| QU | QNSAP | QSSAP | ||
| First order | r2 | 0.6642 | 0.8062 | 0.8261 |
| K | −0.16496 | −0.11478 | −0.08894 | |
| Higuchi-equation | r2 | 0.6348 | 0.88 | 0.8912 |
| KH | 15.23 | 21.41 | 19.88 | |
| Korsmeyer–Peppas | r2 | 0.8842 | 0.8772 | 0.925 |
| N | 0.1483 | 0.3555 | 0.3399 | |
| KHP | 7.83 | 3.151 | 2.51 | |
| Parabolic-diffusion | r2 | 0.611 | 0.8318 | 0.8661 |
| Kp | 0.15 | 0.2126 | 0.2017 | |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
S., K.; Rama Pawar, R.; D. Kevadiya, B.; C. Bajaj, H. Synthesis of Saponite Based Nanocomposites to Improve the Controlled Oral Drug Release of Model Drug Quinine Hydrochloride Dihydrate. Pharmaceuticals 2019, 12, 105. https://doi.org/10.3390/ph12030105
S. K, Rama Pawar R, D. Kevadiya B, C. Bajaj H. Synthesis of Saponite Based Nanocomposites to Improve the Controlled Oral Drug Release of Model Drug Quinine Hydrochloride Dihydrate. Pharmaceuticals. 2019; 12(3):105. https://doi.org/10.3390/ph12030105
Chicago/Turabian StyleS., Kumaresan, Radheshyam Rama Pawar, Bhavesh D. Kevadiya, and Hari C. Bajaj. 2019. "Synthesis of Saponite Based Nanocomposites to Improve the Controlled Oral Drug Release of Model Drug Quinine Hydrochloride Dihydrate" Pharmaceuticals 12, no. 3: 105. https://doi.org/10.3390/ph12030105
APA StyleS., K., Rama Pawar, R., D. Kevadiya, B., & C. Bajaj, H. (2019). Synthesis of Saponite Based Nanocomposites to Improve the Controlled Oral Drug Release of Model Drug Quinine Hydrochloride Dihydrate. Pharmaceuticals, 12(3), 105. https://doi.org/10.3390/ph12030105





