Co-Delivery of Gemcitabine and Honokiol by Lipid Bilayer-Coated Mesoporous Silica Nanoparticles Enhances Pancreatic Cancer Therapy via Targeting Depletion of Tumor Stroma
Abstract
1. Introduction
2. Results and Discussion
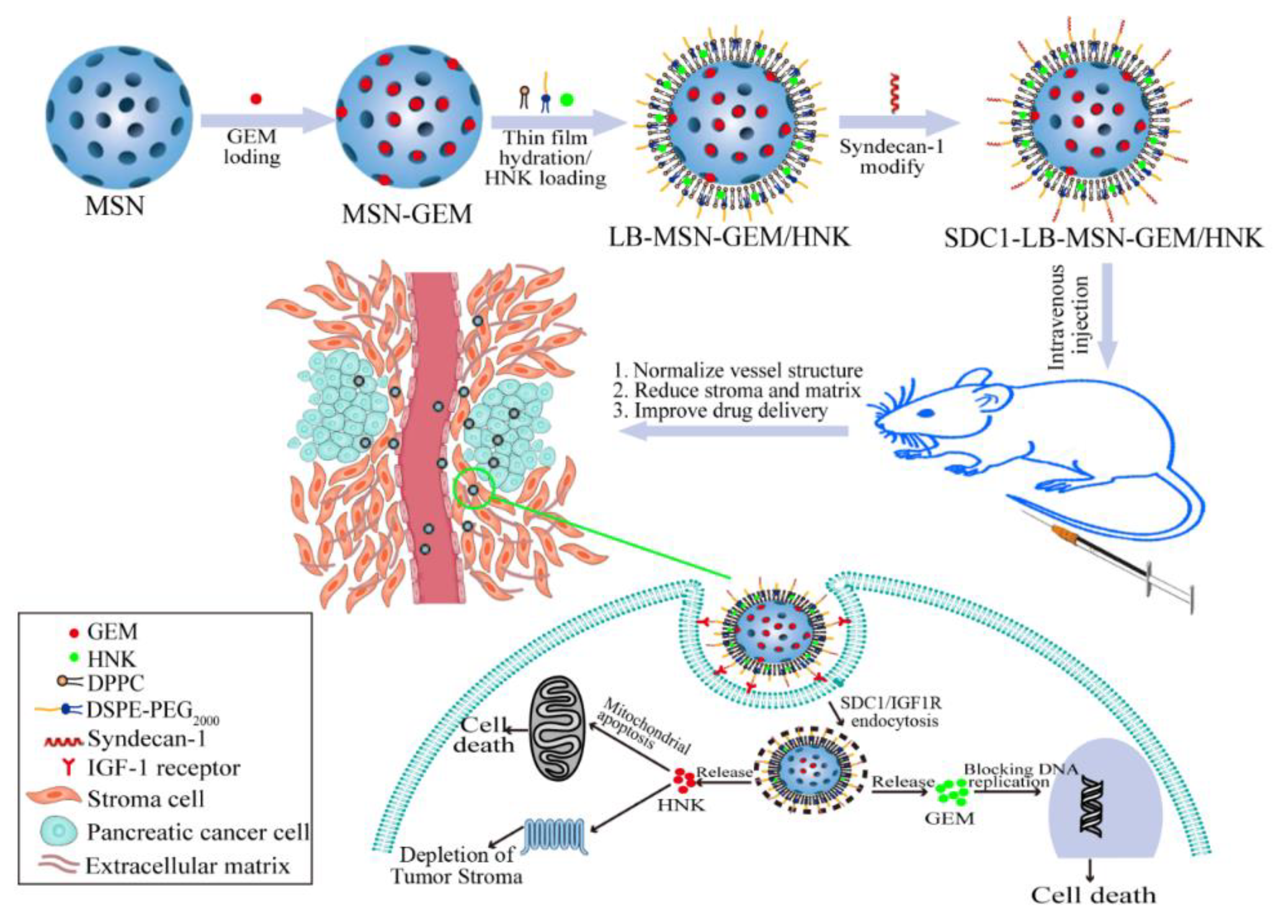
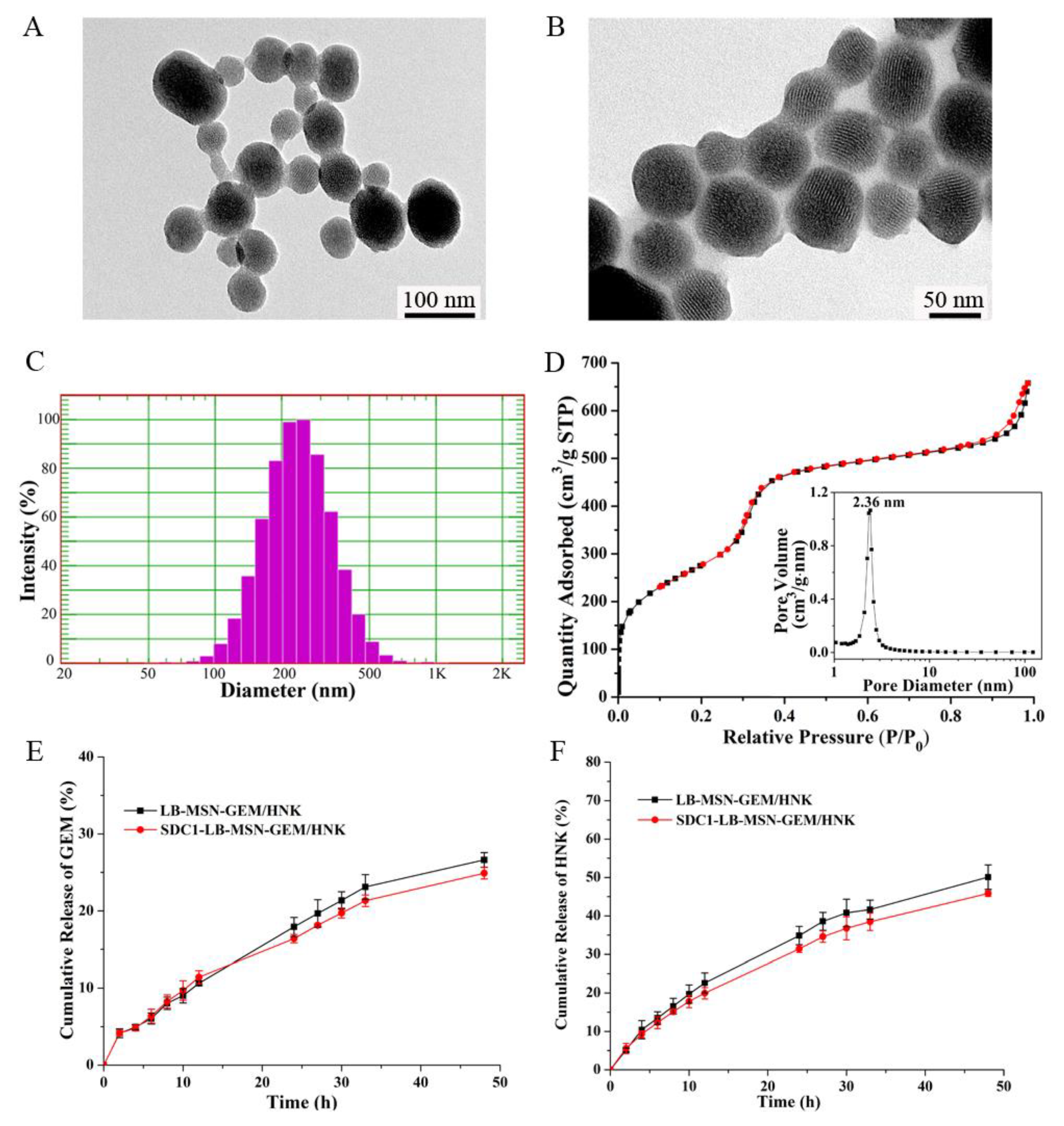
2.1. Preparation and Characterization of SDC1-LB-MSN-GEM/HNK
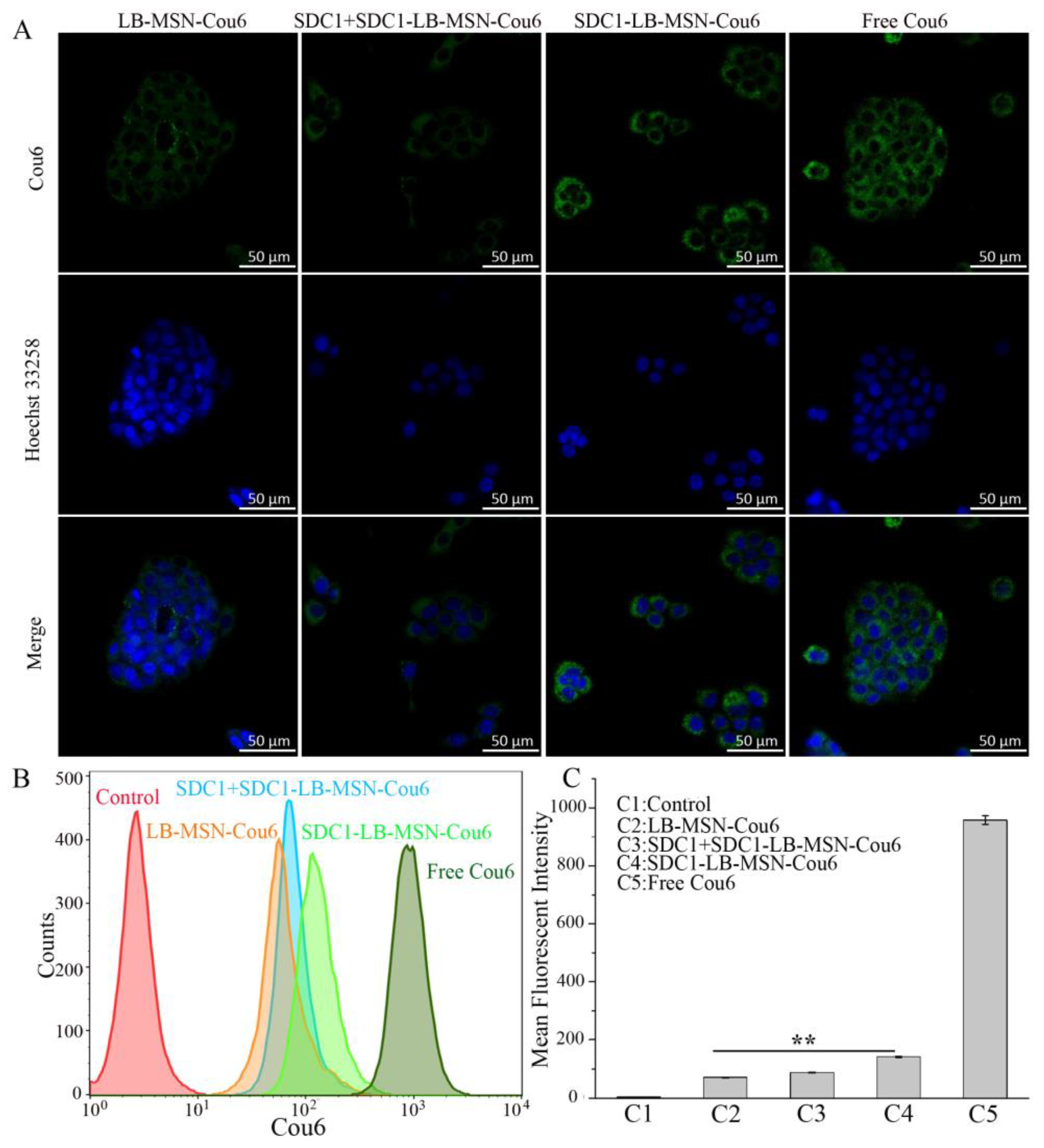
2.2. In Vitro Cellular Uptake of Cou6-Labeled Nanoparticles
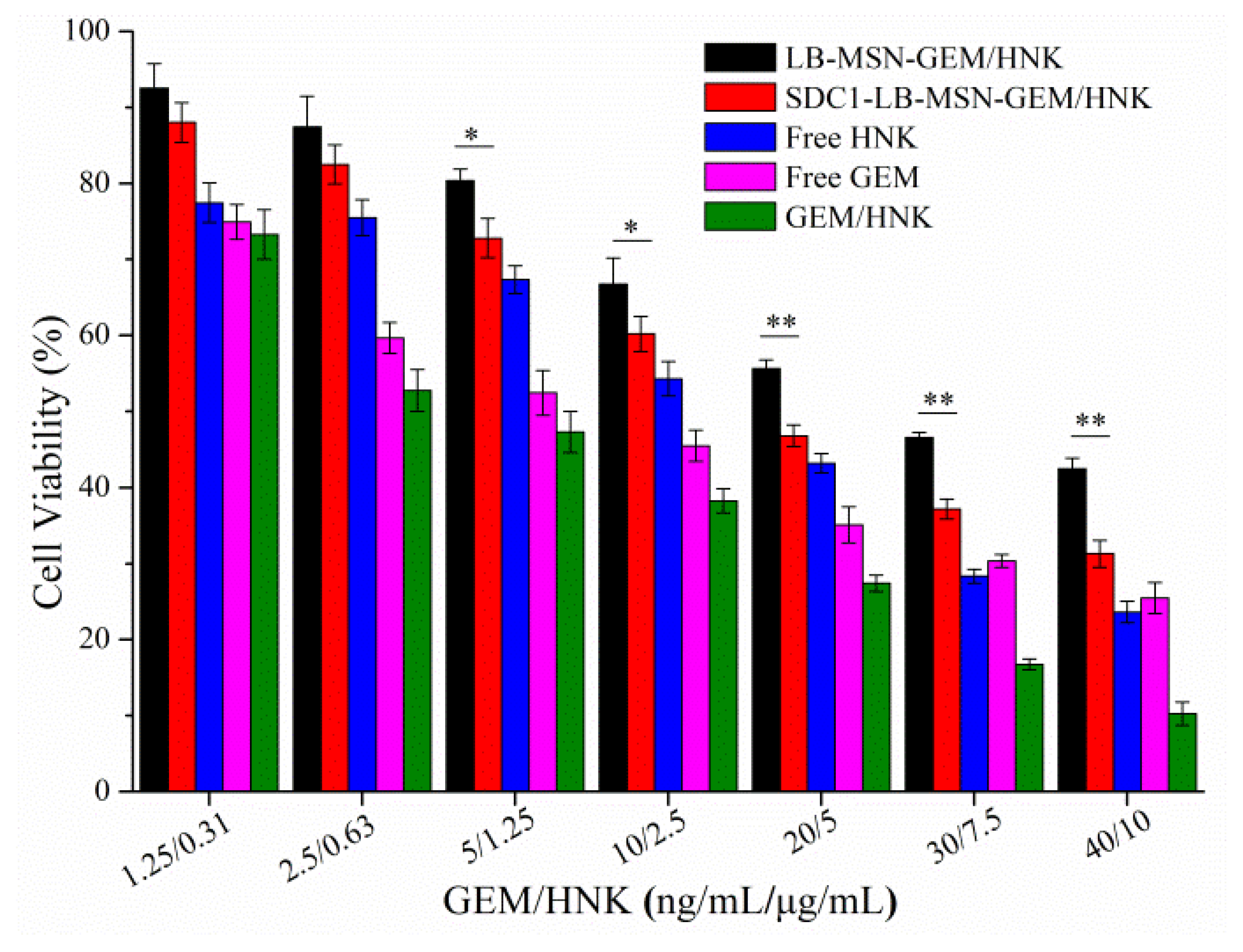
2.3. In Vitro Cytotoxicity Studies of SDC1-LB-MSN-GEM/HNK
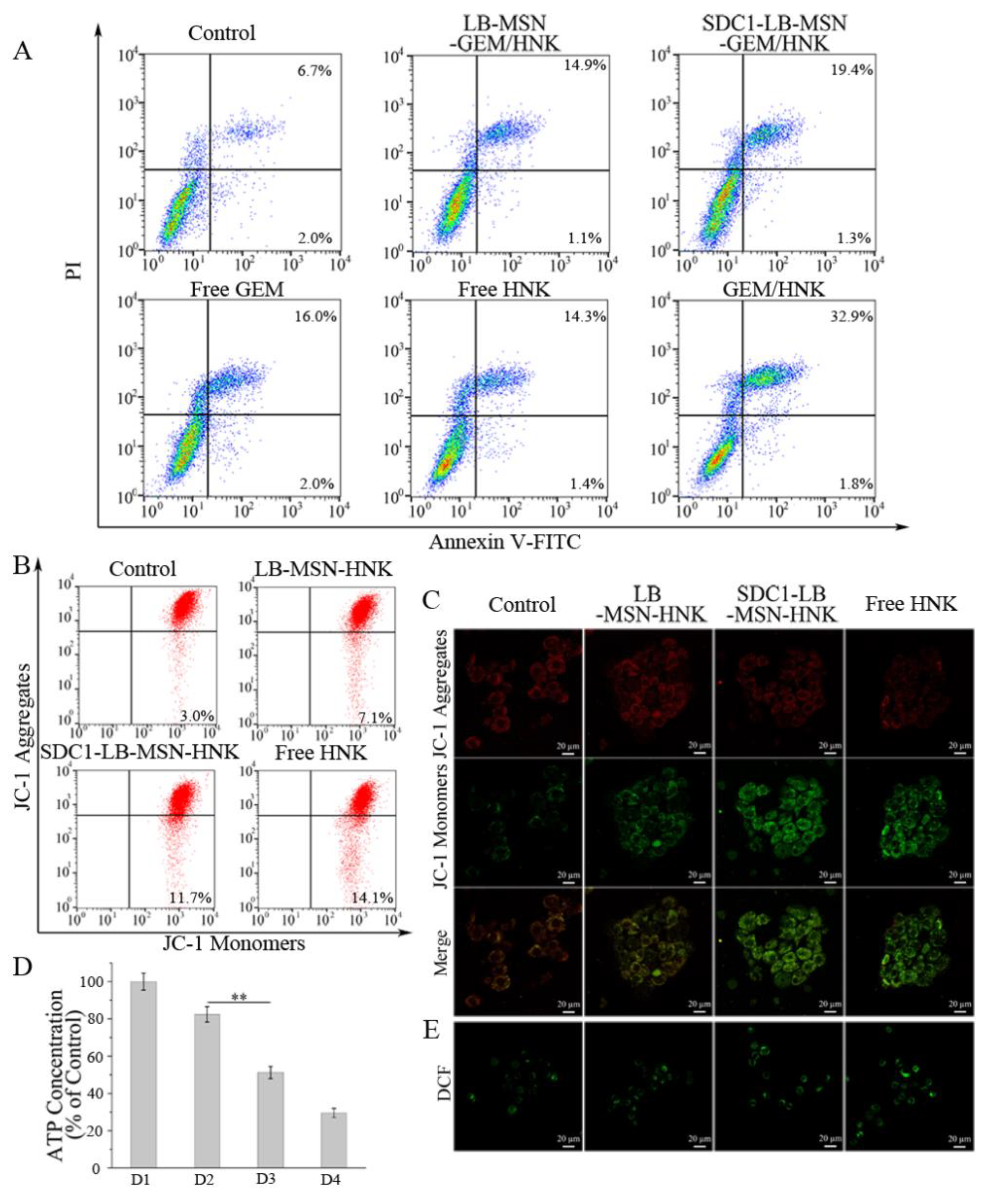
2.4. SDC1-LB-MSN-GEM/HNK Induces Cell Apoptosis and Relevant Mechanism
2.5. In Vivo Tumor Targeting
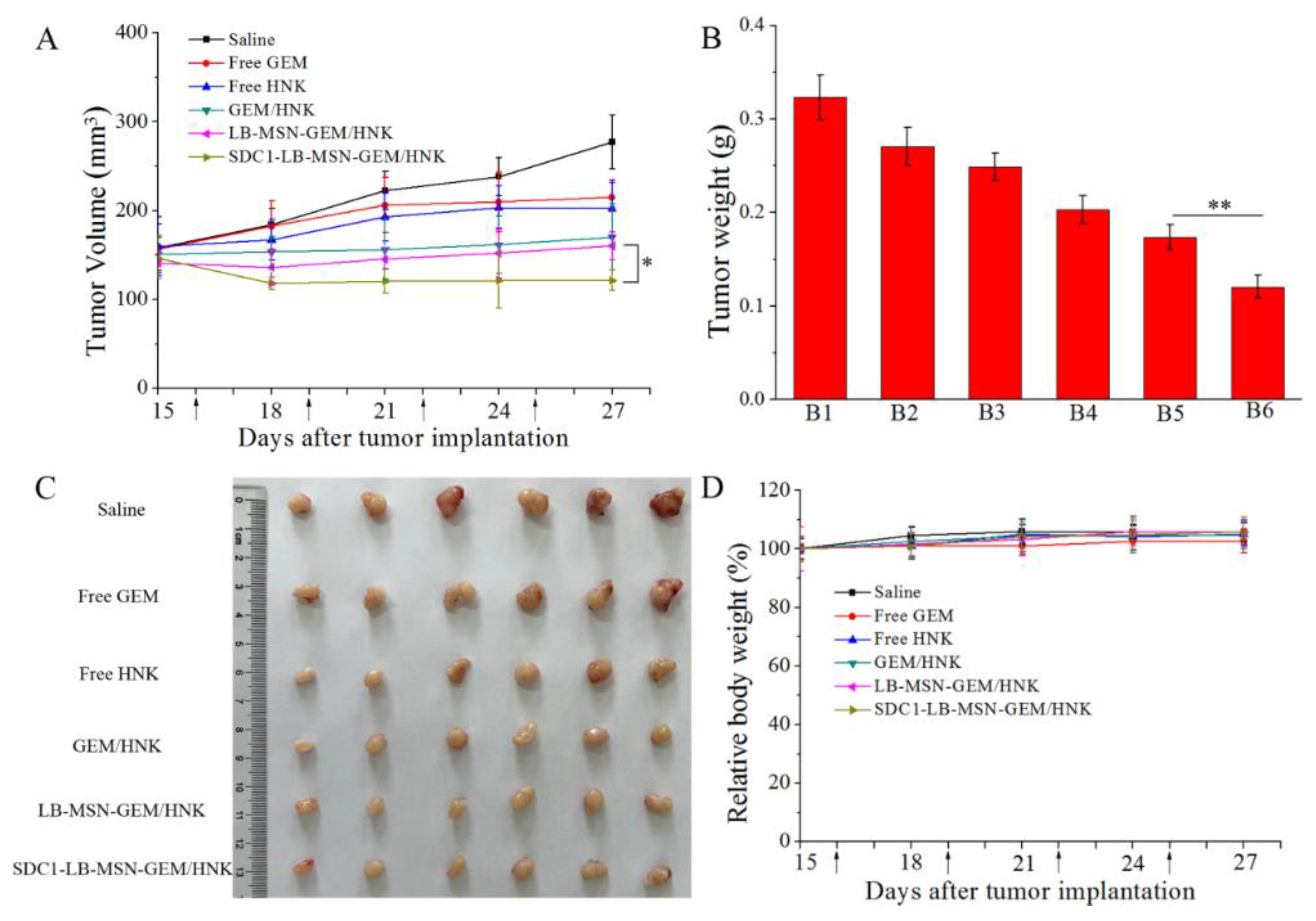
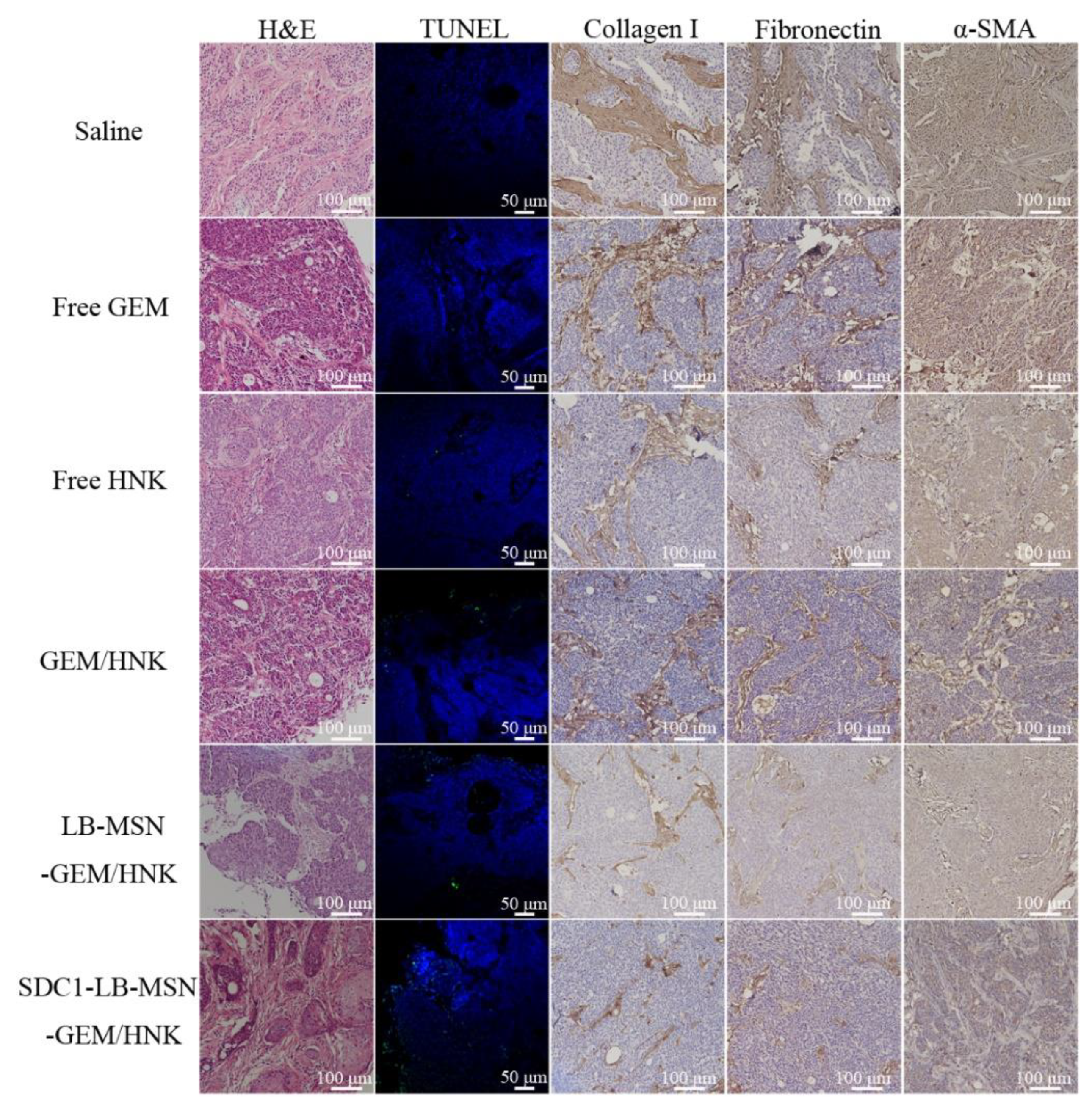
2.6. In Vivo Antitumor Efficiency
3. Materials and Methods
3.1. Chemical Reagents
3.2. Preparation and Characterizations of MSN and SDC1-LB-MSN-GEM/HNK
3.3. Cell Culture and Animals
3.4. Cellular Uptake
3.5. In Vitro Cytotoxicity Assays
3.6. Apoptosis Assays
3.7. Measurement of Mitochondrial Membrane Potential (MMP), ATP, and Reactive Oxygen Species (ROS)
3.8. In Vivo Biodistribution Study
3.9. In Vivo Antitumor Activity
3.10. Statistical Analysis
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Liu, X.S.; Situ, A.; Kang, Y.A.; Villabroza, K.R.; Liao, Y.P.; Chang, C.H.; Donahue, T.; Nel, A.E.; Meng, H. Irinotecan delivery by lipid-coated mesoporous silica nanoparticles shows improved efficacy and safety over liposomes for pancreatic cancer. ACS Nano 2016, 10, 2702–2715. [Google Scholar] [CrossRef]
