Correlation between Patient-Reported Symptoms and Ankle-Brachial Index after Revascularization for Peripheral Arterial Disease
Abstract
:1. Introduction
2. Results
| Variables | Total (n = 149) | Endovascular Revascularization (n = 100) | Bypass Surgery (n = 49) | p Value |
|---|---|---|---|---|
| Age, years | 70.3 ± 9.7 | 70.1 ± 9.9 | 70.7 ± 9.3 | 0.704 |
| Male, % | 125 (84%) | 82 (82%) | 43 (88%) | 0.258 |
| Systolic BP, mmHg | 125.1 ± 18.2 | 124.4 ± 19.8 | 126.7 ± 14.6 | 0.424 |
| Diastolic BP, mmHg | 77.8 ± 10.6 | 77.6 ± 10.6 | 78.2 ± 10.6 | 0.749 |
| Heart rate, bpm | 80.4 ± 13.0 | 80.6 ± 13.6 | 80.2 ± 11.9 | 0.870 |
| Total cholesterol | 163.8 ± 48.2 | 162.4 ± 53.7 | 166.6 ± 34.5 | 0.576 |
| LDL, mg/dL | 103.4 ± 47.5 | 105.6 ± 47.1 | 98.9 ± 48.9 | 0.568 |
| HDL, mg/dL | 40.6 ± 28.8 | 41.6 ± 33.9 | 38.5 ± 14.1 | 0.572 |
| C-reactive protein, mg/L | 4.2 ± 16.1 | 3.85 ± 15.4 | 0.96 ± 2.65 | 0.350 |
| Ankle brachial index | 0.75 ± 0.24 | 0.77 ± 0.24 | 0.70 ± 0.24 | 0.181 |
| Hypertension, % | 95 (64%) | 63 (63%) | 32 (65%) | 0.465 |
| Diabetes, % | 58 (39%) | 38 (38%) | 20 (41%) | 0.438 |
| Dyslipidemia, % | 92 (62%) | 62 (62%) | 30 (61%) | 0.533 |
| Current smoker, % | 48 (32%) | 33 (33%) | 15 (31%) | 0.461 |
| Ex-smoker, % | 21 (14%) | 11 (11%) | 10 (20%) | 0.099 |
| Aspirin, % | 87 (58%) | 60 (60%) | 27 (55%) | 0.329 |
| Clopidogrel, % | 29 (20%) | 20 (20%) | 9 (18%) | 0.500 |
| Cilostazol, % | 10 (7%) | 8 (8%) | 2 (4%) | 0.302 |
| BP medication, % | 88 (59%) | 59 (59%) | 29 (59%) | 0.782 |
| Statin, % | 62 (42%) | 48 (48%) | 14 (29%) | 0.024 |
| Location | ||||
| Aorto-iliac | 48 (32.2%) | 46 (46%) | 2 (4%) | <0.001 |
| Femoropopliteal | 101 (67.8%) | 54 (54%) | 47 (96%) | <0.001 |
2.1. Post-Revascularization Outcome Assessments
| Assessments | Pre-Revascularization | Post-Revascularization | Changes (Δ) | p Value |
|---|---|---|---|---|
| ABI in non-treated limb | 0.94 ± 0.22 | 0.97 ± 0.16 | 0.02 ± 0.17 | 0.360 |
| ABI in treated limb | 0.65 ± 0.17 | 0.94 ± 0.20 | 0.31 ± 0.23 | <0.001 |
| Physical function | 22.4 ± 12.9 | 81.6 ± 19.9 | 59.2 ± 19.8 | <0.001 |
| Symptom | 22.7 ± 19.6 | 83.2 ± 16.7 | 60.5 ± 25.2 | <0.001 |
