Kaempferol: Antimicrobial Properties, Sources, Clinical, and Traditional Applications
Abstract
1. Introduction
2. Biosynthesis and Availability of Kaempferol
2.1. Biosynthetic Pathways of Kaempferol
2.2. Bioavailability of Kaempferol
3. Kaempferol as an Antibacterial Agent
3.1. Antibacterial Activity against Acinetobacter baumannii
3.2. Antibacterial Activity against Bacillus Spp.
3.3. Antibacterial Activity against Escherichia coli
3.4. Antibacterial Activity against Klebsiella pneumoniae
3.5. Antibacterial Activity against Mycobacterium Spp.
3.6. Antibacterial Activity against Pseudomonas aeruginosa
3.7. Antibacterial Activity against Salmonella Spp.
3.8. Antibacterial Activity against Staphylococcus Spp.
3.9. Antibacterial Activity against Enterococci
3.10. Antibacterial Activity against Proteus Spp.
3.11. Antibacterial Activity against Vibrio cholerae
4. Antifungal Properties of Kaempferol
5. Antiprotozoal Properties of Kaempferol
5.1. Antiprotozoal Action against Entamoeba histolytica and Giardia lamblia
5.2. Antiprotozoal Action against Trypanosoma Spp.
5.3. Antiprotozoal Action against Plasmidium Spp.
5.4. Antiprotozoal Action against Leishmania Spp.
6. Kaempferol-Containing Plants in Traditional Medical Systems
Kaempferol-Containing Plants in the Context of Traditional Chinese Medicine
7. Discussion and Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Veeresham, C. Natural products derived from plants as a source of drugs. J. Adv. Pharm. Technol. Res. 2012, 3, 200–201. [Google Scholar] [CrossRef] [PubMed]
- Katiyar, C.; Gupta, A.; Kanjilal, S.; Katiyar, S. Drug discovery from plant sources: An integrated approach. Ayu 2012, 33, 10–19. [Google Scholar] [CrossRef]
- Seidel, V. Plant-Derived Chemicals: A Source of Inspiration for New Drugs. Plants 2020, 9, 1562. [Google Scholar] [CrossRef] [PubMed]
- Petran, M.; Dragos, D.; Gilca, M. Historical ethnobotanical review of medicinal plants used to treat children diseases in Romania (1860s–1970s). J. Ethnobiol. Ethnomedicine 2020, 16, 15. [Google Scholar] [CrossRef] [PubMed]
- Verma, A.R.; Vijayakumar, M.; Mathela, C.S.; Rao, C.V. In vitro and in vivo antioxidant properties of different fractions of Moringa oleifera leaves. Food Chem. Toxicol. 2009, 47, 2196–2201. [Google Scholar] [CrossRef] [PubMed]
- Gilca, M.; Gaman, L.; Panait, E.; Stoian, I.; Atanasiu, V. Chelidonium majus–an integrative review: Traditional knowledge versus modern findings. Complement. Med. Res. 2010, 17, 241–248. [Google Scholar] [CrossRef] [PubMed]
- Singh, N.; Bhalla, M.; de Jager, P.; Gilca, M. An overview on ashwagandha: A Rasayana (rejuvenator) of Ayurveda. Afr. J. Tradit. Complement. Altern. Med. 2011, 8, 208–213. [Google Scholar] [CrossRef]
- Singh, N.; Pandey, B.; Verma, P.; Bhalla, M.; Gilca, M. Phyto-pharmacotherapeutics of Cyperus rotundus Linn.(Motha): An overview. Indian J. Nat. Prod. Res. 2012, 3, 467–476. [Google Scholar]
- Liu, R.H. Health-promoting components of fruits and vegetables in the diet. Adv. Nutr. 2013, 4, 384s–392s. [Google Scholar] [CrossRef] [PubMed]
- Reedy, J.; Krebs-Smith, S.M.; Miller, P.E.; Liese, A.D.; Kahle, L.L.; Park, Y.; Subar, A.F. Higher Diet Quality Is Associated with Decreased Risk of All-Cause, Cardiovascular Disease, and Cancer Mortality among Older Adults. J. Nutr. 2014, 144, 881–889. [Google Scholar] [CrossRef] [PubMed]
- Bontempo, P.; De Masi, L.; Carafa, V.; Rigano, D.; Scisciola, L.; Iside, C.; Grassi, R.; Molinari, A.M.; Aversano, R.; Nebbioso, A.; et al. Anticancer activities of anthocyanin extract from genotyped Solanum tuberosum L. “Vitelotte”. J. Funct. Foods 2015, 19, 584–593. [Google Scholar] [CrossRef]
- Siri-Tarino, P.W.; Krauss, R.M. Diet, lipids, and cardiovascular disease. Curr. Opin. Lipidol. 2016, 27, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Lange, K.W.; Lange, K.M.; Makulska-Gertruda, E.; Nakamura, Y.; Reissmann, A.; Kanaya, S.; Hauser, J. Ketogenic diets and Alzheimer’s disease. Food Sci. Hum. Wellness 2017, 6, 1–9. [Google Scholar] [CrossRef]
- Playdon, M.C.; Nagle, C.M.; Ibiebele, T.I.; Ferrucci, L.M.; Protani, M.M.; Carter, J.; Hyde, S.E.; Neesham, D.; Nicklin, J.L.; Mayne, S.T.; et al. Pre-diagnosis diet and survival after a diagnosis of ovarian cancer. Br. J. Cancer 2017, 116, 1627–1637. [Google Scholar] [CrossRef] [PubMed]
- Periferakis, A.; Periferakis, K. On the Dissemination of Acupuncture to Europe. JournalNX 2020, 6, 201–209. [Google Scholar]
- Farombi, E.O.; Akinmoladun, A.C.; Owumi, S.E. Anti-Cancer Foods: Flavonoids. In Encyclopedia of Food Chemistry; Melton, L., Shahidi, F., Varelis, P., Eds.; Academic Press: Oxford, UK, 2019; pp. 224–236. [Google Scholar] [CrossRef]
- Havsteen, B.H. The biochemistry and medical significance of the flavonoids. Pharmacol. Ther. 2002, 96, 67–202. [Google Scholar] [CrossRef] [PubMed]
- Panche, A.N.; Diwan, A.D.; Chandra, S.R. Flavonoids: An overview. J. Nutr. Sci. 2016, 5, e47. [Google Scholar] [CrossRef] [PubMed]
- Corradini, E.; Foglia, P.; Giansanti, P.; Gubbiotti, R.; Samperi, R.; Laganà, A. Flavonoids: Chemical properties and analytical methodologies of identification and quantitation in foods and plants. Nat. Prod. Res. 2011, 25, 469–495. [Google Scholar] [CrossRef] [PubMed]
- Amawi, H.; Ashby, C.R.; Tiwari, A.K. Cancer chemoprevention through dietary flavonoids: What’s limiting? Chin. J. Cancer 2017, 36, 50. [Google Scholar] [CrossRef] [PubMed]
- George, V.C.; Dellaire, G.; Rupasinghe, H.P.V. Plant flavonoids in cancer chemoprevention: Role in genome stability. J. Nutr. Biochem. 2017, 45, 1–14. [Google Scholar] [CrossRef]
- Farombi, E.O.; Shrotriya, S.; Surh, Y.-J. Kolaviron inhibits dimethyl nitrosamine-induced liver injury by suppressing COX-2 and iNOS expression via NF-κB and AP-1. Life Sci. 2009, 84, 149–155. [Google Scholar] [CrossRef]
- Olaleye, M.T.; Amobonye, A.E.; Komolafe, K.; Akinmoladun, A.C. Protective effects of Parinari curatellifolia flavonoids against acetaminophen-induced hepatic necrosis in rats. Saudi J. Biol. Sci. 2014, 21, 486–492. [Google Scholar] [CrossRef] [PubMed]
- Vázquez-Flores, L.F.; Casas-Grajales, S.; Hernández-Aquino, E.; Vargas-Pozada, E.E.; Muriel, P. Chapter 47—Antioxidant, Antiinflammatory, and Antifibrotic Properties of Quercetin in the Liver. In Liver Pathophysiology; Muriel, P., Ed.; Academic Press: Boston, MA, USA, 2017; pp. 653–674. [Google Scholar] [CrossRef]
- Bahrin, L.G.; Apostu, M.O.; Birsa, L.M.; Stefan, M. The antibacterial properties of sulfur containing flavonoids. Bioorganic Med. Chem. Lett. 2014, 24, 2315–2318. [Google Scholar] [CrossRef] [PubMed]
- Iranshahi, M.; Rezaee, R.; Parhiz, H.; Roohbakhsh, A.; Soltani, F. Protective effects of flavonoids against microbes and toxins: The cases of hesperidin and hesperetin. Life Sci. 2015, 137, 125–132. [Google Scholar] [CrossRef]
- Athira, K.V.; Madhana, R.M.; Lahkar, M. Flavonoids, the emerging dietary supplement against cisplatin-induced nephrotoxicity. Chem. -Biol. Interact. 2016, 248, 18–20. [Google Scholar] [CrossRef]
- Cai, H.-D.; Su, S.-L.; Qian, D.-W.; Guo, S.; Tao, W.-W.; Cong, X.D.; Tang, R.; Duan, J.-A. Renal protective effect and action mechanism of Huangkui capsule and its main five flavonoids. J. Ethnopharmacol. 2017, 206, 152–159. [Google Scholar] [CrossRef] [PubMed]
- Unnikrishnan, M.K.; Veerapur, V.; Nayak, Y.; Mudgal, P.P.; Mathew, G. Chapter 13—Antidiabetic, Antihyperlipidemic and Antioxidant Effects of the Flavonoids. In Polyphenols in Human Health and Disease; Watson, R.R., Preedy, V.R., Zibadi, S., Eds.; Academic Press: San Diego, CA, USA, 2014; pp. 143–161. [Google Scholar] [CrossRef]
- Keshari, A.K.; Kumar, G.; Kushwaha, P.S.; Bhardwaj, M.; Kumar, P.; Rawat, A.; Kumar, D.; Prakash, A.; Ghosh, B.; Saha, S. Isolated flavonoids from Ficus racemosa stem bark possess antidiabetic, hypolipidemic and protective effects in albino Wistar rats. J. Ethnopharmacol. 2016, 181, 252–262. [Google Scholar] [CrossRef] [PubMed]
- Olaleye, M.T.; Crown, O.O.; Akinmoladun, A.C.; Akindahunsi, A.A. Rutin and quercetin show greater efficacy than nifedipin in ameliorating hemodynamic, redox, and metabolite imbalances in sodium chloride-induced hypertensive rats. Hum. Exp. Toxicol. 2014, 33, 602–608. [Google Scholar] [CrossRef]
- Testai, L. Flavonoids and mitochondrial pharmacology: A new paradigm for cardioprotection. Life Sci. 2015, 135, 68–76. [Google Scholar] [CrossRef] [PubMed]
- Somasundaram, S.G.; Oommen, B. Chapter 1—Antioxidant Flavonoids for Arthritis Treatment: Human and Animal Models. In Bioactive Food as Dietary Interventions for Arthritis and Related Inflammatory Diseases; Watson, R.R., Preedy, V.R., Eds.; Academic Press: San Diego, CA, USA, 2013; pp. 1–16. [Google Scholar] [CrossRef]
- Choudhary, N.; Bijjem, K.R.V.; Kalia, A.N. Antiepileptic potential of flavonoids fraction from the leaves of Anisomeles malabarica. J. Ethnopharmacol. 2011, 135, 238–242. [Google Scholar] [CrossRef] [PubMed]
- Nabavi, S.F.; Braidy, N.; Habtemariam, S.; Orhan, I.E.; Daglia, M.; Manayi, A.; Gortzi, O.; Nabavi, S.M. Neuroprotective effects of chrysin: From chemistry to medicine. Neurochem. Int. 2015, 90, 224–231. [Google Scholar] [CrossRef]
- Falode, J.A.; Akinmoladun, A.C.; Olaleye, M.T.; Akindahunsi, A.A. Sausage tree (Kigelia africana) flavonoid extract is neuroprotective in AlCl(3)-induced experimental Alzheimer’s disease. Pathophysiology 2017, 24, 251–259. [Google Scholar] [CrossRef]
- Preethi Pallavi, M.C.; Sampath Kumar, H.M. Chapter 8—Nutraceuticals in Prophylaxis and Therapy of Neurodegenerative Diseases. In Discovery and Development of Neuroprotective Agents from Natural Products; Brahmachari, G., Ed.; Elsevier: Amsterdam, The Netherlands, 2018; pp. 359–376. [Google Scholar] [CrossRef]
- De Lira Mota, K.S.; Dias, G.E.N.; Pinto, M.E.F.; Luiz-Ferreira, Â.; Monteiro Souza-Brito, A.R.; Hiruma-Lima, C.A.; Barbosa-Filho, J.M.; Batista, L.M. Flavonoids with Gastroprotective Activity. Molecules 2009, 14, 979–1012. [Google Scholar] [CrossRef]
- Antonisamy, P.; Subash-Babu, P.; Albert-Baskar, A.; Alshatwi, A.A.; Aravinthan, A.; Ignacimuthu, S.; Choi, K.C.; Lee, S.C.; Kim, J.-H. Experimental study on gastroprotective efficacy and mechanisms of luteolin-7-O-glucoside isolated from Ophiorrhiza mungos Linn. in different experimental models. J. Funct. Foods 2016, 25, 302–313. [Google Scholar] [CrossRef]
- Nwankwo, J.O.; Tahnteng, J.G.; Emerole, G.O. Inhibition of aflatoxin B1 genotoxicity in human liver-derived HepG2 cells by kolaviron biflavonoids and molecular mechanisms of action. Eur. J. Cancer Prev. 2000, 9, 351–361. [Google Scholar] [CrossRef]
- Snijman, P.W.; Swanevelder, S.; Joubert, E.; Green, I.R.; Gelderblom, W.C.A. The antimutagenic activity of the major flavonoids of rooibos (Aspalathus linearis): Some dose–response effects on mutagen activation–flavonoid interactions. Mutat. Res. Genet. Toxicol. Environ. Mutagen. 2007, 631, 111–123. [Google Scholar] [CrossRef]
- Carvalho-Silva, L.B.D.; Dionísio, A.P.; Pereira, A.C.D.S.; Wurlitzer, N.J.; Brito, E.S.D.; Bataglion, G.A.; Brasil, I.M.; Eberlin, M.N.; Liu, R.H. Antiproliferative, antimutagenic and antioxidant activities of a Brazilian tropical fruit juice. LWT—Food Sci. Technol. 2014, 59, 1319–1324. [Google Scholar] [CrossRef]
- Serpeloni, J.M.; Leal Specian, A.F.; Ribeiro, D.L.; Tuttis, K.; Vilegas, W.; Martínez-López, W.; Dokkedal, A.L.; Saldanha, L.L.; de Syllos Cólus, I.M.; Varanda, E.A. Antimutagenicity and induction of antioxidant defense by flavonoid rich extract of Myrcia bella Cambess. in normal and tumor gastric cells. J. Ethnopharmacol. 2015, 176, 345–355. [Google Scholar] [CrossRef]
- Zarev, Y.; Foubert, K.; Lucia de Almeida, V.; Anthonissen, R.; Elgorashi, E.; Apers, S.; Ionkova, I.; Verschaeve, L.; Pieters, L. Antigenotoxic prenylated flavonoids from stem bark of Erythrina latissima. Phytochemistry 2017, 141, 140–146. [Google Scholar] [CrossRef]
- Neuhouser, M.L. Dietary flavonoids and cancer risk: Evidence from human population studies. Nutr. Cancer 2004, 50, 1–7. [Google Scholar] [CrossRef]
- Pei, J.; Chen, A.; Zhao, L.; Cao, F.; Ding, G.; Xiao, W. One-Pot Synthesis of Hyperoside by a Three-Enzyme Cascade Using a UDP-Galactose Regeneration System. J. Agric. Food Chem. 2017, 65, 6042–6048. [Google Scholar] [CrossRef]
- Weng, C.J.; Yen, G.C. Flavonoids, a ubiquitous dietary phenolic subclass, exert extensive in vitro anti-invasive and in vivo anti-metastatic activities. Cancer Metastasis Rev. 2012, 31, 323–351. [Google Scholar] [CrossRef] [PubMed]
- Zamora-Ros, R.; Sacerdote, C.; Ricceri, F.; Weiderpass, E.; Roswall, N.; Buckland, G.; St-Jules, D.E.; Overvad, K.; Kyrø, C.; Fagherazzi, G.; et al. Flavonoid and lignan intake in relation to bladder cancer risk in the European Prospective Investigation into Cancer and Nutrition (EPIC) study. Br. J. Cancer 2014, 111, 1870–1880. [Google Scholar] [CrossRef] [PubMed]
- Petrick, J.L.; Steck, S.E.; Bradshaw, P.T.; Trivers, K.F.; Abrahamson, P.E.; Engel, L.S.; He, K.; Chow, W.H.; Mayne, S.T.; Risch, H.A.; et al. Dietary intake of flavonoids and oesophageal and gastric cancer: Incidence and survival in the United States of America (USA). Br. J. Cancer 2015, 112, 1291–1300. [Google Scholar] [CrossRef] [PubMed]
- Alam, W.; Khan, H.; Shah, M.A.; Cauli, O.; Saso, L. Kaempferol as a Dietary Anti-Inflammatory Agent: Current Therapeutic Standing. Molecules 2020, 25, 4073. [Google Scholar] [CrossRef]
- Park, U.H.; Hwang, J.T.; Youn, H.; Kim, E.J.; Um, S.J. Kaempferol antagonizes adipogenesis by repressing histone H3K4 methylation at PPARγ target genes. Biochem. Biophys. Res. Commun. 2022, 617, 48–54. [Google Scholar] [CrossRef]
- Beltz, L.A.; Bayer, D.K.; Moss, A.L.; Simet, I.M. Mechanisms of cancer prevention by green and black tea polyphenols. Anticancer Agents Med. Chem. 2006, 6, 389–406. [Google Scholar] [CrossRef]
- Kumar, S.; Pandey, A.K. Chemistry and Biological Activities of Flavonoids: An Overview. Sci. World J. 2013, 2013, 162750. [Google Scholar] [CrossRef] [PubMed]
- Calderón-Montaño, J.M.; Burgos-Morón, E.; Pérez-Guerrero, C.; López-Lázaro, M. A review on the dietary flavonoid kaempferol. Mini Rev. Med. Chem. 2011, 11, 298–344. [Google Scholar] [CrossRef]
- Santos-Buelga, C.; Feliciano, A.S. Flavonoids: From Structure to Health Issues. Molecules 2017, 22, 477. [Google Scholar] [CrossRef] [PubMed]
- Mousdale, D.M.; Coggins, J.R. Subcellular localization of the common shikimate-pathway enzymes in Pisum sativum L. Planta 1985, 163, 241–249. [Google Scholar] [CrossRef] [PubMed]
- Jung, E.; Zamir, L.O.; Jensen, R.A. Chloroplasts of higher plants synthesize L-phenylalanine via L-arogenate. Proc. Natl. Acad. Sci. USA 1986, 83, 7231–7235. [Google Scholar] [CrossRef] [PubMed]
- Benesova, M.; Bode, R. Chorismate mutase isoforms from seeds and seedlings of Papaver somniferum. Phytochemistry 1992, 31, 2983–2987. [Google Scholar] [CrossRef]
- Xiao, J. Dietary flavonoid aglycones and their glycosides: Which show better biological significance? Crit. Rev. Food Sci. Nutr. 2017, 57, 1874–1905. [Google Scholar] [CrossRef] [PubMed]
- Santos, M.; Fortunato, R.H.; Spotorno, V.G. Analysis of flavonoid glycosides with potential medicinal properties on Bauhinia uruguayensis and Bauhinia forficata subspecies pruinosa. Nat. Prod. Res. 2019, 33, 2574–2578. [Google Scholar] [CrossRef]
- Rha, C.S.; Jeong, H.W.; Park, S.; Lee, S.; Jung, Y.S.; Kim, D.O. Antioxidative, Anti-Inflammatory, and Anticancer Effects of Purified Flavonol Glycosides and Aglycones in Green Tea. Antioxidants 2019, 8, 278. [Google Scholar] [CrossRef]
- Viskupicova, J.; Ondrejovič, M.; Sturdik, E. Bioavailability and metabolism of flavonoids. J. Food Nutr. Res. 2008, 47, 151–162. [Google Scholar]
- Bangar, S.P.; Chaudhary, V.; Sharma, N.; Bansal, V.; Ozogul, F.; Lorenzo, J.M. Kaempferol: A flavonoid with wider biological activities and its applications. Crit. Rev. Food Sci. Nutr. 2022, 1–25. [Google Scholar] [CrossRef]
- Williamson, G.; Kay, C.D.; Crozier, A. The Bioavailability, Transport, and Bioactivity of Dietary Flavonoids: A Review from a Historical Perspective. Compr. Rev. Food Sci. Food Saf. 2018, 17, 1054–1112. [Google Scholar] [CrossRef]
