An Approach to 3D Printing Techniques, Polymer Materials, and Their Applications in the Production of Drug Delivery Systems
Abstract
1. Introduction
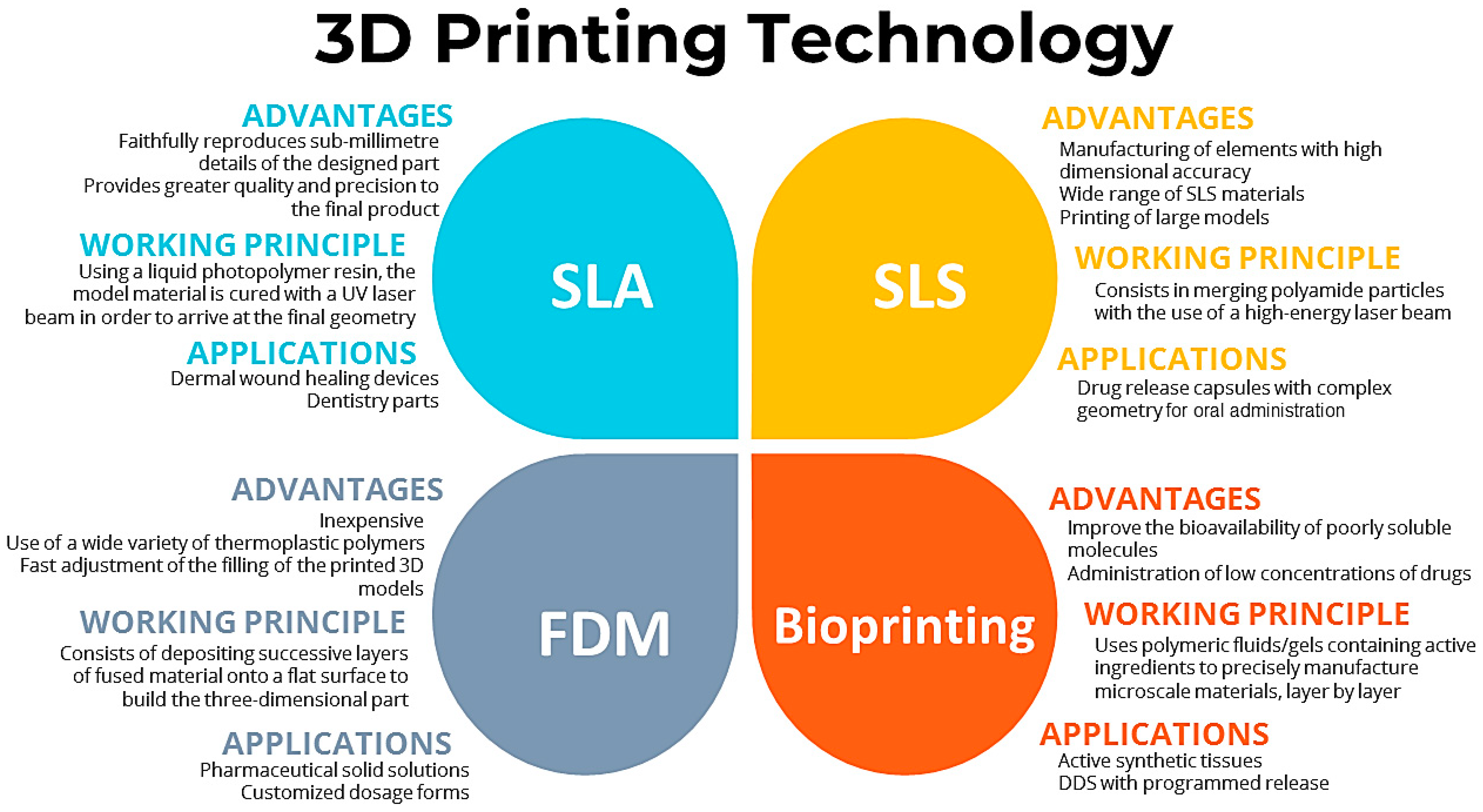
2. Three-Dimensional (3D) Printing Techniques
2.1. Stereolithography (SLA)
2.2. Selective Laser Sintering (SLS)
2.3. Fused Deposition Modeling (FDM)
2.4. Bioprinting
3. Polymers
3.1. Synthetic Biopolymers
3.1.1. Polyvinyl Alcohol (PVA)
3.1.2. Poly(vinyl pyrrolidone) (PVP)
3.1.3. Polyethylene Glycol
3.1.4. Polyurethane (PU)
3.1.5. Poly(lactic acid)
3.1.6. Poly(lactide-co-glycolide)
3.1.7. Polycaprolactone
3.2. Natural Biopolymers
3.2.1. Polysaccharides
Chitosan
Hyaluronic Acid
Cellulose
3.2.2. Proteins
4. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Kantaros, A.; Ganetsos, T.; Petrescu, F.I.T. Three-Dimensional Printing and 3D Scanning: Emerging Technologies Exhibiting High Potential in the Field of Cultural Heritage. Appl. Sci. 2023, 13, 4777. [Google Scholar] [CrossRef]
- Shishatskaya, E.I.; Demidenko, A.V.; Sukovatyi, A.G.; Dudaev, A.E.; Mylnikov, A.V.; Kisterskij, K.A.; Volova, T.G. Three-Dimensional Printing of Poly (3-hydroxybutyrate-co-3-hydroxyvalerate)[P (3HB-co-3HV)] Biodegradable Scaffolds: Properties, In Vitro and In Vivo Evaluation. Int. J. Mol. Sci. 2023, 24, 12969. [Google Scholar] [CrossRef] [PubMed]
- Lakkala, P.; Munnangi, S.R.; Bandari, S.; Repka, M. Additive manufacturing technologies with emphasis on stereolithography 3D printing in pharmaceutical and medical applications: A review. Int. J. Pharm. X 2023, 5, 100159. [Google Scholar] [CrossRef]
- Surini, S.; Bimawanti, Y.; Kurniawan, A. The Application of Polymers in Fabricating 3D Printing Tablets by Fused Deposition Modeling (FDM) and The Impact on Drug Release Profile. Pharm. Sci. 2023, 29, 156–164. [Google Scholar] [CrossRef]
- Karanwad, T.; Lekurwale, S.; Banerjee, S. Chapter 4—Selective Laser Sintering (SLS) in Pharmaceuticals. In Additive Manufacturing in Pharmaceuticals, 1st ed.; Banerjee, S., Ed.; Springer Nature: Singapore, 2023; pp. 125–169. [Google Scholar] [CrossRef]
- Zhang, S.; Chen, X.; Shan, M.; Hao, Z.; Zhang, X.; Meng, L.; Zhai, Z.; Zhang, L.; Liu, X.; Wang, X. Convergence of 3D bioprinting and nanotechnology in tissue engineering scaffolds. Biomimetics 2023, 8, 94. [Google Scholar] [CrossRef] [PubMed]
- Melocchi, A.; Uboldi, M.; Maroni, A.; Foppoli, A.; Palugan, L.; Zema, L.; Gazzaniga, A. 3D printing by fused deposition modeling of single-and multi-compartment hollow systems for oral delivery—A review. Int. J. Pharm. 2020, 579, 119155. [Google Scholar] [CrossRef] [PubMed]
- Stansbury, J.W.; Idacavage, M.J. 3D printing with polymers: Challenges among expanding options and opportunities. Dent. Mater. J. 2016, 32, 54–64. [Google Scholar] [CrossRef] [PubMed]
- Ligon, S.C.; Liska, R.; Stampfl, J.; Gurr, M.; Mülhaupt, R. Polymers for 3D printing and customized additive manufacturing. Chem. Rev. 2017, 117, 10212–10290. [Google Scholar] [CrossRef]
- Puza, F.; Lienkamp, K. 3D printing of polymer hydrogels—From basic techniques to programmable actuation. Adv. Funct. Mater. 2022, 32, 2205345. [Google Scholar] [CrossRef]
- Mohammed, A.; Elshaer, A.; Sareh, P.; Elsayed, M.; Hassanin, H. Additive Manufacturing Technologies for Drug Delivery Applications. Int. J. Pharm. 2020, 580, 119245. [Google Scholar] [CrossRef] [PubMed]
- Ramola, M.; Yadav, V.; Jain, R. On the adoption of additive manufacturing in healthcare: A literature review. J. Manuf. Technol. Manag. 2018, 30, 48–69. [Google Scholar] [CrossRef]
- Healy, A.V.; Fuenmayor, E.; Doran, P.; Geever, L.M.; Higginbotham, C.L.; Lyons, J.G. Additive manufacturing of personalized pharmaceutical dosage forms via stereolithography. Pharmaceutics 2019, 11, 645. [Google Scholar] [CrossRef] [PubMed]
- Mathew, E.; Pitzanti, G.; Larrañeta, E.; Lamprou, D.A. 3D printing of pharmaceuticals and drug delivery devices. Pharmaceutics 2020, 12, 266. [Google Scholar] [CrossRef] [PubMed]
- Bose, S.; Ke, D.; Sahasrabudhe, H.; Bandyopadhyay, A. Additive manufacturing of biomaterials. Prog. Mater. Sci. 2018, 93, 45–111. [Google Scholar] [CrossRef] [PubMed]
- Prajapati, S.K.; Jain, A.; Jain, A.; Jain, S. Biodegradable polymers and constructs: A novel approach in drug delivery. Eur. Polym. J. 2019, 120, 109191. [Google Scholar] [CrossRef]
- Jain, A.; Bansal, K.K.; Tiwari, A.; Rosling, A.; Rosenholm, J.M. Role of Polymers in 3D Printing Technology for Drug Delivery—An Overview. Curr. Pharm. Des. 2018, 24, 4979–4990. [Google Scholar] [CrossRef]
- Ngo, T.D.; Kashani, A.; Imbalzano, G.; Nguyen, K.T.Q.; Hui, D. Additive manufacturing (3D printing): A review of materials, methods, applications and challenges. Compos. B. Eng. 2018, 143, 172–196. [Google Scholar] [CrossRef]
- Awad, A.; Trenfield, S.J.; Gaisford, S.; Basit, A.W. 3D printed medicines: A new branch of digital healthcare. Int. J. Pharm. 2018, 548, 586–596. [Google Scholar] [CrossRef] [PubMed]
- Li, J.; Wu, C.; Chu, P.K.; Gelinsky, M. 3D printing of hydrogels: Rational design strategies and emerging biomedical applications. Mater. Sci. Eng. 2020, 140, 100543. [Google Scholar] [CrossRef]
- Curry, E.J.; Henoun, A.D.; Miller, A.N.; Nguyen, T.D. 3D nano-and micro-patterning of biomaterials for controlled drug delivery. Ther. Deliv. 2016, 8, 15–28. [Google Scholar] [CrossRef]
- Meng, F.; Meyer, C.M.; Joung, D.; Vallera, D.A.; McAlpine, M.C.; Panoskaltsis-Mortari, A. 3D bioprinted in vitro metastatic models via reconstruction of tumor microenvironments. Adv. Mater. 2019, 31, 1806899. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Xu, P.; Vo, A.Q.; Bandari, S.; Yang, F.; Durig, T.; Repka, M.A. Development and evaluation of pharmaceutical 3D printability for hot melt extruded cellulose-based filaments. J. Drug Deliv. Sci. Technol. 2019, 52, 292–302. [Google Scholar] [CrossRef] [PubMed]
- Jamróz, W.; Szafraniec, J.; Kurek, M.; Renata, J. 3D Printing in Pharmaceutical and Medical Applications—Recent Achievements and Challenges. Pharm. Res. 2018, 35, 176. [Google Scholar] [CrossRef]
- Małek, E.; Miedzińska, D.; Popławski, A.; Szymczyk, W. Application of 3D printing technology for mechanical properties study of the photopolymer resin used to print porous structures. Tech. Sci. 2019, 22, 183–194. [Google Scholar] [CrossRef]
- Lamichhane, S.; Bashyal, S.; Keum, T.; Noh, G.; Seo, J.E.; Bastola, R.; Choi, J.; Sohn, D.H.; Lee, S. Complex formulations, simple techniques: Can 3D printing technology be the Midas touch in pharmaceutical industry? Asian J. Pharm. Sci. 2019, 14, 465–479. [Google Scholar] [CrossRef] [PubMed]
- Caballero-Aguilar, L.M.; Silva, S.M.; Moulton, S.E. Chapter 6—Three-dimensional printed drug delivery systems. In Engineering Drug Delivery Systems, 1st ed.; Seyfoddin, A., Dezfooli, S.M., Greene, C.A., Eds.; Woodhead Publishing: Cambridge, UK, 2020; Volume 1, pp. 147–162. [Google Scholar] [CrossRef]
- Wulf, K.; Riess, C.; Rekowska, N.D.; Eickner, T.; Seitz, H.; Grabow, N.; Teske, M. PMMA and PVP based polymers for stereolitho-graphic manufacture of tailored drug release. Trans. Addit. Manuf. Meets Med. 2019, 1, 1–2. [Google Scholar] [CrossRef]
- González-Henríquez, C.M.; Sarabia-Vallejos, M.A.; Rodriguez-Hernandez, J. Polymers for additive manufacturing and 4D-printing: Materials, methodologies, and biomedical applications. Prog. Polym. Sci. 2019, 94, 57–116. [Google Scholar] [CrossRef]
- Han, T.; Kundu, S.; Nag, A.; Xu, Y. 3D printed sensors for biomedical applications: A review. Sensors 2019, 19, 1706. [Google Scholar] [CrossRef]
- Dizon, J.R.C.; Espera, A.H., Jr.; Chen, Q.; Advincula, R.C. Mechanical characterization of 3D-printed polymers. Addit. Manuf. 2018, 20, 44–67. [Google Scholar] [CrossRef]
