Antibacterial Effect of a 4x Cu-TiO2 Coating Simulating Acute Periprosthetic Infection—An Animal Model
Abstract
:1. Introduction
2. Results
2.1. Microbiological Results
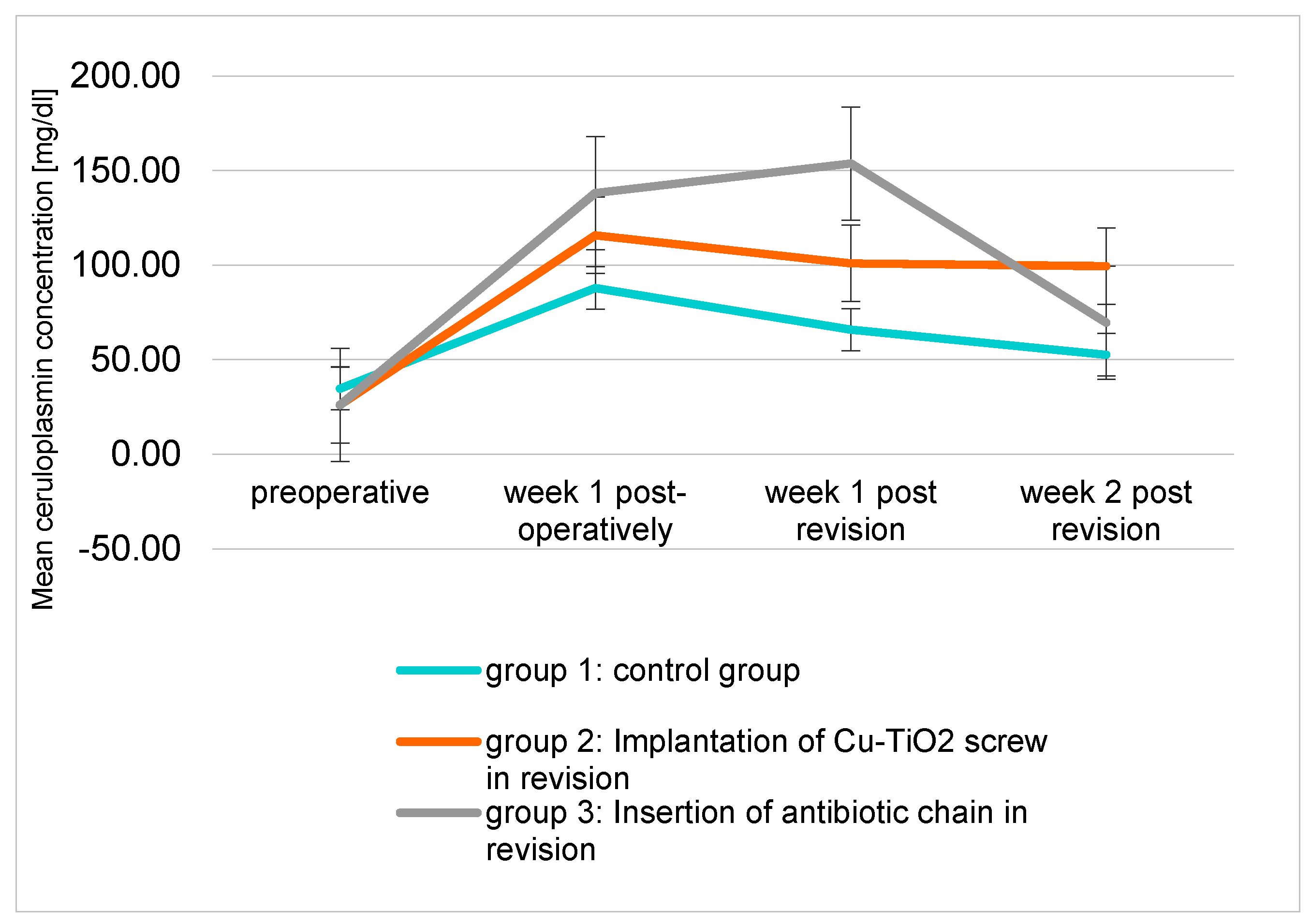
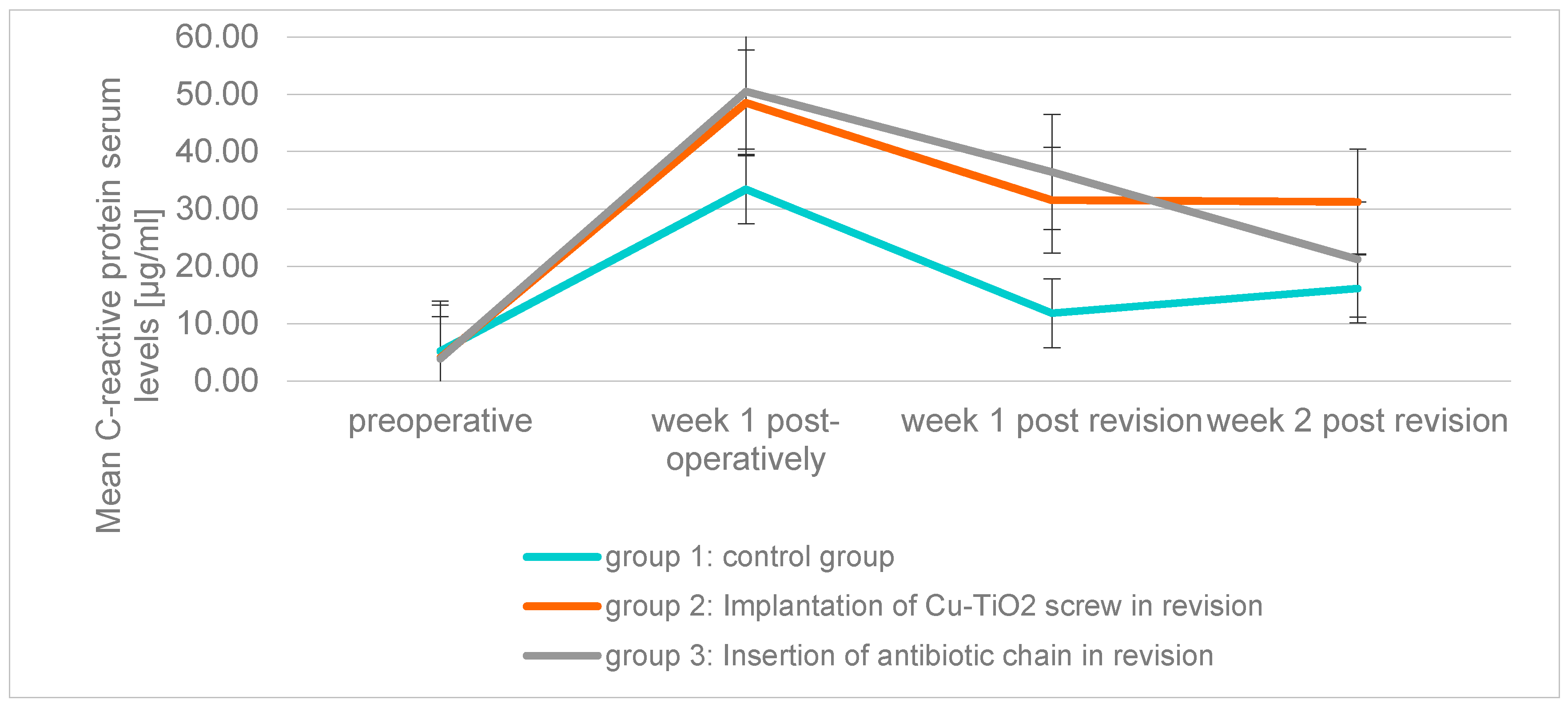
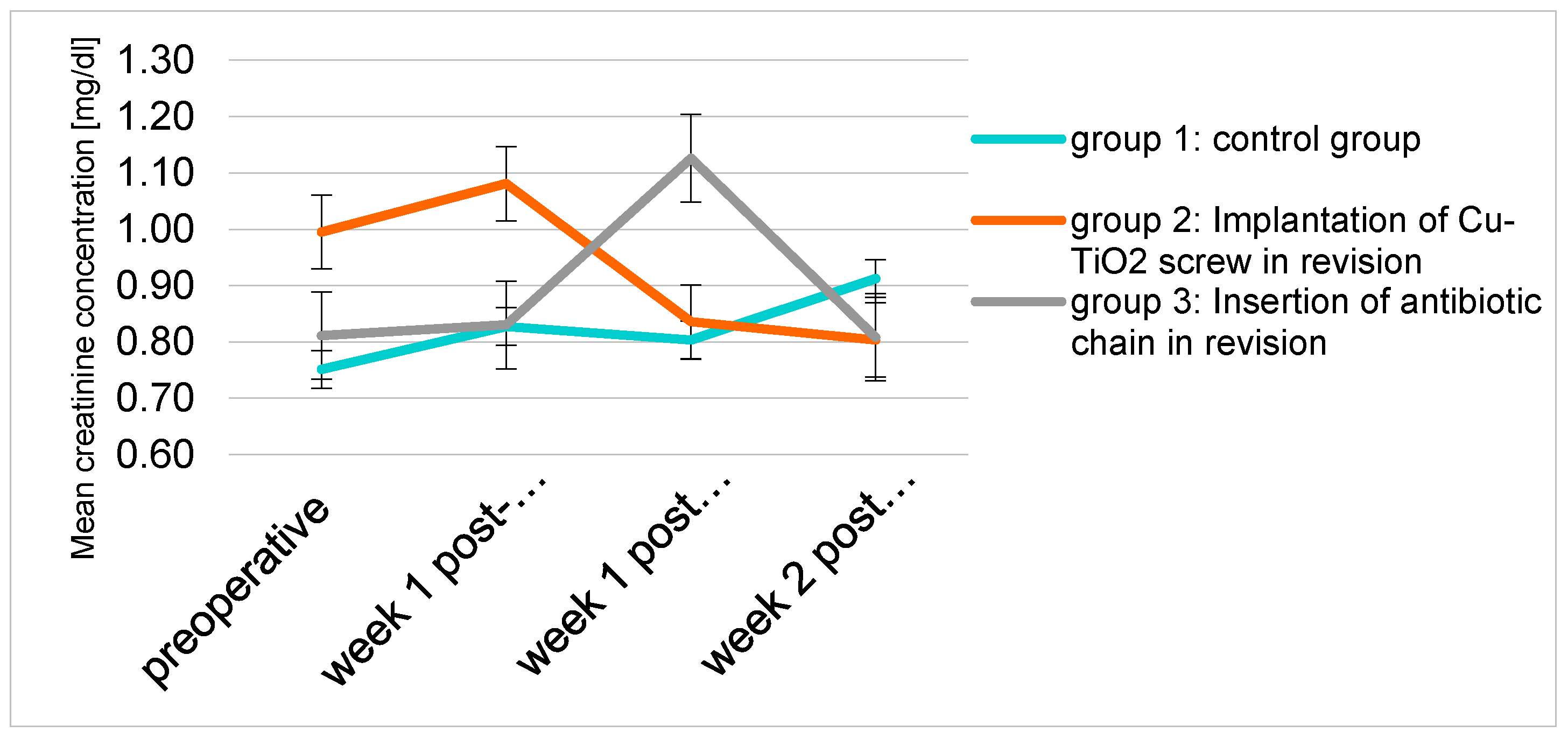
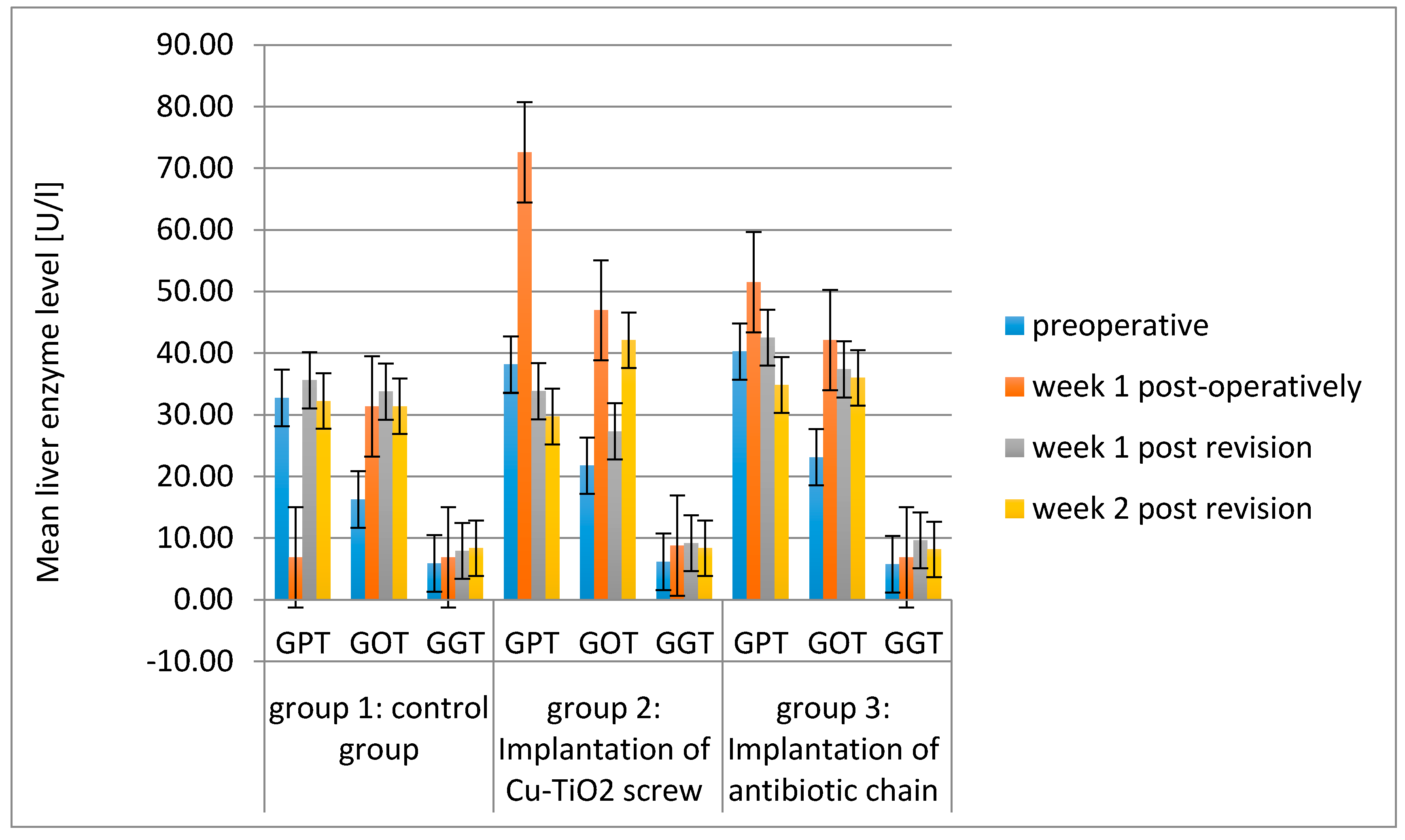
2.2. Blood Tests
3. Discussion
4. Materials and Methods
4.1. Animals
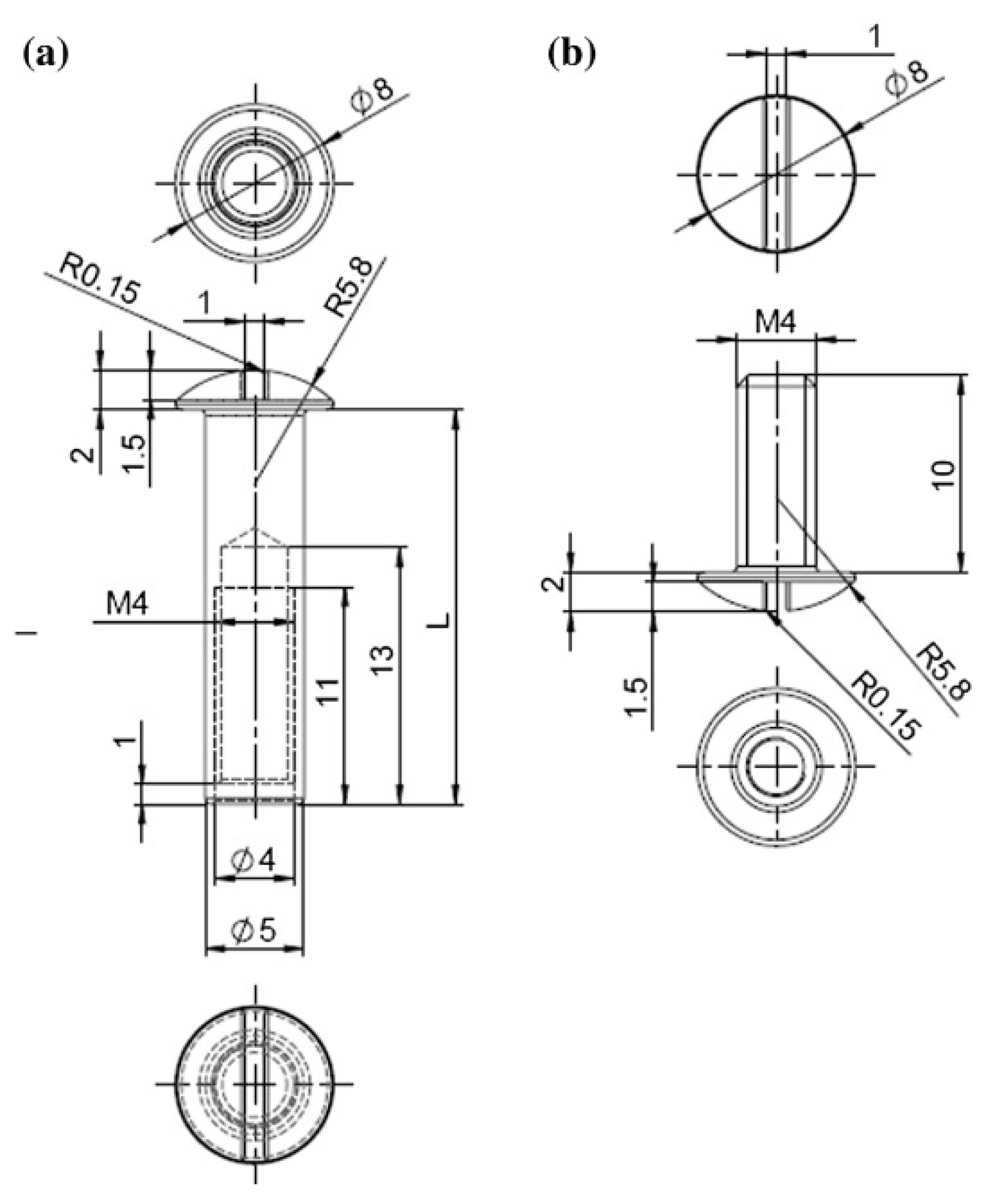
4.2. Design of the Implants
4.3. Preparation of the Copper Modified TiO2-Coatings
4.4. Antibiotic Chain
4.5. Surgical Procedure
4.6. Blood Samples
4.7. Euthanasia
4.8. Microbiology
4.9. Statistics
5. Conclusions
Acknowledgments
Author Contributions
Conflicts of Interest
References
- Organisation for Economic Co-operation and Development (OECD). Health at a Glance 2015; OECD: Paris, France, 2015. [Google Scholar]
- Kurtz, S.M.; Ong, K.L.; Lau, E.; Bozic, K.J.; Berry, D.; Parvizi, J. Prosthetic joint infection risk after TKA in the Medicare population. Clin. Orthop. Relat. Res. 2010, 468, 52–56. [Google Scholar] [CrossRef] [PubMed]
- Berbari, E.F.; Hanssen, A.D.; Duffy, M.C.; Steckelberg, J.M.; Ilstrup, D.M.; Harmsen, W.S.; Osmon, D.R. Risk factors for prosthetic joint infection: Case-control study. Clin. Infect. Dis. 1998, 27, 1247–1254. [Google Scholar] [CrossRef] [PubMed]
