Characteristics, Usability, and Users Experience of a System Combining Cognitive and Physical Therapy in a Virtual Environment: Positive Bike
Abstract
1. Introduction
1.1. The Problem of Frailty
1.2. The Potential of Virtual Reality to Counteract Frailty
2. Positive Bike
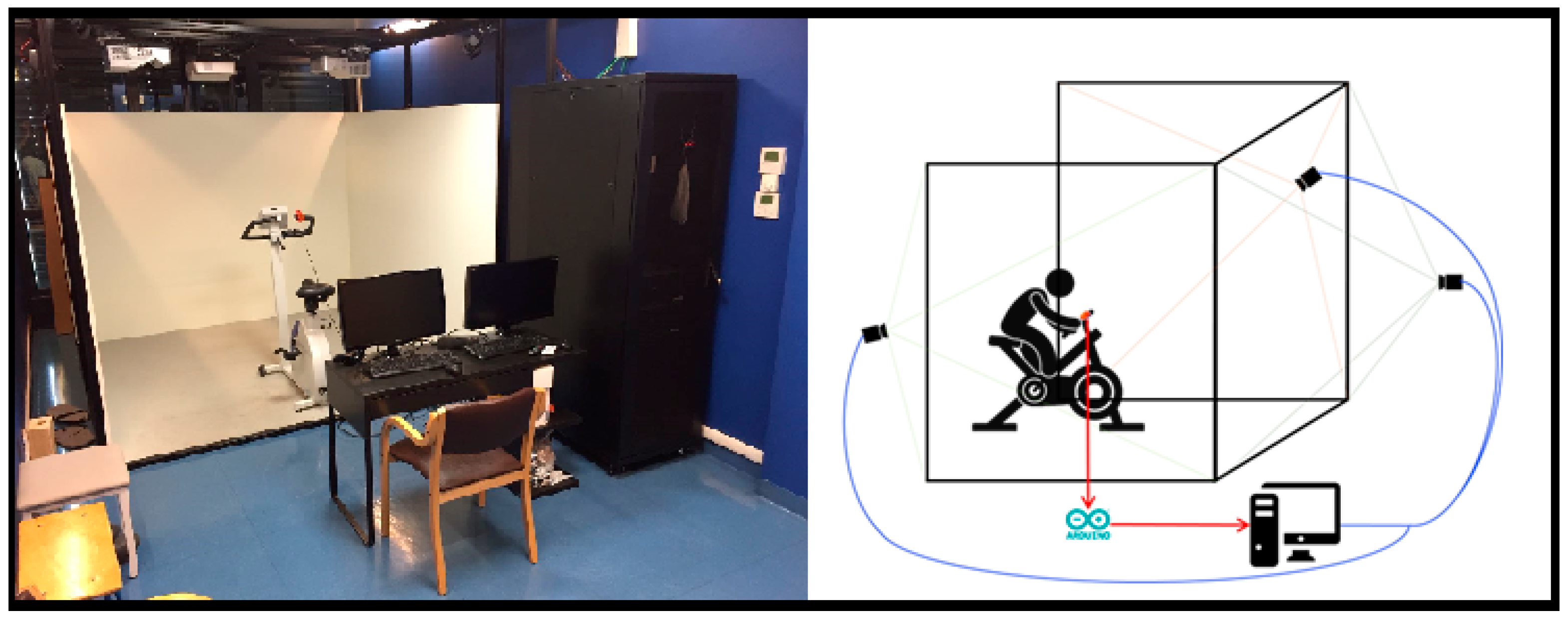
2.1. System Architecture
2.2. Virtual Environments
- Game type: the therapist can set the target typology—and thus define the exercise type—by choosing between animals or street furniture.
- Characteristic of the target to select: for animals, the first letter of the animals’ names (C/G/T/S); for street furniture, distinct colors are available (orange/blue /yellow/violet).
- Level: two levels of difficulty are available; in level 1, targets appear on the route each 15 s, in level 2, each 10 s.
- Cycle-ergometer workload: the operator can set the bike workload selecting among 20/30/40/50 Watt, depending on the patient’s physical condition.
- Time: the duration of the exercise, the therapist can select 15 or 20 min.
3. Usability Study
- Effectiveness: the possibility for the users to achieve goals;
- Efficiency: the effort made by the user to reach the goal;
- Satisfaction: what users think about the interaction with the system.
