Role of Sonographic Second Trimester Soft Markers in the Era of Cell-Free DNA Screening Options: A Review
Abstract
:1. Introduction
2. Soft Markers
2.1. Absent or Hypoplastic Nasal Bone
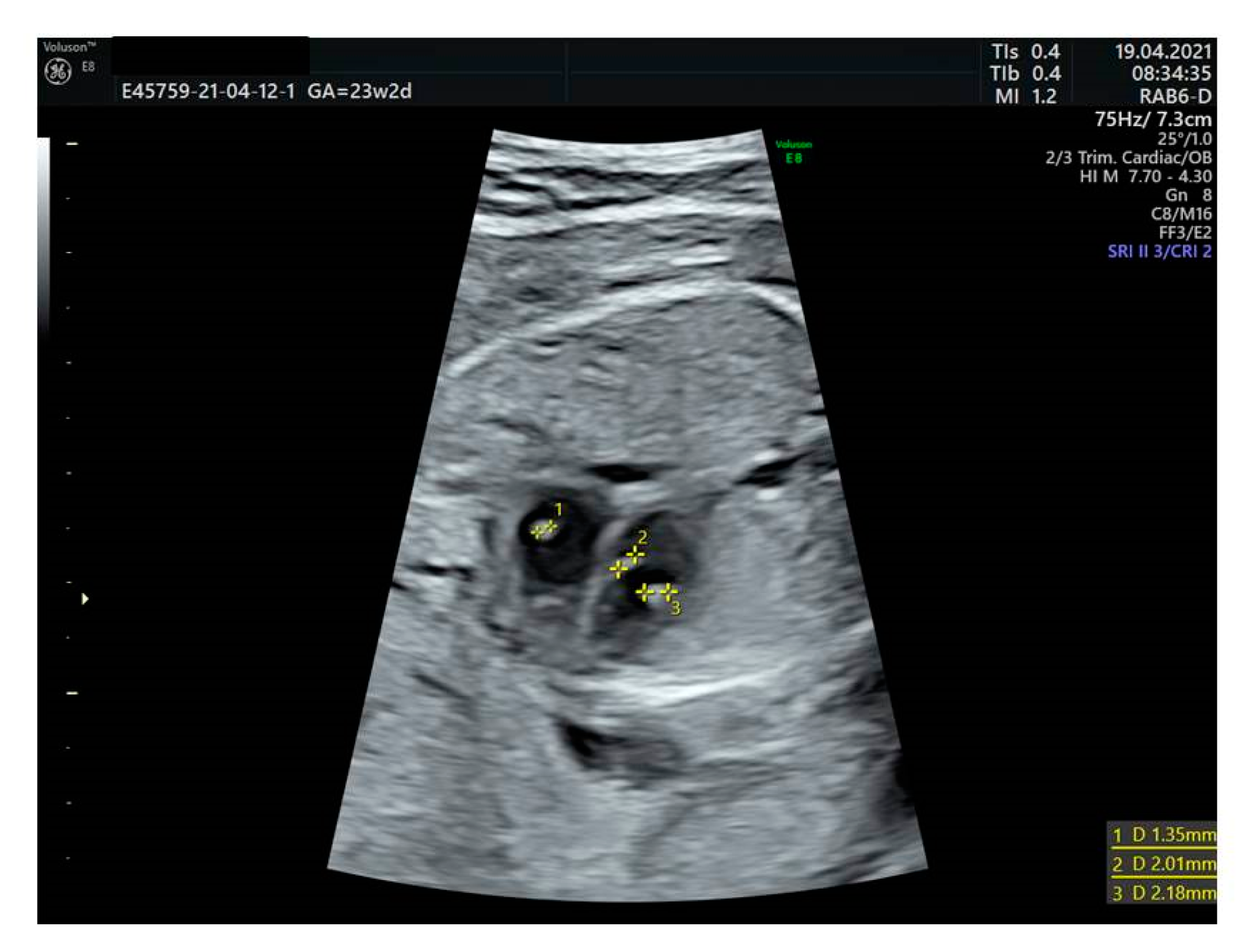
2.2. Intracardiac Echogenic Focus
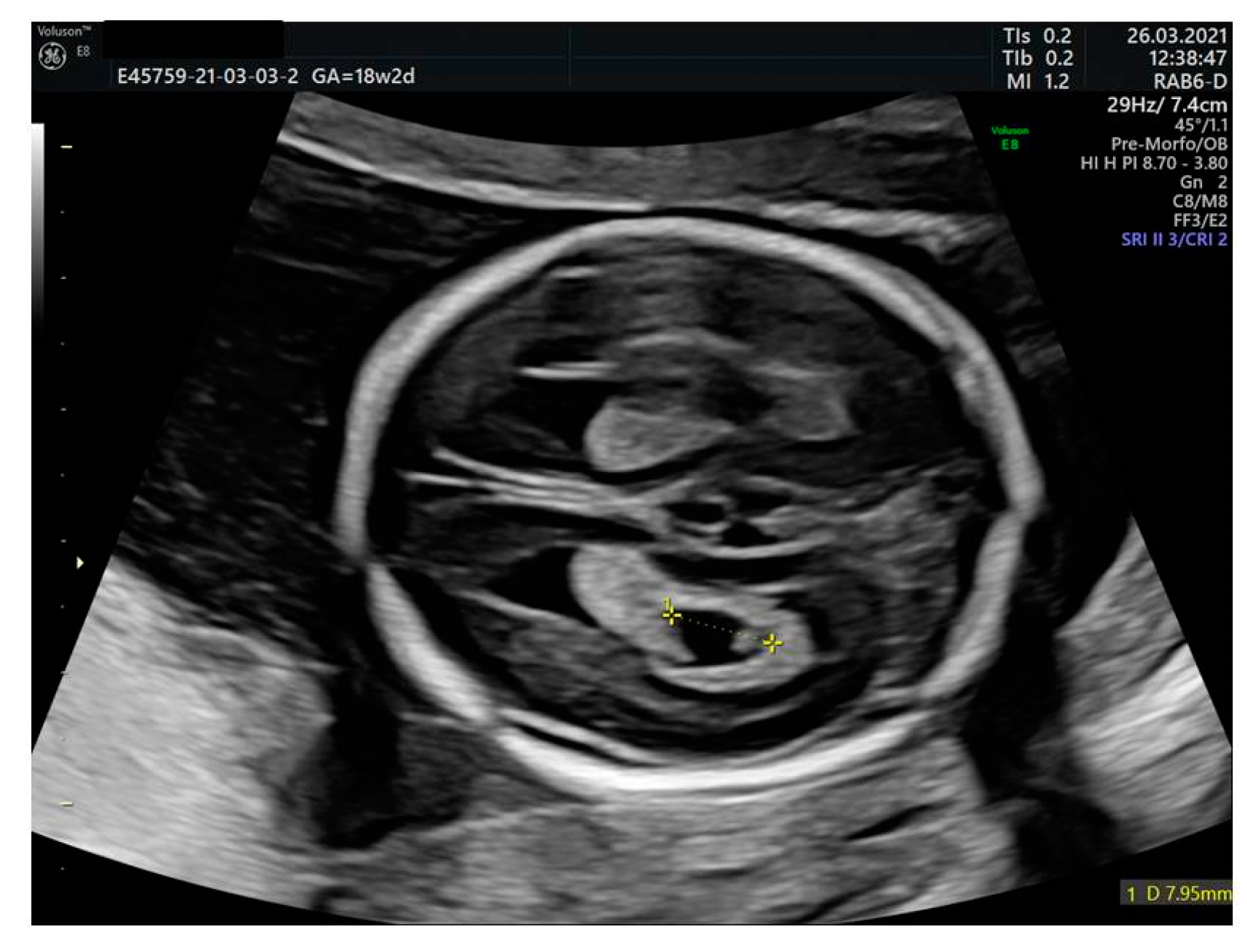
2.3. Ventriculomegaly
2.4. Thickened Nuchal Fold
2.5. Choroid Plexus Cyst
2.6. Echogenic Bowel
2.7. Urinary Tract Dilation
2.8. Shortened Long Bones
| Soft Markers | Imaging Criteria |
|---|---|
| Absent or hypoplastic nasal bone (NB) | The midsagittal plane of the fetal profile should be defined as hypoplastic when it is either absent or with a length of less than 2.5 mm [20]. |
| Echogenic intracardiac foci (EIF) | Hyperechogenicity of fetal soft tissue greater than or equal in brightness to the surrounding bone [23] |
| Mild to moderate ventriculomegaly (VM) | Measured in an axial transventricular plane at the atrium of the posterior horn with calipers placed over the inner edges [31]. Ventriculomegaly is categorized as mild between 10 and 11.9 mm), moderate between 12 and 14.9 mm [31]. |
| Thickened nuchal fold (NF) | Greater than or equal to 6 mm from the outer edge of the occipital bone to the outer skin in the midline at 15–20 weeks [40,41]. |
| Choroid plexus cyst (CPC) | Cyst of ≥ 5 mm in one or both choroid plexus(es) [48,49]. |
| Echogenic bowel (EB) | Fetal intestines display echogenicity equal to or greater than that of the adjacent bone [61,62]. |
| Urinary tract dilation (UTD) | Renal pelvis measuring >4 mm in anterior–posterior renal pelvis diameter up to 20 weeks of gestation [68]. |
| Shortened long bones | Measurement, 2.5th percentile for gestational age [72,73]. |
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Benn, P.; Borrell, A.; Chiu, R.W.K.; Cuckle, H.; Dugoff, L.; Faas, B.; Gross, S.; Huang, T.; Johnson, J.; Maymon, R.; et al. Position statement from the Chromosome Abnormality Screening Committee on behalf of the Board of the International Society for Prenatal Diagnosis. Prenat. Diagn. 2015, 35, 725–734. [Google Scholar] [CrossRef]
- Taylor-Phillips, S.; Freeman, K.; Geppert, J.; Agbebiyi, A.; Uthman, O.A.; Madan, J.; Clarke, A.; Quenby, S.; Clarke, A. Accuracy of non-invasive prenatal testing using cell-free DNA for detection of Down, Edwards and Patau syndromes: A systematic review and meta-analysis. BMJ Open 2016, 6, e010002. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Benacerraf, B.R. The Role of the Second Trimester Genetic Sonogram in Screening for Fetal Down Syndrome. Semin. Perinatol. 2005, 29, 386–394. [Google Scholar] [CrossRef] [PubMed]
- Agathokleous, M.; Chaveeva, P.; Poon, L.C.; Kosinski, P.; Nicolaides, K.H. Meta-analysis of second-trimester markers for trisomy 21. Ultrasound Obstet. Gynecol. 2013, 41, 247–261. [Google Scholar] [CrossRef]
- Hu, T.; Tian, T.; Zhang, Z.; Wang, J.; Hu, R.; Xiao, L.; Zhu, H.; Lai, Y.; Wang, H.; Liu, S. Prenatal chromosomal microarray analysis in 2466 fetuses with ultrasonographic soft markers: A prospective cohort study. Am. J. Obstet. Gynecol. 2021, 224, 516.e1–516.e16. [Google Scholar] [CrossRef] [PubMed]
- Kotsopoulou, I.; Tsoplou, P.; Mavrommatis, K.; Kroupis, C. Non-invasive prenatal testing (NIPT): Limitations on the way to become diagnosis. Diagnosis 2015, 2, 141–158. [Google Scholar] [CrossRef] [PubMed]
- Nicolaides, K.H.; Snijders, R.J.; Gosden, C.M.; Berry, C.; Campbell, S. Ultrasonographically detectable markers of fetal chromosomal abnormalities. Lancet 1992, 340, 704–707. [Google Scholar] [CrossRef]
