Nucleotides and AHCC Enhance Th1 Responses In Vitro in Leishmania-Stimulated/Infected Murine Cells
Abstract
1. Introduction
2. Results
2.1. Cytotoxicity Studies on Murine Macrophages
2.2. Production of Nitric Oxide (NO) by Macrophages
2.3. In Vitro Promastigote and Amastigote Susceptibility Assays
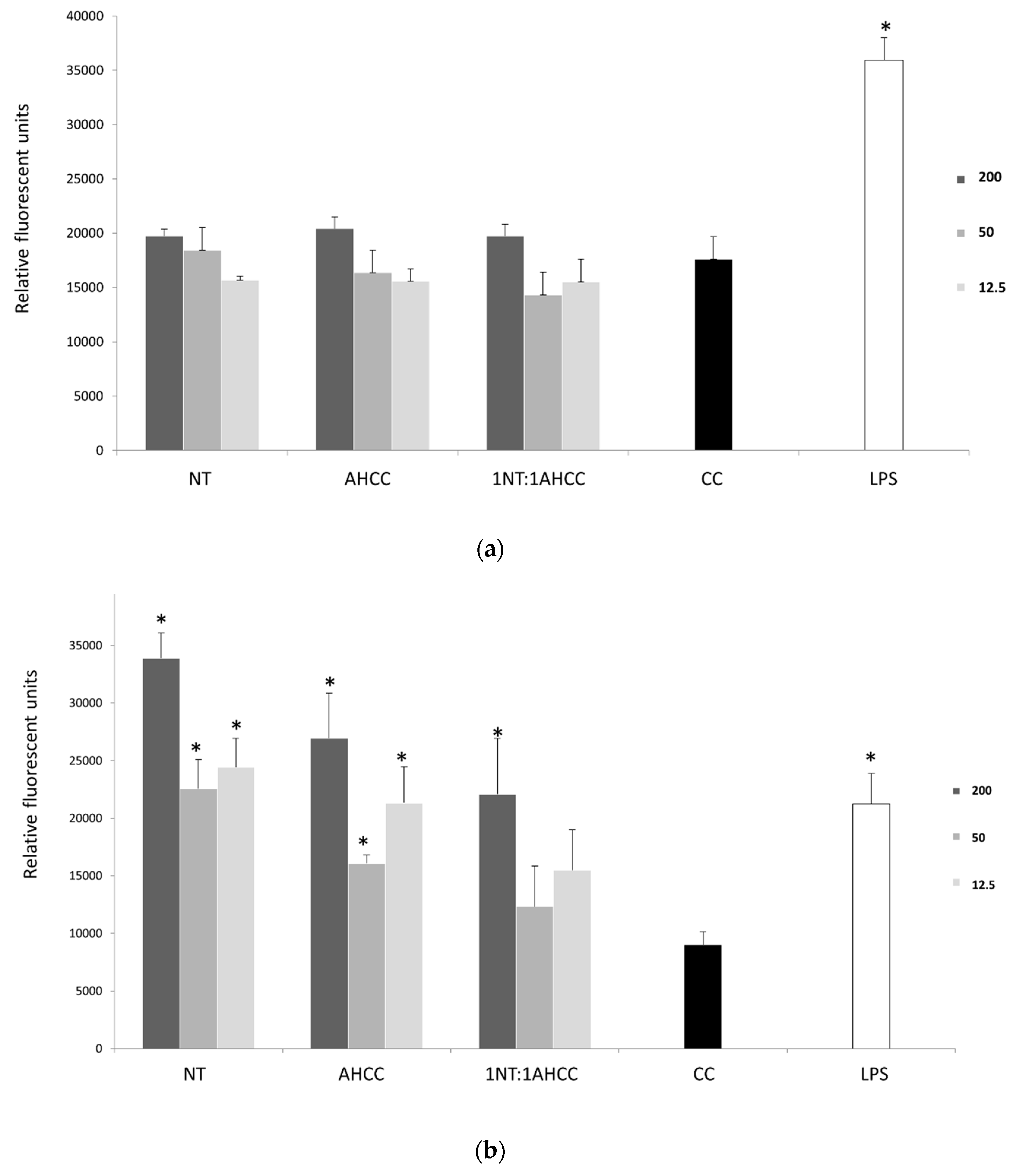
2.4. In Vitro Lymphoproliferation Assay
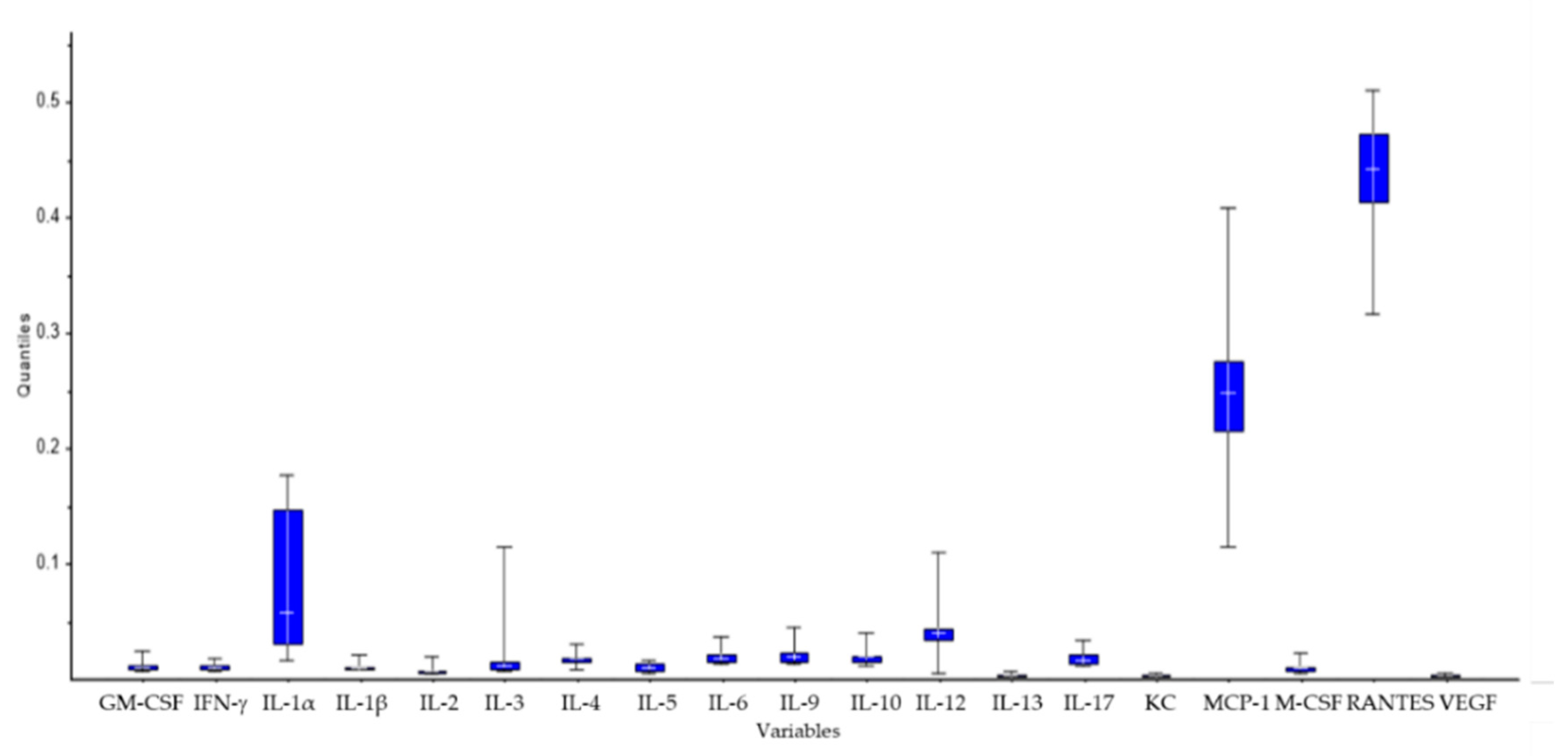
2.5. Analysis of Cytokines
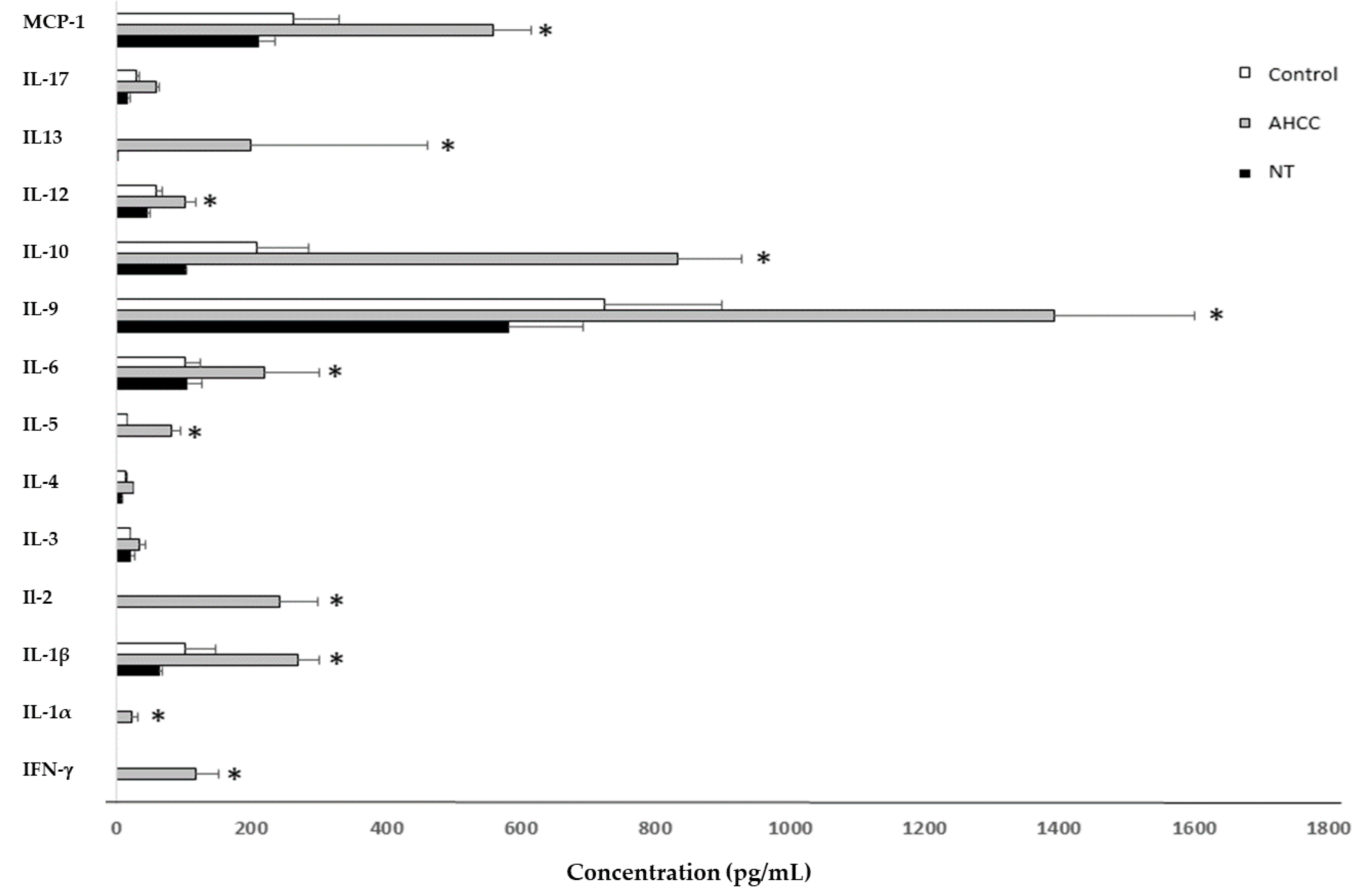
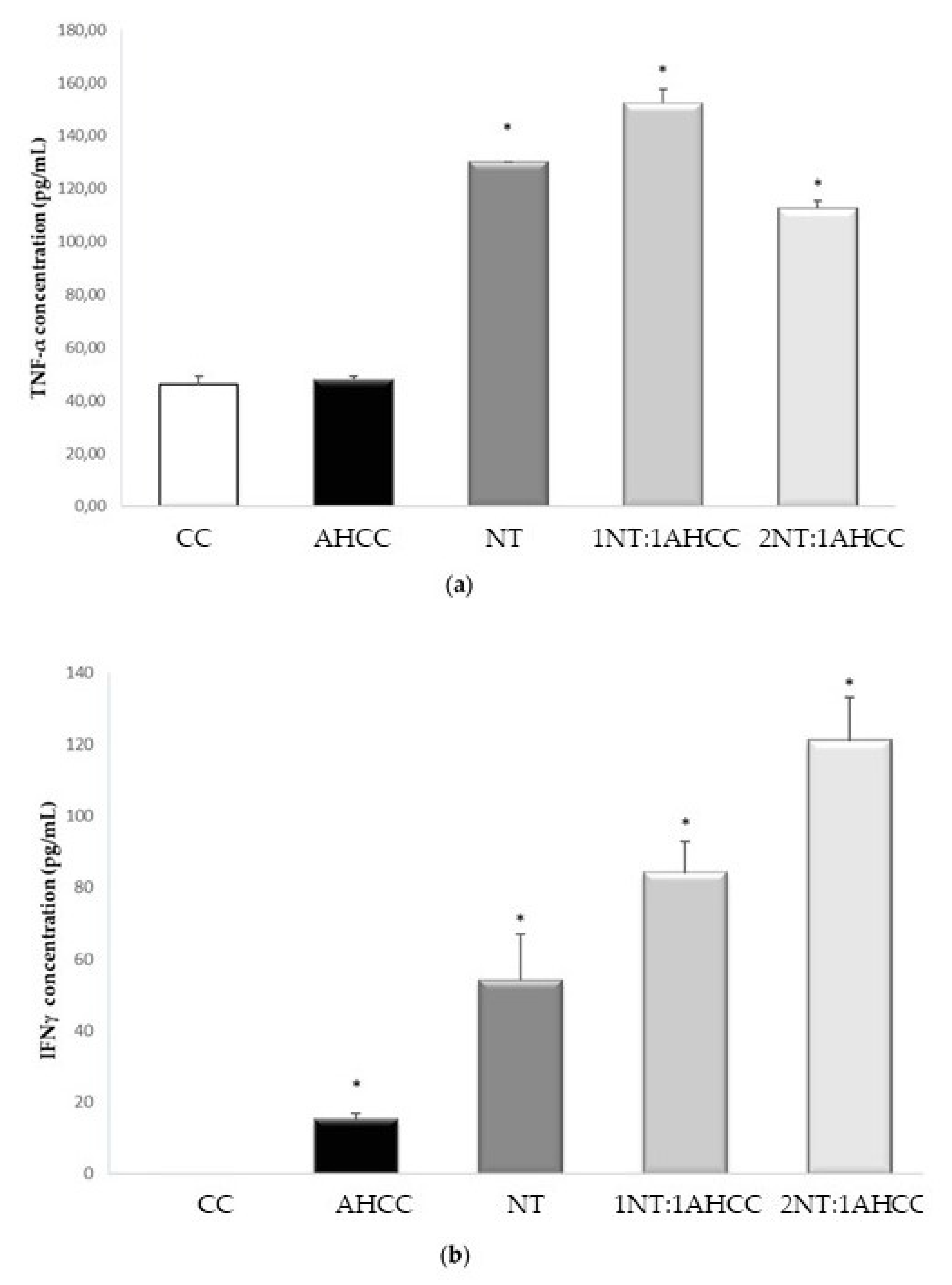
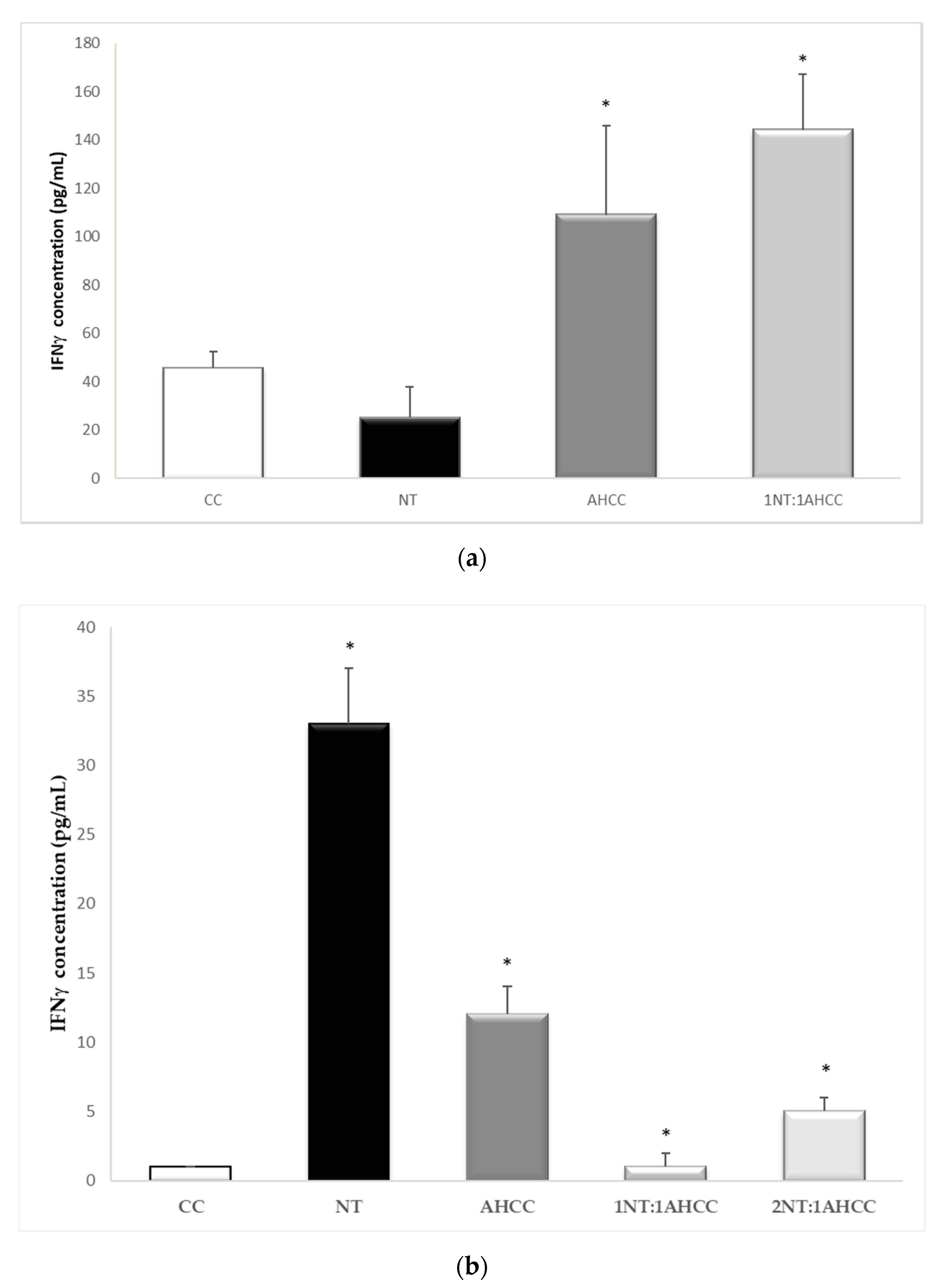
2.5.1. Coculture of Lymphocytes and Naïve Macrophages
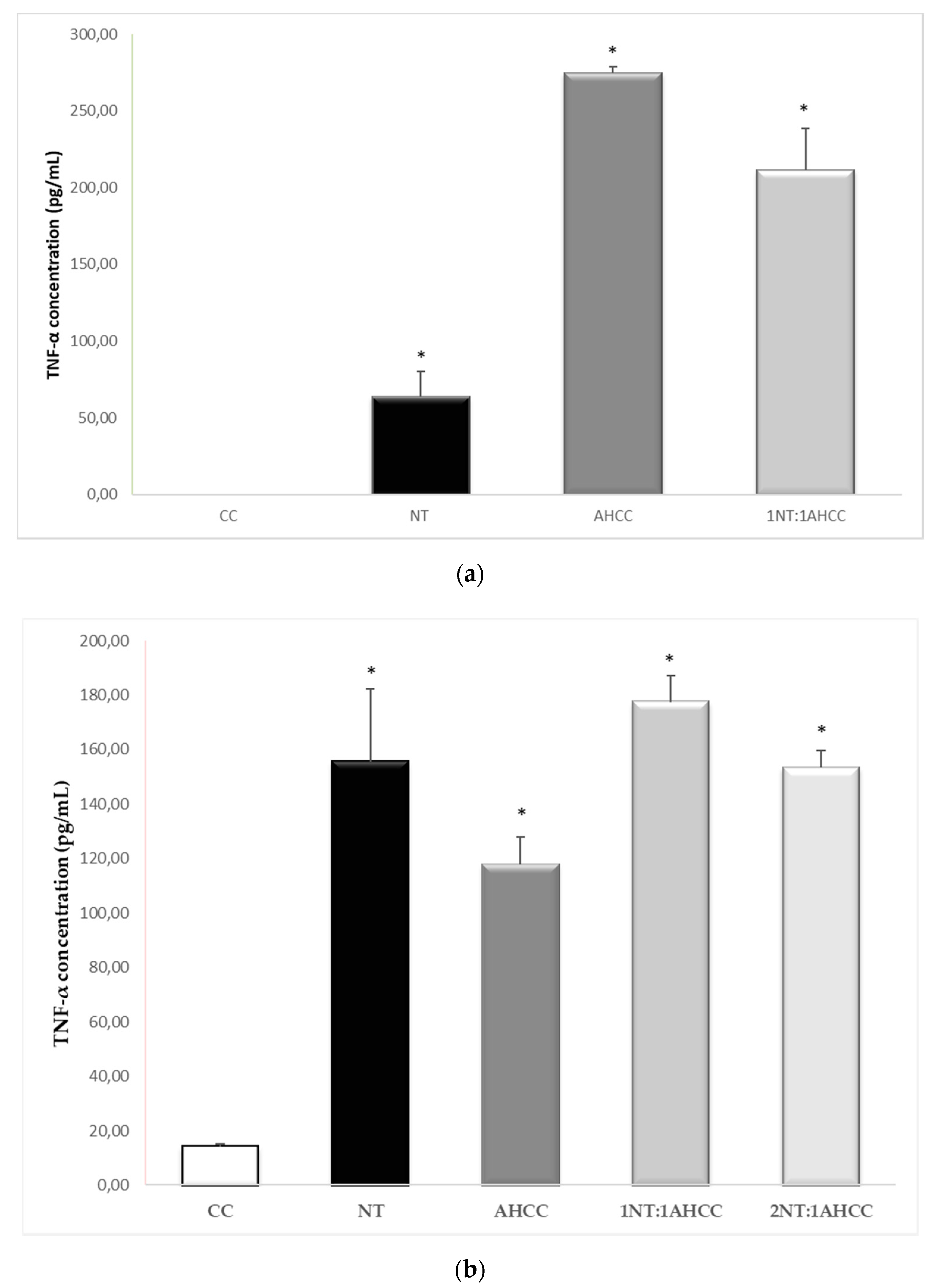
2.5.2. Coculture of Lymphocytes and Leishmania-Infected Macrophages
3. Discussion
4. Materials and Methods
4.1. Compounds
4.2. Mice
4.3. Cytotoxicity Studies on Murine Macrophages
4.4. Quantification of NO Production by Macrophages
4.5. In Vitro Promastigote and Amastigote Susceptibility Assays
4.6. Preparation of Leishmania Infantum Antigen
4.7. In Vitro Lymphoproliferation Assay
4.8. Coculture of Macrophages and Lymphocytes
4.9. Analysis of Cytokines
4.10. Statistical Data Analysis
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Conflicts of Interest
References
- Maslov, D.A.; Opperdoes, F.R.; Kostygov, A.Y.; Hashimi, H.; Lukeš, J.; Yurchenko, V. Recent advances in trypanosomatid research: Genome organization, expression, metabolism, taxonomy and evolution. Parasitology 2019, 146, 1–27. [Google Scholar] [CrossRef] [PubMed]
- Lukeš, J.; Butenko, A.; Hashimi, H.; Maslov, D.A.; Votýpka, J.; Yurchenko, V. Trypanosomatids are much more than just trypanosomes: Clues from the expanded family tree. Trends Parasitol. 2018, 34, 466–480. [Google Scholar] [CrossRef] [PubMed]
- Young, D.G.; Lawyer, P.G. New world vectors of the Leishmaniases. In Current Topics in Vector Research, 1st ed.; Harris, K.F., Ed.; Springer: New York, NY, USA, 1987; Volume 4, pp. 29–71. [Google Scholar]
- Bañuls, A.L.; Bastien, P.; Pomares, C.; Arevalo, J.; Fisa, R.; Hide, M. Clinical pleiomorphism in human leishmaniases, with special mention of asymptomatic infection. Clin. Microbiol. Infect. 2011, 17, 1451–1461. [Google Scholar] [CrossRef]
