Cushing Syndrome due to Inappropriate Corticosteroid Topical Treatment of Undiagnosed Scabies
Abstract
:1. Introduction
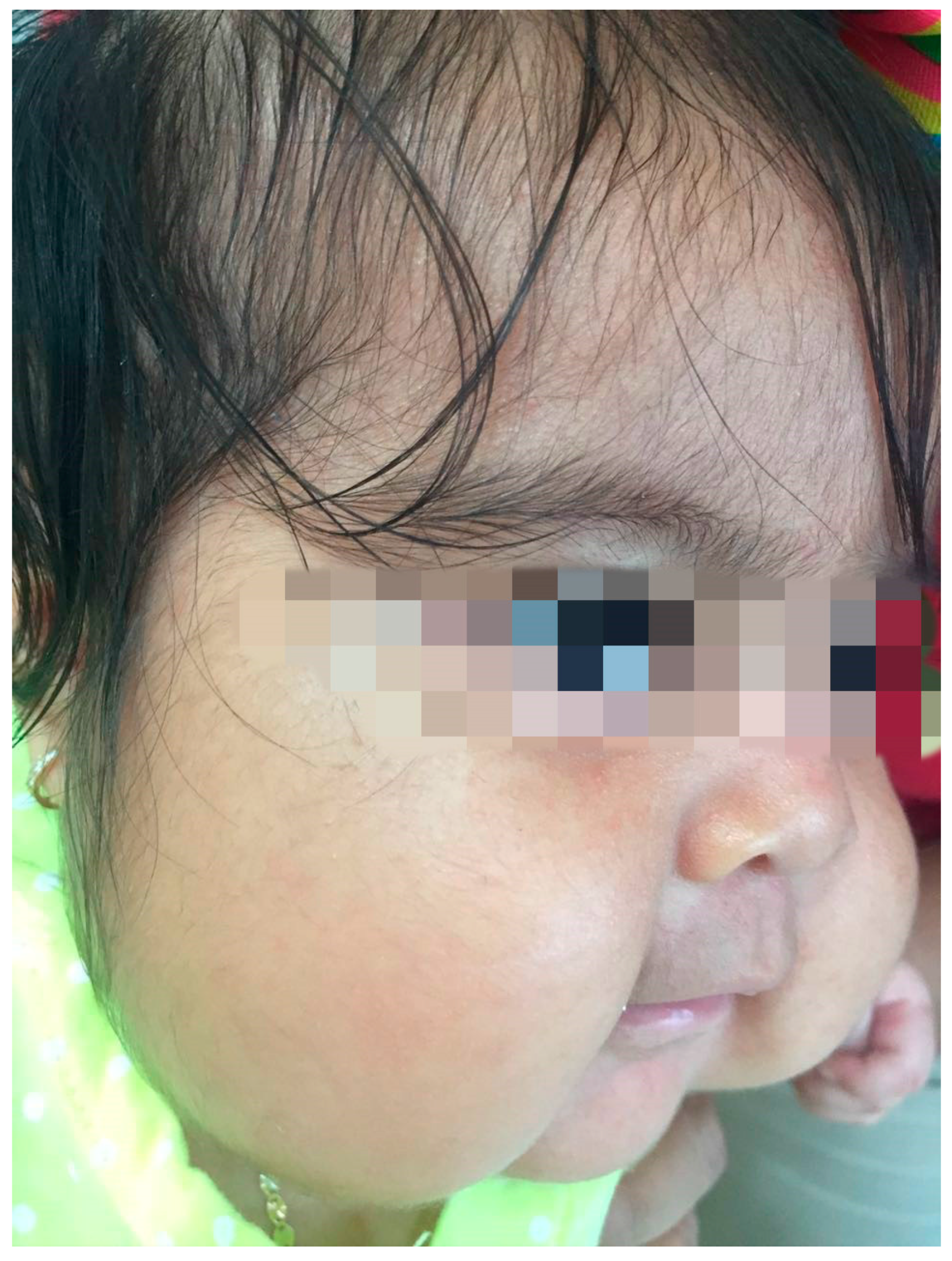
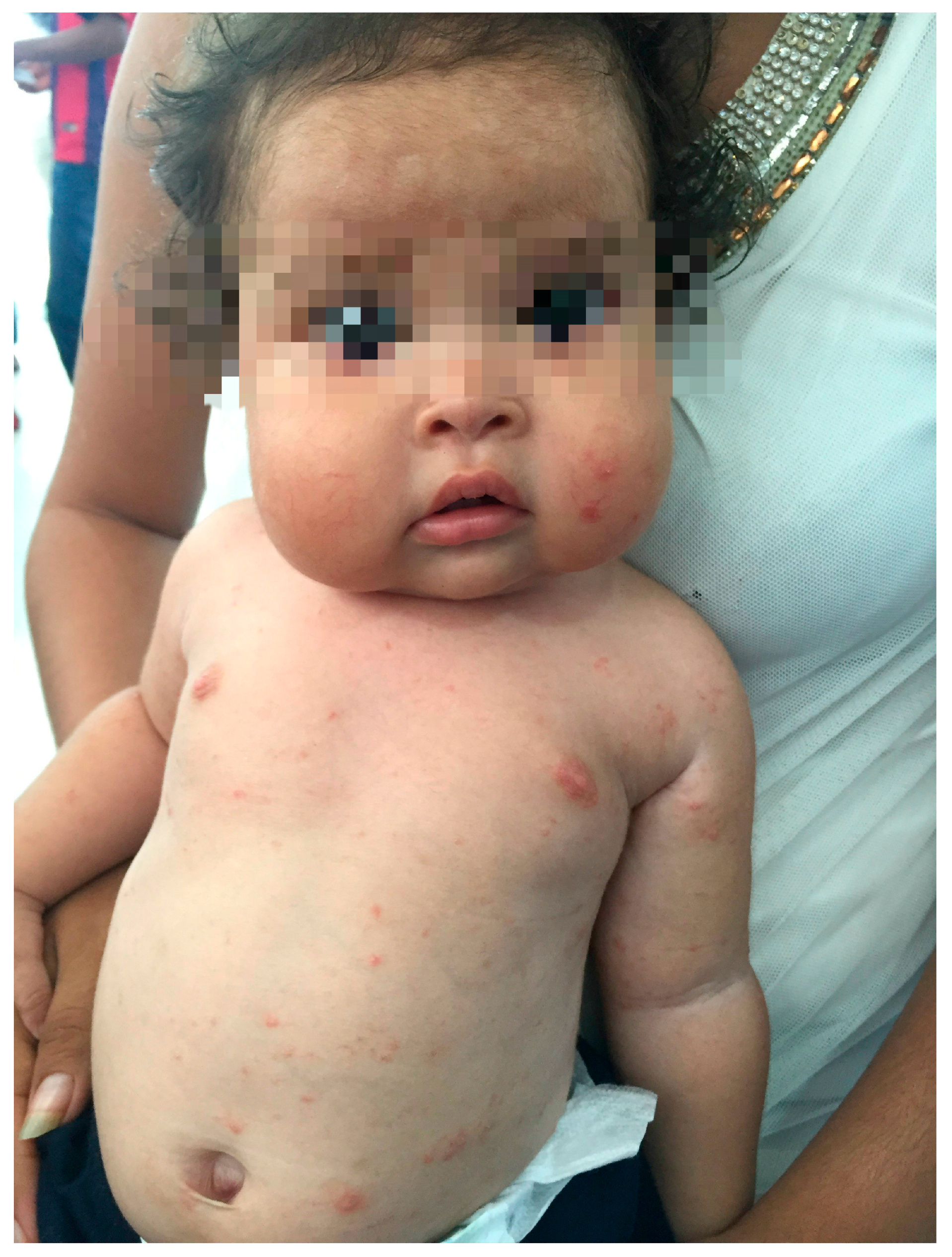
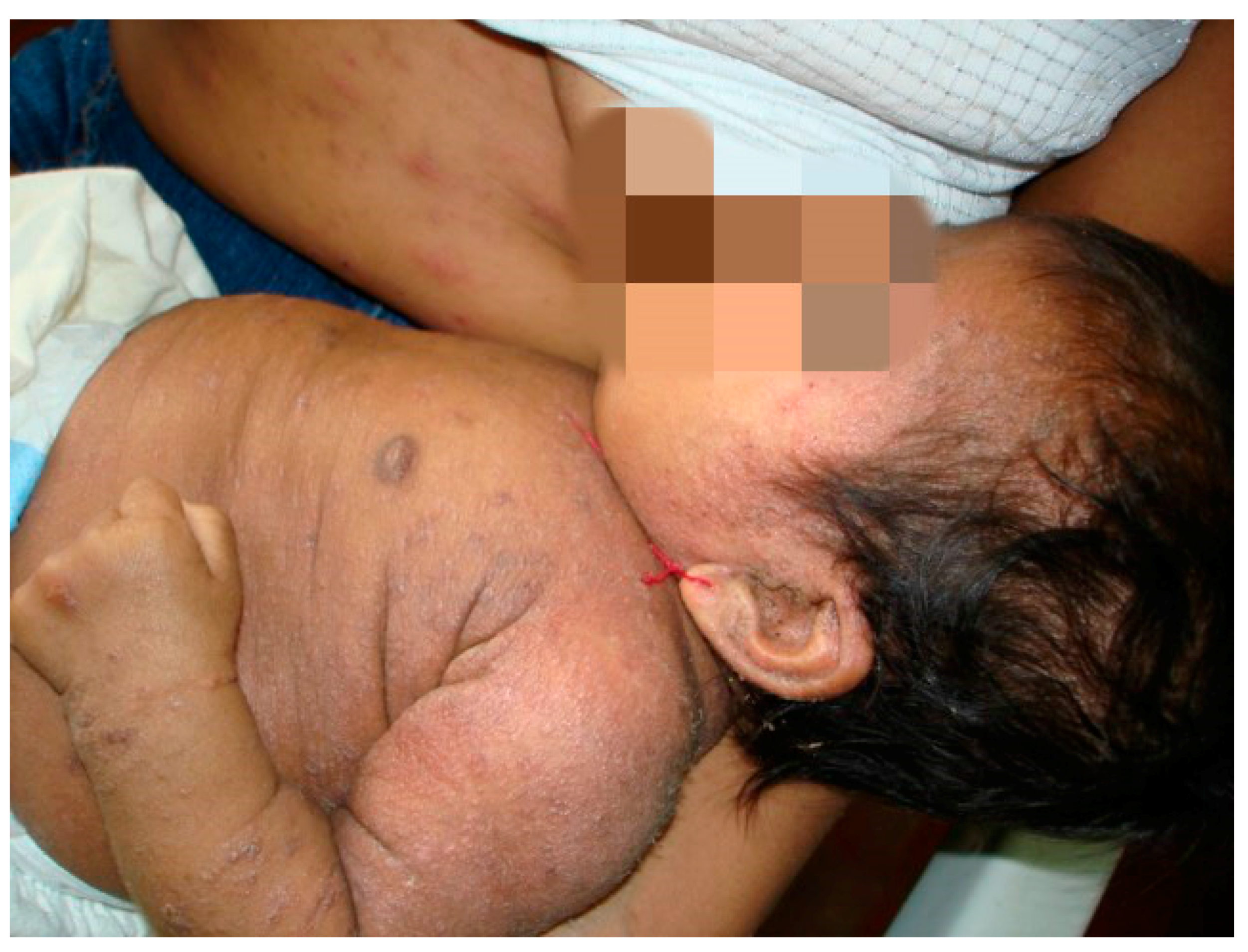
2. Case Series
3. Discussion
4. Ethical Considerations
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Age (Months) | Sex | Topical Steroid Treatment | Clinical Features | |||||
|---|---|---|---|---|---|---|---|---|
| Usage Duration | Frequency | Regularity | Adiposity | Scabies | Symptom Duration | |||
