An Opportunity to END TB: Using the Sustainable Development Goals for Action on Socio-Economic Determinants of TB in High Burden Countries in WHO South-East Asia and the Western Pacific Regions
Abstract
1. Introduction
2. TB Burden: Globally and in the WHO South-East Asia and Western Pacific Regions
3. End TB Strategy
Progress towards the 2020 Milestones of the End TB Strategy
4. Factors Influencing the Risk of Exposure to Mycobacterium tuberculosis (Mtb), Infection, the Progression from Infection to Disease and Adverse Treatment Outcomes
- Close contact with a person with infectious TB disease
- Age, sex, tobacco use, alcohol abuse, malnutrition, HIV infection, diabetes mellitus, exposure to indoor air pollution, silicosis, intake of immunosuppressive drugs/medications (e.g., tumor necrosis factor-alpha (TNF) antagonists, corticosteroids)
- Poverty, socio-economic and gender inequality, overcrowding, food and job insecurity, weak health systems
4.1. Relationship between Various Health-Related Risk factors and Major Underlying Socio-Economic Determinants of TB
4.2. Need for Action on Risk Factors and Major Determinants of TB
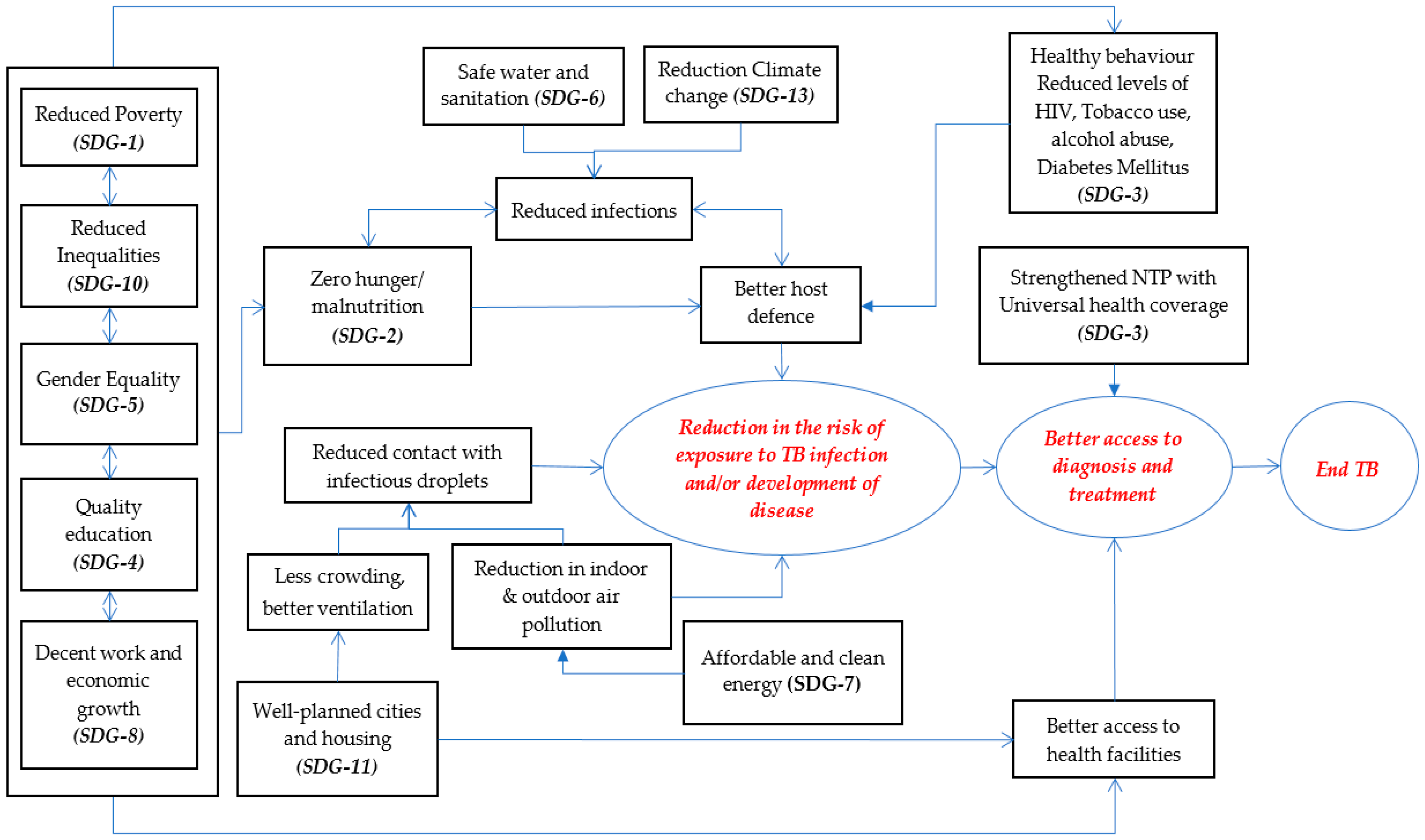
5. Framework for Action on Social Determinants of Tuberculosis: Sustainable Development Goals
- No Poverty
- Zero Hunger
- Good Health and Well-being
- Quality Education
- Gender Equality
- Clean Water and Sanitation
- Affordable and Clean Energy
- Decent Work and Economic Growth
- Industry, Innovation, and Infrastructure
- Reducing Inequality
- Sustainable Cities and Communities
- Responsible Consumption and Production
- Climate Action
- Life Below Water
- Life on Land
- Peace, Justice, and Strong Institutions
- Partnerships for the Goals
5.1. Sustainable Development Goals that Are Likely to Have a Significant Impact on the Burden of TB
5.1.1. SDG Goal 1: No Poverty
5.1.2. SDG Goal 2: Zero Hunger
5.1.3. SDG Goal 3: Good Health and Well Being
5.1.4. SDG Goal 4: Quality Education
5.1.5. SDG Goal 5: Gender Equality
5.1.6. SDG Goal 6: Clean Water and Sanitation
5.1.7. SDG Goal 7: Affordable and Clean Energy
5.1.8. SDG Goal 8: Decent Work and Economic Growth
5.1.9. SDG Goal 10: Reduced Inequalities
5.1.10. SDG Goal 11: Sustainable Cities and Communities
5.1.11. SDG Goal 13: Climate Action
6. Role of National TB Programs in Accelerating the Progress towards Achieving SDGs
- Development of national (and local) strategic and operational plans to end (or eliminate) TB, with a multisectoral perspective involving government and partners, consistent with the End TB Strategy.
- Development and use of a national MAF-TB.
- Establishment, strengthening or maintenance of a national multisectoral mechanism (e.g., inter-ministerial commission), tasked with providing oversight, coordination and a periodic review of the national tuberculosis response.