- -
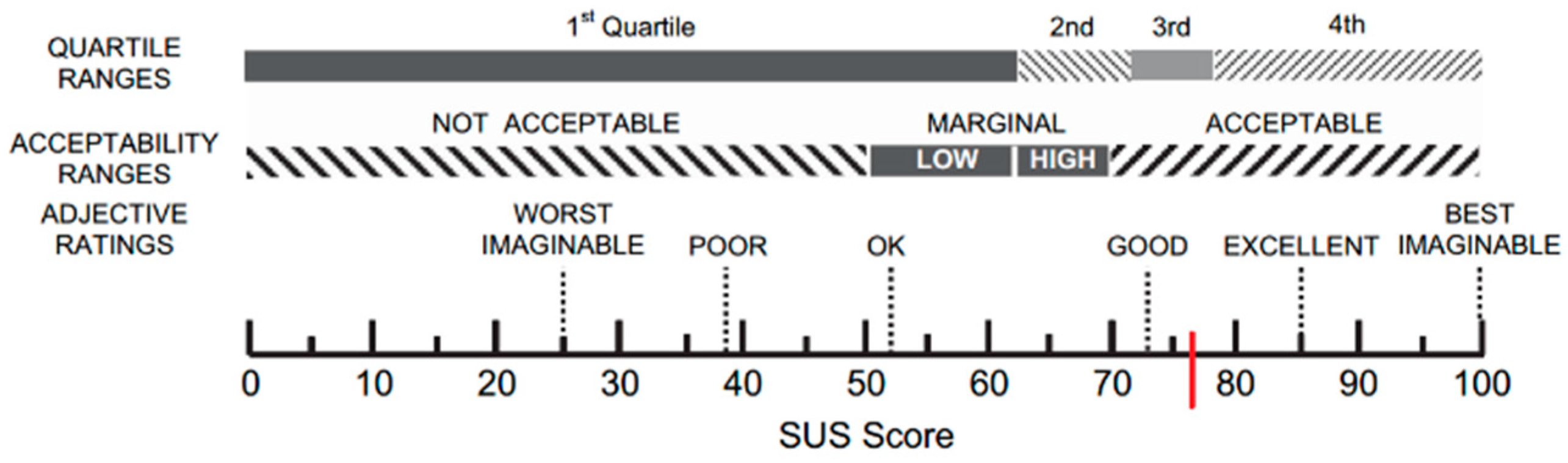
- SUS is a “quick and easy to use” questionnaire composed by ten items and created by Brooke in the 1996 [65]. The final score can range from 0, lack of usability, to 100, best usability (for an interpretation of SUS scores, see [67]). This is a standard scale for the assessment of usability of technological systems and it is easy to use and to understand for the patients.
- -
- The short flow state scale [66] assesses nine key flow dimensions: (1) challenge–skill balance: “I feel I am competent enough to meet the high demands of the situation”; (2) action–awareness merging: “I do things spontaneously and automatically without having to think”; (3) clear goals: “I have a strong sense of what I want to do”; (4) unambiguous feedback: “I have a good idea while I am performing about how well I am doing”; (5) concentration on the task at hand: “I am completely focused on the task at hand”; (6) sense of control: “I have a feeling of total control over what I am doing”; (7) transformation of time: “The way time passes seems to be different from normal”; (8) loss of self-consciousness: “I was not worried about what others may have been thinking of me”; (9) and autotelic experience: “The experience is extremely rewarding”. These characteristics were constructed using the conceptual flow model [68,69]. Subjects have to rate the flow experience on a five-point Likert scale ranging from 1 (strongly disagree) to 5 (strongly agree).
- Usability:
- ○
- Utilization (effectiveness),
- ○
- Learning (efficiency),
- ○
- Pleasantness (satisfaction).
- Sense of presence:
- ○
- Spatial presence,
- ○
- Engagement,
- ○
- Realism.
