1. Introduction
Trigeminal neuralgia (TN) is a debilitating condition affecting structures innervated by the trigeminal nerve. It is often caused by injury or inflammation of the peripheral trigeminal nerve, and the most common cause is that of vascular compression of the trigeminal nerve at the root entry zone [
1]. There are published cases of TN caused by sinusitis, more specifically fungal sinusitis, although these have been reported mainly in immunocompromised patients [
2]. We present a case of fungal sinusitis masquerading as trigeminal neuralgia in an immunocompetent patient, and discuss the potential implications of these two diseases.
2. Case Report
The patient is a 59-year-old gentleman with a past medical history of hypertension. He was initially seen by a neurologist when he first developed left facial pain four years ago, which only involved the left maxillary nerve (V2) distribution. Evaluation with computed tomography (CT) and magnetic resonance imaging (MRI) scans of the brain did not reveal any neurovascular conflict, space-occupying lesions or sinusitis. At this point, the diagnosis made by the neurologist was idiopathic paroxysmal TN affecting the V2 distribution. He was then treated with carbamazepine 200 mg once daily, which was adequate enough to keep his symptoms at bay for the past few years. However, in the past few months, the patient’s left facial pain suddenly worsened and thus his carbamazepine dose was increased to 400 mg twice daily. The patient was also reviewed by a dentist and received a local anaesthetic injection to the upper left teeth which reduced his pain temporarily, but his symptoms subsequently recurred. The patient was then referred to a pain specialist for further intervention. On review, he reported paroxysmal left electric shock-like facial pain corresponding to the V2 distribution, which recurred in episodes lasting seconds to a few minutes. He also reported symptoms of cough and post-nasal drip, although he was unsure how long these symptoms had been going on for. Examination revealed intact cranial nerves, with left facial hyperalgesia to pressure especially over the left upper lip and nasolabial fold area. There was no cervical lymphadenopathy, while examination of the oral cavity showed intact left upper incisors and canines, absent left upper pre-molars and molars, and healthy gums. The initial impression by the pain specialist was still that of left trigeminal neuralgia, but he decided to perform further investigations as the last scans were done a few years ago. The patient subsequently underwent a MRI of the brain which showed left maxillary sinusitis, while the cisternal portions of the trigeminal nerves and Meckel’s caves were normal. He was given a one-week trial of oral antibiotics with amoxicillin/clavulanic acid and doxycycline, but his symptoms did not improve.
The patient was subsequently referred to ENT for further intervention. Nasoendoscopy showed oedematous left middle meatus with mucopus tracking from the left middle meatus to the post-nasal space. The rest of the upper aerodigestive tract was normal. A CT scan of the paranasal sinuses showed marked mucoperiosteal thickening and complex fluid opacifying the left maxillary sinus, with focal soft tissue/mucosal thickening in the left middle meatus obstructing the infundibular region of the left ostiomeatal complex (
