m-SFT: A Novel Mobile Health System to Assess the Elderly Physical Condition
Abstract
1. Introduction
2. Material and Methods
2.1. Related Work
- Chronic care management apps. This category contains the apps designed to deal with Chronic diseases and their symptom. This category enclosed the apps for managing blood pressure, glucose levels for diabetes, mental health and other illnesses. Besides the applications in the public app markets, from the research perspective various interventions have been proposed in the context of clinical studies, such as depression treatment [19], diabetes control [20], hypertension control [21], and psychological support [22,23].
- Healthcare and Fitness Apps. This type of applications seeks for a behavioural change in the users, by tracking their habits with respect to the meals and the sport and providing tailored recommendations. They can be classified in two wide groups: (i) Apps that track the calorie intake such us Lifesum [24]. (ii) Apps that register physical activity using not only the sensors in the phone but other weareable devices such us activity bracelets or smartch watchs. Example of this apps are GoogleFit [25] or Endomondo [26] among others. Among the clinical studies we can remark the one in [27] that aims for a reduction of calorie intake by use of personal digital assistant applications for diet and exercise, or the one in [28] which consist on mobile phone application intervention to increase physical activity levels.
- Medication Management Apps. Within this group they are comprised the apps that keep track of medication intake in order to improve its adherence among patients, they are specially useful among the elderly.
- Personal Health Record Apps. Among this category we can find the applications that allow patients to store their medical conditions data, allergies etc. and share it with their doctors.
- Emergency situations detection. This sector involve the apps that are able to detect if the elderly is in a danger situation, i.e., falls or disorientation, if this is the case, the app fire a flag to the elderly’s caregivers or relative or to the emergency services to assist the person in danger.
- Behaviour changing and physical tele-rehabilitation. Among this category we can find out as well some e-health platforms that provides advice and training exercises on how to recover from certain problems. For example activehip [29] is a tele-rehabilitation platform designed for elderly patients recovering from a hip fracture. DIGIREHAB, [30] that is a Danish platform that provides objective assessment of each patients’ need for assistance and his/her general level of ability. Together, these assessments form a precise image of the patients’ physical potential for rehabilitation. We can find out as well other prototypes of mobile solutions for the elderly population that suffers from low vision based on a digital image enhancement [23,31,32,33,34].
2.2. Senior Fitness Test
3. Results
3.1. The Proposed App, m-SFT
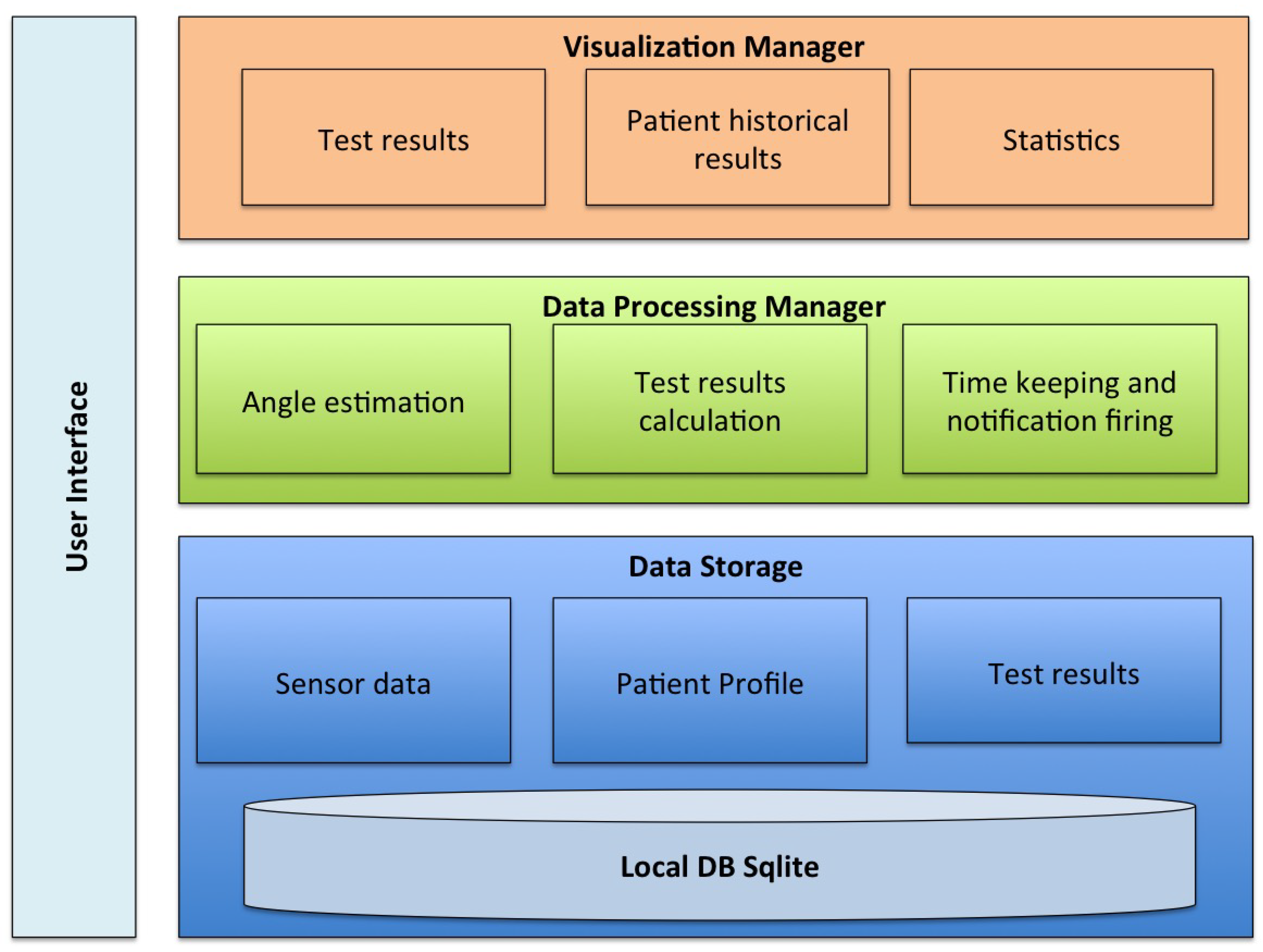
