Abstract
Pressed lithium disilicate is largely used for veneer manufacturing, but a new block formulation has recently been released on the market. This study evaluated the clinical performance of milled lithium disilicate veneers (LiSi Block, GC Co., Tokyo, Japan) realized with a fully digital or hybrid workflow using modified United States Public Health Service (USPHS) evaluation criteria and survival rates after 24 months of clinical service together with the patient’s satisfaction using the Visual Analog Scale (VAS). A total of 105 veneers on natural anterior teeth were made on twenty-nine patients with LiSi Block (GC, Tokyo, Japan). Patients were randomly divided into three groups: Group 1, 35 veneers realized with a completely digital workflow using Trios 3 (3Shape A/S, Copenhagen, Denmark); Group 2, 35 veneers realized with a completely digital workflow using Experimental IOS (GC, Tokyo, Japan); and Group 3, 35 veneers realized with a hybrid workflow. The restorations were followed up for 24 months, and the modified USPHS evaluation was performed at baseline, 12 months, and 24 months together with periodontal evaluation. Repeated measures two-way ANOVA and the Tukey test were applied to compare the modified USPHS method values (α = 0.05). STATISTICA 10.0 software and SIGMAPLOT 12.0 software were used to perform statistical analysis. There were no statistically significant differences between the three groups and with the interaction of group vs. time periods. The satisfaction scores of 7.35 ± 1.8 and 9.4 ± 0.37 were recorded before and after treatment, respectively. Milled lithium disilicate veneers showed a good clinical outcome after 2 years of clinical service. No difference was found between fully digital or hybrid workflow.
1. Introduction
Ceramic laminate veneers are considered a conservative solution for patients requiring an improvement in the shape, color, or position of their anterior teeth [1,2]. Due to growing patient demand for esthetic restorations, during recent decades, the use of veneers has become a widespread, reliable, and successful technique [3]. Traditionally, ceramic veneers are fabricated using a layering technique that incorporates refractory dies to support condensed layers of ceramic [4]. This technique gives the technician full control over the layers incorporated, resulting in a naturally looking restoration, but the process is technique-sensitive, and manual mixing and layering of the porcelain may result in the incorporation of small voids. In recent years, however, lithium disilicate has become one of the most commonly used ceramics in dentistry [5], and veneers are one of its more interesting applications as it gives clinicians the best compromise in terms of esthetics and strength for all-ceramic monolithic restorations [6]. Lithium disilicate was firstly introduced into the market as a core material in 1998 (Empress 2, Ivoclar Vivadent, Schaan, Lichtenstein) and was then replaced by IPS e.max Press (Ivoclar Vivadent, Schaan, Lichtenstein), which is suitable for monolithic restorations. To accommodate the material to the needs of the CAD/CAM production process, partially precrystallized blocks (IPS e.max CAD, Ivoclar Vivadent, Schaan, Lichtenstein) were introduced and are now largely used. Nowadays, many brands are releasing their block formulation into the market and one of the aims of this study was to test a new one (LiSi Block, GC Co., Tokyo, Japan) for veneers. The two types of lithium disilicate have different formulations and differ in their composition, giving them similar, but not identical, mechanical and optical properties. The main advantage of pressed porcelain is that the resulting veneers have a high level of accuracy as the manufacturing process may assure a better margin, resulting in a more precise adaptation of the veneers on preparations with a smaller gap in the marginal area [7,8]. In fact, the use of press lithium disilicate is already largely documented in literature [9,10,11]. Recently, CAD–CAM veneers from glass–ceramic blocks have become available, and their utilization is on the rise [12]. While such veneers are significantly stronger than feldspathic porcelain ones, the color of the blocks available is of a single shade. However, multi-layer blocks are in an experimental stage and may help to overcome this limitation. A great advantage of block lithium disilicate is that it allows a fully digital workflow. In fact, after veneer preparation, the impression can be performed with an intraoral scanner and sent to the lab. The technician will work directly on the digital model, realizing the digital project of the final restoration that will be directly sent to the milling machine. The lithium disilicate blocks will be directly shaped by a 5-axis milling machine into the final shape of the veneers based on the digital project and after being stained and polished will be ready for cementation. In recent studies, milled laminate veneers have shown a lower-quality marginal seal and adaptation and thicker cement layers than pressed veneers [13,14,15,16], but this could also be due to the quality and update of the intraoral scanner, CAD software (DentalCAD version 2.2, exocad GmbH), and the milling machine used in the process. However, the marginal gap that has been recorded when lithium disilicate partial crowns were made through the CAD–CAM process was within clinical acceptability [17]. Survival rates of 94% (95% CI: 87–100%) for glass–ceramic and 87% (95% CI: 82–93%) for feldspathic porcelain veneers were estimated by Morimoto et al. [18] in a systematic review on the clinical outcome of veneers made by different types of ceramic. Their study also found that major complications of veneers include debonding (2%), fracture (4%), secondary caries (1%), marginal discoloration (2%), and endodontic problems (2%). It should be taken into consideration that materials play an important role in the long-lasting results of a restoration but also other factors have to be considered such as: preparation technique [19], thickness of the restoration [20], quantity of residual enamel, and cementation technique [21].
