Herbal Supplement in a Buffer for Dry Eye Syndrome Treatment
Abstract
:1. Introduction
2. Results
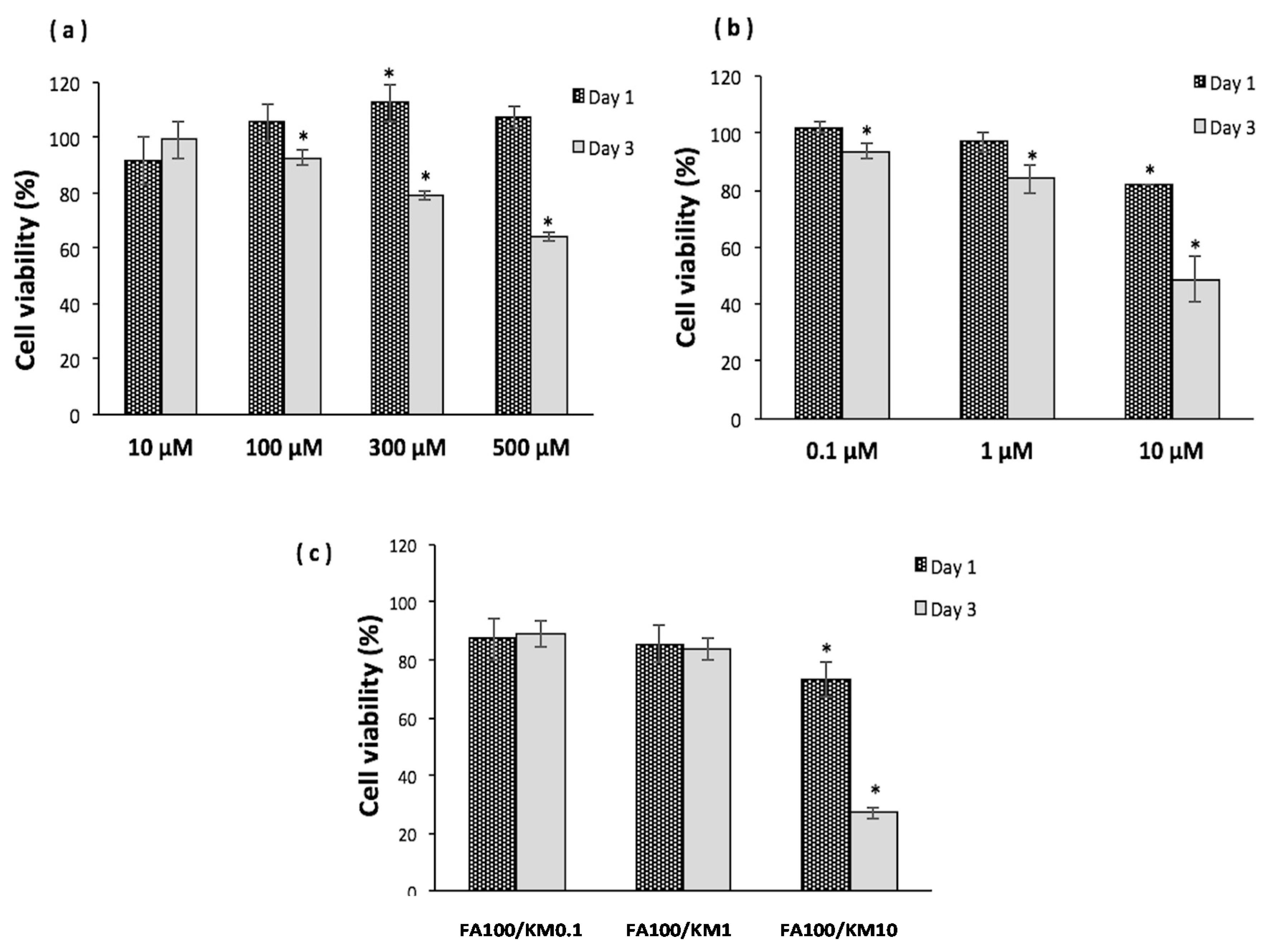
2.1. Optimal Kaempferol and Ferulic Acid Concentration for Cultivating Human Corneal Epithelial Cells
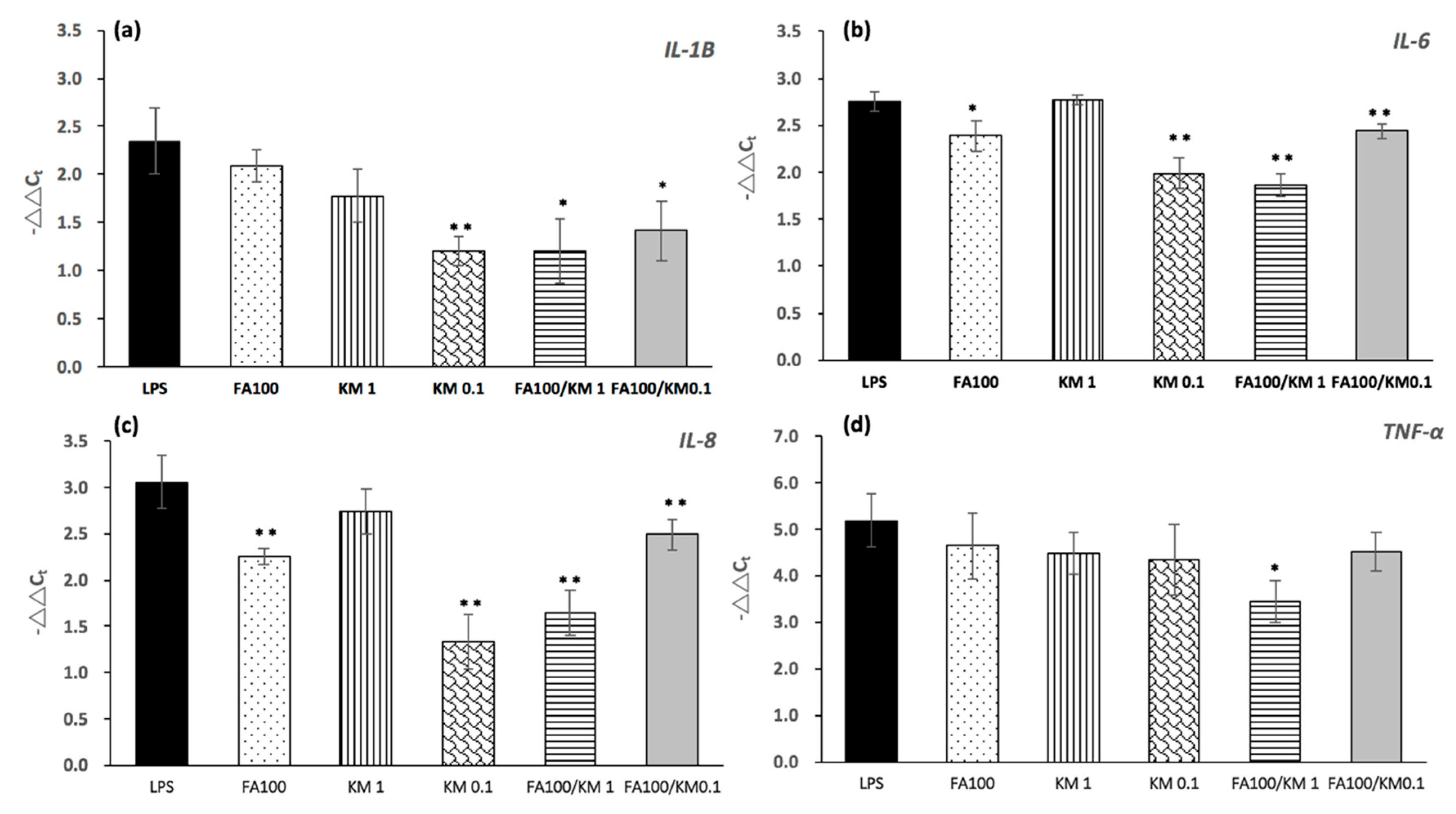
2.2. The Anti-Inflammatory Effects of KM and FA Work on Inflamed HCECs
2.3. Characterization of Buffer Solution Containing FA and KM as Eye Drops
2.4. Irritation Tests in Rabbit Eyes
2.5. Therapeutic Efficacy of Buffer with FA/KM Addition in DES Rabbits
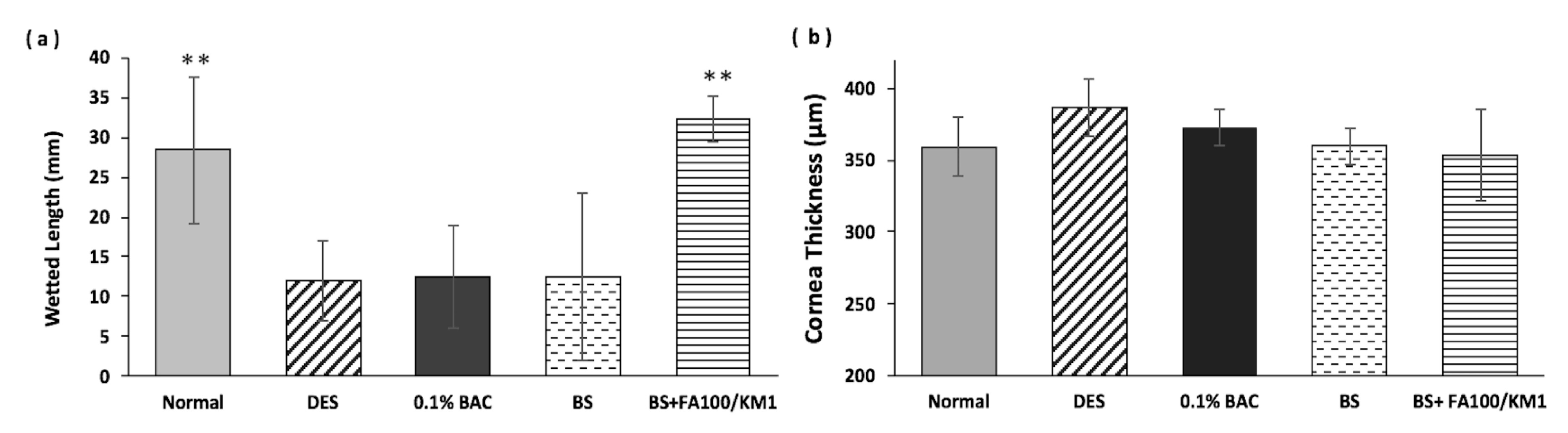
2.5.1. Tear Production Increased on Treatment with the Herbal Combination
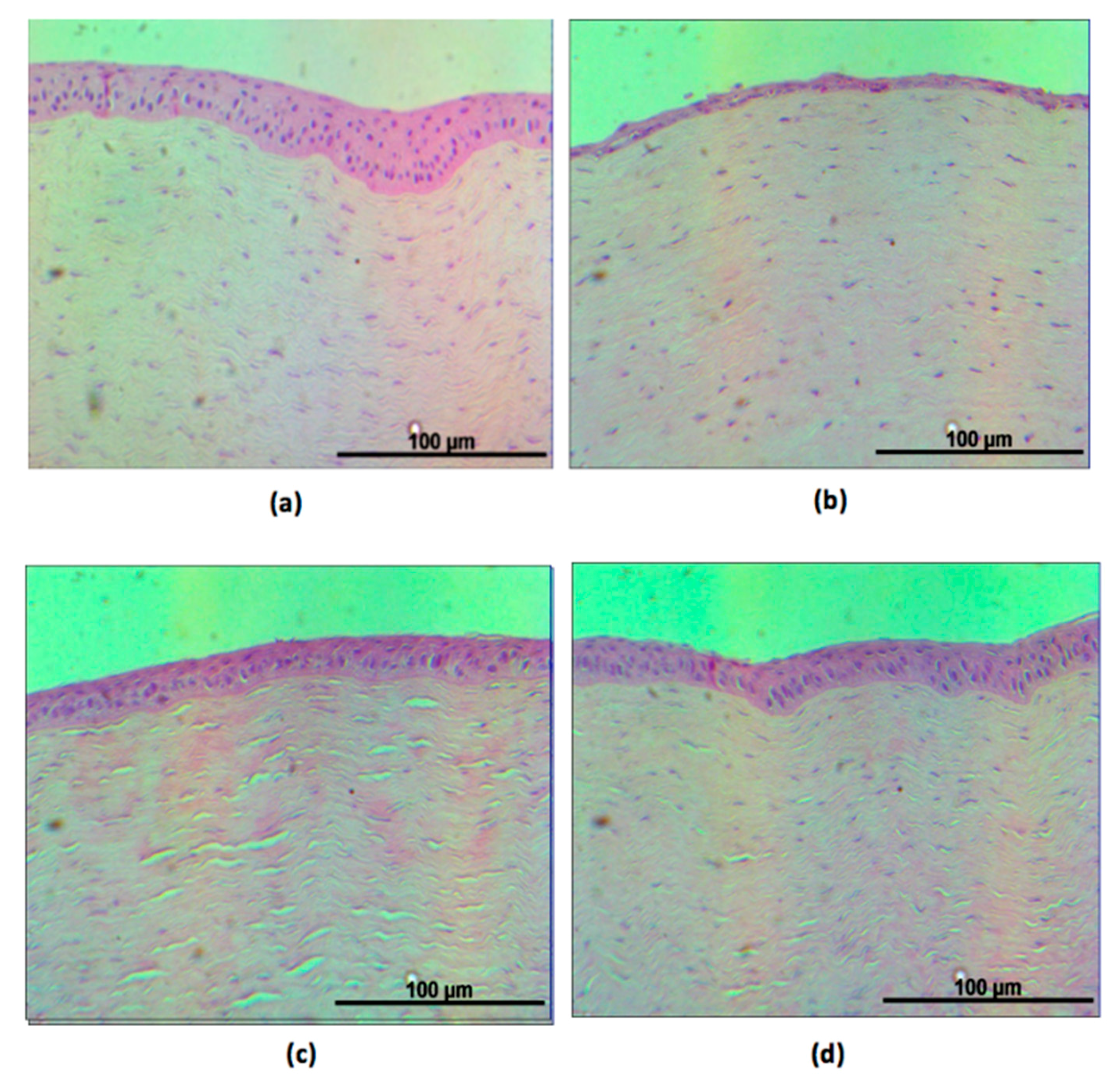
2.5.2. Recovering the Damaged Epithelium in the Cornea
3. Discussion
4. Materials and Methods
4.1. Chemicals and Reagents
4.2. Viability of Human Corneal Epithelial Cells Treated with Herbal Components
4.3. Expression of Genes Encoding Inflammatory Cytokines in HCECs
4.4. Characterization of Buffer Solution Containing Herbal Components as Eye Drops
4.5. Irritation Test of Rabbit Eyes
4.6. DES Inducement in Rabbits and Therapeutic Effect Evaluation of Herbal Eye Drops
4.6.1. Measurement of Aqueous Tear Production and Fluorescence Staining
4.6.2. Histological Examination of the Cornea
4.7. Statistical Analysis
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| DES | Dry eye syndrome |
| BS | Buffer solution made by balance salt solution |
| KM | Kaempferol |
| FA | Ferulic acid |
| BAC | Benzalkonium chloride |
| HCECs | Human corneal epithelium cells |
References
- Hessen, M.; Akpek, E.K. Dry eye: An inflammatory ocular disease. J. Ophthalmic Vis. Res. 2014, 9, 240–250. [Google Scholar] [PubMed]
- Sickenberger, W. Eins, Zwei, Drei—A German’s perspective on dry eye numbers in the world. Contact Lens Anter. Eye 2017, 40, 1–2. [Google Scholar] [CrossRef] [PubMed]
- Short, B.G. Safety evaluation of ocular drug delivery formulations: Techniques and practical considerations. Toxicol. Pathol. 2008, 36, 49–62. [Google Scholar] [CrossRef] [PubMed]
