Doppler Examination of the Testicular Artery of Beagle-Breed Dogs from Birth to Puberty
Abstract
1. Introduction
2. Materials and Methods
2.1. Animals
2.2. Ultrasonographic Examination of the Testes
2.3. Semen Collection and Quality Assessment
2.4. Data Management and Statistical Analysis
3. Results
3.1. Clinical Examination and Semen Examination
3.2. B-Mode Examination
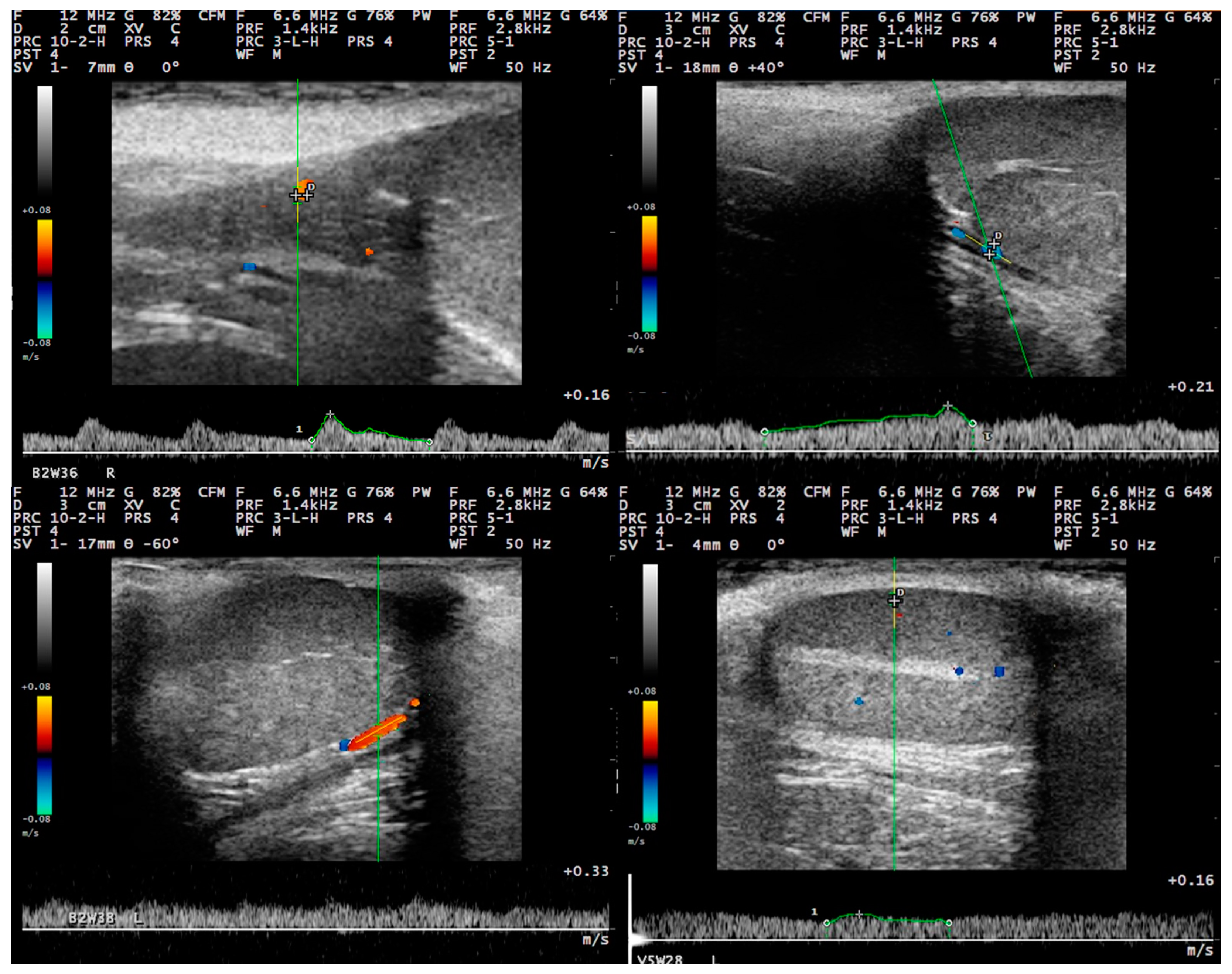
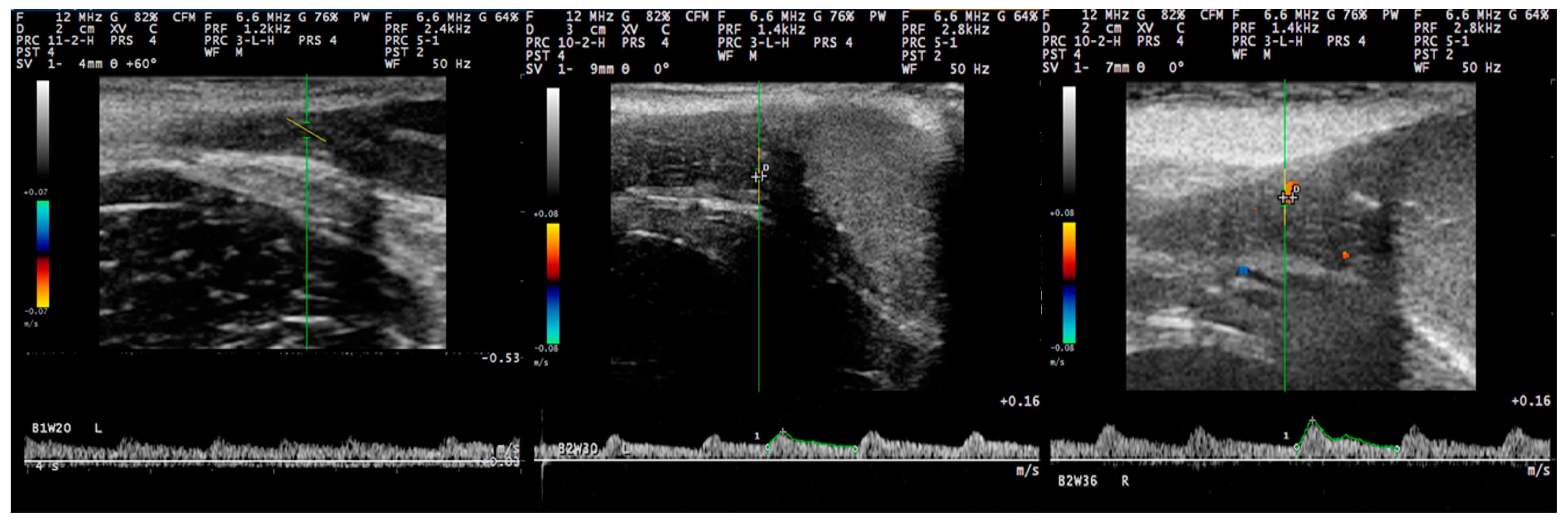
3.3. Pulsed-Wave Doppler
3.4. Correlations between Semen Evaluation Parameters and Haemodynamic Parameters
4. Discussion
4.1. Generalities
4.2. Differences in the Findings between the Regions of the Testis
4.3. Changes in Accord to Age
4.4. Proposed Segments of the Artery and Haemodynamic Parameters for Doppler Evaluation
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- De Souza, Μ.Β.; Silva, L.D.; Moxon, R.; Russo, M.; England, G.C.W. Ultrasonography of the prostate gland and testes in dogs. In Pract. 2017, 39, 21–32. [Google Scholar] [CrossRef]
- Spaziani, M.; Lecis, C.; Tarantino, C.; Sbardella, E.; Pozza, C.; Gianfrilli, D. The role of scrotal ultrasonography from infancy to puberty. Andrology 2021, 9, 1306–1321. [Google Scholar] [CrossRef] [PubMed]
- Orlandi, R.; Vallesi, E.; Boiti, C.; Polisca, A.; Bargellini, P.; Troisi, A. Characterization of testicular tumor lesions in dogs by different ultrasound techniques. Animals 2022, 12, 210. [Google Scholar] [CrossRef] [PubMed]
- Dogra, V.S.; Gottlieb, R.H.; Oka, M.; Rubens, D.J. Sonography of the scrotum. Radiology 2003, 227, 18–36. [Google Scholar] [CrossRef]
- Lerner, R.M.; Mevorach, R.A.; Hulbert, W.C.; Rabinowitz, R. Color Doppler US in the evaluation of acute scrotal disease. Radiology 1990, 176, 355–358. [Google Scholar] [CrossRef]
- Akand, M.; Koplay, M.; Islamoglu, N.; Altintas, E.; Kilic, O.; Gul, M.; Kulaksizoglu, H.; Sivri, M.; Goktas, S. Color Doppler ultrasound characteristics after subinguinal microscopic varicocelectomy. Med. Ultrason. 2017, 19, 59–65. [Google Scholar] [CrossRef]
- Lemos, H.; Dorado, J.; Hidalgo, M.; Gaivão, I.; Martins-Bessa, A. Assessment of dog testis perfusion by colour and pulsed-doppler ultrasonography and correlation with sperm oxidative DNA damage. Top. Companion Anim. Med. 2020, 41, 100452. [Google Scholar] [CrossRef]
- Mattoon, J.S.; Nyland, T.G. Chapter 17—Prostate and Testes. In Small Animal Diagnostic Ultrasound, 3rd ed.; Mattoon, J.S., Nyland, T.G., Eds.; Saunders, Elsevier: St. Louis, MO, USA, 2015; pp. 608–633. [Google Scholar]
- de Souza, M.B.; England, G.C.; Mota Filho, A.C.; Ackermann, C.L.; Sousa, C.V.; de Carvalho, G.G.; Silva, H.V.; Pinto, J.N.; Linhares, J.C.; Oba, E.; et al. Semen quality, testicular B-mode and Doppler ultrasound, and serum testosterone concentrations in dogs with established infertility. Theriogenology 2015, 84, 805–810. [Google Scholar] [CrossRef]
- Trautwein, L.G.C.; Souza, A.K.; Cardoso, G.S.; da Costa Flaiban, K.K.M.; de Oliveira Dearo, A.C.; Martins, M.I.M. Correlation of testicular artery Doppler velocimetry with kinetics and morphologic characteristics of epididymal sperm in dogs. Reprod. Dom. Anim. 2020, 55, 720–725. [Google Scholar] [CrossRef]
- Hedia, M.G.; El-Belely, M.S.; Ismail, S.T.; Abo El-Maaty, A.M. Monthly changes in testicular blood flow dynamics and their association with testicular volume, plasma steroid hormones profile and semen characteristics in rams. Theriogenology 2019, 123, 68–73. [Google Scholar] [CrossRef]
- Hassan, M.A.A.; Sayed, R.K.A.; Abdelsabour-Khalaf, M.; Abd-Elhafez, E.A.; Anel-Lopez, L.; Riesco, M.F.; Ortega-Ferrusola, C.; Montes-Garrido, R.; Neila-Montero, M.; Anel, L.; et al. Morphological and ultrasonographic characterization of the three zones of supratesticular region of testicular artery in Assaf rams. Sci. Rep. 2022, 12, 8334. [Google Scholar] [CrossRef]
- Samir, H.; Nyametease, P.; Elbadawy, M.; Nagaoka, K.; Sasaki, K.; Watanabe, G. Administration of melatonin improves testicular blood flow, circulating hormones, and semen quality in Shiba goats. Theriogenology 2020, 146, 111–119. [Google Scholar] [CrossRef]
- Abdelkhalek, K.G.; Badawy, A.B.A.; Abdelnaby, E.A.; Fathi, M. Relationship between main testicular hemodynamics and computerassisted analysis in prepubertal age for breeding selection in Baladi bucks. J. Adv. Vet. Res. 2022, 12, 54–61. [Google Scholar]
- Ortiz-Rodríguez, J.M.; Anel-Lopez, L.; Martín-Muñoz, P.; Álvarez, M.; Gaitskell-Phillips, G.; Anel, L.; Rodríguez-Medina, P.; Peña, F.J.; Ferrusola, O. Pulse Doppler ultrasound as a tool for the diagnosis of chronic testicular dysfunction in stallions. PLoS ONE 2017, 12, e0175878. [Google Scholar] [CrossRef]
- Abdelnaby, E.A.; Emam, I.A.; Fadl, A.M. Assessment of the accuracy of testicular dysfunction detection in male donkey (Equus asinus) with the aid of colour-spectral Doppler in relation to plasma testosterone and serum nitric oxide levels. Reprod. Dom. Anim. 2021, 56, 764–774. [Google Scholar] [CrossRef]
- Gloria, A.; Carluccio, A.; Wegher, L.; Robbe, D.; Valorz, C.; Contri, A. Pulse wave Doppler ultrasound of testicular arteries and their relationship with semen characteristics in healthy bulls. J. Anim. Sci. Biotechnol. 2018, 9, 14. [Google Scholar] [CrossRef]
- Kutzler, M.; Tyson, R.; Grimes, M.; Timm, K. Determination of testicular blood flow in camelids using vascular casting and color pulsed-wave Doppler ultrasonography. Vet. Med. Int. 2011, 2011, 638602. [Google Scholar] [CrossRef]
- Pozor, M.A. Evaluation of testicular vasculature in stallions. Clin. Tech. Equine Pract. 2007, 6, 271–277. [Google Scholar] [CrossRef]
- Velasco, A.; Ruiz, S. New approaches to assess fertility in domestic animals: Relationship between arterial blood flow to the testicles and seminal quality. Animals 2020, 11, 12. [Google Scholar] [CrossRef]
- Colli, L.G.; Belardin, L.B.; Echem, C.; Akamine, E.H.; Antoniassi, M.P.; Andretta, R.R.; Mathias, L.S.; Rodrigues, S.F.P.; Bertolla, R.P.; de Carvalho, M.H.C. Systemic arterial hypertension leads to decreased semen quality and alterations in the testicular microcirculation in rats. Sci. Rep. 2019, 9, 11047. [Google Scholar] [CrossRef]
- Zelli, R.; Troisi, A.; Elad Ngonput, A.; Cardinali, L.; Polisca, A. Evaluation of testicular artery blood flow by Doppler ultrasonography as a predictor of spermatogenesis in the dog. Res. Vet. Sci. 2013, 95, 632–637. [Google Scholar] [CrossRef]
- Carrillo, J.D.; Soler, M.; Lucas, X.; Agut, A. Colour and pulsed Doppler ultrasonographic study of the canine testis. Reprod. Dom. Anim. 2012, 47, 655–659. [Google Scholar] [CrossRef] [PubMed]
- de Souza, M.B.; da Cunha Barbosa, C.; Pereira, B.S.; Monteiro, C.L.; Pinto, J.N.; Linhares, J.C.; da Silva, L.D. Doppler velocimetric parameters of the testicular artery in healthy dogs. Res. Vet. Sci. 2014, 96, 533–536. [Google Scholar] [CrossRef] [PubMed]
- Ntemka, A.; Kiossis, E.; Boscos, C.; Theodoridis, A.; Kourousekos, G.; Tsakmakidis, I. Effects of testicular hemodynamic and echogenicity changes on ram semen characteristics. Reprod. Dom. Anim. 2018, 53, 50–55. [Google Scholar] [CrossRef] [PubMed]
- Wood, M.M.; Romine, L.E.; Lee, Y.K.; Richman, K.M.; O’Boyle, M.K.; Paz, D.A.; Chu, P.K.; Pretorius, D.H.D.A. Spectral Doppler signatures waveforms in ultrasonography. Ultrasound Q. 2010, 26, 283–299. [Google Scholar] [CrossRef]
- Paltiel, H.J.; Rupich, R.C.; Babcock, D.S. Maturational changes in arterial impedance of the normal testis in boys: Doppler sonographic study. Am. J. Roentgenol. 1994, 163, 1189–1193. [Google Scholar] [CrossRef]
- de Souza, M.B.; Barbosa, C.C.; England, G.C.; Mota Filho, A.C.; Sousa, C.V.; de Carvalho, G.G.; Silva, H.V.; Pinto, J.N.; Linhares, J.C.; Silva, L.D. Regional differences of testicular artery blood flow in post pubertal and pre-pubertal dogs. BMC Vet. Res. 2015, 11, 47. [Google Scholar] [CrossRef]
- Baez, A.D.; Cabrera, W.R.; Llano, E.G. Origen de las arterias testiculares en caninos. Rev. Veter. 2007, 18, 53–54. [Google Scholar]
- Harrison, R.G.; Weiner, J.S. Vascular patterns of the mammalian testis and their functional significance. J. Exp. Biol. 1949, 26, 304–316. [Google Scholar] [CrossRef]
- Strina, A.; Corda, A.; Nieddu, S.; Solinas, G.; Lilliu, M.; Zedda, M.T.; Pau, S.; Ledda, S. Annual variations in resistive index (RI) of testicular artery, volume measurements and testosterone levels in bucks. Comp. Clin. Pathol. 2016, 25, 409–413. [Google Scholar] [CrossRef]
- Gouletsou, P.G.; Galatos, A.D.; Leontides, L.S.; Sideri, A.I. Impact of fine- or large-needle aspiration on canine testes: Clinical, in vivo ultrasonographic and seminological assessment. Reprod. Dom. Anim. 2011, 46, 712–719. [Google Scholar] [CrossRef]
- Cicirelli, V.; Aiudi, G.G.; Carbonara, S.; Caira, M.; Lacalandra, G.M. Case of anorchia in a mixed-breed dog. Top. Companion Anim. Med. 2021, 45, 100554. [Google Scholar] [CrossRef]
- Cicirelli, V.; Burgio, M.; Mrenoshki, D.; Cseh, S.; Aiudi, G.; Lacalandra, G.M. Update on canine anorchia: A review. Vet. Med. Sci. 2023, 9, 600–603. [Google Scholar] [CrossRef]
- Semiz, I.; Tokgöz, O.; Tokgoz, H.; Voyvoda, N.; Serifoglu, I.; Erdem, Z. The investigation of correlation between semen analysis parameters and intraparenchymal testicular spectral Doppler indices in patients with clinical varicocele. Ultrasound Q. 2014, 30, 33–40. [Google Scholar] [CrossRef]
- Moxon, R.; Bright, L.; Pritchard, B.; Bowen, I.M.; de Souza, M.B.; da Silva, L.D.; England, G.C. Digital image analysis of testicular and prostatic ultrasonographic echogencity and heterogeneity in dogs and the relation to semen quality. Anim. Reprod. Sci. 2015, 160, 112–119. [Google Scholar] [CrossRef]
- Kay, G.W.; Grobbelaar, J.A.; Hattingh, J. Effect of surgical restric-tion of growth of the testicular artery on testis size and histology in bulls. J. Reprod. Fert. 1992, 96, 549–553. [Google Scholar] [CrossRef]
- Batissaco, L.; Celeghini, E.C.C.; Pinaffi, F.L.V.; Oliveira, B.M.M.; de Andrade, A.F.C.; de Recalde, E.C.S.; Fernandes, C.B. Correlations between testicular hemodynamic and sperm characteristics in rams. Vet. Res. Anim. Sci. 2013, 50, 384–395. [Google Scholar]
- Elbaz, H.; Elweza, A.E.; Sharshar, A.M. Testicular color doppler ultrasonography in Barki rams. Alex. J. Vet. Sci. 2019, 61, 39–45. [Google Scholar] [CrossRef]
- England, G.; Bright, L.; Pritchard, B.; Bowen, I.M.; de Souza, M.B.; Silva, L.; Moxon, R. Canine reproductive ultrasound examination for predicting future sperm quality. Reprod. Dom. Anim. 2017, 52, 202–207. [Google Scholar] [CrossRef]
- Srivastava, S.; Panchal, S.; Nagori, C.; Thaker, M. Doppler parameters of intratesticular vessels in male factor sub fertility. Andrology 2021, 10, 1000230. [Google Scholar]
- Aguilar-García, J.; Cano-González, H.; Martínez-Jiménez, M.; de la Rosa-Zapata, F.; Sánchez-Aguilar, M. Unilateral Lichtenstein tension-free mesh hernia repair and testicular perfusion: A prospective control study. Hernia 2018, 22, 479–482. [Google Scholar] [CrossRef] [PubMed]
- Maulik, D. Spectral Doppler sonography. Waveform analysis and hemodynamic interpretation. In Doppler Ultrasound in Obstetrics and Gynecology, 2nd ed.; Maulik, D., Ed.; Springer Verlag: Berlin, Germany, 2005; pp. 35–56. [Google Scholar]
- Pozor, M.A.; McDonnell, S.M. Color Doppler ultrasound evaluation of testicular blood flow in stallions. Theriogenology 2004, 61, 799–810. [Google Scholar] [CrossRef] [PubMed]
- Trautwein, L.G.C.; Souza, A.K.; Martins, M.I.M. Can testicular artery Doppler velocimetry values change according to the measured region in dogs? Reprod. Dom. Anim. 2019, 54, 687–695. [Google Scholar] [CrossRef] [PubMed]
- Gumbsch, P.; Holzmann, A.; Gabler, C. Colour-coded duplex sonography of the testes in dogs. Vet. Rec. 2002, 151, 140–144. [Google Scholar] [CrossRef] [PubMed]
- Samir, H.; ElSayed, M.I.; Radwan, F.; Hedia, M.; Hendawy, H.; Hendawy, A.O.; Elbadawy, M.; Watanabe, G. An updated insight on testicular hemodynamics: Environmental, physiological, and technical perspectives in farm and companion animals. Vet. Res. Commun. 2023, 47, 323–345. [Google Scholar] [CrossRef]
- Ahmadi, B.; Lau, C.P.; Giffin, J.; Santos, N.; Hahnel, A.; Raeside, J.; Christie, H.; Bartlewski, P. Suitability of epididymal and testicular ultrasonography and computerized image analysis for assessment of current and future semen quality in the ram. Exp. Biol. Med. 2012, 237, 186–193. [Google Scholar] [CrossRef]
- Elayat, M.A.; Khalil, K.M.; Farag, F.M.; Rizk, H.M. Gross anatomical studies on the pattern and density of the tunica vasculosa testis in some farm animals (buffalo, ram, camel donkey and rabbit). Benha Med. J. 2014, 26, 1–9. [Google Scholar]
- Gacem, S.; Papas, M.; Catalan, J.; Miró, J. Examination of jackass (Equus asinus) accessory sex glands by B-mode ultrasound and of testicular artery blood flow by colour pulsed-wave Doppler ultrasound: Correlations with semen production. Reprod. Dom. Anim. 2020, 55, 181–188. [Google Scholar] [CrossRef]
- Pinggera, G.M.; Mitterberger, M.; Bartsch, G.; Strasser, H.; Gradl, J. Assessment of the intratesticular resistive index by colour Doppler ultrasonography measurements as a predictor of spermatogenesis. BJU Int. 2008, 101, 722–726. [Google Scholar] [CrossRef]
- Middleton, W.D.; Thorne, D.A.; Melson, G.L. Color Doppler ultrasound of the normal testis. Am. J. Roentgenol. 1989, 152, 293–297. [Google Scholar] [CrossRef]
- Ortega-Ferrusola, C.; Gracia-Calvo, L.A.; Ezquerra, J.; Pena, F.J. Use of colour and spectral Doppler ultrasonography in stallion andrology. Reprod. Dom. Anim. 2014, 49, 88–96. [Google Scholar] [CrossRef]
- Saunders, H.M.; Burns, P.N.; Needleman, L.; Liu, J.B.; Boston, R.; Wortman, J.A.; Chan, L. Hemodynamic factors affecting uterine artery Doppler waveform pulsatility in sheep. J. Ultrasound Med. 1998, 17, 357–368. [Google Scholar] [CrossRef]
- Dudea, S.M.; Ciurea, A.; Chiorean, A.; Botar-Jid, C. Doppler applications in testicular and scrotal disease. Med. Ultrason. 2010, 12, 43–51. [Google Scholar]
- Luker, G.D.; Siegel, M.J. Scrotal US in pediatric patients: Comparison of power and standard color Doppler US. Radiology 1996, 198, 381–385. [Google Scholar] [CrossRef]
- Bader, T.R.; Kammerhuber, F.; Herneth, A.M. Testicular blood flow in boys as assessed at color Doppler and power Doppler sonography. Radiology 1997, 202, 559–564. [Google Scholar] [CrossRef]
- Tarhan, S.; Ucer, O.; Sahin, M.O.; Gumus, B. Long-term effect of microsurgical inguinal varicocelectomy on testicular blood flow. J. Androl. 2010, 32, 33–39. [Google Scholar] [CrossRef]
- Marchesini, A.C.; Magrio, F.A.; Berezowski, A.T.; Neto, O.B.; Nogueira, A.A.; Candido dos Reis, F.J. A critical analysis of Doppler velocimetry in the differential diagnosis of malignant and benign ovarian masses. J. Wom. Health 2008, 17, 97–102. [Google Scholar] [CrossRef]
- Sladkevicius, P.; Valentin, L. Reproducibility of doppler measurements of blood flow velocity in the uterine and ovarian arteries in premenopausal women. Ultrasound Med. Biol. 1995, 21, 313. [Google Scholar] [CrossRef]
- Biagiotti, G.; Cavallini, G.; Modenini, F.; Vitali, G.; Gianaroli, L. Spermatogenesis and spectral echo-colour Doppler traces from the main testicular artery. BJU Int. 2002, 90, 903–908. [Google Scholar] [CrossRef]
- Jee, W.H.; Choe, B.Y.; Byun, J.Y.; Shinn, K.S.; Hwang, T.K. Resistive index of the intrascrotal artery in scrotal inflammatory disease. Acta Radiol. 1997, 38, 1026–1030. [Google Scholar] [CrossRef]
- Wielgoś, M.; Bablok, L.; Fracki, S.; Marianowski, L. Doppler flowmetry measurements in testicular artery of aging men. Ginekol. Pol. 1998, 69, 537–540. [Google Scholar] [PubMed]
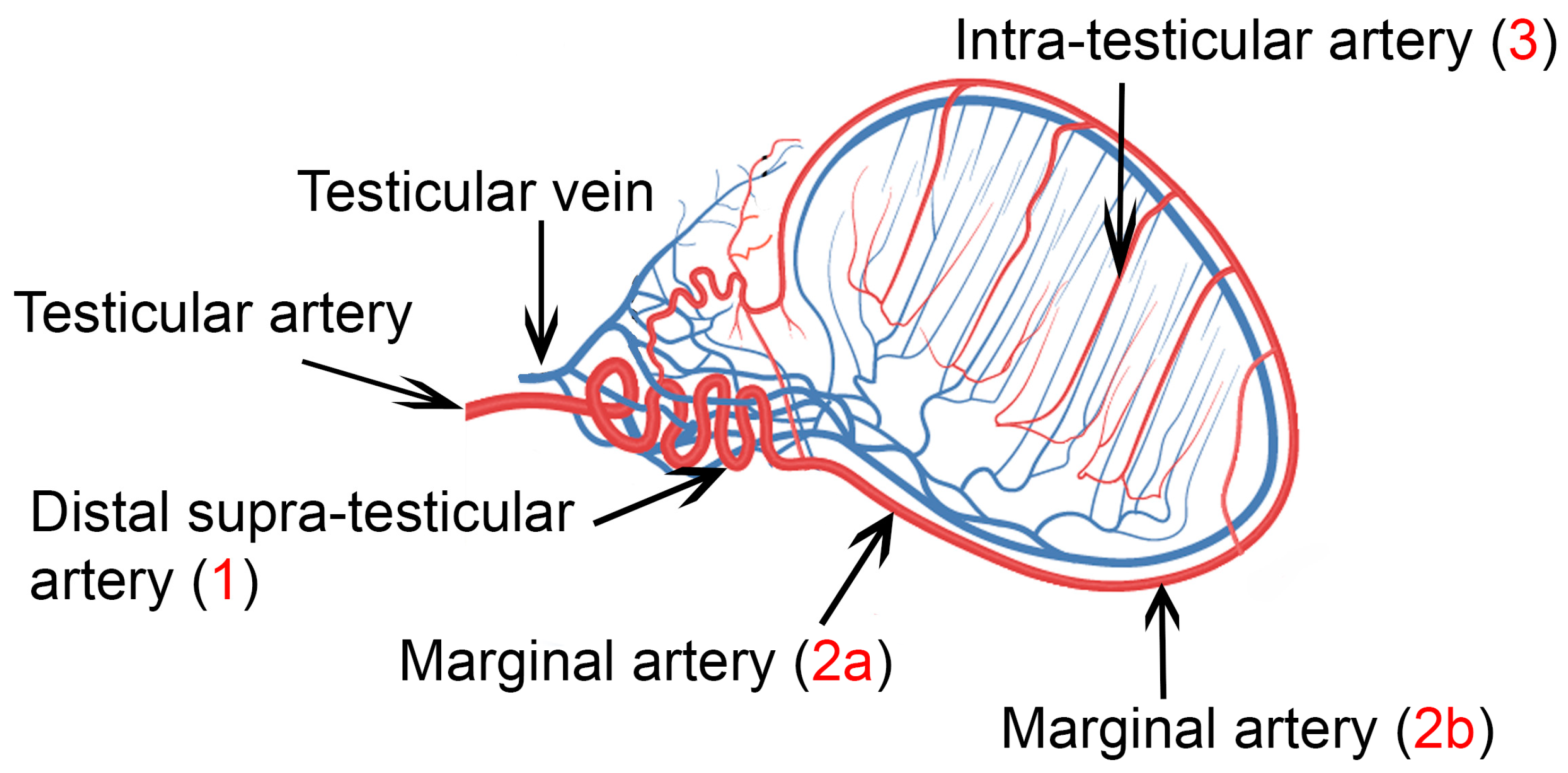
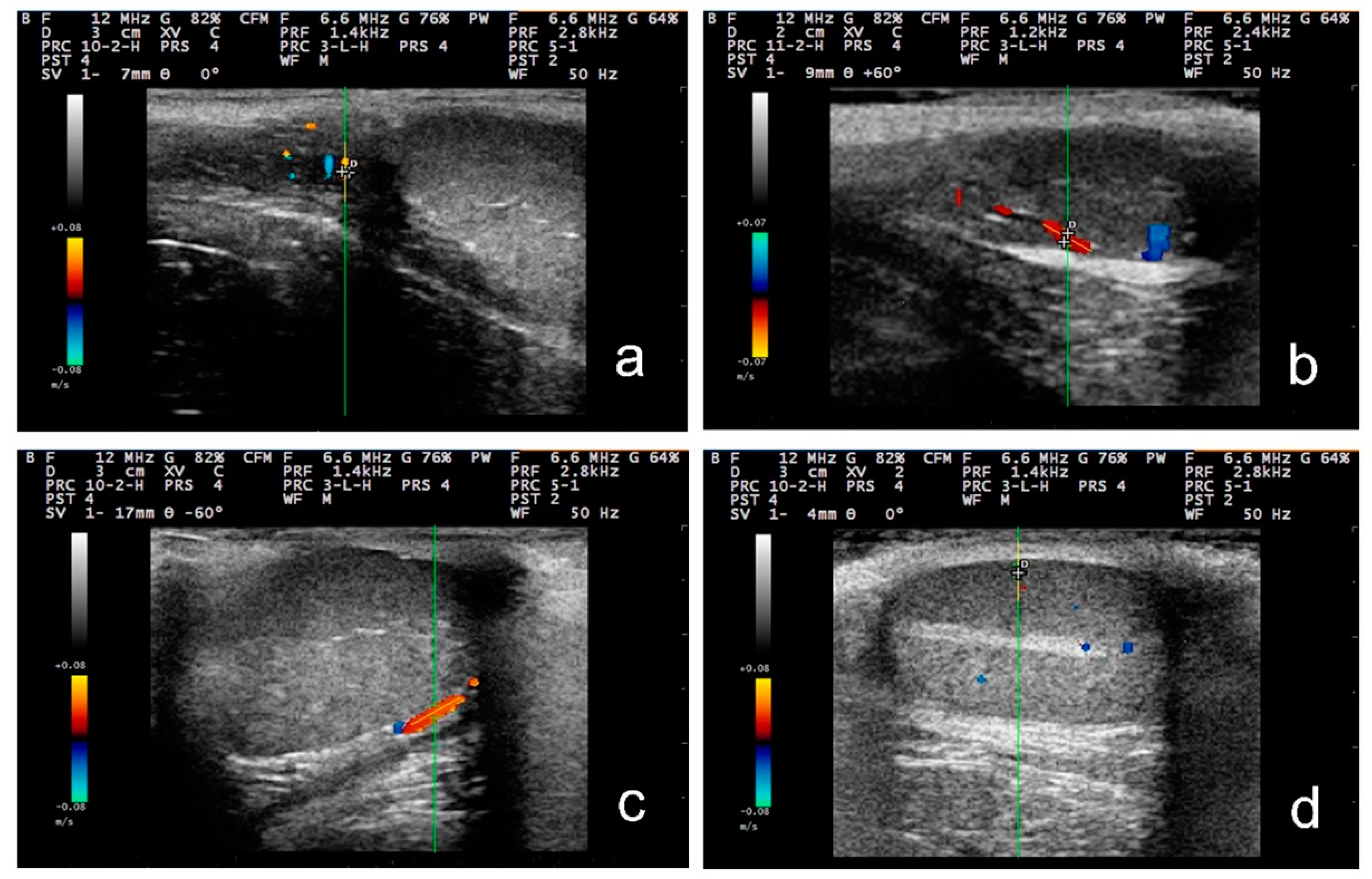
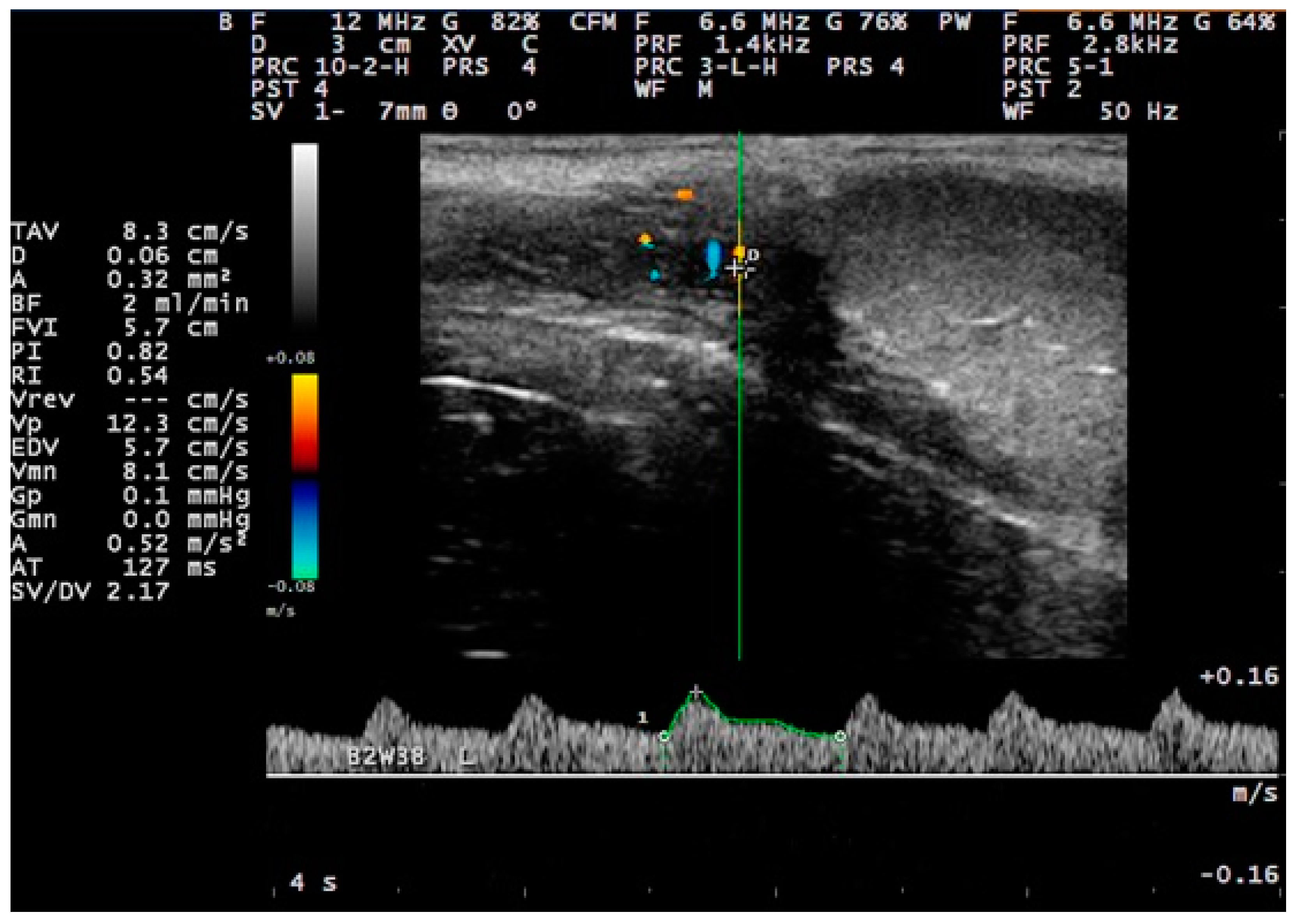
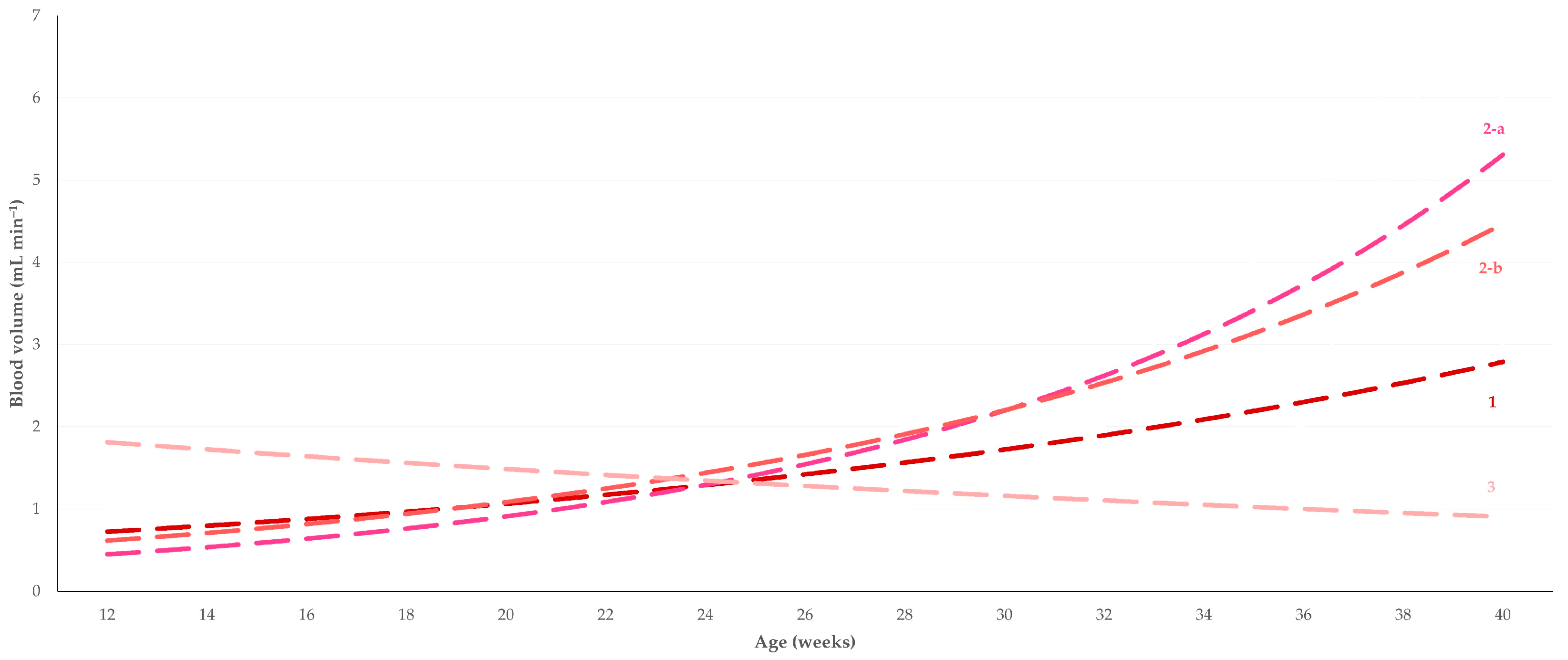

| Segment of the Testicular Artery | Age of Animals | ||
|---|---|---|---|
| Weeks 4–28 (Pre-Pubertal Period) | Weeks 30–34 (Pubertal Period) | Weeks 36–40 (Post-Pubertal Period) | |
| Peak Systolic Velocity (m s−1) | |||
| Distal supra-testicular (region 1 of the testis) | 9.8 (4.9–21.9) a | 8.2 (6.2–16.7) a,b | 9.5 (6.8–16.4) b |
| Marginal-a (region 2 of the testis) | 8.4 (6.4–14.3) a | 9.0 (6.2–12.1) b | 11.9 (6.2–16.1) a,b |
| Marginal-b (region 2 of the testis) | 9.0 (4.4–15.9) | 7.5 (7.0–14.4) | 9.2 (7.0–18.0) |
| Intratesticular (region 3 of the testis) | 5.1 (3.2–8.5) | 4.0 (2.9–8.1) | 5.2 (5.0–5.4) |
| End Diastolic Velocity (m s−1) | |||
| Distal supra-testicular (region 1 of the testis) | 4.2 (1.9–8.1) a | 3.3 (2.6–6.3) a | 5.0 (2.6–7.7) |
| Marginal-a (region 2 of the testis) | 5.0 (2.9–8.2) | 5.2 (3.1–6.8) | 5.8 (3.1–10.0) |
| Marginal-b (region 2 of the testis) | 4.9 (2.6–8.6) | 4.6 (3.5–8.1) | 5.6 (3.5–7.1) |
| Intratesticular (region 3 of the testis) | 5.8 (3.6–9.3) | 4.2 (3.1–8.9) | 5.3 (5.3–5.3) |
| Systolic: Diastolic Velocity Ratio | |||
| Distal supra-testicular (region 1 of the testis) | 2.3 (1.6–4.3) a | 2.8 (1.7–4.1) a | 2.4 (1.7–3.7) |
| Marginal-a (region 2 of the testis) | 1.9 (1.4–2.3) | 1.9 (1.5–2.5) | 1.9 (1.5–2.4) |
| Marginal-b (region 2 of the testis) | 1.9 (1.3–3.0) | 1.8 (1.6–2.0) a | 2.1 (1.6–2.5) a |
| Intratesticular (region 3 of the testis) | 1.3 (1.1–1.9) | 1.4 (1.1–1.8) | 1.1 (1.1–1.1) |
| Systolic Acceleration (m s−2) | |||
| Distal supra-testicular (region 1 of the testis) | 0.45 (0.20–3.39) a | 0.41 (0.32–0.89) a | 0.41 (0.31–1.06) |
| Marginal-a (region 2 of the testis) | 0.35 (0.19–0.50) | 0.35 (0.22–0.40) | 0.42 (0.22–0.64) |
| Marginal-b (region 2 of the testis) | 0.30 (0.06–0.50) | 0.29 (0.20–0.65) | 0.35 (0.20–0.71) |
| Intratesticular (region 3 of the testis) | 0.18 (0.04–0.25) | 0.20 (0.01–0.25) | 0.05 (0.05–0.05) |
| Resistance Index | |||
| Distal supra-testicular (region 1 of the testis) | 0.68 (0.35–1.45) a | 0.71 (0.41–1.70) a | 0.62 (0.41–1.37) |
| Marginal-a (region 2 of the testis) | 0.45 (0.24–0.61) | 0.42 (0.32–0.60) | 0.50 (0.32–0.58) |
| Marginal-b (region 2 of the testis) | 0.44 (0.20–0.67) | 0.42 (0.38–0.50) a | 0.47 (0.38–0.61) a |
| Intratesticular (region 3 of the testis) | 0.10 (0.09–0.37) | 0.09 (0.06–0.22) | 0.08 (0.06–0.10) |
| Pulsatility Index | |||
| Distal supra-testicular (region 1 of the testis) | 0.84 (0.44–1.70) a | 1.10 (0.52–1.70) a | 0.89 (0.52–1.37) |
| Marginal-a (region 2 of the testis) | 0.58 (0.33–0.89) | 0.54 (0.40–1.03) | 0.71 (0.40–0.88) |
| Marginal-b (region 2 of the testis) | 0.57 (0.24–1.14) | 0.49 (0.58–0.74) a | 0.65 (0.49–1.01) a |
| Intratesticular (region 3 of the testis) | 0.11 (0.09–0.46) | 0.09 (0.07–0.25) | 0.08 (0.07–0.09) |
| Blood Volume (mL min−1) | |||
| Distal supra-testicular (region 1 of the testis) | 1 (1–5) a,b | 2 (1–5) a,c | 3 (1–9) b,c |
| Marginal-a (region 2 of the testis) | 1 (1–3) a,b | 2.5 (1–9) a,c | 4.5 (2–9) b,c |
| Marginal-b (region 2 of the testis) | 1 (1–5) a,b | 1 (1–5) a,c | 5 (1–7) b,c |
| Intratesticular (region 3 of the testis) | 1 (1–1) | 1 (1–2) | 1 (1–1) |
| Diameter (cm) | |||
| Distal supra-testicular (region 1 of the testis) | 0.02 (0.01–0.30) a,b | 0.08 (0.03–0.80) a | 0.08 (0.05–0.14) b |
| Marginal-a (region 2 of the testis) | 0.06 (0.01–0.10) a | 0.09 (0.04–0.70) | 0.12 (0.08–0.15) a |
| Marginal-b (region 2 of the testis) | 0.01 (0.01–0.14) a,b | 0.07 (0.01–0.12) a,c | 0.11 (0.03–0.11) b,c |
| Intratesticular (region 3 of the testis) | 0.01 (0.01–0.09) | 0.02 (0.01–0.09) | 0.04 (0.01–0.06) |
| Haemodynamic Parameters | Semen Evaluation Parameters | ||
|---|---|---|---|
| Motility | Total No. of Spermatozoa in Ejaculate | Sperm Viability | |
| Peak Systolic Velocity | 0.415 (0.044) | 0.436 (0.016) | ns |
| End Diastolic Velocity | 0.490 (0.014) | 0.520 (0.003) | ns |
| Systolic: Diastolic Velocity Ratio | ns 1 | ns | ns |
| Systolic Acceleration | ns | ns | ns |
| Resistance Index | ns | −0.335 (0.047) | ns |
| Pulsatility Index | ns | ns | ns |
| Blood Volume | 0.519 (0.010) | 0.493 (0.007) | ns |
| Diameter | ns | ns | ns |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Venianaki, A.P.; Barbagianni, M.S.; Fthenakis, G.C.; Galatos, A.D.; Gouletsou, P.G. Doppler Examination of the Testicular Artery of Beagle-Breed Dogs from Birth to Puberty. Tomography 2023, 9, 1408-1422. https://doi.org/10.3390/tomography9040112
Venianaki AP, Barbagianni MS, Fthenakis GC, Galatos AD, Gouletsou PG. Doppler Examination of the Testicular Artery of Beagle-Breed Dogs from Birth to Puberty. Tomography. 2023; 9(4):1408-1422. https://doi.org/10.3390/tomography9040112
Chicago/Turabian StyleVenianaki, Athina P., Mariana S. Barbagianni, George C. Fthenakis, Apostolos D. Galatos, and Pagona G. Gouletsou. 2023. "Doppler Examination of the Testicular Artery of Beagle-Breed Dogs from Birth to Puberty" Tomography 9, no. 4: 1408-1422. https://doi.org/10.3390/tomography9040112
APA StyleVenianaki, A. P., Barbagianni, M. S., Fthenakis, G. C., Galatos, A. D., & Gouletsou, P. G. (2023). Doppler Examination of the Testicular Artery of Beagle-Breed Dogs from Birth to Puberty. Tomography, 9(4), 1408-1422. https://doi.org/10.3390/tomography9040112