- Brandt, C.M.; Duffy, M.C.; Berbari, E.F.; Hanssen, A.D.; Steckelberg, J.M.; Osmon, D.R. Staphylococcus aureus prosthetic joint infection treated with prosthesis removal and delayed reimplantation arthroplasty. Mayo. Clin. Proc. 1999, 74, 553–558. [Google Scholar] [CrossRef] [PubMed]
- Nijhof, M.W.; Fleer, A.; Hardus, K.; Vogely, H.C.; Schouls, L.M.; Verbout, A.J.; Dhert, W.J. Tobramycin-containing bone cement and systemic cefazolin in a one-stage revision. Treatment of infection in a rabbit model. J. Biomed. Mater. Res. 2001, 58, 747–753. [Google Scholar] [CrossRef] [PubMed]
- Hanssen, A.D.; Osmon, D.R.; Nelson, C.L. Prevention of deep periprosthetic joint infection. Instr. Course Lect. 1997, 46, 555–567. [Google Scholar] [PubMed]
- Segawa, H.; Tsukayama, D.T.; Kyle, R.F.; Becker, D.A.; Gustilo, R.B. Infection after total knee arthroplasty. A retrospective study of the treatment of eighty-one infections. J. Bone Joint Surg. Am. 1999, 81, 1434–1445. [Google Scholar] [CrossRef] [PubMed]
- Wilson, M.G.; Kelley, K.; Thornhill, T.S. Infection as a complication of total knee-replacement arthroplasty. Risk factors and treatment in sixty-seven cases. J. Bone Joint Surg. Am. 1990, 72, 878–883. [Google Scholar] [CrossRef] [PubMed]
