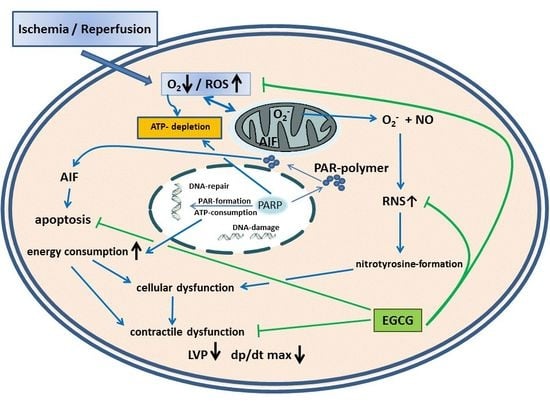
Epigallocatechin Gallate Reduces Ischemia/Reperfusion Injury in Isolated Perfused Rabbit Hearts
Abstract
:1. Introduction
2. Results
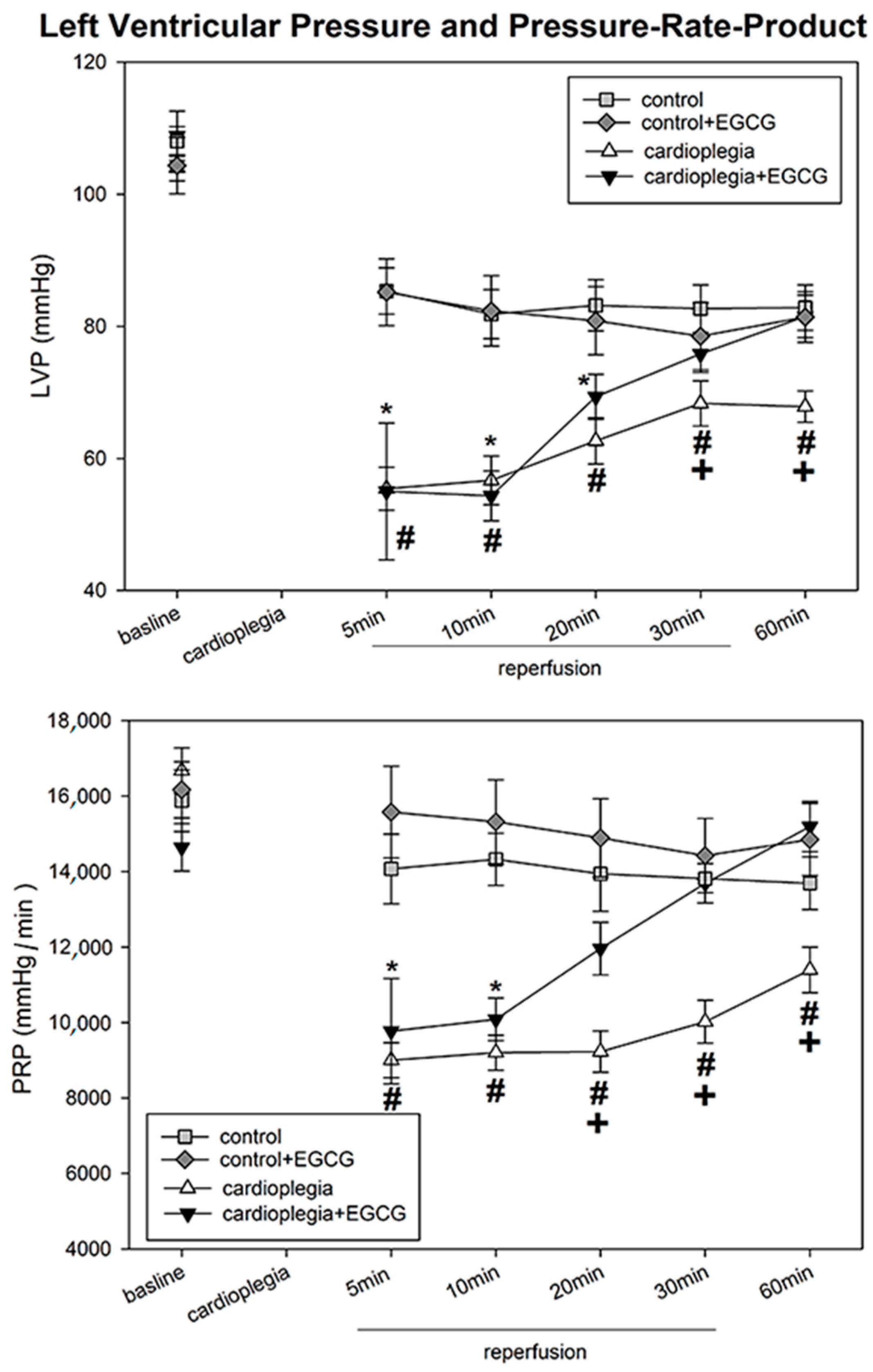
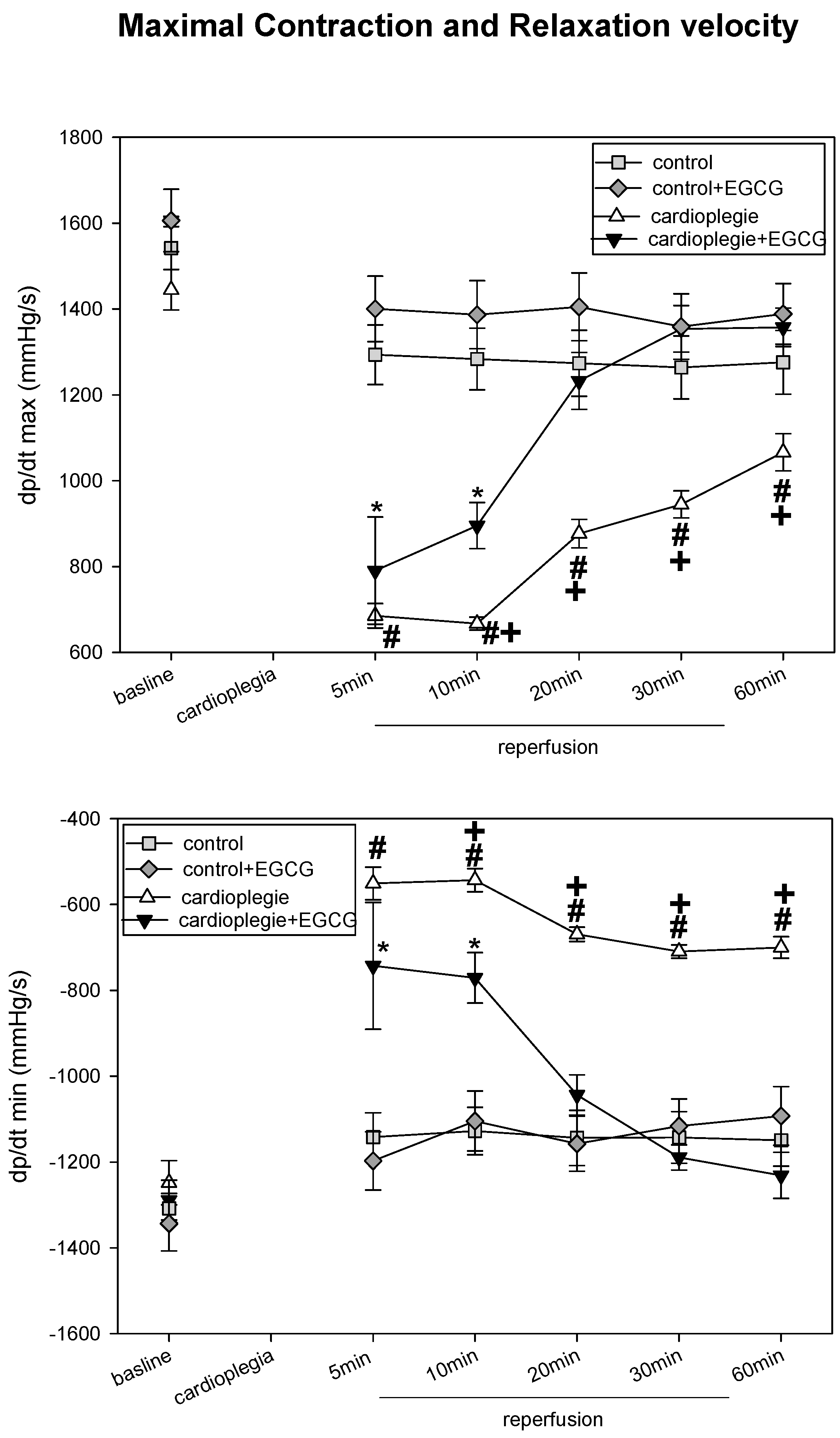
2.1. Hemodynamic Parameter
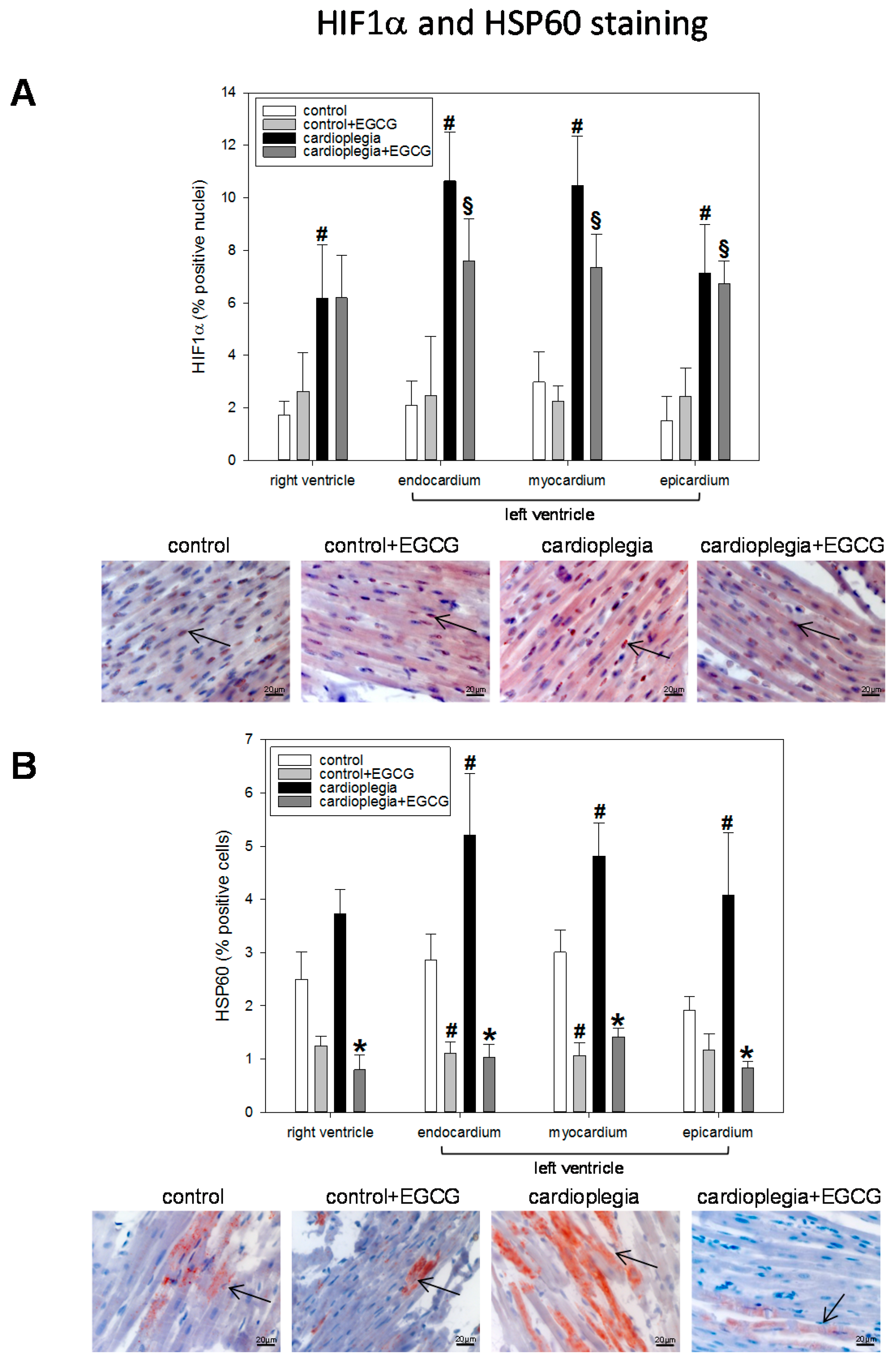
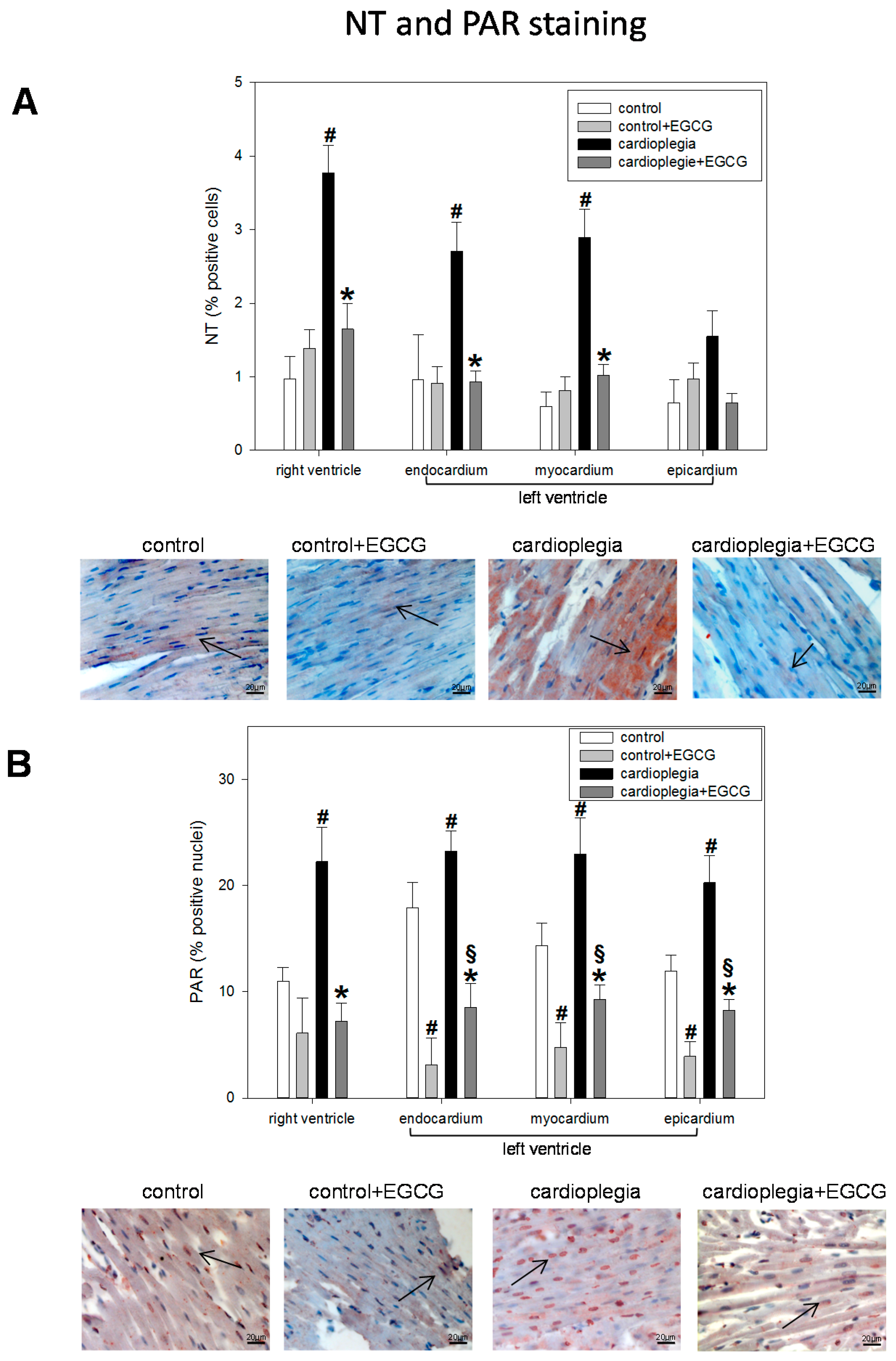
2.2. Histological Analysis
3. Discussion
4. Materials and Methods
4.1. Experimental Protocol
4.2. Histology
HPLC Analysis of ATP Content
4.3. Statistical Analysis
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| AIF | Apoptosis inducing factor |
| ARI | Activation recovery interval |
| ATP | Adenosine triphosphate |
| BCL | Basic cycle length |
| cC3 | Cleaved caspase 3 |
| CF | Coronary flow |
| dp/dt max | Maximal contraction velocity |
| dp/dt min | Maximal relaxation velocity |
| ECG | Electrocardiogram |
| EGCG | (−)-Epigallocatechin gallate |
| HIF1α | Hypoxia induced factor 1α |
| HPLC | High pressure liquid chromatography |
| HR | Heart rate |
| HSP60 | Heat shock protein 60 |
| Ica,L | l-type calcium channel |
| LV | Left ventricle |
| LVP | Left ventricular pressure |
| NT | Nitrotyrosine |
| PAR | Poly-ADP-ribose |
| PARP | Poly-ADP-ribose polymerase |
| pO2 | Partial oxygen pressure |
| PQ | PQ-interval |
| PRP | Pressure-rate product |
| QRS | QRS-interval |
| RNS | reactive nitrogen species |
| RV | Right ventricle |
| TAT | Total activation time |
References
- Khan, N.; Mukhtar, H. Tea and health: Studies in humans. Curr. Pharm. Des. 2013, 19, 6141–6147. [Google Scholar] [CrossRef] [PubMed]
- Graham, H.N. Green tea composition, consumption, and polyphenol chemistry. Prev Med. 1992, 21, 334–350. [Google Scholar] [CrossRef]