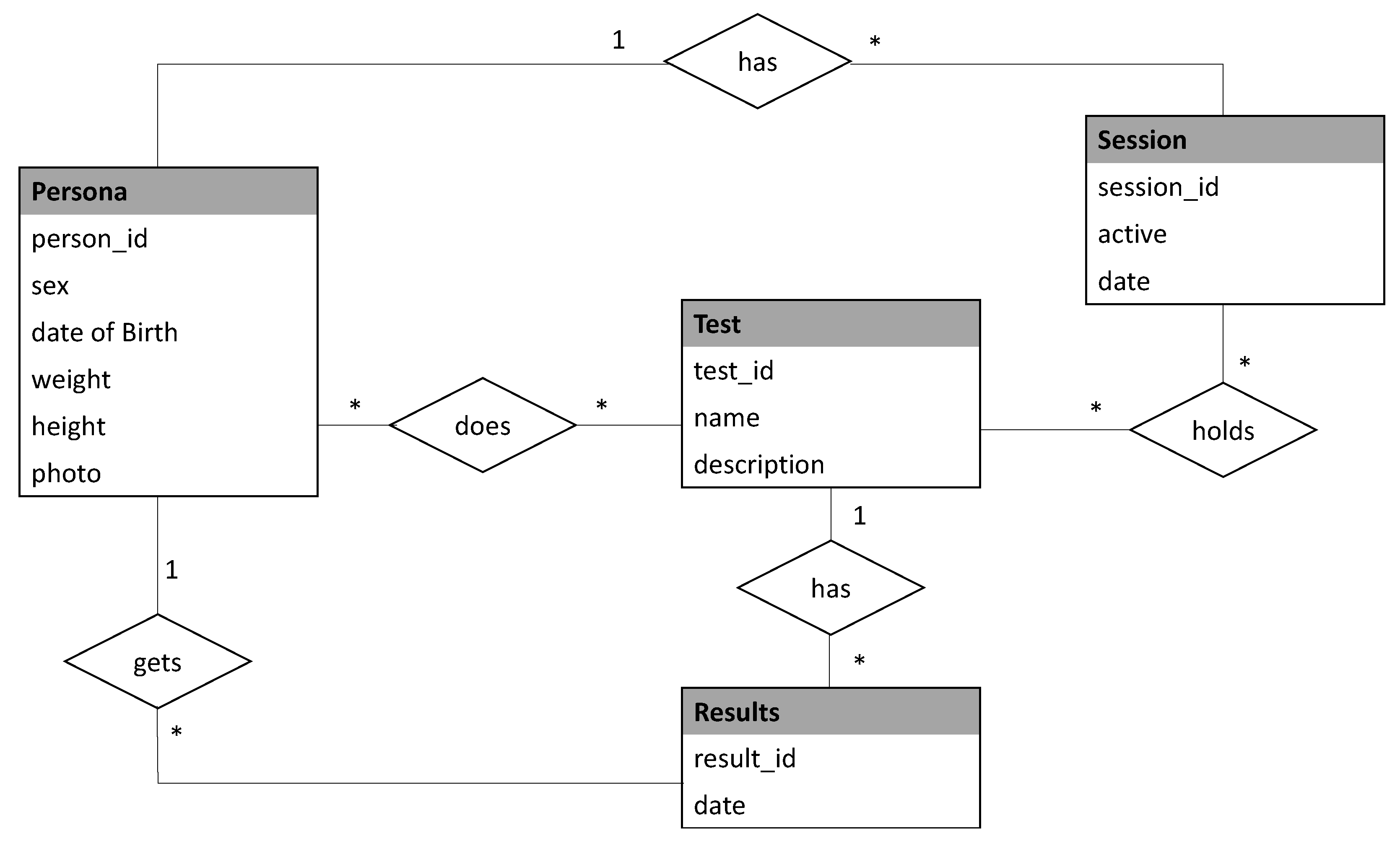
3.1.1. App Implementation
3.1.2. Sensor Interface
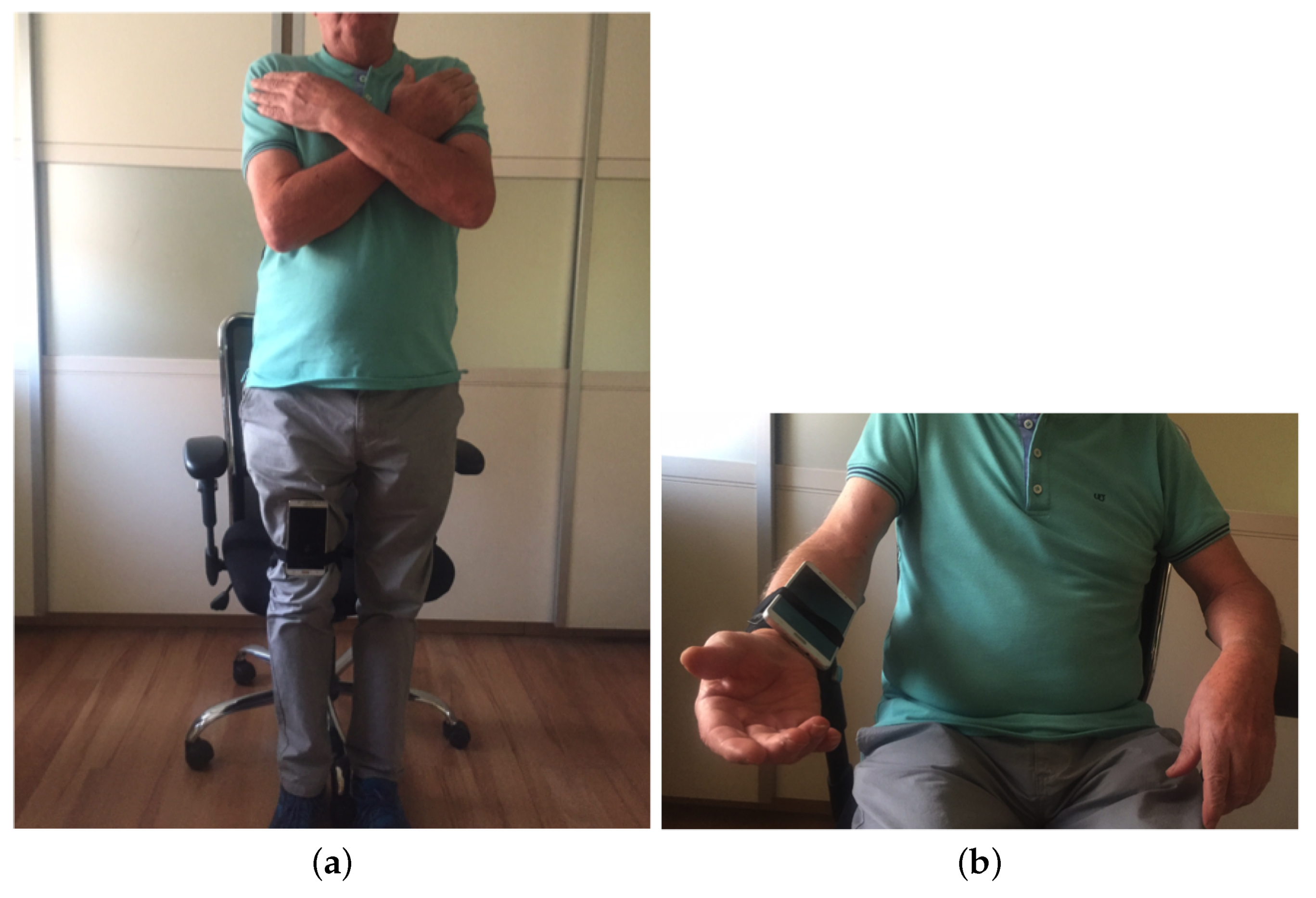
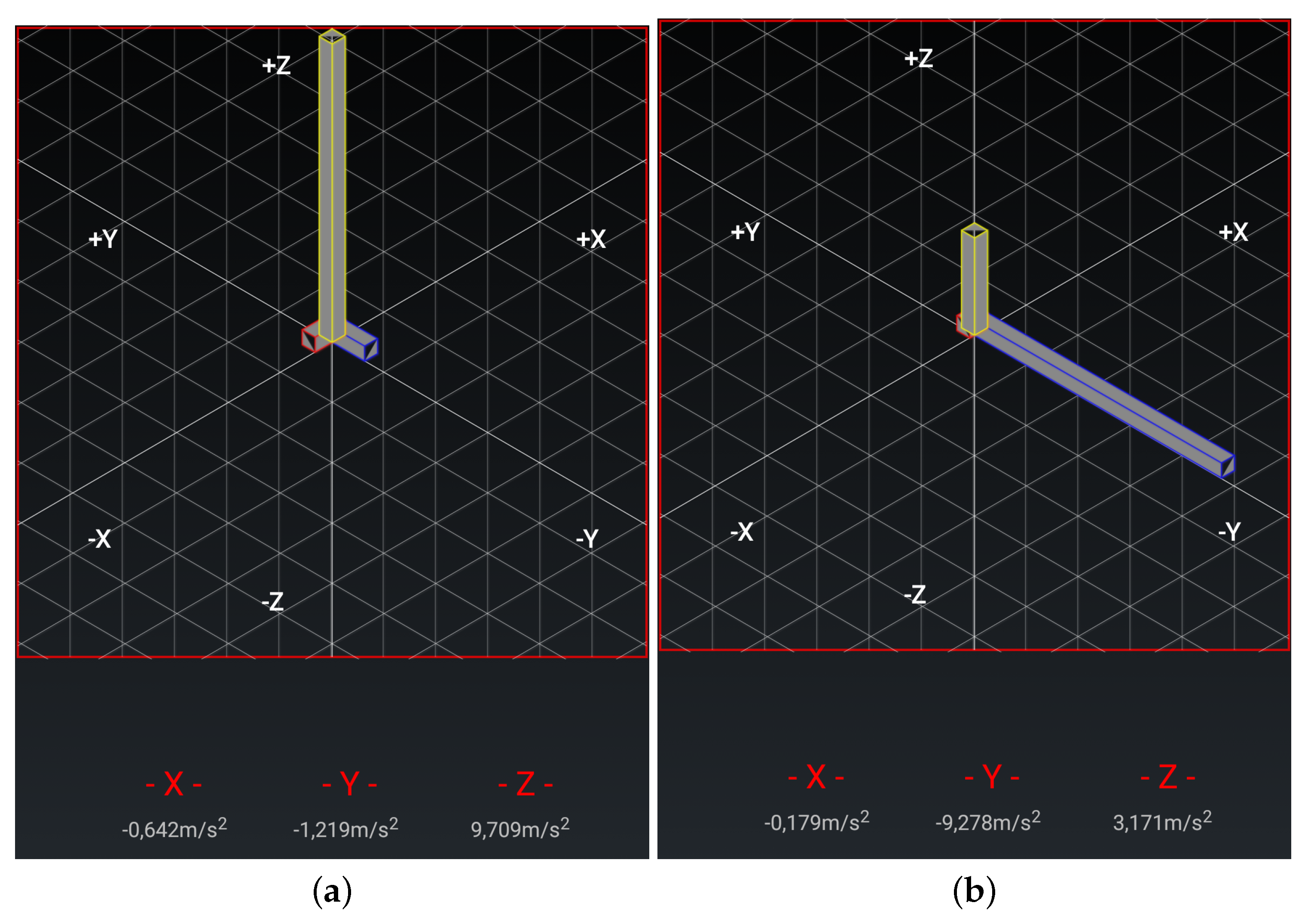
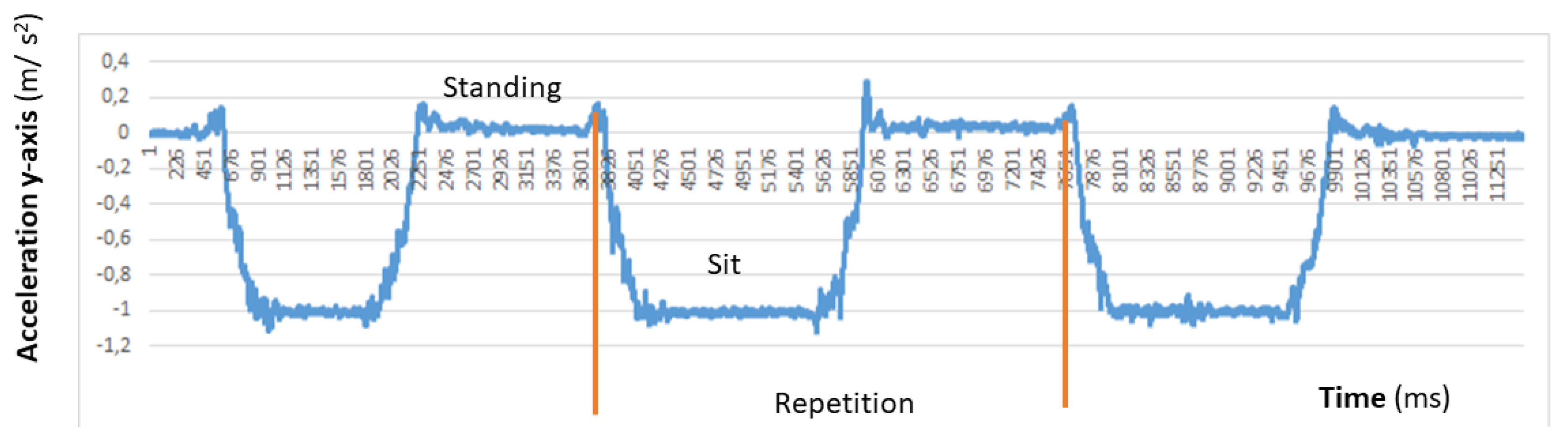
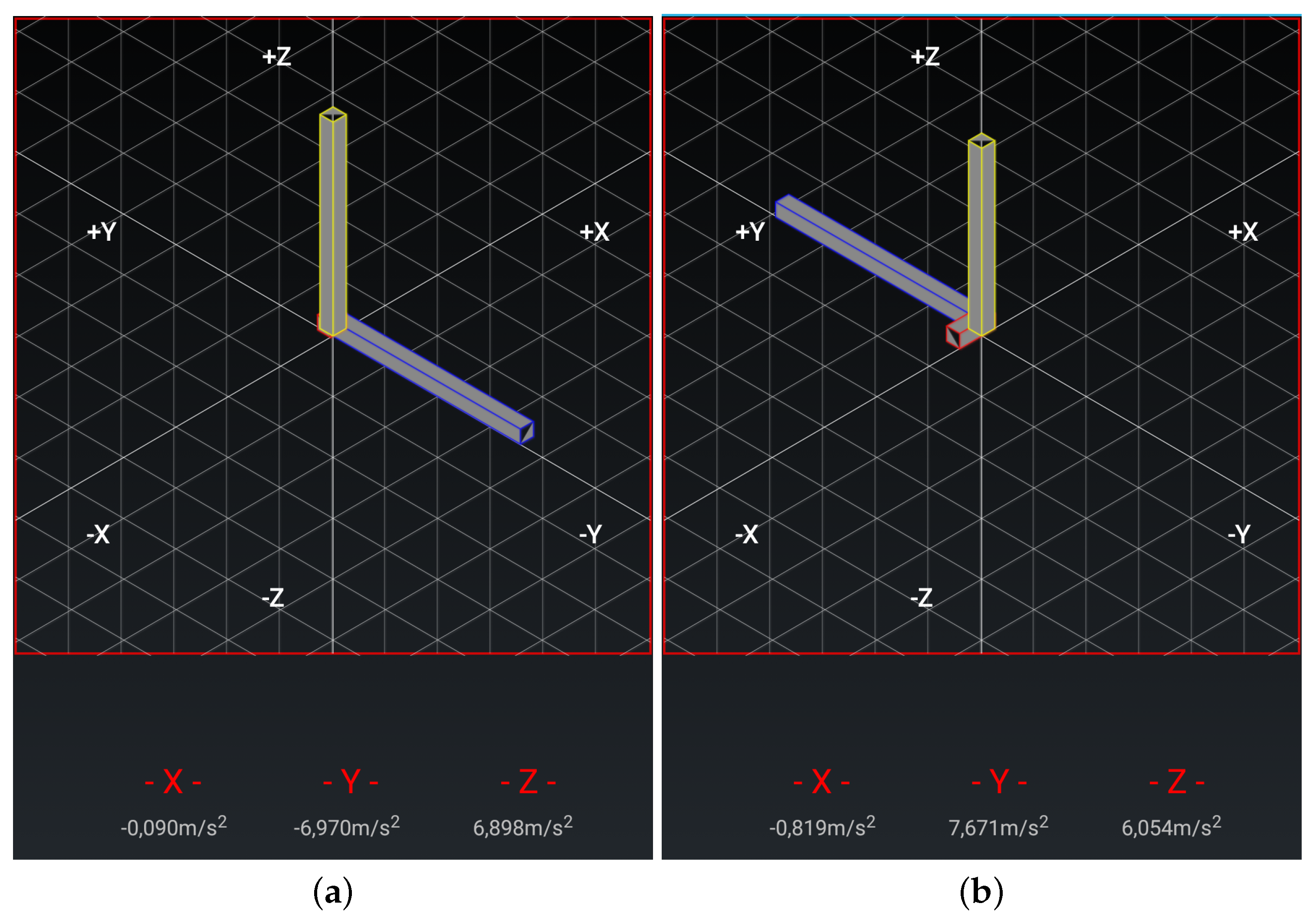
- Chair Stand test To carry out this test item, the mobile device has to be attached to the leg as depicted in Figure 3a. At the beginning of each repetition the acceleration in the direction of the y-axis is about 0 m/s, that is, the user is sat and the phone is almost parallel to the floor. Then the user has to stand up placing the phone upside down and perpendicular to the floor, being the acceleration in the y axis about −9.8 m/s. Finally the repetition is completed once the acceleration in y becomes 0 again. Figure 4 shows the values of the acceleration for this exercise when the user is standing and when is sit, while Figure 5 shows the evolution of the acceleration in the y-axis during several iterations. Note that the changes of the acceleration in the z-axis is not relevant in this case. This change is due to slightly changes in the phone height when attached to the leg and the acceleration in the x axis is not relevant and normally is close to zero. The datum point in the acceleration for the classification is the change in the value of the acceleration in the y-axis when it reaches −9.8 m/s indicating that the user is completely vertical. Finally, it is worth remarking that when designing our system, we considered