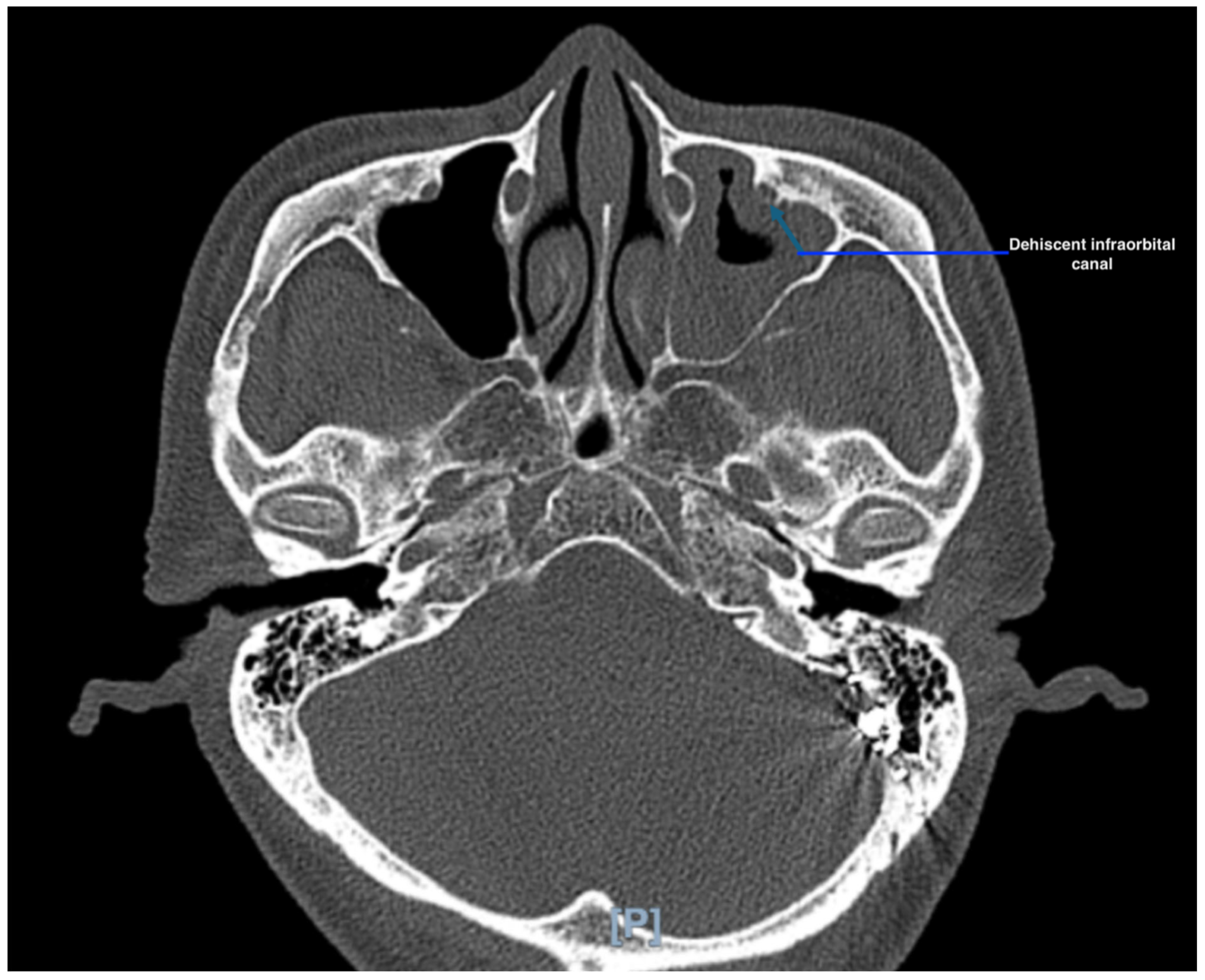
Figure 1). The infraorbital canal adjacent to the mucosal thickening was also noted to be dehiscent (
Figure 2). The patient subsequently underwent left functional endoscopic sinus surgery (FESS) and septoplasty. Intra-operatively, there was a deviated nasal septum to the left with fungal concretions and mucopus in the left maxillary sinus. The left maxillary sinus mucosa was oedematous, and there was left maxillary, anterior ethmoid and frontal sinusitis (
Figure 3). Histology showed fungal hyphae, with acute on chronic sinusitis. The final diagnosis for the patient was that of fungal sinusitis specifically that of the fungal ball (mycetoma) subtype. Post-operatively, the patient was treated with a single course of oral amoxicillin/clavulanic acid as post-operative prophylaxis for secondary bacterial infections and nasal douche. At the last follow-up visit six months after surgery, the patient reported improvement in his left facial pain. Nasoendoscopy showed patent left middle meatal antrostomy with resolution of the oedematous maxillary sinus mucosa.
3. Discussion
Fungal ball sinusitis is a subtype of non-invasive fungal sinusitis, and unlike invasive fungal sinusitis, it has a similar prevalence in immunocompetent and immunocompromised patients [
3]. Patients usually present with symptoms of chronic rhinosinusitis such as facial pain, post-nasal drip and cacosmia, but some may be asymptomatic [
4]. On the other hand, the pain in TN is typically described as a severe paroxysmal electric shock-like pain with short episodes lasting seconds to minutes, although patients with atypical TN (Type 2) may report a more constant pain [
5]. In both conditions, physical examination can be grossly unremarkable, making it difficult to differentiate the two conditions clinically, especially if facial pain is the only presenting symptom. Patients with TN often do not have any neurological deficit in the trigeminal nerve, and therefore physicians may arrive at a diagnosis of TN in these patients with isolated facial pain without pursuing further investigations. Moreover, suspicion of fungal sinusitis may be even lower in an immunocompetent patient as the literature has only described of such cases in immunocompromised patients [
2].
Furthermore, in patients with a dehiscent infraorbital canal, it can predispose the maxillary branch of the trigeminal nerve to neuralgia [
6]. We believe that this patient’s anatomical abnormality could be a contributing factor to his clinical presentation. Fungal ball sinusitis is a type of non-invasive fungal sinusitis, and unlike invasive fungal sinusitis, it usually does not invade into surrounding structures such as nerves, vessels and bone. Therefore, the facial pain in this patient could be due to the infraorbital nerve being more exposed, and thus more susceptible to mucosal inflammation and mechanical irritation from the fungus ball.
