1. Introduction
In recent years, the fragility and vulnerability of basic services around the globe has been revealed. This phenomenon has been particularly evident in the context of healthcare infrastructure and services, which has been the focus of particular attention since the COVID-19 pandemic began. Many countries have faced severe shortcomings with the preparedness of their health services, including the stocking of personal protective equipment. Additionally, the operability of basic services has been altered by the pandemic, including the disruption of public transport which has impacted the ability of staff to commute, the closure of nurseries and schools, and on staff availability.
However, despite the negative conditions brought about by the COVID-19 pandemic, adverse events in countries with strong healthcare systems have shown that healthcare security is not as good as expected. Natural hazards such as floods and storms have severe impacts on critical health infrastructure, limiting their availability at times when their services are particularly needed. For instance, Hurricanes Katrina (2005), Maria (2017), and Ida (2021) severely disrupted healthcare facilities in the US and the Caribbean [
1]. Similarly, the 2021 flood across Germany and portions of Western Europe led to the ongoing impairment of health services in the affected areas [
2]. Two aspects regarding preparedness stand out in particular. First, cascading impacts from impairments or outages of infrastructures are considered only selectively. Although there are often legal requirements for the installation of an emergency power supply [
3], this does not apply to other infrastructure necessary for the functioning of critical health infrastructure systems, including water supply and sanitation. This is particularly critical in countries characterized as having normally well-functioning piped water supplies [
4], and which, therefore, rarely operate on stockpiled reserves. Secondly, organizational and individual aspects such as communication, awareness and learning from past events are underutilized. This paper therefore addresses both factors by analyzing compound impacts of water supply failures in healthcare facilities and resulting organizational challenges to overcome them.
Both policy and research advocate for building resilient infrastructure at a conceptual level; however, there are different understandings of resilience and what it entails. Overall, critical infrastructure literature identifies technical, social, organizational, environmental, and economic dimensions of critical infrastructure resilience [
5,
6,
7]. What has become clear above all is that health infrastructure resilience is not synonymous with functioning technology or the time needed to repair disrupted devices and services. Nevertheless, the technical understanding is still the predominant view on building resilience in this field. Recent research on hospitals and health infrastructure resilience, e.g., deals with structural and internal safety in general [
8]; resilience in the context of COVID-19 [
9,
10]; cyber-attacks [
11,
12]; various natural hazards, including earthquakes [
13,
14], hurricanes [
15], and wildfires [
16]; or specific settings such as urban areas [
17]. It is striking that comparably little research focuses on a broader, more holistic understanding of health infrastructure systems, hospital resilience, or the contribution of health infrastructure resilience to overall societal resilience. Economic aspects are similarly overlooked and are not addressed further in the context of this paper. The economic functionality of hospitals and larger health infrastructures differ fundamentally across countries and hence are not comparable. Overall, the literature remains siloed, by primarily looking at structural supply, or, in some individual cases, organizational aspects. The few papers available that discuss these aspects more broadly [
18,
19,
20,
21] list these categories largely in parallel without appreciating the interlinkages and resulting consequences of overall resilience on healthcare infrastructure.
Reality has shown that an underestimation of the complexity of these aspects can even lead to serious dysfunctions. There is an urgent need to critically investigate whether a solely technical or engineering approach to critical infrastructure resilience is the best strategy to protect essential service delivery. The concept of resilience has already undergone several paradigm shifts in other scientific disciplines and is no longer based exclusively on a technical understanding. However, this paradigm shift does not yet seem to have reached the field of critical health infrastructure. Therefore, a closer look at resilience discourses and the potential benefits of integrated strategies in the context of health infrastructure is necessary to develop more effective approaches and a way forward.
2. Background: The Notion of Resilience
Resilience is an increasingly popular concept in various academic disciplines, such as natural, social, and engineering sciences, and including critical infrastructure research. The broad application of the concept in various disciplines has led to variable resilience approaches and conceptualizations, resulting in a lack of consensus on what resilience entails and how it is defined. There are a variety of established resilience conceptualizations, ranging from the technical resilience perspective (also referred to as engineering resilience), to ecological, or social resilience, and finally the social-ecological resilience perspective.
Despite the fact that a multitude of resilience definitions exist, the technical resilience understanding is most widely used for both academic and practical application. For example, in the Sendai Framework for Disaster Risk Reduction (2015–2030) [
22], resilience is defined as, “
the ability of a system, community, or society exposed to hazards to withstand, absorb, adapt to, and recover from the effects of a hazard in a timely and efficient manner, including by maintaining and restoring its essential basic structures and functions” (p. 9). The definition shows typical technical resilience characteristics, such as the ability of system components to withstand and recover effectively from shocks, measured and quantified by return time and efficiency [
23,
24]. This example of a resilience definition used in an established and internationally recognized document, such as the Sendai Framework, illustrates that in today’s international arena the technical resilience understanding remains dominant, including in the field of critical infrastructures, despite emerging efforts to broaden it, e.g., in the context of drinking water systems [
7] or minimum supply to govern infrastructure failures [
25].
The concept of resilience is originally rooted in ecology. Crawford Holling’s [
26] article on the “
Resilience and the Stability of Ecological Systems” is often cited as the cornerstone of resilience research by providing the resilience understanding in the context of robustness of ecological systems [
27,
28]. This understanding of resilience contrasts with the technical understanding in that it is not measured in terms of time and efficiency, but in terms of the magnitude of disturbance the system can withstand while maintaining functionality [
29]. The concept of ecological resilience is frequently used by authors both within and outside the ecological sciences. The terminology ecological resilience may obscure the fact that the concept is not limited to ecological contexts and is applied, for example, in critical infrastructure research, e.g., by [
30,
31,
32].
