Natural Products to Counteract the Epidemic of Cardiovascular and Metabolic Disorders
Abstract
:1. Introduction
2. Cardiovascular and Metabolic Disorders—A Global Health Problem
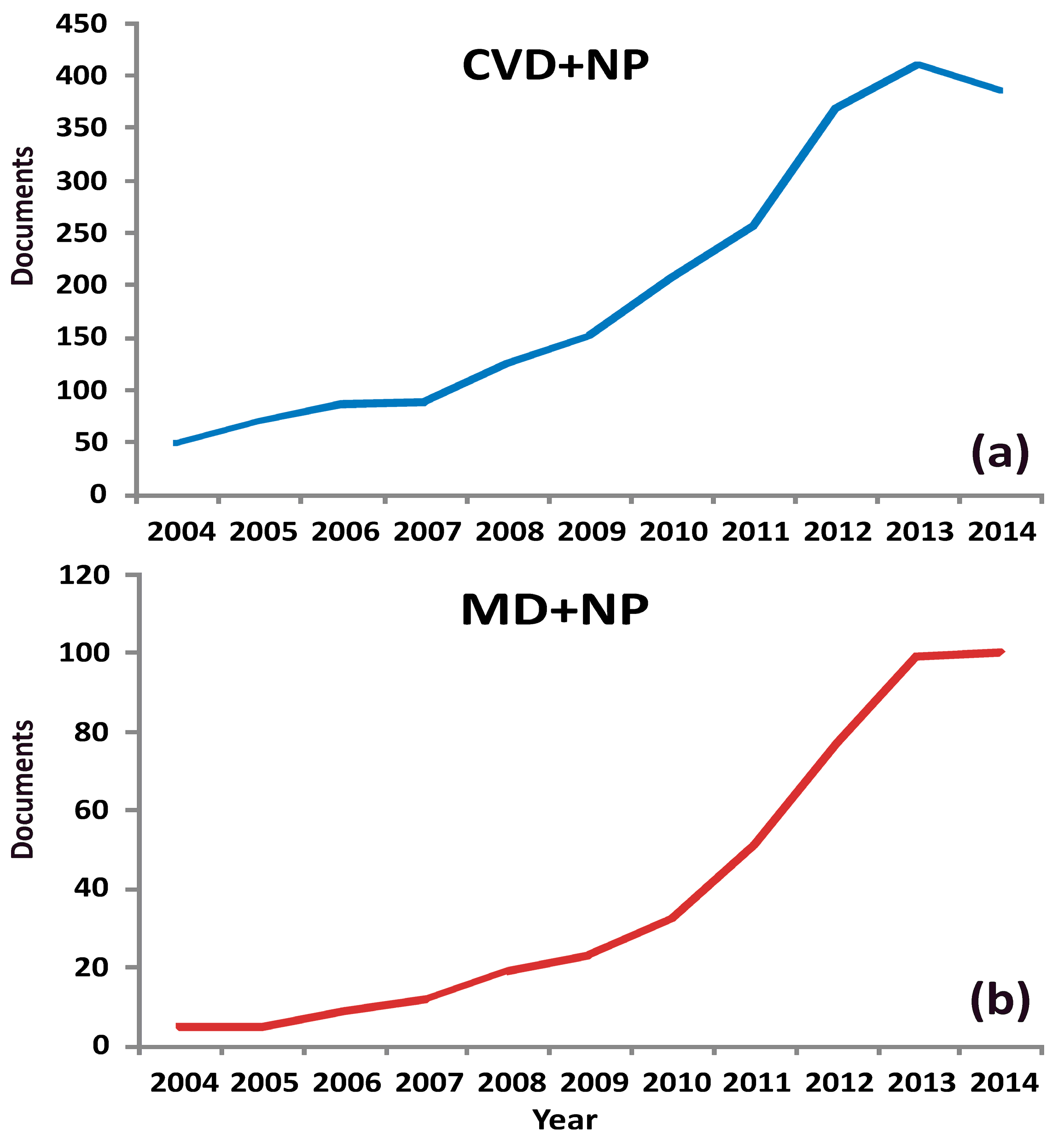
3. Increasing Scientific Interest in Natural Products with Potential Application in Cardiovascular and Metabolic Disorders
4. Plants Traditionally Used in the Context of Cardiovascular and Metabolic Disorders
5. Herbal Products in Recruiting Clinical Trials Targeting Indications Related to Cardiovascular and Metabolic Disorders
6. Dietary Constituents with Potential Benefits in the Context of Cardiovascular and Metabolic Disorders
7. Common Molecular Targets Affected by Natural Compounds in the Context of Cardiovascular and Metabolic Disorders
8. Natural Products (or Their Derivatives) Developed as Drugs for the Treatment of Cardiovascular and Metabolic Disorders
9. Conclusions and Future Perspectives
Acknowledgments
Conflicts of Interest
Abbreviations
| 5-LO | 5-Lipoxygenase |
| AMPK | AMP-Activated Protein Kinase |
| AP-1 | Activator Protein 1 |
| COX-1/2 | Cyclooxygenase-1/2 |
| DPP-4 | Dipeptidyl Peptidase-4 |
| eNOS | Endothelial Nitric Oxide Synthase |
| FDA | US Food and Drug Administration |
| HMG-CoA | 3-Hydroxy-3-Methylglutaryl Coenzyme A |
| HTS | High Throughput Screening |
| IGF-1 | Insulin-Like Growth Factor |
| LDL | Low-Density Lipoprotein |
| NCT | National Clinical Trial |
| NF-κB | Nuclear Factor Kappa B |
| Nrf2 | Nuclear Factor-Erythroid 2-Related Factor 2 |
| NO | Nitric Oxide |
| PPAR | Peroxisome Proliferator-Activated Receptor |
| PTP1B | Protein-Tyrosine Phosphatase 1B |
| TNFα | Tumor Necrosis Factor α |
| VEGF | Vascular Endothelial Growth Factor |
| WHO | World Health Organization |
References
- Atanasov, A.G.; Waltenberger, B.; Pferschy-Wenzig, E.M.; Linder, T.; Wawrosch, C.; Uhrin, P.; Temml, V.; Wang, L.; Schwaiger, S.; Heiss, E.H.; et al. Discovery and resupply of pharmacologically active plant-derived natural products: A review. Biotechnol. Adv. 2015, 33, 1582–1614. [Google Scholar] [CrossRef] [PubMed]
- David, B.; Wolfender, J.-L.; Dias, D.A. The pharmaceutical industry and natural products: Historical status and new trends. Phytochem. Rev. 2015, 14, 299–315. [Google Scholar] [CrossRef]
- Amirkia, V.; Heinrich, M. Natural products and drug discovery: A survey of stakeholders in industry and academia. Front. Pharmacol. 2015, 6. [Google Scholar] [CrossRef] [PubMed]
- Efferth, T.; Zacchino, S.; Georgiev, M.I.; Liu, L.; Wagner, H.; Panossian, A. Nobel Prize for artemisinin brings phytotherapy into the spotlight. Phytomedicine 2015, 22, A1–A3. [Google Scholar] [CrossRef] [PubMed]
- Hertweck, C. Natural products as source of therapeutics against parasitic diseases. Angew. Chem. Int. Ed. Engl. 2015, 54, 14622–14624. [Google Scholar] [CrossRef] [PubMed]
- Cardoso, S.M.; Pereira, O.R.; Seca, A.M.; Pinto, D.C.; Silva, A.M. Seaweeds as preventive agents for cardiovascular diseases: From nutrients to functional foods. Mar. Drugs 2015, 13, 6838–6865. [Google Scholar] [CrossRef] [PubMed]
- Cornish, M.L.; Critchley, A.T.; Mouritsen, O.G. A role for dietary macroalgae in the amelioration of certain risk factors associated with cardiovascular disease. Phycologia 2015, 54, 649–666. [Google Scholar] [CrossRef]
- Tierney, M.S.; Croft, A.K.; Hayes, M. A review of antihypertensive and antioxidant activities in macroalgae. Bot. Mar. 2010, 53, 387–408. [Google Scholar] [CrossRef]
- Wijesekara, I.; Kim, S.K. Angiotensin-I-converting enzyme (ACE) inhibitors from marine resources: Prospects in the pharmaceutical industry. Mar. Drugs 2010, 8, 1080–1093. [Google Scholar] [CrossRef] [PubMed]
- Sperling, L.S.; Mechanick, J.I.; Neeland, I.J.; Herrick, C.J.; Després, J.-P.; Ndumele, C.E.; Vijayaraghavan, K.; Handelsman, Y.; Puckrein, G.A.; Araneta, M.R.G.; et al. The CardioMetabolic Health Alliance: Working toward a new care model for the metabolic syndrome. J. Am. Coll. Cardiol. 2015, 66, 1050–1067. [Google Scholar] [CrossRef] [PubMed]
- Huang, T.H.-W.; Teoh, A.W.; Lin, B.-L.; Lin, D.S.-H.; Roufogalis, B. The role of herbal PPAR modulators in the treatment of cardiometabolic syndrome. Pharmacol. Res. 2009, 60, 195–206. [Google Scholar] [CrossRef] [PubMed]
- Lusis, A.J. Atherosclerosis. Nature 2000, 407, 233–241. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Global Status Report on Noncommunicable Diseases 2014; WHO: Geneva, Switzerland, 2014. [Google Scholar]
- World Health Organization (WHO). Global Report on Diabetes 2016; WHO: Geneva, Switzerland, 2016. [Google Scholar]
- Shaw, J.E.; Sicree, R.A.; Zimmet, P.Z. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Res. Clin. Pract. 2010, 87, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Xiao, J. Natural polyphenols and diabetes: Understanding their mechanism of action. Curr. Med. Chem. 2015, 22, 2–3. [Google Scholar] [CrossRef] [PubMed]
- Cefalu, W.T.; Ye, J.; Wang, Z.Q. Efficacy of dietary supplementation with botanicals on carbohydrate metabolism in humans. Endocr. Metab. Immune Disord. Drug Targets 2008, 8, 78–81. [Google Scholar] [CrossRef] [PubMed]
- Dong, H.; Lu, F.-E.; Zhao, L. Chinese herbal medicine in the treatment of nonalcoholic fatty liver disease. Chin. J. Integr. Med. 2012, 18, 152–160. [Google Scholar] [CrossRef] [PubMed]
- Heber, D. Herbs and atherosclerosis. Curr. Atheroscler. Rep. 2001, 3, 93–96. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization (WHO). Traditional Medicine Strategy 2014–2023; WHO: Geneva, Switzerland, 2013. [Google Scholar]
- Mashour, N.H.; Lin, G.I.; Frishman, W.H. Herbal medicine for the treatment of cardiovascular disease: Clinical considerations. Arch. Intern. Med. 1998, 158, 2225–2234. [Google Scholar] [CrossRef] [PubMed]
- Pittler, M.H.; Ernst, E. Horse chestnut seed extract for chronic venous insufficiency. Cochrane Database Syst. Rev. 2012, 11, CD003230. [Google Scholar] [CrossRef] [PubMed]
- Suter, A.; Bommer, S.; Rechner, J. Treatment of patients with venous insufficiency with fresh plant horse chestnut seed extract: A review of 5 clinical studies. Adv. Ther. 2006, 23, 179–190. [Google Scholar] [CrossRef] [PubMed]
- Siebert, U.; Brach, M.; Sroczynski, G.; Berla, K. Efficacy, routine effectiveness, and safety of horsechestnut seed extract in the treatment of chronic venous insufficiency. A meta-analysis of randomized controlled trials and large observational studies. Int. Angiol. 2002, 21, 305–315. [Google Scholar] [PubMed]
- Rahman, K.; Lowe, G.M. Garlic and cardiovascular disease: A critical review. J. Nutr. 2006, 136, 736S–740S. [Google Scholar] [PubMed]
- Sobenin, I.A.; Nedosugova, L.V.; Filatova, L.V.; Balabolkin, M.I.; Gorchakova, T.V.; Orekhov, A.N. Metabolic effects of time-released garlic powder tablets in type 2 diabetes mellitus: The results of double-blinded placebo-controlled study. Acta Diabetol. 2008, 45, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Al Disi, S.S.; Anwar, M.A.; Eid, A.H. Anti-hypertensive herbs and their mechanism of action: Part I. Front. Pharmacol. 2016, 6. [Google Scholar] [CrossRef] [PubMed]
- Kwak, J.S.; Kim, J.Y.; Paek, J.E.; Lee, Y.J.; Kim, H.R.; Park, D.S.; Kwon, O. Garlic powder intake and cardiovascular risk factors: A meta-analysis of randomized controlled clinical trials. Nutr. Res. Pract. 2014, 8, 644–654. [Google Scholar] [CrossRef] [PubMed]
- Stabler, S.N.; Tejani, A.M.; Huynh, F.; Fowkes, C. Garlic for the prevention of cardiovascular morbidity and mortality in hypertensive patients. Cochrane Database Syst. Rev. 2012, 8, CD007653. [Google Scholar] [PubMed]
- Zeng, T.; Guo, F.F.; Zhang, C.L.; Song, F.Y.; Zhao, X.L.; Xie, K.Q. A meta-analysis of randomized, double-blind, placebo-controlled trials for the effects of garlic on serum lipid profiles. J. Sci. Food Agric. 2012, 92, 1892–1902. [Google Scholar] [CrossRef] [PubMed]
- Okyar, A.; Can, A.; Akev, N.; Baktir, G.; Sütlüpinar, N. Effect of Aloe vera leaves on blood glucose level in type I and type II diabetic rat models. Phytother. Res. 2001, 15, 157–161. [Google Scholar] [CrossRef] [PubMed]
- Rajasekaran, S.; Ravi, K.; Sivagnanam, K.; Subramanian, S. Beneficial effects of Aloe vera leaf gel extract on lipid profile status in rats with streptozotocin diabetes. Clin. Exp. Pharmacol. Physiol. 2006, 33, 232–237. [Google Scholar] [CrossRef] [PubMed]
- Alinejad-Mofrad, S.; Foadoddini, M.; Saadatjoo, S.A.; Shayesteh, M. Improvement of glucose and lipid profile status with Aloe vera in pre-diabetic subjects: A randomized controlled-trial. J. Diabetes Metab. Disord. 2015, 14. [Google Scholar] [CrossRef] [PubMed]
- Dick, W.R.; Fletcher, E.A.; Shah, S.A. Reduction of fasting blood glucose and hemoglobin A1c using oral Aloe vera: A meta-analysis. J. Altern. Complement. Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Devaraj, S.; Yimam, M.; Brownell, L.A.; Jialal, I.; Singh, S.; Jia, Q. Effects of Aloe vera supplementation in subjects with prediabetes/metabolic syndrome. Metab. Syndr. Relat. Disord. 2013, 11, 35–40. [Google Scholar] [CrossRef] [PubMed]
- Hashim, S.; Jan, A.; Marwat, K.B.; Khan, M.A. Phytochemistry and medicinal properties of Ammi visnaga (Apiacae). Pak. J. Bot. 2014, 46, 861–867. [Google Scholar]
- Durate, J.; Vallejo, I.; Perez-Vizcaino, F.; Jimenez, R.; Zarzuelo, A.; Tamargo, J. Effects of visnadine on rat isolated vascular smooth muscles. Planta Med. 1997, 63, 233–236. [Google Scholar] [CrossRef] [PubMed]
- Duarte, J.; Perez-Vizcaino, F.; Torres, A.I.; Zarzuelo, A.; Jimenez, J.; Tamargo, J. Vasodilator effects of visnagin in isolated rat vascular smooth muscle. Eur. J. Pharmacol. 1995, 286, 115–122. [Google Scholar] [CrossRef]
- Hao, P.-P.; Jiang, F.; Chen, Y.-G.; Yang, J.; Zhang, K.; Zhang, M.-X.; Zhang, C.; Zhao, Y.-X.; Zhang, Y. Traditional Chinese medication for cardiovascular disease. Nat. Rev. Cardiol. 2015, 12, 115–122. [Google Scholar] [CrossRef] [PubMed]
- Kim, D.-W.; Yokozawa, T.; Hattori, M.; Kadota, S.; Namba, T. Effects of aqueous extracts of Apocynum venetum leaves on spontaneously hypertensive, renal hypertensive and NaCl-fed-hypertensive rats. J. Ethnopharmacol. 2000, 72, 53–59. [Google Scholar] [CrossRef]