- Zhao, L.; Chu, P.K.; Zhang, Y.; Wu, Z. Antibacterial coatings on titanium implants. J. Biomed. Mater. Res. B Appl. Biomater. 2009, 91, 470–480. [Google Scholar] [CrossRef] [PubMed]
- Heidenau, F.; Mittelmeier, W.; Detsch, R.; Haenle, M.; Stenzel, F.; Ziegler, G.; Gollwitzer, H. A novel antibacterial titania coating: Metal ion toxicity and in vitro surface colonization. J. Mater. Sci. Mater. Med. 2005, 16, 883–888. [Google Scholar] [CrossRef] [PubMed]
- Mauerer, A.; Lange, B.; Welsch, G.H.; Heidenau, F.; Adler, W.; Forst, R.; Richter, R.H. Release of Cu2+ from a copper-filled TiO2 coating in a rabbit model for total knee arthroplasty. J. Mater. Sci. Mater. Med. 2014, 25, 813–821. [Google Scholar] [CrossRef] [PubMed]
- Reference Values for Laboratory Animals. Available online: http://www.ahc.umn.edu/rar/refvalues.html (accessed on 22 June 2017).
- Bergkvist, M.; Mukka, S.S.; Johansson, L.; Ahl, T.E.; Sayed-Noor, A.S.; Sköldenberg, O.G.; Eisler, T. Debridement, antibiotics and implant retention in early periprosthetic joint infection. Hip Int. 2016, 26, 138–143. [Google Scholar] [CrossRef] [PubMed]