In addition to ecological and technical contexts, resilience has also been increasingly addressed in social science. Keck & Sakdapolrak [
33] highlight that social resilience is often vaguely defined but generally refers to “
social entities—be they individuals, organizations or communities—and their abilities or capacities to tolerate, absorb, cope with and adjust to environmental and social threats of various kinds” (p. 8). However, social resilience approaches have been controversially discussed and criticized in terms of whether resilience is an adequate concept to be applied to societal phenomena [
33]. Concerns about the “
re-naturalization of society” [
34] and the return of natural determinism [
35] have been criticized for ignoring power relations and societal structures that are often root causes of risk [
33,
36,
37]. Social science phenomena can hardly be measured or assessed by numerical means, making it difficult to apply a technical understanding of resilience to the social sciences. As organizational challenges are partly inseparable from social aspects, e.g., regarding adaptive and coping abilities, it was decided to use the term organizational aspects in this review. In some cases, however, the authors additionally use social aspects as an umbrella term
Later in the life cycle of the resilience concept, another conceptualization, that of social-ecological systems, was developed by scientists [
29,
33,
38,
39,
40]. Unlike the other resilience perspectives, this represents the most holistic and complex understanding of resilience, viewing social and ecological systems as coupled and interconnected. This understanding of resilience goes beyond the general characteristics of a system’s ability to withstand disruptions and maintain function, and further includes concepts such as adaptability (often referenced in discourses on climate change) and transformability when new system pathways are required [
41,
42]. Recently, technical aspects of resilience thinking have been integrated and applied to coupled social-ecological systems, socio-technical systems (e.g., [
32]), or socio-technical-ecological systems (e.g., [
43]). The realization that system components should be considered together rather than in isolation became a central aspect of resilience research as it evolved.
Such system approaches have, for instance, been advanced in the context of resilience engineering, which seeks to advance resilience in the context of safety [
44]. It acknowledges the complexity of systems and the need to link social and technical aspects [
45]. The concept has been operationalized (including for health services, e.g., in primary care management [
46] and drug administration [
47]. Although this application to health infrastructures is helpful, it has often been done with a focus on the system without considering it in a wider context. The underlying understanding of resilience as having four cornerstones—anticipating, learning, monitoring, and responding [
48]—may not yet embrace more recent understandings that add the system’s abilities to adapt and transform [
49], despite promising studies [
50].
Hence, this paper argues that the predominant view on health infrastructure resilience still needs to be broadened and that this is a viable approach to improve the functionality of health infrastructures during emergency situations. Organizational challenges of emergency preparedness in health care facilities are assessed to generate knowledge on systemic challenges and the potentials of a broadened and holistic understanding of resilience. Based on this context the authors propose their own definition of resilience in the context of critical health infrastructure, which is outlined in the discussion and explains how resilience is conceptualized in the context of this paper. Based on a systematic literature review, carried out under the umbrella of a larger research project, “Emergency preparedness planning for water supply and sanitation in health care facilities—organisational and technical solution strategies to increase resilience” (NOWATER), this paper aims to answer the following questions:
Which knowledge gaps remain in a typically technically oriented understanding of the resilience of critical health infrastructure?
What real-world cases can be found in the literature that specifically deal with water supply failures in health care facilities and which organizational challenges do they address?
What lessons can be learned from these cases for improving risk management and emergency preparedness planning?
How can these findings contribute to advancing critical health infrastructure resilience thinking?
How can these findings contribute to enhancing emergency preparedness and resilience of health care facilities towards future water supply failures?
3. Methodology
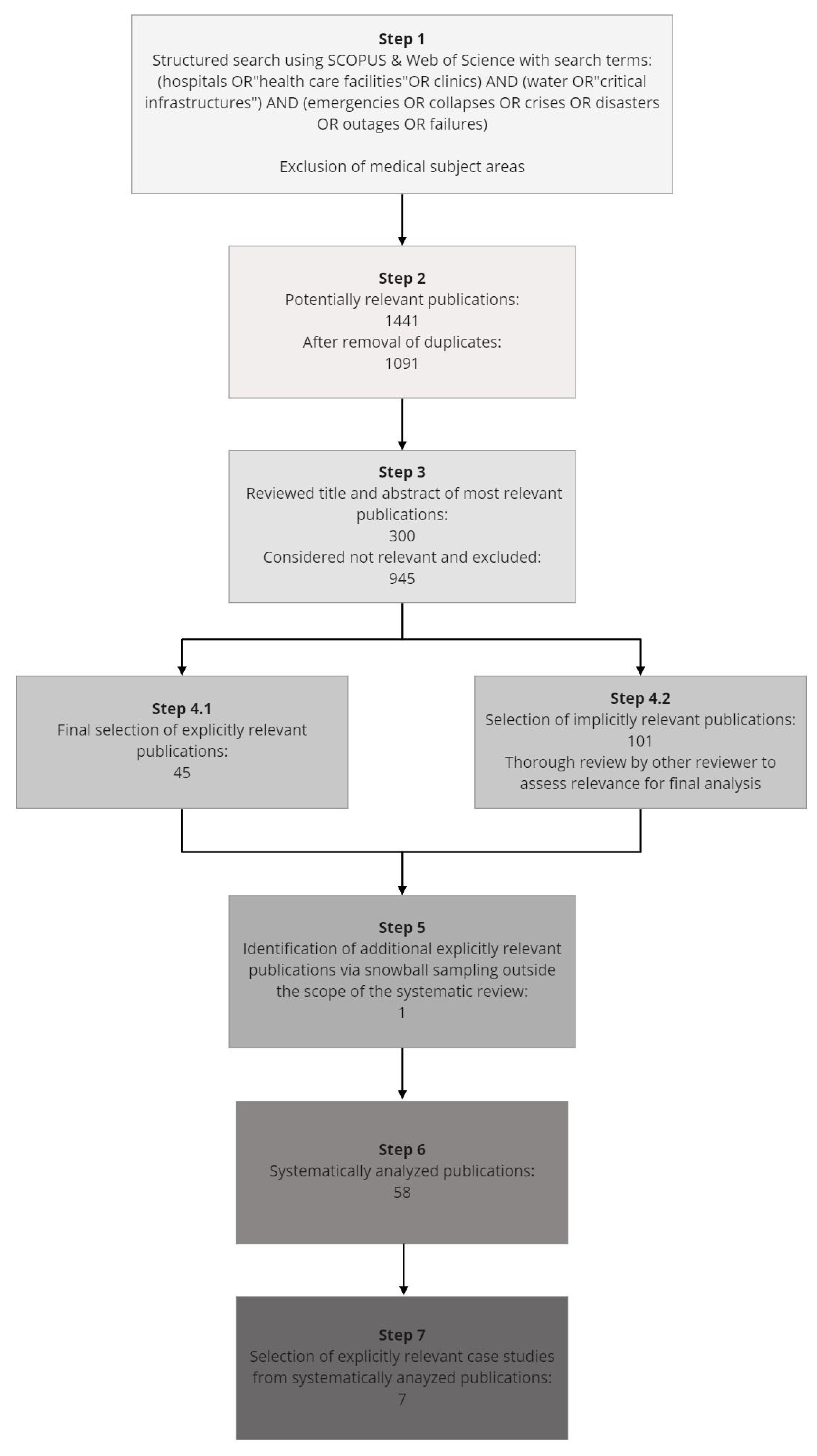
This paper is based on a systematic literature review conducted as part of the ongoing NOWATER research project. The literature review aimed to identify water supply failures in healthcare facilities from global literature to identify organizational challenges and necessary improvements to thereby inform strategies for overall resilience building processes. All steps and results of the systematic literature review are shown in
Figure 1.
