Is the Standard Artificial Urinary Sphincter AMS 800 Still a Treatment Option for the Irradiated Male Patient Presenting with a Devastated Bladder Outlet?
Abstract
1. Introduction
2. Materials and Methods
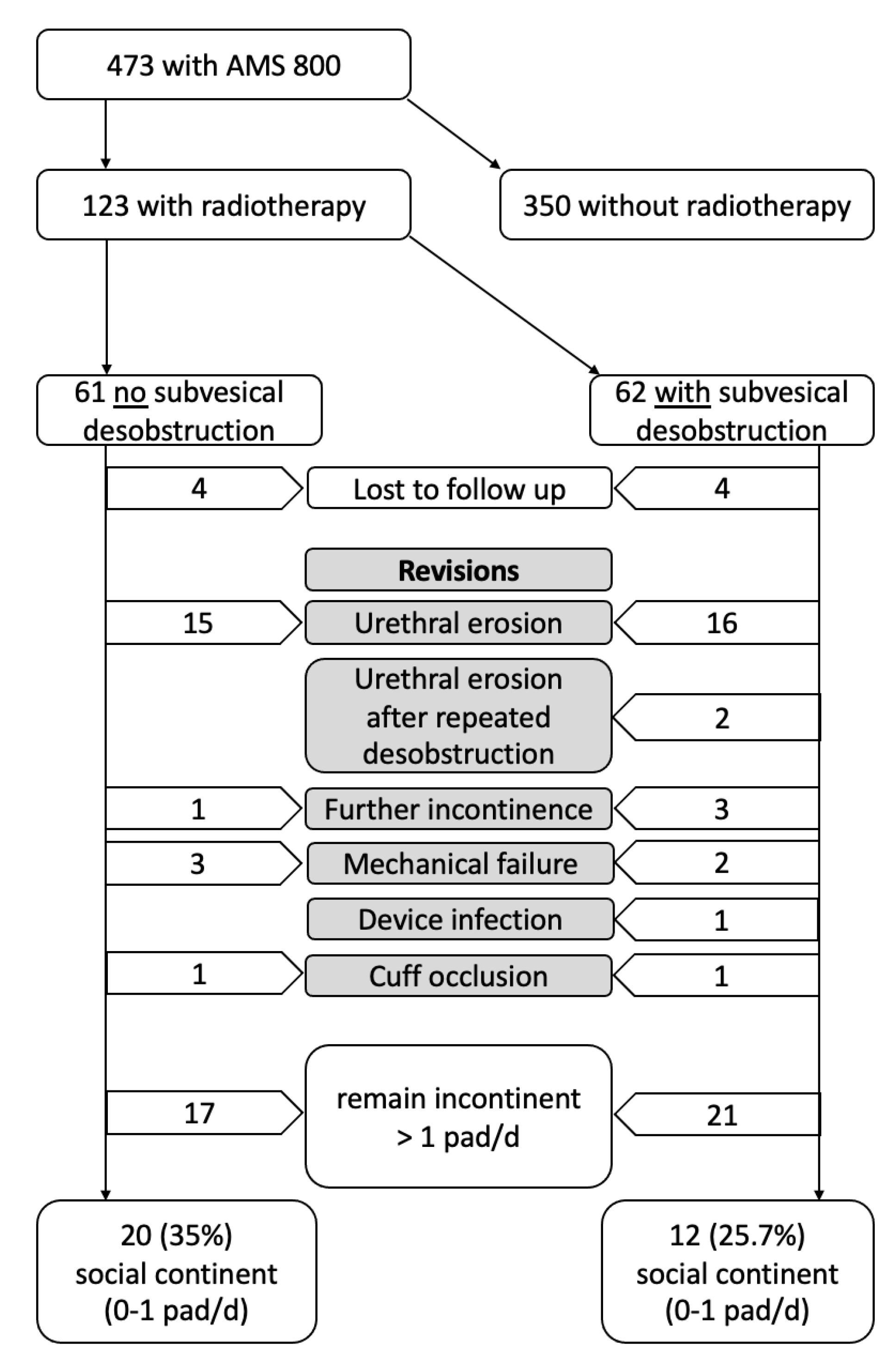
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Gacci, M.; Sakalis, V.I.; Karavitakis, M.; Cornu, J.N.; Gratzke, C.; Herrmann, T.R.; Kyriazis, I.; Malde, S.; Mamoulakis, C.; Rieken, M.; et al. European Association of Urology Guidelines on Male Urinary Incontinence. Eur. Urol. 2022, 82, 387–398. [Google Scholar] [CrossRef] [PubMed]
- Bresolin, A.; Garibaldi, E.; Faiella, A.; Cante, D.; Vavassori, V.; Waskiewicz, J.M.; Girelli, G.; Avuzzi, B.; Villa, E.; Magli, A.; et al. Predictors of 2-Year Incidence of Patient-Reported Urinary Incontinence After Post-Prostatectomy Radiotherapy: Evidence of Dose and Fractionation Effects. Front. Oncol. 2020, 10, 1207. [Google Scholar] [CrossRef] [PubMed]
- Hughes, M.; Caza, T.; Li, G.; Daugherty, M.; Blakley, S.; Nikolavsky, D. Histologic characterization of the post-radiation urethral stenosis in men treated for prostate cancer. World J. Urol. 2020, 38, 2269–2277. [Google Scholar] [CrossRef] [PubMed]
- Nicholson, H.L.; Al-Hakeem, Y.; Maldonado, J.J.; Tse, V. Management of bladder neck stenosis and urethral stricture and stenosis following treatment for prostate cancer. Transl. Androl. Urol. 2017, 6 (Suppl. 2), S92–S102. [Google Scholar] [CrossRef] [PubMed]
- Browne, B.M.; Vanni, A.J. Management of Urethral Stricture and Bladder Neck Contracture Following Primary and Salvage Treatment of Prostate Cancer. Curr. Urol. Rep. 2017, 18, 76. [Google Scholar] [CrossRef]
- Riedmiller, H.; Kocot, A. The devastated bladder outlet: Treatment options. Curr. Opin. Urol. 2015, 25, 352–356. [Google Scholar] [CrossRef]
- Martins, F.E.; Holm, H.V.; Lumen, N. Devastated Bladder Outlet in Pelvic Cancer Survivors: Issues on Surgical Reconstruction and Quality of Life. J. Clin. Med. 2021, 10, 4920. [Google Scholar] [CrossRef]
- Meeks, J.J.; Brandes, S.B.; Morey, A.F.; Thom, M.; Mehdiratta, N.; Valadez, C.; Granieri, M.A.; Gonzalez, C.M. Urethroplasty for radiotherapy induced bulbomembranous strictures: A multi-institutional experience. J. Urol. 2011, 185, 1761–1765. [Google Scholar] [CrossRef]
- Ojima, K.; Horiguchi, A.; Shinchi, M.; Tabei, T.; Hirano, Y.; Ito, K.; Azuma, R. Transperineal bulbovesical anastomosis for extensive posterior urethral stenoses after treatment of prostatic disease. Int. J. Urol. 2022, 29, 1511–1516. [Google Scholar] [CrossRef]
