Endometriosis: Epidemiology, Classification, Pathogenesis, Treatment and Genetics (Review of Literature)
Abstract
1. Endometriosis—History
- -
- First group—includes theories of endometrial transplantation by retrograde menstrual blood as well as mechanical transplantation (e.g., during surgery), and transport by lymphatic and blood vessels.
- -
- Second group—these are theories of the development of endometriosis in situ; that is, from local tissue from the remains of cells or tissues of the fetal embryo or the genitourinary system. The research of Waldeyer, Russell, Reclinghausen, Gebhard and Meyer and Novak contributed to the above theories [4].
- -
2. Endometriosis—Epidemiology
3. Endometriosis—Symptomatology
4. Risk Factors for Endometriosis
- Shorter than 27-day genital cycles, genital defects, including hymen overgrowth or narrowing of the cervical canal [47]. The risk of endometriosis is increased in women with short cycles, i.e., lasting less than 27 days, but is unrelated to the number of bleeding days and the volume of menstruation [48],
- Low BMI,
- Small number of births,
- Caucasian race,
- Age 25–29,
- Daily consumption of alcohol in the amount of at least 10 g per day,
- Endometriosis is more often diagnosed in infertile women who are active smokers and whose body mass index (BMI) is normal or low [49].
5. Theories of the Formation of Endometriosis
6. Types of Endometriosis
- Ovarian endometriosis—occurs in the form of superficial lesions and as endometrial cysts,
- Peritoneal—can occur in various forms: white raids on the peritoneum, peritoneal defects, red, brown, black-blue and black foci, colorless bright vesicles and focal dilated blood vessels and petechiae,
- Deep infiltrating endometriosis—DIE,
- Endometriosis of other locations.
7. Classifications of Endometriosis
- -
- Internal endometriosis affecting the uterine muscle
- -
- External endometriosis occurring outside the uterine muscle
- Mucosal type (occurs in endometrial cysts of the ovary),
- Operitoneal type (exhibits multi-focus and morphological diversity)
- -
- early, active, glandular or follicular lesions,
- -
- advanced, black, wrinkled changes,
- -
- white fibrotic lesions,
- Glandular type (the main element is fibrous-muscular tissue and concerns deeply infiltrating endometriosis).
- -
- Compartment A—foci located in the vagina and the rectovaginal septum,
- -
- Compartment B—foci located in the sacro-uterine ligaments up to the pelvic walls,
- -
- Compartment C—foci located in the sigmoid colon and rectum.
- FA—adenomyosis,
- FB—urinary bladder endometriosis,
- FU—ureter endometriosis,
- FI—endometriosis of the bowel wall above the sigmoid colon,
- FO—infiltration of other anatomical structures, e.g., abdominal integuments.
8. Diagnostics
9. Treatment
9.1. Pharmacological Treatment
9.2. Surgical Treatment
- -
- pelvic pain,
- -
- infertility in endometriosis,
- -
- endometrial ovarian cysts.
9.3. Physiotherapy in Endometriosis
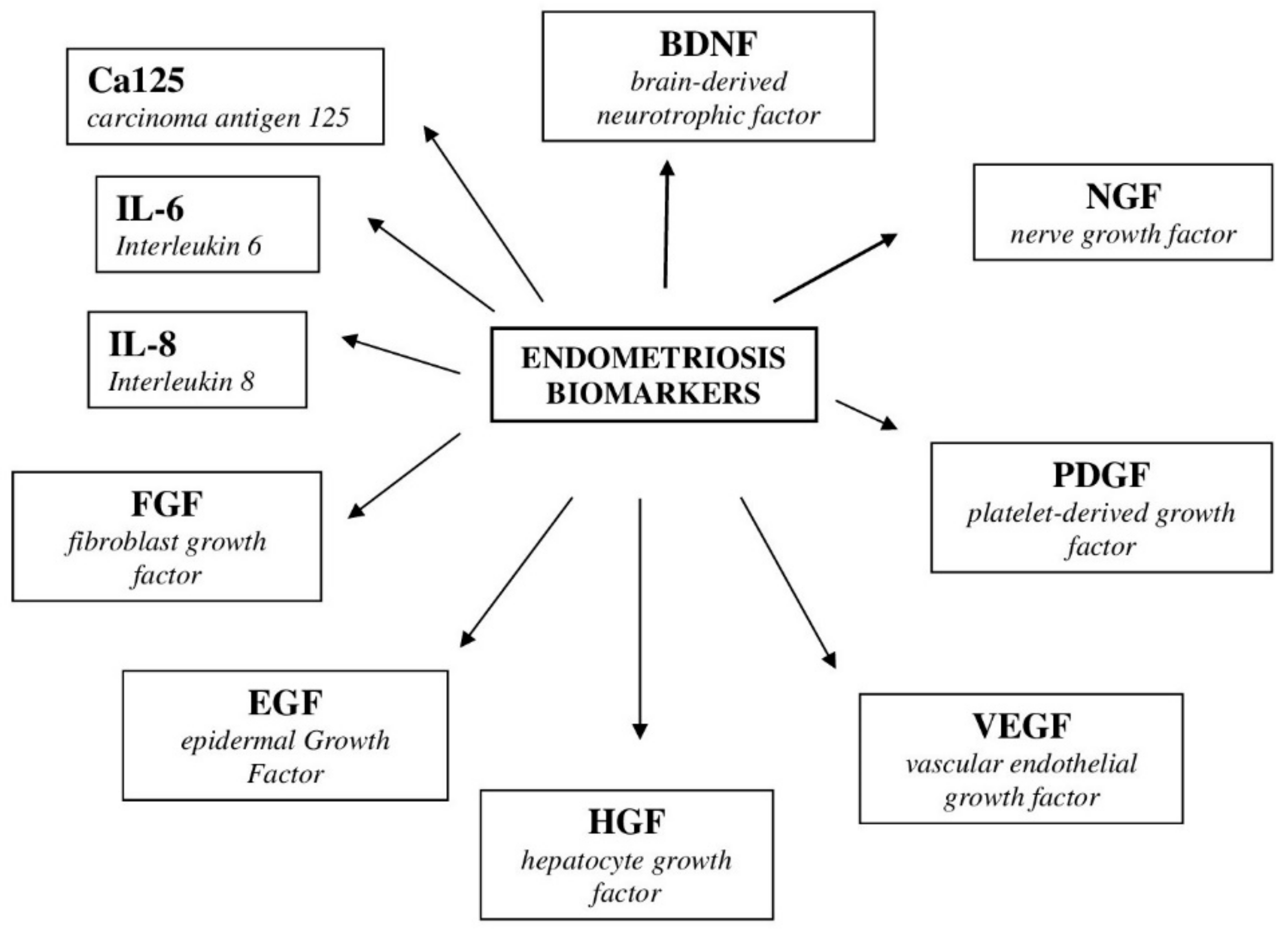
10. Biomarkers
11. Endometriosis—Genetics
11.1. Hereditary Genetic Polymorphism
11.2. Somatic Mutations
12. Summary
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Benagiano, G.; Brosens, I.; Lippi, D. The history of endometriosis. Gynecol. Obstet. Investig. 2014, 78, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Rokitansky, K. Uber uterusdrusen neubildung. Ztchr Gesselsch Arzte Wein 1860, 16, 577. [Google Scholar]
- Benagiano, G.; Brosens, I. History of adenomyosis. Best Pract. Res. Clin. Obstet. Gynaecol. 2006, 20, 449–463. [Google Scholar] [CrossRef] [PubMed]
- Kanikowska, D.; Markowska, J.; Wiktorowicz, K. Historia badań nad endometriozą. Polski Przegląd Nauk Zdrowiu 2010, 1, 42–45. [Google Scholar]
- Sampson, J.A. Metastatic or embolic endometriosis, due to the menstrual dis- semination of endometrial tissue into the venous circulation. Am. J. Pathol. 1927, 3, 93. [Google Scholar] [PubMed]
- Sampson, J.A. Peritoneal endometriosis due to the menstrual dissemination of endometrial tissue into the peritoneal cavity. Am. J. Obstet. Gynecol. 1927, 14, 422–469. [Google Scholar] [CrossRef]
- Nap, A.W.; Groothuis, P.G.; Demir, A.Y.; Evers, J.L.; Dunselman, G.A. Pathogenesis of endometriosis. Best Pract. Res. Clin. Obstet. Gynaecol. 2004, 18, 233–244. [Google Scholar] [CrossRef]
- Quinn, M. Endometriosis: The consequence of neurological disfunction? Med. Hypoth. 2004, 63, 602–608. [Google Scholar] [CrossRef]
- Schindler, A.E. Pathophysiology, diagnosis and treatment of endometriosis. Miverva Ginecol. 2004, 56, 419–435. [Google Scholar]
- Witz, C. Pathogenesis of endometriosis. Gynecol. Obstet. Investig. 2002, 53, 52–62. [Google Scholar] [CrossRef]
- Burney, R.; Giudice, L. Pathogenesis and pathophysiology of endometriosis. Fertil. Steril. 2012, 98, 511–519. [Google Scholar] [CrossRef] [PubMed]
- Giudice, L.C.; Kao, L.C. Endometriosis. Lancet 2004, 364, 1789–1799. [Google Scholar] [CrossRef]
- Nezhat, C.; Falik, R.; McKinney, S.; King, L.P. Pathophysiology and management of urinary tract endometriosis. Nat. Rev. Urol. 2017, 14, 359–372. [Google Scholar] [CrossRef]
- Missmer, S.A.; Hankinson, S.E.; Spiegelman, D.; Barbieri, R.L.; Marshall, L.M.; Hunter, D.J. Incidence of laparoscopically confirmed endometriosis by demographic, anthropometric, and lifestyle factors. Am. J. Epidemiol. 2004, 160, 784–796. [Google Scholar] [CrossRef]
- Agarwal, S.K.; Chapron, C.; Giudice, L.C.; Laufer, M.R.; Leyland, N.; Missmer, S.A.; Singh, S.S.; Taylor, H.S. Clinical diagnosis of endometriosis: A call to action. Am. J. Obstet. Gynecol. 2019, 220, 354.e1–354.e12. [Google Scholar] [CrossRef]
- Maggiore, U.L.R.; Ferrero, S.; Mangili, G.; Bergamini, A.; Inversetti, A.; Giorgione, V.; Viganò, P.; Candiani, M. A systematic review on endometriosis during pregnancy: Diagnosis, misdiagnosis, complications and outcomes. Hum. Reprod. Update 2016, 22, 70–103. [Google Scholar] [CrossRef] [PubMed]
- Defrère, S.; Lousse, J.C.; González-Ramos, R.; Colette, S.; Donnez, J.; Van Langendonckt, A. Potential involvement of iron in the pathogenesis of peritoneal endometriosis. Mol. Hum. Reprod. 2008, 14, 377–385. [Google Scholar] [CrossRef]
- Eskenazi, B.; Warner, M. Epidemiology of endometriosis. Obstet. Gynecol. Clin. N. Am. 1997, 24, 235–258. [Google Scholar] [CrossRef]
- Lu, P.; Ory, S. Endometriosis: Current management. Mayo Clin. Proc. 1995, 70, 453–463. [Google Scholar] [CrossRef] [PubMed]
- Dmowski, W. Endometriosis at the end of the millenium; the controversy remains. Pol. J. Gyn. Investig. 1999, 1, 175–186. [Google Scholar]
- Kao, L.C.; Tulac, S.; Lobo, S.; Imani, B.; Yang, J.P.; Germeyer, A.; Osteen, K.; Taylor, R.N.; Lessey, B.A.; Giudice, L.C. Global gene profiling in human endometrium during the window of implantation. Endocrinology 2002, 143, 2119–2138. [Google Scholar] [CrossRef]