- Lin, P.Y.; Tsai, S.Y.; Cheng, C.Y.; Liu, J.H.; Chou, P.; Hsu, W.M. Prevalence of dry eye among an elderly Chinese population in Taiwan. Ophthalmology 2003, 110, 1096–1101. [Google Scholar] [CrossRef]
- Lee, H.S.; Chauhan, S.K.; Okanobo, A.; Nallasamy, N.; Dana, R. Therapeutic efficacy of topical epigallocatechin gallate in murine dry eye. Cornea 2011, 30, 1465–1472. [Google Scholar] [CrossRef] [PubMed]
- Yoon, K.-C.; de Paiva, C.S.; Qi, H.; Chen, Z.; Farley, W.J.; Li, D.-Q.; Pflugfelder, S.T. Expression of Th-1 chemokines and chemokine receptors on the ocular surface of C57BL/6 mice: Effects of desiccating stress. Investig. Ophthalmol. Vis. Sci. 2007, 48, 2561–2569. [Google Scholar]
- Wilson, S.; Perry, H. Long-term resolution of chronic dry eye symptoms and signs after topical cyclosporine treatment. Ophthalmology 2007, 114, 76–79. [Google Scholar] [CrossRef] [PubMed]
- Larrosa, M.; Lodovici, M.; Morbidelli, L.; Dolara, P. Hydrocaffeic and p-coumaric acids, natural phenolic compounds, inhibit UV-B damage in WKD human conjunctival cells in vitro and rabbit eye in vivo. Free Radic. Res. 2008, 42, 903–910. [Google Scholar] [CrossRef] [PubMed]
- Majumdara, S.; Srirangama, R. Potential of the bioflavonoids in the prevention/treatmentof ocular disorders. J. Pharm. Pharmacol. 2010, 10, 951–965. [Google Scholar] [CrossRef] [PubMed]
- Tseng, C.; Hung, Y.; Chen, Z.; Fang, H.; Chen, K. Synergistic effect of artificial tears containing epigallocatechin gallate and hyaluronic acid for the treatment of rabbits with dry eye syndrome. PLoS ONE 2016, 11, e0157982. [Google Scholar] [CrossRef] [PubMed]
- Rajendran, P.; Rengarajan, T.; Nandakumar, N.; Palaniswami, R.; Nishigaki, Y.; Nishigaki, I. Kaempferol, a potential cytostatic and cure for inflammatory disorders. Eur. J. Med. Chem. 2014, 86, 103–112. [Google Scholar] [CrossRef] [PubMed]