- Implementation of multisectoral actions on the social determinants of tuberculosis.
- Revisions to plans and policies, and associated activities, based on monitoring, reporting, and recommendations from reviews.
- Seven indicators relevant to TB under SDG 1, 2, 7, 8, 10 and 11 and seven indicators within SDG-3.
- (1)
- SDG 1 (No poverty)—Indicator 1.1.1: Proportion of the population living below the international poverty line
- (2)
- SDG 1 (No poverty)—Indicator 1.3.1: Proportion of the population covered by social protection floors or systems
- (3)
- SDG 2 (Zero hunger)—Indicator 2.1.1: Prevalence of undernourishment
- (4)
- SDG 7 (Affordable and clean energy)—Indicator 7.1.2: Proportion of the population with primary reliance on clean fuels and technology
- (5)
- SDG 8 (Decent work and economic growth)—Indicator: 8.1.1: Gross domestic product (GDP) per capita
- (6)
- SDG 10 (Reduced inequalities)—Indicator: 10.1.1: Gini index for income inequality
- (7)
- SDG 11 (Sustainable Cities and Communities)—Indicator: 11.1.1: Proportion of the urban population living in slums
- B.
- Seven indicators relevant to TB within SDG 3 are as follows:
- (1)
- SDG Indicator 3.8.1: Coverage of essential health services (UHC) measure with an UHC index based essential health services and ranges between 0 and 100
- (2)
- SDG Indicator 3.8.2: Proportion of the population with large household expenditures on health, as a share of total household expenditure or income
- (3)
- SDG Indicator 3.c.1: Current health expenditure per capita in current international dollars
- (4)
- SDG Indicator 3.3.1: Prevalence of HIV
- (5)
- SDG Indicator 3.a.1: Prevalence of smoking
- (6)
- SDG Indicator 3.4.1: Prevalence of diabetes
- (7)
- SDG Indicator 3.5.2: Prevalence of alcohol use disorder
7. Conclusions
Author Contributions
Funding
Conflicts of Interest
Disclaimer
References
- World Health Organisation. The Top 10 Causes of Death. Available online: https://www.who.int/en/news-room/fact-sheets/detail/the-top-10-causes-of-death (accessed on 19 March 2020).
- Pai, M.; Behr, M.A.; Dowdy, D.; Dheda, K.; Divangahi, M.; Boehme, C.C.; Ginsberg, A.; Swaminathan, S.; Spigelman, M.; Getahun, H.; et al. Tuberculosis. Nat. Rev. Dis. Prim. 2016, 2, 16076. [Google Scholar] [CrossRef] [PubMed]
- Behr, M.A.; Edelstein, P.H.; Ramakrishnan, L. Revisiting the timetable of tuberculosis. BMJ 2018, 362, k2738. [Google Scholar] [CrossRef] [PubMed]
- Behr, M.A.; Edelstein, P.H.; Ramakrishnan, L. Is Mycobacterium tuberculosis infection life long? BMJ 2019, 367, l5770. [Google Scholar] [CrossRef] [PubMed]
- Houben, R.M.G.J.; Dodd, P.J. The global burden of latent tuberculosis infection: A re-estimation using mathematical modelling. PLoS Med. 2016, 13, e1002152. [Google Scholar] [CrossRef]
- Global Tuberculosis Report 2019. Available online: https://www.who.int/tb/publications/global_report/en/ (accessed on 19 March 2020).