- Odekerken, J.C.; Arts, J.J.; Surtel, D.A.; Walenkamp, G.H.; Welting, T.J. A rabbit osteomyelitis model for the longitudinal assessment of early post-operative implant infections. J. Orthop. Surg. Res. 2013, 8, 38. [Google Scholar] [CrossRef] [PubMed]
- Romanò, C.L.; Gala, L.; Logoluso, N.; Romanò, D.; Drago, L. Two-stage revision of septic knee prosthesis with articulating knee spacers yields better infection eradication rate than one-stage or two-stage revision with static spacers. Knee Surg. Sports Traumatol. Arthrosc. 2012, 20, 2445–2453. [Google Scholar] [CrossRef] [PubMed]
- Bloomfield, M.R.; Klika, A.K.; Barsoum, W.K. Antibiotic-coated spacers for total hip arthroplasty infection. Orthopedics 2010, 33, 649. [Google Scholar] [CrossRef] [PubMed]
- Hofmann, A.A.; Goldberg, T.D.; Tanner, A.M.; Cook, T.M. Ten-year experience using an articulating antibiotic cement hip spacer for the treatment of chronically infected total hip. J. Arthroplasty 2005, 20, 874–879. [Google Scholar] [CrossRef] [PubMed]
- Lee, B.J.; Kyung, H.S.; Yoon, S.D. Two-Stage Revision for Infected Total Knee Arthroplasty: Based on Autoclaving the Recycled Femoral Component and Intraoperative Molding Using Antibiotic-Impregnated Cement on the Tibial Side. Clin. Orthop. Surg. 2015, 7, 310–317. [Google Scholar] [CrossRef] [PubMed]