The structured literature review was conducted between June and December, 2020 using the electronic databases SCOPUS and Web of Science. Studies were identified using combinations of the search terms (in English language only) “hospitals OR health care facilities OR clinics“, “water OR critical infrastructures” and “emergencies OR collapses OR crisis OR disasters OR failures”. To refine the scope of the review, medical subject areas were automatically excluded from the review because they typically do not contain content of interest to technical and organizational emergency planning concerns. During this process, 1441 potentially relevant publications were identified. After removing the duplicates from both databases, 1091 documents remained.
Subsequently, the databases were set to automatically sort papers by relevance. As a next step, titles and abstracts of each individual publication were reviewed with explicit and implicit relevance according to predefined inclusion and exclusion criteria. The criteria included specific relevance to the topic of the research questions, timeliness (not older than 30 years), language (English), and setting (focus on health facilities and disaster context). In addition, practice-based case studies were primarily considered as they were deemed particularly relevant to the review. Saturation was achieved after reviewing the 300 most relevant publications, as no more publications met the inclusion criteria from the past 50 publications. Ultimately, 45 explicitly relevant and 101 implicitly relevant papers were considered. The 101 implicitly relevant papers were then reviewed in a second round by an additional reviewer to classify them as either relevant or not relevant. Finally, 57 relevant publications were selected for systematic analysis.
All relevant publications were systematically analyzed using MAXQDA software for qualitative data and text analyses, using various manual coding features, such as creating hierarchical coding systems including sub-codes, organization of coded segments, and creating memos. The contents of the publications were coded along a predefined category system. Part of the category system was to identify case studies including best and worst practices in response to events of water supply failures. For the sake of simplicity, we refer to these events as “disaster” in this publication, regardless of how the individual events were triggered or their scale. All papers chosen were additionally qualitatively reviewed for their resilience conceptualizations. This process allowed for the evaluation and comparison of applied resilience concepts in the context of critical health infrastructure. However, the term resilience was deliberately not included as a search term in the systematic literature search. This made it possible to include contexts and studies that do not necessarily name resilience as such, but rather list measures in the broader context of emergency preparedness and risk management. This ensured that such contexts were also included in the resilience discourse of this paper.
From the 57 papers systematically analyzed, seven case studies were selected for in-depth evaluation. The case studies were selected because they describe and discuss not only technical aspects, but also organizational measures of emergency preparedness and risk management, which offered enough content from which organizational lessons learned could be derived. Another selection criterion was coverage of a broad range of water outage causes and a wide geographic distribution of cases worldwide. All case studies were identified through a systematic literature search, with the exception of [
51], which was added via the snowballing technique. To provide a holistic and diverse overview, regional distribution across world regions was an additional criterion.
One study limitation detected is the comparably large proportion of the publications and documented cases related to events in the USA, with Hurricane Katrina being one of the most prominent and well-documented case studies in history. Nevertheless, the literature review allowed for the showcasing of a wide-range of events from different regions, but also different events that resulted in disruption of water supply systems, leading to cascading failures of other critical systems. Predominantly, events that caused structural damage on a regional scale (e.g., earthquakes, hurricanes, flooding) were examined. Other events that covered incidents on a smaller scale (e.g., pipe bursts) were also evaluated, in addition to limitations on water usage due to non-structural damage, such as bacterial contamination of drinking water or reduced water availability due to drought.
4. Results
4.1. Uptake of Resilience Concept in Critical Health Infrastructure Literature
In the reviewed literature on critical health infrastructure, resilience has almost invariably been understood, analyzed, and conceptualized from a technical resilience perspective. With the exception of Dippenaar & Bezuidenhout [
30] and McDaniels et al. [
32], resilience has rarely been considered from a social science perspective and irregularly integrates social components into the understanding of resilience, suggesting that the functionality of health systems is dependent on their technical components alone. Dippenaar & Bezuidenhout support this finding, noting in their own literature review on risk management and continuous water supply for hospitals in the Western Cape, that the literature addressing organizational resilience of health infrastructure in the context of water and risk management remains limited [
30]. However, outside of the resilience discourse, our findings also show that the majority of the papers mainly or even exclusively analyzed technical components of critical health infrastructures. A few papers mentioned social and organizational components of health infrastructure, but these concepts were not a predominant focus.
Interestingly, only four publications define resilience at all (see
Table 1), although it is frequently mentioned or referred to in the literature reviewed. The first three definitions in the table present a systems perspective of critical health infrastructure resilience and remain rather vague, as they do not specify (in the definition) which system components they encompass. The definitions presented from Dippenaar & Bezuidenhout [
30] and McDaniels et al. [
32] both relate more to the ecological conceptualization of resilience outlined earlier, whereas the definition from Vugrin et al. [
31] additionally has typical features of the technical resilience conceptualization. The definitions of Vugrin et al. [
31] and Yusoff et al. [
52] additionally include social-ecological components such as adaptability in their resilience definition, which are not included in the first two definitions. Only the definition of Yusoff et al. [
52] can be classified as social resilience as it refers specifically to social entities.
