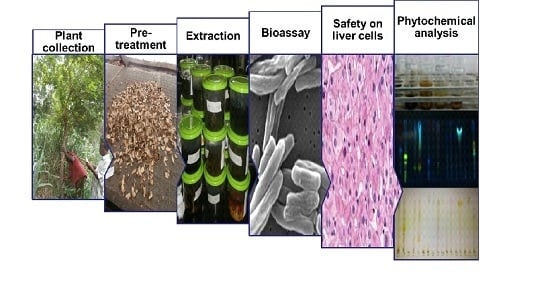
In Vitro Activity of Selected West African Medicinal Plants against Mycobacterium ulcerans Disease
Abstract
:1. Introduction
2. Results and Discussion
2.1. Selection of Plants and Extracts Preparation
2.2. Antimycobacterial Activity of Plants Extracts
2.3. Cell-Based Toxicity Results
2.4. Preliminary Phytochemical Analysis
3. Materials and Methods
3.1. Plant Collection
3.2. Preparation of Plant Extracts
3.3. In vitro Antimycobacterial Assays
3.3.1. Propagation of Mycobacterial Strains
3.3.2. Drug Susceptibility Assays: Determination of MIC
3.4. Cytotoxicity Assay
3.5. Phytochemical Analysis of Active Extracts
Supplementary Materials
Acknowledgments
Author Contributions
Conflicts of Interest
Abbreviations
| BU | Buruli ulcer |
| MIC | Minimum Inhibitory Concentration |
| CC50 | Sample’s concentrations required to inhibit 50% of cell proliferation |
| CPMR | Centre for Plant Medicine Research |
References
- De-an, G.; Wan-Ying, W.; Min, Y.; Xuan, L.; Geoffrey, A.C. A holistic approach to the quality control of traditional Chinese medicines. Science 2015, 347 (Suppl. 6219), S29–S31. [Google Scholar]
- Cunningham, A.B. African Medicinal Plants; United Nations Educational, Scientific and Cultural Organization: Paris, France, 1993. [Google Scholar]
- Tsouh, F.P.V.; Nyarko, A.K.; Appiah-Opong, R.; Tchokouaha Yamthe, L.R.; Addo, P.; Asante, I.K.; Boyom, F.F. Ethnopharmacological reports on anti-Buruli ulcer medicinal plants in three West African countries. J. Ethnopharmacol. 2015, 172, 297–311. [Google Scholar] [CrossRef] [PubMed]
- Van der Werf, T.S.; van der Graaf, W.T.; Tappero, J.W.; Asiedu, K. Mycobacterium ulcerans infection. Lancet 1999, 354, 1013–1038. [Google Scholar] [CrossRef]
- Martins, T.G.; Gama, J.B.; Fraga, A.G.; Saraiva, M.; Silva, M.T.; Castro, A.G.; Pedrosa, J. Local and regional re-establishment of cellular immunity during curative antibiotherapy of murine Mycobacterium ulcerans infection. PLoS ONE 2012, 7, e32740. [Google Scholar] [CrossRef] [PubMed]
- WHO. Buruli ulcer (Mycobacterium ulcerans Infection) Fact Sheet N 199, 2013. Available online: http://www.who.int/mediacentre/factsheets/fs199/en/ (accessed on 18 June 2013).