- Lichstein, P.; Su, S.; Hedlund, H.; Suh, G.; Maloney, W.J.; Goodman, S.B.; Huddleston, J.I. Treatment of Periprosthetic Knee Infection With a Two-stage Protocol Using Static Spacers. Clin. Orthop. Relat. Res. 2016, 474, 120–125. [Google Scholar] [CrossRef] [PubMed]
- Fink, B.; Grossmann, A.; Fuerst, M.; Schäfer, P.; Frommelt, L. Two-stage cementless revision of infected hip endoprostheses. Clin. Orthop. Relat. Res. 2009, 467, 1848–1858. [Google Scholar] [CrossRef] [PubMed]
- Sukeik, M.; Haddad, F.S. Two-stage procedure in the treatment of late chronic hip infections--spacer implantation. Int. J. Med. Sci. 2009, 6, 253–257. [Google Scholar] [CrossRef] [PubMed]
- Ramos, D.; Mar, D.; Ishida, M.; Vargas, R.; Gaite, M.; Montgomery, A.; Linder, M.C. Mechanism of Copper Uptake from Blood Plasma Ceruloplasmin by Mammalian Cells. PLoS ONE 2016, 11, e0149516. [Google Scholar] [CrossRef] [PubMed]
- Cao, D.J.; Hill, J.A. Copper futures: Ceruloplasmin and heart failure. Circ. Res. 2014, 114, 1678–1680. [Google Scholar] [CrossRef] [PubMed]
- Bielli, P.; Calabrese, L. Structure to function relationships in ceruloplasmin: A ‘moonlighting’ protein. Cell. Mol. Life Sci. 2002, 59, 1413–1427. [Google Scholar] [CrossRef] [PubMed]
