The Advances in Epigenetics for Cancer Radiotherapy
Abstract
1. Introduction
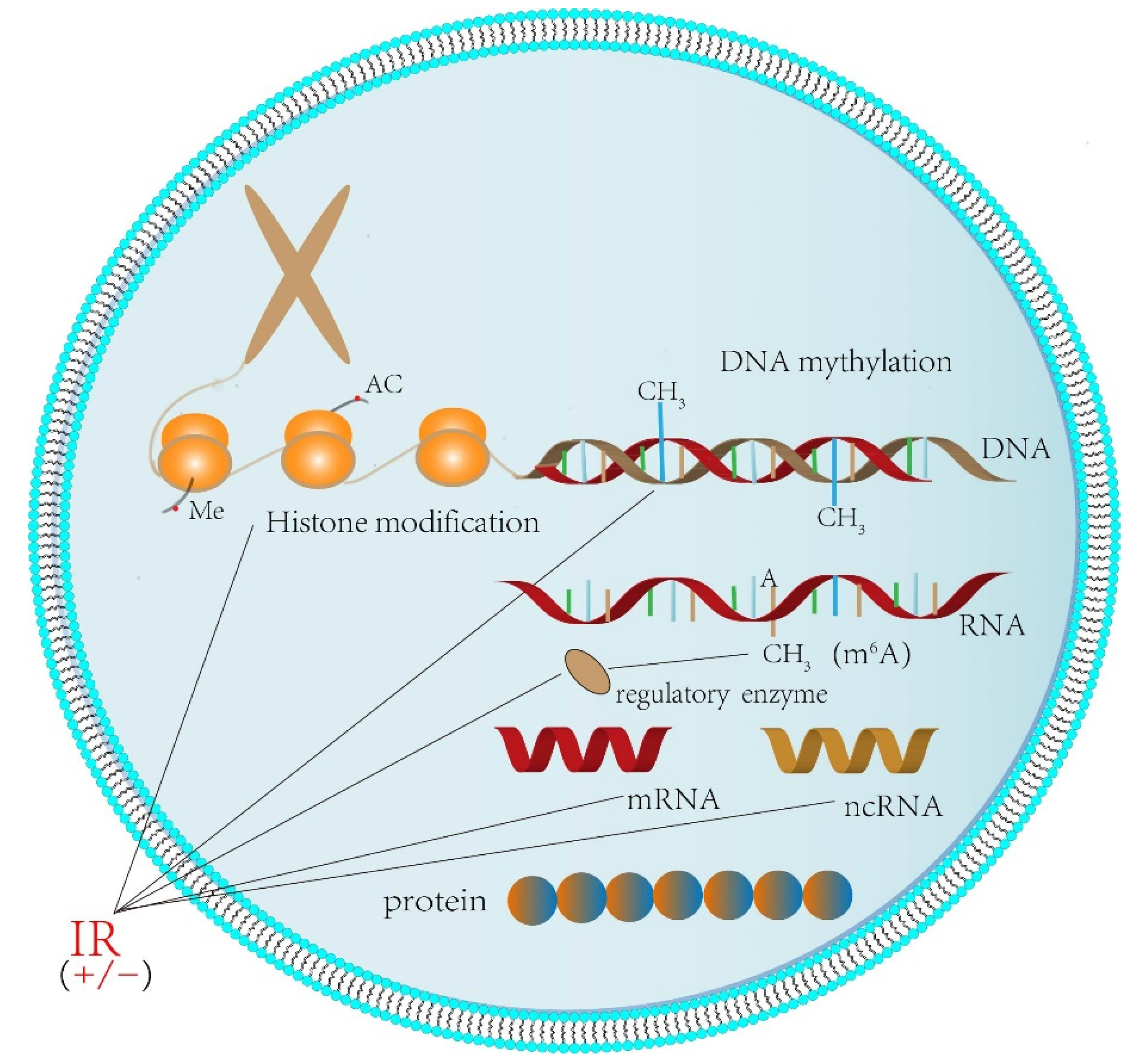
2. Epigenetics
3. Epigenetics in Cancer Occurrence and Cancer Radiotherapy
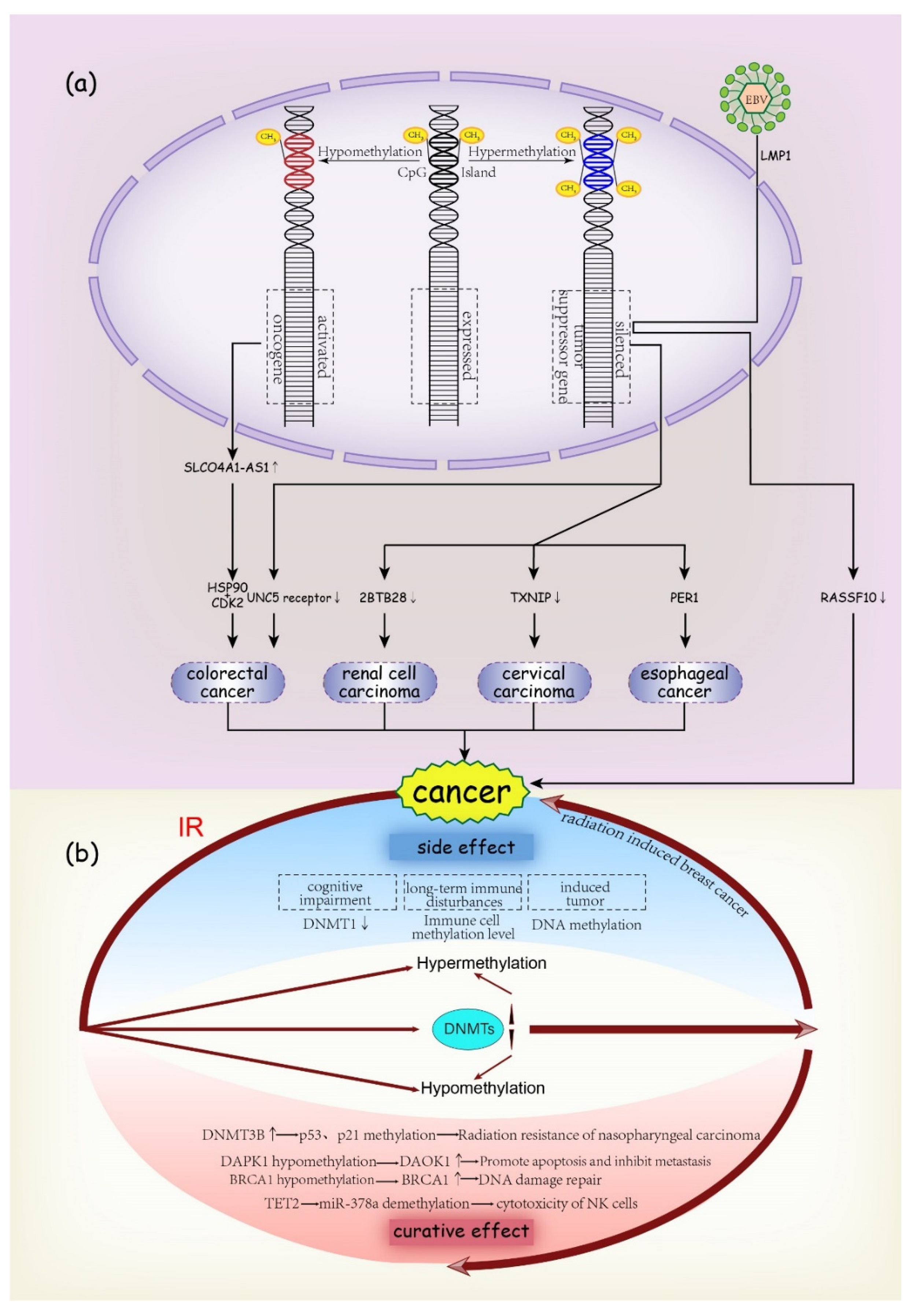
3.1. DNA Methylation
3.1.1. DNA Methylation and Carcinogenesis
3.1.2. Radiotherapy and DNA Methylation
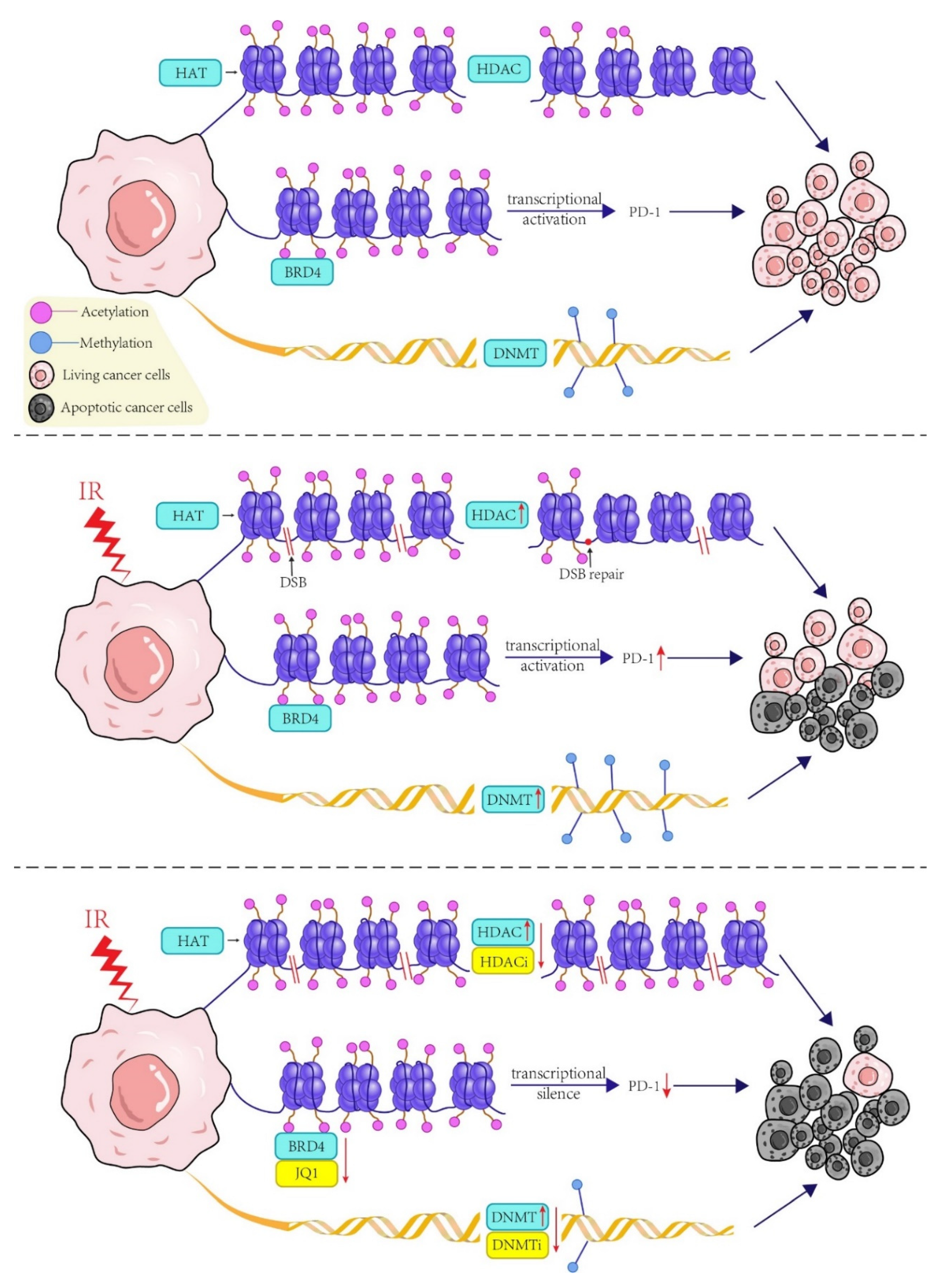
3.2. Histone Modification
3.2.1. Histone Modification and Carcinogenesis
3.2.2. The role of Histone Modification in Radiotherapy
3.3. RNA Modification and Non-Coding RNAs
3.3.1. RNA Modification and Carcinogenesis
3.3.2. Effects of Radiotherapy on RNA Modification
3.3.3. Non-Coding RNAs Are Closely Related to the Occurrence and Development of Cancer
3.3.4. Influences of Radiotherapy on Non-Coding RNA
3.4. Chromosomal Remodeling
3.4.1. Chromosome Remodeling and Cancer
3.4.2. Changes in Chromosome Remodeling during Radiotherapy
4. Application of Epigenetic Modifiers in the Sensitization of Radiotherapy
5. Summary and Prospect
Author Contributions
Funding
Conflicts of Interest
References
- Baskar, R.; Lee, K.A.; Yeo, R.; Yeoh, K.W. Cancer and radiation therapy: Current advances and future directions. Int. J. Med. Sci. 2012, 9, 193–199. [Google Scholar] [CrossRef] [PubMed]
- Minniti, G.; Goldsmith, C.; Brada, M. Radiotherapy. Handb Clin. Neurol. 2012, 104, 215–228. [Google Scholar] [PubMed]
- Nebbioso, A.; Tambaro, F.P.; Dell’Aversana, C.; Altucci, L. Cancer epigenetics: Moving forward. PLoS Genet. 2018, 14, e1007362. [Google Scholar] [CrossRef] [PubMed]
- Toh, T.B.; Lim, J.J.; Chow, E.K. Epigenetics in cancer stem cells. Mol. Cancer 2017, 16, 29. [Google Scholar] [CrossRef] [PubMed]
- Morel, D.; Jeffery, D.; Aspeslagh, S.; Almouzni, G.; Postel-Vinay, S. Combining epigenetic drugs with other therapies for solid tumours—Past lessons and future promise. Nat. Rev. Clin. Oncol. 2020, 17, 91–107. [Google Scholar] [CrossRef] [PubMed]
- Jablonka, E.; Lamb, M.J. The changing concept of epigenetics. Ann. N. Y. Acad. Sci. 2002, 981, 82–96. [Google Scholar] [CrossRef]
- Villota-Salazar, N.A.; Mendoza-Mendoza, A.; González-Prieto, J.M. Epigenetics: From the past to the present. Front. Life Sci. 2016, 9, 347–370. [Google Scholar] [CrossRef]
- Kobayashi, W.; Kurumizaka, H. Structural transition of the nucleosome during chromatin remodeling and transcription. Curr Opin. Struct. Biol. 2019, 59, 107–114. [Google Scholar] [CrossRef]
- Jonkhout, N.; Tran, J.; Smith, M.A.; Schonrock, N.; Mattick, J.S.; Novoa, E.M. The RNA modification landscape in human disease. RNA 2017, 23, 1754–1769. [Google Scholar] [CrossRef]
- Saw, P.E.; Xu, X.; Chen, J.; Song, E.W. Non-coding RNAs: The new central dogma of cancer biology. Sci. China Life Sci. 2021, 64, 22–50. [Google Scholar] [CrossRef]
- Chi, H.-C.; Tsai, C.-Y.; Tsai, M.-M.; Lin, K.-H. Impact of DNA and RNA Methylation on Radiobiology and Cancer Progression. Int. J. Mol. Sci. 2018, 19, 555. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Li, M.Y.; Wang, L.L.; Li, L.; Chen, Q.Y.; Zhu, Y.H.; Li, Y.; Qin, Y.R.; Guan, X.Y. The promoter hypermethylation of SULT2B1 accelerates esophagus tumorigenesis via downregulated PER1. Thorac. Cancer 2021, 12, 3370–3379. [Google Scholar] [CrossRef] [PubMed]
- Gusyatiner, O.; Hegi, M.E. Glioma epigenetics: From subclassification to novel treatment options. Semin Cancer Biol. 2018, 51, 50–58. [Google Scholar] [CrossRef] [PubMed]
- Maierhofer, A.; Flunkert, J.; Dittrich, M.; Muller, T.; Schindler, D.; Nanda, I.; Haaf, T. Analysis of global DNA methylation changes in primary human fibroblasts in the early phase following X-ray irradiation. PLoS ONE 2017, 12, e0177442. [Google Scholar] [CrossRef]
- Zhang, J.; Cui, K.; Huang, L.; Yang, F.; Sun, S.; Bian, Z.; Wang, X.; Li, C.; Yin, Y.; Huang, S.; et al. SLCO4A1-AS1 promotes colorectal tumourigenesis by regulating Cdk2/c-Myc signalling. J. Biomed Sci. 2022, 29, 4. [Google Scholar] [CrossRef]
- Dong, D.; Zhang, R.; Shao, J.; Zhang, A.; Wang, Y.; Zhou, Y.; Li, Y. Promoter methylation-mediated repression of UNC5 receptors and the associated clinical significance in human colorectal cancer. Clin. Epigenetics 2021, 13, 225. [Google Scholar] [CrossRef]
- Tong, X.; Xu, L.; Rong, R.; Su, X.; Xiang, T.; Peng, W.; Shi, T. Epigenetic silencing of ZBTB28 promotes renal cell carcinogenesis. Asia Pac. J. Clin. Oncol. 2021, 18, e79–e86. [Google Scholar] [CrossRef]
- Kim, M.J.; Lee, H.J.; Choi, M.Y.; Kang, S.S.; Kim, Y.S.; Shin, J.K.; Choi, W.S. UHRF1 Induces Methylation of the TXNIP Promoter and Down-Regulates Gene Expression in Cervical Cancer. Mol. Cells 2021, 44, 146–159. [Google Scholar] [CrossRef]
- Gao, Y.; Fu, Y.; Wang, J.; Zheng, X.; Zhou, J.; Ma, J. EBV as a high infection risk factor promotes RASSF10 methylation and induces cell proliferation in EBV-associated gastric cancer. Biochem. Biophys. Res. Commun. 2021, 547, 1–8. [Google Scholar] [CrossRef]
- Moreno-Acosta, P.; Molano, M.; Morales, N.; Acosta, J.; GonzAlez-Prieto, C.; Mayorga, D.; Buitrago, L.; Gamboa, O.; MejIa, J.C.; Castro, J.; et al. hTERT Protein Expression in Cytoplasm and Nucleus and its Association With HPV Infection in Patients With Cervical Cancer. Cancer Genom. Proteom. 2020, 17, 615–625. [Google Scholar] [CrossRef]