- Khare, V.; Kour, S.; Alam, N.; Dubey, R.D.; Saneja, A.; Koul, M.; Gupta, A.P.; Singh, D.; Singh, S.K.; Saxena, A.K.; et al. Synthesis, characterization and mechanistic-insight into the anti-proliferative potential of PLGA-gemcitabine conjugate. Int. J. Pharm. 2014, 470, 51–62. [Google Scholar] [CrossRef]
- Zhou, H.Y.; Qian, W.P.; Uckun, F.M.; Wang, L.Y.; Wang, Y.A.; Chen, H.Y.; Kooby, D.; Yu, Q.; Lipowska, M.; Staley, C.A.; et al. IGF1 receptor targeted theranostic nanoparticles for targeted and image-guided therapy of pancreatic cancer. ACS Nano 2015, 9, 7976–7991. [Google Scholar] [CrossRef]
- Fan, F.; Jin, L.J.; Yang, L.H. pH-sensitive nanoparticles composed solely of membrane-disruptive macromolecules for treating pancreatic cancer. ACS Appl. Mater. Interfaces 2021, 13, 12824–12835. [Google Scholar] [CrossRef]
- Meng, H.; Wang, M.Y.; Liu, H.Y.; Liu, X.S.; Situ, A.; Wu, B.; Ji, Z.X.; Chang, C.H.; Nel, A.E. Use of a lipid-coated mesoporous silica nanoparticle platform for synergistic gemcitabine and paclitaxel delivery to human pancreatic cancer in mice. ACS Nano 2015, 9, 3540–3557. [Google Scholar] [CrossRef] [PubMed]