- Németh, K.; Plumb, G.W.; Berrin, J.G.; Juge, N.; Jacob, R.; Naim, H.Y.; Williamson, G.; Swallow, D.M.; Kroon, P.A. Deglycosylation by small intestinal epithelial cell beta-glucosidases is a critical step in the absorption and metabolism of dietary flavonoid glycosides in humans. Eur. J. Nutr. 2003, 42, 29–42. [Google Scholar] [CrossRef]
- Nielsen, S.E.; Kall, M.; Justesen, U.; Schou, A.; Dragsted, L.O. Human absorption and excretion of flavonoids after broccoli consumption. Cancer Lett. 1997, 114, 173–174. [Google Scholar] [CrossRef] [PubMed]
- Terao, J. Dietary flavonoids as antioxidants. Forum. Nutr. 2009, 61, 87–94. [Google Scholar] [CrossRef] [PubMed]
- Chen, A.Y.; Chen, Y.C. A review of the dietary flavonoid, kaempferol on human health and cancer chemoprevention. Food Chem. 2013, 138, 2099–2107. [Google Scholar] [CrossRef] [PubMed]
- de Vries, J.H.; Hollman, P.C.; Meyboom, S.; Buysman, M.N.; Zock, P.L.; van Staveren, W.A.; Katan, M.B. Plasma concentrations and urinary excretion of the antioxidant flavonols quercetin and kaempferol as biomarkers for dietary intake. Am. J. Clin. Nutr. 1998, 68, 60–65. [Google Scholar] [CrossRef]
- Cassidy, A.; Minihane, A.M. The role of metabolism (and the microbiome) in defining the clinical efficacy of dietary flavonoids. Am. J. Clin. Nutr. 2017, 105, 10–22. [Google Scholar] [CrossRef]
- Dabeek, W.M.; Marra, M.V. Dietary Quercetin and Kaempferol: Bioavailability and Potential Cardiovascular-Related Bioactivity in Humans. Nutrients 2019, 11, 2288. [Google Scholar] [CrossRef]
- Cavalier-Smith, T. A revised six-kingdom system of life. Biol. Rev. Camb. Philos. Soc. 1998, 73, 203–266. [Google Scholar] [CrossRef]
- Markham, K.R.; Geiger, H.; Jaggy, H. Kaempferol-3-O-glucosyl(1-2)rhamnoside from Ginkgo biloba and a reappraisal of other gluco(1-2, 1-3 and 1-4)rhamnoside structures. Phytochemistry 1992, 31, 1009–1011. [Google Scholar] [CrossRef]
- Tang, Y.; Lou, F.; Wang, J.; Li, Y.; Zhuang, S. Coumaroyl flavonol glycosides from the leaves of Ginkgo biloba. Phytochemistry 2001, 58, 1251–1256. [Google Scholar] [CrossRef]
- Zheng, W.; Wang, S.Y. Antioxidant Activity and Phenolic Compounds in Selected Herbs. J. Agric. Food Chem. 2001, 49, 5165–5170. [Google Scholar] [CrossRef]
- Lee, H.S.; Kim, M.J. Selective responses of three Ginkgo biloba leaf-derived constituents on human intestinal bacteria. J. Agric. Food Chem. 2002, 50, 1840–1844. [Google Scholar] [CrossRef] [PubMed]
- Krauze-Baranowska, M. Flavonoids from the genus Taxus. Z. Naturforsch C J. Biosci. 2004, 59, 43–47. [Google Scholar] [CrossRef] [PubMed]
- von Moltke, L.L.; Weemhoff, J.L.; Bedir, E.; Khan, I.A.; Harmatz, J.S.; Goldman, P.; Greenblatt, D.J. Inhibition of human cytochromes P450 by components of Ginkgo biloba. J. Pharm. Pharmacol. 2004, 56, 1039–1044. [Google Scholar] [CrossRef] [PubMed]
- Yoon, K.D.; Jeong, D.G.; Hwang, Y.H.; Ryu, J.M.; Kim, J. Inhibitors of Osteoclast Differentiation from Cephalotaxus koreana. J. Nat. Prod. 2007, 70, 2029–2032. [Google Scholar] [CrossRef] [PubMed]
- Kwon, S.H.; Nam, J.I.; Kim, S.H.; Kim, J.H.; Yoon, J.H.; Kim, K.S. Kaempferol and quercetin, essential ingredients in Ginkgo biloba extract, inhibit interleukin-1beta-induced MUC5AC gene expression in human airway epithelial cells. Phytother. Res. 2009, 23, 1708–1712. [Google Scholar] [CrossRef]
- Group, T.A.P.; Chase, M.W.; Christenhusz, M.J.M.; Fay, M.F.; Byng, J.W.; Judd, W.S.; Soltis, D.E.; Mabberley, D.J.; Sennikov, A.N.; Soltis, P.S.; et al. An update of the Angiosperm Phylogeny Group classification for the orders and families of flowering plants: APG IV. Bot. J. Linn. Soc. 2016, 181, 1–20. [Google Scholar] [CrossRef]
- I, P. A community-derived classification for extant lycophytes and ferns. J. Syst. Evol. 2016, 54, 563–603. [Google Scholar] [CrossRef]
- Christenhusz, M.; Reveal, J.; Farjon, A.; Gardner, M.; Mill, R.; Chase, M. A new classification and linear sequence of extant gymnosperms. Nov. Magnolia Press Phytotaxa 2010, 19, 55–70. [Google Scholar] [CrossRef]
- Arot Manguro, L.O.; Ugi, I.; Hermann, R.; Lemmen, P. Flavonol and drimane-type sesquiterpene glycosides of Warburgia stuhlmannii leaves. Phytochemistry 2003, 63, 497–502. [Google Scholar] [CrossRef]
- Calzada, F.; Correa-Basurto, J.; Barbosa, E.; Mendez-Luna, D.; Yepez-Mulia, L. Antiprotozoal Constituents from Annona cherimola Miller, a Plant Used in Mexican Traditional Medicine for the Treatment of Diarrhea and Dysentery. Pharmacogn. Mag. 2017, 13, 148–152. [Google Scholar] [CrossRef]
- Rodríguez Galdón, B.; Rodríguez Rodríguez, E.M.; Díaz Romero, C. Flavonoids in onion cultivars (Allium cepa L.). J. Food Sci. 2008, 73, C599–C605. [Google Scholar] [CrossRef] [PubMed]
- Keyhanian, S.; Stahl-Biskup, E. Phenolic constituents in dried flowers of aloe vera (Aloe barbadensis) and their in vitro antioxidative capacity. Planta Med. 2007, 73, 599–602. [Google Scholar] [CrossRef] [PubMed]
- Vachálková, A.; Eisenreichová, E.; Haladová, M.; Mucaji, P.; Józová, B.; Novotný, L. Potential carcinogenic and inhibitory activity of compounds isolated from Lilium candidum L. Neoplasma 2000, 47, 313–318. [Google Scholar] [PubMed]
- Francis, J.A.; Rumbeiha, W.; Nair, M.G. Constituents in Easter lily flowers with medicinal activity. Life Sci. 2004, 76, 671–683. [Google Scholar] [CrossRef]
- Xu, J.; Li, X.; Zhang, P.; Li, Z.L.; Wang, Y. Antiinflammatory constituents from the roots of Smilax bockii warb. Arch. Pharmacal Res. 2005, 28, 395–399. [Google Scholar] [CrossRef]
- Jiang, R.-W.; Zhou, J.-R.; Hon, P.-M.; Li, S.-L.; Zhou, Y.; Li, L.-L.; Ye, W.-C.; Xu, H.-X.; Shaw, P.-C.; But, P.P.-H. Lignans from Dysosma versipellis with Inhibitory Effects on Prostate Cancer Cell Lines. J. Nat. Prod. 2007, 70, 283–286. [Google Scholar] [CrossRef]
- Marín, C.; Boutaleb-Charki, S.; Díaz, J.G.; Huertas, O.; Rosales, M.J.; Pérez-Cordon, G.; Guitierrez-Sánchez, R.; Sánchez-Moreno, M. Antileishmaniasis activity of flavonoids from Consolida oliveriana. J. Nat. Prod. 2009, 72, 1069–1074. [Google Scholar] [CrossRef]
- Je Ma, C.; Jung, W.J.; Lee, K.Y.; Kim, Y.C.; Sung, S.H. Calpain inhibitory flavonoids isolated from Orostachys japonicus. J. Enzym. Inhib. Med. Chem. 2009, 24, 676–679. [Google Scholar] [CrossRef]
- Jeong, H.J.; Ryu, Y.B.; Park, S.J.; Kim, J.H.; Kwon, H.J.; Kim, J.H.; Park, K.H.; Rho, M.C.; Lee, W.S. Neuraminidase inhibitory activities of flavonols isolated from Rhodiola rosea roots and their in vitro anti-influenza viral activities. Bioorganic Med. Chem. 2009, 17, 6816–6823. [Google Scholar] [CrossRef]
- Song, E.K.; Kim, J.H.; Kim, J.S.; Cho, H.; Nan, J.X.; Sohn, D.H.; Ko, G.I.; Oh, H.; Kim, Y.C. Hepatoprotective phenolic constituents of Rhodiola sachalinensis on tacrine-induced cytotoxicity in Hep G2 cells. Phytother. Res. 2003, 17, 563–565. [Google Scholar] [CrossRef]
- Richwagen, N.; Lyles, J.T.; Dale, B.L.F.; Quave, C.L. Antibacterial Activity of Kalanchoe mortagei and K. fedtschenkoi Against ESKAPE Pathogens. Front. Pharmacol. 2019, 10, 67. [Google Scholar] [CrossRef] [PubMed]
- Saleem, M.; Kim, H.J.; Jin, C.; Lee, Y.S. Antioxidant caffeic acid derivatives from leaves of Parthenocissus tricuspidata. Arch. Pharmacal Res. 2004, 27, 300–304. [Google Scholar] [CrossRef] [PubMed]
- Kumar, D.; Kumar, S.; Gupta, J.; Arya, R.; Gupta, A. A review on chemical and biological properties of Cayratia trifolia Linn. (Vitaceae). Pharmacogn. Rev. 2011, 5, 184–188. [Google Scholar] [CrossRef] [PubMed]
- Yin, F.; Zhang, Y.; Yang, Z.; Cheng, Q.; Hu, L. Triterpene saponins from Gynostemma cardiospermum. J. Nat. Prod. 2006, 69, 1394–1398. [Google Scholar] [CrossRef] [PubMed]
- Ghaffari, M.A.; Chaudhry, B.A.; Uzair, M.; Imran, M.; Haneef, M.; Ashfaq, K. Biological and phytochemical investigations of crude extracts of Astragalus creticus. Pak. J. Pharm. Sci. 2021, 34, 403–409. [Google Scholar] [PubMed]
- Mazimba, O.; Majinda, R.R.; Modibedi, C.; Masesane, I.B.; Cencič, A.; Chingwaru, W. Tylosema esculentum extractives and their bioactivity. Bioorganic Med. Chem. 2011, 19, 5225–5230. [Google Scholar] [CrossRef]
- Nguyen, T.T.; Ketha, A.; Hieu, H.V.; Tatipamula, V.B. In vitro antimycobacterial studies of flavonols from Bauhinia vahlii Wight and Arn. 3 Biotech 2021, 11, 128. [Google Scholar] [CrossRef]
- Singh, R.; Singh, B.; Singh, S.; Kumar, N.; Kumar, S.; Arora, S. Anti-free radical activities of kaempferol isolated from Acacia nilotica (L.) Willd. Ex. Del. Toxicol. Vitr. 2008, 22, 1965–1970. [Google Scholar] [CrossRef]
- Costa-Lotufo, L.V.; Jimenez, P.C.; Wilke, D.V.; Leal, L.K.; Cunha, G.M.; Silveira, E.R.; Canuto, K.M.; Viana, G.S.; Moraes, M.E.; de Moraes, M.O.; et al. Antiproliferative effects of several compounds isolated from Amburana cearensis A. C. Smith. Z. Naturforsch C J. Biosci. 2003, 58, 675–680. [Google Scholar] [CrossRef]
- Terreaux, C.; Wang, Q.; Ioset, J.R.; Ndjoko, K.; Grimminger, W.; Hostettmann, K. Complete LC/MS analysis of a Tinnevelli senna pod extract and subsequent isolation and identification of two new benzophenone glucosides. Planta Med. 2002, 68, 349–354. [Google Scholar] [CrossRef]
- Nsonde Ntandou, G.F.; Banzouzi, J.T.; Mbatchi, B.; Elion-Itou, R.D.; Etou-Ossibi, A.W.; Ramos, S.; Benoit-Vical, F.; Abena, A.A.; Ouamba, J.M. Analgesic and anti-inflammatory effects of Cassia siamea Lam. stem bark extracts. J. Ethnopharmacol. 2010, 127, 108–111. [Google Scholar] [CrossRef] [PubMed]
- Calvo, T.R.; Cardoso, C.R.P.; da Silva Moura, A.C.; dos Santos, L.C.; Colus, I.M.S.; Vilegas, W.; Varanda, E.A. Mutagenic Activity of Indigofera truxillensis and I. suffruticosa Aerial Parts. Evid. -Based Complement. Altern. Med. 2011, 2011, 323276. [Google Scholar] [CrossRef] [PubMed]
- Jiang, H.; Zhan, W.Q.; Liu, X.; Jiang, S.X. Antioxidant activities of extracts and flavonoid compounds from Oxytropis falcate Bunge. Nat. Prod. Res. 2008, 22, 1650–1656. [Google Scholar] [CrossRef]
- Ali, A.A.; Mohamed, M.H.; Kamel, M.S.; Fouad, M.A.; Spring, O. Studies on Securigera securidacea (L.) Deg. et Dörfl. (Fabaceae) seeds, an antidiabetic Egyptian folk medicine. Pharmazie 1998, 53, 710–715. [Google Scholar]
- Xiang, W.; Li, R.T.; Mao, Y.L.; Zhang, H.J.; Li, S.H.; Song, Q.S.; Sun, H.D. Four new prenylated isoflavonoids in Tadehagi triquetrum. J. Agric. Food Chem. 2005, 53, 267–271. [Google Scholar] [CrossRef] [PubMed]
- Sharaf, M. Chemical constituents from the seeds of Trifolium alexandrinum. Nat. Prod. Res. 2008, 22, 1620–1623. [Google Scholar] [CrossRef] [PubMed]
- Sharma, U.K.; Sharma, K.; Sharma, N.; Sharma, A.; Singh, H.P.; Sinha, A.K. Microwave-assisted efficient extraction of different parts of Hippophae rhamnoides for the comparative evaluation of antioxidant activity and quantification of its phenolic constituents by reverse-phase high-performance liquid chromatography (RP-HPLC). J. Agric. Food Chem. 2008, 56, 374–379. [Google Scholar] [CrossRef]
- Wei, B.L.; Lu, C.M.; Tsao, L.T.; Wang, J.P.; Lin, C.N. In vitro anti-inflammatory effects of quercetin 3-O-methyl ether and other constituents from Rhamnus species. Planta Med. 2001, 67, 745–747. [Google Scholar] [CrossRef]
- Goel, R.K.; Pandey, V.B.; Dwivedi, S.P.; Rao, Y.V. Antiinflammatory and antiulcer effects of kaempferol, a flavone, isolated from Rhamnus procumbens. Indian J. Exp. Biol. 1988, 26, 121–124. [Google Scholar]
- Jung, H.A.; Jung, M.J.; Kim, J.Y.; Chung, H.Y.; Choi, J.S. Inhibitory activity of flavonoids from Prunus davidiana and other flavonoids on total ROS and hydroxyl radical generation. Arch. Pharmacal Res. 2003, 26, 809–815. [Google Scholar] [CrossRef]
- Nowak, R.; Gawlik-Dziki, U. Polyphenols of Rosa L. leaves extracts and their radical scavenging activity. Z. Naturforsch C J. Biosci. 2007, 62, 32–38. [Google Scholar] [CrossRef] [PubMed]
- Mahmood, N.; Piacente, S.; Pizza, C.; Burke, A.; Khan, A.I.; Hay, A.J. The anti-HIV activity and mechanisms of action of pure compounds isolated from Rosa damascena. Biochem. Biophys. Res. Commun. 1996, 229, 73–79. [Google Scholar] [CrossRef] [PubMed]
- Suntornsuk, L.; Anurukvorakun, O. Precision improvement for the analysis of flavonoids in selected Thai plants by capillary zone electrophoresis. Electrophoresis 2005, 26, 648–660. [Google Scholar] [CrossRef] [PubMed]
- Niklas, K.J.; Giannasi, D.E. Flavonoids and other chemical constituents of fossil miocene zelkova (ulmaceae). Science 1977, 196, 877–878. [Google Scholar] [CrossRef]
- Fang, X.K.; Gao, J.; Zhu, D.N. Kaempferol and quercetin isolated from Euonymus alatus improve glucose uptake of 3T3-L1 cells without adipogenesis activity. Life Sci. 2008, 82, 615–622. [Google Scholar] [CrossRef]
- Rocha, L.; Marston, A.; Potterat, O.; Kaplan, M.A.C.; Stoeckli-Evans, H.; Hostettmann, K. Antibacterial phloroglucinols and flavonoids from Hypericum brasiliense. Phytochemistry 1995, 40, 1447–1452. [Google Scholar] [CrossRef]
- Odabas, M.S.; Camas, N.; Cirak, C.; Radusiene, J.; Janulis, V.; Ivanauskas, L. The quantitative effects of temperature and light intensity on phenolics accumulation in St. John’s wort (Hypericum perforatum). Nat. Prod. Commun. 2010, 5, 535–540. [Google Scholar] [CrossRef]
- Nguemeving, J.R.; Azebaze, A.G.B.; Kuete, V.; Eric Carly, N.N.; Beng, V.P.; Meyer, M.; Blond, A.; Bodo, B.; Nkengfack, A.E. Laurentixanthones A and B, antimicrobial xanthones from Vismia laurentii. Phytochemistry 2006, 67, 1341–1346. [Google Scholar] [CrossRef]
- Pattamadilok, D.; Suttisri, R. Seco-Terpenoids and Other Constituents from Elateriospermum tapos. J. Nat. Prod. 2008, 71, 292–294. [Google Scholar] [CrossRef]
- Oksüz, S.; Gürek, F.; Lin, L.Z.; Gil, R.R.; Pezzuto, J.M.; Cordell, G.A. Aleppicatines A and B from Euphorbia aleppica. Phytochemistry 1996, 42, 473–478. [Google Scholar] [CrossRef]
- Sousa, M.; Ousingsawat, J.; Seitz, R.; Puntheeranurak, S.; Regalado, A.; Schmidt, A.; Grego, T.; Jansakul, C.; Amaral, M.D.; Schreiber, R.; et al. An extract from the medicinal plant Phyllanthus acidus and its isolated compounds induce airway chloride secretion: A potential treatment for cystic fibrosis. Mol. Pharmacol. 2007, 71, 366–376. [Google Scholar] [CrossRef] [PubMed]
- Yang, R.Y.; Lin, S.; Kuo, G. Content and distribution of flavonoids among 91 edible plant species. Asia Pac. J. Clin. Nutr. 2008, 17 (Suppl. 1), 275–279. [Google Scholar] [PubMed]
- Penna, C.; Marino, S.; Vivot, E.; Cruañes, M.C.; Muñoz, J.D.D.; Cruañes, J.; Ferraro, G.; Gutkind, G.; Martino, V. Antimicrobial activity of Argentine plants used in the treatment of infectious diseases. Isolation of active compounds from Sebastiania brasiliensis. J. Ethnopharmacol. 2001, 77, 37–40. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Hung, T.M.; Phuong, P.T.; Ngoc, T.M.; Min, B.S.; Song, K.S.; Seong, Y.H.; Bae, K. Anti-inflammatory activity of flavonoids from Populus davidiana. Arch. Pharmacal Res. 2006, 29, 1102–1108. [Google Scholar] [CrossRef]
- Li, J.; Huang, H.; Zhou, W.; Feng, M.; Zhou, P. Anti-hepatitis B virus activities of Geranium carolinianum L. extracts and identification of the active components. Biol. Pharm. Bull. 2008, 31, 743–747. [Google Scholar] [CrossRef]
- Gayosso-De-Lucio, J.A.; Torres-Valencia, J.M.; Cerda-García-Rojas, C.M.; Joseph-Nathan, P. Ellagitannins from Geranium potentillaefolium and G. bellum. Nat. Prod. Commun. 2010, 5, 1934578X1000500407. [Google Scholar] [CrossRef]
- Şeker, M.E.; Ay, E.; Aktaş Karaçelik, A.; Hüseyinoǧlu, R.; Efe, D. First determination of some phenolic compounds and antimicrobial activities of Geranium ibericum subsp. jubatum: A plant endemic to Turkey. Turk. J. Chem. 2021, 45, 60–70. [Google Scholar] [CrossRef]
- Williams, C.A.; Harborne, J.B.; Newman, M.; Greenham, J.; Eagles, J. Chrysin and other leaf exudate flavonoids in the genus Pelargonium. Phytochemistry 1997, 46, 1349–1353. [Google Scholar] [CrossRef]
- Rochfort, S.J.; Imsic, M.; Jones, R.; Trenerry, V.C.; Tomkins, B. Characterization of flavonol conjugates in immature leaves of pak choi [Brassica rapa L. Ssp. chinensis L. (Hanelt.)] by HPLC-DAD and LC-MS/MS. J. Agric. Food Chem. 2006, 54, 4855–4860. [Google Scholar] [CrossRef]
- Bennett, R.N.; Rosa, E.A.; Mellon, F.A.; Kroon, P.A. Ontogenic profiling of glucosinolates, flavonoids, and other secondary metabolites in Eruca sativa (salad rocket), Diplotaxis erucoides (wall rocket), Diplotaxis tenuifolia (wild rocket), and Bunias orientalis (Turkish rocket). J. Agric. Food Chem. 2006, 54, 4005–4015. [Google Scholar] [CrossRef]
- Calzada, F.; Lopéz, R.; Meckes, M.; Cedillo-Rivera, R. Flavonoids of the Aerial Parts of Helianthemum Glomeratum. Int. J. Pharmacogn. 1995, 33, 351–352. [Google Scholar] [CrossRef]
- Papiez, M.; Gancarczyk, M.; Bilińska, B. The compounds from the hollyhock extract (Althaea rosea Cav. var. nigra) affect the aromatization in rat testicular cells in vivo and in vitro. Folia Histochem. Et Cytobiol. 2002, 40, 353–359. [Google Scholar]
- Yang, H.; Protiva, P.; Cui, B.; Ma, C.; Baggett, S.; Hequet, V.; Mori, S.; Weinstein, I.B.; Kennelly, E.J. New Bioactive Polyphenols from Theobroma g randiflorum (“Cupuaçu”). J. Nat. Prod. 2003, 66, 1501–1504. [Google Scholar] [CrossRef] [PubMed]
- Viola, H.; Wolfman, C.; Levi de Stein, M.; Wasowski, C.; Peña, C.; Medina, J.H.; Paladini, A.C. Isolation of pharmacologically active benzodiazepine receptor ligands from Tilia tomentosa (Tiliaceae). J. Ethnopharmacol. 1994, 44, 47–53. [Google Scholar] [CrossRef]
- Martini, N.D.; Katerere, D.R.; Eloff, J.N. Biological activity of five antibacterial flavonoids from Combretum erythrophyllum (Combretaceae). J. Ethnopharmacol. 2004, 93, 207–212. [Google Scholar] [CrossRef]
- Calzada, F. Additional antiprotozoal constituents from Cuphea pinetorum, a plant used in Mayan traditional medicine to treat diarrhoea. Phytother. Res. 2005, 19, 725–727. [Google Scholar] [CrossRef]
- Amakura, Y.; Yoshimura, M.; Sugimoto, N.; Yamazaki, T.; Yoshida, T. Marker Constituents of the Natural Antioxidant Eucalyptus Leaf Extract for the Evaluation of Food Additives. Biosci. Biotechnol. Biochem. 2009, 73, 1060–1065. [Google Scholar] [CrossRef]
- Chen, K.C.; Chuang, C.M.; Lin, L.Y.; Chiu, W.T.; Wang, H.E.; Hsieh, C.L.; Tsai, T.; Peng, R.Y. The polyphenolics in the aqueous extract of Psidium guajava kinetically reveal an inhibition model on LDL glycation. Pharm. Biol. 2010, 48, 23–31. [Google Scholar] [CrossRef][Green Version]
- Cai, L.; Wu, C.D. Compounds from Syzygium aromaticum possessing growth inhibitory activity against oral pathogens. J. Nat. Prod. 1996, 59, 987–990. [Google Scholar] [CrossRef]
- van Elswijk, D.A.; Schobel, U.P.; Lansky, E.P.; Irth, H.; van der Greef, J. Rapid dereplication of estrogenic compounds in pomegranate (Punica granatum) using on-line biochemical detection coupled to mass spectrometry. Phytochemistry 2004, 65, 233–241. [Google Scholar] [CrossRef]
- Tomaino, A.; Martorana, M.; Arcoraci, T.; Monteleone, D.; Giovinazzo, C.; Saija, A. Antioxidant activity and phenolic profile of pistachio (Pistacia vera L., variety Bronte) seeds and skins. Biochimie 2010, 92, 1115–1122. [Google Scholar] [CrossRef] [PubMed]
- Jung, C.H.; Kim, J.H.; Hong, M.H.; Seog, H.M.; Oh, S.H.; Lee, P.J.; Kim, G.J.; Kim, H.M.; Um, J.Y.; Ko, S.-G. Phenolic-rich fraction from Rhus verniciflua Stokes (RVS) suppress inflammatory response via NF-κB and JNK pathway in lipopolysaccharide-induced RAW 264.7 macrophages. J. Ethnopharmacol. 2007, 110, 490–497. [Google Scholar] [CrossRef] [PubMed]
- Abou-Shoer, M.; Ma, G.E.; Li, X.H.; Koonchanok, N.M.; Geahlen, R.L.; Chang, C.J. Flavonoids from Koelreuteria henryi and other sources as protein-tyrosine kinase inhibitors. J. Nat. Prod. 1993, 56, 967–969. [Google Scholar] [CrossRef] [PubMed]
- Lin, W.H.; Deng, Z.W.; Lei, H.M.; Fu, H.Z.; Li, J. Polyphenolic compounds from the leaves of Koelreuteria paniculata Laxm. J. Asian Nat. Prod. Res. 2002, 4, 287–295. [Google Scholar] [CrossRef]
- Arriaga, A.C.; de Mesquita, A.C.; Pouliquen, Y.B.; de Lima, R.A.; Cavalcante, S.H.; de Carvalho, M.G.; de Siqueira, J.A.; Alegrio, L.V.; Braz-Filho, R. Chemical constituents of Simarouba versicolor. An. Da Acad. Bras. De Ciências 2002, 74, 415–424. [Google Scholar] [CrossRef]
- Salvador, M.J.; Ferreira, E.O.; Mertens-Talcott, S.U.; De Castro, W.V.; Butterweck, V.; Derendorf, H.; Dias, D.A. Isolation and HPLC quantitative analysis of antioxidant flavonoids from Alternanthera tenella Colla. Z. Für Nat. C 2006, 61, 19–25. [Google Scholar] [CrossRef]
- Aung, H.H.; Chia, L.S.; Goh, N.K.; Chia, T.F.; Ahmed, A.A.; Pare, P.W.; Mabry, T.J. Phenolic constituents from the leaves of the carnivorous plant Nepenthes gracilis. Fitoterapia 2002, 73, 445–447. [Google Scholar] [CrossRef]
- Kataoka, M.; Hirata, K.; Kunikata, T.; Ushio, S.; Iwaki, K.; Ohashi, K.; Ikeda, M.; Kurimoto, M. Antibacterial action of tryptanthrin and kaempferol, isolated from the indigo plant (Polygonum tinctorium Lour.), against Helicobacter pylori-infected Mongolian gerbils. J. Gastroenterol. 2001, 36, 5–9. [Google Scholar] [CrossRef]
- Parveen, Z.; Deng, Y.; Saeed, M.K.; Dai, R.; Ahamad, W.; Yu, Y.H. Antiinflammatory and analgesic activities of Thesium chinense Turcz extracts and its major flavonoids, kaempferol and kaempferol-3-O-glucoside. Yakugaku Zasshi. J. Pharm. Soc. Jpn. 2007, 127, 1275–1279. [Google Scholar] [CrossRef]
- Loizzo, M.R.; Said, A.; Tundis, R.; Hawas, U.W.; Rashed, K.; Menichini, F.; Frega, N.G.; Menichini, F. Antioxidant and antiproliferative activity of Diospyros lotus L. extract and isolated compounds. Plant Foods Hum. Nutr. 2009, 64, 264–270. [Google Scholar] [CrossRef]
- Crublet, M.-L.; Long, C.; Sévenet, T.; Hadi, H.A.; Lavaud, C. Acylated flavonol glycosides from leaves of Planchonia grandis. Phytochemistry 2003, 64, 589–594. [Google Scholar] [CrossRef]
- Sumino, M.; Sekine, T.; Ruangrungsi, N.; Igarashi, K.; Ikegami, F. Ardisiphenols and other antioxidant principles from the fruits of Ardisia colorata. Chem. Pharm. Bull. 2002, 50, 1484–1487. [Google Scholar] [CrossRef] [PubMed]
- Chien, M.M.; Svoboda, G.H.; Schiff, P.L., Jr.; Slatkin, D.J.; Knapp, J.E. Chemical constituents of Echites hirsuta (Apocynaceae). J. Pharm. Sci. 1979, 68, 247–249. [Google Scholar] [CrossRef] [PubMed]
- Deng, S.; Palu, K.; West, B.J.; Su, C.X.; Zhou, B.N.; Jensen, J.C. Lipoxygenase inhibitory constituents of the fruits of noni (Morinda citrifolia) collected in Tahiti. J. Nat. Prod. 2007, 70, 859–862. [Google Scholar] [CrossRef]
- Cimanga, R.K.; Kambu, K.; Tona, L.; Hermans, N.; Apers, S.; Totté, J.; Pieters, L.; Vlietinck, A.J. Cytotoxicity and in vitro susceptibility of Entamoeba histolytica to Morinda morindoides leaf extracts and its isolated constituents. J. Ethnopharmacol. 2006, 107, 83–90. [Google Scholar] [CrossRef] [PubMed]
- Majinda, R.R.; Motswaledi, M.; Waigh, R.D.; Waterman, P.G. Phenolic and antibacterial constituents of Vahlia capensis. Planta Med. 1997, 63, 268–270. [Google Scholar] [CrossRef]
- Ye, M.; Yan, Y.; Guo, D.A. Characterization of phenolic compounds in the Chinese herbal drug Tu-Si-Zi by liquid chromatography coupled to electrospray ionization mass spectrometry. Rapid Commun. Mass Spectrom. 2005, 19, 1469–1484. [Google Scholar] [CrossRef]
- Umehara, K.; Nemoto, K.; Ohkubo, T.; Miyase, T.; Degawa, M.; Noguchi, H. Isolation of a new 15-membered macrocyclic glycolipid lactone, Cuscutic Resinoside a from the seeds of Cuscuta chinensis: A stimulator of breast cancer cell proliferation. Planta Med. 2004, 70, 299–304. [Google Scholar] [CrossRef]
- Huang, H.-C.; Syu, K.-Y.; Lin, J.-K. Chemical Composition of Solanum nigrum Linn Extract and Induction of Autophagy by Leaf Water Extract and Its Major Flavonoids in AU565 Breast Cancer Cells. J. Agric. Food Chem. 2010, 58, 8699–8708. [Google Scholar] [CrossRef]
- Kwak, J.H.; Kang, M.W.; Roh, J.H.; Choi, S.U.; Zee, O.P. Cytotoxic phenolic compounds from Chionanthus retusus. Arch. Pharmacal Res. 2009, 32, 1681–1687. [Google Scholar] [CrossRef]
- de Laurentis, N.; Stefanizzi, L.; Milillo, M.A.; Tantillo, G. Flavonoids from leaves of Olea europaea L. cultivars. Ann. Pharm. Françaises 1998, 56, 268–273. [Google Scholar]
- Youssef, F.S.; Altyar, A.E.; Omar, A.M.; Ashour, M.L. Phytoconstituents, In Vitro Anti-Infective Activity of Buddleja indica Lam., and In Silico Evaluation of its SARS-CoV-2 Inhibitory Potential. Front. Pharmacol. 2021, 12, 619373. [Google Scholar] [CrossRef] [PubMed]
- Chatzopoulou, A.; Karioti, A.; Gousiadou, C.; Lax Vivancos, V.; Kyriazopoulos, P.; Golegou, S.; Skaltsa, H. Depsides and Other Polar Constituents from Origanum dictamnus L. and Their in Vitro Antimicrobial Activity in Clinical Strains. J. Agric. Food Chem. 2010, 58, 6064–6068. [Google Scholar] [CrossRef] [PubMed]
- Bai, N.; He, K.; Roller, M.; Lai, C.S.; Shao, X.; Pan, M.H.; Ho, C.T. Flavonoids and phenolic compounds from Rosmarinus officinalis. J. Agric. Food Chem. 2010, 58, 5363–5367. [Google Scholar] [CrossRef] [PubMed]
- Sharififar, F.; Yassa, N.; Mozaffarian, V. Bioactivity of major components from the seeds of Bunium persicum (Boiss.) Fedtch. Pak. J. Pharm. Sci. 2010, 23, 300–304. [Google Scholar] [PubMed]
- Pistelli, L.; Noccioli, C.; Giachi, I.; Dimitrova, B.; Gevrenova, R.; Morelli, I.; Potenza, D. Lupane-triterpenes from Bupleurum flavum. Nat. Prod. Res. 2005, 19, 783–788. [Google Scholar] [CrossRef]
- Guo, S.; Guo, R.; Xia, Y.; Dong, T.; Wang, H.; Zhan, H. Quantitative analysis of fermented aerial part of Bupleurum chinense and prediction of their antimicrobial activity. Zhongguo Zhong Yao Za Zhi 2020, 45, 4238–4245. [Google Scholar] [CrossRef]
- Haraguchi, H.; Ishikawa, H.; Sanchez, Y.; Ogura, T.; Kubo, Y.; Kubo, I. Antioxidative constituents in Heterotheca inuloides. Bioorganic Med. Chem. 1997, 5, 865–871. [Google Scholar] [CrossRef]
- Hidalgo Báez, D.; de los Ríos, C.; Crescente, O.; Caserta, A. Antibacterial and chemical evaluation of Chromolaena moritziana. J. Ethnopharmacol. 1998, 59, 203–206. [Google Scholar] [CrossRef]
- Zhang, Y.; Zhao, L.; Shi, Y.-P. Separation and Determination of Flavonoids in Ixeridium gracile by Capillary Electrophoresis. J. Chromatogr. Sci. 2007, 45, 600–604. [Google Scholar] [CrossRef]
- Kim, D.K. Antioxidative components from the aerial parts of Lactuca scariola L. Arch. Pharmacal Res. 2001, 24, 427–430. [Google Scholar] [CrossRef] [PubMed]
- Choi, S.Z.; Choi, S.U.; Lee, K.R. Phytochemical constituents of the aerial parts from Solidago virga-aurea var. gigantea. Arch. Pharmacal Res. 2004, 27, 164–168. [Google Scholar] [CrossRef] [PubMed]
- Süzgeç, S.; Meriçli, A.H.; Houghton, P.J.; Cubukçu, B. Flavonoids of Helichrysum compactum and their antioxidant and antibacterial activity. Fitoterapia 2005, 76, 269–272. [Google Scholar] [CrossRef] [PubMed]
- Maas, M.; Hensel, A.; Costa, F.B.; Brun, R.; Kaiser, M.; Schmidt, T.J. An unusual dimeric guaianolide with antiprotozoal activity and further sesquiterpene lactones from Eupatoriumperfoliatum. Phytochemistry 2011, 72, 635–644. [Google Scholar] [CrossRef]
- Prasasty, V.D.; Cindana, S.; Ivan, F.X.; Zahroh, H.; Sinaga, E. Structure-based discovery of novel inhibitors of Mycobacterium tuberculosis CYP121 from Indonesian natural products. Comput. Biol. Chem. 2020, 85, 107205. [Google Scholar] [CrossRef]
- Schmitzer, V.; Veberic, R.; Slatnar, A.; Stampar, F. Elderberry (Sambucus nigra L.) wine: A product rich in health promoting compounds. J. Agric. Food Chem. 2010, 58, 10143–10146. [Google Scholar] [CrossRef]
- Li, M.M.; Wang, K.; Pan, Z.H.; Chen, X.Q.; Peng, L.Y.; Li, Y.; Cheng, X.; Zhao, Q.S. Two new sesquiterpene glucosides from Dennstaedtia scabra (Wall.) Moore. Chem. Pharm. Bull. 2009, 57, 1123–1125. [Google Scholar] [CrossRef]
- Lin, Y.L.; Shen, C.C.; Huang, Y.J.; Chang, Y.Y. Homoflavonoids from Ophioglossum petiolatum. J. Nat. Prod. 2005, 68, 381–384. [Google Scholar] [CrossRef]
- Bhagwat, S.; Haytowitz, D.B.; Holden, J.M. USDA Database for the Flavonoid Content of Selected Foods; Beltsville Human Nutrition Research Center, Agricultural Research Service: Beltsville, MD, USA, 2011. [Google Scholar]
- Fieschi, M.; Codignola, A.; Luppi Mosca, A.M. Mutagenic Flavonol Aglycones in Infusions and in Fresh and Pickled Vegetables. J. Food Sci. 1989, 54, 1492–1495. [Google Scholar] [CrossRef]
- Miean, K.H.; Mohamed, S. Flavonoid (myricetin, quercetin, kaempferol, luteolin, and apigenin) content of edible tropical plants. J. Agric. Food Chem. 2001, 49, 3106–3112. [Google Scholar] [CrossRef]
- Herrmann, K. Flavonols and flavones in food plants: A review†. Int. J. Food Sci. Technol. 1976, 11, 433–448. [Google Scholar] [CrossRef]
- Häkkinen, S.H.; Kärenlampi, S.O.; Heinonen, I.M.; Mykkänen, H.M.; Törrönen, A.R. Content of the flavonols quercetin, myricetin, and kaempferol in 25 edible berries. J. Agric. Food Chem. 1999, 47, 2274–2279. [Google Scholar] [CrossRef] [PubMed]
- Wallace, R.J. Antimicrobial properties of plant secondary metabolites. Proc. Nutr. Soc. 2004, 63, 621–629. [Google Scholar] [CrossRef] [PubMed]
- Kaspar, F.; Neubauer, P.; Gimpel, M. Bioactive Secondary Metabolites from Bacillus subtilis: A Comprehensive Review. J. Nat. Prod. 2019, 82, 2038–2053. [Google Scholar] [CrossRef]
- Salehi, B.; Zakaria, Z.A.; Gyawali, R.; Ibrahim, S.A.; Rajkovic, J.; Shinwari, Z.K.; Khan, T.; Sharifi-Rad, J.; Ozleyen, A.; Turkdonmez, E.; et al. Piper Species: A Comprehensive Review on Their Phytochemistry, Biological Activities and Applications. Molecules 2019, 24, 1364. [Google Scholar] [CrossRef]
- Makuwa, S.C.; Serepa-Dlamini, M.H. The Antibacterial Activity of Crude Extracts of Secondary Metabolites from Bacterial Endophytes Associated with Dicoma anomala. Int. J. Microbiol. 2021, 2021, 8812043. [Google Scholar] [CrossRef]
- Aminah, N.S.; Laili, E.R.; Rafi, M.; Rochman, A.; Insanu, M.; Tun, K.N.W. Secondary metabolite compounds from Sida genus and their bioactivity. Heliyon 2021, 7, e06682. [Google Scholar] [CrossRef]
- Jubair, N.; Rajagopal, M.; Chinnappan, S.; Abdullah, N.B.; Fatima, A. Review on the Antibacterial Mechanism of Plant-Derived Compounds against Multidrug-Resistant Bacteria (MDR). Evid. -Based Complement. Altern. Med. 2021, 2021, 3663315. [Google Scholar] [CrossRef]
- Bhatia, P.; Sharma, A.; George, A.J.; Anvitha, D.; Kumar, P.; Dwivedi, V.P.; Chandra, N.S. Antibacterial activity of medicinal plants against ESKAPE: An update. Heliyon 2021, 7, e06310. [Google Scholar] [CrossRef]
- Popescu, G.A.; Șerban, R.; Iosif, I.; Codiță, I.; Dorobăț, O.; Tălăpan, D.; Buzea, M.; Szekely, E.; Dorneanu, O.; Bota, K.; et al. Antimicrobial resistance of germs isolated from invasive infections—Romania 2012. BMC Infect. Dis. 2013, 13, O16. [Google Scholar] [CrossRef]
- Rafila, A.; Tălăpan, D.; Dorobat, O.; Popescu, G.; Piţigoi, D.; Florea, D.; Buicu, F. Emergence of Carbapenemase-producing Enterobacteriaceae, a Public Health Threat: A Romanian Infectious Disease Hospital Based Study. Rev. Romana De Med. De Lab. 2015, 23, 295–301. [Google Scholar] [CrossRef]
- Tălăpan, D.; Rafila, A. Five-Year Survey of Asymptomatic Colonization with Multidrug-Resistant Organisms in a Romanian Tertiary Care Hospital. Infect. Drug Resist. 2022, 15, 2959–2967. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Orjala, J.; Sticher, O.; Rali, T. Acylated flavonol glycosides from leaves of Stenochlaena palustris. J. Nat. Prod. 1999, 62, 70–75. [Google Scholar] [CrossRef] [PubMed]
- Li, X.-M.; Luo, X.-G.; Si, C.-L.; Wang, N.; Zhou, H.; He, J.-F.; Zhang, T.-C. Antibacterial active compounds from Hypericum ascyron L. induce bacterial cell death through apoptosis pathway. Eur. J. Med. Chem. 2015, 96, 436–444. [Google Scholar] [CrossRef]
- He, M.; Wu, T.; Pan, S.; Xu, X. Antimicrobial mechanism of flavonoids against Escherichia coli ATCC 25922 by model membrane study. Appl. Surf. Sci. 2014, 305, 515–521. [Google Scholar] [CrossRef]
- Cronan, J.E.; Thomas, J. Bacterial fatty acid synthesis and its relationships with polyketide synthetic pathways. Methods Enzymol. 2009, 459, 395–433. [Google Scholar] [CrossRef] [PubMed]
