In Vitro Anti-Inflammatory Potential of Pomegranate Extract (Pomanox®) in a Reconstituted Human Corneal Epithelium Model
Abstract
1. Introduction
2. Materials and Methods
2.1. Reconstituted Human Corneal Epithelium
2.2. In Vitro Assay
2.3. Study Variables and Assessment of Response
2.4. Statistical Analysis
3. Results
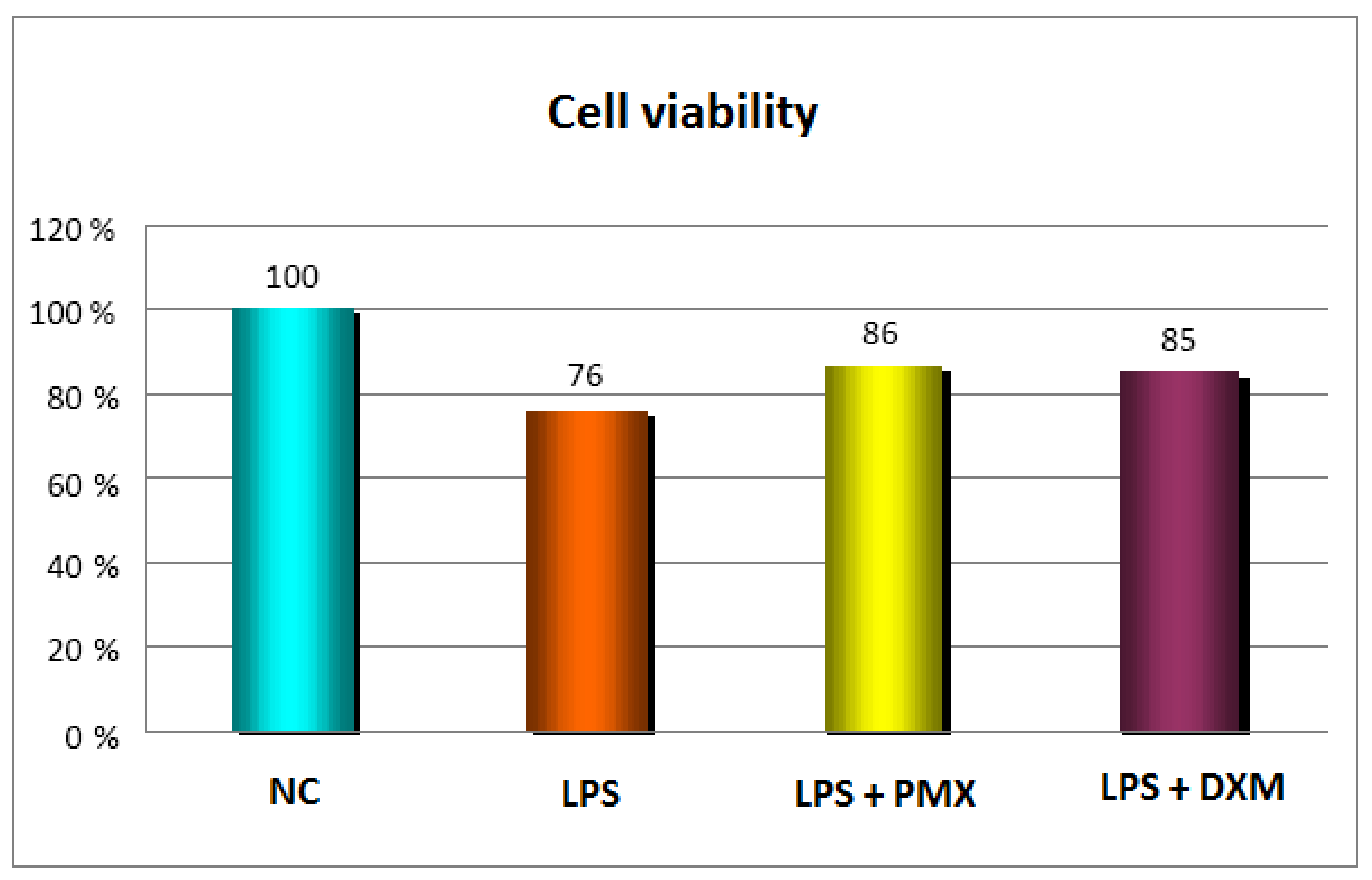
3.1. Cell Viability
3.2. Release of IL-8
3.3. Extrapolation of the Inhibition of IL-8 Release
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Zhang, J.; Wu, X.Y.; Yu, F.S. Inflammatory responses of corneal epithelial cells to Pseudomonas aeruginosa infection. Curr. Eye Res. 2005, 30, 527–534. [Google Scholar] [CrossRef]
- Kumar, A.; Zhang, J.; Yu, F.S. Innate immune response of corneal epithelial cells to Staphylococcus aureus infection: Role of peptidoglycan in stimulating proinflammatory cytokine secretion. Investig. Ophthalmol. Vis. Sci. 2004, 45, 3513–3522. [Google Scholar] [CrossRef] [PubMed]
- Matsushima, K.; Oppenheim, J.J. Interleukin 8 and MCAF: Novel inflammatory cytokines inducible by IL 1 and TNF. Cytokine 1989, 1, 2–13. [Google Scholar] [CrossRef] [PubMed]
- Larsen, C.; Zachariae, C.; Mukaida, N.; Anderson, A.; Yamada, M.; Oppenheim, J.; Matsushima, K. Proinflammatory cytokines interleukin 1 and tumor necrosis factor induce cytokines that are chemotactic for neutrophils, T cells and monocytes. Prog. Clin. Biol. Res. 1990, 349, 419–431. [Google Scholar] [PubMed]
- Qazi, B.S.; Tang, K.; Qazi, A. Recent advances in underlying pathologies provide insight into interleukin-8 expression-mediated inflammation and angiogenesis. Int. J. Inflam. 2011, 2011, 908468. [Google Scholar] [CrossRef]
- Cubitt, C.L.; Tang, Q.; Monteiro, C.A.; Lausch, R.N.; Oakes, J.E. IL-8 gene expression in cultures of human corneal epithelial cells and keratocytes. Investig. Ophthalmol. Vis. Sci. 1993, 34, 3199–31206. [Google Scholar]
- Elner, V.M.; Strieter, R.M.; Pavilack, M.A.; Elner, S.G.; Remick, D.G.; Danforth, J.M.; Kunkel, S.L. Human corneal interleukin-8. IL-1 and TNF-induced gene expression and secretion. Am. J. Pathol. 1991, 139, 977–988. [Google Scholar]
- Oka, M.; Norose, K.; Matsushima, K.; Nishigori, C.; Herlyn, M. Overexpression of IL-8 in the cornea induces ulcer formation in the SCID mouse. Br. J. Ophthalmol. 2006, 90, 612–615. [Google Scholar] [CrossRef]
- Oakes, J.E.; Monteiro, C.A.; Cubitt, C.L.; Lausch, R.N. Induction of interleukin-8 gene expression is associated with herpes simplex virus infection of human corneal keratocytes but not human corneal epithelial cells. J. Virol. 1993, 67, 4777–4784. [Google Scholar] [CrossRef]
- Mo, Y.; Ma, J.; Gao, W.; Zhang, L.; Li, J.; Li, J.; Zang, J. Pomegranate peel as a source of bioactive compounds: A mini review on their physiological functions. Front. Nutr. 2022, 9, 887113. [Google Scholar] [CrossRef]