- Xie, W.; Zhang, X.; Wang, T.; Hu, J. Botany, traditional uses, phytochemistry and pharmacology of Apocynum venetum L. (Luobuma): A review. J. Ethnopharmacol. 2012, 141, 1–8. [Google Scholar] [CrossRef] [PubMed]
- Wang, W.; Liang, X.; Fu, D.; Tie, R.; Xing, W.; Ji, L.; Liu, F.; Zhang, H.; Li, R. Apocynum venetum leaf attenuates myocardial ischemia/reperfusion injury by inhibiting oxidative stress. Am. J. Chin. Med. 2015, 43, 71–85. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, S.; Shailendra, G.; Ribnicky, D.M.; Burk, D.; Karki, N.; Qingxia Wang, M.S. An extract of Artemisia dracunculus L. stimulates insulin secretion from β cells, activates AMPK and suppresses inflammation. J. Ethnopharmacol. 2015, 170, 98–105. [Google Scholar] [CrossRef] [PubMed]
- Watcho, P.; Stavniichuk, R.; Tane, P.; Shevalye, H.; Maksimchyk, Y.; Pacher, P.; Obrosova, I.G. Evaluation of PMI-5011, an ethanolic extract of Artemisia dracunculus L., on peripheral neuropathy in streptozotocin-diabetic mice. Int. J. Mol. Med. 2011, 27, 299–307. [Google Scholar] [PubMed]
- Watcho, P.; Stavniichuk, R.; Ribnicky, D.M.; Raskin, I.; Obrosova, I.G. High-fat diet-induced neuropathy of prediabetes and obesity: Effect of PMI-5011, an ethanolic extract of Artemisia dracunculus L. Mediat. Inflamm. 2010, 2010. [Google Scholar] [CrossRef] [PubMed]
- Hamza, N.; Berke, B.; Cheze, C.; Marais, S.; Lorrain, S.; Abdouelfath, A.; Lassalle, R.; Carles, D.; Gin, H.; Moore, N. Effect of Centaurium erythraea Rafn, Artemisia herba-alba Asso and Trigonella foenum-graecum L. on liver fat accumulation in C57BL/6J mice with high-fat diet-induced type 2 diabetes. J. Ethnopharmacol. 2015, 171, 4–11. [Google Scholar] [CrossRef] [PubMed]
- Boudjelal, A.; Siracusa, L.; Henchiri, C.; Sarri, M.; Abderrahim, B.; Baali, F.; Ruberto, G. Antidiabetic effects of aqueous infusions of Artemisia herba-alba and Ajuga iva in alloxan-induced diabetic rats. Planta Med. 2015, 81, 696–704. [Google Scholar] [CrossRef] [PubMed]
- Hamza, N.; Berke, B.; Cheze, C.; Le Garrec, R.; Lassalle, R.; Agli, A.N.; Robinson, P.; Gin, H.; Moore, N. Treatment of high fat diet induced type 2 diabetes in C57BL/6J mice by two medicinal plants used in traditional treatment of diabetes in the east of Algeria. J. Ethnopharmacol. 2011, 133, 931–933. [Google Scholar] [CrossRef] [PubMed]
- Al-Shamaony, L.; al-Khazraji, S.M.; Twaij, H.A. Hypoglycaemic effect of Artemisia herba alba. II. Effect of a valuable extract on some blood parameters in diabetic animals. J. Ethnopharmacol. 1994, 43, 167–171. [Google Scholar] [CrossRef]
- Hamza, N.; Berke, B.; Cheze, C.; Agli, A.N.; Robinson, P.; Gin, H.; Moore, N. Prevention of type 2 diabetes induced by high fat diet in the C57BL/6J mouse by two medicinal plants used in traditional treatment of diabetes in the east of Algeria. J. Ethnopharmacol. 2010, 128, 513–518. [Google Scholar] [CrossRef] [PubMed]
- Kawano, A.; Nakamura, H.; Hata, S.-I.; Minakawa, M.; Miura, Y.; Yagasaki, K. Hypoglycemic effect of aspalathin, a rooibos tea component from Aspalathus linearis, in type 2 diabetic model db/db mice. Phytomedicine 2009, 16, 437–443. [Google Scholar] [CrossRef] [PubMed]
- Son, M.J.; Minakawa, M.; Miura, Y.; Yagasaki, K. Aspalathin improves hyperglycemia and glucose intolerance in obese diabetic ob/ob mice. Eur. J. Nutr. 2013, 52, 1607–1619. [Google Scholar] [CrossRef] [PubMed]
- Mazibuko, S.E.; Joubert, E.; Johnson, R.; Louw, J.; Opoku, A.R.; Muller, C.J. Aspalathin improves glucose and lipid metabolism in 3T3-L1 adipocytes exposed to palmitate. Mol. Nutr. Food Res. 2015, 59, 2199–2208. [Google Scholar] [CrossRef] [PubMed]
- Ku, S.K.; Kwak, S.; Kim, Y.; Bae, J.S. Aspalathin and nothofagin from rooibos (Aspalathus linearis) inhibits high glucose-induced inflammation in vitro and in vivo. Inflammation 2015, 38, 445–455. [Google Scholar] [CrossRef] [PubMed]
- Chen, W.; Lai, Y.; Wang, L.; Xia, Y.; Chen, W.; Zhao, X.; Yu, M.; Li, Y.; Zhang, Y.; Ye, H. Astragalus polysaccharides repress myocardial lipotoxicity in a PPARalpha-dependent manner in vitro and in vivo in mice. J. Diabetes Complicat. 2015, 29, 164–175. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.; Moon, E.; Kwon, S. Effect of Astragalus membranaceus extract on diabetic nephropathy. Endocrinol. Diabetes Metab. Case Rep. 2014, 2014. [Google Scholar] [CrossRef] [PubMed]
- Qin, H.; Liu, P.; Lin, S. Effects of astragaloside IV on the SDF-1/CXCR4 expression in atherosclerosis of apoE−/− mice induced by hyperlipaemia. Evid. Based Complement. Altern. Med. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Zhao, P.; Wang, Y.; Zeng, S.; Lu, J.; Jiang, T.-M.; Li, Y.-M. Protective effect of astragaloside IV on lipopolysaccharide-induced cardiac dysfunction via downregulation of inflammatory signaling in mice. Immunopharmacol. Immunotoxicol. 2015, 37, 428–433. [Google Scholar] [CrossRef] [PubMed]
- Lu, Y.; Li, S.; Wu, H.; Bian, Z.; Xu, J.; Gu, C.; Chen, X.; Yang, D. Beneficial effects of astragaloside IV against angiotensin II-induced mitochondrial dysfunction in rat vascular smooth muscle cells. Int. J. Mol. Med. 2015, 36, 1223–1232. [Google Scholar] [CrossRef] [PubMed]
- Bai, Y.; Lu, P.; Han, C.; Yu, C.; Chen, M.; He, F.; Yi, D.; Wu, L. Hydroxysafflor yellow A (HSYA) from flowers of Carthamus tinctorius L. and its vasodilatation effects on pulmonary artery. Molecules 2012, 17, 14918–14927. [Google Scholar] [CrossRef] [PubMed]
- Nie, P.H.; Zhang, L.; Zhang, W.H.; Rong, W.F.; Zhi, J.M. The effects of hydroxysafflor yellow A on blood pressure and cardiac function. J. Ethnopharmacol. 2012, 139, 746–750. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.; Deng, J.; Zhang, Y.; Yang, J.; He, Y.; Fu, W.; Xing, P.; Wan, H.T. Lipid-lowering effects of Danhong injection on hyperlipidemia rats. J. Ethnopharmacol. 2014, 154, 437–442. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Dong, P.; Hou, C.; Cao, F.; Sun, S.; He, F.; Song, Y.; Li, S.; Bai, Y.; Zhu, D. Hydroxysafflor yellow A (HSYA) attenuates hypoxic pulmonary arterial remodelling and reverses right ventricular hypertrophy in rats. J. Ethnopharmacol. 2016, 186, 224–233. [Google Scholar] [CrossRef] [PubMed]
- Maneesai, P.; Prasarttong, P.; Bunbupha, S.; Kukongviriyapan, U.; Kukongviriyapan, V.; Tangsucharit, P.; Prachaney, P.; Pakdeechote, P. Synergistic antihypertensive effect of Carthamus tinctorius L. extract and captopril in l-NAME-induced hypertensive rats via restoration of eNOS and AT1R expression. Nutrients 2016, 8. [Google Scholar] [CrossRef] [PubMed]
- Sefi, M.; Fetoui, H.; Lachkar, N.; Tahraoui, A.; Lyoussi, B.; Boudawara, T.; Zeghal, N. Centaurium erythrea (Gentianaceae) leaf extract alleviates streptozotocin-induced oxidative stress and β-cell damage in rat pancreas. J. Ethnopharmacol. 2011, 135, 243–250. [Google Scholar] [CrossRef] [PubMed]
- Stefkov, G.; Miova, B.; Dinevska-Kjovkarovska, S.; Stanoeva, J.P.; Stefova, M.; Petrusevska, G.; Kulevanova, S. Chemical characterization of Centaurium erythrea L. and its effects on carbohydrate and lipid metabolism in experimental diabetes. J. Ethnopharmacol. 2014, 152, 71–77. [Google Scholar] [CrossRef] [PubMed]
- Eddouks, M.; Bidi, A.; El Bouhali, B.; Hajji, L.; Zeggwagh, N.A. Antidiabetic plants improving insulin sensitivity. J. Pharm. Pharmacol. 2014, 66, 1197–1214. [Google Scholar] [CrossRef] [PubMed]
- Yan, Y.-M.; Fang, P.; Yang, M.-T.; Li, N.; Lu, Q.; Cheng, Y.-X. Anti-diabetic nephropathy compounds from Cinnamomum cassia. J. Ethnopharmacol. 2015, 165, 141–147. [Google Scholar] [CrossRef] [PubMed]
- Medagama, A.B. The glycaemic outcomes of cinnamon, a review of the experimental evidence and clinical trials. Nutr. J. 2015, 14. [Google Scholar] [CrossRef] [PubMed]
- Crawford, P. Effectiveness of cinnamon for lowering hemoglobin A1C in patients with type 2 diabetes: A randomized, controlled trial. J. Am. Board Fam. Med. 2009, 22, 507–512. [Google Scholar] [CrossRef] [PubMed]
- Mirfeizi, M.; Mehdizadeh Tourzani, Z.; Mirfeizi, S.Z.; Asghari Jafarabadi, M.; Rezvani, H.R.; Afzali, M.; Gholami, M.J. Controlling diabetes mellitus type 2 with herbal medicines: A triple blind, randomized clinical trial of efficacy and safety. J. Diabetes 2015. [Google Scholar] [CrossRef] [PubMed]
- Ríos, J.L.; Francini, F.; Schinella, G.R. Natural products for the treatment of type 2 diabetes mellitus. Planta Med. 2015, 81, 975–994. [Google Scholar] [CrossRef] [PubMed]
- Whitfield, P.; Parry-Strong, A.; Walsh, E.; Weatherall, M.; Krebs, J.D. The effect of a cinnamon-, chromium- and magnesium-formulated honey on glycaemic control, weight loss and lipid parameters in type 2 diabetes: An open-label cross-over randomised controlled trial. Eur. J. Nutr. 2016, 55, 1123–1131. [Google Scholar] [CrossRef] [PubMed]
- Beejmohun, V.; Peytavy-Izard, M.; Mignon, C.; Muscente-Paque, D.; Deplanque, X.; Ripoll, C.; Chapal, N. Acute effect of Ceylon cinnamon extract on postprandial glycemia: Alpha-amylase inhibition, starch tolerance test in rats, and randomized crossover clinical trial in healthy volunteers. BMC Complement. Altern. Med. 2014, 14. [Google Scholar] [CrossRef] [PubMed]
- Frishman, W.H.; Beravol, P.; Carosella, C. Alternative and complementary medicine for preventing and treating cardiovascular disease. Dis. Mon. 2009, 55, 121–192. [Google Scholar] [CrossRef] [PubMed]
- Ojha, S.K.; Nandave, M.; Arora, S.; Mehra, R.D.; Joshi, S.; Narang, R.; Arya, D.S. Effect of Commiphora mukul extract on cardiac dysfunction and ventricular function in isoproterenol-induced myocardial infarction. Indian J. Exp. Biol. 2008, 46, 646–652. [Google Scholar] [PubMed]
- Yuan, L.; Tu, D.; Ye, X.; Wu, J. Hypoglycemic and hypocholesterolemic effects of Coptis chinensis Franch inflorescence. Plant Foods Hum. Nutr. 2006, 61, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Dong, H.; Wang, J.-H.; Lu, F.-E.; Xu, L.-J.; Gong, Y.-L.; Zou, X. Jiaotai Pill enhances insulin signaling through phosphatidylinositol 3-kinase pathway in skeletal muscle of diabetic rats. Chin. J. Integr. Med. 2013, 19, 668–674. [Google Scholar] [CrossRef] [PubMed]
