Partially Hydrolyzed Guar Gum Attenuates d-Galactose-Induced Oxidative Stress and Restores Gut Microbiota in Rats
Abstract
1. Introduction
2. Results
2.1. Changes in Aging Biomarkers and Antioxidant Activities
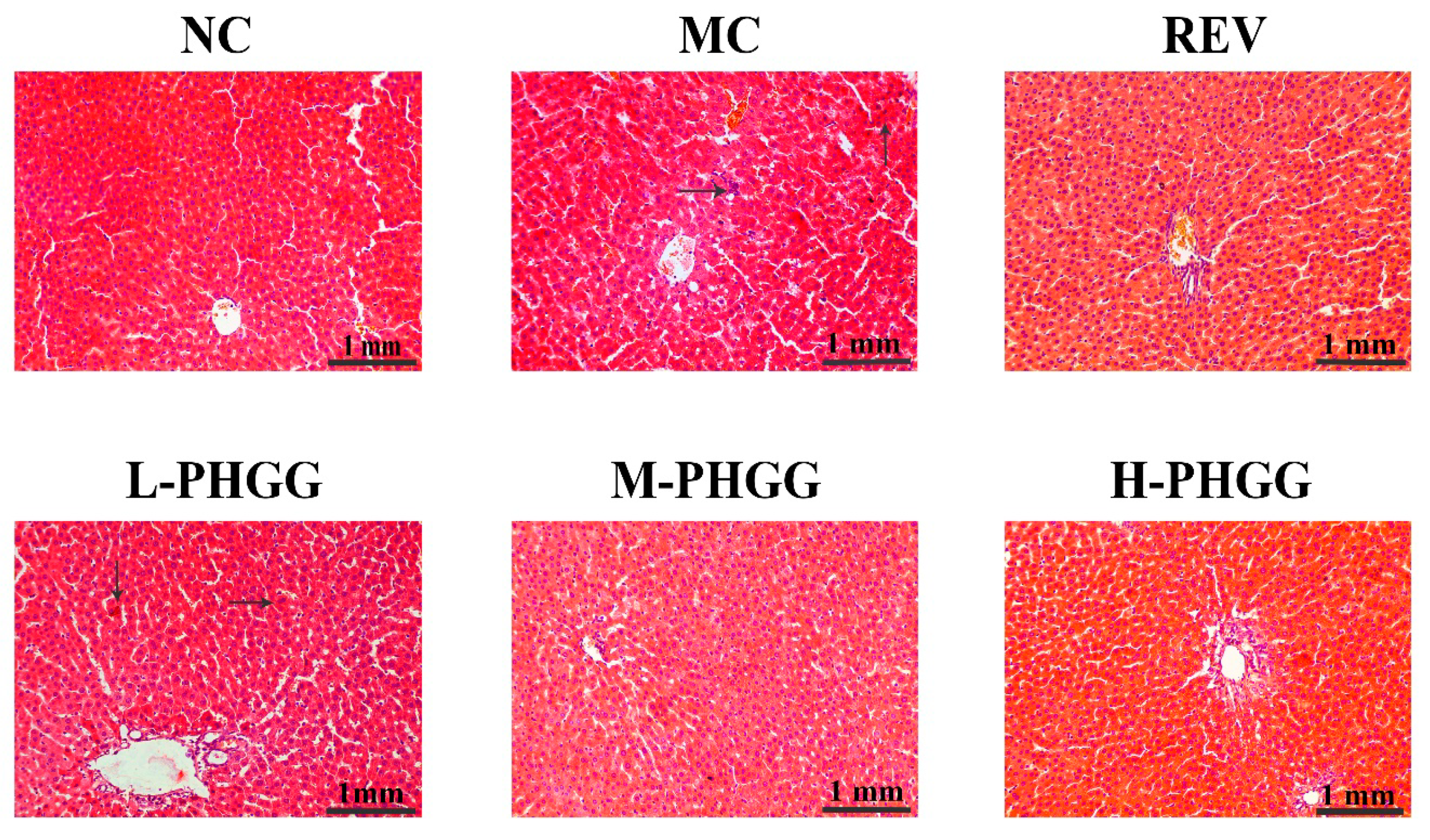
2.2. Histopathological Alterations
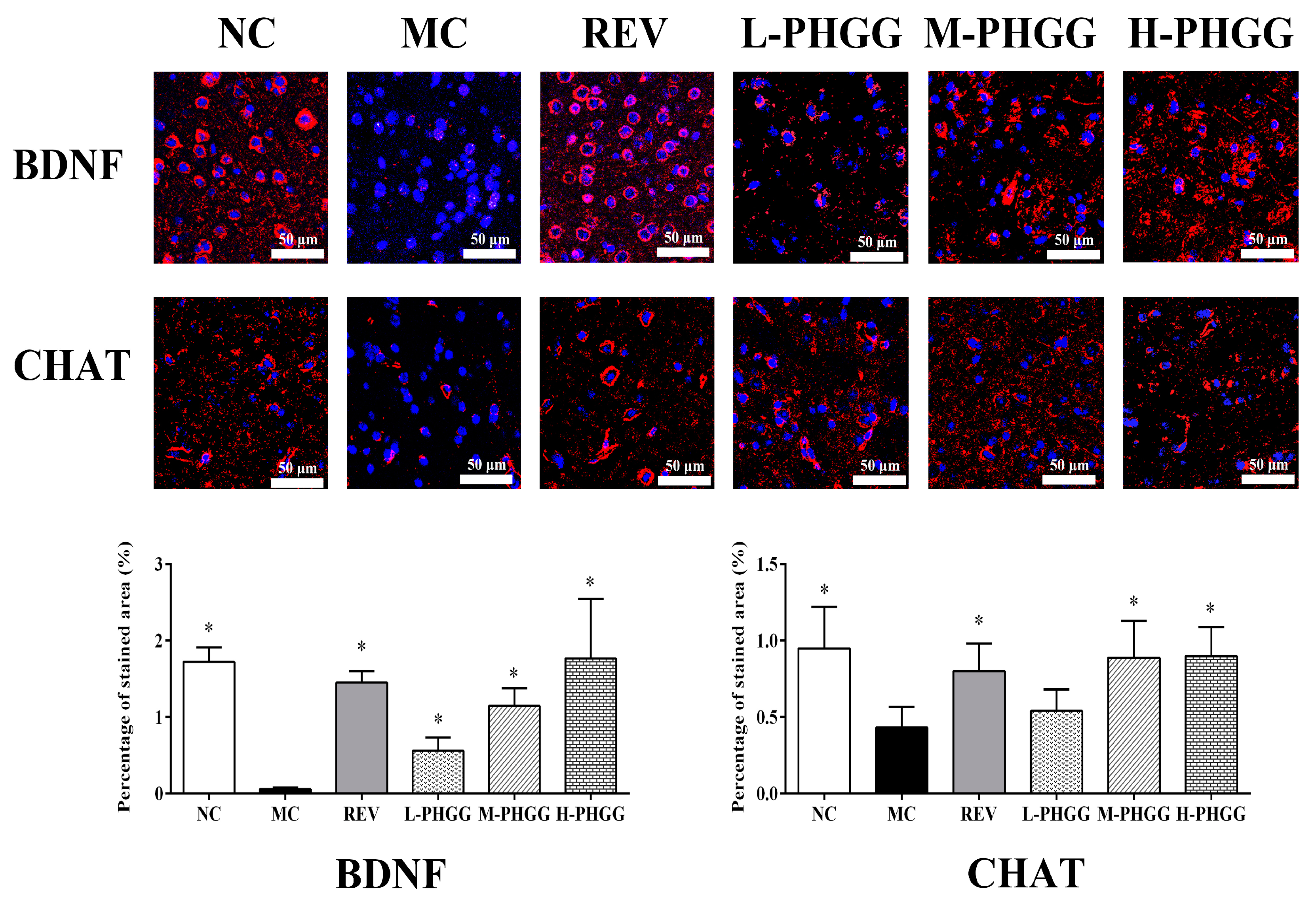
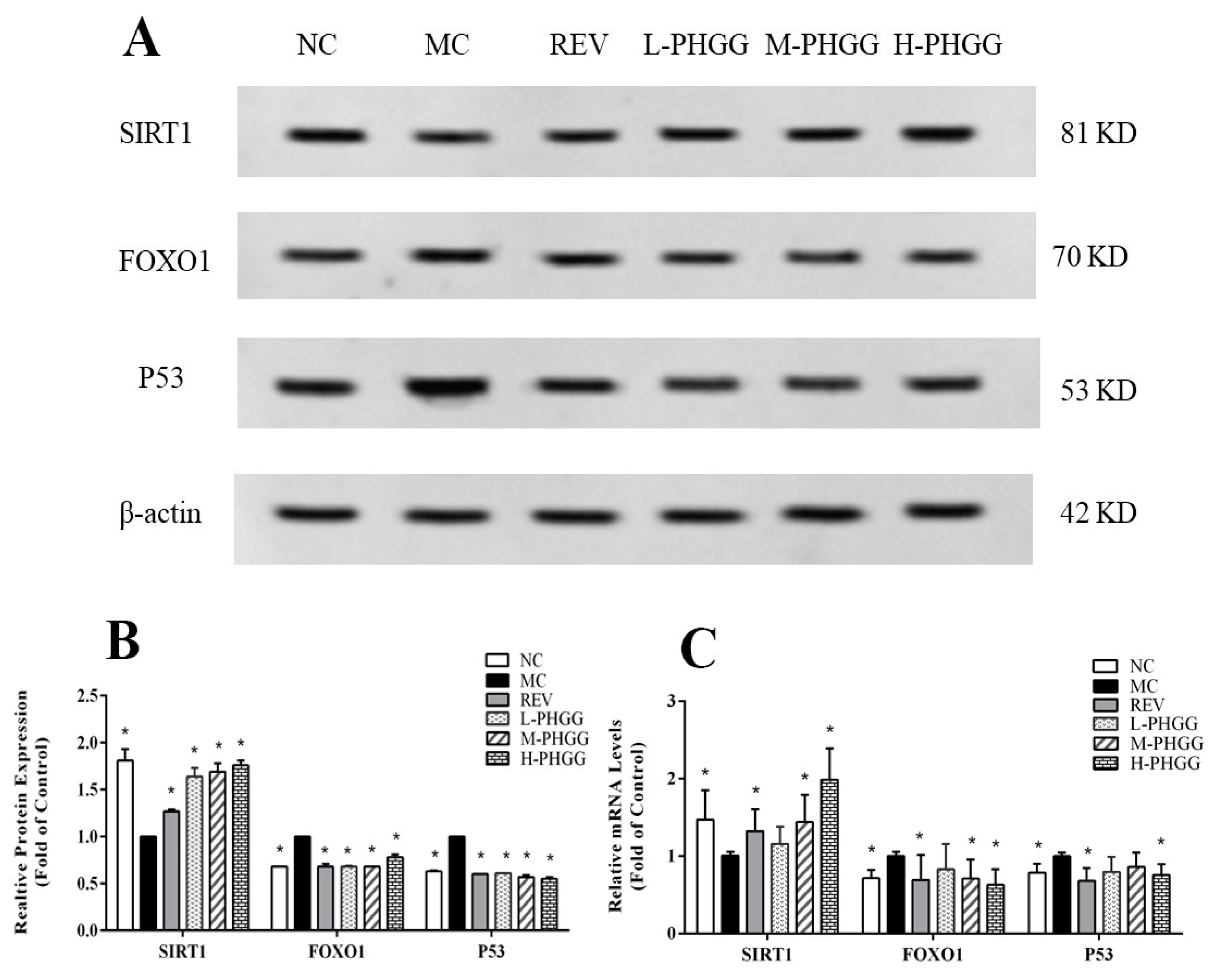
2.3. Changes in the Expression Levels of Aging Related Proteins and Genes
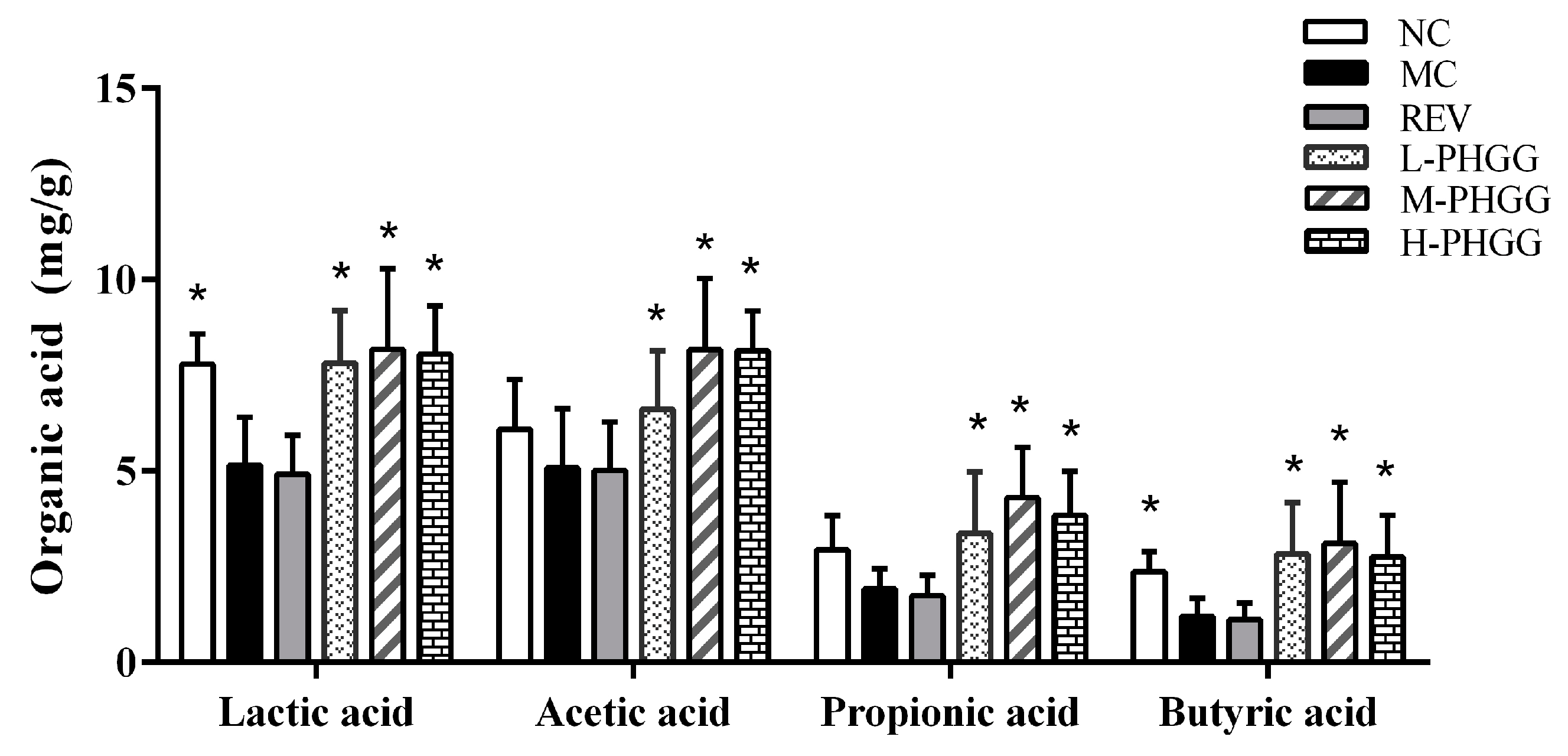
2.4. Changes in Organic Acids Concentration
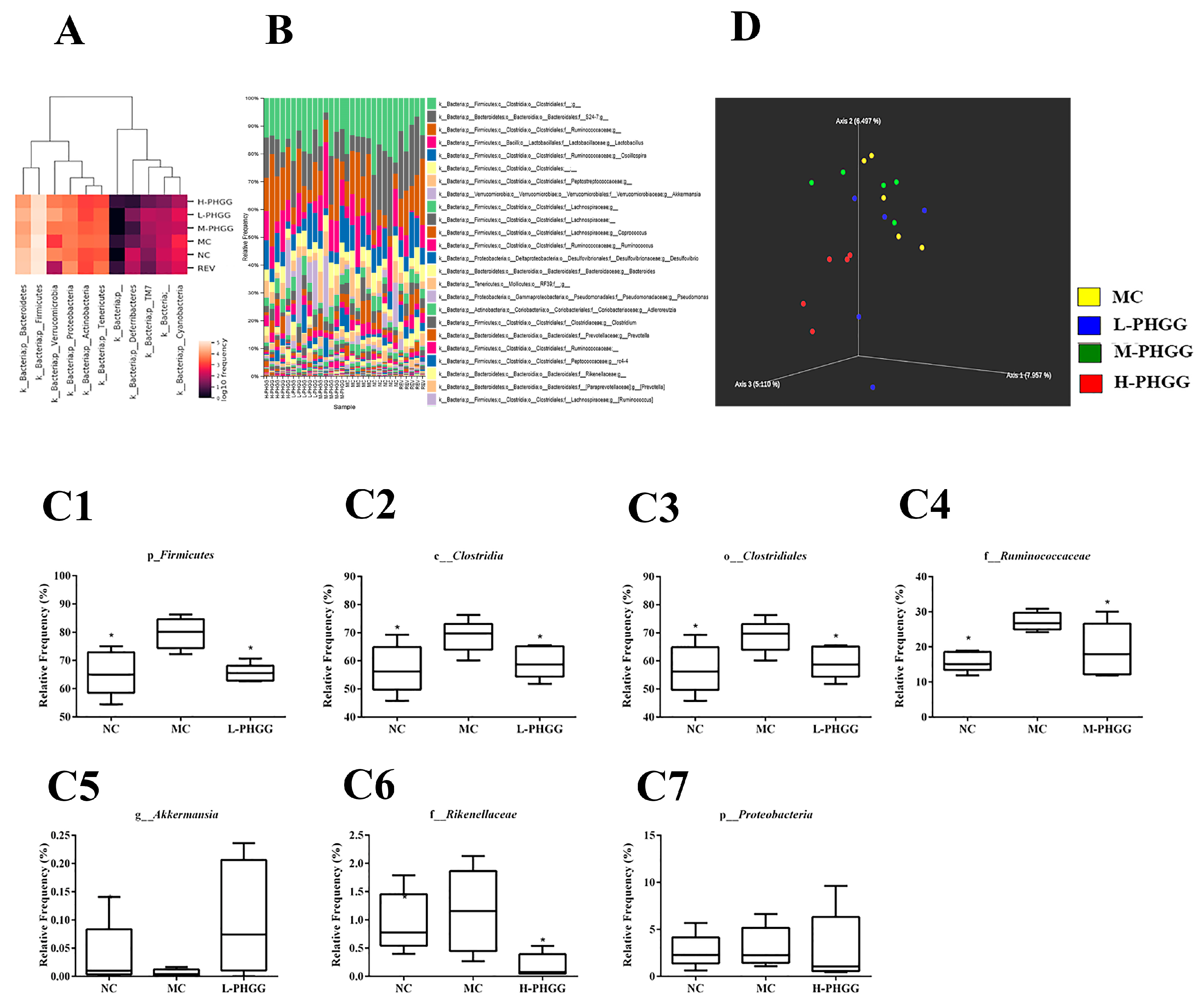
2.5. Changes in Gut Microbiota Composition
3. Discussion
4. Materials and Methods
4.1. Materials and Animals
4.2. Grouping and Drugs Administration
4.3. Measurement of Biochemical Indices
4.4. Histopathological Examination
4.5. Immunofluorescence Assay
4.6. Western blot analysis and Quantitative Real-Time PCR
4.7. Organic Acids Analysis
4.8. Intestinal Microbiota Analysis
4.9. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Sanada, Y.; Asai, S.; Ikemoto, A.; Moriwaki, T.; Nakamura, N.; Miyaji, M.; Zhang-Akiyama, Q.M. Oxidation resistance 1 is essential for protection against oxidative stress and participates in the regulation of aging in Caenorhabditis elegans. Free Radic. Res. 2014, 48, 919–928. [Google Scholar] [CrossRef] [PubMed]
- Garcia-Mesa, Y.; Colie, S.; Corpas, R.; Cristofol, R.; Comellas, F.; Nebreda, A.R.; Gimenez-Llort, L.; Sanfeliu, C. Oxidative stress is a central target for physical exercise neuroprotection against pathological brain aging. J. Gerontol. A Biol. Sci. Med. Sci. 2016, 71, 40–49. [Google Scholar] [CrossRef] [PubMed]
- Donato, A.J.; Eskurza, I.; Silver, A.E.; Levy, A.S.; Pierce, G.L.; Gates, P.E.; Seals, D.R. Direct evidence of endothelial oxidative stress with aging in humans. Relation to impaired endothelium-dependent dilation and upregulation of nuclear factor-κB. Circ. Res. 2007, 100, 1659–1666. [Google Scholar] [CrossRef] [PubMed]