It is striking that most of the authors that do not define the term resilience in more detail look at resilience exclusively from a technical perspective. In contrast, the authors listed in the table who dealt with the concept of resilience in more detail—excluding Vugrin et al. [
31]—use the ecological perspective rather than the technical one. Interestingly, the same paper also includes typical characteristics of the broader understanding of social-ecological resilience, but without elaborating on the resilience discourse and why the authors present this definition. Of all the authors who defined resilience in the context of healthcare infrastructure in the literature review, McDaniels [
28] and Dippenaar & Bezuidenhout [
26] provided the most detailed conceptual elaboration on resilience. Other authors did not discuss resilience in as much detail or did not define resilience at all in their respective contexts. However, even though the authors seem to take a broader viewpoint of resilience by including not only technical but also social resilience components, their approach does not become obvious from the definitions they presented as they did not entail any typical characteristics of the holistic social-ecological resilience concepts. Moreover, these two authors were also the only ones to highlight that organizational processes of risk management and emergency preparedness are critical to the resilience of healthcare facilities. For example, McDaniels [
32] highlights that technical resilience, the physical system performance of infrastructure during disruptions, and organizational resilience, the ability of an organization to make appropriate decisions during a disaster event and take effective action, are required. Dippenaar & Bezuidenhout [
30] highlight that in addition to technical infrastructure, components of organizational processes of business continuity, risk management, and emergency management, in addition to individual behaviors such as leadership, awareness, and communication, are key elements of resilient healthcare infrastructures. This finding suggests that authors who engage in detailed resilience discourses tend to include both system components, social and technical, of critical health infrastructures.
4.2. What Real-World Cases Can Be Found in the Literature That Specifically Address Water Supply Failures in Health Care Facilities?
The threats reported in the reviewed case studies (see
Table 2) are predominantly due to interruptions in the power and water supply system (e.g., [
56]) and structural damage (e.g., [
57]). Water supply interruptions or failures, as the case studies show, can be highly diverse in nature, ranging from power and water supply failure to cascading failure of other critical health infrastructure, tap closure, water intoxication, or bacterial contamination. These generally led to cascading failures and impacts, such as loss of communication (e.g., [
57]), lack of sewage disposal [
58], and bacterial contamination (e.g., [
59]), which in turn limited the functionality of healthcare facilities and authorities (e.g., [
58,
59]). It is essential to consider cascading impacts, because critical infrastructures exist as interconnected networks or systems where each component determines the functioning of the other system components. Disaster risk management must take into account such cascading impacts as they affect the recovery of the population, industry, and other sectors [
60].
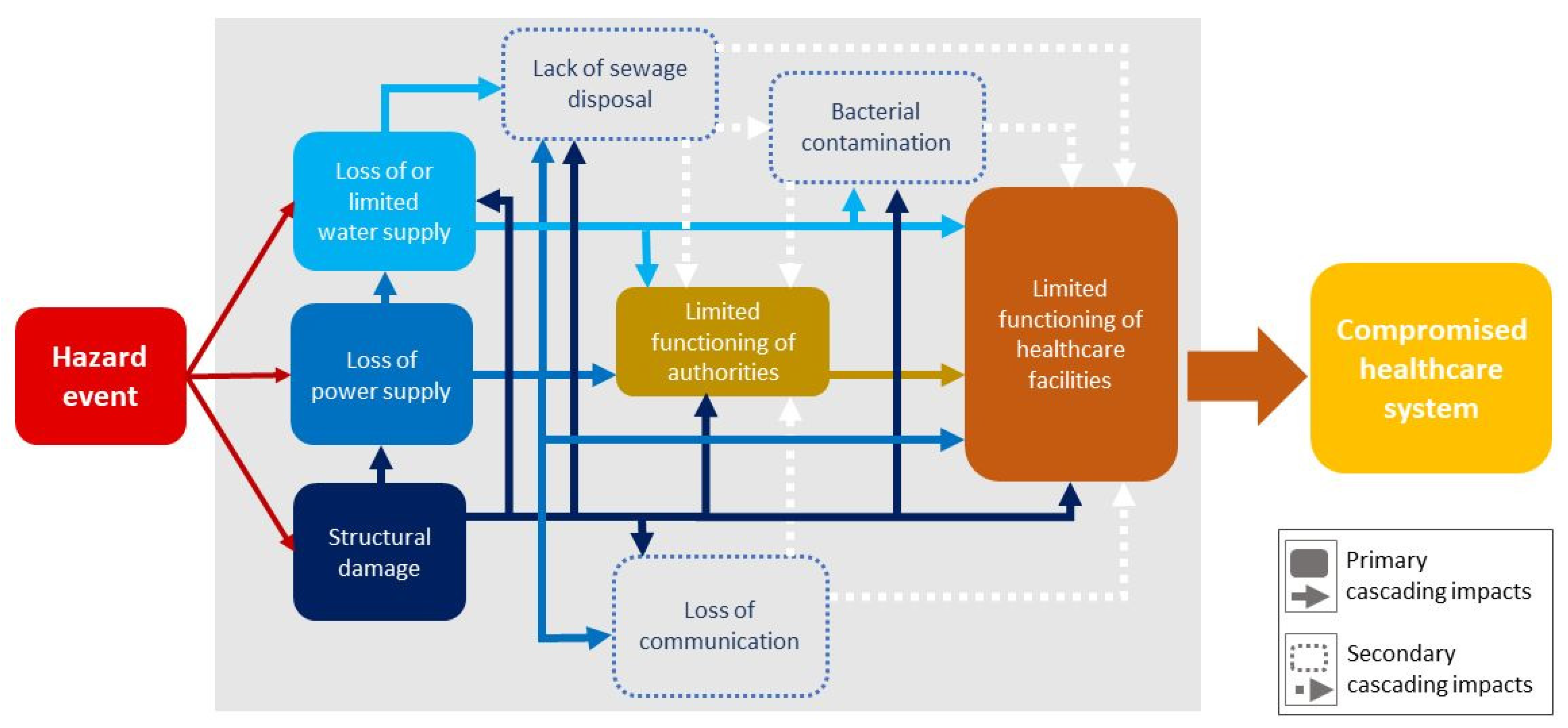
These cascading impacts that could be detected across case studies ultimately resulted in the impairment of the healthcare system. In addition to the direct impacts like a flood resulting in structural damages, several indirect impacts could be determined which ultimately have negative impacts on the overall functionality of healthcare systems (see
Figure 2). Impacts that occurred secondarily to structural damage and the loss of power and water could also have consequences for the ability of government agencies and the health care facilities to function properly. In all cases, the post-event threats and cascading impacts resulted in compromised healthcare systems.