- Gruys, E.; Toussaint, M.J.; Niewold, T.A.; Koopmans, S.J. Acute phase reaction and acute phase proteins. J. Zhejiang Univ. Sci. B 2005, 6, 1045–1056. [Google Scholar] [CrossRef] [PubMed]
- Mathur, T.; Manadan, A.M.; Thiagarajan, S.; Hota, B.; Block, J.A. Serum transaminases are frequently elevated at time of diagnosis of idiopathic inflammatory myopathy and normalize with creatine kinase. J. Clin. Rheumatol. 2014, 20, 130–132. [Google Scholar] [CrossRef] [PubMed]
- Gopinath, C.; Howell, J.M. Experimental chronic copper toxicity in sheep. Changes that follow the cessation of dosing at the onset of haemolysis. Res. Vet. Sci. 1975, 19, 35–43. [Google Scholar] [PubMed]
- Haenle, M.; Fritsche, A.; Zietz, C.; Bader, R.; Heidenau, F.; Mittelmeier, W.; Gollwitzer, H. An extended spectrum bactericidal titanium dioxide (TiO2) coating for metallic implants: In vitro effectiveness against MRSA and mechanical properties. J. Mater. Sci. Mater. Med. 2011, 22, 381–387. [Google Scholar] [CrossRef] [PubMed]
- Owens, G.J.; Singh, R.K.; Foroutan, F.; Alqaysi, M.; Han, C.H.; Mahapatra, C.; Kim, H.W.; Knowles, J.C. Sol-gel based materials for biomedical applications. Prog. Mater. Sci. 2016, 77, 1–79. [Google Scholar] [CrossRef]
- A Language and Environment for Statistical Computing. Available online: https://www.R-project.org/ (accessed on 22 June 2017).