| Stability | 41.6 ± 14.8 | 87.6 ± 19.4 | 46.0 ± 24.3 | <0.001 |
| Treatment satisfaction | 36.8 ± 10.6 | 69.4 ± 16.1 | 32.6 ± 17.5 | <0.001 |
| Quality of life | 22.1 ± 9.5 | 73.0 ± 18.5 | 50.9 ± 20.4 | <0.001 |
| Social limitation | 41.8 ± 19.1 | 87.8 ± 15.5 | 46.0 ± 20.7 | <0.001 |
| Summary | 32.1 ± 11.3 | 81.4 ± 16.4 | 49.3 ± 15.8 | <0.001 |
2.2. Correlation between PAQ Score and ABI
| Assessments | Endovascular Revascularization (n = 100) | Open Surgery (n = 49) | p Value |
|---|---|---|---|
| Baseline ABI in treated limb | 0.68 ± 0.18 | 0.59 ± 0.12 | 0.007 |
| Postoperative ABI in treated limb | 0.96 ± 0.20 | 0.93 ± 0.20 | 0.519 |
| ΔABI in treated limb | 0.29 ± 0. 24 | 0.34 ± 0.19 | 0.391 |
| Baseline physical function | 21.3 ± 11.9 | 24.7 ± 14.7 | 0.164 |
| Postoperative physical function | 80.0 ± 21.9 | 84.9 ± 14.6 | 0.105 |
| ΔPhysical function | 58.7 ± 18.8 | 60.3 ± 19.2 | 0.641 |
| Baseline symptom | 19.8 ± 17.9 | 28.6 ± 21.7 | 0.016 |
| Postoperative symptom | 82.6 ± 17.8 | 84.2 ± 14.4 | 0.584 |
| Δsymptom | 62.9 ± 23.3 | 55.7 ± 28.5 | 0.127 |
| Baseline stability | 41.7 ± 13.9 | 41.3 ± 16.8 | 0.890 |
| Postoperative stability | 86.0 ± 20.8 | 90.8 ± 15.9 | 0.120 |
| Δstability | 44.3 ± 24.2 | 49.5 ± 24.4 | 0.224 |
| Baseline treatment satisfaction | 37.4 ± 9.7 | 35.6 ± 12.3 | 0.311 |
| Postoperative treatment satisfaction | 70.8 ± 16.0 | 66.7 ± 16.2 | 0.147 |
| ΔTreatment satisfaction | 33.3 ± 16.1 | 31.1 ± 20.1 | 0.505 |
| Baseline quality of life | 20.0 ± 7.7 | 26.5 ± 11.3 | 0.001 |
| Postoperative quality of life | 72.8 ± 16.0 | 73.5 ± 18.3 | 0.845 |
| ΔQuality of life | 52.8 ± 18.8 | 47.0 ± 23.0 | 0.125 |
| Baseline social limitation | 38.4 ± 17.2 | 48.6 ± 21.0 | 0.002 |
| Postoperative social limitation | 86.9 ± 16.5 | 89.6 ± 13.2 | 0.283 |
| ΔSocial limitation | 48.5 ± 17.8 | 41.0 ± 25.0 | 0.037 |
| Baseline summary | 30.6 ± 10.0 | 35.4 ± 13.1 | 0.025 |
| Postoperative summary | 80.6 ± 17.4 | 83.1 ± 14.0 | 0.353 |
| Δsummary | 50.0 ± 14.0 | 47.7 ± 19.0 | 0.438 |
| PAQ Domain | Correlation Coefficient | p Value |
|---|---|---|
| Physical function | 0.337 | 0.001 |
| Stability | −0.122 | 0.231 |