- Miousse, I.R.; Kutanzi, K.R.; Koturbash, I. Effects of ionizing radiation on DNA methylation: From experimental biology to clinical applications. Int. J. Radiat. Biol. 2017, 93, 457–469. [Google Scholar] [CrossRef] [PubMed]
- Daino, K.; Nishimura, M.; Imaoka, T.; Takabatake, M.; Morioka, T.; Nishimura, Y.; Shimada, Y.; Kakinuma, S. Epigenetic dysregulation of key developmental genes in radiation-induced rat mammary carcinomas. Int. J. Cancer 2018, 143, 343–354. [Google Scholar] [CrossRef] [PubMed]
- Greene-Schloesser, D.; Moore, E.; Robbins, M.E. Molecular pathways: Radiation-induced cognitive impairment. Clin. Cancer Res. 2013, 19, 2294–2300. [Google Scholar] [CrossRef] [PubMed]
- Ji, S.; Ding, X.; Ji, J.; Wu, H.; Sun, R.; Li, X.; Zhang, L.; Tian, Y. Cranial irradiation inhibits hippocampal neurogenesis via DNMT1 and DNMT3A. Oncol. Lett. 2018, 15, 2899–2904. [Google Scholar] [CrossRef]
- Kang, S.; Son, Y.; Lee, S.; Kim, J.; Kim, J.C.; Kim, J.S.; Jung, U.; Kim, S.H.; Yang, M.; Moon, C. Changes in epigenetic markers, DNMT1 and HDAC1/2, in the adult mouse hippocampus after cranial irradiation. Neurosci. Lett. 2017, 657, 113–119. [Google Scholar] [CrossRef] [PubMed]
- Daniel, S.; Nylander, V.; Ingerslev, L.R.; Zhong, L.; Fabre, O.; Clifford, B.; Johnston, K.; Cohn, R.J.; Barres, R.; Simar, D. T cell epigenetic remodeling and accelerated epigenetic aging are linked to long-term immune alterations in childhood cancer survivors. Clin. Epigenetics 2018, 10, 138. [Google Scholar] [CrossRef] [PubMed]
- Danielsson, A.; Barreau, K.; Kling, T.; Tisell, M.; Caren, H. Accumulation of DNA methylation alterations in paediatric glioma stem cells following fractionated dose irradiation. Clin. Epigenetics 2020, 12, 26. [Google Scholar] [CrossRef]
- Wu, C.; Guo, E.; Ming, J.; Sun, W.; Nie, X.; Sun, L.; Peng, S.; Luo, M.; Liu, D.; Zhang, L.; et al. Radiation-Induced DNMT3B Promotes Radioresistance in Nasopharyngeal Carcinoma through Methylation of p53 and p21. Mol. Ther. Oncolytics 2020, 17, 306–319. [Google Scholar] [CrossRef]
- Sood, S.; Patel, F.D.; Srinivasan, R.; Dhaliwal, L.K. Chemoradiation therapy induces in vivo changes in gene promoter methylation & gene transcript expression in patients with invasive cervical cancer. Indian J Med Res 2018, 147, 151–157. [Google Scholar]
- Metheetrairut, C.; Slack, F.J. MicroRNAs in the ionizing radiation response and in radiotherapy. Curr Opin Genet Dev 2013, 23, 12–19. [Google Scholar] [CrossRef]
- Briand, J.; Garnier, D.; Nadaradjane, A.; Clément-Colmou, K.; Potiron, V.; Supiot, S.; Bougras-Cartron, G.; Frenel, J.S.; Heymann, D.; Vallette, F.M.; et al. Radiotherapy-induced overexpression of exosomal miRNA-378a-3p in cancer cells limits natural killer cells cytotoxicity. Epigenomics 2020, 12, 397–408. [Google Scholar] [CrossRef] [PubMed]
- Xie, Y.; Zhao, J.; Liang, Y.; Chen, M.; Luo, Y.; Cui, X.; Jiang, B.; Peng, L.; Wang, X. MicroRNA-10b controls the metastasis and proliferation of colorectal cancer cells by regulating Kruppel-like factor 4. Artif Cells Nanomed. Biotechnol. 2019, 47, 1722–1729. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.F.; Yu, J.R.; Yang, Z.; Zhu, G.X.; Gao, P.; Wang, H.; Chen, S.Y.; Zhang, J.; Liu, M.Y.; Niu, Y.; et al. Promoter hypomethylation mediated upregulation of MicroRNA-10b-3p targets FOXO3 to promote the progression of esophageal squamous cell carcinoma (ESCC). J. Exp. Clin. Cancer Res. 2018, 37, 301. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Lei, H.; Luo, M.; Wang, Y.; Dong, L.; Ma, Y.; Liu, C.; Song, W.; Wang, F.; Zhang, J.; et al. DNA methylation downregulated mir-10b acts as a tumor suppressor in gastric cancer. Gastric. Cancer 2015, 18, 43–54. [Google Scholar] [CrossRef] [PubMed]
- Penha, R.C.C.; Pellecchia, S.; Pacelli, R.; Pinto, L.F.R.; Fusco, A. Ionizing Radiation Deregulates the MicroRNA Expression Profile in Differentiated Thyroid Cells. Thyroid 2018, 28, 407–421. [Google Scholar] [CrossRef] [PubMed]
- Zhou, W.; Wang, X.; Rosenfeld, M.G. Histone H2A ubiquitination in transcriptional regulation and DNA damage repair. Int. J. Biochem. Cell Biol. 2009, 41, 12–15. [Google Scholar] [CrossRef]
- Williamson, E.A.; Wray, J.W.; Bansal, P.; Hromas, R. Overview for the histone codes for DNA repair. Prog. Mol. Biol. Transl. Sci. 2012, 110, 207–227. [Google Scholar]
- Dawson, M.A.; Kouzarides, T. Cancer epigenetics: From mechanism to therapy. Cell 2012, 150, 12–27. [Google Scholar] [CrossRef]
- Kim, J.-G.; Park, M.-T.; Heo, K.; Yang, K.-M.; Yi, J. Epigenetics Meets Radiation Biology as a New Approach in Cancer Treatment. Int. J. Mol. Sci. 2013, 14, 15059–15073. [Google Scholar] [CrossRef]
- Li, Y.H.; Li, Y.X.; Li, M.; Song, S.W.; Ge, Y.; Jin, J.Y.; Li, X.Y.; Tan, X.D.; Ye, J. The Ras-ERK1/2 signaling pathway regulates H3K9ac through PCAF to promote the development of pancreatic cancer. Life Sci. 2020, 256, 117936. [Google Scholar] [CrossRef]
- Singh, P.; Bhadada, S.K.; Arya, A.K.; Saikia, U.N.; Sachdeva, N.; Dahiya, D.; Kaur, J.; Brandi, M.L.; Rao, S.D. Aberrant Epigenetic Alteration of PAX1 Expression Contributes to Parathyroid Tumorigenesis. J. Clin. Endocrinol. Metab. 2022, 107, e783–e792. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Xiong, D.; Liu, Q.; Luo, Y.; Tian, Y.; Xiao, X.; Sang, Y.; Liu, Y.; Hong, S.; Yu, S.; et al. Genome-Wide Histone H3K27 Acetylation Profiling Identified Genes Correlated With Prognosis in Papillary Thyroid Carcinoma. Front. Cell Dev. Biol. 2021, 9, 682561. [Google Scholar] [CrossRef] [PubMed]
