Evaluation of the Post-Training Hypotensor Effect in Paralympic and Conventional Powerlifting
Abstract
1. Introduction
2. Materials and Methods
2.1. Sample
2.2. Instruments
2.3. Blood Pressure
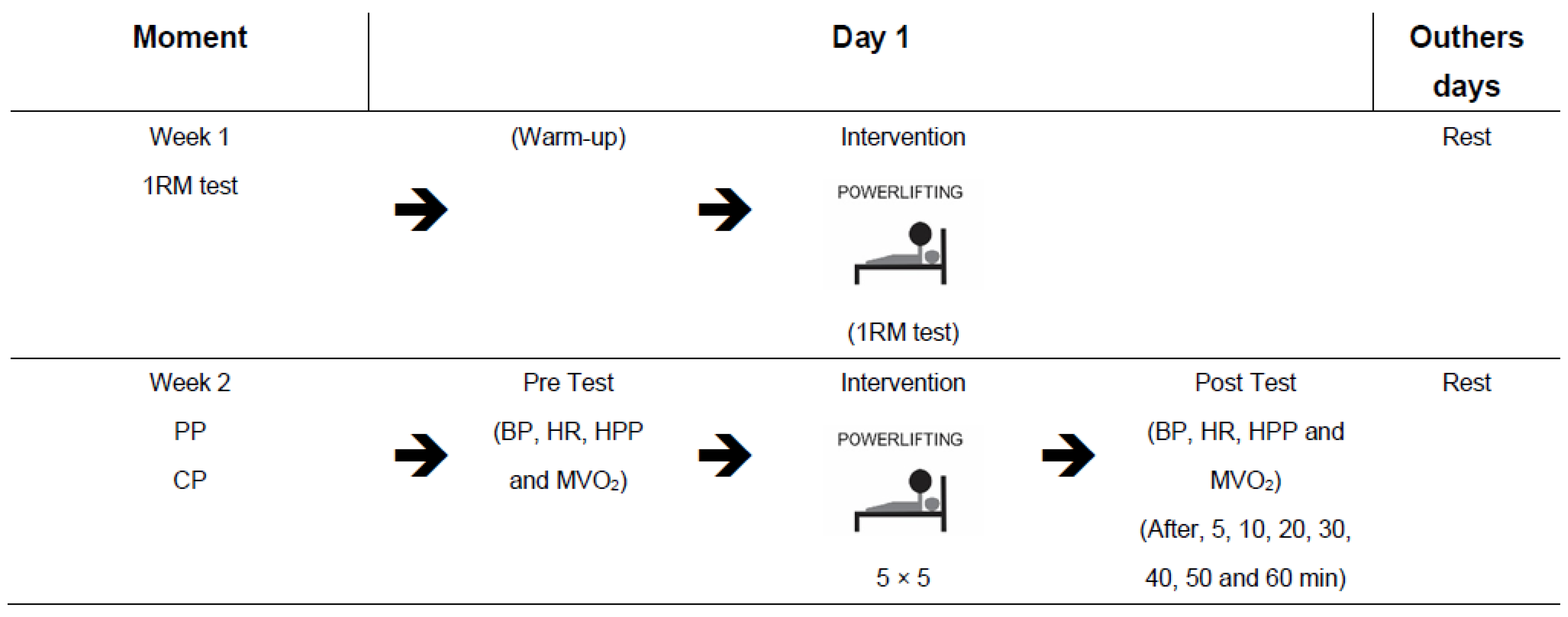
2.4. Procedures
2.5. Statistics
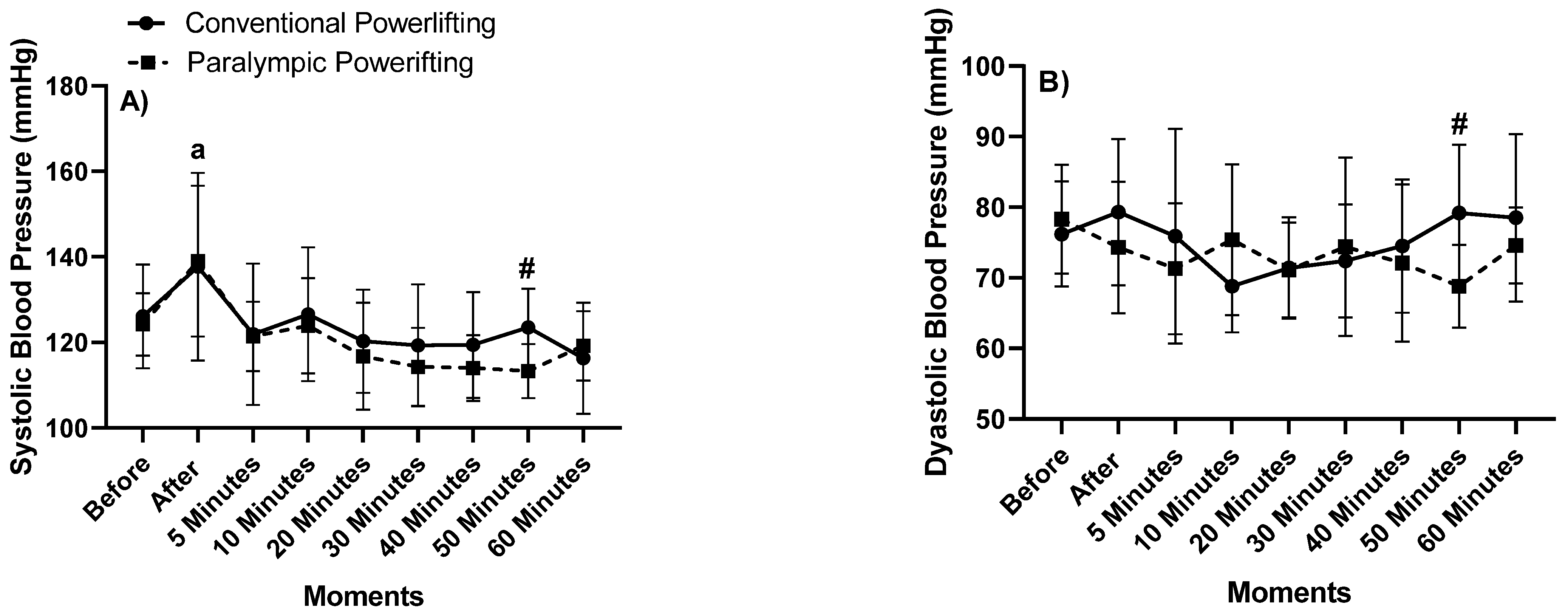
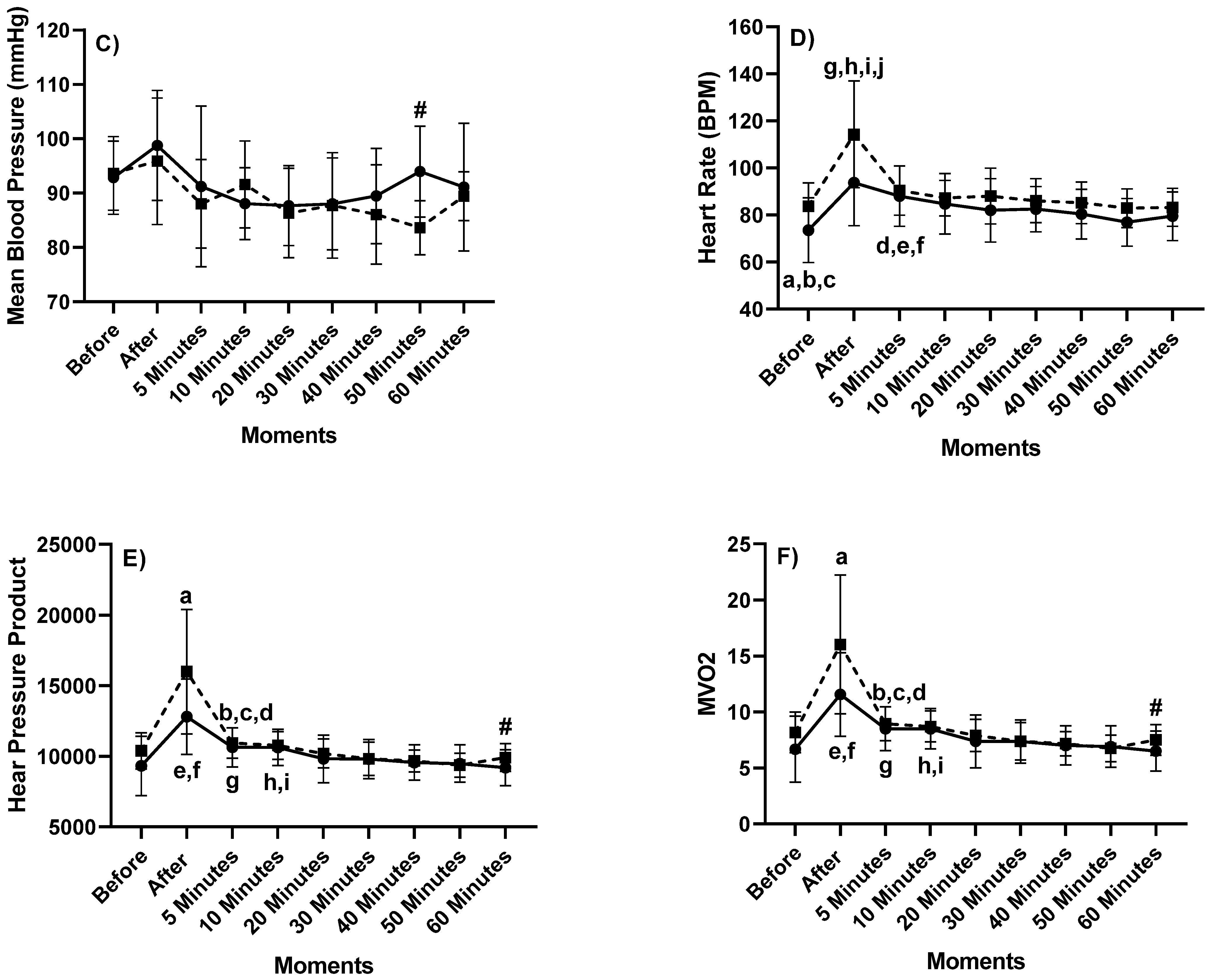
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Rivera, E.C.; Jiménez, J.M.; Rojas, W.S.; Herrera, A.S. Efeito Agudo do Exercício Sobre a Pressão Arterial: Uma Investigação Metanalítica. Arq. Bras. Cardiol. 2016, 106, 422–433. (In Portuguese) [Google Scholar]
- Paz, Â.A.; Aidar, F.J.; de Matos, D.G.; de Souza, R.F.; da Silva-Grigoletto, M.E.; van den Tillaar, R.; Ramirez-Campillo, R.; Nakamura, F.Y.; Costa, M.D.C.; Nunes-Silva, A.; et al. Comparison of post-exercise hypotension responses in paralympic powerlifting athletes after completing two bench press training intensities. Medicina 2020, 56, 156. [Google Scholar] [CrossRef]
- Lewington, S.; Clarke, R.; Qizilbash, N.; Peto, R.; Collins, R. Prospective Studies Collaboration. Age-specific relevance of usual bloodpressure to vascular mortality: A meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 2002, 360, 1903–1913. [Google Scholar] [PubMed]
- Morgan, S.G.; Lee, A. Cost-related non-adherence to prescribed medicines among older adults: A cross-sectional analysis of a survey in 11 developed countries. BMJ Open 2017, 7, e014287. [Google Scholar] [CrossRef] [PubMed]
- Whittaker, A.C.; Eves, F.F.; Carroll, D.; Roseboom, T.J.; Ginty, A.T.; Painter, R.C.; de Rooij, S.R. Daily stair climbing is associated with decreased risk for the metabolic syndrome. BMC Public Health 2021, 21, 923. [Google Scholar] [CrossRef]
- De Sousa, E.C.; Abrahin, O.; Ferreira, A.L.L.; Rodrigues, R.P.; Alves, E.A.C.; Vieira, R.P. Resistance Training alone reduces systolic and diastolic blood pressure in prehypertensive and ypertensive individuals: Meta-analysis. Hypertens Res. 2017, 40, 927–931. [Google Scholar] [CrossRef] [PubMed]