- Vissiennon, C.K.; Nieber, O.K.; Butterweck, V. Route of administration determines the anxiolytic activity of the flavonols kaempferol, quercetin and myricetin—Are they prodrugs? J. Nutr. Biochem. 2012, 23, 733–740. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.K.; Park, H.R.; Lee, J.S.; Chung, T.S.; Chung, H.Y.; Chung, J. Down-regulation of iNOS and TNF-α expression by kaempferol via NF-κB inactivation in aged rat gingival tissues. Biogerontology 2007, 8, 399–408. [Google Scholar] [CrossRef] [PubMed]
- Cao, R.; Fu, K.; Lv, X.; Li, W.; Zhang, N. Protective effects of kaempferol on lipopolysaccharide-induced mastitis in mice. Inflammation 2014, 1453–1458. [Google Scholar] [CrossRef] [PubMed]
- Wilson, W.S.; Duncan, A.J.; Jay, J.L. Effect of benzalkonium chloride on the stability of the precorneal tear film in rabbit and man. Br. J. Ophthalmol. 1975, 59, 667–669. [Google Scholar] [CrossRef] [PubMed]
- De Saint Jean, M.; Debbasch, C.; Brignole, F.; Rat, P.; Warnet, J.M.; Baudouin, C. Toxicity of preserved and unpreserved antiglaucoma topical drugs in an in vitro model of conjunctival cells. Curr. Eye Res. 2000, 20, 85–94. [Google Scholar]
- Trombino, S.; Serini, S.; Nicuolo, F.; Celleno, L.; Andò, S.; Picci, N.; Calviello, G.; Palozza, P. Antioxidant effect of ferulic aicd in isolated membranes and intact cells: Synergistic interactions with tocopherol, carotene, and ascorbic acid. J. Agric. Food Chem. 2004, 53, 2411–2420. [Google Scholar] [CrossRef] [PubMed]
- Tsou, M.F.; Hung, C.F.; Lu, H.F.; Wu, L.T.; Chang, S.H.; Chang, H.L.; Chen, G.W.; Chung, J.G. Effects of caffeic acid, chlorogenic acid and ferulic acid on growth and arylamine N acetyltransferase activity in Shigella sonnei (group D). Microbios 2000, 101, 37–46. [Google Scholar] [PubMed]
- Boz, H.S. Ferulic Acid in Cereals—A Review. Czech J. Food Sci. 2015, 33, 1–7. [Google Scholar] [CrossRef]
- Abelson, M.B.; Udell, I.J.; Weston, J.H. Normal human tear pH by direct measurement. Arch. Ophthalmol. 1981, 99, 301. [Google Scholar] [CrossRef] [PubMed]