- Bishayee, A.; Thoppil, R.J.; Darvesh, A.S.; Ohanyan, V.; Meszaros, J.G.; Bhatia, D. Pomegranate phytoconstituents blunt the inflammatory cascade in a chemically induced rodent model of hepatocellular carcinogenesis. J. Nutr. Biochem. 2013, 24, 178–187. [Google Scholar] [CrossRef] [PubMed]
- Mehdi, A.; Lamiae, B.; Samira, B.; Ramchoun, M.; Abdelouahed, K.; Tamas, F.; Hicham, B. Pomegranate (Punica granatum L.) Attenuates neuroinflammation involved in neurodegenerative diseases. Foods 2022, 11, 2570. [Google Scholar] [CrossRef] [PubMed]
- Kalaycıoğlu, Z.; Erim, F.B. Total phenolic contents, antioxidant activities, and bioactive ingredients of juices from pomegranate cultivars worldwide. Food Chem. 2017, 221, 496–507. [Google Scholar] [CrossRef] [PubMed]
- Lorzadeh, E.; Heidary, Z.; Mohammadi, M.; Nadjarzadeh, A.; Ramezani-Jolfaie, N.; Salehi-Abargouei, A. Does pomegranate consumption improve oxidative stress? A systematic review and meta-analysis of randomized controlled clinical trials. Clin. Nutr. ESPEN 2022, 47, 117–127. [Google Scholar] [CrossRef]
- Vučić, V.; Grabež, M.; Trchounian, A.; Arsić, A. Composition and potential health benefits of pomegranate: A review. Curr. Pharm. Des. 2019, 25, 1817–1827. [Google Scholar] [CrossRef]
- Akuru, E.A.; Chukwuma, C.I.; Oyeagu, C.E.; Erukainure, O.L.; Mashile, B.; Setlhodi, R.; Mashele, S.S.; Makhafola, T.J.; Unuofin, J.O.; Abifarin, T.O.; et al. Nutritional and phytochemical profile of pomegranate ("Wonderful variety") peel and its effects on hepatic oxidative stress and metabolic alterations. J. Food Biochem. 2022, 46, e13913. [Google Scholar] [CrossRef]
- Stockton, A.; Al-Dujaili, E.; McDougall, G.; Davidson, I.; Drummond, S.; Wyness, L. Effect of pomegranate extract consumption on cardiovascular disease risk factors, stress hormones, and quality of life in human volunteers: An exploratory randomised, double-blind, placebo-controlled trial. EC Nutr. 2015, 2, 396–411. [Google Scholar]
- Tomás-Barberán, F.A.; González-Sarrías, A.; García-Villalba, R.; Núñez-Sánchez, M.A.; Selma, M.V.; García-Conesa, M.T.; Espín, J.C. Urolithins, the rescue of “old” metabolites to understand a “new” concept: Metabotypes as a nexus among phenolic metabolism, microbiota dysbiosis, and host health status. Mol. Nutr. Food Res. 2017, 61, 1500901. [Google Scholar] [CrossRef]
- Eghbali, S.; Askari, S.F.; Avan, R.; Sahebkar, A. Therapeutic effects of Punica granatum (Pomegranate): An updated review of clinical trials. J. Nutr. Metab. 2021, 2021, 5297162. [Google Scholar] [CrossRef]
- González-Ortiz, M.; Martínez-Abundis, E.; Espinel-Bermúdez, M.C.; Pérez-Rubio, K.G. Effect of pomegranate juice on insulin secretion and sensitivity in patients with obesity. Ann. Nutr. Metab. 2011, 58, 220–223. [Google Scholar] [CrossRef]