- Jacobetz, M.A.; Chan, D.S.; Neesse, A.; Bapiro, T.E.; Cook, N.; Frese, K.K.; Feig, C.; Nakagawa, T.; Caldwell, M.E.; Zecchini, H.I.; et al. Hyaluronan impairs vascular function and drug delivery in a mouse model of pancreatic cancer. Gut 2013, 62, U112–U153. [Google Scholar] [CrossRef]
- Chen, F.; Wang, T.; Wu, Y.-F.; Gu, Y.; Xu, X.-L.; Zheng, S.; Hu, X. Honokiol: A potent chemotherapy candidate for human colorectal carcinoma. World J. Gastroenterol. 2004, 10, 3459–3463. [Google Scholar] [CrossRef] [PubMed]
- Prasher, P.; Fatima, R.; Sharma, M.; Tynybekov, B.; Alshahrani, A.M.; Atessahin, D.A.; Sharifi-Rad, J.; Calina, D. Honokiol and its analogues as anticancer compounds: Current mechanistic insights and structure-activity relationship. Chem. Biol. Interact. 2023, 386, 110747. [Google Scholar] [CrossRef]
- Zhang, Q.; Wang, J.; Liu, D.; Zhu, W.Q.; Guan, S.; Fan, L.; Cai, D.F. Targeted delivery of honokiol by zein/hyaluronic acid core-shell nanoparticles to suppress breast cancer growth and metastasis. Carbohydr. Polym. 2020, 240, 116325. [Google Scholar] [CrossRef] [PubMed]
- Cho, J.H.; Jeon, Y.J.; Park, S.M.; Shin, J.C.; Lee, T.H.; Jung, S.; Park, H.; Ryu, J.; Chen, H.Y.; Dong, Z.G.; et al. Multifunctional effects of honokiol as an anti-inflammatory and anti-cancer drug in human oral squamous cancer cells and xenograft. Biomaterials 2015, 53, 274–284. [Google Scholar] [CrossRef] [PubMed]
- Rauf, A.; Patel, S.; Imran, M.; Maalik, A.; Arshad, M.U.; Saeed, F.; Mabkhot, Y.N.; Al-Showiman, S.S.; Ahmad, N.; Elsharkawy, E. Honokiol: An anticancer lignan. Biomed. Pharmacother. 2018, 107, 555–562. [Google Scholar] [CrossRef]