| 1 | 5 | Female | 1 month | 4 times a day | Continuous | +++ | Crusted | 1 month |
| 2 | 6 | Female | 5 months | 1–2 times a day | Intermittent | +++ | Common | 6 months |
| 3 | 7 | Male | 3 months | 2 times a day | Continuous | ++++ | Common | 3 months |
| 4 | 7 | Male | 2 months | 2–3 times a day | Intermittent | +++ | Common | 7 months |
| 5 | 8 | Male | 8 months | Daily | Continuous | ++++ | Crusted | 8 months |
| 6 | 9 | Female | 1 month | 3 times a day | Continuous | ++++ | Common | 6 months |
| 7 | 16 | Male | 5 months | Daily | Continuous | ++ | Common | 6 months |
| 8 | 17 | Female | 4 months | 1–2 times a day | Discontinuous | ++ | Common | 3 months |
References
- Karimkhani, C.; Colombara, D.; Drucker, A.M.; Hay, R.; Engelman, D.; Steer, A.; Whitfield, M.; Naghavi, M.; Dellavalle, R.P. The global burden of scabies: A cross-sectional analysis from the Global Burden of Disease Study 2015. Lancet Inf. Dis. 2017, 17, 1247–1254. [Google Scholar] [CrossRef]
- Mahe, A. Epidemiology and Management of Common Skin Diseases in Children in Developing Countries. Available online: http://whqlibdoc.who.int/hq/2005/WHO_FCH_CAH_05.12_eng.pdf (accessed on 24 July 2018).