- Trauer, J.M.; Dodd, P.J.; Gomes, M.G.M.; Gomez, G.B.; Houben, R.M.G.J.; McBryde, E.S.; Melsew, Y.A.; Menzies, N.A.; Arinaminpathy, N.; Shrestha, S. The Importance of Heterogeneity to the Epidemiology of Tuberculosis. Clin. Infect. Dis. 2019, 69, 159–166. [Google Scholar] [CrossRef]
- The End TB Strategy. Available online: https://www.who.int/tb/post2015_strategy/en/ (accessed on 13 June 2020).
- Cadena, A.M.; Fortune, S.M.; Flynn, J.L. Heterogeneity in tuberculosis. Nat. Rev. Immunol. 2017, 17, 691–702. [Google Scholar] [CrossRef] [PubMed]
- Lönnroth, K.; Jaramillo, E.; Williams, B.G.; Dye, C.; Raviglione, M. Drivers of tuberculosis epidemics: The role of risk factors and social determinants. Soc. Sci. Med. 2009, 68, 2240–2246. [Google Scholar] [CrossRef] [PubMed]
- Pedrazzoli, D.; Boccia, D.; Dodd, P.J.; Lönnroth, K.; Dowdy, D.W.; Siroka, A.; Kimerling, M.E.; White, R.G.; Houben, R.M.G.J. Modelling the social and structural determinants of tuberculosis: Opportunities and challenges. Int. J. Tuberc. Lung Dis. 2017, 21, 957–964. [Google Scholar] [CrossRef]
- Avert. HIV and AIDS in the Asia and the Pacific Regional Overview. Available online: https://www.avert.org/professionals/hiv-around-world/asia-pacific/overview (accessed on 11 May 2020).
- Epidemiology of Alcohol Use in the WHO South-East Asia Region. Available online: https://apps.who.int/iris/handle/10665/259831 (accessed on 13 June 2020).
- Hunger Notes. Asia Hunger facts. Available online: https://www.worldhunger.org/asia-hunger-facts-2018/ (accessed on 11 May 2020).
- World Health Statistics Data Visualisation Dashboard: Prevalance of Tobacco Smoking. Available online: https://apps.who.int/gho/data/node.sdg.3-a-viz?lang=en (accessed on 13 June 2020).
- Global Report on Diabetes. Available online: https://apps.who.int/iris/bitstream/handle/10665/204874/WHO_NMH_NVI_16.3_eng.pdf;jsessionid=244DC978B0833D7128BD508B32D46E9A?sequence=1 (accessed on 16 June 2020).
- Lin, H.-H.; Ezzati, M.; Murray, M. Tobacco Smoke, Indoor air pollution and tuberculosis: A systematic review and meta-analysis. PLoS Med. 2007, 4, e20. [Google Scholar] [CrossRef]
- Mansournia, M.A.; Altman, D.G. Population attributable fraction. BMJ 2018, 360, k757. [Google Scholar] [CrossRef]
- Murray, J.F. A Century of Tuberculosis. Am. J. Respir. Crit. Care Med. 2004, 169, 1181–1186. [Google Scholar] [CrossRef] [PubMed]
- Murray, J.F. Tuberculosis and World War I. Am. J. Respir. Crit. Care Med. 2015, 192, 411–414. [Google Scholar] [CrossRef] [PubMed]
- Janssens, J.P.; Rieder, H.L. An ecological analysis of incidence of tuberculosis and per capita gross domestic product. Eur. Respir. J. 2008, 32, 1415–1416. [Google Scholar] [CrossRef] [PubMed]
- Carter, D.J.; Glaziou, P.; Lönnroth, K.; Siroka, A.; Floyd, K.; Weil, D.; Raviglione, M.; Houben, R.M.G.J.; Boccia, D. The impact of social protection and poverty elimination on global tuberculosis incidence: A statistical modelling analysis of Sustainable Development Goal 1. Lancet Glob. Heal. 2018, 6, e514–e522. [Google Scholar] [CrossRef]
- Adler, N.E.; Newman, K. Socioeconomic disparities in health: Pathways and policies. Health Aff. 2002, 21, 60–76. [Google Scholar] [CrossRef] [PubMed]
- Tobacco and Poverty: A Vicious Circle. Available online: https://apps.who.int/iris/handle/10665/68704 (accessed on 16 June 2020).