In our patient, he was diagnosed with primary TN during his initial presentation four years ago as investigations including CT and MRI scans of his brain did not reveal any underlying pathology. Although his symptoms were still consistent with TN when he subsequently reported sudden worsening of his symptoms in the last few months, the decision was made to perform further imaging to evaluate for other underlying pathologies as the previous investigations were done quite a few years ago. Interestingly, the MRI brain incidentally revealed maxillary sinusitis, and it was thus concluded that the patient likely developed left fungal maxillary sinusitis only in the last few months, which exacerbated his left facial pain due to irritation of the trigeminal nerve by an expanding fungal mycetoma. As a result, his facial pain did not improve despite increasing doses of medications that are normally used to treat TN, but only improved after FESS. Given that the patient’s facial pain did not completely resolve, it supports the conclusion that the facial pain he had at baseline was due to the primary TN, but the sudden worsening of his pain in the past few months was due to a new maxillary fungal sinusitis.
Thus, early identification of fungal sinusitis is critical, as delayed diagnosis can cause morbidity due to intracranial or orbital extension. We believe that in patients with stable and chronic TN with a sudden exacerbation in symptoms, further investigations may be required. Even in an immunocompetent host, a high index of suspicion is required to rule out underlying pathologies such as sinusitis that can cause facial pain.
4. Conclusions
We hereby present a case of fungal sinusitis presenting with facial pain mimicking that of trigeminal neuralgia. Even in immunocompetent patients who present with non-resolving or worsening facial pain resembling the original diagnosis of TN, clinicians should remain vigilant for the possibility of alternative underlying pathologies.
Author Contributions
Conceptualisation, A.C.T. and K.Y.H.; Methodology; O.T.W.H. and A.C.T., K.Y.H.; Resources; A.C.T. and K.Y.H.; Investigation, A.C.T. and K.Y.H.; Data curation, O.T.W.H., A.C.T. and K.Y.H.; Writing—original draft, O.T.W.H.; Writing—review and editing, O.T.W.H., A.C.T. and K.Y.H.; Supervision, A.C.T. and K.Y.H. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
In accordance with institutional policy, formal Institutional Review Board approval was not required as this study describes a single case report. All HIPAA identifiers have been removed to ensure patient anonymity.
Informed Consent Statement
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Data Availability Statement
All relevant clinical data supporting this case report are included within the article. Additional patient information cannot be shared due to privacy and confidentiality restrictions.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Arnold, M. Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd edition. Cephalalgia 2018, 38, 1–211. [Google Scholar] [CrossRef] [PubMed]
- Maschio, M.; Mengarelli, A.; Girmenia, C.; Vidiri, A.; Kayal, R.; Gallo, M.T.; Prignano, G.; Dessanti, M.L.; D’Andrea, M.; Petti, M.C. Trigeminal neuralgia as unusual isolated symptom of fungal paranasal sinusitis in patients with haematological malignancies. Neurol Sci. 2012, 33, 647–652. [Google Scholar] [CrossRef] [PubMed]
- Silveira, M.L.; Anselmo-Lima, W.T.; Faria, F.M.; Queiroz, D.L.; Nogueira, R.L.; Leite, M.G.; Lessa, R.M.; Simões, B.P.; Tamashiro, E.; Valera, F.C. Impact of early detection of acute invasive fungal rhinosinusitis in immunocompromised patients. BMC Infect Dis. 2019, 19, 310. [Google Scholar] [CrossRef] [PubMed]
- Deutsch, P.G.; Whittaker, J.; Prasad, S. Invasive and Non-Invasive Fungal Rhinosinusitis—A Review and Update of the Evidence. Medicina 2019, 55, 319. [Google Scholar] [CrossRef] [PubMed]
- Yadav, Y.R.; Nishtha, Y.; Sonjjay, P.; Vijay, P.; Shailendra, R.; Yatin, K. Trigeminal Neuralgia. Asian J. Neurosurg. 2017, 12, 585–597. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.K.; Yang, S.K.; Shin, D.B.; Nam, J.G. Dehiscence of the infraorbital canal with the maxillary antral empyema: A new cause of facial pain. J. Craniofac. Surg. 2015, 26, e227–e229. [Google Scholar] [CrossRef] [PubMed]
| Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |