Potentiation of Low-Dose Doxorubicin Cytotoxicity by Affecting P-Glycoprotein through Caryophyllane Sesquiterpenes in HepG2 Cells: an in Vitro and in Silico Study
Abstract
1. Introduction
2. Results
2.1. Cytotoxicity of Doxorubicin and Caryophyllane Sesquiterpenes after Long-Term and Metronomic Exposures
2.2. Chemosensitizing Effects of Caryophyllane Sesquiterpenes in Combination with Doxorubicin under Long-Term and Metronomic Exposures
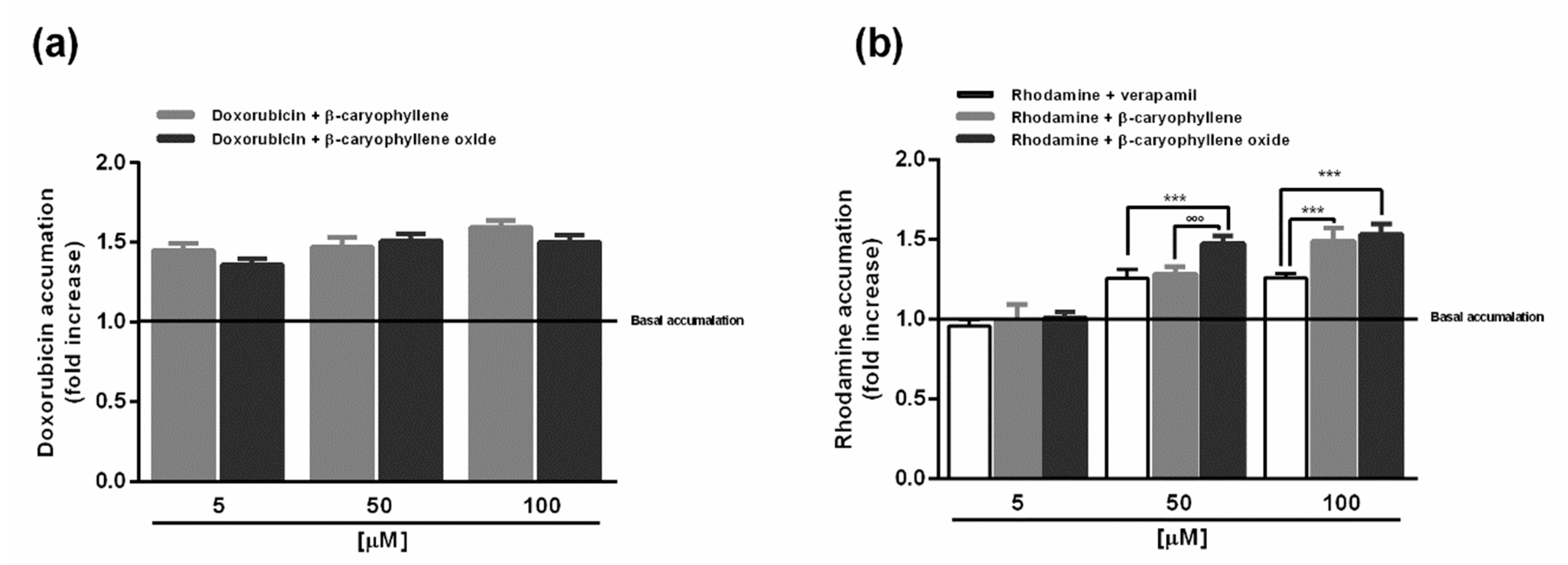
2.3. Caryophyllane Sesquiterpenes Affect Doxorubicin and Rhodamine Accumulation in HepG2 Cells
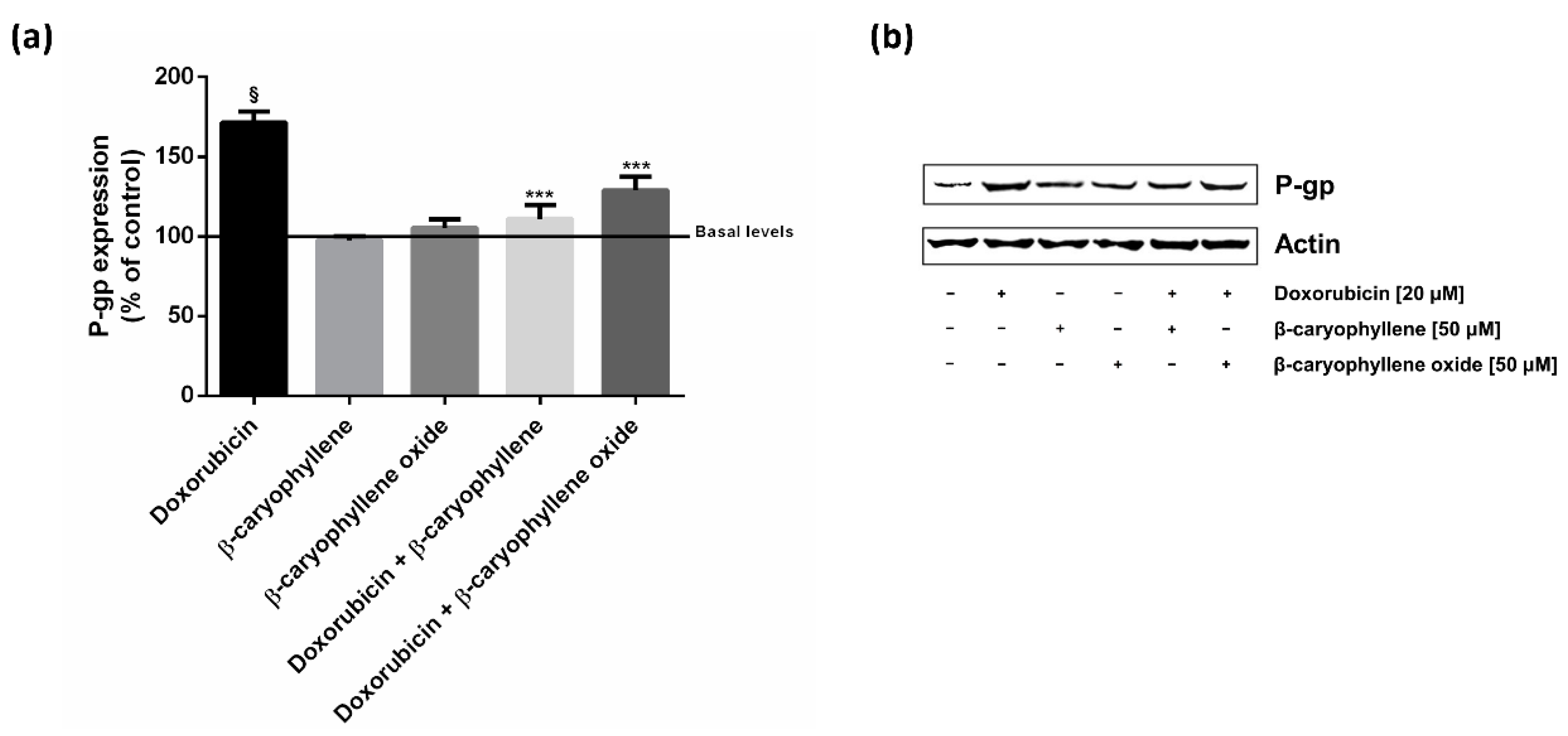
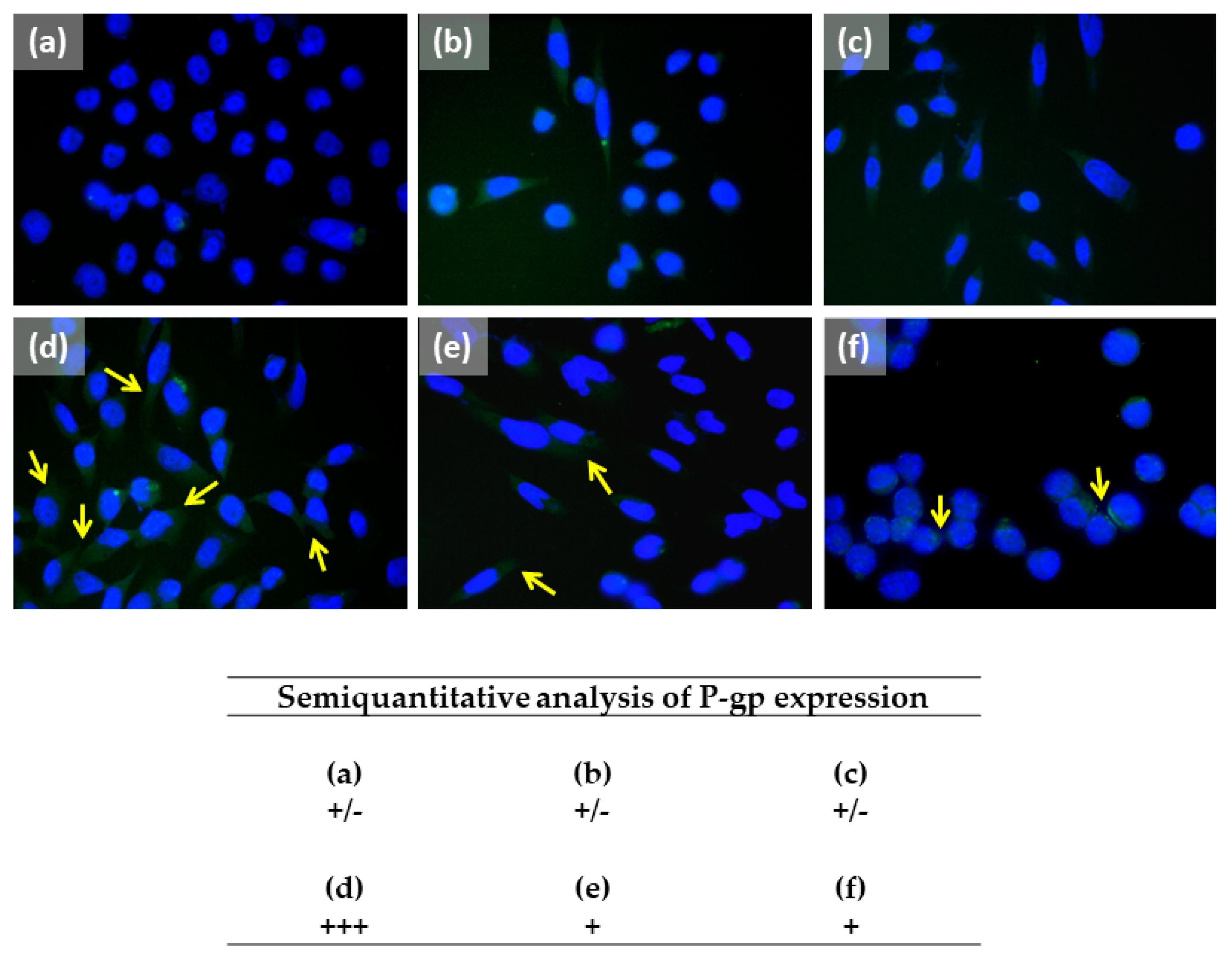
2.4. Caryophyllane Sesquiterpenes Affect the Doxorubicin-Mediated Increase of P-gp Expression in HepG2 Cells
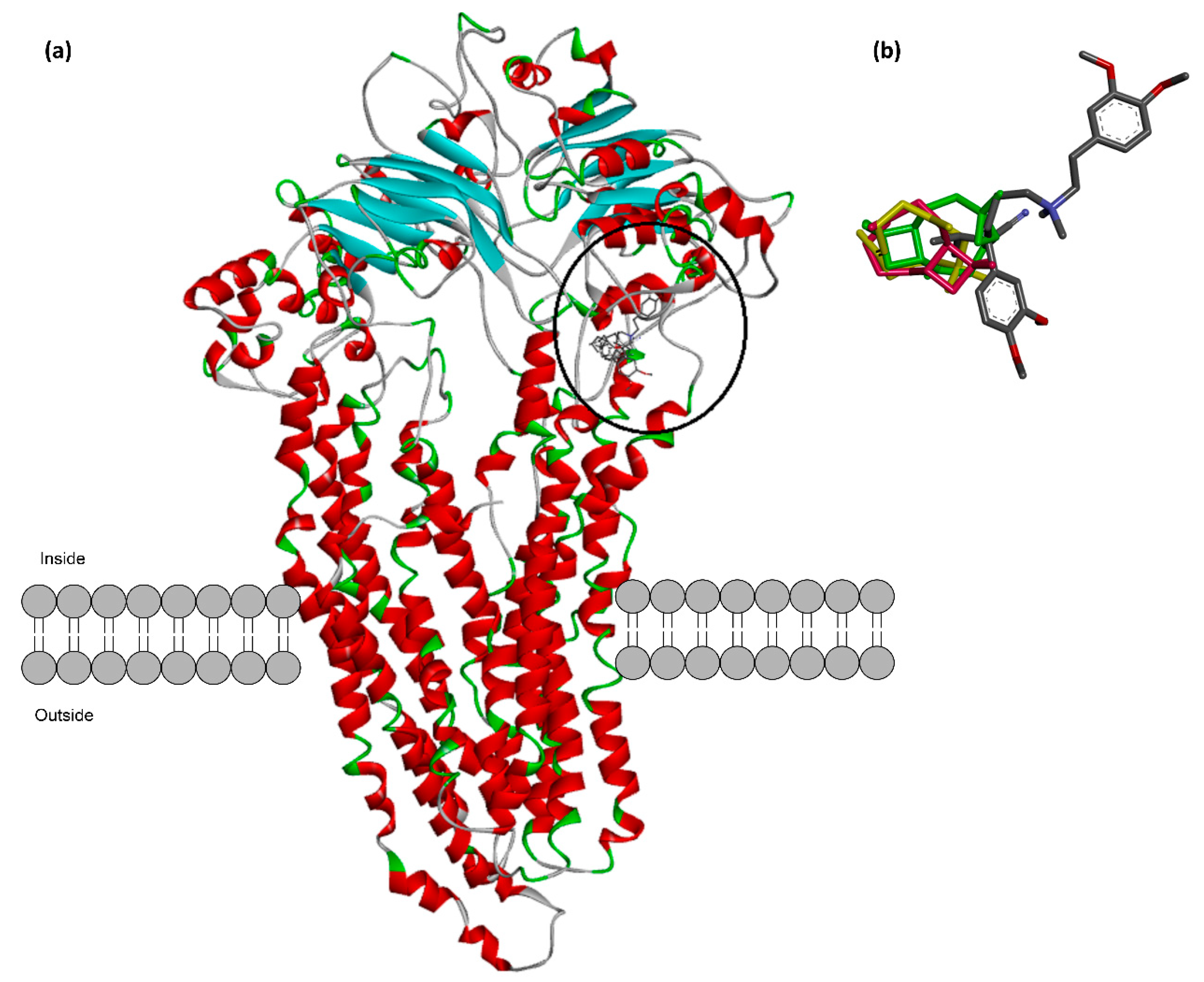
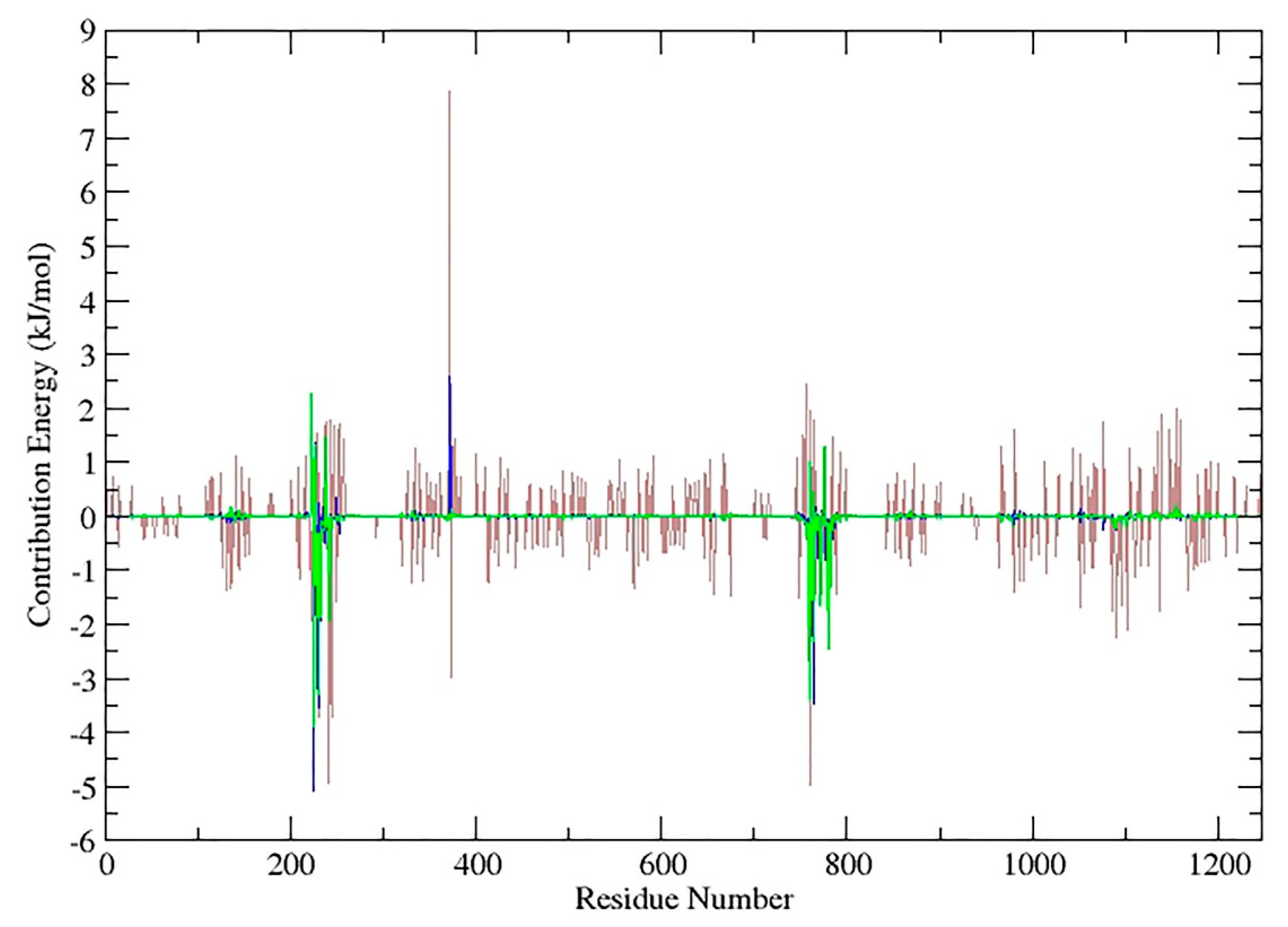
2.5. In Silico Prediction of the Possible Interaction between Caryophyllene Sesquiterpenes and P-Glycoprotein
3. Discussion
4. Materials and Methods
4.1. Chemical and Reagents
4.2. Cell Culture
4.3. Cytotoxicity Assay
4.4. Combination Assay
4.5. Scheduling of Single and Metronomic Treatment Protocols
4.6. Analysis of Sesquiterpene-Drug Interactions
4.7. Doxorubicin Accumulation
4.8. Rhodamine 123 Efflux Assay
4.9. Western Blotting Analysis
4.10. Immunofluorescence
4.11. In Silico Prediction of the P-Glycoprotein Active Site for Caryophyllane Sesquiterpenes
4.11.1. Docking and Active Site Prediction
4.11.2. Molecular Dynamic Simulation and Binding Free Energy Calculation
4.12. Statistical Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Hanušová, V.; Boušová, I.; Skálová, L. Possibilities to increase the effectiveness of doxorubicin in cancer cells killing. Drug Metab. Rev. 2011, 43, 540–557. [Google Scholar] [CrossRef] [PubMed]
- Le Grazie, M.; Biagini, M.R.; Tarocchi, M.; Polvani, S.; Galli, A. Chemotherapy for hepatocellular carcinoma: The present and the future. World J. Hepatol. 2017, 9, 907–920. [Google Scholar] [CrossRef] [PubMed]
- Marin, J.J.G.; Briz, O.; Herraez, E.; Lozano, E.; Asensio, M.; Di Giacomo, S.; Romero, M.R.; Osorio-Padilla, L.M.; Santos-Llamas, A.I.; Serrano, M.A.; et al. Molecular bases of the poor response of liver cancer to chemotherapy. Clin. Res. Hepatol. Gastroenterol. 2018, 42, 182–192. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.E.; Cho, H.J.; Kim, J.S.; Shim, C.K.; Chung, S.J.; Oak, M.H.; Yoon, I.S.; Kim, D.D. The limited intestinal absorption via paracellular pathway is responsible for the low oral bioavailability of doxorubicin. Xenobiotica 2013, 43, 579–591. [Google Scholar] [CrossRef]
- Capelôa, T.; Benyahia, Z.; Zampieri, L.X.; Blackman, M.C.N.M.; Sonveaux, P. Metabolic andnnon-metabolic pathways that control cancer resistance to anthracyclines. Semin. Cell Dev. Biol. 2019. [Google Scholar] [CrossRef]
- Cheng, X.; Gao, F.; Xiang, J.; Jiang, X.; Chen, J.; Zhang, J. Galactosylated alpha,beta-poly[(2-hydroxyethyl)-L-aspartamide]-bound doxorubicisn: Improved antitumor activity against hepatocellular carcinoma with reduced hepatotoxicity. Anti-Cancer Drugs 2011, 22, 136–147. [Google Scholar] [CrossRef]
- Browder, T.; Butterfield, C.E.; Kräling, B.M.; Shi, B.; Marshall, B.; O’Reilly, M.S.; Folkman, J. Antiangiogenic scheduling of chemotherapy improves efficacy against experimental drug-resistant cancer. Cancer Res. 2000, 60, 1878–1886. [Google Scholar]
- Pucci, C.; Martinelli, C.; Ciofani, G. Innovative approaches for cancer treatment: Current perspectives and new challenges. Ecancermedicalscience 2019, 13, 961. [Google Scholar] [CrossRef]
