Color Stability Determination of CAD/CAM Milled and 3D Printed Acrylic Resins for Denture Bases: A Narrative Review
Abstract
1. Introduction
1.1. Optical Properties of CAD/CAM Milled and 3D Printed Denture Base Resins
1.1.1. Color Dimensions and Eye Perception
- Metamerism
- Transparency and translucency
- Hue (color name, color tone). It is dependent on the wavelength, determines the location of the color in the color space and is indicated by its name, red, green, etc., respectively.
- Saturation (color density). The greater the amount of dye, the greater its degree. From a practical point of view, it is assumed that the color is richer, when its saturation is more significant.
- Brightness (bleaching, color vitality). In Munsell’s system, it is measured from 0 (pure black) to 10 (pure white). This indicator measures the amount of white, gray or black in a certain color. By reducing the black color, one goes through the different shades of gray. The spherical color space at the bottom of the sphere in the Munsell system is the magnitude of the bleaching (brightness, vitality) [13].
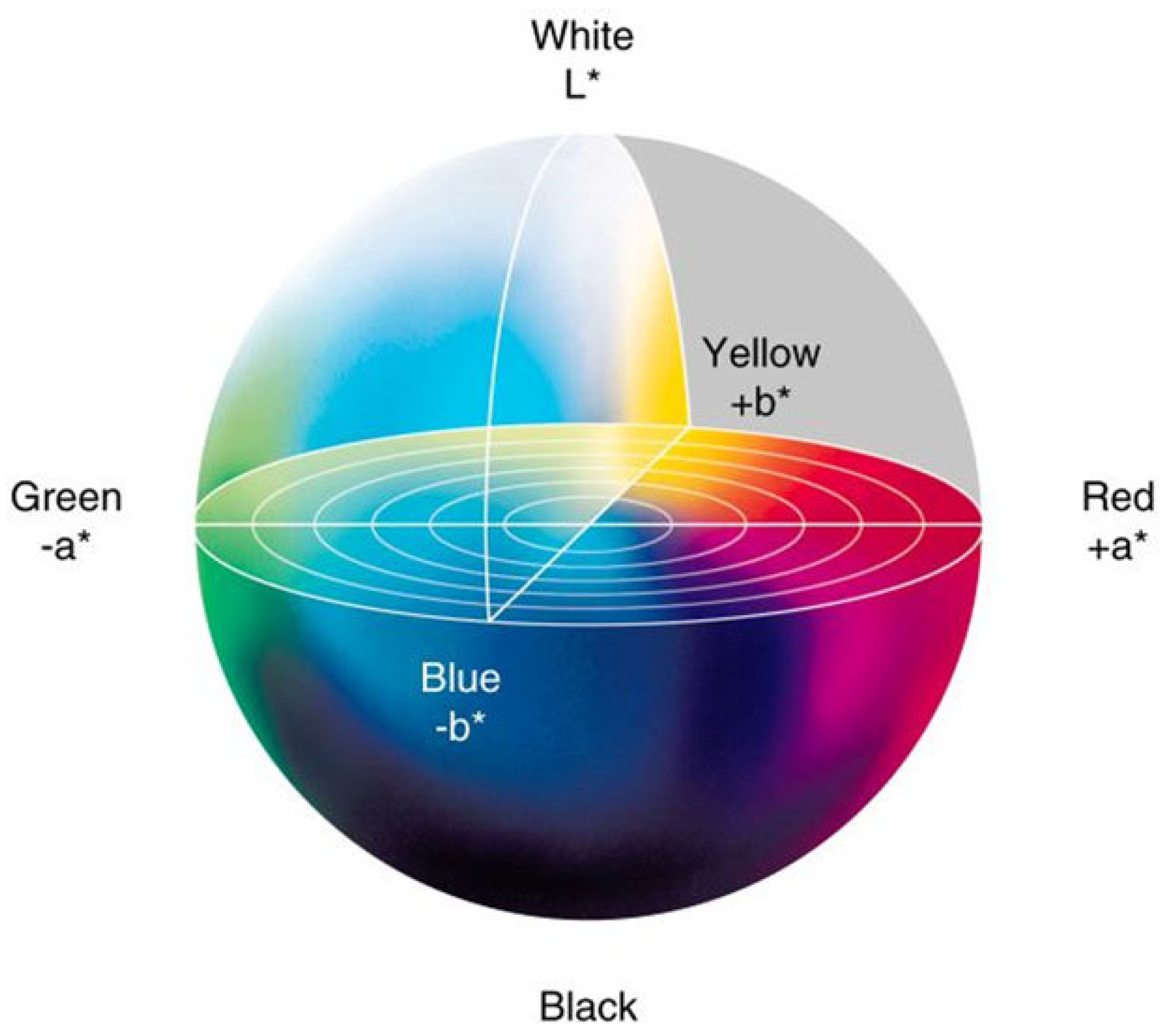
1.1.2. CIELAB Color System
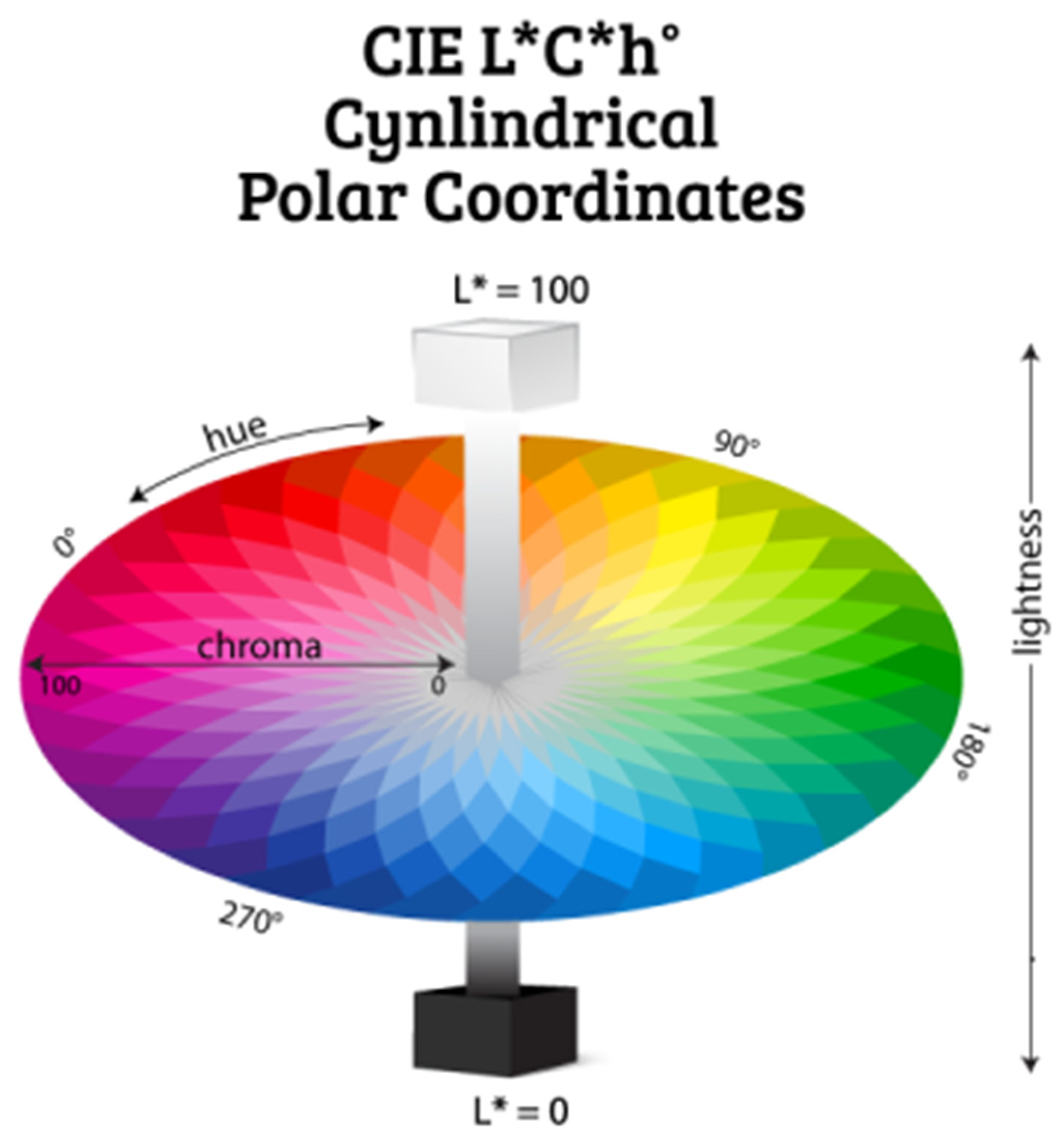
1.1.3. CIEHLC Color System
1.1.4. Conversion between CIELAB and CIEHLC
- Xn = 950,489
- Yn = 100
- Zn = 1,088,840
- Xn = 964,212
- Yn = 100
- Zn = 825,188
1.2. Objective Methods for Color Stability Evaluation of CAD/CAM Acrylic Resins
1.2.1. Visual Methods for Color Determination
1.2.2. Instrumental Methods for Optical Changes Determination
- Colorimeters
- Spectrophotometers
- Delta E(ΔE)