- Harman, D. Aging: A theory based on free radical and radiation chemistry. J. Gerontol. 1956, 11, 298–300. [Google Scholar] [CrossRef] [PubMed]
- Kudryavtseva, A.V.; Krasnov, G.S.; Dmitriev, A.A.; Alekseev, B.Y.; Snezhkina, A.V. Mitochondrial dysfunction and oxidative stress in aging and cancer. Oncotarget 2016, 7, 44879–44905. [Google Scholar] [CrossRef] [PubMed]
- De Picciotto, N.E.; Gano, L.B.; Johnson, L.C.; Martens, C.R.; Sindler, A.L.; Mills, K.F.; Imail, S.; Seals, D.R. Nicotinamide mononucleotide supplementation reverses vascular dysfunction and oxidative stress with aging in mice. Aging Cell 2016, 15, 522–530. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.Q.; Unnikrishnan, A.; Deepa, S.S.; Liu, Y.H.; Li, Y.; Keno, Y.; Sosnowska, D.; Remmen, H.V.; Richardson, A. A new role for oxidative stress in aging: The accelerated aging phenotype in sod1−/−mice is correlated to increased cellular senescence. Redox Biol. 2017, 11, 30–37. [Google Scholar] [CrossRef] [PubMed]
- Aydin, A.F.; Coban, J.; Dogan-Ekici, I.; Betul-Kalaz, E.; Dogru-Abbasoglu, S.; Uysal, M. Carnosine and taurine treatments diminished brain oxidative stress and apoptosis in D-galactose aging model. Metab. Brain Dis. 2016, 31, 337–345. [Google Scholar] [CrossRef] [PubMed]
- Liao, C.H.; Chen, B.H.; Chiang, H.S.; Chen, C.W.; Chen, M.F.; Ke, C.C.; Wang, Y.Y.; Lin, W.N.; Wang, C.C.; Lin, Y.H. Optimizing a male reproductive aging mouse model by D-Galactose injection. Int. J. Mol. Sci. 2016, 17, 98. [Google Scholar] [CrossRef] [PubMed]
- Kundu, P.; Blacher, E.; Elinav, E.; Pettersson, S. Our gut microbiome: The evolving inner self. Cell 2017, 171, 1481–1493. [Google Scholar] [CrossRef] [PubMed]
- Hopkins, M.J.; Macfarlane, G.T. Changes in predominant bacterial populations in human faeces with age and with Clostridium difficile infection. J. Med. Microbiol. 2002, 51, 448–454. [Google Scholar] [CrossRef] [PubMed]
