Monitoring and Assessment of Rehabilitation Progress on Range of Motion After Total Knee Replacement by Sensor-Based System
Abstract
1. Introduction
2. Methodology
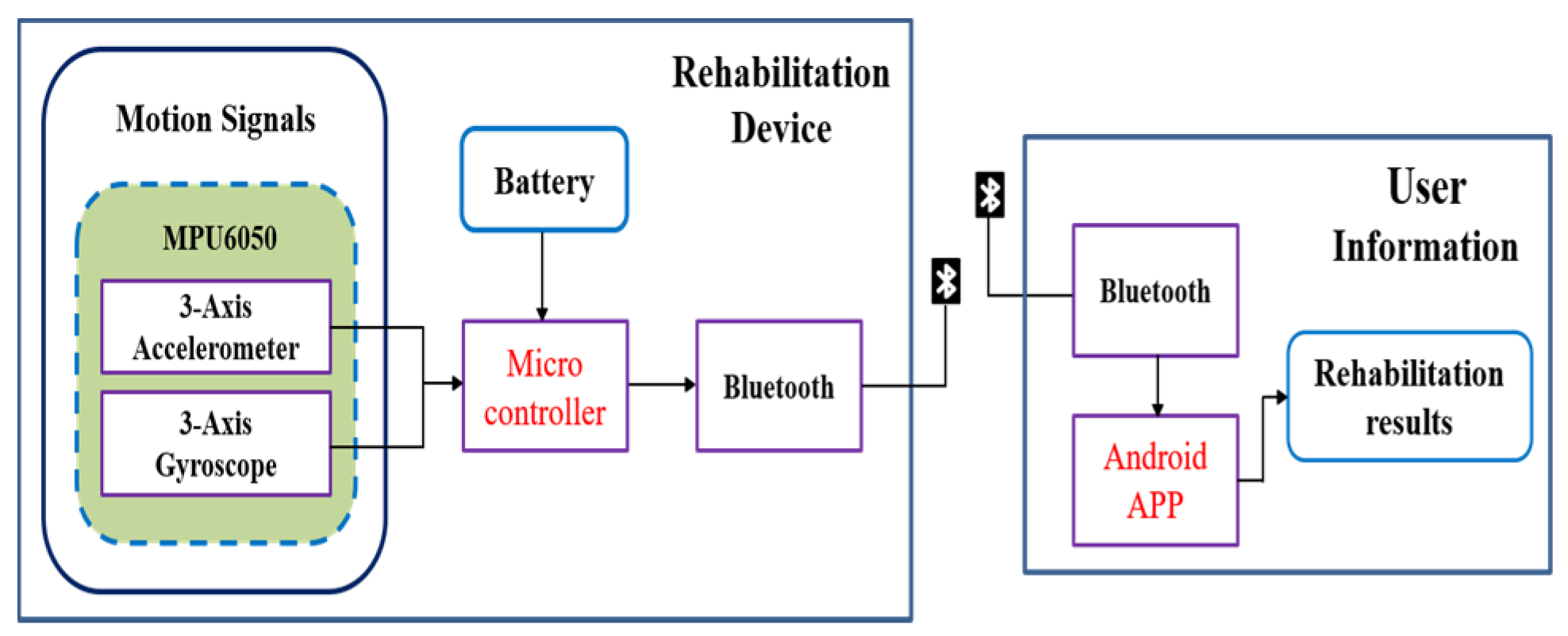
2.1. Hardware Design
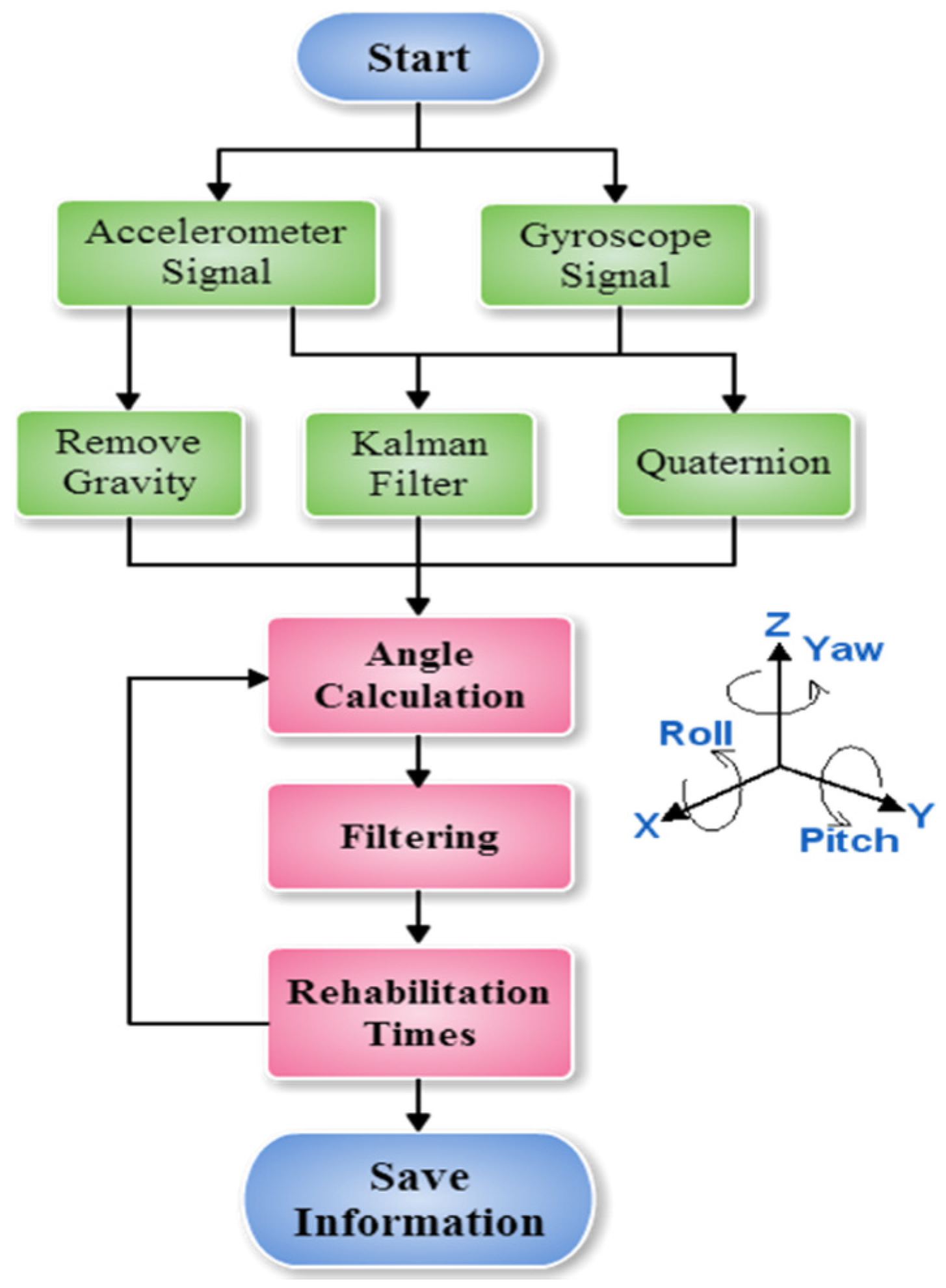