The case studies describe numerous technical and organizational measures to respond to the threats (e.g., implementation of water tanks as an emergency supply option) [
62]. However, organizational processes before, during, and after such events within the healthcare facility and between healthcare facilities and other important actors are only marginally outlined and not put into perspective of the larger event and its impacts. Primarily, processes that take place within healthcare facilities are addressed. These include: (i) identification of the risk, degree of damage, period of disruption, and the consequences to the facility, which is ideally the responsibility of designated employees [
64]; (ii) formation and activation of disaster teams within the facility [
57,
64]; (iii) evacuations when considered necessary (e.g., [
58]); (iv) restrictions on the use of water and organization of alternative water supply (e.g., [
59]); (v) ensuring communication within the facility; and (vi) evaluation of emergency preparedness (or risk management) plans and preparedness of disaster management teams [
30,
56]. Ensuring and maintaining communication with stakeholders outside the facility (e.g., asking for water supplies from authorities [
63] was identified as an organizational measure by the healthcare facility to the externality.
The described events require targeted response strategies and actions in each individual case, largely dependent on effective and appropriate ad hoc human actions and decisions, particularly of those in positions of responsibility [
30,
32]. The key clusters of organizational processes which determined success or failure of response action could be identified across case studies: (i) development and continuous revision of emergency preparedness plans, and (ii) importance of communication and networking in emergency preparedness strategies. In five of seven cases the development or revision of risk management and emergency preparedness plans were addressed. Additionally, five case examples explored the challenges of communication and the importance of networks in emergency preparedness, whereas other factors such as the implementation of organizational evacuation measures [
58] were detected in only a few.
4.2.1. Development and Continuous Revision of Emergency Preparedness Plans
A major finding was that the threats were exacerbated by the absence [
59] or inadequacy [
30] of emergency preparedness plans for disasters and specifically for water supply disruption. As a result, plans were developed [
30,
57,
59] or revised [
30,
56,
63] accordingly. The findings suggest that holistic emergency preparedness plans are an essential part of a strong preparedness strategy and contribute to increasing resilience of healthcare facilities. Such a plan needs to include assignment and clarification of responsibilities in the event of an emergency, so that decision making can be expedited and healthcare facilities can function autonomously [
57]. It is necessary to involve a diverse team, including technicians, nursing staff, and management in the plan development to cover all aspects of a water outage that may be affected. Therefore, the willingness of staff to participate in the formulation of a plan should not be underestimated [
30]. A diverse team and a multidisciplinary approach are especially important when factoring in future developments, such as climate change impacts (for example, more frequent and extreme events) and the growing world population [
30].
The case studies show that it is important for these plans to be individualized for each healthcare facility, as the facilities differ greatly in size and therefore have different needs and capacities [
30]. The process of plan development is influenced by factors such as the number of sites, the availability and accuracy of information (e.g., regarding the water demand of the facility), and the available budget [
30]. Furthermore, the willingness of employees to participate in this process should also not be ignored, as a diversified selection of staff is needed to make the emergency preparedness plan as effective as possible. People’s behavior, therefore, has a decisive impact on the development process [
30]. It is also critical to designate clear responsibilities in emergency plans so that in the event of a disaster event, the healthcare facility can act independently from mandates of authorities, which can reduce the number of decisions needed during a disaster event [
57]. After the disaster event, Kirsch et al. [
57] recommend the deployment of multidisciplinary assessment teams to conduct damage and function assessments. The resulting findings can then be integrated into the emergency preparedness plan to close existing knowledge gaps.
4.2.2. Importance of Communication and Networking in Emergency Preparedness Strategies
Functioning internal communication (within the healthcare facility) and external communication (between the healthcare facility and external actors) plays an essential role in emergency preparedness and response. There are different types of communication (e.g., telephone, email, or media releases) that are used in practice, with social media platforms becoming increasingly relevant in emergency communication [
64].
Internal communication includes communication amongst staff members and between staff and patients in a healthcare facility. An internal staff communication flow during a disaster could include the following steps: First, designated disaster team members disseminate information to unit leaders. In turn, the unit leaders communicate with the staff in “
safety huddles”, ensuring the information is consistent and up-to-date. Relevant information can then be shared with patients [
64]. In an emergency event, staff-to-patient communication involves regularly informing patients about the situation, giving instructions for action, and clarifying questions of patients [
59,
64]. Establishing effective internal communication can help create stability and predictability during a disaster event; however, this can be challenging in the event of a complete loss of power, telephone network, or Internet. In that case, other ways of communication can be considered (e.g., employing couriers to communicate within the healthcare facility) [
64].
External communication involves, above all, the establishment of strong and dependable networks on local, regional, and national scales to increase emergency preparedness and therefore the resilience of a healthcare facility [
51]. Authorities should provide clear guidance to healthcare facilities, especially regarding water outage scenarios and evacuations [
61]. At the same time, healthcare facilities should communicate with utility providers and jointly develop emergency response strategies, such as diversifying water suppliers in the case of a service failure [
63].
The real-world cases indicate that the main actors in the networking process are the state health departments, healthcare facility management, and utility providers regardless of country or context [
56,
63,
64]. Historically, these networks have provided the foundation for developing an adequate emergency plan (as they provide coordination and response in the case of a disaster) and are ideally based on mutual knowledge and trust. To form networks, informal and formal disaster management team meetings on a monthly basis are suggested by Janius et al. [
56], e.g., to provide updates and ensure procedural knowledge remains current amongst staff members. This allows actors to get to know each other and build a foundation of mutual trust, which facilitates, for example, the development of emergency preparedness plans.