- American College of Obstetricians and Gynecologists. Practice bulletin no. 162: Prenatal diagnostic testing for genetic disorders. Obstet. Gynecol. 2016, 127, e108–e122. [Google Scholar] [CrossRef]
- Practice Bulletin No. 162 Summary: Prenatal Diagnostic Testing for Genetic Disorders. Obstet. Gynecol. 2016, 127, 976–978. [CrossRef] [PubMed]
- American College of Obstetricians and Gynecologists’ Committee on Practice Bulletins—Obstetrics; Committee on Genetics; Society for Maternal-Fetal Medicine. Screening for Fetal Chromosomal Abnormalities: ACOG Practice Bulletin, Number 226. Obstet. Gynecol. 2020, 136, e48–e69. [Google Scholar] [CrossRef] [PubMed]
- Perinatal Services BC. Obstetric Guideline: Prenatal Screening for Down Syndrome, Trisomy 18, and Open Neural Tube Defects. June 2016. Available online: www.perinatalservicesbc.ca/health-professionals/professional-resources/screening/prenatal-genetic (accessed on 31 January 2018).
- Society for Maternal-Fetal Medicine (SMFM). Society for Maternal-Fetal Medicine Consult Series #57: Evaluation and management of isolated soft ultrasound markers for aneuploidy in the second trimester: (Replaces Consults #10, Single umbilical artery, October 2010; #16, Isolated echogenic bowel diagnosed on second-trimester ultrasound, August 2011; #17, Evaluation and management of isolated renal pelviectasis on second-trimester ultrasound, December 2011; #25, Isolated fetal choroid plexus cysts, April 2013; #27, Isolated echogenic intracardiac focus, August 2013). Am. J. Obstet. Gynecol. 2021, 225, B2–B15. [Google Scholar] [CrossRef]
- Zoppi, M.A.; Ibba, R.M.; Axiana, C.; Floris, M.; Manca, F.; Monni, G. Absence of fetal nasal bone and aneuploidies at first-trimester nuchal translucency screening in unselected pregnancies. Prenat. Diagn. 2003, 23, 496–500. [Google Scholar] [CrossRef]
- Viora, E.; Masturzo, B.; Errante, G.; Sciarrone, A.; Bastonero, S.; Campogrande, M. Ultrasound evaluation of fetal nasal bone at 11 to 14 weeks in a consecutive series of 1906 fetuses. Prenat. Diagn. 2003, 23, 784–787. [Google Scholar] [CrossRef] [PubMed]
- Bromley, B.; Lieberman, E.; Shipp, T.D.; Benacerraf, B.R. Fetal nose bone length: A marker for Down syndrome in the second trimester. J. Ultrasound Med. 2002, 21, 1387–1394. [Google Scholar] [CrossRef] [PubMed]
- Gianferrari, E.A.; Benn, P.A.; Dries, L.; Brault, K.; Egan, J.F.X.; Zelop, C.M. Absent or Shortened Nasal Bone Length and the Detection of Down Syndrome in Second-Trimester Fetuses. Obstet. Gynecol. 2007, 109, 371–375. [Google Scholar] [CrossRef] [PubMed]
- Vintzileos, A.; Walters, C.; Yeo, L. Absent nasal bone in the prenatal detection of fetuses with trisomy 21 in a high-risk population. Obstet. Gynecol. 2003, 101, 905–908. [Google Scholar] [CrossRef] [PubMed]
- Cicero, S.; Sonek, J.D.; McKenna, D.S.; Croom, C.S.; Johnson, L.; Nicolaides, K.H. Nasal bone hypoplasia in trisomy 21 at 15–22 weeks’ gestation. Ultrasound Obstet. Gynecol. 2003, 21, 15–18. [Google Scholar] [CrossRef] [PubMed]
- Sonek, J.D.; McKenna, D.; Webb, D.; Croom, C.; Nicolaides, K. Nasal bone length throughout gestation: Normal ranges based on 3537 fetal ultrasound measurements. Ultrasound Obstet. Gynecol. 2003, 21, 152–155. [Google Scholar] [CrossRef] [PubMed]