- Yang, Z.; Wang, L.; Zhang, F.; Li, Z. Evaluating the antidiabetic effects of Chinese herbal medicine: Xiao-Ke-An in 3T3-L1 cells and KKAy mice using both conventional and holistic omics approaches. BMC Complement. Altern. Med. 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Eidi, M.; Eidi, A.; Saeidi, A.; Molanaei, S.; Sadeghipour, A.; Bahar, M.; Bahar, K. Effect of coriander seed (Coriandrum sativum L.) ethanol extract on insulin release from pancreatic beta cells in streptozotocin-induced diabetic rats. Phytother. Res. 2009, 23, 404–406. [Google Scholar] [CrossRef] [PubMed]
- Dhanapakiam, P.; Joseph, J.M.; Ramaswamy, V.K.; Moorthi, M.; Kumar, A.S. The cholesterol lowering properties of coriander seeds (Coriandrum sativum): Mechanism of action. J. Environ. Biol. 2008, 29, 53–56. [Google Scholar] [PubMed]
- Sreelatha, S.; Inbavalli, R. Antioxidant, antihyperglycemic, and antihyperlipidemic effects of Coriandrum sativum leaf and stem in alloxan-induced diabetic rats. J. Food Sci. 2012, 77, T119–T123. [Google Scholar] [CrossRef] [PubMed]
- Aissaoui, A.; Zizi, S.; Israili, Z.H.; Lyoussi, B. Hypoglycemic and hypolipidemic effects of Coriandrum sativum L. in Meriones shawi rats. J. Ethnopharmacol. 2011, 137, 652–661. [Google Scholar] [CrossRef] [PubMed]
- Chang, W.-T.; Dao, J.; Shao, Z.-H. Hawthorn: Potential roles in cardiovascular disease. Am. J. Chin. Med. 2005, 33, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Chrysant, S.G. The clinical significance and costs of herbs and food supplements used by complementary and alternative medicine for the treatment of cardiovascular diseases and hypertension. J. Hum. Hypertens. 2016, 30, 1–6. [Google Scholar] [CrossRef] [PubMed]
- Asher, G.N.; Viera, A.J.; Weaver, M.A.; Dominik, R.; Caughey, M.; Hinderliter, A.L. Effect of hawthorn standardized extract on flow mediated dilation in prehypertensive and mildly hypertensive adults: A randomized, controlled cross-over trial. BMC Complement. Altern. Med. 2012, 12. [Google Scholar] [CrossRef] [PubMed]
- Pittler, M.H.; Guo, R.; Ernst, E. Hawthorn extract for treating chronic heart failure. Cochrane Database Syst. Rev. 2008, 1, CD005312. [Google Scholar] [PubMed]
- Bundy, R.; Walker, A.F.; Middleton, R.W.; Wallis, C.; Simpson, H.C.R. Artichoke leaf extract (Cynara scolymus) reduces plasma cholesterol in otherwise healthy hypercholesterolemic adults: A randomized, double blind placebo controlled trial. Phytomedicine 2008, 15, 668–675. [Google Scholar] [CrossRef] [PubMed]
- Ben Salem, M.; Affes, H.; Ksouda, K.; Dhouibi, R.; Sahnoun, Z.; Hammami, S.; Zeghal, K.M. Pharmacological studies of artichoke leaf extract and their health benefits. Plant Foods Hum. Nutr. 2015, 70, 441–453. [Google Scholar] [CrossRef] [PubMed]
- Maghrani, M.; Zeggwagh, N.-A.; Lemhadri, A.; El Amraoui, M.; Michel, J.-B.; Eddouks, M. Study of the hypoglycaemic activity of Fraxinus excelsior and Silybum marianum in an animal model of type 1 diabetes mellitus. J. Ethnopharmacol. 2004, 91, 309–316. [Google Scholar] [CrossRef] [PubMed]
- Eddouks, M.; Maghrani, M. Phlorizin-like effect of Fraxinus excelsior in normal and diabetic rats. J. Ethnopharmacol. 2004, 94, 149–154. [Google Scholar] [CrossRef] [PubMed]
- Gomez-Garcia, F.; Flanagan, J.; García-Molina, O.; Vilaplana-Vivo, V.; García-Carrillo, N.; Berthon, P.F.; Bily, A.; Roller, M.; Ortega, V.V.; Issaly, N. Preventive effect of a Fraxinus excelsior L seeds/fruits extract on hepatic steatosis in obese type 2 diabetic mice. J. Diabetes Metab. 2015, 6. [Google Scholar] [CrossRef]
- Visen, P.; Saraswat, B.; Visen, A.; Roller, M.; Bily, A.; Mermet, C.; He, K.; Bai, N.; Lemaire, B.; Lafay, S.; et al. Acute effects of Fraxinus excelsior L. seed extract on postprandial glycemia and insulin secretion on healthy volunteers. J. Ethnopharmacol. 2009, 126, 226–232. [Google Scholar] [CrossRef] [PubMed]
- Bai, N.; He, K.; Ibarra, A.; Bily, A.; Roller, M.; Chen, X.; Rülh, R. Iridoids from Fraxinus excelsior with adipocyte differentiation-inhibitory and PPARα activation activity. J. Nat. Prod. 2010, 73, 2–6. [Google Scholar] [CrossRef] [PubMed]
- Zulet, M.A.; Navas-Carretero, S.; Lara y Sanchez, D.; Abete, I.; Flanagan, J.; Issaly, N.; Fanca-Berthon, P.; Bily, A.; Roller, M.; Martinez, J.A. A Fraxinus excelsior L. seeds/fruits extract benefits glucose homeostasis and adiposity related markers in elderly overweight/obese subjects: A longitudinal, randomized, crossover, double-blind, placebo-controlled nutritional intervention study. Phytomedicine 2014, 21, 1162–1169. [Google Scholar] [CrossRef] [PubMed]
- Bedekar, A.; Shah, K.; Koffas, M. Natural products for type II diabetes treatment. Adv. Appl. Microbiol. 2010, 71, 21–73. [Google Scholar] [PubMed]
- Perla, V.; Jayanty, S.S. Biguanide related compounds in traditional antidiabetic functional foods. Food Chem. 2013, 138, 1574–1580. [Google Scholar] [CrossRef] [PubMed]
- Witters, L.A. The blooming of the French lilac. J. Clin. Investig. 2001, 108, 1105–1107. [Google Scholar] [CrossRef] [PubMed]
- Gardner, C.D.; Zehnder, J.L.; Rigby, A.J.; Nicholus, J.R.; Farquhar, J.W. Effect of Ginkgo biloba (EGb 761) and aspirin on platelet aggregation and platelet function analysis among older adults at risk of cardiovascular disease: A randomized clinical trial. Blood Coagul. Fibrinolysis 2007, 18, 787–793. [Google Scholar] [CrossRef] [PubMed]
- Lu, Q.; Zuo, W.-Z.; Ji, X.-J.; Zhou, Y.-X.; Liu, Y.-Q.; Yao, X.-Q.; Zhou, X.-Y.; Liu, Y.-W.; Zhang, F.; Yin, X.-X. Ethanolic Ginkgo biloba leaf extract prevents renal fibrosis through Akt/mTOR signaling in diabetic nephropathy. Phytomedicine 2015, 22, 1071–1078. [Google Scholar] [CrossRef] [PubMed]
- Erukainure, O.L.; Ajiboye, J.A.; Lawal, B.A.; Obode, O.C.; Okoro, E.E.; Amisu-Tugbobo, A.O.; Zaruwa, M.Z. Alterations in atherogenic indices and hypolipidemic effect of soybean oil in normocholesteremic rats. Comp. Clin. Pathol. 2016, 25, 75–78. [Google Scholar] [CrossRef]
- Kwon, D.Y.; Daily, J.W.; Kim, H.J.; Park, S. Antidiabetic effects of fermented soybean products on type 2 diabetes. Nutr. Res. 2010, 30, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Jiang, H.; Tong, Y.; Yan, D.; Jia, S.; Ostenson, C.G.; Chen, Z. The soybean peptide vglycin preserves the diabetic beta-cells through improvement of proliferation and inhibition of apoptosis. Sci. Rep. 2015, 5. [Google Scholar] [CrossRef]
- Fuhrman, B.; Volkova, N.; Kaplan, M.; Presser, D.; Attias, J.; Hayek, T.; Aviram, M. Antiatherosclerotic effects of licorice extract supplementation on hypercholesterolemic patients: Increased resistance of LDL to atherogenic modifications, reduced plasma lipid levels, and decreased systolic blood pressure. Nutrition 2002, 18, 268–273. [Google Scholar] [CrossRef]
- Chang, W.-C.; Jia, H.; Aw, W.; Saito, K.; Hasegawa, S.; Kato, H. Beneficial effects of soluble dietary Jerusalem artichoke (Helianthus tuberosus) in the prevention of the onset of type 2 diabetes and non-alcoholic fatty liver disease in high-fructose diet-fed rats. Br. J. Nutr. 2014, 112, 709–717. [Google Scholar] [CrossRef] [PubMed]
- Gambero, A.; Ribeiro, M.L. The positive effects of yerba maté (Ilex paraguariensis) in obesity. Nutrients 2015, 7, 730–750. [Google Scholar] [CrossRef] [PubMed]
- De Moraes Pontilho, P.; Nunes da Costa Teixeira, A.M.; Yuan, C.; Alves Luzia, L.; Markowicz Bastos, D.H.; Rondó, P.H. Yerba mate (Ilex paraguariensis A. St. Hil) and risk factors for cardiovascular diseases. J. Food Nutr. Res. 2015, 3, 182–190. [Google Scholar] [CrossRef]
- Cardozo, E.L., Jr.; Morand, C. Interest of mate (Ilex paraguariensis A. St.-Hil.) as a new natural functional food to preserve human cardiovascular health—A review. J. Funct. Foods 2016, 21, 440–454. [Google Scholar] [CrossRef]
- Chang, C.L.T.; Lin, Y.; Bartolome, A.P.; Chen, Y.-C.; Chiu, S.-C.; Yang, W.-C. Herbal therapies for type 2 diabetes mellitus: Chemistry, biology, and potential application of selected plants and compounds. Evid. Based Complement. Alternat. Med. 2013, 2013. [Google Scholar] [CrossRef] [PubMed]
- Kim, S.-Y.; Oh, M.-R.; Kim, M.-G.; Chae, H.-J.; Chae, S.-W. Anti-obesity effects of yerba mate (Ilex Paraguariensis): A randomized, double-blind, placebo-controlled clinical trial. BMC Complement. Altern. Med. 2015, 15. [Google Scholar] [CrossRef] [PubMed]
- Yu, S.; Yue, S.w.; Liu, Z.; Zhang, T.; Xiang, N.; Fu, H. Yerba mate (Ilex paraguariensis) improves microcirculation of volunteers with high blood viscosity: A randomized, double-blind, placebo-controlled trial. Exp. Gerontol. 2015, 62, 14–22. [Google Scholar] [CrossRef] [PubMed]
- Luo, Q.; Cai, Y.; Yan, J.; Sun, M.; Corke, H. Hypoglycemic and hypolipidemic effects and antioxidant activity of fruit extracts from Lycium barbarum. Life Sci. 2004, 76, 137–149. [Google Scholar] [CrossRef] [PubMed]
- Zhao, R.; Jin, R.; Chen, Y.; Han, F.-m. Hypoglycemic and hypolipidemic effects of Lycium barbarum polysaccharide in diabetic rats. Chin. Herb. Med. 2015, 7, 310–315. [Google Scholar] [CrossRef]
- Amagase, H.; Nance, D.M. A randomized, double-blind, placebo-controlled, clinical study of the general effects of a standardized Lycium barbarum (Goji) juice, GoChi™. J. Altern. Complement. Med. 2008, 14, 403–412. [Google Scholar] [CrossRef] [PubMed]
- Zhang, X.; Yang, X.; Lin, Y.; Suo, M.; Gong, L.; Chen, J.; Hui, R. Anti-hypertensive effect of Lycium barbarum L. with down-regulated expression of renal endothelial lncRNA sONE in a rat model of salt-sensitive hypertension. Int. J. Clin. Exp. Pathol. 2015, 8, 6981–6987. [Google Scholar] [PubMed]
- Lu, S.-P.; Zhao, P.-T. Chemical characterization of Lycium barbarum polysaccharides and their reducing myocardial injury in ischemia/reperfusion of rat heart. Int. J. Biol. Macromol. 2010, 47, 681–684. [Google Scholar] [CrossRef] [PubMed]