- Rajagopalan, K.N.; Chen, X.; Weinberg, D.N.; Chen, H.; Majewski, J.; Allis, C.D.; Lu, C. Depletion of H3K36me2 recapitulates epigenomic and phenotypic changes induced by the H3.3K36M oncohistone mutation. Proc. Natl. Acad. Sci. USA 2021, 118, e2021795118. [Google Scholar] [CrossRef] [PubMed]
- Li, X.; Liu, Z.; Xia, C.; Yan, K.; Fang, Z.; Fan, Y. SETD8 stabilized by USP17 epigenetically activates SREBP1 pathway to drive lipogenesis and oncogenesis of ccRCC. Cancer Lett. 2022, 527, 150–163. [Google Scholar] [CrossRef] [PubMed]
- Sengupta, D.; Zeng, L.; Li, Y.; Hausmann, S.; Ghosh, D.; Yuan, G.; Nguyen, T.N.; Lyu, R.; Caporicci, M.; Morales Benitez, A.; et al. NSD2 dimethylation at H3K36 promotes lung adenocarcinoma pathogenesis. Mol. Cell 2021, 81, 4481–4492.e9. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.H.; Li, Q.; Huang, Z.J.; Sun, M.X.; Lu, J.J.; Zhang, X.H.; Li, G.; Wu, F. Identification of histone methyltransferase NSD2 as an important oncogenic gene in colorectal cancer. Cell Death Dis. 2021, 12, 974. [Google Scholar] [CrossRef] [PubMed]
- Katz, L.M.; Hielscher, T.; Liechty, B.; Silverman, J.; Zagzag, D.; Sen, R.; Wu, P.; Golfinos, J.G.; Reuss, D.; Neidert, M.C.; et al. Loss of histone H3K27me3 identifies a subset of meningiomas with increased risk of recurrence. Acta Neuropathol. 2018, 135, 955–963. [Google Scholar] [CrossRef]
- Di Nisio, E.; Lupo, G.; Licursi, V.; Negri, R. The Role of Histone Lysine Methylation in the Response of Mammalian Cells to Ionizing Radiation. Front Genet. 2021, 12, 639602. [Google Scholar] [CrossRef]
- Rath, B.H.; Waung, I.; Camphausen, K.; Tofilon, P.J. Inhibition of the Histone H3K27 Demethylase UTX Enhances Tumor Cell Radiosensitivity. Mol. Cancer Ther. 2018, 17, 1070–1078. [Google Scholar] [CrossRef]
- An, S.; Camarillo, J.M.; Huang, T.Y.; Li, D.; Morris, J.A.; Zoltek, M.A.; Qi, J.; Behbahani, M.; Kambhampati, M.; Kelleher, N.L.; et al. Histone tail analysis reveals H3K36me2 and H4K16ac as epigenetic signatures of diffuse intrinsic pontine glioma. J. Exp. Clin. Cancer Res. 2020, 39, 261. [Google Scholar] [CrossRef]
- Ahn, H.J.; Hwang, S.Y.; Nguyen, N.H.; Lee, I.J.; Lee, E.J.; Seong, J.; Lee, J.S. Radiation-Induced CXCL12 Upregulation via Histone Modification at the Promoter in the Tumor Microenvironment of Hepatocellular Carcinoma. Mol. Cells 2019, 42, 530–545. [Google Scholar] [PubMed]
- Lee, T.G.; Kim, S.Y.; Kim, H.R.; Kim, H.; Kim, C.H. Radiation Induces Autophagy via Histone H4 Lysine 20 Trimethylation in Non-small Cell Lung Cancer Cells. Anticancer. Res. 2020, 40, 2537–2548. [Google Scholar] [CrossRef] [PubMed]
- Peitzsch, C.; Cojoc, M.; Hein, L.; Kurth, I.; Mabert, K.; Trautmann, F.; Klink, B.; Schrock, E.; Wirth, M.P.; Krause, M.; et al. An Epigenetic Reprogramming Strategy to Resensitize Radioresistant Prostate Cancer Cells. Cancer Res. 2016, 76, 2637–2651. [Google Scholar] [CrossRef] [PubMed]
- Kong, E.; Cheng, S.; Yu, K. Zebrafish as an In Vivo Model to Assess Epigenetic Effects of Ionizing Radiation. Int. J. Mol. Sci. 2016, 17, 2108. [Google Scholar] [CrossRef]
- Lindeman, L.C.; Kamstra, J.H.; Ballangby, J.; Hurem, S.; Martin, L.M.; Brede, D.A.; Teien, H.C.; Oughton, D.H.; Salbu, B.; Lyche, J.L.; et al. Gamma radiation induces locus specific changes to histone modification enrichment in zebrafish and Atlantic salmon. PLoS ONE 2019, 14, e0212123. [Google Scholar] [CrossRef]
- Maroschik, B.; Gürtler, A.; Krämer, A.; Rößler, U.; Gomolka, M.; Hornhardt, S.; Mörtl, S.; Friedl, A.A. Radiation-induced alterations of histone post-translational modification levels in lymphoblastoid cell lines. Radiat. Oncol. 2014, 9, 15. [Google Scholar] [CrossRef][Green Version]
- Sharda, A.; Rashid, M.; Shah, S.G.; Sharma, A.K.; Singh, S.R.; Gera, P.; Chilkapati, M.K.; Gupta, S. Elevated HDAC activity and altered histone phospho-acetylation confer acquired radio-resistant phenotype to breast cancer cells. Clin. Epigenetics 2020, 12, 4. [Google Scholar] [CrossRef]
- Ma, S.; Chen, C.; Ji, X.; Liu, J.; Zhou, Q.; Wang, G.; Yuan, W.; Kan, Q.; Sun, Z. The interplay between m6A RNA methylation and noncoding RNA in cancer. J. Hematol. Oncol. 2019, 12, 121. [Google Scholar] [CrossRef]
- Barbieri, I.; Kouzarides, T. Role of RNA modifications in cancer. Nat. Rev. Cancer 2020, 20, 303–322. [Google Scholar] [CrossRef]
- Sun, T.; Wu, R.; Ming, L. The role of m6A RNA methylation in cancer. Biomed. Pharmacother. 2019, 112, 108613. [Google Scholar] [CrossRef]
- Wang, Q.; Chen, C.; Ding, Q.; Zhao, Y.; Wang, Z.; Chen, J.; Jiang, Z.; Zhang, Y.; Xu, G.; Zhang, J.; et al. METTL3-mediated m(6)A modification of HDGF mRNA promotes gastric cancer progression and has prognostic significance. Gut 2020, 69, 1193–1205. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Xiao, M.; Zhang, L.; Li, L.; Zhu, G.; Shen, E.; Lv, M.; Lu, X.; Sun, Z. The m6A methyltransferase METTL14 inhibits the proliferation, migration, and invasion of gastric cancer by regulating the PI3K/AKT/mTOR signaling pathway. J. Clin. Lab. Anal. 2021, 35, e23655. [Google Scholar] [CrossRef] [PubMed]
- Li, Z.; Weng, H.; Su, R.; Weng, X.; Zuo, Z.; Li, C.; Huang, H.; Nachtergaele, S.; Dong, L.; Hu, C.; et al. FTO Plays an Oncogenic Role in Acute Myeloid Leukemia as a N(6)-Methyladenosine RNA Demethylase. Cancer Cell. 2017, 31, 127–141. [Google Scholar] [CrossRef] [PubMed]
