Abstract
Health monitoring and its related technologies is an attractive research area. The electrocardiogram (ECG) has always been a popular measurement scheme to assess and diagnose cardiovascular diseases (CVDs). The number of ECG monitoring systems in the literature is expanding exponentially. Hence, it is very hard for researchers and healthcare experts to choose, compare, and evaluate systems that serve their needs and fulfill the monitoring requirements. This accentuates the need for a verified reference guiding the design, classification, and analysis of ECG monitoring systems, serving both researchers and professionals in the field. In this paper, we propose a comprehensive, expert-verified taxonomy of ECG monitoring systems and conduct an extensive, systematic review of the literature. This provides evidence-based support for critically understanding ECG monitoring systems’ components, contexts, features, and challenges. Hence, a generic architectural model for ECG monitoring systems is proposed, an extensive analysis of ECG monitoring systems’ value chain is conducted, and a thorough review of the relevant literature, classified against the experts’ taxonomy, is presented, highlighting challenges and current trends. Finally, we identify key challenges and emphasize the importance of smart monitoring systems that leverage new technologies, including deep learning, artificial intelligence (AI), Big Data and Internet of Things (IoT), to provide efficient, cost-aware, and fully connected monitoring systems.
Keywords:
ECG; ECG monitoring system; smart monitoring; heart diseases; cardiovascular diseases; IoT; sensors 1. Introduction
The last decade has witnessed an increasing number of deaths caused by chronic and cardiovascular diseases (CVDs) in all countries across the world. CVDs are disorders affecting the blood vessels and the heart. CVDs involving the blood vessels are known as vascular diseases, such as coronary artery disease. Those involving the heart include heart failure, cardiomyopathy, rheumatic heart diseases, stroke, heart attack, and arrhythmias.
According to the World Health Organization (WHO), CVDs are the number one cause of death globally, with 17.9 million deaths every year [1]. It remains the number one cause of death of all Americans, claiming more than 840,000 lives in 2016 [2]. Furthermore, the European Health Network European Cardiovascular Disease Statistics 2017 edition revealed that CVDs cause 3.9 million deaths in Europe and over 1.8 million deaths in the European Union (EU) yearly. This accounts for 45% of all deaths in Europe and 37% of all deaths in the EU [3].
Continuous heart rate monitoring and immediate heartbeat detection are primary concerns in contemporary healthcare. Experimental evidence has shown that many of the CVDs could be better diagnosed, controlled, and prevented through continuous monitoring, as well as analysis of electrocardiogram (ECG) signals [4,5,6,7,8,9]. Hence, the monitoring of physiological signals, such as electrocardiogram (ECG) signals, offers a new holistic paradigm for the assessment of CVDs, supporting disease control and prevention. With advances in sensor technology, communication infrastructure, data processing, and modeling as well as analytics algorithms the risk of impairments could be better addressed more than ever done before. This, in turn, would introduce a new era of smart, proactive healthcare especially with the great challenge of limited medical resources.
As a result, ECG monitoring systems have been developed and widely used in the healthcare sector for the past few decades and have significantly evolved over time due to the emergence of smart enabling technologies [10,11,12,13]. Nowadays, ECG monitoring systems are used in hospitals [14,15,16,17], homes [18,19,20], outpatient ambulatory settings [21,22,23], and in remote contexts [24]. They also employ a wide range of technologies such as IoT [25,26,27], edge computing [28,29], and mobile computing [30,31,32]. In addition, they implement various computational settings in terms of processing frequencies, as well as monitoring schemes. They have also evolved to serve purposes and targets other than disease diagnosis and control, including daily activities [33,34,35], sports [36,37,38], and even mode-related purposes [39,40,41].
This massive diversity in ECG monitoring systems’ contexts, technologies, computational schemes, and purposes makes it hard for researchers and professionals to design, classify, and analyze ECG monitoring systems. Some efforts attempted to provide a common understanding of ECG monitoring systems’ processes [42,43,44,45,46,47], guiding the design of efficient monitoring systems. However, these studies lack comprehensiveness and completeness. They work for specific contexts, serve specific targets, or are suitable for specific technologies. This makes the available ECG monitoring system processes and architectures hard to generalize and reuse. On the other hand, some studies attempted to analyze ECG monitoring systems’ attributes and provide classification taxonomies, supporting better analysis and understanding of the ECG systems reported in the literature. However, exiting reviews related to ECG monitoring in the literature can be intuitive and incomprehensive [48]. They do not consider the latest technological trends [49,50,51], and they target very narrow research niches, such as wearable sensors [52,53,54,55], mobile sensors [56], disease diagnosis [57], heartbeat detection [58], emotion recognition [59], or ECG compression methods [60]. Hence, there is a need to provide a comprehensive, expert-verified taxonomy of ECG monitoring systems, a common architecture, and a complete set of processes to guide the classification, analysis, and design of these systems.
Therefore, in this work, we propose an expert-verified taxonomy of ECG monitoring systems, a generic architectural model, and a complete, general set of processes to support better understanding, analysis, design, and validation of ECG monitoring systems from a broader perspective. Our experts’ taxonomy is composed of five distinct, cohesive clusters. Each cluster focuses on one dimension of ECG monitoring systems, detailing the features and attributes of these systems in that dimension. These include monitoring contexts, technologies, schemes, targets, and futuristic monitoring systems. In addition to our experts’ taxonomy, the proposed ECG monitoring systems’ layered architecture depicts essential structural components and elements of ECG monitoring systems, their interfaces, and the data inputs/outputs of each layer. We also complement our experts’ taxonomy and the generic architecture with a comprehensive ECG monitoring process model, highlighting the major processes, sub-processes, and supporting processes, emphasizing factors adding value to each process. Based on the proposed taxonomy, architecture, and common process model, we conduct an extensive, thorough analysis of the literature surrounding ECG monitoring systems, highlighting systems’ categories, attributes, functions, challenges, and current trends, leading to a panorama of ECG monitoring systems. To our best knowledge, this is the most comprehensive, expert-verified review of ECG monitoring systems to date.
This paper is organized as follows: Section 2 introduces the ECG monitoring architecture, describes the monitoring value chain and the main processes involved. Section 3 describes the experts’ taxonomy of ECG monitoring systems. It details, compares, and analyzes each cluster of studies, as well as highlights the key features and reviews some research challenges. Section 4 emphasizes the key challenges related to ECG monitoring systems. Finally, the last section summarizes and discusses our findings and points to future research directions for ECG monitoring systems.
2. Overview of ECG Monitoring Systems: Architecture, Processes, and Technologies
2.1. ECG Monitoring Architecture
Figure 1 describes a generic ECG layered monitoring architecture that we have developed to capture the key elements and structural components of ECG monitoring systems. These include the main processes involved, the underlying platforms, and the main actors and their involvement in the ECG-based monitoring processes. The architecture is organized into four horizontal connected layers and one vertical silo on the right in addition to important properties that have to be supported across all layers including security fulfillment, Quality of Service (QoS) enforcement, and smartness integration. This architecture delivers the service through different monitoring contexts, as depicted on the left side of the figure. In fact, the monitoring context represents the environment where the ECG monitoring system is deployed and the monitoring activities take place. Our proposed architecture is designed to fit into contexts of use in which various actors interact with the ECG monitoring system by providing inputs and receiving some sort of output. Hence, we dissociated the contexts of use and possible interactions of various actors within these contexts from the monitoring system.
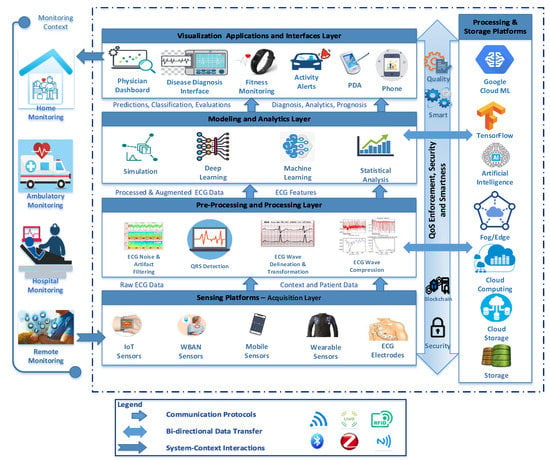
Figure 1.
The overall architecture of electrocardiogram (ECG) monitoring systems.
The monitoring context can vary from home monitoring, to ambulatory monitoring, to hospital monitoring, to remote monitoring. The data comes from the context into input layer, moves through the system, then goes back to the context through the visualization layer. This gives a complete realization of the system within its contexts. The architecture encompasses four layers: the bottom layer is the acquisition layer, which offers various sensing platforms and devices, such as ECG sensors, IoT sensors, Wireless Body Area Network (WBAN) sensors, mobile sensors, and wearable sensors. Sensors vary from embedded sensors mounted on biological tissues to comfortable, easy-to-handle smart watches and smart vests. Cardiac data in the form of ECG signals along with context and patient data are acquired using several communication protocols autonomously using Wifi, Bluetooth, ultra-wide band (UWB), ZigBee, radio-frequency identification (RFID), and near-field communication (NFC) and then transported to the next layer, which is the preprocessing and processing layer. The latter is responsible for handling operations such as ECG noise and artifact filtering, QRS detection, ECG wave delineation, transformation, and compression. Processed and augmented ECG data and features are then relayed using the aforementioned communication protocols to the modeling and analytics layer, where different machine learning, deep learning, and statistical analyses are conducted to analyze, extract patterns from ECG data, and identify and predict various heart diseases, such as arrhythmia, atrial fibrillation, epilepsy, mental fatigue, and fainting. The outputs generated from this layer are then delivered to the visualization layer where different applications and device interfaces (e.g., physician dashboard, disease diagnosis interface, and patient mobile device) are used to visualize analyzed data which can be effectively used in disease diagnosis, physician feedback, activity monitoring and alerts to drivers, fitness and general monitoring.
The right silo provides processing and storage services to all processes in the four horizontal layers of the architecture. For example, processed real-time ECG signals might utilize Fog/Edge computing. Also, Cloud infrastructure offers storage and processing services at various stages of the ECG monitoring lifecycle. The TensorFlow platform provides an execution environment, offering a multitude of deep learning libraries, packages, and visualization tools to test various deep learning models.
At the core of this ECG monitoring architecture, security and data privacy are important characteristics that should be supported in all processes where data are collected, transferred, processed, analyzed, accessed, and visualized by various stakeholders. Blockchain technology can be integrated to provide a trusted, decentralized, and immutable ledger for various transactions which outperforms existing methods, techniques, and mechanisms. It provides a high level of transparency to ensure security and privacy. It can, for example, integrate IoT devices and regulate the IoT device’s behavior automatically. All activities in the IoT and related transactions are recorded into blockchain through smart contracts for secure data logging and auditing at a low cost. QoS is also a very important system’s characteristic that needs to be supported at every single process, including, for instance, ensuring the quality of the data, the quality of the preprocessing and processing, the quality of analytics results, and the quality of visualization. Quality measurement and enforcement are supported through continuous monitoring and control of various proprieties of the monitoring system. Monitoring logs are continuously analyzed and improvement measures are taken to react to any quality degradation. Finally, smartness is another property of the ECG monitoring systems where various intelligent features could be implemented across all layers from data inception to visualization. Such intelligent features encompass instrumenting sensors to preprocess the data at the sensor or at the edge, energy-harvesting of sensors and mobile devices, self-adaptation, and self-learning algorithms that react to dynamic environment changes to make some intelligent decisions.
2.2. ECG Monitoring Value Chain: Comparative Study
ECG monitoring value chain encompasses a set of common processes, including data acquisition, preprocessing, feature extraction, processing, analysis, and visualization. Studying and analyzing the value chain of ECG monitoring systems helped in understanding the value and contribution of each process within the system, the best practices that can be adopted within each process, and the ultimate goal of the overall system in guaranteeing higher quality disease diagnosis and increased resource utilization efficiency in terms of energy and cost. Most of the existing researches agreed on the main ECG monitoring processes mentioned above. However, depending on the nature of the monitoring application, some research work has defined additional distinct or overlapping processes, such as data cleansing, encryption, and compression, but could be incorporated or merged as part of existing primary processes, or isolated as supporting processes.
We intend to identify research gaps in defining the complete lifecycle of ECG monitoring systems and highlight the existing models, which include processes that overlap, or processes that are merged. Our main objective is to highlight the added value these processes provide to the monitoring system’s lifecycle, as well as possibilities for optimization and improvement. One of the most important processes is data acquisition;it involves measuring and recording the heart’s activity using different sensors. The massive data generated by the ECG acquisition process requires preprocessing to prepare the data for the next stages, which are feature extraction and processing. The accuracy of preprocessing indirectly affects the subsequent stage of the value chain. Such preprocessing activities include cleansing the ECG data without losing its main components and features. This is why most of the research work devotes huge efforts to the preprocessing stage. Having huge volumes of ECG signals necessitates the feature extraction process to reduce the amount of processing and save resources prior to the processing and analysis stage. Features extraction is a very critical stage, as it has a significant effect on the subsequent stages of the lifecycle. The processing and analysis stage requires the application of various optimization techniques to achieve higher accuracy, precision and quality results. This is the most important stage in the monitoring system’s lifecycle as it affects the accuracy of signal interpretation and diagnostics. Finally, the different visualization tools enable end-users to clearly and efficiently visualize the results of the monitoring systems. This stage is also significant as it allows accessibility, usability, and understandability of complex data.
A review of the literature on ECG monitoring systems has differentially defined the processes/stages of the ECG monitoring system’s lifecycle, as depicted in Table 1. In this table, the value chain throughout various lifecycle representations of existing ECG monitoring systems is given emphasis. None of the proposed initiatives provides a full description of the complete lifecycle of an ECG monitoring system, including both the primary and the supporting processes. Most of these initiatives barely cover 70% of the primary processes throughout the lifecycle. Supporting processes were described in nearly half of the proposed work included in Table 1, such as data storage and data modeling.

Table 1.
Summary of the most common literature referring to ECG monitoring systems’ lifecycles, primary and supporting processes.
The most inclusive ECG monitoring system’s lifecycles that included the primary processes definition were depicted in [55,58,72,75,78,83]. Few of the researches specified additional supporting processes, such as data storage or encryption. Typically, IoT-based monitoring systems adopt most of the primary processes [12,13,71,72]. Other studies emphasized only a partial lifecycle that has to do with data acquisition, preprocessing, and processing for heartbeat detection or finding an annotation set depending on the purpose of the system [43,44,45,49,63,65]. However, few initiatives focused only on one process, such as processing in [64].
Supporting processes, such as training and modeling, were highlighted to support machine learning and neural network techniques [68,73]. Data cleansing was also defined as a discrete process in [71]. Additional important supporting processes were introduced in [72] to enforce privacy and security; these are responsible for encryption and decryption.
2.3. The ECG Monitoring Key Processes
There is no clear and comprehensive definition of the ECG monitoring system’s lifecycle processes in the literature. Most researchers focus on a subset of key processes; however, they neglect other very important supporting processes. Therefore, we will provide an across-the-board description and classification of primary and supporting processes that should be implemented within an ECG monitoring system, as depicted in Figure 2.
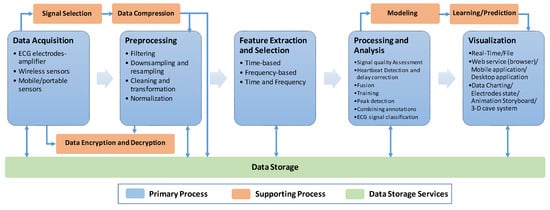
Figure 2.
ECG Monitoring Lifecycle.
The following subsections describe the details of each primary process within the generalized lifecycle of an ECG monitoring system. We intend to eliminate the overlapping and process definition ambiguities and highlight the adaptability of the processes to the unique needs of each system.
2.3.1. ECG Data Extraction and Collection
An ECG is considered the best method for detecting heart abnormalities. The available ECGs vary from single to 12-lead ECG recording devices. On one hand, hospital ECG acquisition devices are usually big in size and support high-precision and long-term monitoring. However, they restrain the patients’ movements and involvement. On the other hand, wearable health-monitoring systems afford real-time continuous monitoring of patients’ through the deployment of multiple sensors.
The process of data acquisition, the first stage/process in the lifecycle of ECG monitoring systems, encompasses the selection of the following: (1) the types of sensors (e.g., wireless, or wired), (2) the placement location of sensors, (3) the number of sensors, and (4) the hardware required for data acquisition, storage, and transmission [51]. Nevertheless, in some ECG monitoring systems, real-time and continuous ECG sensor acquisition is handled. ECG signal acquisition is a challenging task because of its sensitivity towards various quality dimensions including precision, accuracy, and timeliness. Inaccurate data collection may lead to a wrong diagnosis and accordingly affect clinical decisions.
However, most researchers working with ECG monitoring systems favor datasets from well-known databases, rather than creating a data acquisition system of their own, especially when they address diagnosis issues and feature extraction techniques, which constitute the remaining parts of the monitoring lifecycle. A thorough review of existing databases that provide single-lead and multi-lead ECG signals was depicted in [58].
2.3.2. Preprocessing
Preprocessing is intended to enhance the accuracy of prediction; it improves the quality of the raw signal, removes the noise, and removes the baseline wander and powerline interference. The noise is classified, in the literature, into five main groups: powerline interference, baseline wander, electrode contact noise, electrode motion artifacts, and muscle contractions. The most common preprocessing and noise removal techniques are classified into three main categories: Wavelet Transform-based, curvelet transform-based, and adaptive digital filters [86].
The preprocessing of ECG signals related to the cardiac cycle, such as duration of the QRS complex and the ST–T segment level, is better handled using linear filters to prevent phase distortion from fluctuating wave properties [84]. However, reducing the effect of noise caused by muscle activity requires averaging techniques to the time-aligned heartbeats. Existing standard filtering techniques lack efficiency in handling the signals. Therefore, hybrid filtering is rather more adaptive to raw ECG signals and, thus, was introduced in some research work to improve filtering results [89,90].
Despite being challenging for preserving important signal information, and adapting to the patient’s features, preprocessing has attracted the attention of researchers. Cleaning and transformation are also performed during the preprocessing stage [91]. Other techniques are also used during the preprocessing stage, such as downsampling, resampling and signal normalization [58].
2.3.3. Feature Extraction
One of the most important processes in the ECG monitoring lifecycle is the feature extraction process. It contributes significantly to cardiac disease diagnoses, as it retrieves the most representative set of features from the preprocessed ECG, which allows better heartbeat detection. The features comprise a collection of summarized signal information used to characterize patterns. These features are extracted using different computation algorithms and techniques to help researchers, along with the support of visual skills expertise in problem diagnostics.
The features of ECG signals include, but are not limited to, the area under the curve, peak amplitude, time delay between peaks and valleys, and heart rate frequency. The main feature extraction methods are Wavelet Transform-based feature extraction, the autocorrelation function-based feature extraction method (periodic information of ECG signals), principal component analysis-based feature extraction method (finding periodic information in time series signals), and normal feature extraction method (Fast Fourier Transform (FFT)) [92]. Tejedor et al. [58] classified feature extraction techniques into three approaches based on the type of features extracted, these are: (1) time-based, such as the maximum amplitude pair function and the symbolic discretization method from a time series, (2) frequency-based, such as Fast Fourier Transform, power spectral density, and Gaussian and moving average low-pass filters, and (3) a mix of both time and frequency, such as Wavelet Transform, frequency QRS power, and maximum and minimum amplitudes used for the detection of heartbeats.
