Techniques to Assess Long-Term Outcomes after Burn Injuries
Abstract
:1. Introduction
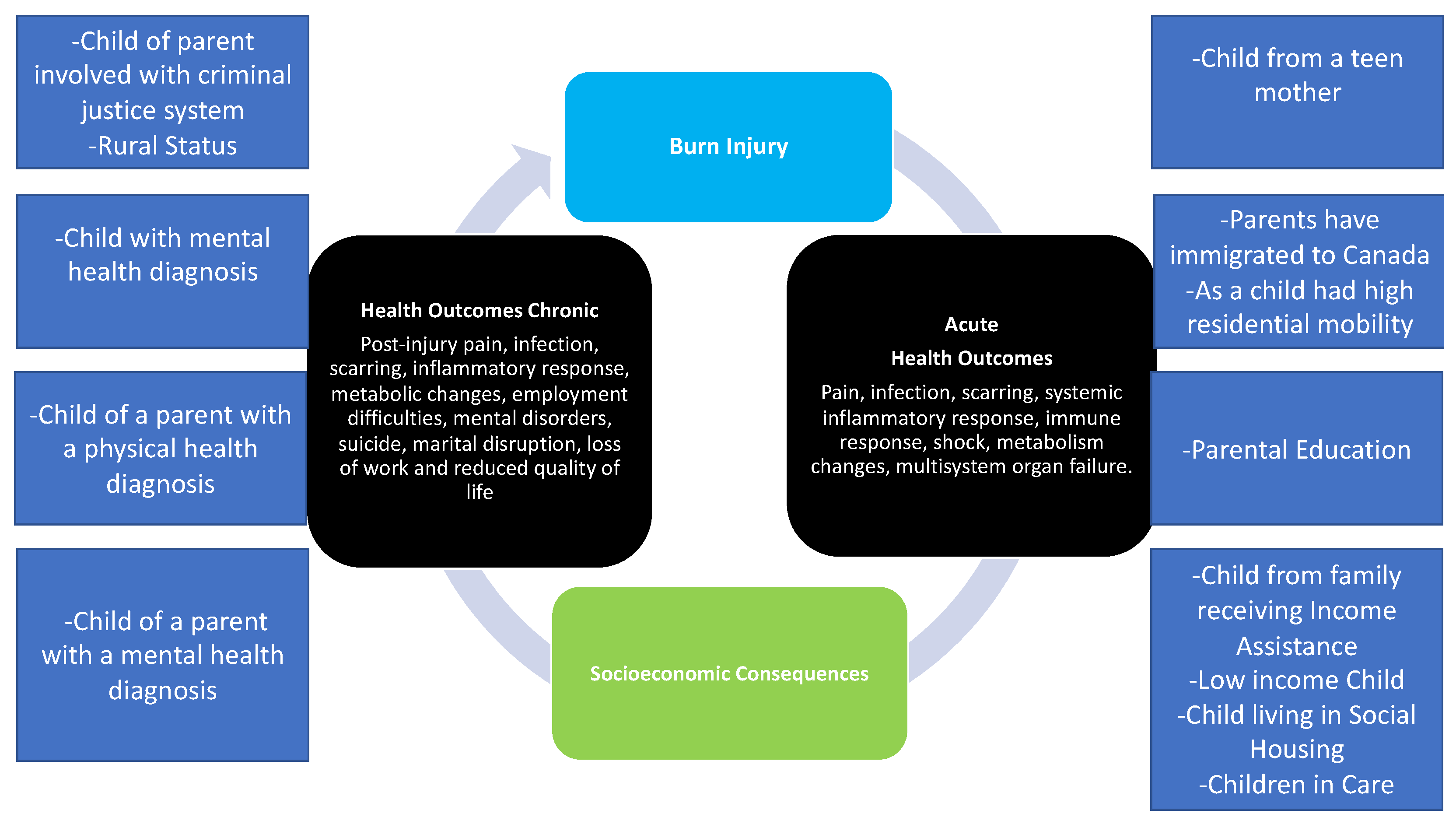
2. Risk Factors for Burn Injury
3. Social Determinants of Health
4. Health Outcomes
4.1. Physical Health Outcomes
4.2. Mental Health Outcomes
4.3. Quality of Life
5. Methods to Examine Long Term Outcomes
5.1. What Are Administrative Data?
5.2. Administrative Data Derived Health Indicators
5.3. How Using Administrative Data Can Advance the Area of Burn Injury
Research
5.4. Combining Data Sources to Study Burn-Related Outcomes
6. Strengths of Using Administrative Data Derived Indicators to Study the Consequences of Burn Injury
6.1. Population-Based Sampling
6.2. Longitudinal Analyses
6.3. Ability to Study Multiple Factors Using Multilevel Statistical Models
6.4. Capture Marginalized Populations
6.5. Ascertainment of Mental and Physical Disorders
7. Social Factors
8. The Importance of Qualitative Research and Mixed Methodology in the Study of Burn Outcomes
9. Conclusions and Future Directions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Burns. 2018. Available online: https://www.who.int/en/news-room/fact-sheets/detail/burns (accessed on 21 October 2021).