- Rowlett, V.W.; Mallampalli, V.; Karlstaedt, A.; Dowhan, W.; Taegtmeyer, H.; Margolin, W.; Vitrac, H. Impact of Membrane Phospholipid Alterations in Escherichia coli on Cellular Function and Bacterial Stress Adaptation. J. Bacteriol. 2017, 199, e00849-16. [Google Scholar] [CrossRef]
- Al-Nour, M.Y.; Ibrahim, M.M.; Elsaman, T. Ellagic Acid, Kaempferol, and Quercetin from Acacia nilotica: Promising Combined Drug With Multiple Mechanisms of Action. Curr. Pharmacol. Rep. 2019, 5, 255–280. [Google Scholar] [CrossRef]
- Wu, T.; Zang, X.; He, M.; Pan, S.; Xu, X. Structure-activity relationship of flavonoids on their anti-Escherichia coli activity and inhibition of DNA gyrase. J. Agric. Food Chem. 2013, 61, 8185–8190. [Google Scholar] [CrossRef]
- Liu, M.H.; Otsuka, N.; Noyori, K.; Shiota, S.; Ogawa, W.; Kuroda, T.; Hatano, T.; Tsuchiya, T. Synergistic effect of kaempferol glycosides purified from Laurus nobilis and fluoroquinolones on methicillin-resistant Staphylococcus aureus. Biol. Pharm. Bull. 2009, 32, 489–492. [Google Scholar] [CrossRef]
- Huang, Y.H.; Huang, C.C.; Chen, C.C.; Yang, K.J.; Huang, C.Y. Inhibition of Staphylococcus aureus PriA Helicase by Flavonol Kaempferol. Protein. J. 2015, 34, 169–172. [Google Scholar] [CrossRef] [PubMed]
- Lim, Y.H.; Kim, I.H.; Seo, J.J. In vitro activity of kaempferol isolated from the Impatiens balsamina alone and in combination with erythromycin or clindamycin against Propionibacterium acnes. J. Microbiol. 2007, 45, 473–477. [Google Scholar] [PubMed]
- Christopoulou, C.; Graikou, K.; Chinou, I. Chemosystematic Value of Chemical Constituents from Scabiosa hymettia (Dipsacaceae). Chem. Biodivers. 2008, 5, 318–323. [Google Scholar] [CrossRef] [PubMed]
- Ragasa, C.Y.; de Luna, R.D.; Cruz, W.C.; Rideout, J.A. Monoterpene Lactones from the Seeds of Nephelium lappaceum. J. Nat. Prod. 2005, 68, 1394–1396. [Google Scholar] [CrossRef] [PubMed]
- Karimi, E.; Jaafar, H.Z.; Ahmad, S. Phytochemical analysis and antimicrobial activities of methanolic extracts of leaf, stem and root from different varieties of Labisa pumila Benth. Molecules 2011, 16, 4438–4450. [Google Scholar] [CrossRef] [PubMed]
- Achika, J.I.; Ayo, R.G.; Oyewale, A.O.; Habila, J.D. Flavonoids with antibacterial and antioxidant potentials from the stem bark of Uapaca heudelotti. Heliyon 2020, 6, e03381. [Google Scholar] [CrossRef] [PubMed]
- de Freitas, M.A.; da Cruz, R.P.; Dos Santos, A.T.L.; Almeida-Bezerra, J.W.; Machado, A.J.T.; Dos Santos, J.F.S.; Rocha, J.E.; Boligon, A.A.; Bezerra, C.F.; de Freitas, T.S.; et al. HPLC-DAD analysis and antimicrobial activities of Spondias mombin L. (Anacardiaceae). 3 Biotech 2022, 12, 61. [Google Scholar] [CrossRef]
- Özçelik, B.; Orhan, I.; Toker, G. Antiviral and Antimicrobial Assessment of Some Selected Flavonoids. Z. Für Nat. C 2006, 61, 632–638. [Google Scholar] [CrossRef]
- Rofeal, M.; El-Malek, F.A.; Qi, X. In vitro assessment of green polyhydroxybutyrate/chitosan blend loaded with kaempferol nanocrystals as a potential dressing for infected wounds. Nanotechnology 2021, 32, 37. [Google Scholar] [CrossRef]
- Šuran, J.; Cepanec, I.; Mašek, T.; Starčević, K.; Tlak Gajger, I.; Vranješ, M.; Radić, B.; Radić, S.; Kosalec, I.; Vlainić, J. Nonaqueous Polyethylene Glycol as a Safer Alternative to Ethanolic Propolis Extracts with Comparable Antioxidant and Antimicrobial Activity. Antioxidants 2021, 10, 978. [Google Scholar] [CrossRef]
- Kannanoor, M.; Lakshmi, B.A.; Kim, S. Synthesis of silver nanoparticles conjugated with kaempferol and hydrocortisone and an evaluation of their antibacterial effects. 3 Biotech 2021, 11, 317. [Google Scholar] [CrossRef] [PubMed]
- Galal, T.M.; Al-Yasi, H.M.; Fawzy, M.A.; Abdelkader, T.G.; Hamza, R.Z.; Eid, E.M.; Ali, E.F. Evaluation of the Phytochemical and Pharmacological Potential of Taif’s Rose (Rosa damascena Mill var. trigintipetala) for Possible Recycling of Pruning Wastes. Life 2022, 12, 273. [Google Scholar] [CrossRef] [PubMed]
- Attallah, N.G.M.; El-Sherbeni, S.A.; El-Kadem, A.H.; Elekhnawy, E.; El-Masry, T.A.; Elmongy, E.I.; Altwaijry, N.; Negm, W.A. Elucidation of the Metabolite Profile of Yucca gigantea and Assessment of Its Cytotoxic, Antimicrobial, and Anti-Inflammatory Activities. Molecules 2022, 27, 1329. [Google Scholar] [CrossRef] [PubMed]
- Habbu, P.V.; Mahadevan, K.M.; Shastry, R.A.; Manjunatha, H. Antimicrobial activity of flavanoid sulphates and other fractions of Argyreia speciosa (Burm.f) Boj. Indian J. Exp. Biol. 2009, 47, 121–128. [Google Scholar]
- Tatsimo, S.J.; Tamokou Jde, D.; Havyarimana, L.; Csupor, D.; Forgo, P.; Hohmann, J.; Kuiate, J.R.; Tane, P. Antimicrobial and antioxidant activity of kaempferol rhamnoside derivatives from Bryophyllum pinnatum. BMC Res. Notes 2012, 5, 158. [Google Scholar] [CrossRef]
- Otsuka, N.; Liu, M.H.; Shiota, S.; Ogawa, W.; Kuroda, T.; Hatano, T.; Tsuchiya, T. Anti-methicillin resistant Staphylococcus aureus (MRSA) compounds isolated from Laurus nobilis. Biol. Pharm. Bull. 2008, 31, 1794–1797. [Google Scholar] [CrossRef] [PubMed]
- Bisignano, G.; Sanogo, R.; Marino, A.; Aquino, R.; D’Angelo, V.; Germanò, M.P.; De Pasquale, R.; Pizza, C. Antimicrobial activity of Mitracarpus scaber extract and isolated constituents. Lett. Appl. Microbiol. 2000, 30, 105–108. [Google Scholar] [CrossRef]
- Ivanova, A.; Mikhova, B.; Najdenski, H.; Tsvetkova, I.; Kostova, I. Chemical composition and antimicrobial activity of wild garlic Allium ursinum of Bulgarian origin. Nat. Prod. Commun. 2009, 4, 1059–1062. [Google Scholar] [CrossRef]
- Ibrahim, M.A.; Mansoor, A.A.; Gross, A.; Ashfaq, M.K.; Jacob, M.; Khan, S.I.; Hamann, M.T. Methicillin-resistant Staphylococcus aureus (MRSA)-active metabolites from Platanus occidentalis (American Sycamore). J. Nat. Prod. 2009, 72, 2141–2144. [Google Scholar] [CrossRef]
- Chan, E.W.; Gray, A.I.; Igoli, J.O.; Lee, S.M.; Goh, J.K. Galloylated flavonol rhamnosides from the leaves of Calliandra tergemina with antibacterial activity against methicillin-resistant Staphylococcus aureus (MRSA). Phytochemistry 2014, 107, 148–154. [Google Scholar] [CrossRef]
- Zhang, Y.; Valeriote, F.; Swartz, K.; Chen, B.; Hamann, M.T.; Rodenburg, D.L.; McChesney, J.D.; Shaw, J. HPLC Plasma Assay of a Novel Anti-MRSA Compound, Kaempferol-3-O-Alpha-L-(2”,3”-di-p-coumaroyl)rhamnoside, from Sycamore Leaves. Nat. Prod. Commun. 2015, 10, 1383–1386. [Google Scholar] [CrossRef] [PubMed]
- Carruthers, N.J.; Stemmer, P.M.; Media, J.; Swartz, K.; Wang, X.; Aube, N.; Hamann, M.T.; Valeriote, F.; Shaw, J. The anti-MRSA compound 3-O-alpha-L-(2″,3″-di-p-coumaroyl)rhamnoside (KCR) inhibits protein synthesis in Staphylococcus aureus. J. Proteom. 2020, 210, 103539. [Google Scholar] [CrossRef] [PubMed]
- Ishikawa, R.B.; Leitão, M.M.; Kassuya, R.M.; Macorini, L.F.; Moreira, F.M.F.; Cardoso, C.A.L.; Coelho, R.G.; Pott, A.; Gelfuso, G.M.; Croda, J.; et al. Anti-inflammatory, antimycobacterial and genotoxic evaluation of Doliocarpus dentatus. J. Ethnopharmacol. 2017, 204, 18–25. [Google Scholar] [CrossRef] [PubMed]
- Santos, E.D.; Silva-Filho, S.E.; Santos Radai, J.A.; Arena, A.C.; Fraga, T.L.; Lima Cardoso, C.A.; Croda, J.; Leite Kassuya, C.A. Anti-inflammatory properties of ethanolic extract from Vatairea macrocarpa leaves. J. Ethnopharmacol. 2021, 278, 114308. [Google Scholar] [CrossRef]
- Asif, M.; Alvi, I.A.; Rehman, S.U. Insight into Acinetobacter baumannii: Pathogenesis, global resistance, mechanisms of resistance, treatment options, and alternative modalities. Infect. Drug Resist. 2018, 11, 1249–1260. [Google Scholar] [CrossRef]
- Pourhajibagher, M.; Hashemi, F.B.; Pourakbari, B.; Aziemzadeh, M.; Bahador, A. Antimicrobial Resistance of Acinetobacter baumannii to Imipenem in Iran: A Systematic Review and Meta-Analysis. Open Microbiol J 2016, 10, 32–42. [Google Scholar] [CrossRef]
- Qi, L.; Li, H.; Zhang, C.; Liang, B.; Li, J.; Wang, L.; Du, X.; Liu, X.; Qiu, S.; Song, H. Relationship between Antibiotic Resistance, Biofilm Formation, and Biofilm-Specific Resistance in Acinetobacter baumannii. Front. Microbiol. 2016, 7, 483. [Google Scholar] [CrossRef] [PubMed]
- Gheorghe-Barbu, I.; Barbu, I.C.; Popa, L.I.; Pîrcălăbioru, G.G.; Popa, M.; Măruțescu, L.; Niță-Lazar, M.; Banciu, A.; Stoica, C.; Gheorghe, Ș.; et al. Temporo-spatial variations in resistance determinants and clonality of Acinetobacter baumannii and Pseudomonas aeruginosa strains from Romanian hospitals and wastewaters. Antimicrob. Resist. Infect. Control 2022, 11, 115. [Google Scholar] [CrossRef]
- Gu, H.-J.; Sun, Q.-L.; Luo, J.-C.; Zhang, J.; Sun, L. A First Study of the Virulence Potential of a Bacillus subtilis Isolate From Deep-Sea Hydrothermal Vent. Front. Cell Infect. Microbiol. 2019, 9, 183. [Google Scholar] [CrossRef]
- Cote, C.K.; Heffron, J.D.; Bozue, J.A.; Welkos, S.L. Chapter 102—Bacillus anthracis and Other Bacillus Species. In Molecular Medical Microbiology, 2nd ed.; Tang, Y.-W., Sussman, M., Liu, D., Poxton, I., Schwartzman, J., Eds.; Academic Press: Boston, MA, USA, 2015; pp. 1789–1844. [Google Scholar] [CrossRef]
- Brown, K.L. Control of bacterial spores. Br. Med. Bull. 2000, 56, 158–171. [Google Scholar] [CrossRef]
- Spencer, R.C. Bacillus anthracis. J. Clin. Pathol. 2003, 56, 182–187. [Google Scholar] [CrossRef]
- Hoffmaster, A.R.; Hill, K.K.; Gee, J.E.; Marston, C.K.; De, B.K.; Popovic, T.; Sue, D.; Wilkins, P.P.; Avashia, S.B.; Drumgoole, R.; et al. Characterization of Bacillus cereus isolates associated with fatal pneumonias: Strains are closely related to Bacillus anthracis and harbor B. anthracis virulence genes. J. Clin. Microbiol. 2006, 44, 3352–3360. [Google Scholar] [CrossRef] [PubMed]
- Ramarao, N.; Sanchis, V. The Pore-Forming Haemolysins of Bacillus Cereus: A Review. Toxins 2013, 5, 1119–1139. [Google Scholar] [CrossRef] [PubMed]
- Kaper, J.B.; Nataro, J.P.; Mobley, H.L.T. Pathogenic Escherichia coli. Nat. Rev. Microbiol. 2004, 2, 123–140. [Google Scholar] [CrossRef]
- Nataro, J.P.; Kaper, J.B. Diarrheagenic Escherichia coli. Clin. Microbiol. Rev. 1998, 11, 142–201. [Google Scholar] [CrossRef]
- Pormohammad, A.; Pouriran, R.; Azimi, H.; Goudarzi, M. Prevalence of integron classes in Gram-negative clinical isolated bacteria in Iran: A systematic review and meta-analysis. Iran. J. Basic Med. Sci. 2019, 22, 118–127. [Google Scholar] [CrossRef] [PubMed]
- Effah, C.Y.; Sun, T.; Liu, S.; Wu, Y. Klebsiella pneumoniae: An increasing threat to public health. Ann. Clin. Microbiol. Antimicrob. 2020, 19, 1. [Google Scholar] [CrossRef]
- Navon-Venezia, S.; Kondratyeva, K.; Carattoli, A. Klebsiella pneumoniae: A major worldwide source and shuttle for antibiotic resistance. FEMS Microbiol. Rev. 2017, 41, 252–275. [Google Scholar] [CrossRef]
- Podschun, R.; Ullmann, U. Klebsiella spp. as nosocomial pathogens: Epidemiology, taxonomy, typing methods, and pathogenicity factors. Clin. Microbiol. Rev. 1998, 11, 589–603. [Google Scholar] [CrossRef]
- Surleac, M.; Barbu, I.; Paraschiv, S.; Popa, L.; Gheorghe, I.; Marutescu, L.; Popa, M.; Avram, I.; Tălăpan, D.; Nita-Lazar, M.; et al. Whole genome sequencing snapshot of multi-drug resistant Klebsiella pneumoniae strains from hospitals and receiving wastewater treatment plants in Southern Romania. PLoS ONE 2020, 15, e0228079. [Google Scholar] [CrossRef]
- Popa, L.; Gheorghe, I.; Barbu, I.; Surleac, M.; Paraschiv, S.; Marutescu, L.; Popa, M.; Gradisteanu Pircalabioru, G.; Tălăpan, D.; Nita-Lazar, M.; et al. Multidrug Resistant Klebsiella pneumoniae ST101 Clone Survival Chain From Inpatients to Hospital Effluent After Chlorine Treatment. Front. Microbiol. 2021, 11, 610296. [Google Scholar] [CrossRef] [PubMed]
- Smith, I. Mycobacterium tuberculosis pathogenesis and molecular determinants of virulence. Clin. Microbiol. Rev. 2003, 16, 463–496. [Google Scholar] [CrossRef] [PubMed]
- Mangtani, P.; Abubakar, I.; Ariti, C.; Beynon, R.; Pimpin, L.; Fine, P.E.; Rodrigues, L.C.; Smith, P.G.; Lipman, M.; Whiting, P.F.; et al. Protection by BCG vaccine against tuberculosis: A systematic review of randomized controlled trials. Clin. Infect. Dis. 2014, 58, 470–480. [Google Scholar] [CrossRef] [PubMed]
- Scriba, T.J.; Netea, M.G.; Ginsberg, A.M. Key recent advances in TB vaccine development and understanding of protective immune responses against Mycobacterium tuberculosis. Semin. Immunol. 2020, 50, 101431. [Google Scholar] [CrossRef]
- Popescu, G.G.; Arghir, O.C.; Fildan, A.P.; Spanu, V.; Cambrea, S.C.; Rafila, A.; Buicu, F.C. Antibiotic resistance of Mycobacterium tuberculosis; mechanism and specific therapeutic response. Farmacia 2020, 68, 197–205. [Google Scholar] [CrossRef]
- Allué-Guardia, A.; García, J.I.; Torrelles, J.B. Evolution of Drug-Resistant Mycobacterium tuberculosis Strains and Their Adaptation to the Human Lung Environment. Front. Microbiol. 2021, 12, 612675. [Google Scholar] [CrossRef] [PubMed]
- Spratt, B.G. Antibiotic resistance: Counting the cost. Curr. Biol. 1996, 6, 1219–1221. [Google Scholar] [CrossRef][Green Version]
- Böttger, E.C.; Springer, B.; Pletschette, M.; Sander, P. Fitness of antibiotic-resistant microorganisms and compensatory mutations. Nat. Med. 1998, 4, 1343–1344. [Google Scholar] [CrossRef]
- Andersson, D.I.; Levin, B.R. The biological cost of antibiotic resistance. Curr. Opin. Microbiol. 1999, 2, 489–493. [Google Scholar] [CrossRef]
- Fanning, A.; Edwards, S. Mycobacterium bovis infection in human beings in contact with elk (Cervus elaphus) in Alberta, Canada. Lancet 1991, 338, 1253–1255. [Google Scholar] [CrossRef]
- Cooke, M.M.; Gear, A.J.; Naidoo, A.; Collins, D.M. Accidental Mycobacterium bovis infection in a veterinarian. New Zealand Vet. J. 2002, 50, 36–38. [Google Scholar] [CrossRef] [PubMed]
- Wilkins, M.; Bartlett, P.; Frawley, B.; O’Brien, D.; Miller, C.; Boulton, M. Mycobacterium bovis (bovine TB) exposure as a recreational risk for hunters: Results of a Michigan Hunter Survey, 2001. Int. J. Tuberc. Lung Dis. 2003, 7, 1001–1009. [Google Scholar] [PubMed]
- Wilkins, M.J.; Meyerson, J.; Bartlett, P.C.; Spieldenner, S.L.; Berry, D.E.; Mosher, L.B.; Kaneene, J.B.; Robinson-Dunn, B.; Stobierski, M.G.; Boulton, M.L. Human Mycobacterium bovis infection and bovine tuberculosis outbreak, Michigan, 1994–2007. Emerg. Infect. Dis. 2008, 14, 657. [Google Scholar] [CrossRef] [PubMed]
- Palmer, M.V.; Thacker, T.C.; Waters, W.R.; Gortázar, C.; Corner, L.A.L. Mycobacterium bovis: A Model Pathogen at the Interface of Livestock, Wildlife, and Humans. Vet. Med. Int. 2012, 2012, 236205. [Google Scholar] [CrossRef] [PubMed]
- Di Chiara, J.M.; Contreras-Martinez, L.M.; Livny, J.; Smith, D.; McDonough, K.A.; Belfort, M. Multiple small RNAs identified in Mycobacterium bovis BCG are also expressed in Mycobacterium tuberculosis and Mycobacterium smegmatis. Nucleic Acids Res. 2010, 38, 4067–4078. [Google Scholar] [CrossRef]
- Klockgether, J.; Tümmler, B. Recent advances in understanding Pseudomonas aeruginosa as a pathogen. F1000Res 2017, 6, 1261. [Google Scholar] [CrossRef]
- Buhl, M.; Peter, S.; Willmann, M. Prevalence and risk factors associated with colonization and infection of extensively drug-resistant Pseudomonas aeruginosa: A systematic review. Expert Rev. Anti Infect. Ther. 2015, 13, 1159–1170. [Google Scholar] [CrossRef]
- Murphy, T.F. Pseudomonas aeruginosa in adults with chronic obstructive pulmonary disease. Curr. Opin. Pulm. Med. 2009, 15, 138–142. [Google Scholar] [CrossRef]
- Gonçalves-de-Albuquerque, C.F.; Silva, A.R.; Burth, P.; Rocco, P.R.; Castro-Faria, M.V.; Castro-Faria-Neto, H.C. Possible mechanisms of Pseudomonas aeruginosa-associated lung disease. Int. J. Med. Microbiol. 2016, 306, 20–28. [Google Scholar] [CrossRef]
- Talwalkar, J.S.; Murray, T.S. The Approach to Pseudomonas aeruginosa in Cystic Fibrosis. Clin. Chest Med. 2016, 37, 69–81. [Google Scholar] [CrossRef]
- Winstanley, C.; O’Brien, S.; Brockhurst, M.A. Pseudomonas aeruginosa Evolutionary Adaptation and Diversification in Cystic Fibrosis Chronic Lung Infections. Trends Microbiol. 2016, 24, 327–337. [Google Scholar] [CrossRef] [PubMed]
- Willcox, M.D. Pseudomonas aeruginosa infection and inflammation during contact lens wear: A review. Optom. Vis. Sci. 2007, 84, 273–278. [Google Scholar] [CrossRef] [PubMed]