3.1. Sample
3.2. Task
4. Results
5. Discussion
6. Conclusions and Future Works
Author Contributions
Funding
Conflicts of Interest
References
- Woollacott, M.; Shumway-Cook, A. Attention and the control of posture and gait: A review of an emerging area of research. Gait Posture 2002, 16, 1–14. [Google Scholar] [CrossRef]
- Fried, L.P.; Tangen, C.M.; Walston, J.; Newman, A.B.; Hirsch, C.; Gottdiener, J.; Seeman, T.; Tracy, R.; Burke, G.; McBurnie, M.A.; et al. Frailty in older adults: Evidence for a phenotype. J. Gerontol. A Biol. 2001, 56, M146–M156. [Google Scholar] [CrossRef]
- Gobbens, R.J.; Luijkx, K.G.; Wijnen-Sponselee, M.T.; Schols, J.M. Toward a conceptual definition of frail community dwelling older people. Nurs. Outlook 2010, 58, 76–86. [Google Scholar] [CrossRef]
- Speechley, M.; Tinetti, M. Falls and injuries in frail and vigorous community elderly persons. J. Am. Geriatr. Soc. 1991, 39, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Fried, L.P.; Ferrucci, L.; Darer, J.; Williamson, J.D.; Anderson, G. Untangling the concepts of disability, frailty, and comorbidity: Implications for improved targeting and care. J. Gerontol. A Biol. 2004, 59, 255–263. [Google Scholar] [CrossRef]
- Rockwood, K. What would make a definition of frailty successful? Age Ageing 2005, 34, 432–434. [Google Scholar] [CrossRef]
- Blake, A.J.; Morgan, K.; Bendall, M.J.; Dallosso, H.; Ebrahim, S.B.J.; Arie, T.H.D.; Fentem, P.H.; Bassey, E.J. Falls by elderly people at home: Prevalence and associated factors. Age Ageing 1988, 17, 365–372. [Google Scholar] [CrossRef] [PubMed]
- Donald, I.P.; Bulpitt, C.J. The prognosis of falls in elderly people living at home. Age Ageing 1999, 28, 121–125. [Google Scholar] [CrossRef] [PubMed]
- Zijlstra, G.A.; Van Haastregt, J.C.M.; Van Eijk, J.T.M.; van Rossum, E.; Stalenhoef, P.A.; Kempen, G.I. Prevalence and correlates of fear of falling, and associated avoidance of activity in the general population of community-living older people. Age Ageing 2007, 36, 304–309. [Google Scholar] [CrossRef] [PubMed]
- Lundin-Olsson, L.; Nyberg, L.; Gustafson, Y. “Stops walking when talking” as a predictor of falls in elderly people. Lancet 1997, 349, 617. [Google Scholar] [CrossRef]
- Montero-Odasso, M.; Verghese, J.; Beauchet, O.; Hausdorff, J.M. Gait and cognition: A complementary approach to understanding brain function and the risk of falling. J. Am. Geriatr. Soc. 2012, 60, 2127–2136. [Google Scholar] [CrossRef] [PubMed]
- Yogev-Seligmann, G.; Hausdorff, J.M.; Giladi, N. The role of executive function and attention in gait. Mov. Disord. 2008, 23, 329–342. [Google Scholar] [CrossRef]
- Plummer, P.; Eskes, G.; Wallace, S.; Giuffrida, C.; Fraas, M.; Campbell, G.; Clifton, G.; Skidmore, E.R.; American Congress of Rehabilitation Medicine Stroke Networking Group Cognition Task Force. Cognitive-motor interference during functional mobility after stroke: State of the science and implications for future research. Arch. Phys. Med. Rehabil. 2013, 94, 2565–2574. [Google Scholar] [CrossRef] [PubMed]
- Leone, C.; Feys, P.; Moumdjian, L.; D’Amico, E.; Zappia, M.; Patti, F. Cognitive-motor dual-task interference: A systematic review of neural correlates. Neurosci. Biobehav. Rev. 2017, 75, 348–360. [Google Scholar] [CrossRef]
- Wickens, C.D. The structure of attentional resources. Atten. Perform. 1980, 8, 239–257. [Google Scholar]
- Pashler, H. Dual-task interference in simple tasks: Data and theory. Pol. Psychol. Bull. 1994, 116, 220–244. [Google Scholar] [CrossRef]
- Al-Yahya, E.; Dawes, H.; Smith, L.; Dennis, A.; Howells, K.; Cockburn, J. Cognitive motor interference while walking: A systematic review and meta-analysis. Neurosci. Biobehav. Rev. 2011, 35, 715–728. [Google Scholar] [CrossRef]
- Ranky, R.; Sivak, M.; Lewis, J.; Gade, V.; Deutsch, J.E.; Mavroidis, C. VRACK—Virtual reality augmented cycling kit: Design and validation. In Proceedings of the IEEE Virtual Reality Conference (VR), Waltham, MA, USA, 20–24 March 2010. [Google Scholar]