- Cramer, D.W.; Missmer, S.A. The epidemiology of endometriosis. Ann. N. Y. Acad. Sci. 2002, 955, 11–22. [Google Scholar] [CrossRef] [PubMed]
- Gadomska, H.; Kamiński, P.; Marianowski, L. Endometrioza. Medipress Ginekol. 1997, 3, 2–5. [Google Scholar]
- Signorile, P.G.; Baldi, F.; Bussani, R.; D’Armiento, M.; De Falco, M.; Boccellino, M.; Quagliuolo, L.; Baldi, A. New evidence of the presence of endometriosis in the human fetus. Reprod. Biomed. Online 2010, 21, 142–147. [Google Scholar] [CrossRef] [PubMed]
- Martin, J.D.; Hauck, A.E. Endometriosis in the male. Am. Surg. 1985, 51, 426–430. [Google Scholar]
- Goldstein, D.P.; de Cholnoky, C.; Emans, S.J.; Leventhal, J.M. Laparoscopy on the diagnosis and management of pelvic pain in adolescents. J. Reprod. Med. 1980, 24, 251–256. [Google Scholar] [PubMed]
- Simoens, S.; Dunselman, G.; Dirksen, C.; Hummelshoj, L.; Bokor, A.; Brandes, I.; Brodszky, V.; Canis, M.; Colombo, G.L.; DeLeire, T.; et al. The burden of endometriosis: Costs and quality of life of women with endometriosis and treated in referral centres. Hum. Reprod. 2012, 27, 1292–1299. [Google Scholar] [CrossRef]
- Nnoaham, K.E.; Hummelshoj, L.; Webster, P.; d’Hooghe, T.; de Cicco Nardone, F.; de Cicco Nardone, C.; Jenkinson, C.; Kennedy, S.H.; Zondervan, K.T. World Endometriosis Research Foundation Global Study of Women’s Health consortium. Impact of endometriosis on quality of life and work productivity: A multi-center study across ten countries. Fertil. Steril. 2011, 96, 366–373. [Google Scholar] [CrossRef]
- De Graaff, A.A.; D’Hooghe, T.M.; Dunselman, G.A.; Dirksen, C.D.; Hummelshoj, L.; WERF EndoCost Consortium; Simoens, S. The significant effect of endometriosis on physical, mental and social well-being: Results from an inter-national cross-sectional survey. Hum. Reprod. 2013, 28, 2677–2685. [Google Scholar] [CrossRef]
- Vessey, M.P.; Villerd-Mackintosh, L.; Painter, R. Epidemiology of endometriosis in women attending family planning clinics. BMJ 1993, 306, 182–184. [Google Scholar] [CrossRef]
- Vigano, P.; Parazzini, F.; Somigliana, E.; Vercellini, P. Endometriosis: Epidemiology and eathiological factors. Best Pract. Res. Clin. Obstet. Gynaecol. 2004, 18, 177–200. [Google Scholar] [CrossRef]
- Bourdel, N.; Matsusakï, S.; Roman, H.; Lenglet, Y.; Botchorischvili, R.; Mage, G.; Canis, M. Endometriosis in teenagers. Gynecol. Obstet. Fertil. 2006, 34, 727–734. [Google Scholar] [CrossRef]
- Kowalczyk-Amico, K.; Szubert, M.; Suzin, J. Angiogenesis and inflammatory response in endometriosis. Przeglad Menopauzalny 2009, 5, 261–264. [Google Scholar]
- Jakiel, G.; Robak-Chołubek, D.; Tkaczuk-Włach, J. Endometriosis. Przeglad Menopauzalny 2006, 2, 126–129. [Google Scholar]
- Loring, M.; Chen, T.Y.; Isaacson, K.B. A Systematic Review of Adenomyosis: It Is Time to Reassess What We Thought We Knew about the Disease. J. Minim. Invasive Gynecol. 2021, 28, 644–655. [Google Scholar] [CrossRef] [PubMed]
- Ferenczy, A. Pathophysiology of adenomyosis. Hum. Reprod. Update 1998, 4, 312–322. [Google Scholar] [CrossRef] [PubMed]
- Kold, M.; Hansen, T.; Vedsted-Hansen, H.; Forman, A. Mindfulness-based psychological intervention for coping with pain in endometriosis. Nord. Psychol. 2016, 68, 144–146. [Google Scholar] [CrossRef]
- Ahn, S.H.; Singh, V.; Tayade, C. Biomarkers in endometriosis: Challenges and opportunities. Fertil. Steril. 2017, 107, 523–532. [Google Scholar] [CrossRef] [PubMed]
- Nisenblat, V.; Bossuyt, P.M.; Shaikh, R.; Farquhar, C.; Jordan, V.; Scheffers, C.S.; Mol, B.W.; Johnson, N.; Hull, M.L. Blood biomarkers for the non-invasive diagnosis of endometriosis. Cochrane Database Syst. Rev. 2016, 1, CD012179. [Google Scholar] [CrossRef]
- Gupta, D.; Hull, M.L.; Fraser, I.; Miller, L.; Bossuyt, P.M.; Johnson, N.; Nisenblat, N.J.V. Endometrial biomarkers for the non-invasive diagnosis of endometriosis. Cochrane Database Syst. Rev. 2016, 4, CD012165. [Google Scholar] [CrossRef]
- Fraga, M.V.; Oliveira Brito, L.G.; Yela, D.A.; de Mira, T.A.; Benetti-Pinto, C.L. Pelvic floor muscle dysfunctions in women with deep infiltrative endometriosis: An underestimated association. Int. J. Clin. Pract. 2021, 75, e14350. [Google Scholar] [CrossRef] [PubMed]
- Mabrouk, M.; Raimondo, D.; Arena, A.; Iodice, R.; Altieri, M.; Sutherland, N.; Salucci, P.; Moro, E.; Seracchioli, R. Parametrial Endometriosis: The Occult Condition that Makes the Hard Harder. J. Minim. Invasive Gynecol. 2019, 26, 871–876. [Google Scholar] [CrossRef] [PubMed]
- Cramer, D.W.; Wilson, E.; Stillman, R.J.; Berger, M.J.; Belisle, S.; Schiff, I.; Albrecht, B.; Gibson, M.; Stadel, B.V.; Schoenbaum, S.C. The relation of endometriosis to menstrual characteristic, smoking, and exercise. JAMA 1986, 255, 1904–1908. [Google Scholar] [CrossRef] [PubMed]
- Parazzini, F.; La Vecchia, C.; Franceschi, S.; Negri, E.; Cecchetti, G. Risk faktors for endometroid, mucinous, and serous benign ovarian cysts. Int. J. Epidemiol. 1989, 18, 108–112. [Google Scholar] [CrossRef]
- Matorras, R.; Rodíquez, F.; Pijoan, J.I.; Ramón, O.; Gutierrez de Terán, G.; Rodríguez-Escudero, F. Epidemiology of endometriosis in infertile woman. Fertil. Steril. 1995, 63, 34–38. [Google Scholar] [CrossRef]
- Parazzini, F.; Ferraroni, M.; Fedele, L.; Bocciolone, L.; Rubessa, S.; Riccardi, A. Pelvic endometriosis: Reproductive and menstrual risk factors at different stages in Lombardy, northern Italy. J. Epidemiol. Community Health 1995, 49, 61–64. [Google Scholar] [CrossRef]
- Falcone, T.; Flyckt, R. Clinical Management of Endometriosis. Obstet. Gynecol. 2018, 131, 557–571. [Google Scholar] [CrossRef]
- Moen, M.H.; Schei, B. Epidemiology of endometriosis in a Norwegian county. Acta Obstet. Gynecol. Scand. 1997, 76, 559–562. [Google Scholar] [CrossRef]
- Molgaard, C.A.; Golbeck, A.L.; Gresham, L. Current concepts in endometriosis. West J. Med. 1985, 143, 42–46. [Google Scholar]
- Tang, Y.; Zhao, M.; Lin, L.; Gao, Y.; Chen, G.Q.; Chen, S.; Chen, Q. Is body mass index associated with the incidence of endometriosis and the severity of dysmenorrhoea: A case-control study in China? BMJ Open 2020, 10, e037095. [Google Scholar] [CrossRef]
- Parazzini, F.; Chiaffarino, F.; Surace, M.; Chatenoud, L.; Cipriani, S.; Chiantera, V.; Benzi, G.; Fedele, L. Selected food intake and risk of endometriosis. Hum. Reprod. 2004, 19, 1755–1759. [Google Scholar] [CrossRef]
- Yamamoto, A.; Harris, H.R.; Vitonis, A.F.; Chavarro, J.E.; Missmer, S.A. A prospective cohort study of meat and fish consumption and endometriosis risk. Am. J. Obstet. Gynecol. 2018, 219, 178.e1–178.e10. [Google Scholar] [CrossRef]
- Vinatier, D.; Orazi, G.; Cosson, M.; Dufour, P. Theories of endometriosis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2001, 96, 21–34. [Google Scholar] [CrossRef]
- Witz, C.A.; Schenken, R.S. Semin Reprod Endocrinol. Pathogenesis 1997, 15, 199–208. [Google Scholar]