- Munoz, F.; Sanguineti, G.; Bresolin, A.; Cante, D.; Vavassori, V.; Waskiewicz, J.M.; Girelli, G.; Avuzzi, B.; Garibaldi, E.; Faiella, A.; et al. Predictors of Patient-Reported Incontinence at Adjuvant/Salvage Radiotherapy after Prostatectomy: Impact of Time between Surgery and Radiotherapy. Cancers 2021, 13, 3243. [Google Scholar] [CrossRef]
- Hüsch, T.; Kretschmer, A.; Thomsen, F.; Kronlachner, D.; Kurosch, M.; Obaje, A.; Anding, R.; Pottek, T.; Rose, A.; Olianas, R.; et al. Risk Factors for Failure of Male Slings and Artificial Urinary Sphincters: Results from a Large Middle European Cohort Study. Urol. Int. 2017, 99, 14–21. [Google Scholar] [CrossRef]
- Kim, J.H.; Jenrow, K.A.; Brown, S.L. Mechanisms of radiation-induced normal tissue toxicity and implications for future clinical trials. Radiat. Oncol. J. 2014, 32, 103–115. [Google Scholar] [CrossRef]
- Sayedahmed, K.; Olianas, R.; Kaftan, B.; Omar, M.; El Shazly, M.; Burger, M.; Mayr, R.; Rosenhammer, B. Impact of previous urethroplasty on the outcome after artificial urinary sphincter implantation: A prospective evaluation. World J. Urol. 2020, 38, 183–191. [Google Scholar] [CrossRef]
- Simonato, A.; Gregori, A.; Lissiani, A.; Carmignani, G. Two-stage transperineal management of posterior urethral strictures or bladder neck contractures associated with urinary incontinence after prostate surgery and endoscopic treatment failures. Eur. Urol. 2007, 52, 1499–1504. [Google Scholar] [CrossRef]
- McGeady, J.B.; McAninch, J.W.; Truesdale, M.D.; Blaschko, S.D.; Kenfield, S.; Breyer, B.N. Artificial urinary sphincter placement in compromised urethras and survival: A comparison of virgin, irradiated and reoperative cases. J. Urol. 2014, 192, 1756–1761. [Google Scholar] [CrossRef]
- Mann, R.A.; Kasabwala, K.; Buckley, J.C.; Smith, T.G.; Westney, O.L.; Amend, G.M.; Breyer, B.N.; Erickson, B.A.; Alsikafi, N.F.; Broghammer, A.J.; et al. The “Fragile” Urethra as a Predictor of Early Artificial Urinary Sphincter Erosion. Urology 2022, 169, 233–236. [Google Scholar] [CrossRef]
- El-Akri, M.; Bentellis, I.; Tricard, T.; Brierre, T.; Cousin, T.; Dupuis, H.; Hermieu, N.; Gaillard, V.; Poussot, B.; Robin, D.; et al. Transcorporal vs. bulbar artificial urinary sphincter implantation in male patients with fragile urethra. World J. Urol. 2021, 39, 4449–4457. [Google Scholar] [CrossRef]