- Romani, L.; Steer, A.C.; Whitfield, M.J.; Kaldor, J.M. Prevalence of Scabies and impetigo worldwide: A systematic review. Lancet Infect. Dis. 2015, 15, 960–967. [Google Scholar] [CrossRef]
- Uriostegui-Flores, A. Cultural specific syndromes treated by traditional doctors. Rev. Salud Publica 2015, 17, 277–288. [Google Scholar] [PubMed]
- Verma, S.B.; Vasani, R. Male genital dermatophytosis- clinical features and the effects of the misuse of topical steroids and steroid combinations- an alarming problem in India. Mycoses 2016, 59, 606–614. [Google Scholar] [CrossRef] [PubMed]
- Estrada-Chavez, G.; Estrada, R.; Chavez-López, G. Misuse of topical steroids in scabies. Comm. Dermatol. J. 2017, 13, 1–12. [Google Scholar]
- Miller, W.L. The adrenal cortex and its disorders. In Clinical Pediatric Endocrinology, 4th ed.; Hindmarsh, P.C., Ed.; Oxford Blackwell Science: Oxford, UK, 2001; pp. 321–376. [Google Scholar]
- Semiz, S.; Balci, Y.I.; Ergin, S.; Candemir, M.; Polat, A. Two cases of Cushing‘s syndrome due to overuse of topical steroid in the diaper area. Pediatr. Dermatol. 2008, 25, 544–547. [Google Scholar] [CrossRef] [PubMed]
- Cómo Utilizar esta Herramienta. Available online: www.profeco.gob.mx/precios/canasta/home.aspx?th=1 (accessed on 23 February 2018).
- Hay, R.J.; Steer, A.C.; Engelman, D.; Walton, S. Scabies in the developing world-its prevalence, complications and management. Clin. Microbiol. Infect. 2012, 18, 313–323. [Google Scholar] [CrossRef] [PubMed]
- La-Vincente, S.; Kearns, T.; Connors, C.; Cameron, S.; Carapetis, J.; Andrews, R. Community management of endemic scabies in remote aboriginal communities of northern Australia: Low treatment uptake and high ongoing acquisition. PLoS Negl. Trop. Dis. 2009, 26, e444. [Google Scholar] [CrossRef] [PubMed]
- Engelman, D.; Kiang, K.; Chosidow, O.; McCarthy, J.; Fuller, C.; Lammie, P.; Hay, R.; Steer, A. Members of The International Alliance For The Control of Scabies. PLoS Negl. Trop. Dis. 2013, 7, e2167. [Google Scholar]
- Hay, R.J.; Johns, N.E.; Williams, H.C.; Bolliger, I.W.; Dellavalle, R.P.; Margolis, D.J.; Marks, R.; Naldi, L.; Weinstock, M.A.; Wulf, S.K.; et al. The global burden of skin disease in 2010: An analysis of the prevalence and impact of skin conditions. J. Investig. Derm. 2014, 134, 1527–1534. [Google Scholar] [CrossRef] [PubMed]
- Razzaghy, A.M.; Mosalla, N.A.; Nasli, E.E. Iatrogenic Cushing’s Syndrome caused by topical corticosteroid application and its life threatening complications. J. Compr. Ped. 2015, 6, e34336. [Google Scholar] [CrossRef]
- Lima, F.C.D.R.; Cerqueira, A.M.M.; Guimaraes, M.B.S.; Padilha, C.B.S.; Craide, F.H.; Bombardelli, M. Crusted scabies due to indiscriminate use of glucocorticoid therapy in infant. Ann. Bras. Dermatol. 2017, 92, 383–385. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Dlova, N.C.; Hendricks, N.E.; Martincgh, B.S. Skin-lightening creams used in Durban, South Africa. I. J. Dermatol. 2012, 51 (Suppl 1), 51–53. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Hay, R.J.; Estrada Castanon, R.; Alarcon Hernandez, H.; Chavez Lopez, G.; Lopez Fuentes, L.F.; Paredes Solis, S.; Andersson, N. Wastage of family income on skin disease in Mexico. BMJ 1994, 309, 848. [Google Scholar] [CrossRef] [PubMed]
- Boscaro, M.; Giacchetti, G.; Ronconi, V. Visceral adipose tissue: Emerging role of gluco- and mineralocorticoid hormones in the setting of cardiometabolic alterations. Ann. N. Y. Acad. Sci. 2012, 1264, 87–102. [Google Scholar] [CrossRef] [PubMed]
