Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants
Abstract
1. Introduction
2. Results
2.1. Characteristics of Human Participants
2.2. Toluene Exposure
2.3. Toluene Exposure Can Negatively Affect the Nervous System by Inducing Epigenetic Changes
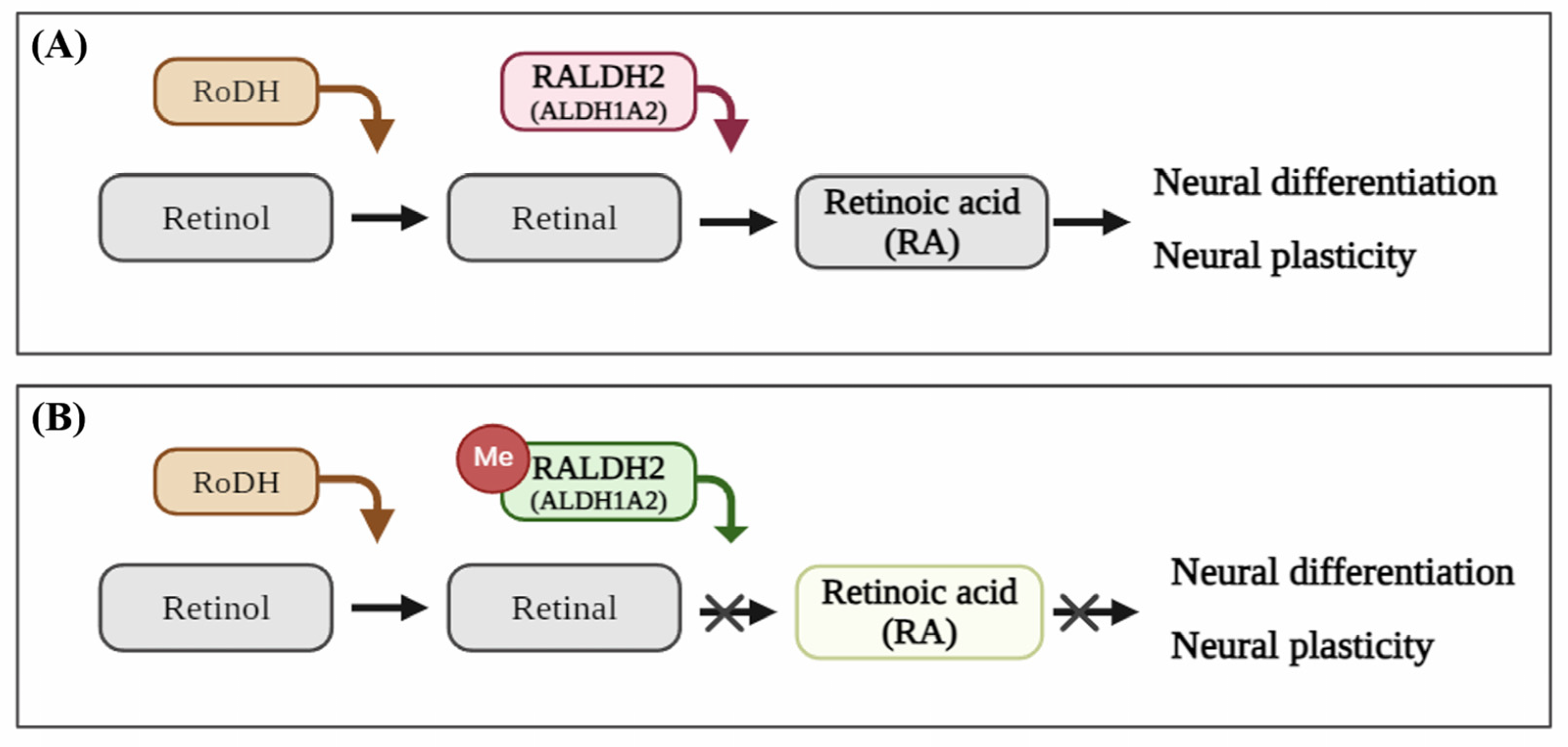
2.4. Toluene Exposure Leads to Hypermethylation-Induced ALDH1A2 Downregulation
2.5. Toluene Exposure Upregulates Genes Involved in Inflammatory Response
3. Discussion
4. Materials and Methods
4.1. Human Participants and Ethical Approval
4.2. Selection of Toluene-Exposed Groups
4.3. Methylated DNA Immunoprecipitation Sequencing (MeDIP) Sequencing and DMR Analysis
4.4. mRNA Sequencing and Differentially Expressed Gene (DEG) Analysis
4.5. Statistical and Functional Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lou, J.; Wu, Y.; Liu, P.; Kota, S.H.; Huang, L. Health effects of climate change through temperature and air pollution. Curr. Pollut. Rep. 2019, 5, 144–158. [Google Scholar] [CrossRef]
- Manisalidis, I.; Stavropoulou, E.; Stavropoulos, A.; Bezirtzoglou, E. Environmental and health impacts of air pollution: A review. Front. Public Health 2020, 8, 505570. [Google Scholar] [CrossRef] [PubMed]
- Vardoulakis, S.; Giagloglou, E.; Steinle, S.; Davis, A.; Sleeuwenhoek, A.; Galea, K.S.; Dixon, K.; Crawford, J.O. Indoor exposure to selected air pollutants in the home environment: A systematic review. Int. J. Environ. Res. Public Health 2020, 17, 8972. [Google Scholar] [CrossRef] [PubMed]
- Barberes, G.A.; Pena dos Reis, R.; Spigolon, A.L.; Fonseca, P.E.; Bandeira de Mello, C.; Barata, M.T. Groundwater natural contamination by toluene in Beja and Faro Districts, Portugal. Geosciences 2018, 8, 9. [Google Scholar] [CrossRef]
- Filley, C.M.; Halliday, W.; Kleinschmidt-DeMasters, B.K. The effects of toluene on the central nervous system. J. Neuropathol. Exp. Neurol. 2004, 63, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Pandey, P.; Yadav, R. A review on volatile organic compounds (VOCs) as environmental pollutants: Fate and distribution. Int. J. Plant Environ. 2018, 4, 14–26. [Google Scholar] [CrossRef]
- Cruz, S.L.; Rivera-García, M.T.; Woodward, J.J. Review of toluene action: Clinical evidence, animal studies and molecular targets. J. Drug Alcohol. Res. 2014, 3, 235840. [Google Scholar] [CrossRef] [PubMed]
- Laslo-Baker, D.; Barrera, M.; Knittel-Keren, D.; Kozer, E.; Wolpin, J.; Khattak, S.; Hackman, R.; Rovet, J.; Koren, G. Child neurodevelopmental outcome and maternal occupational exposure to solvents. Arch. Pediatr. Adolesc. Med. 2004, 158, 956–961. [Google Scholar] [CrossRef] [PubMed]
- Aydın, B.; Botan, E.; Gülensoy, B.; Akyol, S. Hydranencephaly in a newborn due to occupational toluene exposure during pregnancy: A case report. Acute Crit. Care 2022. [Google Scholar] [CrossRef]
- Rani, P.; Dhok, A. Effects of pollution on pregnancy and infants. Cureus 2023, 15, e33906. [Google Scholar] [CrossRef]
- Haugen, A.C.; Schug, T.T.; Collman, G.; Heindel, J.J. Evolution of DOHaD: The impact of environmental health sciences. J. Dev. Orig. Health Dis. 2015, 6, 55–64. [Google Scholar] [CrossRef] [PubMed]