- Xia, T.; Wu, X.; Cao, M.; Zhang, P.; Shi, G.; Zhang, J.; Lu, Z.; Wu, P.; Cai, B.; Miao, Y.; et al. The RNA m6A methyltransferase METTL3 promotes pancreatic cancer cell proliferation and invasion. Pathol. Res. Pract. 2019, 215, 152666. [Google Scholar] [CrossRef] [PubMed]
- Wang, Q.; Guo, X.; Li, L.; Gao, Z.; Su, X.; Ji, M.; Liu, J. N(6)-methyladenosine METTL3 promotes cervical cancer tumorigenesis and Warburg effect through YTHDF1/HK2 modification. Cell Death Dis. 2020, 11, 911. [Google Scholar] [CrossRef]
- Zou, D.; Dong, L.; Li, C.; Yin, Z.; Rao, S.; Zhou, Q. The m(6)A eraser FTO facilitates proliferation and migration of human cervical cancer cells. Cancer Cell Int. 2019, 19, 321. [Google Scholar] [CrossRef]
- Han, H.; Feng, F.; Li, H. Research advances on epigenetics and cancer metabolism. Zhejiang Da Xue Xue Bao Yi Xue Ban 2021, 50, 1–16. [Google Scholar] [CrossRef]
- He, J.J.; Li, Z.; Rong, Z.X.; Gao, J.; Mu, Y.; Guan, Y.D.; Ren, X.X.; Zi, Y.Y.; Liu, L.Y.; Fan, Q.; et al. m(6)A Reader YTHDC2 Promotes Radiotherapy Resistance of Nasopharyngeal Carcinoma via Activating IGF1R/AKT/S6 Signaling Axis. Front Oncol. 2020, 10, 1166. [Google Scholar] [CrossRef]
- Zhou, S.; Bai, Z.L.; Xia, D.; Zhao, Z.J.; Zhao, R.; Wang, Y.Y.; Zhe, H. FTO regulates the chemo-radiotherapy resistance of cervical squamous cell carcinoma (CSCC) by targeting β-catenin through mRNA demethylation. Mol Carcinog 2018, 57, 590–597. [Google Scholar] [CrossRef]
- Taketo, K.; Konno, M.; Asai, A.; Koseki, J.; Toratani, M.; Satoh, T.; Doki, Y.; Mori, M.; Ishii, H.; Ogawa, K. The epitranscriptome m6A writer METTL3 promotes chemo- and radioresistance in pancreatic cancer cells. Int. J. Oncol. 2018, 52, 621–629. [Google Scholar] [CrossRef]
- Visvanathan, A.; Patil, V.; Arora, A.; Hegde, A.S.; Arivazhagan, A.; Santosh, V.; Somasundaram, K. Essential role of METTL3-mediated m(6)A modification in glioma stem-like cells maintenance and radioresistance. Oncogene 2018, 37, 522–533. [Google Scholar] [CrossRef] [PubMed]
- Wu, P.; Fang, X.; Liu, Y.; Tang, Y.; Wang, W.; Li, X.; Fan, Y. N6-methyladenosine modification of circCUX1 confers radioresistance of hypopharyngeal squamous cell carcinoma through caspase1 pathway. Cell Death Dis. 2021, 12, 298. [Google Scholar] [CrossRef] [PubMed]
- Eddy, S.R. Non-coding RNA genes and the modern RNA world. Nat. Rev. Genet. 2001, 2, 919–929. [Google Scholar] [CrossRef] [PubMed]
- Palazzo, A.F.; Lee, E.S. Non-coding RNA: What is functional and what is junk? Front Genet. 2015, 6, 2. [Google Scholar] [CrossRef]
- Zhang, P.; Wu, W.; Chen, Q.; Chen, M. Non-Coding RNAs and their Integrated Networks. J. Integr. Bioinform 2019, 16, 20190027. [Google Scholar] [CrossRef]
- Rouhi, A.; Mager, D.L.; Humphries, R.K.; Kuchenbauer, F. MiRNAs, epigenetics, and cancer. Mamm. Genome 2008, 19, 517–525. [Google Scholar] [CrossRef]
- Romano, G.; Veneziano, D.; Acunzo, M.; Croce, C.M. Small non-coding RNA and cancer. Carcinogenesis 2017, 38, 485–491. [Google Scholar] [CrossRef]
- Braicu, C.; Buiga, R.; Cojocneanu, R.; Buse, M.; Raduly, L.; Pop, L.A.; Chira, S.; Budisan, L.; Jurj, A.; Ciocan, C.; et al. Connecting the dots between different networks: miRNAs associated with bladder cancer risk and progression. J. Exp. Clin. Cancer Res. 2019, 38, 433. [Google Scholar] [CrossRef]
- Taheri, M.; Shirvani-Farsani, Z.; Ghafouri-Fard, S.; Omrani, M.D. Expression profile of microRNAs in bladder cancer and their application as biomarkers. Biomed. Pharmacother. 2020, 131, 110703. [Google Scholar] [CrossRef]
- Zhang, H.H.; Qi, F.; Cao, Y.H.; Zu, X.B.; Chen, M.F. Expression and clinical significance of microRNA-21, maspin and vascular endothelial growth factor-C in bladder cancer. Oncol. Lett. 2015, 10, 2610–2616. [Google Scholar] [CrossRef]
- Yan, L.; Wang, Y.; Liang, J.; Liu, Z.; Sun, X.; Cai, K. MiR-301b promotes the proliferation, mobility, and epithelial-to-mesenchymal transition of bladder cancer cells by targeting EGR1. Biochem. Cell Biol. 2017, 95, 571–577. [Google Scholar] [CrossRef] [PubMed]
- Ghafouri-Fard, S.; Shoorei, H.; Taheri, M. miRNA profile in ovarian cancer. Exp. Mol. Pathol. 2020, 113, 104381. [Google Scholar] [CrossRef] [PubMed]
- Ibrahim, F.F.; Jamal, R.; Syafruddin, S.E.; Ab Mutalib, N.S.; Saidin, S.; MdZin, R.R.; Hossain Mollah, M.M.; Mokhtar, N.M. MicroRNA-200c and microRNA-31 regulate proliferation, colony formation, migration and invasion in serous ovarian cancer. J. Ovarian Res. 2015, 8, 56. [Google Scholar] [CrossRef] [PubMed]
- Tuncer, S.B.; Erdogan, O.S.; Erciyas, S.K.; Saral, M.A.; Celik, B.; Odemis, D.A.; Turkcan, G.K.; Yazici, H. miRNA expression profile changes in the peripheral blood of monozygotic discordant twins for epithelial ovarian carcinoma: Potential new biomarkers for early diagnosis and prognosis of ovarian carcinoma. J. Ovarian Res. 2020, 13, 99. [Google Scholar] [CrossRef]
- Fukagawa, S.; Miyata, K.; Yotsumoto, F.; Kiyoshima, C.; Nam, S.O.; Anan, H.; Katsuda, T.; Miyahara, D.; Murata, M.; Yagi, H.; et al. MicroRNA-135a-3p as a promising biomarker and nucleic acid therapeutic agent for ovarian cancer. Cancer Sci. 2017, 108, 886–896. [Google Scholar] [CrossRef]
- Daoud, A.Z.; Mulholland, E.J.; Cole, G.; McCarthy, H.O. MicroRNAs in Pancreatic Cancer: Biomarkers, prognostic, and therapeutic modulators. BMC Cancer 2019, 19, 1130. [Google Scholar] [CrossRef]
