Abstract
Traditional remedies have been used for thousand years for the prevention and treatment of infectious diseases, particularly in developing countries. Of growing interest, the plant Artemisia annua, known for its malarial properties, has been studied for its numerous biological activities including metabolic, anti-tumor, anti-microbial and immunomodulatory properties. Artemisia annua is very rich in secondary metabolites such as monoterpenes, sesquiterpenes and phenolic compounds, of which the biological properties have been extensively studied. The purpose of this review is to gather and describe the data concerning the main chemical components produced by Artemisia annua and to describe the state of the art about the biological activities reported for this plant and its compounds beyond malaria.
1. Introduction
The family Asteraceae comprises a wide number of genera, of which the genus Artemisia is one of the largest and most widely distributed worldwide [1]. The genus Artemisia L. is heterogeneous and consists of over 500 species widely geographically distributed in all continents except Antarctica. The genus acclimatizes to any environment, from sea level to high altitudes [2]. However, most of Artemisia species grow preferentially in the Northern Hemisphere and at a lower level in the Southern Hemisphere [3,4]. Species of this genus can be perennial, biennial or annual grasses, shrubs or bushes that are generally aromatic, with erect or ascending stems. The leaves of these plants are alternate, often divided, rarely whole and with smooth edges. The origin of the scientific name of the genus Artemisia stems from two major interpretations. The first proposition addresses the name “Artemisia” from the Greek goddess “Artemis” (Diana for the Romans), Zeus’s daughter and Apollo’s sister, who was considered the protector of the wild animals and goddess of the hunt. The second interpretation assigns the origin of the name to the King of Caria’s (Mausolus) sister and wife Artemisia, who was crowned Queen after her husband’s death. The genus Artemisia is commonly known as “wormwood”. Wormwood, though, strictly speaking, refers to Artemisia absinthium L., which is one of the most common and well-known species of the genus [5]. The type species of the genus Artemisia is the Artemisia vulgaris [6]. Apart from Artemisia annua L., other very well-known species of the genus include Artemisia absinthium, Artemisia abrotanum and Artemisia afra. These species were used to treat fever and malaria, respectively, in China, Europe and Africa [7]. Artemisia verlotiorum Lamotte was introduced to, and is still present in, the Mascarene Islands.
Artemisia annua, (Figure 1) commonly named as “annual absinthe” is an annual herbaceous herb, hence its name “annua”. The plant is grown in Asia, India, Central and Eastern Europe, in the temperate regions of America, Africa, Australia and in tropical regions [3,7]. It is widely used as a dietary spice, herbal tea and medicinal plant in the mild climates of Asia, such as China and Korea [8].

Figure 1.
Artemisia annua [9].
The literature describes a confusion over the ancient Chinese names of the species Artemisia annua L. and Artemisia apiacea hance, the latter being native to China, indistinctly referred as “qing hao”. The polymath Shen Gua (1031–1095) of the Song dynasty described two different varieties of qing hao, one with blue–green leaves, and another with yellowish–green leaves in autumn. Based partly on this description, the physician and natural historian Li Shizhen (1518–1593) differentiated between qing hao (blue-green herb) and huang hua hao (yellow blossom herb) in his encyclopedic Classified Materia Medica (Ben cao gang mu) in 1596 [10]. Currently, Artemisia apiacea hance is identified as qing hao, and Artemisia annua as huang hua hao [7]. Unlike Artemisia apiacea hance, Artemisia annua has been introduced to many other countries in Europe, North America, and the tropics. Seed varieties have been adapted by breeding for lower latitudes, and cultivation has been successfully achieved in many tropical countries, for example in the Congo, India, and Brazil. In contrast. Artemisia apiacea hance is less common and is rarely grown outside China [5].
Artemisia annua has been used in traditional medicine for many years in Asia and Africa for the treatment of malaria and fever, in the form of tea or pressed juice [11,12]. The current pharmacopoeia of the People’s Republic of China officially lists the dried herb of Artemisia annua as a remedy for fever and malaria, at a daily dose of 4.5–9 g of dried herb prepared as an infusion [13]. This is the herbal preparation that has been used for clinical trials.
Artemisia annua is also described to have anti-hyperlipidemic, anti-plasmodial, anti-convulsant, anti-inflammatory, anti-microbial, anti-cholesterolemic and antiviral properties [14,15,16]. Artemisia annua would also have important pharmacological activities such as anti-inflammatory, antitumor and anti-obesity activities that contribute to the therapeutic effects of the plant [17,18,19].
Several bioactive metabolites have been identified in Artemisia annua. The most extensively studied is artemisinin, a lactone sesquiterpene endoperoxide [20]. Due to its antimalarial activity, artemisinin is pivotal in current antimalarial drug strategies [21,22,23]. In addition to this active compound, Artemisia annua has also an interesting nutritional profile with the presence of amino acids, vitamins and minerals and essential elements for health [24]. Since its discovery, Artemisia annua has been the subject of extensive research on its chemical composition. More than 600 secondary metabolites have been identified throughout the plant [25], including several sesquiterpenoids, triterpenoids, monoterpenoids, steroids, flavonoids, coumarins, alkaloids and benzenoids [26,27,28].
Thanks to this richness, Artemisia annua has a large number of other biological properties such as hepatoprotective, antifungal, antitumor, antioxidant, anti-inflammatory and anti-asthmatic activities [8,17,18,27,29,30,31,32,33,34,35].
All these works ascertain the potential of Artemisia annua as a candidate for the food, medical, pharmaceutical, cosmetic and nutraceutical industries.
The purpose of this review is to provide a comprehensive synthesis of the various identified chemical compounds of Artemisia annua and to describe the state of the art of the biological activities described of this plant and its compounds beyond malaria.
2. Chemical Compounds from Artemisia annua and Their Biological Activities
Despite enormous geographic diversity, there are almost no morphological differences between the plants of Artemisia annua. However, clear differences are observed in the chemical compositions and health benefits of Artemisia annua plants according to their geographical location [36,37,38].
The chemical composition and biological properties of the aqueous or alcoholic extracts of Artemisia annua can vary considerably depending on its geographical origin, the plant material used and the way it is treated, unlike those of essential oil, which vary only slightly [39].
2.1. Monoterpenes
Monoterpenes are a class of terpenes that consist of two isoprene units, with a molecular formula: C10H16. Monoterpenes may be linear (acyclic) or contain rings. Modified terpenes, such as those containing oxygen functionality or missing a methyl group, are called monoterpenoids. Monoterpenes are secondary metabolites of plants. These molecules, with a very important chemical diversity, allow the plant to defend itself against biotic and abiotic stress factors and act as chemical signals through which the plant communicates with its environment (plants and other organisms) [40].
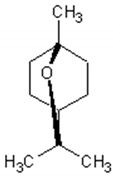
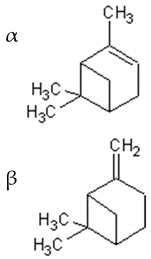
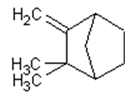
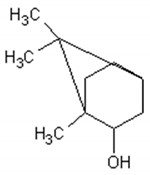
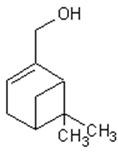
Monoterpenes are the main components of the essential oil of Artemisia annua and give the plant its strong and aromatic fragrance [41]. The main components of the essential oil are 1,8-cineole, α-and-β-pinene, camphene, borneol, camphor, carvone, limonene, α-terpinene and myrtenol [1,39,41,42].
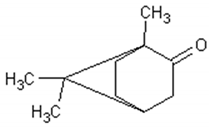
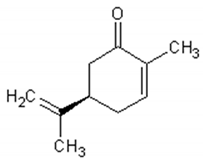
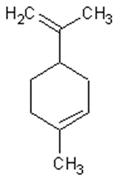
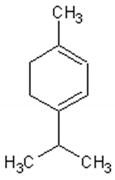
Table 1 describes the structure and biological activities of major monoterpenes of Artemisia annua essential oil.

Table 1.
Structure and biological activities of major monoterpenes of Artemisia annua essential oil.
2.2. Sesquiterpenes
Sesquiterpenes are a class of terpenes that consist of three isoprene units, with the molecular formula C15H24. Like monoterpenes, sesquiterpenes may be acyclic or contain rings, including many unique combinations. Biochemical modifications such as oxidation or rearrangement produce the related sesquiterpenoids. Sesquiterpenes have the known role of defense agent (biocide) against organisms outside the plant.
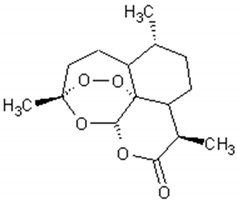
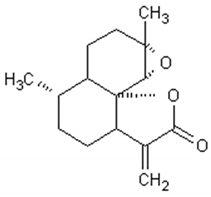
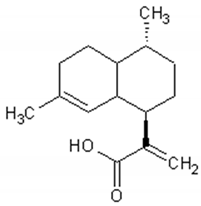
More than thirty sesquiterpenes are present in the Artemisia annua plant, mainly located in the aerial parts. The main compounds are artemisinin, arteannuin B and artemisinic acid [83,84,85,86,87]. Table 2 presents the structure and biological activities of major sesquiterpenes of Artemisia annua.

Table 2.
Structure and biological activities of major sesquiterpenes of Artemisia annua.
The therapeutic value of artemisinin is limited due to its low solubility in both oil and water. Researchers have synthesized a family of artemisinin derivatives including dihydroartemisinin (DHA, active metabolite), artesunate (ART, polar derivative), artemether (lipid-based derivative), arteether (lipid-based derivatives), SM905 (1-(12β-dihydroartemisinoxy)-2-hydroxy-3-tert-butylaminopropane maleate, new water-soluble derivative), artemiside (a 10-alkylamino sulfide derivative, lipophilic with limited water-solubility), artemisone (new 10-alkylamino sulfone derivative with enhanced water-solubility and reduced toxicity) and SM934 (β-aminoarteether maleate, new water-soluble derivative) [91]. Artemisinin and its derivatives can be used in the treatment of various diseases, such as cancer, autoimmune diseases, diabetes, viral infections, parasitosis and atherosclerosis [99]. The antimalarial efficacy of artemisinin is significantly improved when combined with other compounds from Artemisia annua such as terpenes, flavonoids, phenolic acids and polysaccharides [100].
3. Phenolic Compounds
Phenolic compounds are organic molecules that are widely distributed throughout plants from roots to fruits. These molecules have no direct function in the basic activities of the plant organism, such as growth or reproduction. They are secondary metabolites produced by plants to protect themselves from ultraviolet attacks, but also from animals, often acting as repellents due to their bitterness. Phenolic compounds are molecules with at least one aromatic ring (benzene) bearing one alcohol group, the basic structure called phenol. They are widely present in the plant kingdom in the form of simple (one aromatic ring) or more complex structures (aromatic fused rings), generally of high molecular weight.
Several classes of phenolic compounds are found in Artemisa annua aqueous and alcoholic extracts [39,83,101,102,103,104]:
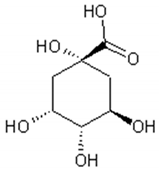
Cyclitol: Quinic acid;
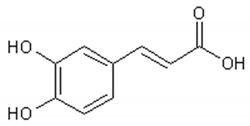
Phenolic acid: Caffeic acid;
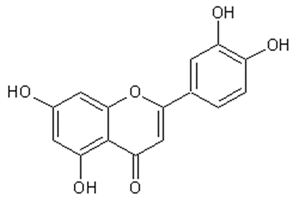
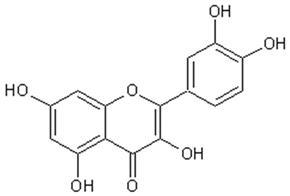
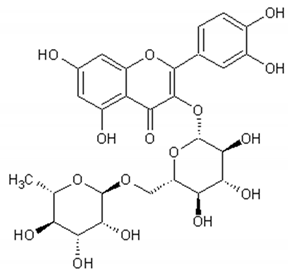
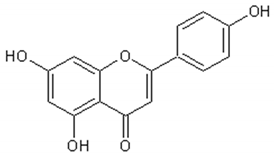
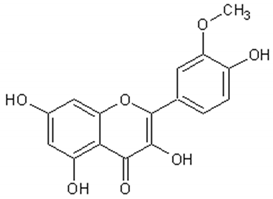
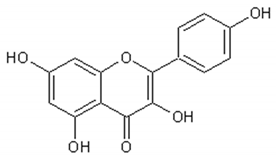
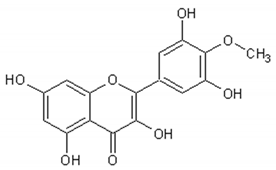
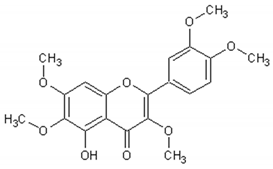
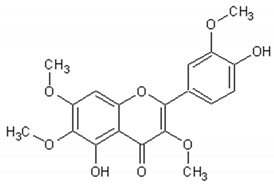
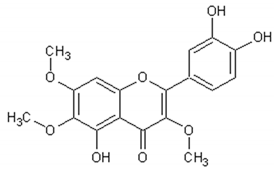
Flavonoids: Luteolin, Quercetin, Rutin, Apigenin, Isorhamnetin, Kaempferol, Mearnsetin, Artemetin, Casticin, Chrysosplenetin, Chrysosplenol D, Cirsilineol, Eupatorine.
The Artemisia annua antioxidant capacity mentioned in the literature is associated with the high content of flavonoids and the diversity of compound types [24,101].
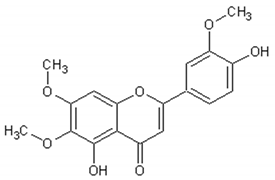
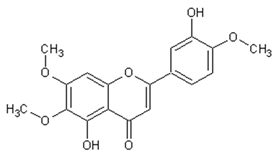
Table 3 presents the chemical structures and biological activities of major phenolic compounds of Artemisia annua extracts.

Table 3.
Structure and chemical activities of major phenolic compounds present in Artemisia annua.
Artemetin, casticin, chrysosplenetin, chrysosplenol D, cirsilineol and eupatorin are flavonoids from Artemisia annua that show some synergic anti-malarial effects with them [7]. Other phenolic compounds increase the antitumor and antimalarial activities of artemisinin [101].
4. Coumarins
Coumarins are natural substances derived from benzo-α-pyrone. They have one or more phenolic functions. Coumarins are widely distributed in the plant kingdom. They are formed in the leaves and accumulate especially in the roots and bark, as well as in old or damaged tissues. Coumarins protect the plant from herbivores and pathogenic microorganisms. They are mainly located on the surface and in the organs most exposed to predation (young leaves, fruit and seeds) in order to “save metabolic energy”.
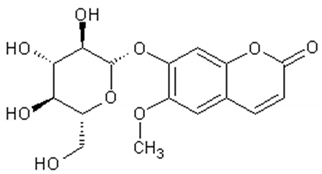
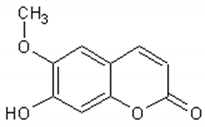
The main coumarins found in Artemisia annua alcoholic extracts are scopolin and scopoletin [83]. Table 4 presents the chemical structures and biological activities of major coumarins present in Artemisia annua extracts.

Table 4.
Structure and biological activities of major coumarins of Artemisia annua.
5. Biological Activities of Artemisia annua
5.1. Antioxidant Activities
Several studies have demonstrated the antioxidant capacity of Artemisia annua [31,39,173], which could be due to the presence of phenolic compounds [30,173].
Messaili et al. [160] demonstrated that the antioxidant activity of Artemisia annua was due to the presence of certain families of compounds, namely terpenes, flavonoids and coumarins. It is worth mentioning that a flavonoid named chrysoprenol D (molecular formula C18H16O8) has been identified as the main molecule contributing to the antioxydant activity of this plant. The authors also showed that the total alcoholic extract of the plant had a stronger antioxidant activity than its fractions, demonstrating the synergistic effect of the molecules present in the plant. The compounds of Artemisia annua extract were found to act primarily by hydrogen atom transfer rather than single-electron transfer.
Another study showed that the essential oil of Artemisia annua had antioxidant properties, based on the use of the 2,2-diphényl-1-picrylhydrazyle (DPPH), 2,2′-azino-bis(3-ethylbenzothiazoline-6-sulfonic acid (ABTS) diammonium salt), Oxygen Radical Absorbance Capacity (ORAC) tests and metal chelating ability using the ferrozine assay [11].
A study investigated the protective effect of the aqueous ethanol extract of Artemisia annua against D-galactose-induced oxidative stress in C57BL / 6J mice. The diet containing the extract of Artemisia annua reduced serum levels of malondialdehyde and 8-OH-Dg, which are biomarkers for lipid peroxidation and DNA damage, respectively. In addition, feeding the mice with Artemisia annua extract diet improved the activity of NQO1 (NAD(P)H: quinone oxidoreductase 1), a typical antioxidant marker enzyme, in organs such as the kidneys, stomach, small intestine and large intestine [18].
5.2. Antidiabetic Activities
Aqueous extracts of Artemisia annua show significant anti-hyperglycemic and anti-hypoinsulinemia activities in diabetic animals. In fact, significant decrease in blood glucose level occurred in animals receiving 28.5 mg/kg twice a day of the aqueous extract [26]. This may be due to stimulation of the secretion of insulin by β cells, inhibition of α cells of the pancreatic islets, or by enhancing insulin activity [174].
In addition, an important link between oxidative stress, inflammatory response and insulin activity is now well established. This can be explained by the ability of antioxidants to protect against the deleterious effects of hyperglycemia and also to improve glucose metabolism. Generally, these antioxidants are flavonoids which were demonstrated to act on biological targets involved in type 2 diabetes mellitus such as α-glycosidase, glucose cotransporter or aldose reductase [175].
The anti-hypoinsulinemic effect of essential oil components of Artemisia annua extract (camphor, germacreneD, artemisia ketone,1,8-cineole) may be attributed to its protective effect against hepatocyte damage through inhibition of the lipopolysaccharide (LPS)-elicited expression of the proinflammatory mediators IL-1β (Interleukin 1 beta), TNF-α (tumor necrosis factor alpha), COX-2 (cyclooxygenase 2) and iNOS (Inducible nitric oxide synthase) [176].
5.3. Cytotoxic and Antitumor Effects
Several studies suggest that artemisinin may not be the most active antitumor compound in Artemisia annua [94,101]. Artemisia annua contains a variety of other biologically active substances [30,101,177], suggesting that this plant could be a source of new herbal anticancer therapies.