- Volk, H.E.; Perera, F.; Braun, J.M.; Kingsley, S.L.; Gray, K.; Buckley, J.; Clougherty, J.E.; Croen, L.A.; Eskenazi, B.; Herting, M.; et al. Prenatal air pollution exposure and neurodevelopment: A review and blueprint for a harmonized approach within ECHO. Environ. Res. 2021, 196, 110320. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y.J.; Oh, E.; Shin, M.; Nam, D.H.; Jeon, S.Y.; Yu, J.H.; Song, J.Y.; Minn, D.; Lee, E. Premature ovarian insufficiency associated with environmental chemical exposure among Korean women: A study based on the Korean National Environmental Health Survey (2009–2012). Mol. Cell. Toxicol. 2023, 1–7. [Google Scholar] [CrossRef]
- Lee, J.; Weerasinghe-Mudiyanselage, P.D.; Kim, B.; Kang, S.; Kim, J.S.; Moon, C. Impact of diesel particulate matter on the olfactory bulb of mice: Insights from behavioral, histological, and molecular assessments. Mol. Cell. Toxicol. 2023, 1–11. [Google Scholar] [CrossRef]
- Kang, S.; Lee, H.J.; Son, Y.; Bae, M.J.; Jo, W.S.; Park, J.H.; Jeong, S.; Moon, C.; Shin, I.S.; Lee, C.G.; et al. Low-dose-rate gamma radiation aggravates titanium dioxide nanoparticle-induced lung injury in mice. Mol. Cell. Toxicol. 2024, 20, 389–398. [Google Scholar] [CrossRef]
- Johnson, C.H.; Athersuch, T.J.; Collman, G.W.; Dhungana, S.; Grant, D.F.; Jones, D.P.; Patel, C.J.; Vasiliou, V. Yale school of public health symposium on lifetime exposures and human health: The exposome; summary and future reflections. Hum. Genomics 2017, 11, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Koh, E.J.; Hwang, S.Y. Multi-omics approaches for understanding environmental exposure and human health. Mol. Cell. Toxicol. 2019, 15, 1–7. [Google Scholar] [CrossRef]
- Wang, D.; Yang, J.; Fan, J.; Chen, W.; Nikolic-Paterson, D.J.; Li, J. Omics technologies for kidney disease research. Anat. Rec. 2020, 303, 2729–2742. [Google Scholar] [CrossRef] [PubMed]
- Hu, J.; Yu, Y. Epigenetic response profiles into environmental epigenotoxicant screening and health risk assessment: A critical review. Chemosphere 2019, 226, 259–272. [Google Scholar] [CrossRef]
- McCartney, D.L.; Stevenson, A.J.; Walker, R.M.; Gibson, J.; Morris, S.W.; Campbell, A.; Murray, A.D.; Whalley, H.C.; Porteous, D.J.; McIntosh, A.M.; et al. Investigating the relationship between DNA methylation age acceleration and risk factors for Alzheimer’s disease. Alzheimers Dement. 2018, 10, 429–437. [Google Scholar] [CrossRef]
- Peters, I.; Dubrowinskaja, N.; Hennenlotter, J.; Antonopoulos, W.I.; Von Klot, C.A.; Tezval, H.; Stenzl, A.; Kuczyk, M.A.; Serth, J. DNA methylation of neural EGFL like 1 (NELL1) is associated with advanced disease and the metastatic state of renal cell cancer patients. Oncol. Rep. 2018, 40, 3861–3868. [Google Scholar] [CrossRef] [PubMed]
- Korea National Health and Nutrition Examination Survey (KNHANES). Available online: https://knhanes.kdca.go.kr/knhanes/sub08/sub08_02.do (accessed on 26 May 2024).