- Trenfield, S.J.; Awad, A.; Madla, C.M.; Hatton, G.B.; Firth, J.; Goyanes, A.; Gaisford, S.; Basit, A.W. Shaping the future: Recent advances of 3D printing in drug delivery and healthcare. Expert Opin. Drug Deliv. 2019, 16, 1081–1094. [Google Scholar] [CrossRef]
- Fina, F.; Goyanes, A.; Gaisford, S.; Basit, A.W. Selective laser sintering (SLS) 3D printing of medicines. Int. J. Pharm. 2017, 519, 285–293. [Google Scholar] [CrossRef] [PubMed]
- Tappa, K.; Jammalamadaka, U. Novel biomaterials used in medical 3D printing techniques. J. Funct. Biomater. 2018, 9, 17. [Google Scholar] [CrossRef] [PubMed]
- Matijašić, G.; Gretić, M.; Vinčić, J.; Poropat, A.; Cuculić, L.; Rahelić, T. Design and 3D printing of multi-compartmental PVA capsules for drug delivery. J. Drug Deliv. Sci. Technol. 2019, 52, 677–686. [Google Scholar] [CrossRef]
- Krause, J.; Bogdahn, M.; Schneider, F.; Koziolek, M.; Weitschies, W. Design and characterization of a novel 3D printed pressure-controlled drug delivery system. Eur. J. Pharm. Sci. 2019, 140, 105060. [Google Scholar] [CrossRef] [PubMed]
- Thayer, P.; Martinez, H.; Gatenholm, E. Chapter 1—History and trends of 3D bioprinting. In 3D Bioprinting: Principles and Protocols, 1st ed.; Crook, J.M., Ed.; Humana Press: New York, NY, USA, 2020; Volume 1, pp. 3–18. [Google Scholar] [CrossRef]
- Mobaraki, M.; Ghaffari, M.; Yazdanpanah, A.; Luo, Y.; Mills, D.K. Bioinks and bioprinting: A focused review. Bioprinting 2020, 18, e00080. [Google Scholar] [CrossRef]
- Chircov, C.; Grumezescu, A.M. Chapter 2—Three-dimensional bioprinting in drug delivery. In Materials for Biomedical Engineering: Nanomaterials-Based Drug Delivery, 1st ed.; Holban, A., Grumezescu, A.M., Eds.; Elsevier: Amsterdam, The Netherlands, 2019; Volume 1, pp. 19–40. [Google Scholar] [CrossRef]
- Huang, Y.; Zhang, X.-F.; Gao, G.; Yonezawa, T.; Cui, X. 3D bioprinting and the current applications in tissue engineering. Biotechnol. J. 2017, 12, 1600734. [Google Scholar] [CrossRef]
- Sahranavard, M.; Zamanian, A.; Ghorbani, F.; Shahrezaee, M.H. A critical review on three dimensional-printed chitosan hydrogels for development of tissue engineering. Bioprinting 2020, 17, e00063. [Google Scholar] [CrossRef]
- Ghilan, A.; Chiriac, A.P.; Nita, L.E.; Rusu, A.G.; Neamtu, I.; Chiriac, V.M. Trends in 3D printing processes for biomedical field: Opportunities and challenges. J. Polym. Environ. 2020, 28, 1345–1367. [Google Scholar] [CrossRef]
- Saygili, E.; Dogan-Gurbuz, A.A.; Yesil-Celiktas, O.; Draz, M.S. A powerful tool to leverage tissue engineering and microbial systems. Bioprinting 2020, 18, e00071. [Google Scholar] [CrossRef]
- Infanger, S.; Haemmerli, A.; Iliev, S.; Baier, A.; Stoyanov, E.; Quodbach, J. Powder bed 3D-printing of highly loaded drug delivery devices with hydroxypropyl cellulose as solid binder. Int. J. Pharm. 2019, 555, 198–206. [Google Scholar] [CrossRef]
- Miyasaka, K. Chapter 3—PVA-Iodine complexes: Formation, structure, and properties. In Structure in Polymers with Special Properties, 1st ed.; Zachmann, H.G., Ed.; Springer: Berlin/Heidelberg, Germany, 1993; Volume 108, pp. 91–129. [Google Scholar] [CrossRef]
- DeMerlis, C.C.; Schoneker, D.R. Review of the oral toxicity of polyvinyl alcohol (PVA). Food Chem. Toxicol. 2003, 41, 319–326. [Google Scholar] [CrossRef]
- Afsana; Jain, V.; Haider, N.; Jain, K. 3D printing in personalized drug delivery. Curr. Pharm. Des. 2018, 24, 5062–5071. [Google Scholar] [CrossRef]
- Musa, B.H.; Hameed, N.J. Study of the mechanical properties of polyvinyl alcohol/starch blends. Mater. Today Proc. 2020, 20, 439–442. [Google Scholar] [CrossRef]
- Curti, C.; Kirby, D.J.; Russell, C.A. Current formulation approaches in design and development of solid oral dosage forms through three-dimensional printing. Prog. Addit. Manuf. 2020, 5, 111–123. [Google Scholar] [CrossRef]
- Wang, C.; Huang, W.; Zhou, Y.; He, L.; He, Z.; Chen, Z.; He, X.; Tian, S.; Liao, J.; Lu, B.; et al. 3D printing of bone tissue engineering scaffolds. Bioact. Mater. 2020, 5, 82–91. [Google Scholar] [CrossRef]
- Saviano, M.; Bowles, B.J.; Penny, M.R.; Ishaq, A.; Muwaffak, Z.; Falcone, G.; Russo, P.; Hilton, S.T. Development and analysis of a novel loading technique for FDM 3D printed systems: Microwave-assisted impregnation of gastro-retentive PVA capsular devices. Int. J. Pharm. 2022, 613, 121386. [Google Scholar] [CrossRef]
- Junqueira, L.A.; Tabriz, A.G.; Rousseau, F.; Raposo, N.R.B.; Brandão, M.A.F.; Douroumis, D. Development of printable inks for 3D printing of personalized dosage forms: Coupling of fused deposition modelling and jet dispensing. J. Drug Deliv. Sci. Technol. 2023, 80, 104108. [Google Scholar] [CrossRef]
- Wei, M.; Liu, D.; Sun, Y.; Xie, H.; Du, L.; Jin, Y. Mesalazine hollow suppositories based on 3D printing for treatment of ulcerative colitis. Int. J. Pharm. 2023, 642, 123196. [Google Scholar] [CrossRef]
- Krueger, L.; Cao, Y.; Zheng, Z.; Ward, J.; Miles, J.A.; Popat, A. D printing tablets for high-precision dose titration of caffeine. Int. J. Pharm. 2023, 642, 123132. [Google Scholar] [CrossRef] [PubMed]
- Topsakal, A.; Midha, S.; Yuca, E.; Tukay, A.; Sasmazel, H.T.; Kalaskar, D.M.; Gunduz, O. Study on the cytocompatibility, mechanical and antimicrobial properties of 3D printed composite scaffolds based on PVA/Gold nanoparticles (AuNP)/Ampicillin (AMP) for bone tissue engineering. Mater. Today Commun. 2021, 28, 102458. [Google Scholar] [CrossRef]
- Pires, F.Q.; Gross, I.P.; Sa-Barreto, L.L.; Gratieri, T.; Gelfuso, G.M.; Bao, S.N.; Cunha-Filho, M. In-situ formation of nanoparticles from drug-loaded 3D polymeric matrices. Eur. J. Pharm. Sci. 2023, 188, 106517. [Google Scholar] [CrossRef] [PubMed]
- Gaurkhede, S.G.; Osipitan, O.O.; Dromgoole, G.; Spencer, S.A.; Di Pasqua, A.J.; Deng, J. 3D printing and dissolution testing of novel capsule shells for use in delivering acetaminophen. J. Pharm. Sci. 2021, 110, 3829–3837. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Xu, P.; Chung, S.; Bandari, S.; Repka, M.A. Fabrication of bilayer tablets using hot melt extrusion-based dual-nozzle fused deposition modeling 3D printing. Int. J. Pharm. 2022, 624, 121972. [Google Scholar] [CrossRef] [PubMed]
- Manini, G.; Benali, S.; Mathew, A.; Napolitano, S.; Raquez, J.M.; Goole, J. Paliperidone palmitate as model of heat-sensitive drug for long-acting 3D printing application. Int. J. Pharm. 2022, 618, 121662. [Google Scholar] [CrossRef]
- Berger, V.; Buzhor, M.G.; Evstafeva, D.; Mügeli, L.; Leroux, J.C. 3D printing of a controlled urea delivery device for the prevention of tooth decay. Int. J. Pharm. 2023, 631, 122528. [Google Scholar] [CrossRef]
- Chen, H.; Li, X.; Gong, Y.; Bu, T.; Wang, X.; Pan, H. Unidirectional drug release from 3D printed personalized buccal patches using FDM technology. Int. J. Pharm. 2023, 645, 123382. [Google Scholar] [CrossRef]
- Tagami, T.; Hayashi, N.; Sakai, N.; Ozeki, T. 3D printing of unique water-soluble polymer-based suppository shell for controlled drug release. Int. J. Pharm. 2019, 568, 118494. [Google Scholar] [CrossRef] [PubMed]
- Alzahrani, A.; Narala, S.; Youssef, A.A.A.; Nyavanandi, D.; Bandari, S.; Mandati, P.; Almotairy, A.; Almutairi, M.; Repka, M. Fabrication of a shell-core fixed-dose combination tablet using fused deposition modeling 3D printing. Eur. J. Pharm. Biopharm. 2022, 177, 211–223. [Google Scholar] [CrossRef]
- Cui, M.; Pan, H.; Li, L.; Fang, D.; Sun, H.; Qiao, S.; Li, X.; Pan, W. Exploration and preparation of patient-specific ciprofloxacin implants drug delivery system via 3D printing technologies. J. Pharm. Sci. 2021, 110, 3678–3689. [Google Scholar] [CrossRef]