- Owusu-Sekyere, E. Managing the Buruli ulcer morbidity in the Amansie West District of Ghana: Can indigenous knowledge succeed? Int. J. Med. Med. Sci. 2012, 4, 180–185. [Google Scholar]
- Yemoa, A.; Gbenou, J.; Affolabi, D.; Moudachirou, M.; Bigot, A.; Anagonou, S.; Portaels, F.; Martin, A.; Quetin-Leclercq, J. Beninese Medicinal Plants as a Source of Antimycobacterial Agents: Bioguided Fractionation and In Vitro Activity of Alkaloids Isolated from Holarrhena floribunda Used in Traditional Treatment of Buruli Ulcer. BioMed. Res. Int. 2015. [Google Scholar] [CrossRef] [PubMed]
- Yemoa, A.; Gbenou, J.; Affolabi, D.; Moudachirou, M.; Bigot, A.; Anagonou, S.; Portaels, F.; Quetin-Leclercq, J.; Martin, A. Buruli Ulcer: A Review of In Vitro Tests to Screen Natural Products for Activity against Mycobacterium ulcerans. Planta Med. 2011, 77, 641–646. [Google Scholar] [CrossRef] [PubMed]
- Addo, P.; Quartey, M.; Abbas, M.; Adu-Addai, B.; Owusu, E.; Okang, I.; Dodoo, A.; de Souza, D.; Ankrah, N.; Ofori-Adjei, D. In -vitro susceptibility of Mycobacterium ulcerans to herbal preparations. Internet J. Trop. Med. 2007, 4, 1–11. [Google Scholar]
- Donfack, V.F.D.; Roque, S.; Trigo, G.; Fokou, P.V.T.; Tchokouaha, L.R.Y.; Tsabang, N.; Zollo, P.H.A.; Correia-Neves, M.; Boyom, F.F. Antimycobacterial activity of selected medicinal plants extracts from Cameroon. Int. J. Biol. Chem. Sci. 2014, 8, 273–288. [Google Scholar] [CrossRef]
- Magori, N.; Nyandoro, S.S.; Munissi, J.J.E.; Heydenreich, M. Antimycobacterial and cytotoxicity evaluation of the constituents of Monodora carolinae. Tanzan. J. Sci. 2013, 39, 13–18. [Google Scholar]
- ChEBI Azadiradione. Available online: http://www.ebi.ac.uk/chebi/searchId.do?printerFriendlyView=true&locale=null&chebiId=67280&viewTermLineage=&structureView=image& (accessed on 9 December 2015).
- Singh, B.; Jain, M.; Singh, S.V.; Dhama, K.; Aseri, G.K.; ain, N.J.; Datta, M.; Kumar, N.; Yadav, P.; Sujata, J.; et al. Plants as Future Source of Anti-Mycobacterial Molecules and Armour for Fighting Drug Resistance. Asian J. Anim. Vet. Adv. 2015, 10, 443–460. [Google Scholar]
- Mayekiso, K.; Eloff, J.N.; McGaw, L. Screening of South African Plants for Antibacterial and Antimycobacterial Activity. In Proceedings of the World Congress on Medicinal and Aromatic Plants, Cape Town, South Africa, 9–14 November 2008; Awunmi, C., Ed.; The African Journal for Traditional, Complementary and Alternative Medicine, and Alternative Medicine: Ile-Ife, Nigeria; p. 319.
- Zaman, K.; Pathak, K. Pharmacognostical and phytochemical studies on the leaf and stem bark of Annona reticulata linn. J. Pharmacogn. Phytochem. 2013, 1, 1–7. [Google Scholar]
- Le Thomas, A. Flore du Gabon, Muséum National d’histoire Naturelle; Laboratoire de Phanérogamie: Paris, France, 1969. [Google Scholar]
- Balde, M.A.; Traore, M.S.; Diane, S.; Diallo, M.S.T.; Tounkara, T.M.; Camara, A.; Baldé, E.S.; Bah, F.; Ouedraogo, U.; Drame, H.; et al. Ethnobotanical survey of medicinal plants traditionally used in Low and Middle-Guinea for the treatment of skin diseases. J. Plant Sci. 2015, 3, 32–39. [Google Scholar]
- Jiofack, T.R.B. Greenwayodendron suaveolens (Engl. & Diels) Verdc. In Prota 7(2): Timbers/Bois d’œuvre 2. [CD-Rom]; Lemmens, R.H.M.J., Louppe, D., Oteng-Amoako, A.A., Eds.; PROTA: Wageningen, The Netherlands, 2011. [Google Scholar]
- Hukkeri, V.; Karadi, R.; Akki, K.; Savadi, R.; Jaiprakash, B.; Kuppast, J.; Patil, M. Wound healing property of Eucalyptus globulus leaf extract. Indian Drugs 2002, 39, 481–483. [Google Scholar]
- Suffness, M.; Pezzuto, J.M. Assays related to cancer drug discovery. In Methods in Plant Biochemistry: Assays for Bioactivity; Hostettmann, K., Ed.; Academic Press: London, UK, 1990; Volume 6. [Google Scholar]
- Santhosh, R.S.; Suriyanarayanan, B. Plants: A source for new antimycobacterial drugs. Planta Med. 2014, 80, 9–21. [Google Scholar] [CrossRef] [PubMed]
- Niessen, W.M.A. Liquid Chromatography–Mass Spectrometry, 3rd ed.; Taylor and Francis Group, LLC: Boca Raton, FL, USA, 2006; p. 602. [Google Scholar]
- Harborne, J.B. Phytochemical Methods—A Guide to Modern Techniques of Plant Analysis; Chapman and Hall: London, UK; New York, NY, USA, 1973. [Google Scholar]
- Sofowora, E.A. Medicinal Plants and Traditional Medicine in Africa, 3rd ed.; Spectrum Books Ltd.: Ibadan, Nigeria, 1993. [Google Scholar]
- Sample Availability: Samples of the extracts are available from the authors.
