Development and Characterization of Aloe vera Mucilaginous-Based Hydrogels for Psoriasis Treatment
Abstract
:1. Introduction
2. Materials and Methods
2.1. Materials
2.2. Methods
2.2.1. Preparation of AE
2.2.2. Polysaccharide Fraction Extraction and Characterization
2.2.3. Hydrogel Based on A. vera Extract
2.2.4. Characterization
Spreadability
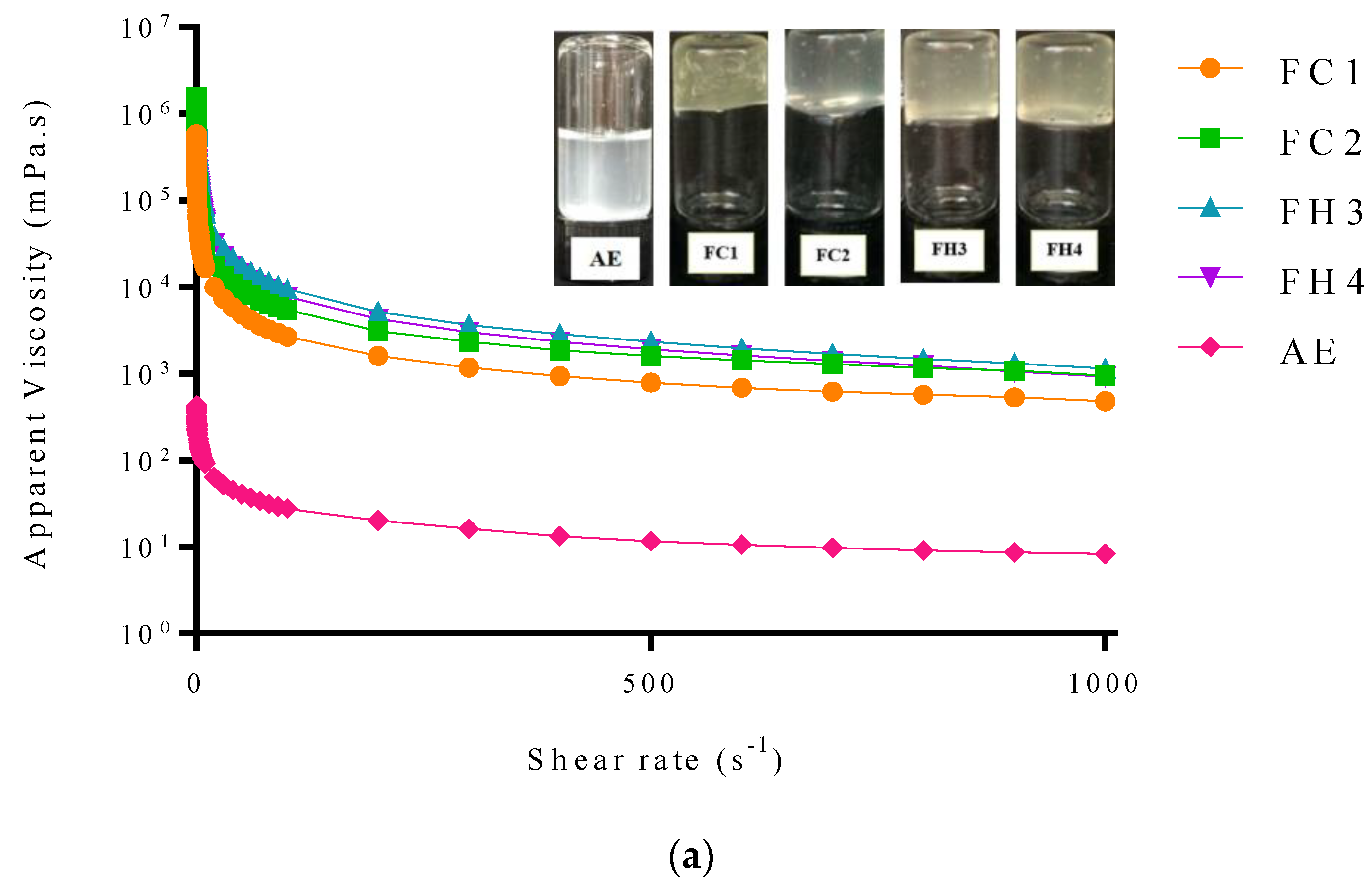
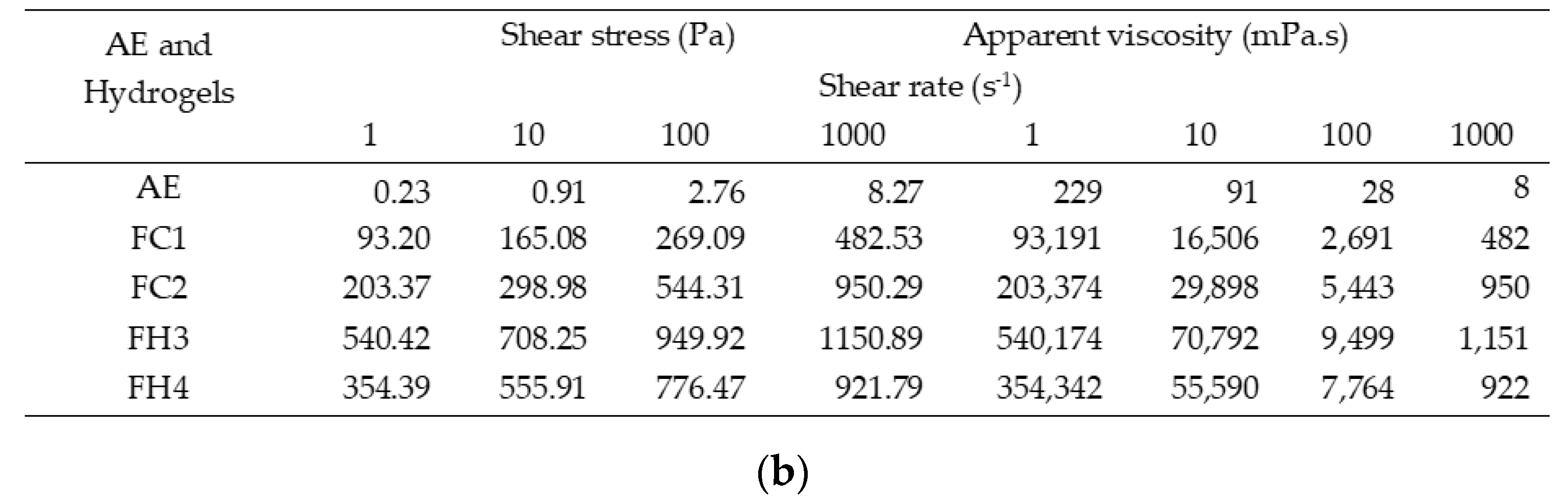
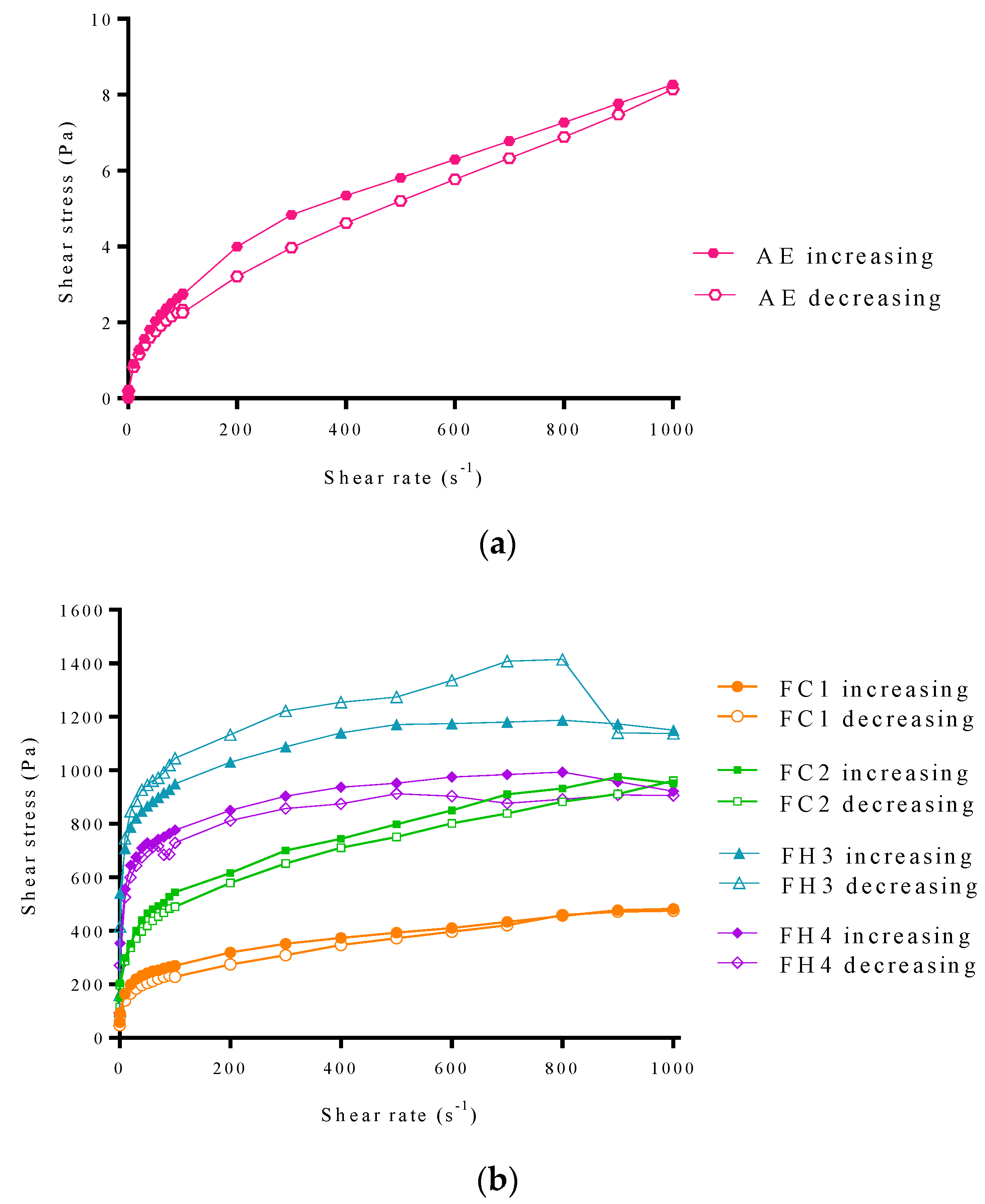
Rheological Properties
Determination of Glucomannan from AE and Hydrogels
2.2.5. In Vivo Antipsoriatic Activity
2.3. Statistical Analysis
3. Results and Discussions
3.1. Identification of Glucomannan by FTIR and 1H-NMR
3.2. Aloe vera Hydrogel Characterization
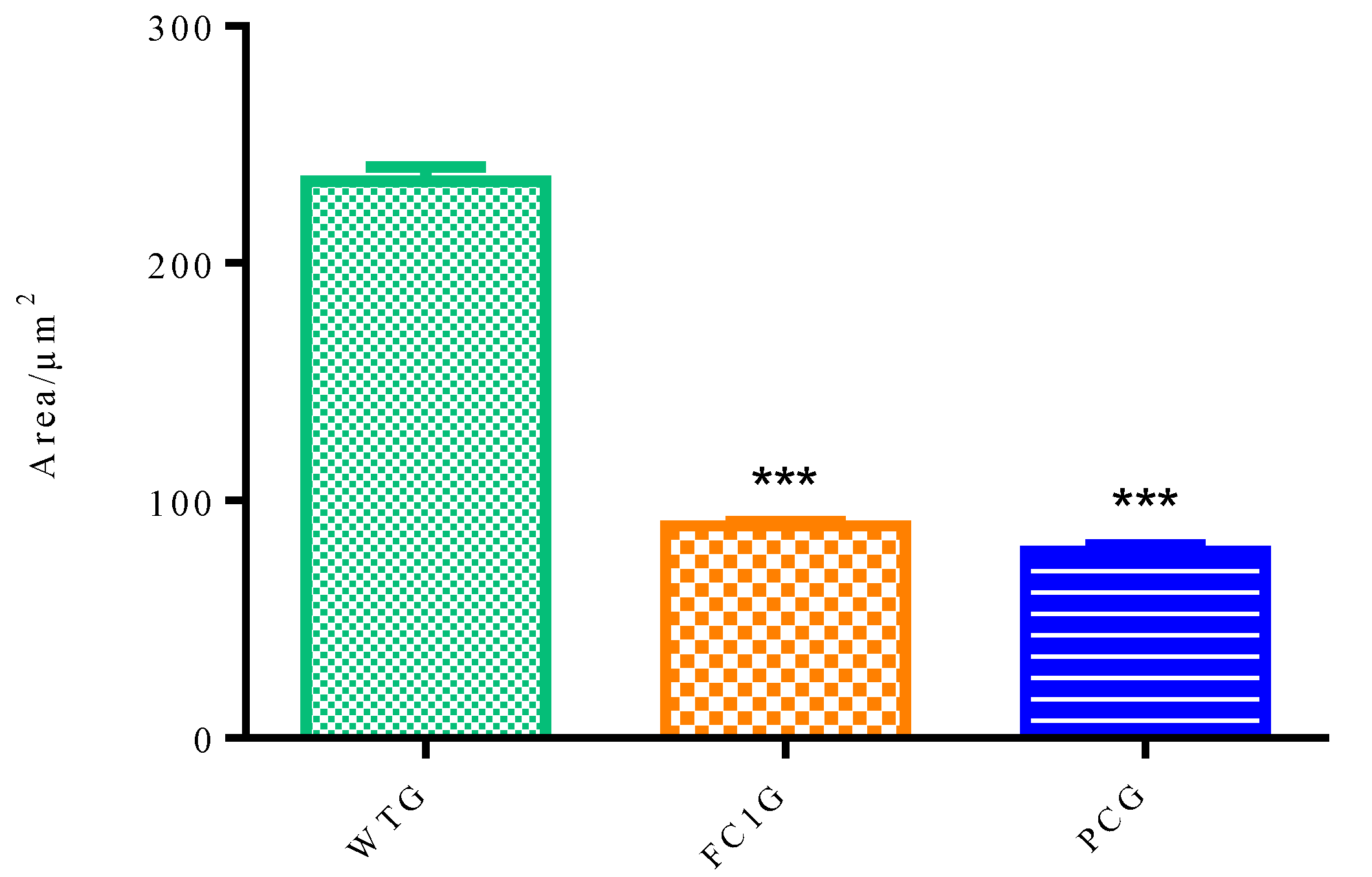
3.3. In Vivo Antipsoriatic Activity
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ray, A.; Aswatha, S.M. An Analysis of the Influence of Growth Periods on Physical Appearance, and Acemannan and Elemental Distribution of Aloe vera L. Gel. Ind. Crops Prod. 2013, 48, 36–42. [Google Scholar] [CrossRef]
- Chang, X.L.; Wang, C.; Feng, Y.; Liu, Z. Effects of Heat Treatments on the Stabilities of Polysaccharides Substances and Barbaloin in Gel Juice from Aloe vera Miller. J. Food Eng. 2006, 75, 245–251. [Google Scholar] [CrossRef]
- Choi, S.; Chung, M.H. A Review on the Relationship between Aloe vera Components and Their Biologic Effects. Semin. Integr. Med. 2003, 1, 53–62. [Google Scholar] [CrossRef]
- Chun-hui, L.; Chang-hai, W.; Zhi-liang, X.; Yi, W. Isolation, Chemical Characterization and Antioxidant Activities of Two Polysaccharides from the Gel and the Skin of Aloe barbadensis Miller Irrigated with Sea Water. Process Biochem. 2007, 42, 961–970. [Google Scholar] [CrossRef]
- Femenia, A.; Sánchez, E.S.; Simal, S.; Rosselló, C. Compositional Features of Polysaccharides from Aloe vera (Aloe barbadensis Miller) Plant Tissues. Carbohydr. Polym. 1999, 39, 109–117. [Google Scholar] [CrossRef]
- Hamman, J.H. Composition and Applications of Aloe vera Leaf Gel. Molecules 2008, 13, 1599–1616. [Google Scholar] [CrossRef]