- Karriker-Jaffe, K.J.; Roberts, S.C.M.; Bond, J. Income inequality, alcohol use, and alcohol-related problems. Am. J. Public Health 2013, 103, 649–656. [Google Scholar] [CrossRef]
- Killewo, J. Poverty, TB, and HIV infection: A vicious cycle. J. Health. Popul. Nutr. 2002, 20, 281–284. [Google Scholar]
- Gaskin, D.J.; Thorpe, R.J.; McGinty, E.E.; Bower, K.; Rohde, C.; Young, J.H.; LaVeist, T.A.; Dubay, L.; Dubay, L. Disparities in diabetes: The nexus of race, poverty, and place. Am. J. Public Health 2014, 104, 2147–2155. [Google Scholar] [CrossRef]
- Agardh, E.; Allebeck, P.; Hallqvist, J.; Moradi, T.; Sidorchuk, A. Type 2 diabetes incidence and socio-economic position: A systematic review and meta-analysis. Int. J. Epidemiol. 2011, 40, 804–818. [Google Scholar] [CrossRef]
- Multisectoral Accountability Framework to Accelerate Progress to End Tuberculosis by 2030; World Health Organisation: Geneva, Switzerland, 3 August 2019.
- MacNeil, A.; Glaziou, P.; Sismanidis, C.; Date, A.; Maloney, S.; Floyd, K. Global Epidemiology of Tuberculosis and Progress Toward Meeting Global Targets—Worldwide, 2018. MMWR. Morb. Mortal. Wkly. Rep. 2020, 69, 281–285. [Google Scholar] [CrossRef]
- Nicola, M.; Alsafi, Z.; Sohrabi, C.; Kerwan, A.; Al-Jabir, A.; Iosifidis, C.; Agha, M.; Agha, R. The Socio-Economic Implications of the Coronavirus and COVID-19 Pandemic: A Review. Int. J. Surg. 2020, 78, 185–193. [Google Scholar] [CrossRef]
- United Nations. Sustainable Development Goals. Available online: https://sustainabledevelopment.un.org/?menu=1300 (accessed on 13 June 2020).
- United Nations. Global indicator framework for the Sustainable Development Goals and targets of the 2030 Agenda for Sustainable Development. Available online: https://unstats.un.org/sdgs/indicators/Global Indicator Framework after 2020 review_Eng.pdf (accessed on 26 March 2020).
- Golden, S.D.; Earp, J.A.L. Social ecological approaches to individuals and their contexts: Twenty years of health education & behavior health promotion interventions. Health Educ. Behav. 2012, 39, 364–372. [Google Scholar] [PubMed]
- Oxlade, O.; Murray, M. Tuberculosis and poverty: Why are the poor at greater risk in India? PLoS One 2012, 7, e47533. [Google Scholar] [CrossRef]
- Stop TB Partnership. What is the Relation between TB and Poverty? Available online: http://www.stoptb.org/assets/documents/events/world_tb_day/2002/1Therelationship.pdf (accessed on 27 March 2020).
- Gupta, K.B.; Gupta, R.; Atreja, A.; Verma, M.; Vishvkarma, S. Tuberculosis and nutrition. Lung India 2009, 26, 9–16. [Google Scholar] [CrossRef]
- Bhargava, A.; Benedetti, A.; Oxlade, O.; Pai, M.; Menzies, D. Undernutrition and the incidence of tuberculosis in India: National and subnational estimates of the population-attributable fraction related to undernutrition. Natl. Med. J. India 2014, 27, 128–133. [Google Scholar]
- Padmapriyadarsini, C.; Shobana, M.; Lakshmi, M.; Beena, T.; Swaminathan, S. Undernutrition & tuberculosis in India: Situation analysis & the way forward. Indian J. Med. Res. 2016, 144, 11–20. [Google Scholar] [PubMed]
- Reid, M.J.A.; Arinaminpathy, N.; Bloom, A.; Bloom, B.R.; Boehme, C.; Chaisson, R.; Chin, D.P.; Churchyard, G.; Cox, H.; Ditiu, L.; et al. Building a tuberculosis-free world: The lancet commission on tuberculosis. Lancet 2019, 393, 1331–1384. [Google Scholar] [CrossRef]
- Hahn, R.A.; Truman, B.I. Education improves public health and promotes health equity. Int. J. Health Serv. 2015, 45, 657–678. [Google Scholar] [CrossRef] [PubMed]
- Cutler, D.M.; Lleras-Muney, A. Understanding differences in health behaviors by education. J. Health Econ. 2010, 29, 1–28. [Google Scholar] [CrossRef]