- Ming, M.; Guanhua, L.; Zhanhai, Y.; Guang, C.; Xuan, Z. Effect of the Lycium barbarum polysaccharides administration on blood lipid metabolism and oxidative stress of mice fed high-fat diet in vivo. Food Chem. 2009, 113, 872–877. [Google Scholar] [CrossRef]
- Cai, H.; Liu, F.; Zuo, P.; Huang, G.; Song, Z.; Wang, T.; Lu, H.; Guo, F.; Han, C.; Sun, G. Practical application of antidiabetic efficacy of Lycium barbarum polysaccharide in patients with type 2 diabetes. Med. Chem. 2015, 11, 383–390. [Google Scholar] [CrossRef] [PubMed]
- Zhu, X.; Hu, S.; Zhu, L.; Ding, J.; Zhou, Y.; Li, G. Effects of Lycium barbarum polysaccharides on oxidative stress in hyperlipidemic mice following chronic composite psychological stress intervention. Mol. Med. Rep. 2015, 11, 3445–3450. [Google Scholar] [CrossRef] [PubMed]
- Mishra, A.; Gautam, S.; Pal, S.; Mishra, A.; Rawat, A.K.; Maurya, R.; Srivastava, A.K. Effect of Momordica charantia fruits on streptozotocin-induced diabetes mellitus and its associated complications. Int. J. Pharm. Pharm. Sci. 2015, 7, 356–363. [Google Scholar]
- Yang, S.J.; Choi, J.M.; Park, S.E.; Rhee, E.J.; Lee, W.Y.; Oh, K.W.; Park, S.W.; Park, C.-Y. Preventive effects of bitter melon (Momordica charantia) against insulin resistance and diabetes are associated with the inhibition of NF-κB and JNK pathways in high-fat-fed OLETF rats. J. Nutr. Biochem. 2015, 26, 234–240. [Google Scholar] [CrossRef] [PubMed]
- Singab, A.N.B.; El-Beshbishy, H.A.; Yonekawa, M.; Nomura, T.; Fukai, T. Hypoglycemic effect of Egyptian Morus alba root bark extract: Effect on diabetes and lipid peroxidation of streptozotocin-induced diabetic rats. J. Ethnopharmacol. 2005, 100, 333–338. [Google Scholar] [CrossRef] [PubMed]
- Hunyadi, A.; Martins, A.; Hsieh, T.-J.; Seres, A.; Zupkó, I. Chlorogenic acid and rutin play a major role in the in vivo anti-diabetic activity of Morus alba leaf extract on type II diabetic rats. PLoS ONE 2012, 7, e50619. [Google Scholar] [CrossRef] [PubMed]
- Butt, M.S.; Nazir, A.; Sultan, M.T.; Schroën, K. Morus alba L. nature’s functional tonic. Trends Food Sci. Technol. 2008, 19, 505–512. [Google Scholar] [CrossRef]
- Cai, S.; Sun, W.; Fan, Y.; Guo, X.; Xu, G.; Xu, T.; Hou, Y.; Zhao, B.; Feng, X.; Liu, T. Effect of mulberry leaf (Folium mori) on insulin resistance via IRS-1/PI3K/Glut-4 signalling pathway in type 2 diabetes mellitus rats. Pharm. Biol. 2016. [Google Scholar] [CrossRef] [PubMed]
- Mahmoud, A.M.; Abd El-Twab, S.M.; Abdel-Reheim, E.S. Consumption of polyphenol-rich Morus alba leaves extract attenuates early diabetic retinopathy: The underlying mechanism. Eur. J. Nutr. 2016. [Google Scholar] [CrossRef] [PubMed]
- Phimarn, W.; Wichaiyo, K.; Silpsavikul, K.; Sungthong, B.; Saramunee, K. A meta-analysis of efficacy of Morus alba Linn. to improve blood glucose and lipid profile. Eur. J. Nutr. 2016. [Google Scholar] [CrossRef] [PubMed]
- Heshmati, J.; Namazi, N. Effects of black seed (Nigella sativa) on metabolic parameters in diabetes mellitus: A systematic review. Complement. Ther. Med. 2015, 23, 275–282. [Google Scholar] [CrossRef] [PubMed]
- Heshmati, J.; Namazi, N.; Memarzadeh, M.-R.; Taghizadeh, M.; Kolahdooz, F. Nigella sativa oil affects glucose metabolism and lipid concentrations in patients with type 2 diabetes: A randomized, double-blind, placebo-controlled trial. Food Res. Int. 2015, 70, 87–93. [Google Scholar] [CrossRef]
- Kaatabi, H.; Bamosa, A.O.; Badar, A.; Al-Elq, A.; Abou-Hozaifa, B.; Lebda, F.; Al-Khadra, A.; Al-Almaie, S. Nigella sativa improves glycemic control and ameliorates oxidative stress in patients with type 2 diabetes mellitus: Placebo controlled participant blinded clinical trial. PLoS ONE 2015, 10, e0113486. [Google Scholar] [CrossRef] [PubMed]
- Mahdavi, R.; Namazi, N.; Alizadeh, M.; Farajnia, S. Effects of Nigella sativa oil with a low-calorie diet on cardiometabolic risk factors in obese women: A randomized controlled clinical trial. Food Funct. 2015, 6, 2041–2048. [Google Scholar] [CrossRef] [PubMed]
- Asgary, S.; Sahebkar, A.; Goli-Malekabadi, N. Ameliorative effects of Nigella sativa on dyslipidemia. J. Endocrinol. Investig. 2015, 38, 1039–1046. [Google Scholar] [CrossRef] [PubMed]
- Husain, I.; Chander, R.; Saxena, J.K.; Mahdi, A.A.; Mahdi, F. Antidyslipidemic effect of Ocimum sanctum leaf extract in streptozotocin induced diabetic rats. Indian J. Clin. Biochem. 2015, 30, 72–77. [Google Scholar] [CrossRef] [PubMed]
- Thadani, S.; Salman, M.T.; Tewari, S.; Singh, S.; Bhagchandani, D.; Ahmad, A. Renoprotective effect of Ocimum sanctum in comparison with olmesartan medoxomil and pitavastatin in metformin treated diabetic rats. Int. J. Pharm. Sci. Res. 2015, 6, 4433–4441. [Google Scholar]
- El, S.N.; Karakaya, S. Olive tree (Olea europaea) leaves: Potential beneficial effects on human health. Nutr. Rev. 2009, 67, 632–638. [Google Scholar] [CrossRef] [PubMed]
- Poudyal, H.; Campbell, F.; Brown, L. Olive leaf extract attenuates cardiac, hepatic, and metabolic changes in high carbohydrate-, high fat-fed rats. J. Nutr. 2010, 140, 946–953. [Google Scholar] [CrossRef] [PubMed]
- Susalit, E.; Agus, N.; Effendi, I.; Tjandrawinata, R.R.; Nofiarny, D.; Perrinjaquet-Moccetti, T.; Verbruggen, M. Olive (Olea europaea) leaf extract effective in patients with stage-1 hypertension: Comparison with captopril. Phytomedicine 2011, 18, 251–258. [Google Scholar] [CrossRef] [PubMed]
- Efentakis, P.; Iliodromitis, E.K.; Mikros, E.; Papachristodoulou, A.; Dagres, N.; Skaltsounis, A.-L.; Andreadou, I. Effects of the olive tree leaf constituents on myocardial oxidative damage and atherosclerosis. Planta Med. 2015, 81, 648–654. [Google Scholar] [CrossRef] [PubMed]
- Wainstein, J.; Ganz, T.; Boaz, M.; Bar Dayan, Y.; Dolev, E.; Kerem, Z.; Madar, Z. Olive leaf extract as a hypoglycemic agent in both human diabetic subjects and in rats. J. Med. Food 2012, 15, 605–610. [Google Scholar] [CrossRef] [PubMed]
- Lepore, S.M.; Morittu, V.M.; Celano, M.; Trimboli, F.; Oliverio, M.; Procopio, A.; Di Loreto, C.; Damante, G.; Britti, D.; Bulotta, S.; et al. Oral administration of oleuropein and its semisynthetic peracetylated derivative prevents hepatic steatosis, hyperinsulinemia, and weight gain in mice fed with high fat cafeteria diet. Int. J. Endocrinol. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Perona, J.S.; Cañizares, J.; Montero, E.; Sánchez-Domínguez, J.M.; Catalá, A.; Ruiz-Gutiérrez, V. Virgin olive oil reduces blood pressure in hypertensive elderly subjects. Clin. Nutr. 2004, 23, 1113–1121. [Google Scholar] [CrossRef] [PubMed]
- Quintieri, A.M.; Filice, E.; Amelio, D.; Pasqua, T.; Lupi, F.R.; Scavello, F.; Cantafio, P.; Rocca, C.; Lauria, A.; Penna, C.; et al. The innovative “Bio-Oil Spread” prevents metabolic disorders and mediates preconditioning-like cardioprotection in rats. Nutr. Metab. Cardiovasc. Dis. 2016. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Y.-G.; Zhang, H.-G.; Zhang, G.-Y.; Fan, J.-S.; Li, X.-H.; Liu, Y.-H.; Li, S.-H.; Lian, X.-M.; Tang, Z. Panax notoginseng saponins attenuate atherosclerosis in rats by regulating the blood lipid profile and an anti-inflammatory action. Clin. Exp. Pharmacol. Physiol. 2008, 35, 1238–1244. [Google Scholar] [CrossRef] [PubMed]
- Bello, C.T.; Turner, L.W. Reserpine as an antihypertensive in the outpatient clinic: A double-blind clinical study. Am. J. Med. Sci. 1956, 232, 194–197. [Google Scholar] [CrossRef] [PubMed]
- Shamon, S.D.; Perez, M.I. Blood pressure lowering efficacy of reserpine for primary hypertension. Cochrane Database Syst. Rev. 2009, 4, CD007655. [Google Scholar] [PubMed]
- Yu, L.; Qin, Y.; Wang, Q.; Zhang, L.; Liu, Y.; Wang, T.; Huang, L.; Wu, L.; Xiong, H. The efficacy and safety of Chinese herbal medicine, Rhodiola formulation in treating ischemic heart disease: A systematic review and meta-analysis of randomized controlled trials. Complement. Ther. Med. 2014, 22, 814–825. [Google Scholar] [CrossRef] [PubMed]
- Wu, T.; Zhou, H.; Jin, Z.; Bi, S.; Yang, X.; Yi, D.; Liu, W. Cardioprotection of salidroside from ischemia/reperfusion injury by increasing N-acetylglucosamine linkage to cellular proteins. Eur. J. Pharmacol. 2009, 613, 93–99. [Google Scholar] [CrossRef] [PubMed]
- Sinkovic, A.; Suran, D.; Lokar, L.; Fliser, E.; Skerget, M.; Novak, Z.; Knez, Z. Rosemary extracts improve flow-mediated dilatation of the brachial artery and plasma PAI-1 activity in healthy young volunteers. Phytother. Res. 2011, 25, 402–407. [Google Scholar] [CrossRef] [PubMed]
- Posadas, S.J.; Caz, V.; Largo, C.; de la Gándara, B.; Matallanas, B.; Reglero, G.; de Miguel, E. Protective effect of supercritical fluid rosemary extract, Rosmarinus officinalis, on antioxidants of major organs of aged rats. Exp. Gerontol. 2009, 44, 383–389. [Google Scholar] [CrossRef] [PubMed]
- Vanscheidt, W.; Jost, V.; Wolna, P.; Lücker, P.W.; Müller, A.; Theurer, C.; Patz, B.; Grützner, K.I. Efficacy and safety of a butcher’s broom preparation (Ruscus aculeatus L. extract) compared to placebo in patients suffering from chronic venous insufficiency. Arzneimittelforschung 2002, 52, 243–250. [Google Scholar] [CrossRef] [PubMed]
- Ciocoiu, M.; Mirón, A.; Mares, L.; Tutunaru, D.; Pohaci, C.; Groza, M.; Badescu, M. The effects of Sambucus nigra polyphenols on oxidative stress and metabolic disorders in experimental diabetes mellitus. J. Physiol. Biochem. 2009, 65, 297–304. [Google Scholar] [CrossRef] [PubMed]
- Bhattacharya, S.; Christensen, K.B.; Olsen, L.C.B.; Christensen, L.P.; Grevsen, K.; Færgeman, N.J.; Kristiansen, K.; Young, J.F.; Oksbjerg, N. Bioactive components from flowers of Sambucus nigra L. increase glucose uptake in primary porcine myotube cultures and reduce fat accumulation in Caenorhabditis elegans. J. Agric. Food Chem. 2013, 61, 11033–11040. [Google Scholar] [CrossRef] [PubMed]
- Christensen, K.B.; Petersen, R.K.; Kristiansen, K.; Christensen, L.P. Identification of bioactive compounds from flowers of black elder (Sambucus nigra L.) that activate the human peroxisome proliferator-activated receptor (PPAR) gamma. Phytother. Res. 2010, 24, S129–S132. [Google Scholar] [CrossRef] [PubMed]