- Ministry of Environment. Results of the National Environmental Health Basic Survey—Exposuref Levels of Harmful Substances in the Human Body. 2020. Available online: https://kosis.kr/statHtml/statHtml.do?orgId=106&tblId=DT_106N_99_1100051&conn_path=I2 (accessed on 24 March 2024).
- Koide, T.; Banno, M.; Aleksic, B.; Yamashita, S.; Kikuchi, T.; Kohmura, K.; Adachi, Y.; Kawano, N.; Kushima, I.; Nakamura, Y.; et al. Common variants in MAGI2 gene are associated with increased risk for cognitive impairment in schizophrenic patients. PLoS ONE 2012, 7, e36836. [Google Scholar] [CrossRef] [PubMed]
- Nunnelly, L.F.; Campbell, M.; Lee, D.I.; Dummer, P.; Gu, G.; Menon, V.; Au, E. St18 specifies globus pallidus projection neuron identity in MGE lineage. Nat. Commun. 2022, 13, 7735. [Google Scholar] [CrossRef] [PubMed]
- Lin, L.; Lesnick, T.G.; Maraganore, D.M.; Isacson, O. Axon guidance and synaptic maintenance: Preclinical markers for neurodegenerative disease and therapeutics. Trends Neurosc. 2009, 32, 142–149. [Google Scholar] [CrossRef] [PubMed]
- Cornejo, F.; Cortés, B.I.; Findlay, G.M.; Cancino, G.I. LAR receptor tyrosine phosphatase family in healthy and diseased brain. Front. Cell Dev. Biol. 2021, 9, 659951. [Google Scholar] [CrossRef]
- Tang, B.L. (WNK) ing at death: With-no-lysine (Wnk) kinases in neuropathies and neuronal survival. Brain Res. Bull. 2016, 125, 92–98. [Google Scholar] [CrossRef] [PubMed]
- Kataoka, M.; Sahashi, K.; Tsujikawa, K.; Takeda, J.I.; Hirunagi, T.; Iida, M.; Katsuno, M. Dysregulation of Aldh1a2 underlies motor neuron degeneration in spinal muscular atrophy. Neurosci. Res. 2023, 194, 58–65. [Google Scholar] [CrossRef]
- Rasi, K.; Hurskainen, M.; Kallio, M.; Stavén, S.; Sormunen, R.; Heape, A.M.; Avila, R.L.; Kirschner, D.; Muona, A.; Tolonen, U.; et al. Lack of collagen XV impairs peripheral nerve maturation and, when combined with laminin-411 deficiency, leads to basement membrane abnormalities and sensorimotor dysfunction. J. Neurosci. 2010, 30, 14490–14501. [Google Scholar] [CrossRef]
- Eysert, F.; Coulon, A.; Boscher, E.; Vreulx, A.C.; Flaig, A.; Mendes, T.; Hughes, S.; Grenier-Boley, B.; Hanoulle, X.; Demiautte, F.; et al. Alzheimer’s genetic risk factor FERMT2 (Kindlin-2) controls axonal growth and synaptic plasticity in an APP-dependent manner. Mol. Psychiatry 2021, 26, 5592–5607. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Huang, Y.; Chen, J.Y.; Ding, Y.Q.; Song, N.N. DSCAM and DSCAML1 regulate the radial migration and callosal projection in developing cerebral cortex. Brain Res. 2015, 1594, 61–70. [Google Scholar] [CrossRef]
- Vega-Vásquez, I.; Lobos, P.; Toledo, J.; Adasme, T.; Paula-Lima, A.; Hidalgo, C. Hippocampal dendritic spines express the RyR3 but not the RyR2 ryanodine receptor isoform. Biochem. Biophys. Res. Commun. 2022, 633, 96–103. [Google Scholar] [CrossRef]
- Li, Q.; Vo, H.T.; Wang, J.; Fox-Quick, S.; Dobrunz, L.E.; King, G.D. Klotho regulates CA1 hippocampal synaptic plasticity. Neuroscience 2017, 347, 123–133. [Google Scholar] [CrossRef] [PubMed]
- Blalock, E.M.; Chen, K.C.; Stromberg, A.J.; Norris, C.M.; Kadish, I.; Kraner, S.D.; Porter, N.M.; Landfield, P.W. Harnessing the power of gene microarrays for the study of brain aging and Alzheimer’s disease: Statistical reliability and functional correlation. Ageing Res. Rev. 2005, 4, 481–512. [Google Scholar] [CrossRef] [PubMed]
- Ge, R.; Wang, C.; Liu, J.; Jiang, H.; Liu, Z. A novel tumor-promoting role for nuclear factor IX in glioblastoma is mediated through transcriptional activation of GINS1. Mol. Cancer Res. 2023, 21, 189–198. [Google Scholar] [CrossRef] [PubMed]
- Li, C.; Yang, J.; Lei, S.; Wang, W. SKA3 promotes glioblastoma proliferation and invasion by enhancing the activation of Wnt/β-catenin signaling via modulation of the Akt/GSK-3β axis. Brain Res. 2021, 1765, 147500. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Devadoss, D.; Nair, M.; Chand, H.S.; Lakshmana, M.K. Novel Alzheimer risk factor IQ motif containing protein K is abundantly expressed in the brain and is markedly increased in patients with Alzheimer’s disease. Front. Cell. Neurosci. 2022, 16, 954071. [Google Scholar] [CrossRef] [PubMed]
- Song, Y.; Zheng, S.; Wang, J.; Long, H.; Fang, L.; Wang, G.; Li, Z.; Que, T.; Liu, Y.; Li, Y.; et al. Hypoxia-induced PLOD2 promotes proliferation, migration and invasion via PI3K/Akt signaling in glioma. Oncotarget 2017, 8, 41947. [Google Scholar] [CrossRef] [PubMed]