- Moreno-Cid, M.; Rubio-Lorente, A.; Rodríguez, M.J.; Bueno-Pacheco, G.; Tenias, J.M.; Román-Ortiz, C.; Arias, Á. Systematic review and meta-analysis of performance of second-trimester nasal bone assessment in detection of fetuses with Down syndrome. Ultrasound Obstet. Gynecol. 2014, 43, 247–253. [Google Scholar] [CrossRef] [Green Version]
- Xing, Y.; Holder, J.L., Jr.; Liu, Y.; Yuan, M.; Sun, Q.; Qu, X.; Deng, L.; Zhou, J.; Yang, Y.; Guo, M.; et al. Prenatal diagnosis of Wolf-Hirschhorn syndrome: From ultrasound findings, diagnostic technology to genetic counseling. Arch. Gynecol. Obstet. 2018, 298, 289–295. [Google Scholar] [CrossRef]
- Sherer, D.M.; Eugene, P.; Dalloul, M.; Khoury-Collado, F.; Abdelmalek, E.; Kheyman, M.; Osho, J.A.; Abulafia, O. Second-Trimester Diagnosis of Cri du Chat (5p-) Syndrome Following Sonographic Depiction of an Absent Fetal Nasal Bone. J. Ultrasound Med. 2006, 25, 387–388. [Google Scholar] [CrossRef]
- Bronshtein, M.; Jakobi, P.; Ofir, C. Multiple fetal intracardiac echogenic foci: Not always a benign sonographic finding. Prenat. Diagn. 1996, 16, 131–135. [Google Scholar] [CrossRef]
- Levy, D.W.; Mintz, M.C. The left ventricular echogenic focus: A normal finding. AJR Am. J. Roentgenol. 1988, 150, 85–86. [Google Scholar] [CrossRef] [PubMed]
- Lorente, A.M.R.; Moreno-Cid, M.; Rodríguez, M.J.; Bueno, G.; Tenias, J.M.; Román, C.; Arias, Á.; Pascual, A. Meta-analysis of validity of echogenic intracardiac foci for calculating the risk of Down syndrome in the second trimester of pregnancy. Taiwan J. Obstet. Gynecol. 2017, 56, 16–22. [Google Scholar] [CrossRef] [PubMed]
- Winter, T.C.; Anderson, A.M.; Cheng, E.Y.; Komarniski, C.A.; Souter, V.L.; Uhrich, S.B.; Nyberg, D.A. Echogenic Intracardiac Focus in 2nd-Trimester Fetuses with Trisomy 21: Usefulness as a US Marker. Radiology 2000, 216, 450–456. [Google Scholar] [CrossRef] [PubMed]
- Chiu, G.; Zhao, A.; Zhang, B.; Zhang, T. Intracardiac echogenic focus and its location: Association with congenital heart defects. J. Matern. Fetal Neonatal Med. 2019, 32, 3074–3078. [Google Scholar] [CrossRef] [PubMed]
- Bradley, K.E.; Santulli, T.S.; Gregory, K.D.; Herbert, W.; Carlson, D.E.; Platt, L.D. An isolated intracardiac echogenic focus as a marker for aneuploidy. Am. J. Obstet. Gynecol. 2005, 192, 2021–2026. [Google Scholar] [CrossRef]
- Wax, J.R.; Royer, D.; Mather, J.; Chen, C.; Aponte-García, A.; Steinfeld, J.D.; Ingardia, C.J. A preliminary study of sonographic grading of fetal intracardiac echogenic foci: Feasibility, reliability and association with aneuploidy. Ultrasound Obstet. Gynecol. 2000, 16, 123–127. [Google Scholar] [CrossRef] [PubMed]
- Sotiriadis, A.; Makrydimas, G.; Ioannidis, J.P. Diagnostic performance of intracardiac echogenic foci for Down syndrome: A meta-analysis. Obstet. Gynecol. 2003, 101, 1009–1016. [Google Scholar] [CrossRef]
- International Society of Ultrasound in Obstetrics & Gynecology Education Committee. Sonographic examination of the fetal central nervous system: Guidelines for performing the ‘basic examination’ and the ‘fetal neurosonogram’. Ultrasound Obstet. Gynecol. 2007, 29, 109–116. [Google Scholar] [CrossRef] [PubMed]
- Cardoza, J.D.; Goldstein, R.B.; Filly, R.A. Exclusion of fetal ventriculomegaly with a single measurement: The width of the lateral ventricular atrium. Radiology 1988, 169, 711–714. [Google Scholar] [CrossRef] [PubMed]
- Society for Maternal-Fetal Medicine (SMFM); Fox, N.S.; Monteagudo, A.; Kuller, J.A.; Craigo, S.; Norton, M.E. Mild fetal ventriculomegaly: Diagnosis, evaluation, and management. Am. J. Obstet. Gynecol. 2018, 219, B2–B9. [Google Scholar] [CrossRef] [PubMed]