- Ren, H.; Wang, C.F. [Diagnosis, treatment and prognosis evaluation of pancreatic cancer by microRNA]. Zhonghua Zhong Liu Za Zhi 2020, 42, 903–906. [Google Scholar]
- Khan, M.A.; Zubair, H.; Srivastava, S.K.; Singh, S.; Singh, A.P. Insights into the Role of microRNAs in Pancreatic Cancer Pathogenesis: Potential for Diagnosis, Prognosis, and Therapy. Adv. Exp. Med. Biol. 2015, 889, 71–87. [Google Scholar]
- Chong, Z.X.; Yeap, S.K.; Ho, W.Y. Role of miRNAs in regulating responses to radiotherapy in human breast cancer. Int. J. Radiat. Biol. 2021, 97, 289–301. [Google Scholar] [CrossRef]
- Li, Z.; Wang, F.; Zhu, Y.; Guo, T.; Lin, M. Long Noncoding RNAs Regulate the Radioresistance of Breast Cancer. Anal. Cell Pathol. 2021, 2021, 9005073. [Google Scholar] [CrossRef]
- Mao, Y.; Xue, P.; Li, L.; Xu, P.; Cai, Y.; Chu, X.; Jiang, P.; Zhu, S. Bioinformatics analysis of mRNA and miRNA microarray to identify the key miRNAgene pairs in smallcell lung cancer. Mol. Med. Rep. 2019, 20, 2199–2208. [Google Scholar] [PubMed]
- Anastasov, N.; Hofig, I.; Vasconcellos, I.G.; Rappl, K.; Braselmann, H.; Ludyga, N.; Auer, G.; Aubele, M.; Atkinson, M.J. Radiation resistance due to high expression of miR-21 and G2/M checkpoint arrest in breast cancer cells. Radiat. Oncol. 2012, 7, 206. [Google Scholar] [CrossRef] [PubMed]
- Zare, A.; Fardid, R.; Tamadon, G.H.H.; Mosleh-Shirazi, M.A. miR-155, miR-21, and let-7a Expressions in MCF-10A and MCF-7 Cell Lines after Low to High Dose Irradiation. Cell J. 2021, 23, 532–537. [Google Scholar] [PubMed]
- Wang, Y.; Sun, L.E. Knockdown of LMP1-induced miR-155 sensitizes nasopharyngeal carcinoma cells to radiotherapy in vitro. Oncol Lett. 2016, 11, 3451–3456. [Google Scholar] [CrossRef]
- Yuan, X.; Qian, N.; Ling, S.; Li, Y.; Sun, W.; Li, J.; Du, R.; Zhong, G.; Liu, C.; Yu, G.; et al. Breast cancer exosomes contribute to pre-metastatic niche formation and promote bone metastasis of tumor cells. Theranostics 2021, 11, 1429–1445. [Google Scholar] [CrossRef]
- Zheng, Q.; Yu, J.J.; Li, C.; Li, J.; Wang, J.; Wang, S. miR-224 targets BTRC and promotes cell migration and invasion in colorectal cancer. 3 Biotech 2020, 10, 485. [Google Scholar] [CrossRef]
- Cui, R.; Kim, T.; Fassan, M.; Meng, W.; Sun, H.L.; Jeon, Y.J.; Vicentini, C.; Tili, E.; Peng, Y.; Scarpa, A.; et al. MicroRNA-224 is implicated in lung cancer pathogenesis through targeting caspase-3 and caspase-7. Oncotarget 2015, 6, 21802–21815. [Google Scholar] [CrossRef]
- Stojanovic, J.; Tognetto, A.; Tiziano, D.F.; Leoncini, E.; Posteraro, B.; Pastorino, R.; Boccia, S. MicroRNAs expression profiles as diagnostic biomarkers of gastric cancer: A systematic literature review. Biomarkers 2019, 24, 110–119. [Google Scholar] [CrossRef]
- Josson, S.; Sung, S.Y.; Lao, K.; Chung, L.W.; Johnstone, P.A. Radiation modulation of microRNA in prostate cancer cell lines. Prostate 2008, 68, 1599–1606. [Google Scholar] [CrossRef]
- Samadi, P.; Afshar, S.; Amini, R.; Najafi, R.; Mahdavinezhad, A.; Sedighi Pashaki, A.; Gholami, M.H.; Saidijam, M. Let-7e enhances the radiosensitivity of colorectal cancer cells by directly targeting insulin-like growth factor 1 receptor. J. Cell Physiol. 2019, 234, 10718–10725. [Google Scholar] [CrossRef]
- Pop-Bica, C.; Pintea, S.; Magdo, L.; Cojocneanu, R.; Gulei, D.; Ferracin, M.; Berindan-Neagoe, I. The Clinical Utility of miR-21 and let-7 in Non-small Cell Lung Cancer (NSCLC). A Systematic Review and Meta-Analysis. Front. Oncol. 2020, 10, 516850. [Google Scholar] [CrossRef] [PubMed]
- Huang, Y.J.; Yadav, V.K.; Srivastava, P.; Wu, A.T.; Huynh, T.T.; Wei, P.L.; Huang, C.F.; Huang, T.H. Antrodia cinnamomea Enhances Chemo-Sensitivity of 5-FU and Suppresses Colon Tumorigenesis and Cancer Stemness via Up-Regulation of Tumor Suppressor miR-142-3p. Biomolecules 2019, 9, 306. [Google Scholar] [CrossRef] [PubMed]
- Chaudhry, M.A. Real-time PCR analysis of micro-RNA expression in ionizing radiation-treated cells. Cancer Biother. Radiopharm. 2009, 24, 49–56. [Google Scholar] [CrossRef] [PubMed]
- Jia, X.P.; Meng, L.L.; Fang, J.C.; Wang, H.W.; Chen, J.; Zhou, J.; Wang, C.N.; Jiang, W.F. Aberrant Expression of miR-142-3p and its Target Gene HMGA1 and FZD7 in Breast Cancer and its Clinical Significance. Clin. Lab. 2018, 64, 915–921. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.J.; Fan, Q.Q.; Li, Y.Y.; Ren, H.M.; Zhang, T.; Liu, S.; Maa, M.; Zheng, Y.C.; Liu, H.M. LSD1 deletion represses gastric cancer migration by upregulating a novel miR-142-5p target protein CD9. Pharmacol. Res. 2020, 159, 104991. [Google Scholar] [CrossRef] [PubMed]
- Xiao, S.; Liu, N.; Yang, X.; Ji, G.; Li, M. Polygalacin D suppresses esophageal squamous cell carcinoma growth and metastasis through regulating miR-142-5p/Nrf2 axis. Free Radic. Biol. Med. 2021, 164, 58–75. [Google Scholar] [CrossRef]
- Chen, Y.; Lin, Y.; Shu, Y.; He, J.; Gao, W. Interaction between N(6)-methyladenosine (m(6)A) modification and noncoding RNAs in cancer. Mol. Cancer 2020, 19, 94. [Google Scholar] [CrossRef]
- Zheng, L.; Chen, J.; Zhou, Z.; He, Z. miR-195 enhances the radiosensitivity of colorectal cancer cells by suppressing CARM1. Onco Targets Ther. 2017, 10, 1027–1038. [Google Scholar] [CrossRef]
- Zhang, Y.; Zheng, L.; Huang, J.; Gao, F.; Lin, X.; He, L.; Li, D.; Li, Z.; Ding, Y.; Chen, L. MiR-124 Radiosensitizes human colorectal cancer cells by targeting PRRX1. PLoS ONE 2014, 9, e93917. [Google Scholar] [CrossRef]