Finding the optimal set of features that capture the true nature of the ECG signals remains a challenging task. Researches tried to apply multiple techniques to address the aforementioned issue, such as adopting Discrete Wavelet Transform and the Pan Tompkins Method to improve heartbeat abnormality classification from ECG signals in [93], or using time domain, frequency domain and distribution features for detection of atrial fibrillation (AF) in [46]. Keeping the good reliability of data and the quality of the signal are also challenges facing smartphone-integrated ECG monitoring systems; such a case was handled in [94] by enhancing the feature extraction process. The Wavelet Transform was also used in [7,60,67,95,96]. Alternatively, Wavelet Transform, combined with other techniques, was also applied in [7,66,97].
2.3.4. Processing and Analysis
Intensive research was devoted to improve the efficiency of processing and analysis of ECG signals to achieve high diagnostic accuracy. During the processing phase, advanced information technologies are carried out through the development of diverse algorithms and intelligent techniques, such as analysis, modification, and synthesis applied to ECG signals to recognize and identify its significant components, with the purpose of discovering diagnostic information. These include, but are not limited to signal quality assessment, ECG signal classification, heartbeat detection and delay correction, peak detection, and training. Processing ECG signals is challenging due to their special characteristics, such as dynamicity, noise vulnerability, and inconsistency among individuals. Therefore, the optimization and development of ECG signal processing techniques has attracted research interest.
AI methods and neural networks are typically very useful in providing ECG signal interpretation. In the following, we depict a few examples from the literature of different techniques used for ECG signal processing [68,98,99,100,101]. Recent research in the literature adopts Neural Network (NN) and decision trees for the diagnosis of different cardiac diseases, the assessment of cardiac health conditions, the detection of chronic problems, sleeping issues including apnea, and mood and emotion recognition [55]. Other examples include using deep learning for the automatic recognition of ECG signals [102], a convolutional neural network (CNN) for arrhythmia classification in [103] and AF in [104], and recurrent neural network (RNN) for activity prediction [105]. Different machine learning algorithms have been applied in IoT Cloud-based monitoring systems in [13] and Cloud-based cardiology services in [106].
2.3.5. Visualization
The visualization process typically includes all the functionalities that will allow users to inspect and interact with recorded or annotated ECG signals in real-time, as well as offline from a file [80,81]. This process acquires its importance throughout the value chain as it helps the human brain to better understand and analyze patterns, and detect abnormalities, especially with large datasets. The visualization applications vary in terms of the hosting application, nature of information projected, and the functionalities supported, which can be implemented as a web service through a browser, mobile applications [71], or desktop applications [107]. There are many commercial applications for ECG monitoring in the market, such as Custo Med, Philips, NORAV, and MEDSET [108].
Motalova et al. [82] proposed a design for web application visualization to display data from the ECG device. The application included data charting, electrode state, and animation storyboard functionalities. A three-dimensional cave interactive system was proposed in [81] which provides a graphic user interface that demonstrates a three-dimensional modeling and animation of a human heart using the R-wave of the electrocardiographic signal.
2.3.6. Supporting Processes
The supporting processes are the activities that provide extra functionalities to support the primary processes to realize an efficient monitoring system. In other words, they are not compulsory for every ECG monitoring system. For example, the signal selection process is performed only in systems using multiple physiological types of signals for heartbeat detection [58,70] or R-peak detection [62]. Additionally, the data compression process is required for many purposes, including storage capacity reduction and faster file transfer, which eventually contributes to efficient bandwidth utilization and cost reduction, especially in the case of continuous ECG monitoring and data streaming. Various data compression techniques were proposed in [84,85,88]. Němcová et al. [79] presented a thorough literature survey on data compression methods, as well as quality assessment techniques applied after compression.
Another example of a supporting process, as depicted in Figure 2, is data encryption and decryption. This process plays an important role in supporting security and data privacy, which are incorporated in very few ECG monitoring systems. Page et al. [72] used a fully homomorphic encryption (FHE) technique for the data encryption in a remote monitoring system.
The modeling and learning processes are considered the most important supporting processes required for machine learning, and prediction or prognosis of cardiovascular diseases. Although they are defined as the main processes for prediction-based systems, not all ECG monitoring systems support prediction. Therefore, we consider it as one of the supporting processes, rather than a primary process. Numerous monitoring systems define modeling, learning and prediction [75]. Some research proposals define a distinct training process [35,68] deep learning (ANN) process [83,87], machine learning (ML) process [86], and ML streaming process [13].
Nevertheless, data storage is considered a supporting process because it services many of the primary processes along the lifecycle of ECG monitoring systems. The data storage process is defined as a standalone process in [13,71,76], and for encrypted data storage in [72].
3. Experts’ Taxonomy of ECG Monitoring Systems
Due to the continuous expansion in the number of ECG monitoring systems proposed in the literature, it is very hard for researchers in this field to analyze and classify these systems into distinct, cohesive clusters of interrelated works. In this research, we use the term “cluster” to refer to a category of research works sharing common characteristics, attributes, and features. We use these clusters to classify papers related to ECG monitoring systems. The authors of this work have adopted a systematic approach that starts with (1) collecting resources (e.g., journal articles, conference papers, and book chapters) from various databases including Scopus, IEEE, Springer, and ACM, (2) conducting numerous preprocessing activities which involve, for instance, cleaning, reorganizing, removing duplications, and deleting non-system based solutions, (3) running extensive meeting sessions to classify and group these systems based on the surveys conducted in more than 600 publications, (4) sharing the clustering results with both medical and technological experts in the field to seek their feedback and inputs, and (5) finally, meeting with all involved parties to finalize and refine the final clusters of ECG monitoring systems.
Figure 3 presents ECG monitoring systems divided into four main clusters, in addition to the fifth cluster, which is considered the future generation of ECG monitoring systems. These are clustered based on the monitoring context for which they are developed, the involved ECG technologies and devices that characterize these systems, the monitoring scheme and frequency adopted, the monitoring target and purpose for which these systems were implemented, and finally, the futuristic monitoring system that leverages new technologies, such as AI, robotics, and nanotechnology, to shape emerging ECG monitoring systems. In addition to the five clusters, a horizontal underneath level represents the communication protocol and the wireless technology used by all the categories of monitoring systems to transport the ECG signals from sensors to the underlying servers and/or devices under which the ECG is processed and visualized.
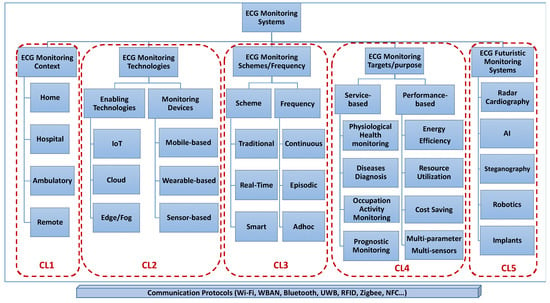
Figure 3.
ECG monitoring system clustering.
In the following sub-sections, we describe and analyze each of the abovementioned clusters and we provide a comprehensive review of each cluster in terms of integrated ECG monitoring systems and solutions.
3.1. Context-Aware ECG Monitoring Systems
The first cluster of work incorporates the group of systems that are organized into monitoring contexts for which ECG monitoring systems were developed and consist of home-based, hospital-based, ambulatory-based, and remote-based ECG monitoring systems. Within each of these environments, commonalities exist and variations are also evident.
In Table 2, we describe the selected context-aware ECG monitoring systems and their categories, along with the selected papers under each category.

Table 2.
Classification of selected context-aware ECG monitoring systems.
3.1.1. Home ECG Monitoring Systems
ECG Monitoring systems deployed in the home environment are generally classified into what is called telemonitoring, wearable continuous monitoring, and monitoring the elderly people in their homes. These systems were developed to reduce the economic burden on hospitals and involve patients in their continuous health monitoring with the comfort of being at home and are designed for people with lifelong and chronic disease or elderly people that require permanent assistance, surveillance and monitoring.
Telemonitoring is one of these systems which is integrated mostly in home or hospice settings to enable nurses to efficiently monitor patients, react to problems, and treat them before they propagate to more serious issues. Many researches proposed telemonitoring systems [109,110,111,112]; an example of these systems includes the work of [109], which uses mobile phones and NFC equipment to support AF monitoring. System feasibility, usability, and patient devotion have been tested in a clinical environment. Another body of work in [110] proposed the use of mobile Cloud computing to overcome issues related to the computational requirement of the large amount of data processing resulting from continuous ECG monitoring. Coronary heart disease risk is identified using feature extraction and an adaptive neuro-fuzzy inference system-based classification has been used. Similarly, in the work of Wang et al. [111] a hybrid mobile-Cloud ECG telemonitoring method has been proposed to allow more effective personalized medical monitoring and convey processing to the Cloud whenever heavy processing is required and cannot be handled by mobile devices. Likewise, Benini et al. [112] proposed a user-friendly single-lead ECG device designed for patients’ use at home. The device requires few calibrations to be operated and it is able to send, transparently, the acquired ECG to the surveillance center through a Bluetooth connection and via an Internet gateway.
The second category of home-based ECG monitoring systems involves wearable continuous monitoring, among which are the following propositions [18,19,20,128]. While according to the authors of [18], the effect of home-based wearable continuous ECG monitoring covers the discovery of undiagnosed AF in a randomized clinical trial, in [20] a real-time wearable ECG monitoring system for cardiac arrhythmia classification is introduced in a living environment. A review paper by the authors of [19] focuses on remote monitoring of cardiac functions, overviews the existing ECG data storage format standards and identifies their limitations.
The third category of home-based ECG monitoring involves elderly monitoring; several systems have been developed, among which include [24,113,114,115]. Mena et al. [115] proposed a mobile personal elderly health monitoring for automated classification of ECG signals using machine learning techniques. A wearable ECG monitor is integrated with a self-designed wireless sensor for ECG signal acquisition and is used with a native, purposely designed smartphone application. Other alternative studies [24,113,114] introduced various smart features to ECG monitoring systems for the elderly people. Smartness is introduced in the elderly monitoring environment where a novel monitoring framework is proposed in [113] to provide flexibility and enable interoperability between a myriad of healthcare monitoring devices. It relies on the analytics of evidence-based data collected from sensors, as well as the massive data collected from social networks. Smartness was also implemented in [114] through smart clothes for elderly ECG monitoring, which consisted of conductive fiber clothes to acquire ECG, a gateway to relay the data, and a server to process the data.
3.1.2. Hospital ECG Monitoring Systems
Hospital-based ECG monitoring systems are classified into systems developed either for an intensive care unit (ICU) clinical setting [16,17], non-ICU clinical setting [14,15,116,117], or a Holter monitoring setting [36,118,119,120,121]. ECG Monitoring systems for ICUs involve, for instance, the work depicted in [16], which used data mining techniques to predict mortality and length of stay in an ICU. The authors presented an analysis of a mortality prediction algorithm to evaluate the extent to which the proposed algorithm can predict mortality rate. Similarly, Ahouandjinou et al. [17] proposed a hybrid architecture to visually monitor the patient for automatic detection of risk situations and alert generation using a multi-camera system and collaborative medical sensors network.
ECG monitoring systems for non-ICUs involve textile-based, contactless ECG monitoring, as proposed in [14]. This consists of monitoring contactless the vital signs with capacity sensors embedded in various patients’ auxiliaries. Also, a monitoring device has been developed for remote monitoring of out-of-hospital patients’ heart conditions in [15]. It consists of a real and flexible collection of ECG data from patients, obtaining valuable information that can be used for remote research and diagnosis. Finally, best practices for hospital ECG monitoring have been proposed in [116] and a set of recommendations are made, which included indications, timeframes, and strategies to improve the diagnostic accuracy of cardiac arrhythmia, ischemia, and QT interval monitoring.
Holter-based ECG monitoring is another type of system proposed in [36,118,119,120,121]; it is connected to the patient’s body through electrodes. In [118], a small and smart ECG Holter monitoring system integrated smartphones to retrieve ECGs from sensors, classify and detect abnormal signs. Other studies [119,121] used a Holter monitoring system to detect and improve AF in stroke patients. This is a very challenging research problem, as episodes are often short, occur randomly, and are frequently asymptomatic. The specific use of a Holter monitor can be found in [36] to record ECG underwater. ECG was analyzed for heart rate, arrhythmias, conduction abnormalities and ischaemic events in relation to various diving stages.
3.1.3. Ambulatory ECG Monitoring Systems
Considerable research and development is being undertaken for ambulatory ECG monitoring systems [8,21,22,23,122,123,124,125]; most of the researches support data collection, transmission, and analytics for ambulatory emergency situations. An example is the project depicted in [123], which implements a low-cost, high-efficiency and effective wireless real-time system for health monitoring through a telemetry system for on-spot-accident patients. The authors of [124] developed a wireless capacitive sensor for ambulatory ECG monitoring over clothes, while the authors of [21] proposed a modified Lewis ECG lead system for the ambulatory monitoring of atrial arrhythmias.. Finally, compressed sensing has been introduced in [23] for real-time energy-efficient ECG compression in a Wireless Body Sensor Network (WBSN).
Several research works on wearable ECG monitoring have been developed in the literature [25,29,125,126,127,128]. These works can be classified into textile-based systems, such as [29,128], and contactless based systems, such as [126]. Textile-based solutions integrate clothing (e.g., a shirt) with integrated sensors recording ECG and an acquisition module for data storage and processing. However, contactless-based monitoring systems are non-invasive and do not require direct body contact to retrieve ECG and other vital signs. Both categories of systems have been implemented for monitoring, for example, heartbeats, to detect patterns that might point to arrhythmia in diverse contexts, such as ambulatory and home settings.
3.1.4. Remote ECG Monitoring Systems
The telemonitoring method proposed within the context of remote ECG monitoring system in [10,129,130] differs from the one described for the home monitoring context above. It is designed and developed for distant patients whose movement is very frequent (e.g. exercising, doing sporting activities, and/or working), which does not necessary require his/her presence at home. Such systems include a remote health monitoring system for detecting varying cardiac disorders, including, for instance, arrhythmia and myocardial conditions, as proposed in [129]. Likewise, Tewary et al. [130] designed and developed a global system for a mobile-based smart wearable system capable of detecting sudden fall situations, cardiac abnormalities, and hypertension/hypotension; thus making it suitable for real-time monitoring, self-diagnosis, and remote diagnosis purposes.
Numerous research initiatives developed smart devices for ECG monitoring [12,24,126,131,132], where these devices implemented intelligence either in the sensors themselves or within the network components. Examples of these researches include a remote patient monitoring system for cardiac care assistance using a self-configured sensor network, as developed in [131]. Also, intelligent wireless sensors have been designed in [132] to perform data acquisition and limited processing. Individual sensor monitors specific physiological signals, communicates with other sensors and connects to a personal server.
A couple of research studies [133,134,135] have adopted compressed ECG sensing as a promising approach to lower energy consumption in wireless body area networks for ECG monitoring. The wavelet representation of the ECG signal has been used to improve the performance of compression and reconstruction of ECG signals [133]. Earlier information about the wavelet dependencies across scales has been incorporated into the reconstruction algorithms and has exploited the high fraction of common support of the wavelet coefficients of consecutive ECG segments. Another research work [134] studied the energy efficiency of compressed sensing for ambulatory ECG monitoring. They propose a compressed sensing architecture, combining a redundancy removal scheme with quantization and Huffman entropy coding, to effectively improve the compression ratio. Comparably, in [135], a real-time energy-aware ECG monitoring system based on the emerging compressed sensing (CS) signal acquisition/compression paradigm for the WBSN applications has been proposed.
3.2. Technology-Aware ECG Monitoring Systems
The second cluster of researches encompasses a group of monitoring systems that emphasizes the use of emerging technologies to support ECG monitoring. This group is classified into two categories: (1) the enabling technologies which involve IoT, Cloud, and Fog and (2) the monitoring devices which comprise mobile devices, wearable devices, and sensor devices. Table 3 depicts a selection of the most relevant work leveraging the new technologies involved in ECG monitoring systems.

Table 3.
Classification of selected technology-aware ECG monitoring systems.
3.2.1. Enabling Technologies
ECG monitoring relies on key technologies to support various ECG processes, including preprocessing, processing, storage, analytics, and visualization of ECG signals. Cloud infrastructure provides storage and processing resources over the internet to support ECG monitoring systems. Fog computing is a very promising technology that brings the processing resources close to where the ECG data are generated, thus providing low latency and energy efficiency. IoT technology enables remote ECG monitoring using IoT devices to retrieve ECG signals, allowing transmission in real-time over the internet to the physician for further analysis.
Of particular interest are systems that propose solutions to optimize processing and reduce the cost of data transmission and storage over the Cloud infrastructure [24,26,71,143,144,145], this is also very crucial in cases of emergency and vital situations when real-time analytics are urgently required for actionable insights. Tuli et al. [26] incorporated ensemble deep learning in edge computing devices and deployed it for the real-life application of automatic heart disease analysis. Similarly, wearable devices were empowered with processing capabilities to locally (at the edge) analyze the signal and identify abnormal behaviors [144]. However, wearable embedded devices, mobile edge devices, and Cloud services were combined to provide reliable, accurate, and real-time heart monitoring [25,143]. Wearable devices are remotely trained to interpret heart abnormalities and the Fog extends the Cloud by migrating data-processing closer to the production site, thus accelerating the system’s responsiveness to events.
Other research initiatives have focused on the development of patient-centric monitoring solutions where patients play an active role in their health monitoring. While in the work of Xia et al. [71] a cloud-based system has been developed to assess the usefulness of the ECG data collected from patients themselves using either mobile devices or web applications. Wu et al. [29] addressed the comfort of monitored patients and designed a non-invasive textile electrode that guarantees excellent quality of ECG reading and offers comfort to patient while they are being monitored.
A great number of researches proposed relevant IoT-based solutions for ECG monitoring [12,27,132,136,137,138,139,140,141,142]; these researches are centered around the use of IoT devices for real-time ECG acquisition, processing, and analytics. The authors in [27,136,137], and [138] proposed an IoT-based patient-continuous monitoring system using the ECG sensor. All systems collect ECG data using sensors and process and analyze in real-time the collected ECG data. Subsequently, they allow remote access to the patient’s health condition, to third parties (e.g., doctor and nurse), in addition, an alert is sent in the case of a critical situation for timely intervention. Other solutions, such as in [132], go beyond the adoption of traditional IoT-based ECG monitoring systems and further incorporate intelligent wireless sensors within a personal area network to handle data acquisition and limited processing, which helped in improving monitoring efficiency and urgent reactions in cases of emergency. Similarly, in [12], nanomaterial-enabled ECG sensors were used, which improved conductivity, electrical proprieties, and reduced the induced monitoring cost. Moreover, in [141], Granados et al. proposed an IoT platform for real-time analysis and management of a network of bio-sensors and gateways. They explored the use of a Cloud deep neural network architecture for the classification of ECG data into multiple cardiovascular conditions.
More comprehensive work has been reported in [139], which proposed an interconnection framework for mobile health (mHealth) based on the IoT. The proposed framework details the hardware and software components along with the underlying network and protocol used, including 6LoWPAN and YOAPY protocols to support secure and scalable integration and deployment of sensors within the patient’s environment. The framework evaluates the system’s capability to provide continuous monitoring, ubiquitous connectivity, extended device integration, reliability, and security and privacy support.
3.2.2. Monitoring Devices
A multitude of devices are being used nowadays for ECG monitoring systems. They are classified into mobile-based, wearable-based, and sensor-based devices.