- Simsek, C.; Esin, E.; Yalcin, S. Metronomic Chemotherapy: A Systematic Review of the Literature and Clinical Experience. J. Oncol. 2019, 2019, 5483791. [Google Scholar] [CrossRef]
- Torimura, T.; Iwamoto, H.; Nakamura, T.; Koga, H.; Ueno, T.; Kerbel, R.S.; Sata, M. Metronomic chemotherapy: Possible clinical application in advanced hepatocellular carcinoma. Transl. Oncol. 2013, 6, 511–519. [Google Scholar] [CrossRef]
- Fisher, B.; Brown, A.M.; Dimitrov, N.V.; Poisson, R.; Redmond, C.; Margolese, R.G.; Bowman, D.; Wolmark, N.; Wickerham, D.L.; Kardinal, C.G. Two months of doxorubicin–cyclophosphamide with and without interval reinduction therapy compared with 6 months of cyclophosphamide, methotrexate, and fluorouracil in positive-node breast cancer patients with tamoxifen nonresponsive tumors: Results from the National Surgical Adjuvant Breast and Bowel Project B-15. J. Clin. Oncol. 1990, 8, 1483–1496. [Google Scholar]
- Sun, W.; Sanderson, P.E.; Zheng, W. Drug combination therapy increases successful drug repositioning. Drug Discov. Today 2016, 21, 1189–1195. [Google Scholar] [CrossRef]
- Tagliamonte, M.; Petrizzo, A.; Tornesello, M.L.; Ciliberto, G.; Buonaguro, F.M.; Buonaguro, L. Combinatorial immunotherapy strategies for hepatocellular carcinoma. Curr. Opin. Immunol. 2016, 39, 103–113. [Google Scholar] [CrossRef] [PubMed]
- Rejhová, A.; Opattová, A.; Čumová, A.; Slíva, D.; Vodička, P. Natural compounds and combination therapy in colorectal cancer treatment. Eur. J. Med. Chem. 2018, 144, 582–594. [Google Scholar] [CrossRef] [PubMed]
- Di Giacomo, S.; Di Sotto, A.; El–Readi, M.Z.; Mazzanti, G.; Wink, M. Chemosensitizing Properties of β-Caryophyllene and β-Caryophyllene Oxide in Combination with Doxorubicin in Human Cancer Cells. Anticancer Res. 2017, 37, 1191–1196. [Google Scholar]
- Di Giacomo, S.; Briz, O.; Monte, M.J.; Sanchez–Vicente, L.; Abete, L.; Lozano, E.; Mazzanti, G.; Di Sotto, A.; Marin, J.J.G. Chemosensitization of hepatocellular carcinoma cells to sorafenib by β-caryophyllene oxide–induced inhibition of ABC export pumps. Arch. Toxicol. 2019, 93, 623–634. [Google Scholar] [CrossRef] [PubMed]
- Legault, J.; Pichette, A. Potentiating effect of beta-caryophyllene on anticancer activity of alpha-humulene, isocaryophyllene and paclitaxel. J. Pharm. Pharmacol. 2007, 59, 1643–1647. [Google Scholar] [CrossRef] [PubMed]
- Kim, C.; Cho, S.K.; Kim, K.D.; Nam, D.; Chung, W.S.; Jang, H.J.; Lee, S.G.; Shim, B.S.; Sethi, G.; Ahn, K.S. β-Caryophyllene oxide potentiates TNFα-induced apoptosis and inhibits invasion through down-modulation of NF-κB-regulated gene products. Apoptosis 2014, 19, 708–718. [Google Scholar] [CrossRef]
- Hanušová, V.; Caltová, K.; Svobodová, H.; Ambrož, M.; Skarka, A.; Murínová, N.; Králová, V.; Tomšík, P.; Skálová, L. The effects of β-caryophyllene oxide and trans-nerolidol on the efficacy of doxorubicin in breast cancer cells and breast tumor-bearing mice. Biomed. Pharmacother. 2017, 95, 828–836. [Google Scholar] [CrossRef]
- Ambrož, M.; Šmatová, M.; Šadibolová, M.; Pospíšilová, E.; Hadravská, P.; Kašparová, M.; Skarková, V.H.; Králová, V.; Skálová, L. Sesquiterpenes α-humulene and β-caryophyllene oxide enhance the efficacy of 5-fluorouracil and oxaliplatin in colon cancer cells. Acta Pharm. 2019, 69, 121–128. [Google Scholar] [CrossRef]
- Louisa, M.; Suyatna, F.D.; Wanandi, S.I.; Asih, P.B.; Syafruddin, D. Differential expression of several drug transporter genes in HepG2 and Huh-7 cell lines. Adv. Biomed. Res. 2016, 5, 104. [Google Scholar] [CrossRef] [PubMed]
- Dubbelboer, I.R.; Pavlovic, N.; Heindryckx, F.; Sjögren, E.; Lennernäs, H. Liver Cancer Cell Lines Treated with Doxorubicin under Normoxia and Hypoxia: Cell Viability and Oncologic Protein Profile. Cancers 2019, 11, 1024. [Google Scholar] [CrossRef] [PubMed]
- Xu, Q.; Guo, J.; Chen, W. Gambogenic acid reverses P-glycoprotein mediated multidrug resistance in HepG2/Adr cells and its underlying mechanism. Biochem. Biophys. Res. Commun. 2019, 508, 882–888. [Google Scholar] [CrossRef] [PubMed]
- Sun, L.; Chen, W.; Qu, L.; Wu, J.; Si, J. Icaritin reverses multidrug resistance of HepG2/ADR human hepatoma cells via downregulation of MDR1 and P-glycoprotein expression. Mol. Med. Rep. 2013, 8, 1883–1887. [Google Scholar] [CrossRef]
- Yahya, S.M.; Hamed, A.R.; Emara, M.; Soltan, M.M.; Abd-Ellatef, G.E.; Abdelnasser, S.M. Differential effects of c-myc and ABCB1 silencing on reversing drug resistance in HepG2/Dox cells. Tumour Biol. 2016, 37, 5925–5932. [Google Scholar] [CrossRef]
- Hosseini Balef, S.S.; Piramoon, M.; Hosseinimehr, S.J.; Irannejad, H. In vitro and in silico evaluation of P-glycoprotein inhibition through (99m) Tc-methoxyisobutylisonitrile uptake. Chem. Biol. Drug Des. 2019, 93, 283–289. [Google Scholar] [CrossRef]
- Di Giacomo, S.; Di Sotto, A.; El-Readi, M.Z.; Mazzanti, G.; Wink, M. α-Hexylcinnamaldehyde Synergistically Increases Doxorubicin Cytotoxicity Towards Human Cancer Cell Lines. Anticancer Res. 2016, 36, 3347–3351. [Google Scholar]
- Pétriz, J.; García-López, J. Flow cytometric analysis of P-glycoprotein function using rhodamine 123. Leukemia 1997, 11, 1124–1130. [Google Scholar] [CrossRef]
- Stewart, D.J. Mechanisms of resistance to cisplatin and carboplatin. Crit. Rev. Oncol. Hematol. 2007, 63, 12–31. [Google Scholar] [CrossRef]
- Chau, Q.; Stewart, D.J. Cisplatin efflux, binding and intracellular pH in the HTB56 human lung adenocarcinoma cell line and the E-8/0.7 cisplatin-resistant variant. Cancer Chemother. Pharmacol. 1999, 44, 193–202. [Google Scholar] [CrossRef][Green Version]
- Wu, N.; Meng, F.; Invernizzi, P.; Bernuzzi, F.; Venter, J.; Standeford, H.; Onori, P.; Marzioni, M.; Alvaro, D.; Franchitto, A.; et al. The secretin/secretin receptor axis modulates liver fibrosis through changes in transforming growth factor-β1 biliary secretion in mice. Hepatology 2016, 64, 865–879. [Google Scholar] [CrossRef] [PubMed]
- Evandri, M.G.; Battinelli, L.; Daniele, C.; Mastrangelo, S.; Bolle, P.; Mazzanti, G. The antimutagenic activity of Lavandula angustifolia (lavender) essential oil in the bacterial reverse mutation assay. Food Chem. Toxicol. 2005, 43, 1381–1387. [Google Scholar] [CrossRef] [PubMed]
- Magina, M.D.; Dalmarco, E.M.; Wisniewski, A., Jr.; Simionatto, E.L.; Dalmarco, J.B.; Pizzolatti, M.G.; Brighente, I.M. Chemical composition and antibacterial activity of essential oils of Eugenia species. J. Nat. Med. 2009, 63, 345–350. [Google Scholar] [CrossRef] [PubMed]
- Zengin, G.; Menghini, L.; Di Sotto, A.; Mancinelli, R.; Sisto, F.; Carradori, S.; Cesa, S.; Fraschetti, C.; Filippi, A.; Angiolella, L.; et al. Chromatographic Analyses, In Vitro Biological Activities, and Cytotoxicity of Cannabis sativa L. Essential Oil: A Multidisciplinary Study. Molecules 2018, 23, 3266. [Google Scholar] [CrossRef] [PubMed]