- Nagalingam, A.; Arbiser, J.L.; Bonner, M.Y.; Saxena, N.K.; Sharma, D. Honokiol activates AMP-activated protein kinase in breast cancer cells via an LKB1-dependent pathway and inhibits breast carcinogenesis. Breast Cancer Res. 2012, 14, R35. [Google Scholar] [CrossRef]
- Autanski, D.B.; Nagalingam, A.; Bonner, M.Y.; Arbiser, J.L.; Saxena, N.K.; Sharma, D. Honokiol inhibits epithelial-mesenchymal transition in breast cancer cells by targeting signal transducer and activator of transcription 3/Zeb1/E-cadherin axis. Mol. Oncol. 2014, 8, 565–580. [Google Scholar] [CrossRef]
- Rauf, A.; Olatunde, A.; Imran, M.; Alhumaydhi, F.A.; Aljohani, A.S.M.; Khan, S.A.; Uddin, M.S.; Mitra, S.; Bin Emran, T.; Khayrullin, M.; et al. Honokiol: A review of its pharmacological potential and therapeutic insights. Phytomedicine 2021, 90, 153647. [Google Scholar] [CrossRef]
- Averett, C.; Bhardwaj, A.; Arora, S.; Srivastava, S.K.; Khan, M.A.; Ahmad, A.; Singh, S.; Carter, J.E.; Khushman, M.; Singh, A.P. Honokiol suppresses pancreatic tumor growth, metastasis and desmoplasia by interfering with tumor-stromal cross-talk. Carcinogenesis 2016, 37, 1052–1061. [Google Scholar] [CrossRef] [PubMed]