- Church, D.; Elsayed, S.; Reid, O.; Winston, B.; Lindsay, R. Burn wound infections. Clin. Microbiol. Rev. 2006, 19, 403–434. [Google Scholar] [CrossRef]
- Fournier, A.; Voirol, P.; Krähenbühl, M.; Bonnemain, C.L.; Fournier, C.; Pantet, O.; Pagani, J.L.; Revelly, J.P.; Dupuis-Lozeron, E.; Sadeghipour, F.; et al. Antibiotic consumption to detect epidemics of Pseudomonas aeruginosa in a burn centre: A paradigm shift in the epidemiological surveillance of Pseudomonas aeruginosa nosocomial infections. Burns 2016, 42, 564–570. [Google Scholar] [CrossRef]
- Döring, G.; Parameswaran, I.G.; Murphy, T.F. Differential adaptation of microbial pathogens to airways of patients with cystic fibrosis and chronic obstructive pulmonary disease. FEMS Microbiol. Rev. 2011, 35, 124–146. [Google Scholar] [CrossRef] [PubMed]
- Langan, K.M.; Kotsimbos, T.; Peleg, A.Y. Managing Pseudomonas aeruginosa respiratory infections in cystic fibrosis. Curr. Opin. Infect. Dis. 2015, 28, 547–556. [Google Scholar] [CrossRef] [PubMed]
- Bassi, G.L.; Ferrer, M.; Marti, J.D.; Comaru, T.; Torres, A. Ventilator-associated pneumonia. Semin. Respir. Crit. Care Med. 2014, 35, 469–481. [Google Scholar] [CrossRef] [PubMed]
- Pang, Z.; Raudonis, R.; Glick, B.R.; Lin, T.-J.; Cheng, Z. Antibiotic resistance in Pseudomonas aeruginosa: Mechanisms and alternative therapeutic strategies. Biotechnol. Adv. 2019, 37, 177–192. [Google Scholar] [CrossRef] [PubMed]
- Crump, J.A.; Luby, S.P.; Mintz, E.D. The global burden of typhoid fever. Bull. World Health Organ. 2004, 82, 346–353. [Google Scholar]
- Popa, G.; Popa, M.I. Salmonella spp. Infection—A continuous threat worldwide. GERMS 2021, 11, 87–96. [Google Scholar] [CrossRef]
- Allerberger, F.; Liesegang, A.; Grif, K.; Khaschabi, D.; Prager, R.; Danzl, J.; Höck, F.; Ottl, J.; Dierich, M.P.; Berghold, C.; et al. Occurrence of Salmonella enterica serovar Dublin in Austria. Wien Med. Wochenschr. 2003, 153, 148–152. [Google Scholar] [CrossRef] [PubMed]
- Eng, S.-K.; Pusparajah, P.; Ab Mutalib, N.-S.; Ser, H.-L.; Chan, K.-G.; Lee, L.-H. Salmonella: A review on pathogenesis, epidemiology and antibiotic resistance. Front. Life Sci. 2015, 8, 284–293. [Google Scholar] [CrossRef]
- Chiu, C.H.; Wu, T.L.; Su, L.H.; Chu, C.; Chia, J.H.; Kuo, A.J.; Chien, M.S.; Lin, T.Y. The emergence in Taiwan of fluoroquinolone resistance in Salmonella enterica serotype choleraesuis. N. Engl. J. Med. 2002, 346, 413–419. [Google Scholar] [CrossRef] [PubMed]
- Tong, S.Y.; Davis, J.S.; Eichenberger, E.; Holland, T.L.; Fowler, V.G., Jr. Staphylococcus aureus infections: Epidemiology, pathophysiology, clinical manifestations, and management. Clin. Microbiol. Rev. 2015, 28, 603–661. [Google Scholar] [CrossRef]
- Sandulescu, O.; Bleotu, C.; Matei, L.; Streinu-Cercel, A.; Oprea, M.; Dragulescu, E.; Chifiriuc, M.; Rafila, A.; Pirici, D.; Tălăpan, D.; et al. Comparative evaluation of aggressiveness traits in staphylococcal strains from severe infections versus nasopharyngeal carriage. Microb. Pathog. 2016, 102, 45–53. [Google Scholar] [CrossRef] [PubMed]
- Malachowa, N.; DeLeo, F.R. Mobile genetic elements of Staphylococcus aureus. Cell Mol. Life Sci. 2010, 67, 3057–3071. [Google Scholar] [CrossRef] [PubMed]
- Howden, B.P.; Davies, J.K.; Johnson, P.D.; Stinear, T.P.; Grayson, M.L. Reduced vancomycin susceptibility in Staphylococcus aureus, including vancomycin-intermediate and heterogeneous vancomycin-intermediate strains: Resistance mechanisms, laboratory detection, and clinical implications. Clin. Microbiol. Rev. 2010, 23, 99–139. [Google Scholar] [CrossRef]
- Klevens, R.M.; Morrison, M.A.; Nadle, J.; Petit, S.; Gershman, K.; Ray, S.; Harrison, L.H.; Lynfield, R.; Dumyati, G.; Townes, J.M.; et al. Invasive methicillin-resistant Staphylococcus aureus infections in the United States. JAMA 2007, 298, 1763–1771. [Google Scholar] [CrossRef]
- Durai, R.; Ng, P.C.; Hoque, H. Methicillin-resistant Staphylococcus aureus: An update. Aorn J. 2010, 91, 599–606. [Google Scholar] [CrossRef]
- Johnson, A.P. Methicillin-resistant Staphylococcus aureus: The European landscape. J. Antimicrob. Chemother. 2011, 66 (Suppl. 4), iv43–iv48. [Google Scholar] [CrossRef]
- Dulon, M.; Haamann, F.; Peters, C.; Schablon, A.; Nienhaus, A. MRSA prevalence in European healthcare settings: A review. BMC Infect. Dis. 2011, 11, 138. [Google Scholar] [CrossRef] [PubMed]
- Grema, H.A.; Geidam, Y.A.; Gadzama, G.B.; Ameh, J.A.; Suleiman, A. Methicillin resistant Staphylococcus aureus (MRSA): A review. Adv. Anim. Vet. Sci. 2015, 3, 79–98. [Google Scholar] [CrossRef]
- Otto, M. Staphylococcus epidermidis—The ‘accidental’ pathogen. Nat. Rev. Microbiol. 2009, 7, 555–567. [Google Scholar] [CrossRef] [PubMed]
- Schaberg, D.R.; Culver, D.H.; Gaynes, R.P. Major trends in the microbial etiology of nosocomial infection. Am. J. Med. 1991, 91, 72s–75s. [Google Scholar] [CrossRef] [PubMed]
- Kaye, D. Enterococci. Biologic and epidemiologic characteristics and in vitro susceptibility. Arch. Intern. Med. 1982, 142, 2006–2009. [Google Scholar] [CrossRef]
- Maki, D.G.; Agger, W.A. Enterococcal Bacteremia: Clinical Features, the Risk of Endocarditis, and Management. Medicine 1988, 67, 248. [Google Scholar] [CrossRef]
- Noskin, G.A.; Peterson, L.R.; Warren, J.R. Enterococcus faecium and Enterococcus faecalis bacteremia: Acquisition and outcome. Clin. Infect. Dis. 1995, 20, 296–301. [Google Scholar] [CrossRef]
- Cetinkaya, Y.; Falk, P.; Mayhall, C.G. Vancomycin-Resistant Enterococci. Clin. Microbiol. Rev. 2000, 13, 686–707. [Google Scholar] [CrossRef]
- Papazafiropoulou, A.; Daniil, I.; Sotiropoulos, A.; Balampani, E.; Kokolaki, A.; Bousboulas, S.; Konstantopoulou, S.; Skliros, E.; Petropoulou, D.; Pappas, S. Prevalence of asymptomatic bacteriuria in type 2 diabetic subjects with and without microalbuminuria. BMC Res. Notes 2010, 3, 169. [Google Scholar] [CrossRef]
- Matthews, S.J.; Lancaster, J.W. Urinary tract infections in the elderly population. Am. J. Geriatr. Pharmacother. 2011, 9, 286–309. [Google Scholar] [CrossRef]
- Schaffer, J.N.; Pearson, M.M. Proteus mirabilis and Urinary Tract Infections. Microbiol. Spectr. 2015, 3, 3–5. [Google Scholar] [CrossRef]
- Charkhian, H.; Bodaqlouie, A.; Soleimannezhadbari, E.; Lotfollahi, L.; Shaykh-Baygloo, N.; Hosseinzadeh, R.; Yousefi, N.; Khodayar, M. Comparing the Bacteriostatic Effects of Different Metal Nanoparticles Against Proteus vulgaris. Curr. Microbiol. 2020, 77, 2674–2684. [Google Scholar] [CrossRef] [PubMed]
- Mobley, H.L.; Warren, J.W. Urease-positive bacteriuria and obstruction of long-term urinary catheters. J. Clin. Microbiol. 1987, 25, 2216–2217. [Google Scholar] [CrossRef] [PubMed]
- Mobley, H.L.; Warren, J.W. Urinary Tract Infections: Molecular Pathogenesis and Clinical Management; ASM Press: Washington, DC, USA, 1996; pp. 3–27. [Google Scholar]
- Jacobsen, S.M.; Shirtliff, M.E. Proteus mirabilis biofilms and catheter-associated urinary tract infections. Virulence 2011, 2, 460–465. [Google Scholar] [CrossRef]
- Yuan, F.; Huang, Z.; Yang, T.; Wang, G.; Li, P.; Yang, B.; Li, J. Pathogenesis of Proteus mirabilis in Catheter-Associated Urinary Tract Infections. Urol. Int. 2021, 105, 354–361. [Google Scholar] [CrossRef] [PubMed]
- Hall, R.M.; Collis, C.M. Antibiotic resistance in gram-negative bacteria: The role of gene cassettes and integrons. Drug Resist. Updat. 1998, 1, 109–119. [Google Scholar] [CrossRef] [PubMed]
- Tumbarello, M.; Trecarichi, E.M.; Fiori, B.; Losito, A.R.; D’Inzeo, T.; Campana, L.; Ruggeri, A.; Di Meco, E.; Liberto, E.; Fadda, G.; et al. Multidrug-resistant Proteus mirabilis bloodstream infections: Risk factors and outcomes. Antimicrob. Agents Chemother. 2012, 56, 3224–3231. [Google Scholar] [CrossRef]
- Pagani, L.; Migliavacca, R.; Pallecchi, L.; Matti, C.; Giacobone, E.; Amicosante, G.; Romero, E.; Rossolini, G.M. Emerging extended-spectrum beta-lactamases in Proteus mirabilis. J. Clin. Microbiol. 2002, 40, 1549–1552. [Google Scholar] [CrossRef]
- Endimiani, A.; Luzzaro, F.; Brigante, G.; Perilli, M.; Lombardi, G.; Amicosante, G.; Rossolini, G.M.; Toniolo, A. Proteus mirabilis bloodstream infections: Risk factors and treatment outcome related to the expression of extended-spectrum beta-lactamases. Antimicrob. Agents Chemother. 2005, 49, 2598–2605. [Google Scholar] [CrossRef] [PubMed]
- Cohen-Nahum, K.; Saidel-Odes, L.; Riesenberg, K.; Schlaeffer, F.; Borer, A. Urinary tract infections caused by multi-drug resistant Proteus mirabilis: Risk factors and clinical outcomes. Infection 2010, 38, 41–46. [Google Scholar] [CrossRef]
- D’Andrea, M.M.; Literacka, E.; Zioga, A.; Giani, T.; Baraniak, A.; Fiett, J.; Sadowy, E.; Tassios, P.T.; Rossolini, G.M.; Gniadkowski, M.; et al. Evolution and spread of a multidrug-resistant Proteus mirabilis clone with chromosomal AmpC-type cephalosporinases in Europe. Antimicrob. Agents Chemother. 2011, 55, 2735–2742. [Google Scholar] [CrossRef] [PubMed]
- Vaez, H.; Kalarestaghi, H.; Sahebkar, A.; Khademi, F. Prevalence of antibiotic resistance of Proteus species in urinary tract infections in Iran: A systematic review and meta-analysis. Gene Rep. 2022, 27, 101632. [Google Scholar] [CrossRef]
- Colwell, R.R.; Kaper, J.; Joseph, S.W. Vibrio cholerae, Vibrio parahaemolyticus, and other vibrios: Occurrence and distribution in Chesapeake Bay. Science 1977, 198, 394–396. [Google Scholar]
- Garay, E.; Arnau, A.; Amaro, C. Incidence of Vibrio cholerae and related vibrios in a coastal lagoon and seawater influenced by lake discharges along an annual cycle. Appl. Environ. Microbiol. 1985, 50, 426–430. [Google Scholar] [CrossRef]
- Colwell, R.R. Global climate and infectious disease: The cholera paradigm. Science 1996, 274, 2025–2031. [Google Scholar] [CrossRef] [PubMed]
- Reidl, J.; Klose, K.E. Vibrio cholerae and cholera: Out of the water and into the host. FEMS Microbiol. Rev. 2002, 26, 125–139. [Google Scholar] [CrossRef] [PubMed]
- Glass, R.I.; Huq, I.; Alim, A.R.M.A.; Yunus, M. Emergence of Multiply Antibiotic-Resistant Vibrio cholerae in Bangladesh. J. Infect. Dis. 1980, 142, 939–942. [Google Scholar] [CrossRef] [PubMed]
- Das, B.; Verma, J.; Kumar, P.; Ghosh, A.; Ramamurthy, T. Antibiotic resistance in Vibrio cholerae: Understanding the ecology of resistance genes and mechanisms. Vaccine 2020, 38, A83–A92. [Google Scholar] [CrossRef]
- Brown, G.D.; Denning, D.W.; Levitz, S.M. Tackling human fungal infections. Science 2012, 336, 647. [Google Scholar] [CrossRef]
- Mayer, F.L.; Wilson, D.; Hube, B. Candida albicans pathogenicity mechanisms. Virulence 2013, 4, 119–128. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Diekema, D.J. Epidemiology of invasive candidiasis: A persistent public health problem. Clin. Microbiol. Rev. 2007, 20, 133–163. [Google Scholar] [CrossRef] [PubMed]
- Pfaller, M.A.; Diekema, D.J. Epidemiology of invasive mycoses in North America. Crit. Rev. Microbiol. 2010, 36, 1–53. [Google Scholar] [CrossRef] [PubMed]
- Hurley, R.; De Louvois, J. Candida vaginitis. Postgrad. Med. J. 1979, 55, 645–647. [Google Scholar] [CrossRef] [PubMed]
- Sobel, J.D. Vulvovaginal candidosis. Lancet 2007, 369, 1961–1971. [Google Scholar] [CrossRef] [PubMed]
- Pappas, P.G.; Kauffman, C.A.; Andes, D.; Benjamin, D.K., Jr.; Calandra, T.F.; Edwards, J.E., Jr.; Filler, S.G.; Fisher, J.F.; Kullberg, B.J.; Ostrosky-Zeichner, L.; et al. Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2009, 48, 503–535. [Google Scholar] [CrossRef]
- Fidel, P.L., Jr. History and new insights into host defense against vaginal candidiasis. Trends Microbiol. 2004, 12, 220–227. [Google Scholar] [CrossRef]
- Cohen, J.; Denning, D.W.; Viviani, M.A. Epidemiology of invasive aspergillosis in European cancer centres. EORTC Invasive Fungal Infections Cooperative Group. Eur. J. Clin. Microbiol. Infect. Dis. 1993, 12, 392–393. [Google Scholar] [CrossRef]
- Rogers, T. Epidemiology and control of nosocomial fungal infections. Curr. Opin. Infect. Dis. 1995, 8, 287–290. [Google Scholar] [CrossRef]
- Ruchlemer, R.; Yinnon, A.M.; Hershko, C. Changes in the natural history of invasive pulmonary aspergillosis in neutropenic leukemic patients. Isr. J. Med. Sci. 1996, 32, 1089–1092. [Google Scholar]
- Meidani, M.; Naeini, A.E.; Rostami, M.; Sherkat, R.; Tayeri, K. Immunocompromised patients: Review of the most common infections happened in 446 hospitalized patients. J. Res. Med. Sci. 2014, 19, S71–S73. [Google Scholar]
- Goodley, J.M.; Clayton, Y.M.; Hay, R.J. Environmental sampling for aspergilli during building construction on a hospital site. J. Hosp. Infect. 1994, 26, 27–35. [Google Scholar] [CrossRef] [PubMed]
- Chazalet, V.; Debeaupuis, J.P.; Sarfati, J.; Lortholary, J.; Ribaud, P.; Shah, P.; Cornet, M.; Vu Thien, H.; Gluckman, E.; Brücker, G.; et al. Molecular typing of environmental and patient isolates of Aspergillus fumigatus from various hospital settings. J. Clin. Microbiol. 1998, 36, 1494–1500. [Google Scholar] [CrossRef] [PubMed]
- Hospenthal, D.R.; Kwon-Chung, K.J.; Bennett, J.E. Concentrations of airborne Aspergillus compared to the incidence of invasive aspergillosis: Lack of correlation. Med. Mycol. 1998, 36, 165–168. [Google Scholar] [CrossRef] [PubMed]
- Kwon-Chung, K.J.; Bennett, J.E. Medical mycology. Rev. Do Inst. De Med. Trop. De São Paulo 1992, 34, 504. [Google Scholar] [CrossRef]
- Pennington, J. Respiratory Infections: Diagnosis and Management; Raven Press: New York, NY, USA, 1983. [Google Scholar]
- Bongomin, F.; Gago, S.; Oladele, R.O.; Denning, D.W. Global and Multi-National Prevalence of Fungal Diseases-Estimate Precision. J. Fungi 2017, 3, 57. [Google Scholar] [CrossRef]
- Rajasingham, R.; Smith, R.M.; Park, B.J.; Jarvis, J.N.; Govender, N.P.; Chiller, T.M.; Denning, D.W.; Loyse, A.; Boulware, D.R. Global burden of disease of HIV-associated cryptococcal meningitis: An updated analysis. Lancet Infect. Dis. 2017, 17, 873–881. [Google Scholar] [CrossRef]
- Knoke, M.; Schwesinger, G. One hundred years ago: The history of cryptococcosis in Greifswald. Medical mycology in the nineteenth century. Mycoses 1994, 37, 229–233. [Google Scholar] [CrossRef]
- Casadevall, A.; Perfect, J.R. Cryptococcus Neoformans; Citeseer: Princeton, NJ, USA, 1998; Volume 595. [Google Scholar]
- Maziarz, E.K.; Perfect, J.R. Cryptococcosis. Infect. Dis. Clin. N. Am. 2016, 30, 179–206. [Google Scholar] [CrossRef]
- Badicut, I.; Paraschiv, S.; Borcan, A.; Tălăpan, D.; Dorobat, O. Risk factors in HIV/AIDS patients with cryptococcal meningitis. BMC Infect. Dis. 2014, 14, P29. [Google Scholar] [CrossRef]
- Revie, N.M.; Iyer, K.R.; Robbins, N.; Cowen, L.E. Antifungal drug resistance: Evolution, mechanisms and impact. Curr. Opin. Microbiol. 2018, 45, 70–76. [Google Scholar] [CrossRef]
- Houšť, J.; Spížek, J.; Havlíček, V. Antifungal Drugs. Metabolites 2020, 10, 106. [Google Scholar] [CrossRef] [PubMed]
- De Leo, M.; Braca, A.; De Tommasi, N.; Norscia, I.; Morelli, I.; Battinelli, L.; Mazzanti, G. Phenolic compounds from Baseonema acuminatum leaves: Isolation and antimicrobial activity. Planta Med. 2004, 70, 841–846. [Google Scholar] [CrossRef] [PubMed]
- Yordanov, M.; Dimitrova, P.; Patkar, S.; Saso, L.; Ivanovska, N. Inhibition of Candida albicans extracellular enzyme activity by selected natural substances and their application in Candida infection. Can. J. Microbiol. 2008, 54, 435–440. [Google Scholar] [CrossRef] [PubMed]
- Dutta, S.; Kundu, A. Macroporous resin-assisted enrichment, characterizations, antioxidant and anticandidal potential of phytochemicals from Trachyspermum ammi. J. Food Biochem. 2022, 46, e13847. [Google Scholar] [CrossRef]
- Pushkala, V.P.; Sulekha, S.M.P.; Mathukumar, S.; Ragavi, B.; Sowmiya, U. Molecular Docking Analysis of Siddha Formulation Parangipattai Chooranam Against Vaginal Candidiasis. Appl. Biochem. Biotechnol. 2022, 194, 1039–1050. [Google Scholar] [CrossRef]
- Slack, A. Parasitic causes of prolonged diarrhoea in travellers—Diagnosis and management. Aust. Fam. Physician 2012, 41, 782–786. [Google Scholar]