- Killane, I.; Fearon, C.; Newman, L.; McDonnell, C.; Waechter, S.M.; Sons, K.; Lynch, T.; Reilly, R.B. Dual motor-cognitive virtual reality training impacts dual-task performance in freezing of gait. IEEE J. Biomed. Health 2015, 19, 1855–1861. [Google Scholar] [CrossRef]
- Dunsky, A.; Fishbein, P.; Hutzler, Y. Dual-task training using virtual reality: Influence on walking and balance in three post stroke survivors. Int. J. Ther. Rehabil. Res. 2013, 2, 22–34. [Google Scholar] [CrossRef]
- Wang, X.; Pi, Y.; Chen, P.; Liu, Y.; Wang, R.; Chan, C. Cognitive motor interference for preventing falls in older adults: A systematic review and meta-analysis of randomised controlled trials. Age Ageing 2015, 44, 205–212. [Google Scholar] [CrossRef] [PubMed]
- Hsu, C.L.; Nagamatsu, L.S.; Davis, J.C.; Liu-Ambrose, T. Examining the relationship between specific cognitive processes and falls risk in older adults: A systematic review. Osteoporos. Int. 2012, 23, 2409–2424. [Google Scholar] [CrossRef] [PubMed]
- Gill, T.M.; Gahbauer, E.A.; Allore, H.G.; Han, L. Transitions between frailty states among community-living older persons. Arch. Intern. Med. 2006, 166, 418–423. [Google Scholar] [CrossRef]
- De Labra, C.; Guimaraes-Pinheiro, C.; Maseda, A.; Lorenzo, T.; Millán-Calenti, J.C. Effects of physical exercise interventions in frail older adults: A systematic review of randomized controlled trials. BMC Geriatr. 2015, 15, 154. [Google Scholar] [CrossRef] [PubMed]
- Aguirre, L.E.; Villareal, D.T. Physical Exercise as Therapy for Frailty. Nestle Nutr. Inst. Workshop Ser. 2015, 83, 83–92. [Google Scholar] [CrossRef] [PubMed]
- Cadore, E.L.; Casas-Herrero, A.; Zambom-Ferraresi, F.; Idoate, F.; Millor, N.; Gómez, M.; Rodriguez-Mañas, L.; Izquierdo, M. Multicomponent exercises including muscle power training enhance muscle mass, power output, and functional outcomes in institutionalized frail nonagenarians. Age 2014, 36, 773–785. [Google Scholar] [CrossRef] [PubMed]
- Inokuchi, S.; Matsusaka, N.; Hayashi, T.; Shindo, H. Feasibility and effectiveness of a nurse-led community exercise programme for prevention of falls among frail elderly people: A multi-centre controlled trial. J. Rehabil. Med. 2007, 39, 479–485. [Google Scholar] [CrossRef] [PubMed]
- Gillespie, L.D.; Robertson, M.C.; Gillespie, W.J.; Lamb, S.E.; Gates, S.; Cumming, R.G.; Rowe, B.H. Interventions for preventing falls in older people living in the community. Cochrane Database Syst. Rev. 2009, 2. [Google Scholar] [CrossRef]
- Sherrington, C.; Whitney, J.C.; Lord, S.R.; Herbert, R.D.; Cumming, R.G.; Close, J.C. Effective exercise for the prevention of falls: A systematic review and meta-analysis. J. Am. Geriatr. Soc. 2008, 56, 2234–2243. [Google Scholar] [CrossRef] [PubMed]
- Kramer, A.F.; Colcombe, S.J.; McAuley, E.; Scalf, P.E.; Erickson, K.I. Fitness, aging and neurocognitive function. Neurobiol. Aging 2005, 26, 124–127. [Google Scholar] [CrossRef] [PubMed]
- Silsupadol, P.; Shumway-Cook, A.; Lugade, V.; van Donkelaar, P.; Chou, L.S.; Mayr, U.; Woollacott, M.H. Effects of single-task versus dual-task training on balance performance in older adults: A double-blind, randomized controlled trial. Arch. Phys. Med. Rehabil. 2009, 90, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Lauenroth, A.; Ioannidis, A.E.; Teichmann, B. Influence of combined physical and cognitive training on cognition: A systematic review. BMC Geriatr. 2016, 16, 141. [Google Scholar] [CrossRef] [PubMed]
- Schoene, D.; Valenzuela, T.; Lord, S.R.; de Bruin, E.D. The effect of interactive cognitive-motor training in reducing fall risk in older people: A systematic review. BMC Geriatr. 2014, 14, 107. [Google Scholar] [CrossRef] [PubMed]