- Kuriyama, S.; Shimazu, T.; Ohmori, K.; Kikuchi, N.; Nakaya, N.; Nishino, Y.; Tsubono, Y.; Tsuji, I. Green tea consumption and mortality due to cardiovascular disease, cancer, and all causes in Japan: The Ohsaki study. JAMA 2006, 296, 1255–1265. [Google Scholar] [CrossRef] [PubMed]
- Mukamal, K.J.; Alert, M.; Maclure, M.; Muller, J.E.; Mittleman, M.A. Tea consumption and infarct-related ventricular arrhythmias: The determinants of myocardial infarction onset study. J. Am. Coll. Nutr. 2006, 25, 472–479. [Google Scholar] [CrossRef] [PubMed]
- Mukamal, K.J.; Maclure, M.; Muller, J.E.; Sherwood, J.B.; Mittleman, M.A. Tea consumption and mortality after acute myocardial infarction. Circulation 2002, 105, 2476–2481. [Google Scholar] [CrossRef] [PubMed]
- Hirano, R.; Momiyama, Y.; Takahashi, R.; Taniguchi, H.; Kondo, K.; Nakamura, H.; Ohsuzu, F. Comparison of green tea intake in Japanese patients with and without angiographic coronary artery disease. Am. J. Cardiol. 2002, 90, 1150–1153. [Google Scholar] [CrossRef]
- Arts, I.C.; Hollman, P.C.; Feskens, E.J.; Bueno de Mesquita, H.B.; Kromhout, D. Catechin intake might explain the inverse relation between tea consumption and ischemic heart disease: The Zutphen Elderly Study. Am. J. Clin. Nutr. 2001, 74, 227–232. [Google Scholar] [CrossRef] [PubMed]
- Geleijnse, J.M.; Launer, L.J.; Van der Kuip, D.A.; Hofman, A.; Witteman, J.C. Inverse association of tea and flavonoid intakes with incident myocardial infarction: The Rotterdam Study. Am. J. Clin. Nutr. 2002, 75, 880–886. [Google Scholar] [CrossRef] [PubMed]
- Song, D.K.; Jang, Y.; Kim, J.H.; Chun, K.J.; Lee, D.; Xu, Z. Polyphenol (−)-epigallocatechin gallate during ischemia limits infarct size via mitochondrial K(ATP) channel activation in isolated rat hearts. J. Korean Med. Sci. 2010, 25, 380–386. [Google Scholar] [CrossRef] [PubMed]
- Piao, C.S.; Kim, D.S.; Ha, K.C.; Kim, H.R.; Chae, H.J.; Chae, S.W. The protective effect of epigallocatechin-3 gallate on ischemia/reperfusion injury in isolated rat hearts: An ex vivo approach. Korean J. Physiol. Pharmacol. 2011, 15, 259–266. [Google Scholar] [CrossRef] [PubMed]
- Othman, A.I.; Elkomy, M.M.; El-Missiry, M.A.; Dardor, M. Epigallocatechin-3-gallate prevents cardiac apoptosis by modulating the intrinsic apoptotic pathway in isoproterenol-induced myocardial infarction. Eur. J. Pharmacol. 2017, 794, 27–36. [Google Scholar] [CrossRef] [PubMed]
- Townsend, P.A.; Scarabelli, T.M.; Pasini, E.; Gitti, G.; Menegazzi, M.; Suzuki, H.; Knight, R.A.; Latchman, D.S.; Stephanou, A. Epigallocatechin-3-gallate inhibits STAT-1 activation and protects cardiac myocytes from ischemia/reperfusion-induced apoptosis. FASEB J. 2004, 18, 1621–1623. [Google Scholar] [CrossRef] [PubMed]
- Yanagi, S.; Matsumura, K.; Marui, A.; Morishima, M.; Hyon, S.H.; Ikeda, T.; Sakata, R. Oral pretreatment with a green tea polyphenol for cardioprotection against ischemia-reperfusion injury in an isolated rat heart model. J. Thorac. Cardiovasc. Surg. 2011, 141, 511–517. [Google Scholar] [CrossRef] [PubMed]
- Mangano, D.T. Biventricular function after myocardial revascularization in humans: Deterioration and recovery patterns during the first 24 hours. Anesthesiology 1985, 62, 571–577. [Google Scholar] [CrossRef] [PubMed]
- Gross, G.J.; Farber, N.E.; Hardman, H.F.; Warltier, D.C. Beneficial actions of superoxide dismutase and catalase in stunned myocardium of dogs. Am. J. Physiol. 1986, 250, H372–H377. [Google Scholar] [CrossRef] [PubMed]
- Funamoto, M.; Masumoto, H.; Takaori, K.; Taki, T.; Setozaki, S.; Yamazaki, K.; Minakata, K.; Ikeda, T.; Hyon, S.H.; Sakata, R. Green Tea Polyphenol Prevents Diabetic Rats From Acute Kidney Injury After Cardiopulmonary Bypass. Ann. Thorac. Surg. 2016, 101, 1507–1513. [Google Scholar] [CrossRef] [PubMed]
- Twal, M.; Kiefer, P.; Salameh, A.; Schnabel, J.; Ossmann, S.; von Salisch, S.; Krämer, K.; Sobiraj, A.; Kostelka, M.; Mohr, F.W.; et al. Reno-protective effects of epigallocatechingallate in a small piglet model of extracorporeal circulation. Pharmacol. Res. 2013, 67, 68–78. [Google Scholar] [CrossRef] [PubMed]
- Salameh, A.; Einenkel, A.; Kühne, L.; Grassl, M.; von Salisch, S.; Kiefer, P.; Vollroth, M.; Dähnert, I.; Dhein, S. Hippocampal neuroprotection by minocycline and epigallo-catechin-3-gallate against cardiopulmonary bypass-associated injury. Brain Pathol. 2015, 25, 733–742. [Google Scholar] [CrossRef] [PubMed]
- Kasper, B.; Salameh, A.; Krausch, M.; Kiefer, P.; Kostelka, M.; Mohr, F.W.; Dhein, S. Epigallocatechin gallate attenuates cardiopulmonary bypass-associated lung injury. J. Surg. Res. 2016, 201, 313–325. [Google Scholar] [CrossRef] [PubMed]
- Aneja, R.; Hake, P.W.; Burroughs, T.J.; Denenberg, A.G.; Wong, H.R.; Zingarelli, B. Epigallocatechin, a green tea polyphenol, attenuates myocardial ischemia reperfusion injury in rats. Mol. Med. 2004, 10, 55–62. [Google Scholar] [CrossRef] [PubMed]
- Zhong, W.; Huan, X.D.; Cao, Q.; Yang, J. Cardioprotective effect of epigallocatechin-3-gallate against myocardial infarction in hypercholesterolemic rats. Exp. Ther. Med. 2015, 9, 405–410. [Google Scholar] [CrossRef] [PubMed]
- Bao, L.; Lu, F.; Chen, H.; Min, Q.; Chen, X.; Song, Y.; Zhao, B.; Bu, H.; Sun, H. High concentration of epigallocatechin-3-gallate increased the incidences of arrhythmia and diastolic dysfunction via β2-adrenoceptor. J. Food Sci. 2015, 80, T659–T663. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.; Cheng, H.; Ji, J.; Incardona, J.; Rampe, D. In vitro electrocardiographic and cardiac ion channel effects of (−)-epigallocatechin-3-gallate, the main catechin of green tea. J. Pharmacol. Exp. Ther. 2010, 334, 619–626. [Google Scholar] [CrossRef] [PubMed]