- Si, Y.; Liu, X.; Ye, K.; Bonfini, A.; Hu, X.Y.; Buchon, N.; Gu, Z. Glucomannan hydrolysate promotes gut proliferative homeostasis and extends life span in Drosophila melanogaster. J. Gerontol. A Biol. Sci. Med. Sci. 2019, 74, 1549–1556. [Google Scholar] [CrossRef] [PubMed]
- Collins, S.M.; Surette, M.; Bercik, P. The interplay between the intestinal microbiota and the brain. Nat. Rev. Microbiol. 2012, 10, 735–742. [Google Scholar] [CrossRef] [PubMed]
- Topping, D.L.; Clifton, P.M. Short-chain fatty acids and human colonic function: Roles of resistantstarch and nonstarch polysaccharides. Physiol. Rev. 2001, 81, 1031–1064. [Google Scholar] [CrossRef] [PubMed]
- Deepak, M.; Sheweta, B.; Bhupendar, S.K. Guar gum: Processing, properties and food applications—A Review. J. Food Sci. Technol. 2014, 51, 409–418. [Google Scholar]
- Li, Y.X.; Yi, P.; Wang, N.N.; Liu, J.; Liu, X.Q.; Yan, Q.J.; Jiang, Z.Q. High level expression of β-mannanase (RmMan5A) in Pichia pastoris for partially hydrolyzed guar gum production. Int. J. Biol. Macromol. 2017, 105, 1171–1179. [Google Scholar] [CrossRef]
- Ohashi, Y.; Sumitani, K.; Tokunaga, M.; Ishihara, N.; Okubo, T.; Fujisawa, T. Consumption of partially hydrolysed guar gum stimulates Bifidobacteria and butyrate-producing bacteria in the human large intestine. Benef. Microbes 2014, 6, 1–6. [Google Scholar] [CrossRef]
- Takagi, T.; Naito, Y.; Higashimura, Y.; Ushiroda, C.; Mizushima, K.; Ohashi, Y.; Yasukawa, Z.; Ozeki, M.; Tokunaga, M.; Okubo, T.; et al. Partially hydrolysed guar gum ameliorates murine intestinal inflammation in association with modulating luminal microbiota and SCFA. Br. J. Nutr. 2016, 116, 1–7. [Google Scholar] [CrossRef]
- Russo, L.; Andreozzi, P.; Zito, F.P.; Vozzella, L.; Savino, I.G.; Sarnelli, G.; Cuomo, R. Partially hydrolyzed guar gum in the treatment of irritable bowel syndrome with constipation: Effects of gender, age, and body mass index. Saudi J. Gastroenterol. 2015, 21, 104–110. [Google Scholar]