Lang et al. [30] demonstrated that Artemisia annua extract free of artemisinin has antitumor activity in vitro and in vivo and identified active compounds. In vitro data were validated in two in vivo cancer models, the chick chorioallantoic membrane (CAM) assay and the orthotopic breast cancer xenografts in nude mice. The Artemisia annua extract, inhibited the viability of breast (MDA-MB-231 and MCF-7), pancreas (MIA PaCa-2), prostate (PC-3), non-small lung cell (A459) cancer cells. Likewise, the extract’s most abundant ingredients, chrysosplenol D, arteannuin B, and casticin, inhibited the viability of MDA-MB-231 breast cancer cells. The extract induced the accumulation of multinucleated cancer cells within 24 h of treatment and increased the number of cells in the S and G2/M phases of the cell cycle, followed by loss of mitochondrial membrane potential, caspase-3 activation, and the formation of an apoptotic hypodiploid cell population. Further, the extract inhibited cancer cell proliferation, decreased tumor growth, and induced apoptosis in vivo in triple negative breast cancer (TNBC) and MDA-MB-231 xenografts grown on CAM as well as in nude mice.
Essential oil isolated from Artemisia annua (100 µg/mL) induced apoptosis in SMMC-7721 hepatocarcinoma cells by nuclear chromatin fragmentation and cytoplasmic condensation [178].
Another study showed that a water-soluble polysaccharide with a molecular weight of 6.3 × 104 Da isolated from Artemisia annua inhibited the growth of HepG2 cells in a dose-dependent manner. phenylindole dihydrochloride (DAPI) staining and flow cytometric analysis revealed that the soluble polysaccharide suppressed cell proliferation via induction of the p65-dependent mitochondrial signaling pathway, as evidenced by the increased activation of caspase-3 and -9, negative regulation of Bcl-2 protein, increased regulation of Bax protein and release of cytochrome c from mitochondria into the cytosol, and suppression of the nuclear factor κB (NF-κB) p65 [179].
Several mechanisms of action regarding the antitumor activities of artemisinin and its derivatives have been identified [99]. The oxidative stress response has a major role, as it has been demonstrated that the endoperoxide moiety is crucial for the bioactivity of artemisinin-type drugs. Its cleavage leads to Reactive Oxygen Species (ROS) formation and presumably oxidative stress. The authors found numerous statistically significant associations between cellular response to artemisinin and mRNA expression of genes involved in oxidative stress response [180,181,182,183]. Artemisinin induces oxidative DNA-damage in dose-dependent manner [99,148]. ROS and oxidative DNA lesions tremendously affect cellular integrity, leading to perturbations in cellular replication and division mechanisms, which ultimately cause cell cycle arrest and cell death. This mechanism is also true for artemisinin-type drugs. Cell cycle arrest has been reported to occur at G1 or G2 checkpoints, presumably depending on individual defects of tumor cell lines in the cell cycle machinery. All these cascades of events lead to cell apoptosis [99]. Depending on the cell model, both mitochondrial (intrinsic) and the extrinsic FAS-receptor-driven pathways of apoptosis can be induced by artemisinin with upregulated Fas/CD95 expression, breakdown of the mitochondrial membrane potential, cytochrome C release, PARP (poly (ADP-ribose) polymerase) cleavage and caspase 3/9activation [184,185]. Other cell death mechanisms induced by artemisinin-type drugs in tumor cells include non-apoptotic cell death mechanisms such as autophagy, necrosis, necroptosis, oncosis (ischemic cell death), anoikis (anchorage-dependent cell death) and ferroptosis [99]. It has been described that ferrous iron enhances the cytotoxicity of artemisinin-type drugs against tumor cells and that the form of iron-dependent cell death termed ferroptosis is tightly linked to artemisinin and its derivatives [186,187].
5.4. Immunomodulatory Effects
Artemisinin and its derivatives have been the subject of several studies on their immunoregulatory properties [188]. They modulate key effectors of the immune system, including toll-like receptors (TLRs) [189,190].
Wojtkowiak-Giera et al. [190] presented two studies demonstrating the immunomodulatory effect of Artemisia annua water extracts on TLR2 and TLR4 immune system components. The first evaluated the effects of Artemisia annua extracts on the expression of TLR2 and TLR4 in the brains of mice with Acanthamoeba infection. The Artemisia annua extract significantly reduced the level of TLR2 expression and altered the level of TLR4 expression.
TLRs are a family of transmembrane proteins belonging to several innate immune receptors located primarily on cells of the immune system and others such as lung cells. These receptors play a key role in the recognition of pathogens, including parasites (by recognizing molecular patterns associated with pathogens (PAMPs) or molecular patterns associated with host-derived damage (DAMPs)) and induce inflammatory mediators production [191]. TLR 2 and 4 are the best known and most studied members of this family [192].
The second study evaluated the effects of Artemisia annua extracts on TLR2 and TLR4 expression in the lungs of mice with acanthamoebiasis [188]. Extracts from Artemisia annua can modulate the expression of both TLRs. The effect of artemisinin and derivatives was suggested to be associated with a decrease in TLR2 expression, TLR4 mRNA expression was found to be increased. Artemisia annua extracts were hence suggested to have anti-inflammatory properties by reducing TLR2 mRNA expression.
Similar effects were reported by Li et al. [193] in in vitro experiments where artesunate, a widely used artemisinin derivative, inhibited the secretion of TNF-α from murine peritoneal macrophages induced by heat-killed Staphylococcus aureus via decreased TLR2 mRNA expression.
Artesunate also decreased the expression of TLR4 and TLR9 mRNA. TLR4 is a receptor that induces inflammatory response activation by the recruitment of adaptor proteins such as MyD88 that leads to the activation of the nuclear factor NF-κB and the production of pro-inflammatory cytokines. It should be noted that artesunate can inhibit the LPS-induced expression of TLR4, MyD88 and NF-κB by blocking the degradation of the inhibitor of NF-κB (IκB) [194].
Artemisinin and its derivatives have been tested for their anti-inflammatory activities in numerous models of auto-immune and allergic conditions.
Artesunate, dihydroartemisinin, artemether and the water-soluble derivative SM905 have been reported to possess protective effects against experimental models of rheumatoid arthritis (RA) [195,196,197,198].
In an experimental RA model, the attenuation of inflammatory symptoms and prevention of tissue damage were obtained with artesunate. Artesunate was found to induce the suppression of proinflammatory cytokines including TNF-α, GM-CSF, IL-1β, IL-6, IL-8 and IL-17α via inhibition of the mitogen activated protein kinase (MAPK), phosphoinositide 3-kinase (PI3K)/Akt and NF-κB signaling pathways [196,198,199]. Artemisinin and derivatives have also been shown to exert anti-angiogenic activities in RA, acting as inhibitors of angiogenesis-related factors such as matrix metalloproteinase-2 (MMP-2) and MMP-9, Vascular Endothelial Growth Factor (VEGF) and hypoxia-inducible factor-1α (HIF-1α) [196,200]. Artemisinin and its derivatives have demonstrated effective antiarthritic properties in RA, with comparable efficacy but a significantly reduced side effect profile as compared to methotrexate [17].
In an experimental murine model of Systemic Lupus Erythematosus (SLE), oral artesunate at 125 mg/kg/d over 16 weeks exhibited comparable immunosuppressive effects to cyclophosphamide, by repressing monocyte chemoattractant protein 1 (MCP-1) and B-cell-activating factor (BAFF) levels, leading to a significant reduction in anti-nuclear antibody and anti-double-strand DNA (dsDNA) antibody production, proteinuria, serum creatinine as well as related renal pathology [201].
Studies have also revealed that a 3–8 week regime of oral water-soluble artemisinin analog SM934 (2.5 and 10 mg/kg/d) exhibited pronounced suppression of proteinuria, glomerulonephritis, development of Th-1 and Th-17 cytokine profiles, and increases in anti-dsDNA, IgG2a and IgG3 antibodies, while promoting increases in Th-2 responses, and serum IL-10 and IL-4 levels in experimental murine models of SLE [202,203].
SM934 demonstrated mixed actions on different subsets of T cells, suppressing the memory/effector T cells, while promoting regulatory T cell development. Notably, these studies have revealed that SM934 can exhibit extensive protective effects in chronic systemic inflammatory condition, comparable to a clinically effective corticosteroid drug like prednisolone [202] or immunosuppressant like rapamycin [203].
In lupus nephritis, a severe and frequently-occurring secondary kidney-specific inflammation following SLE, oral dihydroartemisinin (5–125 mg/kg/d) was found to suppress serum levels of anti-dsDNA antibody and TNF-α and abrogate renal pathology in mice via blockade of NF-κB p65 subunit nuclear translocation [204]. Besides, oral artesunate (150 mg/kg/d) has demonstrated stronger protective effects than prednisone in experimental lupus nephritis, by lowering serum levels of TNF-α and IL-6, and NF-κB p65 subunit and transforming growth factor beta 1 (TGF-1β) expressions in renal tissues [205]. Furthermore, artesunate combined with prednisone was found to induce higher expression of glucocorticoid receptor α (GRα) in peripheral blood mononuclear cells (PBMCs) and to enhance transcriptional coactivator P300/CBP protein expression in renal tissues when compared to prednisone alone in lupus nephritis mice [206].
Artesunate has been shown to possess therapeutic actions against inflammatory bowel disease (IBD) [207]. Artesunate (150 mg/kg/d) dramatically mitigated colon pathology and inflammatory damage in experimental colitis induced by dextran sulfate sodium salt (DSS) or trinitrobenzene sulfonic acid (TNBS). These anti-inflammatory effects of artesunate corroborated well with the suppression of Th-1 and Th-17 cytokines, IFN-γ and TNF-α via the inhibition of NF-κB activities [17].
Artemisinin and its derivatives have been also shown to have anti-allergic activities, which are linked to their immunosuppressive effects mediated by the downregulation of NF-κ p65 subunit, T-bet and IFN-γ expressions [208]. A Chinese trial on 90 subjects with allergic skin disorders has demonstrated that topical artesunate exerts potent efficacy against eczema, erythema multiforme, polymorphous sunlight eruption and hydroa aestivale, and moderate effectiveness against atopic dermatitis, psoriasis vulgaris and dermatomyositis [17].
Cheng et al. [209] demonstrated that artesunate (3–30 mg/kg) prevented IgE-mediated vascular permeability in a passive cutaneous anaphylaxis mouse model, and blocked IgE-induced mast cell degranulation in the lungs, increase in plasma histamine level, and subsequent hypothermia. In RBL-2H3 cells and mature human mast cells, artesunate was found to directly inhibit IgE-induced mast cell degranulation, by blocking Syk tyrosine kinase phosphorylation, the downstream phospholipase Cγ (PLCγ) activation, and elevation in inositol trisphosphate (IP3) and intracellular Ca2+ levels. These findings strongly support a therapeutic role for artemisinin and its derivatives in the treatment of mast-cell-mediated allergic responses.
Artesunate has been shown to protect against experimental allergic asthma. At 3–30 mg/kg/d, artesunate given intraperitoneally markedly inhibited both ovalbumin- and house dust-mite-induced total and eosinophil counts in bronchoalveolar lavage fluid, anti-inflammatory effects comparable to dexamethasone [210,211]. Furthermore, artesunate drastically suppressed aeroallergen induced increases in Th-2 cytokines and chemokines, IL-17, IL-33, MUC5AC, and adhesion molecules in the airways [210]. These protective effects by artesunate in allergic asthma have been associated with its pronounced inhibition of the PI3K/Akt signaling cascade and NF-κB activation. In contrast to the formation of free ROS via cleavage of the endoperoxide bond by heme iron in its structure as a mechanism to kill Plasmodium spp. parasites and to induce cytotoxic effects in cancer cells, in allergic asthma, artesunate was found to decrease the levels of oxidative and nitrosative damage markers including 8-hydroxy-2-deoxyguanosine, 8-isoprostane and 3-nitrotyrosine, in inflamed airways. These antioxidative effects of artesunate were correlated with the inhibition of expression of NADPH oxidases and iNOS, and elevation of superoxide dismutases and catalase, probably via the induction of nuclear factor (erythroid-derived 2)-like 2 (Nrf-2) by artesunate in allergic airways [210]. Four cases of IgE-mediated anaphylactic reactions to oral and intravenous artesunate have been described. These allergic reactions to artemisinin and its derivatives are considerably rare [212].
Artemisinin was demonstrated to be capable of extenuating amyloidogenesis and neuroinflammation in a model of Alzheimer’s disease (AD) in APPswe/PS1dE9 double transgenic mice [213]. Artemisinin (40 mg/kg) given intraperitoneally daily for 30 days abrogated β-secretase activity and decreased neurotic plaque burden in AD mouse model. These anti-inflammatory effects of artesunate have been ascribed to the inhibition of NF-κB activity and the activation of NALP3 inflammasome. Another therapeutic prospect for artemisinin and derivatives has been investigated in an experimental rat model of endometriosis. Artesunate at 150 and 300 mg/kg/d, given intragastrically for 4 weeks, increased apoptosis index and significantly reduced Bcl-2 and microvascular density of the implanted ectopic endometrium, with protective effects comparable to a modified progestogen danazol [214].
5.5. Antibacterial and Antifungal Activities
The essential oil of Artemisia annua has been the subject of numerous studies to test its antibacterial and antifungal activities. Tests were carried out both on the whole oil and on its principal components such as camphor, 1,8-cineol, α-pinene, and artemisia ketone [215].
The main gram-positive bacteria tested with Artemisia annua volatiles organic components obtained by hydrodistillation were Staphylococcus aureus [11,216,217,218,219,220], Enterococcus hirae [217], Enterococcus faecalis [219], Streptococcus pneumonia, Micrococcus luteus [220], Bacillus cereus [219], Sarcina lutea [11], Bacillus subtilis [220], Bacillus spp. [217], and Listeria innocua [221]. For the gram-negative bacteria, Escherichia coli [217,218,219,220], Escherichia coli UPEC-Uropathogenic [220], Escherichia coli ETEC-Enterotoxigenic, Escherichia coli EPEC-Enteropathogenic, Escherichia coli EIEC Enteroinvasive, Escherichia coli STEC-Shiga-toxin producer [222], Shigella sp., Salmonella enteritidis, Klebsiella pneumoniae [11], Haemophilus influenzae [220], and Pseudomonas aeruginosa [218,219,220] were tested. All microorganisms tested were inhibited by this essential oil [11].
The main gram-positive bacteria tested with methanol, chloroform, ethanol, hexane, and petroleum ether extracts of Artemisia annua were Staphylococcus aureus [13,219], Enterococcus faecalis [219], Micrococcus luteus [13], Bacillus cereus [13,219], Bacillus subtilis, Bacillus pumilus [13], and Bacillus sp. [219]. For the gram-negative bacteria, Escherichia coli [13,219], Escherichia coli UPEC [219], Salmonella typhi and Pseudomonas aeruginosa [13,219] were tested. All microorganisms tested were inhibited.
Li et al. [27] studied the antifungal activity of Artemisia annua extracts against Fusarium oxysporum, Fusarium solani and Cylindrocarpon destrutans which are three fairly common agricultural fungal pathogens causing root rot disease in the cultivation of plants such as medicinal materials and crops. This study revealed that a coumarin derivative present in the plant Artemisia annua with an additional acetyl group attached to C-6 has a wide range of antifungal properties and is active against the three agricultural pathogenic fungi.
Further studies have been performed with the main components present in Artemisia. annua essential oil. These studies showed that artemisia ketone is the oil component that has the greatest antimicrobial activity. In fact, it turned out to be effective against bacteria and some fungi (C. albicans and A. fumigatus) at very low concentrations (range 0.07–10 mg/mL). The other compounds tested in the studies have produced variable results. However, it should be emphasized that all the compounds tested were active (range 1.25–5 mg/mL) against A. fumigatus, a dangerous microorganism frequently responsible for nosocomial infections in immunocompromised individuals [215].
The antifungal activity of the essential oil was also evaluated against economically important foliar and soilborne fungal pathogens of tomato. The essential oil was active against Sclerotinia sclerotiorum, Botrytis cinerea, Phytophthora infestans, and Verticillim dahliae [223].
5.6. Antiviral Activities
There is evidence of in vitro and in vivo antiviral activities of the Artemisia annua extract as well as artemisinin and its derivatives. Tested viruses include both DNA and RNA viruses [224].
A methanolic extract of Artemisia annua was tested in a syncytium inhibition assay, which is based on the interaction between the HIV-1 envelope and the CD4 cell membrane protein on T-lymphocytes [225].
An in vitro study has shown that tea infusion of Artemisia annua has anti-HIV activity. The presence of HIV-malaria coinfection in malaria endemic areas has raised the question of anti-HIV activity of Artemesia annua and Artemisia afra folksy used for malaria treatment. It has rapidly been demonstrated that artemisinin was not the main compound by which these plants exerted their anti-HIV activities. In vitro, Artemisia annua tea infusion was found to be highly active, with IC50 values as low as 2.0 μg/mL, while artemisinin was inactive at 25 µg/mL [16]. Nevertheless, in vitro models of NL3.4 HIV-1 infected PBMCs showed that 10 µM of artemisinin inhibited HIV-1 replication by 60% [226]. Jana et al. [227] found that three of their six synthesized 1,5-disubstituted 1,2,3-triazole dihydroartemisinin derivatives showed significant anti-HIV activity with IC50 values ranging from 1.34 to 2.65 µM, while Effert et al. [228] only found weak inhibition rates against two HIV-1 strains.
Artemisinin and its derivatives from the plant Artemisia annua, in particular artesunate, have potent inhibitory effects against double-stranded DNA viruses, including CytoMegaloVirus (CMV), Herpes Simplex Virus 1 (HSV-1), Human Herpes Virus 6A (HHC-6A) and Epstein–Barr Virus (EBV) [229,230].
Most of the studies on the antiviral effects of artemesinin and its derivatives concern the human cytomegalovirus (HCMV) [224]. Effert et al. [228] demonstrated that the artemisinin derivative artesunate inhibited the replication of both sensitive and ganciclovir-resistant strains of HCMV. The authors found that artesunate both inhibits the viral activation of the cellular transcription factor NF-κB and Sp-1 and downregulates the phosphorylation of the upstream kinase P13K. The anti-HCMV activity of artemisinin derivatives was confirmed by other authors, using artemisinin-based dimer and trimer molecules and trioxane-ferrocene hybrids. All the derivatives were highly active and showed very low IC50 value compared to artesunate, artemether, dihydroartemisinin or ganciclovir [97,231,232,233,234]. Hutterer et al. [234] described the drug to bind to NF-κB RelA/p65, this way inhibiting the cell HCMV-upregulated NF-κB activity. The same author described the anti-CMV activity not only for HCMV strains but also for rat, guinea pig and mouse CMV strains.