- Al-Dujaili, E.A.S.; Casey, C.; Stockton, A. Antioxidant properties and beneficial cardiovascular effects of a natural extract of pomegranate in healthy volunteers: A randomized preliminary single-blind controlled study. Antioxidants 2022, 11, 2124. [Google Scholar] [CrossRef] [PubMed]
- Stockton, A.; Al-Dujaili, E.A.S. Effect of pomegranate extract consumption on satiety parameters in healthy volunteers: A preliminary randomized study. Foods 2022, 11, 2639. [Google Scholar] [CrossRef]
- Stockton, A.V.E.; Zangara, A.; Al-Dujaili, E.A.S. Investigating the acute effect of pomegranate extract on indicators of cognitive function in human volunteers: A double-blind, placebo-controlled crossover trial. In Nutraceuticals in Brain Health and Beyond; Ghosh, D., Ed.; Academic Press: Cambridge, MA, USA, 2021; pp. 141–154. [Google Scholar] [CrossRef]
- Torregrosa-García, A.; Ávila-Gandía, V.; Luque-Rubia, A.J.; Abellán-Ruiz, M.S.; Querol-Calderón, M.; López-Román, F.J. Pomegranate extract improves maximal performance of trained cyclists after an exhausting endurance trial: A randomised controlled trial. Nutrients 2019, 11, 721. [Google Scholar] [CrossRef]
- Kamal, E.-N.S.; Gomaa, A.M.; Aziz, M.A.; Ebrahim, N.F.; Ahmed, S.S. The protective effect of Punica granatum (pomegranate) against glaucoma development. Saudi J. Health Sci. 2015, 4, 171–178. [Google Scholar] [CrossRef]
- Belal, S.K.M.; Al Ghamdi, A. Protective effect of pomegranate peel extract on diabetic ocular structural changes in experimental diabetic rats: A histological, immunohistochemical and clinical study. Adv. Med. Plant Res. 2021, 9, 11–21. [Google Scholar] [CrossRef]
- Hashem, H.E.; El-Haleem, M.R.A.; Amer, M.G.; Bor’I, A. Pomegranate protective effect on experimental ischemia/reperfusion retinal injury in rats (histological and biochemical study). Ultrastruct. Pathol. 2017, 41, 346–357. [Google Scholar] [CrossRef]
- Ceriotti, L.; Balzaretti, S.; Barone, S.; Meloni, M. Eye irritation potential of microglycine and microglycine-containing ointments: An in vitro study on reconstructed human corneal epithelium. Clin. Ophthalmol. 2020, 14, 257–267. [Google Scholar] [CrossRef]
- Cotovio, J.; Grandidier, M.H.; Lelièvre, D.; Bremond, C.; Amsellem, C.; Maloug, S.; Ovigne, J.M.; Loisel-Joubert, S.; Lee, A.V.; Minondo, A.M.; et al. In vitro assessment of eye irritancy using the Reconstructed Human Corneal Epithelial SkinEthic HCE model: Application to 435 substances from consumer products industry. Toxicol. Vitr. 2010, 24, 523–537. [Google Scholar] [CrossRef]
- Cao, Y.; Bindslev, D.A.; Kjærgaard, S.K. Estimation of the in vitro eye irritating and inflammatory potential of lipopolysaccharide (LPS) and dust by using reconstituted human corneal epithelium tissue cultures. Toxicol. Mech. Methods 2015, 25, 402–409. [Google Scholar] [CrossRef]
- Alépée, N.; Leblanc, V.; Grandidier, M.H.; Teluob, S.; Viricel, A.; Adriaens, E.; Michaut, V. SkinEthic HCE time-to-toxicity on solids: A test method for distinguishing chemicals inducing serious eye damage, eye irritation and not requiring classification and labelling. Toxicol. Vitr. 2021, 75, 105203. [Google Scholar] [CrossRef] [PubMed]