- Figueiredo, T.; Rhea, M.R.; Peterson, M.; Miranda, H.L.; Bentes, C.M.; Reis, V.M.R.; Simão, R. Influence of number of sets on blood pressure and heart rate variability after a strength training session. J. Strength Cond. Res. 2015, 29, 1556–1563. [Google Scholar] [CrossRef]
- Bentes, C.M.; Costa, P.B.; Corrêa Neto, V.G.; Simão, R.; Paz, G.; Maia, M.F.; Figueiredo, T.; Neto, G.R.; Novaes, J.S.; Miranda, H. Hypotensive Responses of Reciprocal Supersets versus Traditional Resistance Training in Apparently Healthy Men. Int. J. Exerc. Sci. 2017, 10, 406–416. [Google Scholar]
- Cavalcante, P.A.M.; Rica, R.L.; Evangelista, A.L.; Serra, A.J.; Figueira, A., Jr.; Pontes, F.L., Jr.; Kilgore, L.; Baker, J.; Bocalini, D. Effects of exercise intensity on postexercise hypotension after resistance training session in overweight hypertensive patients. Clin. Interv. Aging 2015, 10, 1487–1495. [Google Scholar] [CrossRef]
- Cunha, G.A.; Rios, A.C.S.; Moreno, J.R.; Braga, P.L.; Campbell, C.S.G.; Simões, H.G.; Ruiz Denadai, M.L.D. Hipotensão pós-exercício em hipertensos submetidos ao exercício aeróbico de intensidades variadas e exercício de intensidade constante. Rev. Bras. Med. Esporte 2006, 12, 313–317. [Google Scholar] [CrossRef]
- João, G.A.; Bocalini, D.S.; Rodriguez, D.; Charro, M.A.; Ceschini, F.; Martins, A.; Figueira, A., Jr. Powerlifting sessions promote significant post-exercise hypotension. Rev. Bras. Med. Esporte 2017, 23, 118–122. [Google Scholar] [CrossRef][Green Version]
- Maior, A.S.; Simão, R.; Martins, M.S.; de Salles, B.F.; Willardson, J.M. Influence of Blood Flow Restriction during Low-Intensity Resistance Exercise on the Postexercise Hypotensive Response. J. Strength Cond. Res. 2015, 29, 2894–2899. [Google Scholar] [CrossRef] [PubMed]
- MacDonald, H.V.; Johnson, B.T.; Huedo-Medina, T.B.; Livingston, J.; Forsyth, K.C.; Kraemer, W.J.; Farinatti, P.T.V.; Pescatello, L.S. Dyniamic resistance training as stand-alone antihypertensive lifestyle therapy: A meta-analysis. J. Am. Heart Assoc. 2016, 5, e003231. [Google Scholar] [CrossRef]