| Symptom | 0.376 | <0.001 |
| Treatment satisfaction | 0.427 | <0.001 |
| Quality of life | 0.371 | 0.001 |
| Social limitation | 0.333 | 0.001 |
| Summary score | 0.374 | <0.001 |
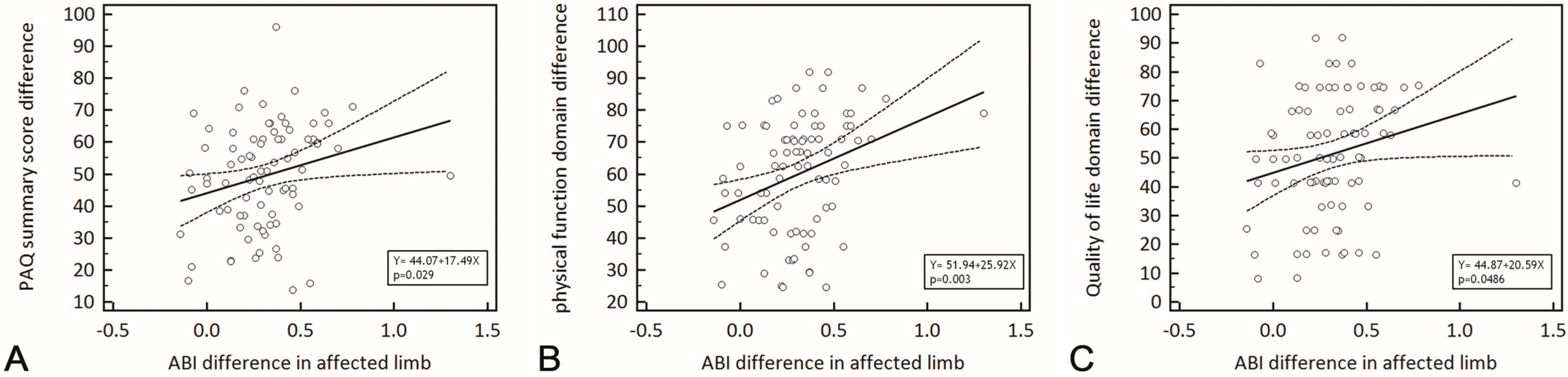
2.3. Differences in PAQ Scores in Patients Who Did or Did not Respond to Revascularization
| Assessments | Responders (n = 116) | Non-Responders (n = 33) | p Value |
|---|---|---|---|
| ΔABI, ischemic side | 0.39 ± 0.18 | 0.02 ± 0.10 | <0.001 |
| Post-physical function | 85.4 ± 16.7 | 77.1 ± 16.3 | 0.066 |
| Post-symptom score | 86.3 ± 15.2 | 77.3 ± 16.5 | 0.033 |
| Post-stability | 88.1 ± 21.5 | 88.9 ± 17.6 | 0.886 |
| Post-treatment satisfaction | 73.0 ± 14.5 | 63.0 ± 19.8 | 0.020 |
| Post-quality of life | 75.7 ± 17.9 | 67.1 ± 18.2 | 0.080 |
| Post-social limitation | 90.2 ± 14.0 | 81.5 ± 17.7 | 0.031 |
| Post-summary score | 84.4 ± 15.0 | 75.8 ± 16.4 | 0.039 |
| ΔPhysical function | 61.9 ± 18.5 | 53.3 ± 15.2 | 0.051 |
| ΔSymptom | 61.3 ± 25.3 | 53.7 ± 22.8 | 0.234 |
| ΔStability | 44.9 ± 26.0 | 47.9 ± 21.7 | 0.620 |
| ΔTreatment satisfaction | 35.5 ± 17.7 | 25.9 ± 18.7 | 0.047 |
| ΔQuality of life | 53.1 ± 20.8 | 44.7 ± 22.3 | 0.165 |
| ΔSocial limitation | 46.5 ± 20.5 | 43.5 ± 20.5 | 0.585 |
| ΔSummary | 51.0 ± 16.3 | 44.2 ± 16.0 | 0.123 |
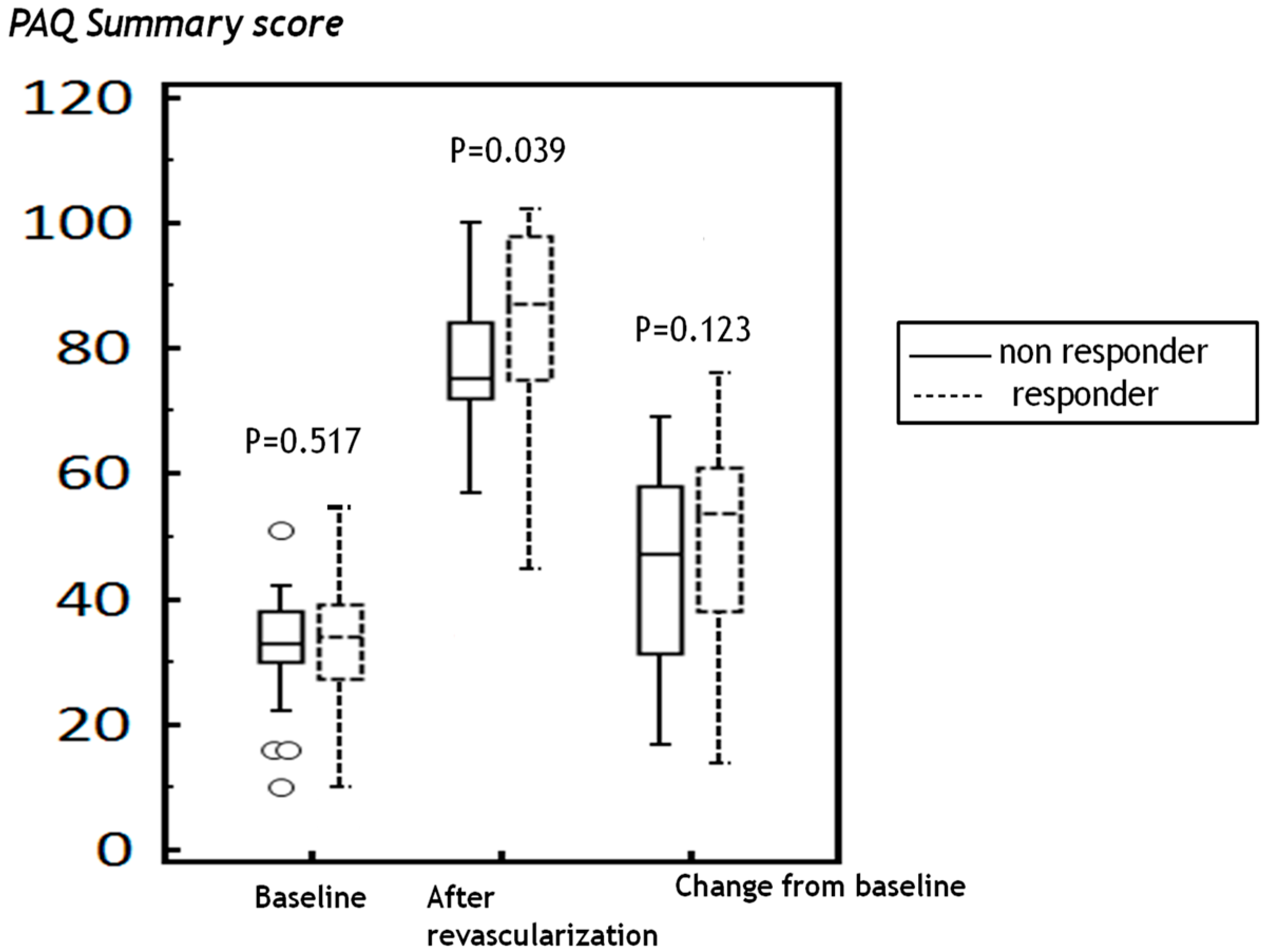
3. Discussion
4. Experimental Section
4.1. Participants and Selection Criteria
4.2. Questionnaires Administered
4.3. Measurement of Ankle Brachial Index
4.4. Statistical Analyses
5. Conclusions
Supplementary Materials
Author Contributions
Conflicts of Interest
References
- McDermott, M.M.; Liu, K.; Greenland, P.; Guralnik, J.M.; Criqui, M.H.; Chan, C.; Pearce, W.H.; Schneider, J.R.; Ferrucci, L.; Celic, L.; et al. Functional decline in peripheral arterial disease: Associations with the ankle brachial index and leg symptoms. JAMA 2004, 292, 453–461. [Google Scholar] [CrossRef] [PubMed]
- Selvin, E.; Erlinger, T.P. Prevalence of and risk factors for peripheral arterial disease in the United States: Results from the National Health and Nutrition Examination Survey, 1999–2000. Circulation 2004, 110, 738–743. [Google Scholar] [CrossRef] [PubMed]