The use of combined therapy strategies to fight against ganciclovir-resistant HCMV also brought to light the importance of anti-HCMV activity of artemisinin and its derivatives. Such combinations were found in patients with complications of CMV infection after hematopoietic stem cell transplantation. Oral administration of artesunate isolated from Artemisia annua (100 mg/d) resulted in a rapid reduction in viral load (1.7 to 2.1 log reduction) in whole blood and improved hematopoiesis within 10 days [235].
Activities of artesunate were also evaluated with Human Herpes Simplex Virus 1 (HSV1). Effert et al. [228] showed that artesunate strongly inhibited HSV1 in vitro, with no effect on cell viability. In the same vein, Canivet et al. [230] showed an improved outcome of HSV1-induced encephalitis in mice treated with combination of artesunate-valacyclovir compared to valacyclovir monotherapy. The authors also described a decrease in proinflammatory cytokines (IL-1β, IL-2, IL-6, IFN-γ) and chemokines (CCL2, CCL4, CCL6) with the combined treatment compared to valacyclovir alone.
Data on the activities of artemisinin and its derivatives on Human Herpes Virus 6 (HHV6) are inconclusive. Some authors described an inhibitory effect of artemisinin on HHV-6A replication and early and late protein synthesis with an IC50 of 3.80 ± 1.06 μM with no drug-induced apoptosis or necrotic cytotoxicity [230], while such an observation was not found in another study on HHV-6A and HHV-B [236]. Hakacova and al. [237] described a case of a decreased HHV-6B DNA in endomyocardial biopsies of a child with HHV-6 myocarditis and an improvement in clinical status after artesunate treatment, with no adverse effects of the molecule.
Artesunate has also been shown to be effective against hepatitis B virus (HBV) replication [238]. Artesunate was found to suppress HBV surface antigen (HBsAg) secretion with an IC50 value of 2.3 μM, and to reduce HBV-DNA levels with an IC50 value of 0.5 μM [239] in vitro, at a concentration range below the plasma drug concentration required in anti-malarial treatment (~ 7 μM) [240].
Other studies with DNA viruses showed that artesunate inhibited the polyomavirus BK (BKV) infection in human primary proximal tubular epithelial cells. The loads of extracellular BKV DNA, reflecting viral progeny production, were reduced in a concentration-dependent manner. At 10 μM, artesunate reduced the extracellular viral load by 65% and early large T antigen mRNA and protein expression by 30% and 75%, respectively. It also decreased DNA replication by 73%; and late VP1 mRNA and protein expression by 47% and 64%, respectively. The authors also highlighted that artesunate was inhibiting the proliferation of the proximal tubular epithelial cells in a concentration-dependent manner. The inhibition mechanism involved was a cytostatic rather than a cytotoxic mechanism [241]. The same authors described the inhibitory effects of artesunate on the human JC polyomavirus (JCPyV) in a concentration-dependent manner. With an EC50 of 2.9 µM, artesunate decreased extracellular viral DNA load correlated with a decreased expression of capsid protein VP1 and a reduced release of viral progeny. Cell cytotoxicity was observed for high concentrations of artesunate [242].
In human papillomavirus (HPV)-immortalized and transformed cervix cells, apoptosis was observed with artesunate and dihydroartemisinin treatment. Cell death induced by dihydroartemisinin involved the activation of the mitochondrial caspase pathway and was independent of the p53 pathway. However, no change was found regarding the HPV-related oncogene expression. These observations lead the authors to the conclusion that dihydroartemisinin might be useful for the topic treatment of mucosal HPV lesions, including lesions which had reached the neoplastic state [243]. The same antiproliferative effect was described using artemisinin in HPV39-infected cervical carcinoma cells [244].
Regarding RNA viruses, it has been demonstrated in vitro that artemisinin and its derivatives are also effective against single-stranded RNA viruses from the Flaviviridae family including Hepatitis C Virus (HCV) [245,246,247] and bovine viral diarrhea virus (BVDV) [248,249]. Co-treatment with hemin or ferrosanol resulted in enhanced anti-Flaviviridae activity of artemisinin derivatives (224).
In a case report about a malaria patient suffering from dengue shock syndrome acute renal failure, a treatment with intravenous artemisinin in addition to standard therapy was successful. However, the specific effect of artemisinin against the dengue virus (DENV) has not been demonstrated [250]. Artesunate seems not to be active against influenza viruses [228].
5.7. Antiparasitic Activities
5.7.1. Antiplasmodial Activity
Malaria patients in Central Africa treated with Artemisia annua tea, at a dose corresponding to the recommendations of the Chinese pharmacopoeia, have shown a very rapid disappearance of malaria parasites in the blood.
Five malaria patients treated with Artemisia annua tea showed a rapid disappearance of the parasitemia in 2 to 4 days. An additional trial with 48 malaria patients showed a disappearance of parasitemia in 44 patients (92%) in 4 days. Both trials showed a clear improvement in symptoms [12].
A double blind, randomized clinical trial with 957 malaria-infected patients had two treatment arms: 472 patients for artesunate-amodiaquine and 471 for Artemisia extracts (248 Artemisia annua, 223 Artemisia afra). Artesunate-amodiaquine-treated patients were treated per manufacturer posology, and Artemisia-treated patients received 1 L/d of dry leaf/twig infusions for 7 days; both arms had 28 days follow-up. Trophozoites disappeared after 24 h with Artemisia annua treatment but took up to 14 days to disappear in patients treated with artesunate-amodiaquine. Cure rates for Day 28 defined as the absence of parasitaemia were 91%, 100% and 30% for adults for Artemisia afra, Artemisia annua and artesunate-amodiaquine, respectively. The onset of fever took 48 h for artesunate-amodiaquine, but 24 h for Artemisia annua [251].
A specially prepared ether extract of Artemisia annua, when fed to mice infected with malaria, was effective in 95–100% of cases [252]. However, artemisinin did not kill the liver stages of the parasite, was metabolized rapidly, and remained in the bloodstream for only a few hours [253]. Hence, it cannot be used as a prophylactic drug. The World Health Organization now recommends the use of artemisinin combination therapies for the first-line treatment of uncomplicated malaria [254], to reduce the risk of parasite resistance and recrudescence.
5.7.2. Anti-Helminthic Activities
Schistosomiasis affects 250 million people in 78 countries with 280,000 deaths each year [255] and with an estimated 172 million infected in sub-Saharan Africa [256]. The disease is caused by trematode worms of the genus Schistosoma with six species (S. haematobium, S. mansoni, S. japonicum, S. mekongi, S. intercalatum, and S. malayensis). S. mansoni and S. haematobium are the main responsible agents for intestinal and urinary schistosomiasis, respectively, that occur mainly in Africa (230). The majority of in vivo investigations reported an anti-schistosomal effect of artemether. Other derivatives (artesunate, arteether, dihydroartemisinin) were studied to a lesser extent. The drugs have been applied to animals per os or intragastrically. Artemisinin derivatives strongly reduced the total worm rates independent of application routes, with observed stronger reduction rates for female than male worms. Artemisinin derivatives also significantly reduced worm eggs burden and egg-caused granulomata in the liver of host animals. It has been described that artemether and arteether were as active against praziquantel-resistant S. japonicum as they were against the sensitive strain [33]. As it has been proposed that cleavage of the endoperoxide moiety, which is crucial for bioactivity, is facilitated in the presence of ferrous iron (Fe3+) from hemin or other sources by a Fenton-type reaction [21,22,23,24], and the combination of artemether and hemin led to higher worm reduction rates than artemether alone [35]. Artemisinin and its derivatives were found to exert oxidative stress in the worms, which leads to glutathione (GSH) depletion and lipid peroxidation. Several anti-oxidant enzymes were reported to be able to inhibit, e.g., glutathione S-transferase (GST), glutathione peroxidase (GPx), glutathione reductase (GR), superoxide dismutase (SOD), cytochrome C peroxidase (cytC). The impaired oxidative stress response in the parasite led to severe morphological damage, e.g., lesions in tegument (swelling, vesiculation, erosion, and peeling), subtegumental musculature, parenchymal tissue, gastrodermis and degeneration of male and female reproduction organs. Furthermore, a number of metabolic enzymes were inhibited, such as glucose-6-phosphate isomerase (GPI), phosphofructokinase (PFK), glyceraldehyde-3-phosphate dehydrogenase (GAPDH), lactate dehydrogenase (LDH), phosphoglycerate kinase PGK), pyruvate kinase (PK), phosphoglycerate mutase (PGAM), aldolase (ALDO), enolase (ENO), hexokinase (HK), malate dehydrogenase (MDH), malic enzyme (ME), glucose-6-phosphate dehydrogenase (G6PD), 6-phosphogluconate dehydrogenase (PGD), mannose-6-phosphateisomerase (MPI), alkaline and acidic phosphatases (ALP, ACP), adenosine triphosphatase, Ca2+-ATPase, Mg2+-ATPase, and Na+/K+-ATPase. Both oxidative and metabolic stress led to damage to tegument, tissues and reproductive organs, as well as growth accompanied by decreased worm length [257].
Artemisinin and its derivatives were also found to be active against a number of nematodes. In an in vitro study, artemether treatment caused cuticular changes on adult Toxocara canis similar to those induced by albendazole sulfoxide with faster onset of action [258]. Several potential mechanisms of action were described, including disruption of the functions of ion pumps on the apical plasma membrane, of sarcoplasmic/endoplasmic reticulum Ca2+-ATPase PfATP6, or mitochondria of the parasite [258,259]. Artemisinin has also been reported to treat adult and larva Toxocara spiralis in both in vitro and in vivo studies). Incubation of adult Toxocara spiralis worms in 0.05 mg/mL artemisinin solution for 24 h revealed marked swellings, sloughing, and blebbing of the cuticle and loss of normal creases, ridges, and annulations of fissures and vesicles [260]. Abou Rayia et al. [260] observed a significant decrease in the mean number of adult worms in the small intestine and the total larvae in muscles of mice, 75% (17.6 ± 1.82) and 72% (12,490 ± 336.15), respectively, after treatment with an oral dose of 400 mg/kg of artemisinin. The results were comparable to those obtained with mice treated with mebendazole showing a 78.7% (15 ± 1.41) reduction in adult worm number and a 68% (14,300 ± 877.5) reduction in muscle larva number, respectively. Histopathology of the small intestine showed a reduction in the inflammatory infiltrates with both drugs and a significant reduction in both the number of deposited larvae and the intensity of the inflammatory infiltrate in the skeletal muscle of the mice. The reduction in the number of deposited larvae was more evident in the artemisinin-treated group. Moreover, the extent of reduction in COX-2 and VEGF expressions in the cytoplasm of inflammatory cells was greater in mice treated with artemisinin than in those treated with mebendazole. Mechanisms of action of artemisinin towards adult and larva worms of Toxocara spiralis are assumed to derive from damage by toxic free radicals and the inhibition of the parasite angiogenesis by suppression of VEGF expression, which may affect the nutrition status and waste removal of the larva worms [261].
Other nematodes on which artemisinin and Artemisia extracts have been tested include Haemonchus contortus in ruminants and plant nematodes (Meloidogyne spp., Globodera rostochiensis, and Xiphinema index) [262].
Many other helminthic infections were tested with artemisinin and its derivatives including cestode infections (Echinococcus spp., Taenia crassiceps) and other trematodes infections (Echinostoma spp., Fasciola spp., Clonorchis sinensis, Opisthorchis viverrini, Paragonimus westermani, Heterophyes heterophyes, and Paramphistomum microbothrium) [263].
5.7.3. Activity against Other Protozoa
Beside the outstanding antimalarial and antischistosomal activities, artemisinin and its derivatives also possess activities against other protozoan parasites.
Many studies describe the in vitro and in vivo activities of artemisinin and its derivatives against protozoan parasites, including Leishmania spp., Trypanosoma spp., Toxoplasma gondii, Neospora caninum, Eimeria tenella, Acanthamoeba castellanii, Naegleria fowleri, Cryptosporidium parvum, Giardia lamblia, and Babesia spp [264].
A study on the activity of Artemisia annua on the genus Acanthamoeba showed that water, alcohol and chloroform extracts from Artemisia annua can be applied in general and local treatment or in combined therapy with antibiotics in the treatment of acanthamoebiasis. Extracts from Artemisia annua showed not only in vitro but also in vivo effects. The pure artemisinin preparation affected amoebae from 100 to 300 times more strongly than the studied extracts. The most active anti-amoeba extract was chloroform extract. Studies carried out on experimental animals infected with amoebae showed that the application of these extracts significantly prolonged the survival of the animals [265].
6. Conclusions
Artemisia annua is widely distributed throughout the world. It is one of the most important plants used in traditional medicine in China and Africa. It has been brought to light again very recently in Madagascar for the prevention and treatment of COVID-19. The aim of this review was to list the molecules most present in this species, regardless of its geolocation, and to describe what is currently known about their properties in the treatment of various diseases in vitro and in vivo models. On the whole, the main objective of this review was to bring together all the available scientific research that has been conducted on this species.
Differences in the chemical composition of Artemisia annua extracts can be linked to several factors: geolocation, plant parts used, methods of sample preparation and extraction, genetic differences and cultivation process. These variations can influence the biological properties of this plant. Future research should focus on establishing a reproducible quality control protocol to minimize metabolic variations between individuals. This quality control should include the climate, the season of harvest, the humidity, the richness of the soil, the altitude, the maturity of the plant and the part of the plant used.
Artemisia annua has been extensively investigated and shows promising activities: antiplasmodial, antiviral, antimicrobial, antitumor, antiinflammatory, antioxidant. Studies present artemisinin as the active compound of this plant especially for the antimalarial activity. However, other studies show that the species Artemisia afra, which does not produce artemisinin, has similar antimalarial properties to Artemisia annua. The fact that artemisinin is absent would be beneficial in the fight against parasite resistance. Bio-guided studies should be considered to identify the active molecule(s). A comparative study of the compounds present in the two species shall be considered and in vitro and in vivo experiments shall be considered. In Madagascar, a drink based on an infusion of Artemisia annua in mixtures with other plants to prevent and combat COVID-19, is recommended; however, in vitro and in vivo studies are needed to validate these claims. In addition, this plant is not authorized in the French Pharmacopoeia. To date, the State of Madagascar has not received any marketing authorization for this drink. Studies to check for toxic or harmful effects of this plant are extremely important and necessary.
On the basis of the data presented in this review, it can be concluded that Artemisia annua may become a future flagship species in the treatment of various pathologies, if the problems associated with quality control and authorization for use could be resolved and, more importantly, if we can identify the potentially active component(s), in particular the secondary metabolites active against the new coronavirus SARS-CoV-2 responsible for COVID-19. Studies are in progress in this direction but also on the comparison between Artemisia annua and Artemisia afra in our laboratory. Artemisinin is a compound of interest which is not necessarily the most active molecule of the genus Artemisia and does not have the most promising antiviral activity. With this in mind, a clinical trial began in early July in Madagascar to test the antiviral effect of artesunate, a derivative of artemisinin coupled with a high dose of vitamin C, against SARS-CoV-2. The first results will be known by August. The use of artesunate and not artemisinin shows that it is not obvious that this molecule has the most interesting bioactivity.
Author Contributions
Conceptualization and writing—original draft preparation, A.S.-M. and M.L.R.; review and editing, all authors. All authors have read and agree to the published version of the manuscript.
Funding
This work was financially supported by the European Union and La Région Réunion (CPER/FEDER, VIROPAM project).
Conflicts of Interest
The authors declare no conflict of interest.