- Parachute; Public Health Agency of Canada. Costs by Cause of Injury. 2018. Available online: https://parachute.ca/en/professional-resource/cost-of-injury-in-canada/costs-by-cause-of-injury/ (accessed on 19 January 2022).
- Jeschke, M.G.; van Baar, M.E.; Choudhry, M.A.; Chung, K.K.; Gibran, N.S.; Logsetty, S. Burn injury. Nat. Rev. Dis. Prim. 2020, 6, 11. [Google Scholar] [CrossRef] [PubMed]
- Cleary, M.; Visentin, D.C.; West, S.; Kornhaber, R. The importance of mental health considerations for critical care burns patients. J. Adv. Nurs. 2018, 74, 1233–1235. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Enns, J.; Gawaziuk, J.P.; Khan, S.; Chateau, D.; Bolton, J.M.; Sareen, J.; Stone, J.; Doupe, M.; Logsetty, S. Mental and Physical Health Outcomes in Parents of Children with Burn Injuries as Compared with Matched Controls. J. Burn Care Res. 2016, 37, e18–e26. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- O’Donnell, M.L.; Bryant, R.A.; Creamer, M.; Carty, J. Mental health following traumatic injury: Toward a health system model of early psychological intervention. Clin. Psychol. Rev. 2008, 28, 387–406. [Google Scholar] [CrossRef]
- Logsetty, S.; Shamlou, A.; Gawaziuk, J.P.; March, J.; Doupe, M.; Chateau, D.; Hoppensack, M.; Khan, S.; Medved, M.; Leslie, W.D.; et al. Mental health outcomes of burn: A longitudinal population-based study of adults hospitalized for burns. Burns 2016, 42, 738–744. [Google Scholar] [CrossRef]
- WHO Violence and Injury Prevention Department. Facts about Injuries-Burns. 2016. Available online: https://www.who.int/violence_injury_prevention/media/en/116.pdf (accessed on 21 October 2021).
- Spiwak, R.; Logsetty, S.; Afifi, T.O.; Sareen, J. Severe partner perpetrated burn: Examining a nationally representative sample of women in India. Burns 2015, 41, 1847–1854. [Google Scholar] [CrossRef]
- The World Bank. Population, Female-India. 2020. Available online: https://data.worldbank.org/indicator/SP.POP.TOTL.FE.IN?end=2020&locations=IN&start=2015 (accessed on 28 October 2021).
- Swann, J.A.; Matthews, M.R.; Bay, C.; Foster, K.N. Burn injury outcome differences in Native Americans. Burns 2019, 45, 494–501. [Google Scholar] [CrossRef]
- Padalko, A.; Cristall, N.; Gawaziuk, J.P.; Logsetty, S. Social Complexity and Risk for Pediatric Burn Injury: A Systematic Review. J. Burn Care Res. 2019, 40, 478–498. [Google Scholar] [CrossRef]
- Leslie, W.D.; Metge, C.J.; Azimaee, M.; Lix, L.M.; Finlayson, G.S.; Morin, S.N.; Caetano, P. Direct costs of fractures in Canada and trends 1996–2006: A population-based cost-of-illness analysis. J. Bone Miner. Res. Off. J. Am. Soc. Bone Miner. Res. 2011, 26, 2419–2429. [Google Scholar] [CrossRef]
- Lix, L.; Yogendran, M.M.; Mann, J. Defining and Validating Chronic Diseases: An Administrative Data Approach: An Update with ICD-10-CA; Manitoba Centre For Health Policy: Winnipeg, MB, Canada, 2008. [Google Scholar]
- Fransoo, R.; Martens, P.; The Need to Know Team; Prior, H.; Burchill, C.; Koseva, I.; Bailly, A.; Allegro, E. The 2013 RHA Indicators Atlas; Manitoba Centre for Health Policy: Winnipeg, MB, Canada, 2013. [Google Scholar]
- Padalko, A.A.; Gawaziuk, J.; Logsetty, S.; Chateau, D.; Sareen, J.; Logsetty, S. Social Determinants Associated with Paediatric Burn Injury: A Population Based, Case-Control Study. J. Burn Care Res. 2020, 41, S210–S211. [Google Scholar] [CrossRef]