- Lee, D.; Porras, C.; Spencer, C.; Pjanic, M.; Weiler, P.; Kosoy, R.; Bendl, J.; NM, P.; Wang, X.; Zheng, S.; et al. Plasticity of human microglia and brain perivascular macrophages in aging and Alzheimer’s disease. medRxiv 2023. [Google Scholar] [CrossRef]
- Wilmot, B.; Fry, R.; Smeester, L.; Musser, E.D.; Mill, J.; Nigg, J.T. Methylomic analysis of salivary DNA in childhood ADHD identifies altered DNA methylation in VIPR 2. J. Child Psychol. Psychiatry 2016, 57, 152–160. [Google Scholar] [CrossRef]
- Zhang, L.; He, C.H.; Coffey, S.; Yin, D.; Hsu, I.U.; Su, C.; Ye, Y.; Zhang, C.; Spurrier, J.; Nicholson, L.; et al. Single-cell transcriptomic atlas of Alzheimer’s disease middle temporal gyrus reveals region, cell type and sex specificity of gene expression with novel genetic risk for MERTK in female. medRxiv 2023. Preprint. [Google Scholar] [CrossRef]
- Li, Z.; Jin, Y.; Zhang, P.; Zhang, X.A.; Yi, G.; Zheng, H.; Yuan, X.; Wang, X.; Xu, H.; Qiu, X.; et al. A Four-Gene Panel for the Prediction of Prognosis and Immune Cell Enrichment in Gliomas. Mol. Biotechnol. 2023, 1–14. [Google Scholar] [CrossRef]
- Leandro, G.S.; Evangelista, A.F.; Lobo, R.R.; Xavier, D.J.; Moriguti, J.C.; Sakamoto-Hojo, E.T. Changes in expression profiles revealed by transcriptomic analysis in peripheral blood mononuclear cells of Alzheimer’s disease patients. J. Alzheimer’s Dis. 2018, 66, 1483–1495. [Google Scholar] [CrossRef] [PubMed]
- He, Y.; Zheng, W.; Huo, Y.; Sa, L.; Zhang, H.; He, G.; Shang, P. PLEKHA4 promotes glioblastoma progression through apoptosis inhibition, tumor cell migration, and macrophage infiltration. Immunobiology 2023, 228, 152746. [Google Scholar] [CrossRef]
- Korbecki, J.; Rębacz-Maron, E.; Kupnicka, P.; Chlubek, D.; Baranowska-Bosiacka, I. Synthesis and significance of arachidonic acid, a substrate for cyclooxygenases, lipoxygenases, and cytochrome P450 pathways in the tumorigenesis of glioblastoma multiforme, including a pan-cancer comparative analysis. Cancers 2023, 15, 946. [Google Scholar] [CrossRef]
- Li, F.; Jin, D.; Guan, L.; Zhang, C.C.; Wu, T.; Wang, Y.J.; Gao, D.S. CEP55 promoted the migration, invasion and neuroshpere formation of the glioma cell line U251. Neurosci. Lett. 2019, 705, 80–86. [Google Scholar] [CrossRef]
- Soles, A.; Selimovic, A.; Sbrocco, K.; Ghannoum, F.; Hamel, K.; Moncada, E.L.; Gilliat, S.; Cvetanovic, M. Extracellular matrix regulation in physiology and in brain disease. Int. J. Mol. Sci. 2023, 24, 7049. [Google Scholar] [CrossRef] [PubMed]
- Uzay, B.; Bahadır-Varol, A.; Hökelekli, F.Ö.; Yılmaz, M.; Esen, E.C.; Başar, K.; Ayhan, Y.; Dalkara, T.; Eren-Koçak, E. FGF2 gene’s antisense protein, NUDT6, the antisense protein of FGF2 gene, plays a depressogenic role by promoting inflammation and suppressing neurogenesis without altering FGF2 signaling. J. Physiol. 2024, 602, 1427–1442. [Google Scholar] [CrossRef]
- Tsai, Y.T.; Wu, A.C.; Yang, W.B.; Kao, T.J.; Chuang, J.Y.; Chang, W.C.; Hsu, T.I. ANGPTL4 induces TMZ resistance of glioblastoma by promoting cancer stemness enrichment via the EGFR/AKT/4E-BP1 cascade. Int. J. Mol. Sci. 2019, 20, 5625. [Google Scholar] [CrossRef]
- Begcevic, I.; Brinc, D.; Brown, M.; Martinez-Morillo, E.; Goldhardt, O.; Grimmer, T.; Magdolen, V.; Batruch, I.; Diamandis, E.P. Brain-related proteins as potential CSF biomarkers of Alzheimer’s disease: A targeted mass spectrometry approach. J. Proteom. 2018, 182, 12–20. [Google Scholar] [CrossRef]
- Yu, F.; Li, G.; Gao, J.; Sun, Y.; Liu, P.; Gao, H.; Li, P.; Lei, T.; Chen, Y.; Cheng, Y.; et al. SPOCK1 is upregulated in recurrent glioblastoma and contributes to metastasis and Temozolomide resistance. Cell Prolif. 2016, 49, 195–206. [Google Scholar] [CrossRef]
- Qi, H.; Wang, P.; Sun, H.; Li, X.; Hao, X.; Tian, W.; Yu, L.; Tang, J.; Dong, J.; Wang, H. ADAMDEC1 accelerates GBM progression via activation of the MMP2-related pathway. Front. Oncol. 2022, 12, 945025. [Google Scholar] [CrossRef]
- Gottschalk, W.K.; Mihovilovic, M.; Roses, A.D.; Chiba-Falek, O. The role of upregulated APOE in Alzheimer’s disease etiology. J. Alzheimers Dis. Park. 2016, 6, 209. [Google Scholar] [CrossRef] [PubMed]
- Zhu, W.; Krishna, S.; Garcia, C.; Lin, C.C.J.; Mitchell, B.D.; Scott, K.L.; Mohila, C.A.; Creighton, C.J.; Yoo, S.H.; Lee, H.K.; et al. Daam2 driven degradation of VHL promotes gliomagenesis. Elife 2017, 6, e31926. [Google Scholar] [CrossRef] [PubMed]