- Mehta, T.; Venkata, S.A.; Chetter, I.; McCollum, P. Assessing the validity and responsiveness of disease-specific quality of life instruments in intermittent claudication. Eur. J. Vasc. Endovasc. Surg. 2006, 31, 46–52. [Google Scholar] [CrossRef] [PubMed]
- Aboyans, V.; Lacroix, P.; Doucet, S.; Preux, P.M.; Criqui, M.H.; Laskar, M. Diagnosis of peripheral arterial disease in general practice: can the ankle-brachial index be measured either by pulse palpation or an automatic blood pressure device? Int. J. Clin. Pract. 2008, 62, 1001–1007. [Google Scholar] [CrossRef] [PubMed]
- Spertus, J.; Jones, P.; Poler, S.; Rocha-Singh, K. The peripheral artery questionnaire: A new disease-specific health status measure for patients with peripheral arterial disease. Am. Heart J. 2004, 147, 301–308. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.H.; Cho, K.I.; Spertus, J.; Kim, S.M. Cross-cultural adaptation and validation of the Peripheral Artery Questionnaire: Korean version for patients with peripheral vascular diseases. Vasc. Med. 2012, 17, 215–222. [Google Scholar] [CrossRef] [PubMed]
- Kim, B.H.; Cho, K.I.; Spertus, J.; Park, Y.H.; Je, H.G.; Shin, M.S.; Lee, J.H.; Jang, J.S. Peripheral Artery Questionnaire improves ankle brachial index screening in symptomatic patients with peripheral artery disease. Int. J. Clin. Pract. 2014, 68, 1488–1495. [Google Scholar] [CrossRef] [PubMed]
- Meijer, W.T.; Hoes, A.W.; Rutgers, D.; Bots, M.L.; Hofman, A.; Grobbee, D.E. Peripheral arterial disease in the elderly: The rotterdam study. Arterioscler. Thromb. Vasc. Biol. 1998, 18, 185–192. [Google Scholar] [CrossRef] [PubMed]
- Feinglass, J.; McCarthy, W.J.; Slavensky, R.; Manheim, L.M.; Martin, G.J. Effect of lower extremity blood pressure on physical functioning in patients with intermittent claudication. J. Vasc. Surg. 1996, 24, 503–511. [Google Scholar] [CrossRef] [PubMed]
- Newman, A.B.; Shemanski, L.; Manolio, T.A.; Cushman, M.; Mittelmark, M.; Polak, J.F.; Powe, N.R.; Siscovick, D. Ankle-arm index as a predictor of cardiovascular disease and mortality in the Cardiovascular Health Study. Arterioscler. Thromb. Vasc. Biol. 1999, 19, 538–545. [Google Scholar] [CrossRef] [PubMed]