- Alépée, N.; Leblanc, V.; Adriaens, E.; Grandidier, M.H.; Lelièvre, D.; Meloni, M.; Nardelli, L.; Roper, C.S.; Santirocco, E.; Toner, F.; et al. Multi-laboratory validation of SkinEthic HCE test method for testing serious eye damage/eye irritation using liquid chemicals. Toxicol. Vitr. 2016, 31, 43–53. [Google Scholar] [CrossRef] [PubMed]
- Doucet, O.; Lanvin, M.; Thillou, C.; Linossier, C.; Pupat, C.; Merlin, B.; Zastrow, L. Reconstituted human corneal epithelium: A new alternative to the Draize eye test for the assessment of the eye irritation potential of chemicals and cosmetic products. Toxicol. Vitr. 2006, 20, 499–512. [Google Scholar] [CrossRef] [PubMed]
- Lopez Más, J.A.; Streitenberger, S.A.; Peñalver Mellado, M.; Martínez Ortís, P. Process for Preparing Pomegranate Extract. European Patent Specification EP1967079B1; filed 7 March 2008, 27 October 2010. [Google Scholar]
- Tornier, C.; Rosdy, M.; Maibach, H.I. In vitro skin irritation testing on reconstituted human epidermis: Reproducibility for 50 chemicals tested with two protocols. Toxicol. Vitr. 2006, 20, 401–416. [Google Scholar] [CrossRef] [PubMed]
- Rönkkö, S.; Vellonen, K.S.; Järvinen, K.; Toropainen, E.; Urtti, A. Human corneal cell culture models for drug toxicity studies. Drug Deliv. Transl. Res. 2016, 6, 660–675. [Google Scholar] [CrossRef]
- Clementi, M.E.; Maulucci, G.; Bianchetti, G.; Pizzoferrato, M.; Sampaolese, B.; Tringali, G. Cytoprotective effects of punicalagin on hydrogen-peroxide-mediated oxidative stress and mitochondrial dysfunction in retinal pigment epithelium cells. Antioxidants 2021, 10, 192. [Google Scholar] [CrossRef]
- Xu, J.; Cao, K.; Liu, X.; Zhao, L.; Feng, Z.; Liu, J. Punicalagin regulates signaling pathways in inflammation-associated chronic diseases. Antioxidants 2021, 11, 29. [Google Scholar] [CrossRef]
- Huang, M.; Wu, K.; Zeng, S.; Liu, W.; Cui, T.; Chen, Z.; Lin, L.; Chen, D.; Ouyang, H. Punicalagin inhibited inflammation and migration of fibroblast-like synoviocytes through NF-κB pathway in the experimental study of rheumatoid arthritis. J. Inflamm. Res. 2021, 14, 1901–1913. [Google Scholar] [CrossRef]
- Cao, Y.; Chen, J.; Ren, G.; Zhang, Y.; Tan, X.; Yang, L. Punicalagin prevents inflammation in LPS-induced RAW264.7 macrophages by inhibiting FoxO3a/Autophagy signaling pathway. Nutrients 2019, 11, 2794. [Google Scholar] [CrossRef]
- Venusova, E.; Kolesarova, A.; Horky, P.; Slama, P. Physiological and immune functions of punicalagin. Nutrients 2021, 13, 2150. [Google Scholar] [CrossRef]
- Hollebeeck, S.; Winand, J.; Hérent, M.F.; During, A.; Leclercq, J.; Larondelle, Y.; Schneider, Y.J. Anti-inflammatory effects of pomegranate (Punica granatum L.) husk ellagitannins in Caco-2 cells, an in vitro model of human intestine. Food Funct. 2012, 3, 875–885. [Google Scholar] [CrossRef]