- Rana, N.; Braun, D.P.; House, R.; Gebel, H.; Rotman, C.; Dmowski, W.P. Basal and stimulated secretion of cytokines by peritoneal macrophages in women with endometriosis. Fertil. Steril. 1996, 65, 925–930. [Google Scholar] [CrossRef]
- Lebovic, D.I.; Mueller, M.D.; Taylor, R.N. Immunobiology of endometriosis. Fertil. Steril. 2001, 75, 1–10. [Google Scholar] [CrossRef]
- Sinaii, N.; Cleary, S.D.; Ballweg, M.L.; Nieman, L.K.; Stratton, P. High rates of autoimmune and endocrine disorders, fibromyalgia, chronic fatigue syndrome and atopic diseases among women with endometriosis: A survey analysis. Hum. Reprod. 2002, 17, 2715–2724. [Google Scholar] [CrossRef] [PubMed]
- Fujii, S. Secondary Müllerian system and endometriosis. Am. J. Obstet. Gynecol. 1991, 165, 219–225. [Google Scholar] [CrossRef]
- Laganà, A.S.; Garzon, S.; Götte, M.; Viganò, P.; Franchi, M.; Ghezzi, F.; Martin, D.C. The Pathogenesis of Endometriosis: Molecular and Cell Biology Insights. Int. J. Mol. Sci. 2019, 20, 5615. [Google Scholar] [CrossRef]
- Koninckx, P.R.; Kennedy, S.H.; Barlow, D.H. Endometriotic disease: The role of peritoneal fluid. Hum. Reprod. Update 1998, 4, 741–751. [Google Scholar] [CrossRef]
- Reese, K.A.; Reddy, S.; Rock, J.A. Endometriosis in an adolescent population: The emory experience. J. Pediatr. Adolesc. Gynecol. 1996, 9, 125–128. [Google Scholar] [CrossRef]
- Matarese, G.; DePlacido, G.; Nikas, Y.; Alviggi, C. Pathogenesis of endometriosis: Natura limmunity dysfunction or autoimmune disease? Trends Mol. Med. 2003, 9, 223–228. [Google Scholar] [CrossRef]
- Dmowski, W.; Steele, R.; Baker, G. Deficient cellular immunity in endometriosis. Am. J. Obstet. Gynecol. 1981, 14, 377–388. [Google Scholar] [CrossRef]
- Burney, R.O. Biomarker development in endometriosis. Scand. J. Clin. Lab. Investig. Suppl. 2014, 244, 75–81. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Asghari, S.; Valizadeh, A.; Aghebati-Maleki, L.; Nouri, M.; Yousefi, M. Endometriosis: Perspective, lights, and shadows of etiology. Biomed. Pharm. 2018, 106, 163–174. [Google Scholar] [CrossRef]
- Lee, Y.H.; Cui, L.; Fang, J.; Chern, B.S.; Tan, H.H.; Chan, J.K. Limited value of pro-inflammatory oxylipins and cytokines as circulating biomarkers in endometriosis—A targeted ‘omics study. Sci. Rep. 2016, 6, 1–7. [Google Scholar] [CrossRef]
- Ulukus, M.; Ulukus, E.C.; Tavmergen Goker, E.N.; Tavmergen, E.; Zheng, W.; Arici, A. Expression of interleukin-8 and monocyte chemotactic protein 1 in women with endometriosis. Fertil. Steril. 2009, 91, 687–693. [Google Scholar] [CrossRef]
- King, A.E.; Critchley, H.O.; Kelly, R.W. The NF-κB pathway in human endometrium and first trimester decidua. Mol. Hum. Reprod. 2001, 7, 175–183. [Google Scholar] [CrossRef]
- Yoshida, S.; Amano, H.; Hayashi, I.; Kitasato, H.; Kamata, M.; Inukai, M.; Yoshimura, H.; Majima, M. COX-2/VEGF-dependent facilitation of tumor-associated angiogenesis and tumor growth in vivo. Lab. Investig. 2003, 83, 1385–1394. [Google Scholar] [CrossRef] [PubMed]
- Sikora, J.; Mielczarek-Palacz, A.; Kondera-Anasz, Z. Role of natural killer cell activity in the pathogenesis of endometriosis. Curr. Med. Chem. 2011, 18, 200–208. [Google Scholar] [CrossRef]
- Suen, J.L.; Chang, Y.; Chiu, P.R.; Hsieh, T.H.; Hsi, E.; Chen, Y.C.; Chen, Y.F.; Tsai, E.M. Serum level of IL-10 is increased in patients with endometriosis, and IL-10 promotes the growth of lesions in a murine model. Am. J. Pathol. 2014, 184, 464–471. [Google Scholar] [CrossRef]
- Dunn, C.L.; Critchley, H.O.; Kelly, R.W. IL-15 regulation in human endometrial stromal cells. J. Clin. Endocrinol. Metab. 2002, 87, 1898–1901. [Google Scholar] [CrossRef] [PubMed]
- Koga, K.; Osuga, Y.; Yoshino, O.; Hirota, Y.; Yano, T.; Tsutsumi, O.; Taketani, Y. Elevated interleukin-16 levels in the peritoneal fluid of women with endometriosis may be a mechanism for inflammatory reactions associated with endometriosis. Fertil. Steril. 2005, 83, 878–882. [Google Scholar] [CrossRef]
- Azimzadeh, P.; Khorram Khorshid, H.R.; Akhondi, M.M.; Shirazi, A. Association of interleukin-16 polymorphisms with disease progression and susceptibility in endometriosis. Int. J. Immunogenet. 2016, 43, 297–302. [Google Scholar] [CrossRef] [PubMed]
- Borrelli, G.M.; Carvalho, K.; Kallas, E.G.; Mechsner, S.; Baracat, E.C.; Abrão, M.S. Chemokines in the pathogenesis of endometriosis and infertility. J. Reprod. Immunol. 2013, 98, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Meka, R.R.; Venkatesha, S.H.; Dudics, S.; Acharya, B.; Moudgil, K.D. IL-27-induced modulation of autoimmunity and its therapeutic potential. Autoimmun. Rev. 2015, 14, 1131–1141. [Google Scholar] [CrossRef]
- Santulli, P.; Borghese, B.; Chouzenoux, S.; Vaiman, D.; Borderie, D.; Streuli, I.; Goffinet, F.; de Ziegler, D.; Weill, B.; Batteux, F.; et al. Serum and peritoneal interleukin-33 levels are elevated in deeply infiltrating endometriosis. Hum. Reprod. 2012, 27, 2001–2009. [Google Scholar] [CrossRef]
- Kaabachi, W.; Kacem, O.; Belhaj, R.; Hamzaoui, A.; Hamzaoui, K. Interleukin-37 in endometriosis. Immunol. Lett. 2017, 185, 52–55. [Google Scholar] [CrossRef]
- Witz, C.A.; Allsup, K.T.; Montoya-Rodriguez, I.A.; Vaughan, S.L.; Centonze, V.E.; Schenken, R.S. Pathogenesis of endometriosis--current research. Hum. Fertil. 2003, 6, 34–40. [Google Scholar] [CrossRef]
- Hill, J. Immunology and endometriosis. Fertil. Steril. 1992, 58, 262–264. [Google Scholar] [CrossRef]
- Laschke, M.W.; Giebels, C.; Menger, M.D. Vasculogenesis: A new piece of the endometriosis puzzle. Hum. Reprod. Update 2011, 17, 628–636. [Google Scholar] [CrossRef]
- McLaren, J.; Prentice, A.; Charnock-Jones, D.S.; Smith, S.K. Vascular endothelial growth factor (VEGF) concentrations are elevated in peritoneal fluid of women with endometriosis. Hum. Reprod. 1996, 11, 220–223. [Google Scholar] [CrossRef] [PubMed]
- Halis, G.; Arici, A. Endometriosis and inflammation in infertility. Ann. N. Y. Acad. Sci. 2004, 1034, 300–315. [Google Scholar] [CrossRef] [PubMed]
- Florova, M.S.; Yarmolinskaya, M.I.; Potin, V.V. Prospects of metformin in the treatment of endometriosis. J. Obstet. Woman Dis. 2017, 66, 67–76. [Google Scholar] [CrossRef][Green Version]
- Hudelist, G.; Ballard, K.; English, J.; Wright, J.; Banerjee, S.; Mastoroudes, H.; Thomas, A.; Singer, C.F.; Keckstein, J. Transvaginal sonography vs clinical examination in the preoperative diagnosis of deep infiltrating endometriosis. Ultrasound Obstet. Gynecol. 2011, 37, 480–487. [Google Scholar] [CrossRef] [PubMed]
- Crispi, C.P.; de Souza, C.A.; Oliveira, M.A.; Dibi, R.P.; Cardeman, L.; Sato, H.; Schor, E. Endometriosis of the round ligament of uterus. J. Minim. Invasive Gynecol. 2012, 19, 46–51. [Google Scholar] [CrossRef]
- Dunselman, G.A.; Vermeulen, N.; Becker, C.; Calhaz-Jorge, C.; D’Hooghe, T.; De Bie, B.; Heikinheimo, O.; Horne, A.W.; Kiesel, L.; Nap, A.; et al. ESHRE guideline: Management of women with endometriosis. Hum. Reprod. 2014, 29, 400–412. [Google Scholar] [CrossRef]