- Benelli, U.; Nardi, M.; Posarelli, C.; Albert, T.G. Tear osmolarity measurement using the TearLab™ Osmolarity System in the assessment of dry eye treatment effectiveness. Contact Lens Anter. Eye 2010, 33, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Craig, J.; Simmons, P.; Patel, S.; Tomlinson, A. Refractive index and osmolality of human tears. Optom. Vis. Sci. 1995, 72, 718–724. [Google Scholar] [CrossRef] [PubMed]
- International Organization for Standardization. Biological evaluation of medical devices. In Part 10: Tests for Irritation and Skin Sensitization; International Organization for Standardization: Geneva, Switzerland, 2010. [Google Scholar]
- Gökçe, E.H.; Sandri, G.; Eğrilmez, S.; Bonferoni, M.C.; Güneri, T.; Caramella, C. Cyclosporine A-loaded solid lipid nanoparticles: Ocular tolerance and in vivo drug release in rabbit eyes. Curr. Eye Res. 2009, 34, 996–1003. [Google Scholar] [CrossRef] [PubMed]
- Hutak, C.M.; Jacaruso, R.B. Evaluation of primary ocular irritation: Alternatives to the Draize test. In Ocular Therapeutics and Drug Delivery; IK, R., Ed.; Technomic Publishing: Lancaster, PA, USA, 1996. [Google Scholar]
- Lemp, M.A.; Baudouin, C.; Baum, J.; Dogru, M.; Foulks, G.N.; Kinoshita, S. The definition and classification of dry eye disease: Report of the definition and classification subcommittee of the international Dry Eye WorkShop. Ocul. Surf. 2007, 5, 75–92. [Google Scholar]
- Erdinest, N.; Shmueli, O.; Grossman, Y.; Ovadia, H.; Solomon, A. Anti-Inflammatory effects of α linolenic acid on human corneal epithelial cells. Investig. Ophthalmol. Vis. Sci. 2012, 53, 4396–4406. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Z.; Yang, W.Z.; Zhu, Z.Z.; Hu, Q.Q.; Chen, Y.F.; He, H.; Chen, Y.X.; Liu, Z.G. Therapeutic effects of topical doxycycline in a benzalkonium chloride-induced mouse dry eye model. Investig. Ophthalmol. Vis. Sci. 2014, 13, 2963–2974. [Google Scholar] [CrossRef] [PubMed]