- Vilhais-Neto, G.C.; Pourquié, O. Retinoic acid. Curr. Biol. 2008, 18, R191–R192. [Google Scholar] [CrossRef] [PubMed]
- Maden, M. Retinoid signalling in the development of the central nervous system. Nat. Rev. Neurosci. 2002, 3, 843–853. [Google Scholar] [CrossRef]
- Maden, M. Retinoic acid in the development, regeneration and maintenance of the nervous system. Nat. Rev. Neurosci. 2007, 8, 755–765. [Google Scholar] [CrossRef] [PubMed]
- Sui, Y.; Stehno-Bittel, L.; Li, S.; Loganathan, R.; Dhillon, N.K.; Pinson, D.; Nath, A.; Kolson, D.; Narayan, O.; Buch, S. CXCL10-induced cell death in neurons: Role of calcium dysregulation. Eur. J. Neurosci. 2006, 23, 957–964. [Google Scholar] [CrossRef] [PubMed]
- Hong, H.; Kim, B.S.; Im, H.I. Pathophysiological role of neuroinflammation in neurodegenerative diseases and psychiatric disorders. Int. Neurourol. J. 2016, 20, S2–S7. [Google Scholar] [CrossRef] [PubMed]
- Lin, D.; Li, W.; Zhang, N.; Cai, M. Identification of TNFAIP6 as a hub gene associated with the progression of glioblastoma by weighted gene co-expression network analysis. IET Syst. Biol. 2022, 16, 145–156. [Google Scholar] [CrossRef]
- Duan, Z.; Shi, L.; He, Z.N.T.; Kuang, C.; Han, T.; Yang, Q. The protective effect of IDO1 inhibition in Aβ-treated neurons and APP/PS1 mice. Am. J. Alzheimers Dis. Other Demen. 2023, 38, 15333175231214861. [Google Scholar] [CrossRef]
- Solas, M.; Zamarbide, M.; Ardanaz, C.G.; Ramírez, M.J.; Pérez-Mediavilla, A. The cognitive improvement and alleviation of brain hypermetabolism caused by FFAR3 ablation in Tg2576 mice is persistent under diet-induced obesity. Int. J. Mol. Sci. 2022, 23, 13591. [Google Scholar] [CrossRef] [PubMed]
- Lei, C.; Zhongyan, Z.; Wenting, S.; Jing, Z.; Liyun, Q.; Hongyi, H.; Juntao, Y.; Qing, Y. Identification of necroptosis-related genes in Parkinson’s disease by integrated bioinformatics analysis and experimental validation. Front. Neurosci. 2023, 17, 1097293. [Google Scholar] [CrossRef] [PubMed]
- Sanfilippo, C.; Longo, A.; Lazzara, F.; Cambria, D.; Distefano, G.; Palumbo, M.; Cantarella, A.; Malaguarnera, L.; Di Rosa, M. CHI3L1 and CHI3L2 overexpression in motor cortex and spinal cord of sALS patients. Mol. Cell. Neurosci. 2017, 85, 162–169. [Google Scholar] [CrossRef] [PubMed]
- Zhang, R.; Hadlock, K.G.; Do, H.; Yu, S.; Honrada, R.; Champion, S.; Forshew, D.; Madison, C.; Katz, J.; Miller, R.G.; et al. Gene expression profiling in peripheral blood mononuclear cells from patients with sporadic amyotrophic lateral sclerosis (sALS). J. Neuroimmunol. 2011, 230, 114–123. [Google Scholar] [CrossRef] [PubMed]
- Silva, C.R.S.; Biselli-Périco, J.M.; Zampieri, B.L.; Silva, W.A.; de Souza, J.E.S.; Bürger, M.C.; Goloni-Bertollo, E.M.; Pavarino, É.C. Differential expression of inflammation-related genes in children with Down syndrome. Mediat. Inflamm. 2016, 2016, 6985903. [Google Scholar] [CrossRef] [PubMed]
- Duc Nguyen, H.; Hoang, N.M.H.; Ko, M.; Seo, D.; Kim, S.; Jo, W.H.; Bae, J.W.; Kim, M.S. Association between serum prolactin levels and neurodegenerative diseases: Systematic review and meta-analysis. Neuroimmunomodulation 2022, 29, 85–96. [Google Scholar] [CrossRef] [PubMed]
- Litvinchuk, A.; Wan, Y.W.; Swartzlander, D.B.; Chen, F.; Cole, A.; Propson, N.E.; Wang, Q.; Zhang, B.; Liu, Z.; Zheng, H. Complement C3aR inactivation attenuates tau pathology and reverses an immune network deregulated in tauopathy models and Alzheimer’s disease. Neuron 2018, 100, 1337–1353.e5. [Google Scholar] [CrossRef] [PubMed]
- Kampa, M.; Castanas, E. Human health effects of air pollution. Environ. Pollut. 2008, 151, 362–367. [Google Scholar] [CrossRef] [PubMed]
- Shin, S.S.; Yang, E.H.; Lee, H.C.; Moon, S.H.; Ryoo, J.H. Association of metabolites of benzene and toluene with lipid profiles in Korean adults: Korean National Environmental Health Survey (2015–2017). BMC Public Health 2022, 22, 1917. [Google Scholar] [CrossRef]
- Jung, S.K.; Choi, W.H.; Kim, S.Y.; Hong, S.Y.; Jeon, H.L.; Joo, Y.K.; Lee, C.W.; Choi, K.H.; Kim, S.K.; Lee, K.J.; et al. Profile of environmental chemicals in the Korean population—Results of the Korean national environmental health survey (KoNEHS) cycle 3, 2015–2017. Int. J. Environ. Res. Public Health 2022, 19, 626. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention (CDC). Fourth National Report on Human Exposure to Environmental Chemicals; Centers for Disease Control and Prevention, Division of Laboratory Sciences: Atlanta, GA, USA, 2019.