Mobile-based devices for ECG monitoring involve a wide range of devices, including, for instance, smartphones, smartwatches, and pocket ECG monitors. Aljuaid et al. [146] evaluated the effectiveness of using a smartphone-based ECG monitoring device on the frequency of clinic visits of patients who experienced ablation of AF. This study proved that the use of smartphone-based ECG monitoring led to a significant reduction in patient visits to the clinic after the surgical intervention. Likewise, a mobile device was integrated with an Arduino microcontroller and various sensors, including an ECG sensor, to retrieve sensory data and display vital sign measurements and send notification messages and the user’s location to the healthcare provider if any abnormality was discovered [31]. Another piece of work reported in [32] combined an Arduino microcontroller with an Android-based smartphone to develop an intelligent healthcare system and provide elderly patients with medical services at home. The system integrates an artificial bee colony (ABC) algorithm for ECG R-peak detection. It is able to detect various abnormalities, such as high blood pressure, low blood pressure, fever, tachycardia and bradycardia; it also sends notifications in case of unexpected events.
Various research initiatives proposed solutions that integrate wearable devices within an ECG monitoring system [14,21,22,29,30,125,126,127,147]. These solutions are either integrated within an ambulatory setup, home environment, or patient/user setup and are used for the monitoring of various vital signs. While the authors in [21,125] proposed an ECG monitoring device for wireless monitoring of atrial arrhythmia, and Fung et al. [22] explored a wearable “on-body” ECG patch, which was unobtrusive, easy to use device, leading to increased device wear time and diagnosis yield. Another category of an ECG monitoring system involves innovative contactless sensors to retrieve ECG signals without disturbing the patient’s comfort. Rachim and Chung [126] proposed a system consisting of capacitive coupled electrodes embedded in an armband. The system integrates analysis features to detect a real-time heartbeat, and a filtering algorithm to filter distractions generated by body movement or other noises. Likewise, according to the authors of [147] a smartwatch was embedded with various built-in sensors such as an accelerometer, gyroscope and optical heart rate sensor and compared with a commercially available and clinically used non-contact sleep sensor. Also, in [14] a textile-based, contactless ECG monitoring system with sensors embedded in non-ICU environments was proposed. The system measures ECG signals non-obtrusively using capacitive sensors integrated within patients’ stretchers, beds, and wheelchairs. These contactless monitoring systems prove their robustness, and efficiency in recording quality signals and generate effective real-time analysis.
Most of the abovementioned ECG monitoring systems integrate sensing devices as a core component of the system to retrieve ECG signals and ultimately to do some light processing either at the edge or at the Cloud. Therefore, overlapping might be apparent with the other abovementioned categories, since they are embedding sensors within the ECG monitoring solution. Among these research initiatives include the subsequent propositions from [12,26,28,136,138,139,142]. For instance, Villarrubia et al. [142] proposed a monitoring and tracking system that uses virtual organization of agents for easy integration of different devices. It facilitates the integration of interactive television to moderate activity with the user under monitoring. Additionally, [148] proposes a button-like wearable wireless non-contact system for long-term multiple biopotential monitoring. It relies on ultra-high input impedance and is able to retrieve various biopotential signals, including ECG, through multiple layers of cloth without directly contacting human skin. This system proves its feasibility of extended monitoring without disturbing daily activities.
3.3. ECG Monitoring Systems Based on Schemes and Frequency
The third cluster of our experts’ classifications of ECG monitoring systems focuses on computational aspects. In this dimension, two subcategories are recognized. These are the monitoring scheme and the processing frequency. The monitoring scheme defines the spatial screening setup. ECG signals can be measured in stationary setups in different contexts while the patient is directly connected to screening and processing devices for diagnostic/prognostic purposes, which we refer to as a “Traditional Monitoring Setup”. Alternatively, ECG signals can be measured in mobile setups, where the patient is experiencing real-life activities for a full spectrum of monitoring purposes, such as activity monitoring, diagnosis, prognosis, or fitness monitoring, which we refer to as a “Real-time Monitoring Setup”.
In contrast to the monitoring scheme, the processing frequency defines the temporal screening setup. ECG signals can be processed in a constant setup that we refer to as “continuous monitoring,” a one-time setup that we refer to as “ad hoc monitoring,” or a recurring, prescheduled, and preplanned set up, which we refer to as “episodic monitoring.”
In this section, several ECG monitoring system research work are reviewed against the aforementioned criteria, highlighting technical complexities, sampling rates, advantages, and disadvantages of different approaches. Table 4 summarizes the research works reviewed in this section.

Table 4.
Classification of ECG monitoring systems based on scheme and frequency.
3.3.1. Traditional ECG Monitoring
A number of research work addressed traditional ECG monitoring setups in various contexts such as hospitals [149,150,151], homes, or remote ambulatory settings [31,32,112,146,152]. Screening devices can be physically connected to processing devices [31,32,149,150], or wirelessly accessed [17,112,152,153].
Ad hoc (i.e., one-time), immotile monitoring has been deployed in many research studies to address various healthcare situations using different types of ECG sensors and monitoring platforms. For instance, Aljuaid et al. [146] used ECG Check (https://www.cardiacdesigns.com/) with smartphone technology to monitor AF patients post-ablation; Benini et al. [112] designed a single-lead sensor for home telemonitoring; Yousef and Hau [31] used an analog heart rate sensor in their mobile-based system (myVitalGear) for general health monitoring, and Rafiq et al. [152] designed a system with three-lead wet electrodes for home health monitoring. It was emphasized by a number of researchers that ad hoc, non-mobile monitoring can potentially lower the burden of outpatient clinical visits and AF-related visits in the post-ablation period. In their study, Aljuaid et al. [146] mentioned that traditional smartphone-based ad hoc home monitoring helped reduce the number of post-ablation patients’ visits by more than 50%.
However, in ad hoc monitoring settings, patients may forget to perform the monitoring tasks. In addition, for patients with critical health situations, it is vital to have regular recurrent screenings. To address these concerns, some research works proposed episodic monitoring that can be done at pre-scheduled intervals. For example, Hsieh and Len [32] incorporated an alarm function into the system to remind the patient to use the screening device. They pointed out that their monitoring system not only saves medical resources, but also enables elderly people to care for themselves, thereby promoting their health.
For critical and life-threatening cases in traditional setups, continuous monitoring is necessary, especially in ICUs. A number of research work focused mainly on neonatal patients, for instance, Bambang et al. [149] and Bouwstra et al. [150] who designed smart jacket-based continuous monitoring systems for prematurely born babies in the neonatal ICU (NICU). Alternatively, for elderly people who would be moving around, Ahmed et al. [17] utilized IoT-based technology for wireless sensor nodes positioned in the ICU and nursing rooms to provide continuous ECG monitoring of patients with severe cases and then transmit the signal to remote doctors. Precision in these situations is vital; therefore, a major challenge faced in ICU continuous and smart monitoring is the need to select a suitable filtering technique, since ECG signals are noisy, which need a suitable amplifying technique should be used, given that the ECG signal is measured in millivolts.
3.3.2. Real-Time ECG Monitoring
In some cases, cardiologists may recommend 24-hour Holter monitoring for patient monitoring. A Holter monitor is a 12-lead medical device that records the heartbeat and checks for unusual signs. It is usually uncomfortable to apply the Holter 12-lead device to the patient’s body for 24 hours. Some attempts have improved the 24-hour Holter monitoring and utilized an adhesive patch that can be attached to the patient’s body, reducing the number of required leads in a typical Holter. For instance, Karaoğuz et al. [125] used a BeyondCare device applied to the upper left upper region of the subject’s chest beside the 12-lead Holter device, simultaneously, for palpitation assessment.
Recent advancements in wireless ECG monitoring systems have produced a wide variety of real-time monitoring systems, ranging from wearable textile-based monitoring systems, such as smart shirts [5] and textile electrodes [154,155,156], to contactless [157] ECG monitoring systems. In real-time setups, patients can measure ECG signals while doing normal real-life activities [161]. This has allowed for more prompt assessment and medical intervention when necessary. Furthermore, it substantially reduced the cost of healthcare expenses by lowering the number of hospital visits for traditional regular monitoring. For instance, Lee and Chung [5] designed a smart shirt that continuously measures ECG and acceleration signals remotely in real-time setup for health monitoring. Bianchi et al. [154] proposed the use of T-shirts and/or bed sheets with sensor electrodes to measure ECG signals and other vital signs to assess sleep and respiratory problems in real-life settings. Bsoul et al. [6] designed MedAssist, a continuous, real-time, single-lead, wireless monitoring system for the diagnosis of sleep apnea. On the other hand, the authors of [155,156] designed washable long-term wearable sensors for fitness and activity monitoring.
Despite the advantages of continuous monitoring in real-time setups, it generates an abundant amount of ECG signal data, which can give substantial signal noise and artifacts caused, sometimes, by abnormal physical activities, a problem that has been highlighted by many researchers [5,154]. This, in turn, emphasizes the need for noise filters and smart feature selection algorithms. Alternatively, episodic monitoring was adopted in several researches to limit the causes of motion artifacts and constrain the amount of generated ECG signal data, allowing for easier processing and analysis. For example, Yoon and Gho [157] utilized a commercial contactless ECG monitoring device for remote home telemedicine. In their experiments, they considered pre-planned, pre-scheduled three-time intervals focusing on the patient’s resting state and post-exercise state. Lee et al. [158] proposed a mobile cardiopulmonary rehabilitation system with a wireless ECG Holter to give real-time feedback during exercise in home-based environments. In contrast to pre-scheduled continuous monitoring, some researchers adopted signal-sampling techniques that can be used for event-based ECG monitoring. Signal sampling algorithms convert continuous-time signals into discrete-time signals. For example, Ravanshar et al. [159,160] implemented a level-crossing sampling technique to reduce the sampling rate from 1 kS/s to around 120 S/s. Consequently, a considerable reduction is achieved not only in the amount of processed signals but also in power consumption.
3.4. ECG Monitoring System Targets and Purposes
Several ECG monitoring systems in the literature have been developed to serve a certain purpose or to target a specific functionality, which we grouped into the fourth cluster. In this cluster, we classify ECG monitoring systems as service-based or performance-based systems. The service-based systems are focus on either medical or non-medical purposes. However, performance-based monitoring systems intend to concentrate on performance improvements. The following subsections detail the classification of several proposed ECG monitoring systems, along with examples of selected systems highlighting special key features and key research problems.
3.4.1. Service-Based Monitoring Systems
In this section, we classify the service-based ECG monitoring systems into three main categories: diagnoses, activities, and prognoses. Numerous ECG monitoring systems have been developed for diagnosing specific or multiple diseases. Table 5 summarizes the aforementioned service-based ECG monitoring system classification. In Table 5, we further classify the systems focusing on disease diagnosis into two main categories: (1) general CVDs, having three subcategories including Arrhythmia, AF, and other abnormalities, such as, such as left ventricular hypertrophy [11]; unexplained syncope [162]; long QT syndrome [163]; depression [164] and coronary heart disease [165], and (2) sleep apnea.

Table 5.
Classification of selected service-based ECG monitoring systems.
In general, most of the systems use wireless and wearable devices for data acquisition and were designed for diagnosis purposes [166,167,168]. Other ECG monitoring systems mainly focus on the interpretation of diagnostic algorithms [88,166,169,170]. Arrhythmia diagnosis is one of the most common diseases diagnosed based on ECG signals [171,172,173,174]. Real-time Cloud-based ECG monitoring systems for arrhythmia detection were proposed in [175,176], whereas AF is commonly diagnosed based on ECG signals [57,67,177,178,179]. ECG signals contribute to the detection of several cardiovascular abnormalities, which were addressed in [180,181,182]. Developing evolutionary, efficient, and accurate automatic diagnostic techniques have been always an open area of research to overcome many challenges, among which are medical device capabilities, ECG diagnostics overlapping patterns, and other ECG signal-related issues throughout the system’s lifecycle.
Other systems support the objective of monitoring user activities; examples include sports, driving, daily activities, and elderly activities. ECG monitoring systems dedicated to sports activities represent a significant share among existing monitoring systems [37,38,183]. For example, Peritz et al. proposed a method for diagnosing athletes’ heart palpitations [184]. Additionally, a solution using multi-sensor wearable sports devices was proposed for heart rate detection under different subjects’ activity states, that is, different types of movements [185]. Another exercise evaluation platform has been developed by Sun et al. [186]. Furthermore, Pollonini et al. [187] proposed an integrated device for measuring oxygen transport during physical exercise based on ECG and PhotoPlethysmoGraphy (PPG) monitoring. The health of professional athletes, such as footballers was the main study in [188], where cardiovascular conditions and other health problems were evaluated for health risk assessment during their preretirement and postretirement years. Moreover, water sports monitoring was discussed in [36].
Other activities, such as driving, was tackled in the literature in [189,190,191,192,193,194,195]. These studies proposed ECG monitoring for the purpose of observing drivers’ health and emotions, with the ultimate goal of enhancing transport safety on the roads.
The elderly population was the objective of a good number of publications in the reviewed literature. Some of these researches study wearable devices for monitoring elderly activities [114,196], others propose the use of smartphones for monitoring [197], and forecasting short-term health conditions [198]. Daily activities using wearable monitoring devices were addressed in [33,34,35]. Furthermore, real-time activity monitoring at different premises, such as home, healthcare or sports facilities, was discussed in [155,156,199].
ECG systems related to activity monitoring tend to suffer from similar challenges faced by remote systems, among which are sensor characteristics, hardware constraints of on-board data processing, complexity and robustness of classification algorithms for mobility detection. Additionally, these systems have several ethical issues, including data collection (e.g., subjects’ privacy), as well as lack of monitoring system usage confidence (e.g., subject can manually manipulate the monitoring device). Prognosis is one of the main objectives of ECG monitoring systems attracting much research interest. This is because predicting the likelihood of expected disease development is considered a major human health concern nowadays. Many ECG monitoring systems were proposed not only to diagnose, but also to predict certain diseases such as arrhythmia [200,201], AF [63,202], Epilepsy [203,204], and other cardiovascular diseases [89,205,206,207,208,209,210,211,212]. Many studies that are related to daily monitoring and activities during sleep, proposed different designs and specifications for wearable devices, such as shirts [33,34,35].
Additionally, prediction based on ECG monitoring was addressed in various aspects of health status, such as survival chances, mood and behavior, and health status. Survival, risk of cardiac death and other predictions related to cardiac problems were discussed in [213,214,215]. Alternatively, the prediction of mood changes and response to depression treatment were addressed in [39,40,41]. General health status and activity prediction were proposed in [105,216]. An interesting study related to predicting heart motion to assist in robotic heart surgery was detailed in [217].
3.4.2. Performance-Based Monitoring Systems
We define performance-based monitoring systems as those that address performance advances in different aspects and characteristics. In this section, we classify the performance-based systems into three main categories, considering the main factors affecting the performance, such as energy, cost and resource provision. Table 6 summarizes the researches reviewed in this section.

Table 6.
Classification of selected performance-based ECG monitoring systems.
Energy conservation is one of the main contributors to better system performance and to enhance life quality. Several reviewed ECG monitoring systems proposed solutions for lower energy consumption by reducing signal transmission, processing, and supporting signal compression. Most of the studies promoted the use of Bluetooth Low Energy (BLE) for signal transmission to support low energy consumption [126,155,222,223,224,225,226,227,228,229,230,231,232]. Few other studies used alternative wireless methods to reduce transmission and eventually reduce power consumption [234,235]. However, the use of the aforementioned approaches implicate some challenges regarding the lack of interoperability of different wireless devices, short battery life, and some security problems. Another way of reducing energy consumption is optimizing processing techniques and proposing new enhanced algorithms for signal processing [222,233,236,237]. Alternatively, signal compression is used for lower energy consumption in [134,135,239,240,241,242,243].
In general, cost reduction is also an extremely important objective of many performance-based monitoring systems. Different approaches lead to cost reduction, including the use of low-cost devices, such as smartphones [232,244,245,246]. Other studies proposed special low-cost circuit designs [247]. Reducing the cost could also be achieved by using a low-cost wearable devices for signal acquisition, especially in IoT-based systems [248,249]. Other low-cost devices were used, such as portable ECG monitoring devices in [250,252]. Sanghavi et al. [10] proposed an IoT-based remote monitoring system, which includes a Raspberry Pi, Arduino Uno, ECG Sensor and an IoT Cloud for storing and plotting ECG data in real-time. A home-based monitoring system with low-cost data acquisition was proposed in [251]. Disease prevention is another perspective in reducing monitoring costs. This issue was addressed in several papers in the literature. Yong et al. [253] suggested prolonged ECG monitoring for secondary stroke prevention, which eventually eliminates the cost of stroke treatment consequences. Additionally, prolonged and active monitoring significantly improved the diagnosis of AF and was associated with significantly lower emergency department visits and hospitalization requirements [254].
Other resource-aware monitoring systems were proposed for efficiency improvement. For example, Wang et al. [255] proposed resource-aware Body Sensor Network (BSN) architecture for real-time healthcare monitoring.
Management, processing, and storage of data in ECG monitoring systems introduce several challenges, one of which is the storage of an enormous volume of data efficiently while responding to dynamicity and scalability requirements. Storage and transmission improvements were proposed in a resource-efficient ECG monitoring system named Generative Model-Driven Resource Efficient ECG Monitoring (GeM-REM). In this system, the ECG data are stored as model parameters rather than data samples to reduce the storage space, and only the abnormal sensed ECG signals are transmitted to reduce energy [232]. Other resource allocation approaches were addressed in [222,233].
3.5. ECG Futuristic Monitoring Systems
The latest trends in ECG monitoring systems will revolutionize the way ECG signals are collected and processed to give valuable insights serving various purposes while protecting patients’ privacy and emotional health. Personalization and adaptation to various contexts as well as to various stakeholders will offer a new level of high-quality smart healthcare. Modern technologies will play a vital role in this radical transformation. These include radar cardiography, implants, robotics, steganography, and other AI technologies. Table 7 summarizes selected research works related to these five categories.

Table 7.
Classification of selected futuristic ECG monitoring systems.
Continuous heart rate monitoring and immediate heartbeat detection are primary concerns in contemporary healthcare. Most of the research work reviewed in this study focuses on ECG signal monitoring that generally requires touch-based sensing of the patient’s skin. Patient skin irritation caused by touch-based sensory devices were highlighted by a number of researchers [97,125]. A convenient and reliable touch-free alternative is radar cardiography. Radar systems enable touchless, contactless, and continuous monitoring of heart rate through clothes, blankets, or other isolators. Plenty of the research work investigated the possibility of using radar systems for continuous heartbeat monitoring and detection of vital signs [256,257,258,259,260,261].
Alternatively, some researchers investigated implanted sensor technology for durable and long-term continuous monitoring [263,264]. For instance, Giancaterino et al. [262] utilized insertable cardiac monitors (ICMs) which are small, medically implanted devices to offer continuous ambulatory ECG monitoring with a lifespan of up to three years. Sunnet et al. [265] used an implantable loop recorder (ILR), which is a small devices with integrated leads that are implanted in a small subcutaneous pocket after a simple surgery, with a dedicated AF detection algorithm for long-term ECG monitoring in patients with atrial flutter. Implants offer a practical solution for long-term monitoring, given that continuous external monitoring for such a long period of time can be unfeasible.
On the other hand, advancements in robotics introduced new opportunities for cardiac healthcare, especially with the great challenge of limited medical resources. Some researchers investigated the dimensions of the practical use of robotic-assisted heart surgeries [217,266]. Others studied the possibility of having a robot assistant providing medical feedback, diagnosis, and notifications [267,268].
New AI technologies will extend ECG monitoring systems’ horizons beyond physiological disease assessment. ECG signal can be used to evaluate psychological state, emotions, and stress levels to aid mental healthcare for people living in stressful environments [59,269,270]. Advancement in deep learning technologies and algorithms can provide interesting opportunities for adaptation and personalization, overcoming individual differences by periodical retraining [271,272].