- Zardi–Bergaoui, A.; Znati, M.; Harzallah-Skhiri, F.; Jannet, H.B. Caryophyllene Sesquiterpenes from Pulicaria vulgaris Gaertn: Isolation, Structure Determination, Bioactivity and Structure-Activity Relationship. Chem. Biodivers. 2019, 16, e1800483. [Google Scholar] [CrossRef]
- Dosoky, N.S.; Satyal, P.; Barata, L.M.; da Silva, J.K.R.; Setzer, W.N. Volatiles of Black Pepper Fruits (Piper nigrum L.). Molecules 2019, 24, 4244. [Google Scholar] [CrossRef]
- Li, Y.; Cui, C.; Liu, X.; Che, Y. Cytosporinols A–C, new caryophyllene sesquiterpenoids from Cytospora sp. Nat. Prod. Bioprospecting 2012, 2, 70–75. [Google Scholar] [CrossRef]
- Wu, J.; Wang, G.; Du, X.; Song, N.; Zou, Z.; Chen, J.; Zhang, Y.; Li, T.; Wang, X.; Kuang, H. A caryophyllane-type sesquiterpene, caryophyllenol A from Valeriana amurensis. Fitoterapia 2014, 96, 18–24. [Google Scholar] [CrossRef]
- Ahmed, A.F.; Su, J.H.; Shiue, R.T.; Pan, X.J.; Dai, C.F.; Kuo, Y.H.; Sheu, J.H. New beta-caryophyllene-derived terpenoids from the soft coral Sinularia nanolobata. J. Nat. Prod. 2004, 67, 592–597. [Google Scholar] [CrossRef]
- Chung, H.M.; Wang, W.H.; Hwang, T.L.; Wu, Y.C.; Sung, P.J. Natural Caryophyllane Sesquiterpenoids from Rumphella antipathies. Nat. Prod. Commun. 2015, 10, 835–838. [Google Scholar] [CrossRef]
- Wiebach, V.; Surup, F.; Kuhnert, E.; Stadler, M. Rickicaryophyllane A, a Caryophyllane from the Ascomyceteous Fungus Hypoxylon rickii and a 10-Norbotryane Congener. Nat. Prod. Commun. 2016, 11, 909–912. [Google Scholar] [CrossRef] [PubMed]
- Atta-ur-Rahman; Ahmad, V.U. Caryophyllane. In 13C-NMR of Natural Products; Springer: Boston, MA, USA, 1992; pp. 583–584. [Google Scholar]
- Di Sotto, A.; Maffei, F.; Hrelia, P.; Castelli, F.; Sarpietro, M.G.; Mazzanti, G. Genotoxicity assessment of β–caryophyllene oxide. Regul. Toxicol. Pharmacol. 2013, 66, 264–268. [Google Scholar] [CrossRef]
- EFSA Panel on Additives and Products or Substances used in Animal Feed (FEEDAP). Safety and efficacy of eight compounds belonging to chemical group 31 (aliphatic and aromatic hydrocarbons) when used as flavourings for all animal species and categories. EFSA J. 2016, 14, 4339. [Google Scholar] [CrossRef]
- Bastaki, M.; Api, A.M.; Aubanel, M.; Bauter, M.; Cachet, T.; Demyttenaere, J.C.R.; Diop, M.M.; Harman, C.L.; Hayashi, S.M.; Krammer, G.; et al. Dietary administration of β-caryophyllene and its epoxide to Sprague-Dawley rats for 90 days. Food Chem. Toxicol. 2019, 11, 110876. [Google Scholar] [CrossRef] [PubMed]
- Chávez–Hurtado, P.; González-Castañeda, R.E.; Beas-Zarate, C.; Flores-Soto, M.E.; Viveros-Paredes, J.M. β-Caryophyllene Reduces DNA Oxidation and the Overexpression of Glial Fibrillary Acidic Protein in the Prefrontal Cortex and Hippocampus of d-Galactose-Induced Aged BALB/c Mice. J. Med. Food 2019. [Google Scholar] [CrossRef] [PubMed]
- Fidyt, K.; Fiedorowicz, A.; Strządała, L.; Szumny, A. β-caryophyllene and β-caryophyllene oxide-natural compounds of anticancer and analgesic properties. Cancer Med. 2016, 5, 3007–3017. [Google Scholar] [CrossRef] [PubMed]
- Santos, N.A.; Martins, N.M.; Sisti, F.M.; Fernandes, L.S.; Ferreira, R.S.; de Freitas, O.; Santos, A.C. The cannabinoid beta-caryophyllene (BCP) induces neuritogenesis in PC12 cells by a cannabinoid-receptor-independent mechanism. Chem. Biol. Interact. 2017, 261, 86–95. [Google Scholar] [CrossRef]
- Di Giacomo, S.; Abete, L.; Cocchiola, R.; Mazzanti, G.; Eufemi, M.; Di Sotto, A. Caryophyllane sesquiterpenes inhibit DNA–damage by tobacco smoke in bacterial and mammalian cells. Food Chem. Toxicol. 2018, 111, 393–404. [Google Scholar] [CrossRef]