- Hirai, M.; Hotta, Y.; Ishikawa, N.; Wakida, Y.; Fukuzawa, Y.; Isobe, F.; Nakano, A.; Chiba, T.; Kawamura, N. Protective effects of EGCg or GCg, a green tea catechin epimer, against postischemic myocardial dysfunction in guinea-pig hearts. Life Sci. 2007, 80, 1020–1032. [Google Scholar] [CrossRef] [PubMed]
- Tipoe, G.L.; Leung, T.M.; Hung, M.W.; Fung, M.L. Green tea polyphenols as an anti-oxidant and anti-inflammatory agent for cardiovascular protection. Cardiovasc. Hematol. Disord. Drug Targets 2007, 7, 135–144. [Google Scholar] [CrossRef] [PubMed]
- Wang, X.; Wang, Y.; Parapanov, R.; Abdelnour, E.; Gronchi, F.; Perentes, J.Y.; Piquilloud, L.; Ris, H.B.; Letovanec, I.; Liaudet, L.; et al. Pharmacological reconditioning of marginal donor rat lungs using inhibitors of peroxynitrite and poly (ADP-ribose) polymerase during ex vivo lung perfusion. Transplantation 2016, 100, 1465–1473. [Google Scholar] [CrossRef] [PubMed]
- Gerö, D.; Szoleczky, P.; Chatzianastasiou, A.; Papapetropoulos, A.; Szabo, C. Modulation of poly(ADP-ribose) polymerase-1 (PARP-1)-mediated oxidative cell injury by ring finger protein 146 (RNF146) in cardiac myocytes. Mol. Med. 2014, 20, 313–328. [Google Scholar] [CrossRef] [PubMed]
- Olmos, A.; Giner, R.M.; Recio, M.C.; Ríos, J.L.; Gil-Benso, R.; Máñez, S. Interaction of dicaffeoylquinic derivatives with peroxynitrite and other reactive nitrogen species. Arch. Biochem. Biophys. 2008, 475, 66–71. [Google Scholar] [CrossRef] [PubMed]