In using the aforementioned technologies for monitoring patients’ heartbeats and other vital signs, not only an enormous amount of ECG signal is collected, but also other physiological measurements, such as temperature, blood pressure, glucose levels, as well as patients’ personal data, are required. It is, therefore, utterly important that patients’ privacy is protected during data transfer over the communication networks, as well as being stored in hospital servers or used by remote monitoring systems. Several techniques and security protocols were proposed in the literature to protect users’ privacy. Techniques used can be categorized into two main classes. The first class of security techniques are focused on encryption and cryptographic algorithms [276,277]. These techniques are accused of having a large computational overhead, which makes them unsuitable in a resource-constrained mobile environment. The second class of security techniques is focused on concealing sensitive information inside another set of insensitive host data, with no increase in the host data size or computational overhead. These techniques are called steganography techniques. Steganography is defined as: “the art of hiding secret information inside another type of data called host data” [278]. A number of research work investigated steganography techniques to secure patients’ privacy during ECG signal collection, storage, and transmission [48,273,274,275].
4. Key Challenges of ECG Monitoring Systems
As discussed in this paper, ECG monitoring systems involve many components, variable contexts, and various stakeholders and encompasses diverse technologies. This diversity and variability of ECG monitoring system contexts and components impose a number of challenges that have been highlighted by several researchers. In the subsequent sections, we discuss ECG monitoring challenges related to the use of monitoring devices, signal quality, sensor design, durability, the size of the data, visualization, and integration.
4.1. Challenges Related to Usage of Monitoring Devices
Aljuaid et al. [146] pointed out that manual static screening (i.e., traditional monitoring) has a major limitation when carried out in home settings, since patients have to learn how to operate monitoring devices, such as ECG Check (https://www.cardiacdesigns.com/) or Kardia (https://www.alivecor.com/), as well as having sufficient knowledge in using heart monitoring smartphone applications, which sometimes may be a challenge for elderly and illiterate people. Hsieh and Len [32] highlighted that patients may forget to carry out monitoring tasks in ad hoc monitoring in home settings, reducing the gains sought from regular monitoring. Hence, alarm and screening reminder needs to be considered when designing home manual monitoring systems.
4.2. Challenges Related to Signal Quality
In real-time monitoring, patients can enjoy real-life activities, including physical exercise and running, which usually result in motion artifacts, signal noise, and deterioration. Lee and Chung [5] highlighted in their research the importance of combining efficient filtering methods for real-time monitoring setups with motion artifacts removal during running or physical exercise of a person. They proposed the use of an accelerometer as a source of noise reference.
High precision is very important in continuous ICU monitoring. However, the ECG signal is noisy and measured in millivolts, which accentuates the need for good filtering and amplifying techniques. This challenge was highlighted and addressed in [149,17].
4.3. Challenges Related to Monitoring Durability
For real-time monitoring, it is important to use energy-efficient devices and communication technologies to allow for long-term monitoring. This challenge was highlighted by many researchers [159,160,279]. Sampling algorithms were used by the authors of [159,160] to help conserving energy. Also, the authors of [279,146] used Bluetooth as a low-energy communication protocol. Furthermore, data dimensionality reduction techniques can be used to reduce data size, thus alleviating its processing, which will support monitoring durability.
4.4. Challenges Related to Size of ECG Signal Data
Real-time screening is usually conducted for a relatively longer period of time compared to traditional screening (e.g., days or even months). As a result, the amount of generated ECG signal data is usually large and sometimes massive. Subsequently, the process of signal analysis and interpretation turns into rather a challenging task. This accentuates the need for automatic analysis and interpretation of signal data for these monitoring setups in order to generate useful notifications for patients as well as health caregivers. Bianchi et al. [154] pointed out that for real-time remote monitoring setups, it is imperative to implement intelligent feature extraction algorithms to select informative time windows only from the signals and, eventually, transmit them to a remote station for interpretation.
4.5. Challenges Related to Electrode/Sensor Type and Design
In addition to challenges related to the size and quality of ECG signal data, some challenges are related to electrode design, the number of leads, and the type of conductor used. For example, Fensli et al. [161] highlighted that the ECG signal recording differs in some ways depending on the type and number of electrodes used. It is, therefore, necessary to further explore the suitability of this recording principle for disease diagnostic purposes. Different diseases require different types of recordings, which should be supported by the selected electrode. Another design challenge is related to the patient’s comfort with sticky electrodes. Concerns around the adverse effect of electrodes on the human body were addressed in [97]. Moreover, Karaoğuz et al. [125] highlighted in their study that 7.3% of participants had minor skin irritations related to the sticky gel electrodes. Alternatively, the authors of [155,156] proposed a chemical formulation appropriate for the dipping of various textile fabrics (e.g., cotton, polyamide, and polyester), making flexible washable electrodes for long-term monitoring compared to gel electrodes, which are disposable and cause skin irritation. These textile washable electrodes also solved the common challenge known in gel electrodes related to the low signal quality when electrodes dry out. Nevertheless, challenges regarding the design of wearable devices require further research.
4.6. Challenges Related to Visualization
Gusev et al. [279] highlighted a few challenges in handling visualization for continuous ECG monitoring. Mainly, the problems were related to handling different refreshing rate requirements via multiple platforms installed on displaying devices with low processing requirements.
Long-term ECG data analysis can be challenging as it tends to oversimplify the visualized information, which results in losing significant components. Therefore, Jarchi et al. [280] proposed a visualization approach using classification for identifying heartbeats using long-term single-channel ECG.
Display adaptation and customization are another challenging issues for the ECG monitoring system. Display customization of data reporting for each stakeholder, such as the doctor, the nurse, the caregiver, and the patient, is included. Each stakeholder requires a different reporting context. Real-time display is also required to be automatically customized according to the visualizing device’s screen size and even the device battery level. These challenges were addressed in [281], in which special dashboard functionalities were integrated with visualization features, such as zoom-in and zoom-out, and filtering.
4.7. Challenges Related to System Integration
Baig et al. [54] highlighted a few system integration challenges that face the existing clinical decision support models concerning scalability and reliability, pointing this out as a future research direction. They suggested exploiting Cloud resources for real-time processing to handle the integration issue. Furthermore, Jovanov et al. [282] proposed the seamless integration of information with sensors and other networks and the use of public resources and standard Internet methods for authentication and secure communication. Additionally, Spanò et al. [283] discussed opportunities for the seamless integration of remote monitoring systems with other smart home systems over an IoT infrastructure. Service-Oriented Architecture (SOA) has also been considered a very promising solution for integrating heterogeneous systems. This is the case for ECG monitoring systems where various technologies, data sources, and devices are used to collect, process, analyze, and visualize data over various interfaces.
4.8. Other Challenges
Other challenges related to ECG monitoring systems that are different from those mentioned earlier include those related to complex computational requirements, energy harvesting, and patient/user resistance to contributing to his/her monitoring using various technologies and sensors. The involvement of mobile devices in continuous ECG monitoring makes them less effective for computational, data-intensive processing. Though the mobile device improves some flexibility to the monitoring process, problems related to battery consumption and the limited processing capability of the device are still not resolved completely.
5. Discussion, Conclusion, and Future Direction
ECG monitoring systems have been studied thoroughly in the literature; however, the multi-dimensional aspects of these systems make it difficult for researchers, medical practitioners, and others to select, among these systems, those that fulfill their monitoring needs, match the context of their use, and support the required disease monitoring requirements.
In this paper, we carried out an extensive review of the literature related to ECG monitoring systems, focusing on different aspects including applicability, the technology used, architecture, lifecycle, classification, and challenges. We presented and discussed an expert-verified classification model. In our experts’ taxonomy, we decomposed ECG monitoring systems into context-aware ECG monitoring systems, technology-aware ECG monitoring systems, ECG monitoring systems based on schemes and frequency, ECG monitoring systems targets and purposes, and futuristic ECG monitoring systems.
Current development in ECG monitoring systems leveraged new technologies, such as deep learning, AI, Big Data and IoT to provide efficient, cost-efficient, fully connected, and powerful monitoring system. Enabling technologies provide huge opportunities for the advancement of ECG monitoring systems. IoT brings in remote, unconstrained connectivity and services that leverage data and facilitate timely, meaningful, and critical decisions for a better lifestyle. Furthermore, Fog processing and cloud processing contribute to an increased opportunity to improve efficiency and fulfill numerous in-demand scalable application services. Furthermore, blockchain technology enables security over a distributed environment for various transactions throughout the different layers of the ECG monitoring system architecture.
We shed light on this work on the ECG monitoring system’s lifecycle, which incorporates various processes that can be classified into primary processes and supporting processes. However, these processes are not distinctly defined in the literature; some overlap and others are better merged. None of the researches addressed the details of the complete lifecycle of an ECG monitoring system. In this paper, to the best of our knowledge, we tried to generalize a complete lifecycle, including all main processes starting from data acquisition, preprocessing, feature extraction, processing and, finally, visualization. We have also defined a set of supporting processes, such as signal selection, encryption, and compression, which are only required by specialized systems.
As a future direction, exploring the field of robotics and healthcare automation has the potential to transform the next generation of ECG monitoring systems and to simplify robotic-assisted surgery procedures, elderly care, and remote and in-hospital continuous patient monitoring. Robotic-assisted surgery should be performed with higher precision, control, and improved vision, paving the way for the revolutionary healthcare of tomorrow. Further future research directions include exploring the use of the fast-growing IoT and smart connected devices for preventive healthcare and supporting the detection of patients’ unusual medical problems or a change in behavioral patterns. Also, personalized monitoring systems should be raised to the next level in terms of being highly customized according to patients’ needs and interactive to allow special configurations and adaptations to users’ requirements for a better quality of life. Finally, another possible research direction is to add more intelligence to the patients’ surroundings, for example, embedding more sensors in the carpet to accurately detect patients’ movements in order to establish behavior patterns and detect any abnormalities, as suggested in [282].
To that end, we endorse that this work, with a detailed discussion on many relevant research work, provides a comprehensive state-of-the-art review of ECG monitoring systems. It can serve as reference for various researchers and stakeholders in the field to compare, understand, and value ECG monitoring system features. It also highlights the main challenges these systems exhibit in terms of adaptability, integration, monitoring quality and durability. Finally, it outlines a future vision of the next-generation ECG monitoring systems for healthcare.
Author Contributions
M.A.S conceived the main conceptual ideas related to taxonomy, architecture, value chain, and proof outline, supervised the study and was in charge of overall direction and planning. M.A.S., H.T.E.K., and H.I. contributed to the design and implementation of all research components, to the analysis of the results, and to the writing of the manuscript. A.N.N. contributed to early stages of design and analysis. All authors contributed to the revision and proofreading of the final version of the manuscript.
Funding
This work is supported by Zayed Health Center at UAE University under Fund code 31R227.
Conflicts of Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- World Health Organization. Cardiovascular Diseases. Available online: www.who.int/health-topics/cardiovascular-diseases/#tab=tab_1. (accessed on 16 March 2020).
- Scutti, S. Nearly Half of US Adults Have Cardiovascular Disease, Study Says. CNN, Cable News Network. 31 January 2019. Available online: www.cnn.com/2019/01/31/health/heart-disease-statistics-report/index.html (accessed on 15 March 2020).
- European Cardiovascular Disease Statistics 2017; The European Heart Network (EHN): Brussels, Belgium, 2017; Available online: http://www.ehnheart.org/cvd-statistics.html (accessed on 15 March 2020).
- Hassan, M.F.U.; Lai, D.; Bu, Y. Characterization of Single Lead Continuous ECG Recording with Various Dry Electrodes. In Proceedings of the 2019 3rd International Conference on Computational Biology and Bioinformatics, Nagoya, Japan, 17–19 October 2019; pp. 76–79. [Google Scholar]
- Preejith, S.P.; Dhinesh, R.; Joseph, J.; Sivaprakasam, M. Wearable ECG platform for continuous cardiac monitoring. In Proceedings of the 38th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Lake Buena Vista, FL, USA, 16–20 August 2016; pp. 623–626. [Google Scholar]
- Bsoul, M.; Minn, H.; Tamil, L. Apnea MedAssist: Real-time sleep apnea monitor using single-lead ECG. IEEE Trans. Inf. Technol. Biomed. 2011, 15, 416–427. [Google Scholar] [CrossRef] [PubMed]
- Azariadi, D.; Tsoutsouras, V.; Xydis, S.; Soudris, D. ECG signal analysis and arrhythmia detection on IoT wearable medical devices. In Proceedings of the 2016 5th International Conference on Modern Circuits and Systems Technologies, MOCAST, Thessaloniki, Greece, 12–14 May 2016. [Google Scholar] [CrossRef]
- Satija, U.; Ramkumar, B.; Manikandan, S.M. Real-time signal quality-aware ECG telemetry system for IoT-based health care monitoring. IEEE Intern. Things J. 2017, 4, 815–823. [Google Scholar] [CrossRef]
- Scrugli, M.A.; Loi, D.; Raffo, L.; Meloni, P. A runtime-adaptive cognitive IoT node for healthcare monitoring. In Proceedings of the ACM International Conference on Computing Frontiers 2019, CF 2019–Proceedings, Alghero, Italy, 30 April–2 May 2019. [Google Scholar] [CrossRef]
- Sanghavi, D.R.; Athawale, S.V.; Professor, A. An IoT Based Low-Cost ECG Monitoring System for Remote Patient. Int. J. Res. Trends Innov. 2018, 3, 70. [Google Scholar]
- Kim, K. Europace Comparing the performance of artificial intelligence and conventional diagnosis criteria for detecting left ventricular hypertrophy using electrocardiography. Europace 2018, 1–8. [Google Scholar] [CrossRef]
- Bansal, M.; Gandhi, B. IoT big data in smart healthcare (ECG monitoring). In Proceedings of the International Conference on Machine Learning, Big Data, Cloud and Parallel Computing: Trends, Prespectives and Prospects, COMITCon, Faridabad, India, 14–16 February 2019. [Google Scholar] [CrossRef]
- Taher, N.C.; Mallat, I.; Agoulmine, N.; El-Mawass, N. An IoT-Cloud based solution for real-time and batch processing of big data: Application in healthcare. In Proceedings of the 2019 3rd International Conference on Bio-engineering for Smart Technologies BioSMART, Paris, France, 22–26 April 2019; pp. 1–8. [Google Scholar] [CrossRef]
- Chamadiya, B.; Mankodiya, K.; Wagner, M.; Hofmann, U.G. Textile-based, contactless ECG monitoring for non-ICU clinical settings. J. Ambient Intell. Humaniz. Comput. 2013, 4. [Google Scholar] [CrossRef]
- Zagan, I.; Gaitan, V.G.; Iuga, N.; Brezulianu, A. M-GreenCARDIO embedded system designed for out-of-hospital cardiac patients. In Proceedings of the 2018 14th International Conference on Development and Application Systems, DAS, Suceava, Romania, 24–26 May 2018. [Google Scholar] [CrossRef]
- Navaz, A.N.; Mohammed, E.; Serhani, M.A.; Zaki, N. The use of data mining techniques to predict mortality and length of stay in an ICU. In Proceedings of the 2016 12th International Conference on Innovations in Information Technology IIT, Al-Ain, United Arab Emirates, 28–30 November 2016. [Google Scholar] [CrossRef]
- Ahouandjinou, A.S.R.M.; Assogba, K.; Motamed, C. Smart and pervasive ICU based-IoT for improving intensive health care. In Proceedings of the 2016 International Conference on Bio-Engineering for Smart Technologies BioSMART, Dubai, United Arab Emirates, 4–7 December 2016. [Google Scholar] [CrossRef]
- Steinhubl, S.R.; Waalen, J.; Edwards, A.M.; Ariniello, L.M.; Mehta, R.R.; Ebner, G.S.; Carter, C.; Baca-Motes, K.; Felicione, E.; Sarich, T.; et al. Effect of a home-Based wearable continuous ECG monitoring patch on detection of undiagnosed atrial fibrillation the mSToPS randomized clinical trial. JAMA J. Am. Med. Assoc. 2018, 320, 146–155. [Google Scholar] [CrossRef]
- Benhamida, A.; Zouaoui, A.; Szócska, G.; Karóczkai, K.; Slimani, G.; Kozlovszky, M. Problems in archiving long-term continuous ECG data - A review. In Proceedings of the SAMI 2019 - IEEE 17th World Symposium on Applied Machine Intelligence and Informatics, Herlany, Slovakia, 24–26 January 2019. [Google Scholar] [CrossRef]
- Shakthi Murugan, K.H.; Sriram, T.J.; Jerold, P.M.; Peeran, A.S.A.; Abisheik, P. Wearable ECG electrodes for detection of heart rate and arrhythmia classification. In Proceedings of the 2019 3rd IEEE International Conference on Electrical, Computer and Communication Technologies ICECCT, Coimbatore, India, 20–22 February 2019. [Google Scholar] [CrossRef]
- Petrenas, A.; Marozas, V.; Jaruševičius, G.; Sörnmo, L. A modified Lewis ECG lead system for ambulatory monitoring of atrial arrhythmias. J. Electrocardiol. 2015, 48, 157–163. [Google Scholar] [CrossRef]
- Fung, E.; Järvelin, M.R.; Doshi, R.N.; Shinbane, J.S.; Carlson, S.K.; Grazette, L.P.; Chang, P.M.; Sangha, R.S.; Huikuri, H.V.; Peters, N.S. Electrocardiographic patch devices and contemporary wireless cardiac monitoring. Front. Physiol. 2015, 6, 149. [Google Scholar] [CrossRef]
- Mamaghanian, H.; Khaled, N.; Atienza, D.; Vandergheynst, P. Compressed sensing for real-time energy-efficient ECG compression on wireless body sensor nodes. IEEE Trans. Biomed. Eng. 2011, 58, 2456–2466. [Google Scholar] [CrossRef]
- Guan, K.; Shao, M.; Wu, S. A remote health monitoring system for the elderly based on smart home gateway. J. Healthc. Eng. 2017, 2017. [Google Scholar] [CrossRef]