- Barbosa, J.F.; de Figueiredo, S.M.; Monteiro, F.M.; Rocha-Silva, F.; Gaciele-Melo, C.; Coelho, S.S.; Lyon, S.; Caligiorne, R.B. New approaches on leishmaniasis treatment and prevention: A review of recent patents. Recent Pat. Endocr. Metab. Immune Drug Discov. 2015, 9, 90–102. [Google Scholar] [CrossRef]
- Manna, L.; Corso, R.; Galiero, G.; Cerrone, A.; Muzj, P.; Gravino, A.E. Long-term follow-up of dogs with leishmaniosis treated with meglumine antimoniate plus allopurinol versus miltefosine plus allopurinol. Parasites Vectors 2015, 8, 289–298. [Google Scholar] [CrossRef]
- Reguera, R.M.; Morán, M.; Pérez-Pertejo, Y.; García-Estrada, C.; Balaña-Fouce, R. Current status on prevention and treatment of canine leishmaniasis. Vet. Parasitol. 2016, 227, 98–114. [Google Scholar] [CrossRef]
- Baneth, G.; Aroch, I. Canine leishmaniasis: A diagnostic and clinical challenge. Vet. J. 2008, 175, 14–15. [Google Scholar] [CrossRef]
- Yasur-Landau, D.; Jaffe, C.L.; David, L.; Baneth, G. Allopurinol resistance in Leishmania infantum from dogs with disease relapse. PLoS Negl. Trop. Dis. 2016, 10, e0004341. [Google Scholar] [CrossRef]
- Sindermann, H.; Engel, J. Development of miltefosine as an oral treatment for leishmaniasis. Trans. R. Soc. Trop. Med. Hyg. 2006, 100, S17–S20. [Google Scholar] [CrossRef]
- Reis, A.B.; Giunchetti, R.C.; Carrillo, E.; Martins-Filho, O.A.; Moreno, J. Immunity to Leishmania and the rational search for vaccines against canine leishmaniasis. Trends Parasitol. 2010, 26, 341–349. [Google Scholar] [CrossRef]
- Reis, M.L.; Ferreira, V.M.; Zhang, X.; Gonçalves, R.; Vieira, L.Q.; Tafuri, W.L.; Mosser, D.M.; Tafuri, W.L. Murine immune response induced by Leishmania major during the implantation of paraffin tablets. Virchows Arch. 2010, 457, 609–618. [Google Scholar] [CrossRef]
- Manna, L.; Reale, S.; Picillo, E.; Vitale, F.; Gravino, A.E. Interferon-gamma (INF-gamma), IL4 expression levels and Leishmania DNA load as prognostic markers for monitoring response to treatment of leishmaniotic dogs with miltefosine and allopurinol. Cytokine 2008, 44, 288–292. [Google Scholar] [CrossRef]
- Esch, K.J.; Juelsgaard, R.; Martinez, P.A.; Jones, D.E.; Petersen, C.A. Programmed death 1-mediated T cell exhaustion during visceral leishmaniasis impairs phagocyte function. J. Immunol. 2013, 191, 5542–5550. [Google Scholar] [CrossRef]