- Zhang, N.; Hu, X.; Du, Y.; Du, J. The role of miRNAs in colorectal cancer progression and chemoradiotherapy. Biomed. Pharmacother 2021, 134, 111099. [Google Scholar] [CrossRef]
- Afshar, S.; Najafi, R.; Sedighi Pashaki, A.; Sharifi, M.; Nikzad, S.; Gholami, M.H.; Khoshghadam, A.; Amini, R.; Karimi, J.; Saidijam, M. MiR-185 enhances radiosensitivity of colorectal cancer cells by targeting IGF1R and IGF2. Biomed. Pharmacother. 2018, 106, 763–769. [Google Scholar] [CrossRef] [PubMed]
- Powrozek, T.; Malecka-Massalska, T. MiRNA and lung cancer radiosensitivity: A mini-review. Eur. Rev. Med. Pharmacol. Sci. 2019, 23, 8422–8428. [Google Scholar] [PubMed]
- Vannini, I.; Fanini, F.; Fabbri, M. MicroRNAs as lung cancer biomarkers and key players in lung carcinogenesis. Clin. Biochem. 2013, 46, 918–925. [Google Scholar] [CrossRef] [PubMed]
- Zheng, L.; Zhang, Y.; Liu, Y.; Zhou, M.; Lu, Y.; Yuan, L.; Zhang, C.; Hong, M.; Wang, S.; Li, X. MiR-106b induces cell radioresistance via the PTEN/PI3K/AKT pathways and p21 in colorectal cancer. J. Transl. Med. 2015, 13, 252. [Google Scholar] [CrossRef] [PubMed]
- Ahmadov, U.; Picard, D.; Bartl, J.; Silginer, M.; Trajkovic-Arsic, M.; Qin, N.; Blumel, L.; Wolter, M.; Lim, J.K.M.; Pauck, D.; et al. The long non-coding RNA HOTAIRM1 promotes tumor aggressiveness and radiotherapy resistance in glioblastoma. Cell Death Dis. 2021, 12, 885. [Google Scholar] [CrossRef] [PubMed]
- Luo, R.X.; Dean, D.C. Chromatin remodeling and transcriptional regulation. J. Natl. Cancer Inst. 1999, 91, 1288–1294. [Google Scholar] [CrossRef]
- Woodcock, C.L.; Dimitrov, S. Higher-order structure of chromatin and chromosomes. Curr. Opin. Genet. Dev. 2001, 11, 130–135. [Google Scholar] [CrossRef]
- Davis, P.K.; Brackmann, R.K. Chromatin remodeling and cancer. Cancer Biol. Ther. 2003, 2, 22–29. [Google Scholar] [CrossRef]
- Tsukiyama, T.; Wu, C. Chromatin remodeling and transcription. Curr. Opin. Genet. Dev. 1997, 7, 182–191. [Google Scholar] [CrossRef]
- Kim, J.H. Chromatin Remodeling and Epigenetic Regulation in Plant DNA Damage Repair. Int. J. Mol. Sci. 2019, 20, 4093. [Google Scholar] [CrossRef]
- Wang, G.G.; Allis, C.D.; Chi, P. Chromatin remodeling and cancer, Part II: ATP-dependent chromatin remodeling. Trends. Mol. Med 2007, 13, 373–380. [Google Scholar] [CrossRef] [PubMed]
- Kumar, R.; Li, D.Q.; Muller, S.; Knapp, S. Epigenomic regulation of oncogenesis by chromatin remodeling. Oncogene 2016, 35, 4423–4436. [Google Scholar] [CrossRef] [PubMed]
- Ding, H.; Huang, Y.; Shi, J.; Wang, L.; Liu, S.; Zhao, B.; Liu, Y.; Yang, J.; Chen, Z. Attenuated expression of SNF5 facilitates progression of bladder cancer via STAT3 activation. Cancer Cell Int. 2021, 21, 655. [Google Scholar] [CrossRef]
- Roberts, C.W.; Galusha, S.A.; McMenamin, M.E.; Fletcher, C.D.; Orkin, S.H. Haploinsufficiency of Snf5 (integrase interactor 1) predisposes to malignant rhabdoid tumors in mice. Proc. Natl. Acad. Sci. USA 2000, 97, 13796–13800. [Google Scholar] [CrossRef]
- Sarnowska, E.; Szymanski, M.; Rusetska, N.; Ligaj, M.; Jancewicz, I.; Cwiek, P.; Skrodzka, M.; Leszczynski, M.; Szarkowska, J.; Chrzan, A.; et al. Evaluation of the role of downregulation of SNF5/INI1 core subunit of SWI/SNF complex in clear cell renal cell carcinoma development. Am. J. Cancer Res. 2017, 7, 2275–2289. [Google Scholar] [PubMed]
- Biegel, J.A.; Zhou, J.Y.; Rorke, L.B.; Stenstrom, C.; Wainwright, L.M.; Fogelgren, B. Germ-line and acquired mutations of INI1 in atypical teratoid and rhabdoid tumors. Cancer Res. 1999, 59, 74–79. [Google Scholar] [PubMed]
- Jones, S.; Li, M.; Parsons, D.W.; Zhang, X.; Wesseling, J.; Kristel, P.; Schmidt, M.K.; Markowitz, S.; Yan, H.; Bigner, D.; et al. Somatic mutations in the chromatin remodeling gene ARID1A occur in several tumor types. Hum. Mutat. 2012, 33, 100–103. [Google Scholar] [CrossRef]
- Wiegand, K.C.; Shah, S.P.; Al-Agha, O.M.; Zhao, Y.; Tse, K.; Zeng, T.; Senz, J.; McConechy, M.K.; Anglesio, M.S.; Kalloger, S.E.; et al. ARID1A mutations in endometriosis-associated ovarian carcinomas. N. Engl. J. Med. 2010, 363, 1532–1543. [Google Scholar] [CrossRef]
- Schulze, K.; Imbeaud, S.; Letouze, E.; Alexandrov, L.B.; Calderaro, J.; Rebouissou, S.; Couchy, G.; Meiller, C.; Shinde, J.; Soysouvanh, F.; et al. Exome sequencing of hepatocellular carcinomas identifies new mutational signatures and potential therapeutic targets. Nat. Genet. 2015, 47, 505–511. [Google Scholar] [CrossRef]
- Le Gallo, M.; O’Hara, A.J.; Rudd, M.L.; Urick, M.E.; Hansen, N.F.; O’Neil, N.J.; Price, J.C.; Zhang, S.; England, B.M.; Godwin, A.K.; et al. Exome sequencing of serous endometrial tumors identifies recurrent somatic mutations in chromatin-remodeling and ubiquitin ligase complex genes. Nat. Genet. 2012, 44, 1310–1315. [Google Scholar] [CrossRef]
- Pavlidis, E.T.; Pavlidis, T.E. Current Molecular and Genetic Aspects of Pancreatic Cancer, the Role of Metastasis Associated Proteins (MTA): A Review. J. Invest. Surg. 2018, 31, 54–66. [Google Scholar] [CrossRef] [PubMed]
- Li, W.F.; Liu, N.; Cui, R.X.; He, Q.M.; Chen, M.; Jiang, N.; Sun, Y.; Zeng, J.; Liu, L.Z.; Ma, J. Nuclear overexpression of metastasis-associated protein 1 correlates significantly with poor survival in nasopharyngeal carcinoma. J. Transl. Med. 2012, 10, 78. [Google Scholar] [CrossRef] [PubMed]