- Alam, N.H.; Ashraf, H.; Kamruzzaman, M.; Tahmeed, A.; Sufia, I.; Olesen, M.K.; Gyr, N.; Meier, R. Efficacy of partially hydrolyzed guar gum (PHGG) supplemented modified oral rehydration solution in the treatment of severely malnourished children with watery diarrhoea: A randomised double-blind controlled trial. J. Health Popul. Nutr. 2015, 34, 3–12. [Google Scholar] [CrossRef]
- Minekus, M.; Jelier, M.; Xiao, J.Z.; Kondo, S.; Iwatsuki, K.; Kokubo, S.; Bos, M.; Dunnewind, B.; Havenaar, R. Effect of partially hydrolyzed guar gum (PHGG) on the bioaccessibility of fat and cholesterol. Biosci. Biotechnol. Biochem. 2005, 69, 932–938. [Google Scholar] [CrossRef] [PubMed]
- Hung, T.V.; Suzuki, T. Dietary fermentable fibers attenuate chronic kidney disease in mice by protecting the intestinal barrier. J. Nutr. 2018, 148, 552–561. [Google Scholar] [CrossRef] [PubMed]
- Lin, Y.; Yao, J.; Chen, Y.; Pang, L.; Li, H.; Cao, Z.; You, K.; Dai, H.; Wu, R. Hippocampal neurochemical changes in senescent mice induced with chronic injection of D-galactose and NaNO2: An in vitro high-resolution NMR spectroscopy study at 9.4T. PLoS ONE 2014, 9, e88562. [Google Scholar] [CrossRef] [PubMed]
- Xu, S.; Bao, M.; Li, D.; Yong, M.L. Advanced glycation in D-galactose induced mouse aging model. Mech. Ageing Dev. 1999, 108, 239–251. [Google Scholar]
- Shi, Y.; Camici, G.G.; Lüscher, T.F. Cardiovascular determinants of life span. Pflüg. Arch. Eur. J. Physiol. 2010, 459, 315–324. [Google Scholar] [CrossRef] [PubMed]
- Parameshwaran, K.; Irwin, M.H.; Steliou, K.; Pinkert, C.A. D-galactose effectiveness in modeling aging and therapeutic antioxidant treatment in mice. Rejuvenation Res. 2010, 13, 729–735. [Google Scholar] [CrossRef] [PubMed]
- Levcik, D.; Nekovarova, T.; Stuchlik, A.; Klement, D. Rats use hippocampus to recognize positions of objects located in an inaccessible space. Hippocampus 2013, 23, 153–161. [Google Scholar] [CrossRef] [PubMed]
- Bordone, L.; Cohen, D.; Robinson, A.; Motta, M.C.; Van, V.E.; Czopik, A.; Steele, A.D.; Crowe, H.; Marmor, S.; Luo, J.; et al. SIRT1 transgenic mice show phenotypes resembling calorie restriction. Aging Cell 2007, 6, 759–767. [Google Scholar] [CrossRef] [PubMed]
- Brunet, A.; Sweeney, L.B.; Sturgill, J.F.; Chua, K.F.; Greer, P.L.; Lin, Y.; Tran, H.; Ross, S.E.; Mostoslavsky, R.; Cohen, H.Y.; et al. Stress-dependent regulation of FOXO transcription factors by the SIRT1 deacetylase. Science 2004, 303, 2011–2015. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.H.; Song, M.Y.; Song, E.K.; Kim, E.K.; Moon, W.S.; Han, M.K.; Park, J.W.; Kwon, K.B.; Park, B.H. Overexpression of SIRT1 protects pancreatic β-cells against cytokine toxicity by suppressing the nuclear factor-κB signaling pathway. Diabetes 2009, 58, 344–351. [Google Scholar] [CrossRef] [PubMed]
- Rufini, A.; Tucci, P.; Celardo, I.; Melino, G. Senescence and aging: The critical roles of p53. Oncogene 2013, 32, 5129–5143. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Wang, L.; Li, L.; Wang, Z.; Ho, Y.; McDonald, T.; Holyoake, T.L.; Chen, W.; Bhatia, R. Activation of p53 by SIRT1 inhibition enhances elimination of CML leukemia stem cells in combination with imatinib. Cancer Cell 2012, 21, 266–281. [Google Scholar] [CrossRef] [PubMed]
- Villalba, J.M.; Alcaín, F.J. Sirtuin activators and inhibitors. BioFactors 2012, 38, 349–359. [Google Scholar] [CrossRef] [PubMed]
- Baur, J.A.; Pearson, K.J.; Price, N.L.; Jamieson, H.A.; Lerin, C.; Kalra, A.; Prabhu, V.V.; Allard, J.S.; Lopez-Lluch, G.; Lewis, K.; et al. Resveratrol improves health and survival of mice on a high-calorie diet. Nature 2006, 444, 337–342. [Google Scholar] [CrossRef] [PubMed]
- Langille, M.G.; Meehan, C.J.; Koenig, J.E.; Dhanani, A.S.; Rose, R.A.; Howlett, S.E. Microbial shifts in the aging mouse gut. Microbiome 2014, 2, 50–62. [Google Scholar] [CrossRef] [PubMed]
- Rampelli, S.; Candela, M.; Turroni, S.; Biagi, E.; Collino, S.; Franceschi, C.; O’Toole, P.W.; Brigidi, P. Functional metagenomic profiling of intestinal microbiome in extreme ageing. Aging 2013, 5, 902–912. [Google Scholar] [CrossRef] [PubMed]
- Arumugam, M.; Raes, J.; Pelletier, E.; Paslier, D.L.; Yamada, T.; Mende, D.R. Addendum: Enterotypes of the human gut microbiome. Nature 2011, 473, 174–180. [Google Scholar] [CrossRef]
- Vermeij, W.P.; Dollé, M.E.T.; Reiling, E.; Jaarsma, D.; Payan-Gomez, D.; Bombardieri, C.R. Restricted diet delays accelerated ageing and genomic stress in DNA-repair-deficient mice. Nature 2016, 537, 427–431. [Google Scholar] [CrossRef]
- Vogel, H.G.; Vogel, W.H.; Schölkens, B.A.; Sandow, J.; Müller, P.G.; Vogel, W.F. Drug Discovery and Evaluation; Springer: Berlin/Heidelberg, Germany, 2002; pp. 1369–1382. [Google Scholar]
- Xing, S.; Shen, D.; Chen, C.; Wang, J.; Yu, Z. Early induction of oxidative stress in a mouse model of Alzheimer’s disease with heme oxygenase activity. Mol. Med. Rep. 2014, 10, 599–604. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.Y.; Chen, S.; Yan, Q.J.; Li, Y.X.; Jiang, Z.Q. Effect of Konjac mannan oligosaccharides on diphenoxylate-induced constipation in mice. J. Funct. Foods 2019, 57, 399–407. [Google Scholar] [CrossRef]
- Dostal, A.; Baumgartner, J.; Riesen, N.; Chassard, C.; Smuts, C.M.; Zimmermann, M.B.; Lacroix, C. Effects of iron supplementation on dominant bacterial groups in the gut, faecal SCFA and gut inflammation: A randomised, placebo-controlled intervention trial in South African children. Br. J. Nutr. 2014, 112, 547–556. [Google Scholar] [CrossRef] [PubMed]
- Callahan, B.J.; Mcmurdie, P.J.; Rosen, M.J.; Han, A.W.; Johnson, A.J.; Holmes, S.P. DADA2: High-resolution sample inference from Illumina amplicon data. Nat. Methods 2016, 13, 581–583. [Google Scholar] [CrossRef] [PubMed]
- Callahan, B.J.; Mcmurdie, P.J.; Holmes, S.P. Exact sequence variants should replace operational taxonomic units in marker-gene data analysis. ISME J. 2017, 11, 2639–2643. [Google Scholar] [CrossRef] [PubMed]