- Anderson, D.J.; Sexton, D.J.; Kanafani, Z.A.; Auten, G.; Kaye, K.S. Severe surgical site infection in community hospitals: Epidemiology, key procedures, and the changing prevalence of methicillin-resistant Staphylococcus aureus. Infect. Control. Hosp. Epidemiol. 2007, 28, 1047–1053. [Google Scholar] [CrossRef] [PubMed]
- Bjerke-Kroll, B.T.; Christ, A.B.; McLawhorn, A.S.; Sculco, P.K.; Jules-Elysee, K.M.; Sculco, T.P. Periprosthetic joint infections treated with two-stage revision over 14 years: An evolving microbiology profile. J. Arthroplasty 2014, 29, 877–882. [Google Scholar] [CrossRef] [PubMed]
- Parvizi, J.; Adeli, B.; Zmistowski, B.; Restrepo, C.; Greenwald, A.S. Management of periprosthetic joint infection: The current knowledge: AAOS exhibit selection. J. Bone Joint Surg. Am. 2012, 94, e104. [Google Scholar] [CrossRef] [PubMed]
- Parvizi, J.; Erkocak, O.F.; Della Valle, C.J. Culture-negative periprosthetic joint infection. J. Bone Joint Surg. Am. 2014, 96, 430–436. [Google Scholar] [CrossRef] [PubMed]
- Parvizi, J.; Pawasarat, I.M.; Azzam, K.A.; Joshi, A.; Hansen, E.N.; Bozic, K.J. Periprosthetic joint infection: The economic impact of methicillin-resistant infections. J. Arthroplasty 2010, 25, 103–107. [Google Scholar] [CrossRef] [PubMed]
Sample Availability: Samples of the Ti6Al4 bolts are available from the authors. |

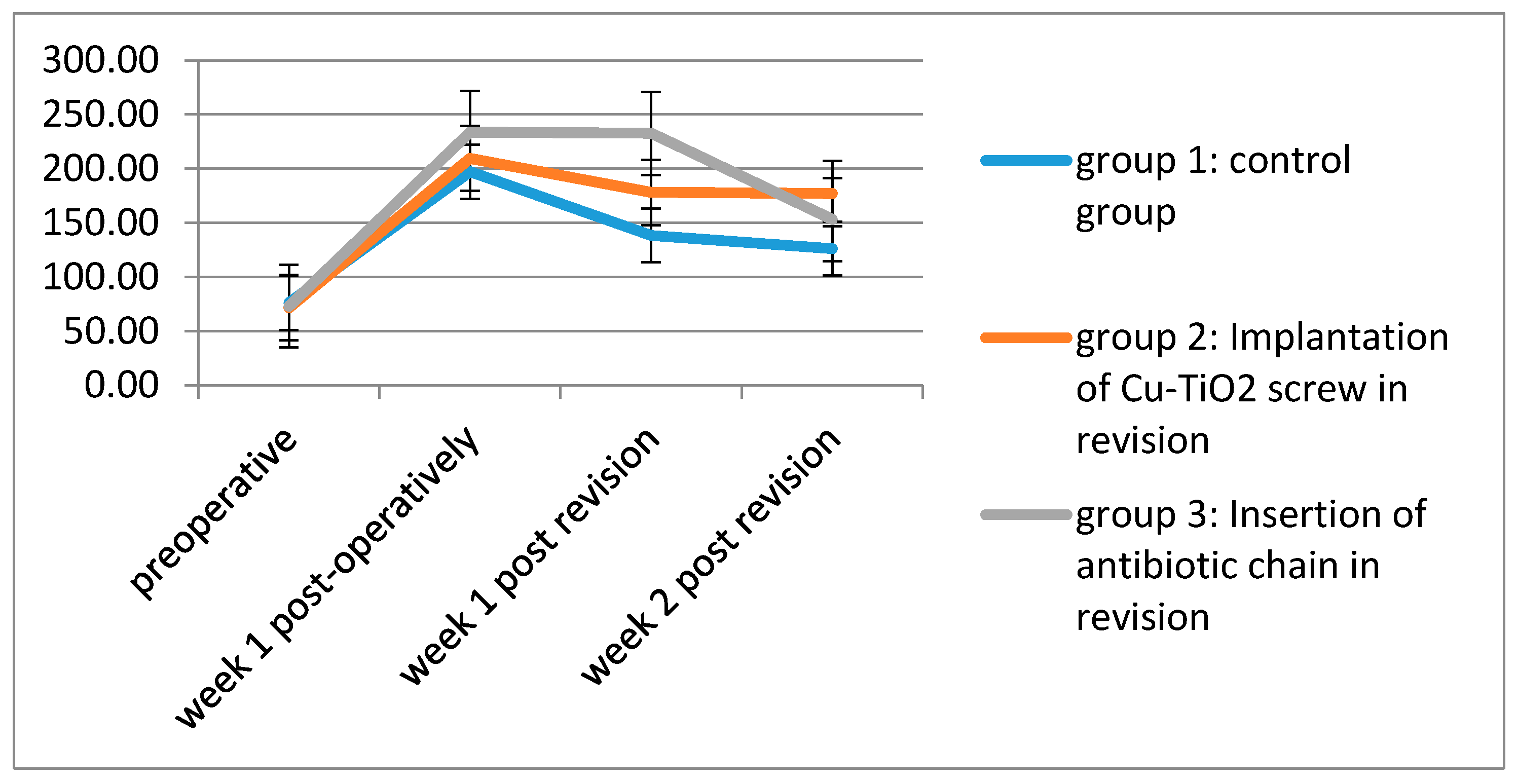


| Units | Group | Preoperative Mean n ± SD | Week 1 Post-Operatively Mean n ± SD | Week 1 Post Revision Mean n ± SD | Week 2 Post Revision Mean n ± SD | |
|---|---|---|---|---|---|---|
| Copper | (μg/dL) | group 1 | 75.98 ±14.86 | 197.21 ± 9.76 | 138.32 ± 73.30 | 126.2 ± 61.14 |
| group 2 | 71.61 ± 17.4 | 209.45 ± 105.2 | 178.06 ± 92.77 | 176.91 ± 92.03 | ||
| group 3 | 73.13 ± 8.3 | 233.51 ± 81.32 | 232.57 ± 102.58 | 153.03 ± 73.76 | ||
| Ceruloplasmin | (mg/dL) | group 1 | 34.68 ± 9.68 | 87.84 ± 56.68 | 65.80 ± 49.20 | 52.55 ± 31.53 |
| group 2 | 26.03 ± 6.68 | 115.71 ± 67.12 | 100.92 ± 48.68 | 99.39 ± 58.08 | ||
| group 3 | 25.98 ± 5.27 | 138.07 ± 67.94 | 153.67 ± 81.37 | 69.53 ± 34.80 | ||
| C-reactive Protein | (μg/mL) | group 1 | 5.2 ± 1.32 | 33.43 ± 28.53 | 11.82 ± 16.44 | 16.14 ± 19.85 |
| group 2 | 4.03 ± 1.07 | 48.49 ± 37.58 | 31.54 ± 21.63 | 31.21 ± 28.87 | ||
| group 3 | 3.89 ± 0.94 | 50.48 ± 27.73 | 36.46 ± 23.25 | 21.20 ± 21.24 | ||
| Leucocytes | (1000/μL) | group 1 | 6.83 ± 1.32 | 8.37 ± 2.47 | 9.23 ± 3.79 | 7.74 ± 2.28 |
| group 2 | 6.31 ± 1.25 | 8.07 ± 1.15 | 10.91 ± 4.11 | 9.24 ± 3.04 | ||
| group 3 | 6.57 ± 1.55 | 8.37 ± 1.97 | 10.37 ± 3.43 | 7.16 ± 2.9 | ||
| Glutamic-Pyruvate Transaminase (GPT) | [U/l] | group 1 | 32.57 ±15.82 | 38.12 ± 82.9 | 35.58 ± 10.82 | 32.25 ± 11.24 |
| group 2 | 38.14 ±11.44 | 72.59 ± 50.20 | 33.83 ± 29.73 | 29.73 ± 12.25 | ||
| group 3 | 40.25 ± 14.59 | 51.5 ± 25.42 | 42.50 ± 24.16 | 34.83 ± 15.58 | ||
| Glutamic-Oxaloacetic Transaminase (GOT) | [U/l] | group 1 | 16.25 ± 4.41 | 31.38 ± 20.54 | 33.75 ± 22.2 | 31.38 ± 16.3 |
| group 2 | 21.76 ± 5.98 | 46.94 ± 30.65 | 27.33 ± 13.4 | 42.09 ± 36.89 | ||
| group 3 | 23.12 ± 4.87 | 42.12 ± 10.05 | 37.38 ± 10.76 | 36.00 ± 12.66 | ||
| Gamma-Glutanyl-Transferase (GGT) | [U/l] | group 1 | 5.88 ± 1.82 | 6.88 ± 2.35 | 7.92 ± 2.23 | 8.38 ± 2.5 |
| group 2 | 6.14 ± 2.15 | 8.76 ± 4.12 | 9.17 ± 3.69 | 8.36 ± 1.22 | ||
| group 3 | 5.75 ± 1.38 | 6.88 ± 1.4 | 9.62 ± 6.27 | 8.17 ± 3.5 | ||
| Creatinine | (mg/dL) | group 1 | 0.75 ± 0.12 | 0.83 ± 0.14 | 0.80 ± 0.18 | 0.91 ± 0.2 |
| group 2 | 1.00 ± 0.29 | 1.08 ± 0.25 | 0.84 ± 0.2 | 0.8 ± 0.15 | ||
| group 3 | 0.81 ± 0.23 | 0.83 ± 0.18 | 1.13 ± 0.66 | 0.81 ± 0.22 |
© 2017 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mauerer, A.; Stenglein, S.; Schulz-Drost, S.; Schoerner, C.; Taylor, D.; Krinner, S.; Heidenau, F.; Adler, W.; Forst, R. Antibacterial Effect of a 4x Cu-TiO2 Coating Simulating Acute Periprosthetic Infection—An Animal Model. Molecules 2017, 22, 1042. https://doi.org/10.3390/molecules22071042
Mauerer A, Stenglein S, Schulz-Drost S, Schoerner C, Taylor D, Krinner S, Heidenau F, Adler W, Forst R. Antibacterial Effect of a 4x Cu-TiO2 Coating Simulating Acute Periprosthetic Infection—An Animal Model. Molecules. 2017; 22(7):1042. https://doi.org/10.3390/molecules22071042
Chicago/Turabian StyleMauerer, Andreas, Stefanie Stenglein, Stefan Schulz-Drost, Christoph Schoerner, Dominic Taylor, Sebastian Krinner, Frank Heidenau, Werner Adler, and Raimund Forst. 2017. "Antibacterial Effect of a 4x Cu-TiO2 Coating Simulating Acute Periprosthetic Infection—An Animal Model" Molecules 22, no. 7: 1042. https://doi.org/10.3390/molecules22071042
APA StyleMauerer, A., Stenglein, S., Schulz-Drost, S., Schoerner, C., Taylor, D., Krinner, S., Heidenau, F., Adler, W., & Forst, R. (2017). Antibacterial Effect of a 4x Cu-TiO2 Coating Simulating Acute Periprosthetic Infection—An Animal Model. Molecules, 22(7), 1042. https://doi.org/10.3390/molecules22071042