In summary, the insights gained from the case studies suggest that internal and external communication of healthcare facilities and the preparation and continuous updating of emergency preparedness plans are two essential factors in emergency preparedness. These insights can help to increase the organizational resilience of healthcare facilities in the context of water supply failures, which is discussed in the next section.
5. Discussion
5.1. Enhancing Emergency Preparedness and Overall Resilience of Health Care Facilities
After a thorough literature analysis, the results indicate an urgent need for advancing critical health infrastructure resilience, both in conceptualization and practical implementation. Because hazard events trigger technological failures such as outages or disruptions of water supply in healthcare facilities, solution approaches also tend to prioritize physical infrastructure components. The case studies, however, demonstrate the extent to which technical and organizational processes are intertwined in the context of water supply failures following hazard events in healthcare infrastructure. This is evident, for example, in the implementation of backup or alternative water supply measures, such as water tanks or bottled drinking water [
62,
64]. The technical resources have to be available in general (e.g., the water tanks themselves), but the organizational effort involved in procuring backup and alternative water supply measures must also be emphasized.
The two key activity clusters ((i) development and continuous revision of emergency preparedness plans, and (ii) the importance of communication and networking for emergency preparedness strategies) identified in the results section show how organizational processes can enhance the overall resilience of healthcare facilities in regards to technical problems such as water supply failures. Establishing an emergency preparedness plan that specifically includes water failures should be an important consideration in any emergency preparedness strategy. It is essential to create a customized plan that specifies both technical aspects, such as the specific water consumption of the healthcare facility, and organizational processes.
The results suggest that communication networks at local, regional, and national scales provide a solid foundation for the development of emergency preparedness plans. Other research based on field experience confirms this insight from the literature review [
65,
66]. Although it is known that organizational actions such as networking and knowledge transfer can increase the resilience of healthcare facilities [
67,
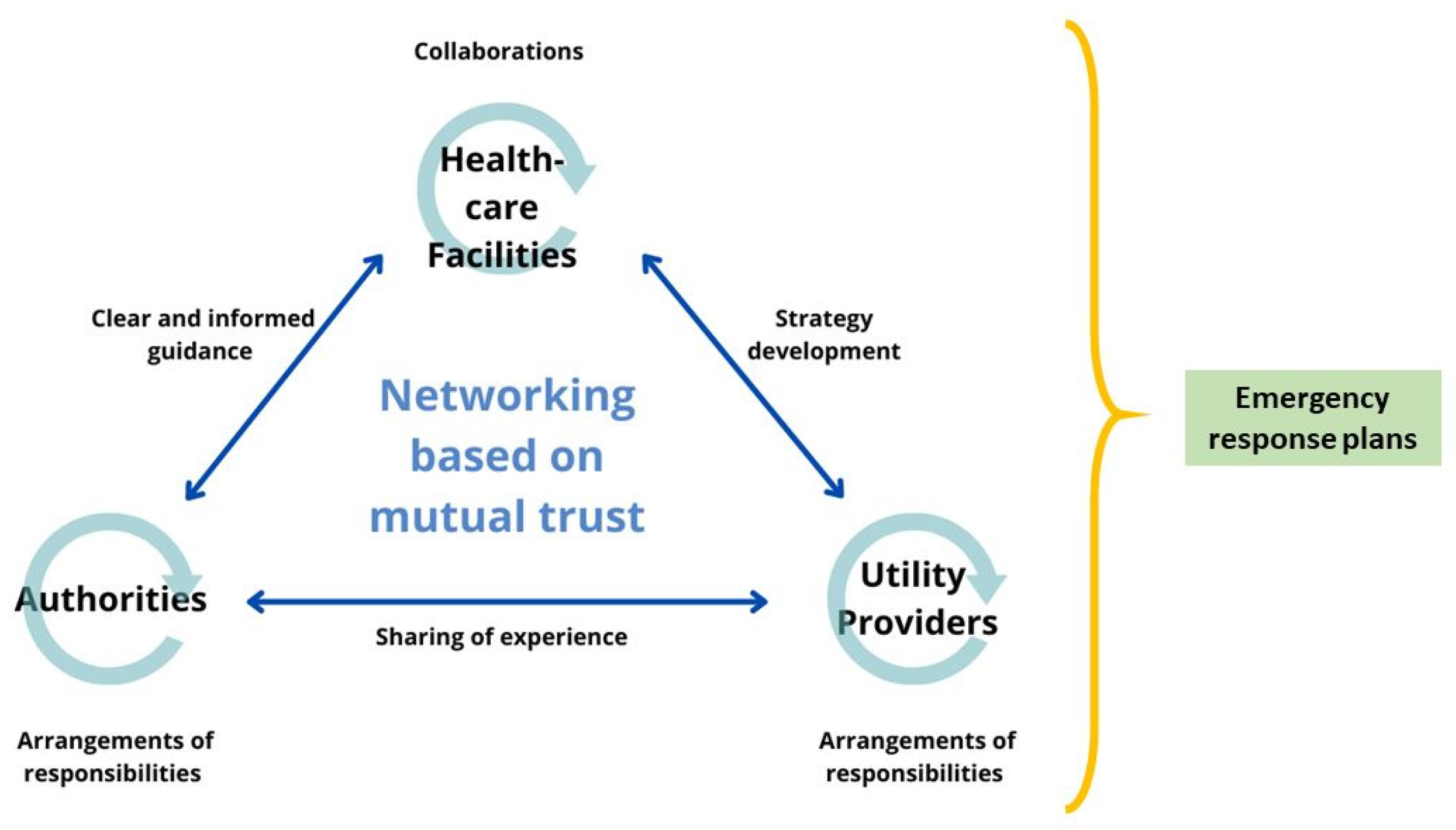
68], this remains unrepresented in research specifically for the case of water supply failures. Here, the formation or expansion of a network between healthcare facility management, authorities, and utility providers could establish the basis for creating an adequate emergency preparedness plan (see
Figure 3). For instance, partnerships between neighboring healthcare facilities are recommended as alternative means when water supplies are interrupted [
64]. From the analysis of the cases, it can be deduced that authorities such as health and civil defense departments can improve their efforts by exchanging information and defining responsibilities in arrangements between the departments. The same applies to utility providers including water suppliers.