- Desantis, T.Z.; Hugenholtz, P.; Larsen, N.; Rojas, M.; Brodie, E.L.; Keller, K.; Huber, T.; Dalevi, D.; Hu, P.; Andersen, G.L. Greengenes: Chimera-checked 16S rRNA gene database and workbenchcompatible in ARB. Appl. Environ. Microbiol. 2006, 72, 5069–5072. [Google Scholar] [CrossRef] [PubMed]
- Qiong, W.; Garrity, G.M.; Tiedje, J.M.; Cole, J.R. Naive Bayesian classifier for rapid assignment of rRNA sequences into the new bacterial taxonomy. Appl. Environ. Microbiol. 2007, 73, 5261–5267. [Google Scholar]
- Bokulich, N.A.; Kaehler, B.D.; Rideout, J.R.; Dillon, M.; Bolyen, E.; Knight, R.; Huttley, G.A.; Caporaso, J.G. Optimizing taxonomic classification of marker-gene amplicon sequences with QIIME 2′s q2-feature-classifier plugin. Microbiome 2018, 6, 90–106. [Google Scholar] [CrossRef] [PubMed]
| NC | MC | REV | L-PHGG | M-PHGG | H-PHGG | |
|---|---|---|---|---|---|---|
| Aging biomarkers | ||||||
| AGEs (ng/gprot) | 394.53 ± 37.12 * | 586.00 ± 71.97 | 429.70 ± 52.90 * | 527.98 ± 91.13 | 533.05 ± 66.92 | 500.54 ± 56.71 * |
| NO (µmol/gprot) | 0.81 ± 0.05 * | 1.08 ± 0.04 | 0.94 ± 0.07 * | 1.06 ± 0.08 | 1.02 ± 0.08 * | 0.98 ± 0.12 * |
| iNOS (U/mgprot) | 0.45 ± 0.06 * | 0.57 ± 0.07 | 0.43 ± 0.07 * | 0.51 ± 0.05 | 0.50 ± 0.04 * | 0.50 ± 0.05 * |
| Lactic acid (µmol/gprot) | 14.15 ± 1.64 * | 21.96 ± 1.56 | 15.83 ± 2.63 * | 20.59 ± 2.19 | 21.46 ± 2.19 | 20.29 ± 1.79 * |
| Telomerase (nU/mgprot) | 103.92 ± 9.96 * | 77.79 ± 7.58 | 104.21 ± 7.81 * | 87.37 ± 6.82 * | 88.42 ± 10.88 * | 84.80 ± 7.62 |
| Antioxidant activity in brain | ||||||
| T-AOC (U/mgprot) | 3.69 ± 0.24 * | 3.42 ± 0.32 | 4.71 ± 0.28 * | 3.69 ± 0.28 | 4.93 ± 0.43 * | 4.66 ± 0.37 * |
| CAT (U/mgprot) | 18.33 ± 1.69 | 17.57 ± 2.35 | 22.37 ± 1.30 * | 19.73 ± 2.38 | 20.21 ± 2.62 * | 19.22 ± 2.99 |
| GSH-Px (U/mgprot) | 536.63 ± 21.36 * | 517.14 ± 19.56 | 612.94 ± 16.54 * | 530.44 ± 27.18 | 534.42 ± 31.41 | 526.26 ± 19.01 |
| MDA (nmol/mgprot) | 1.12 ± 0.21 | 1.25 ± 0.32 | 0.87 ± 0.11 * | 1.07 ± 0.34 | 0.87 ± 0.17 * | 0.95 ± 0.11 * |