- Daines, C.L.; Hansen, D.; Novilla, M.L.B.; Crandall, A.A. Effects of positive and negative childhood experiences on adult family health. BMC Pub Health 2021, 21, 651. [Google Scholar] [CrossRef] [PubMed]
- Jeschke, M.G.; Chinkes, D.L.; Finnerty, C.C.; Kulp, G.; Suman, O.E.; Norbury, W.B.; Branski, L.K.; Gauglitz, G.G.; Mlcak, R.P.; Herndon, D.N. Pathophysiologic response to severe burn injury. Ann. Surg. 2008, 248, 387–401. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gauffin, E.; Öster, C.; Gerdin, B.; Ekselius, L. Prevalence and Prediction of Prolonged Pruritus after Severe Burns. J. Burn Care Res. 2015, 36, 405–413. [Google Scholar] [CrossRef] [PubMed]
- Altier, N.; Malenfant, A.; Forget, R.; Choinière, M. Long-term adjustment in burn victims: A matched-control study. Psychol. Med. 2002, 32, 677–685. [Google Scholar] [CrossRef] [PubMed]
- Lee, A.F.; Ryan, C.M.; Schneider, J.C.; Kazis, L.E.; Li, N.C.; Rose, M.; Liang, M.H.; Wang, C.; Palmieri, T.; Meyer, W.J.; et al. Quantifying Risk Factors for Long-Term Sleep Problems After Burn Injury in Young Adults. J. Burn Care Res. 2017, 38, e510–e520. [Google Scholar] [CrossRef]
- Magnusson, S.; Logsetty, S. Burn Care and Treatment; Springer: Cham, Switzerland, 2021; pp. 165–171. [Google Scholar] [CrossRef]
- Van Loey, N.E.; Van Son, M.J. Psychopathology and psychological problems in patients with burn scars: Epidemiology and management. Am. J. Clin. Dermatol. 2003, 4, 245–272. [Google Scholar] [CrossRef]
- Palmu, R.; Suominen, K.; Vuola, J.; Isometsä, E. Mental disorders among acute burn patients. Burns 2010, 36, 1072–1079. [Google Scholar] [CrossRef]
- Wisely, J.A.; Wilson, E.; Duncan, R.T.; Tarrier, N. Pre-existing psychiatric disorders, psychological reactions to stress and the recovery of burn survivors. Burn. J. Int. Soc. Burn Inj. 2010, 36, 183–191. [Google Scholar] [CrossRef] [PubMed]
- Pavan, C.; Grasso, G.; Costantini, M.V.; Pavan, L.; Masier, F.; Azzi, M.F.; Azzena, B.; Marini, M.; Vindigni, V. Accident proneness and impulsiveness in an Italian group of burn patients. Burns 2009, 35, 247–255. [Google Scholar] [CrossRef]
- Schulte, M.T.; Hser, Y.I. Substance Use and Associated Health Conditions throughout the Lifespan. Public Health Rev. 2014, 35, 3. [Google Scholar] [CrossRef] [Green Version]
- Guyatt, G.H.; Jaeschke, R.; Feeny, D.H.; Patrick, D.L. Measurements in Clinical Trials: Choosing the Right Approach. In Quality of Life and Pharmacoeconomics in Clinical Trials, 2nd ed.; Spilker, B., Ed.; Lippincott-Raven: Philadelphia, PA, USA, 1996. [Google Scholar]
- Miller, T.; Bhattacharya, S.; Zamula, W.; Lezotte, D.; Kowalske, K.; Herndon, D.; Fauerbach, J.; Engrav, L. Quality-of-life loss of people admitted to burn centers, United States. Qual. Life Res. 2013, 22, 2293–2305. [Google Scholar] [CrossRef] [PubMed]
- Spronk, I.; Polinder, S.; van Loey, N.E.E.; van der Vlies, C.H.; Pijpe, A.; Haagsma, J.A.; van Baar, M.E. Health related quality of life 5–7 years after minor and severe burn injuries: A multicentre cross-sectional study. Burns 2019, 45, 1291–1299. [Google Scholar] [CrossRef] [PubMed]
- Öster, C.; Willebrand, M.; Ekselius, L. Health-related quality of life 2 years to 7 years after burn injury. J. Trauma-Inj. Infect. Crit. Care 2011, 71, 1435–1441. [Google Scholar] [CrossRef] [PubMed]