- Health Canada. Fifth Report on Human Biomonitoring of Environmental Chemicals in Canada; Health Canada: Ottawa, ON, Canada, 2019.
- Wang, N.; Wang, M.; Jeevaratnam, S.; Rosenberg, C.; Ikezu, T.C.; Shue, F.; Doss, S.V.; Alnobani, A.; Martens, Y.A.; Wren, M.; et al. Opposing effects of apoE2 and apoE4 on microglial activation and lipid metabolism in response to demyelination. Mol. Neurodegener. 2022, 17, 75. [Google Scholar] [CrossRef] [PubMed]
- Liu, C.C.; Liu, C.C.; Kanekiyo, T.; Xu, H.; Bu, G. Apolipoprotein E and Alzheimer disease: Risk, mechanisms and therapy. Nat. Rev. Neurol. 2013, 9, 106–118. [Google Scholar] [CrossRef] [PubMed]
- Yang, L.G.; March, Z.M.; Stephenson, R.A.; Narayan, P.S. Apolipoprotein E in lipid metabolism and neurodegenerative disease. Trends Endocrinol. Metab. 2023, 34, 430–445. [Google Scholar] [CrossRef]
- De Schepper, S.; Ge, J.Z.; Crowley, G.; Ferreira, L.S.; Garceau, D.; Toomey, C.E.; Sokolova, D.; Rueda-Carrasco, J.; Shin, S.H.; Kim, J.S.; et al. Perivascular cells induce microglial phagocytic states and synaptic engulfment via SPP1 in mouse models of Alzheimer’s disease. Nat. Neurosci. 2023, 26, 406–415. [Google Scholar] [CrossRef] [PubMed]
- Kot-Leibovich, H.; Fainsod, A. Ethanol induces embryonic malformations by competing for retinaldehyde dehydrogenase activity during vertebrate gastrulation. Dis. Model. Mech. 2009, 2, 295–305. [Google Scholar] [CrossRef] [PubMed]
- Shabab, T.; Khanabdali, R.; Moghadamtousi, S.Z.; Kadir, H.A.; Mohan, G. Neuroinflammation pathways: A general review. Int. J. Neurosci. 2017, 127, 624–633. [Google Scholar] [CrossRef] [PubMed]
- Ng, A.; Tam, W.W.; Zhang, M.W.; Ho, C.S.; Husain, S.F.; McIntyre, R.S.; Ho, R.C. IL-1β, IL-6, TNF-α and CRP in elderly patients with depression or Alzheimer’s disease: Systematic review and meta-analysis. Sci. Rep. 2018, 8, 12050. [Google Scholar] [CrossRef]
- Liu, J.; Zhang, J.; Ao, Y. Exosomes derived from regulatory T cells attenuates MPP+-induced inflammatory response and oxidative stress in BV-2 cells by inhibiting the TLR4/NF-κB signaling. Mol. Cell. Toxicol. 2023, 19, 283–291. [Google Scholar] [CrossRef]
- Cho, J.; Nelson, T.E.; Bajova, H.; Gruol, D.L. Chronic CXCL10 alters neuronal properties in rat hippocampal culture. J. Neuroimmunol. 2009, 207, 92–100. [Google Scholar] [CrossRef]
- Hashemi, F.; Hamidinejad, F.S.; Hoepner, L.; Rafiee, A.; Abbasi, A.; Hoseini, M. BTEX exposure of pregnant women and associations with pro-inflammatory cytokines (IL-6 and TNF-α). Air Qual. Atmos. Health 2021, 15, 707–719. [Google Scholar] [CrossRef]

| Personal Characteristics | Low Exposure | High Exposure | p |
|---|---|---|---|
| Maternal group | n = 72 | n = 25 | |
| BMA (μg/g creatinine) | 2.9 ± 1.3 | 30.5 ± 96.0 | 0.163 |
| Age | 37.5 ± 3.0 | 36.8 ± 3.6 | 0.425 |
| Smoking | 0.368 | ||
| No | 58 (80.6%) | 17 (68.0%) | |
| Yes | 3 (4.2%) | 1 (4.0%) | |
| Missing data | 11 (15.3%) | 7 (28.0%) | |
| Childbirth | 0.724 | ||
| 1 | 32 (52.5%) | 10 (55.6%) | |
| 2 | 21 (34.4%) | 7 (38.9%) | |
| 3 | 5 (8.2%) | 0 (0.0%) | |
| 4 | 2 (3.3%) | 1 (5.6%) | |
| 5 | 1 (1.6%) | 0 (0.0%) | |
| Infant group | n = 72 | n = 25 | |
| Sex | 0.213 | ||
| Male | 43 (59.7%) | 10 (40.0%) | |
| Female | 21 (29.2%) | 10 (40.0%) | |
| Missing data | 8 (11.1%) | 5 (20.0%) | |
| Height | 50.0 ± 1.9 | 49.3 ± 2.0 | 0.232 |
| Weight | 3.3 ± 0.4 | 3.2 ± 0.4 | 0.871 |
| Head circumference | 34.5 ± 1.3 | 34.2 ± 1.3 | 0.460 |
| Denver test (6 M) | 0.076 | ||
| Normal | 62 (86.1%) | 17 (68.0%) | |