- Rathi, S.K.; D’Souza, P. Rational and ethical use of topical corticosteroids based on safety and efficacy. Indian J. Dermatol. 2012, 57, 251–259. [Google Scholar] [CrossRef] [PubMed]
- Tempark, T.; Phatarakijnirund, V.; Chatproedprai, S.; Watcharasindhu, S.; Supornsilchai, V.; Wananukul, S. Exogenous Cushing’s syndrome due to topical corticosteroid application: Case report and review literature. Endocrine 2010, 38, 328–334. [Google Scholar] [CrossRef] [PubMed]
- Gen, R.; Akbay, E.; Sezer, K. Cushing syndrome caused by topical corticosteroid: A case report. Am. J. Med. Sci. 2007, 333, 173–174. [Google Scholar] [CrossRef] [PubMed]
- Selahattin, K.; Sedat, A.; Özbek, M.N.; Ahmet, Y. Infantile Iatrogenic Cushing’s Syndrome. Indian J. Dermatol. 2008, 53, 190–191. [Google Scholar]
- Messina, M.F.; Valenzise, M.; Aversa, S.; Arrigo, T.; De-Luca, F. Iatrogenic Cushing syndrome caused by ocular glucocorticoids in a child. BMJ Case Rep. 2009. [Google Scholar] [CrossRef] [PubMed]
- West, D.P.; Micali, G. Principles of paediatric dermatological therapy. In Textbook of Pediatric Dermatology, 1st ed.; Harper, J., Oranje, A., Prose, N., Eds.; Blackwell Science Ltd: Oxford, UK, 2000; pp. 1731–1742. [Google Scholar]
- Siklar, Z.; Bostancı, İ.; Atli, Ö.; Dallar, Y. An infantile Cushing syndrome due to misuse of tropical steroid. Pediatr. Dermatol. 2004, 21, 561–563. [Google Scholar] [CrossRef] [PubMed]
- Azizi, F.; Jahed, A.; Hedayati, M.; Lankarani, M.; Bejestani, H.S.; Esfahanian, F.; Beyraghi, N.; Noroozi, A.; Kobarfard, F. Outbreak of exogenous Cushing’s syndrome due to unlicensed medications. Clin. Endocrinol. 2008, 69, 921–925. [Google Scholar] [CrossRef] [PubMed]
- Thomas, J.; Carson, C.; Peterson, G.M.; Walton, S.F.; Hammer, K.A.; Naunton, M.; Davey, R.C.; Spelman, T.; Dettwiller, P.; Kyle, G.; et al. Therapeutic potential of tea tree oil for scabies. Am. J. Trop. Med. Hyg. 2016, 94, 258–266. [Google Scholar] [CrossRef] [PubMed]
- Hay, R.J.; Fuller, L.C. The assessment of dermatological needs in resource-poor regions. Int. J. Dermatol. 2012, 50, 552–557. [Google Scholar] [CrossRef] [PubMed]
- Estrada, R.; Chavez-López, M.G.; Estrada-Chavez, G.; Paredes-Solis, S. specialized dermatological care for marginalized populations and education at the primary care level: Is community dermatology a feasible proposal? Int. J. Dermatol. 2012, 51, 1345–1350. [Google Scholar] [CrossRef] [PubMed]
- Estrada-Chavez, G.E.; Estrada, C.R.; Chavez, L.G.; Paredes-Solis, S. Estudio preliminar de la prescripción indiscriminada de corticosteroides tópicos en medicina general. Dermatol. Rev. Mex. 2013, 57, 433–437. [Google Scholar]
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Estrada-Chávez, G.; Estrada, R.; Engelman, D.; Molina, J.; Chávez-López, G. Cushing Syndrome due to Inappropriate Corticosteroid Topical Treatment of Undiagnosed Scabies. Trop. Med. Infect. Dis. 2018, 3, 82. https://doi.org/10.3390/tropicalmed3030082
Estrada-Chávez G, Estrada R, Engelman D, Molina J, Chávez-López G. Cushing Syndrome due to Inappropriate Corticosteroid Topical Treatment of Undiagnosed Scabies. Tropical Medicine and Infectious Disease. 2018; 3(3):82. https://doi.org/10.3390/tropicalmed3030082
Chicago/Turabian StyleEstrada-Chávez, Guadalupe, Roberto Estrada, Daniel Engelman, Jesus Molina, and Guadalupe Chávez-López. 2018. "Cushing Syndrome due to Inappropriate Corticosteroid Topical Treatment of Undiagnosed Scabies" Tropical Medicine and Infectious Disease 3, no. 3: 82. https://doi.org/10.3390/tropicalmed3030082