2.2. System Flowchart
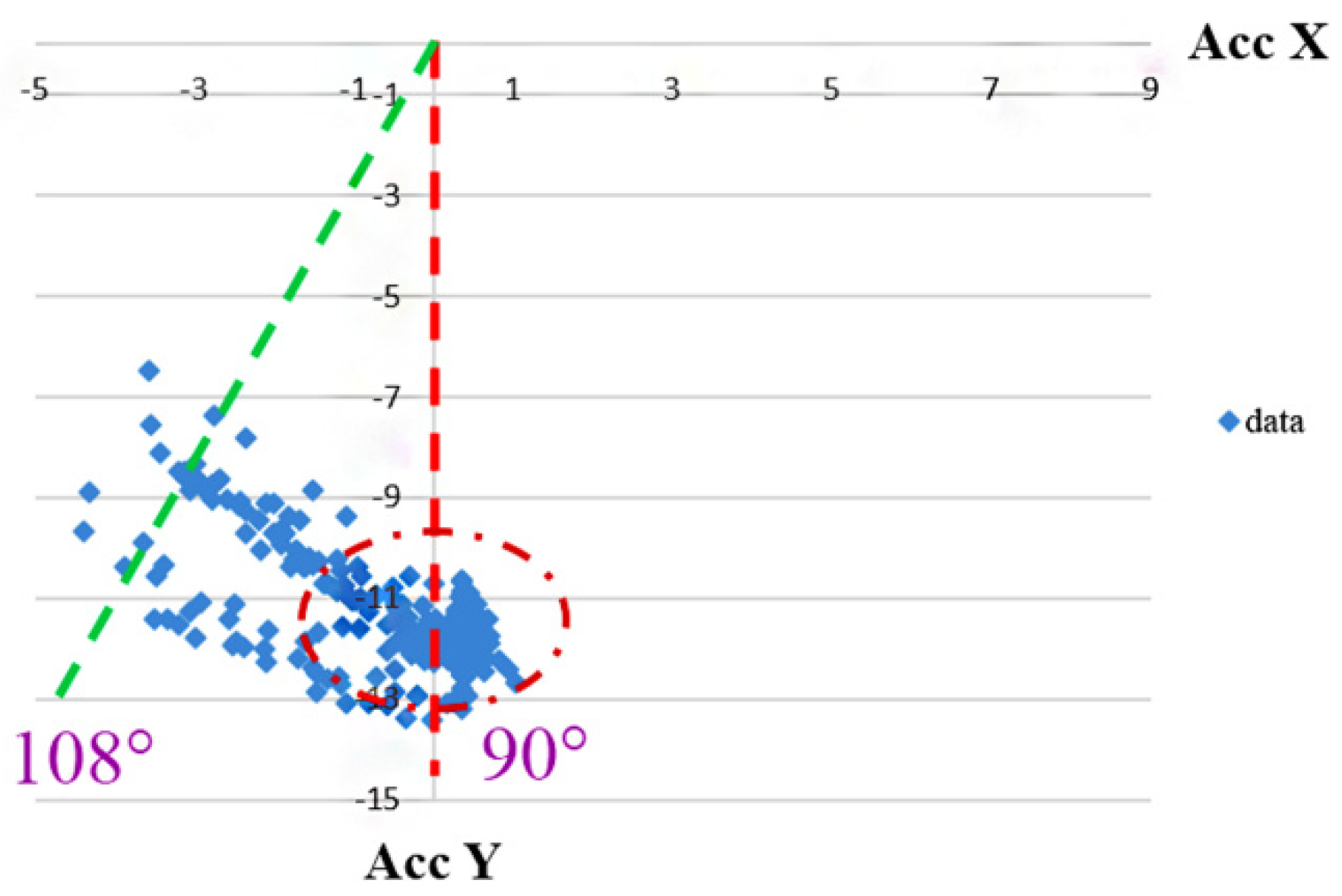
2.3. Effect of Gravity on Angle Measurement
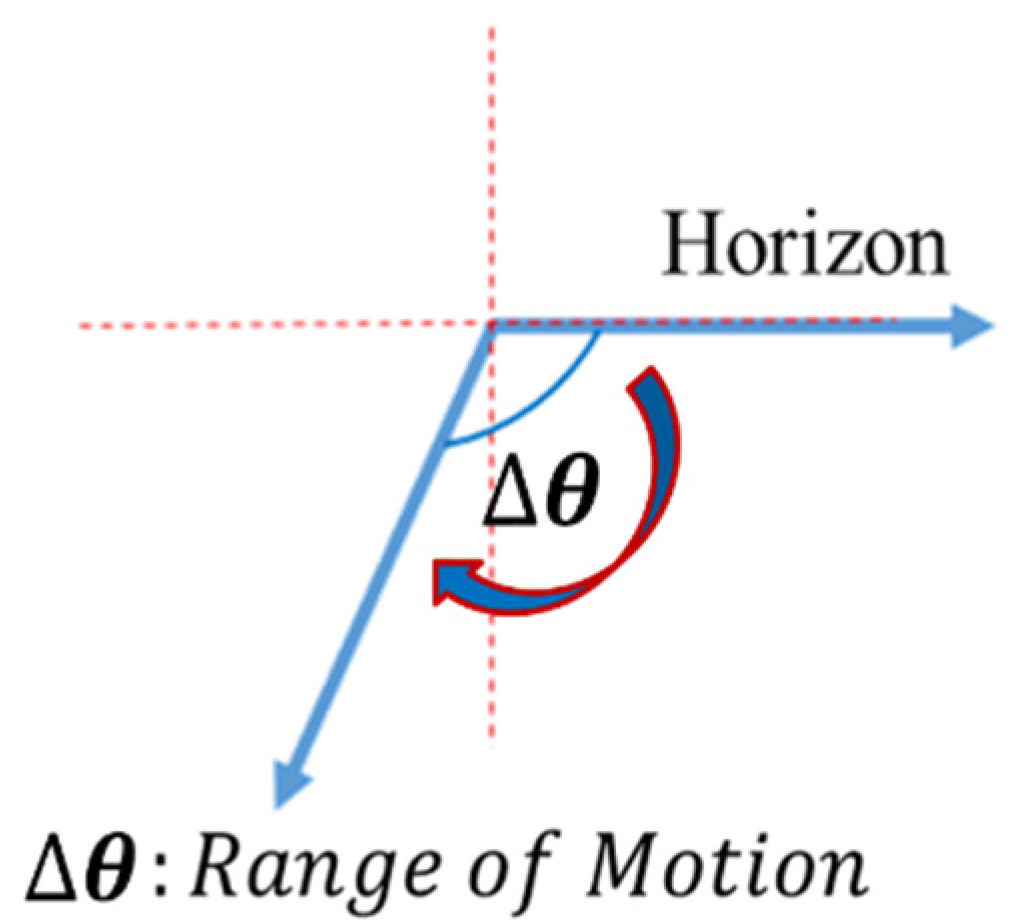
2.4. Knee Angle Calculation
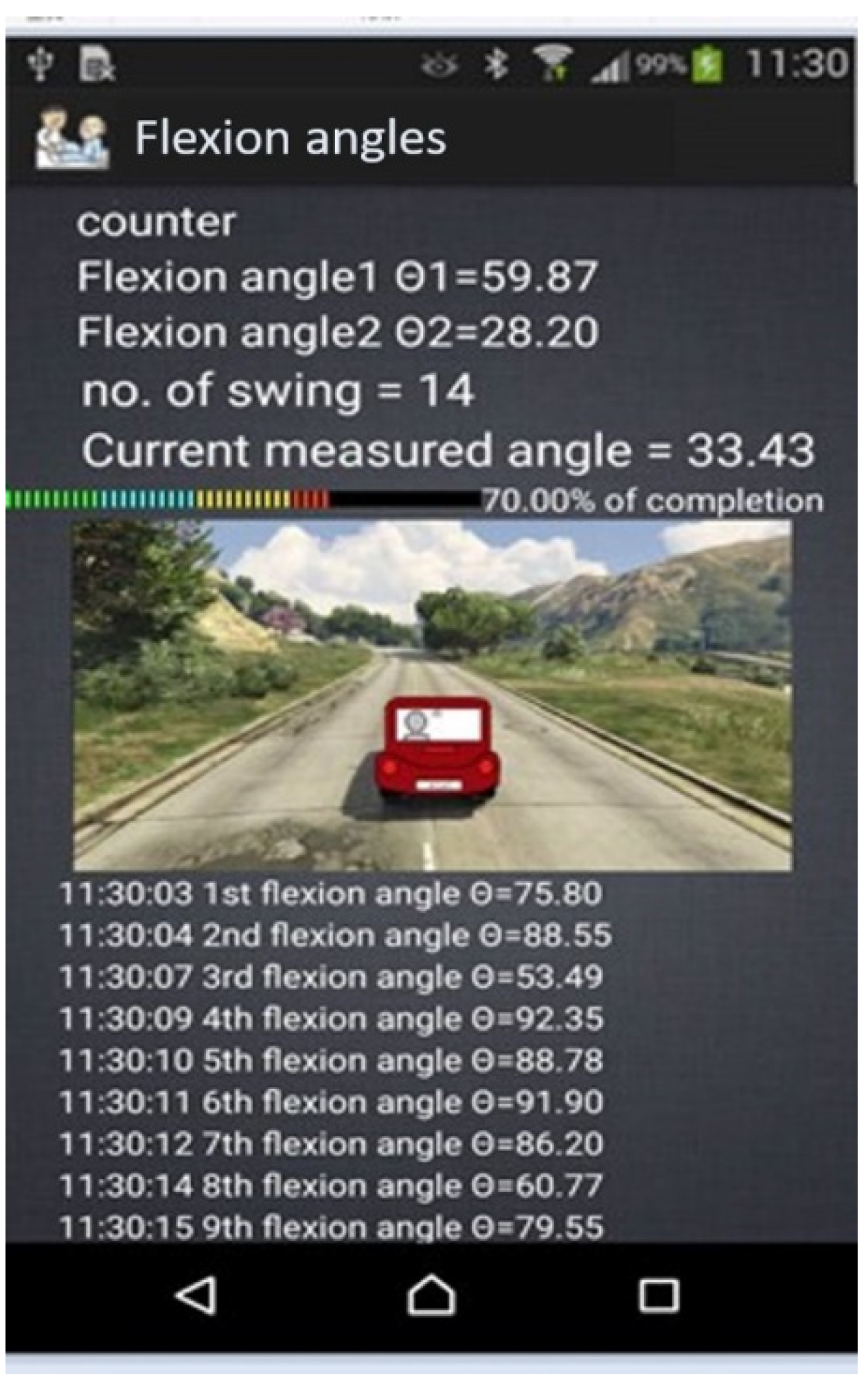
3. Monitoring Rehabilitation Progress