| Untested | 10 (13.9%) | 8 (32.0%) | |
| Denver test (12 M) | 0.035 | ||
| Normal | 62 (86.1%) | 16 (64.0%) | |
| Untested | 10 (13.9%) | 9 (36.0%) |
| BMA (μg/g Creatinine) | Maternal Group | |
|---|---|---|
| Low-Exposure | High-Exposure | |
| Limit of Detection (LOD) | 0.03 (μg/L) | |
| Minimum | 0.33 | 5.99 |
| Maximum | 5.74 | 489.83 |
| Geometric mean | 2.52 | 11.47 |
| Arithmetic mean | 2.86 | 30.46 |
| Standard Deviation (SD) | 1.26 | 95.97 |
| Independent Variable | B | SE | Wald | p | OR | 95% CI | ||
|---|---|---|---|---|---|---|---|---|
| LLCI | ULCI | |||||||
| Sample collection area | Areas other than Seoul | 0.97 | 0.60 | 2.65 | 0.10 | 2.64 | 0.82 | 8.51 |
| Age range | 20–30 s | 0.54 | 0.71 | 0.58 | 0.45 | 1.71 | 0.430 | 6.84 |
| Smoking | yes | −0.08 | 1.24 | 0.004 | 0.95 | 0.93 | 0.08 | 10.45 |
| Childbirth | 2 times | 0.78 | 1.16 | 0.45 | 0.50 | 2.18 | 0.22 | 21.28 |
| 3 or more times | 0.79 | 1.17 | 046 | 0.50 | 2.21 | 0.22 | 22.06 | |
| Group | Genes | Hyper-Methylated (LogFC/p) | Downregulated (LogFC/FDR) | Functional Characteristics | Reference |
|---|---|---|---|---|---|
| Maternal group | MAGI2 | 1.49/0.02 | −1.69/2.02 × 10−5 | Underdevelopment of nerve dendrites and loss of synapses in nerve cells. | [24] |
| ST18 | 1.45/0.01 | −1.60/1.55 × 10−4 | Knockout reduces axonal outgrowth, synaptic density, and punctate size. | [25] | |
| SLIT3 | 1.87/5.78 × 10−4 | −1.55/2.63 × 10−3 | Participate in lipopolysaccharide-induced inflammatory response, which may contribute to the pathogenesis of Parkinson’s disease. | [26] | |
| PTPRD | 1.14/0.02 | −1.41/0.02 | Dendrite branching, length and thickness are reduced. | [27] | |
| WNK2 | 1.96/1.00 × 10−3 | −1.35/1.50 × 10−3 | Significant reduction in gliomas and meningiomas due to hyper-methylation. | [28] | |
| ALDH1A2 | 1.03/0.02 | −1.30/8.91 × 10−4 | Knockdown causes neurite degeneration in motor neurons. | [29] | |
| COL15A1 | 1.45/0.03 | −1.28/5.35 × 10−3 | Deficient mice suffer from motor impairment. | [30] | |
| FERMT2 | 1.00/0.04 | −1.10/0.02 | Downregulated expression reduces synaptic connectivity. | [31] | |
| DSCAML1 | 1.51/0.01 | −1.10/0.02 | Interferes with axonal growth in cultured neurons. | [32] | |
| Infant group | RYR2 | 1.40/0.01 | −1.21/0.04 | Loss of RyR2 impairs neuronal activity-dependent remodeling of dendrites. | [33] |
| Group | Genes | Hypo-Methylated (LogFC/p) | Upregulated (LogFC/FDR) | Functional Characteristics | Reference |
|---|---|---|---|---|---|
| Maternal group | KL | −1.23/0.02 | 1.37/5.88 × 10−5 | Decreases long-term potentiation at CA1 synapses. | [34] |
| SERPINI2 | −1.08/0.04 | 1.41/7.15 × 10−5 | Over-expressed in Alzheimer’s disease (AD). | [35] | |
| GINS1 | −0.89/0.04 | 1.13/1.16 × 10−3 | Over-expressed in glioblastoma multiforme (GBM). | [36] | |
| SKA3 | −0.66/0.05 | 1.13/2.09 × 10−3 | Over-expressed in GBM. | [37] | |
| IQCK | −1.11/0.01 | 1.07/4.24 × 10−3 | Over-expressed in astrocytes, neurons, and oligodendrocytes in AD brain. | [38] | |
| PLOD2 | −1.07/0.04 | 1.02/8.86 × 10−3 | Upregulated in glioma. | [39] | |
| PTPRG | −1.10/0.01 | 1.01/8.16 × 10−3 | Over-expressed in AD. | [40] | |
| VIPR2 | −1.36/0.02 | 1.01/7.08 × 10−3 | Hypo-methylated in GBM. | [41] | |
| TPRG1 | −1.42/1.91 × 10−3 | 1.01/0.01 | Over-expressed in AD (Women-specific). | [42] | |
| DLGAP5 | −1.22/0.01 | 0.96/0.01 | Over-expression in Gliomas. | [43] | |
| CYP4F3 | −0.87/0.03 | 0.95/0.01 | Over-expressed in AD. | [44] | |
| PLEKHA4 | −1.12/0.04 | 0.91/0.02 | Over-expressed in GBM. | [45] | |