- Samal, J. Health Seeking Behaviour among Tuberculosis Patients in India: A Systematic Review. J. Clin. Diagn. Res. 2016, 10, LE01. [Google Scholar] [CrossRef]
- Nhamoyebonde, S.; Leslie, A. Biological differences between the sexes and susceptibility to tuberculosis. J. Infect. Dis. 2014, 209, S100–S106. [Google Scholar] [CrossRef] [PubMed]
- Holmes, C.B.; Hausler, H.; Nunn, P. A review of sex differences in the epidemiology of tuberculosis. Int. J. Tuberc. Lung Dis. 1998, 2, 96–104. [Google Scholar] [PubMed]
- Connolly, M.; Nunn, P. Women and tuberculosis. World Health Stat. Q. 1996, 49, 115–119. [Google Scholar] [PubMed]
- Krishnan, L.; Akande, T.; Shankar, A.V.; McIntire, K.N.; Gounder, C.R.; Gupta, A.; Yang, W.-T. Gender-Related Barriers and Delays in Accessing Tuberculosis Diagnostic and Treatment Services: A Systematic Review of Qualitative Studies. Tuberc. Res. Treat. 2014, 2014, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Horton, K.C.; MacPherson, P.; Houben, R.M.G.J.; White, R.G.; Corbett, E.L. Sex Differences in Tuberculosis Burden and Notifications in Low- and Middle-Income Countries: A Systematic Review and Meta-analysis. PLoS Med. 2016. [Google Scholar] [CrossRef]
- Yang, W.-T.; Gounder, C.R.; Akande, T.; De Neve, J.-W.; McIntire, K.N.; Chandrasekhar, A.; de Lima Pereira, A.; Gummadi, N.; Samanta, S.; Gupta, A. Barriers and Delays in Tuberculosis Diagnosis and Treatment Services: Does Gender Matter? Tuberc. Res. Treat. 2014, 2014, 1–15. [Google Scholar] [CrossRef]
- Quansah, R.; Semple, S.; Ochieng, C.A.; Juvekar, S.; Armah, F.A.; Luginaah, I.; Emina, J. Effectiveness of interventions to reduce household air pollution and/or improve health in homes using solid fuel in low-and-middle income countries: A systematic review and meta-analysis. Environ. Int. 2017, 103, 73–90. [Google Scholar] [CrossRef]
- Jafta, N.; Jeena, P.M.; Barregard, L.; Naidoo, R.N. Childhood tuberculosis and exposure to indoor air pollution: A systematic review and meta-analysis. Int. J. Tuberc. Lung Dis. 2015, 19, 596–602. [Google Scholar] [CrossRef]
- Sumpter, C.; Chandramohan, D. Systematic review and meta-analysis of the associations between indoor air pollution and tuberculosis. Trop. Med. Int. Heal. 2013, 18, 101–108. [Google Scholar] [CrossRef]
- Lin, H.-H.; Suk, C.-W.; Lo, H.-L.; Huang, R.-Y.; Enarson, D.A.; Chiang, C.-Y. Indoor air pollution from solid fuel and tuberculosis: A systematic review and meta-analysis. Int. J. Tuberc. Lung Dis. 2014, 18, 613–621. [Google Scholar] [CrossRef]
- Lai, T.C.; Chiang, C.-Y.; Wu, C.-F.; Yang, S.-L.; Liu, D.-P.; Chan, C.-C.; Lin, H.-H. Ambient air pollution and risk of tuberculosis: A cohort study. Occup. Environ. Med. 2016, 73, 56–61. [Google Scholar] [CrossRef]
- Lin, Y.J.; Lin, H.-C.; Yang, Y.-F.; Chen, C.-Y.; Ling, M.-P.; Chen, S.-C.; Chen, W.-Y.; You, S.-H.; Lu, T.-H.; Liao, C.-M. Association between ambient air pollution and elevated risk of tuberculosis development. Infect. Drug Resist. 2019, 12, 3835–3847. [Google Scholar] [CrossRef] [PubMed]
- Donald, P.R.; Marais, B.J.; Barry, C.E. Age and the epidemiology and pathogenesis of tuberculosis. Lancet 2010, 375, 1852–1854. [Google Scholar] [CrossRef]
- Maher, D.; Boldrini, F.; Alli, B.O.; Gabriel, P.; Kisting, S.; Norval, P.-Y. Guidelines for workplace TB control activities the contribution of workplace TB control activities to TB control in the community. Available online: http://www.stoptb.org/assets/documents/resources/publications/technical/workplace_guidelines.pdf (accessed on 27 March 2020).