- Li, L.; Zhou, X.; Li, N.; Sun, M.; Lv, J.; Xu, Z. Herbal drugs against cardiovascular disease: Traditional medicine and modern development. Drug Discov. Today 2015, 20, 1074–1086. [Google Scholar] [CrossRef] [PubMed]
- Chun, J.N.; Cho, M.; So, I.; Jeon, J.-H. The protective effects of Schisandra chinensis fruit extract and its lignans against cardiovascular disease: A review of the molecular mechanisms. Fitoterapia 2014, 97, 224–233. [Google Scholar] [CrossRef] [PubMed]
- Liu, H.; Wu, C.; Wang, S.; Gao, S.; Liu, J.; Dong, Z.; Zhang, B.; Liu, M.; Sun, X.; Guo, P. Extracts and lignans of Schisandra chinensis fruit alter lipid and glucose metabolism in vivo and in vitro. J. Funct. Foods 2015, 19, 296–307. [Google Scholar] [CrossRef]
- Zhang, M.; Liu, M.; Xiong, M.; Gong, J.; Tan, X. Schisandra chinensis fruit extract attenuates albuminuria and protects podocyte integrity in a mouse model of streptozotocin-induced diabetic nephropathy. J. Ethnopharmacol. 2012, 141, 111–118. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wang, J.; Shao, J.-Q.; Du, H.; Wang, Y.-T.; Peng, L. Effect of Schisandra chinensis on interleukins, glucose metabolism, and pituitary-adrenal and gonadal axis in rats under strenuous swimming exercise. Chin. J. Integr. Med. 2015, 21, 43–48. [Google Scholar] [CrossRef] [PubMed]
- Huseini, H.F.; Larijani, B.; Heshmat, R.; Fakhrzadeh, H.; Radjabipour, B.; Toliat, T.; Raza, M. The efficacy of Silybum marianum (L.) Gaertn. (silymarin) in the treatment of type II diabetes: A randomized, double-blind, placebo-controlled, clinical trial. Phytother. Res. 2006, 20, 1036–1039. [Google Scholar] [CrossRef] [PubMed]
- Tamayo, C.; Diamond, S. Review of clinical trials evaluating safety and efficacy of milk thistle (Silybum marianum [L.] Gaertn.). Integr. Cancer Ther. 2007, 6, 146–157. [Google Scholar] [CrossRef] [PubMed]
- Derosa, G.; D’Angelo, A.; Maffioli, P. The role of a fixed Berberis aristata/Silybum marianum combination in the treatment of type 1 diabetes mellitus. Clin. Nutr. 2015. [Google Scholar] [CrossRef] [PubMed]
- Ebrahimpour Koujan, S.; Gargari, B.P.; Mobasseri, M.; Valizadeh, H.; Asghari-Jafarabadi, M. Effects of Silybum marianum (L.) Gaertn. (silymarin) extract supplementation on antioxidant status and hs-CRP in patients with type 2 diabetes mellitus: A randomized, triple-blind, placebo-controlled clinical trial. Phytomedicine 2015, 22, 290–296. [Google Scholar] [CrossRef] [PubMed]
- Di Pierro, F.; Bellone, I.; Rapacioli, G.; Putignano, P. Clinical role of a fixed combination of standardized Berberis aristata and Silybum marianum extracts in diabetic and hypercholesterolemic patients intolerant to statins. Diabetes Metab. Syndr. Obes. 2015, 8, 89–96. [Google Scholar] [CrossRef] [PubMed]
- Bhasker, S.; Madhav, H.; Chinnamma, M. Molecular evidence of insulinomimetic property exhibited by steviol and stevioside in diabetes induced L6 and 3T3L1 cells. Phytomedicine 2015, 22, 1037–1044. [Google Scholar] [CrossRef] [PubMed]
- Ritu, M.; Nandini, J. Nutritional composition of Stevia rebaudiana—A sweet herb and its hypoglycaemic and hypolipidaemic effect on patients with non insulin dependent diabetes mellitus. J. Sci. Food Agric. 2016. [Google Scholar] [CrossRef] [PubMed]
- Asemi, Z.; Khorrami-Rad, A.; Alizadeh, S.A.; Shakeri, H.; Esmaillzadeh, A. Effects of synbiotic food consumption on metabolic status of diabetic patients: A double-blind randomized cross-over controlled clinical trial. Clin. Nutr. 2014, 33, 198–203. [Google Scholar] [CrossRef] [PubMed]
- Saravanan, R.; Vengatash babu, K.; Ramachandran, V. Effect of rebaudioside A, a diterpenoid on glucose homeostasis in STZ-induced diabetic rats. J. Physiol. Biochem. 2012, 68, 421–431. [Google Scholar] [CrossRef] [PubMed]
- Fuller, S.; Stephens, J.M. Diosgenin, 4-hydroxyisoleucine, and fiber from fenugreek: Mechanisms of actions and potential effects on metabolic syndrome. Adv. Nutr. 2015, 6, 189–197. [Google Scholar] [CrossRef] [PubMed]
- Gaddam, A.; Galla, C.; Thummisetti, S.; Marikanty, R.K.; Palanisamy, U.D.; Rao, P.V. Role of fenugreek in the prevention of type 2 diabetes mellitus in prediabetes. J. Diabetes Metab. Disord. 2015, 14. [Google Scholar] [CrossRef] [PubMed]
- Basu, A.; Du, M.; Leyva, M.J.; Sanchez, K.; Betts, N.M.; Wu, M.; Aston, C.E.; Lyons, T.J. Blueberries decrease cardiovascular risk factors in obese men and women with metabolic syndrome. J. Nutr. 2010, 140, 1582–1587. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.H.; de Mejia, E.G. Phenolic compounds from fermented berry beverages modulated gene and protein expression to increase insulin secretion from pancreatic beta-cells in vitro. J. Agric. Food Chem. 2016, 64, 2569–2581. [Google Scholar] [CrossRef] [PubMed]
- Johnson, M.H.; de Mejia, E.G.; Fan, J.; Lila, M.A.; Yousef, G.G. Anthocyanins and proanthocyanidins from blueberry-blackberry fermented beverages inhibit markers of inflammation in macrophages and carbohydrate-utilizing enzymes in vitro. Mol. Nutr. Food Res. 2013, 57, 1182–1197. [Google Scholar] [CrossRef] [PubMed]
- Vendrame, S.; Daugherty, A.; Kristo, A.S.; Riso, P.; Klimis-Zacas, D. Wild blueberry (Vaccinium angustifolium) consumption improves inflammatory status in the obese Zucker rat model of the metabolic syndrome. J. Nutr. Biochem. 2013, 24, 1508–1512. [Google Scholar] [CrossRef] [PubMed]
- Elek, S.R.; McNair, J.D.; Griffith, G.C. Veratrum viride: Hypotensive and cardiac effects of intravenous use. Calif. Med. 1953, 79, 300–305. [Google Scholar] [PubMed]
- Nand, V.; Doggrell, S.A.; Barnett, C.W. Effects of veratridine on the action potentials and contractility of right and left ventricles from normo- and hypertensive rats. Clin. Exp. Pharmacol. Physiol. 1997, 24, 570–576. [Google Scholar] [CrossRef] [PubMed]
- Singh, B.N.; Saha, C.; Galun, D.; Upreti, D.K.; Bayry, J.; Kaveri, S.V. European Viscum album: A potent phytotherapeutic agent with multifarious phytochemicals, pharmacological properties and clinical evidence. RSC Adv. 2016, 6, 23837–23857. [Google Scholar] [CrossRef]
- Tang, T.Y.; Li, F.-Z.; Afseth, J. Review of the regulations for clinical research in herbal medicines in USA. Chin. J. Integr. Med. 2014, 20, 883–893. [Google Scholar] [CrossRef] [PubMed]
- Nelson, H.S. Oral/sublingual Phleum pretense grass tablet (Grazax/Grastek) to treat allergic rhinitis in the USA. Expert Rev. Clin. Immunol. 2014, 10, 1437–1451. [Google Scholar] [CrossRef] [PubMed]
- Mozaffarian, D. Dietary and policy priorities for cardiovascular disease, diabetes, and obesity: A comprehensive review. Circulation 2016, 133, 187–225. [Google Scholar] [CrossRef] [PubMed]
- Xiao, J.B.; Högger, P. Dietary polyphenols and type 2 diabetes: Current insights and future perspectives. Curr. Med. Chem. 2015, 22, 23–38. [Google Scholar] [CrossRef] [PubMed]
- Rohn, S.; van Griensven, L. Grain legumes and further gluten free legumes—Science, technology and impacts on human health. Food Res. Int. 2015, 76, 1–2. [Google Scholar] [CrossRef]
- Barringer, T.A. Mediterranean diets and cardiovascular disease. Curr. Atheroscler. Rep. 2001, 3, 437–445. [Google Scholar] [CrossRef] [PubMed]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; Covas, M.-I.; Corella, D.; Arós, F.; Gómez-Gracia, E.; Ruiz-Gutiérrez, V.; Fiol, M.; Lapetra, J.; et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N. Engl. J. Med. 2013, 368, 1279–1290. [Google Scholar] [CrossRef] [PubMed]
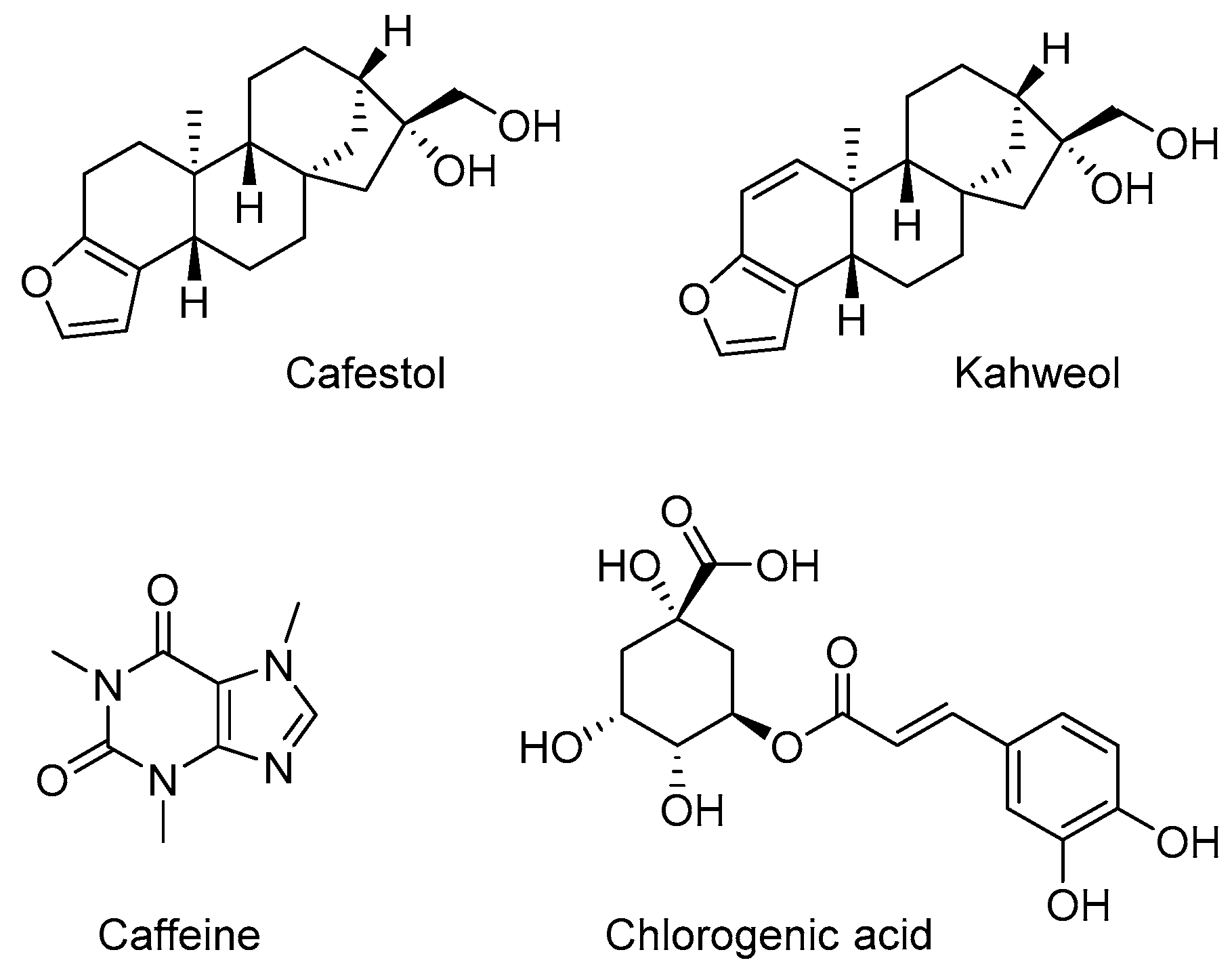
- Naismith, D.J.; Akinyanju, P.A.; Szanto, S.; Yudkin, J. The effect, in volunteers, of coffee and decaffeinated coffee on blood glucose, insulin, plasma lipids and some factors involved in blood clotting. Nutr. Metabol. 1970, 12, 144–151. [Google Scholar] [CrossRef]
- Barone, J.J.; Roberts, H.R. Caffeine consumption. Food Chem. Toxicol. 1996, 34, 119–129. [Google Scholar] [CrossRef]
- Santos, R.M.; Lima, D.R. Coffee consumption, obesity and type 2 diabetes: A mini-review. Eur. J. Nutr. 2016, 55, 1345–1358. [Google Scholar] [CrossRef] [PubMed]
- Morisco, F.; Lembo, V.; Mazzone, G.; Camera, S.; Caporaso, N. Coffee and liver health. J. Clin. Gastroenterol. 2014, 48 (Suppl. 1), S87–S90. [Google Scholar] [CrossRef] [PubMed]
- Akash, M.S.; Rehman, K.; Chen, S. Effects of coffee on type 2 diabetes mellitus. Nutrition 2014, 30, 755–763. [Google Scholar] [CrossRef] [PubMed]
- Zulli, A.; Smith, R.M.; Kubatka, P.; Novak, J.; Uehara, Y.; Loftus, H.; Qaradakhi, T.; Pohanka, M.; Kobyliak, N.; Zagatina, A.; et al. Caffeine and cardiovascular diseases: Critical review of current research. Eur. J. Nutr. 2016, 55, 1331–1343. [Google Scholar] [CrossRef] [PubMed]
- Ding, M.; Bhupathiraju, S.N.; Satija, A.; van Dam, R.M.; Hu, F.B. Long-term coffee consumption and risk of cardiovascular disease: A systematic review and a dose-response meta-analysis of prospective cohort studies. Circulation 2014, 129, 643–659. [Google Scholar] [CrossRef] [PubMed]
- Ding, M.; Satija, A.; Bhupathiraju, S.N.; Hu, Y.; Sun, Q.; Han, J.; Lopez-Garcia, E.; Willett, W.; van Dam, R.M.; Hu, F.B. Association of coffee consumption with total and cause-specific mortality in three large prospective cohorts. Circulation 2015, 132, 2305–2315. [Google Scholar] [CrossRef] [PubMed]
- Natella, F.; Scaccini, C. Role of coffee in modulation of diabetes risk. Nutr. Rev. 2012, 70, 207–217. [Google Scholar] [CrossRef] [PubMed]
- Vinson, J.A.; Proch, J.; Bose, P.; Muchler, S.; Taffera, P.; Shuta, D.; Samman, N.; Agbor, G.A. Chocolate is a powerful ex vivo and in vivo antioxidant, an antiatherosclerotic agent in an animal model, and a significant contributor to antioxidants in the European and American diets. J. Agric. Food Chem. 2006, 54, 8071–8076. [Google Scholar] [CrossRef] [PubMed]
- Bonita, J.S.; Mandarano, M.; Shuta, D.; Vinson, J. Coffee and cardiovascular disease: In vitro, cellular, animal, and human studies. Pharmacol. Res. 2007, 55, 187–198. [Google Scholar] [CrossRef] [PubMed]