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| PMMA | Polymethyl methacrylate |
| STL | Stereolithography, standard triangle language, standard tessellation language |
| 3D | Three-dimensional |
| CAD/CAM | Computer-aided design/computer-aided manufacturing |
| CD | Complete dentures |
| CIE | International Commission of Illumination |
| NBS | National Bureau of Standards |
| OD | Optical density |
References
- Davidowitz, G.; Kotick, P.G. The use of CAD/CAM in dentistry. Dent. Clin. N. Am. 2011, 55, 559–570. [Google Scholar] [CrossRef] [PubMed]
- Gao, W.; Zhang, Y.; Ramanujan, D.; Ramani, K.; Chen, Y.; Williams, C.B.; Wang, C.C.L.; Shin, Y.C.; Zhang, S.; Zavattieri, P.D. The status, challenges, and future of additive manufacturing in engineering. Comput. Aided Des. 2015, 69, 65–89. [Google Scholar] [CrossRef]
- Okubo, S.R.; Kanawati, A.; Richards, M.W.; Childress, S. Evaluation of visual and instrument shade matching. J. Prosthet. Dent. 1998, 80, 642–648. [Google Scholar] [CrossRef]
- Batisse, C.; Nicolas, E. Comparison of CAD/CAM and Conventional Denture Base Resins: A Systematic Review. Appl. Sci. 2021, 11, 5990. [Google Scholar] [CrossRef]
- Grande, F.; Tesini, F.; Pozzan, M.C.; Zamperoli, E.M.; Carossa, M.; Catapano, S. Comparison of the Accuracy between Denture Bases Produced by Subtractive and Additive Manufacturing Methods: A Pilot Study. Prosthesis 2022, 4, 151–159. [Google Scholar] [CrossRef]
- Anadioti, E.; Musharbash, L.; Blatz, M.B.; Papavasiliou, G.; Kamposiora, P. 3D printed complete removable dental prostheses: A narrative review. BMC Oral Health 2020, 20, 343. [Google Scholar] [CrossRef] [PubMed]