- Spronk, I.; Legemate, C.M.; Dokter, J.; van Loey, N.E.E.; van Baar, M.E.; Polinder, S. Predictors of health-related quality of life after burn injuries: A systematic review. Crit. Care 2018, 22, 160. [Google Scholar] [CrossRef] [Green Version]
- Tyack, Z.; Ziviani, J.; Kimble, R.; Plaza, A.; Jones, A.; Cuttle, L.; Simons, M. Measuring the impact of burn scarring on health-related quality of life: Development and preliminary content validation of the Brisbane Burn Scar Impact Profile (BBSIP) for children and adults. Burns 2015, 41, 1405–1419. [Google Scholar] [CrossRef]
- Tyack, Z.; Kimble, R.; McPhail, S.; Plaza, A.; Simons, M. Psychometric properties of the Brisbane burn scar impact profile in adults with burn scars. PLoS ONE 2017, 12, e0184452. [Google Scholar] [CrossRef] [Green Version]
- Griffiths, C.; Guest, E.; Pickles, T.; Hollén, L.; Grzeda, M.; White, P.; Tollow, P.; Harcourt, D. The development and validation of the care burn scale-adult form: A patient-reported outcome measure (PROM) to assess quality of life for adults living with a burn injury. J. Burn Care Res. 2019, 40, 312–326. [Google Scholar] [CrossRef]
- Kazis, L.E.; Marino, M.; Ni, P.; Soley Bori, M.; Amaya, F.; Dore, E.; Ryan, C.M.; Schneider, J.C.; Shie, V.; Acton, A.; et al. Development of the life impact burn recovery evaluation (LIBRE) profile: Assessing burn survivors’ social participation. Qual. Life Res. 2017, 26, 2851–2866. [Google Scholar] [CrossRef]
- Stavrou, D.; Weissman, O.; Tessone, A.; Zilinsky, I.; Holloway, S.; Boyd, J.; Haik, J. Health Related Quality of Life in burn patients—A review of the literature. Burns 2014, 40, 788–796. [Google Scholar] [CrossRef]
- Anzarut, A.; Chen, M.; Shankowsky, H.; Tredget, E.E. Quality-of-life and outcome predictors following massive burn injury. Plast. Reconstr. Surg. 2005, 116, 791–797. [Google Scholar] [CrossRef]
- Gojowy, D.; Kauke, M.; Ohmann, T.; Homann, H.H.; Mannil, L. Early and late-recorded predictors of health-related quality of life of burn patients on long-term follow-up. Burns 2019, 45, 1300–1310. [Google Scholar] [CrossRef] [PubMed]
- Cimino, S.R.; Rios, J.N.; Godleski, M.; Hitzig, S.L. A scoping review on the long-term outcomes in persons with adult-acquired burn injuries. J. Burn Care Res. 2020, 41, 472–502. [Google Scholar] [CrossRef] [PubMed]
- Jutte, D.P.; Roos, L.L.; Brownell, M.D. Administrative record linkage as a tool for public health research. Annu. Rev. Public Health 2011, 32, 91–108. [Google Scholar] [CrossRef]
- Brackstone, G.J. Issues in the use of administrative records for statistical purposes. Surv. Methodol. 1987, 13, 29–43. [Google Scholar]
- Asian Development Bank. Administrative Data Sources for Compiling Millennium Development Goals and Related Indicators: A Reference Handbook for Using Data from Education, Health, and Vital Registration Systems Featuring Practices and Experiences from Selected Countries; Asian Development Bank: Metro Manila, Philippines, 2010. [Google Scholar]
- Canadian Institute of Health Information. CIHI Data Quality Study of the 2009–2010 Discharge Abstract Database; Canadian Institute of Health Information: Ottawa, ON, Canada, 2012. [Google Scholar]
- Statistics Canada. Health Indicators Framework. 2011. Available online: https://www150.statcan.gc.ca/n1/pub/82-221-x/2011002/hifw-eng.htm (accessed on 28 October 2021).