more complex machine learning based classifiers. Nevertheless, these type of classifiers are not suitable to provide real time operation in a low resource smartphone. Therefore, giving that the performance of the proposed detection algorithm is good enough in practice, we decided to keep it to ensure the reliability of the system and the real time performance even with a low cost smartphone. However the inclusion of more sophisticated movement detection algorithms for powerful smartphones will be considered as future work.
- Arm curl test In this case the user has the arm fully extended with the fist towards down, and with the mobile device attached to the forearm, leaving it upside down as in Figure 3b. In this posture, the acceleration in y is negative. At the mid point of the exercise the acceleration on y becomes positive and higher to 7.5 m/s, finally, the repetition is considered as completed when the acceleration comes back to the initial state. In Figure 6a,b we can observe both the acceleration at the beginning and at the midpoint of the exercise respectively.
- 2-min step in place test To accomplish this test item the phone should be attached in the same way than for the chair stand test, (see Figure 3a). At the beginning the user is standing, and so the phone is upside down and perpendicular to the floor, being the acceleration in y around −9.8 m/s. At the mid point of the exercise the acceleration in y evolves to 0 m/s (the user will be sit and so the phone will be almost parallel to the floor). The repetition is complete once the acceleration comes back to the initial state.
- Chair sit and reach test and back scratch test For this test item we have not implemented yet the feature that allows assessing the distance between the two hands, therefore in this first version of the platform this distance needs to be measured and introduce manually in the system by the practitioner. For future implementation, the option that we are considering is the inclusion of image analysis techniques to determine this distance in both tests [42] from a calibrated image taken during the test execution. We are aware that this is a valid option when the system is used by a health professional to monitor and track patients, but is difficult to use by an end-user, in that second case probably additional sensors will be required.
- 8-foot up and go test This test item does not requires the patient to attach the phone, since the only sensor required is the chronometer. Therefore either the patient or the health practitioner has to start and stop the chronometer in the app, and the completion time will be automatically updated in the patient records.
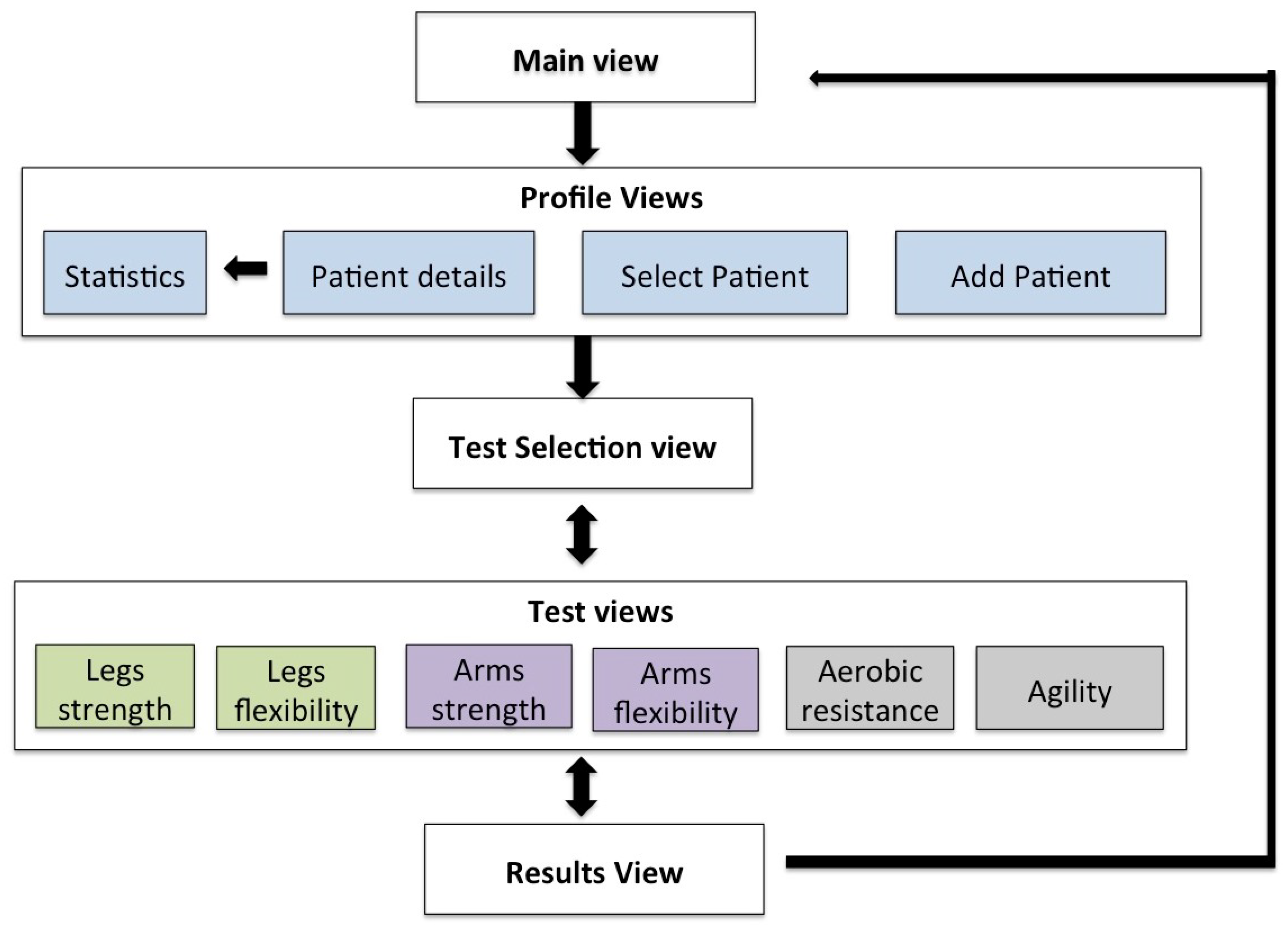
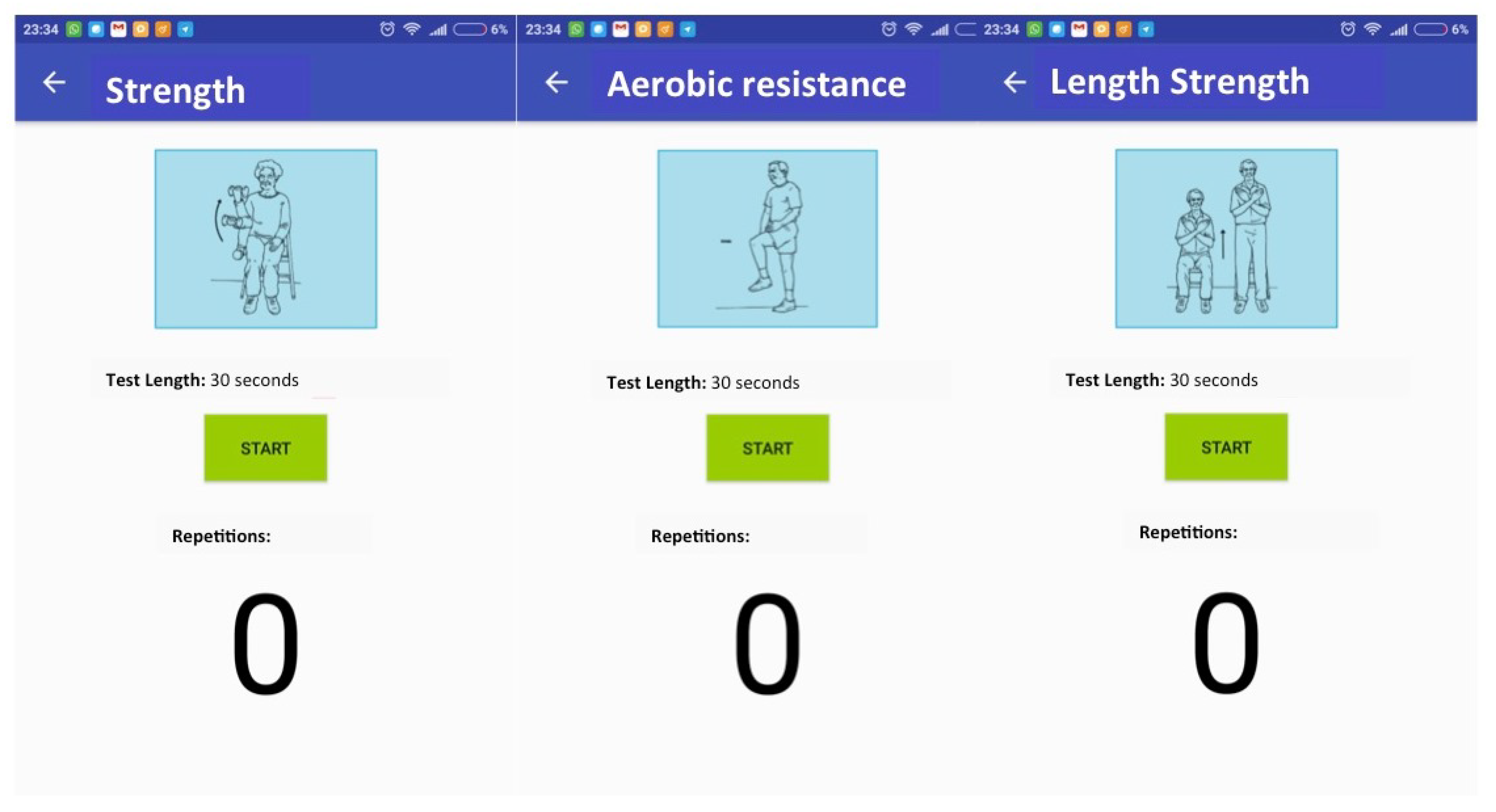
3.1.3. User Interface
3.2. m-SFT Evaluation
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- OECD. OECD Health at a Glance 2013: OECD Indicators. 2013. Available online: http://www.oecd.org/els/healthsystems/Health-at-a-Glance-2013.pdf (accessed on 21 November 2019).
- EU-Statistics. Eurostat People in the EU-Statistics on an Ageing Society; Technical Report; Statistical Office of the European Communities (EUROSTAT): Luxembourg, 2016. [Google Scholar]
- Oshima Lee, E.; Emanuel, E.J. Shared Decision Making to Improve Care and Reduce Costs. N. Engl. J. Med. 2013, 368, 6–8. [Google Scholar] [CrossRef] [PubMed]
- Merrell, R.C.; Author, C. Geriatric Telemedicine: Background and Evidence for Telemedicine as a Way to Address the Challenges of Geriatrics. Heal. Inf. Res 2015, 21, 223–229. [Google Scholar] [CrossRef] [PubMed][Green Version]
- National Council on Aging. Healthy Aging Facts; National Council on Aging: Arlington, VA, USA, 2014. [Google Scholar]
- Helbostad, J.L.; Vereijken, B.; Becker, C.; Todd, C.; Taraldsen, K.; Pijnappels, M.; Aminian, K.; Mellone, S. Mobile Health Applications to Promote Active and Healthy Ageing. Sensors 2017, 17, 622. [Google Scholar] [CrossRef] [PubMed]
- Caspersen, C.J.; Powell, K.E.; Christenson, G.M. Physical activity, exercise, and physical fitness: Definitions and distinctions for health-related research. Public Health Rep. 1985, 100, 126–131. [Google Scholar]
- College and Position Stand. Exercise and Physical Activity in older adults. Med. Sci. Sport Exerc. 1998, 30, 992–1008. [Google Scholar]
- Iliffe, S.; Kendrick, D.; Morris, R.; Griffin, M.; Haworth, D.; Carpenter, H. Promoting physical activity in older people in general practice: ProAct65 cluster randomised controlled trial. Br. J. Gen. Pract. 2015, 65, e731–e738. [Google Scholar] [CrossRef]
- Peek, S.T.; Wouters, E.J.; van Hoof, J.; Luijkx, K.G.; Boeije, H.R.; Vrijhoef, H.J. Factors influencing acceptance of technology for aging in place: A systematic review. Int. J. Med. Inform. 2014, 83, 235–248. [Google Scholar] [CrossRef]
- Hassett, L.; van den Berg, M.; Lindley, R.I.; Crotty, M.; McCluskey, A.; van der Ploeg, H.P.; Smith, S.T.; Schurr, K.; Killington, M.; Bongers, B.; et al. Effect of affordable technology on physical activity levels and mobility outcomes in rehabilitation: A protocol for the Activity and MObility UsiNg Technology (AMOUNT) rehabilitation trial. BMJ Open 2016, 6, e012074. [Google Scholar] [CrossRef]
- Eysenbach, G. What is e-health? J. Med. Internet Res. 2001, 3, e20. [Google Scholar] [CrossRef]
- For eHealth, W.G.O. mHealth: New Horizons for Health through Mobile Technologies: Second Global Survey on eHealth. 2011. Available online: http://www.who.int/goe/publications/goe_mhealth_web.pdf (accessed on 22 May 2019).
- Rikli, R.E.; Jones, C.J. Senior Fitness Test Manual; Human Kinetics: New York, NY, USA, 2013; p. 176. [Google Scholar]
- Ignatov, A. Real-time human activity recognition from accelerometer data using Convolutional Neural Networks. Appl. Soft Comput. 2018, 62, 915–922. [Google Scholar] [CrossRef]
- Joosen, P.; Piette, D.; Buekers, J.; Taelman, J.; Berckmans, D.; De Boever, P. A smartphone-based solution to monitor daily physical activity in a care home. J. Telemed. Telecare 2019, 25, 611–622. [Google Scholar] [CrossRef] [PubMed]
- Research, Z.M. mHealth Market by Devices, by Stakeholder, by Service, by Therapeutics and by Applications: Global Industry Perspective, Comprehensive Analysis and Forecast, 2014–2022. Available online: https://www.zionmarketresearch.com/report/mhealth-market (accessed on 24 April 2018).
- Boulos, M.N.K.; Wheeler, S.; Tavares, C.; Jones, R. How Smartphones are Changing the Face of Mobile and Participatory Healthcare: An Overview, with Example from eCAALYX. Biomed. Eng. 2011, 10, 24. [Google Scholar] [CrossRef] [PubMed]
- Bexelius, C.; Löf, M.; Sandin, S.; Trolle Lagerros, Y.; Forsum, E.; Litton, J.E. Measures of Physical Activity Using Cell Phones: Validation Using Criterion Methods. J. Med. Internet Res. 2010, 12, e2. [Google Scholar] [CrossRef] [PubMed]
- Desveaux, L.; Shaw, J.; Saragosa, M.; Soobiah, C.; Marani, H.; Hensel, J.; Agarwal, P.; Onabajo, N.; Bhatia, S.R.; Jeffs, L. A Mobile App to Improve Self-Management of Individuals With Type 2 Diabetes: Qualitative Realist Evaluation. J. Med. Internet Res. 2018, 20, e81. [Google Scholar] [CrossRef]
- Carrasco, M.; Salvador, C.; Sagredo, P.; Marquez-Montes, J.; Gonzalez de Mingo, M.; Fragua, J.; Rodriguez, M.; Garcia-Olmos, L.; Garcia-Lopez, F.; Carrero, A. Impact of Patient-General Practitioner Short-Messages-Based Interaction on The Control of Hypertension in a Follow-up Service for Low-to-Medium Risk Hypertensive Patients: A Randomized Controlled Trial. IEEE Trans. Inf. Technol. Biomed. 2008, 12, 780–791. [Google Scholar] [CrossRef]
- Grassi, A.; Gaggioli, A.; Riva, G. The Use of Mobile Narratives for Reducing Stress in Commuters. Cyberpsychol. Behav. 2009, 12, 155–161. [Google Scholar] [CrossRef]
- Chacon-Lopez, H.; Pelayo, F.J.; Lopez-Justicia, M.D.; Morillas, C.A.; Urena, R.; Chacon-Medina, A.; Pino, B. Visual training and emotional state of people with retinitis pigmentosa. J. Rehabil. Res. Dev. 2013, 50, 1157–1168. [Google Scholar] [CrossRef]
- LifeSum. LifeSum. 2018. Available online: https://lifesum.com/ (accessed on 27 August 2018).
- Google. GoogleFit. 2018. Available online: https://www.google.com/fit/ (accessed on 27 August 2018).
- Endomondo. Endomondo Sport Tracker. 2018. Available online: https://www.endomondo.com/ (accessed on 27 August 2018).
- Burke, L.E.; Conroy, M.B.; Sereika, S.M.; Elci, O.U.; Styn, M.A.; Acharya, S.D.; Sevick, M.A.; Ewing, L.J.; Glanz, K. The Effect of Electronic Self-Monitoring on Weight Loss and Dietary Intake: A Randomized Behavioral Weight Loss Trial. Obesity 2011, 19, 338–344. [Google Scholar] [CrossRef]
- King, A.C.; Ahn, D.K.; Oliveira, B.M.; Atienza, A.A.; Castro, C.M.; Gardner, C.D. Promoting Physical Activity through Hand-Held Computer Technology. Am. J. Prev. Med. 2008, 34, 138–142. [Google Scholar] [CrossRef]
- Active Hip, Plataforma de Telerehabilitacion de Cadera. Available online: http://activehip.es/ (accessed on 24 August 2018).
- DigiRehab. DigiRehab. Available online: https://portal.digirehab.dk/ContentId/8214/Default.aspx?Language=2057 (accessed on 27 August 2018).
- Ureña, R.; Martínez-Cañada, P.; Gómez-López, J.M.; Morillas, C.A.; Pelayo, F.J. A Portable Low Vision Aid based on GPU. In Proceedings of the 1st International Conference on Pervasive and Embedded Computing and Communication Systems, PECCS 2011, Vilamoura, Algarve, Portugal, 5–7 March 2011; pp. 201–206. [Google Scholar]
- Ureña, R.; Martínez-Cañada, P.; Gómez-López, J.M.; Morillas, C.A.; Pelayo, F.J. Real-time tone mapping on GPU and FPGA. EURASIP J. Image Video Process. 2012, 2012, 1. [Google Scholar] [CrossRef]
- Martínez-Cañada, P.; Morillas, C.A.; Ureña, R.; López, F.M.G.; Pelayo, F.J. Embedded system for contrast enhancement in low-vision. J. Syst. Archit. Embed. Syst. Des. 2013, 59, 30–38. [Google Scholar] [CrossRef]
- Ureña, R.; Morillas, C.A.; Pelayo, F.J. Real-time bio-inspired contrast enhancement on GPU. Neurocomputing 2013, 121, 40–52. [Google Scholar] [CrossRef]
- Mellone, S.; Tacconi, C.; Chiari, L. Validity of a Smartphone-Based Instrumented Timed Up and Go. Gait Posture 2012, 36, 163–165. [Google Scholar] [CrossRef] [PubMed]
- Banos, O.; Moral-Munoz, J.A.; Diaz-Reyes, I.; Arroyo-Morales, M.; Damas, M.; Herrera-Viedma, E.; Hong, C.S.; Lee, S.; Pomares, H.; Rojas, I.; et al. MDurance: A novel mobile health system to support trunk endurance assessment. Sensors 2015, 15, 13159–13183. [Google Scholar] [CrossRef] [PubMed]
- Senior Fitness Test 2.0. Available online: https://sft.humankinetics.com/login?ReturnUrl=%2f (accessed on 24 August 2018).
- Android Developers, G. Save Data Using SQLite. Available online: https://developer.android.com/training/data-storage/sqlite.html (accessed on 24 August 2018).
- Jay, P. MP Android Chart. Available online: https://github.com/PhilJay/MPAndroidChart (accessed on 24 August 2018).
- Android Developers, G. Motion Sensors. Available online: https://developer.android.com/guide/topics/sensors/sensors_motion.html (accessed on 24 August 2018).
- Android Sensors Overview. Available online: https://developer.android.com/guide/topics/sensors/sensors_overview (accessed on 4 February 2020).
- White, P.J.; Podaima, B.W.; Friesen, M.R. Algorithms for smartphone and tablet image analysis for healthcare applications. IEEE Access 2014, 2, 831–840. [Google Scholar] [CrossRef]
- Palacín-Marín, F.; Esteban-Moreno, B.; Olea, N.; Herrera-Viedma, E.; Arroyo-Morales, M. Agreement between telerehabilitation and face-to-face clinical outcome assessments for low back pain in primary care. Spine 2013, 38, 947–952. [Google Scholar] [CrossRef]
- Moral-Muñoz, J.A.; Esteban-Moreno, B.; Arroyo-Morales, M.; Cobo, M.J.; Herrera-Viedma, E. Agreement Between Face-to-Face and Free Software Video Analysis for Assessing Hamstring Flexibility in Adolescents. J. Strength Cond. Res. 2015, 29, 2661–2665. [Google Scholar] [CrossRef]
- Gliem, J.A.; Gliem, R.R. Calculating, interpreting, and reporting Cronbach’s alpha reliability coefficient for Likert-type scales. In Proceedings of the Midwest Research-to-Practice Conference in Adult, Continuing, and Community Education, DeKalb, IL, USA, 23–28 September 2003. [Google Scholar]
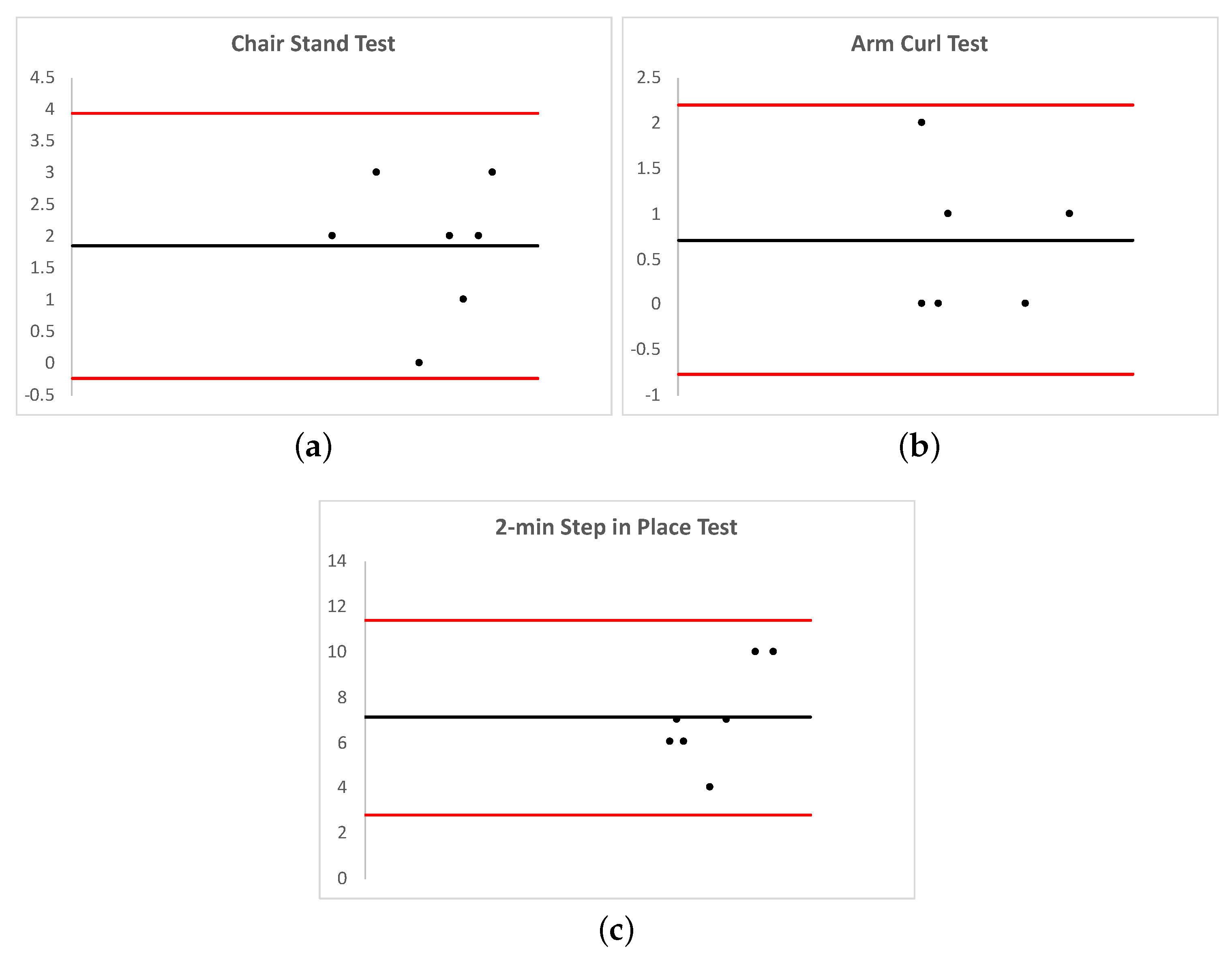
- Myles, P.S.; Cui, J. Using the Bland—Altman method to measure agreement with repeated measures. Br. J. Anaesth. 2007, 99, 309–311. [Google Scholar] [CrossRef]
- Brooke, J. SUS-A quick and dirty usability scale. Usability Eval. Ind. 1996, 189, 4–7. [Google Scholar]
- Lewis, J.R.; Sauro, J. The factor structure of the system usability scale. In Human Centered Design; Springer: Berlin/Heidelberg, Germany, 2009; pp. 94–103. [Google Scholar]
- Bangor, A.; Kortum, P.T.; Miller, J.T. An empirical evaluation of the system usability scale. Intl. J. Hum. Interact. 2008, 24, 574–594. [Google Scholar] [CrossRef]
- Milanese, S.; Gordon, S.; Buettner, P.; Flavell, C.; Ruston, S.; Coe, D.; O’Sullivan, W.; McCormack, S. Reliability and concurrent validity of knee angle measurement: Smart phone app versus universal goniometer used by experienced and novice clinicians. Man. Ther. 2014, 19, 569–574. [Google Scholar] [CrossRef] [PubMed]
- Vohralik, S.L.; Bowen, A.R.; Burns, J.; Hiller, C.E.; Nightingale, E.J. Reliability and validity of a smartphone app to measure joint range. Am. J. Phys. Med. Rehabil. 2015, 94, 325–330. [Google Scholar] [CrossRef] [PubMed]
- Galán-Mercant, A.; Barón-López, F.J.; Labajos-Manzanares, M.T.; Cuesta-Vargas, A.I. Reliability and criterion-related validity with a smartphone used in timed-up-and-go test. Biomed. Eng. Online 2014, 13, 156. [Google Scholar] [CrossRef] [PubMed]
- Loh, K.P.; Ramsdale, E.; Culakova, E.; Mendler, J.H.; Liesveld, J.L.; O’Dwyer, K.M.; McHugh, C.; Gilles, M.; Lloyd, T.; Goodman, M.; et al. Novel mHealth app to deliver geriatric assessment-driven interventions for older adults with cancer: Pilot feasibility and usability study. JMIR Cancer 2018, 4, e10296. [Google Scholar] [CrossRef]
- Hsieh, K.L.; Fanning, J.T.; Rogers, W.A.; Wood, T.A.; Sosnoff, J.J. A fall risk mhealth app for older adults: Development and usability study. JMIR Aging 2018, 1, e11569. [Google Scholar] [CrossRef]

| Test | Measure | Description | 60–69 Years | 70–79 Year | 80–89 Years |
|---|---|---|---|---|---|
| Chair Stand Test (n) | Strength of lower limbs | The number of times that person is able to stand up and sit without using the arms during a lapse of time of 30 s | 14.0 (2.4) | 12.9 (3.0) | 11.9 (3.6) |