A factor playing a fundamental role in the realization of well-fitted, long-lasting veneers together with the accuracy of the laboratory phases is the quality of the final impression sent to the lab technician, whether traditional or digital. The accuracy of an intraoral impression depends on many factors, mainly related to the operator [22], the patient [23], and the quality of the intraoral scanners in terms of version and software update [24,25].
Technologies are developing fast, and new intraoral scanners (IOSs) are being introduced on the market and their software is updated periodically. In this study, two IOSs were compared, one well known (Trios 3, 3 Shape, A/S, Copenhagen, Denmark) and the other an experimental system (Aadva 200, GC, Tokyo, Japan), versus a hybrid workflow: analogic impression, gypsum model, and then scanned with a laboratory scanner (Aadva Lab Scanner, GC, Tokyo, Japan).
Randomized clinical trials on CAD/CAM veneers are scarce, as are reports about restorations made by early generations of chair-side CAD/CAM systems [26]. A 96.9% survival rate at 5-years follow-up of CAD/CAM veneers was reported by Wiedhahn et al. [26]. In a more recent study by Nejatidanesh et al. [27], the chair-side CEREC AC veneer survival rate was 99.0% after 5 years. In another study, milled and pressed lithium disilicate veneers had a similar clinical performance after the 1-year follow-up and both showed a great level of esthetic patient satisfaction [7]. However, only a few articles have evaluated the clinical performance of the block formulation of lithium disilicate [7,27]. The aim of this clinical trial was to assess the clinical performance of block lithium disilicate veneers obtained with a fully digital workflow with two different intraoral scanners in terms of modified United States Public Health Service (USPHS) method [28] periodontal values and patient satisfaction [15] versus a hybrid workflow. The null hypotheses were: (1) the CAD/CAM ceramic veneers made using two different IOSs do not have statistically significant differences in clinical performance compared to those obtained with an analogic workflow, and (2) the laminates made digitally did not show a better and statistically significant degree of patient satisfaction before and after treatment than those analogically made.
2. Materials and Methods
Laminate veneers were realized on 29 patients for a total of 105 restorations equally distributed in the three groups between September 2021 and December 2021 and included in the present study. All patients were informed about the scope of the trial and provided their written consent. The study protocol was approved by the Ethical Committee of University of Siena (clinicaltrial.gov #CT01932049). Also, the clinical treatment was performed in accordance with the ethical standards of the Institutional and National Research Committee and with the Declaration of Helsinki of 1964 and its later amendments or comparable ethical standards. This study adhered to the CONSORT guidelines (as reported in Table S1). Patients enrolled in the present clinical trial were referred to the Prosthodontic Department of the University of Siena asking for the esthetic and functional rehabilitation of teeth in the esthetic area. Patients were recruited according to the following inclusion and exclusion criteria:
Inclusion criteria: Periodontally healthy, and without sign of parafunctions, adults (18+ years), requiring between one to six laminate veneers for the esthetic and functional rehabilitation of anterior teeth.
Exclusion criteria: Not adult age (<18 years), pregnancy, disabilities, previous prosthodontic restorations of abutment teeth, endodontic-treated teeth, severe and/or chronic periodontitis (plaque index higher than 20 or bleeding on probing higher than 10), parafunctions or bruxism, systemic disease, allergic history concerning methacrylates, rampant caries, xerostomia, lack of compliance, language barriers.
CONSORT 2010 Flow Diagram (Figure 1) shows how the participants were selected.
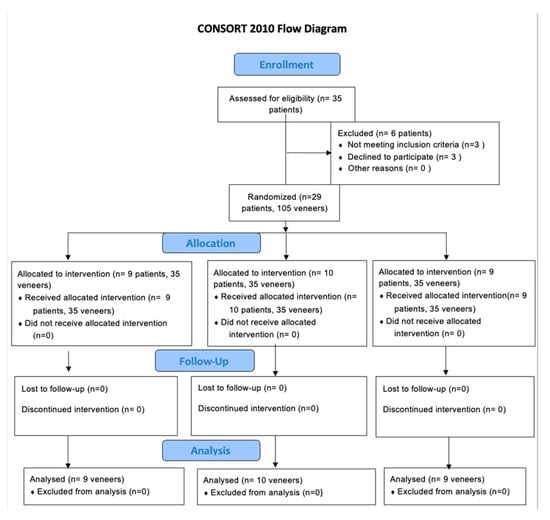
Figure 1.
CONSORT 2010 flow diagram.
The mean age was 44 years (range 18 to 65). There were 16 females and 13 males.
After being recruited, all patients underwent professional oral hygiene instruction and prophylaxis to achieve optimal plaque control and gingival health. Periodontal probing depth (PPD), bleeding on probing (BoP) [29], and full-mouth plaque index (PI) were recorded on each patient. Intraoral radiographs were taken, by customized radiographic trays made for each patient, to ensure that the teeth were vital and in endodontic health. No patients reported any sign of parafunctions or bruxism.
Before starting the clinical procedures, the patients were randomly divided into 3 groups by a file generated by software so that the 105 future restorations were realized by fully digital or hybrid workflow:
- Group 1: 35 restorations scanned with Trios 3 (3Shape A/S, Copenhagen, Denmark);
- Group 2: 35 restorations scanned with Experimental Aadva (GC, Tokyo, Japan);
- Group 3: 35 restorations made by a hybrid workflow.
The mechanism used to implement the random allocation sequence (such as sequentially numbered containers) was electronically generated.
Group 1: 4 patients received 6 laminate veneers, 2 patients 2 laminate veneers, 2 other patients 3 laminate veneers, and 1 patient only 1 laminate veneer.
Group 2: 4 patients received 6 laminate veneers, 2 patients 2 laminate veneers, 3 other patients 1 laminate veneer, and 1 patient 4 laminate veneers.
Group 3: 4 patients received 6 laminate veneers, 4 patients 2 laminate veneers, and 3 patients 1 laminate veneer.
Groups 1 and 2: The initial situation of the patient was acquired using the selected IOS to realize an .stl file of the initial situation that was sent to the same laboratory.
The files were imported to Exocad software (DentalCAD version 2.2, exocad GmbH) and for each patient a digital wax up was realized by the same technician to obtain a simulation of the future restoration. All the restorations were designed in centric occlusion of the patient without any change in vertical dimension. The final model was then printed with an Asiga 3D printer (Asiga, NSW, Sydney, Australia) and then a silicon guide was realized to make the mock-up in the patient’s mouth.
Group 3: The initial situation of each patient was acquired by alginate impressions. Then, in the lab, a wax up was realized on the stone casts and a silicon guide was made to realize the mock-up in the mouth of the patient.
At the second appointment, the same prosthodontist (M.F.) realized the mock-up in each patient’s mouth with self-curing resin (Temp Print, GC, Tokyo, Japan) to obtain an esthetic simulation of the final rehabilitation. After the patient accepted the mock-up, the teeth were prepared. The preparation was guided by the mock-up [19] in order to minimize the tooth preparation and remain in the enamel as much as possible. The teeth reductions were checked with the silicone guide index. Laminate veneers were prepared with a buccal thickness ranging between 0.5 and 1.0 mm and a 1.0 mm incisal thickness [30].
In order to standardize the clinical procedures, the same trained prosthodontist (M.F.) performed the clinical treatments, using a depth cutter bur (0.4 mm in thickness), and a round-end taper bur mounted on a handpiece and under irrigation with water spray. The first bur made parallel horizontal grooves that were marked with a pencil and then connected using the second bur. A thin 3.0 cord was gently placed as a retraction cord into the sulcus and the specimens were prepared with a mini-chamfer cervical finish line of 0.3 mm and buccal depth of 0.6 mm. The incisal margin was removed to a length of 2mm, and a thin palatal chamfer preparation was placed as a stop.
Then, the prepared surfaces were gently polished with rubber points. The quantity of exposed enamel was visually evaluated with 3.5X magnification loops by a trained prosthodontist (M.F.) for each group: 10% for Group 1, 7–8% for Group 2, and 9% for Group 3 [31]. Then, the prepared teeth received an impression: Groups 1 (Trios 3, 3 Shape Co., Copenhagen, Denmark ) and 2 (Experimental Aadva, GC Co., Tokyo, Japan) were scanned with the selected IOS, and in Group 3 an analogic impression was taken using Exa’lance (GC, Tokyo, Japan). The digital and analogic impressions of each patient were made strictly following the manufacturers’ instructions. After the impression was made, temporary restorations were made directly at the chair, using the same silicon guide and the same bis-acrylic resin used for the mock-up.