- Lu, X.Y.; Lu, X.Y.; Yang, P.; Zhang, Z.H.; Lv, H.X. Honokiol nanosuspensions loaded thermosensitive hydrogels as the local delivery system in combination with systemic paclitaxel for synergistic therapy of breast cancer. Eur. J. Pharm. Sci. 2022, 175, 106212. [Google Scholar] [CrossRef] [PubMed]
- Zhu, H.J.; Chen, H.B.; Zeng, X.W.; Wang, Z.Y.; Zhang, X.D.; Wu, Y.P.; Gao, Y.F.; Zhang, J.X.; Liu, K.W.; Liu, R.Y.; et al. Co-delivery of chemotherapeutic drugs with vitamin E TPGS by porous PLGA nanoparticles for enhanced chemotherapy against multi-drug resistance. Biomaterials 2014, 35, 2391–2400. [Google Scholar] [CrossRef] [PubMed]
- Beh, C.Y.; Prajnamitra, R.P.; Chen, L.-L.; Hsieh, P.C.-H. Advances in Biomimetic Nanoparticles for Targeted Cancer Therapy and Diagnosis. Molecules 2021, 26, 5052. [Google Scholar] [CrossRef] [PubMed]
- Zhang, L.; Su, H.T.; Liu, Y.J.; Pang, N.; Li, J.; Qi, X.R. Enhancing solid tumor therapy with sequential delivery of dexamethasone and docetaxel engineered in a single carrier to overcome stromal resistance to drug delivery. J. Control. Release 2019, 294, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Shi, H.D.; Liu, S.Z.; Cheng, J.J.; Yuan, S.M.; Yang, Y.; Fang, T.T.; Cao, K.M.; Wei, K.J.; Zhang, Q.L.; Liu, Y.Z. Charge-Selective Delivery of Proteins Using Mesoporous Silica Nanoparticles Fused with Lipid Bilayers. ACS Appl. Mater. Interfaces 2019, 11, 3645–3653. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.W.; Jiang, X.M.; Ashley, C.; Brinker, C.J. Electrostatically Mediated Liposome Fusion and Lipid Exchange with a Nanoparticle-Supported Bilayer for Control of Surface Charge, Drug Containment, and Delivery. J. Am. Chem. Soc. 2009, 131, 7567–7569. [Google Scholar] [CrossRef]