- Akrivopoulos, O.; Antoniou, A.; Amaxilatis, D.; Chatzigiannakis, I. Design and evaluation of a person-centric heart monitoring system over fog computing infrastructure. In Proceedings of the HumanSys 2017 - 1st International Workshop on Human-Centered Sensing, Networking, and Systems, Part of SenSys, Delft, The Netherlands, 6–8 November 2017; pp. 25–30. [Google Scholar] [CrossRef]
- Tuli, S.; Basumatary, N.; Gill, S.S.; Kahani, M.; Arya, R.C.; Wander, G.S.; Buyya, R. HealthFog: An ensemble deep learning based Smart Healthcare System for Automatic Diagnosis of Heart Diseases in integrated IoT and fog computing environments. Futur. Gener. Comput. Syst. 2020, 104, 187–200. [Google Scholar] [CrossRef]
- Neyja, M.; Mumtaz, S.; Huq, K.M.S.; Busari, S.A.; Rodriguez, J.; Zhou, Z. An IoT-based e-health monitoring system using ECG signal. In Proceedings of the GLOBECOM 2017 IEEE Global Communications Conference, Singapore, 4–8 December 2017. [Google Scholar] [CrossRef]
- Akrivopoulos, O.; Amaxilatis, D.; Mavrommati, I.; Chatzigiannakis, I. Utilising fog computing for developing a person-centric heart monitoring system. J. Ambient Intell. Smart Environ. 2019, 11, 237–259. [Google Scholar] [CrossRef]
- Wu, W.; Pirbhulal, S.; Sangaiah, A.K.; Mukhopadhyay, S.C.; Li, G. Optimization of signal quality over comfortability of textile electrodes for ECG monitoring in fog computing based medical applications. Futur. Gener. Comput. Syst. 2018, 86, 515–526. [Google Scholar] [CrossRef]
- Smoleń, M.; Kańtoch, E.; Augustyniak, P.; Kowalski, P. Wearable patient home monitoring based on ECG and ACC sensors. IFMBE Proc. 2011, 37, 941–944. [Google Scholar] [CrossRef]
- Yusof, M.A.; Hau, Y.W. Mini home-based vital sign monitor with android mobile application (myVitalGear). In Proceedings of the 2018 IEEE EMBS Conference on Biomedical Engineering and Science IECBES, Sarawak, Malaysia, 3–6 December 2018. [Google Scholar] [CrossRef]
- Hsieh, S.-T.; Lin, C.-L. Intelligent healthcare system using an arduino microcontroller and an android-based smartphone. BioMed Res. 2017, 28, 9940–9946. [Google Scholar]
- Lee, Y.D.; Chung, W.Y. Wireless sensor network based wearable smart shirt for ubiquitous health and activity monitoring. Sens. Actuators B Chem. 2009, 140, 390–395. [Google Scholar] [CrossRef]
- Pirozzi, M.; Pietroni, F.; Casaccia, S.; Scalise, L.; Revel, G.M. Cardiac activity classification using an E-health app for a wearable device. In Proceedings of the 2018 IEEE International Symposium on Medical Measurements and Applications MeMeA, Rome, Italy, 11–13 June 2018. [Google Scholar] [CrossRef]
- Schneider, J.; Schroth, M.; Ottenbacher, J.; Stork, W. A novel wearable sensor device for continuous monitoring of cardiac activity during sleep. In Proceedings of the 2018 IEEE Sensors Applications Symposium SAS, Seoul, Korea, 12–14 March 2018. [Google Scholar] [CrossRef]
- Bosco, G.; De Marzi, E.; Michieli, P.; Omar, H.R.; Camporesi, E.M.; Padulo, J.; Paoli, A.; Mangar, D.; Schiavon, M. 12-lead Holter monitoring in diving and water sports: A preliminary investigation. Diving Hyperb. Med. 2014, 44, 202–207. [Google Scholar]
- Raković, P.; Lutovac, B. A cloud computing architecture with wireless body area network for professional athletes health monitoring in sports organizations—Case study of Montenegro. In Proceedings of the 2015 4th Mediterranean Conference on Embedded Computing (MECO), Budva, Montenegro, 14–18 June 2015; pp. 387–390. [Google Scholar]
- Octaviani, V.; Kurniawan, A.; Suprapto, Y.K.; Zaini, A. Alerting system for sport activity based on ECG signals using proportional integral derivative. In Proceedings of the 2017 4th International Conference on Electrical Engineering, Computer Science and Informatics (EECSI), Yogyakarta, Indonesia, 19–21 September 2017; pp. 1–6. [Google Scholar]
- Carney, R.M.; Freedland, K.E.; Steinmeyer, B.C.; Rubin, E.H.; Stein, P.K.; Rich, M.W. Nighttime heart rate predicts response to depression treatment in patients with coronary heart disease. J. Affect. Disord. 2016, 200, 165–171. [Google Scholar] [CrossRef]
- Valenza, G.; Nardelli, M.; Lanata, A.; Gentili, C.; Bertschy, G.; Kosel, M.; Scilingo, E.P. Predicting mood changes in bipolar disorder through heartbeat nonlinear dynamics. IEEE J. Biomed. Health Inform. 2016, 20, 1034–1043. [Google Scholar] [CrossRef]
- Migliorini, M.; Mariani, S.; Bertschy, G.; Kosel, M.; Bianchi, A.M. Can home-monitoring of sleep predict depressive episodes in bipolar patients? In Proceedings of the 2015 37th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBS), Milano, Italy, 25–29 August 2015; pp. 2215–2218. [Google Scholar]
- Gierałtowski, J.; Ciuchciński, K.; Grzegorczyk, I.; Kośna, K.; Soliński, M.; Podziemski, P. RS slope detection algorithm for extraction of heart rate from noisy, multimodal recordings. Physiol. Meas. 2015, 36, 1743. [Google Scholar] [CrossRef]
- Ghosh, S.; Feng, M.; Nguyen, H.; Li, J. Predicting heart beats using co-occurring constrained sequential patterns. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 265–268. [Google Scholar]
- Yang, B.; Teo, S.K.; Hoeben, B.; Monterola, C.; Su, Y. Robust identification of heartbeats with blood pressure signals and noise detection. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 565–568. [Google Scholar]
- Gierałtowski, J.J.; Ciuchciński, K.; Grzegorczyk, I.; Kośna, K.; Soliński, M.; Podziemski, P. Heart rate variability discovery: Algorithm for detection of heart rate from noisy, multimodal recordings. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 253–256. [Google Scholar]
- Sadr, N.; Jayawardhana, M.; Pham, T.T.; Tang, R.; Balaei, A.T.; de Chazal, P. A low-complexity algorithm for detection of atrial fibrillation using an ECG. Physiol. Meas. 2018, 39, 64003. [Google Scholar] [CrossRef] [PubMed]
- Satija, U.; Ramkumar, B.; Manikandan, M.S. Automated ECG noise detection and classification system for unsupervised healthcare monitoring. IEEE J. Biomed. Health Inform. 2018, 22, 722–732. [Google Scholar] [CrossRef] [PubMed]
- Bhattacherjee, P.; Ganguly, D.; Chatterjee, K. A review of Steganography techniques suitable for ECG signal. In Proceedings of the International Conference on Emerging Technologies for Sustainable Development (ICETSD ’19), Kolkata, India, 5–6 March 2019; pp. 1–7. [Google Scholar]
- Mora, F.A.; Passariello, G.; Carrault, G.; Le Pichon, J.-P. Intelligent patient monitoring and management systems: A review. IEEE Eng. Med. Biol. Mag. 1993, 12, 23–33. [Google Scholar] [CrossRef]
- Kundu, M.; Nasipuri, M.; Basu, D.K. Knowledge-based ECG interpretation: A critical review. Pattern Recognit. 2000, 33, 351–373. [Google Scholar] [CrossRef]
- Sohn, H.; Farrar, C.R.; Hemez, F.M.; Shunk, D.D.; Stinemates, D.W.; Nadler, B.R.; Czarnecki, J.J. A Review of Structural Health Monitoring Literature: 1996–2001; Los Alamos National Laboratory: Los Alamos, NM USA, 2003; pp. 1–7.
- Windmiller, J.R.; Wang, J. Wearable electrochemical sensors and biosensors: A review. Electroanalysis 2013, 25. [Google Scholar] [CrossRef]
- Baig, M.M.; Gholamhosseini, H.; Connolly, M.J. A comprehensive survey of wearable and wireless ECG monitoring systems for older adults. Med. Biol. Eng. Comput. 2013, 51, 485–495. [Google Scholar] [CrossRef]
- Baig, M.M.; GholamHosseini, H.; Moqeem, A.A.; Mirza, F.; Lindén, M. A systematic review of wearable patient monitoring systems–current challenges and opportunities for clinical adoption. J. Med. Syst. 2017, 41, 115. [Google Scholar] [CrossRef]
- Banaee, H.; Ahmed, M.; Loutfi, A. Data mining for wearable sensors in health monitoring systems: A review of recent trends and challenges. Sensors 2013, 13, 17472–17500. [Google Scholar] [CrossRef]
- Marston, H.R.; Hadley, R.; Banks, D.; Duro, M.D.C.M. Mobile self-monitoring ECG devices to diagnose arrhythmia that coincide with palpitations: A scoping review. Healthcare 2019, 7, 96. [Google Scholar] [CrossRef]
- Sposato, L.A.; Cipriano, L.E.; Saposnik, G.; Vargas, E.R.; Riccio, P.M.; Hachinski, V. Diagnosis of atrial fibrillation after stroke and transient ischaemic attack: A systematic review and meta-analysis. Lancet Neurol. 2015, 14, 377–387. [Google Scholar] [CrossRef]
- Tejedor, J.; García, C.A.; Márquez, D.G.; Raya, R.; Otero, A. Multiple physiological signals fusion techniques for improving heartbeat detection: A review. Sensors 2019, 19. [Google Scholar] [CrossRef] [PubMed]
- Egger, M.; Ley, M.; Hanke, S. Emotion recognition from physiological signal analysis: A review. Electron. Notes Theor. Comput. Sci. 2019, 343, 35–55. [Google Scholar] [CrossRef]
- Sabarimalai Sur, M.; Dandapat, S. Wavelet-based electrocardiogram signal compression methods and their performances: A prospective review. Biomed. Signal Process. Control 2014, 14, 73–107. [Google Scholar] [CrossRef]
- Jeong, D.-U.; Kim, S.-J. Development of a technique for cancelling motion artifact in ambulatory ECG monitoring system. In Proceedings of the 2008 Third International Conference on Convergence and Hybrid Information Technology, Busan, Korea, 11–13 November 2008; Volume 1, pp. 954–961. [Google Scholar]
- De Cooman, T.; Goovaerts, G.; Varon, C.; Widjaja, D.; Van Huffel, S. Heart beat detection in multimodal data using signal recognition and beat location estimation. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 257–260. [Google Scholar]
- Li, Z.; Derksen, H.; Gryak, J.; Ghanbari, H.; Gunaratne, P.; Najarian, K. A novel atrial fibrillation prediction algorithm applicable to recordings from portable devices. In Proceedings of the 2018 40th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Honolulu, HA, USA, 18–21 July 2018; pp. 4034–4037. [Google Scholar] [CrossRef]
- Ding, Q.; Bai, Y.; Erol, Y.B.; Salas-Boni, R.; Zhang, X.; Li, L.; Hu, X. Multimodal information fusion for robust heart beat detection. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 261–264. [Google Scholar]
- Vollmer, M. Robust detection of heart beats using dynamic thresholds and moving windows. In Proceedings of the Computing in Cardiology 2014, Cambridge, MA, USA, 7–10 September 2014; pp. 569–572. [Google Scholar]
- Yusuf, S.A.A.; Hidayat, R. MFCC feature extraction and KNN classification in ECG signals. In Proceedings of the 2019 6th International Conference on Information Technology, Computer and Electrical Engineering (ICITACEE), Semarang, Indonesia, 26–27 September 2019; pp. 1–5. [Google Scholar]
- Kora, P.; Kumari, C.U.; Swaraja, K.; Meenakshi, K. Atrial Fibrillation detection using Discrete Wavelet Transform. In Proceedings of the 2019 3rd IEEE International Conference on Electrical, Computer and Communication Technologies (ICECCT), Coimbatore, India, 20–22 February 2019; pp. 1–3. [Google Scholar] [CrossRef]
- Vernekar, S.; Vijaysenan, D.; Ranjan, R. A novel approach for Robust Detection of Heart Beats in Multimodal Data using neural networks and boosted trees. In Proceedings of the 2016 Computing in Cardiology Conference (CinC), Vancouver, BC, Canada, 11–14 September 2016; pp. 1137–1140. [Google Scholar]
- Zhang, H.; Wang, Z.; Dong, K.; Ng, S.H.; Lin, Z. Towards precise tracking of electric-mechanical cardiac time intervals through joint ECG and BCG sensing and signal processing. In Proceedings of the 2017 39th Annual International Conference of the IEEE Engineering in Medicine and Biology Society (EMBC), Seogwipo, Korea, 11–15 July 2017; pp. 751–754. [Google Scholar] [CrossRef]
- De Cooman, T.; Goovaerts, G.; Varon, C.; Widjaja, D.; Willemen, T.; Van Huffel, S. Heart beat detection in multimodal data using automatic relevant signal detection. Physiol. Meas. 2015, 36, 1691. [Google Scholar] [CrossRef]
- Xia, H.; Asif, I.; Zhao, X. Cloud-ECG for real time ECG monitoring and analysis. Comput. Methods Programs Biomed. 2013, 110, 253–259. [Google Scholar] [CrossRef]
- Page, A.; Kocabas, O.; Soyata, T.; Aktas, M.; Couderc, J.P. Cloud-based privacy-preserving remote ECG monitoring and surveillance. Ann. Noninvasive Electrocardiol. 2015, 20, 328–337. [Google Scholar] [CrossRef]
- Kim, H.; Kim, S.; Van Helleputte, N.; Artes, A.; Konijnenburg, M.; Huisken, J.; Van Hoof, C.; Yazicioglu, R.F. A configurable and low-power mixed signal SoC for portable ECG monitoring applications. IEEE Trans. Biomed. Circ. Syst. 2014, 8, 257–267. [Google Scholar] [CrossRef]
- Martín-Yebra, A.; Landreani, F.; Casellato, C.; Pavan, E.; Frigo, C.; Migeotte, P.; Caiani, E.G. Studying heart rate variability from ballistocardiography acquired by force platform: Comparison with conventional ECG. In Proceedings of the 2015 Computing in Cardiology Conference (CinC), Nice, France, 6–9 September 2015; pp. 929–932. [Google Scholar] [CrossRef]
- Mohaar, G.; Maleque, M.; Singh, R. Framework for stochastic modelling of multi-dimensional real-time sensor data. In Proceedings of the 2015 10th International Conference on Intelligent Systems and Knowledge Engineering (ISKE), Taipei, Taiwan, 24–27 November 2015; pp. 244–251. [Google Scholar]
- Serhani, M.A.; Benharref, A.; Nujum, A.R. Intelligent remote health monitoring using evident-based DSS for automated assistance. In Proceedings of the 2014 36th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, Chicago, IL, USA, 26–30 August 2014; pp. 2674–2677. [Google Scholar]
- Nawal, M.; Purohit, G.N. ECG based human authentication: A review. Int. J. Emerg. Eng. Res. Technol. 2014, 2, 178–185. [Google Scholar]
- Gusev, M.; Stojmenski, A.; Guseva, A. ECGalert: A Heart Attack Alerting System. In Proceedings of the 9th International Conference, Skopje, Macedonia, 18–23 September 2017. [Google Scholar]
- Němcová, A.; Smíšek, R.; Maršánová, L.; Smital, L.; Vítek, M. A comparative analysis of methods for evaluation of ECG signal quality after compression. BioMed Res. Int. 2018, 2018. [Google Scholar] [CrossRef]
- Villegas, A.; McEneaney, D.; Escalona, O. Arm-ECG wireless sensor system for wearable long-term surveillance of heart arrhythmias. Electronics 2019, 8, 1300. [Google Scholar] [CrossRef]
- Llanas, A.; Guillén, J.; Cardiel, E.; Hernández, P.-R. Development of an interactive system for the visualization of a cardiac model activated by the R-Wave of ECG in a 3D CAVE. In Proceedings of the 2018 15th International Conference on Electrical Engineering, Computing Science and Automatic Control (CCE), Mexico City, Mexico, 5–7 September 2018; pp. 1–5. [Google Scholar]
- Motalova, L.; Krejcar, O.; Polak, T.; Janckulik, D.; Cernohorsky, J. ECG data visualisation in web application using MS Silverlight. In Proceedings of the 2011 1st Middle East Conference on Biomedical Engineering, Sharjah, United Arab Emirates, 21–24 February 2011; pp. 347–350. [Google Scholar] [CrossRef]
- Oresko, J.J.; Jin, Z.; Cheng, J.; Huang, S.; Sun, Y.; Duschl, H.; Cheng, A.C. A wearable smartphone-based platform for real-time cardiovascular disease detection via electrocardiogram processing. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 734–740. [Google Scholar] [CrossRef] [PubMed]
- Sörnmo, L.; Laguna, P. Electrocardiogram (ECG) signal processing. Wiley Encycl. Biomed. Eng. 2006. [Google Scholar] [CrossRef]
- Ding, H.; Sun, H.; Hou, K. Abnormal ECG signal detection based on compressed sampling in Wearable ECG sensor. In Proceedings of the 2011 International Conference on Wireless Communications and Signal Processing (WCSP), Nanjing, China, 9–11 November 2011; pp. 1–5. [Google Scholar]
- Shankar, M.G.; Babu, C.G. An exploration of ECG signal feature selection and classification using machine learning techniques. Int. J. Innovative Technol. Exploring Eng. Regul. Issue 2020, 9, 797–804. [Google Scholar] [CrossRef]
- Karnewar, J.S.; Shandilya, D.V.K.; Tambakhe, M.D. A study on ECG signal analysis and ECG databases. Int. J. Res. Advent Technol. 2019, 7, 188–195. [Google Scholar] [CrossRef]
- Moses, D. A survey of data mining algorithms used in cardiovascular disease diagnosis from multi-lead ECG data. Kuwait J. Sci. 2015, 42, 206–235. [Google Scholar]
- Ghodake, S.; Ghumbre, S.; Deshmukh, S. Electrocardiogram Signal Denoising Using Hybrid Filtering for Cardiovascular Diseases Prediction. In Techno-Societal 2018; Springer: Berlin, Germany, 2020; pp. 271–278. [Google Scholar]
- Padmavathi, C.; Veenadevi, S.V. An automated detection of CAD using the method of signal decomposition and non linear entropy using heart signals. Int. J. Image Graph. Signal Process. 2019, 11, 30–39. [Google Scholar] [CrossRef]
- Tychkov, A.; Alimuradov, A.; Churakov, P. The emperical mode decomposition for ECG signal preprocessing. In Proceedings of the 2019 3rd School on Dynamics of Complex Networks and their Application in Intellectual Robotics, DCNAIR, Innopolis, Russia, 9–11 December 2019. [Google Scholar] [CrossRef]
- Wang, Y. An automated ECG Signal Quality Assessment Method with Supervised Learning Algorithm; Delft University of Technology: Delft, The Netherlands, 2018. [Google Scholar]
- Deriche, M.; Aljabri, S.; Al-Akhras, M.; Siddiqui, M.; Deriche, N. An optimal set of features for multi-class heart beat abnormality classification. In Proceedings of the 2019 16th International Multi-Conference on Systems, Signals & Devices (SSD), Istanbul, Turkey, 21–24 March 2019; pp. 418–422. [Google Scholar] [CrossRef]
- Kwon, S.; Lee, D.; Kim, J.; Lee, Y.; Kang, S.; Seo, S.; Park, K. Sinabro: A smartphone-integrated opportunistic electrocardiogram monitoring system. Sensors 2016, 16, 361. [Google Scholar] [CrossRef]
- Alfaouri, M.; Daqrouq, K. ECG signal denoising by wavelet transform thresholding. Am. J. Appl. Sci. 2008, 5, 276–281. [Google Scholar] [CrossRef]
- Valupadasu, R.; Chunduri, B.R.R. Automatic classification of cardiac disorders using MLP algorithm. In Proceedings of the 2019 Prognostics and System Health Management Conference PHM-Paris, Paris, France, 2–5 May 2019. [Google Scholar] [CrossRef]
- El-Saadawy, H.; Tantawi, M.; Shedeed, H.A.; Tolba, M.F. Electrocardiogram (ECG) classification based on dynamic beats segmentation. ACM Int. Conf. Proc. Ser. 2016, 09-11-May-, 75–80. [Google Scholar] [CrossRef]
- Zhang, J.; Wang, L.; Zhang, W.; Yao, J. A signal quality assessment method for electrocardiography acquired by mobile device. In Proceedings of the 2018 IEEE International Conference on Bioinformatics and Biomedicine BIBM, Madrid, Spain, 3–6 December 2018. [Google Scholar] [CrossRef]
- Mirbagheri, M.; Hakimi, N.; Ebrahimzadeh, E.; Setarehdan, S.K. Quality analysis of heart rate derived from functional near-infrared spectroscopy in stress assessment. Inform. Med. Unlocked 2019, 18, 100286. [Google Scholar] [CrossRef]
- Satija, U.; Ramkumar, B.; Manikandan, M.S. A simple method for detection and classification of ECG noises for wearable ECG monitoring devices. In Proceedings of the 2nd International Conference on Signal Processing and Integrated Networks SPIN, Noida, India, 19–20 February 2015. [Google Scholar] [CrossRef]
- Lamba, P.; Rawal, K. A survey of algorithms for feature extraction and feature classification methods. In Proceedings of the 2019 International Conference on Automation, Computational and Technology Management (ICACTM), London, UK, 24–26 April 2019; pp. 338–341. [Google Scholar] [CrossRef]
- Butun, E.; Yildirim, O.; Talo, M.; Tan, R.-S.; Acharya, U.R. 1D-CADCapsNet: One dimensional deep capsule networks for coronary artery disease detection using ECG signals. Phys. Medica 2020, 70, 39–48. [Google Scholar] [CrossRef] [PubMed]
- ŞEN, S.Y.; ÖZKURT, N. ECG arrhythmia classification by using convolutional neural network and spectrogram. In Proceedings of the 2019 Innovations in Intelligent Systems and Applications Conference (ASYU), Izmir, Turkey, 31 October–2 November 2019; pp. 1–6. [Google Scholar]
- Shashikumar, S.P.; Shah, A.J.; Li, Q.; Clifford, G.D.; Nemati, S. A deep learning approach to monitoring and detecting atrial fibrillation using wearable technology. In Proceedings of the 2017 IEEE EMBS International Conference on Biomedical and Health Informatics BHI, Orlando, FL, USA, 16–19 February 2017. [Google Scholar] [CrossRef]
- Uddin, M.Z. A wearable sensor-based activity prediction system to facilitate edge computing in smart healthcare system. J. Parallel Distrib. Comput. 2019, 123, 46–53. [Google Scholar] [CrossRef]
- Carnevale, L.; Celesti, A.; Fazio, M.; Villari, M. A Big Data Analytics Approach for the Development of Advanced Cardiology Applications. Information 2020, 11, 60. [Google Scholar] [CrossRef]
- Krejcar, O.; Janckulik, D.; Motalova, L.; Musil, K.; Penhaker, M. Real time measurement and visualization of ECG on mobile monitoring stations of biotelemetric system. In Advances in Intelligent Information and Database Systems; Springer: Berlin, Germany, 2010; pp. 67–78. [Google Scholar]
- Medical Expo, the Online Medical Device Exhibition. Available online: https://www.medicalexpo.com/medical-manufacturer/electrocardiography-software-16421.html (accessed on 10 February 2020).