The .stl files generated by the intraoral scanners used in Groups 1 and 2 were delivered to the lab to be processed. Also, in the lab, the traditional impressions of Group 3 patients were poured using type 4 stone (FujiRock, GC Co., Tokyo, Japan) to realize a master model that was digitalized using an Aadva Lab Scanner (GC, Tokyo, Japan) to obtain .stl files as a reference.
All .stl files were elaborated by Exocad software (DentalCAD version 2.2, exocad GmbH)and the final project of the restorations was realized using the initial one approved by the patients as a reference. When the final projects of the veneers were ready, the generated .stl files were exported to the milling machine (n4 Plus, Vhf AG, Ammerbuch, Germany).
All the veneers were realized using Initial LiSi Block (GC, Tokyo, Japan).
Laminate veneers were delivered to the patient approximately after one week and then luted following the manufacturers’ instructions. The intaglio surface of each restoration was etched with 5% hydrofluoric acid (IPS Ceramic, Ivoclar, Vivadent, Schaan, Lichtenstein) for 20 s, silanized with G-Multi Primer (GC, Tokyo, Japan) and then luted using G-Cem One (GC, Tokyo, Japan) in both groups. A rubber dam was placed in all cases to perform luting steps.
Finally, all patients were enrolled in an oral hygiene program in which recalls were planned every 6 months for professional cleaning and patients’ motivation. Full periodontal charting was performed at baseline and 1- and 2-years recall. Modified USPHS scores [28] were used to score the clinical outcomes of this study, as reported in Table 1.

Table 1.
Criteria of the modified United States Public Health Service method.
The criteria were evaluated clinically using a mirror and an explorer with a sharp tip was used to evaluate the marginal integrity, adaptation, and discrepancies of the veneers. Two blinded and calibrated clinicians (G.V., E.F.C.) evaluated the outcomes at baseline, 12 months, and 24 months.
Regarding periodontal parameters, periodontal probing depth (PPD), bleeding on probing (BoP) and full-mouth plaque index (PI) were recorded [29].
All the patients agreed to answer a questionnaire and grade their satisfaction using a VAS before and after treatment [7]. The patients had to answer 10 questions, scoring from 0 (very unsatisfied) to 10 (very satisfied). The questions were:
1. Are you happy with the appearance of your smile? 2. Are you happy of the color of your teeth? 3. Are you happy with the shape of your teeth? 4. Are you happy with the size of your teeth? 5. How are you feeling when chewing? 6. Regarding comfort, how are you feeling? 7. How are you feeling when speaking? 8. How are you feeling about your gums? 9. Are you satisfied with the shape of your lips? 10. What do you think about the alignment of your teeth?
Values were assigned to each clinical score as follows: Alpha = 1, Bravo = 2, Charlie = 3, accordingly with modified USPHS scores. The Tukey test and repeated measures two-way ANOVA were used to compare the modified USPHS method values (α = 0.05). STATISTICA 10.0 software and SIGMAPLOT 12.0 software were used to perform statistical analysis.
3. Results
3.1. Clinical Assessment
At the 2-year recall, all patients came back and answered the ‘patient’s satisfaction questionnaire’; therefore, 100% of the sample teeth were evaluated.
All the scores of the clinical outcomes are reported in Table 2a–e.

Table 2.
Scores of clinical outcomes: (a). Group 1. Longitudinal findings for the different study parameters and significance of changes over time (non-parametric linear-by-linear test); (b). Group 2. Longitudinal findings for the different study parameters and significance of changes over time (non-parametric linear-by-linear test); (c). Group 3. Longitudinal findings for the different study parameters and significance of changes over time (non-parametric linear-by-linear test); (d). Comparison of findings at one-year recall for the parameters in which changes were observed and between-group significance of changes (time dependent Cox regression analysis); (e). Comparison of findings at two-year recall for the parameters in which changes were observed and between-group significance of changes (time dependent Cox regression analysis).
At the baseline, an Alpha score was recorded for all laminate veneers for COA, RESF, TFRA, RESW, ANTW, CARP, and POSTS.
At the 1-year recall, only two restorations of all groups scored Bravo for MARA and MARD.
At the 2-year recall, there was an increase in Bravo scores in Groups 1 and 2 and 3, and 1 Charlie score for RESF in Group 3 (Table 2c). In this last case, a delamination of the veneer was recorded, and the restoration was replaced.
There were no statistically significant differences between the three groups and with interaction of group vs. time periods.
Regardless of color alteration, marginal discoloration, tooth fracture, restoration wear, tooth antagonist wear, and caries presence, all restorations of all groups always scored Alpha.