- Sampson, J.A. Perforating hemorrhagic (chocolate) cysts of the ovary: Their importance and especially their relation to pelvic adenomas of endometrial type (“adenomyoma” of the uterus, rectovaginal septum, sigmoid, etc.). Arch. Surg. 1921, 3, 245–323. [Google Scholar] [CrossRef]
- Krasa, A.; Kozioł, M.; Piecewicz-Szczęsna, H.; Pawlicki, M.; Łopuszyńska, A.; Krawiec, P.; Piekarska, E. Endometriosis and an increased risk of malignancies. A literature review. J. Educ. Health Sport 2020, 10, 290–298. [Google Scholar] [CrossRef]
- Kistner, R.W.; Siegler, A.M.; Behrman, S.J. Suggested classification for endometriosis: Relationship to infertility. Fertil. Steril. 1977, 28, 1008–1010. [Google Scholar] [CrossRef]
- Brosens, I.A. Classification of endometriosis revisited. Lancet 1993, 341, 630. [Google Scholar] [CrossRef]
- Damario, M.A.; Rock, J.A. Classification of endometriosis. Semin. Reprod. Endocrinol. 1997, 15, 235–244. [Google Scholar] [CrossRef] [PubMed]
- Gilmour, J.A.; Huntington, A.; Wilson, H.V. The impact of endometriosis on work and social participation. Int. J. Nurs. Pract. 2008, 14, 443–448. [Google Scholar] [CrossRef]
- Szamatowicz, M. Endometriosis—Still an enigmatic disease. What are the causes, how to diagnose it and how to treat successfully? Gynecol. Endocrinol. 2008, 24, 535–536. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tuttlies, F.; Keckstein, J.; Ulrich, U.; Possover, M.; Schweppe, K.W.; Wustlich, M.; Buchweitz, O.; Greb, R.; Kandolf, O.; Mangold, R.; et al. ENZIAN-score, a classification of deep infiltrating endometriosis. Zent. Gynakol. 2005, 127, 275–281. [Google Scholar] [CrossRef] [PubMed]
- Plodeck, V.; Sommer, U.; Baretton, G.B.; Aust, D.E.; Laniado, M.; Hoffmann, R.T.; Platzek, I. A rare case of pancreatic endometriosis in a postmenopausal woman and review of the literature. Acta Radiol. Open 2016, 5, 2058460116669385. [Google Scholar] [CrossRef] [PubMed]
- Andrade, M.T.; de Freitas, C.V.; Câmara, S.F.; Vieira, J.J. Umbilical nodule with cyclical bleeding: A case report and literature review of atypical endometriosis. Case Rep. Obstet. Gynecol. 2016, 2016, 7401409. [Google Scholar] [CrossRef]
- Fassbender, A.; Vodolazkaia, A.; Saunders, P.; Lebovic, D.; Waelkens, E.; De Moor, B.; D’Hooghe, T. Biomarkers of endometriosis. Fertil. Steril. 2013, 99, 1135–1145. [Google Scholar] [CrossRef]
- Leyland, N.; Casper, R.; Laberge, P.; Singh, S.S.; SOGC. Endometriosis: Diagnosis and management. J. Obstet. Gynaecol. Can. 2010, 32, S1–S32. [Google Scholar] [CrossRef]
- Cornillie, F.J.; Oosterlynck, D.; Lauweryns, J.M.; Koninckx, P.R. Deeply infiltrating pelvic endometriosis: Histology and clinical significance. Fertil. Steril. 1990, 53, 978–983. [Google Scholar] [CrossRef]
- Chapron, C.; Chopin, N.; Borghese, B.; Foulot, H.; Dousset, B.; Vacher-Lavenu, M.C.; Vieira, M.; Hasan, W.; Bricou, A. Deeply infiltrating endometriosis: Pathogenetic implications of the anatomical distribution. Hum. Reprod. 2006, 21, 1839–1845. [Google Scholar] [CrossRef]
- Seracchioli, R.; Poggioli, G.; Pierangeli, F.; Manuzzi, L.; Gualerzi, B.; Savelli, L.; Remorgida, V.; Mabrouk, M.; Venturoli, S. Surgical outcome and long-term follow up after laparoscopic rectosigmoid resection in women with deep infiltrating endometriosis. BJOG 2007, 114, 889–895. [Google Scholar] [CrossRef]
- Raimondo, D.; Youssef, A.; Mabrouk, M.; Del Forno, S.; Martelli, V.; Pilu, G.; Rizzo, N.; Zannoni, L.; Paradisi, R.; Seracchioli, R. Pelvic floor muscle dysfunction on 3D/4D transperineal ultrasound in patients with deep infiltrating endometriosis: A pilot study. Ultrasound Obstet. Gynecol. 2017, 50, 527–532. [Google Scholar] [CrossRef] [PubMed]
- Dietz, H.P. Pelvic floor ultrasound: A review. Am. J. Obstet. Gynecol. 2010, 202, 321–334. [Google Scholar] [CrossRef] [PubMed]
- Youssef, A.; Montaguti, E.; Sanlorenzo, O.; Cariello, L.; Salsi, G.; Morganelli, G.; Azzarone, C.; Pilu, G.; Rizzo, N. Reliability of new three-dimensional ultrasound technique for pelvic hiatal area measurement. Ultrasound Obstet. Gynecol. 2016, 47, 629–635. [Google Scholar] [CrossRef]
- Mabrouk, M.; Raimondo, D.; Parisotto, M.; Del Forno, S.; Arena, A.; Seracchioli, R. Pelvic floor dysfunction at transperineal ultrasound and voiding alteration in women with posterior deep endometriosis. Int. Urogynecol. J. 2019, 30, 1527–1532. [Google Scholar] [CrossRef]
- Mabrouk, M.; Raimondo, D.; Del Forno, S.; Baruffini, F.; Arena, A.; Benfenati, A.; Youssef, A.; Martelli, V.; Seracchioli, R. Pelvic floor muscle assessment on three- and four-dimensional transperineal ultrasound in women with ovarian endometriosis with or without retroperitoneal infiltration: A step towards complete functional assessment. Ultrasound Obstet. Gynecol. 2018, 52, 265–268. [Google Scholar] [CrossRef]
- Youssef, A.; Montaguti, E.; Sanlorenzo, O.; Cariello, L.; Awad, E.E.; Pacella, G.; Ghi, T.; Pilu, G.; Rizzo, N. A new simple technique for 3-dimensional sonographic assessment of the pelvic floor muscles. J. Ultrasound Med. 2015, 34, 65–72. [Google Scholar] [CrossRef]
- Faubion, S.S.; Shuster, L.T.; Bharucha, A.E. Recognition and management of nonrelaxing pelvic floor dysfunction. Mayo Clin. Proc. 2012, 87, 187–193. [Google Scholar] [CrossRef]
- Gehrich, A.P.; Aseff, J.N.; Iglesia, C.B.; Fischer, J.R.; Buller, J.L. Chronic urinary retention and pelvic floor hypertonicity after surgery for endometriosis: A case series. Am. J. Obstet. Gynecol. 2005, 193, 2133–2137. [Google Scholar] [CrossRef] [PubMed]
- Tu, F.F.; Holt, J.; Gonzales, J.; Fitzgerald, C.M. Physical therapy evaluation of patients with chronic pelvic pain: A controlled study. Am. J. Obstet. Gynecol. 2008, 198, 272.e1–272.e7. [Google Scholar] [CrossRef] [PubMed]
- Beck, J.J.; Elzevier, H.W.; Pelger, R.C.; Putter, H.; Voorham-van der Zalm, P.J. Multiple pelvic floor complaints are correlated with sexual abuse history. J. Sex. Med. 2009, 6, 193–198. [Google Scholar] [CrossRef] [PubMed]
- Chapron, C.; Santulli, P.; de Ziegler, D.; Noel, J.C.; Anaf, V.; Streuli, I.; Foulot, H.; Souza, C.; Borghese, B. Ovarian endometrioma: Severe pelvic pain is associated with deeply infiltrating endometriosis. Hum. Reprod. 2012, 27, 702–711. [Google Scholar] [CrossRef] [PubMed]
- Horne, A.W.; Daniels, J.; Hummelshoj, L.; Cox, E.; Cooper, K.G. Surgical removal of superficial peritoneal endometriosis for managing women with chronic pelvic pain: Time for a rethink? BJOG 2019, 126, 1414–1416. [Google Scholar] [CrossRef] [PubMed]
- Basta, A.; Brucka, A.; Górski, J.; Kotarski, J.; Kulig, B.; Oszukowski, P.; Poręba, R.; Radowicki, S.; Radwan, J.; Sikora, J.; et al. Stanowisko Zespołu Ekspertów Polskiego Towarzystwa Ginekologicznego dotyczące diagnostyki i metod leczenia endometriozy. Ginekol. Pol. 2012, 83, 871–876. [Google Scholar] [PubMed]