- Hess, J.R.; Greenberg, N.A. The role of nucleotides in the immune and gastrointestinal systems potential clinical applications. Nutr. Clin. Pract. 2012, 27, 281–294. [Google Scholar] [CrossRef]
- Martínez-Augustín, O.; Gil, A. Role of dietary nucleotides in immunity. Funct. Food Rev. 2010, 2, 91–100. [Google Scholar]
- Gil, A. Modulation of the immune response mediated by dietary nucleotides. Eur. J. Clin. Nutr. 2002, 56, S1–S4. [Google Scholar] [CrossRef]
- Smith, J.A.; Mathew, L.; Gaikwad, A.; Rech, B.; Burney, M.N.; Faro, J.P.; Lucci, J.A., 3rd; Bai, Y.; Olsen, R.J.; Byrd, T.T. From bench to bedside: Evaluation of AHCC supplementation to modulate the host immunity to clear high-risk human papillomavirus infections. Front. Oncol. 2019, 9, 173. [Google Scholar] [CrossRef]
- Lee, W.W.; Lee, N.; Fujii, H.; Kang, I. Active hexose correlated compound promotes T helper (Th) 17 and 1 cell responses via inducing IL-1β production from monocytes in humans. Cell Immunol. 2012, 275, 19–23. [Google Scholar] [CrossRef][Green Version]
- Ulbricht, C.; Brigham, A.; Bryan, J.K.; Catapang, M.; Chowdary, D.; Costa, D.; Culwell, S.; D’Auria, D.; Giese, N.; Iovin, R.; et al. An evidence-based systematic review of active hexose correlated compound (AHCC) by the Natural Standard Research Collaboration. J. Diet. Suppl. 2013, 10, 264–308. [Google Scholar] [CrossRef]
- Yin, Z.; Fujii, H.; Walshe, T. Effects of active hexose correlated compound on frequency of CD4+ and CD8+ T cells producing interferon-γ and/or tumor necrosis factor-α in healthy adults. Hum. Immunol. 2010, 71, 1187–1190. [Google Scholar] [CrossRef]
- Daddaoua, A.; Martínez-Plata, E.; Ortega-González, M.; Ocón, B.; Aranda, C.J.; Zarzuelo, A.; Suárez, M.D.; de Medina, F.S.; Martínez-Augustin, O. The nutritional supplement active hexose correlated compound (AHCC) has direct immunomodulatory actions on intestinal epithelial cells and macrophages involving TLR/MyD88 and NF-κB/MAPK activation. Food Chem. 2013, 136, 1288–1295. [Google Scholar] [CrossRef] [PubMed]
- Mallet, J.F.; Graham, É.; Ritz, B.W.; Homma, K.; Matar, C. Active hexose correlated compound (AHCC) promotes an intestinal immune response in BALB/c mice and in primary intestinal epithelial cell culture involving toll-like receptors TLR-2 and TLR-4. Eur. J. Nutr. 2016, 55, 139–146. [Google Scholar] [CrossRef] [PubMed]