- Zhang, B.J.; Lan, G.P.; Si, J.Y.; Li, Y.L.; Huang, B.; Deng, Z.X.; Si, Y.F.; Chen, M.M.; Shen, X.Y.; Wang, Y. Correlation of metastasis-associated protein expression with prognosis and chemotherapy in nasopharyngeal carcinoma. Int. J. Clin. Exp. Pathol. 2018, 11, 2537–2549. [Google Scholar] [PubMed]
- Liu, T.; Yang, M.; Yang, S.; Ge, T.; Gu, L.; Lou, G. Metastasis-associated protein 1 is a novel marker predicting survival and lymph nodes metastasis in cervical cancer. Hum. Pathol. 2013, 44, 2275–2281. [Google Scholar] [CrossRef] [PubMed]
- Kwon, S.J.; Lee, S.K.; Na, J.; Lee, S.A.; Lee, H.S.; Park, J.H.; Chung, J.K.; Youn, H.; Kwon, J. Targeting BRG1 chromatin remodeler via its bromodomain for enhanced tumor cell radiosensitivity in vitro and in vivo. Mol. Cancer Ther. 2015, 14, 597–607. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.Y.; Liu, Y.Y.; Yang, F.; Zhang, L.; Zhang, F.L.; Hu, X.; Shao, Z.M.; Li, D.Q. Acetylation of MORC2 by NAT10 regulates cell-cycle checkpoint control and resistance to DNA-damaging chemotherapy and radiotherapy in breast cancer. Nucleic. Acids. Res. 2020, 48, 3638–3656. [Google Scholar] [CrossRef] [PubMed]
- Citrin, D.E.; Mitchell, J.B. Altering the response to radiation: Sensitizers and protectors. Semin. Oncol. 2014, 41, 848–859. [Google Scholar] [CrossRef]
- Russo, A.; Mitchell, J.; Kinsella, T.; Morstyn, G.; Glatstein, E. Determinants of radiosensitivity. Semin. Oncol. 1985, 12, 332–349. [Google Scholar]
- Tsai, C.L.; Liu, W.L.; Hsu, F.M.; Yang, P.S.; Yen, R.F.; Tzen, K.Y.; Cheng, A.L.; Chen, P.J.; Cheng, J.C. Targeting histone deacetylase 4/ubiquitin-conjugating enzyme 9 impairs DNA repair for radiosensitization of hepatocellular carcinoma cells in mice. Hepatology 2018, 67, 586–599. [Google Scholar] [CrossRef]
- Tang, F.; Choy, E.; Tu, C.; Hornicek, F.; Duan, Z. Therapeutic applications of histone deacetylase inhibitors in sarcoma. Cancer Treat. Rev. 2017, 59, 33–45. [Google Scholar] [CrossRef]
- Reda, M.; Bagley, A.F.; Zaidan, H.Y.; Yantasee, W. Augmenting the therapeutic window of radiotherapy: A perspective on molecularly targeted therapies and nanomaterials. Radiother. Oncol. 2020, 150, 225–235. [Google Scholar] [CrossRef] [PubMed]
- Chiu, H.W.; Yeh, Y.L.; Wang, Y.C.; Huang, W.J.; Chen, Y.A.; Chiou, Y.S.; Ho, S.Y.; Lin, P.; Wang, Y.J. Suberoylanilide hydroxamic acid, an inhibitor of histone deacetylase, enhances radiosensitivity and suppresses lung metastasis in breast cancer in vitro and in vivo. PLoS ONE 2013, 8, e76340. [Google Scholar] [CrossRef] [PubMed]
- Baschnagel, A.; Russo, A.; Burgan, W.E.; Carter, D.; Beam, K.; Palmieri, D.; Steeg, P.S.; Tofilon, P.; Camphausen, K. Vorinostat enhances the radiosensitivity of a breast cancer brain metastatic cell line grown in vitro and as intracranial xenografts. Mol. Cancer Ther. 2009, 8, 1589–1595. [Google Scholar] [CrossRef] [PubMed]
- McLaughlin, K.A.; Nemeth, Z.; Bradley, C.A.; Humphreys, L.; Stasik, I.; Fenning, C.; Majkut, J.; Higgins, C.; Crawford, N.; Holohan, C.; et al. FLIP: A Targetable Mediator of Resistance to Radiation in Non-Small Cell Lung Cancer. Mol. Cancer Ther. 2016, 15, 2432–2441. [Google Scholar] [CrossRef]
- Wang, S.; Song, M.; Zhang, B. Trichostatin A enhances radiosensitivity and radiation-induced DNA damage of esophageal cancer cells. J. Gastrointest. Oncol. 2021, 12, 1985–1995. [Google Scholar] [CrossRef]
- Rauscher, S.; Greil, R.; Geisberger, R. Re-Sensitizing Tumor Cells to Cancer Drugs with Epigenetic Regulators. Curr. Cancer Drug Targets. 2021, 21, 353–359. [Google Scholar] [CrossRef]
- Komatsu, S.; Moriya, S.; Che, X.F.; Yokoyama, T.; Kohno, N.; Miyazawa, K. Combined treatment with SAHA, bortezomib, and clarithromycin for concomitant targeting of aggresome formation and intracellular proteolytic pathways enhances ER stress-mediated cell death in breast cancer cells. Biochem. Biophys. Res. Commun. 2013, 437, 41–47. [Google Scholar] [CrossRef]
- Fang, F.; Balch, C.; Schilder, J.; Breen, T.; Zhang, S.; Shen, C.; Li, L.; Kulesavage, C.; Snyder, A.J.; Nephew, K.P.; et al. A phase 1 and pharmacodynamic study of decitabine in combination with carboplatin in patients with recurrent, platinum-resistant, epithelial ovarian cancer. Cancer 2010, 116, 4043–4053. [Google Scholar] [CrossRef]
- McMullen, M.; Karakasis, K.; Madariaga, A.; Oza, A.M. Overcoming Platinum and PARP-Inhibitor Resistance in Ovarian Cancer. Cancers 2020, 12, 1607. [Google Scholar] [CrossRef]
- Glasspool, R.M.; Brown, R.; Gore, M.E.; Rustin, G.J.; McNeish, I.A.; Wilson, R.H.; Pledge, S.; Paul, J.; Mackean, M.; Hall, G.D.; et al. A randomised, phase II trial of the DNA-hypomethylating agent 5-aza-2'-deoxycytidine (decitabine) in combination with carboplatin vs carboplatin alone in patients with recurrent, partially platinum-sensitive ovarian cancer. Br. J. Cancer 2014, 110, 1923–1929. [Google Scholar] [CrossRef]
- Matei, D.; Fang, F.; Shen, C.; Schilder, J.; Arnold, A.; Zeng, Y.; Berry, W.A.; Huang, T.; Nephew, K.P. Epigenetic resensitization to platinum in ovarian cancer. Cancer Res. 2012, 72, 2197–2205. [Google Scholar] [CrossRef] [PubMed]
- Park, M.T.; Kim, S.D.; Han, Y.K.; Hyun, J.W.; Lee, H.J.; Yi, J.M. Enhancement of Radiosensitivity by DNA Hypomethylating Drugs through Apoptosis and Autophagy in Human Sarcoma Cells. Biomol. Ther. 2022, 30, 80–89. [Google Scholar] [CrossRef] [PubMed]