- Redmond, E.; Rourke, K.F.; Tong, S.; Zemp, L.; Hoy, N. Improved artificial urinary sphincter outcomes using a transcorporal cuff placement in patients with a “fragile urethra”. Can. Urol. Assoc. J. 2020, 14, E621–E624. [Google Scholar] [CrossRef]
- Hoy, N.Y.; Rourke, K.F. Artificial Urinary Sphincter Outcomes in the “Fragile Urethra”. Urology 2015, 86, 618–624. [Google Scholar] [CrossRef]
- Long, E.L.; Rebibo, J.D.; Nouhaud, F.X.; Grise, P. Transcorporal artificial urinary sphincter in irradiated and non-irradiated compromised urethra. Assessment with a minimum 2 year follow-up. Int. Braz. J. Urol. 2016, 42, 494–500. [Google Scholar] [CrossRef]
- Wiedemann, L.; Cornu, J.-N.; Haab, E.; Peyrat, L.; Beley, S.; Cathelineau, X.; Haab, F. Transcorporal artificial urinary sphincter implantation as a salvage surgical procedure for challenging cases of male stress urinary incontinence: Surgical technique and functional outcomes in a contemporary series. BJU Int. 2013, 112, 1163–1168. [Google Scholar] [CrossRef] [PubMed]
- Miller, D.; Pekala, K.; Zhang, X.; Orikogbo, O.; Rogers, D.; Fuller, T.W.; Maganty, A.; Rusilko, P. Outcomes of Initial Transcorporal Versus Standard Placement of Artificial Urinary Sphincter in Patients With Prior Radiation. Cureus 2022, 14, e25519. [Google Scholar] [CrossRef] [PubMed]
- Guralnick, M.L.; Miller, E.; Toh, K.L.; Webster, G.D. Transcorporal artificial urinary sphincter cuff placement in cases requiring revision for erosion and urethral atrophy. J. Urol. 2002, 167, 2075–2078, discussion 2079. [Google Scholar] [CrossRef] [PubMed]
- Ortiz, N.M.; Wolfe, A.R.; Baumgarten, A.S.; Ward, E.E.; VanDyke, M.E.; Hudak, S.J.; Morey, A.F. Artificial Urinary Sphincter Cuff Erosion Heat Map Shows Similar Anatomical Characteristics for Transcorporal and Standard Approach. J. Urol. 2020, 204, 1027–1032. [Google Scholar] [CrossRef]
- Queissert, F.; Huesch, T.; Kretschmer, A.; Anding, R.; Kurosch, M.; Kirschner-Hermanns, R.; Pottek, T.; Olianas, R.; Friedl, A.; Pfitzenmaier, J.; et al. Artificial Urinary Sphincter Cuff Size Predicts Outcome in Male Patients Treated for Stress Incontinence: Results of a Large Central European Multicenter Cohort Study. Int. Neurourol. J. 2019, 23, 219–225. [Google Scholar] [CrossRef]