Furthermore, regular communication and networking between healthcare facility management, authorities, and utility providers is important. The findings indicate a gap in this communication triangle (
Figure 3). Although contacts between local authorities and health care facilities, and between utility providers and healthcare facilities, do exist, this is not necessarily descriptive of the relationship between the utility providers and local authorities. However, utility providers should be in close contact with local authorities to communicate service disruptions and procedures for most efficiently restoring water supply. Such contacts are a foundation of mutual trust, which facilitates, for example, the exchange of sensitive information and ultimately the development of mutually beneficial emergency preparedness plans.
The example of strengthening networks to create a foundation for emergency plan development also demonstrates the interdependence of social and technical components in the emergency preparedness of healthcare infrastructure. It highlights the necessity of considering both components equally when implementing measures to increase resilience in healthcare facilities.
5.2. Advancing Critical Health Infrastructure Resilience Thinking
The results show that both social and organizational aspects of emergency preparedness are fundamental in the adequate planning for healthcare facilities. Technical components and measures to ensure an alternate or backup water supply (e.g., implementation of on-site water storage options (such as groundwater wells), use of emergency water tanker trucks, and enabling backup service from adjacent public water supply service zones [
62]) can only be established through effective organizational procedures, both before and during disruptive events. The interdependence of social and technical components calls for fundamentally shifting the way that critical health infrastructure is conceptualized to social-technical systems.
A lesson learned from our research is that improving resilience thinking in critical health infrastructure contexts can be facilitated by real world cases, including their cascading impacts. Although this may seem relatively straightforward, in reality impacts are not always disclosed or linked to one another. The role of the “human factor” and the agency of individuals acting within social-technical systems have been underappreciated not only in critical health infrastructure literature, but also in overarching resilience discourse. While acknowledging that there are some limitations to incorporating social dimensions into resilience thinking [
33,
35,
36,
37], this review shapes resilience rather through a conceptual lens, offering the opportunity to demonstrate and learn how critical health infrastructure can broaden its scope to encompass additional aspects and ultimately increase its resilience.
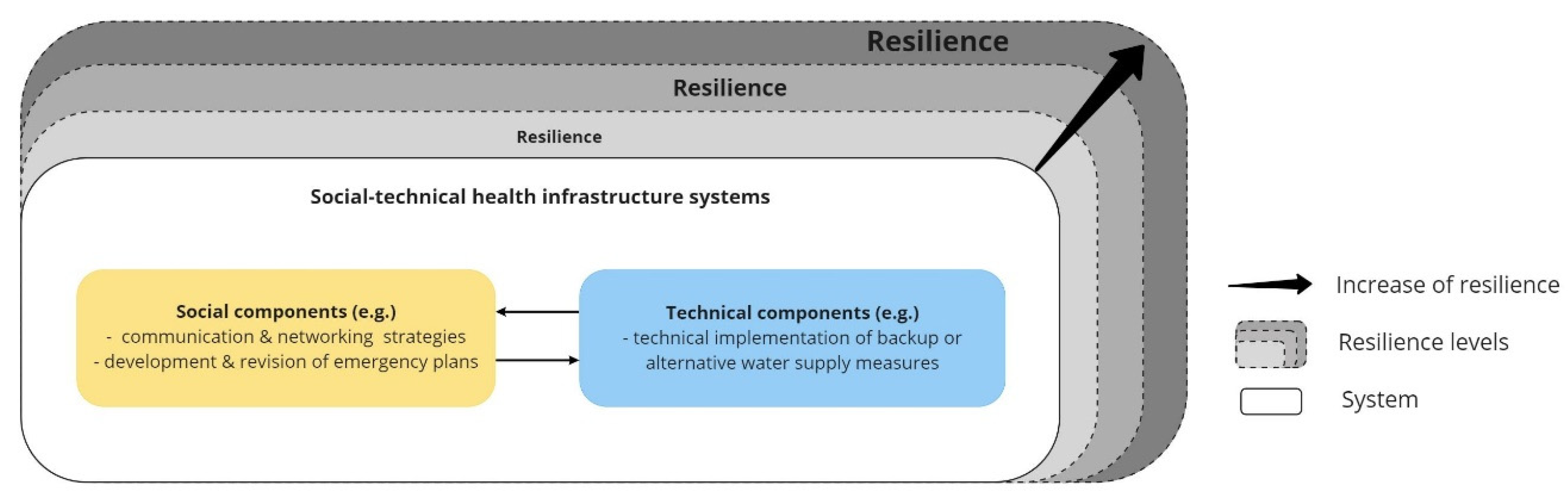
Based on these findings, resilience is heightened by incorporating social components into resilience thinking. These lessons need to be included into the conceptual understanding of resilience, which in turn underscores the need for a more holistic understanding of social-technical system resilience (see
Figure 4). Overall resilience can be increased by the system’s ability to adapt and transform, allowing the system to achieve more advanced “levels” of resilience.
The literature review uncovered a lack of a commonly accepted definition of resilience in the context of critical health infrastructure. Although critical health infrastructure is often discussed in the context of resilience, authors frequently do not explicitly define the term, which conceptualization they follow, and which aspects of critical health infrastructure they consider relevant and for what purposes. This vagueness and lack of a clearly outlined resilience definition, in specific contexts, underlines the need for additional discourse on the resilience of critical health infrastructure. This, in turn, further compromises the understanding of resilience and reinforces the lack of consensus on how studies define and conceptualize critical health infrastructure resilience. The lack of understanding in resilience discourse may also have contributed to the fact that prevailing resilience concepts are rarely challenged in the context of critical health infrastructure, often remaining with technical or ecological resilience perspectives which are regularly applied without proper contextual understanding. Thus, we argue that it is critical to more precisely define and conceptualize the meaning of resilience.