- Chee, P.S.; Arsat, R.; He, X.; Kalantar-zadeh, K.; Arsat, M.; Wlodarski, W. Polyvinylpyrrolidone/Multiwall Carbon Nanotube Composite Based 36° YX LiTaO3 Surface Acoustic Wave For Hydrogen Gas Sensing Applications. In Proceedings of the International Conference on Enabling Science and Nanotechnology (ESciNano), Lumpur, Malaysia, 1–3 December 2010. [Google Scholar] [CrossRef]
- Koczkur, K.M.; Mourdikoudis, S.; Polavarapu, L.; Skrabalak, S.E. Polyvinylpyrrolidone (PVP) in nanoparticle synthesis. Dalton Trans. 2015, 44, 17883. [Google Scholar] [CrossRef]
- Wang, H.; Li, X.; Yang, H.; Wang, J.; Li, Q.; Qu, R.; Wu, X. Nanocomplexes based polyvinylpyrrolidone K-17PF for ocular drug delivery of naringenin. Int. J. Pharm. 2020, 578, 119133. [Google Scholar] [CrossRef]
- Bianchi, M.; Pegoretti, A.; Fredi, G. An overview of poly (vinyl alcohol) and poly (vinyl pyrrolidone) in pharmaceutical additive manufacturing. J. Vinyl Addit. Technol. 2023, 29, 223–239. [Google Scholar] [CrossRef]
- Windolf, H.; Chamberlain, R.; Quodbach, J. Dose-independent drug release from 3D printed oral medicines for patient-specific dosing to improve therapy safety. Int. J. Pharm. 2022, 616, 121555. [Google Scholar] [CrossRef]
- Jovanović, M.; Petrović, M.; Cvijić, S.; Tomić, N.; Stojanović, D.; Ibrić, S.; Uskoković, P. 3d printed buccal films for prolonged-release of propranolol hydrochloride: Development, characterization and bioavailability prediction. Pharmaceutics 2021, 13, 2143. [Google Scholar] [CrossRef]
- Than, Y.M.; Titapiwatanakun, V. Statistical design of experiment-based formulation development and optimization of 3D printed oral controlled release drug delivery with multi target product profile. J. Pharm. Investig. 2021, 51, 715–734. [Google Scholar] [CrossRef]
- D’souza, A.A.; Shegokar, R. Polyethylene glycol (PEG): A versatile polymer for pharmaceutical applications. Expert Opin. Drug Deliv. 2016, 13, 1257–1275. [Google Scholar] [CrossRef]
- Salehi, S.; Ghomi, H.; Hassanzadeh-Tabrizi, S.A.; Koupaei, N.; Khodaei, M. The effect of polyethylene glycol on printability, physical and mechanical properties and osteogenic potential of 3D-printed poly (l-lactic acid)/polyethylene glycol scaffold for bone tissue engineering. Int. J. Biol. Macromol. 2022, 221, 1325–1334. [Google Scholar] [CrossRef] [PubMed]
- Digkas, T.; Porfire, A.; Renterghem, J.V.; Samaro, A.; Borodi, G.; Vervaet, C.; Crisan, A.G.; Iurian, S.; Beer, T.; Tomuta, I. Development of Diclofenac Sodium 3D Printed Cylindrical and Tubular-Shaped Tablets through Hot Melt Extrusion and Fused Deposition Modelling Techniques. Pharmaceuticals 2023, 16, 1062. [Google Scholar] [CrossRef]
- Picco, C.J.; Utomo, E.; McClean, A.; Domínguez-Robles, J.; Anjani, Q.K.; Volpe-Zanutto, F.; McKenna, P.E.; Acheson, J.G.; Malinova, D.; Donnelly, R.F.; et al. Development of 3D-printed subcutaneous implants using concentrated polymer/drug solutions. Int. J. Pharm. 2023, 631, 122477. [Google Scholar] [CrossRef]
- Cherng, J.Y.; Hou, T.Y.; Shih, M.F.; Talsma, H.; Hennink, W.E. Polyurethane-based drug delivery systems. Int. J. Pharm. 2013, 450, 145–162. [Google Scholar] [CrossRef]
- Atiqah, A.; Mastura, M.T.; Ali, B.A.A.; Jawaid, M.; Sapuan, S.M. A Review on Polyurethane and its Polymer Composites. Curr. Org. Synth. 2017, 14, 233–248. [Google Scholar] [CrossRef]
- Hung, K.C.; Tseng, C.S.; Hsu, S.H. 3D printing of polyurethane biomaterials. In Advances in Polyurethane Biomaterials, 1st ed.; Cooper, S.L., Guan, J., Eds.; Elsevier: Amsterdam, The Netherlands, 2016; Volume 1, pp. 149–170. [Google Scholar] [CrossRef]
- Wan, L.; Deng, C.; Chen, H.; Zhao, Z.; Huang, S.; Wei, W.; Yang, A.; Zhao, H.; Wang, Y. Flame-retarded thermoplastic polyurethane elastomer: From organic materials to nanocomposites and new prospects. Chem. Eng. J. 2021, 417, 129314. [Google Scholar] [CrossRef]
- Verstraete, G.; Samaro, A.; Grymonpré, W.; Vanhoorne, V.; Snick, V.B.; Boone, M.N.; Hellemans, T.; Hoorebeke, L.V.; Remon, J.P.; Vervaet, C. 3D printing of high drug loaded dosage forms using thermoplastic polyurethanes. Int. J. Pharm. 2018, 536, 318–325. [Google Scholar] [CrossRef]
- Domínguez-Robles, J.; Utomo, E.; Cornelius, V.A.; Anjani, Q.K.; Korelidou, A.; Gonzalez, Z.; Donnelly, R.F.; Margariti, A.; Delgado-Aguilar, M.; Tarrés, Q.; et al. TPU-based antiplatelet cardiovascular prostheses prepared using fused deposition modelling. Mater. Des. 2022, 220, 110837. [Google Scholar] [CrossRef]
- Zhang, H.; Shao, Y.; Gao, B.; Li, J. Spidroin-based multifunctional microneedles with controlled drug release for efficient wound management. Eur. Polym. J. 2023, 198, 112429. [Google Scholar] [CrossRef]
- Martorana, A.; Fiorica, C.; Palumbo, F.S.; Federico, S.; Giammona, G.; Pitarresi, G. Redox responsive 3D-printed nanocomposite polyurethane-urea scaffold for Doxorubicin local delivery. J. Drug Deliv. Sci. Technol. 2023, 88, 104890. [Google Scholar] [CrossRef]
- Salimi, S.; Wu, Y.; Barreiros, M.I.E.; Natfji, A.A.; Khaled, S.; Wildman, R.; Hart, L.R.; Greco, F.; Clark, E.A.; Roberts, C.J.; et al. 3D printed drug delivery implant formed from a dynamic supramolecular polyurethane formulation. Polym. Chem. 2020, 11, 3453–3464. [Google Scholar] [CrossRef]
- Hu, C.; Chen, Z.; Tang, L.; Liu, J.; Yang, J.; Lai, W.; Wu, T.; Liao, S.; Zhang, X.; Pan, H.; et al. A universally dispersible graphene-based ink modifier facilitates 3D printing of multi-functional tissue-engineered scaffolds. Mater. Des. 2022, 216, 110551. [Google Scholar] [CrossRef]
- Goyanes, A.; Det-Amornrat, U.; Wang, J.; Basit, A.W.; Gaisford, S. 3D scanning and 3D printing as innovative technologies for fabricating personalized topical drug delivery systems. J. Control. Release 2016, 234, 41–48. [Google Scholar] [CrossRef]
- Henry, S.; Samaro, A.; Marchesini, F.H.; Shaqour, B.; Macedo, J.; Vanhoorne, V.; Vervaet, C. Extrusion-based 3D printing of oral solid dosage forms: Material requirements and equipment dependencies. Int. J. Pharm. 2021, 598, 120361. [Google Scholar] [CrossRef] [PubMed]
- Linares, V.; Galdón, E.; Casas, M.; Caraballo, I. Critical points for predicting 3D printable filaments behaviour. J. Drug Deliv. Sci. Technol. 2021, 66, 102933. [Google Scholar] [CrossRef]
- Wen, Y.T.; Dai, N.T.; Hsu, S.H. Biodegradable water-based polyurethane scaffolds with a sequential release function for cell-free cartilage tissue engineering. Acta Biomater. 2019, 88, 301–313. [Google Scholar] [CrossRef] [PubMed]
- Tiboni, M.; Campana, R.; Frangipani, E.; Casettari, L. 3D printed clotrimazole intravaginal ring for the treatment of recurrent vaginal candidiasis. Int. J. Pharm. 2021, 596, 120290. [Google Scholar] [CrossRef]
- Bil, M.; Kijeńska-Gawrońska, E.; Głodkowska-Mrówka, E.; Manda-Handzlik, A.; Mrowka, P. Design and in vitro evaluation of electrospun shape memory polyurethanes for self-fitting tissue engineering grafts and drug delivery systems. Mater. Sci. Eng. C 2020, 110, 110675. [Google Scholar] [CrossRef] [PubMed]
- Zhao, C.; Wang, Z.; Hua, C.; Ji, J.; Zhou, Z.; Fang, Y.; Weng, D.; Lu, L.; Pang, Y.; Sun, W. Design, modeling and 3D printing of a personalized cervix tissue implant with protein release function. Biomed. Mater. 2020, 15, 045005. [Google Scholar] [CrossRef] [PubMed]
- Mathew, E.; Domínguez-Robles, J.; Stewart, S.A.; Mancuso, E.; O’Donnell, K.; Larrañeta, E. Fused deposition modeling as an effective tool for anti-infective dialysis catheter fabrication. ACS Biomater. Sci. Eng. 2019, 5, 6300–6310. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.; Hao, M.; Wang, G.; Peng, H.; Wahid, F.; Yang, Y.; Liang, L.; Liu, S.; Li, R.; Feng, S. Zein nanospheres assisting inorganic and organic drug combination to overcome stent implantation-induced thrombosis and infection. Sci. Total Environ. 2023, 873, 162438. [Google Scholar] [CrossRef] [PubMed]