- Morak, J.; Kumpusch, H.; Hayn, D.; Leitner, M.; Scherr, D.; Fruhwald, F.M.; Schreier, G. Near field communication-based telemonitoring with integrated ECG recordings. Appl. Clin. Inform. 2011, 2, 481–498. [Google Scholar] [CrossRef]
- Venkatesan, C.; Karthigaikumar, P.; Satheeskumaran, S. Mobile cloud computing for ECG telemonitoring and real-time coronary heart disease risk detection. Biomed. Signal Process. Control 2018, 44, 138–145. [Google Scholar] [CrossRef]
- Wang, X.; Gui, Q.; Liu, B.; Jin, Z.; Chen, Y. Enabling smart personalized healthcare: A hybrid mobile-cloud approach for ECG telemonitoring. IEEE J. Biomed. Health Inform. 2014, 18, 739–745. [Google Scholar] [CrossRef]
- Benini, A.; Donati, M.; Iacopetti, F.; Fanucci, L. User-friendly single-lead ECG device for home telemonitoring applications. In Proceedings of the International Symposium on Medical Information and Communication Technology ISMICT, Firenze, Italy, 2–4 April 2014. [Google Scholar] [CrossRef]
- Al Hemairy, M.; Serhani, M.; Amin, S.; Alahmad, M. A Comprehensive Framework for Elderly Healthcare Monitoring in Smart Environment; Springer: Berlin/Heidelberg, Germany, 2018; pp. 113–140. [Google Scholar]
- Wang, Y.H.; Chung, C.G.; Lin, C.C.; Lin, C.M. The study of the electrocardiography monitoring for the elderly based on smart clothes. In Proceedings of the 8th International Conference on Information Science and Technology ICIST, Cordoba, Spain, 30 June–6 July 2018. [Google Scholar] [CrossRef]
- Mena, L.J.; Félix, V.G.; Ochoa, A.; Ostos, R.; González, E.; Aspuru, J.; Velarde, P.; Maestre, G.E. Mobile personal health monitoring for automated classification of electrocardiogram signals in elderly. Comput. Math. Methods Med. 2018, 2018, 9128054. [Google Scholar] [CrossRef]
- Drew, B.J.; Califf, R.M.; Funk, M.; Kaufman, E.S.; Krucoff, M.W.; Laks, M.M.; Macfarlane, P.W.; Sommargren, C.; Swiryn, S.; Van Hare, G.F. Practice standards for electrocardiographic monitoring in hospital settings: An American Heart Association scientific statement from the councils on cardiovascular nursing, clinical cardiology, and cardiovascular disease in the young. Circulation 2004, 110, 2721–2746. [Google Scholar] [CrossRef]
- Thorén, A.; Rawshani, A.; Herlitz, J.; Engdahl, J.; Kahan, T.; Djärv, T. ECG monitoring in in-hospital cardiac arrest (IHCA). Resuscitation 2019, 142, e13. [Google Scholar] [CrossRef]
- Mahdy, L.N.; Ezzat, K.A.; Tan, Q. Smart ECG Holter monitoring system using smartphone. In Proceedings of the 2018 IEEE International Conference on Internet of Things and Intelligence System IOTAIS, Bali, Indonesia, 1–3 November 2018. [Google Scholar] [CrossRef]
- Grond, M.; Jauss, M.; Hamann, G.; Stark, E.; Veltkamp, R.; Nabavi, D.; Horn, M.; Weimar, C.; Köhrmann, M.; Wachter, R.; et al. Improved detection of silent atrial fibrillation using 72-hour holter ecg in patients with ischemic stroke: A prospective multicenter cohort study. Stroke 2013, 44, 3357–3364. [Google Scholar] [CrossRef]
- Barrett, P.M.; Komatireddy, R.; Haaser, S.; Topol, S.; Sheard, J.; Encinas, J.; Fought, A.J.; Topol, E.J. Comparison of 24-hour Holter monitoring with 14-day novel adhesive patch electrocardiographic monitoring. Am. J. Med. 2014, 127, 95.e11–95.e17. [Google Scholar] [CrossRef] [PubMed]
- Weber-Krüger, M.; Gelbrich, G.; Stahrenberg, R.; Liman, J.; Kermer, P.; Hamann, G.F.; Seegers, J.; Gröschel, K.; Wachter, R. Finding atrial fibrillation in stroke patients: Randomized evaluation of enhanced and prolonged Holter monitoring—Find-AFRANDOMISED—Rationale and design. Am. Heart J. 2014, 168, 438–445. [Google Scholar] [CrossRef] [PubMed]
- Steinberg, J.S.; Varma, N.; Cygankiewicz, I.; Aziz, P.; Balsam Pawełand Baranchuk, A.; Cantillon, D.J.; Dilaveris, P.; Dubner, S.J.; El-Sherif, N.; Krol, J.; et al. 2017 ISHNE-HRS expert consensus statement on ambulatory ECG and external cardiac monitoring/telemetry. Heart Rhythm 2017, 14, e55–e96. [Google Scholar] [CrossRef] [PubMed]
- Jebin, S.R.; Mohamedbeemubeen, N. Real time physiological status monitorinig through telemetry system for on-spot-accident patients using IoT. Int. J. Trend Sci. Res. Dev. 2019, 3, 1580–1583. [Google Scholar] [CrossRef]
- Yama, Y.; Ueno, A.; Uchikawa, Y. Development of a wireless capacitive sensor for ambulatory ECG monitoring over clothes. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology, Lyon, France, 23–26 August 2007; pp. 5727–5730. [Google Scholar] [CrossRef]
- Karaoğuz, M.R.; Yurtseven, E.; Aslan, G.; Deliormanlı, B.G.; Adıgüzel, Ö.; Gönen, M.; Li, K.M.; Yılmaz, E.N. The quality of ECG data acquisition, and diagnostic performance of a novel adhesive patch for ambulatory cardiac rhythm monitoring in arrhythmia detection. J. Electrocardiol. 2019, 54, 28–35. [Google Scholar] [CrossRef]
- Rachim, V.P.; Chung, W.Y. Wearable noncontact armband for mobile ECG monitoring system. IEEE Trans. Biomed. Circ. Syst. 2016, 10, 1112–1118. [Google Scholar] [CrossRef]
- Wang, Y.; Doleschel, S.; Wunderlich, R.; Heinen, S. A wearable wireless ECG monitoring system With dynamic transmission power control for long-term homecare. J. Med. Syst. 2015, 39. [Google Scholar] [CrossRef]
- Steinberg, C.; Sanchez, M.; Philippon, F.; O’Hara, G.; Molin, F.; Sarrazin, J.; Nault, I.; Blier, L.; Roy, K.; Plourde, B.; et al. A novel form of wearable ecg sensors for continuous ambulatory rhythm monitoring: Proof of concept and assessment of signal quality. Can. J. Cardiol. 2018, 34, S24–S25. [Google Scholar] [CrossRef][Green Version]
- Bansal, A.; Kumar, S.; Bajpai, A.; Tiwari, V.N.; Nayak, M.; Venkatesan, S.; Narayanan, R. Remote health monitoring system for detecting cardiac disorders. IET Syst. Biol. 2015, 9, 309–314. [Google Scholar] [CrossRef]
- Tewary, S.; Chakraborty, S.; Majumdar, J.; Majumder, R.; Kundu, D.; Ghosh, S.; Das Gupta, S. A novel approach towards designing a wearable Smart Health Monitoring System measuring the vital parameters and emergency situations in real-time and providing the necessary medical care through telemedicine. In Proceedings of the 2016 IEEE Students’ Conference on Electrical, Electronics and Computer Science, SCEECS, Bhopal, India, 5–6 March 2016; pp. 1–8. [Google Scholar]
- Sarma Dhulipala, V.R.; Kanagachidambaresan, G.R. Cardiac care assistance using self configured sensor network—A remote patient monitoring system. J. Inst. Eng. Ser. B 2014, 95, 101–106. [Google Scholar] [CrossRef]
- Jovanov, E.; Raskovic, D.; Price, J.; Chapman, J.; Moore, A.; Krishnamurthy, A. Patient monitoring using personal area networks of wireless intelligent sensors. Biomed. Sci. Instrum. 2001, 37, 373–378. [Google Scholar] [PubMed]
- Polania, L.F.; Carrillo, R.E.; Blanco-Velasco, M.; Barner, K.E. Exploiting prior knowledge in compressed sensing wireless ECG systems. IEEE J. Biomed. Heath Inform. 2015, 19, 508–519. [Google Scholar] [CrossRef] [PubMed]
- Craven, D.; McGinley, B.; Kilmartin, L.; Glavin, M.; Jones, E. Energy-efficient Compressed Sensing for ambulatory ECG monitoring. Comput. Biol. Med. 2016, 71, 1–13. [Google Scholar] [CrossRef]
- Kanoun, K.; Mamaghanian, H.; Khaled, N.; Atienza, D. A real-time compressed sensing-based personal electrocardiogram monitoring system. In Proceedings of the 2011 Design, Automation and Test in Europe, Grenoble, France, 14–18 March 2011. [Google Scholar] [CrossRef]
- Rahman, A.; Rahman, T.; Ghani, N.H.; Hossain, S.; Uddin, J. IoT Based patient monitoring system using ECG sensor. In Proceedings of the 1st International Conference on Robotics, Electrical and Signal Processing Techniques ICREST, Dhaka, Bangladesh, 10–12 January 2019; pp. 378–382. [Google Scholar] [CrossRef]
- Singh, P.; Jasuja, A. IoT based low-cost distant patient ECG monitoring system. In Proceedings of the IEEE International Conference on Computing, Communication and Automation ICCCA, Greater Noida, India, 5–6 May 2017; pp. 1330–1334. [Google Scholar] [CrossRef]
- Sobya, D.; Muruganandham, S.K.; Nallusamy, S.; Chakraborty, P.S. Wireless ECG monitoring system using IoT based signal conditioning module for real time signal acquisition. Indian J. Public Health Res. Dev. 2018, 9, 294–299. [Google Scholar] [CrossRef]
- Jara, A.J.; Zamora-Izquierdo, M.A.; Skarmeta, A.F. Interconnection framework for mHealth and remote monitoring based on the internet of things. IEEE J. Sel. Areas Commun. 2013, 31, 47–65. [Google Scholar] [CrossRef]
- Mohanraj, K.; Balaji, N.; Chithrakkannan, R. IoT based patient monitoring system using raspberry pi 3 and Lab view. Pak. J. Biotechnol. 2017, 14, 337–343. [Google Scholar]
- Granados, J.; Westerlund, T.; Zheng, L.; Zou, Z. IoT platform for real-time multichannel ECG monitoring and classification with neural networks. Lect. Notes Bus. Inf. Process. 2018, 310, 181–191. [Google Scholar] [CrossRef]
- Villarrubia, G.; Bajo, J.; De Paz, J.F.; Corchado, J.M. Monitoring and detection platform to prevent anomalous situations in home care. Sensors 2014, 14, 9900–9921. [Google Scholar] [CrossRef]
- Akrivopoulos, O.; Amaxilatis, D.; Mavrommati, I.; Chatzigiannakis, I. Utilising fog computing for developing a person-centric heart monitoring system. In Proceedings of the 2018 International Conference on Intelligent Environments IE, Rome, Italy, 25–28 June 2018. [Google Scholar] [CrossRef]
- Ji, C.; Liu, F.; Wang, Z.; Li, Y.; Qi, C.; Li, Z. Mobile cloud ECG intelligent monitoring and data processing system. In Proceedings of the 2017 IEEE 19th International Conference on e-Health Networking, Applications and Services Healthcom, Dalian, China, 12–15 October 2017; pp. 1–6. [Google Scholar] [CrossRef]
- Chatzigiannakis, I.; Valchinov, E.S.; Antoniou, A.; Kalogeras, A.; Alexakos, C.; Konstantinopoulos, P. Advanced observation and telemetry heart system utilizing wearable ECG device and a Cloud platform. In Proceedings of the IEEE Symposium on Computers and Communications, Larnaca, Cyprus, 6–9 July 2016; pp. 25–30. [Google Scholar] [CrossRef]
- Aljuaid, M.; Marashly, Q.; AlDanaf, J.; Tawhari, I.; Barakat, M.; Barakat, R.; Zobell, B.; Cho, W.; Chelu, M.G.; Marrouche, N.F. Smartphone ECG monitoring system helps lower emergency room and clinic visits in post–atrial fibrillation ablation patients. Clin. Med. Insights Cardiol. 2020, 14. [Google Scholar] [CrossRef]
- Phan, D.; Siong, L.Y.; Pathirana, P.N.; Seneviratne, A. Smartwatch: Performance evaluation for long-term heart rate monitoring. In Proceedings of the 4th International Symposium on Bioelectronics and Bioinformatics ISBB, Beijing, China, 14–17 October 2015. [Google Scholar] [CrossRef]
- Li, X.; Sun, Y. NCMB-Button: A wearable non-contact system for long-term multiple biopotential monitoring. In Proceedings of the 2017 2nd IEEE/ACM International Conference on Connected Health: Applications, Systems and Engineering Technologies (CHASE), Philadelphia, PA, USA, 17–19 July 2017; pp. 348–355. [Google Scholar]
- Bambang-Oetomo, S.; Feijs, L.; Cluitmans, P.J.M. Designing for reliable textile neonatal ECG monitoring using multi-sensor recordings Medical Simulations View project DOCHANGE View project. IEEE Eng. Med. Biol. Soc. 2011, 2011, 2488–2491. [Google Scholar] [CrossRef]
- Bouwstra, S.; Chen, W.; Feijs, L.; Oetomo, S.B. Smart jacket design for neonatal monitoring with wearable sensors. In Proceedings of the 2009 Sixth International Workshop on Wearable and Implantable Body Sensor Networks, Berkeley, CA, USA, 3–5 June 2009. [Google Scholar]
- Attin, M.; Feld, G.; Lemus, H.; Najarian, K.; Shandilya, S.; Wang, L.; Sabouriazad, P.; Lin, C.D. Electrocardiogram characteristics prior to in-hospital cardiac arrest. J. clin. Monit. Comput. 2015, 29, 385–392. [Google Scholar]
- Rafiq, S.; Alam, A.H.M.Z.; Islam, M.R. Development of ECG home monitoring system. In Proceedings of the 2017 IEEE Regional Symposium on Micro and Nanoelectronics RSM, Penang, Malaysia, 23–25 August 2017; pp. 80–83. [Google Scholar] [CrossRef]
- Brugarolas, R.; Latif, T.; Dieffenderfer, J.; Walker, K.; Yuschak, S.; Sherman, B.L.; Roberts, D.L.; Bozkurt, A. Wearable heart rate sensor systems for wireless canine health monitoring. IEEE Sens. J. 2015, 16, 3454–3464. [Google Scholar] [CrossRef]
- Bianchi, A.M.; Di Milano, P.; Politecnico, S.C.; Milano, D.; Mendez, M.O.; Cerutti, S. Processing of signals recorded through smart devices: Sleep-quality assessment central nervous system view project LINK-Linking excellence in biomedical knowledge and computational intelligence research for personalized management of CVD within PHC View p. IEEE Trans. Inf. Technol. Biomed. 2010, 14, 741. [Google Scholar] [CrossRef] [PubMed]
- Tao, X.; Huang, T.; Shen, C.; Ko, Y.; Jou, G.; Koncar, V. Bluetooth low energy-based washable wearable activity motion and electrocardiogram textronic monitoring and communicating system. Adv. Mater. Technol. 2018, 3, 1700309. [Google Scholar] [CrossRef]
- Ankhili, A.; Tao, X.; Cochrane, C.; Coulon, D.; Koncar, V. Washable and reliable textile electrodes embedded into underwear fabric for electrocardiography (ECG) monitoring. Materials 2018, 11, E256. [Google Scholar] [CrossRef]
- Yoon, Y.; Cho, J.H.; Yoon, G. Non-constrained blood pressure monitoring using ECG and PPG for personal healthcare. J. Med. Syst. 2009, 33, 261–266. [Google Scholar] [CrossRef]
- Lee, H.E.; Wang, W.C.; Lu, S.W.; Wu, B.Y.; Ko, L.W. Home-based mobile cardio-pulmonary rehabilitation consultant system. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society EMBC, Boston, MA, USA, 30 August – 3 September 2011; pp. 989–992. [Google Scholar] [CrossRef]
- Ravanshad, N.; Rezaee-Dehsorkh, H. An event-based ECG-monitoring and QRS-detection system based on level-crossing sampling. In Proceedings of the 2017 25th Iranian Conference on Electrical Engineering ICEE, Tehran, Iran, 2–4 May 2017; pp. 302–307. [Google Scholar]
- Ravanshad, N.; Rezaee-Dehsorkh, H.; Lotfi, R.; Lian, Y. A level-crossing based QRS-detection algorithm for wearable ECG sensors. IEEE J. Biomed. Health Inform. 2014, 18, 183–192. [Google Scholar] [CrossRef]
- Fensli, R.; Gunnarson, E.; Gundersen, T. A wearable ECG-recording system for continuous arrhythmia monitoring in a wireless tele-home-care situation. In Proceedings of the IEEE Symposium on Computer-Based Medical Systems, Dublin, Ireland, 23–24 June 2005; pp. 407–412. [Google Scholar]
- Ruwald, M.H.; Zareba, W. ECG monitoring in syncope. Prog. Cardiovasc. Dis. 2013, 56, 203–210. [Google Scholar] [CrossRef]
- Viskin, S.; Postema, P.G.; Bhuiyan, Z.A.; Rosso, R.; Kalman, J.M.; Vohra, J.K.; Guevara-Valdivia, M.E.; Marquez, M.F.; Kogan, E.; Belhassen, B. The response of the QT interval to the brief tachycardia provoked by standing: a bedside test for diagnosing long QT syndrome. J. Am. Coll. Cardiol. 2010, 55, 1955–1961. [Google Scholar] [CrossRef]
- Zhang, Z.-X.; Tian, X.-W.; Lim, J.S. New algorithm for the depression diagnosis using HRV: A neuro-fuzzy approach. In Proceedings of the International Symposium on Bioelectronics and Bioinformations, Suzhou, China, 3–5 November 2011; pp. 283–286. [Google Scholar]
- Yin, L.; Chen, Y.; Ji, W. A novel method of diagnosing coronary heart disease by analysing ECG signals combined with motion activity. In Proceedings of the 2011 IEEE International Workshop on Machine Learning for Signal Processing, Santander, Spain, 18–21 September 2011; pp. 1–5. [Google Scholar]
- Garudadri, H.; Chi, Y.; Baker, S.; Majumdar, S.; Baheti, P.K.; Ballard, D. Diagnostic grade wireless ECG monitoring. In Proceedings of the Annual International Conference of the IEEE Engineering in Medicine and Biology Society EMBS, Boston, USA, 30 August – 3 September 2011; pp. 850–855. [Google Scholar] [CrossRef]