- Heymann, J.; Rho, H.J.; Schmitt, J.; Earle, A. Ensuring a healthy and productive workforce: Comparing the generosity of paid sick day and sick leave policies in 22 countries. Int. J. Health Serv. 2010, 40, 1–22. [Google Scholar] [CrossRef]
- Asfaw, A.; Pana-Cryan, R.; Rosa, R. Paid sick leave and nonfatal occupational injuries. Am. J. Public Health 2012, 102, e59–e64. [Google Scholar] [CrossRef] [PubMed]
- Kim, D. Paid Sick Leave and Risks of All-Cause and Cause-Specific Mortality among Adult Workers in the USA. Int. J. Environ. Res. Public Health 2017, 14, 1247. [Google Scholar] [CrossRef]
- Duarte, R.; Lönnroth, K.; Carvalho, C.; Lima, F.; Carvalho, A.C.C.; Muñoz-Torrico, M.; Centis, R. Tuberculosis, social determinants and co-morbidities (including HIV). Pulmonology 2018, 24, 115–119. [Google Scholar] [CrossRef]
- Reyes, R.; Ahn, R.; Thurber, K.; Burke, T.F. Urbanization and Infectious Diseases: General Principles, Historical Perspectives, and Contemporary Challenges. In Challenges in Infectious Diseases; Springer New York: New York, NY, USA, 2013; pp. 123–146. [Google Scholar]
- Prasad, A.; Ross, A.; Rosenberg, P.; Dye, C. A world of cities and the end of TB. Trans. R. Soc. Trop. Med. Hyg. 2016, 110, 151–152. [Google Scholar] [CrossRef][Green Version]
- Nardell, E.; Lederer, P.; Mishra, H.; Nathavitharana, R.; Theron, G. Cool but dangerous: How climate change is increasing the risk of airborne infections. Indoor Air 2020, 30, 195–197. [Google Scholar] [CrossRef]
- Harries, A.D. Chronic kidney disease, tuberculosis and climate change. Int. J. Tuberc. Lung Dis. 2020, 24, 132–133. [Google Scholar] [CrossRef]
- WHO Global TB Report App launched. Available online: https://www.who.int/tb/features_archive/TB-report-App/en/ (accessed on 11 June 2020).
- Tuberculosis Country Profiles. Available online: https://www.who.int/tb/country/data/profiles/en/ (accessed on 11 June 2020).
- Measuring progress towards the Sustainable Development Goals - SDG Tracker. Available online: https://sdg-tracker.org/ (accessed on 27 March 2020).
- Pradhan Mantri Kaushal Vikas Yojana (PMKVY). Available online: https://pmkvyofficial.org/ (accessed on 11 May 2020).
- Mahatma Gandhi National Rural Employment Gurantee Act. Available online: https://nrega.nic.in/netnrega/home.aspx (accessed on 11 May 2020).
- Pradhan Mantri Ujjwala Yojana. Available online: https://pmuy.gov.in/ (accessed on 11 May 2020).
- Ministry of Skill Development and Entrepreneurship. Available online: https://www.msde.gov.in/proposed-scheme.html (accessed on 11 May 2020).
- Pradhan Mantri Jan-Dhan Yojana, Ministry of Finance, Government of India. Available online: https://www.pmjdy.gov.in/scheme (accessed on 11 May 2020).
- Jawaharlal Nehru National Urban Renewal Mission: Ministry of Housing and Urban Affairs, Goverment of India. Available online: http://mohua.gov.in/cms/jawaharlal-nehru-national-urban-renewal-mission.php (accessed on 11 May 2020).
- School Education, Government of India, Ministry of Human Resource Development. Available online: https://mhrd.gov.in/mid-day-meal (accessed on 11 May 2020).
- Samagra Shiksha. Available online: http://samagra.mhrd.gov.in/ (accessed on 11 May 2020).
- Beti Bachao Beti Padhao, Ministry of Women & Child Development, Government of India. Available online: https://wcd.nic.in/bbbp-schemes (accessed on 11 May 2020).
- Governement of India. Ministry of Women and Child Development, Revised Guidelines and Application Format on Support to Training and Employment Programmer for Women (STEP) 2009. Available online: https://wcd.nic.in/sites/default/files/Revised scheme of STEP_0.pdf (accessed on 11 May 2020).
- Ministry of Women & Child Development. Available online: http://mahilaehaat-rmk.gov.in/en/ (accessed on 11 May 2020).
- Swachh Bharat Mission-Gramin. Available online: https://sbm.gov.in/sbmReport/home.aspx (accessed on 11 May 2020).
- National Water and Sanitation Programmer, Ministry of Environment & Forest, Govt. of India. Available online: http://www.sulabhenvis.nic.in/Database/NationalWater_176.aspx (accessed on 11 May 2020).
- National Rural Drinking Water Programmer. Available online: https://www.prsindia.org/content/national-rural-drinking-water-programme-22 (accessed on 16 May 2020).
- Jawaharlal Nehru National Solar Mission. Available online: https://vikaspedia.in/energy/policy-support/renewable-energy-1/solar-energy/jawaharlal-nehru-national-solar-mission (accessed on 1 June 2020).