- Donnez, J.; Dolmans, M.M. Endometriosis and Medical Therapy: From Progestogens to Progesterone Resistance to GnRH Antagonists: A Review. J. Clin. Med. 2021, 10, 1085. [Google Scholar] [CrossRef]
- Taylor, H.S.; Giudice, L.C.; Lessey, B.A.; Abrao, M.S.; Kotarski, J.; Archer, D.F.; Diamond, M.P.; Surrey, E.; Johnson, N.P.; Watts, N.B.; et al. Treatment of Endometriosis-Associated Pain with Elagolix, an Oral GnRH Antagonist. N. Engl. J. Med. 2017, 377, 28–40. [Google Scholar] [CrossRef]
- Shebley, M.; Polepally, A.R.; Nader, A.; Ng, J.W.; Winzenborg, I.; Klein, C.E.; Noertersheuser, P.; Gibbs, M.A.; Mostafa, N.M. Clinical Pharmacology of Elagolix: An Oral Gonadotropin-Releasing Hormone Receptor Antagonist for Endometriosis. Clin. Pharm. 2020, 59, 297–309. [Google Scholar] [CrossRef]
- Bradley, C.A. Reproductive endocrinology: Elagolix in endometriosis. Nat. Rev. Endocrinol. 2017, 13, 439. [Google Scholar] [CrossRef]
- Kilpatrick, R.D.; Chiuve, S.E.; Leslie, W.D.; Wegrzyn, L.R.; Gao, W.; Yang, H.; Soliman, A.M.; Snabes, M.C.; Koenigsberg, S.; Zhong, J.; et al. Estimating the Effect of Elagolix Treatment for Endometriosis on Postmenopausal Bone Outcomes: A Model Bridging Phase III Trials to an Older Real-World Population. JBMR Plus 2020, 4, e10401. [Google Scholar] [CrossRef]
- Abbas Suleiman, A.; Nader, A.; Winzenborg, I.; Beck, D.; Polepally, A.R.; Ng, J.; Noertersheuser, P.; Mostafa, N.M. Exposure-Safety Analyses Identify Predictors of Change in Bone Mineral Density and Support Elagolix Labeling for Endometriosis-Associated Pain. CPT Pharmacometrics. Syst. Pharm. 2020, 9, 639–648. [Google Scholar]
- Schipper, E.; Nezhat, C. Video-assisted laparoscopy for the detection and diagnosis of endometriosis: Safety, reliability, and invasiveness. Int. J. Womens Health 2012, 4, 383–393. [Google Scholar]
- Roman, H.; Vassilieff, M.; Tuech, J.; Huet, E.; Savoye, G.; Marpeau, L.; Puscasiu, L. Postoperative digestive function after radical versus conservative surgical philosophy for deep endometriosis infiltrating the rectum. Fertil. Steril. 2013, 99, 1695–1704. [Google Scholar] [CrossRef]
- Spagnolo, E.; Zannoni, L.; Raimondo, D.; Ferrini, G.; Mabrouk, M.; Benfenati, A.; Villa, G.; Bertoldo, V.; Seracchioli, R. Urodynamic Evaluation and Anorectal Manometry Pre- and Post-operative Bowel Shaving Surgical Procedure for Posterior Deep Infiltrating Endometriosis: A Pilot Study. J. Minim. Invasive Gynecol. 2014, 21, 1080–1085. [Google Scholar] [CrossRef]
- Mabrouk, M.; Raimondo, D.; Altieri, M.; Arena, A.; Del Forno, S.; Moro, E.; Mattioli, G.; Iodice, R.; Seracchioli, R. Surgical, Clinical, and Functional Outcomes in Patients with Rectosigmoid Endometriosis in the Gray Zone: 13-Year Long-Term Follow-up. J. Minim. Invasive Gynecol. 2019, 26, 1110–1116. [Google Scholar] [CrossRef] [PubMed]
- Soto, E.; Luu, T.H.; Liu, X.; Magrina, J.F.; Wasson, M.N.; Einarsson, J.I.; Cohen, S.L.; Falcone, T. Laparoscopy vs. Robotic Surgery for Endometriosis (LAROSE): A multicenter, randomized, controlled trial. Fertil. Steril. 2017, 107, 996–1002. [Google Scholar] [CrossRef] [PubMed]
- Nezhat, F.R.; Sirota, I. Perioperative Outcomes of Robotic Assisted Laparoscopic Surgery Versus Conventional Laparoscopy Surgery for Advanced-Stage Endometriosis. JSLS 2014, 18, e2014.00094. [Google Scholar] [CrossRef]
- Restaino, S.; Mereu, L.; Finelli, A.A.; Spina, M.R.; Marini, G.; Catena, U.; Turco, L.C.; Moroni, R.; Milani, M.; Cela, V.; et al. Robotic surgery vs laparoscopic surgery in patients with diagnosis of endometriosis: A systematic review and meta-analysis. J. Robot. Surg. 2020, 14, 687–694. [Google Scholar] [CrossRef]
- Magrina, J.F.; Espada, M.; Kho, R.M.; Cetta, R.; Chang, Y.H.; Magtibay, P.M. Surgical Excision of Advanced Endometriosis: Perioperative Outcomes and Impacting Factors. J. Minim. Invasive Gynecol. 2015, 22, 944–950. [Google Scholar] [CrossRef]
- Nezhat, C.R.; Stevens, A.; Balassiano, E.; Soliemannjad, R. Robotic-assisted laparoscopy vs conventional laparoscopy for the treatment of advanced stage endometriosis. J. Minim. Invasive Gynecol. 2015, 22, 40–44. [Google Scholar] [CrossRef]
- Hur, C.; Falcone, T. Robotic treatment of bowel endometriosis. Best Pract. Res. Clin. Obstet. Gynaecol. 2021, 71, 129–143. [Google Scholar] [CrossRef]
- Chen, S.H.; Li, Z.A.; Du, X.P. Robot-assisted versus conventional laparoscopic surgery in the treatment of advanced stage endometriosis: A meta-analysis. Clin. Exp. Obstet. Gynecol. 2016, 43, 422–426. [Google Scholar]
- Ercoli, A.; Bassi, E.; Ferrari, S.; Surico, D.; Fagotti, A.; Fanfani, F.; De Cicco, F.; Surico, N.; Scambia, G. Robotic-assisted conservative excision of retrocervical-rectal deep infiltrating endometriosis: A case series. J. Minim. Invasive Gynecol. 2017, 24, 863–868. [Google Scholar] [CrossRef] [PubMed]
- Hiltunen, J.; Eloranta, M.L.; Lindgren, A.; Keski-Nisula, L.; Anttila, M.; Sallinen, H. Robotic-assisted laparoscopy is a feasible method for resection of deep infiltrating endometriosis, especially in the rectosigmoid area. J. Int. Med. Res. 2021, 49, 3000605211032788. [Google Scholar] [CrossRef]
- Vural, M. Pelvic pain rehabilitation. Turk. J. Phys. Med. Rehabil. 2018, 64, 291–299. [Google Scholar] [CrossRef] [PubMed]
- Troyer, M.R. Differential diagnosis of endometriosis in a young adult woman with nonspecific low back pain. Phys. Ther. 2007, 87, 801–810. [Google Scholar] [CrossRef]
- Arya, P.; Shaw, R. Endometriosis: Current thinking. Curr. Obstet. Gynaecol. 2005, 15, 191–198. [Google Scholar] [CrossRef]
- Febbraio, M.A. Exercise and inflammation. J. Appl. Physiol. 2007, 103, 376–377. [Google Scholar] [CrossRef]
- Warren, M.P.; Perlroth, N.E. The effects of intense exercise on the female reproductive system. J. Endocrinol. 2001, 170, 3–11. [Google Scholar] [CrossRef] [PubMed]
- Koppan, A.; Hamori, J.; Vranics, I.; Garai, J.; Kriszbacher, I.; Bodis, J.; Rebek-Nagy, G.; Koppan, M. Pelvic pain in endometriosis: Painkillers or sport to alleviate symptoms? Acta Physiol. Hung. 2010, 97, 234–239. [Google Scholar] [CrossRef]
- Awad, E.; Ahmed, H.; Yousef, A.; Abbas, R. Efficacy of exercise on pelvic pain and posture associated with endometriosis: Within subject design. J. Phys. Sci. 2017, 29, 2112–2115. [Google Scholar] [CrossRef]
- Zhao, L.; Wu, H.; Zhou, X.; Wang, Q.; Zhu, W.; Chen, J. Effects of progressive muscular relaxation training on anxiety, depression and quality of life of endometriosis patients under gonadotrophin-releasing hormone agonist therapy. Eur. J. Obstet. Gynecol. Reprod. Biol. 2012, 162, 211–215. [Google Scholar] [CrossRef]
- Carpenter, S.E.; Tjaden, B.; Rock, J.A.; Kimball, A. The effect of regular exercise on women receiving danazol for treatment of endometriosis. Int. J. Gynaecol. Obstet. 1995, 49, 299–304. [Google Scholar] [CrossRef]
- Lund, I.; Lundeberg, T. Is acupuncture effective in the treatment of pain in endometriosis? J. Pain Res. 2016, 9, 157–165. [Google Scholar] [CrossRef] [PubMed]