- João, G.A.; Evangelista, A.L.; Gomes, J.H.; Charro, M.A.; Bocalini, D.S.; Cardozo, D.; Seixas da Silva, D.A.d.C.; Simão, R.; Figueira, A., Jr. Effect of 16 weeks of periodized resistance training on gains of powerlifting athletes. JEPonline 2014, 17, 102–109. [Google Scholar]
- Pritchard, H.J.; Morton, R. Powerlifting: Success and failure at the 2012 Oceania and 2013 classic world championships. J. Aust. Strength Cond. 2015, 23, 67–70. [Google Scholar]
- Santos, W.Y.H.D.; Aidar, F.J.; Matos, D.G.; Van den Tillaar, R.; Marçal, A.C.; Lobo, L.F.; Marcucci-Barbosa, L.S.; Machado, S.D.C.; Almeida-Neto, P.F.; Garrido, N.D.; et al. Physiological and Biochemical Evaluation of Different Types of Recovery in National Level Paralympic Powerlifting. Int. J. Environ. Res. Public Health 2021, 18, 5155. [Google Scholar] [CrossRef]
- La Motte, R.H.; Campbell, J.N. Comparison of the responses of warmth and nociceptive C fiber afferents in monkey with human judgments of thermal pain. J. Neurop. 1978, 41, 509–528. [Google Scholar] [CrossRef]
- Bonsu, B.; Terblanche, E. The training and detraining effect of high-intensity interval training on post-exercise hypotensionin young overweight/obese women. Eur. J. Appl. Physiol. 2016, 116, 77–84. [Google Scholar] [CrossRef]
- Fraga, G.S.; Aidar, F.J.; Matos, D.G.; Marçal, A.C.; Santos, J.L.; Souza, R.F.; Carneiro, A.L.; Vasconcelos, A.B.; Da Silva-Grigoletto, M.E.; van den Tillaar, R.; et al. Effects of Ibuprofen Intake in Muscle Damage, Body Temperature and Muscle Power in Paralympic Powerlifting Athletes. Int. J. Environ. Res. Public Health 2020, 17, 5157. [Google Scholar] [CrossRef]
- Ball, R.; Weidman, D. Analysis of USA Powerlifting federation data from January 1, 2012–June 11, 2016. J. Strength Cond. Res. 2018, 32, 1843–1851. [Google Scholar] [CrossRef] [PubMed]
- International Paralympic Comite (IPC). Rules. Official website of IPC Powerlifting. Available online: http://www.paralympic.org/powerlifting/about (accessed on 20 October 2020).