This helps expand the operationalization of resilience beyond technical components to also include social ones. Here, critical reflection using real-world examples will help to identify linkages and cascading effects, and to understand which components most contribute to improving the resilience of critical health infrastructure. The authors reviewed, who were more engaged in the resilience discourse applied a more multidimensional approach. In contrast, other authors described organizational challenges associated with water disruptions but did not necessarily consider them as relevant in their approaches to resilience building. Learning from real-world emergency situations leads to adaptability and transformability, which are essential characteristics of the more holistic resilience understanding utilized in social-ecological [
41,
42] or social-technical systems [
32].
Finally, our literature review revealed that most studies are primarily concerned with the technical aspects of water outages (preparedness, response, recovery), whereas the organizational processes are mentioned rather briefly. As a consequence, the focus is still on the technical aspects of crisis preparation and management, whereas organizational processes are often taken for granted. Studies of critical health infrastructure fail to acknowledge health infrastructure as a larger system, in which the organizational processes of emergency preparedness and risk management are critical. By critically reflecting on Carpenter’s et al. [
29] question “
resilience of what to what?”, it becomes clear that resilience of health care facilities to water supply failures is about more than just technical efficiency and the time in which water supplies can be restored. The technical resilience understanding overlooks social dimensions, including organizational procedures, aspects of resilience building that are essential to success. It is crucial to look closely at the strengths and weaknesses of specific organizational procedures before, during, and after a disaster event. Doing so advances resilience thinking, which will identify leverage points for improvement and further improve the resilience of critical infrastructures in reality.
Defining the resilience of health infrastructures can be a promising way forward. Therefore, after carefully reviewing the key shortcomings of the resilience understanding in the discourse on health infrastructures and expanding this understanding to a more holistic approach, we propose the following resilience definition specifically for this context:
The ability of health care infrastructure and its social and technical system components to cope with disruptions while maintaining essential functions, and at the same time facilitate adaptive, innovative, and transformative approaches to be better prepared for future disruptions (partially drawing on [
33,
41,
42]).
6. Conclusions
This study demonstrated the importance of evaluating health infrastructure resilience for identifying and addressing gaps. Our findings have shown that a hazard event may trigger multiple and cascading effects that severely affect the continued operation of healthcare facilities, and thus their functionality. Although this in itself is not new, the study showed that, in reality, there are serious shortcomings in the implementation of emergency preparedness (or risk management) planning.
The first major conclusion of this review, which addresses the research gaps, is that emergency preparedness planning must also include organizational components, which have been underrepresented to date, and are key to increasing overall resilience. This is especially true in the case of water supply failures, which would pose a major threat to communities, but for which there is a one-sided approach in the literature and few plans exist in reality. Two factors for increasing the resilience of health care facilities in the context of water outages are (i) the development and continuous revision of emergency plans, and (ii) communication and networking within and across involved actors. As a key component of a preparedness strategy for water outages, an emergency preparedness plan is ideally formulated by a diverse team of staff to address as many aspects as possible. The plan should be developed in close collaboration with healthcare facilities, authorities, and utility providers, and needs to be continuously updated. These two strategies in parallel serve to build trust and strong, reliable networks amongst the actors, contributing to increasing the overall resilience of health facilities.
To close the research gap on real-world cases, this review identified case studies showing not only technical aspects, but also organizational measures of emergency preparedness and risk management specifically dealing with water supply failures in health care facilities. Water supply interruptions or failures, as the case studies show, can be highly diverse in nature, ranging from power and water supply failure to cascading failure of other critical health infrastructure, tap closure, water intoxication, or bacterial contamination. One outcome of the literature review is that organizational processes within and between healthcare facilities, including actor constellations, are only marginally outlined. We conclude that the various organizational challenges outlined in this paper require targeted response strategies.
Another main conclusion to answer the research question on lessons learned is that in the context of critical health infrastructure, resilience components should not be considered in isolation, but as parts of social-technical systems. Reappraisal of, and access to, real-world case studies can help to improve the understanding of the interconnected and cascading impacts of hazard events and resilience thinking, while improving risk management and emergency preparedness planning. Not only did the COVID-19 pandemic highlight the vulnerability of critical public health infrastructure, but the results of our literature review in the specific context of water supply failures underscore the diversity of factors that must be considered to increase the resilience of healthcare infrastructures. Organizational components should not be seen as separate from technical measures. To increase the resilience of health care facilities to hazardous events leading to water supply failures, not only technical but also social system components need to be considered and should be continuously reviewed and developed as needed.
At the conceptual level, we conclude that the understanding of critical health infrastructure resilience has to take a more holistic approach to resilience that combines social and technical resilience components, thereby contributing to advancing critical health infrastructure resilience thinking. Therefore, this paper proposes to view health infrastructure as a larger social-technical system, thereby building upon and advancing ongoing resilience discourses. Social and technical components are interconnected and influence each other. A paradigm shift is needed away from the one-dimensional, often technically dominated conceptualization of resilience to a holistic conceptualization based on real-world evidence. Therefore, we propose a more holistic resilience definition specifically for the context of healthcare infrastructures.
Based on these conclusions, a key takeaway of this study is that the uptake of such a definition into emergency planning can improve resilience thinking, but it can also strengthen the actual resilience of health facilities before, during, and after hazard events, which answers research question five. Not only is this consistent with the Sustainable Development Goals (SDGs), particularly SDG 3 on Good Health and Well-being, but it is also one of the priorities highlighted in the Sendai Framework for Disaster Risk Reduction (2015–2030). A broader view on critical health infrastructure resilience fits well with the Sendai Framework’s priority of “Build Back Better” because it permits learning more from disaster events, and improving more than technical assets within the health infrastructure itself to enhance future preparedness and thereby transform the larger system. Such a paradigm shift is particularly relevant in the context of growing and more frequently occurring natural hazard events, in addition to the current COVID-19 pandemic, which has shown that functioning healthcare has numerous components, including the availability, cooperation, and preparedness of the involved actors.
The analysis has also shown how intrinsically linked critical infrastructures such as water and healthcare are, and how impairment or outage of one can result in severe cascading impacts on others and ultimately on the functioning of society. To date, this has barely been taken into account. We must overcome a casual and haphazard understanding of resilience and introduce a definition and understanding that allows the healthcare sector to operationalize and implement more holistic approaches to protecting their critical infrastructure from future disaster events and their cascading impacts.