| Antioxidant activity in serum | ||||||
| T-AOC (U/mL) | 9.5 ± 2.10 | 8.52 ± 0.81 | 10.36 ± 1.05 * | 8.74 ± 0.96 | 9.66 ± 0.83 * | 8.7 ± 0.78 |
| CAT (U/mL) | 24.90 ± 9.56 | 18.78 ± 1.37 | 29.16 ± 14.8 | 24.65 ± 6.48 * | 26.02 ± 6.58 * | 23.64 ± 6.25 * |
| GSH-Px (U/mL) | 848.95 ± 73.77 | 857.93 ± 86.69 | 895.55 ± 124.19 | 864.45 ± 50.10 | 852.97 ± 55.23 | 801.00 ± 34.12 |
| MDA (nmol/mL) | 2.97 ± 0.88 | 4.07 ± 1.57 | 2.29 ± 0.21 * | 3.10 ± 0.40 | 2.94 ± 0.31 * | 3.12 ± 0.56 |
| Forward Primer | Reverse Primer | |
|---|---|---|
| SIRT 1 | GAAAATGCTGGCCTAATAGACTTG | TGGTACAAACAAGTATTGATTACCG |
| FOXO1 | TCCCACACAGTGTCAAGACTACAA | CTGCTGTCAGACAATCTGAAGGA |
| P53 | AACTTACCAAGGCAACTATG | CTTGTAGATGGCCATGGCAC |
| GAPDH | CTTCTTGTGCAGTGCCAGCC | CAAGAGAAGGCAGCCCTGGT |
© 2019 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, X.; Wu, C.; Han, D.; Liu, J.; Liu, H.; Jiang, Z. Partially Hydrolyzed Guar Gum Attenuates d-Galactose-Induced Oxidative Stress and Restores Gut Microbiota in Rats. Int. J. Mol. Sci. 2019, 20, 4861. https://doi.org/10.3390/ijms20194861
Liu X, Wu C, Han D, Liu J, Liu H, Jiang Z. Partially Hydrolyzed Guar Gum Attenuates d-Galactose-Induced Oxidative Stress and Restores Gut Microbiota in Rats. International Journal of Molecular Sciences. 2019; 20(19):4861. https://doi.org/10.3390/ijms20194861
Chicago/Turabian StyleLiu, Xiaoyan, Chenxuan Wu, Dong Han, Jun Liu, Haijie Liu, and Zhengqiang Jiang. 2019. "Partially Hydrolyzed Guar Gum Attenuates d-Galactose-Induced Oxidative Stress and Restores Gut Microbiota in Rats" International Journal of Molecular Sciences 20, no. 19: 4861. https://doi.org/10.3390/ijms20194861
APA StyleLiu, X., Wu, C., Han, D., Liu, J., Liu, H., & Jiang, Z. (2019). Partially Hydrolyzed Guar Gum Attenuates d-Galactose-Induced Oxidative Stress and Restores Gut Microbiota in Rats. International Journal of Molecular Sciences, 20(19), 4861. https://doi.org/10.3390/ijms20194861