Abbreviations
| ABTS | Acide 2,2′-azino-bis(3-éthylbenzothiazoline-6-sulphonique) |
| ACP | Acidic Phosphatases |
| ART | Artesunate |
| AD | Alzheimer’s Disease |
| ALDO | Aldolase |
| ALP | Alkaline Phosphatases |
| BAFF | B cell-activating factor |
| BKV | Polyomavirus BK |
| BVDV | Bovine Viral Diarrhea Virus |
| CAM | Chorioallantoic Membrane |
| CMV | CytoMegaloVirus |
| COX-2 | Cyclooxygenase 2 |
| CytC | Cytochrome C peroxidase |
| DAPI | Phenylindole dihydrochloride |
| DENV | Dengue Virus |
| DHA | Dihydroartemisinin |
| DPPH | 2,2-diphényl-1-picrylhydrazyle |
| DSS | Sulfate Sodium Salt |
| EBV | Epstein-Barr Virus |
| ENO | Enolase |
| GAPDH | Glyceraldehyde-3-Phosphate Dehydrogenase |
| G6PD | Glucose-6-Phosphate Dehydrogenase |
| GPI | Glucose-6-Phosphate Isomerase |
| GPx | Glutathione Peroxidase |
| GR | Glutathione Reductase |
| GRα | Glucocorticoid receptor α |
| GSH | Glutathione |
| GST | Glutathione S-Transferase |
| HBsAg | HBV surface antigen |
| HBV | Hepatitis B Virus |
| HCMV | Human Cytomegalovirus |
| HCV | Hepatitis C Virus |
| HHC-6A | Human Herpes Virus 6A |
| HIF-1α | Hypoxia-Inducible Factor-1α |
| HK | Hexokinase |
| HPV | Human Papillomavirus |
| HSV-1 | Herpes Simplex Virus 1 |
| IBD | Inflammatory Bowel Disease |
| IL-1β | Interleukin 1 beta |
| iNOS | Inducible Nitric Oxide Synthase |
| IP3 | Inositol trisphosphate |
| JCPyV | Human JC Polyomavirus |
| LDH | Lactate Dehydrogenase |
| LDL | Low Density Lipoprotein |
| LPS | Lipopolysaccharide |
| MAPK | Mitogen Activated Protein Kinase |
| MCP-1 | Monocyte Chemoattractant Protein 1 |
| MDH | Malate Dehydrogenase |
| ME | Malic Enzyme |
| MMP-2 | Metalloproteinase-2 |
| MPI | Mannose-6-Phosphateisomerase |
| NF-κB | Nuclear Factor κB |
| Nrf-2 | Nuclear Factor (erythroid-derived 2)-like 2 |
| ORAC | Oxygen Radical Absorbance Capacity |
| PARP | Poly (ADP-ribose) Polymerase |
| PFK | Phosphofructokinase |
| PGAM | Phosphoglycerate Mutase |
| PGD | 6-Phosphogluconate Dehydrogenase |
| PGK | Phosphoglycerate Kinase |
| PI3K | Phosphoinositide 3-kinase |
| PK | Pyruvate Kinase |
| PLCγ | Phospholipase Cγ |
| RA | Rheumatoid Arthritis |
| ROS | Reactive Oxygen Species |
| SLE | Systemic Lupus Erythematosus |
| SM905 | 1-(12β-dihydroartemisinoxy)-2-hydroxy-3-tert-butylaminopropane maleate, new water-soluble derivative |
| SM934 | β-aminoarteether maleate, new water-soluble derivative |
| SOD | Superoxide Dismutase |
| TGF-1β | Transforming Growth Factor beta 1 |
| TNBC | Triple Negative Breast cancer |
| TNBS | Trinitrobenzene Sulfonic acid |
| TNF-α | Tumor Necrosis Factor alpha |
| VEGF | Vascular Endothelial Growth Factor |
References
- Bora, K.S.; Sharma, A. The Genus Artemisia: A Comprehensive Review. Pharm. Biol. 2011, 49, 101–109. [Google Scholar] [CrossRef]
- Sanz, M.; Vilatersana, R.; Hidalgo, O.; Garcia-Jacas, N.; Susanna, A.; Schneeweiss, G.M.; Vallès, J. Molecular Phylogeny and Evolution of Floral Characters of Artemisia and Allies (Anthemideae, Asteraceae): Evidence from NrDNA ETS and ITS Sequences. TAXON 2008, 57, 66–78. [Google Scholar] [CrossRef]
- Alesaeidi, S.; Miraj, S. A Systematic Review of Anti-Malarial Properties, Immunosuppressive Properties, Anti-Inflammatory Properties, and Anti-Cancer Properties of Artemisia Annua. Electron. Physician 2016, 8, 3150–3155. [Google Scholar] [CrossRef] [PubMed]
- Funk, V.A.; Bayer, R.J.; Keeley, S.; Chan, R.; Watson, L.; Gemeinholzer, B.; Schilling, E.; Panero, J.L.; Baldwin, B.G.; Garcia-Jacas, N.; et al. Everywhere but Antarctica: Using a Supertree to Understand the Diversity and Distribution of the Compositae. Biol. Skr. 2005, 55, 343–374. [Google Scholar]
- Vallès, J.; Garcia, S.; Hidalgo, O.; Martín, J.; Pellicer, J.; Sanz, M.; Garnatje, T. Biology, Genome Evolution, Biotechnological Issues and Research Including Applied Perspectives in Artemisia (Asteraceae). Adv. Bot. Res. 2011. [Google Scholar] [CrossRef]
- Jarvis, C.E. A List of Linnaean Generic Names and Their Types; Koeltz Sciebtific Books; International Association for Plant Taxonomy: Bratislava, Slovakia, 1993; Volume 127, p. 100. [Google Scholar]
- Willcox, M. Artemisia Species: From Traditional Medicines to Modern Antimalarials—and Back Again. J. Altern. Complement. Med. 2009, 15, 101–109. [Google Scholar] [CrossRef]
- Ko, Y.S.; Lee, W.S.; Panchanathan, R.; Joo, Y.N.; Choi, Y.H.; Kim, G.S.; Jung, J.-M.; Ryu, C.H.; Shin, S.C.; Kim, H.J. Polyphenols from Artemisia Annua L Inhibit Adhesion and EMT of Highly Metastatic Breast Cancer Cells MDA-MB-231. Phytother. Res. 2016, 30, 1180–1188. [Google Scholar] [CrossRef]
- L’Artemisia annua. La Maison de l’Artemisia-Cette Plante Peut Sauver des Millions de Vie. Available online: https://maison-artemisia.org/l-artemisia-du-cote-agronomique/artemisia-annua/ (accessed on 3 June 2020).
- Hsu, E. The History of Qing Hao in the Chinese Materia Medica. Trans. R. Soc. Trop. Med. Hyg. 2006, 100, 505–508. [Google Scholar] [CrossRef]
- Ćavar, S.; Maksimović, M.; Vidic, D.; Parić, A. Chemical Composition and Antioxidant and Antimicrobial Activity of Essential Oil of Artemisia Annua L. from Bosnia. Ind. Crop. Prod. 2012, 37, 479–485. [Google Scholar] [CrossRef]
- Mueller, M.S.; Karhagomba, I.B.; Hirt, H.M.; Wemakor, E. The Potential of Artemisia Annua L. as a Locally Produced Remedy for Malaria in the Tropics: Agricultural, Chemical and Clinical Aspects. J. Ethnopharmacol. 2000, 73, 487–493. [Google Scholar] [CrossRef]
- Gupta, P.C.; Dutta, B.; Pant, D.; Joshi, P.; Lohar, D.R. In Vitro Antibacterial Activity of Artemisia Annua Linn. Growing in India. Int. J. Green Pharm. 2009, 3. [Google Scholar] [CrossRef]
- Abad, M.J.; Bedoya, L.M.; Apaza, L.; Bermejo, P. The Artemisia L. Genus: A Review of Bioactive Essential Oils. Molecules 2012, 17, 2542–2566. [Google Scholar] [CrossRef] [PubMed]
- Wang, D.; Cui, L.; Chang, X.; Guan, D. Biosynthesis and Characterization of Zinc Oxide Nanoparticles from Artemisia Annua and Investigate Their Effect on Proliferation, Osteogenic Differentiation and Mineralization in Human Osteoblast-like MG-63 Cells. J. Photochem. Photobiol. B 2020, 202, 111652. [Google Scholar] [CrossRef]
- Lubbe, A.; Seibert, I.; Klimkait, T.; van der Kooy, F. Ethnopharmacology in Overdrive: The Remarkable Anti-HIV Activity of Artemisia Annua. J. Ethnopharmacol. 2012, 141, 854–859. [Google Scholar] [CrossRef]
- Ho, W.E.; Peh, H.Y.; Chan, T.K.; Wong, W.S.F. Artemisinins: Pharmacological Actions beyond Anti-Malarial. Pharmacol. Ther. 2014, 142, 126–139. [Google Scholar] [CrossRef]
- Kim, M.H.; Seo, J.Y.; Liu, K.H.; Kim, J.-S. Protective Effect of Artemisia Annua L. Extract against Galactose-Induced Oxidative Stress in Mice. PLoS ONE 2014, 9, e101486. [Google Scholar] [CrossRef]
- Wang, Y.; Chen, J.; Zhang, D.; Zhang, Y.; Wen, Y.; Li, L.; Zheng, L. Tumoricidal Effects of a Selenium (Se)-Polysaccharide from Ziyang Green Tea on Human Osteosarcoma U-2 OS Cells. Carbohydr. Polym. 2013, 98, 1186–1190. [Google Scholar] [CrossRef]
- Castilho, P.C.; Gouveia, S.C.; Rodrigues, A.I. Quantification of Artemisinin in Artemisia Annua Extracts by 1H-NMR. Phytochem. Anal. 2008, 19, 329–334. [Google Scholar] [CrossRef]
- Chaudhary, V.; Kapoor, R.; Bhatnagar, A.K. Effectiveness of Two Arbuscular Mycorrhizal Fungi on Concentrations of Essential Oil and Artemisinin in Three Accessions of Artemisia Annua L. Appl. Soil Ecol. 2008, 40, 174–181. [Google Scholar] [CrossRef]
- Slezakova, S.; Ruda-Kucerova, J. Anticancer Activity of Artemisinin and Its Derivatives. Anticancer Res. 2017, 37, 5995–6003. [Google Scholar] [CrossRef]
- Tse, E.G.; Korsik, M.; Todd, M.H. The Past, Present and Future of Anti-Malarial Medicines. Malar. J. 2019, 18, 93. [Google Scholar] [CrossRef]
- Brisibe, E.A.; Umoren, U.E.; Brisibe, F.; Magalhäes, P.M.; Ferreira, J.F.S.; Luthria, D.; Wu, X.; Prior, R.L. Nutritional Characterisation and Antioxidant Capacity of Different Tissues of Artemisia Annua L. Food Chem. 2009, 115, 1240–1246. [Google Scholar] [CrossRef]
- Van der Kooy, F.; Sullivan, S.E. The Complexity of Medicinal Plants: The Traditional Artemisia Annua Formulation, Current Status and Future Perspectives. J. Ethnopharmacol. 2013, 150. [Google Scholar] [CrossRef]
- Bhakuni, R.S.; Jain, D.C.; Sharma, R.P.; Kumar, S. Secondary Metabolites of Artemisia Annua and Their Biological Activity. Curr. Sci. 2001, 80, 35–48. [Google Scholar]
- Li, K.-M.; Dong, X.; Ma, Y.-N.; Wu, Z.-H.; Yan, Y.-M.; Cheng, Y.-X. Antifungal Coumarins and Lignans from Artemisia Annua. Fitoterapia 2019, 134, 323–328. [Google Scholar] [CrossRef] [PubMed]
- Yw, Z.; Fy, N.; Yl, S.; Sy, W.; Wz, H.; Zz, W.; Wei, X. Chemical Constituents from Artemisia Annua. Zhongguo Zhong Yao Za Zhi 2014, 39, 4816–4821. [Google Scholar]
- El-Askary, H.; Handoussa, H.; Badria, F.; El-Khatib, A.H.; Alsayari, A.; Linscheid, M.W.; Abdel Motaal, A. Characterization of Hepatoprotective Metabolites from Artemisia Annua and Cleome Droserifolia Using HPLC/PDA/ESI/MS–MS. Rev. Bras. De Farmacogn. 2019, 29, 213–220. [Google Scholar] [CrossRef]
- Lang, S.J.; Schmiech, M.; Hafner, S.; Paetz, C.; Steinborn, C.; Huber, R.; Gaafary, M.E.; Werner, K.; Schmidt, C.Q.; Syrovets, T.; et al. Antitumor Activity of an Artemisia Annua Herbal Preparation and Identification of Active Ingredients. Phytomedicine 2019, 62, 152962. [Google Scholar] [CrossRef]
- Wan, X.L.; Niu, Y.; Zheng, X.C.; Huang, Q.; Su, W.P.; Zhang, J.F.; Zhang, L.L.; Wang, T. Antioxidant Capacities of Artemisia Annua L. Leaves and Enzymatically Treated Artemisia Annua L. in Vitro and in Broilers. Anim. Feed Sci. Technol. 2016, 221, 27–34. [Google Scholar] [CrossRef]
- Song, Y.; Desta, K.T.; Kim, G.-S.; Lee, S.J.; Lee, W.S.; Kim, Y.-H.; Jin, J.S.; Abd El-Aty, A.M.; Shin, H.-C.; Shim, J.-H.; et al. Polyphenolic Profile and Antioxidant Effects of Various Parts of Artemisia Annua L. Biomed. Chromatogr. 2016, 30, 588–595. [Google Scholar] [CrossRef]
- Li, Y.-J.; Guo, Y.; Yang, Q.; Weng, X.-G.; Yang, L.; Wang, Y.-J.; Chen, Y.; Zhang, D.; Li, Q.; Liu, X.-C.; et al. Flavonoids Casticin and Chrysosplenol D from Artemisia Annua L. Inhibit Inflammation in Vitro and in Vivo. Toxicol. Appl. Pharmacol. 2015, 286, 151–158. [Google Scholar] [CrossRef] [PubMed]
- Wang, J. Casticin Alleviates Lipopolysaccharide-Induced Inflammatory Responses and Expression of Mucus and Extracellular Matrix in Human Airway Epithelial Cells through Nrf2/Keap1 and NF-ΚB Pathways. Phytother. Res. 2018, 32, 1346–1353. [Google Scholar] [CrossRef]
- Shin, N.-R.; Ryu, H.-W.; Ko, J.-W.; Park, S.-H.; Yuk, H.-J.; Kim, H.-J.; Kim, J.-C.; Jeong, S.-H.; Shin, I.-S. Artemisia Argyi Attenuates Airway Inflammation in Ovalbumin-Induced Asthmatic Animals. J. Ethnopharmacol. 2017, 209, 108–115. [Google Scholar] [CrossRef]
- Qiu, F.; Wu, S.; Lu, X.; Zhang, C.; Li, J.; Gong, M.; Wang, M. Quality Evaluation of the Artemisinin-Producing Plant Artemisia Annua L. Based on Simultaneous Quantification of Artemisinin and Six Synergistic Components and Hierarchical Cluster Analysis. Ind. Crop. Prod. 2018, 118, 131–141. [Google Scholar] [CrossRef]
- Zhang, X.-B.; Guo, L.-P.; Qiu, Z.-D.; Qu, X.-B.; Wang, H.; Jing, Z.-X.; Huang, L.-Q. [Analysis of spatial distribution of artemisinin in Artemisia annua in China]. Zhongguo Zhong Yao Za Zhi 2017, 42, 4277–4281. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.-B.; Zhao, Y.-P.; Huang, X.-W.; Qiu, Z.-D.; Guo, L.-P.; Qu, X.-B.; Huang, L.-Q. [Review on study of Dao-di herbs Artemisiae Annuae Herba]. Zhongguo Zhong Yao Za Zhi 2016, 41, 2015–2018. [Google Scholar] [CrossRef]
- Gouveia, S.C.; Castilho, P.C. Artemisia Annua L.: Essential Oil and Acetone Extract Composition and Antioxidant Capacity. Ind. Crop. Prod. 2013, 45, 170–181. [Google Scholar] [CrossRef]
- Marlet, C.; Lognay, G. Les monoterpènes: Sources et implications dans la qualité de l’air intérieur. Biotechnol. Agron. Soc. Environ. 2011, 15, 611–622. [Google Scholar]
- Janaćković, P.; Rajčević, N.; Gavrilović, M.; Novaković, J.; Giweli, A.; Stešević, D.; Marin, P.D. Essential Oil Composition of Five Artemisia (Compositae) Species in Regards to Chemophenetics. Biochem. Syst. Ecol. 2019, 87, 103960. [Google Scholar] [CrossRef]
- De Magalhães, P.M.; Pereira, B.; Sartoratto, A. Yields of antimalarial artemisia Annua L. species. Acta Hortic. 2004, 629, 421–424. [Google Scholar] [CrossRef]
- Durden, K.; Sellars, S.; Cowell, B.; Brown, J.J.; Pszczolkowski, M.A. Artemisia Annua Extracts, Artemisinin and 1,8-Cineole, Prevent Fruit Infestation by a Major, Cosmopolitan Pest of Apples. Pharm. Biol. 2011, 49, 563–568. [Google Scholar] [CrossRef][Green Version]
- Santos, F.A.; Rao, V.S.N. Antiinflammatory and Antinociceptive Effects of 1,8-Cineole a Terpenoid Oxide Present in Many Plant Essential Oils. Phytother. Res. 2000, 14, 240–244. [Google Scholar] [CrossRef]
- Vilela, G.R.; de Almeida, G.S.; D’Arce, M.A.B.R.; Moraes, M.H.D.; Brito, J.O.; da Silva, M.F.d.G.F.; Silva, S.C.; de Stefano Piedade, S.M.; Calori-Domingues, M.A.; da Gloria, E.M. Activity of Essential Oil and Its Major Compound, 1,8-Cineole, from Eucalyptus Globulus Labill., against the Storage Fungi Aspergillus Flavus Link and Aspergillus Parasiticus Speare. J. Stored Prod. Res. 2009, 45, 108–111. [Google Scholar] [CrossRef]
- Murata, S.; Shiragami, R.; Kosugi, C.; Tezuka, T.; Yamazaki, M.; Hirano, A.; Yoshimura, Y.; Suzuki, M.; Shuto, K.; Ohkohchi, N.; et al. Antitumor Effect of 1, 8-Cineole against Colon Cancer. Oncol. Rep. 2013, 30, 2647–2652. [Google Scholar] [CrossRef]
- De Figuêiredo, F.R.; Monteiro, Á.B.; de Menezes, I.R.; dos Sales, V.S.; do Nascimento, E.; de Souza Rodrigues, C.; Bitu Primo, A.J.; da Cruz, L.; do Amaro, É.N.; de Araújo Delmondes, G.; et al. Effects of the Hyptis Martiusii Benth. Leaf Essential Oil and 1,8-Cineole (Eucalyptol) on the Central Nervous System of Mice. Food Chem. Toxicol. 2019, 133, 110802. [Google Scholar] [CrossRef]
- Sampath, S.; Subramani, S.; Janardhanam, S.; Subramani, P.; Yuvaraj, A.; Chellan, R. Bioactive Compound 1,8-Cineole Selectively Induces G2/M Arrest in A431 Cells through the Upregulation of the P53 Signaling Pathway and Molecular Docking Studies. Phytomedicine 2018, 46, 57–68. [Google Scholar] [CrossRef]
- Rodenak-Kladniew, B.; Castro, A.; Stärkel, P.; Galle, M.; Crespo, R. 1,8-Cineole Promotes G0/G1 Cell Cycle Arrest and Oxidative Stress-Induced Senescence in HepG2 Cells and Sensitizes Cells to Anti-Senescence Drugs. Life Sci. 2020, 243, 117271. [Google Scholar] [CrossRef]
- Yang, H.; Woo, J.; Pae, A.N.; Um, M.Y.; Cho, N.-C.; Park, K.D.; Yoon, M.; Kim, J.; Lee, C.J.; Cho, S. α-Pinene, a Major Constituent of Pine Tree Oils, Enhances Non-Rapid Eye Movement Sleep in Mice through GABAA-Benzodiazepine Receptors. Mol. Pharm. 2016, 90, 530–539. [Google Scholar] [CrossRef]
- Albuquerque, M.R.J.R.; Costa, S.M.O.; Bandeira, P.N.; Santiago, G.M.P.; Andrade-Neto, M.; Silveira, E.R.; Pessoa, O.D.L. Nematicidal and Larvicidal Activities of the Essential Oils from Aerial Parts of Pectis Oligocephala and Pectis Apodocephala Baker. An. Da Acad. Bras. De Ciências 2007, 79, 209–213. [Google Scholar] [CrossRef]