- Weichert, J.; Hartge, D.; Krapp, M.; Germer, U.; Gembruch, U.; Axt-Fliedner, R. Prevalence, Characteristics and Perinatal Outcome of Fetal Ventriculomegaly in 29,000 Pregnancies Followed at a Single Institution. Fetal Diagn. Ther. 2010, 27, 142–148. [Google Scholar] [CrossRef] [PubMed]
- Bromley, B.; Frigoletto, F.D., Jr.; Benacerraf, B.R. Mild fetal lateral cerebral ventriculomegaly: Clinical course and outcome. Am. J. Obstet. Gynecol. 1991, 164, 863–867. [Google Scholar] [CrossRef]
- Graham, E.; Duhl, A.; Ural, S.; Allen, M.; Blakemore, K.; Witter, F. The degree of antenatal ventriculomegaly is related to pediatric neurological morbidity. J. Matern. Fetal Neonatal Med. 2001, 10, 258–263. [Google Scholar] [CrossRef]
- Pilu, G.; Falco, P.; Gabrielli, S.; Perolo, A.; Sandri, F.; Bovicelli, L. The clinical significance of fetal isolated cerebral borderline ventriculomegaly: Report of 31 cases and review of the literature. Ultrasound Obstet. Gynecol. 1999, 14, 320–326. [Google Scholar] [CrossRef] [PubMed]
- Simioli, S.; Napolitano, R.; Quaglia, F.; Mazzarelli, L.L.; Agangi, A.; Milanes, G.M.; Tessitore, G.; Iannaccone, A.; Maruotti, G.M.; Martinelli, P. Fetal borderline cerebral ventriculomegaly: Clinical significance and management. Minerva Ginecol. 2009, 61, 109–112. [Google Scholar]
- Wang, Y.; Hu, P.; Xu, Z. Copy number variations and fetal ventriculomegaly. Curr. Opin. Obstet. Gynecol. 2018, 30, 104–110. [Google Scholar] [CrossRef] [PubMed]
- Shipp, T.D.; Benacerraf, B.R. Second trimester ultrasound screening for chromosomal abnormalities. Prenat. Diagn. 2002, 22, 296–307. [Google Scholar] [CrossRef] [PubMed]
- Miguelez, J.; De Lourdes Brizot, M.; Liao, A.W.; De Carvalho, M.H.; Zugaib, M. Second-trimester soft markers: Relation to first-trimester nuchal translucency in unaffected pregnancies. Ultrasound Obstet Gynecol. 2012, 39, 274–278. [Google Scholar] [CrossRef]
- Borrell, A.; Costa, D.; Martinez, J.M.; Delgado, R.D.; Farguell, T.; Fortuny, A. Criteria for fetal nuchal thickness cut-off: A re-evaluation. Prenat. Diagn. 1997, 17, 23–29. [Google Scholar] [CrossRef]
- Crane, J.P.; Gray, D.L. Sonographically measured nuchal skinfold thickness as a screening tool for Down syndrome: Results of a prospective clinical trial. Obstet. Gynecol. 1991, 77, 533–536. [Google Scholar] [PubMed]
- Nyberg, D.A.; Souter, V.L.; El-Bastawissi, A.; Young, S.; Luthhardt, F.; Luthy, D.A. Isolated sonographic markers for detection of fetal Down syndrome in the second trimester of pregnancy. J Ultrasound Med. 2001, 20, 1053–1063. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mula, R.; Goncé, A.; Bennásar, M.; Arigita, M.; Meler, E.; Nadal, A.; Sánchez, A.; Botet, F.; Borrell, A. Increased nuchal translucency and normal karyotype: Perinatal and pediatric outcomes at 2 years of age. Ultrasound Obstet. Gynecol. 2012, 39, 34–41. [Google Scholar] [CrossRef] [PubMed]
- Smith-Bindman, R.; Hosmer, W.; Feldstein, V.A.; Deeks, J.J.; Goldberg, J.D. Second-trimester ultrasound to detect fetuses with Down syndrome: A meta-analysis. JAMA 2001, 285, 1044–1055. [Google Scholar] [CrossRef] [PubMed]
- Jelliffe-Pawlowski, L.L.; Walton-Haynes, L.; Currier, R.J. Identification of second trimester screen positive pregnancies at increased risk for congenital heart defects. Prenat. Diagn. 2009, 29, 570–577. [Google Scholar] [CrossRef]