- Lee, M.; Nam, H.Y.; Kang, H.B.; Lee, W.H.; Lee, G.H.; Sung, G.J.; Han, M.W.; Cho, K.J.; Chang, E.J.; Choi, K.C.; et al. Epigenetic regulation of p62/SQSTM1 overcomes the radioresistance of head and neck cancer cells via autophagy-dependent senescence induction. Cell Death Dis. 2021, 12, 250. [Google Scholar] [CrossRef] [PubMed]
- Gao, C.; Qiao, T.; Yuan, S.; Zhuang, X. The Preliminary Study for Postoperative Radiotherapy Survival Associated with RUNX3 and TLR9 Expression in Lung Cancer. Cancer Manag. Res. 2021, 13, 4497–4507. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.; Pei, X.; Li, S.W.; Yang, J.; Li, C.; Tang, J.; Hu, K.; Huang, G.; Min, W.P.; Sang, Y. CRISPR/Cas9 library screening uncovered methylated PKP2 as a critical driver of lung cancer radioresistance by stabilizing beta-catenin. Oncogene 2021, 40, 2842–2857. [Google Scholar] [CrossRef]
- Wang, J.; Xu, Y.; Rao, X.; Zhang, R.; Tang, J.; Zhang, D.; Jie, X.; Zhu, K.; Wang, X.; Xu, Y.; et al. BRD4-IRF1 axis regulates chemoradiotherapy-induced PD-L1 expression and immune evasion in non-small cell lung cancer. Clin. Transl. Med. 2022, 12, e718. [Google Scholar] [CrossRef]
- Ni, M.; Li, J.; Zhao, H.; Xu, F.; Cheng, J.; Yu, M.; Ke, G.; Wu, X. BRD4 inhibition sensitizes cervical cancer to radiotherapy by attenuating DNA repair. Oncogene 2021, 40, 2711–2724. [Google Scholar] [CrossRef]
- Oronsky, B.; Scicinski, J.; Cabrales, P.; Minchinton, A. RRx-001, an epigenetic-based radio- and chemosensitizer, has vascular normalizing effects on SCCVII and U87 tumors. Clin. Epigenetics 2016, 8, 53. [Google Scholar] [CrossRef]
- Xiang, M.; Liu, W.; Tian, W.; You, A.; Deng, D. RNA N-6-methyladenosine enzymes and resistance of cancer cells to chemotherapy and radiotherapy. Epigenomics 2020, 12, 801–809. [Google Scholar] [CrossRef]
- Hogg, S.J.; Vervoort, S.J.; Deswal, S.; Ott, C.J.; Li, J.; Cluse, L.A.; Beavis, P.A.; Darcy, P.K.; Martin, B.P.; Spencer, A.; et al. BET-Bromodomain Inhibitors Engage the Host Immune System and Regulate Expression of the Immune Checkpoint Ligand PD-L1. Cell Rep. 2017, 18, 2162–2174. [Google Scholar] [CrossRef]
- Jie, X.; Fong, W.P.; Zhou, R.; Zhao, Y.; Zhao, Y.; Meng, R.; Zhang, S.; Dong, X.; Zhang, T.; Yang, K.; et al. USP9X-mediated KDM4C deubiquitination promotes lung cancer radioresistance by epigenetically inducing TGF-beta2 transcription. Cell Death Differ. 2021, 28, 2095–2111. [Google Scholar] [CrossRef] [PubMed]
| MiRNA | Cancer | Changes and Effects in Cancer before Radiotherapy | Radiation Therapy Affects Its Expression | References |
|---|---|---|---|---|
| MiR-21 | Bladder cancer, breast cancer | Up-regulation, promoting cancer progression, migration and invasion | Increase or decrease | [79,92,93] |
| MiR-155 | Bladder cancer, breast cancer and nasopharyngeal cancer | Up-regulation, promote cancer proliferation and poor prognosis | Increase | [79,80,94,95] |
| MiR-224 | Non-small-cell lung cancer, colorectal cancer and bladder cancer | Up-regulation, promoted cancer proliferation and predicted disease course markers | - | [79,96,97] |
| MiR-196a | Prostate cancer, gastric cancer | Up-regulation, with increased radiosensitivity | Decrease | [98,99] |
| Let-7 | Breast, lung, colorectal cancer | Up-regulation, with increased radiation sensitivity | Decrease | [93,100,101] |
| MiR-142-3p | Breast cancer and Colon cancer | Up-regulation, to stimulate the apoptosis-related genes | Increase | [102,103,104] |
| MiR-142-5p | Gastric cancer, esophageal cancer | Down-regulation, promotes macrophage apoptosis and is closely related to cancer development | Increase | [103,105,106] |
| Sensitizer | Type | Target Spot | Cancer | Reference |
|---|---|---|---|---|
| 5-Aza | DNMT inhibitor | DNMT | Ovarian cancer, sarcoma | [149,152] |
| 5-Aza | DNMT inhibitors | P62/SQSTM1 | Head and neck cancer | [153] |
| SGI-110 | DNMT inhibitor | DNMT | Sarcoma | [152] |
| MS-275 | HDAC inhibitors | P62/SQSTM1 | Head and neck cancer | [153] |
| Entinostat | HDAC inhibitors | FILP | Non-small cell carcinoma | [144] |
| 5-Aza-Cdr | DNMT inhibitors | RUNX3/TLR9 | Carcinoma of the lungs | [154] |
| C-7280948 | PRTM1 inhibitors | PKP2 | Carcinoma of the lungs | [155] |
| JQ1 | BRD4 inhibitors | PD-L1 | Non-small cell carcinoma | [156] |
| JQ1 | BRD4 inhibitors | RAD51AP1 | Cervical carcinoma | [157] |
| RRX-001 | G-6-PD inhibitors | G -6-PD | U87 tumor | [158] |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Wang, Y.; Han, Y.; Jin, Y.; He, Q.; Wang, Z. The Advances in Epigenetics for Cancer Radiotherapy. Int. J. Mol. Sci. 2022, 23, 5654. https://doi.org/10.3390/ijms23105654
Wang Y, Han Y, Jin Y, He Q, Wang Z. The Advances in Epigenetics for Cancer Radiotherapy. International Journal of Molecular Sciences. 2022; 23(10):5654. https://doi.org/10.3390/ijms23105654
Chicago/Turabian StyleWang, Yuexuan, Yu Han, Yuzhen Jin, Qiang He, and Zhicheng Wang. 2022. "The Advances in Epigenetics for Cancer Radiotherapy" International Journal of Molecular Sciences 23, no. 10: 5654. https://doi.org/10.3390/ijms23105654
APA StyleWang, Y., Han, Y., Jin, Y., He, Q., & Wang, Z. (2022). The Advances in Epigenetics for Cancer Radiotherapy. International Journal of Molecular Sciences, 23(10), 5654. https://doi.org/10.3390/ijms23105654