| Plant Family | Plant Species | Country of Collection | Voucher Specimen Number | Plant Part Tested (x) and Extraction Yield (%) |
|---|---|---|---|---|
| Anacardiaceae | Mangifera indica L. | Ghana | CSRPM/010914 | R(he) (6.2); L(he) (10.9) |
| Sorindeia juglandifolia (A.Rich.) Planch. ex Oliv. | Cameroon | 9176 SRF/Cam | F(e) (13); T(e) (1.4); L(e) (5.4) | |
| Annonaceae | Annickia chlorantha (Oliv.) Setten & Maas | Cameroon | 32,065/SRF/Cam | SB(m) (1.2); SB(e) (2.9) |
| Annona muricata L. | Cameroon | 32,879/HNC | P(e) (5.7); S(m) (4.8); SB(e) (5.9); Sd (m) (3.5); R(m) (3.5); R(e) (6.2) | |
| Annona reticulata L. | Cameroon | 66,886/HNC | F(e) (5.1); T(e) (5); R(e) (5.1); L(e) (10.4); SB(d) (3.7); T(d); SB(e) (6.02); L(he) (1.04); F(d) (9.9); R(d) (4.5) | |
| Annona senegalensis Pers. | Cameroon | 40,060/HNC | S(e) (2.5); SB(d) (1.5); T(e) (1.8); S(d) (1.04); L(e) (11.6) | |
| Artabotrys rufus De Wild. | Cameroon | 48,757/HNC | L(e) (5.0); S(e) (4.02) | |
| Cleistopholis patens (Benth.) Engl. & Diels | Cameroon | 23,169/SRF/Cam | SB(d) (5.5); T(e) (7.5); L(d) (5.5); L(e) (10.5) | |
| Polyalthia suaveolens Engl. & Diels | Cameroon | 1227/SRF/CAM | SB(e) (4); T(e) (2.0); Tr(d) (0.4); S(e) (3.7); Tr(e) (1.54); S(d) (0.5); SB(d) (2.9); T(d) (0.73) | |
| Apocynaceae | Alstonia boonei De Wild. | Ghana | CSRPM/100714 | L(he) (7.78) |
| Holarrhena floribunda (G.Don) T. Durand & Schinz | Ghana | CSRPM/021214 | SB(he) (6.93); L(he) (7.8) | |
| Bignoniaceae | Spathodea campanulata P. Beauv. | Ghana | CSRPM/120714 | R(he) (6.63) |
| Caricaceae | Carica papaya L. | Ghana | CSRPM/070714 | L(he) (16.0); R(he) (5.06) |
| Cameroon | 18647/SFRCam | L(e) (15.1); SB(e) (5.54) | ||
| Compositae | Ageratum conyzoides (L.) L. | Ghana | CSRPM/090714 | L(he) (10.23) |
| Chromolaena odorata (L.) R.M.King & H.Rob. | Ghana | CSRPM/011214 | L(he) (8.96) | |
| Vernonia amygdalina Delile | Ghana | CSRPM/060714 | L(he) (7.7) | |
| Cameroon | 42362/HNC | L(e) (6.0) | ||
| Euphorbiaceae | Alchornea cordifolia (Schumach. & Thonn.) Müll.Arg. | Ghana | CSRPM/110714 | L(he) (10.2) |
| Jatropha curcas L. | Ghana | CSRPM/030714 | L(he) (13) | |
| Ricinus communis L. | Ghana | CSRPM/031214 | L(he) (7.4) | |
| Meliaceae | Azadirachta indica A.Juss. | Ghana | CSRPM/010714 | SB(he) (15) |
| Myrtaceae | Eucalyptus globulus Labill. | Cameroon | 4077/SRFC | L(e) (8.7) |
| Phyllanthaceae | Bridelia ferruginea Benth | Ghana | CSRPM/080714 | L(he) (7.4); SB(he) (7) |
| Phyllanthus fraternus G.L.Webster | Ghana | CSRPM/040714 | WP(he) (40) | |
| Rutaceae | Zanthoxylum zanthoxyloides (Lam.) Zepern. & Timler | Ghana | CSRPM/090714 | R(he) (10.4) |