- Xu, J.; Wu, Y.; Su, H.; Hu, W.; Li, J.; Wang, W.; Liu, X.; Cheng, X. The value of a BP determination method using a novel non-invasive BP device against the invasive catheter measurement. PLoS ONE 2014, 9, e100287. [Google Scholar] [CrossRef]
- Malachias, M.V.B.; Póvoa, R.M.S., Jr.; Nogueira, A.R.; Souza, D.; Costa, L.S.; Magalhães, M.E. 7th Brazilian Guideline of Arterial Hypertension: Chapter 3-Clinical and Complementary Assessment. Arq. Bras. Cardiol. 2016, 107 (Suppl. 3), 14–17. [Google Scholar] [PubMed]
- Barroso, W.K.S.; Rodrigues, C.I.S.; Bortolotto, L.A.; Mota-Gomes, M.A.; Brandão, A.A.; Feitosa, A.D.M.; Machado, C.A.; Poli-de-Figueiredo, C.E.; Amodeo, C.; Mion, D., Jr.; et al. Brazilian Guidelines of Hypertension-2020. Arq. Bras. Cardiol. 2021, 116, 516–658. [Google Scholar] [CrossRef]
- American College of Sports Medicine (ACSM). American College of Sports Medicine position stand. Progression models in resistance training for healthy adults. Med. Sci. Sports Exerc. 2009, 41, 687–708. [Google Scholar] [CrossRef] [PubMed]
- Aksentijević, D.; Lewis, H.R.; Shattock, M.J. Is rate–pressure product of any use in the isolated rat heart? Assessing cardiac ‘effort’ and oxygen consumption in the Langendorff-perfused heart. Exp. Physiol. 2016, 101, 282–294. [Google Scholar] [CrossRef] [PubMed]
- Soares Freitas Sampaio, C.R.; Aidar, F.J.; Ferreira, A.R.P.; Santos, J.L.D.; Marçal, A.C.; Matos, D.G.; Souza, R.F.; Moreira, O.C.; Guerra, I.; Fernandes Filho, J.; et al. Can Creatine Supplementation Interfere with Muscle Strength and Fatigue in Brazilian National Level Paralympic Powerlifting? Nutrients 2020, 12, 2492. [Google Scholar] [CrossRef] [PubMed]
- Aidar, F.J.; Clemente, F.M.; Matos, D.G.; Marçal, A.C.; de Souza, R.F.; Moreira, O.C.; Almeida-Neto, P.F.; Vilaça-Alves, J.; Garrido, N.D.; Dos Santos, J.L.; et al. Evaluation of Strength and Muscle Activation Indicators in Sticking Point Region of National-Level Paralympic Powerlifting Athletes. J. Funct. Morphol. Kinesiol. 2021, 6, 43. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences; Lawrence Erlbaum, Associates: Hillsdale, NJ, USA, 1988. [Google Scholar]