- Crespo, I.; García-Mediavilla, M.V.; Gutiírrez, B.; Sánchez-Campos, S.; Tuñón, M.J.; González-Gallego, J. A comparison of the effects of kaempferol and quercetin on cytokine-induced pro-inflammatory status of cultured human endothelial cells. Br. J. Nutr. 2008, 100, 968–976. [Google Scholar] [CrossRef] [PubMed]
- Sharma, V.; Joseph, C.; Ghosh, S. Kaempferol induces apoptosis in glioblastoma cells through oxidative stress. Mol. Cancer Ther. 2007, 6, 2544–2554. [Google Scholar] [CrossRef] [PubMed]
- Redfern, R.L.; McDermott, A.M. Toll-like receptors in ocular surface disease. Exp. Eye Res. 2010, 90, 679–687. [Google Scholar] [CrossRef] [PubMed]
- Guha, M.; Mackman, N. LPS induction of gene expression in human monocytes. Cell. Signal. 2001, 13, 85–94. [Google Scholar] [CrossRef]
- Kogut, M.H.; He, H.; Kaiser, P. Lipopolysaccharide binding protein/CD14/TLR4-dependent recognition of Salmonella LPS induces the functional activation of chicken heterophils and up-regulation of proinflammatory cytokine and chemokine gene expression in these cells. Anim. Biotechnol. 2005, 16, 165–181. [Google Scholar] [CrossRef] [PubMed]
- Cao, Y.; Bindslev, D.A.; Kjærgaard, S.K. Estimation of the in vitro eye irritating and inflammatory potential of lipopolysaccharide (LPS) and dust by using reconstituted human corneal epithelium tissue cultures. Toxicol. Mech. Methods 2015, 25, 402–409. [Google Scholar] [CrossRef] [PubMed]
- Tang, X.L.; Liu, J.X.; Dong, W.; Li, P.; Li, L.; Hou, J.C.; Zheng, Y.Q.; Lin, C.R.; Ren, J.G. Protective effect of kaempferol on LPS plus ATP-Induced inflammatory response in cardiac fibroblasts. Inflammation 2015, 38, 94–101. [Google Scholar] [CrossRef] [PubMed]
- Kim, H.P.; Son, K.H.; Chang, H.W.; Kang, S.S. Anti-inflammatory Plant Flavonoids and Cellular Action Mechanisms. J. Pharmacol. Sci. 2004, 96, 229–245. [Google Scholar] [CrossRef] [PubMed]
- Liang, Y.C.; Huang, Y.T.; Tsai, S.H.; Lin-Shiau, S.Y.; Chen, C.F.; Lin, J.K. Suppression of inducible cyclooxygenase and inducible nitric oxide synthase by apigenin and related flavonoids in mouse macrophages. Carcinogenesis 1999, 20, 1945–1952. [Google Scholar] [CrossRef] [PubMed]