- Chitkara, U.; Cogswell, C.; Norton, K.; Wilkins, I.A.; Mehalek, K.; Berkowitz, R.L. Choroid plexus cysts in the fetus: A benign anatomic variant or pathologic entity? Report of 41 cases and review of the literature. Obstet. Gynecol. 1988, 72, 185–189. [Google Scholar]
- Achiron, R.; Barkai, G.; Katznelson, M.B.; Mashiach, S. Fetal lateral ventricle choroid plexus cysts: The dilemma of amniocentesis. Int. J. Gynecol. Obstet. 1991, 38, 343. [Google Scholar] [CrossRef]
- Cho, R.C.; Chu, P.; Smith-Bindman, R. Second trimester prenatal ultrasound for the detection of pregnancies at increased risk of Trisomy 18 based on serum screening. Prenat. Diagn. 2009, 29, 129–139. [Google Scholar] [CrossRef] [PubMed]
- Cheng, P.J.; Shaw, S.W.; Soong, Y.K. Association of Fetal Choroid Plexus Cysts With Trisomy 18 in a Population Previously Screened by Nuchal Translucency Thickness Measurement. J. Soc. Gynecol. Investig. 2006, 13, 280–284. [Google Scholar] [CrossRef] [PubMed]
- Reinsch, R.C. Choroid plexus cysts—Association with trisomy: Prospective review of 16,059 patients. Am. J. Obstet. Gynecol. 1997, 176, 1381–1383. [Google Scholar] [CrossRef]
- DeRoo, T.R.; Harris, R.D.; Sargent, S.K.; Denholm, T.A.; Crow, H.C. Fetal choroid plexus cysts: Prevalence, clinical significance, and sonographic appearance. AJR Am. J. Roentgenol. 1988, 151, 1179–1181. [Google Scholar] [CrossRef] [PubMed]
- Morcos, C.L.; Platt, L.D.; Carlson, D.E.; Gregory, K.D.; Greene, N.H.; Korst, L.M. The isolated choroid plexus cyst. Obstet. Gynecol. 1998, 92, 232–236. [Google Scholar] [CrossRef] [PubMed]
- Walkinshaw, S.; Pilling, D.; Spriggs, A. Isolated choroid plexus cysts—the need for routine offer of karyotyping. Prenat. Diagn. 1994, 14, 663–667. [Google Scholar] [CrossRef] [PubMed]
- Gross, S.J.; Shulman, L.P.; Tolley, E.A.; Emerson, D.S.; Felker, R.E.; Simpson, J.L.; Elias, S. Isolated fetal choroid plexus cysts and trisomy 18: A review and meta-analysis. Am. J. Obstet. Gynecol. 1995, 172, 83–87. [Google Scholar] [CrossRef]
- Ouzounian, J.G.; Ludington, C.; Chan, S. Isolated choroid plexus cyst or echogenic cardiac focus on prenatal ultrasound: Is genetic amniocentesis indicated? Am. J. Obstet. Gynecol. 2007, 196, 595.e1–595.e3. [Google Scholar] [CrossRef] [PubMed]
- Yoder, P.R.; Sabbagha, R.E.; Gross, S.J.; Zelop, C.M. The second-trimester fetus with isolated choroid plexus cysts: A meta-analysis of risk of trisomies 18 and 21. Obstet. Gynecol. 1999, 93, 869–872. [Google Scholar] [CrossRef] [PubMed]
- Goetzinger, K.R.; Stamilio, D.M.; Dicke, J.M.; Macones, G.A.; Odibo, A.O. Evaluating the incidence and likelihood ratios for chromosomal abnormalities in fetuses with common central nervous system malformations. Am. J. Obstet. Gynecol. 2008, 199, 285.e1–285.e6. [Google Scholar] [CrossRef] [PubMed]
- Geary, M.; Patel, S.; Lamont, R. Isolated choroid plexus cysts and association with fetal aneuploidy in an unselected population. Ultrasound Obstet. Gynecol. 1997, 10, 171–173. [Google Scholar] [CrossRef] [PubMed]
- Goetzinger, K.R.; Cahill, A.G.; Macones, G.A.; Odibo, A.O. Echogenic Bowel on Second-Trimester Ultrasonography: Evaluating the risk of adverse pregnancy outcome. Obstet. Gynecol. 2011, 117, 1341–1348. [Google Scholar] [CrossRef] [Green Version]
- Hurt, L.; Wright, M.; Dunstan, F.; Thomas, S.; Brook, F.; Morris, S.; Tucker, D.; Wills, M.A.; Davies, C.; John, G.; et al. Prevalence of defined ultrasound findings of unknown significance at the second trimester fetal anomaly scan and their association with adverse pregnancy outcomes: The Welsh study of mothers and babies population-based cohort. Prenat. Diagn. 2016, 36, 40–48. [Google Scholar] [CrossRef]