| Solanaceae | Solanum erianthum D. Don | Ghana | CSRPM/020914 | L(he) (7.02); F(he) (9.5) |
| Solanum torvum Sw. | Ghana | CSRPM/050714 | L(he) (8.9) |
| Plant Species | Part | Extract Code | *MIC (µg/mL) on M. smegmatis | *MIC (µg/mL) on M. ulcerans | CC50 (µg/mL) Chang Liver Cell |
|---|---|---|---|---|---|
| Mangifera indica L. | Root | MIR (he) | >250 | >250 | ND |
| Leaf | MIL (he) | 250 | >250 | ND | |
| Sorindeia juglandifolia (A.Rich.) Planch. ex Oliv. | Twig | SJT (e) | >250 | >250 | ND |
| Leaf | SJL (e) | >250 | >250 | ND | |
| Fruit | SJF (e) | 63 | 250 | >250 | |
| Annona muricata L. | Pericarp | AMP (e) | >250 | >250 | ND |
| Stem | AMS (m) | 250 | >250 | ND | |
| Stem bark | AMSB (e) | >250 | >250 | ND | |
| Seed | AMSd (m) | >250 | >250 | ND | |
| Root | AMR (m) | 250 | >250 | ND | |
| Root | AMR (e) | 125 | >250 | ND | |
| Annona reticulata L. | Fruit | ARF (e) | 31 | >250 | >250 |
| Twig | ART (e) | >250 | >250 | ||
| Root | ARR (e) | 250 | 250 | >250 | |
| Leaf | ARL (e) | >250 | >250 | ND | |
| Stem bark | ARSB (d) | 63 | >250 | ND | |
| Twig | ART (d) | >250 | >250 | ND | |
| Stem bark | ARSB (e) | 125 | >250 | ND | |
| Leaf | ARL (he) | >250 | >250 | ND | |
| Fruit | ARF (d) | 31 | 250 | >250 | |
| Root | ARR (d) | 125 | 250 | >250 | |
| Annona senegalensis L. | Stem | ASS (e) | >250 | >250 | ND |
| Stem bark | ASSB (d) | >250 | >250 | ND | |
| Twig | AST (e) | >100 | >100 | ND | |
| Stem | ASS (d) | 31 | 250 | ND | |
| Leaf | ASL (e) | >250 | >250 | ND | |
| Artabotrys rufus De Wild. | Leaf | ArRL (d) | 125 | >125 | ND |
| Stem | ArRS (e) | 250 | >250 | ND | |
| Cleistopholis patens (Benth.) Engl. & Diels | Stem bark | CPSB (d) | 125 | 125 | 20.8 ± 2 |
| Twig | CPT (e) | 125 | >250 | ND | |
| Leaf | CPL (d) | ND | >250 | ND | |
| Leaf | CPL (e) | >250 | >250 | ND | |
| Annickia chlorantha (Oliv.) Setten & Maas syn | Stem bark | ACSB (m) | 125 | 250 | ND |
| Stem bark | ACSB (e) | ND | >250 | ND | |
| Polyalthia suaveolens Engl. & Diels | Stem bark | PSSB (e) | >250 | >250 | ND |
| Twig | PST (e) | 250 | >250 | ND | |
| Trunk | PSTr (d) | >250 | >250 | ND | |
| Stem | PSS (e) | >250 | >250 | ND | |
| Trunk | PSTr (e) | >250 | 250 | 223 ± 2 | |
| Stem | PSS (d) | 16 | 250 | >250 | |
| Stem bark | PSSB (d) | >250 | 250 | >250 | |
| Twig | PST (d) | >250 | >250 | ND | |
| Alstonia boonei De Wild. | Leaf | ABL (he) | >250 | 250 | >250 |
| Holarrhena floribunda (G.Don) T. Durand et Schinz | Stem bark | HFSB (he) | ND | >250 | ND |
| Leaf | HFL (he) | ND | >250 | ND | |