- BenSaad, L.A.; Kim, K.H.; Quah, C.C.; Kim, W.R.; Shahimi, M. Anti-inflammatory potential of ellagic acid, gallic acid and punicalagin A&B isolated from Punica granatum. BMC Complement. Altern. Med. 2017, 17, 47. [Google Scholar] [CrossRef]
- Rodriguez, J.; Caille, O.; Ferreira, D.; Francaux, M. Pomegranate extract prevents skeletal muscle of mice against wasting induced by acute TNF-α injection. Mol. Nutr. Food Res. 2017, 61, 1600169. [Google Scholar] [CrossRef] [PubMed]
- Vilahur, G.; Padró, T.; Casaní, L.; Mendieta, G.; López, J.A.; Streitenberger, S.; Badimon, L. Polyphenol-enriched diet prevents coronary endothelial dysfunction by activating the Akt/eNOS pathway. Rev. Esp. Cardiol. 2015, 68, 216–225. [Google Scholar] [CrossRef]
- Mariné-Casadó, R.; Teichenné, J.; Tobajas, Y.; Caimari, A.; Villar, A.; Zangara, A.; Mulà, A.; Del Bas, J.M. Pomegranate natural extract Pomanox® positively modulates skin health-related parameters in normal and UV-induced photoaging conditions in Hs68 human fibroblast cells. Int. J. Food Sci. Nutr. 2022, 74, 51–63. [Google Scholar] [CrossRef] [PubMed]

| Test Condition | IL-8 Levels, pg/mL | |
|---|---|---|
| Mean ± SEM | 95% CI | |
| Negative control (PBS), n = 3 | 26.6 ± 1.2 | 21.6 to 31.7 |
| Positive inflammatory control (LPS E. coli), n = 4 | 172.7 ± 19.3 | 111.2 to 234.2 |
| Positive anti-inflammatory control (LPS + DXM), n = 2 | 93.8 ± 8.7 | −17.1 to 204.7 |
| Test sample (LPS + PMX), n = 4 | 48.7 ± 5.1 | 32.6 to 64.8 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Peñalver-Mellado, M.; Silva-Fuentes, F.; Villar, A.; Mula, A.; Zangara, A. In Vitro Anti-Inflammatory Potential of Pomegranate Extract (Pomanox®) in a Reconstituted Human Corneal Epithelium Model. J. Clin. Transl. Ophthalmol. 2023, 1, 52-60. https://doi.org/10.3390/jcto1020007
Peñalver-Mellado M, Silva-Fuentes F, Villar A, Mula A, Zangara A. In Vitro Anti-Inflammatory Potential of Pomegranate Extract (Pomanox®) in a Reconstituted Human Corneal Epithelium Model. Journal of Clinical & Translational Ophthalmology. 2023; 1(2):52-60. https://doi.org/10.3390/jcto1020007
Chicago/Turabian StylePeñalver-Mellado, Marcos, Fredy Silva-Fuentes, Agustín Villar, Anna Mula, and Andrea Zangara. 2023. "In Vitro Anti-Inflammatory Potential of Pomegranate Extract (Pomanox®) in a Reconstituted Human Corneal Epithelium Model" Journal of Clinical & Translational Ophthalmology 1, no. 2: 52-60. https://doi.org/10.3390/jcto1020007
APA StylePeñalver-Mellado, M., Silva-Fuentes, F., Villar, A., Mula, A., & Zangara, A. (2023). In Vitro Anti-Inflammatory Potential of Pomegranate Extract (Pomanox®) in a Reconstituted Human Corneal Epithelium Model. Journal of Clinical & Translational Ophthalmology, 1(2), 52-60. https://doi.org/10.3390/jcto1020007