- National Afforestation Programmer, Ministry of Environment and Forests, Government of India. Available online: http://www.naeb.nic.in/documents/NAP_intro.htm (accessed on 31 May 2020).
| Country | Annual TB Incidence in Thousands (Uncertainty Intervals) | The Approximate Annual Number of TB Deaths in Thousands (Best Estimates) |
|---|---|---|
| Bangladesh | 357 (260–469) | 47.2 |
| Cambodia | 49 (27–77) | 6.7 |
| China | 866 (740–1000) | 39.4 |
| DPR Korea | 131 (114–149) | 20.0 |
| India | 2690 (1840–3700) | 449.7 |
| Indonesia | 845 (770–923) | 98.3 |
| Myanmar | 181 (119–256) | 24.7 |
| Papua New Guinea | 37 (30–45) | 4.7 |
| Philippines | 591 (332–924) | 26.6 |
| Thailand | 106 (81–136) | 11.5 |
| Vietnam | 174 (111–251) | 13.2 |
| Country | TB Incidence Rate (Per 100,000 Population) | Number of TB Deaths (in Thousands) | Proportion of TB Patients Experiencing Catastrophic Costs (in 2018) | ||||
|---|---|---|---|---|---|---|---|
| 2015 | 2018 | Reduction * | 2015 | 2018 | Reduction * | ||
| Bangladesh | 221 | 221 | 0% | 66.0 | 47.0 | 29% | NA |
| Cambodia | 367 | 302 | 18% | 3.8 | 3.4 | 11% | NA |
| China | 65 | 61 | 6% | 43.0 | 40.0 | 7% | NA |
| DPR Korea | 513 | 513 | 0% | 10.0 | 20.0 | −100% | NA |
| India | 217 | 199 | 8% | 470.0 | 449.0 | 4% | NA |
| Indonesia | 325 | 316 | 3% | 102.0 | 98.0 | 4% | NA |
| Myanmar | 391 | 338 | 14% | 36.0 | 25.0 | 31% | NA |
| Papua New Guinea | 432 | 432 | 0% | 4.3 | 4.7 | −9% | NA |
| Philippines | 550 | 554 | −1% | 28.0 | 26.0 | 7% | NA |
| Thailand | 163 | 153 | 6% | 15.0 | 11.0 | 27% | NA |
| Vietnam | 199 | 182 | 9% | 17.0 | 13.0 | 24% | NA |
| Risk Factor | Relative Risk of TB (95% Confidence Intervals) * | Estimated Prevalence of Risk Factor in the South-East Asia and Pacific Region ** | Estimated Population Attributable Fraction (PAF) *** |
|---|---|---|---|
| HIV | 19 (16–22) | 0.2% [12] | 3.5% (2.9–4.0%) |
| Alcohol abuse | 3.3 (2.1–5.2) | 13.5% [13] | 23.7% (12.9–36.2%) |
| Undernourishment | 3.2 (3.1–3.3) | 11.5% [14] | 20.2% (19.5–20.9%) |
| Smoking | 1.6 (1.2–2.1) | 24.8% [15] | 13.0% (4.7–21.4%) |
| Diabetes Mellitus | 1.5 (1.3–1.8) | 8.6% [16] | 4.1% (2.5–6.4%) |
| Indoor Air Pollution | 2.0 (1.2–3.2) | 38.6% [17] | 27.8% (7.2–45.9%) |
| Country | SDG Indicators | ||||||
|---|---|---|---|---|---|---|---|
| 1.1.1 Proportion of the Population Living below the International Poverty Line | 1.3.1 Proportion of the Population Covered by Social Protection Floors or Systems | 2.1.1 Prevalence of Undernourishment | 7.1.2 Proportion of the Population with Primary Reliance on Clean Fuels and Technology | 8.1.1 Gross Domestic Product (GDP) Per Capita, PPP (Constant 2011 International Dollars) | 10.1.1 Gini Index for Income Inequality * | 11.1.1 Proportion of the Urban Population Living in Slums | |
| Bangladesh | 15% | 18% | 15% | 18% | 3500 | 32 | 55% |
| Cambodia | NA | 3.1% | 18% | 18% | 3700 | NA | 55% |
| China | 0.7% | 63% | 8.7% | 59% | 15,300 | 39 | 25% |
| DPR Korea | NA | NA | 43% | 11% | NA | NA | NA |
| India | 21% | 30% | 15% | 41% | 6500 | 36 | 24% |
| Indonesia | 5.7% | 57% | 7.7% | 58% | 11,200 | 38 | 22% |
| Myanmar | 6.4% | 2.3% | 10% | 18% | 5600 | 38 | 41% |
| Papua New Guinea | 38% | 4.2% | NA | 13% | 3800 | 48 | NA |
| Philippines | NA | 41% | 14% | 43% | 7600 | 40 | 38% |
| Thailand | 0% | 79% | 9% | 74% | 16,300 | 36 | 25% |
| Vietnam | 2% | 35% | 11% | 67% | 6200 | 35 | 27% |
| Country | SDG-3 Indicators | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|