- Hurt, L.; Wright, M.; Brook, F.; Thomas, S.; Dunstan, F.; Fone, D.; John, G.; Morris, S.; Tucker, D.; Wills, M.A.; et al. The Welsh study of mothers and babies: Protocol for a population-based cohort study to investigate the clinical significance of defined ultrasound findings of uncertain significance. BMC Pregnancy Childbirth. 2014, 14, 164. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Al-Kouatly, H.B.; Chasen, S.T.; Streltzoff, J.; Chervenak, F.A. The clinical significance of fetal echogenic bowel. Am. J. Obstet. Gynecol. 2001, 185, 1035–1038. [Google Scholar] [CrossRef] [PubMed]
- Nyberg, D.A.; Souter, V.L. Sonographic markers of fetal trisomies: Second trimester. J. Ultrasound Med. 2001, 20, 655–674. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hill, L.M.; Fries, J.; Hecker, J.; Grzybek, P. Second-trimester echogenic small bowel: An increased risk for adverse perinatal outcome. Prenat. Diagn. 1994, 14, 845–850. [Google Scholar] [CrossRef] [PubMed]
- D’Amico, A.; Buca, D.; Rizzo, G.; Khalil, A.; Silvi, C.; Makatsariya, A.; Nappi, L.; Liberati, M.; D’Antonio, F. Outcome of fetal echogenic bowel: A systematic review and meta-analysis. Prenat. Diagn. 2021, 41, 391–399. [Google Scholar] [CrossRef]
- Nguyen, H.T.; Benson, C.B.; Bromley, B.; Campbell, J.B.; Chow, J.; Coleman, B.; Cooper, C.; Crino, J.; Darge, K.; Herndon, C.D.; et al. Multidisciplinary consensus on the classification of prenatal and postnatal urinary tract dilation (UTD classification system). J. Pediatr. Urol. 2014, 10, 982–998. [Google Scholar] [CrossRef] [Green Version]
- Bromley, B.; Lieberman, E.; Shipp, T.D.; Benacerraf, B.R. The genetic sonogram: A method of risk assessment for Down syndrome in the second trimester. J. Ultrasound Med. 2002, 21, 1087–1096. [Google Scholar] [CrossRef] [PubMed]
- Orzechowski, K.M.; Berghella, V. Isolated fetal pyelectasis and the risk of Down syndrome: A meta-analysis. Ultrasound Obstet. Gynecol. 2013, 42, 615–621. [Google Scholar] [CrossRef] [Green Version]
- Al-Hazmi, H.; Dreux, S.; Delezoide, A.L.; Dommergues, M.; Lortat-Jacob, S.; Oury, J.F.; El-Ghoneimi, A.; Muller, F. Outcome of prenatally detected bilateral higher urinary tract obstruction or megacystis: Sex-related study on a series of 709 cases. Prenat. Diagn. 2012, 32, 649–654. [Google Scholar] [CrossRef] [PubMed]
- Weisz, B.; David, A.L.; Chitty, L.; Peebles, D.; Pandya, P.; Patel, P.; Rodeck, C.H. Association of isolated short femur in the mid-trimester fetus with perinatal outcome. Ultrasound Obstet. Gynecol. 2008, 31, 512–516. [Google Scholar] [CrossRef] [PubMed]
- Todros, T.; Massarenti, I.; Gaglioti, P.; Biolcati, M.; Botta, G.; De Felice, C. Fetal short femur length in the second trimester and the outcome of pregnancy. BJOG 2004, 111, 83–85. [Google Scholar] [CrossRef] [PubMed]
- Nyberg, D.A.; Resta, R.G.; Luthy, D.A.; Hickok, D.E.; Williams, M.A. Humerus and femur length shortening in the detection of Down’s syndrome. Am. J. Obstet. Gynecol. 1993, 168, 534–538. [Google Scholar] [CrossRef]
- Benacerraf, B.R.; Neuberg, D.; Frigoletto, F.D., Jr. Humeral Shortening in Second-Trimester Fetuses With Down Syndrome. Obstet. Gynecol. 1991, 77, 223–227. [Google Scholar] [CrossRef] [PubMed]
- Kurtz, A.B.; Needleman, L.; Wapner, R.J.; Hilpert, P.; Kuhlman, K.; Burns, P.N.; Feld, R.I.; Mitchell, D.G.; Segal, S.; Blum, L. Usefulness of a short femur in the in utero detection of skeletal dysplasias. Radiology 1990, 177, 197–200. [Google Scholar] [CrossRef] [PubMed]