- Rivas da Silva, A.C.; Lopes, P.M.; Barros de Azevedo, M.M.; Costa, D.C.M.; Alviano, C.S.; Alviano, D.S. Biological Activities of α-Pinene and β-Pinene Enantiomers. Molecules 2012, 17, 6305–6316. [Google Scholar] [CrossRef]
- Kim, M.; Sowndhararajan, K.; Park, S.J.; Kim, S. Effect of Inhalation of Isomers, (+)-α-Pinene and (+)-β-Pinene on Human Electroencephalographic Activity According to Gender Difference. Eur. J. Integr. Med. 2018, 17, 33–39. [Google Scholar] [CrossRef]
- Benelli, G.; Govindarajan, M.; Rajeswary, M.; Vaseeharan, B.; Alyahya, S.A.; Alharbi, N.S.; Kadaikunnan, S.; Khaled, J.M.; Maggi, F. Insecticidal Activity of Camphene, Zerumbone and α-Humulene from Cheilocostus Speciosus Rhizome Essential Oil against the Old-World Bollworm, Helicoverpa Armigera. Ecotoxicol. Environ. Saf. 2018, 148, 781–786. [Google Scholar] [CrossRef] [PubMed]
- Okuniewski, M.; Paduszyński, K.; Domańska, U. Thermodynamic Study of Molecular Interactions in Eutectic Mixtures Containing Camphene. J. Phys. Chem. B 2016, 120, 12928–12936. [Google Scholar] [CrossRef] [PubMed]
- Wang, S.; Zhang, D.; Hu, J.; Jia, Q.; Xu, W.; Su, D.; Song, H.; Xu, Z.; Cui, J.; Zhou, M.; et al. A Clinical and Mechanistic Study of Topical Borneol-induced Analgesia. Embo Mol. Med. 2017, 9, 802–815. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.-Y.; Ryu, A.-R.; Jin, S.; Jeon, Y.-M.; Lee, M.-Y. Chlorin E6-Mediated Photodynamic Therapy Suppresses P. Acnes-Induced Inflammatory Response via NFκB and MAPKs Signaling Pathway. PLoS ONE 2017, 12, e0170599. [Google Scholar] [CrossRef]
- Ji, J.; Zhang, R.; Li, H.; Zhu, J.; Pan, Y.; Guo, Q. Analgesic and Anti-Inflammatory Effects and Mechanism of Action of Borneol on Photodynamic Therapy of Acne. Environ. Toxicol. Pharmacol. 2020, 75, 103329. [Google Scholar] [CrossRef]
- Ge, Y.; Wang, Z.; Xiong, Y.; Huang, X.; Mei, Z.; Hong, Z. Anti-Inflammatory and Blood Stasis Activities of Essential Oil Extracted from Artemisia Argyi Leaf in Animals. J. Nat. Med. 2016, 70, 531–538. [Google Scholar] [CrossRef]
- Chen, X.; Lin, Z.; Liu, A.; Ye, J.; Luo, Y.; Luo, Y.; Mao, X.; Liu, P.; Pi, R. The Orally Combined Neuroprotective Effects of Sodium Ferulate and Borneol against Transient Global Ischaemia in C57 BL/6J Mice. J. Pharm. Pharmacol. 2010, 62, 915–923. [Google Scholar] [CrossRef]
- Ho, D.-D.; Lau, C.-P.; Ng, K.-H.; Kong, Y.-C.; Cheng, K.-F.; Chan, K.-P. Anti-Implantation Activity of S(−)- and R(+)-Camphor-Yuehchukene in Rats. Eur. J. Pharmacol. 1991, 205, 209–212. [Google Scholar] [CrossRef]
- Ng, P.C.; Ho, D.D.; Ng, K.H.; Kong, Y.C.; Cheng, K.F.; Stone, G. Mixed Estrogenic and Anti-Estrogenic Activities of Yuehchukene--a Bis-Indole Alkaloid. Eur. J. Pharmacol. 1994, 264, 1–12. [Google Scholar] [CrossRef]
- Chatterjie, N.; Alexander, G.J. Anticonvulsant Properties of Spirohydantoins Derived from Optical Isomers of Camphor. Neurochem. Res. 1986, 11, 1669–1676. [Google Scholar] [CrossRef] [PubMed]
- Laude, E.A.; Morice, A.H.; Grattan, T.J. The Antitussive Effects of Menthol, Camphor and Cineole in Conscious Guinea-Pigs. Pulm. Pharmacol. 1994, 7, 179–184. [Google Scholar] [CrossRef]
- Tinwell, H.; Lefevre Paul, A.; Moffat Graeme, J.; Burns, A.; Odum, J.; Spurway, T.D.; Orphanides, G.; Ashby, J. Confirmation of Uterotrophic Activity of 3-(4-Methylbenzylidine)Camphor in the Immature Rat. Environ. Health Perspect. 2002, 110, 533–536. [Google Scholar] [CrossRef]
- Park, T.J.; Seo, H.K.; Kang, B.J.; Kim, K.T. Noncompetitive Inhibition by Camphor of Nicotinic Acetylcholine Receptors. Biochem. Pharmacol. 2001, 61, 787–793. [Google Scholar] [CrossRef]
- Schlumpf, M.; Cotton, B.; Conscience, M.; Haller, V.; Steinmann, B.; Lichtensteiger, W. In Vitro and in Vivo Estrogenicity of UV Screens. Environ. Health Perspect 2001, 109, 239–244. [Google Scholar] [CrossRef] [PubMed]
- Holbech, H.; Nørum, U.; Korsgaard, B.; Poul, B. The Chemical UV-Filter 3-Benzylidene Camphor Causes an Oestrogenic Effect in an in Vivo Fish Assay. Pharmacol. Toxicol. 2002, 91, 204–208. [Google Scholar] [CrossRef]
- Mueller, S.O.; Kling, M.; Arifin Firzani, P.; Mecky, A.; Duranti, E.; Shields-Botella, J.; Delansorne, R.; Broschard, T.; Kramer, P.-J. Activation of Estrogen Receptor α and ERβ by 4-Methylbenzylidene-Camphor in Human and Rat Cells: Comparison with Phyto- and Xenoestrogens. Toxicol. Lett. 2003, 142, 89–101. [Google Scholar] [CrossRef]
- Arakaki, N.; Shimoji, Y.; Wakamura, S. Camphor: An Attractant for the Cupreous Polished Chafer, Protaetia Pryeri Pryeri (Janson) (Coleoptera: Scarabaeidae). Appl. Entomol. Zool. 2009, 44, 621–625. [Google Scholar] [CrossRef][Green Version]
- Zhao, M.; Du, J. Anti-Inflammatory and Protective Effects of D-Carvone on Lipopolysaccharide (LPS)-Induced Acute Lung Injury in Mice. J. King Saud Univ.-Sci. 2020, 32, 1592–1596. [Google Scholar] [CrossRef]
- Vinothkumar, R.; Sudha, M.; Viswanathan, P.; Kabalimoorthy, J.; Balasubramanian, T.; Nalini, N. Modulating Effect of D-Carvone on 1,2-Dimethylhydrazine-Induced Pre-Neoplastic Lesions, Oxidative Stress and Biotransforming Enzymes, in an Experimental Model of Rat Colon Carcinogenesis. Cell Prolif. 2013, 46, 705–720. [Google Scholar] [CrossRef]
- Moro, I.J.; Gondo, G.D.G.A.; Pierri, E.G.; Pietro, R.C.L.R.; Soares, C.P.; de Sousa, D.P.; Santos, A.G. Evaluation of Antimicrobial, Cytotoxic and Chemopreventive Activities of Carvone and Its Derivatives. Braz. J. Pharm. Sci. 2017, 53. [Google Scholar] [CrossRef]
- De Cássia da Silveira e Sá, R.; Andrade, L.N.; de Sousa, D.P. A Review on Anti-Inflammatory Activity of Monoterpenes. Molecules 2013, 18, 1227–1254. [Google Scholar] [CrossRef] [PubMed]
- Bier, M.C.J.; Medeiros, A.B.P.; De Kimpe, N.; Soccol, C.R. Evaluation of Antioxidant Activity of the Fermented Product from the Biotransformation of R-(+)-Limonene in Solid-State Fermentation of Orange Waste by Diaporthe Sp. Biotechnol. Res. Innov. 2019, 3, 168–176. [Google Scholar] [CrossRef]
- Bacanlı, M.; Başaran, A.A.; Başaran, N. The Antioxidant and Antigenotoxic Properties of Citrus Phenolics Limonene and Naringin. Food Chem. Toxicol. 2015, 81, 160–170. [Google Scholar] [CrossRef] [PubMed]
- Chidambara Murthy, K.N.; Jayaprakasha, G.K.; Patil, B.S. D-Limonene Rich Volatile Oil from Blood Oranges Inhibits Angiogenesis, Metastasis and Cell Death in Human Colon Cancer Cells. Life Sci. 2012, 91, 429–439. [Google Scholar] [CrossRef]
- Quiroga, P.R.; Nepote, V.; Baumgartner, M.T. Contribution of Organic Acids to α-Terpinene Antioxidant Activity. Food Chem. 2019, 277, 267–272. [Google Scholar] [CrossRef]
- Bejeshk, M.A.; Samareh Fekri, M.; Najafipour, H.; Rostamzadeh, F.; Jafari, E.; Rajizadeh, M.A.; Masoumi-Ardakani, Y. Anti-Inflammatory and Anti-Remodeling Effects of Myrtenol in the Lungs of Asthmatic Rats: Histopathological and Biochemical Findings. Allergol. Et Immunopathol. 2019, 47, 185–193. [Google Scholar] [CrossRef]
- Sepici, A.; Gürbüz, I.; Çevik, C.; Yesilada, E. Hypoglycaemic Effects of Myrtle Oil in Normal and Alloxan-Diabetic Rabbits. J. Ethnopharmacol. 2004, 93, 311–318. [Google Scholar] [CrossRef]
- Aleksic, V.; Knezevic, P. Antimicrobial and Antioxidative Activity of Extracts and Essential Oils of Myrtus Communis L. Microbiol. Res. 2014, 169, 240–254. [Google Scholar] [CrossRef]
- Clark, A.M. Natural Products as a Resource for New Drugs. Pharm. Res. 1996, 13, 1133–1144. [Google Scholar] [CrossRef]
- Fu, C.; Yu, P.; Wang, M.; Qiu, F. Phytochemical Analysis and Geographic Assessment of Flavonoids, Coumarins and Sesquiterpenes in Artemisia Annua L. Based on HPLC-DAD Quantification and LC-ESI-QTOF-MS/MS Confirmation. Food Chem. 2020, 312, 126070. [Google Scholar] [CrossRef]
- Dandan, Z.; Jianjiang, Z. Two Cytotoxic Sesquiterpenes from Hairy Root Cultures of Artemisia Annua L. Induced Apoptosis of Highly Metastatic Lung Carcinoma Cell Line 95-D. J. Biosci. Bioeng. 2009, 108, S24–S25. [Google Scholar] [CrossRef]
- Li, Y.; Wu, J.-M.; Shan, F.; Wu, G.-S.; Ding, J.; Xiao, D.; Han, J.-X.; Atassi, G.; Leonce, S.; Caignard, D.-H.; et al. Synthesis and Cytotoxicity of Dihydroartemisinin Ethers Containing Cyanoarylmethyl Group. Bioorg. Med. Chem. 2003, 11, 977–984. [Google Scholar] [CrossRef]
- Nam, W.; Tak, J.; Ryu, J.-K.; Jung, M.; Yook, J.-I.; Kim, H.-J.; Cha, I.-H. Effects of Artemisinin and Its Derivatives on Growth Inhibition and Apoptosis of Oral Cancer Cells. Head Neck 2007, 29, 335–340. [Google Scholar] [CrossRef] [PubMed]
- Zhai, D.-D.; Supaibulwatana, K.; Zhong, J.-J. Inhibition of Tumor Cell Proliferation and Induction of Apoptosis in Human Lung Carcinoma 95-D Cells by a New Sesquiterpene from Hairy Root Cultures of Artemisia Annua. Phytomedicine 2010, 17, 856–861. [Google Scholar] [CrossRef]
- Wang, X.; Zheng, B.; Ashraf, U.; Zhang, H.; Cao, C.; Li, Q.; Chen, Z.; Imran, M.; Chen, H.; Cao, S.; et al. Artemisinin Inhibits the Replication of Flaviviruses by Promoting the Type I Interferon Production. Antivir. Res. 2020. [Google Scholar] [CrossRef]
- Wong, Y.K.; Xu, C.; Kalesh, K.A.; He, Y.; Lin, Q.; Wong, W.S.F.; Shen, H.-M.; Wang, J. Artemisinin as an Anticancer Drug: Recent Advances in Target Profiling and Mechanisms of Action. Med. Res. Rev. 2017, 37, 1492–1517. [Google Scholar] [CrossRef] [PubMed]
- Idowu, A.O.; Bhattacharyya, S.; Gradus, S.; Oyibo, W.; George, Z.; Black, C.; Igietseme, J.; Azenabor, A.A. Plasmodium Falciparum Treated with Artemisinin-Based Combined Therapy Exhibits Enhanced Mutation, Heightened Cortisol and TNF-α Induction. Int. J. Med. Sci. 2018, 15, 1449–1457. [Google Scholar] [CrossRef]
- Wang, Y.; Wang, Y.; You, F.; Xue, J. Novel Use for Old Drugs: The Emerging Role of Artemisinin and Its Derivatives in Fibrosis. Pharmacol. Res. 2020. [Google Scholar] [CrossRef]
- Martino, E.; Tarantino, M.; Bergamini, M.; Castelluccio, V.; Coricello, A.; Falcicchio, M.; Lorusso, E.; Collina, S. Artemisinin and Its Derivatives; Ancient Tradition Inspiring the Latest Therapeutic Approaches against Malaria. Future Med. Chem. 2019, 11, 1443–1459. [Google Scholar] [CrossRef]
- Suberu, J.O.; Gorka, A.P.; Jacobs, L.; Roepe, P.D.; Sullivan, N.; Barker, G.C.; Lapkin, A.A. Anti-Plasmodial Polyvalent Interactions in Artemisia Annua L. Aqueous Extract--Possible Synergistic and Resistance Mechanisms. PLoS ONE 2013, 8, e80790. [Google Scholar] [CrossRef] [PubMed]
- Efferth, T.; Herrmann, F.; Tahrani, A.; Wink, M. Cytotoxic Activity of Secondary Metabolites Derived from Artemisia Annua L. towards Cancer Cells in Comparison to Its Designated Active Constituent Artemisinin. Phytomedicine 2011, 18, 959–969. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.X.; Yang, L.; Li, Y.J.; Zhang, D.; Chen, Y.; Kostecká, P.; Kmoníèková, E.; Zídek, Z. Effects of Sesquiterpene, Flavonoid and Coumarin Types of Compounds from Artemisia Annua L. on Production of Mediators of Angiogenesis. Pharmacol. Rep. 2013, 65, 410–420. [Google Scholar] [CrossRef]
- Sharma, G.; Kapoor, H.; Chopra, M.; Kumar, K.; Agrawal, V. Strong Larvicidal Potential of Artemisia Annua Leaf Extract against Malaria (Anopheles Stephensi Liston) and Dengue (Aedes Aegypti L.) Vectors and Bioassay-Driven Isolation of the Marker Compounds. Parasitol. Res. 2014, 113, 197–209. [Google Scholar] [CrossRef]
- Flobinus, A.; Taudon, N.; Desbordes, M.; Labrosse, B.; Simon, F.; Mazeron, M.-C.; Schnepf, N. Stability and Antiviral Activity against Human Cytomegalovirus of Artemisinin Derivatives. J. Antimicrob. Chemother. 2014, 69, 34–40. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.; Kim, M.-H.; Lee, J.-H.; Jung, E.; Yoo, E.-S.; Park, D. Artemisinic Acid Is a Regulator of Adipocyte Differentiation and C/EBP δ Expression. J. Cell Biochem. 2012, 113, 2488–2499. [Google Scholar] [CrossRef]
- Efferth, T. From Ancient Herb to Modern Drug: Artemisia Annua and Artemisinin for Cancer Therapy. Semin. Cancer Biol. 2017, 46, 65–83. [Google Scholar] [CrossRef]
- Weathers, P.J.; Arsenault, P.R.; Covello, P.S.; McMickle, A.; Teoh, K.H.; Reed, D.W. Artemisinin Production in Artemisia Annua: Studies in Planta and Results of a Novel Delivery Method for Treating Malaria and Other Neglected Diseases. Phytochem. Rev. 2011, 10, 173–183. [Google Scholar] [CrossRef]
- Ferreira, J.F.S.; Luthria, D.L.; Sasaki, T.; Heyerick, A. Flavonoids from Artemisia Annua L. as Antioxidants and Their Potential Synergism with Artemisinin against Malaria and Cancer. Molecules 2010, 15, 3135–3170. [Google Scholar] [CrossRef]
- Han, J.; Ye, M.; Qiao, X.; Xu, M.; Wang, B.; Guo, D.-A. Characterization of Phenolic Compounds in the Chinese Herbal Drug Artemisia Annua by Liquid Chromatography Coupled to Electrospray Ionization Mass Spectrometry. J. Pharm. Biomed. Anal. 2008, 47, 516–525. [Google Scholar] [CrossRef]
- Lai, J.-P.; Lim, Y.H.; Su, J.; Shen, H.-M.; Ong, C.N. Identification and Characterization of Major Flavonoids and Caffeoylquinic Acids in Three Compositae Plants by LC/DAD-APCI/MS. J. Chromatogr. B 2007, 848, 215–225. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, I.S.; Cavaco, T.; Brodelius, M. Phenolic Composition and Antioxidant Capacity of Six Artemisia Species. Ind. Crop. Prod. 2011, 33, 382–388. [Google Scholar] [CrossRef]
- Tsevegsuren, N.; Edrada, R.; Lin, W.; Ebel, R.; Torre, C.; Ortlepp, S.; Wray, V.; Proksch, P. Biologically Active Natural Products from Mongolian Medicinal Plants Scorzonera Divaricata and Scorzonera Pseudodivaricata. J. Nat. Prod. 2007, 70, 962–967. [Google Scholar] [CrossRef]
- Zidorn, C.; Petersen, B.O.; Udovičić, V.; Larsen, T.O.; Duus, J.Ø.; Rollinger, J.M.; Ongania, K.-H.; Ellmerer, E.P.; Stuppner, H. Podospermic Acid, 1,3,5-Tri-O-(7,8-Dihydrocaffeoyl)Quinic Acid from Podospermum Laciniatum (Asteraceae). Tetrahedron Lett. 2005, 46, 1291–1294. [Google Scholar] [CrossRef]
- Yang, Y.-J.; Liu, X.; Wu, H.-R.; He, X.-F.; Bi, Y.-R.; Zhu, Y.; Liu, Z.-L. Radical Scavenging Activity and Cytotoxicity of Active Quinic Acid Derivatives from Scorzonera Divaricata Roots. Food Chem. 2013, 138, 2057–2063. [Google Scholar] [CrossRef] [PubMed]
- Yazdi, S.E.; Prinsloo, G.; Heyman, H.M.; Oosthuizen, C.B.; Klimkait, T.; Meyer, J.J.M. Anti-HIV-1 Activity of Quinic Acid Isolated from Helichrysum Mimetes Using NMR-Based Metabolomics and Computational Analysis. S. Afr. J. Bot. 2019, 126, 328–339. [Google Scholar] [CrossRef]
- Zhang, J.-L.; Yan, R.-J.; Yu, N.; Zhang, X.; Chen, D.-J.; Wu, T.; Xin, J.-G. A New Caffeic Acid Tetramer from the Dracocephalum Moldavica L. Nat. Prod. Res. 2018, 32, 370–373. [Google Scholar] [CrossRef]
- Choi, H.G.; Tran, P.T.; Lee, J.-H.; Min, B.S.; Kim, J.A. Anti-Inflammatory Activity of Caffeic Acid Derivatives Isolated from the Roots of Salvia Miltiorrhiza Bunge. Arch. Pharm. Res. 2018, 41, 64–70. [Google Scholar] [CrossRef]
- Langland, J.; Jacobs, B.; Wagner, C.E.; Ruiz, G.; Cahill, T.M. Antiviral Activity of Metal Chelates of Caffeic Acid and Similar Compounds towards Herpes Simplex, VSV-Ebola Pseudotyped and Vaccinia Viruses. Antivir. Res. 2018, 160, 143–150. [Google Scholar] [CrossRef]
- Mishra, M.; Panta, R.; Miyares, M. Influence of Coffee and Its Components on Breast Cancer: A Review. Asian Pac. J. Trop. Dis. 2016, 6, 827–831. [Google Scholar] [CrossRef]
- Habtemariam, S. Protective Effects of Caffeic Acid and the Alzheimer’s Brain. Available online: http://www.eurekaselect.com/147781/article (accessed on 5 May 2020).