- Matsuzaki, S.; Darcha, C. Epithelial to mesenchymal transition-like and mesench-ymal to epithelial transition-like processes might be involved in the pathogenesis of pelvic endometriosis. Hum. Reprod. 2012, 27, 712–721. [Google Scholar] [CrossRef]
- Sourial, S.; Tempest, N.; Hapangama, D.K. Theories on the pathogenesis of endometriosis. Int. J. Reprod. Med. 2014, 2014, 179515. [Google Scholar] [CrossRef]
- Wessels, J.M.; Kay, V.R.; Leyland, N.A.; Agarwal, S.K.; Foster, W.G. Assessing brain-derived neurotrophic factor as a novel clinical marker of endometriosis. Fertil. Steril. 2016, 105, 119–128.e5. [Google Scholar] [CrossRef] [PubMed]
- Rocha, A.L.; Vieira, E.L.; Ferreira, M.C.; Maia, L.M.; Teixeira, A.L.; Reis, F.M. Plasma brain-derived neurotrophic factor in women with pelvic pain: A potential biomarker for endometriosis? Biomark. Med. 2017, 11, 313–317. [Google Scholar] [CrossRef]
- Nisenblat, V.; Prentice, L.; Bossuyt, P.M.; Farquhar, C.; Hull, M.L.; Johnson, N. Combination of the non-invasive tests for the diagnosis of endometriosis. Cochrane Database Syst. Rev. 2016, 7, CD012281. [Google Scholar] [CrossRef]
- Ural, U.M.; Tekin, Y.B.; Cure, M.; Sahin, F.K. Serum YKL-40 levels as a novel marker of inflammation in patients with endometriosis. Clin. Exp. Obstet. Gynecol. 2015, 42, 495–497. [Google Scholar]
- Agarwal, A.; Gupta, S.; Sharma, R.K. Role of oxidative stress in female reproduction. Reprod. Biol. Endocrinol. 2005, 3, 28. [Google Scholar] [CrossRef]
- Christodoulakos, G.; Augoulea, A.; Lambrinoudaki, I.; Sioulas, V.; Creatsas, G. Pathogenesis of endometriosis: The role of defective ‘immunosurveillance’. Eur. J. Contracept. Reprod. Health Care 2007, 12, 194–202. [Google Scholar] [CrossRef] [PubMed]
- Augoulea, A.; Mastorakos, G.; Lambrinoudaki, I.; Christodoulakos, G.; Creatsas, G. The role of the oxidative-stress in the endometriosis-relatedinfertility. Gynecol. Endocrinol. 2009, 25, 75–81. [Google Scholar] [CrossRef]
- Polak, G.; Barczyński, B.; Wertel, I.; Kwaśniewski, W.; Bednarek, W.; Derewianka-Polak, M.; Frąszczak, K.; Olajossy, M.; Kotarski, J. Disrupted iron metabolism in peritoneal fluid may induce oxidative stress in the peritoneal cavity of women with endometriosis. Ann. Agric. Environ. Med. 2018, 25, 587–592. [Google Scholar] [CrossRef] [PubMed]
- Morgan, M.; Liu, Z. Crosstalk of reactive oxygen species and NF-κB signaling. Cell Res. 2011, 21, 103–115. [Google Scholar] [CrossRef]
- Hirsch, M.; Duffy, J.; Davis, C.J.; Nieves Plana, M.; Khan, K.S. International Collaboration to Harmonise Outcomes and Measures for Endometriosis. Diagnostic accuracy of cancer antigen 125 for endometriosis: A systematic review and meta-analysis. BJOG 2016, 123, 1761–1768. [Google Scholar] [CrossRef]
- May, K.E.; Conduit-Hulbert, S.A.; Villar, J.; Kirtley, S.; Kennedy, S.H.; Becker, C.M. Peripheral biomarkers of endometriosis: A systematic review. Hum. Reprod. Update 2010, 16, 651–674. [Google Scholar] [CrossRef]
- Nisenblat, V.; Sharkey, D.J.; Wang, Z.; Evans, S.F.; Healey, M.; Ohlsson Teague, E.M.C.; Print, C.G.; Robertson, S.A.; Hull, M.L. Plasma microRNAs display limited potential as diagnostic tools for endometriosis. J. Clin. Endocrinol. Metab. 2019, 104, 1999–2022. [Google Scholar] [CrossRef] [PubMed]
- Sahin, C.; Mamillapalli, R.; Yi, K.W.; Taylor, H.S. microRNA Let-7b: A Novel treatment for endometriosis. J. Cell Mol. Med. 2018, 22, 5346–5353. [Google Scholar] [CrossRef]
- Liu, Y.; Chen, J.; Zhu, X.; Tang, L.; Luo, X.; Shi, Y. Role of miR-449b-3p in endometriosis via effects on endometrial stromal cell proliferation and angiogenesis. Mol. Med. Rep. 2018, 18, 3359–3365. [Google Scholar] [CrossRef]
- Rekker, K.; Tasa, T.; Saare, M.; Samuel, K.; Kadastik, Ü.; Karro, H.; Götte, M.; Salumets, A.; Peters, M. Differentially-Expressed miRNAs in Ectopic Stromal Cells Contribute to Endometriosis Development: The Plausible Role of miR-139-5p and miR-375. Int. J. Mol. Sci. 2018, 19, 3789. [Google Scholar] [CrossRef] [PubMed]
- Laudanski, P.; Charkiewicz, R.; Tolwinska, A.; Szamatowicz, J.; Charkiewicz, A.; Niklinski, J. Profiling of Selected MicroRNAs in Proliferative Eutopic Endometrium of Women with Ovarian Endometriosis. Biomed. Res. Int. 2015, 2015, 760698. [Google Scholar] [CrossRef]
- Laudanski, P.; Charkiewicz, R.; Kuzmicki, M.; Szamatowicz, J.; Charkiewicz, A.; Niklinski, J. MicroRNAs expression profiling of eutopic proliferative endometrium in women with ovarian endometriosis. Reprod. Biol. Endocrinol. 2013, 11, 78. [Google Scholar] [CrossRef] [PubMed]
- Gu, C.L.; Zhang, Z.; Fan, W.S.; Li, L.A.; Ye, M.X.; Zhang, Q.; Zhang, N.N.; Li, Z.; Meng, Y.G. Identification of MicroRNAs as Potential Biomarkers in Ovarian Endometriosis. Reprod. Sci. 2020, 27, 1715–1723. [Google Scholar] [CrossRef]
- Zafari, N.; Tarafdari, A.M.; Izadi, P.; Noruzinia, M.; Yekaninejad, M.S.; Bahramy, A.; Mohebalian, A. A Panel of Plasma miRNAs 199b-3p, 224–225p and Let-7d-3p as Non-Invasive Diagnostic Biomarkers for Endometriosis. Reprod. Sci. 2021, 28, 991–999. [Google Scholar] [CrossRef]
- Farsimadan, M.; Ismail Haje, M.; Khudhur Mawlood, C.; Arabipour, I.; Emamvirdizadeh, A.; Takamoli, S.; Masumi, M.; Vaziri, H. MicroRNA variants in endometriosis and its severity. Br. J. Biomed. Sci. 2021, 12, 1–5. [Google Scholar]
- Raja, M.H.R.; Farooqui, N.; Zuberi, N.; Ashraf, M.; Azhar, A.; Baig, R.; Badar, B.; Rehman, R. Endometriosis, infertility and MicroRNA’s: A review. J. Gynecol. Obstet. Hum. Reprod. 2021, 50, 102157. [Google Scholar] [CrossRef]
- Monnaka, V.U.; Hernandes, C.; Heller, D.; Podgaec, S. Overview of miRNAs for the non-invasive diagnosis of endometriosis: Evidence, challenges and strategies. A systematic review. Einstein 2021, 19, eRW5704. [Google Scholar] [CrossRef]
- Coutinho, L.M.; Ferreira, M.C.; Rocha, A.L.L.; Carneiro, M.M.; Reis, F.M. New biomarkers in endometriosis. Adv. Clin. Chem. 2019, 89, 59–77. [Google Scholar]
- Bjorkman, S.; Taylor, H.S. microRNAs in endometriosis: Biological function and emerging biomarker candidates. Biol. Reprod. 2019, 100, 1135–1146. [Google Scholar] [CrossRef]
- Zhou, C.; Zhang, T.; Liu, F.; Zhou, J.; Ni, X.; Huo, R.; Shi, Z. The differential expression of mRNAs and long noncoding RNAs between ectopic and eutopic endometria provides new insights into adenomyosis. Mol. Biosyst. 2016, 12, 362–370. [Google Scholar] [CrossRef]
- Liu, S.; Xin, W.; Tang, X.; Qiu, J.; Zhang, Y.; Hua, K. LncRNA H19 Overexpression in Endometriosis and its Utility as a Novel Biomarker for Predicting Recurrence. Reprod. Sci. 2020, 27, 1687–1697. [Google Scholar] [CrossRef]
- Huan, Q.; Cheng, S.C.; Du, Z.H.; Ma, H.F.; Li, C. LncRNA AFAP1-AS1 regulates proliferation and apoptosis of endometriosis through activating STAT3/TGF-β/Smad signaling via miR-424-5p. J. Obstet. Gynaecol. Res. 2021, 47, 2394–2405. [Google Scholar] [CrossRef]