- Chuchulska, B.; Zlatev, S. Linear dimensional change and ultimate tensile strength of polyamide materials for denture bases. Polymers 2021, 13, 3446. [Google Scholar] [CrossRef]
- Arana-Correa, B.E.; Sepúlveda-Navarro, W.F.; Florez, F.L.; Urban, V.M.; Jorge, J.H.; Campanha, N.H. Colour stability of acrylic resin denture teeth after immersion in different beverages. Eur. J. Prosthodont. Restor. Dent. 2014, 22, 56–61. [Google Scholar]
- Da Costa, G.C.; Aras, M.A.; Chalakkal, P. Shade guide for the fabrication of acrylic denture based on mucosal colour. J. Clin. Diagn Res. 2017, 11, ZD12–ZD13. [Google Scholar] [CrossRef]
- Bonatti, M.R.; Cunha, T.R.; Regis, R.R.; Silva-Lovato, C.H.; Paranhos, H.F.; de Souza, R.F. The effect of polymerization cycles on color stability of microwave-processed denture base resin. J. Prosthodont. 2009, 18, 432–437. [Google Scholar] [CrossRef]
- Sharma, D.; Bhat, A.M.; Arora, H. Comparison of color stability of four heat-cured denture resins in various staining solutions. J. Pre. Clin. Dent. Res. 2015, 2, 2–8. [Google Scholar]
- Lee, Y.-K. Translucency of human teeth and dental restorative materials and its clinical relevance. J. Biomed. Opt. 2015, 20, 45002. [Google Scholar] [CrossRef] [PubMed]
- Chu, S.J.; Trushkowsky, R.D.; Paravina, R.D. Dental color matching instruments and systems. Review of clinical and research aspects. J. Dent. 2010, 38, e2–e16. [Google Scholar] [CrossRef] [PubMed]
- CIE 15, Colorimetry, 3rd ed.; Technical Report; Commission Internationale de 1′Eclairage: Vienna, Austria, 2004; ISBN 3-901-906-33-9.
- Fairchild, M.D. Color Appearance Models; John Wiley and Sons: Hoboken, NJ, USA, 2005; p. 340. ISBN 0-470-01216-1. [Google Scholar]
- Official Web Page. Available online: www.en.wikipedia.org/wiki/CIELAB_color_space (accessed on 29 January 2022).
- Available online: https://cie.co.at/e-ilv (accessed on 28 December 2019).
- Available online: https://www.w3.org/TR/css-color-4/ (accessed on 29 January 2022).
- Keenan, P.L.; Radford, D.R.; Clark, R.K. Dimensional change in complete dentures fabricated by injection molding and microwave processing. J. Prosthet. Dent. 2003, 89, 37–44. [Google Scholar] [CrossRef] [PubMed]
- Sarkis, E. Color change of some aesthetic dental materials: Effect of immersion solutions and finishing of their surfaces. Saudi Dent. J. 2012, 24, 85–89. [Google Scholar] [CrossRef]
- Jarad, F.D.; Russell, M.D.; Moss, B.W. The use of digital imaging for colour matching and communication in restorative dentistry. Br. Dent. J. 2005, 199, 43–49. [Google Scholar] [CrossRef]
- Berns, R.S.; Bilmeyer, F.W.; Saltzman, M. Principles of Color Technology, 3rd ed.; Wiley: New York, NY, USA, 2000; pp. 71–74. [Google Scholar]
- Gregorius, W.C.; Kattadiyil, M.T.; Goodacre, C.J.; Roggenkamp, C.L.; Powers, J.M.; Paravina, R.D. Effects of ageing and staining on color of acrylic resin denture teeth. J. Dent. 2012, 40, e47–e54. [Google Scholar] [CrossRef]
- Todorov, R. Transparency and Color Characteristics of Frontal Teeth—Measurement, Objectification and Individual Features. Ph.D. Thesis, MU-Plovdiv, Plovdiv, Bulgaria, 2015. [Google Scholar]
- Todorov, R.; Peev, T.; Zlatev, S. Shade guides used in the dental practice. J. IMAB 2020, 26, 3168–3173. [Google Scholar] [CrossRef]
- Singh, K.; Suvarna, S.; Agnihotri, Y.; Sahoo, S.; Kumar, P. Color stability of aesthetic restorative materials after exposure to commonly consumed beverages. Eur. J. Prosthodont. 2014, 2, 15–22. [Google Scholar] [CrossRef]
- Vadher, R.K.; Parmar, G.J.; Kanodia, S.; Chaudhary, A.; Kaur, M.; Savadhariya, T. Basics of Color in Dentistry: A Review. IOSR J. Dent. Med. Sci. 2014, 13, 78–85. [Google Scholar] [CrossRef]
- Ragain, J.C. A review of color science in dentistry: Shade matching in the contemporary dental practice. J. Dent. Oral Disord. Ther. 2016, 4, 1–5. [Google Scholar] [CrossRef]
- Official Web Page. Available online: www.en.wikipedia.org/wiki/Color_difference (accessed on 29 January 2022).
- Heimer, S.; Schmidlin, P.R.; Stawarczyk, B. Discoloration of PMMA, composite, and PEEK. Clin. Oral Investig. 2017, 21, 1191–1200. [Google Scholar] [CrossRef] [PubMed]
- Mortazavi, H.; Baharvand, M.; Khodadoustan, A. Colors in tooth discoloration: A new classification and literature review. Int. J. Clin. Dent. 2014, 7, 17–28. [Google Scholar]
- Miyazaki, T.; Hotta, Y.; Kunii, J.; Kuriyama, S.; Tamaki, Y. A review of dental CAD/CAM: Current status and future perspectives from 20 years of experience. Dent. Mater. J. 2009, 28, 44–56. [Google Scholar] [CrossRef]
- Hunter Labs. Hunter Lab Color Scale. In Insight on Color; Hunter Associates Laboratories: Reston, VA, USA, 1996; Available online: https://measurecolour.com.my/wp-content/uploads/2019/02/Hunter-Lab-Color-Scale-an08_96a2.pdf (accessed on 29 January 2022).
- Zeileis, A.; Hornik, K.; Murrell, P. Escaping RGBland: Selecting colors for statistical graphics. Comput. Stat. Data Anal. 2009, 53, 3259–3270. [Google Scholar] [CrossRef]
- Oguz, S.; Mutluay, M.M.; Dogan, O.M.; Bek, B. Color change evaluation of denture soft lining materials in coffee and tea. Dent. Mater. J. 2007, 26, 209–216. [Google Scholar] [CrossRef]
- Buyukyilmaz, S.; Ruyter, S.E. Colour stability of denture base polymers. Int. J. Prosthodont. 1994, 7, 372–382. [Google Scholar]
- Ruyter, I.E.; Um, C.M. Staining of resin-based veneering materials with coffee and tea. Quintessence Int. 1991, 22, 377–386. [Google Scholar]
- Lai, Y.; Lui, H.; Lee, S. In vitro color stability, stain resistance, and water sorption of four removable gingival flange materials. J. Prosthet Dent. 2003, 90, 293–300. [Google Scholar] [CrossRef]
- Kim, Y.J.; Ha, S.K.; Kim, H.C.; Bang, Y.; Choh, H. Measuring sensitivity of the visual system to reflection optical density variation. In Proceedings of the 31th Conference of Korea Society for Imaging Science and Technology, Busan, Korea, 12 June 2009; pp. 90–91. [Google Scholar]
- Kim, A.-R.; Kim, H.-S.; Park, S.-O. Measuring of the Perceptibility and Acceptability in Various Color Quality Measures. J. Opt. Soc. Korea 2011, 15, 310–317. [Google Scholar] [CrossRef]
- Guler, A.U.; Yilmaz, F.; Kulunk, T.; Guler, E.; Kurt, S. Effects of different drinks on stainability of resin composite provisional restorative materials. J. Prosthet. Dent. 2005, 94, 118–124. [Google Scholar] [CrossRef] [PubMed]
- Koksal, T.; Dikbas, I. Color stability of different denture teeth materials against various staining agents. Dent. Mater. J. 2008, 27, 139–144. [Google Scholar] [CrossRef] [PubMed]
- Polyzois, G.L.; Yannikakis, S.A.; Zissis, A.J.; Demetriou, P.P. Color changes of denture base materials after disinfection and sterilization immersion. Int. J. Prosthodont. 1997, 10, 83–89. [Google Scholar] [PubMed]
- Babikir, M.O.; Gilada, M.W.; Fahmy, F.; Ismail, I.A.; Alhajj, M.N.; Fadul, A.A.; Elasyouti, A. Effect of commonly consumed beverages on color stability of polymethyl methacrylate denture base material. Compend. Contin. Educ. Dent. 2019, 40, e1–e8. [Google Scholar] [PubMed]
- Brewer, J.D.; Wee, A.; Seghi, R. Advances in color matching. Dent. Clin. N. Am. 2004, 48, 341–358. [Google Scholar] [CrossRef] [PubMed]