- Adisakwattana, S. Cinnamic Acid and Its Derivatives: Mechanisms for Prevention and Management of Diabetes and Its Complications. Nutrients 2017, 9, 163. [Google Scholar] [CrossRef] [PubMed]
- Murillo, A.G.; Fernandez, M.L. The Relevance of Dietary Polyphenols in Cardiovascular Protection. Curr. Pharm. Des. 2017, 23, 2444–2452. [Google Scholar] [CrossRef]
- Silva, T.; Oliveira, C.; Borges, F. Caffeic Acid Derivatives, Analogs and Applications: A Patent Review (2009–2013). Expert Opin. Ther. Pat. 2014, 24, 1257–1270. [Google Scholar] [CrossRef] [PubMed]
- Cao, Z.; Zhang, H.; Cai, X.; Fang, W.; Chai, D.; Wen, Y.; Chen, H.; Chu, F.; Zhang, Y. Luteolin Promotes Cell Apoptosis by Inducing Autophagy in Hepatocellular Carcinoma. Cell. Physiol. Biochem. 2017, 43, 1803–1812. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.; Tian, X.-H.; Yi, Y.-S.; Jiang, W.-S.; Zhou, Y.-J.; Cheng, W.-J. Luteolin-Induced Protection of H2O2-Induced Apoptosis in PC12 Cells and the Associated Pathway. Mol. Med. Rep. 2015, 12, 7699–7704. [Google Scholar] [CrossRef]
- Nunes, C.; Almeida, L.; Barbosa, R.M.; Laranjinha, J. Luteolin Suppresses the JAK/STAT Pathway in a Cellular Model of Intestinal Inflammation. Food Funct. 2017, 8, 387–396. [Google Scholar] [CrossRef] [PubMed]
- Yao, Z.-H.; Yao, X.-L.; Zhang, Y.; Zhang, S.-F.; Hu, J.-C. Luteolin Could Improve Cognitive Dysfunction by Inhibiting Neuroinflammation. Neurochem. Res. 2018, 43, 806–820. [Google Scholar] [CrossRef]
- Wei, B.; Lin, Q.; Ji, Y.-G.; Zhao, Y.-C.; Ding, L.-N.; Zhou, W.-J.; Zhang, L.-H.; Gao, C.-Y.; Zhao, W. Luteolin Ameliorates Rat Myocardial Ischaemia-Reperfusion Injury through Activation of Peroxiredoxin II. Br. J. Pharmacol. 2018, 175, 3315–3332. [Google Scholar] [CrossRef]
- Jang, C.H.; Moon, N.; Oh, J.; Kim, J.-S. Luteolin Shifts Oxaliplatin-Induced Cell Cycle Arrest at G0/G1 to Apoptosis in HCT116 Human Colorectal Carcinoma Cells. Nutrients 2019, 11, 770. [Google Scholar] [CrossRef]
- Lesjak, M.; Beara, I.; Simin, N.; Pintać, D.; Majkić, T.; Bekvalac, K.; Orčić, D.; Mimica-Dukić, N. Antioxidant and Anti-Inflammatory Activities of Quercetin and Its Derivatives. J. Funct. Foods 2018, 40, 68–75. [Google Scholar] [CrossRef]
- Duarte, J.; Pérez-Vizcaíno, F.; Zarzuelo, A.; Jiménez, J.; Tamargo, J. Vasodilator Effects of Quercetin in Isolated Rat Vascular Smooth Muscle. Eur. J. Pharmacol. 1993, 239. [Google Scholar] [CrossRef]
- Luna-Vázquez, F.J.; Ibarra-Alvarado, C.; Rojas-Molina, A.; Rojas-Molina, I.; Zavala-Sánchez, M.Á. Vasodilator Compounds Derived from Plants and Their Mechanisms of Action. Molecules 2013, 18, 5814–5857. [Google Scholar] [CrossRef]
- Li, Y.; Yao, J.; Han, C.; Yang, J.; Chaudhry, M.T.; Wang, S.; Liu, H.; Yin, Y. Quercetin, Inflammation and Immunity. Nutrients 2016, 8, 167. [Google Scholar] [CrossRef] [PubMed]
- Kashyap, D.; Mittal, S.; Sak, K.; Singhal, P.; Tuli, H.S. Molecular Mechanisms of Action of Quercetin in Cancer: Recent Advances. Tumor Biol. 2016, 37, 12927–12939. [Google Scholar] [CrossRef]
- Ezzati, M.; Yousefi, B.; Velaei, K.; Safa, A. A Review on Anti-Cancer Properties of Quercetin in Breast Cancer. Life Sci. 2020, 248, 117463. [Google Scholar] [CrossRef] [PubMed]
- Patel, R.V.; Mistry, B.M.; Shinde, S.K.; Syed, R.; Singh, V.; Shin, H.-S. Therapeutic Potential of Quercetin as a Cardiovascular Agent. Eur. J. Med. Chem. 2018, 155, 889–904. [Google Scholar] [CrossRef]
- Ferreira, C.G.T.; Campos, M.G.; Felix, D.M.; Santos, M.R.; de Carvalho, O.V.; Diaz, M.A.N.; Fietto, J.L.R.; Bressan, G.C.; Silva-Júnior, A.; de Almeida, M.R. Evaluation of the Antiviral Activities of Bacharis Dracunculifolia and Quercetin on Equid Herpesvirus 1 in a Murine Model. Res. Vet. Sci. 2018, 120, 70–77. [Google Scholar] [CrossRef]
- Ganeshpurkar, A.; Saluja, A.K. The Pharmacological Potential of Rutin. Saudi Pharm. J. 2017, 25, 149–164. [Google Scholar] [CrossRef]
- Suganya, S.N.; Sumathi, T. Effect of Rutin against a Mitochondrial Toxin, 3-Nitropropionicacid Induced Biochemical, Behavioral and Histological Alterations-a Pilot Study on Huntington’s Disease Model in Rats. Metab. Brain Dis. 2017, 32, 471–481. [Google Scholar] [CrossRef] [PubMed]
- Al-Dhabi, N.A.; Arasu, M.V.; Park, C.H.; Park, S.U. An Up-to-Date Review of Rutin and Its Biological and Pharmacological Activities. Excli. J. 2015, 14, 59–63. [Google Scholar] [CrossRef] [PubMed]
- Singh, M.; Kaur, M.; Silakari, O. Flavones: An Important Scaffold for Medicinal Chemistry. Eur. J. Med. Chem. 2014, 84, 206–239. [Google Scholar] [CrossRef] [PubMed]
- Kaur, P.; Shukla, S.; Gupta, S. Plant Flavonoid Apigenin Inactivates Akt to Trigger Apoptosis in Human Prostate Cancer: An in Vitro and in Vivo Study. Carcinogenesis 2008, 29, 2210–2217. [Google Scholar] [CrossRef]
- Bao, Y.-Y.; Zhou, S.-H.; Fan, J.; Wang, Q.-Y. Anticancer Mechanism of Apigenin and the Implications of GLUT-1 Expression in Head and Neck Cancers. Future Oncol. 2013, 9, 1353–1364. [Google Scholar] [CrossRef] [PubMed]
- Banerjee, K.; Mandal, M. Oxidative Stress Triggered by Naturally Occurring Flavone Apigenin Results in Senescence and Chemotherapeutic Effect in Human Colorectal Cancer Cells. Redox Biol. 2015, 5, 153–162. [Google Scholar] [CrossRef] [PubMed]
- Bian, M.; Zhang, Y.; Du, X.; Xu, J.; Cui, J.; Gu, J.; Zhu, W.; Zhang, T.; Chen, Y. Apigenin-7-Diglucuronide Protects Retinas against Bright Light-Induced Photoreceptor Degeneration through the Inhibition of Retinal Oxidative Stress and Inflammation. Brain Res. 2017, 1663, 141–150. [Google Scholar] [CrossRef]
- Shukla, S.; Gupta, S. Apigenin: A Promising Molecule for Cancer Prevention. Pharm Res. 2010, 27, 962–978. [Google Scholar] [CrossRef]
- Jamali-Raeufy, N.; Baluchnejadmojarad, T.; Roghani, M.; Keimasi, S.; Goudarzi, M. Isorhamnetin Exerts Neuroprotective Effects in STZ-Induced Diabetic Rats via Attenuation of Oxidative Stress, Inflammation and Apoptosis. J. Chem. Neuroanat. 2019, 102, 101709. [Google Scholar] [CrossRef]
- Yang, J.H.; Kim, S.C.; Shin, B.Y.; Jin, S.H.; Jo, M.J.; Jegal, K.H.; Kim, Y.W.; Lee, J.R.; Ku, S.K.; Cho, I.J.; et al. O-Methylated Flavonol Isorhamnetin Prevents Acute Inflammation through Blocking of NF-ΚB Activation. Food Chem. Toxicol. 2013, 59, 362–372. [Google Scholar] [CrossRef]
- Wu, Q.; Kroon, P.A.; Shao, H.; Needs, P.W.; Yang, X. Differential Effects of Quercetin and Two of Its Derivatives, Isorhamnetin and Isorhamnetin-3-Glucuronide, in Inhibiting the Proliferation of Human Breast-Cancer MCF-7 Cells. J. Agric. Food Chem. 2018, 66, 7181–7189. [Google Scholar] [CrossRef]
- Yang, J.H.; Shin, B.Y.; Han, J.Y.; Kim, M.G.; Wi, J.E.; Kim, Y.W.; Cho, I.J.; Kim, S.C.; Shin, S.M.; Ki, S.H. Isorhamnetin Protects against Oxidative Stress by Activating Nrf2 and Inducing the Expression of Its Target Genes. Toxicol. Appl. Pharmacol. 2014, 274, 293–301. [Google Scholar] [CrossRef]
- Lee, Y.S.; Lee, S.; Lee, H.S.; Kim, B.-K.; Ohuchi, K.; Shin, K.H. Inhibitory Effects of Isorhamnetin-3-O-Beta-D-Glucoside from Salicornia Herbacea on Rat Lens Aldose Reductase and Sorbitol Accumulation in Streptozotocin-Induced Diabetic Rat Tissues. Biol. Pharm. Bull. 2005, 28, 916–918. [Google Scholar] [CrossRef] [PubMed]
- Jamali-Raoufi, N.; Keimasi, S.; Baluchnejadmojarad, T. Isorhamnetin Mitigates Learning and Memory Disturbances in Streptozotocin-Induced Diabetic Rats. J. Basic Clin. Pathophysiol. 2018, 6, 37–42. [Google Scholar] [CrossRef]
- Yang, E.-J.; Kim, G.-S.; Jun, M.; Song, K.-S. Kaempferol Attenuates the Glutamate-Induced Oxidative Stress in Mouse-Derived Hippocampal Neuronal HT22 Cells. Food Funct. 2014, 5, 1395–1402. [Google Scholar] [CrossRef] [PubMed]
- Rajendran, P.; Rengarajan, T.; Nandakumar, N.; Palaniswami, R.; Nishigaki, Y.; Nishigaki, I. Kaempferol, a Potential Cytostatic and Cure for Inflammatory Disorders. Eur. J. Med. Chem. 2014, 86, 103–112. [Google Scholar] [CrossRef]
- Dang, Q.; Song, W.; Xu, D.; Ma, Y.; Li, F.; Zeng, J.; Zhu, G.; Wang, X.; Chang, L.S.; He, D.; et al. Kaempferol Suppresses Bladder Cancer Tumor Growth by Inhibiting Cell Proliferation and Inducing Apoptosis. Mol. Carcinog. 2015, 54, 831–840. [Google Scholar] [CrossRef] [PubMed]
- Sekiguchi, A.; Motegi, S.; Fujiwara, C.; Yamazaki, S.; Inoue, Y.; Uchiyama, A.; Akai, R.; Iwawaki, T.; Ishikawa, O. Inhibitory Effect of Kaempferol on Skin Fibrosis in Systemic Sclerosis by the Suppression of Oxidative Stress. J. Dermatol. Sci. 2019, 96, 8–17. [Google Scholar] [CrossRef] [PubMed]
- Sadasivam, K.; Kumaresan, R. Antioxidant Behavior of Mearnsetin and Myricetin Flavonoid Compounds—A DFT Study. Spectrochim. Acta Part A 2011, 79, 282–293. [Google Scholar] [CrossRef]
- De Souza, P.; Gasparotto, A.; Crestani, S.; Stefanello, M.É.A.; Marques, M.C.A.; da Silva-Santos, J.E.; Kassuya, C.A.L. Hypotensive Mechanism of the Extracts and Artemetin Isolated from Achillea Millefolium L. (Asteraceae) in Rats. Phytomedicine 2011, 18, 819–825. [Google Scholar] [CrossRef]
- Lee, D.; Kim, C.-E.; Park, S.-Y.; Kim, K.O.; Hiep, N.T.; Lee, D.; Jang, H.-J.; Lee, J.W.; Kang, K.S. Protective Effect of Artemisia Argyi and Its Flavonoid Constituents against Contrast-Induced Cytotoxicity by Iodixanol in LLC-PK1 Cells. Int. J. Mol. Sci. 2018, 19, 1387. [Google Scholar] [CrossRef]
- Hu, J.; Ma, W.; Li, N.; Wang, K.-J.; Hu, J.; Ma, W.; Li, N.; Wang, K.-J. Antioxidant and Anti-Inflammatory Flavonoids from the Flowers of Chuju, a Medical Cultivar of Chrysanthemum Morifolim Ramat. J. Mex. Chem. Soc. 2017, 61, 282–289. [Google Scholar] [CrossRef]
- Li, W.-X.; Cui, C.-B.; Cai, B.; Wang, H.-Y.; Yao, X.-S. Flavonoids from Vitex Trifolia L. Inhibit Cell Cycle Progression at G2/M Phase and Induce Apoptosis in Mammalian Cancer Cells. J. Asian Nat. Prod. Res. 2005, 7, 615–626. [Google Scholar] [CrossRef] [PubMed]
- Langa, E.; Pardo, J.I.; Giménez-Rota, C.; González-Coloma, A.; Hernáiz, M.J.; Mainar, A.M. Supercritical Anti-Solvent Fractionation of Artemisia Absinthium L. Conventional Extracts: Tracking Artemetin and Casticin. J. Supercrit. Fluids 2019, 151, 15–23. [Google Scholar] [CrossRef]
- Chan, E.W.C.; Wong, S.K.; Chan, H.T. Casticin from Vitex Species: A Short Review on Its Anticancer and Anti-Inflammatory Properties. J. Integr. Med. 2018, 16, 147–152. [Google Scholar] [CrossRef] [PubMed]
- Lee, H.; Jung, K.-H.; Lee, H.; Park, S.; Choi, W.; Bae, H. Casticin, an Active Compound Isolated from Vitex Fructus, Ameliorates the Cigarette Smoke-Induced Acute Lung Inflammatory Response in a Murine Model. Int. Immunopharmacol. 2015, 28, 1097–1101. [Google Scholar] [CrossRef] [PubMed]
- Liou, C.-J.; Len, W.-B.; Wu, S.-J.; Lin, C.-F.; Wu, X.-L.; Huang, W.-C. Casticin Inhibits COX-2 and INOS Expression via Suppression of NF-ΚB and MAPK Signaling in Lipopolysaccharide-Stimulated Mouse Macrophages. J. Ethnopharmacol. 2014, 158, 310–316. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Q.-C.; Wang, Y.; Liu, Y.-P.; Zhang, R.-Q.; Li, X.; Su, W.-H.; Long, F.; Luo, X.-D.; Peng, T. Inhibition of Enterovirus 71 Replication by Chrysosplenetin and Penduletin. Eur. J. Pharm. Sci. 2011, 44, 392–398. [Google Scholar] [CrossRef]
- Messaili, S.; Colas, C.; Fougère, L.; Destandau, E. Combination of Molecular Network and Centrifugal Partition Chromatography Fractionation for Targeting and Identifying Artemisia Annua L. Antioxidant Compounds. J. Chromatogr. A 2020, 1615, 460785. [Google Scholar] [CrossRef] [PubMed]
- Yin, Y.; Gong, F.-Y.; Wu, X.-X.; Sun, Y.; Li, Y.-H.; Chen, T.; Xu, Q. Anti-Inflammatory and Immunosuppressive Effect of Flavones Isolated from Artemisia Vestita. J. Ethnopharmacol. 2008, 120. [Google Scholar] [CrossRef]
- Sheng, X.; Sun, Y.; Yin, Y.; Chen, T.; Xu, Q. Cirsilineol Inhibits Proliferation of Cancer Cells by Inducing Apoptosis via Mitochondrial Pathway. J. Pharm. Pharmacol. 2008, 60, 1523–1529. [Google Scholar] [CrossRef]
- Sun, Y.; Wu, X.-X.; Yin, Y.; Gong, F.-Y.; Shen, Y.; Cai, T.-T.; Zhou, X.-B.; Wu, X.-F.; Xu, Q. Novel Immunomodulatory Properties of Cirsilineol through Selective Inhibition of IFN-γ Signaling in a Murine Model of Inflammatory Bowel Disease. Biochem. Pharmacol. 2010, 79, 229–238. [Google Scholar] [CrossRef] [PubMed]
- Tezuka, Y.; Stampoulis, P.; Banskota, A.H.; Awale, S.; Tran, K.Q.; Saiki, I.; Kadota, S. Constituents of the Vietnamese Medicinal Plant Orthosiphon Stamineus. Chem. Pharm. Bull. 2000, 48, 1711–1719. [Google Scholar] [CrossRef]
- Nagao, T.; Abe, F.; Kinjo, J.; Okabe, H. Antiproliferative Constituents in Plants 10. Flavones from the Leaves of Lantana Montevidensis Briq. and Consideration of Structure-Activity Relationship. Biol. Pharm. Bull. 2002, 25, 875–879. [Google Scholar] [CrossRef]
- Androutsopoulos, V.; Arroo, R.R.J.; Hall, J.F.; Surichan, S.; Potter, G.A. Antiproliferative and Cytostatic Effects of the Natural Product Eupatorin on MDA-MB-468 Human Breast Cancer Cells Due to CYP1-Mediated Metabolism. Breast Cancer Res. 2008, 10, R39. [Google Scholar] [CrossRef]