- Lix, L.; Finlayson, G.; Yogendran, M.; Bond, R.; Bodnarchuk, J.; Soodeen, R.-A. Primary Prevention: An Examination of Data Capabilities in Manitoba; Manitoba Centre for Health Policy: Winnipeg, MB, Canada, 2005. [Google Scholar]
- Brownell, M.; Fransoo, R.; Roos, L.; Guèvremont, A.; MacWilliam, L.; Yallop, L.; Levin, B. Is the Class Half Empty? A Population-Based Perspective on Socioeconomic Status and Educational Outcomes. IRPP Choices 2006, 12, 1–30. [Google Scholar]
- Mason, S.; Spiwak, R.; Logsetty, S. Population-Based Research Using Administrative Data to Evaluate Long-Term Outcomes in Burn Injury. In Handbook of Burns; Springer: Cham, Switzerland, 2020; Volume 1, pp. 85–92. [Google Scholar] [CrossRef]
- Martens, P.; Fransoo, R.; McKeen, N.; Burland, E.; Jebamani, L.; Burchill, C.; De Coster, C.; Ekuma, O.; Prior, H.; Chateau, D.; et al. Patterns of Regional Mental Illness Disorder Diagnoses and Service Use in Manitoba: A Population-Based Study; Manitoba Health: Winnipeg, MB, Canada, 2004.
- Tricco, A.C.; Pham, B.; Rawson, N.S.B. Manitoba and Saskatchewan administrative health care utilization databases are used differently to answer epidemiologic research questions. J. Clin. Epidemiol. 2008, 61, 192–197. [Google Scholar] [CrossRef]
- Roos, L.L.; Brownell, M.; Lix, L.; Roos, N.P.; Walld, R.; MacWilliam, L. From health research to social research: Privacy, methods, approaches. Soc. Sci. Med. 2008, 66, 117–129. [Google Scholar] [CrossRef]
- Roos, L.L.; Gupta, S.; Soodeen, R.-A.; Jebamani, L. Data quality in an information-rich environment: Canada as an example. Can. J. Aging 2005, 24 (Suppl. S1), 153–170. [Google Scholar] [CrossRef]
- Roos, L.L.; Mustard, C.A.; Nicol, J.P.; McLerran, D.F.; Malenka, D.J.; Young, T.K.; Cohen, M.M. Registries and administrative data: Organization and accuracy. Med. Care 1993, 31, 201–212. [Google Scholar] [CrossRef]
- Smith, P.M.; Stock, S.R.; McLeod, C.B.; Koehoorn, M.; Marchand, A.; Mustard, C.A. Research opportunities using administrative databases and existing surveys for new knowledge in occupational health and safety in Canada, Quebec, Ontario and British Columbia. Can. J. Public Heal. Rev. Can. Santé Publique 2010, 101, S46–S52. [Google Scholar] [CrossRef]
- De Coster, C.; Quan, H.; Finlayson, A.; Gao, M.; Halfon, P.; Humphries, K.H.; Johansen, H.; Lix, L.M.; Luthi, J.C.; Ma, J.; et al. Identifying priorities in methodological research using ICD-9-CM and ICD-10 administrative data: Report from an international consortium. BMC Health Serv. Res. 2006, 6, 77. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Roos, L.L.; Menec, V.; Currie, R.J. Policy analysis in an information-rich environment. Soc. Sci. Med. 2004, 58, 2231–2241. [Google Scholar] [CrossRef] [PubMed]
- Cvinar, J.G. Do suicide survivors suffer social stigma: A review of the literature. Perspect. Psychiatr. Care 2005, 41, 14–21. [Google Scholar] [CrossRef] [PubMed]
- Stone, J.; Gawaziuk, J.P.; Khan, S.; Chateau, D.; Bolton, J.M.; Sareen, J.; Enns, J.; Doupe, M.; Brownell, M.; Logsetty, S. Outcomes in adult survivors of childhood burn injuries as compared with matched controls. J. Burn Care Res. 2016, 37, e166–e173. [Google Scholar] [CrossRef] [PubMed]
- Lix, L.M.; Yogendran, M.S.; Shaw, S.Y.; Burchill, C.; Metge, C.; Bond, R. Population-based data sources for chronic disease surveillance. Chronic Dis. Can. 2008, 29, 31–38. [Google Scholar] [CrossRef] [PubMed]
- Jutte, D.P.; Brownell, M.; Roos, N.P.; Schippers, C.; Boyce, W.T.; Syme, S.L. Rethinking what is important: Biologic versus social predictors of childhood health and educational outcomes. Epidemiology 2010, 21, 314–323. [Google Scholar] [CrossRef]