- Eder, S.; Wiltschko, L.; Koutsamanis, I.; Urich, J.A.A.; Arbeiter, F.; Roblegg, E.; Spoerk, M. Toward a new generation of vaginal pessaries via 3D-printing: Concomitant mechanical support and drug delivery. Eur. J. Pharm. Biopharm. 2022, 174, 77–89. [Google Scholar] [CrossRef]
- Farmer, Z.L.; Utomo, E.; Domínguez-Robles, J.; Mancinelli, C.; Mathew, E.; Larrañeta, E.; Lamprou, D.A. 3D printed estradiol-eluting urogynecological mesh implants: Influence of material and mesh geometry on their mechanical properties. Int. J. Pharm. 2021, 593, 120145. [Google Scholar] [CrossRef]
- Martin, N.K.; Domínguez-Robles, J.; Stewart, S.A.; Cornelius, V.A.; Anjani, Q.K.; Utomo, E.; García-Romero, I.; Donnelly, R.F.; Margariti, A.; Lamprou, D.A.; et al. Fused deposition modelling for the development of drug loaded cardiovascular prosthesis. Int. J. Pharm. 2021, 595, 120243. [Google Scholar] [CrossRef]
- Shao, Y.; Dong, K.; Lu, X.; Gao, B.; He, B. Bioinspired 3D-Printed MXene and Spidroin-Based Near-Infrared Light-Responsive Microneedle Scaffolds for Efficient Wound Management. ACS Appl. Mater. Interfaces 2022, 14, 56525–56534. [Google Scholar] [CrossRef]
- Masutani, K.; Kimura, Y. Chapter 1—PLA Synthesis. From the Monomer to the Polymer. In Poly(lactic acid) Science and Technology: Processing, Properties, Additives and Applications, 1st ed.; Jiménez, A., Peltzer, M.A., Ruseckaite, R.A., Eds.; The Royal Society of Chemistry: London, UK, 2015; Volume 12, pp. 3–36. [Google Scholar] [CrossRef]
- Vatansever, E.; Arslan, D.; Nofar, M. Polylactide cellulose-based nanocomposites. Int. J. Biol. Macromol. 2019, 137, 912–938. [Google Scholar] [CrossRef]
- Gowrav, M.P.; Siree, K.G.; Amulya, T.M.; Bharathi, M.B.; Ghazwani, M.; Alamri, A.; Alalkami, A.Y.; Kumar, T.M.P.; Ahmed, M.M.; Rahamathulla, M. Novel Rhinological Application of Polylactic Acid—An In Vitro Study. Polymers 2023, 15, 2521. [Google Scholar] [CrossRef] [PubMed]
- Gao, X.; Xu, Z.; Li, S.; Cheng, L.; Xu, D.; Li, L.; Chen, L.; Xu, Y.; Liu, Z.; Liu, Y.; et al. Chitosan-vancomycin hydrogel incorporated bone repair scaffold based on staggered orthogonal structure: A viable dually controlled drug delivery system. RSC Adv. 2023, 13, 3759–3765. [Google Scholar] [CrossRef] [PubMed]
- Asadi, M.; Salehi, Z.; Akrami, M.; Hosseinpour, M.; Jockenhövel, S.; Ghazanfari, S. 3D printed pH-responsive tablets containing N-acetylglucosamine-loaded methylcellulose hydrogel for colon drug delivery applications. Int. J. Pharm. 2023, 645, 123366. [Google Scholar] [CrossRef] [PubMed]
- Sri, K.H.; Ganapathy, D.; Nallasamy, D.; Venugopalan, S.; Sivaswamy, V.; Kamath, S.M. Sustained release of resveratrol from fused deposition modelling guided 3D porous scaffold for bone tissue engineering. Process Biochem. 2023, 131, 188–198. [Google Scholar] [CrossRef]
- Cui, M.; Pan, H.; Fang, D.; Sun, H.; Pan, W. 3D printed personalized amikacin sulfate local drug delivery system for bone defect therapy. J. Drug Deliv. Sci. Technol. 2022, 70, 103208. [Google Scholar] [CrossRef]
- Mei, Y.; He, C.; Gao, C.; Zhu, P.; Lu, G.; Li, H. 3D-printed degradable anti-tumor scaffolds for controllable drug delivery. Int. J. Bioprint. 2021, 7, 135–144. [Google Scholar] [CrossRef]
- Han, S.H.; Cha, M.; Jin, Y.Z.; Lee, K.M.; Lee, J.H. BMP-2 and hMSC dual delivery onto 3D printed PLA-Biogel scaffold for critical-size bone defect regeneration in rabbit tibia. Biomed. Mater. 2021, 16, 015019. [Google Scholar] [CrossRef]
- Cheng, L.; Xu, Z.; Liu, Y.; Zhou, D.; Sun, M.; Xu, Y.; Chen, L.; Sun, J. 3D-Printed Drug-Loaded Composite Scaffolds to Promote Osteogenesis and Antibacterial Activity. ACS Appl. Polym. Mater. 2022, 4, 4476–4485. [Google Scholar] [CrossRef]
- Khosraviboroujeni, A.; Mirdamadian, S.Z.; Minaiyan, M.; Taheri, A. Preparation and characterization of 3D printed PLA microneedle arrays for prolonged transdermal drug delivery of estradiol valerate. Drug Deliv. Transl. Res. 2021, 12, 1195–1208. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X.; Wei, W.; Niu, R.; Li, Q.; Hu, C.; Jiang, S. 3D printed intragastric floating and sustained-release tablets with air chambers. J. Pharm. Sci. 2022, 111, 116–123. [Google Scholar] [CrossRef] [PubMed]
- Wu, L.; Park, J.; Kamaki, Y.; Kim, B. Optimization of the fused deposition modeling-based fabrication process for polylactic acid microneedles. Microsystems Nanoeng. 2021, 7, 58. [Google Scholar] [CrossRef] [PubMed]
- Cisneros, K.; Chowdhury, N.; Coleman, E.; Ferdous, T.; Su, H.; Jennings, J.A.; Bumgardner, J.D.; Fujiwara, T. Long-Term Controlled Release of Simvastatin from Photoprinted Triple-Networked Hydrogels Composed of Modified Chitosan and PLA–PEG Micelles. Macromol. Biosci. 2021, 21, 2100123. [Google Scholar] [CrossRef]
- Basa, B.; Jakab, G.; Kállai-Szabó, N.; Borbás, B.; Fülöp, V.; Balogh, E.; Antal, I. Evaluation of biodegradable PVA-based 3D printed carriers during dissolution. Materials 2021, 14, 1350. [Google Scholar] [CrossRef] [PubMed]
- Huanbutta, K.; Sriamornsak, P.; Kittanaphon, T.; Suwanpitak, K.; Klinkesorn, N.; Sangnim, T. Development of a zero-order kinetics drug release floating tablet with anti–flip-up design fabricated by 3D-printing technique. J. Pharm. Investig. 2021, 51, 213–222. [Google Scholar] [CrossRef]
- Wu, L.; Shrestha, P.; Iapichino, M.; Cai, Y.; Kim, B.; Stoeber, B. Characterization method for calculating diffusion coefficient of drug from polylactic acid (PLA) microneedles into the skin. J. Drug Deliv. Sci. Technol. 2021, 61, 102192. [Google Scholar] [CrossRef]
- Stewart, S.A.; Domínguez-Robles, J.; McIlorum, V.J.; Gonzalez, Z.; Utomo, E.; Mancuso, E.; Lamprou, D.A.; Donnelly, R.F.; Larrañeta, E. Poly (caprolactone)-based coatings on 3D-printed biodegradable implants: A novel strategy to prolong delivery of hydrophilic drugs. Mol. Pharm. 2020, 17, 3487–3500. [Google Scholar] [CrossRef]
- Auvinen, V.V.; Virtanen, J.; Merivaara, A.; Virtanen, V.; Laurén, P.; Tuukkanen, S.; Laaksonen, T. Modulating sustained drug release from nanocellulose hydrogel by adjusting the inner geometry of implantable capsules. J. Drug Deliv. Technol. 2020, 57, 101625. [Google Scholar] [CrossRef]
- Martin, V.; Ribeiro, I.A.; Alves, M.M.; Gonçalves, L.; Claudio, R.A.; Grenho, L.; Fernandes, M.H.; Gomes, P.; Santos, C.F.; Bettencourt, A.F. Engineering a multifunctional 3D-printed PLA-collagen-minocycline-nanoHydroxyapatite scaffold with combined antimicrobial and osteogenic effects for bone regeneration. Mater. Sci. Eng. C 2019, 101, 15–26. [Google Scholar] [CrossRef]
- Niese, S.; Breitkreutz, J.; Quodbach, J. Development of a dosing device for individualized dosing of orodispersible warfarin films. Int. J. Pharm. 2019, 561, 314–323. [Google Scholar] [CrossRef]
- Silva, A.T.C.R.; Cardoso, B.C.O.; Silva, M.E.S.R.; Freitas, R.F.S.; Sousa, R.G. Synthesis, Characterization, and Study of PLGA Copolymer in Vitro Degradation. J. Biomater. Nanobiotechnol. 2015, 6, 8–19. [Google Scholar] [CrossRef]
- Dang, Y.; Guan, J. Nanoparticle-based drug delivery systems for cancer therapy. Smart Mater. Med. 2020, 1, 10–19. [Google Scholar] [CrossRef] [PubMed]
- Bassand, C.; Siepmann, F.; Benabed, L.; Verin, J.; Freitag, J.; Charlon, S.; Soulestin, J.; Siepmann, J. 3D printed PLGA implants: How the filling density affects drug release. J. Control. Release 2023, 363, 1–11. [Google Scholar] [CrossRef]
- Bendicho-Lavilla, C.; Seoane-Viaño, I.; Santos-Rosales, V.; Díaz-Tomé, V.; Carracedo-Pérez, M.; Luzardo-Álvarez, A.M.; García-Gonzalez, C.A.; Otero-Espinar, F.J. Intravitreal implants manufactured by supercritical foaming for treating retinal diseases. J. Control. Release 2023, 362, 342–355. [Google Scholar] [CrossRef] [PubMed]