- Abo-Zahhad, M.; Ahmed, S.M.; Elnahas, O. A wireless emergency telemedicine system for patients monitoring and diagnosis. Int. J. Telemed. Appl. 2014, 2014, 380787. [Google Scholar] [CrossRef]
- Dong, J.; Zhang, J.; Zhu, H.; Wang, L.; Liu, X.; Li, Z. A remote diagnosis service platform for wearable ECG monitors. IEEE Intell. Syst. 2012, 27, 36–43. [Google Scholar] [CrossRef]
- Knoery, C.R.; Bond, R.; Iftikhar, A.; Rjoob, K.; McGilligan, V.; Peace, A.; Heaton, J.; Leslie, S.J. SPICED-ACS: Study of the potential impact of a computer-generated ECG diagnostic algorithmic certainty index in STEMI diagnosis: Towards transparent AI. J. Electrocardiol. 2019, 57, S86–S91. [Google Scholar] [CrossRef] [PubMed]
- Calzone, R.; Pagana, G.; Perez, M.D.; Augustine, R. Innovations in biomedicine: Measuring physiological parameters becomes as simple as applying a plaster on the body. In Proceedings of the 2019 21st International Conference on Electromagnetics in Advanced Applications ICEAA, Granada, Spain, 9–13 September 2019. [Google Scholar] [CrossRef]
- Fensli, R.; Gundersen, T.; Snaprud, T.; Hejlesen, O. Clinical evaluation of a wireless ECG sensor system for arrhythmia diagnostic purposes. Med. Eng. Phys. 2013, 35, 697–703. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Aldana Blanco, A.L.; Grautoff, S.; Hermann, T. CardioSounds: Real-time auditory assistance for supporting cardiac diagnostic and monitoring. ACM Int. Conf. Proc. Ser. 2017, Part F1319, 4–7. [Google Scholar] [CrossRef]
- Chen, Y.P.; Jeon, D.; Lee, Y.; Kim, Y.; Foo, Z.; Lee, I.; Langhals, N.B.; Kruger, G.; Oral, H.; Berenfeld, O.; et al. An injectable 64 nW ECG mixed-signal SoC in 65 nm for arrhythmia monitoring. IEEE J. Solid State Circ. 2015, 50, 375–390. [Google Scholar] [CrossRef]
- Huang, Y.-P.; Huang, C.-Y.; Liu, S.-I. Hybrid intelligent methods for arrhythmia detection and geriatric depression diagnosis. Appl. Soft Comput. 2014, 14, 38–46. [Google Scholar] [CrossRef]
- Chen, X.; Ji, J.; Loparo, K.; Li, P. Real-time personalized cardiac arrhythmia detection and diagnosis: A cloud computing architecture. In Proceedings of the 2017 IEEE EMBS International Conference on Biomedical & Health Informatics (BHI), Orlando, FL, USA, 16–19 February 2017; pp. 201–204. [Google Scholar]
- Dziubiński, M. PocketECG: A new continuous and real-time ambulatory arrhythmia diagnostic method. Cardiol. J. 2011, 18, 454–460. [Google Scholar]
- Lip, G.Y.H.; Hunter, T.D.; Quiroz, M.E.; Ziegler, P.D.; Turakhia, M.P. Atrial fibrillation diagnosis timing, ambulatory ECG monitoring utilization, and risk of recurrent stroke. Circ. Cardiovasc. Qual. Outcomes 2017, 10, e002864. [Google Scholar] [CrossRef]
- Uittenbogaart, S.B.; Verbiest-van Gurp, N.; Erkens, P.M.G.; Lucassen, W.A.M.; Knottnerus, J.A.; Winkens, B.; van Weert, H.C.P.M.; Stoffers, H.E.J.H. Detecting and diagnosing atrial fibrillation (D 2 AF): study protocol for a cluster randomised controlled trial. Trials 2015, 16, 478. [Google Scholar] [CrossRef]
- Borowsky, L.H.; Regan, S.; Chang, Y.; Ayres, A.; Greenberg, S.M.; Singer, D.E. First diagnosis of atrial fibrillation at the time of stroke. Cerebrovasc. Dis. 2017, 43, 192–199. [Google Scholar] [CrossRef]
- Sufi, F.; Khalil, I. Diagnosis of cardiovascular abnormalities from compressed ECG: A data mining-based approach. IEEE Trans. Inf. Technol. Biomed. 2010, 15, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Tinnakornsrisuphap, T.; Billo, R.E. An interoperable system for automated diagnosis of cardiac abnormalities from electrocardiogram data. IEEE J. Biomed. Health inform. 2014, 19, 493–500. [Google Scholar] [CrossRef] [PubMed]
- Hadjem, M.; Salem, O.; Nait-Abdesselam, F. An ECG monitoring system for prediction of cardiac anomalies using WBAN. In Proceedings of the 2014 IEEE 16th International Conference on e-Health Networking, Applications and Services Healthcom, Natal, Brazil, 15–18 October 2014. [Google Scholar] [CrossRef]
- Perego, P.; Moltani, A.; Andreoni, G. Sport monitoring with smart wearable system. Stud. Health Technol. Inform. 2012, 177, 224–228. [Google Scholar] [PubMed]
- Peritz, D.C.; Howard, A.; Ciocca, M.; Chung, E.H. Smartphone ECG aids real time diagnosis of palpitations in the competitive college athlete. J. Electrocardiol. 2015, 48, 896–899. [Google Scholar] [CrossRef] [PubMed]
- Xia, W.; Zhou, Y.; Fang, Y.; Liu, H. ECG-Enhanced multi-sensor solution for wearable sports devices. In Proceedings of the 2018 IEEE International Conference on Systems, Man, and Cybernetics SMC, Miyazaki, Japan, 7–10 October 2018. [Google Scholar]
- Sun, F.; Yi, C.; Li, W.; Li, Y. A wearable H-shirt for exercise ECG monitoring and individual lactate threshold computing. Comput. Ind. 2017, 92–93, 1–11. [Google Scholar] [CrossRef]
- Pollonini, L.; Re, R.; Simpson, R.J.; Dacso, C.C. Integrated device for the measurement of systemic and local oxygen transport during physical exercise. In Proceedings of the 2012 Annual International Conference of the IEEE Engineering in Medicine and Biology Society, San Diego, CA, USA, 28 August–1 September 2012; pp. 3760–3763. [Google Scholar]
- Gouttebarge, V.; Andersen, T.E.; Cowie, C.; Goedhart, E.; Jorstad, H.; Kemp, S.; Königs, M.; Maas, M.; Orhant, E.; Rantanen, J.; et al. Monitoring the health of transitioning professional footballers: Protocol of an observational prospective cohort study. BMJ Open Sport Exerc. Med. 2019, 5, 1–10. [Google Scholar] [CrossRef]
- Jung, S.J.; Shin, H.S.; Chung, W.Y. Driver fatigue and drowsiness monitoring system with embedded electrocardiogram sensor on steering wheel. IET Intell. Transp. Syst. 2014, 8, 43–50. [Google Scholar] [CrossRef]
- Matsuda, T.; Makikawa, M. ECG monitoring of a car driver using capacitively-coupled electrodes. In Proceedings of the 30th Annual International Conference of the IEEE Engineering in Medicine and Biology Society, EMBS’08—“Personalized Healthcare through Technology, Vancouver, BC, Canada, 20–25 August 2008. [Google Scholar] [CrossRef]
- Sun, Y.; Yu, X. An innovative nonintrusive driver assistance system for vital signal monitoring. IEEE J. Biomed. Health Inform. 2014, 18, 1923–1929. [Google Scholar] [CrossRef]
- Zeng, C.; Wang, W.; Chen, C.; Zhang, C.; Cheng, B. Poincaré plot indices of heart rate variability for monitoring driving fatigue. In Proceedings of the CICTP 2019: Transportation in China—Connecting the World - Proceedings of the 19th COTA International Conference of Transportation Professionals; Jiangsu, China, 6–8 July 2019, pp. 652–660. [CrossRef]
- Shin, H.S.; Jung, S.J.; Kim, J.J.; Chung, W.Y. Real time car driver’s condition monitoring system. In Proceedings of the IEEE Sensors, Kona, HI, USA, 1–4 November 2010. [Google Scholar] [CrossRef]
- Trenta, F.; Conoci, S.; Rundo, F.; Battiato, S. Advanced motion-tracking system with multi-layers deep learning framework for innovative car-driver drowsiness monitoring. In Proceedings of the Proceedings - 14th IEEE International Conference on Automatic Face and Gesture Recognition FG, Lille, France, 14–18 May 2019. [Google Scholar] [CrossRef]
- De Nadai, S.; D’Incà, M.; Parodi, F.; Benza, M.; Trotta, A.; Zero, E.; Zero, L.; Sacile, R. Enhancing safety of transport by road by on-line monitoring of driver emotions. In Proceedings of the 2016 11th System of Systems Engineering Conference (SoSE), Kongsberg, Norway, 12–16 June 2016; pp. 1–4. [Google Scholar]
- Kumari, P.; Mathew, L.; Syal, P. Increasing trend of wearables and multimodal interface for human activity monitoring: A review. Biosens. Bioelectron. 2017, 90, 298–307. [Google Scholar] [CrossRef]
- Lee, H.J.; Lee, S.H.; Ha, K.S.; Jang, H.C.; Chung, W.Y.; Kim, J.Y.; Chang, Y.S.; Yoo, D.H. Ubiquitous healthcare service using Zigbee and mobile phone for elderly patients. Int. J. Med. Inform. 2009, 78, 193–198. [Google Scholar] [CrossRef]
- Fan, X.; Zhao, Y.; Wang, H.; Tsui, K.L. Forecasting one-day-forward wellness conditions for community-dwelling elderly with single lead short electrocardiogram signals. BMC Med. Inform. Decis. Mak. 2019, 19, 285. [Google Scholar] [CrossRef] [PubMed]
- Valchinov, E.; Antoniou, A.; Rotas, K.; Pallikarakis, N. Wearable ECG system for health and sports monitoring. In Proceedings of the 2014 4th International Conference on Wireless Mobile Communication and Healthcare-Transforming Healthcare Through Innovations in Mobile and Wireless Technologies (MOBIHEALTH), Athens, Greece, 3–5 November 2014; pp. 63–66. [Google Scholar]
- Walinjkar, A.; Woods, J. ECG classification and prognostic approach towards personalized healthcare. In Proceedings of the 2017 International Conference On Social Media, Wearable And Web Analytics, Social Media, London, UK, 19–20 June 2017. [Google Scholar] [CrossRef]
- Katritsis, D.G.; Siontis, G.C.M.; Camm, A.J. Prognostic significance of ambulatory ECG monitoring for ventricular arrhythmias. Prog. Cardiovasc. Dis. 2013, 56, 133–142. [Google Scholar] [CrossRef] [PubMed]
- Benchaira, K.; Bitam, S.; Mellouk, A.; Tahri, A.; Okbi, R. AfibPred: A Novel Atrial Fibrillation Prediction Approach Based on Short Single-Lead ECG Using Deep Transfer Knowledge. In Proceedings of the 4th International Conference on Big Data and Internet of Things, Tangier-Tetuan, Morocco, 23–24 October 2019; pp. 1–6. [Google Scholar]
- El Halabi, N.; Daou, R.A.Z.; Achkar, R.; Hayek, A.; Borcsok, J. Monitoring system for prediction and detection of epilepsy seizure. In Proceedings of the 2019 4th International Conference on Advances in Computational Tools for Engineering Applications ACTEA, Beirut, Lebanon, 3–5 July 2019. [Google Scholar] [CrossRef]
- Behbahani, S.; Dabanloo, N.J.; Nasrabadi, A.M.; Dourado, A. Prediction of epileptic seizures based on heart rate variability. Technol. Health Care 2016, 24, 795–810. [Google Scholar] [CrossRef] [PubMed]
- Barison, A.; Del Torto, A.; Chiappino, S.; Aquaro, G.D.; Todiere, G.; Vergaro, G.; Passino, C.; Lombardi, M.; Emdin, M.; Masci, P.G. Prognostic significance of myocardial extracellular volume fraction in nonischaemic dilated cardiomyopathy. J. Cardiovasc. Med. 2015, 16, 681. [Google Scholar] [CrossRef] [PubMed]
- Massoullié, G.; Bordachar, P.; Irles, D.; Caussin, C.; Da Costa, A.; Defaye, P.; Jean, F.; Mechulan, A.; Mondoly, P.; Souteyrand, G. Prognosis assessment of persistent left bundle branch block after TAVI by an electrophysiological and remote monitoring risk-adapted algorithm: Rationale and design of the multicentre LBBB–TAVI study. BMJ Open 2016, 6, e010485. [Google Scholar] [CrossRef] [PubMed]
- Liu, N.; Koh, Z.X.; Chua, E.C.-P.; Tan, L.M.-L.; Lin, Z.; Mirza, B.; Ong, M.E.H. Risk scoring for prediction of acute cardiac complications from imbalanced clinical data. IEEE J. Biomed. Health Inform. 2014, 18, 1894–1902. [Google Scholar] [CrossRef]
- Liu, N.; Koh, Z.X.; Goh, J.; Lin, Z.; Haaland, B.; Ting, B.P.; Ong, M.E.H. Prediction of adverse cardiac events in emergency department patients with chest pain using intelligent variable selection and heart rate variability. BMC Med. Inform. Decis. Mak. 2014, 14, 75. [Google Scholar] [CrossRef]
- Nikolaiev, S.; Timoshenko, Y. Reinvention of the cardiovascular diseases prevention and prediction due to ubiquitous convergence of mobile apps and machine learning. In Proceedings of the 2015 Information Technologies in Innovation Business Conference (ITIB), Kharkiv, Ukraine, 7–9 October 2015; pp. 23–26. [Google Scholar]
- Forkan, A.R.M.; Hu, W. A context-aware, predictive and protective approach for wellness monitoring of cardiac patients. In Proceedings of the 2016 Computing in Cardiology Conference (CinC), Vancouver, BC, Canada, 11–14 September 2016; pp. 369–372. [Google Scholar]
- Bazan, J.G.; Buregwa-Czuma, S.; Pardel, P.W.; Bazan-Socha, S.; Sokołowska, B.; Dziedzina, S. Predicting the presence of serious coronary artery disease based on 24 hour Holter ECG monitoring. In Transactions on Rough Sets XIX; Springer: Berelin, Germany, 2015; pp. 95–113. [Google Scholar]
- Gupta, N.; Haft, J.I.; Bajaj, S.; Samuel, A.; Parikh, R.; Pandya, D.; Shamoon, F. Role of the combined CHADS2 score and echocardiographic abnormalities in predicting stroke in patients with paroxysmal atrial fibrillation. J. Clin. Neurosci. 2012, 19, 1242–1245. [Google Scholar] [CrossRef]
- Siriphuwanun, V.; Punjasawadwong, Y.; Lapisatepun, W.; Charuluxananan, S.; Uerpairojkit, K. Prognostic factors for death and survival with or without complications in cardiac arrest patients receiving CPR within 24 hours of anesthesia for emergency surgery. Risk Manag. Healthc. Policy 2014, 7, 199. [Google Scholar]
- Jing, B.; Zhang, T.; Wang, Z.; Jin, Y.; Liu, K.; Qiu, W.; Ke, L.; Sun, Y.; He, C.; Hou, D.; et al. A deep survival analysis method based on ranking. Artif. Intell. Med. 2019, 98, 1–9. [Google Scholar] [CrossRef]
- Biagini, E.; Pazzi, C.; Olivotto, I.; Musumeci, B.; Limongelli, G.; Boriani, G.; Pacileo, G.; Mastromarino, V.; Reggiani, M.L.B.; Lorenzini, M. Usefulness of electrocardiographic patterns at presentation to predict long-term risk of cardiac death in patients with hypertrophic cardiomyopathy. Am. J. Cardiol. 2016, 118, 432–439. [Google Scholar] [CrossRef] [PubMed]
- Zamanifar, A.; Nazemi, E. An approach for predicting health status in IoT health care. J. Netw. Comput. Appl. 2019, 134, 100–113. [Google Scholar] [CrossRef]
- Mansouri, S.; Farahmand, F.; Vossoughi, G.; Ghavidel, A.A. A comprehensive multimodality heart motion prediction algorithm for robotic-assisted beating heart surgery. Int. J. Med. Robot. Comput. Assist. Surg. 2019, 15, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Bie, R.; Zhang, G.; Sun, Y.; Xu, S.; Li, Z.; Song, H. Smart assisted diagnosis solution with multi-sensor Holter. Neurocomputing 2017, 220, 67–75. [Google Scholar] [CrossRef]
- Somanna, J.; Joshi, D.; Gundu, H.; Srinivasa, G. Automated classification of sleep apnea and hypopnea on polysomnography data. In Proceedings of the 2019 12th Biomedical Engineering International Conference (BMEiCON), Laos, Thailand, 18–21 December 2019; pp. 1–5. [Google Scholar]
- Fahruzi, I.; Purnama, I.K.E.; Purnomo, M.H. Screening of non-overlapping apnea and non-apnea from single lead ECG-apnea recordings using time-frequency approach. In Proceedings of the 2019 International Conference on Computer Engineering, Network, and Intelligent Multimedia (CENIM), Surabaya City, Indonesia, 19–20 November 2019; pp. 1–6. [Google Scholar]
- Chen, Z.; Tian, F.; Zhao, Q.; Hu, B. A Non-contact and unconstrained sleep health monitoring system. In Proceedings of the International Conference on Human Centered Computing, Čačak, Serbia, 5–9 August 2019; pp. 56–66. [Google Scholar]
- Pirbhulal, S.; Samuel, O.W.; Wu, W.; Sangaiah, A.K.; Li, G. A joint resource-aware and medical data security framework for wearable healthcare systems. Futur. Gener. Comput. Syst. 2019, 95, 382–391. [Google Scholar] [CrossRef]
- Yu, B.; Xu, L.; Li, Y. Bluetooth Low Energy (BLE) based mobile electrocardiogram monitoring system. In Proceedings of the 2012 IEEE International Conference on Information and Automation ICIA, Shenyang, China, 6–8 June 2012. [Google Scholar] [CrossRef]
- Mahmud, M.S.; Wang, H.; Esfar-E-Alam, A.M.; Fang, H. A wireless health monitoring system using mobile phone accessories. IEEE Intern. Things J. 2017, 4, 2009–2018. [Google Scholar] [CrossRef]
- Nia, A.M.; Mozaffari-Kermani, M.; Sur-Kolay, S.; Raghunathan, A.; Jha, N.K. Energy-efficient long-term continuous personal health monitoring. IEEE Trans. Multi Scale Comput. Syst. 2015, 1, 85–98. [Google Scholar] [CrossRef]
- Ma, T.; Shrestha, P.L.; Hempel, M.; Peng, D.; Sharif, H.; Chen, H.-H. Assurance of energy efficiency and data security for ECG transmission in BASNs. IEEE Trans. Biomed. Eng. 2012, 59, 1041–1048. [Google Scholar]