- Mojtabai, R.; Olfson, M.; Mechanic, D. Perceived need and help-seeking in adults with mood, anxiety, or substance use disorders. Arch. Gen. Psychiatry 2002, 59, 77–84. [Google Scholar] [CrossRef]
- Wang, P.S.; Angermeyer, M.; Borges, G.; Bruffaerts, R.; Tat Chiu, W.; DE Girolamo, G.; Fayyad, J.; Gureje, O.; Haro, J.M.; Huang, Y.; et al. Delay and failure in treatment seeking after first onset of mental disorders in the World Health Organization’s World Mental Health Survey Initiative. World Psychiatry 2007, 6, 177–185. [Google Scholar]
- Pagura, J.; Fotti, S.; Katz, L.Y.; Sareen, J. Help seeking and perceived need for mental health care among individuals in Canada with suicidal behaviors. Psychiatr. Serv. 2009, 60, 943–949. [Google Scholar] [CrossRef]
- Martens, P.; Fransoo, R.; The Need to Know Team; Burland, E.; Prior, H.; Burchill, C.; Romphf, L.; Chateau, D.; Bailly, A.; Ouelette, C. What Works? A First Look at Evaluating Manitoba’s Regional Health Programs and Policies at the Population Level; Manitoba Centre for Health Policy: Winnipeg, MB, Canada, 2008. [Google Scholar]
- Moi, A.L.; Wentzel-Larsen, T.; Salemark, L.; Hanestad, B.R. Long-term risk factors for impaired burn-specific health and unemployment in patients with thermal injury. Burns 2007, 33, 37–45. [Google Scholar] [CrossRef]
- Cromes, G.F.; Holavanahalli, R.; Kowalske, K.; Helm, P.; Doctor, M.; Lawrence, J.W.; Fauerbach, J.A. Predictors of quality of life as measured by the burn specific health scale in persons with major burn injury. J. Burn Care Rehabil. 2002, 23, 229–234. [Google Scholar] [CrossRef] [PubMed]
- Klinge, K.; Chamberlain, D.J.; Redden, M.; King, L. Psychological adjustments made by postburn injury patients: An integrative literature review. J. Adv. Nurs. 2009, 65, 2274–2292. [Google Scholar] [CrossRef] [PubMed]
- Ajoudani, F.; Jasemi, M.; Lotfi, M. Social participation, social support, and body image in the first year of rehabilitation in burn survivors: A longitudinal, three-wave cross-lagged panel analysis using structural equation modeling. Burns 2018, 44, 1141–1150. [Google Scholar] [CrossRef]
- Ross, E.; Crijns, T.J.; Ring, D.; Coopwood, B. Social factors and injury characteristics associated with the development of perceived injury stigma among burn survivors. Burns 2021, 47, 692–697. [Google Scholar] [CrossRef] [PubMed]
- Kornhaber, R.A.; De Jong, A.E.E.; McLean, L. Rigorous, robust and systematic: Qualitative research and its contribution to burn care. An integrative review. Burns 2015, 41, 1619–1626. [Google Scholar] [CrossRef] [PubMed]
- Rencken, C.A.; Harrison, A.D.; Aluisio, A.R.; Allorto, N. A Qualitative Analysis of Burn Injury Patient and Caregiver Experiences in Kwazulu-Natal, South Africa: Enduring the Transition to a Post-Burn Life. Eur. Burn J. 2021, 2, 75–87. [Google Scholar] [CrossRef]
- Kornhaber, R.; Childs, C.; Cleary, M. Experiences of guilt, shame and blame in those affected by burns: A qualitative systematic review. Burns 2018, 44, 1026–1039. [Google Scholar] [CrossRef] [PubMed]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Spiwak, R.; Sareen, S.; Logsetty, S. Techniques to Assess Long-Term Outcomes after Burn Injuries. Eur. Burn J. 2022, 3, 328-339. https://doi.org/10.3390/ebj3020028
Spiwak R, Sareen S, Logsetty S. Techniques to Assess Long-Term Outcomes after Burn Injuries. European Burn Journal. 2022; 3(2):328-339. https://doi.org/10.3390/ebj3020028
Chicago/Turabian StyleSpiwak, Rae, Shaan Sareen, and Sarvesh Logsetty. 2022. "Techniques to Assess Long-Term Outcomes after Burn Injuries" European Burn Journal 3, no. 2: 328-339. https://doi.org/10.3390/ebj3020028
APA StyleSpiwak, R., Sareen, S., & Logsetty, S. (2022). Techniques to Assess Long-Term Outcomes after Burn Injuries. European Burn Journal, 3(2), 328-339. https://doi.org/10.3390/ebj3020028