- Ullate, A.; Arance, I.; Virseda-Chamorro, M.; Ruiz, S.; Szczesniewski, J.; Téllez, C.; Queissert, F.; Dorado, J.F.; Angulo, J.C. ATOMS (Adjustable Trans-Obturator Male System) in Patients with Post-Prostatectomy Incontinence and Previously Treated Urethral Stricture or Bladder Neck Contracture. J. Clin. Med. 2022, 11, 4882. [Google Scholar] [CrossRef]
- Agarwal, D.K.; Linder, B.J.; Elliott, D.S. Artificial urinary sphincter urethral erosions: Temporal patterns, management, and incidence of preventable erosions. Indian J. Urol. 2017, 33, 26–29. [Google Scholar]
- Weissbart, S.J.; Chughtai, B.; Elterman, D.; Sandhu, J.S. Management of anastomotic stricture after artificial urinary sphincter placement in patients who underwent salvage prostatectomy. Urology 2013, 82, 476–479. [Google Scholar] [CrossRef]
- Ramirez, D.; Simhan, J.; Hudak, S.J.; Morey, A.F. Standardized approach for the treatment of refractory bladder neck contractures. Urol. Clin. N. Am. 2013, 40, 371–380. [Google Scholar] [CrossRef]
- Myers, J.B.; Brant, W.O.; Hotaling, J.N.; Lenherr, S.M. Urethral Strictures and Artificial Urinary Sphincter Placement. Urol. Clin. N. Am. 2017, 44, 93–103. [Google Scholar] [CrossRef]

| RT Only | RT and Surgery for mU/BN Stenosis | ||
|---|---|---|---|
| Pat. (n) | 61 | 62 | |
| Age (mean) | 75.5 (± 6.8) | 74.4 (± 6.0) | p = 0.3 * |
| BMI (mean) | 28.6 (± 4.9) | 28.0 (± 4.2) | p = 0.4 * |
| Diab. mel. (n) | 16 (26.2%) | 10 (16.1%) | p = 0.17 ** |
| Brachytherapy (n) | 1 (1.6%) | 2 (3.2%) | p = 1 ** |
| External irradiation | 60 (98.4%) | 60 (96.8%) | p = 1 ** |
| Prior incontinence surgery | 19 (31.1%) | 19 (30.6%) | p = 1 ** |
| >1 prior surgery | 6 (9.8%) | 3 (4.8%) | p = 0.3 ** |
| Bulking agent | 4 (6.7%) | 4 (6.5%) | p = 1 ** |
| Fixed sling | 8 (13.1%) | 6 (9.7%) | p = 0.6 ** |
| Adjustable sling | 4 (6.7%) | 3 (4.8%) | p = 0.7 ** |
| proAct | 2 (3.2%) | 0 | p = 0.2 ** |
| AUS | 6 (9.8%) | 7 (11.3%) | p = 1 ** |
| RT Only | RT and Surgery for mU/BN Stenosis | ||
| Prior surgery for mU/BN Stenosis | |||
| n > 1 | 33 (53.2%) | ||
| UI | 29 (46.8%) | ||
| Bladder-neck resection/incision | 32 (51.6%) | ||
| Stent | 5 (8.1%) | ||
| Open urethroplasty | 7 (11.3%) | ||
| AUS surgery | |||
| SC | 26 (42.6%) | 30 (48.4%) | p = 0.6 ** |
| DC | 35 (57.4%) | 32 (51.6%) | p = 0.6 ** |
| Perineal | 44 (72.1%) | 50 (80.6%) | p = 0.3 ** |
| Penoscrotal | 17 (27.9% | 12 (19.4%) | p = 0.3 ** |
| TC | unknown | 10 of 41 (24.4%) | |
| Cuff size (cm, mean) | 4.26 | 4.48 | p = 0.03 *** |
| Cuff 3.5 cm | 4 (6.7%) | 7 (11.3%) | p = 0.4 *** |
| RT Only | RT and Surgery for mU/BN Stenosis | ||
|---|---|---|---|
| Lost to follow-up | 4 (6.6%) | 4 (6.5%) | |
| Follow-up (mean month) | 20.5 | 21.5 | |
| Revisions | 15 (26.3%) | 25 (43.1%) | p = 0.05 * |
| Erosion | 11 (17.5%) | 18 (31.0%) | p = 0.15 * |
| Incontinence | 1 (1.8%) | 3 (5.2%) | p = 0.3 * |
| Mechanical failure | 3 (5.3%) | 2 (3.4%) | p = 0.6 * |
| Infection | 0 | 1 (1.7%) | p = 0.3 * |
| Cuff occlusion | 1 (1.8%) | 1 (1.7%) | p = 1 * |
| Functional outcome | |||
| Social continence (0–1 pad/24 h) | 20 (35.0%) | 12 (25.7%) | p = 0.08 * |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Queissert, F.; Huesch, T.; Kretschmer, A.; Kirschner-Hermanns, R.; Pottek, T.; Olianas, R.; Friedl, A.; Homberg, R.; Pfitzenmaier, J.; Naumann, C.M.; et al. Is the Standard Artificial Urinary Sphincter AMS 800 Still a Treatment Option for the Irradiated Male Patient Presenting with a Devastated Bladder Outlet? J. Clin. Med. 2023, 12, 4002. https://doi.org/10.3390/jcm12124002
Queissert F, Huesch T, Kretschmer A, Kirschner-Hermanns R, Pottek T, Olianas R, Friedl A, Homberg R, Pfitzenmaier J, Naumann CM, et al. Is the Standard Artificial Urinary Sphincter AMS 800 Still a Treatment Option for the Irradiated Male Patient Presenting with a Devastated Bladder Outlet? Journal of Clinical Medicine. 2023; 12(12):4002. https://doi.org/10.3390/jcm12124002
Chicago/Turabian StyleQueissert, Fabian, Tanja Huesch, Alexander Kretschmer, Ruth Kirschner-Hermanns, Tobias Pottek, Roberto Olianas, Alexander Friedl, Roland Homberg, Jesco Pfitzenmaier, Carsten M. Naumann, and et al. 2023. "Is the Standard Artificial Urinary Sphincter AMS 800 Still a Treatment Option for the Irradiated Male Patient Presenting with a Devastated Bladder Outlet?" Journal of Clinical Medicine 12, no. 12: 4002. https://doi.org/10.3390/jcm12124002
APA StyleQueissert, F., Huesch, T., Kretschmer, A., Kirschner-Hermanns, R., Pottek, T., Olianas, R., Friedl, A., Homberg, R., Pfitzenmaier, J., Naumann, C. M., Nyarangi-Dix, J., Hofmann, T., Rose, A., Weidemann, C., Wotzka, C., Hübner, W., Loertzer, H., Abdunnur, R., Grabbert, M., ... Schrader, A. J., on behalf of the Debates on Male Incontinence (DOMINO)-Project. (2023). Is the Standard Artificial Urinary Sphincter AMS 800 Still a Treatment Option for the Irradiated Male Patient Presenting with a Devastated Bladder Outlet? Journal of Clinical Medicine, 12(12), 4002. https://doi.org/10.3390/jcm12124002