- El-Dib, N.A. Entamoeba histolytica: An Overview. Curr. Trop. Med. Rep. 2017, 4, 11–20. [Google Scholar] [CrossRef]
- Wolfe, M.S. Giardiasis. Clin. Microbiol. Rev. 1992, 5, 93–100. [Google Scholar] [CrossRef]
- Minetti, C.; Chalmers, R.M.; Beeching, N.J.; Probert, C.; Lamden, K. Giardiasis. BMJ 2016, 355, i5369. [Google Scholar] [CrossRef]
- Brun, R.; Blum, J.; Chappuis, F.; Burri, C. Human African trypanosomiasis. Lancet 2010, 375, 148–159. [Google Scholar] [CrossRef]
- Greenwood, B. The use of anti-malarial drugs to prevent malaria in the population of malaria-endemic areas. Am. J. Trop. Med. Hyg. 2004, 70, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Autino, B.; Noris, A.; Russo, R.; Castelli, F. Epidemiology of malaria in endemic areas. Mediterr. J. Hematol. Infect. Dis. 2012, 4, e2012060. [Google Scholar] [CrossRef] [PubMed]
- Abdo, M.G.; Elamin, W.M.; Khalil, E.A.; Mukhtar, M.M. Antimony-resistant Leishmania donovaniin eastern Sudan: Incidence and in vitro correlation. East Mediterr. Health J. 2003, 9, 837–843. [Google Scholar] [CrossRef] [PubMed]
- Majumdar, D.; Elsayed, G.A.; Buskas, T.; Boons, G.-J. Synthesis of Proteophosphoglycans of Leishmania major and Leishmania mexicana. J. Org. Chem. 2005, 70, 1691–1697. [Google Scholar] [CrossRef]
- Alvar, J.; Vélez, I.D.; Bern, C.; Herrero, M.; Desjeux, P.; Cano, J.; Jannin, J.; den Boer, M. Leishmaniasis worldwide and global estimates of its incidence. PLoS ONE 2012, 7, e35671. [Google Scholar] [CrossRef]
- Calzada, F.; Alanis, A.D.; Meckes, M.; Tapia-Contreras, A.; Cedillo-Rivera, R. In vitro susceptibility of Entamoeba histolytica and Giardia lamblia to some medicinal plants used by the people of Southern Mexico. Phytother. Res. 1998, 12, 70–72. [Google Scholar] [CrossRef]
- Calzada, F.; Meckes, M.; Cedillo-Rivera, R. Antiamoebic and antigiardial activity of plant flavonoids. Planta Med. 1999, 65, 78–80. [Google Scholar] [CrossRef]
- Meckes, M.; Calzada, F.; Tapia-Contreras, A.; Cedillo-Rivera, R. Antiprotozoal properties of Helianthemum glomeratum. Phytother. Res. 1999, 13, 102–105. [Google Scholar] [CrossRef]
- Scio, E.; Ribeiro, A.; Alves, T.M.; Romanha, A.J.; Dias de Souza Filho, J.; Cordell, G.A.; Zani, C.L. Diterpenes from Alomia myriadenia (Asteraceae) with cytotoxic and trypanocidal activity. Phytochemistry 2003, 64, 1125–1131. [Google Scholar] [CrossRef]
- Muzitano, M.F.; Tinoco, L.W.; Guette, C.; Kaiser, C.R.; Rossi-Bergmann, B.; Costa, S.S. The antileishmanial activity assessment of unusual flavonoids from Kalanchoe pinnata. Phytochemistry 2006, 67, 2071–2077. [Google Scholar] [CrossRef]
- de Monbrison, F.; Maitrejean, M.; Latour, C.; Bugnazet, F.; Peyron, F.; Barron, D.; Picot, S. In vitro antimalarial activity of flavonoid derivatives dehydrosilybin and 8-(1;1)-DMA-kaempferide. Acta Trop. 2006, 97, 102–107. [Google Scholar] [CrossRef] [PubMed]
- Cai, S.; Risinger, A.L.; Nair, S.; Peng, J.; Anderson, T.J.; Du, L.; Powell, D.R.; Mooberry, S.L.; Cichewicz, R.H. Identification of Compounds with Efficacy against Malaria Parasites from Common North American Plants. J. Nat. Prod. 2016, 79, 490–498. [Google Scholar] [CrossRef]
- Pérez-González, M.Z.; Gutiérrez-Rebolledo, G.A.; Yépez-Mulia, L.; Rojas-Tomé, I.S.; Luna-Herrera, J.; Jiménez-Arellanes, M.A. Antiprotozoal, antimycobacterial, and anti-inflammatory evaluation of Cnidoscolus chayamansa (Mc Vaugh) extract and the isolated compounds. Biomed Pharmacother. 2017, 89, 89–97. [Google Scholar] [CrossRef] [PubMed]
- Araújo, M.V.; Queiroz, A.C.; Silva, J.F.M.; Silva, A.E.; Silva, J.K.S.; Silva, G.R.; Silva, E.C.O.; Souza, S.T.; Fonseca, E.J.S.; Camara, C.A.; et al. Flavonoids induce cell death in Leishmania amazonensis: In vitro characterization by flow cytometry and Raman spectroscopy. Analyst 2019, 144, 5232–5244. [Google Scholar] [CrossRef] [PubMed]
- Alotaibi, A.; Ebiloma, G.U.; Williams, R.; Alfayez, I.A.; Natto, M.J.; Alenezi, S.; Siheri, W.; AlQarni, M.; Igoli, J.O.; Fearnley, J.; et al. Activity of Compounds from Temperate Propolis against Trypanosoma brucei and Leishmania mexicana. Molecules 2021, 26, 3912. [Google Scholar] [CrossRef] [PubMed]
- Abdallah, R.M.; Hammoda, H.M.; Radwan, M.M.; El-Gazzar, N.S.; Wanas, A.S.; ElSohly, M.A.; El-Demellawy, M.A.; Abdel-Rahman, N.M.; Sallam, S.M. Phytochemical and pharmacological appraisal of the aerial parts of Lotus corniculatus L. growing in Egypt. Nat. Prod. Res. 2021, 35, 5914–5917. [Google Scholar] [CrossRef]
- Martínez-Castillo, M.; Pacheco-Yepez, J.; Flores-Huerta, N.; Guzmán-Téllez, P.; Jarillo-Luna, R.A.; Cárdenas-Jaramillo, L.M.; Campos-Rodríguez, R.; Shibayama, M. Flavonoids as a Natural Treatment Against Entamoeba histolytica. Front. Cell Infect. Microbiol. 2018, 8, 209. [Google Scholar] [CrossRef]
- Simarro, P.P.; Cecchi, G.; Paone, M.; Franco, J.R.; Diarra, A.; Ruiz, J.A.; Fèvre, E.M.; Courtin, F.; Mattioli, R.C.; Jannin, J.G. The Atlas of human African trypanosomiasis: A contribution to global mapping of neglected tropical diseases. Int. J. Health Geogr. 2010, 9, 57. [Google Scholar] [CrossRef]
- Desquesnes, M.; Dia, M.L. Mechanical transmission of Trypanosoma congolense in cattle by the African tabanid Atylotus agrestis. Exp. Parasitol. 2003, 105, 226–231. [Google Scholar] [CrossRef]
- Desquesnes, M.; Dia, M.L. Trypanosoma vivax: Mechanical transmission in cattle by one of the most common African tabanids, Atylotus agrestis. Exp. Parasitol. 2003, 103, 35–43. [Google Scholar] [CrossRef]
- Büscher, P.; Bart, J.M.; Boelaert, M.; Bucheton, B.; Cecchi, G.; Chitnis, N.; Courtin, D.; Figueiredo, L.M.; Franco, J.R.; Grébaut, P.; et al. Do Cryptic Reservoirs Threaten Gambiense-Sleeping Sickness Elimination? Trends Parasitol. 2018, 34, 197–207. [Google Scholar] [CrossRef] [PubMed]
- Bouteille, B.; Oukem, O.; Bisser, S.; Dumas, M. Treatment perspectives for human African trypanosomiasis. Fundam. Clin. Pharmacol. 2003, 17, 171–181. [Google Scholar] [CrossRef] [PubMed]
- Gao, J.M.; Qian, Z.Y.; Hide, G.; Lai, D.H.; Lun, Z.R.; Wu, Z.D. Human African trypanosomiasis: The current situation in endemic regions and the risks for non-endemic regions from imported cases. Parasitology 2020, 147, 922–931. [Google Scholar] [CrossRef]
- Baker, N.; de Koning, H.P.; Mäser, P.; Horn, D. Drug resistance in African trypanosomiasis: The melarsoprol and pentamidine story. Trends Parasitol. 2013, 29, 110–118. [Google Scholar] [CrossRef] [PubMed]
- Calzada, F.; Cedillo-Rivera, R.; Mata, R. Antiprotozoal activity of the constituents of Conyza filaginoides. J. Nat. Prod. 2001, 64, 671–673. [Google Scholar] [CrossRef] [PubMed]
- Kozykeyeva, R.A.; Datkhayev, U.M.; Srivedavyasasri, R.; Ajayi, T.O.; Patsayev, A.K.; Kozykeyeva, R.A.; Ross, S.A. Isolation of Chemical Compounds and Essential Oil from Agrimonia asiatica Juz. and Their Antimicrobial and Antiplasmodial Activities. Sci. World J. 2020, 2020, 7821310. [Google Scholar] [CrossRef] [PubMed]
- Heredia Díaz, Y.; Tuenter, E.; Garcia-Díaz, J.; Ochoa Pacheco, A.; Cos, P.; Pieters, L.; Escalona Arranz, J.C. Novel flavonol-3-O-methylethers from Zanthoxylum pistaciifolium Griseb. (Rutaceae). Nat. Prod. Res. 2021, 36, 4869–4878. [Google Scholar] [CrossRef]
- Antinori, S.; Galimberti, L.; Milazzo, L.; Corbellino, M. Biology of human malaria plasmodia including Plasmodium knowlesi. Mediterr. J. Hematol. Infect. Dis. 2012, 4, e2012013. [Google Scholar] [CrossRef]
- Singh, B.; Daneshvar, C. Human infections and detection of Plasmodium knowlesi. Clin. Microbiol. Rev. 2013, 26, 165–184. [Google Scholar] [CrossRef]
- Ashley, E.A.; Pyae Phyo, A.; Woodrow, C.J. Malaria. Lancet 2018, 391, 1608–1621. [Google Scholar] [CrossRef]
- Vuk, I.; Rajic, Z.; Zorc, B. Malaria and antimalarial drugs. Farm. Glas. 2008, 64, 51. [Google Scholar]
- Josling, G.A.; Llinás, M. Sexual development in Plasmodium parasites: Knowing when it’s time to commit. Nat. Rev. Microbiol. 2015, 13, 573–587. [Google Scholar] [CrossRef] [PubMed]
- Cowman, A.F.; Healer, J.; Marapana, D.; Marsh, K. Malaria: Biology and Disease. Cell 2016, 167, 610–624. [Google Scholar] [CrossRef]
- Castelli, F.; Tomasoni, L.R.; Matteelli, A. Advances in the treatment of malaria. Mediterr. J. Hematol. Infect. Dis. 2012, 4, e2012064. [Google Scholar] [CrossRef] [PubMed]
- Menard, D.; Dondorp, A. Antimalarial Drug Resistance: A Threat to Malaria Elimination. Cold Spring Harb. Perspect. Med. 2017, 7, a025619. [Google Scholar] [CrossRef]
- Lipan, L.; Alexandru, M.; Dedu, A.; Viaşu, A.; Piţigoi, D.; Rafila, A. Current state of the epidemiology of malaria in Romania. Bacteriol. Virusol. Parazitol. Epidemiol. 2011, 56, 25–38. [Google Scholar] [PubMed]
- Rashid, M.I.; Fareed, M.I.; Rashid, H.; Aziz, H.; Ehsan, N.; Khalid, S.; Ghaffar, I.; Ali, R.; Gul, A.; Hakeem, K.R. Flavonoids and Their Biological Secrets. In Plant and Human Health, Volume 2: Phytochemistry and Molecular Aspects; Ozturk, M., Hakeem, K.R., Eds.; Springer International Publishing: Cham, Switzerland, 2019; pp. 579–605. [Google Scholar] [CrossRef]
- Ortiz, S.; Vásquez-Ocmín, P.G.; Cojean, S.; Bouzidi, C.; Michel, S.; Figadère, B.; Grougnet, R.; Boutefnouchet, S.; Maciuk, A. Correlation study on methoxylation pattern of flavonoids and their heme-targeted antiplasmodial activity. Bioorg. Chem. 2020, 104, 104243. [Google Scholar] [CrossRef] [PubMed]
- Torres-Guerrero, E.; Quintanilla-Cedillo, M.R.; Ruiz-Esmenjaud, J.; Arenas, R. Leishmaniasis: A review. F1000Res 2017, 6, 750. [Google Scholar] [CrossRef]
- Andrade-Narváez, F.J.; Vargas-González, A.; Canto-Lara, S.B.; Damián-Centeno, A.G. Clinical picture of cutaneous leishmaniases due to Leishmania (Leishmania) mexicana in the Yucatan peninsula, Mexico. Mem. Inst. Oswaldo Cruz. 2001, 96, 163–167. [Google Scholar] [CrossRef]
- Mann, S.; Frasca, K.; Scherrer, S.; Henao-Martínez, A.F.; Newman, S.; Ramanan, P.; Suarez, J.A. A Review of Leishmaniasis: Current Knowledge and Future Directions. Curr. Trop. Med. Rep. 2021, 8, 121–132. [Google Scholar] [CrossRef]
- Periferakis, A.; Caruntu, A.; Periferakis, A.-T.; Scheau, A.-E.; Badarau, I.A.; Caruntu, C.; Scheau, C. Availability, Toxicology and Medical Significance of Antimony. Int. J. Environ. Res. Public Health 2022, 19, 4669. [Google Scholar] [CrossRef] [PubMed]
- Frézard, F.; Demicheli, C.; Ribeiro, R.R. Pentavalent antimonials: New perspectives for old drugs. Molecules 2009, 14, 2317–2336. [Google Scholar] [CrossRef] [PubMed]
- Marques, S.A.; Merlotto, M.R.; Ramos, P.M.; Marques, M.E.A. American tegumentary leishmaniasis: Severe side effects of pentavalent antimonial in a patient with chronic renal failure. An. Bras. De Dermatol. 2019, 94, 355–357. [Google Scholar] [CrossRef]
- Vasarri, M.; Barletta, E.; Vinci, S.; Ramazzotti, M.; Francesconi, A.; Manetti, F.; Degl’Innocenti, D. Annona cherimola Miller fruit as a promising candidate against diabetic complications: An in vitro study and preliminary clinical results. Foods 2020, 9, 1350. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Solís, J.; Calzada, F.; Barbosa, E.; Valdés, M. Antihyperglycemic and antilipidemic properties of a tea infusion of the leaves from Annona cherimola miller on streptozocin-induced type 2 diabetic mice. Molecules 2021, 26, 2408. [Google Scholar] [CrossRef] [PubMed]
- Galani, V.J.; Patel, B.G.; Patel, N.B. Argyreia speciosa (Linn. f.) sweet: A comprehensive review. Pharmacogn. Rev. 2010, 4, 172–178. [Google Scholar] [CrossRef]
- Joseph, A.; Mathew, S.; Skaria, B.P.; Sheeja, E. Medicinal uses and biological activities of Argyreia speciosa sweet (Hawaiian baby woodrose)-an overview. Indian J. Nat. Prod. Resour. 2011, 2, 286–291. [Google Scholar]
- Ullah, M.; Khan, M.U.; Mahmood, A.; Malik, R.N.; Hussain, M.; Wazir, S.M.; Daud, M.; Shinwari, Z.K. An ethnobotanical survey of indigenous medicinal plants in Wana district south Waziristan agency, Pakistan. J. Ethnopharmacol. 2013, 150, 918–924. [Google Scholar] [CrossRef]
- Mali, R.G.; Mahajan, S.G.; Mehta, A.A. Phcog Rev.: Plant review Rakta Kanchan (Bauhinia variegata): Chemistry traditional and medicinal uses—A review. Pharmacogn. Rev. 2007, 1, 314–319. [Google Scholar]
- Dhale, D. Phytochemical screening and antimicrobial activity of Bauhinia variegata Linn. J. Ecobiotechnol. 2011, 3, 4–7. [Google Scholar]
- Akinpelu, D.A. Antimicrobial activity of Bryophyllum pinnatum leaves. Fitoterapia 2000, 71, 193–194. [Google Scholar] [CrossRef] [PubMed]
- Kamboj, A.; Saluja, A. Bryophyllum pinnatum (Lam.) Kurz.: Phytochemical and pharmacological profile: A review. Pharmacogn. Rev. 2009, 3, 364. [Google Scholar]
- Youssef, F.S.; Ashour, M.L.; El-Beshbishy, H.A.; Singab, A.N.B.; Wink, M. Metabolic Profiling of Buddleia indica Leaves using LC/MS and Evidence of their Antioxidant and Hepatoprotective Activity Using Different In Vitro and In Vivo Experimental Models. Antioxidants 2019, 8, 412. [Google Scholar] [CrossRef]
- Yao, R.Y.; Zou, Y.F.; Chen, X.F. Traditional Use, Pharmacology, Toxicology, and Quality Control of Species in Genus Bupleurum L. Chin. Herb. Med. 2013, 5, 245–255. [Google Scholar] [CrossRef] [PubMed]
- Dang, Z.; Li, Q.; Sun, S.; Wang, Y.; Lin, R.; Zhang, Y.; Dai, J.; Zheng, N. The Medicinal Plant Pair Bupleurum chinense-Scutellaria baicalensis—Metabolomics and Metallomics Analysis in a Model for Alcoholic Liver Injury. Front. Pharmacol. 2019, 10, 254. [Google Scholar] [CrossRef] [PubMed]
- Angelica, B.C.; Maria, R.A.V.A.; Gabino, A.M.G.; Patricia, S.S.M.; Rafael, P.P. The traditional medicinal and food uses of four plants in Oaxaca, Mexico. J. Med. Plants Res. 2011, 5, 3404–3411. [Google Scholar]
- Barbosa, E.; Calzada, F.; Campos, R. In vivo antigiardial activity of three flavonoids isolated of some medicinal plants used in Mexican traditional medicine for the treatment of diarrhea. J. Ethnopharmacol. 2007, 109, 552–554. [Google Scholar] [CrossRef]
- Aponte, J.C.; Vaisberg, A.J.; Rojas, R.; Caviedes, L.; Lewis, W.H.; Lamas, G.; Sarasara, C.; Gilman, R.H.; Hammond, G.B. Isolation of Cytotoxic Metabolites from Targeted Peruvian Amazonian Medicinal Plants. J. Nat. Prod. 2008, 71, 102–105. [Google Scholar] [CrossRef]
- Tetik, F.; Civelek, S.; Cakilcioglu, U. Traditional uses of some medicinal plants in Malatya (Turkey). J. Ethnopharmacol. 2013, 146, 331–346. [Google Scholar] [CrossRef]
- Meckes, M.; Torres, J.; Calzada, F.; Rivera, J.; Camorlinga, M.; Lemus, H.; Rodríguez, G. Antibacterial Properties of Helianthemum glomeratum, a Plant Used in Maya Traditional Medicine to Treat Diarrhoea. Phytother. Res. 1997, 11, 128–131. [Google Scholar] [CrossRef]
- Yang, X.; Summerhurst, D.K.; Koval, S.F.; Ficker, C.; Smith, M.L.; Bernards, M.A. Isolation of an antimicrobial compound from Impatiens balsamina L. using bioassay-guided fractionation. Phytother. Res. 2001, 15, 676–680. [Google Scholar] [CrossRef] [PubMed]
- Li, Q.; Cao, J.; Yuan, W.; Li, M.; Yang, L.; Sun, Y.; Wang, X.; Zhao, Y. New triterpene saponins from flowers of Impatiens balsamina L. and their anti-hepatic fibrosis activity. J. Funct. Foods 2017, 33, 188–193. [Google Scholar] [CrossRef]
- Costa, S.S.; Muzitano, M.F.; Camargo, L.M.M.; Coutinho, M.A.S. Therapeutic Potential of Kalanchoe Species: Flavonoids and other Secondary Metabolites. Nat. Prod. Commun. 2008, 3, 1934578X0800301236. [Google Scholar] [CrossRef]
- Abdullah, N.; Hosseinpour Chermahini, D.S.; Chua, L.S.; Sarmidi, M. Labisia pumila: A review on its traditional, phytochemical and biological uses. World Appl. Sci. J. 2013, 27, 1297–1306. [Google Scholar] [CrossRef]
- Zakaria, A.A.; Noor, M.H.M.; Ahmad, H.; Hassim, H.A.; Mazlan, M.; Latip, M.Q.A. A Review on Therapeutic Effects of Labisia pumila on Female Reproductive Diseases. Biomed Res. Int. 2021, 2021, 9928199. [Google Scholar] [CrossRef] [PubMed]
- Zmeeva, O.; Kolomiets, N.; Abramets, N.; Bondarchuk, R. Lotus corniculatus L. is a perspective species of the genus Lotus L. 2017, 5–14. [Google Scholar]
- Gürağaç Dereli, F.T.; Khan, H.; Sobarzo-Sánchez, E.; Akkol, E.K. Antidepressant Potential of Lotus corniculatus L. subsp. corniculatus: An Ethnobotany Based Approach. Molecules 2020, 25, 1299. [Google Scholar] [CrossRef]
- Germano, M.; Sanogo, R.; Costa, C.; Fulco, R.; D’angelo, V.; Torre, E.; Viscomi, M.; De Pasquale, R. Hepatoprotective properties in the rat of Mitracarpus scaber (Rubiaceae). J. Pharm. Pharmacol. 1999, 51, 729–734. [Google Scholar] [CrossRef]
- Meite, S.; N’guessan, J.; Bahi, C.; Yapi, H.; Djaman, A.; Guina, F.G. Antidiarrheal activity of the ethyl acetate extract of Morinda morindoides in rats. Trop. J. Pharm. Res. 2009, 8, 201–207. [Google Scholar] [CrossRef]
- Mohammed, A.; Tam, D.N.H.; Vu, T.L.H.; Tieu, T.M.; Elfaituri, M.K.; Trinh, N.N.; Sagheir, E.A.; Tran, L.; Loc, T.T.H.; Low, S.K.; et al. Morinda morindoides: A systematic review of its therapeutic activities. South Afr. J. Bot. 2020, 131, 93–103. [Google Scholar] [CrossRef]
- Suriyaphan, O. Nutrition, health benefits and applications of Pluchea indica (L.) Less leaves. Mahidol Univ. J. Pharm. Sci. 2014, 41, 1–10. [Google Scholar]
- Vongsak, B.; Kongkiatpaiboon, S.; Jaisamut, S.; Konsap, K. Comparison of active constituents, antioxidant capacity, and α-glucosidase inhibition in Pluchea indica leaf extracts at different maturity stages. Food Biosci. 2018, 25, 68–73. [Google Scholar] [CrossRef]
- Kuropatnicki, A.K.; Szliszka, E.; Krol, W. Historical aspects of propolis research in modern times. Evid Based Complement Altern. Med. 2013, 2013, 964149. [Google Scholar] [CrossRef] [PubMed]
- Rusanov, K.; Kovacheva, N.; Vosman, B.; Zhang, L.; Rajapakse, S.; Atanassov, A.; Atanassov, I. Microsatellite analysis of Rosa damascena Mill. accessions reveals genetic similarity between genotypes used for rose oil production and old Damask rose varieties. Theor. Appl. Genet. 2005, 111, 804–809. [Google Scholar] [CrossRef]
- Dalfardi, B.; Heydari, M.; Golzari, S.E.J.; Mahmoudi Nezhad, G.S.; Hashempur, M.H. Al-Baghdadi’s description of venous blood circulation. Int. J. Cardiol. 2014, 174, 209–210. [Google Scholar] [CrossRef]
- Mahboubi, M. Rosa damascena as holy ancient herb with novel applications. J. Tradit. Complement. Med. 2016, 6, 10–16. [Google Scholar] [CrossRef]
- Nayebi, N.; Khalili, N.; Kamalinejad, M.; Emtiazy, M. A systematic review of the efficacy and safety of Rosa damascena Mill. with an overview on its phytopharmacological properties. Complement. Ther. Med. 2017, 34, 129–140. [Google Scholar] [CrossRef]
- Vlachou, G.; Papafotiou, M.; Akoumianaki, A.; Bertsouklis, K.F. Propagation of Scabiosa hymettia (Boiss. & Spruner) by stem cuttings. Acta Hortic. 2019, 1242, 763–766. [Google Scholar]
- Siqueira, S.; dos Santos Falcão-Silva, V.; de Fátima Agra, M.; Dariva, C.; de Siqueira-Júnior, J.P.; Fonseca, M.J.V. Biological activities of Solanum paludosum Moric. extracts obtained by maceration and supercritical fluid extraction. J. Supercrit. Fluids 2011, 58, 391–397. [Google Scholar] [CrossRef]
- El-Saber Batiha, G.; Alkazmi, L.M.; Wasef, L.G.; Beshbishy, A.M.; Nadwa, E.H.; Rashwan, E.K. Syzygium aromaticum L. (Myrtaceae): Traditional Uses, Bioactive Chemical Constituents, Pharmacological and Toxicological Activities. Biomolecules 2020, 10, 202. [Google Scholar] [CrossRef]
- Ngbolua, K.; Tshibangu, D.; Mpiana, P.; Mihigo, S.; Mavakala, B.; Ashande, M.; Muanyishay, L. Anti-sickling and antibacterial activities of Some Extracts from Gardenia ternifolia subsp. jovis-tonantis (Welw.) Verdc.(Rubiaceae) and Uapaca heudelotii Baill.(Phyllanthaceae). Infection 2015, 4, 6. [Google Scholar] [CrossRef]
- Asante-Kwatia, E.; Gyimah, L.; Mensah, A.Y.; Sarpong, K.; Obeng, A.K. Authentication and quality control of Uapaca heudelotii Baill.—An investigation of pharmacognostic, phytochemical and physicochemical properties of its leaves and stem bark. Plant Sci. Today 2022, 9, 477–485. [Google Scholar] [CrossRef]
- Baviloni, P.D.; dos Santos, M.P.; Aiko, G.M.; de Lima Reis, S.R.; Latorraca, M.Q.; da Silva, V.C.; Dall’Oglio, E.L.; de Sousa Júnior, P.T.; Lopes, C.F.; Baviera, A.M.; et al. Mechanism of anti-hyperglycemic action of Vatairea macrocarpa (Leguminosae): Investigation in peripheral tissues. J. Ethnopharmacol. 2010, 131, 135–139. [Google Scholar] [CrossRef] [PubMed]
- Patel, S. Yucca: A medicinally significant genus with manifold therapeutic attributes. Nat. Prod. Bioprospecting 2012, 2, 231–234. [Google Scholar] [CrossRef]
- Andrews, C.M.; Wyne, K.; Svenson, J.E. The use of traditional and complementary medicine for diabetes in rural Guatemala. J. Health Care Poor Underserved 2018, 29, 1188–1208. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.-P.; Woerdenbag, H.J. Traditional Chinese herbal medicine. Pharm. World Sci. 1995, 17, 103–112. [Google Scholar] [CrossRef]
- Gu, S.; Pei, J. Innovating Chinese Herbal Medicine: From Traditional Health Practice to Scientific Drug Discovery. Front. Pharmacol. 2017, 8, 381. [Google Scholar] [CrossRef]
- Gongwang, L. Chinese Herbal Medicine; Hua Xia Publishing House: Beijing, China, 1999. [Google Scholar]
- Bensky, D.; Barolet, R. Chinese Herbal Medicine—Formulas & Strategies; Eastland Press Inc.: Seattle, WA, USA, 1990. [Google Scholar]
- Yang, F.; Dong, X.; Yin, X.; Wang, W.; You, L.; Ni, J. Radix Bupleuri: A Review of Traditional Uses, Botany, Phytochemistry, Pharmacology, and Toxicology. Biomed Res. Int. 2017, 2017, 7597596. [Google Scholar] [CrossRef]
- Cheng, Y.L.; Chang, W.L.; Lee, S.C.; Liu, Y.G.; Lin, H.C.; Chen, C.J.; Yen, C.Y.; Yu, D.S.; Lin, S.Z.; Harn, H.J. Acetone extract of Bupleurum scorzonerifolium inhibits proliferation of A549 human lung cancer cells via inducing apoptosis and suppressing telomerase activity. Life Sci. 2003, 73, 2383–2394. [Google Scholar] [CrossRef]
- Chiang, L.C.; Ng, L.T.; Liu, L.T.; Shieh, D.E.; Lin, C.C. Cytotoxicity and anti-hepatitis B virus activities of saikosaponins from Bupleurum species. Planta Med. 2003, 69, 705–709. [Google Scholar] [CrossRef]
- Xie, Y.; Lu, W.; Cao, S.; Jiang, X.; Yin, M.; Tang, W. Preparation of bupleurum nasal spray and evaluation on its safety and efficacy. Chem. Pharm. Bull. 2006, 54, 48–53. [Google Scholar] [CrossRef] [PubMed]
- Xie, J.Y.; Di, H.Y.; Li, H.; Cheng, X.Q.; Zhang, Y.Y.; Chen, D.F. Bupleurum chinense DC polysaccharides attenuates lipopolysaccharide-induced acute lung injury in mice. Phytomedicine 2012, 19, 130–137. [Google Scholar] [CrossRef] [PubMed]
- Zhu, J.; Luo, C.; Wang, P.; He, Q.; Zhou, J.; Peng, H. Saikosaponin A mediates the inflammatory response by inhibiting the MAPK and NF-κB pathways in LPS-stimulated RAW 264.7 cells. Exp. Ther. Med. 2013, 5, 1345–1350. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.Y.; Sun, H.M.; Xing, J.; Qin, X.M.; Du, G.H. Chemical and biological comparison of raw and vinegar-baked Radix Bupleuri. J. Ethnopharmacol. 2015, 165, 20–28. [Google Scholar] [CrossRef] [PubMed]
- He, C.; Chen, J.; Liu, J.; Li, Y.; Zhou, Y.; Mao, T.; Li, Z.; Qin, X.; Jin, S. Geranium wilfordii maxim.: A review of its traditional uses, phytochemistry, pharmacology, quality control and toxicology. J. Ethnopharmacol. 2022, 285, 114907. [Google Scholar] [CrossRef]
- Huang, M.; Yao, P.W.; Chang, M.D.; Ng, S.K.; Yu, C.H.; Zhang, Y.F.; Wen, M.L.; Yang, X.Y.; Lai, Y.K. Identification of anti-inflammatory fractions of Geranium wilfordii using tumor necrosis factor-alpha as a drug target on Herbochip®—An array-based high throughput screening platform. BMC Complement. Altern. Med. 2015, 15, 146. [Google Scholar] [CrossRef] [PubMed]
- Tilikidis, A. Chinese Herbal Therapy—Herbs and Formulas; Akadimia of Ancient Greek and Traditional Chinese Medicine Athens: Athens, Greece, 2017. (In Greek) [Google Scholar]
- Amiri, M.S.; Joharchi, M.R.; Nadaf, M.; Nasseh, Y. Ethnobotanical knowledge of Astragalus spp.: The world’s largest genus of vascular plants. Avicenna J. Phytomed. 2020, 10, 128–142. [Google Scholar]
- Lev, E.; Amar, Z. Ethnopharmacological survey of traditional drugs sold in the Kingdom of Jordan. J. Ethnopharmacol. 2002, 82, 131–145. [Google Scholar] [CrossRef]
- Chaudhary, L.B.; Rana, T.S.; Anand, K.K. Current status of the systematics of Astragalus L.(Fabaceae) with special reference to the Himalayan species in India. Taiwania 2008, 53, 338–355. [Google Scholar]
- Kumar, G.P.; Gupta, S.; Murugan, M.P.; Bala Singh, S. Ethnobotanical studies of Nubra Valley-A cold arid zone of Himalaya. Ethnobot. Leafl. 2009, 2009, 9. [Google Scholar]
- Ghasemi Pirbalouti, A.; Momeni, M.; Bahmani, M. Ethnobotanical study of medicinal plants used by Kurd tribe in Dehloran and Abdanan Districts, Ilam Province, Iran. Afr. J. Tradit. Complement. Altern. Med. 2013, 10, 368–385. [Google Scholar] [CrossRef] [PubMed]
- Dexter, D.F.; Martin, K.; Travis, L. Prehistoric plant use at beaver creek rock shelter, Southwestern Montana, USA. Ethnobot. Res. Appl. 2014, 12, 355–384. [Google Scholar] [CrossRef][Green Version]
- Chermat, S.; Gharzouli, R. Ethnobotanical study of medicinal flora in the North East of Algeria-An empirical knowledge in Djebel Zdimm (Setif). J. Mater. Sci. Eng. 2015, 5, 50–59. [Google Scholar]
- Lakhdari, W.; Dehliz, A.; Acheuk, F.; Mlik, R.; Hammi, H.; DOUMANDJI-MITICHE, B.; Gheriani, S.; Berrekbia, M.; Guermit, K.; Chergui, S. Ethnobotanical study of some plants used in traditional medicine in the region of Oued Righ (Algerian Sahara). J. Med. Plants 2016, 4, 204–211. [Google Scholar]
- Sun, L.; Liao, L.; Wang, B. Potential Antinociceptive Effects of Chinese Propolis and Identification on Its Active Compounds. J. Immunol. Res. 2018, 2018, 5429543. [Google Scholar] [CrossRef]
- Zhu, W.; Chen, M.; Shou, Q.; Li, Y.; Hu, F. Biological activities of chinese propolis and brazilian propolis on streptozotocin-induced type 1 diabetes mellitus in rats. Evid. -Based Complement. Altern. Med. 2011, 2011, 468529. [Google Scholar] [CrossRef]
- Periferakis, A.; Bolocan, A.; Ion, D. A Review of Innovation in Medicine. Technol. Innov. Life Sci. 2022, 1, 42–48. [Google Scholar] [CrossRef]
- Newman, D.J.; Cragg, G.M. Natural Products as Sources of New Drugs over the Nearly Four Decades from 01/1981 to 09/2019. J. Nat. Prod. 2020, 83, 770–803. [Google Scholar] [CrossRef]
- Scheau, C.; Mihai, L.; Bădărău, I.; Caruntu, C. Emerging applications of some important natural compounds in the field of oncology. Farmacia 2020, 68, 984–991. [Google Scholar] [CrossRef]
- Dehelean, C.A.; Marcovici, I.; Soica, C.; Mioc, M.; Coricovac, D.; Iurciuc, S.; Cretu, O.M.; Pinzaru, I. Plant-Derived Anticancer Compounds as New Perspectives in Drug Discovery and Alternative Therapy. Molecules 2021, 26, 1109. [Google Scholar] [CrossRef]
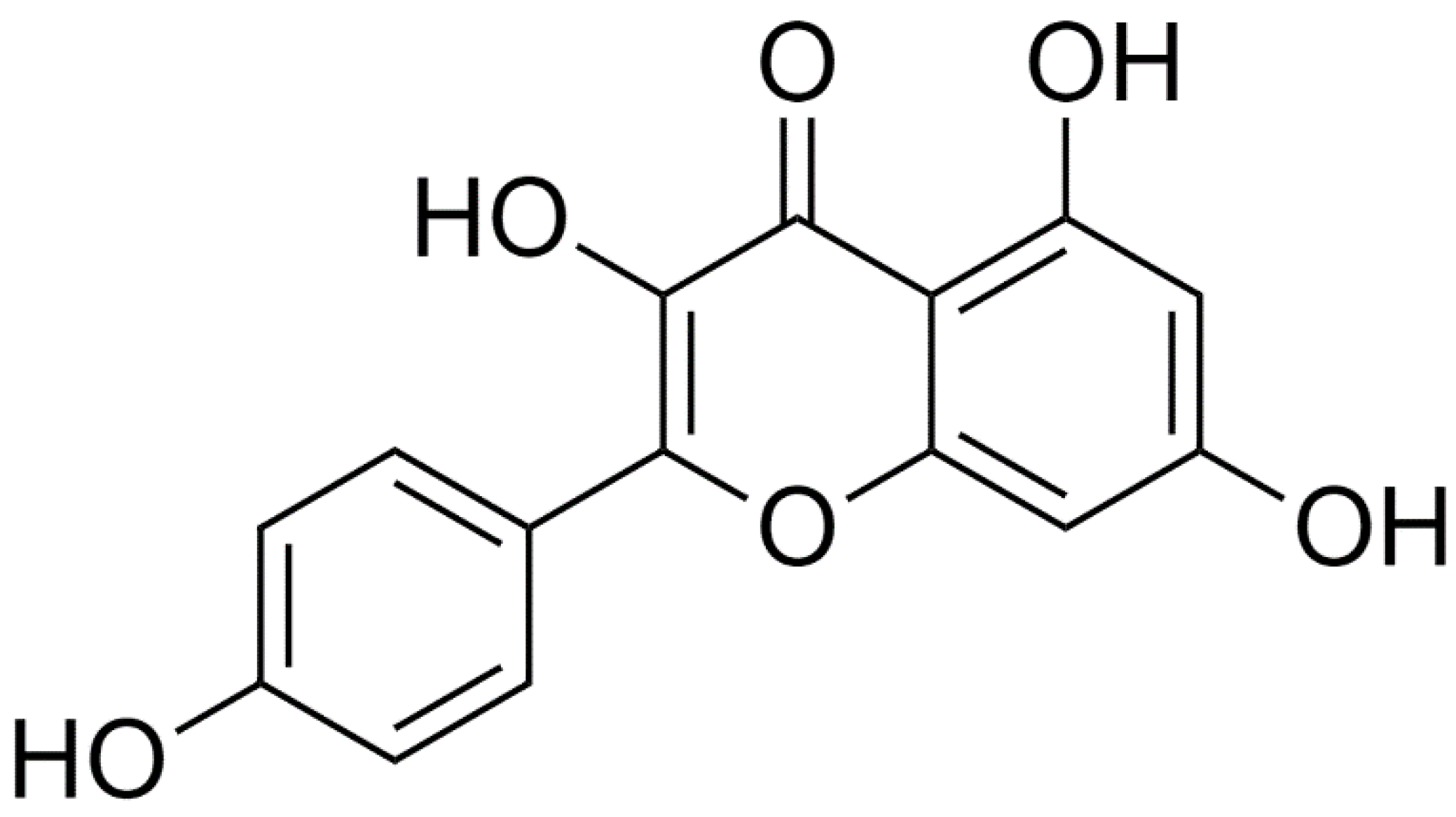
| Clade | Order | Family | Species | Reference |
|---|---|---|---|---|
| Gymnosperms, Tracheophytes | Pinales | Taxaceae | Taxus baccata | [77] |
| Mesangiosperms, Magnoliids | Canellales | Canellaceae | Warburgia stuhlmannii | [84] |
| Magnoliales | Annonaceae | Annona cherimola Miller | [85] | |
| Mesangiosperms, Monocots | Asparagales | Alliaceae | Allium cepa | [86] |
| Asphodelaceae | Aloe vera | [87] | ||
| Liliales | Liliaceae | Lilium candidum | [88] | |
| Lilium longiflorum | [89] | |||
| Smilacaceae | Smilax bockii | [90] | ||
| Mesangiosperms, Eudicots | Ranunculales | Berberidaceae | Dysosma versipellis | [91] |
| Ranunculaceae | Consolida oliveriana | [92] | ||
| Saxifragales | Crassulaceae | Orostachys japonicus | [93] | |
| Rhodiola rosea | [94] | |||
| Rhodiola sachalinensis | [95] | |||
| Kalanchoe fedtschenkoi | [96] | |||
| Vitales | Vitaceae | Parthenocissus tricuspidata | [97] | |
| Cayratia trifolia Linn | [98] | |||
| Cucurbitales | Cucurbitaceae | Gynostemma cardiospermum | [99] | |
| Fabales | Fabaceae | Astragalus creticus Lam. | [100] | |
| Tylosema esculentum | [101] | |||
| Bauhinia vahlii | [102] | |||
| Acacia nilotica | [103] | |||
| Amburana cearensis | [104] | |||
| Cassia angustifolia | [105] | |||
| Cassia siamea | [106] | |||
| Indigofera suffruticosa | [107] | |||
| Indigofera truxillensis | [107] | |||
| Oxytropis falcate | [108] | |||
| Securigera securidaca | [109] | |||
| Tadehagi triquetrum | [110] | |||
| Trifolium alexandrinum | [111] | |||
| Rosales | Elaeagnaceae | Hippophae rhamnoides | [112] | |
| Rhamnaceae | Rhamnus nakaharai | [113] | ||
| Rhamnus procumbens | [114] | |||
| Rosaceae | Prunus davidiana | [115] | ||
| Rosa spp. | [116] | |||
| Rosa damascena | [117] | |||
| Rosa hybrids | [118] | |||
| Ulmaceae | Zelkova oregoniana | [119] | ||
| Celastrales | Celastraceae | Euonymus alatus | [120] | |
| Malpighiales | Clusiaceae | Hypericum brasiliense | [121] | |
| Hypericum perforatum | [122] | |||
| Vismia laurentii | [123] | |||
| Euphorbiaceae | Elateriospermum tapos | [124] | ||
| Euphorbia aleppica | [125] | |||
| Phyllanthus acidus | [126] | |||
| Sauropus androgynus | [127] | |||
| Sebastiania brasiliensis | [128] | |||
| Salicaceae | Populus davidiana | [129] | ||
| Geraniales | Geraniaceae | Geranium carolinianum | [130] | |
| Geranium potentillaefolium | [131] | |||
| G. ibericum subs. jubatum | [132] | |||
| Pelargonium quercifolium | [133] | |||
| Brassicales | Brassicaceae | Brassica rapa | [134] | |
| Bunias orientalis | [135] | |||
| Diplotaxis erucoides | [135] | |||
| Diplotaxis tenuifolia | [135] | |||
| Malvales | Cistaceae | Helianthemum glomeratum | [136] | |
| Malvaceae | Althaea rosea | [137] | ||
| Sterculiaceae | Theobroma grandiflorum | [138] | ||
| Tiliaceae | Tilia tomentosa | [139] | ||
| Myrtales | Combretaceae | Combretum erythrophyllum | [140] | |
| Lythraceae | Cuphea pinetorum | [141] | ||
| Myrtaceae | Eucalyptus spp. | [142] | ||
| Psidium guajava | [143] | |||
| Syzygium aromaticum | [144] | |||
| Punicaceae | Punica granatum | [145] | ||
| Sapindales | Anacardiaceae | Pistacia vera | [146] | |
| Rhus verniciflua | [147] | |||
| Sapindaceae | Koelreuteria henryi | [148] | ||
| Koelreuteria paniculata | [149] | |||
| Simaroubaceae | Simarouba versicolor | [150] | ||
| Caryophyllales | Amaranthaceae | Alternanthera tenella | [151] | |
| Nepenthaceae | Nepenthes gracilis | [152] | ||
| Polygonaceae | Polygonum tinctorium | [153] | ||
| Santalales | Santalaceae | Thesium chinense | [154] | |
| Ericales | Ebenaceae | Diospyros lotus | [155] | |
| Lecythidaceae | Planchonia grandis | [156] | ||
| Myrsinoideae | Ardisia colorata | [157] | ||
| Gentianales | Apocynaceae | Echites hirsuta | [158] | |
| Rubiaceae | Morinda citrifolia | [159] | ||
| Morinda morindoides | [160] | |||
| Vahliales | Vahliaceae | Vahlia capensis | [161] | |
| Solanales | Convolvulaceae | Cuscuta australis | [162] | |
| Cuscuta chinensis | [163] | |||
| Solanaceae | Solanum nigrum | [164] | ||
| Lamiales | Oleaceae | Chionanthus retusus | [165] | |
| Olea europaea | [166] | |||
| Scrophulariaceae | Buddleja indica Lam. | [167] | ||
| Lamiaceae | Origanum dictamnus | [168] | ||
| Rosmarinus officinalis | [169] | |||
| Apiales | Apiaceae | Bunium persicum | [170] | |
| Bupleurum flavum | [171] | |||
| Bupleurum chinense | [172] | |||
| Asterales | Asteraceae | Heterotheca inuloides | [173] | |
| Chromolaena moritziana | [174] | |||
| Ixeridium gracile | [175] | |||
| Lactuca scariola | [176] | |||
| Solidago virga-aurea | [177] | |||
| Helichrysum compactum | [178] | |||
| Europatorium perfoliatum L. | [179] | |||
| Pluchea indica | [180] | |||
| Dipsacales | Caprifoliaceae | Sambucus nigra | [181] | |
| Polypodiopsida, Moniliformopses | Polypodiales | Dennstaedtiaceae | Dennstaedtia scabra | [182] |
| Polypodiopsida, Ophioglossidae | Ophioglossales | Ophioglossaceae | Ophioglossum petiolatum | [183] |
| Food | Quantity (mg/kg) | Reference |
|---|---|---|
| Capers | 2590 | [184] |
| Saffron | 2050 | [184] |
| Onion leaves | 832 | [185] |
| Arugula | 590 | [184] |
| Kale | 470 | [184] |
| Brown mustard | 380 | [184] |
| Pumpkin | 371 | [186] |
| Ginger | 340 | [184] |
| Cauliflower | 270 | [187] |
| Common beans | 260 | [184] |
| Carrot | 140 | [186] |
| Black tea | 118 | [186] |
| Chive | 100 | [184] |
| Endive | 100 | [184] |
| Collard | 90 | [184] |
| Broccoli | 80 | [184] |
| Fennel leaves | 70 | [184] |
| Goji berry (dried) | 60 | [184] |
| Green chilli | 39 | [186] |
| Strawberry | 5–8 | [188] |
| Genus | Species | Tested Substance | MIC (μg/mL) | Year of Research | Reference |
|---|---|---|---|---|---|
| Gram-Negative Bacteria | |||||
| Acinetobacter | A. baumannii | Pure kaempferol-3,7-O-α-L-dirhamnoside | 8 | 2006 | [214] |
| Extract from Kalanchoe fedtschenkoi | 128–256 | 2019 | [96] | ||
| Artificial blend with nanocrystals | n/a—no adm. of sole kaempferol | 2021 | [215] | ||
| Extract from Geranium ibericum subsp. jubatum | 400 | 2021 | [132] | ||
| Extracts from propolis | n/a—expressed as % of propolis | 2021 | [216] | ||
| Enterobacter | E. cloacae, E. aerogenes | Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] |
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Escherichia | E. coli | Pure kaempferol-3,7-O-α-L-dirhamnoside | 2 | 2006 | [214] |
| Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] | ||
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Extract from Bupleurum chinense | n/a | 2020 | [172] | ||
| Extracts from propolis | n/a—expressed as % of propolis | 2021 | [216] | ||
| Conjugation of pure kaempferol with Ag nanoparticles | 62.5 | 2021 | [217] | ||
| Extract from Rosa damascena Mill var. trigintipetala | n/a (only inh. zone data) | 2022 | [218] | ||
| Extract from Yucca gigantea | 13.3 | 2022 | [219] | ||
| Klebsiella | K. pneumoniae | Pure kaempferol-3,7-O-α-L-dirhamnoside | 4 | 2006 | [214] |
| Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] | ||
| Extract from Argyreia speciosa | 2 | 2009 | [220] | ||
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Extract from Bupleurum chinense | n/a | 2020 | [172] | ||
| Extract from Geranium ibericum subsp. jubatum | 400 | 2021 | [132] | ||
| Extract from Yucca gigantea | 12.5 | 2022 | [219] | ||
| Porphyromonas | P. gingivalis | Extract from Syzygium aromaticum | 20 | 1996 | [144] |
| Prevotella | P. intermedia | Extract from Syzygium aromaticum | 20 | 1996 | [144] |
| Proteus | P. mirabilis, P. vulgaris | Extract from Uapaca heudelotti | 2 | 2020 | [212] |
| Extract from Geranium ibericum subsp. jubatum | 300 | 2021 | [132] | ||
| Extract from Rosa damascena Mill var. trigintipetala | n/a (only inh. zone data) | 2022 | [218] | ||
| Extract from Yucca gigantea | 14.8 | 2022 | [219] | ||
| Pseudomonas | P. aeruginosa | Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] |
| Extract from Labisa pumila Benth | n/a (only inh. zone data) | 2011 | [211] | ||
| Extract from Bryophyllum pinnatum (Lank.) Oken | Various depending on extract | 2012 | [221] | ||
| Extract from Kalanchoe fedtschenkoi | 256 | 2019 | [96] | ||
| Extract from Bupleurum chinense | n/a | 2020 | [172] | ||
| Extract from Yucca gigantea | 10.2 | 2022 | [219] | ||
| Salmonella | S. typhi, S. typhimurium | Extract from Bryophyllum pinnatum (Lank.) Oken | Various depending on extract | 2012 | [221] |
| Extract from Uapaca heudelotti | 12.5 | 2020 | [212] | ||
| Extract from Yucca gigantea | 10.5 | 2022 | [219] | ||
| Vibrio | V. cholerae | Extract from Combretum erythrophyllum | n/a | 2004 | [140] |
| Gram-Positive Bacteria | |||||
| Enterococcus | E. faecium, E. faecalis | Extract from Combretum erythrophyllum | n/a | 2004 | [140] |
| Pure kaempferol-3,7-O-α-L-dirhamnoside | 0.5 | 2006 | [214] | ||
| Extract from Laurus nobilis | >256 | 2008 | [222] | ||
| Micrococcus | M. luteus | Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] |
| Staphylococcus | S. aureus, S. epidermidis | Extract from Mitracarpus scaber | 125 | 2000 | [223] |
| Pure kaempferol-3,7-O-α-L-dirhamnoside | 0.5 | 2006 | [214] | ||
| Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] | ||
| Extract from Laurus nobilis | >256 | 2008 | [222] | ||
| Extract from Allium ursinum | 625 | 2009 | [224] | ||
| Extract from Platanus occidentalis | Various depending on the kaempferol compound | 2009 | [225] | ||
| Extract from Laurus nobilis | Various depending on synergistic effects | 2009 | [206] | ||
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Extract from Bryophyllum pinnatum (Lank.) Oken | Various depending on extract | 2012 | [221] | ||
| Extract from Calliandra tergemina (L.) Benth | Various depending on extract type and compound | 2014 | [226] | ||
| Extract from Platanus occidentalis | n/a | 2015 | [227] | ||
| Extract from Kalanchoe fedtschenkoi | 256 | 2019 | [96] | ||
| Extract from Platanus occidentalis | 16 | 2020 | [228] | ||
| Extract from Bupleurum chinense | n/a | 2020 | [172] | ||
| Extract from Uapaca heudelotti | 12.5 | 2020 | [212] | ||
| Conjugation of pure kaempferol with Ag nanoparticles | n/a | 2021 | [217] | ||
| Extracts from propolis | n/a—expressed as % of propolis | 2021 | [216] | ||
| Artificial blend with nanocrystals | n/a—no adm. of sole kaempferol | 2021 | [215] | ||
| Extract from Yucca gigantea | 14.46 | 2022 | [219] | ||
| Streptococcus | S. pyogenes | Extract from Uapaca heudelotti | 6.25 | 2020 | [212] |
| Bacillus | B. subtilis, B. cereus | Pure kaempferol-3,7-O-α-L-dirhamnoside | 8 | 2006 | [214] |
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Extract from Bupleurum chinense | n/a | 2020 | [172] | ||
| Extract from Uapaca heudelotti | 6.25 | 2020 | [212] | ||
| Extract from Buddleja indica Lam. | 0.48 | 2021 | [167] | ||
| Extract from Astragalus creticus | n/a (expr. as inhibition %) | 2021 | [100] | ||
| Conjugation of pure kaempferol with Ag nanoparticles | n/a | 2021 | [217] | ||
| Extract from Rosa damascena Mill var. trigintipetala | n/a (only inh. zone data) | 2022 | [218] | ||
| Cutibacterium | C. acnes | Extract from Impatiens balsamina | 32–64 | 2007 | [208] |
| Ziehl-Neelsen Stain | |||||
| Mycobacterium | M. bovis, M. tuberculosis | Extract from Argyreia speciosa | 25 | 2009 | [220] |
| Extract from Doliocarpus dentatus | 62.5 | 2017 | [229] | ||
| Extract from Pluchea indica | n/a | 2020 | [180] | ||
| Extract from Bauhinia vahlii | n/a (expr. as inhibition %) | 2021 | [102] | ||
| Extract from Vatairea macrocarpa | n/a | 2021 | [230] | ||
| Genus | Species | Tested Substance | MIC (μg/mL) | Year of Research | Reference |
|---|---|---|---|---|---|
| Aspergillus | A. fumigatus | Extract from Rosa damascena Mill var. trigintipetala | n/a (only inh. zone data) | 2022 | [218] |
| Candida | C. albicans, C. tropicalis, C. glabrata | Extract from Mitracarpus scaber | 250–500 | 2000 | [223] |
| Pure kaempferol-3-O-(6”-galloyl)-β-D-glucopyranoside | 200 | 2004 | [342] | ||
| Extract from Scabiosa hymettia | n/a (only inh. zone data) | 2008 | [209] | ||
| Pure kaempferol | 25 | 2008 | [343] | ||
| Extract from Allium ursinum | >625 | 2009 | [224] | ||
| Extract from Labisa pumila Benth | Various depending on extract | 2011 | [211] | ||
| Extract from Bryophyllum pinnatum (Lank.) Oken | Various depending on extract | 2012 | [221] | ||
| Extract from Geranium ibericum subsp. jubatum | 400 | 2021 | [132] | ||
| Extract from Rosa damascena Mill var. trigintipetala | n/a (only inh. zone data) | 2022 | [218] | ||
| Bark extract from Spondias mombin | n/a | 2022 | [213] | ||
| Cryptococcus | C. neoformans | Extract from Bryophyllum pinnatum (Lank.) Oken | Various depending on extract | 2012 | [221] |
| Disease | Causative Agents | Endemic Areas | References |
|---|---|---|---|
| Amoebiasis | Entamoeba histolytica | Central and South America, Africa, India | [346,347] |
| Giardiasis | Giardia lamblia | Worldwide | [348,349] |
| Human African trypanosomiasis | Trypanosoma brucei gambiense, Trypanosoma brucei rhodensiense, Trypanosoma brucei brucei, Trypanosoma congolense, Trypanosoma evansi | Sub-Saharan (Central and West Africa) | [350] |
| Malaria | Plasmodium malariae, Plasmodium falciparum, Plasmodium vivax, Plasmodium ovale, Plasmodium knowlesi | South America, Africa, India, and South Pacific islands | [351,352] |
| Leishmaniasis | Leishmania donovani, Leishmania major, Leishmania mexicana, Leishmania tropica, etc. | Africa, Central and South Asia, Central and South America | [353,354,355] |
| Active Kaempferol Compound | Extracted from | Active against | IC50 (μg/mL) | Year of Study | References |
|---|---|---|---|---|---|
| Kaempferol | Helianthemum glomeratum | E. histolytica | 9.7 | 1995 | [136] |
| Kaempferol | Helianthemum glomeratum | E. histolytica, G. lamblia | 7.93, 8.73 | 1998 | [356] |
| Kaempferol | Helianthemum glomeratum | E. histolytica, G. lamblia | 7.93, 8.73 | 1999 | [357] |
| Kaempferol | Helianthemum glomeratum | E. histolytica, G. lamblia | 7.93, 8.73 | 1999 | [358] |
| Kaempferol-7-methylether | Alomia myriadenia | T. cruzi | n/a (expressed as % of T. cruzi lysis) | 2003 | [359] |
| Kaempferol | Cuphea pinetorum | E. histolytica, G. lamblia | 7.9–8.3 | 2005 | [141] |
| Kaempferol | Morinda morindoides | E. histolytica | Various depending on kaempferol compound | 2006 | [160] |
| Kaempferol-3-O-α-L-arabinopyranosyl (1→2)-α-L-rhamnopyranoside | Kalanchoe pinnata | Leishmania spp. | >100 | 2006 | [360] |
| 8-(1;1)-DMA-kaempferide | Pure compound | P. falciparum | n/a (expressed in μΜ) | 2006 | [361] |
| Kaempferol | Eupatorium perfoliatum L. | P. falciparum | 2.7 (whole extract) | 2011 | [179] |
| Kaempferol | Cayratia trifolia Linn | Trypanosoma spp. | n/a | 2011 | [98] |
| Kaempferol rhamnosides and glycosides | Pure compounds | Plasmidium spp. | n/a (expressed in μΜ) | 2016 | [362] |
| Kaempferol | Annona cherimola Miller | E. histolytica, G. lamblia | 7.9, 8.7 | 2017 | [85] |
| Kaempferol-3,7-dimethylether | Cnidoscolus chayamansa | E. histolytica, G. lamblia | ≤27.43 | 2017 | [363] |
| Kaempferol-3,7-di-O-methylether | Solanum paludosum Moric | L. amazonensis | n/a (expressed in μΜ) | 2019 | [364] |
| Kaempferol, 4′-methoxykaempferol, 4′,7-dimethoxykaempferol | Propolis | T. brucei, L. mexicana | n/a (expressed in μΜ) | 2021 | [365] |
| Kaempferol, kaempferol 3-O-α-L-rhamnoside, and other kaempferol compounds | Lotus corniculatus L. | Trypanosoma spp., Plasmodium spp. | 0.98, 1.57 | 2021 | [366] |
| Plant | Traditional/Ethnobotanical Uses | Uses Described in This Paper | References |
|---|---|---|---|
| Annona cherimola Miller | Traditional Mexican medicine | Antiprotozoal (against E. histolytica, G. lamblia) | [85,395,396] |
| Argyreia speciosa | Traditional Indian medicine | Antibacterial (against K. pneumoniae, M. tuberculosis) | [220,397,398] |
| Astragalus creticus | Traditional Chinese medicine, traditional Pakistani medicine | Antibacterial (against B. subtilis) | [100,399] |
| Bauhinia vahlii | Traditional Indian medicine | Antibacterial (against M. tuberculosis) | [102,400,401] |
| Bryophyllum pinatum | Traditional Chinese medicine, various traditional medical systems of tropical Africa and America, traditional Indian medicine | Antibacterial (against P. aeruginosa, S. aureus, S. typhi); antifungal (against C. neoformans) | [221,402,403] |
| Buddleja indica Lam | Traditional African medicine | Antibacterial (against B. subtilis) | [167,404] |
| Bupleurum chinense | Traditional Chinese medicine | Antibacterial (against B. subtilis, E. coli, K. pneumoniae, P. aeruginosa, S. aureus, S. aureus) | [172,405,406] |
| Cnidoscolus chayamansa | Traditional Mexican medicine | Antiprotozoal (against E. histolytica, G. lamblia) | [363,407] |
| Cuphea pinetorum | Traditional Mayan medicine, traditional Mexican medicine | Antiprotozoal (against E. histolytica, G. lamblia) | [141,408] |
| Doliocarpus dentatus | Traditional Brazilian medicine, traditional Peruvian medicine | Antibacterial (against M. tuberculosis) | [229,409] |
| Geranium ibericum jubatum | Ethnobotanical usage in Malaya, Eastern Anatolia | Antibacterial (against A. baumannii, K. pneumoniae) | [132,410] |
| Helianthemum glomeratum | Traditional Mayan medicine | Antiprotozoal (against E. histolytica, G. lamblia) | [358,411] |
| Impatiens balsamina | Traditional Chinese medicine and traditional medicinal systems of Asia | Antibacterial (against P. acnes) | [208,412,413] |
| Kalanchoe fedtschenkoi | Indian traditional medicine, traditional Chinese medicine, traditional Brazilian medicine, Traditional African medicine | Antibacterial (against A. baumannii, P. aeruginosa, S. aureus) | [96,414] |
| Labisia pumila Benth | Traditional Malayan medicine | Antibacterial (against B. cereus, B. subtilis, E. aerogenes, E. coli, K. pneumoniae, M. luteus, P. aeruginosa, S. aureus); antifungal (against C. albicans) | [211,415,416] |
| Lotus corniculatus L. | Traditional Turkish medicine, traditional Russian medicine, traditional Egyptian medicine | Antiprotozoal (against Trypanosoma spp.) | [366,417,418] |
| Mitracarpus scaber | Traditional Malian medicine | Antibacterial (against S. aureus; antifungal (against A. fumigatus) | [223,419] |
| Morinda morindoides | Various traditional African medical systems | Antiprotozoal (against E. histolytica) | [160,420,421] |
| Pluchea indica | Traditional Thai medicine, traditional Indian medicine | Antibacterial (against M. tuberculosis) | [180,422,423] |
| Propolis | Ancient Greek medicine, Ancient Roman medicine, Ancient Egyptian medicine, European medieval medical systems | Antibacterial (against A. baumannii, E. coli, S. aureus); antiprotozoan (against T. brucei, L. mexicana) | [216,365,424] |
| Rosa damascena Mill var. trigintipetala | Ancient Persian medicine, traditional Arab medicine, traditional Iranian medicine | Antibacterial (against B. subtilis, E. coli, P. vulgaris); antifungal (A. fumigatus, C. albicans) | [218,425,426,427,428] |
| Scabiosa hymettia | Traditional Greek medicine | Antibacterial (against E. coli, K. pneumoniae, P. aeruginosa, S. aureus, S. epidermidis, E. cloacae); antifungal (C. albicans, C. glabrata, C. tropicalis) | [209,429] |
| Solanum paludosum Moric | South American folk medicine | Antiprotozoal (against L. amazonensis) | [364,430] |
| Syzygium aromaticum | Various traditional medicinal systems of Asia | Antibacterial (against P. gingivalis, P. intermedia) | [144,431] |
| Uapaca heudelotii | Traditional Congolese medicine, various other local African medical traditions | Antibacterial (against S. pneumoniae, S. aureus, S. typhi, P. mirabilis, B. subtilis) | [212,432,433] |
| Uapaca heudelotti | Traditional African medicine | Antibacterial (against B. subtilis, S. aureus, S. pneumoniae, S. typhi) | [212,433] |
| Vatairea macrocarpa (Benth) Ducke | Traditional Brazilian medicine | Antibacterial (against M. bovis) | [230,434] |
| Yucca gigantea | Native American medicine, traditional Guatemalan medicine | Antibacterial (against E. coli, K. pneumoniae, P. aeruginosa, S. aureus, S. epidermidis, S. typhimurium, P. mirabilis) | [219,435,436] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Periferakis, A.; Periferakis, K.; Badarau, I.A.; Petran, E.M.; Popa, D.C.; Caruntu, A.; Costache, R.S.; Scheau, C.; Caruntu, C.; Costache, D.O. Kaempferol: Antimicrobial Properties, Sources, Clinical, and Traditional Applications. Int. J. Mol. Sci. 2022, 23, 15054. https://doi.org/10.3390/ijms232315054
Periferakis A, Periferakis K, Badarau IA, Petran EM, Popa DC, Caruntu A, Costache RS, Scheau C, Caruntu C, Costache DO. Kaempferol: Antimicrobial Properties, Sources, Clinical, and Traditional Applications. International Journal of Molecular Sciences. 2022; 23(23):15054. https://doi.org/10.3390/ijms232315054
Chicago/Turabian StylePeriferakis, Argyrios, Konstantinos Periferakis, Ioana Anca Badarau, Elena Madalina Petran, Delia Codruta Popa, Ana Caruntu, Raluca Simona Costache, Cristian Scheau, Constantin Caruntu, and Daniel Octavian Costache. 2022. "Kaempferol: Antimicrobial Properties, Sources, Clinical, and Traditional Applications" International Journal of Molecular Sciences 23, no. 23: 15054. https://doi.org/10.3390/ijms232315054
APA StylePeriferakis, A., Periferakis, K., Badarau, I. A., Petran, E. M., Popa, D. C., Caruntu, A., Costache, R. S., Scheau, C., Caruntu, C., & Costache, D. O. (2022). Kaempferol: Antimicrobial Properties, Sources, Clinical, and Traditional Applications. International Journal of Molecular Sciences, 23(23), 15054. https://doi.org/10.3390/ijms232315054