- Cui, L.; Chen, S.; Wang, D.; Yang, Q. LINC01116 promotes proliferation and migration of endometrial stromal cells by targeting FOXP1 via sponging miR-9-5p in endometriosis. J. Cell Mol. Med. 2021, 25, 2000–2012. [Google Scholar] [CrossRef] [PubMed]
- Chang, C.Y.; Tseng, C.C.; Lai, M.T.; Chiang, A.J.; Lo, L.C.; Chen, C.M.; Yen, M.J.; Sun, L.; Yang, L.; Hwang, T.; et al. Genetic impacts on thermostability of onco-lncRNA HOTAIR during the development and progression of endometriosis. PLoS ONE 2021, 16, e0248168. [Google Scholar] [CrossRef]
- Wang, X.; Zhang, J.; Liu, X.; Wei, B.; Zhan, L. Long noncoding RNAs in endometriosis: Biological functions, expressions, and mechanisms. J. Cell Physiol. 2021, 236, 6–14. [Google Scholar] [CrossRef] [PubMed]
- Hadfield, R.M.; Mardon, H.J.; Barlow, D.H.; Kennedy, S.H. Endometriosis in monozygotic twins. Fertil. Steril. 1997, 68, 941–942. [Google Scholar] [CrossRef]
- Montgomery, G.W.; Mortlock, S.; Giudice, L.C. Should genetics now be considered the pre-eminent etiologic factor in endometriosis? J. Minim. Invasive Gynecol. 2020, 27, 280–286. [Google Scholar] [CrossRef]
- Koninckx, P.R.; Ussia, A.; Adamyan, L.; Wattiez, A.; Gomel, V.; Martin, D.C. Pathogenesis of endometriosis: The genetic/epigenetic theory. Fertil. Steril. 2019, 111, 327–340. [Google Scholar] [CrossRef]
- Uno, S.; Zembutsu, H.; Hirasawa, A.; Takahashi, A.; Kubo, M.; Akahane, T.; Aoki, D.; Kamatani, N.; Hirata, K.; Nakamura, Y. A genome-wide association study identifies genetic variants in the CDKN2BAS locus associated with endometriosis in Japanese. Nat. Genet. 2010, 42, 707–710. [Google Scholar] [CrossRef]
- Adachi, S.; Tajima, A.; Quan, J.; Haino, K.; Yoshihara, K.; Masuzaki, H.; Katabuchi, H.; Ikuma, K.; Suginami, H.; Nishida, N.; et al. Meta-analysis of genome-wide association scans for genetic susceptibility to endometriosis in Japanese population. J. Hum. Genet. 2010, 55, 816–821. [Google Scholar] [CrossRef] [PubMed]
- Painter, J.N.; Anderson, C.A.; Nyholt, J.R.; Macgregor, S.; Lin, J.; Lee, S.H.; Lambert, A.; Zhao, Z.Z.; Roseman, F.; Guo, Q.; et al. Genome-wide association study identifies a locus at 7p15.2 associated with endometriosis. Nat. Genet. 2011, 43, 51–54. [Google Scholar] [CrossRef] [PubMed]
- Nyholt, D.R.; Low, S.K.; Anderson, C.A.; Painter, J.N.; Uno, S.; Morris, A.P.; MacGregor, S.; Gordon, S.D.; Henders, A.K.; Martin, N.G.; et al. Genome-wide association meta-analysis identifies new endometriosis risk loci. Nat. Genet. 2012, 44, 1355–1359. [Google Scholar] [CrossRef] [PubMed]
- Pagliardini, L.; Gentilini, D.; Vigano’, P.; Panina-Bordignon, P.; Busacca, M.; Candiani, M.; Di Blasio, A.M. An Italian association study and meta-analysis with previous GWAS confirm WNT4, CDKN2BAS and FN1 as the first identified susceptibility loci for endometriosis. J. Med. Genet. 2013, 50, 43–46. [Google Scholar] [CrossRef]
- Fung, J.N.; Holdsworth-Carson, S.J.; Sapkota, Y.; Zhao, Z.Z.; Jones, L.; Girling, J.E.; Paiva, P.; Healey, M.; Nyholt, D.R.; Rogers, P.A.; et al. Functional evaluation of genetic variants associated with endometriosis near GREB1. Hum. Reprod. 2015, 30, 1263–1275. [Google Scholar] [CrossRef]
- Sapkota, Y.; Fassbender, A.; Bowdler, L.; Fung, J.N.; Peterse, D.; Montgomery, G.W.; Nyholt, D.R.; D’Hooghe, T.M. Independent Replication and Meta-Analysis for Endometriosis Risk Loci. Twin Res. Hum. Genet. 2015, 18, 518–525. [Google Scholar] [CrossRef]
- Mafra, F.; Catto, M.; Bianco, B.; Barbosa, C.P.; Christofolini, D. Association of WNT4 polymorphisms with endometriosis in infertile patients. J. Assist. Reprod. Genet. 2015, 32, 1359–1364. [Google Scholar] [CrossRef]
- Albertsen, H.M.; Chettier, R.; Farrington, P.; Ward, K. Genome-wide association study link novel loci to endometriosis. PLoS ONE 2013, 8, e58257. [Google Scholar] [CrossRef]
- Sobalska-Kwapis, M.; Smolarz, B.; Słomka, M.; Szaflik, T.; Kępka, E.; Kulig, B.; Siewierska-Górska, A.; Polak, G.; Romanowicz, H.; Strapagiel, D.; et al. New variants near RHOJ and C2, HLA-DRA region and susceptibility to endometriosis in the Polish population-The genome-wide association study. Eur. J. Obstet. Gynecol. Reprod. Biol. 2017, 217, 106–112. [Google Scholar] [CrossRef]
- Kim, C.; Yang, H.; Fukushima, Y.; Saw, P.E.; Lee, J.; Park, J.S.; Park, I.; Jung, J.; Kataoka, H.; Lee, D.; et al. Vascular RhoJ is an effective and selective target for tumor angiogenesis and vascular disruption. Cancer Cell 2014, 25, 102–117. [Google Scholar] [CrossRef]
- Savaris, R.F.; Hamilton, A.E.; Lessey, B.A.; Giudice, L.C. Endometrial gene expression in early pregnancy: Lessons from human ectopic pregnancy. Reprod. Sci. 2008, 15, 797–816. [Google Scholar] [CrossRef][Green Version]
- Bylińska, A.; Wilczyńska, K.; Malejczyk, J.; Milewski, Ł.; Wagner, M.; Jasek, M.; Niepiekło-Miniewska, W.; Wiśniewski, A.; Płoski, R.; Barcz, E.; et al. The impact of HLA-G, LILRB1 and LILRB2 gene polymorphisms on susceptibility to and severity of endometriosis. Mol. Genet. Genom. 2018, 293, 601–613. [Google Scholar] [CrossRef]
- Osiński, M.; Mostowska, A.; Wirstlein, P.; Wender-Ożegowska, E.; Jagodziński, P.P.; Szczepańska, M. The assessment of GWAS—Identified polymorphisms associated with infertility risk in Polish women with endometriosis. Ginekol. Pol. 2018, 89, 304–310. [Google Scholar] [CrossRef]
- Christofolini, D.M.; Mafra, F.A.; Catto, M.C.; Bianco, B.; Barbosa, C.P. New candidate genes associated to endometriosis. Gynecol. Endocrinol. 2019, 35, 62–65. [Google Scholar] [CrossRef]
- Rahmioglu, N.; Montgomery, G.W.; Zondervan, K.T. Genetics of endometriosis. Womens Health 2015, 11, 577–586. [Google Scholar] [CrossRef]
- Cardoso, J.V.; Perini, J.A.; Machado, D.E.; Pinto, R.; Medeiros, R. Systematic review of genome-wide association studies on susceptibility to endometriosis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2020, 255, 74–82. [Google Scholar] [CrossRef] [PubMed]
- Mear, L.; Herr, M.; Fauconnier, A.; Pineau, C.; Vialard, F. Polymorphisms and endometriosis: A systematic review and meta-analyses. Hum. Reprod. Update 2020, 26, 73–102. [Google Scholar] [CrossRef] [PubMed]
- Bulun, S.E.; Monsavais, D.; Pavone, M.E.; Dyson, M.; Xue, Q.; Attar, E.; Tokunaga, H.; Su, E.J. Role of estrogen receptor-β in endometriosis. Semin. Reprod. Med. 2012, 30, 39–45. [Google Scholar] [CrossRef]
- Szaflik, T.; Smolarz, B.; Mroczkowska, B.; Kulig, B.; Soja, M.; Romanowicz, H.; Bryś, M.; Forma, E.; Szyłło, K. An Analysis of ESR2 and CYP19A1 Gene Expression Levels in Women with Endometriosis. In Vivo 2020, 34, 1765–1771. [Google Scholar] [CrossRef] [PubMed]
- Szaflik, T.; Smolarz, B.; Romanowicz, H.; Bryś, M.; Forma, E.; Szyłło, K. Polymorphisms in the 3′UTR Region of ESR2 and CYP19A1 Genes in Women with Endometriosis. Eur. J. Obstet. Gynecol. Reprod. Biol. 2020, 250, 241–245. [Google Scholar] [CrossRef]