| Spathodea campanulata P. Beauv. | Root | SCR (he) | >250 | 250 | >250 |
| Carica papaya L. | Leaf | CPL (he) | >250 | >250 | ND |
| Root | CPR (he) | >250 | >250 | ND | |
| Leaf | CPL (e) | >250 | 250 | 3.8 ± 1 | |
| Stem bark | CPSB (e) | >250 | 250 | 54 ± 1 | |
| Ageratum conyzoides (L.) L. | Leaf | ACL (he) | >250 | >250 | ND |
| Chromolaena odorata (L.) R.M.King & H.Rob. | Leaf | COL (he) | ND | >250 | ND |
| Vernonia amygdalina Delile | Leaf | VAL (he) | >250 | >250 | ND |
| Leaf | VAL (e) | >250 | 250 | ND | |
| Alchornea cordifolia (Schumach. & Thonn.) Müll.Arg. | Leaf | ACL (he) | 250 | >250 | ND |
| Jatropha curcas L. | Leaf | JCL (he) | >250 | >250 | ND |
| Ricinus communis L. | Leaf | RCL (he) | 125 | >250 | ND |
| Azadirachta indica A.Juss. | Stem bark | AISB (he) | 250 | >250 | ND |
| Eucalyptus globulus Labill. | Leaf | EGL (e) | 125 | 250 | >250 |
| Bridelia ferruginea Benth | Leaf | BFL (he) | >250 | >250 | ND |
| Stem bark | BFSB (he) | >250 | 250 | ND | |
| Phyllanthus fraternus G.L.Webster | Whole plant | PFWP (he) | 250 | >250 | ND |
| Zanthoxylum zanthoxyloides (Lam.) Zepern. & Timler | Root | ZZR (he) | 63 | 250 | >250 |
| Solanum erianthum D. Don | Leaf | SEL (he) | ND | >250 | ND |
| Fruit | SEF (he) | ND | >250 | ND | |
| Solanum torvum Sw. | Leaf | STL (he) | >250 | >250 | ND |
| Streptomycin | / | ND | 1 | / | |
| Rifampicin | / | 8 | 0.12 | / | |
| Curcumin | / | / | / | 31 ± 2 |
| Plant Species | Part | Extract Code | Phenols | Tannins | Flavonoids | Saponines | Alkaloids | Anthraquinones | Anthocyanns | Glycosides | Triterpenes |
|---|---|---|---|---|---|---|---|---|---|---|---|
| Sorindeia juglandifolia (A.Rich.) Planch. ex Oliv. | Fruit | SJF (e) | + | + | + | + | - | + | - | + | + |
| Annona muricata L. | Stem | AMS (m) | |||||||||
| Root | AMR (m) | + | + | + | - | + | - | - | + | + | |
| Root | AMR (e) | + | + | + | + | + | - | - | + | + | |
| Annona reticulata L. | Fruit | ARF (e) | + | + | +- | - | + | + | - | + | + |
| Root | ARR (e) | + | + | + | - | + | + | - | + | + | |
| Stem bark | ARSB (d) | + | + | + | - | + | + | - | + | + | |
| Stem bark | ARSB (e) | + | + | + | + | + | + | - | + | + | |
| Fruit | ARF (d) | + | + | + | - | + | + | - | + | + | |
| Root | ARR (d) | + | - | + | - | + | + | - | + | + | |
| Annona senegalensis L. | Stem | ASS(d) | + | - | + | - | + | + | - | + | + |
| Artabotrys rufus De Wild. | Leaf | ArL (d) | + | - | + | + | + | - | - | + | + |
| Stem | ArS (e) | + | + | + | + | + | - | - | + | + | |
| Cleistopholis patens (Benth.) Engl. & Diels | Stem bark | CPSB (d) | + | - | + | + | + | - | + | + | + |
| Twig | CPT (e) | + | - | + | + | + | - | - | + | + | |
| Annickia chlorantha (Oliv.) Setten & Maas syn | Stem bark | ANSB (m) | + | - | - | + | + | - | - | + | + |
| Polyalthia suaveolens Engl. & Diels | Twig | PST (e) | + | + | - | + | - | ND | ND | - | - |
| Trunk | PSTr (e) | + | - | + | + | + | ND | ND | - | - | |
| Stem | PSS(d) | + | + | + | + | + | ND | ND | + | + | |
| Alstonia boonei De Wild. | Leaf | ABL (he) | + | + | + | + | + | - | - | - | - |
| Spathodea campanulata P. Beauv. | Root | SCR (he) | - | + | + | + | - | - | - | - | - |
| Carica papaya L. | Leaf | CPL (e) | - | + | - | + | + | ND | ND | + | + |
| Stem bark | CPSB (e) | + | + | - | + | + | - | ND | + | - | |
| Vernonia amygdalina Delile | Leaf | VAL (e) | + | + | + | + | + | ND | ND | + | + |
| Eucalyptus globulus Labill. | Leaf | EGL (e) | + | + | + | - | + | ND | ND | - | - |
| Bridelia ferruginea Benth | Stem bark | BFSB (he) | + | + | + | + | - | - | - | - | - |
| Zanthoxylum zanthoxyloides (Lam.) Zepern. & Timler | Root | ZZR (he) | + | + | + | + | + | - | - | - | - |
© 2016 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons by Attribution (CC-BY) license ( http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Tsouh Fokou, P.V.; Kissi-Twum, A.A.; Yeboah-Manu, D.; Appiah-Opong, R.; Addo, P.; Tchokouaha Yamthe, L.R.; Ngoutane Mfopa, A.; Fekam Boyom, F.; Nyarko, A.K. In Vitro Activity of Selected West African Medicinal Plants against Mycobacterium ulcerans Disease. Molecules 2016, 21, 445. https://doi.org/10.3390/molecules21040445
Tsouh Fokou PV, Kissi-Twum AA, Yeboah-Manu D, Appiah-Opong R, Addo P, Tchokouaha Yamthe LR, Ngoutane Mfopa A, Fekam Boyom F, Nyarko AK. In Vitro Activity of Selected West African Medicinal Plants against Mycobacterium ulcerans Disease. Molecules. 2016; 21(4):445. https://doi.org/10.3390/molecules21040445
Chicago/Turabian StyleTsouh Fokou, Patrick Valere, Abena Adomah Kissi-Twum, Dorothy Yeboah-Manu, Regina Appiah-Opong, Phyllis Addo, Lauve Rachel Tchokouaha Yamthe, Alvine Ngoutane Mfopa, Fabrice Fekam Boyom, and Alexander Kwadwo Nyarko. 2016. "In Vitro Activity of Selected West African Medicinal Plants against Mycobacterium ulcerans Disease" Molecules 21, no. 4: 445. https://doi.org/10.3390/molecules21040445
APA StyleTsouh Fokou, P. V., Kissi-Twum, A. A., Yeboah-Manu, D., Appiah-Opong, R., Addo, P., Tchokouaha Yamthe, L. R., Ngoutane Mfopa, A., Fekam Boyom, F., & Nyarko, A. K. (2016). In Vitro Activity of Selected West African Medicinal Plants against Mycobacterium ulcerans Disease. Molecules, 21(4), 445. https://doi.org/10.3390/molecules21040445