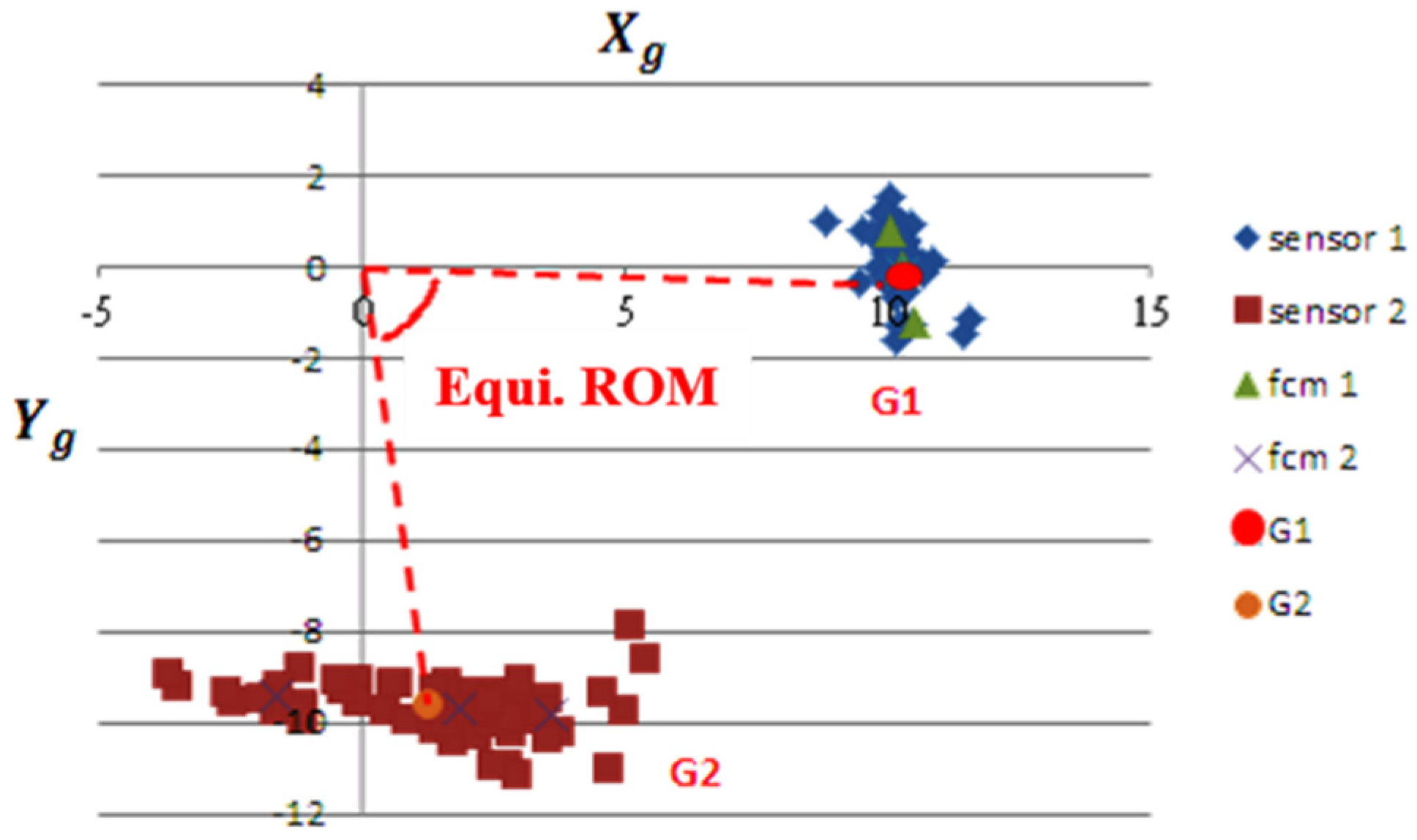
3.1. Equivalent Angles of Knee Motion from FCM
3.2. Monitoring the Effect of Rehabilitation
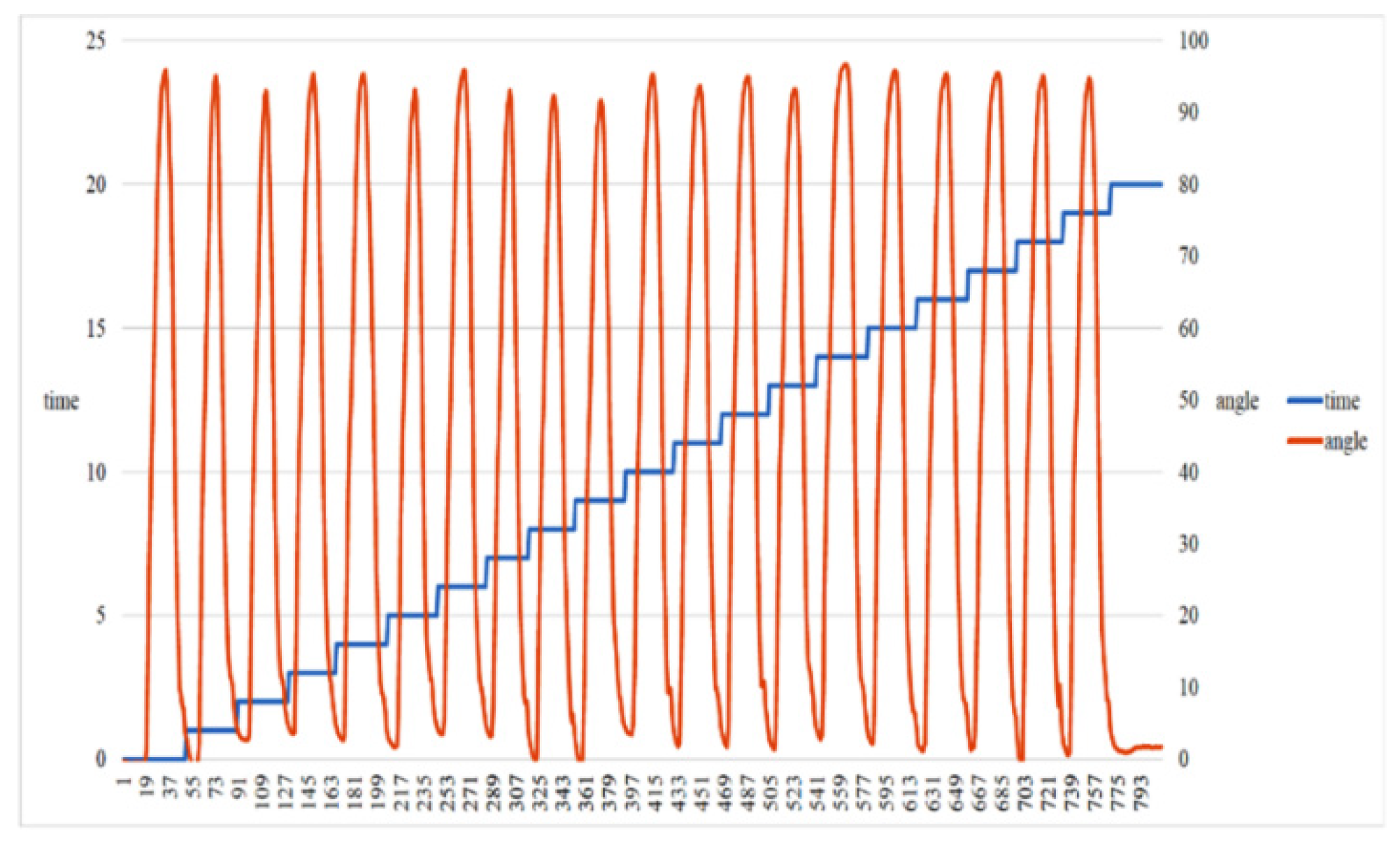
3.3. Quantile Plot for Swing Progress
4. Experimental Results and Analysis
4.1. Results from Subjects Without Using Cybex
4.2. Equivalent ROM
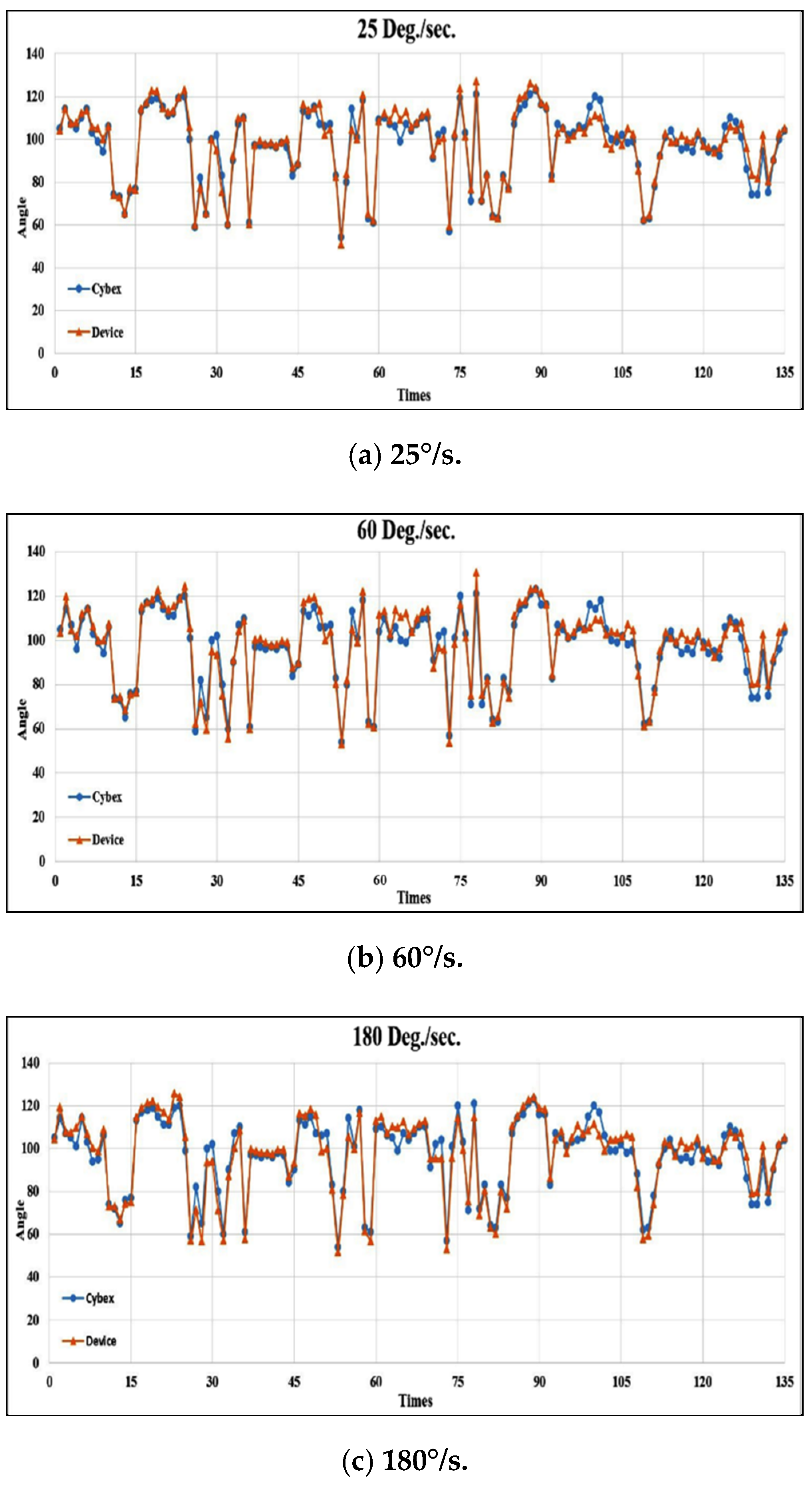
4.3. Results from Healthy Control Subjects
4.4. Results from TKR Subjects
5. Conclusions and Future Work
Author Contributions
Funding
Conflicts of Interest
References
- Baird, C. Self-caring of women with osteoarthritis living at different levels of independence. Health Care Women Int. 2003, 24, 617–634. [Google Scholar] [CrossRef] [PubMed]
- Available online: http://jtfhealth.pixnet.net/blog/post/37419968 (accessed on 15 August 2019). (In Chinese).
- Available online: https://orthoinfo.aaos.org/en/treatment/total-knee-replacement/ (accessed on 12 August 2019).
- Available online: https://www.cgmh.org.tw/cgmn/category.asp?id_seq=1608036#.XEsUd0xuJZU (accessed on 10 August 2019). (In Chinese).
- Zhang, Z.; Liparulo, L.; Panella, M.; Gu, X.; Fang, Q. A fuzzy kernel motion classifier for autonomous stroke rehabilitation. IEEE J. Biomed. Health Inf. 2016, 20, 893–901. [Google Scholar] [CrossRef] [PubMed]
- Jones, P.; Woodgate, S.; Williams, D.; Biggs, P.; Nicholas, K.; Button, K.; Corcoran, P.; Holt, C. Distinguishing between knee rehabilitation exercises using inertial measurement units. Osteoarthr. Cartil. 2018, 26, S380–S381. [Google Scholar] [CrossRef]
- Bahadori, S.; Immins, T.; Wainwright, T.W. A review of wearable motion tracking systems used in rehabilitation following hip and knee replacement. J. Rehabil. Assist. Technol. Eng. 2018, 5, 1–8. [Google Scholar] [CrossRef]
- Friedman, N.; Rowe, J.B.; Reinkensmeyer, D.J.; Bachman, M. The manumeter: A wearable device for monitoring daily use of the wrist and fingers. IEEE J. Biomed. Health Inf. 2014, 18, 1804–1812. [Google Scholar] [CrossRef]
- Mariani, B.; Rochat, S.; Büla, C.J.; Aminian, K. Heel and toe clearance estimation for gait analysis using wireless inertial sensors. IEEE Trans. Biomed. Eng. 2012, 59, 3162–3168. [Google Scholar] [CrossRef]
- Van Der Straaten, R.; De Baets, L.; Jonkers, I.; Timmermans, A. Mobile assessment of the lower limb kinematics in healthy persons and in persons with degenerative knee disorders: A systematic review. Gait Posture 2018, 59, 229–241. [Google Scholar] [CrossRef]
- Kontadakis, G.; Chasiouras, D.; Proimaki, D.; Halkiadakis, M.; Fyntikaki, M.; Mania, K. Gamified platform for rehabilitation after total knee replacement surgery employing low cost and portable inertial measurement sensor node. Multimed. Tools Appl. 2018, 79, 3161–3188. [Google Scholar] [CrossRef]
- Seel, T.; Raisch, J.; Schauer, T. IMU-based joint angle measurement for gait analysis. Sensors 2014, 14, 6891–6909. [Google Scholar] [CrossRef]
- Bakhshi, S.; Mahoor, M.H.; Davidson, B.S. Development of a body joint angle measurement system using IMU sensors. In Proceedings of the 33rd Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Boston, MA, USA, 30 August–3 September 2011; pp. 6923–6926. [Google Scholar]
- Huang, Y.-P.; Liu, W.-H.; Chen, S.-Y.; Sandnes, F.E. Using type-2 fuzzy models to detect fall incidents and abnormal gaits among elderly. In Proceedings of the IEEE International Conference on Systems, Man and Cybernetics, Manchester, UK, 13–16 October 2013; pp. 3441–3446. [Google Scholar]
- Hsu, Y.-L.; Chung, P.-C. (Julia); Wang, W.-H.; Pai, M.-C.; Wang, C.-Y.; Lin, C.-W.; Wu, H.-L.; Wang, J.-S. Gait and balance analysis for patients with Alzheimer’s disease using an inertial-sensor-based wearable instrument. IEEE J. Biomed. Health Inf. 2014, 18, 1822–1830. [Google Scholar] [CrossRef]
- Bei, S.; Zhen, Z.; Xing, Z.; Taocheng, L.; Qin, L. Movement disorder detection via adaptively fused gait analysis based on Kinect sensors. IEEE Sens. J. 2018, 18, 7305–7314. [Google Scholar] [CrossRef]
- Cole, B.T.; Roy, S.H.; De Luca, C.J.; Nawab, S.H. Dynamical learning and tracking of tremor and dyskinesia from wearable sensors. IEEE Trans. Neural Syst. Rehabil. Eng. 2014, 22, 982–991. [Google Scholar] [CrossRef]
- Kluge, F.; Gaßner, H.; Hannink, J.; Pasluosta, C.; Klucken, J.; Eskofier, B.M. A determination method for gait event based on acceleration sensors. Sensors 2019, 19, 5499. [Google Scholar]
- Teufl, W.; Lorenz, M.; Miezal, M.; Taetz, B.; Fröhlich, M.; Bleser, G. Towards inertial sensor based mobile gait analysis: Event-detection and spatio-temporal parameters. Sensors 2018, 19, 38. [Google Scholar] [CrossRef]
- Müller, B.; Ilg, W.; Giese, M.A.; Ludolph, N. Validation of enhanced kinect sensor based motion capturing for gait assessment. PLoS ONE. 2017, 12, e0175813. [Google Scholar] [CrossRef]
- Lorenzi, P.; Rao, R.; Romano, G.; Kita, A.; Irrera, F. Mobile devices for the real-time detection of specific human motion disorders. IEEE Sens. J. 2016, 16, 8220–8227. [Google Scholar]
- Gholami, F.; Trojan, D.A.; Kövecses, J.; Haddad, W.M.; Gholami, B. A Microsoft Kinect-based point-of-care gait assessment framework for multiple sclerosis patients. IEEE J. Biomed. Health Inf. 2017, 21, 1376–1385. [Google Scholar] [CrossRef]
- Kun, L.; Inoue, Y.; Shibata, K.; Enguo, C. Ambulatory estimation of knee-joint kinematics in anatomical coordinate system using accelerometers and magnetometers. IEEE Trans. Biomed. Eng. 2011, 58, 435–442. [Google Scholar] [CrossRef]
- Milosevic, M.; McConville, K.M.V.; Sejdic, E.; Masani, K.; Kyan, M.J.; Popovic, M.R. Visualization of trunk muscle synergies during sitting perturbations using self-organizing maps (SOM). IEEE Trans. Biomed. Eng. 2012, 59, 2516–2523. [Google Scholar] [CrossRef]
- Han, Y.C.; Wong, K.I.; Murray, I. Gait phase detection for normal and abnormal gaits using IMU. IEEE Sens. J. 2019, 19, 3439–3448. [Google Scholar] [CrossRef]
- Hanakova, L.; Kutilek, P.; Socha, V.; Skoda, D.; Takac, P.; Schlenker, J.; Svoboda, Z. An evaluation method of complex movement of the arm during walking based on gyroscope data and angle-angle diagram. In Proceedings of the 38th International Conference on Telecommunications and Signal Processing, Prague, Czech Republic, 9–11 July 2015; pp. 397–402. [Google Scholar]
- Wang, L.; Liu, Z.; Chen, C.L.P.; Zhang, Y.; Lee, S.; Chen, X.A. UKF-based predictable SVR learning controller for biped walking. IEEE Trans. Syst. Man Cybern. Syst. 2013, 43, 1440–1450. [Google Scholar] [CrossRef]
- Zihajehzadeh, S.; Park, E.J. A novel biomechanical model-aided IMU/UWB fusion for magnetometer-free lower body motion capture. IEEE Trans. Syst. Man Cybern. Syst. 2017, 47, 927–938. [Google Scholar] [CrossRef]
- Wang, W.; Hou, Z.-G.; Cheng, L.; Tong, L.; Peng, L.; Peng, L.; Tan, M. Toward patients’ motion intention recognition: Dynamics modeling and identification of iLeg—An LLRR under motion constraints. IEEE Trans. Syst. Man Cybern. Syst. 2016, 46, 980–992. [Google Scholar] [CrossRef]
- Ahmed, H.; Tahir, M. Improving the accuracy of human body orientation estimation with wearable IMU sensors. IEEE Trans. Instrum. Meas. 2017, 66, 535–542. [Google Scholar] [CrossRef]
- Huang, Y.-P.; Singh, P.; Kuo, H.-C. A hybrid fuzzy clustering approach for the recognition and visualization of MRI images of Parkinson’s disease. IEEE Access 2020, 8, 25041–25051. [Google Scholar] [CrossRef]








| Size | 33 mm × 32.5 mm × 16 mm |
| MCU | ATMEGA328P |
| IMU | GY-521(MPU6050) |
| Bluetooth | Arduino HC06 |
| Battery | Lithium battery 7.4 V |
| Endurance | 17.5 h |
| Gender | M | F |
| Number | 7 | 4 |
| Age (years) | 33.71 ± 13.50 | 42.25 ± 12.97 |
| Height (cm) | 172.29 ± 8.10 | 154.50 ± 4.33 |
| Weight (Kg) | 70.29 ± 7.83 | 53.00 ± 1.87 |
| Knee | Normal | Normal |
| Gender | M | F |
| Number | 8 | 8 |
| Age (years) | 64 ± 9.97 | 32.13 ± 16.06 |
| Height (cm) | 162.13 ± 2.52 | 159.38 ± 3.28 |
| Weight (Kg) | 68.39 ± 4.33 | 54.5 ± 4.15 |
| Knee | Normal | Normal |
| Gender | M | F |
| Number | 2 | 6 |
| Age (years) | 63.00 ± 3.00 | 70.67 ± 8.24 |
| Height (cm) | 161.70 ± 5.7 | 150.82 ± 3.75 |
| Weight (Kg) | 79.10 ± 9.10 | 57.43 ± 6.89 |
| TKR (month) | 7.50 ± 4.50 | 24.17 ± 16.80 |
| Cybex | 25°/s | 60°/s | 180°/s |
| Average absolute error (degree) | 2.90 | 3.51 | 4.00 |
| Standard Deviation (degree) | 2.57 | 2.67 | 2.49 |
| Accuracy (%) | 97.01 | 96.31 | 95.77 |
| Cybex | 25°/s | 60°/s | 180°/s |
| Average absolute error (degree) | 1.65 | 2.74 | 3.27 |
| Standard Deviation (degree) | 1.29 | 2.05 | 1.54 |
| Average accuracy (%) | 98.09 | 96.71 | 96.16 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Huang, Y.-P.; Liu, Y.-Y.; Hsu, W.-H.; Lai, L.-J.; Lee, M.S. Monitoring and Assessment of Rehabilitation Progress on Range of Motion After Total Knee Replacement by Sensor-Based System. Sensors 2020, 20, 1703. https://doi.org/10.3390/s20061703
Huang Y-P, Liu Y-Y, Hsu W-H, Lai L-J, Lee MS. Monitoring and Assessment of Rehabilitation Progress on Range of Motion After Total Knee Replacement by Sensor-Based System. Sensors. 2020; 20(6):1703. https://doi.org/10.3390/s20061703
Chicago/Turabian StyleHuang, Yo-Ping, Yu-Yu Liu, Wei-Hsiu Hsu, Li-Ju Lai, and Mel S. Lee. 2020. "Monitoring and Assessment of Rehabilitation Progress on Range of Motion After Total Knee Replacement by Sensor-Based System" Sensors 20, no. 6: 1703. https://doi.org/10.3390/s20061703
APA StyleHuang, Y.-P., Liu, Y.-Y., Hsu, W.-H., Lai, L.-J., & Lee, M. S. (2020). Monitoring and Assessment of Rehabilitation Progress on Range of Motion After Total Knee Replacement by Sensor-Based System. Sensors, 20(6), 1703. https://doi.org/10.3390/s20061703