- Butler, K.S.; Durfee, P.N.; Theron, C.; Ashley, C.E.; Carnes, E.C.; Brinker, C.J. Protocells: Modular mesoporous silica nanoparticle-supported lipid bilayers for drug delivery. Small 2016, 12, 2173–2185. [Google Scholar] [CrossRef]
- Yildirim, A.; Chattaraj, R.; Blum, N.T.; Shi, D.; Kumar, K.; Goodwin, A.P. Phospholipid capped mesoporous nanoparticles for targeted high intensity focused ultrasound ablation. Adv. Health. Mater. 2017, 6, 1700514. [Google Scholar] [CrossRef]
- Xue, T.; Xu, P.J.; Padelford, J.; Xue, X.K.; Wu, A.Y.; Li, Y.C.; Wang, L.Y. Actively targeted delivery of SN38 by ultrafine iron oxide nanoparticle for treating pancreatic cancer. Investig. New Drugs 2022, 40, 546–555. [Google Scholar] [CrossRef]
- Erkan, M.; Hausmann, S.; Michalski, C.W.; Fingerle, A.A.; Dobritz, M.; Kleeff, J.; Friess, H. The role of stroma in pancreatic cancer: Diagnostic and therapeutic implications. Nat. Rev. Gastroenterol. Hepatol. 2012, 9, 454–467. [Google Scholar] [CrossRef]
- Szatmari, T.; Otvos, R.; Hjerpe, A.; Dobra, K. Syndecan-1 in Cancer: Implications for Cell Signaling, Differentiation, and Prognostication. Dis. Markers 2015, 2015, 796052. [Google Scholar] [CrossRef] [PubMed]
- Yin, W.Y.; Kimbrough, C.W.; Gomez-Gutierrez, J.G.; Burns, C.T.; Chuong, P.; Grizzle, W.E.; McNally, L.R. Tumor specific liposomes improve detection of pancreatic adenocarcinoma in vivo using optoacoustic tomography. J. Nanobiotechnol. 2015, 13, 90. [Google Scholar] [CrossRef]
- Shailaja, V.L.; Christina, V.S.; Mohanapriya, C.D.; Sneha, P.; Sundaram, R.L.; Magesh, R.; Doss, C.G.P.; Gnanambal, K.M.E. A natural anticancer pigment, Pheophytin a, from a seagrass acts as a high affinity human mitochondrial translocator protein (TSPO) ligand, in silico, to reduce mitochondrial membrane Potential (Delta psi(mit)) in adenocarcinomic A549 cells. Phytomedicine 2019, 61, 152858. [Google Scholar] [CrossRef] [PubMed]
- Sazanov, L.A. A giant molecular proton pump: Structure and mechanism of respiratory complex I. Nat. Rev. Mol. Cell Biol. 2015, 16, 375–388. [Google Scholar] [CrossRef]
- Chen, Y.; Yang, S.; Tavormina, J.; Tampe, D.; Zeisberg, M.; Wang, H.; Mahadevan, K.K.; Wu, C.J.; Sugimoto, H.; Chang, C.C.; et al. Oncogenic collagen I homotrimers from cancer cells bind to α3β1 integrin and impact tumor microbiome and immunity to promote pancreatic cancer. Cancer Cell 2022, 40, 818–834.e819. [Google Scholar] [CrossRef] [PubMed]
- Hu, X.X.; Hao, X.H.; Wu, Y.; Zhang, J.C.; Zhang, X.N.; Wang, P.C.; Zou, G.Z.; Liang, X.J. Multifunctional hybrid silica nanoparticles for controlled doxorubicin loading and release with thermal and pH dual response. J. Mater. Chem. B 2013, 1, 1109–1118. [Google Scholar] [CrossRef] [PubMed]

Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Liu, D.; Wang, L.; Li, H.; Li, D.; Zhou, J.; Wang, J.; Zhang, Q.; Cai, D. Co-Delivery of Gemcitabine and Honokiol by Lipid Bilayer-Coated Mesoporous Silica Nanoparticles Enhances Pancreatic Cancer Therapy via Targeting Depletion of Tumor Stroma. Molecules 2024, 29, 675. https://doi.org/10.3390/molecules29030675
Liu D, Wang L, Li H, Li D, Zhou J, Wang J, Zhang Q, Cai D. Co-Delivery of Gemcitabine and Honokiol by Lipid Bilayer-Coated Mesoporous Silica Nanoparticles Enhances Pancreatic Cancer Therapy via Targeting Depletion of Tumor Stroma. Molecules. 2024; 29(3):675. https://doi.org/10.3390/molecules29030675
Chicago/Turabian StyleLiu, Dan, Linjiang Wang, Henan Li, Dong Li, Jianwen Zhou, Jing Wang, Qi Zhang, and Defu Cai. 2024. "Co-Delivery of Gemcitabine and Honokiol by Lipid Bilayer-Coated Mesoporous Silica Nanoparticles Enhances Pancreatic Cancer Therapy via Targeting Depletion of Tumor Stroma" Molecules 29, no. 3: 675. https://doi.org/10.3390/molecules29030675
APA StyleLiu, D., Wang, L., Li, H., Li, D., Zhou, J., Wang, J., Zhang, Q., & Cai, D. (2024). Co-Delivery of Gemcitabine and Honokiol by Lipid Bilayer-Coated Mesoporous Silica Nanoparticles Enhances Pancreatic Cancer Therapy via Targeting Depletion of Tumor Stroma. Molecules, 29(3), 675. https://doi.org/10.3390/molecules29030675