- Segarra, S.; Miró, G.; Montoya, A.; Pardo-Marín, L.; Boqué, N.; Ferrer, L.; Cerón, J. Randomized, allopurinol-controlled trial of the effects of dietary nucleotides and active hexose correlated compound in the treatment of canine leishmaniosis. Vet. Parasitol. 2017, 239, 50–56. [Google Scholar] [CrossRef] [PubMed]
- Segarra, S.; Miró, G.; Montoya, A.; Pardo-Marín, L.; Teichenné, J.; Ferrer, L.; Cerón, J.J. Prevention of disease progression in Leishmania infantum-infected dogs with dietary nucleotides and active hexose correlated compound. Parasites Vectors 2018, 11, 103. [Google Scholar] [CrossRef]
- Liu, D.; Uzonna, J.E. The early interaction of Leishmania with macrophages and dendritic cells and its influence on the host immune response. Cell. Infect. Microbiol. 2012, 12, 83–90. [Google Scholar] [CrossRef]
- Melo, L.M.; Perosso, J.; Almeida, B.F.; Silva, K.L.; Somenzari, M.A.; de Lima, V.M. Effects of P-MAPA immunomodulator on Toll-like receptor 2, ROS, nitric oxide, MAPKp38 and IKK in PBMC and macrophages from dogs with visceral leishmaniasis. Int. Immunopharmacol. 2014, 18, 373–378. [Google Scholar] [CrossRef]
- Jyonouchi, H.; Sun, S.; Winship, T.; Kuchan, M.J. Dietary ribonucleotides increase antigen-specific type 1 T-helper cells in the regional draining lymph nodes in young BALB/cJ mice. Nutrition 2003, 19, 41–46. [Google Scholar] [CrossRef]
- Ibarra-Meneses, A.V.; Sanchez, C.; Alvar, J.; Moreno, J.; Carrillo, E. Monocyte Chemotactic Protein 1 in plasma from soluble Leishmania antigen-stimulated whole blood as a potential biomarker of the cellular immune response to Leishmania infantum. Front. Immunol. 2017, 8, 1208–1212. [Google Scholar] [CrossRef]
- Ritter, U.; Moll, H. Monocyte chemotactic protein-1 stimulates the killing of Leishmania major by human monocytes, acts synergistically with IFN-gamma and is antagonized by IL-4. Eur. J. Immunol. 2000, 30, 3111–3120. [Google Scholar] [CrossRef]
- Matte, C.; Olivier, M. Leishmania-induced cellular recruitment during the early inflammatory response: Modulation of proinflammatory mediators. J. Infect. Dis. 2002, 185, 673–681. [Google Scholar] [CrossRef]
- Arendse, B.; Van Snick, J.; Brombacher, F. IL-9 is a susceptibility factor in Leishmania infection by promoting detrimental Th2/type 2 responses. J. Immunol. 2005, 174, 2205–2211. [Google Scholar] [CrossRef]