3.2. Assessment of the Patient’s Level of Satisfaction
All patients answered the questionnaire before and after treatment. Patients gave a score of 7.35 ± 1.8 and 9.4 ± 0.37 before and after treatment, respectively, as reported in Table 3a,b.

Table 3.
(a). Mean and standard deviation of the patient’s level of satisfaction for each group; (b). Overall, the VAS of patients’ satisfaction of the three groups at the 2-year recall.
3.3. Assessment of Periodontal Parameters
All patients showed no periodontal probing depth (PPD) around the laminate veneers, no bleeding on probing (BoP), and a full-mouth plaque index (PI) lower than 20%, as reported in Table 4a–c. No statistically significant differences were found at the baseline, 1- and 2-year recall between the two groups.

Table 4.
Periodontal parameters. (a) Baseline; (b) 1-Year Recall; (c) 2-Year Recall.
4. Discussion
The outcomes of the laminate veneers recorded in the three groups were shown to be equivalent. Also, the clinical outcomes recorded when the two intraoral scanners (Groups 1 and 2) were used showed no differences. The intraoral scanner used in Group 1 is already well known and is considered as the gold standard. The experimental IOS that was used in Group 2 is a new device with new software and was shown to be very promising. The hybrid procedure followed in Group 3 is a standard clinical procedure very commonly used by practitioners.
The second null hypothesis was also accepted. In fact, no statistically significant differences in patients’ satisfaction were recorded among the three groups. The patients’ satisfaction increased significantly from baseline to last recall.
All the periodontal values showed very positive outcomes. It must be noted that, after being recruited, all patients underwent professional oral hygiene instruction and prophylaxis to achieve optimal plaque control and gingival health and then they were inserted in a maintenance program with professional oral hygiene sessions every 6 months. Periodontal probing depth (PPD), bleeding on probing (BoP), and full-mouth plaque index (PI) were recorded for each patient before treatment, at baseline, and every 12 months, so it is probable that patient collaboration and the easy position to be reached with the toothbrush and floss played a fundamental role in maintaining good periodontal parameters.
Another factor that played an important role in the maintenance of the periodontal parameters was probably the chamfer finish line placed juxta-gingivally that easily allowed the margin to be kept clean. The use of a knife-edge finishing line was avoided because more often this can cause a marginal fracture and discoloration. The limited infiltration at the margin can be due to the precision of the restoration on the chamfer finish line that was acquired using an intraoral scanner. In fact, it is largely documented in literature that intraoral scanners report good results in accuracy when used to scan supra- or juxta-gingival preparations [24,25].
Another important factor that guaranteed the absence of infiltration was probably that the preparation design was maintained as much as possible into the enamel.
In fact, the bond between the tooth substrate, adhesive cement, and the restoration is fundamental for the success of veneers. Marginal gaps and subsequent staining of the interface between the tooth and the restoration can be due to bond failures.
Despite the advances in dentin bonding agents, bonding to enamel is more stable than dentin [32,33]. Adhesion to enamel consists of mechanical interlocking, while dentin is non-homogenous, has moisture, and may have sclerotic areas [32,33]. Additionally, porcelain has a much higher modulus of elasticity than dentin, more comparable to that of enamel. Higher debonding and fractures of ceramic laminate veneers are reported when the restoration is bonded to dentin instead of enamel due to a difference in the flexibility of the two substrates [31]. Preparations confined to enamel should be preferred, when possible, to guarantee greater strength of the tooth and a high bond strength. Also, the absence of postoperative sensitivity is probably due to the preparation design that was maintained as much as possible into the enamel [34].
Digital devices can be used in a complete digital workflow or in a hybrid workflow, where a traditional impression is firstly poured and then the stone model is scanned with a laboratory scanner. In this clinical study, Groups 1 and 2 laminate veneers were fabricated by a complete digital workflow, while those of Group 3 were fabricated with a hybrid workflow (analogic clinically and digital in the lab). Many studies have reported on the digital versus hybrid workflow [35,36]. The most recent studies have shown that the digital workflow can achieve positive outcomes similar to those obtained with traditional and hybrid workflows [37,38]. This clinical trial confirms these findings. Additionally, the IOSs demonstrated higher time efficiency, faster communication with the technician and the patients, and better patient acceptance compared with those of conventional impression methods [35,36,37,38]. The high level of patients’ satisfaction may be due to the previsualization of the final work through the intraoral mock-up and its exact reproduction in the final restoration thanks to digital technologies.
The juxta-gingival location of the margin, easier to be scanned, and the good health of the periodontal tissues might played a fundamental role for the outcomes of this study.