- Altini, M.; Polito, S.; Penders, J.; Kim, H.; Van Helleputte, N.; Kim, S.; Yazicioglu, F. An ECG patch combining a customized ultra-low-power ECG SoC with Bluetooth low energy for long term ambulatory monitoring. In Proceedings of the 2nd Conference on Wireless Health, San Diego, CA, USA, 5–9 August 2011; pp. 1–2. [Google Scholar]
- Zhou, B.; Chen, X.; Hu, X.; Ren, R.; Tan, X.; Fang, Z.; Xia, S. A Bluetooth low energy approach for monitoring electrocardiography and respiration. In Proceedings of the 2013 IEEE 15th International Conference on e-Health Networking, Applications and Services (Healthcom 2013), Lisbon, Portugal, 9–12 October 2013; pp. 130–134. [Google Scholar]
- Touati, F.; Erdene-Ochir, O.; Mehmood, W.; Hassan, A.; Mnaouer, A.B.; Gaabab, B.; Rasid, M.F.A.; Khriji, L. An experimental performance evaluation and compatibility study of the Bluetooth low energy based platform for ECG monitoring in WBANs. Int. J. Distrib. Sens. Netw. 2015, 11, 645781. [Google Scholar] [CrossRef]
- Chen, X.; Xie, J.; Fang, Z.; Xia, S. Low power electrocardiography and impedance cardiography detection system based on labview and bluetooth low energy. In Proceedings of the 2015 IET International Conference on Biomedical Image and Signal Processing (ICBISP 2015), Beijing, China, 19 November 2015. [Google Scholar] [CrossRef]
- Pandya, U.T.; Desai, U.B. Feasibility study of filtering algorithms for low cost wireless physiological monitoring system. In Proceedings of the 2011 2nd International Conference on Wireless Communication, Vehicular Technology, Information Theory and Aerospace & Electronic Systems Technology (Wireless VITAE), Chennai, India, 28 February–3 March 2011; pp. 1–6. [Google Scholar]
- Nabar, S.; Banerjee, A.; Gupta, S.K.S.; Poovendran, R. GeM-REM: Generative model-driven resource efficient ECG monitoring in body sensor networks. In Proceedings of the 2011 International Conference on Body Sensor Networks, Dallas, TX, USA, 23–25 May 2011; pp. 1–6. [Google Scholar]
- Samie, F.; Tsoutsouras, V.; Xydis, S.; Bauer, L.; Soudris, D.; Henkel, J. Distributed QoS management for internet of things under resource constraints. In Proceedings of the Eleventh IEEE/ACM/IFIP International Conference on Hardware/Software Codesign and System Synthesis, Pittsburgh, PA, USA, 11–16 October 2016; pp. 1–10. [Google Scholar]
- Pathak, S.; Kumar, M.; Mohan, A.; Kumar, B. Energy optimization of zigBee based WBAN for patient monitoring. Procedia Comput. Sci. 2015, 70, 414–420. [Google Scholar] [CrossRef]
- Milis, M.; Michaelides, K.; Kounoudes, A.; Ansaloni, G.; Atienza, D.; Giroud, F.; Ruedi, P.-F.; Masson, F. IcyHeart: Highly integrated ultra-low-power SoC solution for unobtrusive and energy efficient wireless cardiac monitoring: Research project for the benefit of specific groups (FP7, Capacities). In Proceedings of the 2012 IEEE 12th International Conference on Bioinformatics & Bioengineering (BIBE), Chania, Greece, 11–13 November 2012; pp. 105–109. [Google Scholar]
- Sudha, G.; Karthik, S.; Kumar, N.S. Activity aware energy efficient priority based multi patient monitoring adaptive system for body sensor networks. Technol. Health Care 2014, 22, 167–177. [Google Scholar] [CrossRef] [PubMed]
- Aldammas, M.A.; Tabbabi, E.; Soudani, A. Low-Energy ECG Processing for Accurate Features’ Extraction in Wireless Body Sensor Networks. In Proceedings of the 2nd International Conference on Computer Applications and Information Security ICCAIS, Riyadh, Saudi Arabia, 1–3 May 2019. [Google Scholar] [CrossRef]
- Ferretti, L.; Ansaloni, G.; Pozzi, L.; Aminifar, A.; Atienza, D.; Cammoun, L.; Ryvlin, P. Tailoring SVM inference for resource-efficient ECG-based epilepsy monitors. In Proceedings of the 2019 Design, Automation and Test in Europe Conference and Exhibition DATE, Florence, Italy, 25–29 March 2019. [Google Scholar] [CrossRef]
- Huang, H.; Hu, S.; Sun, Y. Energy-Efficient ECG Signal Compression for User Data Input in Cyber-Physical Systems by Leveraging Empirical Mode Decomposition. ACM Trans. Cyber Phys. Syst. 2019, 3, 1–19. [Google Scholar] [CrossRef]
- Zhang, Z.; Jung, T.-P.; Makeig, S.; Rao, B.D. Compressed sensing for energy-efficient wireless telemonitoring of noninvasive fetal ECG via block sparse Bayesian learning. IEEE Trans. Biomed. Eng. 2012, 60, 300–309. [Google Scholar] [CrossRef] [PubMed]
- Bortolotti, D.; Bartolini, A.; Mangia, M.; Rovatti, R.; Setti, G.; Benini, L. Energy-aware bio-signal compressed sensing reconstruction: FOCUSS on the WBSN-gateway. In Proceedings of the 2015 IEEE 9th International Symposium on Embedded Multicore/Many-core Systems-on-Chip, Turin, Italy, 23–25 September 2015; pp. 120–126. [Google Scholar]
- Biswas, D.; Mazomenos, E.B.; Maharatna, K. ECG compression for remote healthcare systems using selective thresholding based on energy compaction. In Proceedings of the 2012 International Symposium on Signals, Systems, and Electronics (ISSSE), Potsdam, Germany, 3–5 October 2012; pp. 1–6. [Google Scholar]
- Bortolotti, D.; Mangia, M.; Bartolini, A.; Rovatti, R.; Setti, G.; Benini, L. Energy-aware bio-signal compressed sensing reconstruction on the WBSN-gateway. IEEE Trans. Emerg. Top. Comput. 2016, 6, 370–381. [Google Scholar] [CrossRef]
- Gavriel, C.; Parker, K.H.; Faisal, A.A. Smartphone as an ultra-low cost medical tricorder for real-time cardiological measurements via ballistocardiography. In Proceedings of the 2015 IEEE 12th International Conference on Wearable and Implantable Body Sensor Networks (BSN), Turin, Italy, 23–25 September 2015; pp. 1–6. [Google Scholar]
- Rebolledo-Nandi, Z.; Chavez-Olivera, A.; Cuevas-Valencia, R.E.; Alarcon-Paredes, A.; Alonso, G.A. Design of a versatile low cost mobile health care monitoring system using an android application. In Proceedings of the 2015 Pan American Health Care Exchanges (PAHCE), Vina del Mar, Chile, 23–28 March 2015; pp. 1–4. [Google Scholar]
- Abrar, S.; Aziz, U.S.; Choudhry, F.; Mansoor, A. Design and implementation of an embedded system for transmitting human ECG and web server for emergency services and remote health monitoring: A low cost ECG signal simulator and its transmitter, to send and store data in electronic databases, in remote l. In Proceedings of the 2012 International Conference on Open Source Systems and Technologies, Lahore, Pakistan, 20–22 December 2012; pp. 1–6. [Google Scholar]
- Deb, S.; Islam, S.M.R.; Robaiatmou, J.; Islam, M.T. Design and implementation of low Cost ECG monitoring system for the patient using smart device. In Proceedings of the ECCE 2017—International Conference on Electrical, Computer and Communication Engineering, Cox’s Bazar, Bangladesh, 16–18 February 2017. [Google Scholar] [CrossRef]
- Krachunov, S.; Beach, C.; Casson, A.J.; Pope, J.; Fafoutis, X.; Piechocki, R.J.; Craddock, I. Energy efficient heart rate sensing using a painted electrode ECG wearable. In Proceedings of the GIoTS 2017—Global Internet of Things Summit, Geneva, Switzerland, 6–9 June 2017. [Google Scholar] [CrossRef]
- Nguyen Gia, T.; Jiang, M.; Sarker, V.K.; Rahmani, A.M.; Westerlund, T.; Liljeberg, P.; Tenhunen, H. Low-cost fog-assisted health-care IoT system with energy-efficient sensor nodes. In Proceedings of the 2017 13th International Wireless Communications and Mobile Computing Conference IWCMC, Valencia, Spain, 26–30 June 2017. [Google Scholar] [CrossRef]
- Preučil, T.; Novotný, M. Low-cost portable ECG. In Proceedings of the 2019 8th Mediterranean Conference on Embedded Computing MECO, Budva, Montenegro, 10–14 June 2019. [Google Scholar] [CrossRef]
- Alhalabi, W. Patient monitoring at home using 32-channel cost-effective data acquisition device. Telemat. Inform. 2018, 35, 883–891. [Google Scholar] [CrossRef]
- Piuzzi, E.; Pisa, S.; Pittella, E.; Podestà, L.; Sangiovanni, S. Low-cost and portable impedance plethysmography system for the simultaneous detection of respiratory and heart activities. IEEE Sens. J. 2018, 19, 2735–2746. [Google Scholar] [CrossRef]
- Yong, J.H.E.; Thavorn, K.; Hoch, J.S.; Mamdani, M.; Thorpe, K.E.; Dorian, P.; Sharma, M.; Laupacis, A.; Gladstone, D.J. Potential Cost-Effectiveness of Ambulatory Cardiac Rhythm Monitoring after Cryptogenic Stroke. Stroke 2016, 47, 2380–2385. [Google Scholar] [CrossRef]
- Steinhubl, S.R.; Edwards, A.M.; Waalen, J.; Zambon, R.; Mehta, R.; Ariniello, L.; Ebner, G.; Baca-Motes, K.; Carter, C.; Felicione, E.; et al. Healthcare resource UTILIZATION associated with electrocardiograph (ECG) sensor patch screening for atrial fibrillation (AF): Results from the mhealth screening to prevent strokes (MSTOPS) trial. J. Am. Coll. Cardiol. 2019, 73, 296. [Google Scholar] [CrossRef]
- Wang, H.; Peng, D.; Wang, W.; Sharif, H.; Chen, H.H.; Khoynezhad, A. Resource-aware secure ECG healthcare monitoring through body sensor networks. IEEE Wirel. Commun. 2010, 17, 12–19. [Google Scholar] [CrossRef]
- Majhi, R.R.; Chattopadhyay, S.; Chattopadhyay, S.; Ghosh, A. Analysis of electro-cardiogram by radar and DWT based Kurtosis comparison. In Proceedings of the IET Conference Publications, Kolkata, India, 12–13 September 2015; Volume 2015, pp. 621–625. [Google Scholar] [CrossRef]
- Chioukh, L.; Boutayeb, H.; Deslandes, D.; Wu, K. Noise and sensitivity of harmonic radar architecture for remote sensing and detection of vital signs. IEEE Trans. Microw. Theory Tech. 2014, 62, 1847–1855. [Google Scholar] [CrossRef]
- Mostov, K.; Liptsen, E.; Boutchko, R. Medical applications of shortwave FM radar: Remote monitoring of cardiac and respiratory motion. Med. Phys. 2010, 37, 1332–1338. [Google Scholar] [CrossRef] [PubMed]
- Vinci, G.; Lindner, S.; Barbon, F.; Mann, S.; Hofmann, M.; Duda, A.; Weigel, R.; Koelpin, A. Six-port radar sensor for remote respiration rate and heartbeat vital-sign monitoring. IEEE Trans. Microw. Theory Tech. 2013, 61, 2093–2100. [Google Scholar] [CrossRef]
- Tu, J.; Lin, J. Fast acquisition of heart rate in noncontact vital sign radar measurement using time-window-variation technique. IEEE Trans. Instrum. Meas. 2016, 65, 112–122. [Google Scholar] [CrossRef]
- Xiong, Y.; Chen, S.; Dong, X.; Peng, Z.; Zhang, W. Accurate measurement in doppler radar vital sign detection based on parameterized demodulation. IEEE Trans. Microw. Theory Tech. 2017, 65, 4483–4492. [Google Scholar] [CrossRef]
- Giancaterino, S.; Lupercio, F.; Nishimura, M.; Hsu, J.C. Current and future use of insertable cardiac monitors. JACC Clin. Electrophysiol. 2018, 4, 1383–1396. [Google Scholar] [CrossRef] [PubMed]
- Lee, J.-H. Miniaturized human insertable cardiac monitoring system with wireless power transmission technique. J. Sens. 2016, 2016, 1–7. [Google Scholar] [CrossRef]
- Riistama, J.; Väisänen, J.; Heinisuo, S.; Harjunpää, H.; Arra, S.; Kokko, K.; Mäntylä, M.; Kaihilahti, J.; Heino, P.; Kellomäki, M.; et al. Wireless and inductively powered implant for measuring electrocardiogram. Med. Biol. Eng. Comput. 2007, 45, 1163–1174. [Google Scholar] [CrossRef]
- Mittal, S.; Pokushalov, E.; Romanov, A.; Ferrara, M.; Arshad, A.; Musat, D.; Preminger, M.; Sichrovsky, T.; Steinberg, J.S. Long-term ECG monitoring using an implantable loop recorder for the detection of atrial fibrillation after cavotricuspid isthmus ablation in patients with atrial flutter. Heart Rhythm 2013, 10, 1598–1604. [Google Scholar] [CrossRef]
- Ishikawa, N.; Watanabe, G. Robot-assisted cardiac surgery. Ann. Thorac. Cardiovasc. Surg. 2015, 21, 322–328. [Google Scholar] [CrossRef]
- Ma, Y.; Zhang, Y.; Wan, J.; Zhang, D.; Pan, N.; Org, D. Robot and cloud-assisted multi-modal healthcare system Enabling comfortable sports therapy for patient: A novel lightweight durable and portable ECG monitoring system View project VENDNET: Vehicular Named Data Network View project Robot and cloud-assisted. Comput. Netw. 2015, 18, 1295–1306. [Google Scholar]
- Deng, Z.Y.; Li, H.C.; Chiang, H.H.; Lee, T.T. Robotic Aids for ECG Monitoring and Diagnosis in Assisted Living Environments. In Proceedings of the 2018 IEEE International Conference on Systems, Man, and Cybernetics, SMC, Miyazaki, Japan, 7–10 October 2018; pp. 2176–2181. [Google Scholar]
- Hattori, K.; Asamoto, M.; Otsuji, M.; Ito, N.; Kasahara, S.; Hashimoto, Y.; Yamada, Y. Quantitative evaluation of stress in Japanese anesthesiology residents based on heart rate variability and psychological testing. J. Clin. Monit. Comput. 2019, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Sarkar, P.; Etemad, A. Self-supervised ecg representation learning for emotion recognition under review. arXiv 2020, arXiv:2002.03898. [Google Scholar]
- Yin, W.; Yang, X.; Li, L.; Zhang, L.; Kitsuwan, N.; Shinkuma, R.; Oki, E. Self-adjustable domain adaptation in personalized ECG monitoring integrated with IR-UWB radar. Biomed. Signal Process. Control 2019, 47, 75–87. [Google Scholar] [CrossRef]
- Golany, T.; Radinsky, K. PGANs: Personalized Generative Adversarial Networks for ECG Synthesis to Improve Patient-Specific Deep ECG Classification. Proc. AAAI Conf. Artif. Intell. 2019, 33, 557–564. [Google Scholar] [CrossRef]
- Meghani, D.; Geetha, S. ECG steganography to secure patient data in an E-healthcare system. ACM Int. Conf. Proc. Ser. 2016, 21–22, 66–70. [Google Scholar]
- Yang, C.-Y.; Cheng, L.-T.; Wang, W.-F. Effective reversible data hiding in electrocardiogram based on fast discrete cosine transform. In Proceedings of the Future Technologies Conference, Vancouver, BC, Canada, 13–14 November 2018; pp. 640–648. [Google Scholar]
- Ibaida, A.; Khalil, I. Wavelet-based ECG steganography for protecting patient confidential information in point-of-care systems. IEEE Trans. Biomed. Eng. 2013, 60, 3322–3330. [Google Scholar] [CrossRef]
- Malasri, K.; Wang, L. Addressing security in medical sensor networks. In Proceedings of the HealthNet’07: 1st ACM SIGMOBILE International Workshop on Systems and Networking Support for Healthcare and Assisted Living Environments, San Juan, Puerto Rico, 11 June 2007; pp. 7–12. [Google Scholar] [CrossRef]
- Lee, W.B.; Lee, C.D. A cryptographic key management solution for HIPAA privacy/security regulations. IEEE Trans. Inf. Technol. Biomed. 2008, 12, 34–41. [Google Scholar] [CrossRef]
- Marvel, L.M.; Boncelet, C.G.; Retter, C.T. Spread spectrum image steganography. IEEE Trans. Image Process. 1999, 8, 1075–1083. [Google Scholar] [CrossRef]
- Gusev, M.; Stojmenski, A.; Chorbev, I. Challenges for development of an ECG m-Health solution ECGalert View project SIARS (Smart I (eye) Advisory Rescue System) View project Challenges for development of an ECG m-Health solution. J. Emerging Res. Solutions 2016, 1, 25–38. [Google Scholar] [CrossRef][Green Version]
- Jarchi, D.; Mahdi, A.; Tarassenko, L.; Clifton, D.A. Visualisation of long-term ECG signals applied to post-intensive care patients. In Proceedings of the 2018 IEEE 15th International Conference on Wearable and Implantable Body Sensor Networks (BSN), Las Vegas, NV, USA, 4–7 March 2018; pp. 165–168. [Google Scholar] [CrossRef]
- Navaz, A.N.; Serhani, M.A.; Al-Qirim, N.; Gergely, M. Towards an efficient and Energy-Aware mobile big health data architecture. Comput. Methods Programs Biomed. 2018, 166, 137–154. [Google Scholar] [CrossRef]
- Jovanov, E.; Milenkovic, A. Body area networks for ubiquitous healthcare applications: Opportunities and challenges. J. Med. Syst. 2011, 35, 1245–1254. [Google Scholar] [CrossRef] [PubMed]
- Spanò, E.; Di Pascoli, S.; Iannaccone, G. Low-power wearable ECG monitoring system for multiple-patient remote monitoring. IEEE Sens. J. 2016, 16, 5452–5462. [Google Scholar] [CrossRef]
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).