- Doobay, A.V.; Anand, S.S. Sensitivity and specificity of the ankle-brachial index to predict future cardiovascular outcomes: A systematic review. Arterioscler. Thromb. Vasc. Biol. 2005, 25, 1463–1469. [Google Scholar] [CrossRef] [PubMed]
- Atkins, L.M.; Gardner, A.W. The relationship between lower extremity functional strength and severity of peripheral arterial disease. Angiology 2004, 55, 347–355. [Google Scholar] [CrossRef] [PubMed]
- Szuba, A.; Oka, R.K.; Harada, R.; Cooke, J.P. Limb hemodynamics are not predictive of functional capacity in patients with PAD. Vasc. Med. 2006, 11, 155–163. [Google Scholar] [CrossRef] [PubMed]
- Safley, D.M.; House, J.A.; Laster, S.B.; Daniel, W.C.; Spertus, J.A.; Marso, S.P. Quantifying improvement in symptoms, functioning, and quality of life after peripheral endovascular revascularization. Circulation 2007, 115, 569–575. [Google Scholar] [CrossRef] [PubMed]
- Hoeks, S.E.; Smolderen, K.G.; Scholte, O.R.W.J.; Verhagen, H.J.; Spertus, J.A.; Poldermans, D.J. Clinical validity of a disease-specific health status questionnaire: the peripheral artery questionnaire. Vasc. Surg. 2009, 49, 371–377. [Google Scholar] [CrossRef]
- Murphy, T.P.; Cutlip, D.E.; Regensteiner, J.G.; Mohler, E.R.; Cohen, D.J.; Reynolds, M.R.; Massaro, J.M.; Lewis, B.A.; Cerezo, J.; Oldenburg, N.C.; et al. Supervised exercise versus primary stenting for claudication resulting from aortoiliac peripheral artery disease: Six-month outcomes from the claudication: Exercise versus endoluminal revascularization (CLEVER) study. Circulation 2012, 125, 130–139. [Google Scholar] [CrossRef] [PubMed]
- Hiatt, W.R.; Hirsch, A.T.; Regensteiner, J.G.; Brass, E.P. Clinical trials for claudication: Assessment of exercise performance, functional status, and clinical end points. Circulation 1995, 92, 614–621. [Google Scholar] [CrossRef] [PubMed]
- Murphy, T.P.; Soares, G.M.; Kim, H.M.; Ahn, S.H.; Haas, R.A. Quality of life and exercise performance after aortoiliac stent placement for claudication. J. Vasc. Interv. Radiol. 2005, 16, 947–953. [Google Scholar] [CrossRef] [PubMed]