- Dos Santos, P.L.; de Oliveira, F.A.; Santos, M.L.; Cunha, L.C.; Lino, M.T.; De Oliveira, M.F.; Bomfim, M.O.; Silva, A.M.; De Moura, T.R.; De Jesus, A.R.; et al. The severity of visceral leishmaniasis correlates with elevated levels of serum IL-6, IL-27 and sCD14. PLoS Negl. Trop. Dis. 2016, 10, e0004375. [Google Scholar] [CrossRef]
- Maia, C.; Nunes, M.; Marques, M.; Henriques, S.; Rolão, N.; Campino, L. In vitro drug susceptibility of Leishmania infantum isolated from humans and dogs. Exp. Parasitol. 2013, 135, 36–41. [Google Scholar] [CrossRef]
- Borja-Cabrera, G.P.; Santos, F.N.; Santos, F.B.; Trivellato, F.A.; Kawasaki, J.K.; Costa, A.C.; Castro, T.; Nogueira, F.S.; Moreira, M.A.; Luvizotto, M.C.; et al. Immunotherapy with the saponin enriched-Leishmune vaccine versus immunochemotherapy in dogs with natural canine visceral leishmaniasis. Vaccine 2010, 28, 597–603. [Google Scholar] [CrossRef]
- Baxarias, M.; Martínez-Orellana, P.; Baneth, G.; Solano-Gallego, L. Immunotherapy in clinical canine leishmaniosis: A comparative update. Res. Vet. Sci. 2019, 125, 218–226. [Google Scholar] [CrossRef]
- Dantas-Torres, F.; Miró, G.; Baneth, G.; Bourdeau, P.; Breitschwerdt, E.; Capelli, G.; Cardoso, L.; Day, M.J.; Dobler, G.; Ferrer, L.; et al. Canine leishmaniasis control in the context of One Health. Emerg. Infect. Dis. 2019, 25, 1–4. [Google Scholar] [CrossRef]
- Dea-Ayuela, M.A.; Castillo, E.; Gonzalez-Alvarez, M.; Vega, C.; Rolón, M.; Bolás-Fernández, F.; Borrás, J.; González-Rosende, M.E. In vivo and anti-leishmanial activities of 4-nitro-N-pyrimidin- and N-pyrazin-2-ylbenzenesulfonamides, and N2- 4-nitrophenyl)-N1-propylglycinamide. Bioorg. Med Chem. 2009, 17, 7449–7456. [Google Scholar] [CrossRef]
- Galiana-Roselló, C.; Bilbao-Ramos, P.; Dea-Ayuela, M.A.; Rolón, M.; Vega, C.; Bolás-Fernández, F.; García-España, E.; Alfonso, J.; Coronel, C.; González-Rosende, M.E. In vitro and in vivo antileishmanial and trypanocidal studies of new N-benzene- and N-naphthalenesulfonamide derivatives. J. Med. Chem. 2013, 56, 8984–8998. [Google Scholar] [CrossRef]
- Serrano, D.R.; Lalatsa, A.; Dea-Ayuela, M.A. Engineering synergistically active and bioavailable cost-effective medicines for neglected tropical diseases: The role of excipients. Curr. Top. Med. Chem. 2017, 17, 2888–2900. [Google Scholar] [CrossRef]