- Van Dijk, A.E.; Olthof, M.R.; Meeuse, J.C.; Seebus, E.; Heine, R.J.; van Dam, R.M. Acute effects of decaffeinated coffee and the major coffee components chlorogenic acid and trigonelline on glucose tolerance. Diabetes Care 2009, 32, 1023–1025. [Google Scholar] [CrossRef] [PubMed]
- Meng, S.; Cao, J.; Feng, Q.; Peng, J.; Hu, Y. Roles of chlorogenic acid on regulating glucose and lipids metabolism: A review. Evid. Based Complement. Altern. Med. 2013, 2013. [Google Scholar] [CrossRef] [PubMed]
- Murase, T.; Misawa, K.; Minegishi, Y.; Aoki, M.; Ominami, H.; Suzuki, Y.; Shibuya, Y.; Hase, T. Coffee polyphenols suppress diet-induced body fat accumulation by downregulating SREBP-1c and related molecules in C57BL/6J mice. Am. J. Physiol. Endocrinol. Metab. 2011, 300, E122–E133. [Google Scholar] [CrossRef] [PubMed]
- Murase, T.; Yokoi, Y.; Misawa, K.; Ominami, H.; Suzuki, Y.; Shibuya, Y.; Hase, T. Coffee polyphenols modulate whole-body substrate oxidation and suppress postprandial hyperglycaemia, hyperinsulinaemia and hyperlipidaemia. Br. J. Nutr. 2012, 107, 1757–1765. [Google Scholar] [CrossRef] [PubMed]
- Gramza-Michalowska, A. Caffeine in tea Camellia sinensis—Content, absorption, benefits and risks of consumption. J. Nutr. Health Aging 2014, 18, 143–149. [Google Scholar] [CrossRef] [PubMed]
- Beecher, G.R.; Warden, B.A.; Merken, H. Analysis of tea polyphenols. Proc. Soc. Exp. Biol. Med. 1999, 220, 267–270. [Google Scholar] [CrossRef] [PubMed]
- Li, S.; Lo, C.Y.; Pan, M.H.; Lai, C.S.; Ho, C.T. Black tea: Chemical analysis and stability. Food Funct. 2013, 4, 10–18. [Google Scholar] [CrossRef] [PubMed]
- Gormaz, J.G.; Valls, N.; Sotomayor, C.; Turner, T.; Rodrigo, R. Potential role of polyphenols in the prevention of cardiovascular diseases: Molecular bases. Curr. Med. Chem. 2016, 23, 115–128. [Google Scholar] [CrossRef] [PubMed]
- Peters, U.; Poole, C.; Arab, L. Does tea affect cardiovascular disease? A meta-analysis. Am. J. Epidemiol. 2001, 154, 495–503. [Google Scholar] [CrossRef] [PubMed]
- Zhang, C.; Qin, Y.Y.; Wei, X.; Yu, F.F.; Zhou, Y.H.; He, J. Tea consumption and risk of cardiovascular outcomes and total mortality: A systematic review and meta-analysis of prospective observational studies. Eur. J. Epidemiol. 2015, 30, 103–113. [Google Scholar] [CrossRef] [PubMed]
- Basu, A.; Lucas, E.A. Mechanisms and effects of green tea on cardiovascular health. Nutr. Rev. 2007, 65, 361–375. [Google Scholar] [CrossRef] [PubMed]
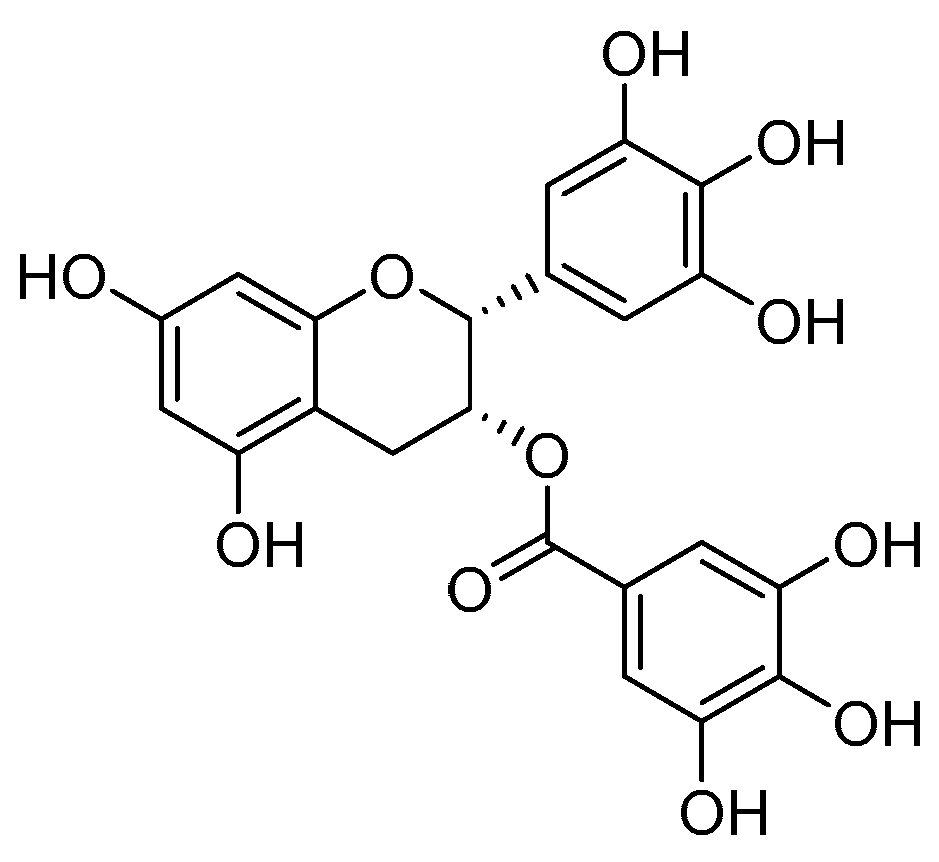
- Sano, M.; Tabata, M.; Suzuki, M.; Degawa, M.; Miyase, T.; Maeda-Yamamoto, M. Simultaneous determination of twelve tea catechins by high-performance liquid chromatography with electrochemical detection. Analyst 2001, 126, 816–820. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury, A.; Sarkar, J.; Chakraborti, T.; Pramanik, P.K.; Chakraborti, S. Protective role of epigallocatechin-3-gallate in health and disease: A perspective. Biomed. Pharmacother. 2016, 78, 50–59. [Google Scholar] [CrossRef] [PubMed]
- Chen, G.; Wang, H.; Zhang, X.; Yang, S.-T. Nutraceuticals and functional foods in the management of hyperlipidemia. Crit. Rev. Food Sci. Nutr. 2014, 54, 1180–1201. [Google Scholar] [CrossRef] [PubMed]
- Magrone, T.; Perez De Heredia, F.; Jirillo, E.; Morabito, G.; Marcos, A.; Serafini, M. Functional foods and nutraceuticals as therapeutic tools for the treatment of diet-related diseases. Can. J. Physiol. Pharmacol. 2013, 91, 387–396. [Google Scholar] [CrossRef] [PubMed]
- Liu, R.H. Dietary bioactive compounds and their health implications. J. Food Sci. 2013, 78, A18–A25. [Google Scholar] [CrossRef] [PubMed]
- Badimon, L.; Vilahur, G.; Padro, T. Nutraceuticals and atherosclerosis: Human trials. Cardiovasc. Ther. 2010, 28, 202–215. [Google Scholar] [CrossRef] [PubMed]
- Zuchi, C.; Ambrosio, G.; Lüscher, T.F.; Landmesser, U. Nutraceuticals in cardiovascular prevention: Lessons from studies on endothelial function. Cardiovasc. Ther. 2010, 28, 187–201. [Google Scholar] [CrossRef] [PubMed]
- Lacroix, I.M.; Li-Chan, E.C. Overview of food products and dietary constituents with antidiabetic properties and their putative mechanisms of action: A natural approach to complement pharmacotherapy in the management of diabetes. Mol. Nutr. Food Res. 2014, 58, 61–78. [Google Scholar] [CrossRef] [PubMed]
- Hung, H.Y.; Qian, K.; Morris-Natschke, S.L.; Hsu, C.S.; Lee, K.H. Recent discovery of plant-derived anti-diabetic natural products. Nat. Prod. Rep. 2012, 29, 580–606. [Google Scholar] [CrossRef] [PubMed]
- Gautam, R.; Jachak, S.M. Recent developments in anti-inflammatory natural products. Med. Res. Rev. 2009, 29, 767–820. [Google Scholar] [CrossRef] [PubMed]
- Hermansen, K.; Dinesen, B.; Hoie, L.H.; Morgenstern, E.; Gruenwald, J. Effects of soy and other natural products on LDL:HDL ratio and other lipid parameters: A literature review. Adv. Ther. 2003, 20, 50–78. [Google Scholar] [CrossRef] [PubMed]
- Vasanthi, H.R.; ShriShriMal, N.; Das, D.K. Phytochemicals from plants to combat cardiovascular disease. Curr. Med. Chem. 2012, 19, 2242–2251. [Google Scholar] [CrossRef] [PubMed]
- Hardie, D.G. AMPK: A target for drugs and natural products with effects on both diabetes and cancer. Diabetes 2013, 62, 2164–2172. [Google Scholar] [CrossRef] [PubMed]
- Yuan, T.; Nahar, P.; Sharma, M.; Liu, K.; Slitt, A.; Aisa, H.A.; Seeram, N.P. Indazole-type alkaloids from Nigella sativa seeds exhibit antihyperglycemic effects via AMPK activation in vitro. J. Nat. Prod. 2014, 77, 2316–2320. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, P.H.; Nguyen, T.N.; Dao, T.T.; Kang, H.W.; Ndinteh, D.T.; Mbafor, J.T.; Oh, W.K. AMP-activated protein kinase (AMPK) activation by benzofurans and coumestans isolated from Erythrina abyssinica. J. Nat. Prod. 2010, 73, 598–602. [Google Scholar] [CrossRef] [PubMed]
- Zimmermann, K.; Baldinger, J.; Mayerhofer, B.; Atanasov, A.G.; Dirsch, V.M.; Heiss, E.H. Activated AMPK boosts the Nrf2/HO-1 signaling axis—A role for the unfolded protein response. Free Radic. Biol. Med. 2015, 88, 417–426. [Google Scholar] [CrossRef] [PubMed]
- Chen, S. Natural products triggering biological targets—A review of the anti-inflammatory phytochemicals targeting the arachidonic acid pathway in allergy asthma and rheumatoid arthritis. Curr. Drug Targets 2011, 12, 288–301. [Google Scholar] [CrossRef] [PubMed]
- Jachak, S.M. Cyclooxygenase inhibitory natural products: Current status. Curr. Med. Chem. 2006, 13, 659–678. [Google Scholar] [CrossRef] [PubMed]
- Chi, Y.S.; Jong, H.G.; Son, K.H.; Chang, H.W.; Kang, S.S.; Kim, H.P. Effects of naturally occurring prenylated flavonoids on enzymes metabolizing arachidonic acid: Cyclooxygenases and lipoxygenases. Biochem. Pharmacol. 2001, 62, 1185–1191. [Google Scholar] [CrossRef]
- Gao, Y.; Zhang, Y.; Zhu, J.; Li, B.; Li, Z.; Zhu, W.; Shi, J.; Jia, Q.; Li, Y. Recent progress in natural products as DPP-4 inhibitors. Future Med. Chem. 2015, 7, 1079–1089. [Google Scholar] [CrossRef] [PubMed]
- Abe, M.; Akiyama, T.; Nakamura, H.; Kojima, F.; Harada, S.; Muraoka, Y. First synthesis and determination of the absolute configuration of sulphostin, a novel inhibitor of dipeptidyl peptidase IV. J. Nat. Prod. 2004, 67, 999–1004. [Google Scholar] [CrossRef] [PubMed]
- Saleem, S.; Jafri, L.; ul Haq, I.; Chang, L.C.; Calderwood, D.; Green, B.D.; Mirza, B. Plants Fagonia cretica L. and Hedera nepalensis K. Koch contain natural compounds with potent dipeptidyl peptidase-4 (DPP-4) inhibitory activity. J. Ethnopharmacol. 2014, 156, 26–32. [Google Scholar] [CrossRef] [PubMed]
- Schmitt, C.A.; Dirsch, V.M. Modulation of endothelial nitric oxide by plant-derived products. Nitric Oxide 2009, 21, 77–91. [Google Scholar] [CrossRef] [PubMed]
- Waldbauer, K.; Seiringer, G.; Nguyen, D.L.; Winkler, J.; Blaschke, M.; McKinnon, R.; Urban, E.; Ladurner, A.; Dirsch, V.M.; Zehl, M.; et al. Triterpenoic acids from apple pomace enhance the activity of the endothelial nitric oxide synthase (eNOS). J. Agric. Food Chem. 2016, 64, 185–194. [Google Scholar] [CrossRef] [PubMed]
- Xia, N.; Pautz, A.; Wollscheid, U.; Reifenberg, G.; Förstermann, U.; Li, H. Artichoke, cynarin and cyanidin downregulate the expression of inducible nitric oxide synthase in human coronary smooth muscle cells. Molecules 2014, 19, 3654–3668. [Google Scholar] [CrossRef] [PubMed]
- Shen, K.; Leung, S.W.; Ji, L.; Huang, Y.; Hou, M.; Xu, A.; Wang, Z.; Vanhoutte, P.M. Notoginsenoside Ft1 activates both glucocorticoid and estrogen receptors to induce endothelium-dependent, nitric oxide-mediated relaxations in rat mesenteric arteries. Biochem. Pharmacol. 2014, 88, 66–74. [Google Scholar] [CrossRef] [PubMed]
- Auger, C.; Chaabi, M.; Anselm, E.; Lobstein, A.; Schini-Kerth, V.B. The red wine extract-induced activation of endothelial nitric oxide synthase is mediated by a great variety of polyphenolic compounds. Mol. Nutr. Food Res. 2010, 54 (Suppl. 2), S171–S183. [Google Scholar] [CrossRef] [PubMed]
- Leung, K.W.; Cheng, Y.K.; Mak, N.K.; Chan, K.K.; Fan, T.P.; Wong, R.N. Signaling pathway of ginsenoside-Rg1 leading to nitric oxide production in endothelial cells. FEBS Lett. 2006, 580, 3211–3216. [Google Scholar] [CrossRef] [PubMed]
- Ndiaye, M.; Chataigneau, M.; Lobysheva, I.; Chataigneau, T.; Schini-Kerth, V.B. Red wine polyphenol-induced, endothelium-dependent NO-mediated relaxation is due to the redox-sensitive PI3-kinase/Akt-dependent phosphorylation of endothelial NO-synthase in the isolated porcine coronary artery. FASEB J. 2005, 19, 455–457. [Google Scholar] [CrossRef] [PubMed]
- Golan-Goldhirsh, A.; Gopas, J. Plant derived inhibitors of NF-κB. Phytochem. Rev. 2014, 13, 107–121. [Google Scholar] [CrossRef]
- Chan, M.M. Inhibition of tumor necrosis factor by curcumin, a phytochemical. Biochem. Pharmacol. 1995, 49, 1551–1556. [Google Scholar] [CrossRef]
- Siedle, B.; Garcia-Pineres, A.J.; Murillo, R.; Schulte-Mönting, J.; Castro, V.; Rüngeler, P.; Klaas, C.A.; da Costa, F.B.; Kisiel, W.; Merfort, I. Quantitative structure-activity relationship of sesquiterpene lactones as inhibitors of the transcription factor NF-κB. J. Med. Chem. 2004, 47, 6042–6054. [Google Scholar] [CrossRef] [PubMed]
- Fakhrudin, N.; Waltenberger, B.; Cabaravdic, M.; Atanasov, A.G.; Malainer, C.; Schachner, D.; Heiss, E.H.; Liu, R.; Noha, S.M.; Grzywacz, A.M.; et al. Identification of plumericin as a potent new inhibitor of the NF-κB pathway with anti-inflammatory activity in vitro and in vivo. Br. J. Pharmacol. 2014, 171, 1676–1686. [Google Scholar] [CrossRef] [PubMed]
- Kopp, E.; Ghosh, S. Inhibition of NF-κB by sodium salicylate and aspirin. Science 1994, 265, 956–959. [Google Scholar] [CrossRef] [PubMed]
- Kumar, H.; Kim, I.S.; More, S.V.; Kim, B.W.; Choi, D.K. Natural product-derived pharmacological modulators of Nrf2/ARE pathway for chronic diseases. Nat. Prod. Rep. 2014, 31, 109–139. [Google Scholar] [CrossRef] [PubMed]
- Balogun, E.; Hoque, M.; Gong, P.; Killeen, E.; Green, C.J.; Foresti, R.; Alam, J.; Motterlini, R. Curcumin activates the haem oxygenase-1 gene via regulation of Nrf2 and the antioxidant-responsive element. Biochem. J. 2003, 371, 887–895. [Google Scholar] [CrossRef] [PubMed]
- Heiss, E.H.; Tran, T.V.; Zimmermann, K.; Schwaiger, S.; Vouk, C.; Mayerhofer, B.; Malainer, C.; Atanasov, A.G.; Stuppner, H.; Dirsch, V.M. Identification of chromomoric acid C-I as an Nrf2 activator in Chromolaena odorata. J. Nat. Prod. 2014, 77, 503–508. [Google Scholar] [CrossRef] [PubMed]
- Ahn, Y.H.; Hwang, Y.; Liu, H.; Wang, X.J.; Zhang, Y.; Stephenson, K.K.; Boronina, T.N.; Cole, R.N.; Dinkova-Kostova, A.T.; Talalay, P.; et al. Electrophilic tuning of the chemoprotective natural product sulforaphane. Proc. Natl. Acad. Sci. USA 2010, 107, 9590–9595. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Waltenberger, B.; Pferschy-Wenzig, E.M.; Blunder, M.; Liu, X.; Malainer, C.; Blazevic, T.; Schwaiger, S.; Rollinger, J.M.; Heiss, E.H.; et al. Natural product agonists of peroxisome proliferator-activated receptor gamma (PPARgamma): A review. Biochem. Pharmacol. 2014, 92, 73–89. [Google Scholar] [CrossRef] [PubMed]
- Atanasov, A.G.; Blunder, M.; Fakhrudin, N.; Liu, X.; Noha, S.M.; Malainer, C.; Kramer, M.P.; Cocic, A.; Kunert, O.; Schinkovitz, A.; et al. Polyacetylenes from Notopterygium incisum—New selective partial agonists of peroxisome proliferator-activated receptor-gamma. PLoS ONE 2013, 8, e61755. [Google Scholar] [CrossRef] [PubMed]
- Atanasov, A.G.; Wang, J.N.; Gu, S.P.; Bu, J.; Kramer, M.P.; Baumgartner, L.; Fakhrudin, N.; Ladurner, A.; Malainer, C.; Vuorinen, A.; et al. Honokiol: A non-adipogenic PPARgamma agonist from nature. Biochim. Biophys. Acta 2013, 1830, 4813–4819. [Google Scholar] [CrossRef] [PubMed]
- Fakhrudin, N.; Ladurner, A.; Atanasov, A.G.; Heiss, E.H.; Baumgartner, L.; Markt, P.; Schuster, D.; Ellmerer, E.P.; Wolber, G.; Rollinger, J.M.; et al. Computer-aided discovery, validation, and mechanistic characterization of novel neolignan activators of peroxisome proliferator-activated receptor gamma. Mol. Pharmacol. 2010, 77, 559–566. [Google Scholar] [CrossRef] [PubMed]
- Puhl, A.C.; Bernardes, A.; Silveira, R.L.; Yuan, J.; Campos, J.L.; Saidemberg, D.M.; Palma, M.S.; Cvoro, A.; Ayers, S.D.; Webb, P.; et al. Mode of peroxisome proliferator-activated receptor gamma activation by luteolin. Mol. Pharmacol. 2012, 81, 788–799. [Google Scholar] [CrossRef] [PubMed]
- Weidner, C.; de Groot, J.C.; Prasad, A.; Freiwald, A.; Quedenau, C.; Kliem, M.; Witzke, A.; Kodelja, V.; Han, C.T.; Giegold, S.; et al. Amorfrutins are potent antidiabetic dietary natural products. Proc. Natl. Acad. Sci. USA 2012, 109, 7257–7262. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.-J.; Jiang, B.; Wu, N.; Wang, S.-Y.; Shi, D.-Y. Natural and semisynthetic protein tyrosine phosphatase 1B (PTP1B) inhibitors as anti-diabetic agents. RSC Adv. 2015, 5, 48822–48834. [Google Scholar] [CrossRef]
- Jiang, C.S.; Liang, L.F.; Guo, Y.W. Natural products possessing protein tyrosine phosphatase 1B (PTP1B) inhibitory activity found in the last decades. Acta Pharmacol. Sin. 2012, 33, 1217–1245. [Google Scholar] [CrossRef] [PubMed]
- Heiss, E.H.; Baumgartner, L.; Schwaiger, S.; Heredia, R.J.; Atanasov, A.G.; Rollinger, J.M.; Stuppner, H.; Dirsch, V.M. Ratanhiaphenol III from Ratanhiae radix is a PTP1B inhibitor. Planta Med. 2012, 78, 678–681. [Google Scholar] [CrossRef] [PubMed]
- Feng, Y.; Carroll, A.R.; Addepalli, R.; Fechner, G.A.; Avery, V.M.; Quinn, R.J. Vanillic acid derivatives from the green algae Cladophora socialis as potent protein tyrosine phosphatase 1B inhibitors. J. Nat. Prod. 2007, 70, 1790–1792. [Google Scholar] [CrossRef] [PubMed]
- Yoon, G.; Lee, W.; Kim, S.N.; Cheon, S.H. Inhibitory effect of chalcones and their derivatives from Glycyrrhiza inflata on protein tyrosine phosphatase 1B. Bioorg. Med. Chem. Lett. 2009, 19, 5155–5157. [Google Scholar] [CrossRef] [PubMed]
- Werz, O. Inhibition of 5-lipoxygenase product synthesis by natural compounds of plant origin. Planta Med. 2007, 73, 1331–1357. [Google Scholar] [CrossRef] [PubMed]
- Oettl, S.K.; Gerstmeier, J.; Khan, S.Y.; Wiechmann, K.; Bauer, J.; Atanasov, A.G.; Malainer, C.; Awad, E.M.; Uhrin, P.; Heiss, E.H.; et al. Imbricaric acid and perlatolic acid: Multi-targeting anti-inflammatory depsides from Cetrelia monachorum. PLoS ONE 2013, 8, e76929. [Google Scholar] [CrossRef] [PubMed]
- De la Puerta, R.; Ruiz Gutierrez, V.; Hoult, J.R. Inhibition of leukocyte 5-lipoxygenase by phenolics from virgin olive oil. Biochem. Pharmacol. 1999, 57, 445–449. [Google Scholar] [CrossRef]
- Winekenstädde, D.; Angelis, A.; Waltenberger, B.; Schwaiger, S.; Tchoumtchoua, J.; König, S.; Werz, O.; Aligiannis, N.; Skaltsounis, A.-L.; Stuppner, H. Phytochemical profile of the aerial parts of Sedum sediforme and anti-inflammatory activity of myricitrin. Nat. Prod. Commun. 2015, 10, 83–88. [Google Scholar] [PubMed]
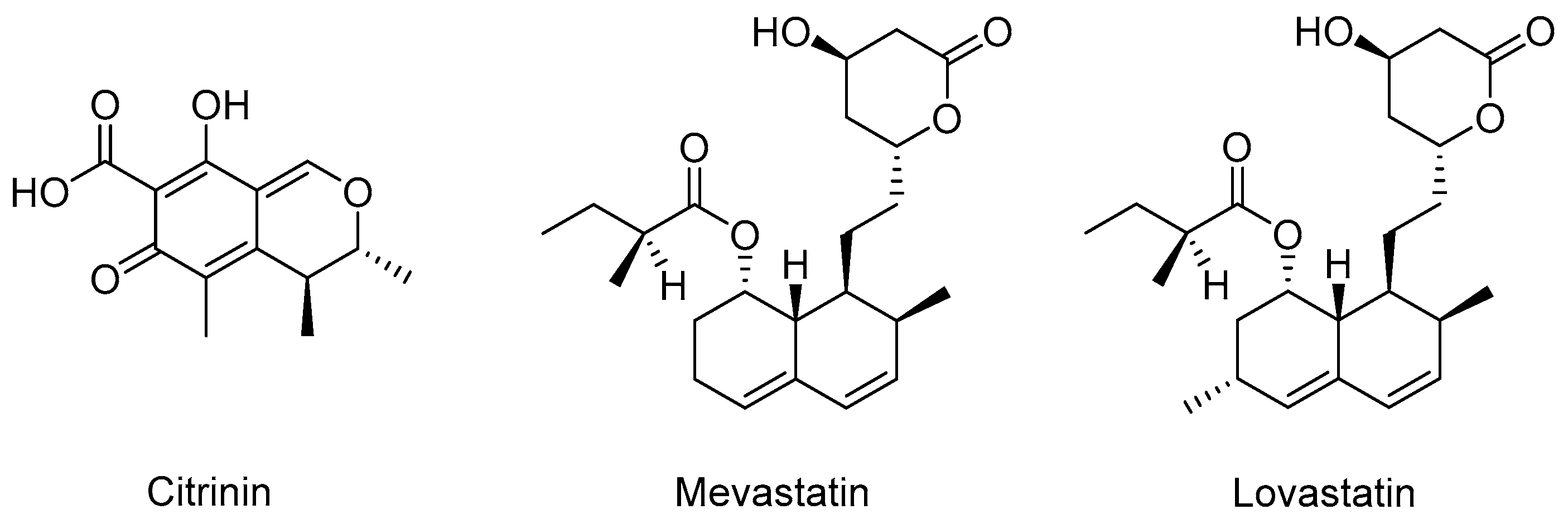
- Endo, A. A historical perspective on the discovery of statins. Proc. Jpn. Acad. Ser. B Phys. Biol. Sci. 2010, 86, 484–493. [Google Scholar] [CrossRef] [PubMed]
- Tanzawa, K.; Kuroda, M.; Endo, A. Time-dependent, irreversible inhibition of 3-hydroxy-3-methylglutaryl-coenzyme A reductase by the antibiotic citrinin. Biochim. Biophys. Acta 1977, 488, 97–101. [Google Scholar] [PubMed]
- Endo, A.; Kuroda, M. Citrinin, an inhibitor of cholesterol synthesis. J. Antibiot. Tokyo 1976, 29, 841–843. [Google Scholar] [CrossRef] [PubMed]
- Endo, A.; Kuroda, M.; Tsujita, Y. ML-236A, ML-236B, and ML-236C, new inhibitors of cholesterogenesis produced by Penicillium citrinium. J. Antibiot. Tokyo 1976, 29, 1346–1348. [Google Scholar] [CrossRef] [PubMed]
- Endo, A.; Kuroda, M.; Tanzawa, K. Competitive inhibition of 3-hydroxy-3-methylglutaryl coenzyme A reductase by ML-236A and ML-236B fungal metabolites, having hypocholesterolemic activity. FEBS Lett. 1976, 72, 323–326. [Google Scholar] [CrossRef]
- Endo, A.; Tsujita, Y.; Kuroda, M.; Tanzawa, K. Inhibition of cholesterol synthesis in vitro and in vivo by ML-236A and ML-236B, competitive inhibitors of 3-hydroxy-3-methylglutaryl-coenzyme A reductase. Eur. J. Biochem. 1977, 77, 31–36. [Google Scholar] [CrossRef] [PubMed]
- Alberts, A.W.; Chen, J.; Kuron, G.; Hunt, V.; Huff, J.; Hoffman, C.; Rothrock, J.; Lopez, M.; Joshua, H.; Harris, E.; et al. Mevinolin: A highly potent competitive inhibitor of hydroxymethylglutaryl-coenzyme A reductase and a cholesterol-lowering agent. Proc. Natl. Acad. Sci. USA 1980, 77, 3957–3961. [Google Scholar] [CrossRef] [PubMed]
- Endo, A. Monacolin K, a new hypocholesterolemic agent produced by a Monascus species. J. Antibiot. Tokyo 1979, 32, 852–854. [Google Scholar] [CrossRef] [PubMed]
- Endo, A. A gift from nature: The birth of the statins. Nat. Med. 2008, 14, 1050–1052. [Google Scholar] [CrossRef] [PubMed]
- Grundy, S.M. Dyslipidaemia in 2015: Advances in treatment of dyslipidaemia. Nat. Rev. Cardiol. 2016, 13, 74–75. [Google Scholar] [CrossRef] [PubMed]
- Bailey, C.; Day, C. Metformin: Its botanical background. Pract. Diab. Int. 2004, 21, 115–117. [Google Scholar] [CrossRef]
- Müller, H.; Reinwein, H. Pharmacology of galegin. Arch. Exp. Pathol. Pharmakol. 1927, 125, 212–228. [Google Scholar] [CrossRef]
- Tanret, G. An alkaloid extracted from Galega officinalis. Compt. Rend. 1914, 158, 1182–1184. [Google Scholar]
- Barger, G.; White, F.D. The constitution of galegine. Biochem. J. 1923, 17, 827–835. [Google Scholar] [CrossRef] [PubMed]
- Watanabe, C.K. Studies in the metabolic changes induced by administration of guanidine bases. I. The influence of injected guanidine hydrochloride upon blood sugar content. J. Biol. Chem. 1918, 33, 253–265. [Google Scholar]
- Bailey, C.; Campbell, I.; Chan, J.; Davidson, J.; Howlett, H.; Ritz, P. Metformin: The Gold Standard. A Scientific Handbook; Wiley: Chichester, UK, 2007. [Google Scholar]
- Cusi, K.; DeFronzo, R.A. Metformin: A review of its metabolic effects. Diabetes Rev. 1998, 6, 89–131. [Google Scholar]
| Scientific Name of the Medicinal Plant | Common Name of the Medicinal Plant | Plant Organ | Indications |
|---|---|---|---|
| Aesculus hippocastanum L. | Horse-chestnut | Seeds | Venous insufficiency, varicose veins [21,22,23,24] |
| Allium sativum L. | Garlic | Bulbs/whole plant | Hypertension, hypercholesterolemia, diabetes mellitus type 2 [25,26,27,28,29,30] |
| Aloe vera (L.) Burm. f. | Aloe vera | Leaves | Diabetes mellitus type 2, hypercholesterolemia [31,32,33,34,35] |
| Ammi visnaga (L.) Lam. | Toothpick weed, bisnaga, khella | Fruits | Angina pectoris [36,37,38] |
| Apocynum venetum L. | Dogbane | Leaves | Hypertension [39,40,41,42] |
| Artemisia dracunculus L. | Tarragon | Leaves, aerial parts | Hyperglycemia [17,43,44,45] |
| Artemisia herba-alba Asso | White wormwood | Aerial parts | Hyperlipidemia, diabetes mellitus [46,47,48,49,50] |
| Aspalathus linearis (Burm. f.) R. Dahlgr. | Rooibos | Leaves | Diabetes mellitus type 2 [51,52,53,54] |
| Astragalus membranaceus Moench | Chinese milk vetch | Roots | Angina pectoris, atherosclerosis, diabetic nephropathy [39,55,56,57,58,59] |
| Carthamus tinctorius L. | Safflower | Flowers | Angina pectoris, hypertension, hyperlipidemia [39,60,61,62,63,64] |
| Centaurium erythraea Rafn | Common centaury | Whole plant, leaves | Diabetes mellitus [46,48,65,66,67] |
| Cinnamomum cassia (L.) J. Presl | Chinese cinnamon | Bark | Diabetes mellitus, diabetic nephropathy [68,69,70] |
| Cinnamomum verum J. Presl | Ceylon cinnamon | Bark | Diabetes mellitus type 2 [69,71,72,73,74] |
| Commiphora mukul (Hook. ex Stocks) Engl. | Gugal, guggul, gugul, Indian bdellium-tree, mukul myrrh tree | Resin | Hypercholesterolemia, hypertriglyceridemia [21,75,76] |
| Coptis chinensis Franch. | Chinese goldthread | Roots, flowers | Hypercholesterolemia, diabetes mellitus, non-alcoholic fatty liver disease [18,77,78,79] |
| Coriandrum sativum L. | Coriander | Seeds | Diabetes mellitus, hypercholesterolemia [80,81,82,83] |
| Crataegus monogyna Jacq./C. oxyacantha Jacq./C. laevigata (Poir.) DC./C. pinnatifida Bunge | Hawthorn | Sprigs with both leaves and flowers, fruits | Angina pectoris, atherosclerosis, hyperlipidemia [84,85,86,87] |
| Cynara scolimus L. | Globe artichoke | Leaves | Hypercholesterolemia [88,89] |
| Fraxinus excelsior L. | European ash | Fruits, seeds | Diabetes mellitus type 2, hepatic steatosis [90,91,92,93,94,95] |
| Galega officinalis L. | French lilac | Aerial parts | Diabetes mellitus [72,96,97,98] |
| Gingko biloba L. | Gingko, maidenhair tree | Leaves | Cerebrovascular disease, peripheral vascular disease, hypertension, diabetes nephropathy [75,85,99,100] |
| Glycine max (L.) Merr. | Soybean | Fruits, seeds | Diabetes mellitus, hyperlipidemia [101,102,103] |
| Glycyrrhiza glabra L. | Licorice | Roots | Atherosclerosis, hypercholesterolemia [85,104] |
| Helianthus tuberosus L. | Jerusalem artichoke | Tubers | Diabetes mellitus type 2, non-alcoholic fatty liver disease [105] |
| Ilex paraguariensis A. St.-Hil. | Yerba mate | Leaves | Obesity, diabetes mellitus [106,107,108,109,110,111] |
| Lycium barbarum L. | Chinese wolfberry | Fruits, roots | Diabetes mellitus, hyperlipidemia, hypertension [112,113,114,115,116,117,118,119] |
| Momordica charantia L. | Bitter melon | Fruits | Diabetes mellitus type 2 [109,120,121] |
| Morus alba L. | White mulberry tree | Root bark, leaves | Hyperglycemia [122,123,124,125,126,127] |
| Nigella sativa L. | Black cumin, black seed | Seeds, seed oil | Diabetes mellitus type 2, dyslipidemia [128,129,130,131,132] |
| Ocimum sanctum L. | Holy basil | Leaves, whole plant | Hypertension, dyslipidemia, diabetes mellitus [133,134] |
| Olea europaea L. | Olive | Leaves, fruit oil | Hypertension, atherosclerosis, diabetes mellitus, hepatic steatosis [135,136,137,138,139,140,141,142] |
| Panax notoginseng (Burkill) F.H. Chen ex C.H. Chow | Notoginseng, pseudoginseng | Roots | Angina pectoris, coronary artery disease [21,75,143] |
| Rauvolfia serpentina (L.) Benth. ex Kurz | Indian snakeroot | Roots | Hypertension [75,144,145] |
| Rhodiola rosea L. | Golden root | Roots | Angina pectoris, ischemic heart disease [39,146,147] |
| Rosmarinus officinalis L. | Rosemary | Leaves | Capillary permeability and fragility disturbances [21,148,149] |
| Ruscus aculeatus L. | Butcher’s broom | Rhizomes | Venous insufficiency, varicose veins [21,150] |
| Sambucus nigra L. | European elder, black elder | Flowers | Diabetes mellitus type 2 [151,152,153] |
| Schisandra chinensis (Turcz.) Baill. | Five-flavor berry | Fruits, seeds | Hypertension, myocardial infarction, hyperlipidemia, diabetic nephropathy, diabetes mellitus [154,155,156,157,158] |
| Silybum marianum (L.) Gaertn. | Milk thistle | Seeds, aerial parts | Diabetes mellitus type 1 and 2 [90,159,160,161,162,163] |
| Stevia rebaudiana (Bertoni) Bertoni | Sweet leaf, candyleaf | Leaves | Diabetes mellitus type 2 [164,165,166,167] |
| Trigonella foenum-graecum L. | Fenugreek | Seeds | Metabolic syndrome, diabetes mellitus type 2 [168,169] |
| Vaccinium spp. | Blueberries | Fruits, leaves | Diabetes mellitus type 2, metabolic syndrome [96,109,170,171,172,173] |
| Veratrum album L./V. nigrum L./V. japonicum (Baker) Loes./V. viride Aiton | False helleborine/black false hellebore | Rhizomes | Hypertension [75,174,175] |
| Viscum album L. | Mistletoe | Aerial parts | Hypertension [176] |
| Name of the Product | National Clinical Trial (NCT) Identifier | Phase | Studied Condition |
|---|---|---|---|
| BeneFlax® (Flaxseed (Linum usitatissimum L.) lignans) | NCT02391779 | Phase 2 | Hypertension |
| Biscuit containing “Kothala Himbutu” (Salacia reticulata Wight) | NCT02290925 | Phase 3 | Diabetes mellitus type 2 |
| Coleus forskohlii (Willd.) Briq. | NCT02143349 | Phase 3 | Risk factors of metabolic syndrome |
| Combined Rg3-enriched Korean red ginseng and American ginseng | NCT01578837 | Phase 1 and 2 | Diabetes mellitus type 2, hypertension |
| Curcumin | NCT01968564 | - 2 | Vascular aging |
| Curcumin | NCT02529982 | Phase 2 | Non insulin dependent diabetes |
| Curcumin | NCT02529969 | Phase 2 | Non insulin dependent diabetes |
| Dantonic® (T89) | NCT01659580 | Phase 3 | Angina pectoris |
| Euiiyin-tang | NCT01724099 | Phase 2 and 3 | Obesity |
| Fibre grain herb | NCT02553382 | Phase 3 | Diabetes mellitus type 2 |
| “Fu-zheng-qu-zhuo” oral liquid | NCT02044835 | Phase 2 and 3 | Ischemic nephropathy |
| Ginger | NCT02289235 | Phase 0 | Non-alcoholic fatty liver disease |
| Phyllanthus niruri L. and Sida cordifolia L. (Vedicine) | NCT02107469 | - | Diabetic peripheral polyneuropathy |
| Quercetin | NCT00065676 | Phase 2 | Diabetes mellitus, obesity |
| Red grapes polyphenol supplementation | NCT02633150 | - | Obesity, insulin resistance |
| Resveratrol | NCT02245932 | Phase 3 | Overweight |
| Resveratrol | NCT01564381 | Phase 1 and 2 | Cardiovascular disease |
| Resveratrol | NCT01842399 | Phase 1 and 2 | Vascular resistance, hypertension |
| Resveratrol | NCT02246660 | - | Peripheral arterial disease |
| Resveratrol | NCT02137421 | - | Metabolic syndrome, coronary artery disease |
| Resveratrol | NCT02129595 | - | Pre-diabetes |
| Resveratrol | NCT01997762 | Phase 4 | Gestational diabetes |
| Resveratrol | NCT02216552 | Phase 2 and 3 | Non-alcoholic fatty liver disease, diabetes mellitus type 2, metabolic syndrome |
| Resveratrol | NCT02419092 | - | Obesity |
| Resveratrol | NCT01881347 | - | Diabetes mellitus |
| Resveratrol | NCT02549924 | Phase 2 | Diabetes mellitus type 2 |
| Resveratrol | NCT02244879 | Phase 3 | Diabetes mellitus type 2, inflammation, insulin resistance |
| Molecular Target/Pathway | Major Physiological Consequence | Selected Compound Classes of Interacting Natural Products |
|---|---|---|
| AMPK | Activation leads among others to inhibition of fat and cholesterol synthesis, promotion of fat oxidation, enhancement of mitochondrial biogenesis, and promotion of glucose uptake in skeletal muscle and fat cells | Alkaloids, chalcones, flavonoids and other polyphenols, galegine, salicylate, terpenoids [214,218,219,220,221] |
| COX-1/-2 | Inhibition leads to reduced biosynthesis of pro-inflammatory prostaglandins | Alkaloids, stilbenes, flavonoids and other polyphenols, terpenoids [222,223,224] |
| DPP-4 | Inhibition leads to decreased incretin degradation (and thus increased insulin secretion) | Alkaloids, flavonoids and other polyphenols, polypeptides, terpenoids [225,226,227] |
| eNOS | Activation leads to increased availability of anti-inflammatory nitric oxide (NO), a major antiatherogenic factor in the vasculature | Anthocyanidins, fatty acids, flavonoids and other polyphenols, ginsenosides, triterpenoic acids [228,229,230,231,232,233,234] |
| NF-κB pathway | Inhibition leads to impaired expression of pro-inflammatory mediators | Alkaloids, curcuminoids, chalcones, diterpenes, flavonoids, iridoids, naphtoquinones, salicylates, sesquiterpene lactones, stilbenes, triterpenes [235,236,237,238,239] |
| Nrf2 pathway | Activation leads to increased expression of cytoprotective (e.g., antioxidant) and reduced expression of lipo-and gluconeogenic genes | Carotenoids, chalcones, curcuminoids, diterpenes, flavonoids and other polyphenols, isothiocyanates, phytoprostanes, sesquiterpenes, sesquiterpene lactones, triterpenes [240,241,242,243] |
| PPARγ | Activation leads to insulin sensitization and normalization of blood glucose levels | Amorfrutins, diterpenequinones, flavonoids, neolignans, polyacetylenes, sesquiterpene lactones, stilbenes [244,245,246,247,248,249] |
| PTP1B | Inhibition leads to prolonged and enhanced insulin and leptin signaling (increased insulin sensitivity and reduced food intake) | Alkaloids, bromophenols, chalcones, coumarins, diterpenes, flavonoids, lignans, N- or S-containing compounds, sesquiterpenes, sesterterpenes, steroids, triterpenes [250,251,252,253,254] |
| 5-LO | Inhibition leads to reduced biosynthesis of pro-inflammatory leukotrienes | Alkaloids, coumarins, depsides, quinones, flavonoids and other polyphenols, polyacetylenes, sesquiterpenes, triterpenes [222,255,256,257,258] |
© 2016 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Waltenberger, B.; Mocan, A.; Šmejkal, K.; Heiss, E.H.; Atanasov, A.G. Natural Products to Counteract the Epidemic of Cardiovascular and Metabolic Disorders. Molecules 2016, 21, 807. https://doi.org/10.3390/molecules21060807
Waltenberger B, Mocan A, Šmejkal K, Heiss EH, Atanasov AG. Natural Products to Counteract the Epidemic of Cardiovascular and Metabolic Disorders. Molecules. 2016; 21(6):807. https://doi.org/10.3390/molecules21060807
Chicago/Turabian StyleWaltenberger, Birgit, Andrei Mocan, Karel Šmejkal, Elke H. Heiss, and Atanas G. Atanasov. 2016. "Natural Products to Counteract the Epidemic of Cardiovascular and Metabolic Disorders" Molecules 21, no. 6: 807. https://doi.org/10.3390/molecules21060807
APA StyleWaltenberger, B., Mocan, A., Šmejkal, K., Heiss, E. H., & Atanasov, A. G. (2016). Natural Products to Counteract the Epidemic of Cardiovascular and Metabolic Disorders. Molecules, 21(6), 807. https://doi.org/10.3390/molecules21060807