A limitation of the study is that the study protocol was performed to standardize the clinical procedures. All the restorations were realized from the same type of material (Initial LiSi Block, GC, Tokyo, Japan), using a standardized procedure for preparation and cementation. Recent studies have highlighted the differences of fracture resistance of CAD–CAM lithium disilicate crowns and found statistically significant differences depending on the type of lithium disilicate ceramic material used [39] and the adhesive luting cement used [40].
Also, other limitations of this study are the limited number of patients and of the restorations that were tested, and the limited time of clinical service. Longer clinical trials of a wider number of patients and restorations, and with a multicenter design, are desirable to confirm the outcomes of this study.
5. Conclusions
From the outcomes of this study the following conclusions can be drawn:
The two intraoral scanners used in this study are reliable and equivalent to the hybrid workflow for the realization of milled lithium disilicate veneers.
The satisfaction of the patients of all three groups at the 2-year recall (9.4 ± 0.37) is superior to the one recorded at the baseline (7.35 ± 1.8).
Supplementary Materials
The following supporting information can be downloaded at: https://www.mdpi.com/article/10.3390/prosthesis6020025/s1, Table S1: CONSORT 2010 checklist of information to include when reporting a randomised trial.
Author Contributions
Conceptualization, M.F. and E.F.C.; methodology, G.V. and M.F.; software, D.M.; validation, M.F., G.V. and E.F.C.; investigation, M.F. and E.F.C.; resources, M.F.; data curation, E.F.C. and D.M.; writing—original draft preparation, G.V.; writing—review and editing, E.F.C.; visualization, M.F. and D.M.; supervision, M.F.; project administration, E.F.C.; funding acquisition, M.F. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
The study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board (or Ethics Committee) of the University of Siena (protocol code PR001; date of approval 6 May 2021).
Informed Consent Statement
Informed consent was obtained from all subjects involved in the study.
Data Availability Statement
The data presented in this study are available on request from the corresponding author. The data are not publicly available due to University of Siena policy.
Conflicts of Interest
The authors declare no conflicts of interest.
References
- Calamia, J.R.; Calamia, C.H.S. Ceramic laminate veneers: Reasons for 25 years of success. Dent. Clin. N. Am. 2007, 51, 399–417. [Google Scholar] [CrossRef] [PubMed]
- Chen, J.H.; Shi, C.X.; Wang, M.; Zhao, S.J.; Wang, H. Clinical evaluation of 546 tetracycline-stained teeth treated with porcelain laminate veneers. J. Dent. 2005, 33, 3–8. [Google Scholar] [CrossRef] [PubMed]
- Peumans, M.; Van Meerbeek, B.; Lambrechts, P.; Vanherle, G. Porcelain veneers: A review of the literature. J. Dent. 2000, 28, 163–177. [Google Scholar] [CrossRef] [PubMed]
- Horn, H.R. Porcelain laminate veneers bonded to etched enamel. Dent. Clin. N. Am. 1983, 27, 671–684. [Google Scholar] [CrossRef] [PubMed]
- Martins, F.V.; Vasques, W.F.; Fonseca, E.M. How the Variations of the Thickness in Ceramic Restorations of Lithium Disilicate and the Use of Different Photopolymerizers Influence the Degree of Conversion of the Resin Cements: A Systematic Review and Meta-Analysis. J. Prosthodont. 2019, 28, e395–e403. [Google Scholar] [CrossRef] [PubMed]
- Nawafleh, N.; Hatamleh, M.; Elshiyab, S.; Mack, F. Lithium Disilicate Restorations Fatigue Testing Parameters: A Systematic Review. J. Prosthodont. 2016, 25, 116–126. [Google Scholar] [CrossRef] [PubMed]
- Soares-Rusu, I.; Villavicencio-Espinoza, C.A.; de Oliveira, N.A.; Wang, L.; Honório, H.M.; Rubo, J.H.; Francisconi, P.; Borges, A. Clinical Evaluation of Lithium Disilicate Veneers Manufactured by CAD/CAM Compared with Heat-pressed Methods: Randomized Controlled Clinical Trial. Oper. Dent. 2021, 46, 4–14. [Google Scholar] [CrossRef] [PubMed]
- Mörmann, W.H. The evolution of the CEREC system. J. Am. Dent. Assoc. 2006, 137 (Suppl. S1), 7S–13S. [Google Scholar] [CrossRef] [PubMed]
- Gehrt, M.; Wolfart, S.; Rafai, N.; Reich, S.; Edelhoff, D. Clinical results of lithium-disilicate crowns after up to 9 years of service. Clin. Oral. Investig. 2013, 17, 275–284. [Google Scholar] [CrossRef]
- Phark, J.H.; Duarte, S., Jr. Microstructural considerations for novel lithium disilicate glass ceramics: A review. J. Esthet. Restor. Dent. 2022, 34, 92–103. [Google Scholar] [CrossRef]
- Ferrari, M.; Cagidiaco, E.F.; Goracci, C.; Sorrentino, R.; Zarone, F.; Grandini, S.; Joda, T. Posterior partial crowns out of lithium disilicate (LS2) with or without posts: A randomized controlled prospective clinical trial with a 3-year follow up. J. Dent. 2019, 83, 12–17. [Google Scholar] [CrossRef] [PubMed]
- Ferrari Cagidiaco, E.; Sorrentino, R.; Pontoriero, D.I.; Ferrari, M. A randomized controlled clinical trial of two types of lithium disilicate partial crowns. Am. J. Dent. 2020, 33, 291–295. [Google Scholar] [PubMed]
- Aboushelib, M.N.; Elmahy, W.A.; Ghazy, M.H. Internal adaptation, marginal accuracy and microleakage of a pressable versus a machinable ceramic laminate veneers. J. Dent. 2012, 40, 670–677. [Google Scholar] [CrossRef] [PubMed]
- Azar, B.; Eckert, S.; Kunkela, J.; Ingr, T.; Mounajjed, R. The marginal fit of lithium disilicate crowns: Press vs. CAD/CAM. Braz. Oral. Res. 2018, 32, e001. [Google Scholar] [CrossRef]
- Carlile, R.S.; Owens, W.H.; Greenwood, W.J.; Guevara, P.H. A comparison of marginal fit between press-fabricated and CAD/ CAM lithium disilicate crowns. Gen. Dent. 2018, 66, 45–48. [Google Scholar] [PubMed]
- Mounajjed, R.M.; Layton, D.; Azar, B. The marginal fit of E.max Press and E.max CAD lithium disilicate restorations: A critical review. Dent. Mater. J. 2016, 35, 835–844. [Google Scholar] [CrossRef] [PubMed]
- McLean, J.W.; von Fraunhofer, J.A. The estimation of cement film thickness by an in vivo technique. Br. Dent. J. 1971, 131, 107–111. [Google Scholar] [CrossRef] [PubMed]
- Morimoto, S.; Albanesi, R.B.; Sesma, N.; Agra, C.M.; Braga, M.M. Main clinical outcomes of feldspathic porcelain and glass-ceramic laminate veneers: A systematic review and meta-analysis of survival and complication rates. Int. J. Prosthodont. 2016, 29, 38–49. [Google Scholar] [CrossRef] [PubMed]
- Gurel, G.; Morimoto, S.; Calamita, M.A.; Coachman, C.; Sesma, N. Clinical performance of porcelain laminate veneers: Outcomes of the aesthetic pre-evaluative temporary (APT) technique. Int. J. Periodontics Restor. Dent. 2012, 32, 625–635. [Google Scholar]
- Blunck, U.; Fischer, S.; Hajtó, J.; Frei, S.; Frankenberger, R. Ceramic laminate veneers: Effect of preparation design and ceramic thickness on fracture resistance and marginal quality in vitro. Clin. Oral. Investig. 2020, 24, 2745–2754. [Google Scholar] [CrossRef]
- Blatz, M.B.; Vonderheide, M.; Conejo, J. The Effect of Resin Bonding on Long-Term Success of High-Strength Ceramics. J. Dent. Res. 2018, 97, 132–139. [Google Scholar] [CrossRef] [PubMed]
- Revilla-Leon, M.; Kois, D.E.; Kois, J.C. A guide for maximizing the accuracy of intraoral digital scans. Part 1: Operator factors. J. Esthet. Restor. Dent. 2022, 1, 11. [Google Scholar]
- Revilla-Leon, M.; Kois, D.E.; Kois, J.C. A guide for maximizing the accuracy of intraoral digital scans. Part 2: Patient factors. J. Esthet. Restor. Dent. 2023, 1, 9. [Google Scholar] [CrossRef] [PubMed]