- Bilbao-Ramos, P.; Sifontes-Rodríguez, S.; Dea-Ayuela, M.A.; Bolás-Fernández, F. A fluorometric method for evaluation of pharmacological activity against intracellular Leishmania amastigotes. J. Microbiol. Methods 2012, 89, 8–11. [Google Scholar] [CrossRef]
- Viana, K.F.; Aguiar-Soares, R.D.; Roatt, B.M.; Resende, L.A.; da Silveira-Lemos, D.; Corrêa-Oliveira, R.; Martins-Filho, O.A.; Moura, S.L.; Zanini, M.S.; Araújo, M.S.; et al. Analysis using canine peripheral blood for establishing in vitro conditions for monocyte differentiation into macrophages for Leishmania chagasi infection and T-cell subset purification. Vet Parasitol. 2013, 98, 62–71. [Google Scholar] [CrossRef][Green Version]
Sample Availability: Samples of the compounds in these studies are available from the authors. |
| Concentration (pg/mL) | CC | NT | 1NT:1AHCC | 2NT:1AHCC | NT + SLA | 1NT:1AHCC + SLA | 2NT:1AHCC + SLA | LPS |
|---|---|---|---|---|---|---|---|---|
| GM-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 | 2 +/− 0 | 1 +/− 0 | 2 +/− 0 | 0 +/− 0 |
| IFN-γ | 3 +/− 0 | 2 +/− 0 | 4 +/− 0 | 2 +/− 0 | 9 +/− 0 * | 5 +/− 0 * | 9 +/− 0 * | 4 +/− 0 |
| IL-1α | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 2 +/− 1 |
| IL-1β | 1 +/− 0 | 3 +/− 1 | 1 +/− 0 | 1 +/− 0 | 3 +/− 0 | 1 +/− 0 | 3 +/− 0 | 0 +/− 0 |
| IL-2 | 0 +/− 0 | 2 +/− 0 | 1 +/− 0 | 7 +/− 1 * | 9 +/− 1 * | 8 +/− 0 * | 11 +/− 1 * | 0 +/− 0 |
| IL-3 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-4 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-5 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-6 | 4 +/− 0 | 5 +/− 0 | 19 +/− 2 * | 24 +/− 2 * | 9 +/− 1 * | 25 +/− 3 * | 26 +/− 2 * | 1229 +/− 7 * |
| IL-9 | 48 +/− 5 | 62 +/− 10 | 50 +/− 4 | 79 +/− 3 * | 103 +/− 10 * | 33 +/− 3 | 114 +/− 7 * | 138 +/− 12 * |
| IL-10 | 0 +/− 0 | 0 +/− 0 | 5 +/− 0 | 19 +/− 1 * | 5 +/− 0 | 0 +/− 0 | 0 +/− 0 | 45 +/− 2 * |
| IL-12 | 2 +/− 0 | 2 +/− 0 | 4 +/− 0 | 5 +/− 0 * | 5 +/− 0 * | 1 +/− 0 | 4 +/− 0 | 4 +/− 0 |
| IL-13 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-17 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 |
| KC | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 38 +/− 1 |
| MCP-1 | 0 +/− 0 | 12 +/− 1 * | 4 +/− 0 | 8 +/− 1 * | 12 +/− 1 * | 0 +/− 0 | 9 +/− 0 * | 0 +/− 0 |
| M-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 | 0 +/− 0 |
| RANTES | 1 +/− 0 | 1 +/− 0 | 0 +/− 0 | 1 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 82 +/− 2 * |
| TNF-α | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 12 +/− 1 * | 0 +/− 0 | 10 +/− 0 * | 0 +/− 0 |
| VEGF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 |
| Concentration (pg/mL) | CC | AHCC | NT | 1NT:1AHCC | 2NT:1AHCC |
|---|---|---|---|---|---|
| GM-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IFN-γ | 0 +/− 0 | 15 +/− 2 * | 54 +/− 13 * | 84 +/− 9 * | 121 +/− 12 * |
| IL-1α | 0 +/− 0 | 24 +/− 12 * | 103 +/− 19 * | 36 +/− 10 * | 26 +/− 11 * |
| IL-1β | 0 +/− 0 | 0 +/− 0 | 20 +/− 5 * | 84 +/− 3 * | 113 +/− 12 * |
| IL-2 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 | − | 1 +/− 0 |
| IL-3 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 6 +/− 1 * | 6 +/− 1 * |
| IL-4 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-5 | 0 +/− 0 | 0 +/− 0 | 2 +/− 1 | 26 +/− 7 * | 32 +/− 10 * |
| IL-6 | 50 +/− 6 | 86 +/− 9 * | 60 +/− 5 | 168 +/− 18 * | 133 +/− 8 * |
| IL-9 | 188 +/− 29 | 0 +/− 0 | 134 +/− 21 | 341 +/− 47 * | 382 +/− 64 * |
| IL-10 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 18 +/− 3 * |
| IL-12 | 4 +/− 1 | 1 +/− 0 | 14 +/− 1 * | 22 +/− 3 * | 28 +/− 2 * |
| IL-13 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-17 | 5 +/− 1 | 4 +/− 1 | 0 +/− 0 | 22 +/− 4 * | 18 +/− 2 |
| TNF-α | 45.7+/− 3.5 | 47.72+/−1.5 | 129.94+/− 0 * | 152.1+/− 5.4 * | 112.44+/− 2.74 * |
| KC | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| MCP-1 | 604 +/− 64 | 1133 +/− 303 * | 715 +/− 159 | 830 +/− 105 * | 941 +/− 143 * |
| M-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| RANTES | 191 +/− 14 | 194 +/− 22 | 181 +/− 8 | 234 +/− 17 * | 261 +/− 10 * |
| VEGF | 2 +/− 1 | 0 +/− 0 | 0 +/− 0 | 2 +/− 0 | 3 +/− 0 |
| Concentration (pg/mL) | Noninfected Coculture | Coculture | AHCC | NT | 1NT:1AHCC | 2NT:1AHCC |
|---|---|---|---|---|---|---|
| GM-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IFN-γ | 0 +/− 0 | 1 +/− 0 | 12 +/− 2 * | 33 +/− 4 * | 1 +/− 0 | 5 +/− 1 * |
| IL-1α | 0 +/− 0 | 0 +/− 0 | 85 +/− 83 * | 97 +/− 80 * | 29 +/− 12 * | 122 +/− 51 * |
| IL-1β | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-2 | 0 +/− 0 | 12 +/− 1 * | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-3 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-4 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-5 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 3 +/− 1 | 0 +/− 0 |
| IL-6 | 50 +/− 6 | 34 +/− 4 | 91 +/− 19 * | 43 +/− 2 | 57 +/− 3 | 44 +/− 7 |
| IL-9 | 188 +/− 29 | 223 +/− 37 | 0 +/− 0 | 33 +/− 3 * | 161 +/− 20 | 53 +/− 13 * |
| IL-10 | 0 +/− 0 | 2 +/− 0 | 0 +/− 0 | 10 +/− 0 * | 26 +/− 1 * | 0 +/− 0 |
| IL-12 | 4 +/− 1 | 0 +/− 0 | 1 +/− 0 | 8 +/− 1 | 13 +/− 1 * | 3 +/− 1 |
| IL-13 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| IL-17 | 5 +/− 1 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 1 +/− 0 | 0 +/− 0 |
| TNF-α | 45.7+/− 3.5 | 14.11+/−1.18 | 117.72+/−10.21 * | 155.50+/−26.71 * | 177.44+/−9.82 * | 153.28+/−6.28 * |
| KC | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 |
| MCP-1 | 604 +/− 64 | 764 +/− 100 | 2410 +/− 327 * | 2144 +/− 269 * | 2096 +/− 540 * | 1318 +/− 546 * |
| M-CSF | 0 +/− 0 | 0 +/− 0 | 0 +/− 0 | 12 +/− 2 | 0 +/− 0 | 0 +/− 0 |
| RANTES | 191 +/− 14 | 149 +/− 22 | 347 +/− 45 * | 304 +/− 19 * | 308 +/− 14 * | 319 +/− 22 * |
| VEGF | 2 +/− 1 | 0 +/− 0 | 2 +/− 0 | 6 +/− 1 | 5 +/− 1 | 2 +/− 0 |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dea-Ayuela, M.A.; Segarra, S.; Serrano, D.R.; Bolás-Fernández, F. Nucleotides and AHCC Enhance Th1 Responses In Vitro in Leishmania-Stimulated/Infected Murine Cells. Molecules 2020, 25, 3918. https://doi.org/10.3390/molecules25173918
Dea-Ayuela MA, Segarra S, Serrano DR, Bolás-Fernández F. Nucleotides and AHCC Enhance Th1 Responses In Vitro in Leishmania-Stimulated/Infected Murine Cells. Molecules. 2020; 25(17):3918. https://doi.org/10.3390/molecules25173918
Chicago/Turabian StyleDea-Ayuela, María Auxiliadora, Sergi Segarra, Dolores R. Serrano, and Francisco Bolás-Fernández. 2020. "Nucleotides and AHCC Enhance Th1 Responses In Vitro in Leishmania-Stimulated/Infected Murine Cells" Molecules 25, no. 17: 3918. https://doi.org/10.3390/molecules25173918
APA StyleDea-Ayuela, M. A., Segarra, S., Serrano, D. R., & Bolás-Fernández, F. (2020). Nucleotides and AHCC Enhance Th1 Responses In Vitro in Leishmania-Stimulated/Infected Murine Cells. Molecules, 25(17), 3918. https://doi.org/10.3390/molecules25173918