- Rodis, J.F.; Vintzileos, A.M.; Fleming, A.D.; Ciarleglio, L.; Nardi, D.A.; Feeney, L.; Scorza, W.E.; Campbell, W.A.; Ingardia, C. Comparison of humerus length with femur length in fetuses with Down syndrome. Am. J. Obstet. Gynecol. 1991, 165, 1051–1056. [Google Scholar] [CrossRef]
- Mathiesen, J.M.; Aksglaede, L.; Skibsted, L.; Petersen, O.B.; Tabor, A. Danish Fetal Medicine Study Group Outcome of fetuses with short femur length detected at second-trimester anomaly scan: A national survey. Ultrasound Obstet. Gynecol. 2014, 44, 160–165. [Google Scholar] [CrossRef] [PubMed]
- Özlü, T.; Ozcan, T. Fetal isolated short femur in the second trimester and adverse pregnancy outcomes. Prenat. Diagn. 2013, 33, 1063–1069. [Google Scholar] [CrossRef]
- Goetzinger, K.R.; Cahill, A.G.; Macones, G.A.; Odibo, A.O. Isolated short femur length on second-trimester sonography: A marker for fetal growth restriction and other adverse perinatal outcomes. J. Ultrasound Med. 2012, 31, 1935–1941. [Google Scholar] [CrossRef] [Green Version]
| Soft Marker | Screening Tests | Society for Maternal-Fetal Medicine (SMFM), 2021 | American College Obstetrics and Gynecology (ACOG), 2020 | Perinatal Services BC, 2020 |
|---|---|---|---|---|
| Absent or hypoplastic nasal bone | cfDNA | If negative: no further testing | If negative: no further testing | Genetic counseling. |
| Serum screen | If negative: no further testing vs noninvasive vs invasive testing for aneuploidy. | If negative: no further testing | Genetic counseling. | |
| No previous screening/other recommendations | Counseling for noninvasive vs invasive testing for aneuploidy | Detailed ultrasound to assess fetal anatomy. Genetic counseling. Offer aneuploidy testing. | Genetic counseling. | |
| Echogenic intracardiac foci | cfDNA | If negative: no further testing | If negative: no further testing | If negative: no further testing |
| Serum screen | If negative: no further testing | If negative: no further testing | If negative ((SIPS/IPS/Quad): no further testing | |
| No previous screening/other recommendations | Counseling for noninvasive tests for aneuploidy | If isolated, aneuploidy tests should be offered. | Offer Quad screening. | |
| Mild to moderate ventriculomegaly | cfDNA | Consider cf-DNA for patients who decline diagnostic testing after counseling about the limitations of this approach. If ventriculomegaly is detected, SMFM recommends that diagnostic testing (amniocentesis) with chromosomal micro-array. | If negative: no further testing | Fetal Diagnosis Service |
| Serum screen | Independently of the result, offer diagnostic testing | If negative: no further testing | Fetal Diagnosis Service | |
| No previous screening/other recommendations | Offer diagnostic test | Detailed anatomic survey. Genetic counseling. Offer diagnostic tests for genetic conditions, CMV, fetal MRI and US in third trimester. | Fetal Diagnosis Service | |
| Thickened nuchal fold | cfDNA | If negative: no further testing | If negative: no further testing | |
| Serum screen | If negative: no further tests vs noninvasive vs invasive tests for aneuploidy | If negative: no further testing | ||
| No previous screening/other recommendations | Counseling for noninvasive vs invasive testing for aneuploidy | Detailed anatomic survey. Genetic counseling. Aneuploidy testing should be offered if not previously performed. | Genetic counseling. | |