- Ni, Y.; Turner, D.; Yates, K.M.; Tizard, I. Isolation and Characterization of Structural Components of Aloe vera L. Leaf Pulp. Int. Immunopharmacol. 2004, 4, 1745–1755. [Google Scholar] [CrossRef]
- Ray, A.; Dutta Gupta, S.; Ghosh, S. Isolation and Characterization of Potent Bioactive Fraction with Antioxidant and UV Absorbing Activity from Aloe barbadensis Miller Gel. J. Plant Biochem. Biotechnol. 2013, 22, 483–487. [Google Scholar] [CrossRef]
- Reynolds, T.; Dweck, A.C. Aloe vera Leaf Gel: A Review Update. J. Ethnopharmacol. 1999, 68, 3–37. [Google Scholar] [CrossRef]
- Rodríguez-González, V.M.; Femenia, A.; González-Laredo, R.F.; Rocha-Guzmán, N.E.; Gallegos-Infante, J.A.; Candelas-Cadillo, M.G.; Ramírez-Baca, P.; Simal, S.; Rosselló, C. Effects of Pasteurization on Bioactive Polysaccharide Acemannan and Cell Wall Polymers from Aloe barbadensis Miller. Carbohydr. Polym. 2011, 86, 1675–1683. [Google Scholar] [CrossRef]
- Talmadge, J.; Chavez, J.; Jacobs, L.; Munger, C.; Chinnah, T.; Chow, J.T.; Williamson, D.; Yates, K. Fractionation of Aloe vera L. Inner Gel, Purification and Molecular Profiling of Activity. Int. Immunopharmacol. 2004, 4, 1757–1773. [Google Scholar] [CrossRef] [PubMed]
- Turner, C.E.; Williamson, D.A.; Stroud, P.A.; Talley, D.J. Evaluation and Comparison of Commercially Available Aloe vera L. Products Using Size Exclusion Chromatography with Refractive Index and Multi-Angle Laser Light Scattering Detection. Int. Immunopharmacol. 2004, 4, 1727–1737. [Google Scholar] [CrossRef] [PubMed]
- Davis, B.; Goux, W.J. Single-Laboratory Validation of an NMR Method for the Determination of Aloe vera Polysaccharide in Pharmaceutical Formulations. J. AOAC Int. 2009, 92, 1607–1616. [Google Scholar] [CrossRef]
- Jiao, P.; Jia, Q. Quantitative H-NMR Spectrometry Method for Quality Control of Loe Ver Products. J. AOAC Int. 2010, 93, 842–848. [Google Scholar] [CrossRef]
- Simões, J.; Nunes, F.M.; Domingues, P.; Coimbra, M.A.; Domingues, M.R. Mass Spectrometry Characterization of an Aloe vera Mannan Presenting Immunostimulatory Activity. Carbohydr. Polym. 2012, 90, 229–236. [Google Scholar] [CrossRef] [PubMed]
- Bozzi, A.; Perrin, C.; Austin, S.; Arce Vera, F. Quality and Authenticity of Commercial Aloe vera Gel Powders. Food Chem. 2007, 103, 22–30. [Google Scholar] [CrossRef]
- Khan, A.W.; Kotta, S.; Ansari, S.H.; Sharma, R.K.; Kumar, A.; Ali, J. Formulation Development, Optimization and Evaluation of Aloe vera Gel for Wound Healing. Pharmacogn. Mag. 2013, 9, 6–10. [Google Scholar] [CrossRef]
- Boateng, J.S.; Matthews, K.H.; Stevens, H.N.E.; Eccleston, G.M. Wound Healing Dressings and Drug Delivery Systems: A Review. J. Pharm. Sci. 2008, 97, 2892–2923. [Google Scholar] [CrossRef]
- Korać, R.; Khambholja, K. Potential of Herbs in Skin Protection from Ultraviolet Radiation. Pharmacogn. Rev. 2011, 5, 164. [Google Scholar] [CrossRef]
- Maenthaisong, R.; Chaiyakunapruk, N.; Niruntraporn, S.; Kongkaew, C. The Efficacy of Aloe vera Used for Burn Wound Healing: A Systematic Review. Burns 2007, 33, 713–718. [Google Scholar] [CrossRef]
- Somboonwong, J.; Thanamittramanee, S. Therapeutic Effects of Aloe vera on Cutaneous Microcirculation and Wound Healing in Second Degree Burn Model in Rats. J. Med. Assoc. Thail. 2000, 83, 417–425. [Google Scholar]
- Brasil. Tecnologia E Insumos Estratégicos Em Saúde; Ministério da Saúde Secretaria de Atenção Especializada À Saúde Secretaria de Ciência: Brasília, Brazil, 2021. [Google Scholar]
- Leng, H.; Pu, L.; Xu, L.; Shi, X.; Ji, J.; Chen, K. Effects of Aloe Polysaccharide, a Polysaccharide Extracted from Aloe vera, on TNF-a-Induced HaCaT Cell Proliferation and the Underlying Mechanism in Psoriasis. Mol. Med. Rep. 2018, 18, 3537–3543. [Google Scholar] [CrossRef] [PubMed]
- Yadav, K.; Soni, A.; Singh, D.; Singh, M.R. Polymers in Topical Delivery of Anti-Psoriatic Medications and Other Topical Agents in Overcoming the Barriers of Conventional Treatment Strategies. Prog. Biomater. 2021, 10, 1–17. [Google Scholar] [CrossRef]
- Sabat, R.; Philipp, S.; Höflich, C.; Kreutzer, S.; Wallace, E.; Asadullah, K.; Volk, H.-D.; Sterry, W.; Wolk, K. Immunopathogenesis of Psoriasis. Exp. Dermatol. 2007, 16, 779–798. [Google Scholar] [CrossRef] [PubMed]
- Raut, A.S.; Prabhu, R.H.; Patravale, V.B. Psoriasis Clinical Implications and Treatment: A Review. Crit. Rev.TM Ther. Drug Carr. Syst. 2013, 30, 183–216. [Google Scholar] [CrossRef]
- World Health Organization. Global Report on Psoriasis; World Health Organization: Geneva, Switzerland, 2016. [Google Scholar]
- Lowes, M.A.; Russell, C.B.; Martin, D.A.; Towne, J.E.; Krueger, J.G. The IL-23/T17 Pathogenic Axis in Psoriasis Is Amplified by Keratinocyte Responses. Trends Immunol. 2013, 34, 174–181. [Google Scholar] [CrossRef] [PubMed]
- Sala, M.; Elaissari, A.; Fessi, H. Advances in Psoriasis Physiopathology and Treatments: Up to Date of Mechanistic Insights and Perspectives of Novel Therapies Based on Innovative Skin Drug Delivery Systems (ISDDS). J. Control. Release 2016, 239, 182–202. [Google Scholar] [CrossRef]
- Choonhakarn, C.; Busaracome, P.; Sripanidkulchai, B.; Sarakarn, P. A Prospective, Randomized Clinical Trial Comparing Topical Aloe vera with 0.1% Triamcinolone Acetonide in Mild to Moderate Plaque Psoriasis. J. Eur. Acad. Dermatol. Venereol. 2009, 24, 168–172. [Google Scholar] [CrossRef]
- Deng, S.; May, B.H.; Zhang, A.L.; Lu, C.; Xue, C.C.L. Plant Extracts for the Topical Management of Psoriasis: A Systematic Review and Meta-Analysis. Br. J. Dermatol. 2013, 169, 769–782. [Google Scholar] [CrossRef]
- Miroddi, M.; Navarra, M.; Calapai, F.; Mancari, F.; Giofrè, S.V.; Gangemi, S.; Calapai, G. Review of Clinical Pharmacology of Aloe vera L. in the Treatment of Psoriasis. Phytother. Res. 2015, 29, 648–655. [Google Scholar] [CrossRef]
- Syed, T.A.; Ahmad, S.A.; Holt, A.H.; Ahmad, S.H.; Ahmad, S.A.; Afzal, M. Management of Psoriasis with Aloe vera Extract in a Hydrophilic Cream: A Placebo-Controlled, Double-Blind Study. Trop. Med. Int. Health 1996, 1, 505–509. [Google Scholar] [CrossRef] [PubMed]
- Menter, A.; Korman, N.J.; Elmets, C.A.; Feldman, S.R.; Gelfand, J.M.; Gordon, K.B.; Gottlieb, A.; Koo, J.Y.M.; Lebwohl, M.; Lim, H.W.; et al. Guidelines of Care for the Management of Psoriasis and Psoriatic Arthritis. J. Am. Acad. Dermatol. 2010, 62, 114–135. [Google Scholar] [CrossRef] [PubMed]
- Wollina, U.; França, K.; Lotti, T.; Tirant, M. Adjuvant Treatment of Chronic Plaque Psoriasis in Adults by a Herbal Combination: Open German Trial and Review of the Literature. Dermatol. Ther. 2020, 33, e12624. [Google Scholar] [CrossRef] [PubMed]
- Dhanabal, S.P.; Priyanka Dwarampudi, L.; Muruganantham, N.; Vadivelan, R. Evaluation of the Antipsoriatic Activity of Aloe vera Leaf Extract Using a Mouse Tail Model of Psoriasis. Phytother. Res. 2012, 26, 617–619. [Google Scholar] [CrossRef]
- Vogel, G.H. Drug Discovery and Evaluation: Pharmacological Assays, 3rd ed.; Springer: Berlin/Heidelberg, Germany, 2008; Volume 2. [Google Scholar]
- Brazil. Guia de Controle de Qualidade de Produtos Cosméticos; Agencia Nacional de Vigilancia Sanitaria (ANVISA): Brasília, Brazil, 2008. [Google Scholar]
- Kiran, P.; Rao, P.S. Rheological and Structural Characterization of Prepared Aqueous Aloe vera Dispersions. Food Res. Int. 2014, 62, 1029–1037. [Google Scholar] [CrossRef]
- Kiran, P.; Rao, P.S. Development and Characterization of Reconstituted Hydrogel from Aloe vera (Aloe barbadensis Miller) Powder. J. Food Meas. Charact. 2016, 10, 411–424. [Google Scholar] [CrossRef]
- Brazil. Farmacopeia Brasileira, 6th ed.; ANVISA, Ed.; Agencia Nacional de Vigilancia Sanitaria (ANVISA): Brasília, Brazil, 2019. [Google Scholar]
- Borghetti, G.S.; Knorst, M.T. Desenvolvimento e Avaliação Da Estabilidade Física de Loções O/A Contendo Filtros Solares. Rev. Bras. Cienc. Farm./Braz. J. Pharm. Sci. 2006, 42, 531–537. [Google Scholar] [CrossRef]
- Knorst, M.T. Desenvolvimento Tecnologico de Forma Farmaceutica Plastica Contendo Extrato Concentrado de Achyrocline Satureiodes (LAM.) DC. Compositae (Marcela). Ph.D. Thesis, Universidade Federal Do Rio Grande Do Sul, Porto Alegre, Brazil, 1991. [Google Scholar]
- Campestrini, L.H.; Silveira, J.L.M.; Duarte, M.E.R.; Koop, H.S.; Noseda, M.D. NMR and Rheological Study of Aloe barbadensis Partially Acetylated Glucomannan. Carbohydr. Polym. 2013, 94, 511–519. [Google Scholar] [CrossRef]
- Eberendu, A.N.R.; McAnalley, B.H. Colorimetric Assay for Bioactive Polysaccharide. U.S. Patent 5,512,488, 30 April 1996. [Google Scholar]
- Eberendu, A.R.; Luta, G.; Edwards, J.A.; Mcanalley, B.H.; Davis, B.; Rodriguez, S.; Ray Henry, C. Quantitative Colorimetric Analysis of Aloe Polysaccharides as a Measure of Aloe vera Quality in Commercial Products. J. AOAC Int. 2005, 88, 684–691. [Google Scholar] [CrossRef]
- Chang, X.L.; Chen, B.Y.; Feng, Y.M. Water-Soluble Polysaccharides Isolated from Skin Juice, Gel Juice and Flower of Aloe vera Miller. J. Taiwan Inst. Chem. Eng. 2011, 42, 197–203. [Google Scholar] [CrossRef]
- Yaron, A.; Cohen, E.; Arad, S. Stabilization of Aloe vera Gel by Interaction with Sulfated Polysaccharides from Red Microalgae and with Xanthan Gum. J. Agric. Food Chem. 1992, 40, 1316–1320. [Google Scholar] [CrossRef]
- Nejatzadeh-Barandozi, F.; Enferadi, S. FT-IR Study of the Polysaccharides Isolated from the Skin Juice, Gel Juice, and Flower of Aloe vera Tissues Affected by Fertilizer Treatment. Org. Med. Chem. Lett. 2012, 2, 33. [Google Scholar] [CrossRef] [PubMed]
- Diehl, B.; Teichmuller, E.E. Aloe vera, Quality Inspection and Identification. Agro Food Ind. Hi-Tech 1998, 9, 14–16. [Google Scholar]
- Minjares-Fuentes, R.; Eim, V.; González-Centeno, M.R.; Femenia, A.; Rodríguez-González, V.M.; González-Laredo, R.F. Effect of Different Drying Procedures on the Bioactive Polysaccharide Acemannan from Aloe vera (Aloe barbadensis Miller). Carbohydr. Polym. 2017, 168, 327–336. [Google Scholar] [CrossRef] [PubMed]
- American Herbal Pharmacopoeia. Aloe vera (L.) Burm. f., Standards of Identity, Analysis, and Quality Control; Upton, R., Axentiev, P., Swisher, D., Eds.; American Herbal Pharmacopoeia®: Scotts Valley, CA, USA, 2012; pp. 1–52. [Google Scholar]
- Prista, L.N.; Alves, A.C.; Morgado, R. Técnicas Farmaceuticas e Farmácia Galênica, 4th ed.; Fundação Calouste Gulbenkian, Ed.; Fundaçao Calouste Gulbenkian: Lisboa, Portugal, 1991. [Google Scholar]
- Powar, T.A.; Nadaf, S.J.; Patil-vibhute, P.B.; Otari, A.R. Design, Fabrication, In Vitro and In Vivo Assessment of Aloe vera Containing Transgel for Delivery of Meloxicam. Asian J. Pharm. 2016, 10, 222–231. [Google Scholar] [CrossRef]
- Al-Suwayeh, S.A.; Taha, E.I.; Al-Qahtani, F.M.; Ahmed, M.O.; Badran, M.M. Evaluation of Skin Permeation and Analgesic Activity Effects of Carbopol Lornoxicam Topical Gels Containing Penetration Enhancer. Sci. World J. 2014, 2014, 127495. [Google Scholar] [CrossRef]
- Medina-Torres, L.; Calderas, F.; Minjares, R.; Femenia, A.; Sánchez-Olivares, G.; Gónzalez-Laredo, F.R.; Santiago-Adame, R.; Ramirez-Nuñez, D.M.; Rodríguez-Ramírez, J.; Manero, O. Structure Preservation of Aloe vera (Barbadensis Miller) Mucilage in a Spray Drying Process. LWT—Food Sci. Technol. 2016, 66, 93–100. [Google Scholar] [CrossRef]
- Schramm, G. Reologia e Reometria: Fundamentos Teóricos e Práticos, 1st ed.; Artliber: São Paulo, Brazil, 2006. [Google Scholar]
- Femenia, A.; García-Pascual, P.; Simal, S.; Roselló, C. Effects of Heat Treatment and Dehydration on Bioactive Polysaccaride Acemannan and Cell Wall Polymers from Aloe barbadensis Miller. Carbohydr. Polym. 2003, 51, 397–405. [Google Scholar] [CrossRef]





| Ingredients (g) | FC1 | FC2 | FH3 | FH4 | Function |
|---|---|---|---|---|---|
| A. vera (L.) extract | 80.0 | 80.0 | 80.0 | 80.0 | API * |
| Carbopol 940 | 1.0 | 1.0 | - | - | Gelling |
| Hydroxyethylcellulose | - | - | 2.0 | 2.0 | Gelling |
| Citric acid | 0.5 | - | - | 0.5 | Acidulant |
| Aminomethylpropanol | qs. | qs. | - | - | Alkalizing |
| Methylparaben | 0.2 | 0.2 | 0.2 | 0.2 | Preservative |
| Imidazolidinyl urea | 0.3 | 0.3 | 0.3 | 0.3 | Preservative |
| Propylene glycol | 5.0 | 5.0 | 5.0 | 5.0 | Humectant |
| Disodium edetate | 0.1 | 0.1 | 0.1 | 0.1 | Chelator |
| Sodium metabisulphite | 0.05 | 0.05 | 0.05 | 0.05 | Antioxidant |
| Distilled water q.s.p. | 100.0 | 100.0 | 100.0 | 100.0 | Vehicle |
| Parameters | FC1 | FC2 | FH3 | FH4 |
|---|---|---|---|---|
| Odor | typical | Typical | typical | typical |
| Color | Yellow | light Yellow | light Yellow | light Yellow |
| Aspect | Homogeneous | Homogeneous | Homogeneous | Homogeneous |
| Opacity | Opaque | Opaque | Opaque | Opaque |
| Fluidity | Absent | Absent | Absent | Absent |
| pH | 6.70 ± 0.03 | 7.18 ± 0.19 | 6.31 ± 0.14 | 4.67 ± 0.11 |
| Parameters | FC1 | FC2 | FH3 | FH4 |
|---|---|---|---|---|
| Maximum spreadability (mm2) | 5155.5 ± 279.3 | 5243.1 ± 394.2 | 3421.7 ± 103.7 | 3614.0 ± 30.7 |
| Rheological behavior | Thixotropic | Thixotropic | Rheopectic | Thixotropic |
| Glucomannan content of AE (mg/g) * and (w/w) | 13.87 ± 0.53(1.4%) | |||
| Glucomannan content of hydrogels (mg/g) ** and (w/w) | 8.69 ± 0.24 (0.87%) | 9.17 ± 0.20 (0.92%) | 6.76 ± 1.06 (0.67%) | 4.01 ± 0.51 (0.40%) |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Jales, S.T.L.; Barbosa, R.d.M.; de Albuquerque, A.C.; Duarte, L.H.V.; da Silva, G.R.; Meirelles, L.M.A.; da Silva, T.M.S.; Alves, A.F.; Viseras, C.; Raffin, F.N.; et al. Development and Characterization of Aloe vera Mucilaginous-Based Hydrogels for Psoriasis Treatment. J. Compos. Sci. 2022, 6, 231. https://doi.org/10.3390/jcs6080231
Jales STL, Barbosa RdM, de Albuquerque AC, Duarte LHV, da Silva GR, Meirelles LMA, da Silva TMS, Alves AF, Viseras C, Raffin FN, et al. Development and Characterization of Aloe vera Mucilaginous-Based Hydrogels for Psoriasis Treatment. Journal of Composites Science. 2022; 6(8):231. https://doi.org/10.3390/jcs6080231
Chicago/Turabian StyleJales, Silvana T. L., Raquel de M. Barbosa, André C. de Albuquerque, Luan H. V. Duarte, Girliane R. da Silva, Lyghia M. A. Meirelles, Tania M. S. da Silva, Adriano F. Alves, César Viseras, Fernanda N. Raffin, and et al. 2022. "Development and Characterization of Aloe vera Mucilaginous-Based Hydrogels for Psoriasis Treatment" Journal of Composites Science 6, no. 8: 231. https://doi.org/10.3390/jcs6080231
APA StyleJales, S. T. L., Barbosa, R. d. M., de Albuquerque, A. C., Duarte, L. H. V., da Silva, G. R., Meirelles, L. M. A., da Silva, T. M. S., Alves, A. F., Viseras, C., Raffin, F. N., & Moura, T. F. A. d. L. (2022). Development and Characterization of Aloe vera Mucilaginous-Based Hydrogels for Psoriasis Treatment. Journal of Composites Science, 6(8), 231. https://doi.org/10.3390/jcs6080231