- Hamalainenalainen, M.; Nieminen, R.; Vuorela, P.; Heinonen, M.; Moilanen, E. Anti-Inflammatory effects of flavonoids: Genistein, kaempferol, quercetin, and daidzein inhibit STAT-1 and NF-κB activations, whereas flavone, isorhamnetin, naringenin, and pelargonidin inhibit only NF-κB activation along with their inhibitory effect on iNOS expression and NO production in activated macrophages. Mediat. Inflamm. 2007, 4, 45673. [Google Scholar]
- Prouillet, C.; Maziere, J.C.; Maziere, C.; Wattel, A.; Brazier, M.; Kamel, S. Stimulatory effect of naturally occurring flavonols quercetin and kaempferol on alkaline phosphatase activity in MG-63 human osteoblasts through ERK and estrogen receptor pathway. Biochem. Pharmacol. 2004, 67, 1307–1313. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.; Ma, X.; Meng, F.; Li, G. The electron transfer reactivity of kaempferol and its interaction with amino acid residues. Bioelectrochemistry 2008, 72, 169–173. [Google Scholar] [CrossRef] [PubMed]
- Srinivasan, M.; Sudheer, A.R.; P.Menon, V. Ferulic Acid: Therapeutic potential through its antioxidant property. Clin. Biochem. Nutr. 2007, 40, 92–100. [Google Scholar] [CrossRef] [PubMed]
- BSS PLUS® Sterile Irrigating Solution. Available online: https://www.accessdata.fda.gov/drugsatfda_docs/label/2013/018469s052lbl.pdf (accessed on 28 May 2017).
- Schulz, D.; Iliev, M.E.; Frueh, B.E.; Goldblum, D. In Vivo pachymetry in normal eyes of rats, mice and rabbits with the optical low coherence reflectometer. Vis. Res. 2003, 43, 723–728. [Google Scholar] [CrossRef]
- Wang, X.; Wu, Q. Normal corneal thickness measurements in pigmented rabbits usingspectral-domain anterior segment optical coherence tomography. Vet. Ophthalmol. 2013, 16, 130–134. [Google Scholar] [CrossRef] [PubMed]
- Burstein, N.L. Preservative cytotoxic threshold for benzalkonium chloride and chlorhexidine digluconate in cat and rabbit corneas. Investig. Ophthalmol. Vis. Sci. 1980, 19, 308–313. [Google Scholar]
- Lin, Z.; Liu, X.; Zhou, T.; Wang, Y.; Bai, L.; He, H.; Liu, Z. A mouse dry eye model induced by topical administration of benzalkonium chloride. Mol. Vis. 2011, 17, 257–264. [Google Scholar] [PubMed]
- Xiong, C.; Chen, D.; Liu, J.; Liu, B.; Li, N.; Zhou, Y.; Liang, X.; Ma, P.; Ye, C.; Ge, J.; et al. A rabbit dry eye model induced by topical medication of a preservative benzalkonium chloride. Investig. Ophthalmol. Vis. Sci. 2008, 49, 1850–1856. [Google Scholar] [CrossRef] [PubMed]
- Kwon, Y.S.; Park, J.S.; Yun, S.H.; Ku, S.K.; Jang, K.H. A dog dry eye model induced by benzalkonium chloride. Investig. Ophthalmol. Vis. Sci. 2011, 52, 3765. [Google Scholar]
- Cavet, M.E.; Harrington, K.L.; Vollmer, T.R.; Ward, K.W.; Zhang, J.Z. Anti-inflammatory and anti-oxidative effects of the green tea polyphenol epigallocatechin gallate in human corneal epithelial cells. Mol. Vis. 2011, 17, 533–542. [Google Scholar] [PubMed]
- Li, C.; Song, Y.; Luan, S.; Wan, P.; Li, N.; Tang, J.; Han, Y.; Xiong, C.; Wang, Z. Research on the stability of a rabbit dry eye model induced by topical application of the preservative benzalkonium chloride. PLoS ONE 2012, 7, e33688. [Google Scholar]
- Baudouin, C.; Liang, H.; Hamard, P.; Riancho, L.; Creuzot, G.C.; Warnet, J.M.; Brignole, B.F. The ocular surface of glaucoma patients treated over the long term expresses inflammatory markers related to both T-helper 1 and T-helper 2 pathways. Ophthalmology 2008, 115, 109–115. [Google Scholar] [CrossRef] [PubMed]
- Yang, Q.; Zhang, Y.; Liu, X.; Wang, N.; Song, Z.; Wu, K. A comparison of the effects of benzalkonium chloride on ocular surfaces between C57BL/6 and BALB/c Mice. Int. J. Mol. Sci. 2017, 18, 509. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.H.; Kim, E.J.; Kim, Y.H.; Kim, Y.I.; Lee, S.H.; Jung, J.C.; Lee, K.W.; Park, Y.J. In Vivo effects of preservative-free and preserved prostaglandin analogs: Mouse ocular surface study. Korean J. Ophthalmol. 2015, 29, 270–279. [Google Scholar] [CrossRef] [PubMed]