| GGT5 | −1.08/0.01 | 0.95/0.03 | Over-expressed in GBM. | [46] | |
| CEP55 | −0.74/0.03 | 0.87/0.05 | Over-expressed promotes glioma cell invasion. | [47] | |
| Infant group | COL5A3 | −1.59/2.50 × 10−4 | 2.00/5.11 × 10−11 | Upregulated in a mouse model of neuropathic pain. | [48] |
| NUDT6 | −0.95/0.01 | 1.59/1.11 × 10−5 | Over-expression increases anxiety and depression-like behavior in mice. | [49] | |
| ANGPTL4 | −1.91/3.11 × 10−5 | 1.36/3.19 × 10−5 | Over-expressed in GBM, usually associated with poor prognosis. | [50] | |
| SPP1 | −1.43/7.34 × 10−4 | 1.07/6.68 × 10−3 | Upregulated in mild cognitive impairment (MCI). | [51] | |
| SPOCK1 | −1.69/4.08 × 10−5 | 1.05/0.03 | Expression is significantly upregulated in recurrent GBM. | [52] | |
| ADAMDEC1 | −1.13/0.03 | 1.04/0.04 | The higher the expression, the higher the malignancy of glioma and the worse the prognosis. | [53] | |
| APOE | −1.03/0.02 | 1.02/0.01 | Over-expressed and contributes to the pathogenesis of late-onset AD (LOAD). | [54] | |
| DAAM2 | −1.48/1.07 × 10−3 | 0.99/0.03 | Over-expression accelerates glioma tumor development. | [55] |
| Group | Genes | LogFC | FDR | Functional Characteristics | Reference |
|---|---|---|---|---|---|
| Maternal group | IL6 | 2.64 | 7.37 × 10−24 | Neuroinflammation and neuron degeneration. | [60] |
| CXCL10 | 1.95 | 2.36 × 10−12 | Upregulated in various neurodegenerative diseases. | [59] | |
| TNFAIP6 | 1.89 | 1.18 × 10−11 | Upregulation is associated with poor prognosis in patients with glioblastoma multiforme. | [61] | |
| IDO1 | 1.83 | 2.38 × 10−10 | Over-expressed in Alzheimer’s disease (AD). | [62] | |
| FFAR3 | 1.19 | 5.06 × 10−4 | Upregulated in early stages of AD pathology. | [63] | |
| TNIP3 | 1.14 | 9.51 × 10−4 | Over-expressed in Parkinson’s disease. | [64] | |
| CHI3L1 | 1.09 | 1.84 × 10−3 | Expressed during nerve degeneration. | [65] | |
| ORM1 | 1.09 | 1.92 × 10−3 | Upregulated in patients with sporadic amyotrophic lateral sclerosis (sALS). | [66] | |
| PLA2G2D | 1.17 | 4.50 × 10−3 | Over-expressed in Down’s syndrome (DS). | [67] | |
| IL1RN | 0.96 | 8.69 × 10−3 | Upregulated in patients with sALS. | [66] | |
| ADORA2A | 0.91 | 0.02 | Upregulated when synapses in neurons are damaged. | [68] | |
| Infant group | CXCL10 | 1.13 | 0.04 | Upregulated in various neurodegenerative diseases. | [59] |
| C3AR1 | 0.91 | 0.04 | Confirmed that over-expression correlates with cognitive decline in patients with AD. | [69] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Yu, S.Y.; Kim, S.H.; Choo, J.H.; Jang, S.; Kim, J.; Ahn, K.; Hwang, S.Y. Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants. Int. J. Mol. Sci. 2024, 25, 6215. https://doi.org/10.3390/ijms25116215
Yu SY, Kim SH, Choo JH, Jang S, Kim J, Ahn K, Hwang SY. Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants. International Journal of Molecular Sciences. 2024; 25(11):6215. https://doi.org/10.3390/ijms25116215
Chicago/Turabian StyleYu, So Yeon, Seung Hwan Kim, Jeong Hyeop Choo, Sehun Jang, Jihyun Kim, Kangmo Ahn, and Seung Yong Hwang. 2024. "Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants" International Journal of Molecular Sciences 25, no. 11: 6215. https://doi.org/10.3390/ijms25116215
APA StyleYu, S. Y., Kim, S. H., Choo, J. H., Jang, S., Kim, J., Ahn, K., & Hwang, S. Y. (2024). Potential Effects of Low-Level Toluene Exposure on the Nervous System of Mothers and Infants. International Journal of Molecular Sciences, 25(11), 6215. https://doi.org/10.3390/ijms25116215