| Choroid plexus cyst | cfDNA | If negative: no further testing | If negative: no further testing | If negative: no further testing |
| Serum screen | If negative: no further testing | If negative: no further testing | If negative ((SIPS/IPS/Quad): no further testing | |
| No previous screening/other recommendations | Counseling for noninvasive testing for aneuploidy | Offer aneuploidy testing. | Offer Quad screening. Genetic counseling is recommended only if CPC is seen in combination with other structural abnormalities or FGR. | |
| Echogenic bowel | cfDNA | If negative: no further testing | If negative: no further testing | Genetic counseling. |
| Serum screen | If negative: no further testing | If negative: no further testing | Genetic counseling. | |
| No previous screening/other recommendations | Counselingfor noninvasive testing for aneuploidy. Third trimester scan for evaluation of fetal growth. | Detailed anatomic evaluation. Genetic counseling. Offer CMV, CF, and aneuploidy testing. Consider follow up US for fetal growth because of the association with FGR. | Genetic counseling. | |
| Urinary tract dilation | cfDNA | If negative: no further testing | If negative: no further testing | If negative: no further testing. |
| Serum screen | If negative: no further testing | If negative: no further testing | If negative (SIPS/IPS/Quad or NIPT): no further testing | |
| No previous screening/other recommendations | No previous screening: counseling for noninvasive testing for aneuploidy. Third trimester ultrasound examination to determine if postnatal pediatric nephrology or urology follow-up is needed. | Offer aneuploidy testing. Repeat US in third trimester to assess need for postnatal imaging. | Offer Quad screening and postnatal renal scan between 5 and 30 days of age. | |
| Shortened long bones | cfDNA | If negative: no further testing | If negative: no further testing | If negative: no further testing |
| Serum screen | If negative: no further testing | If negative: no further testing | If negative (SIPS/IPS/Quad or NIPT): no further testing | |
| No previous screening/other recommendations | Counseling for noninvasive testing for aneuploidy. Third trimester ultrasound examination for reassessment and evaluation of growth. | Offer aneuploidy testing. Consider repeat US in third trimester for fetal growth. | Offer Quad screening. |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Taliento, C.; Salmeri, N.; Greco, P.; Morano, D. Role of Sonographic Second Trimester Soft Markers in the Era of Cell-Free DNA Screening Options: A Review. Reprod. Med. 2022, 3, 222-234. https://doi.org/10.3390/reprodmed3030017
Taliento C, Salmeri N, Greco P, Morano D. Role of Sonographic Second Trimester Soft Markers in the Era of Cell-Free DNA Screening Options: A Review. Reproductive Medicine. 2022; 3(3):222-234. https://doi.org/10.3390/reprodmed3030017
Chicago/Turabian StyleTaliento, Cristina, Noemi Salmeri, Pantaleo Greco, and Danila Morano. 2022. "Role of Sonographic Second Trimester Soft Markers in the Era of Cell-Free DNA Screening Options: A Review" Reproductive Medicine 3, no. 3: 222-234. https://doi.org/10.3390/reprodmed3030017
APA StyleTaliento, C., Salmeri, N., Greco, P., & Morano, D. (2022). Role of Sonographic Second Trimester Soft Markers in the Era of Cell-Free DNA Screening Options: A Review. Reproductive Medicine, 3(3), 222-234. https://doi.org/10.3390/reprodmed3030017