- Leibrock, A.; Rosentritt, M.; Lang, R.; Behr, M.; Handel, G. Colour stability of visible light curing hybrid composites. Eur. J. Prosthodont. Restor. Dent. 1997, 5, 125–130. [Google Scholar] [PubMed]
- Moon, A.; Powers, J.M.; Kiat-Amnuay, S. Color stability of denture teeth and acrylic base resin subjected daily to various consumer cleansers. J. Esthet. Restor. Dent. 2014, 26, 247–255. [Google Scholar] [CrossRef][Green Version]
- Ozcelik, T.B.; Yilmaz, B.; Ozcan, I.; Kircelli, C. Colorimetric analysis of opaque porcelain fired to different base metal ceramic restoration. J. Prosthet. Dent. 2008, 99, 193–202. [Google Scholar] [CrossRef]
- Hatim, N.A.; Al-Tahho, O.Z. Comparative evaluation of color change between two types of acrylic resin and flexible resin after thermocycling. An in vitro study. J. Indian Prosthodont. Soc. 2013, 13, 327–337. [Google Scholar] [CrossRef]
- Turker, S.B.; Sener, I.D.; Akkus, E.; Bugurman, B. Effect of staining solutions on the colour stability and surface properties of denture base material. Balk. J. Stom. 2012, 16, 49–56. [Google Scholar] [CrossRef]
- Waldemarin, R.F.; Terra, P.C.; Pinto, L.R.; Faot, F.; Camacho, G.B. Color change in acrylic resin processed in three ways after immersion in water, cola, coffee, mate and wine. Acta Odontol Lat. 2013, 26, 138–143. [Google Scholar]
- Amin, F.; Rehman, A.; Azizudin, S. Spectrophotometric assessment of color changes of heat cure acrylic resins after exposure to commonly consumed beverages. J. Dow Univ. Health Sci. 2014, 8, 62–66. [Google Scholar]
- O’Brien, W.; Groh, C.; Boenke, K. A new, small color difference equation for dental shades. J. Dent. Res. 1990, 69, 1762–1764. [Google Scholar] [CrossRef] [PubMed]
- Daries, C. Relève de la Couleur au Cabinet Dentaire: Connaissances et Moyens D’optimisation Actuels. Ph.D. Thesis, Université Toulouse III-Paul Sabatier, Toulouse, France, 2013. [Google Scholar]
- Türker, S.B.; Koçak, A.; Aktepe, E. Effect of five staining solutions on the colour stability of two acrylics and three composite resins based provisional restorations. Eur. J. Prosthodont Restor. Dent. 2006, 14, 121–125. [Google Scholar] [PubMed]
- Chuchulska, B. Comparative Study of the Strength Properties of Injectable Resins in Removable Prosthodontics. Ph.D. Thesis, MU-Plovdiv, Plovdiv, Bulgaria, 2021. [Google Scholar]
- Samra, A.P.; Pereira, S.K.; Delgado, L.C.; Borges, C.P. Color stability evaluation of aesthetic restorative materials. Braz. Oral. Res. 2008, 22, 205–210. [Google Scholar] [CrossRef]
- Hatim, N.A.; Taqa, A.A.; Hasan, R.H. Evaluation of the effect of curing techniques on color property of acrylic resins. Al-Rafidain Dent. J. 2004, 4, 28–33. [Google Scholar] [CrossRef]
- Duymus, Z.Y.; Yanikoglu, N.; Arik, M. Evaluation of colour changed of acrylic resin materials in the different solutions. Asian J. Chem. 2010, 22, 6669–6676. [Google Scholar]
- Dimitrova, M.; Corsalini, M.; Kazakova, R.; Vlahova, A.; Chuchulska, B.; Barile, G.; Capodiferro, S.; Kazakov, S. Comparison between Conventional PMMA and 3D Printed Resins for Denture Bases: A Narrative Review. J. Compos. Sci. 2022, 6, 87. [Google Scholar] [CrossRef]
- Banu, F.; Jeyapalan, K.; Anand Kumar, V.; Modi, K. Comparison of Colour Stability between Various Denture Base Resins on Staining and Denture Cleansing Using Commercially Available Denture Cleansers. Cureus 2020, 12, e6698. [Google Scholar] [CrossRef]
- Dayan, C.; Guven, M.C.; Gencel, B.; Bural, C. A Comparison of the Color Stability of Conventional and CAD/CAM Polymethyl Methacrylate Denture Base Materials. Acta Stomatol. Croat. 2019, 53, 158–167. [Google Scholar] [CrossRef]
- Alp, G.; Johnston, W.M.; Yilmaz, B. Optical properties and surface roughness of prepolymerized poly(methyl methacrylate) denture base materials. J. Prosthet. Dent. 2019, 121, 347–352. [Google Scholar] [CrossRef] [PubMed]
- Papathanasiou, I.; Papavasiliou, G.; Kamposiora, P.; Zoidis, P. Effect of Staining Solutions on Color Stability, Gloss and Surface Roughness of Removable Partial Dental Prosthetic Polymers. J. Prosthodont. 2022, 31, 65–71. [Google Scholar] [CrossRef] [PubMed]
- Zuo, W.; Feng, D.; Song, A.; Gong, H.; Zhu, S. Effects of organic-inorganic hybrid coating on the color stability of denture base resins. J. Prosthet. Dent. 2016, 115, 103–108. [Google Scholar] [CrossRef] [PubMed]
- Kerby, R.E.; Knobloch, L.A.; Schricker, S.; Gregg, B. Synthesis and evaluation of modified urethane dimethacrylate resins with reduced water sorption and solubility. Dent. Mater. 2009, 25, 302–313. [Google Scholar] [CrossRef] [PubMed]
- Shin, J.W.; Kim, J.E.; Choi, Y.J.; Shin, S.H.; Nam, N.E.; Shim, J.S.; Lee, K.W. Evaluation of the color stability of 3D-printed crown and bridge materials against various sources of discoloration: An in vitro study. Materials 2020, 13, 5359. [Google Scholar] [CrossRef]
- Berli, C.; Thieringer, F.M.; Sharma, N.; Müller, J.A.; Dedem, P.; Fischer, J.; Rohr, N. Comparing the mechanical properties of pressed, milled, and 3D-printed resins for occlusal devices. J. Prosthet. Dent. 2020, 124, 780–786. [Google Scholar] [CrossRef]
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2022 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Dimitrova, M.; Corsalini, M.; Kazakova, R.; Vlahova, A.; Barile, G.; Dell’Olio, F.; Tomova, Z.; Kazakov, S.; Capodiferro, S. Color Stability Determination of CAD/CAM Milled and 3D Printed Acrylic Resins for Denture Bases: A Narrative Review. J. Compos. Sci. 2022, 6, 201. https://doi.org/10.3390/jcs6070201
Dimitrova M, Corsalini M, Kazakova R, Vlahova A, Barile G, Dell’Olio F, Tomova Z, Kazakov S, Capodiferro S. Color Stability Determination of CAD/CAM Milled and 3D Printed Acrylic Resins for Denture Bases: A Narrative Review. Journal of Composites Science. 2022; 6(7):201. https://doi.org/10.3390/jcs6070201
Chicago/Turabian StyleDimitrova, Mariya, Massimo Corsalini, Rada Kazakova, Angelina Vlahova, Giuseppe Barile, Fabio Dell’Olio, Zlatina Tomova, Stoyan Kazakov, and Saverio Capodiferro. 2022. "Color Stability Determination of CAD/CAM Milled and 3D Printed Acrylic Resins for Denture Bases: A Narrative Review" Journal of Composites Science 6, no. 7: 201. https://doi.org/10.3390/jcs6070201
APA StyleDimitrova, M., Corsalini, M., Kazakova, R., Vlahova, A., Barile, G., Dell’Olio, F., Tomova, Z., Kazakov, S., & Capodiferro, S. (2022). Color Stability Determination of CAD/CAM Milled and 3D Printed Acrylic Resins for Denture Bases: A Narrative Review. Journal of Composites Science, 6(7), 201. https://doi.org/10.3390/jcs6070201