- Bosch, J.L.; Hunink, M.G. Comparison of the Health Utilities Index Mark 3 (HUI3) and the EuroQol EQ-5D in patients treated for intermittent claudication. Qual. Life Res. 2000, 9, 591–601. [Google Scholar] [CrossRef] [PubMed]
- Taft, C.; Karlsson, J.; Gelin, J.; Jivegard, L.; Sandstrom, R.; Arfvidsson, B.; Dahllöf, A.G.; Lundholm, K.; Sullivan, M. Treatment efficacy of intermittent claudication by invasive therapy, supervised physical exercise training compared to no treatment in unselected randomised patients II: One-year results of health-related quality of life. Eur. J. Vasc. Endovasc. Surg. 2001, 22, 114–123. [Google Scholar] [CrossRef] [PubMed]
- Chetter, I.C.; Spark, J.I.; Scott, D.J.; Kester, R.C. Does angioplasty improve the quality of life for claudicants?: A prospective study. Ann. Vasc. Surg. 1999, 13, 93–103. [Google Scholar] [CrossRef] [PubMed]
- Patterson, R.B.; Pinto, B.; Marcus, B.; Colucci, A.; Braun, T.; Roberts, M. Value of a supervised exercise program for the therapy of arterial claudication. J. Vasc. Surg. 1997, 25, 312–318. [Google Scholar] [CrossRef] [PubMed]
- Spronk, S.; Bosch, J.L.; Veen, H.F.; den Hoed, P.T.; Hunink, M.G. Intermittent claudication: functional capacity and quality of life after exercise training or percutaneous transluminal angioplasty—Systematic review. Radiology 2005, 235, 833–842. [Google Scholar] [CrossRef] [PubMed]
- Ahimastos, A.A.; Pappas, E.P.; Buttner, P.G.; Walker, P.J.; Kingwell, B.A.; Golledge, J. A meta-analysis of the outcome of endovascular and noninvasive therapies in the treatment of intermittent claudication. J. Vasc. Surg. 2011, 54, 1511–1521. [Google Scholar] [CrossRef] [PubMed]
- Murphy, T.P.; Reynolds, M.R.; Cohen, D.J.; Regensteiner, J.G.; Massaro, J.M.; Cutlip, D.E.; Mohler, E.R.; Cerezo, J.; Oldenburg, N.C.; Thum, C.C.; et al. Correlation of patient-reported symptom outcomes and treadmill test outcomes after treatment for aortoiliac claudication. J. Vasc. Interv. Radiol. 2013, 24, 1427–1435. [Google Scholar] [CrossRef] [PubMed]