- Chen, Z.; Liao, L.; Zhang, Z.; Wu, L.; Wang, Z. Comparison of Active Constituents, Acute Toxicity, Anti-Nociceptive and Anti-Inflammatory Activities of Porana Sinensis Hemsl., Erycibe Obtusifolia Benth. and Erycibe Schmidtii Craib. J. Ethnopharmacol. 2013, 150, 501–506. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.-J.; Jang, S.I.; Kim, Y.-J.; Chung, H.-T.; Yun, Y.-G.; Kang, T.-H.; Jeong, O.-S.; Kim, Y.-C. Scopoletin Suppresses Pro-Inflammatory Cytokines and PGE2 from LPS-Stimulated Cell Line, RAW 264.7 Cells. Fitoterapia 2004, 75, 261–266. [Google Scholar] [CrossRef]
- Pan, R.; Dai, Y.; Gao, X.; Xia, Y. Scopolin Isolated from Erycibe Obtusifolia Benth Stems Suppresses Adjuvant-Induced Rat Arthritis by Inhibiting Inflammation and Angiogenesis. Int. Immunopharmacol. 2009, 9, 859–869. [Google Scholar] [CrossRef] [PubMed]
- Shaw, C.-Y.; Chen, C.-H.; Hsu, C.-C.; Chen, C.-C.; Tsai, Y.-C. Antioxidant Properties of Scopoletin Isolated from Sinomonium Acutum. Phytother. Res. 2003, 17, 823–825. [Google Scholar] [CrossRef] [PubMed]
- Moon, P.-D.; Lee, B.-H.; Jeong, H.-J.; An, H.-J.; Park, S.-J.; Kim, H.-R.; Ko, S.-G.; Um, J.-Y.; Hong, S.-H.; Kim, H.-M. Use of Scopoletin to Inhibit the Production of Inflammatory Cytokines through Inhibition of the IκB/NF-ΚB Signal Cascade in the Human Mast Cell Line HMC-1. Eur. J. Pharmacol. 2007, 555, 218–225. [Google Scholar] [CrossRef]
- Thabet, A.A.; Youssef, F.S.; Korinek, M.; Chang, F.-R.; Wu, Y.-C.; Chen, B.-H.; El-Shazly, M.; Singab, A.N.B.; Hwang, T.-L. Study of the Anti-Allergic and Anti-Inflammatory Activity of Brachychiton Rupestris and Brachychiton Discolor Leaves (Malvaceae) Using in Vitro Models. BMC Complement. Altern. Med. 2018, 18, 299. [Google Scholar] [CrossRef]
- Iqbal, S.; Younas, U.; Chan, K.W.; Zia-Ul-Haq, M.; Ismail, M. Chemical Composition of Artemisia Annua L. Leaves and Antioxidant Potential of Extracts as a Function of Extraction Solvents. Molecules 2012, 17, 6020–6032. [Google Scholar] [CrossRef]
- Winkelman, M. Ethnobotanical Treatments of Diabetes in Baja California Norte. Med. Anthr. 1989, 11, 255–268. [Google Scholar] [CrossRef]
- Helal, E.G.E.; Abou-Aouf, N.; Khattab, A.L.M.; Zoair, M.A. Anti-Diabetic Effect of Artemisia Annua (Kaysom) in Alloxan-Induced Diabetic Rats. EJHM 2014, 57, 422–430. [Google Scholar] [CrossRef][Green Version]
- Woerdenbag, H.J.; Pras, N.; Bos, R.; Visser, J.F.; Hendriks, H.; Malingré, T.M. Analysis of Artemisinin and Related Sesquiterpenoids from Artemisia Annua L. by Combined Gas Chromatography/Mass Spectrometry. Phytochem. Anal. 1991, 2, 215–219. [Google Scholar] [CrossRef]
- Wang, H.; Ma, C.; Ma, L.; Du, Z.; Wang, H.; Ye, H.; Li, G.; Liu, B.; Xu, G. Secondary Metabolic Profiling and Artemisinin Biosynthesis of Two Genotypes of Artemisia Annua. Planta Med. 2009, 75, 1625–1633. [Google Scholar] [CrossRef] [PubMed]
- Taleghani, A.; Emami, S.A.; Tayarani-Najaran, Z. Artemisia: A Promising Plant for the Treatment of Cancer. Bioorg. Med. Chem. 2020, 28, 115180. [Google Scholar] [CrossRef]
- Huo, J.; Lu, Y.; Xia, L.; Chen, D. Structural Characterization and Anticomplement Activities of Three Acidic Homogeneous Polysaccharides from Artemisia Annua. J. Ethnopharmacol. 2020, 247, 112281. [Google Scholar] [CrossRef] [PubMed]
- Efferth, T.; Olbrich, A.; Bauer, R. MRNA Expression Profiles for the Response of Human Tumor Cell Lines to the Antimalarial Drugs Artesunate, Arteether, and Artemether. Biochem. Pharmacol. 2002, 64, 617–623. [Google Scholar] [CrossRef]
- Efferth, T.; Sauerbrey, A.; Olbrich, A.; Gebhart, E.; Rauch, P.; Weber, H.O.; Hengstler, J.G.; Halatsch, M.-E.; Volm, M.; Tew, K.D.; et al. Molecular Modes of Action of Artesunate in Tumor Cell Lines. Mol. Pharm. 2003, 64, 382–394. [Google Scholar] [CrossRef]
- Efferth, T.; Oesch, F. Oxidative Stress Response of Tumor Cells: Microarray-Based Comparison between Artemisinins and Anthracyclines. Biochem. Pharmacol. 2004, 68, 3–10. [Google Scholar] [CrossRef]
- Efferth, T.; Volm, M. Glutathione-Related Enzymes Contribute to Resistance of Tumor Cells and Low Toxicity in Normal Organs to Artesunate. Vivo 2005, 19, 225–232. [Google Scholar]
- Efferth, T.; Giaisi, M.; Merling, A.; Krammer, P.H.; Li-Weber, M. Artesunate Induces ROS-Mediated Apoptosis in Doxorubicin-Resistant T Leukemia Cells. PLoS ONE 2007, 2, e693. [Google Scholar] [CrossRef] [PubMed]
- Sieber, S.; Gdynia, G.; Roth, W.; Bonavida, B.; Efferth, T. Combination Treatment of Malignant B Cells Using the Anti-CD20 Antibody Rituximab and the Anti-Malarial Artesunate. Int. J. Oncol. 2009, 35, 149–158. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Ooko, E.; Saeed, M.E.M.; Kadioglu, O.; Sarvi, S.; Colak, M.; Elmasaoudi, K.; Janah, R.; Greten, H.J.; Efferth, T. Artemisinin Derivatives Induce Iron-Dependent Cell Death (Ferroptosis) in Tumor Cells. Phytomedicine 2015, 22, 1045–1054. [Google Scholar] [CrossRef]
- Lin, R.; Zhang, Z.; Chen, L.; Zhou, Y.; Zou, P.; Feng, C.; Wang, L.; Liang, G. Dihydroartemisinin (DHA) Induces Ferroptosis and Causes Cell Cycle Arrest in Head and Neck Carcinoma Cells. Cancer Lett. 2016, 381, 165–175. [Google Scholar] [CrossRef] [PubMed]
- Wojtkowiak-Giera, A.; Derda, M.; Kosik-Bogacka, D.; Kolasa-Wołosiuk, A.; Wandurska-Nowak, E.; Jagodziński, P.P.; Hadaś, E. The Modulatory Effect of Artemisia Annua L. on Toll-like Receptor Expression in Acanthamoeba Infected Mouse Lungs. Exp. Parasitol. 2019, 199, 24–29. [Google Scholar] [CrossRef]
- Yao, W.; Wang, F.; Wang, H. Immunomodulation of Artemisinin and Its Derivatives. Sci. Bull. 2016, 61, 1399–1406. [Google Scholar] [CrossRef]
- Wojtkowiak-Giera, A.; Derda, M.; Kosik-Bogacka, D.; Kolasa-Wołosiuk, A.; Solarczyk, P.; Cholewiński, M.; Wandurska-Nowak, E.; Jagodziński, P.P.; Hadaś, E. Influence of Artemisia Annua L. on Toll-like Receptor Expression in Brain of Mice Infected with Acanthamoeba Sp. Exp. Parasitol. 2018, 185, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Kawai, T.; Akira, S. The Roles of TLRs, RLRs and NLRs in Pathogen Recognition. Int. Immunol. 2009, 21, 317–337. [Google Scholar] [CrossRef]
- Cario, E.; Brown, D.; McKee, M.; Lynch-Devaney, K.; Gerken, G.; Podolsky, D.K. Commensal-Associated Molecular Patterns Induce Selective Toll-Like Receptor-Trafficking from Apical Membrane to Cytoplasmic Compartments in Polarized Intestinal Epithelium. Am. J. Pathol. 2002, 160, 165–173. [Google Scholar] [CrossRef]
- Li, B.; Li, J.; Pan, X.; Ding, G.; Cao, H.; Jiang, W.; Zheng, J.; Zhou, H. Artesunate Protects Sepsis Model Mice Challenged with Staphylococcus Aureus by Decreasing TNF-α Release via Inhibition TLR2 and Nod2 MRNA Expressions and Transcription Factor NF-ΚB Activation. Int. Immunopharmacol. 2010, 10, 344–350. [Google Scholar] [CrossRef]
- Huang, X.; Xie, Z.; Liu, F.; Han, C.; Zhang, D.; Wang, D.; Bao, X.; Sun, J.; Wen, C.; Fan, Y. Dihydroartemisinin Inhibits Activation of the Toll-like Receptor 4 Signaling Pathway and Production of Type I Interferon in Spleen Cells from Lupus-Prone MRL/Lpr Mice. Int. Immunopharmacol. 2014, 22, 266–272. [Google Scholar] [CrossRef] [PubMed]
- Cuzzocrea, S.; Saadat, F.; Paola, R.D.; Mirshafiey, A. Artemether: A New Therapeutic Strategy in Experimental Rheumatoid Arthritis. Immunopharmacol. Immunotoxicol. 2005, 27, 615–630. [Google Scholar] [CrossRef] [PubMed]
- Mirshafiey, A.; Saadat, F.; Attar, M.; Paola, R.D.; Sedaghat, R.; Cuzzocrea, S. Design of a New Line in Treatment of Experimental Rheumatoid Arthritis by Artesunate. Immunopharmacol. Immunotoxicol. 2006, 28, 397–410. [Google Scholar] [CrossRef] [PubMed]
- Wang, J.-X.; Tang, W.; Zhou, R.; Wan, J.; Shi, L.-P.; Zhang, Y.; Yang, Y.-F.; Li, Y.; Zuo, J.-P. The New Water-Soluble Artemisinin Derivative SM905 Ameliorates Collagen-Induced Arthritis by Suppression of Inflammatory and Th17 Responses. Br. J. Pharmacol. 2008, 153, 1303–1310. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Wang, S.; Wang, Y.; Zhou, C.; Chen, G.; Shen, W.; Li, C.; Lin, W.; Lin, S.; Huang, H.; et al. Inhibitory Effect of the Antimalarial Agent Artesunate on Collagen-Induced Arthritis in Rats through Nuclear Factor Kappa B and Mitogen-Activated Protein Kinase Signaling Pathway. Transl. Res. 2013, 161, 89–98. [Google Scholar] [CrossRef]
- Xu, H.; He, Y.; Yang, X.; Liang, L.; Zhan, Z.; Ye, Y.; Yang, X.; Lian, F.; Sun, L. Anti-Malarial Agent Artesunate Inhibits TNF-α-Induced Production of Proinflammatory Cytokines via Inhibition of NF-ΚB and PI3 Kinase/Akt Signal Pathway in Human Rheumatoid Arthritis Fibroblast-like Synoviocytes. Rheumatol. Oxf. 2007, 46, 920–926. [Google Scholar] [CrossRef]
- He, Y.; Fan, J.; Lin, H.; Yang, X.; Ye, Y.; Liang, L.; Zhan, Z.; Dong, X.; Sun, L.; Xu, H. The Anti-Malaria Agent Artesunate Inhibits Expression of Vascular Endothelial Growth Factor and Hypoxia-Inducible Factor-1α in Human Rheumatoid Arthritis Fibroblast-like Synoviocyte. Rheumatol. Int. 2011, 31, 53–60. [Google Scholar] [CrossRef] [PubMed]
- Jin, O.; Zhang, H.; Gu, Z.; Zhao, S.; Xu, T.; Zhou, K.; Jiang, B.; Wang, J.; Zeng, X.; Sun, L. A Pilot Study of the Therapeutic Efficacy and Mechanism of Artesunate in the MRL/Lpr Murine Model of Systemic Lupus Erythematosus. Cell. Mol. Immunol. 2009, 6, 461–467. [Google Scholar] [CrossRef] [PubMed]
- Hou, L.-F.; He, S.-J.; Li, X.; Wan, C.-P.; Yang, Y.; Zhang, X.-H.; He, P.-L.; Zhou, Y.; Zhu, F.-H.; Yang, Y.-F.; et al. SM934 Treated Lupus-Prone NZB×NZW F1 Mice by Enhancing Macrophage Interleukin-10 Production and Suppressing Pathogenic T Cell Development. PLoS ONE 2012, 7, e32424. [Google Scholar] [CrossRef] [PubMed]
- Hou, L.-F.; He, S.-J.; Li, X.; Yang, Y.; He, P.-L.; Zhou, Y.; Zhu, F.-H.; Yang, Y.-F.; Li, Y.; Tang, W.; et al. Oral Administration of Artemisinin Analog SM934 Ameliorates Lupus Syndromes in MRL/Lpr Mice by Inhibiting Th1 and Th17 Cell Responses. Arthritis Rheum. 2011, 63, 2445–2455. [Google Scholar] [CrossRef] [PubMed]
- Li, W.; Dong, Y.; Tu, Y.; Lin, Z. Dihydroarteannuin Ameliorates Lupus Symptom of BXSB Mice by Inhibiting Production of TNF-Alpha and Blocking the Signaling Pathway NF-Kappa B Translocation. Int. Immunopharmacol. 2006, 6, 1243–1250. [Google Scholar] [CrossRef]
- Wu, X.; Zhang, W.; Shi, X.; An, P.; Sun, W.; Wang, Z. Therapeutic Effect of Artemisinin on Lupus Nephritis Mice and Its Mechanisms. Acta Biochim. Biophys. Sin. 2010, 42, 916–923. [Google Scholar] [CrossRef] [PubMed]
- Wu, X.; Zhang, W.; Shi, X.; An, P.; Sun, W.; Qiao, C.; Wang, Z. Effect of Artemisinin Combined with Glucocorticoid on the Expressions of Glucocorticoid Receptor α MRNA, Glucocorticoid Receptor β MRNA and P300/CBP Protein in Lupus Nephritis Mice. Chin. J. Integr. Med. 2011, 17, 277–282. [Google Scholar] [CrossRef]
- Yang, Z.; Ding, J.; Yang, C.; Gao, Y.; Li, X.; Chen, X.; Peng, Y.; Fang, J.; Xiao, S. Immunomodulatory and Anti-Inflammatory Properties of Artesunate in Experimental Colitis. Curr. Med. Chem. 2012, 19, 4541–4551. [Google Scholar] [CrossRef] [PubMed]
- Li, T.; Chen, H.; Wei, N.; Mei, X.; Zhang, S.; Liu, D.; Gao, Y.; Bai, S.; Liu, X.; Zhou, Y. Anti-Inflammatory and Immunomodulatory Mechanisms of Artemisinin on Contact Hypersensitivity. Int. Immunopharmacol. 2012, 12, 144–150. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.; Ng, D.S.W.; Chan, T.K.; Guan, S.P.; Ho, W.E.; Koh, A.H.M.; Bian, J.S.; Lau, H.Y.A.; Wong, W.S.F. Anti-Allergic Action of Anti-Malarial Drug Artesunate in Experimental Mast Cell-Mediated Anaphylactic Models. Allergy 2013, 68, 195–203. [Google Scholar] [CrossRef] [PubMed]
- Cheng, C.; Ho, W.E.; Goh, F.Y.; Guan, S.P.; Kong, L.R.; Lai, W.-Q.; Leung, B.P.; Wong, W.S.F. Anti-Malarial Drug Artesunate Attenuates Experimental Allergic Asthma via Inhibition of the Phosphoinositide 3-Kinase/Akt Pathway. PLoS ONE 2011, 6, e20932. [Google Scholar] [CrossRef] [PubMed]
- Ho, W.E.; Cheng, C.; Peh, H.Y.; Xu, F.; Tannenbaum, S.R.; Ong, C.N.; Wong, W.S.F. Anti-Malarial Drug Artesunate Ameliorates Oxidative Lung Damage in Experimental Allergic Asthma. Free Radic. Biol. Med. 2012, 53, 498–507. [Google Scholar] [CrossRef]
- Dube, S.K.; Panda, P.S.; Agrawal, G.R.; Singh, D.K. Anaphylaxis to Artesunate? Indian J. Crit. Care Med. 2012, 16, 55–57. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Shi, J.-Q.; Zhang, C.-C.; Sun, X.-L.; Cheng, X.-X.; Wang, J.-B.; Zhang, Y.-D.; Xu, J.; Zou, H.-Q. Antimalarial Drug Artemisinin Extenuates Amyloidogenesis and Neuroinflammation in APPswe/PS1dE9 Transgenic Mice via Inhibition of Nuclear Factor-ΚB and NLRP3 Inflammasome Activation. Cns. Neurosci. Ther. 2013, 19, 262–268. [Google Scholar] [CrossRef]