- Martínez-Pérez, D.; Guarch-Pérez, C.; Purbayanto, M.A.K.; Choińska, E.; Riool, M.; Zaat, S.A.J.; Święszkowski, W. 3D-printed dual drug delivery nanoparticle-loaded hydrogels to combat antibiotic-resistant bacteria. Int. J. Bioprint. 2023, 9, 683. [Google Scholar] [CrossRef]
- Zhang, Y.; Wang, H.; Huangfu, H.; Zhang, X.; Zhang, H.; Qin, Q.; Fu, L.; Wang, D.; Wang, C.; Wang, L.; et al. 3D printing of bone scaffolds for treating infected mandible bone defects through adjustable dual-release of chlorhexidine and osteogenic peptide. Mater. Des. 2022, 224, 111288. [Google Scholar] [CrossRef]
- Ji, J.; Wang, C.; Xiong, Z.; Pang, Y.; Sun, W. 3D-printed scaffold with halloysite nanotubes laden as a sequential drug delivery system regulates vascularized bone tissue healing. Mater. Today Adv. 2022, 15, 100259. [Google Scholar] [CrossRef]
- Zheng, C.; Attarilar, S.; Li, K.; Wang, C.; Liu, J.; Wang, L.; Yang, J.; Tang, Y. 3D-printed HA15-loaded β-tricalcium phosphate/poly (Lactic-co-glycolic acid) bone tissue scaffold promotes bone regeneration in rabbit radial defects. Int. J. Bioprint. 2021, 7, 317. [Google Scholar] [CrossRef]
- Banche-Niclot, F.; Licini, C.; Montalbano, G.; Fiorilli, S.; Mattioli-Belmonte, M.; Vitale-Brovarone, C. 3D Printed Scaffold Based on Type I Collagen/PLGA_TGF-β1 Nanoparticles Mimicking the Growth Factor Footprint of Human Bone Tissue. Polymers 2022, 14, 857. [Google Scholar] [CrossRef]
- Chen, Y.P.; Lo, T.S.; Lin, Y.T.; Chien, Y.H.; Lu, C.J.; Liu, S.J. Fabrication of drug-eluting polycaprolactone/poly (lactic-co-glycolic acid) prolapse mats using solution-extrusion 3D printing and coaxial electrospinning techniques. Polymers 2021, 13, 2295. [Google Scholar] [CrossRef] [PubMed]
- Serris, I.; Serris, P.; Frey, K.M.; Cho, H. Development of 3D-printed layered PLGA films for drug delivery and evaluation of drug release behaviors. AAPS Pharm. Sci. Tech. 2020, 21, 256. [Google Scholar] [CrossRef]
- Wang, Y.; Qiao, X.; Yang, X.; Yuan, M.; Xian, S.; Zhang, L.; Yang, D.; Liu, S.; Dai, F.; Tan, Z.; et al. The role of a drug-loaded poly (lactic co-glycolic acid)(PLGA) copolymer stent in the treatment of ovarian cancer. Cancer Biol. Med. 2020, 17, 237–250. [Google Scholar] [CrossRef]
- Qiao, Y.; Xu, S.; Zhu, T.; Tang, N.; Bai, X.; Zheng, C. Preparation of printable double-network hydrogels with rapid self-healing and high elasticity based on hyaluronic acid for controlled drug release. Polymer 2020, 186, 121994. [Google Scholar] [CrossRef]
- Hosseinzadeh, R.; Mirani, B.; Pagan, E.; Mirzaaghaei, S.; Nasimian, A.; Kawalec, P.; Rosa, S.C.S.; Hamadi, D.; Fernandez, N.P.; Toyota, B.D.; et al. A drug-eluting 3D-printed mesh (GlioMesh) for management of glioblastoma. Adv. Ther. 2019, 2, 1900113. [Google Scholar] [CrossRef]
- Deng, N.; Sun, J.; Li, Y.; Chen, L.; Chen, C.; Wu, Y.; Wang, Z.; Li, L. Experimental study of rhBMP-2 chitosan nano-sustained release carrier-loaded PLGA/nHA scaffolds to construct mandibular tissue-engineered bone. Arch. Oral Biol. 2019, 102, 16–25. [Google Scholar] [CrossRef] [PubMed]
- Cameron, R.E.; Kamvari-Moghaddam, A. Chapter 5—Synthetic bioresorbable polymers. In Durability and Reliability of Medical Polymers, 1st ed.; Jenkins, A., Stamboulis, A., Eds.; Woodhead Publishing: Cambridge, UK, 2012; Volume 1, pp. 96–118. [Google Scholar]
- Chen, J.; Lee, D.; Yang, J.; Lin, S.; Lin, Y.; Liu, S. Solution extrusion additive manufacturing of biodegradable polycaprolactone. Appl. Sci. 2020, 10, 3189. [Google Scholar] [CrossRef]
- Li, Y.; Peng, Y.; Hu, Y.; Liu, J.; Yuan, T.; Zhou, W.; Dong, X.; Wang, C.; Binks, B.P.; Yang, Z. Fabrication of Poly (ε-caprolactone)-embedded Lignin-Chitosan Nanocomposite Porous Scaffolds from Pickering Emulsions. Langmuir 2023, 39, 6947–6956. [Google Scholar] [CrossRef]
- Ghosh, S.; Yadav, A.; Rani, S.; Takkar, S.; Kulshreshtha, R.; Nandan, B.; Srivastava, R.K. 3D Printed Hierarchical Porous Poly (ε-Caprolactone) Scaffolds from Pickering High Internal Phase Emulsion Templating. Langmuir 2023, 39, 1927–1946. [Google Scholar] [CrossRef]
- Mohsenifard, S.; Mashayekhan, S.; Safari, H. A hybrid cartilage extracellular matrix-based hydrogel/poly (ε-caprolactone) scaffold incorporated with Kartogenin for cartilage tissue engineering. J. Biomater. Appl. 2023, 37, 1243–1258. [Google Scholar] [CrossRef]
- Gong, W.; Li, M.; Zhao, L.; Wang, P.; Wang, X.; Wang, B.; Liu, X.; Tu, X. Sustained release of a highly specific GSK3β inhibitor SB216763 in the PCL scaffold creates an osteogenic niche for osteogenesis, anti-adipogenesis, and potential angiogenesis. Front. Bioeng. Biotechnol. 2023, 11, 1215233. [Google Scholar] [CrossRef] [PubMed]
- Korelidou, A.; Domínguez-Robles, J.; Magill, E.R.; Eleftheriadou, M.; Cornelius, V.A.; Donnelly, R.F.; Margariti, A.; Larrañeta, E. 3D-printed reservoir-type implants containing poly (lactic acid)/poly (caprolactone) porous membranes for sustained drug delivery. Biomater. Adv. 2022, 139, 213024. [Google Scholar] [CrossRef]
- Berger, V.; Luo, Z.; Leroux, J. 3D printing of a controlled fluoride delivery device for the prevention and treatment of tooth decay. J. Control. Release 2022, 348, 870–880. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Liao, Z.; Yang, Z.; Gao, C.; Fu, L.; Li, P.; Zhao, T.; Cao, F.; Chen, W.; Yuan, Z.; et al. 3D printed poly (ε-caprolactone)/meniscus extracellular matrix composite scaffold functionalized with kartogenin-releasing PLGA microspheres for meniscus tissue engineering. Front. Bioeng. Biotechnol. 2021, 9, 662381. [Google Scholar] [CrossRef]
- Muldoon, K.; Ahmad, Z.; Su, Y.; Tseng, F.; Chen, X.; McLaughlin, J.A.D.; Chang, M. A Refined Hot Melt Printing Technique with Real-Time CT Imaging Capability. Micromachines 2022, 13, 1794. [Google Scholar] [CrossRef] [PubMed]
- Elbadawi, M.; Gustaffson, T.; Gaisford, S.; Basit, A.W. 3D printing tablets: Predicting printability and drug dissolution from rheological data. Int. J. Pharm. 2020, 590, 119868. [Google Scholar] [CrossRef]
- Stewart, S.A.; Domínguez-Robles, J.; McIlorum, V.J.; Mancuso, E.; Lamprou, D.A.; Donnelly, R.F.; Larrañeta, E. Development of a biodegradable subcutaneous implant for prolonged drug delivery using 3D printing. Pharmaceutics 2020, 12, 105. [Google Scholar] [CrossRef]
- Zhang, W.; Shi, W.; Wu, S.; Kuss, M.; Jiang, X.; Untrauer, J.B.; Reid, S.T.; Duan, B. 3D printed composite scaffolds with dual small molecule delivery for mandibular bone regeneration. Biofabrication 2020, 12, 035020. [Google Scholar] [CrossRef]
- Dang, H.P.; Hutmacher, D.W.; Tran, P.A. The use of 3D printed microporous-strut polycaprolactone scaffolds for targeted local delivery of chemotherapeutic agent for breast cancer application. In Proceedings of the 7th International Conference on the Development of Biomedical Engineering in Vietnam (BME7), Ho Chi Minh, Vietnam, 27–29 June 2018. [Google Scholar] [CrossRef]
- Harmanci, S.; Dutta, A.; Cesur, S.; Sahin, A.; Gunduz, O.; Kalaskar, D.M.; Ustundag, C.B. Production of 3D Printed Bi-Layer and Tri-Layer Sandwich Scaffolds with Polycaprolactone and Poly (vinyl alcohol)-Metformin towards Diabetic Wound Healing. Polymers 2022, 14, 5306. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.H.; Lee, Y.W.; Jung, W.K.; Oh, J.; Nam, S.Y. Enhanced rheological behaviors of alginate hydrogels with carrageenan for extrusion-based bioprinting. J. Mech. Behav. Biomed. Mater. 2019, 98, 187–194. [Google Scholar] [CrossRef]
- López-González, I.; Hernández-Heredia, A.B.; Rodríguez-López, M.I.; Auñón-Calles, D.; Boudifa, M.; Gabaldón, J.A.; Meseguer-Olmo, L. Evaluation of the In Vitro Antimicrobial Efficacy against Staphylococcus aureus and epidermidis of a Novel 3D-Printed Degradable Drug Delivery System Based on Polycaprolactone/Chitosan/Vancomycin—Preclinical Study. Pharmaceutics 2023, 15, 1763. [Google Scholar] [CrossRef]
- Utomo, E.; Domínguez-Robles, J.; Anjani, Q.K.; Picco, C.J.; Korelidou, A.; Magee, E.; Donnelly, R.F.; Larrañeta, E. Development of 3D-printed vaginal devices containing metronidazole for alternative bacterial vaginosis treatment. Int. J. Pharm. X 2023, 5, 100142. [Google Scholar] [CrossRef] [PubMed]
- Jeong, Y.; Jeong, S.; Kim, S.; Kim, H.J.; Jo, J.; Shanmugasundaram, A.; Kim, H.; Choi, E.; Lee, D. 3D-printed cardiovascular polymer scaffold reinforced by functional nanofiber additives for tunable mechanical strength and controlled drug release. Chem. Eng. J. 2023, 454, 140118. [Google Scholar] [CrossRef]
- Asiri, S.M.; Khan, F.A.; Bozkurt, A. Synthesis of chitosan nanoparticles, chitosan-bulk, chitosan nanoparticles conjugated with glutaraldehyde with strong anti-cancer proliferative capabilities. Artif. Cells Nanomed. Biotechnol. 2018, 46 (Suppl. S3), 1152–1161. [Google Scholar] [CrossRef]
- Guibal, E. Interactions of metal ions with chitosan-based sorbents: A review. Sep. Purif. Technol. 2004, 38, 43–74. [Google Scholar] [CrossRef]
- Sabbatini, B.; Cambriani, A.; Cespi, M.; Palmieri, G.F.; Perinelli, D.R.; Bonacucina, G. An overview of natural polymers as reinforcing agents for 3D printing. ChemEngineering 2021, 5, 78. [Google Scholar] [CrossRef]
- Baykara, D.; Pilavci, E.; Ulag, S.; Okoro, O.V.; Nie, L.; Shavandi, A.; Koyuncu, A.C.; Ozakpinar, O.B.; Eroglu, M.; Gunduz, O. In vitro electrically controlled amoxicillin release from 3D-printed chitosan/bismuth ferrite scaffolds. Eur. Polym. J. 2023, 193, 112105. [Google Scholar] [CrossRef]
- Koumentakou, I.; Noordam, M.J.; Michopoulou, A.; Terzopoulou, Z.; Bikiaris, D.N. 3D-Printed Chitosan-Based Hydrogels Loaded with Levofloxacin for Tissue Engineering Applications. Biomacromolecules 2023, 24, 4019–4032. [Google Scholar] [CrossRef]
- Ioannou, N.; Luo, J.; Qin, M.; Di Luca, M.; Mathew, E.; Tagalakis, A.D.; Lamprou2, D.A.; Yu-Wai-Man, C. 3D-printed long-acting 5-fluorouracil implant to prevent conjunctival fibrosis in glaucoma. J. Pharm. Pharmacol. 2023, 75, 276–286. [Google Scholar] [CrossRef] [PubMed]
- Necas, J.; Bartosikova, L.; Brauner, P.; Kolar, J. Hyaluronic acid (hyaluronan): A review. Vet. Med. 2008, 53, 397–411. [Google Scholar] [CrossRef]
- Ouyang, L.; Highley, C.B.; Rodell, C.B.; Sun, W.; Burdick, J.A. 3D printing of shear-thinning hyaluronic acid hydrogels with secondary cross-linking. ACS Biomater. Sci. Eng. 2016, 2, 1743–1751. [Google Scholar] [CrossRef] [PubMed]
- Liu, F.; Chen, Q.; Liu, C.; Ao, Q.; Tian, X.; Fan, J.; Tong, H.; Wang, X. Natural Polymers for Organ 3D Bioprinting. Polymers 2018, 10, 1278. [Google Scholar] [CrossRef]
- Shi, W.; Hass, B.; Kuss, M.A.; Zhang, H.; Ryu, S.; Zhang, D.; Li, T.; Li, Y.; Duan, B. Fabrication of versatile dynamic hyaluronic acid-based hydrogels. Carbohydr. Polym. 2020, 233, 115803. [Google Scholar] [CrossRef] [PubMed]
- Zhang, Q.; Zhou, X.; Du, H.; Ha, Y.; Xu, Y.; Ao, R.; He, C. Bifunctional Hydrogel-Integrated 3D Printed Scaffold for Repairing Infected Bone Defects. ACS Biomater. Sci. Eng. 2023, 9, 4583–4596. [Google Scholar] [CrossRef] [PubMed]
- Hwang, S.H.; Kim, J.; Heo, C.; Yoon, J.; Kim, H.; Lee, S.; Park, H.W.; Heo, M.S.; Moon, H.E.; Kim, C.; et al. 3D printed multi-growth factor delivery patches fabricated using dual-crosslinked decellularized extracellular matrix-based hybrid inks to promote cerebral angiogenesis. Acta Biomater. 2023, 157, 137–148. [Google Scholar] [CrossRef] [PubMed]
- Hao, L.; Tianyuan, Z.; Zhen, Y.; Fuyang, C.; Jiang, W.; Zineng, Y.; Zhengang, D.; Shuyun, L.; Chunxiang, H.; Zhiguo, Y.; et al. Biofabrication of cell-free dual drug-releasing biomimetic scaffolds for meniscal regeneration. Biofabrication 2022, 14, 015001. [Google Scholar] [CrossRef] [PubMed]
- Srivastava, N.; Srivastava, M.; Mishra, P.K.; Gupta, V.K. Substrate Analysis for Effective Biofuels Production, 1st ed.; Springer Nature: Singapore, 2020; pp. 149–168. [Google Scholar] [CrossRef]
- Xu, W.; Wang, X.; Sandler, N.; Willfor, S.; Xu, C. Three-dimensional printing of wood-derived biopolymers: A review focused on biomedical applications. ACS Sustain. Chem. Eng. 2018, 6, 5663–5680. [Google Scholar] [CrossRef] [PubMed]
- Dai, L.; Cheng, T.; Duan, C.; Zhao, W.; Zhang, W.; Zou, X.; Aspler, J.; Ni, Y. 3D printing using plant-derived cellulose and its derivatives: A review. Carbohydr. Polym. 2019, 203, 71–86. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.; Durand, H.; Zeno, E.; Balsollier, C.; Watbled, B.; Sillard, C.; Fort, S.; Baussanne, I.; Belgacem, N.; Lee, D.; et al. The surface chemistry of a nanocellulose drug carrier unravelled by MAS-DNP. Chem. Sci. 2020, 11, 3868. [Google Scholar] [CrossRef]
- Johannesson, J.; Pathare, M.M.; Johansson, M.; Bergström, C.A.; Teleki, A. Synergistic stabilization of emulsion gel by nanoparticles and surfactant enables 3D printing of lipid-rich solid oral dosage forms. J. Colloid Interface Sci. 2023, 650, 1253–1264. [Google Scholar] [CrossRef] [PubMed]
- Roche, A.; Sanchez-Ballester, N.M.; Aubert, A.; Rossi, J.C.; Begu, S.; Soulairol, I. Preliminary Study on the Development of Caffeine Oral Solid Form 3D Printed by Semi-Solid Extrusion for Application in Neonates. AAPS PharmSciTech 2023, 24, 122. [Google Scholar] [CrossRef] [PubMed]
- Deshmukh, S.N.; Dive, A.M.; Moharil, R.; Munde, P. Enigmatic insight into collagen. J. Oral Maxillofac. Pathol. 2016, 20, 276. [Google Scholar] [CrossRef] [PubMed]
- Nocera, A.D.; Salvatierra, N.A.; Cid, M.P. Printing Collagen 3D Structures. In Proceedings of the VI Latin American Congress on Biomedical Engineering, Paraná, Argentina, 29–31 October 2014. [Google Scholar] [CrossRef]
- Liu, H.; Wang, C.; Sun, X.; Zhan, C.; Li, Z.; Qiu, L.; Luo, R.; Liu, H.; Sun, X.; Li, R.; et al. Silk fibroin/collagen/hydroxyapatite scaffolds obtained by 3D printing technology and loaded with recombinant human erythropoietin in the reconstruction of alveolar bone defects. ACS Biomater. Sci. Eng. 2022, 8, 5245–5256. [Google Scholar] [CrossRef]
- Song, Y.; Hu, Q.; Liu, Q.; Liu, S.; Wang, Y.; Zhang, H. Design and fabrication of drug-loaded alginate/hydroxyapatite/collagen composite scaffolds for repairing infected bone defects. J. Mater. Sci. 2023, 58, 911–926. [Google Scholar] [CrossRef]
- Mutlu, M.E.; Ulag, S.; Sengor, M.; Daglılar, S.; Narayan, R.; Gunduz, O. Electrosprayed Collagen/Gentamicin nanoparticles coated microneedle patches for skin treatment. Mater. Lett. 2021, 305, 130844. [Google Scholar] [CrossRef]
- Khan, S.A. Mini-Review: Opportunities and challenges in the techniques used for preparation of gelatin nanoparticles. Pak. J. Pharm. Sci. 2020, 33, 221–228. [Google Scholar] [PubMed]
- Zaer, M.; Moeinzadeh, A.; Abolhassani, H.; Rostami, N.; Yaraki, M.T.; Seyedi, S.A.; Nabipoorashrafi, S.A.; Bashiri, Z.; Moeinabadi-Bidgoli, K.; Moradbeygi, F.; et al. Doxorubicin-loaded Niosomes functionalized with gelatine and alginate as pH-responsive drug delivery system: A 3D printing approach. Int. J. Biol. Macromol. 2023, 253, 126808. [Google Scholar] [CrossRef]
- Dai, X.; Zhang, J.; Bao, X.; Guo, Y.; Jin, Y.; Yang, C.; Zhang, H.; Liu, L.; Gao, Y.; Ye, C.; et al. Induction of Tumor Ferroptosis-Dependent Immunity via an Injectable Attractive Pickering Emulsion Gel. Adv. Mater. 2023, 35, e2303542. [Google Scholar] [CrossRef]
- Wei, H.; Luo, Y.; Ma, R.; Li, Y. Three-Dimensional Printing Multi-Drug Delivery Core/Shell Fiber Systems with Designed Release Capability. Pharmaceutics 2023, 15, 2336. [Google Scholar] [CrossRef]
- Cardoso, P.H.N.; Oliveira, C.Y.B.; Nunes, M.; Tavares, G.F.; Faia, P.M.; Araújo, E.S. Eudragit E100/Hesperidin 3D Printing Filaments: Preparation, Characterization, and In Vitro Release Studies. Appl. Sci. 2023, 13, 11558. [Google Scholar] [CrossRef]
- Alhnan, M.A. Solid Dosage Form. Production. Patent EP3191084B1, 28 November 2018. [Google Scholar]

| Active Pharmaceutical Ingredient | Additives for Filament Improvement | Printing Technique | Drug Dosage Form | Application | Ref. |
|---|---|---|---|---|---|
| Dronedarone hydrochloride (DH) and ascorbic acid (AC); 100 mg per capsule | none | FDM | oral capsules | normalization of sinus rhythm (DH) and vitamin C supplier (AC) | [35] |
| Ampicillin; 10 mg per 13% w/v of PVA | gold nanoparticles (osteogenic differentiation, increase biocompatibility and bone tissue development) | custom modified extrusion printing at room temperature | biomimetic scaffolds | bone tissue regeneration with antimicrobial properties | [55] |
| Naringenin; 5% of total mass | glycerol (plasticizer) | FDM | oral tablets | regulator of tumor cell growth and angiogenesis | [56] |
| Acetaminophen; 500 mg per tablet | hydroxypropyl methylcellulose (emulsifier and thickening agent) | FDM | oral capsules | [57] | |
| Acetaminophen (AC) and caffeine citrate (CC); 20% of total mass | PEO (plasticizer) | FDM | oral tablets | treatment of moderate pain and fever (AC); stimulant for fatigue reduction (CC) | [58] |
| Paliperidone palmitate; 10% of total mass | PEG, Poloxamer® 188 (plasticizers), and EVA (hydrophobicity and low processing temperature) | FDM | implantable dosage forms | treatment of schizophrenia | [59] |
| Urea; 10%, 30%, and 50% of total mass | PCL and PEG (improves urea release) | FDM | buccal patches | counteracts tooth decay | [60] |
| Dexamethasone acetate; 1.5% and 3.0% of total mass | xylitol (plasticizer), Chitosan (enhances penetration and adhesive capacity) | FDM | buccal patches | treatment of recurrent oral ulcer | [61] |
| Progesterone; 16.5% of total mass | PEG (plasticizer) | FDM | water-soluble suppository shell | hormone replacement | [62] |
| Amlodipine besylate; 2%, 2.5%, and 5% of total mass | sorbitol (improves mechanical properties and printability) | FDM | oral shell–core tablets | treatment of hypertension | [63] |
| Ciprofloxacin; 15.38% of total mass | nanohydroxyapatite (enhances bone regeneration) | FDM | bone implants | antibacterial activity | [64] |
| Polymer/Drug | Additives for Filament Improvement | Printing Technique | Pharmaceutical Form | Application | Ref. |
|---|---|---|---|---|---|
| TPU/Metformin hydrochloride and Theophylline anhydrous 60 wt% in different samples | PEO and pTHF (stiffness reduction) | FDM | oral tablets | treatment for diabetes and lung diseases (such as asthma) | [80] |
| PU/Paracetamol (16% w/w) | PEG (plasticizer) | hot-melt extrusion printing | drug-eluting implants | treatment of moderate pain and fever | [84] |
| PU/Minocycline (0.1 mg per sample) | PEG; PEGDA (plasticizers) and graphene (enhances mechanical strength and phototriggered release) | extrusion-based printing | bioscaffolds | tissue regeneration with antimicrobial activity | [85] |
| TPU/Salicylic acid (2% w/w) | Tetrahydrofuran or dichloromethane (solvents); PLA (increases mechanical strength) or PCL (flexibility enhancement) | FDM and SLA | nose patches/masks | treatment for acne | [86] |
| TPU/Ibuprofen (20% w/w) | none | FDM | oral tablets | relieves pain, fever, and inflammation | [87] |
| TPU/Theophylline (10% to 70% w/w) | none | FDM | drug-loaded filaments | treatment of pulmonary diseases | [88] |
| PU/Y27632 (0.100 µg mL−1 and 3.38 µg mL−1) | chemokine SDF-1 (improves controlled release) | inkjet printing | tissue engineering scaffolds | inhibition of calcium sensitization | [89] |
| TPU/Clotrimazole (2% and 10% w/w) | Castor oil (solvent) | FDM | intravaginal ring | treatment of recurrent vaginal candidiasis | [90] |
| PU/Rapamycin, 1% wt% | PLGA, PLLA (increases mechanical strength) and PEG (plasticizer) | extrusion- based printing | cardiovascular implant | prevention of organ transplant rejection | [91] |
| PU/Penicillin and Streptomycin, 1% wt%; insulin, 40 µU mL−1 | fetal bovine serum and nonessential amino acid solution (supplements for cell culture) | low-temperature deposition | cervical implants | repairs defected cervix and prevents virus infection | [92] |
| TPU/Tetracycline hydrochloride, 0.25, 0.5, and 1% wt% | Castor oil (solvent) | FDM | catheter | infection prevention | [93] |
| PU/zinc oxide (0.2 to 10 g/L) and Heparin (5.2 mg/mL) | Zein nanospheres (improve controlled release) | FDM | stent (implant) | prevention of thrombosis and infection | [94] |
| TPU/Acyclovir, 0.25 wt% | none | FFF | vaginal pessaries | treatment of stress urinary incontinence | [95] |
| TPU/17-β-estradiol, 0.25 and 1 wt% | Castor oil (solvent) | FDM | vaginal meshes (transvaginal implantation) | treatment of stress urinary incontinence and pelvic organ prolapse | [96] |
| TPU/Rifampicin, range between 0 and 1% (w/w) | Castor oil (solvent) | FDM | cardiovascular prosthesis | reduces the risk of infection or blood clot formation | [97] |
| PU/aloe vera gel, 13.31% of polyurethane weight | Titanium carbide (improves biodegradability) and Spidroin (improves biodegradability and mechanical strength) | extrusion- based printing | microneedle scaffolds | wound healing | [98] |
| Drug | Additives for Filament Improvement | Printing Technique | Pharmaceutical Form | Application | Ref. |
|---|---|---|---|---|---|
| Resveratrol (2 mg/mL and 4 mg/mL) | albumin nanoparticles (improve controlled release) and PCL (embedment into the scaffolds’ milipores) | FDM | scaffolds for bone tissue regeneration | osteoporosis and bone structuration treatment | [104] |
| Amikacin sulfate (14.29 wt%) | nanohydroxyapatite (enhances bone regeneration) | FDM | scaffolds for bone tissue regeneration | treatment of orthopedic infections (antibiotic) | [105] |
| Methotrexate (0.5, 1.5, and 2.5 wt%) | none | FDM | implantable and degradable scaffolds | treatment for cancer in the diseased area | [106] |
| Recombinant human bone morphogenetic protein-2 (0.3 µg/scaffold) | alginate- and gelatin-based biogels (enhance bone regeneration) | FDM | scaffolds for bone tissue regeneration | bone tissue regeneration | [107] |
| Chlorhexidine Clathrate (3 wt%) | nanohydroxyapatite (enhances bone regeneration) and β-cyclodextrin (improves sustained release) | FFF | scaffolds for bone tissue engineering | osteogenesis treatment with anti-infective properties | [108] |
| Estradiol Valerate (29.79 mg per device) | almond oil, PEG (solvents), and silicon dioxide (mechanical strength improvement) | FDM | transdermal microneedle arrays | hormone therapy | [109] |
| Venlafaxine Hydrochloride, 25 wt% | hydroxypropyl methylcellulose (solvent) and triethyl citrate (plasticizer) | FDM | intragastric floating device with insoluble PLA shell and internal soluble substrate | treatment of depression | [110] |
| Rhodamine B, 0.02 mg per microneedle (surface) | carboxymethyl cellulose (solvent for drug coating) | FDM | microneedles | not specified | [111] |
| Simvastatin (3% of dry polymer weight) | PEG (plasticizer), N-methacryloyl Chitosan, and polyethylene glycol di(meth)acrylate (increase the cross-linking velocity) | inkjet-based printing | implantable hydrogels | osteogenic stimulation | [112] |
| Riboflavin, 20 mg/g of PEG | PEG (solvent and plasticizer) | FDM | oral tablets | vitamin B2 supplement | [113] |