- Tseng, C.; Chen, Z.; Renn, T.; Hsiao, S.; Burnouf, T. Solvent/detergent virally inactivated serum eye drops restore healthy ocular epithelium in a rabbit model of dry-eye syndrome. PLoS ONE 2016, 11, e0153573. [Google Scholar] [CrossRef] [PubMed]
- Li, N.; Deng, X.; Gao, Y.; Zhang, S.; He, M.; Zhao, D. Establishment of the mild, moderate and severe dry eye models using three methods in rabbits. BMC Ophthalmol. 2013, 13, 50. [Google Scholar] [CrossRef] [PubMed]



| Group | pH | Osmotic Pressure (mOsm/kg) | Refractive Index (RI) |
|---|---|---|---|
| Normal human tears | 6.5–7.6 [20] | 260–340 [21] | 1.3369 ± 0.0011 [22] |
| BS | 7.15 ± 0.05 | 301.3 ± 0.6 | 1.3345 ± 0.0001 |
| BS + FA100 | 7.20 ± 0.02 | 306.7 ± 1.5 | 1.3345 ± 0.0001 |
| BS + KM1 | 7.20 ± 0.04 | 301.7 ± 1.2 | 1.3344 ± 0.0001 |
| BS + FA100/KM1 | 7.25 ± 0.15 | 302.0 ± 1.0 | 1.3344 ± 0.0000 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Chen, H.-C.; Chen, Z.-Y.; Wang, T.-J.; Drew, V.J.; Tseng, C.-L.; Fang, H.-W.; Lin, F.-H. Herbal Supplement in a Buffer for Dry Eye Syndrome Treatment. Int. J. Mol. Sci. 2017, 18, 1697. https://doi.org/10.3390/ijms18081697
Chen H-C, Chen Z-Y, Wang T-J, Drew VJ, Tseng C-L, Fang H-W, Lin F-H. Herbal Supplement in a Buffer for Dry Eye Syndrome Treatment. International Journal of Molecular Sciences. 2017; 18(8):1697. https://doi.org/10.3390/ijms18081697
Chicago/Turabian StyleChen, Hung-Chang, Zhi-Yu Chen, Tsung-Jen Wang, Victor J. Drew, Ching-Li Tseng, Hsu-Wei Fang, and Feng-Huei Lin. 2017. "Herbal Supplement in a Buffer for Dry Eye Syndrome Treatment" International Journal of Molecular Sciences 18, no. 8: 1697. https://doi.org/10.3390/ijms18081697
APA StyleChen, H.-C., Chen, Z.-Y., Wang, T.-J., Drew, V. J., Tseng, C.-L., Fang, H.-W., & Lin, F.-H. (2017). Herbal Supplement in a Buffer for Dry Eye Syndrome Treatment. International Journal of Molecular Sciences, 18(8), 1697. https://doi.org/10.3390/ijms18081697