- Cohen, J. Statistics a power primer. Psychol. Bull. 1992, 112, 155–159. [Google Scholar] [CrossRef]
- Selya, A.S.; Rose, J.S.; Dierker, L.C.; Hedeker, D.; Mermelstein, R.J. A Practical Guide to Calculating Cohen’s f2, a Measure of Local Effect Size, from PROC MIXED. Front. Psychol. 2012, 3, 111. [Google Scholar] [CrossRef]
- Lakens, D. Calculating and reporting effect sizes to facilitate cumulative science: A practical primer for t-tests and ANOVAs. Front. Psychol. 2013, 4, 863. [Google Scholar] [CrossRef] [PubMed]
- Bentes, C.M.; Costa, P.B.; Neto, G.R.; Costa e Silva, G.V.; de Salles, B.F.; Miranda, H.L.; Novaes, J.S. Hypotensive effects and performance responses between diferente resistance training intensities and exercise orders in apparently health women. Clin. Physiol. Funct. Imaging. 2015, 35, 185–190. [Google Scholar] [CrossRef] [PubMed]
- Lizardo, J.H.F.; Simões, H.G. Efeitos de diferentes sessões de exercícios resistidos sobre a hipotensão pos-exercício. Rev. Braz. Fisioter. 2005, 9, 289–295. [Google Scholar]
- Keese, F.; Farinatti, P.; Pescatello, L.; Monteiro, W. A comparison of the immediate effects of resistance, aerobic, and concurrent exercise on postexercise hypotension. J. Strength Cond. Res. 2011, 25, 1429–1436. [Google Scholar] [CrossRef]
- Polito, M.D.; Farinatti, P.T. The effects of muscle mass and number of sets during resistance exercise on postexercise hypotension. J. Strength Con. Res. 2009, 23, 2351–2357. [Google Scholar] [CrossRef] [PubMed]
- Polito, M.D.; Farinatti, P.T.V. Comportamento da pressão arterial após exercícios contra-resistência: Uma revisão sistemática sobre variáveis determinantes e possíveis mecanismo. Rev. Bras. Med. Esporte 2006, 12, 386–392. [Google Scholar] [CrossRef]