- Smolarz, B.; Szaflik, T.; Romanowicz, H.; Szyłło, K. Polymorphisms in the 3′ UTR Region of ESR2 and CYP19A1 Genes and Its Influence on Allele-Specific Gene Expression in Endometriosis. Dis. Markers 2020, 2020, 7. [Google Scholar] [CrossRef]
- Smolarz, B.; Romanowicz, H. Association between single nucleotide polymorphism of the CYP19A1 and ESR2 genes and endometriosis. Arch. Gynecol. Obstet. 2021, 304, 439–445. [Google Scholar] [CrossRef] [PubMed]
- Zondervan, K.T.; Becker, C.M.; Missmer, S.A. Endometriosis. N. Engl. J. Med. 2020, 382, 1244–1256. [Google Scholar] [CrossRef] [PubMed]
- Redwine, D. Regarding “Should Genetics Now Be Considered the Pre-eminent Etiologic Factor in Endometriosis?”. J. Minim. Invasive Gynecol. 2020, 27, 1426–1427. [Google Scholar] [CrossRef]
- Panir, K.; Schjenken, J.E.; Robertson, S.A.; Hull, M.L. Non-coding RNAs in endometriosis: A narrative review. Hum. Reprod. Update 2018, 24, 497–515. [Google Scholar] [CrossRef]
| Name of the Investigator | Year | Theory |
|---|---|---|
| Recklinghausen | 1885 | from Wolff wires |
| Cullen | 1896 | from Müller cables |
| Iwanhofen | 1898 | metaplasia theory—the assumption of the theory is the existence of cells capable of differentiating in the endometrium, and being precursors of the epithelium of the pelvic peritoneum |
| Meyer | 1903 | metaplasia theory—the assumption of the theory is the existence of cells capable of differentiating in the endometrium, and being precursors of the mesodermal epithelium of the ovary |
| Pick | 1905 | metaplasia theory; regarding the sexual epithelium of the ovary |
| Sampson | 1927 | “retrograde menstruation” |
| Halban | 1924 | endometrial elements can enter the peritoneal cavity by the blood or lymphatic route |
| Navrital i Kramer | 1936 | vascular spread |
| Javert | 1949 | a combination of implantation theory, transport by the blood and lymphatic routes, as well as the theory of direct penetration of the endometrium through the uterine muscle |
| Mc Weigh | 1955 | from the cells of the radial wreath of the egg |
| Weed i wsp | 1980 | failure of the immune system derived from the Müller ducts |
| Malick | 1982 | congenital or acquired weakened fibrinolytic activity of the peritoneum |
| Immune Factor | Role in Endometriosis |
|---|---|
| TNF-α | Increasing vascular permeability and transformation of inflammatory factors in the peritoneal cavity, which exacerbate peritonitis [66]. |
| NF-κB | Controlling gene expression associated with immune response, cellular proliferation, and cytokine production [67]. |
| MCP-1 | Stimulation of monocytes to migrate from peripheral blood to the peritoneal cavity to turn into macrophages, leading to local inflammation [68]. |
| IL-1β | Induction of VEGF and COX-2 expression leading to the progression of endometriosis [69]. |
| IL-6 | In the tide to impair the function of NK cells (natural killer) by regulating the protein expression of tyrosine phosphatase (SHP-2) in endometriosis [70]. |
| IL-10 | In a mouse model with induced endometriosis, inhibition of IL-10 activity was found to be helpful in reducing lesions [71]. |
| IL-15 | In normal endometrial cells, ovarian steroid hormones control the production of IL-15. Endometriotic cells in patients with endometriosis show higher concentrations of this cytokine in endometrial patients [72]. |
| IL-16 | Higher concentrations of IL-16 in women with endometriosis are associated with the development of the disease by stimulating the secretion of IL-6, TNF-α and IL-1β. IL-16 polymorphisms are associated with women’s susceptibility to the development of endometriosis and its severity [73]. |
| IL-17A | In endometriosis, IL-17A is expressed in endometrial lesions, and therefore the inflammatory environment of the peritoneal cavity of patients with endometriosis may be associated with the production of IL-17A [74]. |
| IL-18 | IL-18 regulates the production of TNF-α and IL-8, acts as a potent angiogenic factor, and also regulates the intercellular expression of adhesion molecule 1 through NFκB and may increase MMP production. IL-18 is a major regulator of the immune response process in a wide range of cells that decreases in both eutopic and ectopic endometrium in endometriosis [75]. |
| IL-27 IL-33 | IL-10 + Th17 stimulate the proliferation and implantation of ectopic lesions and accelerate the progression of endometriosis, making IL-27 a key regulator in endometriotic lesions [76]. Member of the IL-1 family. IL-33 induces the synthesis of Th2-type cytokines through its orphan receptor ST2. Increased IL-33 expression has been correlated with fibrotic disorders such as skin scleroderma, liver and lung fibrosis, making IL-33 a key profibrotic mediator [77]. |
| IL-37 | Increased levels of IL-37 expression in eutopic and ectopic endometrium in women with stage III-IV ovarian endometriosis may be involved in inflammatory processes leading to endometriosis [78]. |
| According to the Classical Classification of Martius | According to Kistner’s Classification |
|---|---|
| - endometriosis genitalis interna (adenomyosis) is present in the uterus or the Fallopian tube - endometriosis genitalis externa (in the remaining parts of the reproductive organ) - endometriosis extragenitalis (endometriotic lesions are present outside the reproductive organs) | 1. Overlapping peritoneal endometriosis Ovaries serous membrane of the uterus uterine ligaments Fallopian tubes large intestine, thin intestine, appendix 2. Retroperitoneal endometriosis inguinal regio neck, vagina, vulva, perineum drainage pathways pleural and lungs skin, skeletal muscles, limbs |
| Types of Drugs | |
|---|---|
| 1. | non-steroidal anti-inflammatory drugs |
| 2. | hormonal drugs: progestogens hormonal contraceptives, danazol, analogues and gonadoliberin (GnRH)–gonadoliberin agonists and antagonists |
| 3. | selective progesterone receptor modulators |
| 4. | aromatase inhibitors |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Smolarz, B.; Szyłło, K.; Romanowicz, H. Endometriosis: Epidemiology, Classification, Pathogenesis, Treatment and Genetics (Review of Literature). Int. J. Mol. Sci. 2021, 22, 10554. https://doi.org/10.3390/ijms221910554
Smolarz B, Szyłło K, Romanowicz H. Endometriosis: Epidemiology, Classification, Pathogenesis, Treatment and Genetics (Review of Literature). International Journal of Molecular Sciences. 2021; 22(19):10554. https://doi.org/10.3390/ijms221910554
Chicago/Turabian StyleSmolarz, Beata, Krzysztof Szyłło, and Hanna Romanowicz. 2021. "Endometriosis: Epidemiology, Classification, Pathogenesis, Treatment and Genetics (Review of Literature)" International Journal of Molecular Sciences 22, no. 19: 10554. https://doi.org/10.3390/ijms221910554
APA StyleSmolarz, B., Szyłło, K., & Romanowicz, H. (2021). Endometriosis: Epidemiology, Classification, Pathogenesis, Treatment and Genetics (Review of Literature). International Journal of Molecular Sciences, 22(19), 10554. https://doi.org/10.3390/ijms221910554