- Bastianetto, S.; Krantic, S.; Chabot, J.G.; Quirion, R. Possible involvement of programmed cell death pathways in the neuroprotective action of polyphenols. Curr. Alzheimer Res. 2011, 8, 445–451. [Google Scholar] [CrossRef] [PubMed]
- Kim, G.T.; Chun, Y.S.; Park, J.W.; Kim, M.S. Role of apoptosis-inducing factor in myocardial cell death by ischemia-reperfusion. Biochem. Biophys. Res. Commun. 2003, 309, 619–624. [Google Scholar] [CrossRef] [PubMed]
- Salameh, A.; Keller, M.; Dähnert, I.; Dhein, S. Olesoxime Inhibits Cardioplegia-Induced Ischemia/Reperfusion Injury. A Study in Langendorff-Perfused Rabbit Hearts. Front. Physiol. 2017, 8, 324. [Google Scholar] [CrossRef] [PubMed]
- Dhein, S.; Müller, A.; Gerwin, R.; Klaus, W. Comparative study on the proarrhythmic effects of some antiarrhythmic agents. Circulation 1993, 87, 617–630. [Google Scholar] [CrossRef] [PubMed]
- Salameh, A.; Halling, M.; Seidel, T.; Dhein, S. Effects of minocycline on parameters of cardiovascular recovery after cardioplegic arrest in a rabbit Langendorff heart model. Clin. Exp. Pharmacol. Physiol. 2015, 42, 1258–1265. [Google Scholar] [CrossRef] [PubMed]

| Parameters | Baseline | Reperfusion 5 min | Reperfusion 10 min | Reperfusion 20 min | Reperfusion 30 min | Reperfusion 60 min |
|---|---|---|---|---|---|---|
| ARI (ms) control control + EGCG cardioplegia cardioplegia + EGCG | 126 ± 3.9 133 ± 4.4 138 ± 4.7 131 ± 3.5 | 136 ± 3.5 126 ± 4.9 150 ± 6.5 141 ± 3.7 § | 139 ± 4.3 124 ± 4.6 # 150 ± 4.5 136 ± 4.2 §,* | 142 ± 4.5 121 ± 4.3 # 148 ± 5.6 132 ± 4.4 #,* | 140 ± 3.8 122 ± 4.5 # 145 ± 5.7 126 ± 3.2 * | 137 ± 3.6 123 ± 4.6 # 141 ± 5.6 125 ± 2.9 * |
| TAT (ms) control control + EGCG cardioplegia cardioplegia + EGCG | 14.3 ± 1.8 13.7 ± 1.0 15.1 ± 1.6 14.9 ± 1.2 | 13.9 ± 2.6 15.0 ± 0.9 18.0 ± 2.1 18.3 ± 1.2 | 15.6 ± 3.5 13.9 ± 0.9 19.3 ± 2.3 19.8 ± 2.5 | 13.4 ± 1.1 15.6 ± 1.1 18.4 ± 1.6 17.0 ± 2.2 | 13.1 ± 0.5 14.7 ± 0.6 20.0 ± 2.0 # 17.0 ± 2.2 | 13.4 ± 1.4 14.4 ± 0.9 19.9 ± 2.2 # 16.5 ± 2.1 |
| Vector similarity (%) control control + EGCG cardioplegia cardioplegia + EGCG | 55 ± 7.3 58 ± 7.9 54 ± 5.5 58 ± 7.6 | 35 ± 9.5 33 ± 9.4 22 ± 5.3 17 ± 5.0 | 30 ± 8.3 30 ± 8.6 22 ± 5.5 20 ± 5.8 | 36 ± 9.2 33 ± 8.2 25 ± 6.2 21 ± 4.4 | 34 ± 8.9 32 ± 8.8 24 ± 6.9 23 ± 4.9 | 33 ± 7.9 30 ± 9.9 23 ± 6.2 24 ± 4.9 |
| PQ (ms) control control + EGCG cardioplegia cardioplegia + EGCG | 64 ± 2.0 62 ± 1.3 63 ± 2.0 64 ± 1.5 | 64 ± 0.9 61 ± 1.6 65 ± 2.9 68 ± 4.0 | 64 ± 1.0 60 ± 1.2 64 ± 3.6 60 ± 2.4 | 64 ± 1.1 65 ± 1.7 64 ± 2.5 66 ± 1.3 | 65 ± 1.2 62 ± 2.5 65 ± 2.1 66 ± 1.3 | 64 ± 1.4 63 ± 2.6 63 ± 2.4 63 ± 0.7 |
| QRS (ms) control control + EGCG cardioplegia cardioplegia + EGCG | 28 ± 1.0 25 ± 0.6 26 ± 0.6 24 ± 0.7 | 27 ± 1.0 27 ± 0.6 25 ± 0.4 27 ± 1.2 | 28 ± 0.8 25 ± 0.7 25 ± 0.7 28 ± 1.0 | 26 ± 0.7 27 ± 0.7 26 ± 0.4 26 ± 0.6 | 27 ± 1.0 26 ± 0.6 24 ± 0.4 24 ± 0.8 | 28 ± 0.8 27 ± 0.5 25 ± 0.9 26 ± 1.0 |
| BCL (ms) control control + EGCG cardioplegia cardioplegia + EGCG | 375 ± 12 359 ± 8 387 ± 10 366 ± 9 | 390 ± 20 352 ± 19 365 ± 9 327 ± 21 | 400 ± 21 332 ± 14 368 ± 13 322 ± 10 | 399 ± 22 339 ± 16 421 ± 16 356 ± 8 | 393 ± 24 337 ± 15 434 ± 24 338 ± 10 | 400 ± 25 350 ± 20 375 ± 15 328 ± 9 |
| HR (min−1) control control + EGCG cardioplegia cardioplegia + EGCG | 163 ± 5.3 170 ± 3.6 159 ± 4.0 166 ± 4.2 | 161 ± 6.7 182 ± 7.5 167 ± 4.7 188 ± 11 | 157 ± 6.9 188 ± 6.1 170 ± 6.5 192 ± 6.5 | 158 ± 6.8 187 ± 7.4 150 ± 7.0 171 ± 4.2 | 162 ± 7.7 187 ± 7.2 150 ± 7.6 182 ± 5.4 | 160 ± 7.9 185 ± 8.4 168 ± 6.7 187 ± 5.1 |
| CF/PRP (µL/mmHg) control control + EGCG cardioplegia cardioplegia + EGCG | 1.86 ± 0.12 1.71 ± 0.06 1.81 ± 0.04 1.68 ± 0.06 | 1.83 ± 0.06 1.74 ± 0.09 3.09 ± 0.11 # 3.33 ± 0.47 § | 1.73 ± 0.05 1.75 ± 0.09 2.78 ± 0.14 # 2.95 ± 0.16 § | 1.88 ± 0.06 1.78 ± 0.06 2.35 ± 0.08 # 2.27 ± 0.12 § | 1.90 ± 0.07 1.80 ± 0.05 2.05 ± 0.04 1.96 ± 0.08 | 1.74 ± 0.05 1.77 ± 0.09 1.91 ± 0.10 1.89 ± 0.09 |
| pO2art-ven (mmHg) control control + EGCG cardioplegia cardioplegia + EGCG | 400 ± 11 398 ± 11 384 ± 8.0 404 ± 6.7 | 411 ± 6.5 401 ± 9.4 313 ± 10 # 262 ± 6.2 § | 400 ± 6.3 407 ± 11 312 ± 9.0 # 285 ± 7.2 § | 414 ± 5.7 406 ± 11 360 ± 6.9 368 ± 8.7 | 425 ± 5.3 411 ± 13 360 ± 9.0 387 ± 7.7 | 435 ± 6.0 433 ± 12 368 ± 8.6 380 ± 8.8 |
| ATP content µg/g control control + EGCG cardioplegia cardioplegia + EGCG | 60 ± 6.5 73 ± 9.0 43 ± 8.2 # 69 ± 5.4 * |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Salameh, A.; Schuster, R.; Dähnert, I.; Seeger, J.; Dhein, S. Epigallocatechin Gallate Reduces Ischemia/Reperfusion Injury in Isolated Perfused Rabbit Hearts. Int. J. Mol. Sci. 2018, 19, 628. https://doi.org/10.3390/ijms19020628
Salameh A, Schuster R, Dähnert I, Seeger J, Dhein S. Epigallocatechin Gallate Reduces Ischemia/Reperfusion Injury in Isolated Perfused Rabbit Hearts. International Journal of Molecular Sciences. 2018; 19(2):628. https://doi.org/10.3390/ijms19020628
Chicago/Turabian StyleSalameh, Aida, Roxana Schuster, Ingo Dähnert, Johannes Seeger, and Stefan Dhein. 2018. "Epigallocatechin Gallate Reduces Ischemia/Reperfusion Injury in Isolated Perfused Rabbit Hearts" International Journal of Molecular Sciences 19, no. 2: 628. https://doi.org/10.3390/ijms19020628
APA StyleSalameh, A., Schuster, R., Dähnert, I., Seeger, J., & Dhein, S. (2018). Epigallocatechin Gallate Reduces Ischemia/Reperfusion Injury in Isolated Perfused Rabbit Hearts. International Journal of Molecular Sciences, 19(2), 628. https://doi.org/10.3390/ijms19020628