- McDermott, M.M.; Kibbe, M.; Guralnik, J.M.; Pearce, W.H.; Tian, L.; Liao, Y.; Zhao, L.; Criqui, M.H. Comparative effectiveness study of self-directed walking exercise, lower extremity revascularization, and functional decline in peripheral artery disease. J. Vasc. Surg. 2013, 57, 990–996. [Google Scholar] [CrossRef] [PubMed]
- Setacci, C.; de Donato, G.; Teraa, M.; Moll, F.L.; Ricco, J.B.; Becker, F.; Robert-Ebadi, H.; Cao, P.; Eckstein, H.H.; de Rango, P.; et al. Chapter IV: Treatment of critical limb ischaemia. Eur. J. Vasc. Endovasc. Surg. 2011, 42, S43–S59. [Google Scholar] [CrossRef] [PubMed]
- McDermott, M.M.; Criqui, M.H.; Liu, K.; Guralnik, J.M.; Greenland, P.; Martin, G.J.; Pearce, W. Lower ankle brachial index calculated by averaging the dorsalis pedis and posterior tibial arterial pressures is most closely associated with leg functioning in peripheral arterial disease. J. Vasc. Surg. 2000, 32, 1164–1171. [Google Scholar] [CrossRef] [PubMed]
© 2015 by the authors; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Je, H.G.; Kim, B.H.; Cho, K.I.; Jang, J.S.; Park, Y.H.; Spertus, J. Correlation between Patient-Reported Symptoms and Ankle-Brachial Index after Revascularization for Peripheral Arterial Disease. Int. J. Mol. Sci. 2015, 16, 11355-11368. https://doi.org/10.3390/ijms160511355
Je HG, Kim BH, Cho KI, Jang JS, Park YH, Spertus J. Correlation between Patient-Reported Symptoms and Ankle-Brachial Index after Revascularization for Peripheral Arterial Disease. International Journal of Molecular Sciences. 2015; 16(5):11355-11368. https://doi.org/10.3390/ijms160511355
Chicago/Turabian StyleJe, Hyung Gon, Bo Hyun Kim, Kyoung Im Cho, Jae Sik Jang, Yong Hyun Park, and John Spertus. 2015. "Correlation between Patient-Reported Symptoms and Ankle-Brachial Index after Revascularization for Peripheral Arterial Disease" International Journal of Molecular Sciences 16, no. 5: 11355-11368. https://doi.org/10.3390/ijms160511355
APA StyleJe, H. G., Kim, B. H., Cho, K. I., Jang, J. S., Park, Y. H., & Spertus, J. (2015). Correlation between Patient-Reported Symptoms and Ankle-Brachial Index after Revascularization for Peripheral Arterial Disease. International Journal of Molecular Sciences, 16(5), 11355-11368. https://doi.org/10.3390/ijms160511355