- Di Giacomo, S.; Mazzanti, G.; Di Sotto, A. Mutagenicity of cigarette butt waste in the bacterial reverse mutation assay: The protective effects of β-caryophyllene and β-caryophyllene oxide. Environ. Toxicol. 2016, 31, 1319–1328. [Google Scholar] [CrossRef]
- Di Sotto, A.; Mazzanti, G.; Carbone, F.; Hrelia, P.; Maffei, F. Inhibition by beta-caryophyllene of ethyl methanesulfonate-induced clastogenicity in cultured human lymphocytes. Mutat. Res. Genet. Toxicol. Environ. Mutagenesis 2010, 699, 23–28. [Google Scholar] [CrossRef]
- Di Sotto, A.; Evandri, M.G.; Mazzanti, G. Antimutagenic and mutagenic activities of some terpenes in the bacterial reverse mutation assay. Mutat. Res. Genet. Toxicol. Environ. Mutagenesis 2008, 653, 130–133. [Google Scholar] [CrossRef] [PubMed]
- Jun, N.J.; Mosaddik, A.; Moon, J.Y.; Jang, K.C.; Lee, D.S.; Ahn, K.S.; Cho, S.K. Cytotoxic activity of β-caryophyllene oxide isolated from Jeju Guava (Psidium cattleianum Sabine) leaf. Rec. Nat. Prod. 2011, 5, 242–246. [Google Scholar]
- Jung, J.I.; Kim, E.J.; Kwon, G.T.; Jung, Y.J.; Park, T.; Kim, Y.; Yu, R.; Choi, M.S.; Chun, H.S.; Kwon, S.H.; et al. β-Caryophyllene potently inhibits solid tumor growth and lymph node metastasis of B16F10 melanoma cells in high-fat diet-induced obese C57BL/6N mice. Carcinogenesis 2015, 36, 1028–1039. [Google Scholar] [CrossRef] [PubMed]
- Di Sotto, A.; Paolicelli, P.; Nardoni, M.; Abete, L.; Garzoli, S.; Di Giacomo, S.; Mazzanti, G.; Casadei, M.A.; Petralito, S. SPC Liposomes as Possible Delivery Systems for Improving Bioavailability of the Natural Sesquiterpene β-Caryophyllene:Lamellarity and Drug–Loading as Key Features for a Rational Drug Delivery Design. Pharmaceutics 2018, 10, 274. [Google Scholar] [CrossRef]
- Ramachandhiran, D.; Sankaranarayanan, C.; Murali, R.; Babukumar, S.; Vinothkumar, V. β-Caryophyllene promotes oxidative stress and apoptosis in KB cells through activation of mitochondrial–mediated pathway—An in-vitro and in-silico study. Arch. Physiol. Biochem. 2019, 4, 1–15. [Google Scholar] [CrossRef]
- Bains, O.S.; Szeitz, A.; Lubieniecka, J.M.; Cragg, G.E.; Grigliatti, T.A.; Riggs, K.W.; Reid, R.E. A correlation between cytotoxicity and reductase-mediated metabolism in cell lines treated with doxorubicin and daunorubicin. J. Pharmacol. Exp. Ther. 2013, 347, 375–387. [Google Scholar] [CrossRef]
- To, H. Construction of combined chemotherapy of anti–tumor drugs based on chronotherapy. Yakugaku Zasshi J. Pharm. Soc. Jpn. 2006, 126, 415–422. [Google Scholar] [CrossRef][Green Version]
- Munzone, E.; Di Pietro, A.; Goldhirsch, A.; Minchella, I.; Verri, E.; Cossu Rocca, M.; Marenghi, C.; Curigliano, G.; Radice, D.; Adamoli, L.; et al. Metronomic administration of pegylated liposomal-doxorubicin in extensively pre-treated metastatic breast cancer patients: A mono-institutional case-series report. Breast 2010, 19, 33–37. [Google Scholar] [CrossRef]
- Dellapasqua, S.; Mazza, M.; Rosa, D.; Ghisini, R.; Scarano, E.; Torrisi, R.; Maisonneuve, P.; Viale, G.; Cassano, E.; Veronesi, P.; et al. Pegylated liposomal doxorubicin in combination with low–dose metronomic cyclophosphamide as preoperative treatment for patients with locally advanced breast cancer. Breast 2011, 20, 319–323. [Google Scholar] [CrossRef]
- Manso, L.; Valdiviezo, N.; Sepúlveda, J.; Ciruelos, E.; Mendiola, C.; Ghanem, I.; Vega, E.; Manneh, R.; Dorta, M.; Cortés–Funes, H. Safety and efficacy of metronomic non–pegylated liposomal encapsulated doxorubicin in heavily pretreated advanced breast cancer patients. Clin. Transl. Oncol. 2013, 15, 467–471. [Google Scholar] [CrossRef]
- Riganti, C.; Gazzano, E.; Gulino, G.R.; Volante, M.; Ghigo, D.; Kopecka, J. Two repeated low doses of doxorubicin are more effective than a single high dose against tumors overexpressing P-glycoprotein. Cancer Lett. 2015, 360, 219–226. [Google Scholar] [CrossRef] [PubMed]
- Asakawa, Y.; Taira, Z.; Takemoto, T.; Ishida, T.; Kido, M.; Ichikawa, Y. X-ray crystal structure analysis of 14-hydroxycaryophyllene oxide, a new metabolite of (−)-caryophyllene, in rabbits. J. Pharm. Sci. 1981, 70, 710–711. [Google Scholar] [CrossRef] [PubMed]
- Asakawa, Y.; Ishida, T.; Toyota, M.; Takemoto, T. Terpenoid biotransformation in mammals. IV Biotransformation of (+)–longifolene, (−)–caryophyllene, (−)–caryophyllene oxide, (−)–cyclocolorenone, (+)–nootkatone, (−)–elemol, (−)–abietic acid and (+)–dehydroabietic acid in rabbits. Xenobiotica 1986, 16, 753–767. [Google Scholar] [CrossRef]
- Dewanjee, S.; Dua, T.K.; Bhattacharjee, N.; Das, A.; Gangopadhyay, M.; Khanra, R.; Joardar, S.; Riaz, M.; Feo, V.; Zia-Ul-Haq, M. Natural Products as Alternative Choices for P-Glycoprotein (P-gp) Inhibition. Molecules 2017, 22, 871. [Google Scholar] [CrossRef] [PubMed]
- Zhou, S.F. Structure, function and regulation of P-glycoprotein and its clinical relevance in drug disposition. Xenobiotica 2008, 38, 802–832. [Google Scholar] [CrossRef] [PubMed]
- Hung, L.W.; Wang, I.X.; Nikaido, K.; Liu, P.Q.; Ames, G.F.; Kim, S.H. Crystal structure of the ATP-binding subunit of an ABC transporter. Nature 1998, 396, 703–707. [Google Scholar] [CrossRef]
- Sharom, F.J. Complex Interplay between the P–Glycoprotein Multidrug Efflux Pump and the Membrane: Its Role in Modulating Protein Function. Front. Oncol. 2014, 4, 41. [Google Scholar] [CrossRef]
- Higgins, C.F.; Gottesman, M.M. Is the multidrug transporter a flippase? Trends Biochem. Sci. 1992, 17, 18–21. [Google Scholar] [CrossRef]
- Akhtar, N.; Ahad, A.; Khar, R.K.; Jaggi, M.; Aqil, M.; Iqbal, Z.; Ahmad, F.J.; Talegaonkar, S. The emerging role of P–glycoprotein inhibitors in drug delivery: A patent review. Expert Opin. Ther. Pat. 2011, 21, 561–576. [Google Scholar] [CrossRef]
- Sulová, Z.; Seres, M.; Barancík, M.; Gibalová, L.; Uhrík, B.; Poleková, L.; Breier, A. Does any relationship exist between P-glycoprotein-mediated multidrug resistance and intracellular calcium homeostasis. Gen. Physiol. Biophys. 2009, 28, F89–F95. [Google Scholar]
- Varma, M.V.; Ashokraj, Y.; Dey, C.S.; Panchagnula, R. P-glycoprotein inhibitors and their screening: A perspective from bioavailability enhancement. Pharmacol. Res. 2003, 48, 347–359. [Google Scholar] [CrossRef]
- Eid, S.Y.; El-Readi, M.Z.; Eldin, E.E.; Fatani, S.H.; Wink, M. Influence of combinations of digitonin with selected phenolics, terpenoids, and alkaloids on the expression and activity of P-glycoprotein in leukaemia and colon cancer cells. Phytomedicine 2013, 21, 47–61. [Google Scholar] [CrossRef] [PubMed]
- Wink, M. Evolutionary advantage and molecular modes of action of multi-component mixtures used in phytomedicine. Curr. Drug Metab. 2008, 9, 996–1009. [Google Scholar] [CrossRef] [PubMed]
- Sarpietro, M.G.; Di Sotto, A.; Accolla, M.L.; Castelli, F. Differential Scanning Calorimetry Study on the Interaction of β-Caryophyllene and β-Caryophyllene Oxide with Phospholipid Bilayers. Thermochim. Acta 2015, 600, 28–34. [Google Scholar] [CrossRef]
- Eckford, P.D.; Sharom, F.J. Interaction of the P-glycoprotein multidrug efflux pump with cholesterol: Effects on ATPase activity, drug binding and transport. Biochemistry 2008, 47, 13686–13698. [Google Scholar] [CrossRef]
- Kimura, Y.; Kioka, N.; Kato, H.; Matsuo, M.; Ueda, K. Modulation of drug–stimulated ATPaseactivityofhumanMDR1/P–glycoprotein by cholesterol. Biochem. J. 2007, 401, 597–605. [Google Scholar] [CrossRef]
- Kantharidis, P.; El-Osta, S.; Silva, M.; Lee, G.; Hu, X.F.; Zalcberg, J. Regulation ofMDR1 gene expression: Emerging concepts. Drug Resist. Updates 2000, 3, 99–108. [Google Scholar] [CrossRef]
- Yang, J.M.; Sullivan, G.F.; Hiat, W.N. Regulation of the function of Pglycoprotein by epidermal growth factor through phospholipase C. Biochem. Pharmacol. 1997, 53, 1597–1604. [Google Scholar] [CrossRef]
- Zhang, X.; Xiao, W.; Wang, L.; Tian, Z.; Zhang, J. Deactivation of signal transducer and activator of transcription 3 reverses chemotherapeutics resistance of leukemia cells via down-regulating P-gp. PLoS ONE 2011, 6, e20965. [Google Scholar] [CrossRef]
- Zhang, X.; Liu, P.; Zhang, B.; Wang, A.; Yang, M. Role of STAT3 decoy oligodeoxynucleotides on cell invasion and chemosensitivity in human epithelial ovarian cancer cells. Cancer Genet. Cytogenet. 2010, 197, 46–53. [Google Scholar] [CrossRef]
- Kim, C.; Cho, S.K.; Kapoor, S.; Kumar, A.; Vali, S.; Abbasi, T.; Kim, S.H.; Sethi, G.; Ahn, K.S. β-Caryophyllene oxide inhibits constitutive and inducible STAT3 signaling pathway through induction of the SHP-1 protein tyrosine phosphatase. Mol. Carcinog. 2014, 53, 793–806. [Google Scholar] [CrossRef] [PubMed]
- Di Sotto, A.; Di Giacomo, S.; Abete, L.; Božović, M.; Parisi, O.A.; Barile, F.; Vitalone, A.; Izzo, A.A.; Ragno, R.; Mazzanti, G. Genotoxicity assessment of piperitenone oxide: An in vitro and in silico evaluation. Food Chem. Toxicol. 2017, 106, 506–513. [Google Scholar] [CrossRef] [PubMed]
- Biological Evaluation of Medical Devices Part 5: Tests for Invitro Cytotoxicity. In Geneva (Switzerland): International Organization for Standardization/ANSI, 2nd ed.; ISO 10993-5:2009; ISO: Geneva, Switzerland, 2009.
- Cocchiola, R.; Rubini, E.; Altieri, F.; Chichiarelli, S.; Paglia, G.; Romaniello, D.; Carissimi, S.; Giorgi, A.; Giamogante, F.; Macone, A.; et al. STAT3 Post–Translational Modifications Drive Cellular Signaling Pathways in Prostate Cancer Cells. Int. J. Mol. Sci. 2019, 20, 1815. [Google Scholar] [CrossRef] [PubMed]
- Mancinelli, R.; Olivero, F.; Carpino, G.; Overi, D.; Rosa, L.; Lepanto, M.S.; Cutone, A.; Franchitto, A.; Alpini, G.; Onori, P.; et al. Role of lactoferrin and its receptors on biliary epithelium. Biometals 2018, 31, 369–379. [Google Scholar] [CrossRef] [PubMed]
- Kumari, R.; Kumar, R.; Open Source Drug Discovery, C.; Lynn, A. g_mmpbsa-a GROMACS tool for high throughput MM–PBSA calculations. J. Chem. Inf. Model. 2014, 54, 1951–1962. [Google Scholar] [CrossRef]
- Hosseini Balef, S.S.; Chippindale, A.M.; Irannejad, H. A crystallographic and theoretical study of an (E)-2-Hydroxyiminoethanone derivative: Prediction of cyclooxygenase inhibition selectivity of stilbenoids by MM-PBSA and the role of atomic charge. J. Biomol. Struct. Dyn. 2019, 37, 1555–1566. [Google Scholar] [CrossRef]
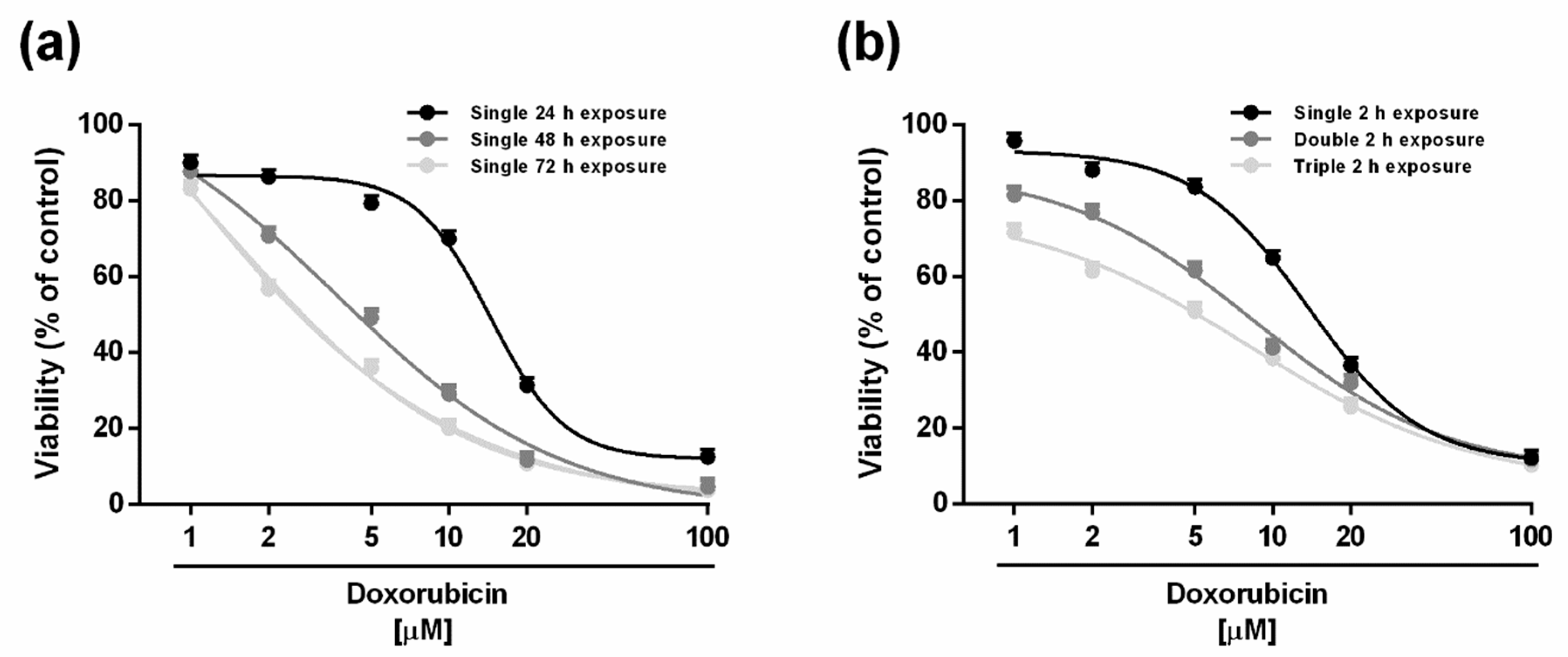
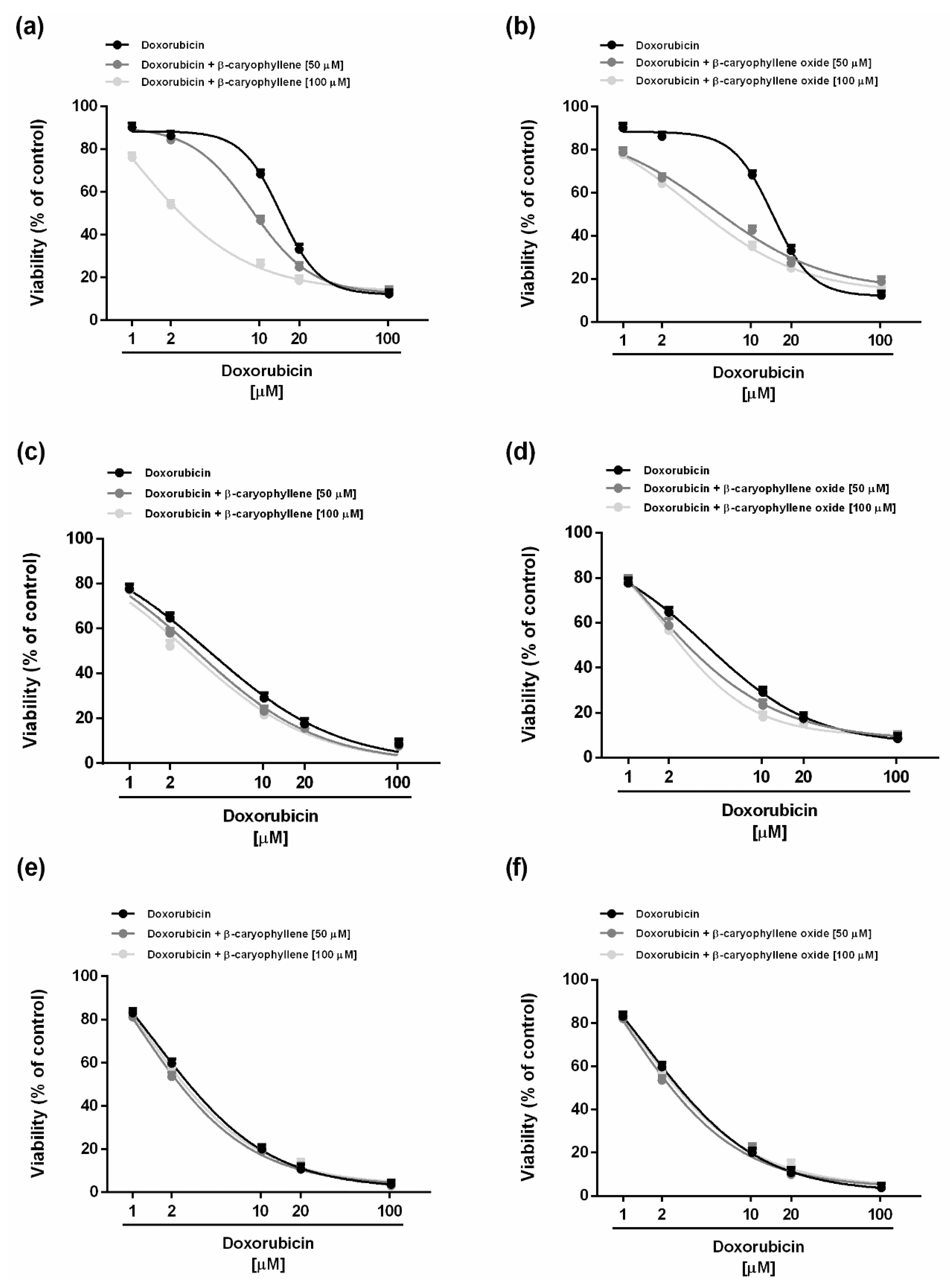
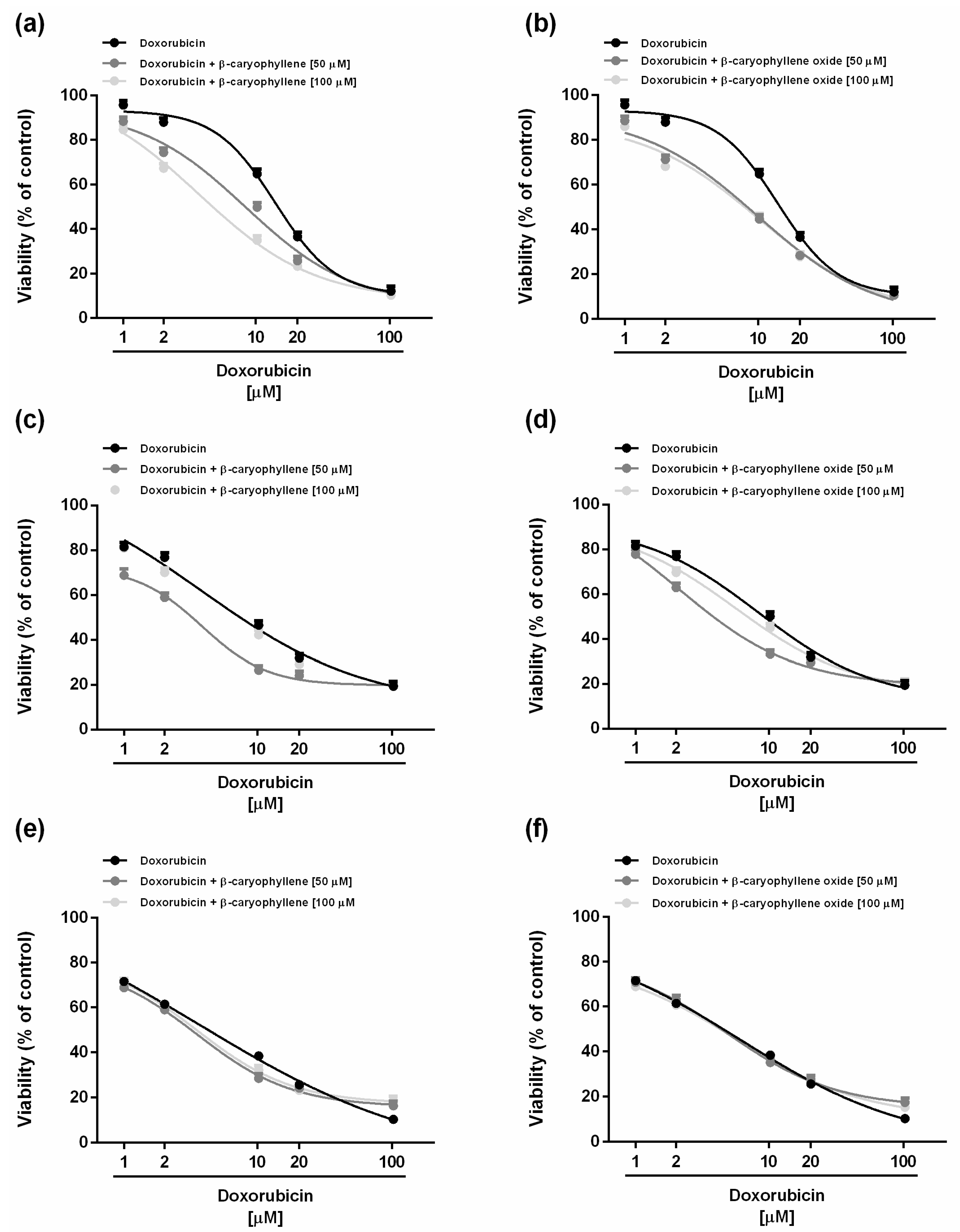
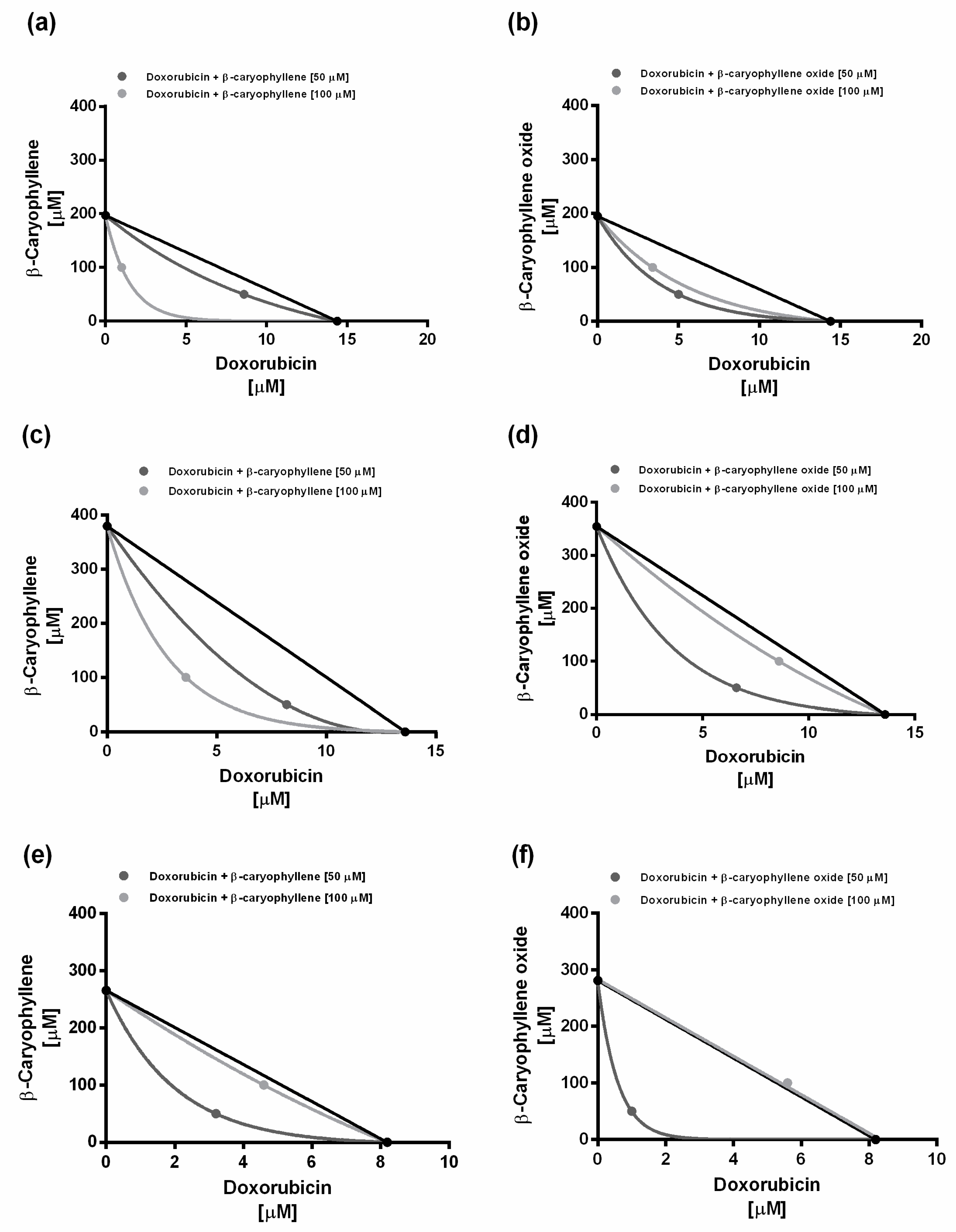

| Time Exposure | IC50 [µM] (CL) | ||
|---|---|---|---|
| Doxorubicin | β-Caryophyllene | β-Caryophyllene Oxide | |
| 24 h | 14.4 (12.8–16.2) | 197.0 (127.0–314.5) | 195.0 (172.5–219.5) |
| 48 h | 3.6 (2.6–5.2) §** | 121.0 (94.0–159.5) § | 162.0 (146.0–180.0) |
| 72 h | 1.6 (1.4–1.8) §** | 113.0 (88.5–144.0) § | 152.5 (136.5–170.0) |
| 2 h | 13.6 (2.6–20.2) | 379.5 (171.5–460.5) | 354.5 (190.5–441.0) |
| 2 h double | 11.6 (6.4–20.4) §* | 265.5 (110.5–327.0) | 281.0 (157.5–360.5) |
| 2 h triple | 5.8 (2.8–11.6) §** | 251.0 (71.5–372.0) | 256.5 (123.5–334.0) |
| Time Exposure | IC50 [µM] (Confidential Limits) RR a | ||||
|---|---|---|---|---|---|
| Doxorubicin | Doxorubicin + β-Caryophyllene [50 µM] | Doxorubicin + β-Caryophyllene [100 µM] | Doxorubicin + β-Caryophyllene Oxide [50 µM] | Doxorubicin + β-Caryophyllene Oxide [100 µM] | |
| 24 h | 14.4 (12.8–16.2) | 8.6 (7.6–13.8) ** 1.7 | 1 (0.4–1.8) *** 14.4 | 5.0 (4.2–5.8) *** 2.9 | 3.4 (2.2–4.6) *** 4.2 |
| 48 h | 3.6 (2.6–5.2) | 3.2 (2.0–5.2) 1.4 | 2.8 (1.2–5.2) 1.7 | 3.2 (1.6–5.2) 1.6 | 2.8 (1.2–4.8) 1.8 |
| 72 h | 1.6 (1.4–1.8) | 1.0 (0.8–1.4) 1.6 | 1.2 (0.6–3.4) 1.3 | 1.0 (0.8–1.6) 1.6 | 1.2 (0.6–2.6) 1.3 |
| 2 h | 13.6 (2.6–20.2) | 8.2 (3.2–21.4) ** 1.7 | 3.6 (1.8–7.2) *** 3.8 | 6.6 (2.4–18.0) ** 2.1 | 8.6 (5.0–14.0) ** 1.6 |
| 2 h double | 11.6 (6.4–20.4) | 3.2 (1.4–7.0) ** 2.6 | 4.6 (2.2–9.6) ** 1.8 | 2.2 (0.2–8.4) *** 3.7 | 5.6 (2.6–12.2) ** 1.5 |
| 2 h triple | 5.8 (2.8–11.6) | 3.2 (1.8–5.4) * 1.8 | 3.4 (2.0–6.6) * 1.7 | 4.6 (3.0–6.2) 1.3 | 5.4 (3.6–9.0) 1.1 |
| Compound | Van Der Waals Energy | Electrostatic Energy | Polar Solvation Energy | SASA Energy | Mean Binding Energy |
|---|---|---|---|---|---|
| α-Caryophyllene | −133.59 | 23.59 | 49.38 | −12.40 | −73.01 |
| β-Caryophyllene | −108.27 | −0.22 | 32.02 | −12.00 | −88.46 |
| β-Caryophyllene oxide | −106.92 | −2.60 | 39.94 | −12.98 | −82.57 |
| Verapamil | −212.66 | −11.34 | 104.62 | −23.58 | −142.97 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Di Sotto, A.; Irannejad, H.; Eufemi, M.; Mancinelli, R.; Abete, L.; Mammola, C.L.; Altieri, F.; Mazzanti, G.; Di Giacomo, S. Potentiation of Low-Dose Doxorubicin Cytotoxicity by Affecting P-Glycoprotein through Caryophyllane Sesquiterpenes in HepG2 Cells: an in Vitro and in Silico Study. Int. J. Mol. Sci. 2020, 21, 633. https://doi.org/10.3390/ijms21020633
Di Sotto A, Irannejad H, Eufemi M, Mancinelli R, Abete L, Mammola CL, Altieri F, Mazzanti G, Di Giacomo S. Potentiation of Low-Dose Doxorubicin Cytotoxicity by Affecting P-Glycoprotein through Caryophyllane Sesquiterpenes in HepG2 Cells: an in Vitro and in Silico Study. International Journal of Molecular Sciences. 2020; 21(2):633. https://doi.org/10.3390/ijms21020633
Chicago/Turabian StyleDi Sotto, Antonella, Hamid Irannejad, Margherita Eufemi, Romina Mancinelli, Lorena Abete, Caterina Loredana Mammola, Fabio Altieri, Gabriela Mazzanti, and Silvia Di Giacomo. 2020. "Potentiation of Low-Dose Doxorubicin Cytotoxicity by Affecting P-Glycoprotein through Caryophyllane Sesquiterpenes in HepG2 Cells: an in Vitro and in Silico Study" International Journal of Molecular Sciences 21, no. 2: 633. https://doi.org/10.3390/ijms21020633
APA StyleDi Sotto, A., Irannejad, H., Eufemi, M., Mancinelli, R., Abete, L., Mammola, C. L., Altieri, F., Mazzanti, G., & Di Giacomo, S. (2020). Potentiation of Low-Dose Doxorubicin Cytotoxicity by Affecting P-Glycoprotein through Caryophyllane Sesquiterpenes in HepG2 Cells: an in Vitro and in Silico Study. International Journal of Molecular Sciences, 21(2), 633. https://doi.org/10.3390/ijms21020633