- Casucci, A.; Verniani, G.; Habib, R.; Ricci, N.M.; Carboncini, C.; Ferrari, M. Accuracy of Four Intra-Oral Scanners in Subgingival Vertical Preparation: An In Vitro 3-Dimensional Comparative Analysis. Materials 2023, 16, 6553. [Google Scholar] [CrossRef] [PubMed]
- Verniani, G.; Casucci, A.; Ferrero, E.; Gaeta, C.; Ferrari Cagidiaco, E. Accuracy evaluation of digital impressions on horizontal finish line designs. J. Osseointegration 2023, 15, 276–283. [Google Scholar]
- Wiedhahn, K.; Kerschbaum, T.; Fasbinder, D.F. Clinical long-term results with 617 Cerec veneers: A nine-year report. Int. J. Comput. Dent. 2005, 8, 233–246. [Google Scholar] [PubMed]
- Nejatidanesh, F.; Savabi, G.; Amjadi, M.; Abbasi, M.; Savabi, O. Five year clinical outcomes and survival of chairside CAD/CAM ceramic laminate veneers—A retrospective study. J. Prosthodont. Res. 2018, 62, 462–467. [Google Scholar] [CrossRef] [PubMed]
- Ryge, G.; Jendresen, M.D.; Glantz, P.O.; Mjör, I. Standardization of clinical investigators for studies of restorative materials. Swed. Dent. J. 1981, 5, 235–239. [Google Scholar] [PubMed]
- Caton, J.G.; Armitage, G.; Berglundh, T.; Chapple, I.L.; Jepsen, S.; Kornman, K.S.; Mealey, B.L.; Papapanou, P.N.; Sanz, M.; Tonetti, M.S. A new classification scheme for periodontal and peri-implant diseases and conditions—Introduction and key changes from the 1999 classification. J. Clin. Periodontol. 2018, 89, S1–S8. [Google Scholar]
- Da Costa, D.C.; Coutinho, M.; de Sousa, A.S.; Ennes, J.P. A meta-analysis of the most indicated preparation design for porcelain laminate veneers. J. Adhes. Dent. 2013, 15, 215–220. [Google Scholar]
- Sorrentino, R.; Ruggiero, G.; Borelli, B.; Barlattani, A.; Zarone, F. Dentin Exposure after Tooth Preparation for Laminate Veneers: A Microscopical Analysis to Evaluate the Influence of Operators’ Expertise. Materials 2022, 15, 1763. [Google Scholar] [CrossRef]
- Piemjai, M.; Arksornnukit, M. Compressive fracture resistance of porcelain laminates bonded to enamel or dentin with four adhesive systems. J. Prosthodont. 2007, 16, 457–464. [Google Scholar] [CrossRef]
- Aykor, A.; Ozel, E. Five-year clinical evaluation of 300 teeth restored with porcelain laminate veneers using total-etch and a modified self-etch adhesive system. Oper. Dent. 2009, 34, 516–523. [Google Scholar] [CrossRef]
- Magne, P.; Belser, U.C. Novel porcelain laminate preparation approach driven by a diagnostic mock-up. J. Esthet. Restor. Dent. 2004, 16, 7–18. [Google Scholar] [CrossRef]
- Bernauer, S.A.; Zitzmann, N.U.; Joda, T. The Complete Digital Workflow in Fixed Prosthodontics Updated: A Systematic Review. Healthcare 2023, 11, 679. [Google Scholar] [CrossRef]
- Joda, T.; Zarone, F.; Ferrari, M. The complete digital workflow in fixed prosthodontics: A systematic review. BMC Oral. Health 2017, 17, 124. [Google Scholar] [CrossRef]
- Ahlholm, P.; Sipilä, K.; Vallittu, P.; Jakonen, M.; Kotiranta, U. Digital Versus Conventional Impressions in Fixed Prosthodontics: A Review. J. Prosthodont. 2018, 27, 35–41. [Google Scholar] [CrossRef]
- Chochlidakis, K.M.; Papaspyridakos, P.; Geminiani, A.; Chen, C.J.; Feng, I.J.; Ercoli, C. Digital versus conventional impressions for fixed prosthodontics: A systematic review and meta-analysis. J. Prosthet. Dent. 2016, 116, 184–190. [Google Scholar] [CrossRef]
- Jurado, C.A.; Lee, D.; Cortes, D.; Kaleinikova, Z.; Hernandez, A.I.; Donato, M.V.; Tsujimoto, A. Fracture Resistance of Chairside CAD/CAM Molar Crowns Fabricated with Different Lithium Disilicate Ceramic Materials. Int. J. Prosthodont. 2023, 36, 722–729. [Google Scholar] [CrossRef] [PubMed]
- Jurado, C.A.; Bora, P.V.; Azpiazu-Flores, F.X.; Cho, S.H.; Afrashtehfar, K.I. Effect of resin cement selection on fracture resistance of chairside CAD-CAM lithium disilicate crowns containing virgilite: A comparative in vitro study. J. Prosthet. Dent. 2023, in press. [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).