- Wajda, D.A.; Mirelman, A.; Hausdorff, J.M.; Sosnoff, J.J. Intervention modalities for targeting cognitive-motor interference in individuals with neurodegenerative disease: A systematic review. Expert Rev. Neurother. 2017, 17, 251–261. [Google Scholar] [CrossRef] [PubMed]
- Donath, L.; Rossler, R.; Faude, O. Effects of Virtual Reality Training (Exergaming) Compared to Alternative Exercise Training and Passive Control on Standing Balance and Functional Mobility in Healthy Community-Dwelling Seniors: A Meta-Analytical Review. Sports Med. 2016, 46, 1293–1309. [Google Scholar] [CrossRef] [PubMed]
- Neri, S.G.; Cardoso, J.R.; Cruz, L.; Lima, R.M.; de Oliveira, R.J.; Iversen, M.D.; Carregaro, R.L. Do virtual reality games improve mobility skills and balance measurements in community-dwelling older adults? Systematic review and meta-analysis. Clin. Rehabil. 2017, 31, 1292–1304. [Google Scholar] [CrossRef] [PubMed]
- Rendon, A.A.; Lohman, E.B.; Thorpe, D.; Johnson, E.G.; Medina, E.; Bradley, B. The effect of virtual reality gaming on dynamic balance in older adults. Age Ageing 2012, 41, 549–552. [Google Scholar] [CrossRef]
- Franco, J.R.; Jacobs, K.; Inzerillo, C.; Kluzik, J. The effect of the Nintendo Wii Fit and exercise in improving balance and quality of life in community dwelling elders. Technol. Health Care 2012, 20, 95–115. [Google Scholar] [CrossRef] [PubMed]
- Bieryla, K.A.; Dold, N.M. Feasibility of Wii Fit training to improve clinical measures of balance in older adults. Clin. Interv. Aging 2013, 8, 775. [Google Scholar] [CrossRef] [PubMed]
- Gschwind, Y.J.; Schoene, D.; Lord, S.R.; Ejupi, A.; Valenzuela, T.; Aal, K.; Woodbury, A.; Delbaere, K. The effect of sensor-based exercise at home on functional performance associated with fall risk in older people—A comparison of two exergame interventions. Eur. Rev. Aging Phys. Act. 2015, 12, 11. [Google Scholar] [CrossRef] [PubMed]
- Schoene, D.; Lord, S.R.; Delbaere, K.; Severino, C.; Davies, T.A.; Smith, S.T. A randomized controlled pilot study of home-based step training in older people using videogame technology. PLoS ONE 2013, 8, e57734. [Google Scholar] [CrossRef]
- Mirelman, A.; Rochester, L.; Maidan, I.; Del Din, S.; Alcock, L.; Nieuwhof, F.; Rikkert, M.O.; Bloem, B.R.; Pelosin, E.; Avanzino, L.; et al. Addition of a non-immersive virtual reality component to treadmill training to reduce fall risk in older adults (V-TIME): A randomised controlled trial. Lancet 2016, 388, 1170–1182. [Google Scholar] [CrossRef]
- Yin, C.; Hsueh, Y.H.; Yeh, C.Y.; Lo, H.C.; Lan, Y.T. A Virtual Reality-Cycling Training System for Lower Limb Balance Improvement. Biomed. Res. Int. 2016, 2016, 9276508. [Google Scholar] [CrossRef] [PubMed]
- Anderson-Hanley, C.; Arciero, P.J.; Brickman, A.M.; Nimon, J.P.; Okuma, N.; Westen, S.C.; Merz, M.E.; Pence, B.D.; Woods, J.A.; Kramer, A.F.; et al. Exergaming and older adult cognition: A cluster randomized clinical tria. Am. J. Prev. Med. 2012, 42, 109–119. [Google Scholar] [CrossRef] [PubMed]
- Deutsch, J.E.; Myslinski, M.J.; Kafri, M.; Ranky, R.; Sivak, M.; Mavroidis, C.; Lewis, J.A. Feasibility of virtual reality augmented cycling for health promotion of people poststroke. J. Neurol. Phys. Ther. 2013, 37, 118–124. [Google Scholar] [CrossRef] [PubMed]
- Kim, N.G.; Kim, Y.Y.; Kwon, T.K. Development of a virtual reality bicycle simulator for rehabilitation training of postural balance. In Computational Science and Its Applications—ICCSA 2006; Gavrilova, M., Gervasi, O., Kumar, V., Tan, C.J.K., Taniar, D., Laganá, A., Mun, Y., Choo, H., Eds.; Springer: Berlin/Heidelberg, Germany, 2006; Volume 3980, pp. 241–250. ISBN 978-3-540-34070-6. [Google Scholar]
- Song, C.G.; Kim, J.Y.; Kim, N.G. A new postural balance control system for rehabilitation training based on virtual cycling. IEEE Trans. Inf. Technol. Biomed. 2004, 8, 200–207. [Google Scholar] [CrossRef] [PubMed]
- Kizony, R.; Levin, M.F.; Hughey, L.; Perez, C.; Fung, J. Cognitive load and dual-task performance during locomotion poststroke: A feasibility study using a functional virtual environment. Phys. Ther. 2010, 90, 252–260. [Google Scholar] [CrossRef] [PubMed]
- Dorfman, M.; Herman, T.; Brozgol, M.; Shema, S.; Weiss, A.; Hausdorff, J.M.; Mirelman, A. Dual-task training on a treadmill to improve gait and cognitive function in elderly idiopathic fallers. J. Neurol. Phys. Ther. 2014, 38, 246–253. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.W.; Cho, G.H. Effect of stationary cycle exercise on gait and balance of elderly women. J. Phys. Ther. Sci. 2014, 26, 431–433. [Google Scholar] [CrossRef] [PubMed]
- Brown, D.A.; Kautz, S.A. Increased workload enhances force output during pedaling exercise in persons with poststroke hemiplegia. Stroke 1998, 29, 598–606. [Google Scholar] [CrossRef] [PubMed]
- Raasch, C.C.; Zajac, F.E. Locomotor strategy for pedaling: Muscle groups and biomechanical functions. J. Neurophysiol. 1999, 82, 515–525. [Google Scholar] [CrossRef] [PubMed]
- Mazzocchio, R.; Meunier, S.; Ferrante, S.; Molteni, F. Cycling, a tool for locomotor recovery after motor lesions? NeuroRehabilitation 2008, 23, 67–80. [Google Scholar] [PubMed]
- Fujiwara, T.; Liu, M.; Tanuma, A.; Hase, K.; Tsuji, T. Pedaling exercise for neuromuscular re-education: A review. Crit. Rev. Phys. Rehabil. Med. 2005, 17, 163–178. [Google Scholar] [CrossRef]
- Astrand, P. Measurement of maximal aerobic capacity. Can. Med. Assoc. J. 1967, 96, 732. [Google Scholar] [PubMed]
- Riva, G.; Mantovani, F.; Gaggioli, A. Presence and rehabilitation: Toward second-generation virtual reality applications in neuropsychology. J. Neuroeng. Rehabil. 2004, 1, 9. [Google Scholar] [CrossRef] [PubMed]
- Riva, G.; Castelnuovo, G.; Mantovani, F. Transformation of flow in rehabilitation: The role of advanced communication technologies. Behav. Res. Methods 2006, 38, 237–244. [Google Scholar] [CrossRef] [PubMed]
- Robinson, J.; Dixon, J.; Macsween, A.; van Schaik, P.; Martin, D. The effects of exergaming on balance, gait, technology acceptance and flow experience in people with multiple sclerosis: A randomized controlled trial. BMC Sports Sci. Med. Rehabil. 2015, 7, 8. [Google Scholar] [CrossRef] [PubMed]
- Pedroli, E.; Serino, S.; Cipresso, P.; Pallavicini, F.; Riva, G. Assessment and rehabilitation of neglect using virtual reality: A systematic review. Front. Behav. Neurosci. 2015, 9, 226. [Google Scholar] [CrossRef] [PubMed]
- Nichols, S.; Patel, H. Health and safety implications of virtual reality: A review of empirical evidence. Appl. Ergon. 2002, 33, 251–271. [Google Scholar] [CrossRef]
- Blattner, M.M.; Sumikawa, D.A.; Greenberg, R.M. Earcons and icons: Their structure and common design principles. Int. J. Hum. Comput. Int. 1989, 4, 11–44. [Google Scholar] [CrossRef]
- Rosati, G.; Rodà, A.; Avanzini, F.; Masiero, S. On the role of auditory feedback in robot-assisted movement training after stroke: Review of the literature. Comput. Intell. Neurosci. 2013, 2013, 11. [Google Scholar] [CrossRef] [PubMed]
- Bruun-Pedersen, J.R.; Serafin, S.; Kofoed, L.B. Augmented Exercise Biking with Virtual Environments for Elderly Users: Considerations on the use of auditory feedback. In Proceedings of the 40th International Computer Music Conference, ICMC 2014 and 11th Sound and Music Computing Conference, SMC 2014: Music Technology Meets Philosophy: From Digital Echos to Virtual Ethos, Athens, Greece, 14–20 September 2014; pp. 1665–1668. [Google Scholar]
- ISO 9241-11:1998. Ergonomic Requirements for Office Work with Visual Display Terminals (VDTs); ISO: Geneva, Switzerland, 1998. [Google Scholar]
- Brooke, J. SUS—A quick and dirty usability scale. Usability Eval. Ind. 1996, 189, 4–7. [Google Scholar]
- Jackson, S.A.; Marsh, H.W. Development and validation of a scale to measure optimal experience: The Flow State Scale. J. Sport Exerc. Psychol. 1996, 18, 17–35. [Google Scholar] [CrossRef]
- Bangor, A.; Kortum, P.; Miller, J. Determining what individual SUS scores mean: Adding an adjective rating scale. J. Usability Stud. 2009, 4, 114–123. [Google Scholar]
- Jackson, S.A.; Martin, A.J.; Eklund, R.C. Long and short measures of flow: The construct validity of the FSS-2, DFS-2, and new brief counterparts. J. Sport Exerc. Psychol. 2008, 30, 561–587. [Google Scholar] [CrossRef] [PubMed]
- Csikszentmihalyi, M. Flow: The Psychology of Optimal Experience, 1st ed.; Harper Perennial Modern Classics: New York, NY, USA, 2008; ISBN 978-0061339202. [Google Scholar]
- Holland, A.E.; Hill, C.J.; Rochford, P.; Fiore, J.; Berlowitz, D.J.; McDonald, C.F. Telerehabilitation for people with chronic obstructive pulmonary disease: Feasibility of a simple, real time model of supervised exercise training. J. Telemed. Telecare 2013, 19, 222–226. [Google Scholar] [CrossRef] [PubMed]
- Waters, R.C.; Anderson, D.B.; Barrus, J.W.; Brogan, D.C.; Casey, M.A.; McKeown, S.G.; Nitta, T.; Sterns, I.B.; Yerazunis, W.S. Diamond Park and Spline: A Social Virtual Reality System with 3D Animation, Spoken Interaction, and Runtime Modifiability. Technical Report TR96-02a, 1997 MERL—A Mitsubishi Electronic Research Laboratory. Available online: http://www.merl.com/reports/TR96-02a/index.html (accessed on 18 June 2018).
- Marston, H.R.; Kroll, M.; Fink, D.; Gschwind, Y.J. Flow experience of older adults using the iStoppFalls exergame. Games Cult. 2016, 11, 201–222. [Google Scholar] [CrossRef]
- Galna, B.; Jackson, D.; Schofield, G.; McNaney, R.; Webster, M.; Barry, G.; Mhiripiri, D.; Balaam, M.; Olivier, P.; Rochester, L. Retraining function in people with Parkinson’s disease using the Microsoft kinect: Game design and pilot testing. J. Neuroeng. Rehabil. 2014, 11, 60. [Google Scholar] [CrossRef] [PubMed]
- Gaggioli, A.; Greci, L.; Arlati, S.; Stramba-Badiale, M.; Pedroli, E.; Colombo, D.; Serino, S.; Cipresso, P.; Riva, G. “Positive Bike”—An Immersive Biking Experience for Combined Physical and Cognitive Training of Elderly Patients. Annu. Rev. Cyberther. Telemed. 2017, 15, 196–199. [Google Scholar]
- Zimmerli, L.; Jacky, M.; Lünenburger, L.; Riener, R.; Bolliger, M. Increasing patient engagement during virtual reality-based motor rehabilitation. Arch. Phys. Med. Rehabil. 2013, 94, 1737–1746. [Google Scholar] [CrossRef] [PubMed]

| Topic | Sub-Topic | Questions |
|---|---|---|
| Usability | Utilization | What difficulties did you encounter in carrying out the task? Was it difficult to use the instrument? There were technical issues during the session? |
| Learning | Did you have to ask for help to understand how to use the system? Did it take a long time to figure out how the instrument works? Was exercise complicated? | |
| Pleasantness | Did you like the virtual environment? Some parts of the system were uncomfortable? Did you have any trouble riding a stationary bike with 3D glasses? | |
| Sense of Presence | Spatial presence | Did you feel part of the environment? Do you feel you have control over the environment? |
| Engagement | Were you happy that the exercise was over? What do you think about the duration of the experience? Did you easily get distracted during exercise? | |
| Realism | How did you find the environment, realistic or too artificial? | |
| Cyber Sickness | Physical side-effects | Did you feel bad during exercise? Did you have nausea, dizziness or other physical symptoms during exercise? |
| Expectations | Would you like to use this system to do exercise? Do you think this system can be useful for other types of patients? |
| Age | y.o.e. | Gender | MMSE | |
|---|---|---|---|---|
| Subject 1 | 87 | 5 | M | 27 |
| Subject 2 | 65 | 16 | F | 25.2 |
| Subject 3 | 77 | 5 | M | 20.9 |
| Subject 4 | 59 | 16 | F | 25.2 |
| Subject 5 | 62 | 13 | F | 30 |
| Mean | 70.00 | 11.70 | 25.66 | |
| SD | 11.70 | 5.61 | 3.31 |
| Dimension | Mean | SD | |
|---|---|---|---|
| Q1 | Challenge-skill | 4.6 | 0.49 |
| Q2 | Action-awareness | 4 | 1.26 |
| Q3 | Clear goals | 4.4 | 0.80 |
| Q4 | Unambiguous feedback | 4.2 | 0.98 |
| Q5 | Concentration | 4.4 | 0.80 |
| Q6 | Sense of control | 4.4 | 0.80 |
| Q7 | Loss of self-consciousness | 5 | 0.00 |
| Q8 | Transformation of time | 3.8 | 1.60 |
| Q9 | Autotelic experience | 4.2 | 1.60 |
| Q10 | Total | 4.33 | 0.75 |
| Value | Std. Err. | ||
|---|---|---|---|
| Measure of agreement | Kappa | 0.850 | 0.102 |
| No. of valid cases | 27 | ||
| Topic | Sub-Topic | Positive Feedback |
|---|---|---|
| Usability | Utilization | “Both the motor and cognitive tasks were easy.” |
| Learning | “There was no problem in learning the use of the system.” | |
| Pleasantness | “The 3D glass was not uncomfortable.” “The environment was beautiful.” “The cycle-ergometer was manageable.” | |
| Sense of Presence | Spatial Presence | “The feeling was to be in the real park.” “I had the feeling of being suspended.” “The environment was relaxing.” |
| Engagement | “I was focused on the task.” “I think I’ve been pedaling for 5 min.” “I forget you (the examiners) were here too.” | |
| Realism | “The environment was realistic.” | |
| Cyber Sickness | Physical side-effects | None present side effect like cyber-sickness or nausea |
| Expectations | “This system could be useful for several types of patients.” “I think it’s easier to train with this tool.” |
| Topic | Sub-Topic | Negative Feedback |
|---|---|---|
| Usability | Utilization | “It’s difficult to recognize small animals.” “It’s not easy to identify animals placed backward.” “Some similar animals were confused (zebra–horse and turkey–swan).” |
| Learning | The sound of the bike might be confused with the sound that give a feedback about speed. “When frequency increases the exercise becomes more difficult.” | |
| Pleasantness | “Animals are repetitive.” | |
| Sense of Presence | Spatial Presence | “I had the feeling that animals bumped me.” |
| Engagement | “I felt passive and not active in the environment.” | |
| Realism | “The environment was nice but did not look very real.” “Some animals are ‘out of context’.” | |
| Cyber Sickness | Physical side-effects | One patient was tired before the end of the task. |
| Expectations | There is no difference between this type of treatment and another. |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pedroli, E.; Greci, L.; Colombo, D.; Serino, S.; Cipresso, P.; Arlati, S.; Mondellini, M.; Boilini, L.; Giussani, V.; Goulene, K.; et al. Characteristics, Usability, and Users Experience of a System Combining Cognitive and Physical Therapy in a Virtual Environment: Positive Bike. Sensors 2018, 18, 2343. https://doi.org/10.3390/s18072343
Pedroli E, Greci L, Colombo D, Serino S, Cipresso P, Arlati S, Mondellini M, Boilini L, Giussani V, Goulene K, et al. Characteristics, Usability, and Users Experience of a System Combining Cognitive and Physical Therapy in a Virtual Environment: Positive Bike. Sensors. 2018; 18(7):2343. https://doi.org/10.3390/s18072343
Chicago/Turabian StylePedroli, Elisa, Luca Greci, Desirèe Colombo, Silvia Serino, Pietro Cipresso, Sara Arlati, Marta Mondellini, Lorenzo Boilini, Valentina Giussani, Karine Goulene, and et al. 2018. "Characteristics, Usability, and Users Experience of a System Combining Cognitive and Physical Therapy in a Virtual Environment: Positive Bike" Sensors 18, no. 7: 2343. https://doi.org/10.3390/s18072343
APA StylePedroli, E., Greci, L., Colombo, D., Serino, S., Cipresso, P., Arlati, S., Mondellini, M., Boilini, L., Giussani, V., Goulene, K., Agostoni, M., Sacco, M., Stramba-Badiale, M., Riva, G., & Gaggioli, A. (2018). Characteristics, Usability, and Users Experience of a System Combining Cognitive and Physical Therapy in a Virtual Environment: Positive Bike. Sensors, 18(7), 2343. https://doi.org/10.3390/s18072343