| Arm Curl Test (n) | Strength of upper limbs | The number of times that a person is able to fold the arm between 90 to 0 degrees holding a lift of 5 lb (2.27 kg) for women and 8 lb (3.63 kg) for men during a lapse of time of 30 s | 19.8 (4.1) | 18.2 (3.9) | 16.5 (4.1) |
| 2-min Step in Place Test (n) | Aerobic endurance | the number of times that starting in a stand up position, a person can raise the knees to a height halfway between the iliac crest and middle of the patella during the lapse of time of two minutes. | 100.4 (9.0) | 92.6 (16.0) | 83.5 (22.6) |
| Chair Sit and Reach Test (cm) | Flexibility of the lower body | This test item asses the distance that a person can reach the toe (minus score) or beyond the toe (plus score) with fingers. The starting position is seated on the edge of a chair, with a leg extended straight in front of the hip with heel on floor flexed at 90°. | −1 (14) | −1 (15) | −8 (15) |
| Back Scratch Test (cm) | Flexibility of the upper limbs | Distance between (or the overlap of) the middle fingers behind the back when trying to touch the middle fingers of both hands together behind the back (measure to the nearest 1/2 inch). | 3.0 (5.0) | −1 (8) | −5 (11) |
| 8-Feet (2.45 m) Up and Go Test (s) | Agility and dynamic balance | The lapse of time a person takes to stand up from a chair, walk 8 feet (2.45 m) to and around a cone, and return to the chair (perform twice and measure time to the nearest 1/10th of a second, recording fastest time). | 5.2 (0.6) | 6.1 (1.2) | 7.1 (2.0) |
| Patient ID | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 |
|---|---|---|---|---|---|---|---|---|
| Gender | Male | Female | Female | Male | Female | Female | Male | |
| Age | 54 | 53 | 60 | 61 | 59 | 57 | 61 | |
| Chair Stand Test (SFT) | 14 | 15 | 12 | 14 | 10 | 16 | 12 | |
| Chair Stand Test (m-SFT) | 12 | 13 | 12 | 13 | 8 | 13 | 9 | |
| Arm Curl Test (SFT) | 23 | 16 | 15 | 20 | 14 | 16 | 15 | |
| Arm Curl Test (m-SFT) | 22 | 15 | 15 | 20 | 14 | 15 | 13 | |
| 2-min Step in Place Test (SFT) | 75 | 80 | 93 | 97 | 72 | 74 | 85 | |
| 2-min Step in Place Test (m-SFT) | 69 | 76 | 83 | 87 | 66 | 67 | 78 | |
| Chair Sit and Reach Test (SFT) | −1 | 3 | 5 | −3 | 2.5 | 2 | −2 | |
| Chair Sit and Reach Test (m-SFT) | −1 | 3.5 | 5 | −2.5 | 3 | 2 | −2 | |
| Back Scratch Test (SFT) | −3.5 | 1 | 2 | −2.5 | 2.5 | −1 | −4 | |
| Back Scratch Test (m-SFT) | −3 | 1.5 | 2.5 | −2 | 2.5 | −1 | −3.5 | |
| 8-Foot Up and Go Test (SFT) | 5.3 | 6.2 | 3.5 | 4.1 | 6.1 | 3.3 | 6 | |
| 8-Foot Up and Go Test (m-SFT) | 5 | 6.4 | 3.6 | 4.5 | 5.4 | 3.5 | 6.2 |
| Variable | ICC () | CI 95% of ICC | Cronbach’s |
|---|---|---|---|
| Chair Stand Test | 0.93 | 0.58–0.99 | 0.93 |
| Arm Curl Test | 0.99 | 0.86–0.99 | 0.99 |
| 2-min Step in Place Test | 0.98 | 0.83–0.99 | 0.98 |
| Chair Sit and Reach Test | 0.99 | 0.98–0.99 | 0.99 |
| Back Scratch Test | 0.99 | 0.99–1 | 0.99 |
| 8-Foot Up and Go Test | 0.97 | 0.85–0.99 | 0.97 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Ureña, R.; Chiclana, F.; Gonzalez-Alvarez, A.; Herrera-Viedma, E.; Moral-Munoz, J.A. m-SFT: A Novel Mobile Health System to Assess the Elderly Physical Condition. Sensors 2020, 20, 1462. https://doi.org/10.3390/s20051462
Ureña R, Chiclana F, Gonzalez-Alvarez A, Herrera-Viedma E, Moral-Munoz JA. m-SFT: A Novel Mobile Health System to Assess the Elderly Physical Condition. Sensors. 2020; 20(5):1462. https://doi.org/10.3390/s20051462
Chicago/Turabian StyleUreña, Raquel, Francisco Chiclana, Alvaro Gonzalez-Alvarez, Enrique Herrera-Viedma, and Jose A. Moral-Munoz. 2020. "m-SFT: A Novel Mobile Health System to Assess the Elderly Physical Condition" Sensors 20, no. 5: 1462. https://doi.org/10.3390/s20051462
APA StyleUreña, R., Chiclana, F., Gonzalez-Alvarez, A., Herrera-Viedma, E., & Moral-Munoz, J. A. (2020). m-SFT: A Novel Mobile Health System to Assess the Elderly Physical Condition. Sensors, 20(5), 1462. https://doi.org/10.3390/s20051462