- Rezk, C.C.; Marrache, R.C.; Tinucci, T.; Mion, D., Jr.; Forjaz, C.L. Post-resistance exercise hypotension, hemodynamics, and heart rate variability: Influence of exercise intensity. Eur. J. Appl. Physiol. 2006, 98, 105–112. [Google Scholar] [CrossRef] [PubMed]
- Negrão, C.E.; Rodon, M.U.P.B. Exercício físico hipertensão e controle barorreflexo da pressão arterial. Rev. Bras. Hypertens. 2001, 8, 89–95. [Google Scholar]
- Damorim, I.R.; Santos, T.M.; Barros, G.W.P.; Carvalho, P.R.C. Kinetics of Hypotension during 50 Sessions of Resistance and Aerobic Training in Hypertensive Patients: A Randomized Clinical Trial. Arq. Bras. Cardiol. 2017, 108, 323–330. [Google Scholar] [CrossRef]
- Boroujerd, S.S.; Rahimi, R.; Noori, S.R. Effect os high-versus low-intensity resistance training on post-exercise hypotension in male athletes. Int. Sport Med. J. 2009, 10, 95–100. [Google Scholar]
- Goto, C.; Higashi, Y.; Kimura, M.; Noma, K.; Hará, K.; Nakagawa, K.; Kawamura, M.; Chayama, K.; Yoshizumi, M.; Nara, I. Effect of different intensities of exercise on endothelium-dependent vasodilation in humans: Role of endothelium-dependent nitric oxide and oxidative stress. Circulation 2003, 108, 530–535. [Google Scholar] [CrossRef]
- Ribeiro Neto, F.; Dorneles, J.R.; Luna, R.M.; Spina, M.A.; Gonçalves, C.W.; Gomes Costa, R.R. Performance Differences Between the Arched and Flat Bench Press in Beginner and Experienced Paralympic Powerlifters. J. Strength Cond. Res. 2020. [epub ahead]. [Google Scholar] [CrossRef] [PubMed]
- García-Ramos, A.; Pérez-Castilla, A.; Villar Macias, F.J.; Latorre-Román, P.Á.; Párraga, J.A.; García-Pinillos, F. Differences in the one-repetition maximum and load-velocity profile between the flat and arched bench press in competitive powerlifters. Sports Biomech. 2021, 20, 261–273. [Google Scholar] [CrossRef] [PubMed]
| PP X ± SD (CI 95%) | CP X ± SD (CI 95%) | p | Cohen’s d | α | ICC | |
|---|---|---|---|---|---|---|
| Age (Years) | 26.10 ± 6.95 (21.13–31.07) | 23.20 ± 2.62 (21.33–25.07) | 0.242 | 0.55 | 0.208 | 0.197 |
| Body Mass (Kg) | 76.80 ± 17.42 (64.34–89.26) | 77.10 ± 7.68 (71.61–82.59) | 0.961 | 0.02 | 0.419 | 0.445 |
| Experience (Years) | 2.61 ± 0.46 (2.18–2.99) | 2.40 ± 0.16 (2.28–2.51) | 0.011 * | 0.61 | 0.18 | 0.017 |
| 1RM (Kg) | 123.00 ± 29.93 (101.59–144.41) | 92.80 ± 9.60 (85.93–99.67) | 0.006 * | 1.36 | 0.020 | 0.011 |
| 1RM/Body Mass | 1.64 ± 0.39 ** (1.36–1.92) | 1.21 ± 0.06 (1.16–1.25) | 0.201 | 1.54 | 0.049 | 0.023 |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Aidar, F.J.; Paz, Â.d.A.; Gama, D.d.M.; de Souza, R.F.; Vieira Souza, L.M.; Santos, J.L.d.; Almeida-Neto, P.F.; Marçal, A.C.; Neves, E.B.; Moreira, O.C.; et al. Evaluation of the Post-Training Hypotensor Effect in Paralympic and Conventional Powerlifting. J. Funct. Morphol. Kinesiol. 2021, 6, 92. https://doi.org/10.3390/jfmk6040092
Aidar FJ, Paz ÂdA, Gama DdM, de Souza RF, Vieira Souza LM, Santos JLd, Almeida-Neto PF, Marçal AC, Neves EB, Moreira OC, et al. Evaluation of the Post-Training Hypotensor Effect in Paralympic and Conventional Powerlifting. Journal of Functional Morphology and Kinesiology. 2021; 6(4):92. https://doi.org/10.3390/jfmk6040092
Chicago/Turabian StyleAidar, Felipe J., Ângelo de Almeida Paz, Dihogo de Matos Gama, Raphael Fabricio de Souza, Lúcio Marques Vieira Souza, Jymmys Lopes dos Santos, Paulo Francisco Almeida-Neto, Anderson Carlos Marçal, Eduardo Borba Neves, Osvaldo Costa Moreira, and et al. 2021. "Evaluation of the Post-Training Hypotensor Effect in Paralympic and Conventional Powerlifting" Journal of Functional Morphology and Kinesiology 6, no. 4: 92. https://doi.org/10.3390/jfmk6040092
APA StyleAidar, F. J., Paz, Â. d. A., Gama, D. d. M., de Souza, R. F., Vieira Souza, L. M., Santos, J. L. d., Almeida-Neto, P. F., Marçal, A. C., Neves, E. B., Moreira, O. C., Garrido, N. D., Cabral, B. G. A. T., Clemente, F. M., Reis, V. M., Nikolaidis, P. T., & Knechtle, B. (2021). Evaluation of the Post-Training Hypotensor Effect in Paralympic and Conventional Powerlifting. Journal of Functional Morphology and Kinesiology, 6(4), 92. https://doi.org/10.3390/jfmk6040092
