| 3.8.1 Coverage of Essential Health Services (UHC) Measure with an UHC Index Based Essential Health Services and Ranges between 0 and 100 | 3.8.2 Proportion of the Population with Large Household Expenditures on Health as a Share of Total Household Expenditure or Income | 3.c.1 Current Health Expenditure Per Capita in Current International Dollars | 3.3.1 Prevalence of HIV | 3.a.1 Prevalence of Smoking | 3.4.1 Prevalence of Diabetes | 3.5.2 Prevalence of Alcohol Use Disorder | ||||
| Male | Female | Male | Female | Male | Female | |||||
| Bangladesh | 48 | 25% | 91 | 0.1% | 45% | 1% | 10% | 9.3% | 1.4% | 0.3% |
| Cambodia | 60 | 15% | 229 | 0.5% | 34% | 2% | 7.4% | 6.9% | 8.7% | 1.8% |
| China | 79 | 20% | 761 | NA | 48% | 1.9% | 9.9% | 7.6% | 8.4% | 0.2% |
| DPR Korea | 71 | NA | NA | NA | NA | NA | 5.8% | 5.9% | 6.2% | 1.0% |
| India | 55 | 17% | 241 | 0.2% | 21% | 1.9% | 9.1% | 8.3% | 9.1% | 0.5% |
| Indonesia | 57 | 2.7% | 363 | 0.4% | 76% | 2.8% | 7.6% | 8.0% | 1.4% | 0.3% |
| Myanmar | 61 | 14% | 291 | 0.7% | 35% | 6.3% | 6.9% | 7.9% | 3.2% | 0.6% |
| Papua New Guinea | 40 | NA | 92 | 0.9% | 49% | 24% | 15% | 14% | 8.8% | 1.8% |
| Philippines | 61 | 6.3% | 342 | 0.1% | 41% | 7.8% | 7.1% | 7.3% | 8.8% | 1.8% |
| Thailand | 80 | 2.2% | 635 | 1.1% | 39% | 1.9% | 8.3% | 8.8% | 10% | 0.9% |
| Vietnam | 75 | 9.4% | 356 | 0.3% | 46% | 1.0% | 5.5% | 5.1% | 9.8% | 1.2% |
| Determinant of TB | Sample Community Level Policies/Interventions to Address the Determinant | Example: Public Programs in India that Can Be Galvanized to Address the Determinant at the Local Level |
|---|---|---|
| To reduce poverty (SDG-1) |
| |
| To reduce hunger (SDG-2) |
|
|
| Improve the quality of education (SDG-4) |
|
|
| Gender equality (SDG-5) |
|
|
| Clean water and sanitation (SDG-6) |
|
|
| Affordable and clean energy (SDG-7) |
|
|
| Decent work and economic growth (SDG-8) |
| |
| Reduced inequalities (SDG-10) |
|
|
| Sustainable cities and communities (SDG-11) |
|
|
| Climate action (SDG-13) |
|
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Satyanarayana, S.; Thekkur, P.; Kumar, A.M.V.; Lin, Y.; Dlodlo, R.A.; Khogali, M.; Zachariah, R.; Harries, A.D. An Opportunity to END TB: Using the Sustainable Development Goals for Action on Socio-Economic Determinants of TB in High Burden Countries in WHO South-East Asia and the Western Pacific Regions. Trop. Med. Infect. Dis. 2020, 5, 101. https://doi.org/10.3390/tropicalmed5020101
Satyanarayana S, Thekkur P, Kumar AMV, Lin Y, Dlodlo RA, Khogali M, Zachariah R, Harries AD. An Opportunity to END TB: Using the Sustainable Development Goals for Action on Socio-Economic Determinants of TB in High Burden Countries in WHO South-East Asia and the Western Pacific Regions. Tropical Medicine and Infectious Disease. 2020; 5(2):101. https://doi.org/10.3390/tropicalmed5020101
Chicago/Turabian StyleSatyanarayana, Srinath, Pruthu Thekkur, Ajay M. V. Kumar, Yan Lin, Riitta A. Dlodlo, Mohammed Khogali, Rony Zachariah, and Anthony David Harries. 2020. "An Opportunity to END TB: Using the Sustainable Development Goals for Action on Socio-Economic Determinants of TB in High Burden Countries in WHO South-East Asia and the Western Pacific Regions" Tropical Medicine and Infectious Disease 5, no. 2: 101. https://doi.org/10.3390/tropicalmed5020101
APA StyleSatyanarayana, S., Thekkur, P., Kumar, A. M. V., Lin, Y., Dlodlo, R. A., Khogali, M., Zachariah, R., & Harries, A. D. (2020). An Opportunity to END TB: Using the Sustainable Development Goals for Action on Socio-Economic Determinants of TB in High Burden Countries in WHO South-East Asia and the Western Pacific Regions. Tropical Medicine and Infectious Disease, 5(2), 101. https://doi.org/10.3390/tropicalmed5020101