- Wang, S.-J.; Sun, B.; Cheng, Z.-X.; Zhou, H.-X.; Gao, Y.; Kong, R.; Chen, H.; Jiang, H.-C.; Pan, S.-H.; Xue, D.-B.; et al. Dihydroartemisinin Inhibits Angiogenesis in Pancreatic Cancer by Targeting the NF-ΚB Pathway. Cancer Chemother. Pharm. 2011, 68, 1421–1430. [Google Scholar] [CrossRef]
- Bilia, A.R.; Santomauro, F.; Sacco, C.; Bergonzi, M.C.; Donato, R. Essential Oil of Artemisia Annua L.: An Extraordinary Component with Numerous Antimicrobial Properties. Evid. Based Complement. Altern. Med. 2014, 2014, 159819. [Google Scholar] [CrossRef]
- Stojanović, N.M.; Randjelović, P.J.; Mladenović, M.Z.; Ilić, I.R.; Petrović, V.; Stojiljković, N.; Ilić, S.; Radulović, N.S. Toxic Essential Oils, Part VI: Acute Oral Toxicity of Lemon Balm (Melissa Officinalis L.) Essential Oil in BALB/c Mice. Food Chem. Toxicol. 2019, 133, 110794. [Google Scholar] [CrossRef] [PubMed]
- Li, Y.; Hu, H.; Zheng, X.; Zhu, J.; Liu, L. Composition and Antimicrobial Activity of Essential Oil from the Aerial Part of Artemisia Annua. JMPR 2011, 5, 3629–3633. [Google Scholar]
- Juteau, F.; Masotti, V.; Bessière, J.M.; Dherbomez, M.; Viano, J. Antibacterial and Antioxidant Activities of Artemisia Annua Essential Oil. Fitoterapia 2002, 73, 532–535. [Google Scholar] [CrossRef]
- Verdian-rizi, M.R. Chemical Composition and Antimicrobial Activity of the Essential Oil of Artemisia Annua L. from Iran. Pharmacogn. Res. 2009, 1, 21. [Google Scholar]
- Massiha, A.; Khoshkholgh-Pahlaviani, M.M.; Issazadeh, K.; Bidarigh, S.; Zarrabi, S. Antibacterial Activity of Essential Oils and Plant Extracts of Artemisia (Artemisia Annua L.) in Vitro. Zahedan J. Res. Med. Sci. 2013, 15, 14–18. [Google Scholar]
- Viuda-Martos, M.; El Gendy, A.E.-N.G.S.; Sendra, E.; Fernández-López, J.; Abd El Razik, K.A.; Omer, E.A.; Pérez-Alvarez, J.A. Chemical Composition and Antioxidant and Anti-Listeria Activities of Essential Oils Obtained from Some Egyptian Plants. J. Agric. Food Chem. 2010, 58, 9063–9070. [Google Scholar] [CrossRef] [PubMed]
- Duarte, M.C.T.; Leme, E.E.; Delarmelina, C.; Soares, A.A.; Figueira, G.M.; Sartoratto, A. Activity of Essential Oils from Brazilian Medicinal Plants on Escherichia Coli. J. Ethnopharmacol. 2007, 111, 197–201. [Google Scholar] [CrossRef]
- Soylu, E.M.; Yiğitbaş, H.; Tok, F.M.; Soylu, S.; Kurt, Ş.; Baysal, Ö.; Kaya, A.D. Chemical Composition and Antifungal Activity of the Essential Oil of Artemisia Annua L. against Foliar and Soil-Borne Fungal Pathogens/Die Chemische Zusammensetzung Und Antimikrobielle Aktivität Das Ätherischen Öls von Artemisia Annua L. Gegen Blatt- Und Bodenbürtige Pilzliche Krankheitserreger. Z. Pflanzenkrankh. Pflanzenschutz/J. Plant Dis. Prot. 2005, 112, 229–239. [Google Scholar]
- Efferth, T. Beyond Malaria: The Inhibition of Viruses by Artemisinin-Type Compounds. Biotechnol. Adv. 2018, 36, 1730–1737. [Google Scholar] [CrossRef]
- Chang, Y.-S.; Woo, E.-R. Korean Medicinal Plants Inhibiting to Human Immunodeficiency Virus Type 1 (HIV-1) Fusion. Phytother. Res. 2003, 17, 426–429. [Google Scholar] [CrossRef]
- Oguariri, R.M.; Adelsberger, J.W.; Baseler, M.W.; Imamichi, T. Evaluation of the Effect of Pyrimethamine, an Anti-Malarial Drug, on HIV-1 Replication. Virus Res. 2010, 153, 269–276. [Google Scholar] [CrossRef]
- Jana, S.; Iram, S.; Thomas, J.; Hayat, M.Q.; Pannecouque, C.; Dehaen, W. Application of the Triazolization Reaction to Afford Dihydroartemisinin Derivatives with Anti-HIV Activity. Molecules 2017, 22, 303. [Google Scholar] [CrossRef]
- Efferth, T.; Marschall, M.; Wang, X.; Huong, S.-M.; Hauber, I.; Olbrich, A.; Kronschnabl, M.; Stamminger, T.; Huang, E.-S. Antiviral Activity of Artesunate towards Wild-Type, Recombinant, and Ganciclovir-Resistant Human Cytomegaloviruses. J. Mol. Med. 2002, 80, 233–242. [Google Scholar] [CrossRef]
- Efferth, T.; Romero, M.R.; Wolf, D.G.; Stamminger, T.; Marin, J.J.G.; Marschall, M. The Antiviral Activities of Artemisinin and Artesunate. Clin. Infect. Dis. 2008, 47, 804–811. [Google Scholar] [CrossRef]
- Milbradt, J.; Auerochs, S.; Korn, K.; Marschall, M. Sensitivity of Human Herpesvirus 6 and Other Human Herpesviruses to the Broad-Spectrum Antiinfective Drug Artesunate. J. Clin. Virol. 2009, 46, 24–28. [Google Scholar] [CrossRef]
- Arav-Boger, R.; He, R.; Chiou, C.-J.; Liu, J.; Woodard, L.; Rosenthal, A.; Jones-Brando, L.; Forman, M.; Posner, G. Artemisinin-Derived Dimers Have Greatly Improved Anti-Cytomegalovirus Activity Compared to Artemisinin Monomers. PLoS ONE 2010, 5, e10370. [Google Scholar] [CrossRef]
- He, R.; Mott, B.T.; Rosenthal, A.S.; Genna, D.T.; Posner, G.H.; Arav-Boger, R. An Artemisinin-Derived Dimer Has Highly Potent Anti-Cytomegalovirus (CMV) and Anti-Cancer Activities. PLoS ONE 2011, 6, e24334. [Google Scholar] [CrossRef]
- Reiter, C.; Fröhlich, T.; Zeino, M.; Marschall, M.; Bahsi, H.; Leidenberger, M.; Friedrich, O.; Kappes, B.; Hampel, F.; Efferth, T.; et al. New Efficient Artemisinin Derived Agents against Human Leukemia Cells, Human Cytomegalovirus and Plasmodium Falciparum: 2nd Generation 1,2,4-Trioxane-Ferrocene Hybrids. Eur. J. Med. Chem. 2015, 97, 164–172. [Google Scholar] [CrossRef]
- Hutterer, C.; Niemann, I.; Milbradt, J.; Fröhlich, T.; Reiter, C.; Kadioglu, O.; Bahsi, H.; Zeitträger, I.; Wagner, S.; Einsiedel, J.; et al. The Broad-Spectrum Antiinfective Drug Artesunate Interferes with the Canonical Nuclear Factor Kappa B (NF-ΚB) Pathway by Targeting RelA/P65. Antivir. Res. 2015, 124, 101–109. [Google Scholar] [CrossRef]
- Shapira, M.Y.; Resnick, I.B.; Chou, S.; Neumann, A.U.; Lurain, N.S.; Stamminger, T.; Caplan, O.; Saleh, N.; Efferth, T.; Marschall, M.; et al. Artesunate as a Potent Antiviral Agent in a Patient with Late Drug-Resistant Cytomegalovirus Infection after Hematopoietic Stem Cell Transplantation. Clin. Infect. Dis. 2008, 46, 1455–1457. [Google Scholar] [CrossRef] [PubMed]
- Naesens, L.; Bonnafous, P.; Agut, H.; De Clercq, E. Antiviral Activity of Diverse Classes of Broad-Acting Agents and Natural Compounds in HHV-6-Infected Lymphoblasts. J. Clin. Virol. 2006, 37, S69–S75. [Google Scholar] [CrossRef]
- Hakacova, N.; Klingel, K.; Kandolf, R.; Engdahl, E.; Fogdell-Hahn, A.; Higgins, T. First Therapeutic Use of Artesunate in Treatment of Human Herpesvirus 6B Myocarditis in a Child. J. Clin. Virol. 2013, 57, 157–160. [Google Scholar] [CrossRef]
- Qi, F.H.; Wang, Z.X.; Cai, P.P.; Zhao, L.; Gao, J.J.; Kokudo, N.; Li, A.Y.; Han, J.Q.; Tang, W. Traditional Chinese Medicine and Related Active Compounds: A Review of Their Role on Hepatitis B Virus Infection. Drug Discov. 2013, 7, 212–224. [Google Scholar] [CrossRef]
- Romero, M.R.; Efferth, T.; Serrano, M.A.; Castaño, B.; Macias, R.I.R.; Briz, O.; Marin, J.J.G. Effect of Artemisinin/Artesunate as Inhibitors of Hepatitis B Virus Production in an “in Vitro” Replicative System. Antivir. Res. 2005, 68, 75–83. [Google Scholar] [CrossRef] [PubMed]
- Batty, K.T.; Davis, T.M.E.; Thu, L.T.A.; Quang Binh, T.; Kim Anh, T.; Ilett, K.F. Selective High-Performance Liquid Chromatographic Determination of Artesunate and α- and β-Dihydroartemisinin in Patients with Falciparum Malaria. J. Chromatogr. B 1996, 677, 345–350. [Google Scholar] [CrossRef]
- Sharma, B.N.; Marschall, M.; Henriksen, S.; Rinaldo, C.H. Antiviral Effects of Artesunate on Polyomavirus BK Replication in Primary Human Kidney Cells. Antimicrob. Agents Chemother. 2013. [Google Scholar] [CrossRef]
- Sharma, B.N.; Marschall, M.; Rinaldo, C.H. Antiviral Effects of Artesunate on JC Polyomavirus Replication in COS-7 Cells. Antimicrob. Agents Chemother. 2014, 58, 6724–6734. [Google Scholar] [CrossRef]
- Disbrow, G.L.; Baege, A.C.; Kierpiec, K.A.; Yuan, H.; Centeno, J.A.; Thibodeaux, C.A.; Hartmann, D.; Schlegel, R. Dihydroartemisinin Is Cytotoxic to Papillomavirus-Expressing Epithelial Cells In Vitro and In Vivo. Cancer Res. 2005, 65, 10854–10861. [Google Scholar] [CrossRef]
- Mondal, A.; Chatterji, U. Artemisinin Represses Telomerase Subunits and Induces Apoptosis in HPV-39 Infected Human Cervical Cancer Cells. J. Cell. Biochem. 2015, 116, 1968–1981. [Google Scholar] [CrossRef] [PubMed]
- Paeshuyse, J.; Coelmont, L.; Vliegen, I.; hemel, J.V.; Vandenkerckhove, J.; Peys, E.; Sas, B.; Clercq, E.D.; Neyts, J. Hemin Potentiates the Anti-Hepatitis C Virus Activity of the Antimalarial Drug Artemisinin. Biochem. Biophys. Res. Commun. 2006, 348, 139–144. [Google Scholar] [CrossRef]
- Obeid, S.; Alen, J.; Nguyen, V.H.; Pham, V.C.; Meuleman, P.; Pannecouque, C.; Le, T.N.; Neyts, J.; Dehaen, W.; Paeshuyse, J. Artemisinin Analogues as Potent Inhibitors of In Vitro Hepatitis C Virus Replication. PLoS ONE 2013, 8, e81783. [Google Scholar] [CrossRef]
- Dai, R.; Xiao, X.; Peng, F.; Li, M.; Gong, G. Artesunate, an Anti-Malarial Drug, Has a Potential to Inhibit HCV Replication. Virus Genes 2016, 52, 22–28. [Google Scholar] [CrossRef]
- Romero, M.R.; Serrano, M.A.; Vallejo, M.; Efferth, T.; Alvarez, M.; Marin, J.J.G. Antiviral Effect of Artemisinin from Artemisia Annua against a Model Member of the Flaviviridae Family, the Bovine Viral Diarrhoea Virus (BVDV). Planta Med. 2006, 72, 1169–1174. [Google Scholar] [CrossRef]
- Blazquez, A.G.; Fernandez-Dolon, M.; Sanchez-Vicente, L.; Maestre, A.D.; Miguel, A.B.G.; Alvarez, M.l.; Serrano, M.A.; Jansen, H.; Efferth, T.; Marin, J.J.G.; et al. Novel Artemisinin Derivatives with Potential Usefulness against Liver/Colon Cancer and Viral Hepatitis. Bioorg. Med. Chem. 2013, 21, 4432–4441. [Google Scholar] [CrossRef] [PubMed]
- Thaha, M.; Pranawa, N.; Yogiantoro, M.; Tanimoto, M.; Tomino, Y. Acute Renal Failure in a Patient with Severe Malaria and Dengue Shock Syndrome. Clin. Nephrol. 2008, 70, 427–430. [Google Scholar] [CrossRef]
- Munyangi, J.; Cornet-Vernet, L.; Idumbo, M.; Lu, C.; Lutgen, P.; Perronne, C.; Ngombe, N.; Bianga, J.; Mupenda, B.; Lalukala, P.; et al. Artemisia Annua and Artemisia Afra Tea Infusions vs. Artesunate-Amodiaquine (ASAQ) in Treating Plasmodium Falciparum Malaria in a Large Scale, Double Blind, Randomized Clinical Trial. Phytomedicine 2019, 57, 49–56. [Google Scholar] [CrossRef]
- Hsu, E. Reflections on the ‘Discovery’ of the Antimalarial Qinghao. Br. J. Clin. Pharm. 2006, 61, 666–670. [Google Scholar] [CrossRef]
- White, N.J. Qinghaosu (Artemisinin): The Price of Success. Science 2008, 320, 330–334. [Google Scholar] [CrossRef]
- World Health Organization. Guidelines for the Treatment of Malaria; World Health Organization: Geneva, Switzerland, 2006. [Google Scholar]
- LoVerde, P.T. Digenetic Trematodes. In Schistosomiasis; Toledo, R., Fried, B., Eds.; Advances in Experimental Medicine and Biology; Springer International Publishing: Berlin/Heidelberg, Germany, 2019; pp. 45–70. [Google Scholar] [CrossRef]
- Steinmann, P.; Keiser, J.; Bos, R.; Tanner, M.; Utzinger, J. Schistosomiasis and Water Resources Development: Systematic Review, Meta-Analysis, and Estimates of People at Risk. Lancet Infect. Dis. 2006, 6, 411–425. [Google Scholar] [CrossRef]
- Saeed, M.E.M.; Krishna, S.; Greten, H.J.; Kremsner, P.G.; Efferth, T. Antischistosomal Activity of Artemisinin Derivatives in Vivo and in Patients. Pharmacol. Res. 2016, 110, 216–226. [Google Scholar] [CrossRef]
- Shalaby, H.A.; Abdel-Shafy, S.; Abdel-Rahman, K.A.; Derbala, A.A. Comparative in Vitro Effect of Artemether and Albendazole on Adult Toxocara Canis. Parasitol. Res. 2009, 105, 967–976. [Google Scholar] [CrossRef] [PubMed]
- Golenser, J.; Waknine, J.H.; Krugliak, M.; Hunt, N.H.; Ge, G. Current Perspectives on the Mechanism of Action of Artemisinins. Int. J. Parasitol. 2006, 36, 1427–1441. [Google Scholar] [CrossRef]
- Abou Rayia, D.M.; Saad, A.E.; Ashour, D.S.; Oreiby, R.M. Implication of Artemisinin Nematocidal Activity on Experimental Trichinellosis: In Vitro and in Vivo Studies. Parasitol. Int. 2017, 66, 56–63. [Google Scholar] [CrossRef] [PubMed]
- Kang, Y.-J.; Jo, J.-O.; Cho, M.-K.; Yu, H.-S.; Ock, M.S.; Cha, H.-J. Trichinella Spiralis Infection Induces Angiogenic Factor Thymosin Β4 Expression. Vet. Parasitol. 2011, 181, 222–228. [Google Scholar] [CrossRef] [PubMed]
- Echeverrigaray, S.; Zacaria, J.; Beltrão, R. Nematicidal Activity of Monoterpenoids Against the Root-Knot Nematode Meloidogyne Incognita. Phytopathology 2010, 100, 199–203. [Google Scholar] [CrossRef]
- Lam, N.S.; Long, X.; Su, X.-Z.; Lu, F. Artemisinin and Its Derivatives in Treating Helminthic Infections beyond Schistosomiasis. Pharmacol. Res. 2018, 133, 77–100. [Google Scholar] [CrossRef]
- Loo, C.S.N.; Lam, N.S.K.; Yu, D.; Su, X.-Z.; Lu, F. Artemisinin and Its Derivatives in Treating Protozoan Infections beyond Malaria. Pharmacol. Res. 2017, 117, 192–217. [Google Scholar] [CrossRef]
- Derda, M.; Hadaś, E.; Cholewiński, M.; Skrzypczak, Ł.; Grzondziel, A.; Wojtkowiak-Giera, A. Artemisia Annua L. as a Plant with Potential Use in the Treatment of Acanthamoebiasis. Parasitol. Res. 2016, 115, 1635–1639. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).