| Metronidazole, 500 mg per tablet | PVP (mechanical strength improvement) | FDM | oral tablets with anti-flip-up design | treatment for Helicobacter pylori infection | [114] |
| Rhodamine B (dissolvable coating), 15.38 wt% | carboxymethyl cellulose (solvent for drug coating) | SLA | transdermal microneedles | not specified | [115] |
| Methylene blue (68.6 mg per implant) and Ibuprofen sodium (68.1 mg per implant) | PEG (plasticizer), PVA, and PCL (mechanical strength improvement) | FFF | implantable devices | release test of hydrophilic model compounds | [116] |
| Nadolol (131 mg, 110 mg, and 91 mg per capsule) and Metoprolol Tartrate (152 mg, 130 mg, and 105 mg per capsule) | anionic cellulose nanofiber hydrogel (improves sustained release) | FDM | implantable capsules | hypertension treatment | [117] |
| Minocycline hydrochloride, 0.1 mg/mg of collagen | collagen (improves biocompatibility) and citrate- hydroxyapatite nanoparticles (enhances bone regeneration) | FDM | scaffolds for bone structural support | antimicrobial and osteogenic effects for bone regeneration | [118] |
| Warfarin sodium, 8.5 and 10.16 mg/cm of film length | glycerol and PEG (plasticizers) | FFF | oro-dispersible films | treatment for blood clots | [119] |
| Drug | Additives for Filament Improvement | Printing Technique | Pharmaceutical Form | Application | Ref. |
|---|---|---|---|---|---|
| Ibuprofen (15 wt%) | none | FDM | biodegradable implants | relieves pain, fever, and inflammation | [122] |
| Chlorhexidine (20 mg/mL) | β-tricalcium phosphate nanoparticles (improve osteoconductive characteristics), dichloromethane (solvent), and graphene oxide (improves sustained release) | inkjet-based printing | implantable scaffolds for bone regeneration | prevents implant- related bone infection and osteogenic therapy | [125] |
| Deferoxamine (3.3 wt%) | bone morphogenetic protein (bone healing enhancement) and tricalcium phosphate (improves osteoconductive characteristics) | low- temperature deposition printing | implantable scaffolds | coupling regeneration of blood vessels and bones | [126] |
| HA15 (200 μg per 3 g of PLGA) | β-tricalcium phosphate (improves osteoconductive characteristics) | inkjet-based printing | bone tissue scaffold | treatment of bone defects | [127] |
| Transforming growth factor- beta 1 (TGF-β1), 4.47 wt% | collagen (improves sustained release) | extrusion- based printing | implantable scaffolds | management of bone cell behavior | [128] |
| Lidocaine (224 mg per device), Metronidazole, and Estradiol (112 mg per device-each) | connective tissue growth factor (improves biocompatibility) and PCL (improves sustained release) | extrusion-based printing | degradable meshes | treatment for female pelvic organ prolapse | [129] |
| Paclitaxel, Rapamycin, and Lidocaine (60 mg per device-each) | PEG (plasticizer) | FDM | multilayered films and single-layered discs (local implants) | treatment for brain cancer | [130] |
| Cisplatin (6 mg per 0.3 g of PLGA) | PLA (improves absorption) | extrusion- based printing | topical implant stents | treatment for ovarian cancer | [131] |
| Doxorubicin (18 mg) and Cisplatin (1.15 mg) per 3 g of PLGA | N,N- dimethylformamide (solvent) | customized jet printing | implantable scaffolds | treatment for breast cancer | [132] |
| Temozolomide (7 to 61 wt%) | PVA, dichloromethane (solvent) | inkjet-based bioprinting | implantable drug-releasing mesh | treatment for glioblastoma | [133] |
| Recombinant human bone morphogenetic protein 2 (4 μg/g of chitosan) | nanohydroxyapatite (enhances bone regeneration); cytokine and chitosan (improve sustained release) | extrusion-based printing | implantable scaffolds | bone repair | [134] |
| Drug | Additives for Filament Improvement | Printing Technique | Pharmaceutical Form | Application | Ref. |
|---|---|---|---|---|---|
| Enrofloxacin (4 wt%) | oil, genipin (solvents), and chitosan (emulsion droplet costabilizer) | inkjet-based printing | implantable scaffolds | antibacterial activity | [137] |
| Ibuprofen (2.5 wt%) | aqueous PVA (solvent) and nanoclay (mechanical strength improvement) | extrusion- based printing | implantable scaffolds | anti-inflammatory treatment | [138] |
| Kartogenin (50 μM/g of extracellular matrix) | beta cyclodextrin (improves interaction between drug and polymer), alginate (increases biocompatibility), cartilage (enhancement of cartilage tissue reconstruction), extracellular matrix (mimics tissue properties), and starch (increases polymer flexibility) | extrusion- based printing | microfiber network (polymer) with incorporated hydrogel | reinforces the construct for cartilage tissue engineering | [139] |
| SB216763 and ICRT-14 (2 μM per 105 ST2 cells, for both drugs) | cultured cells, antibodies (interaction with bone formation), and plasmid (improves cell interaction) | extrusion- based printing | bioactive implantable scaffolds | osteogenic treatment | [140] |
| Tetracycline (40 to 60 mg per device) | PLA (improves sustained release), glycerol (improves bacteria incubation) | FDM | reservoir-type implants | antimicrobial treatment | [141] |
| Sodium fluoride (0, 10, 15, and 30 wt%) | PEG (plasticizer) or PVA (mechanical strength improvement) | FDM | personalized mouthguards | treatment for dental decay | [142] |
| Kartogenin (4 mg per 120 mg of PLGA) | meniscus extracellular matrix (improves cell activity) and PLGA (improves sustained release) | FDM | implantable scaffolds | repairs meniscus defects | [143] |
| Tetracycline hydrochloride (0.5, 0.75, and 1.0 wt%) | iron oxide nanoparticles (substances for supramagnetic contrast) | FDM | micropored capsules | infection prevention | [144] |
| Ciprofloxacin (0, 10, and 20 wt%) | PEG (plasticizer) | FDM | oral tablets | antimicrobial treatment | [145] |
| Methylene blue (MB-68.6 mg per device) and Ibuprofen sodium (IB-68.1 mg per device) | PEG (plasticizer) | FFF | implant coatings | treatment for methemoglobinemia (MB) and relief of pain, fever, and inflammation (IB) | [146] |
| Resveratrol and Strontium ranelate (10 mg per device) | β-tricalcium phosphate (improves continuous bioactivity), Hyaluronic acid, and Gelatin (increases biocompatibility) | inkjet-based printing | implantable scaffolds | mandibular bone regeneration | [147] |
| Doxorubicin (0.4 and 2 mg/g of PCL) | none | FDM | implantable scaffolds | therapy for breast cancer | [148] |
| Metformin (3 wt%) | PVA (mechanical strength improvement and accelerates drug release) | extrusion- based printing | implantable scaffolds | therapy for type 2 diabetes mellitus | [149] |
| Amoxicillin (0.4, 0.8, and 1.6 wt%) and Cefotaxime (0.8, 1.8, and 3.1 wt %) | none | extrusion-based printing | stents | treatment for obstructive salivary gland disease | [150] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Cardoso, P.H.N.; Araújo, E.S. An Approach to 3D Printing Techniques, Polymer Materials, and Their Applications in the Production of Drug Delivery Systems. Compounds 2024, 4, 71-105. https://doi.org/10.3390/compounds4010004
Cardoso PHN, Araújo ES. An Approach to 3D Printing Techniques, Polymer Materials, and Their Applications in the Production of Drug Delivery Systems. Compounds. 2024; 4(1):71-105. https://doi.org/10.3390/compounds4010004
Chicago/Turabian StyleCardoso, Pedro H. N., and Evando S. Araújo. 2024. "An Approach to 3D Printing Techniques, Polymer Materials, and Their Applications in the Production of Drug Delivery Systems" Compounds 4, no. 1: 71-105. https://doi.org/10.3390/compounds4010004
APA StyleCardoso, P. H. N., & Araújo, E. S. (2024). An Approach to 3D Printing Techniques, Polymer Materials, and Their Applications in the Production of Drug Delivery Systems. Compounds, 4(1), 71-105. https://doi.org/10.3390/compounds4010004






