Pericardial Calcification: An Uncommon Case with Intraventricular Extension
Abstract
1. Introduction
2. Case Presentation
2.1. Patient Information
2.2. Past Medical History and Interventions
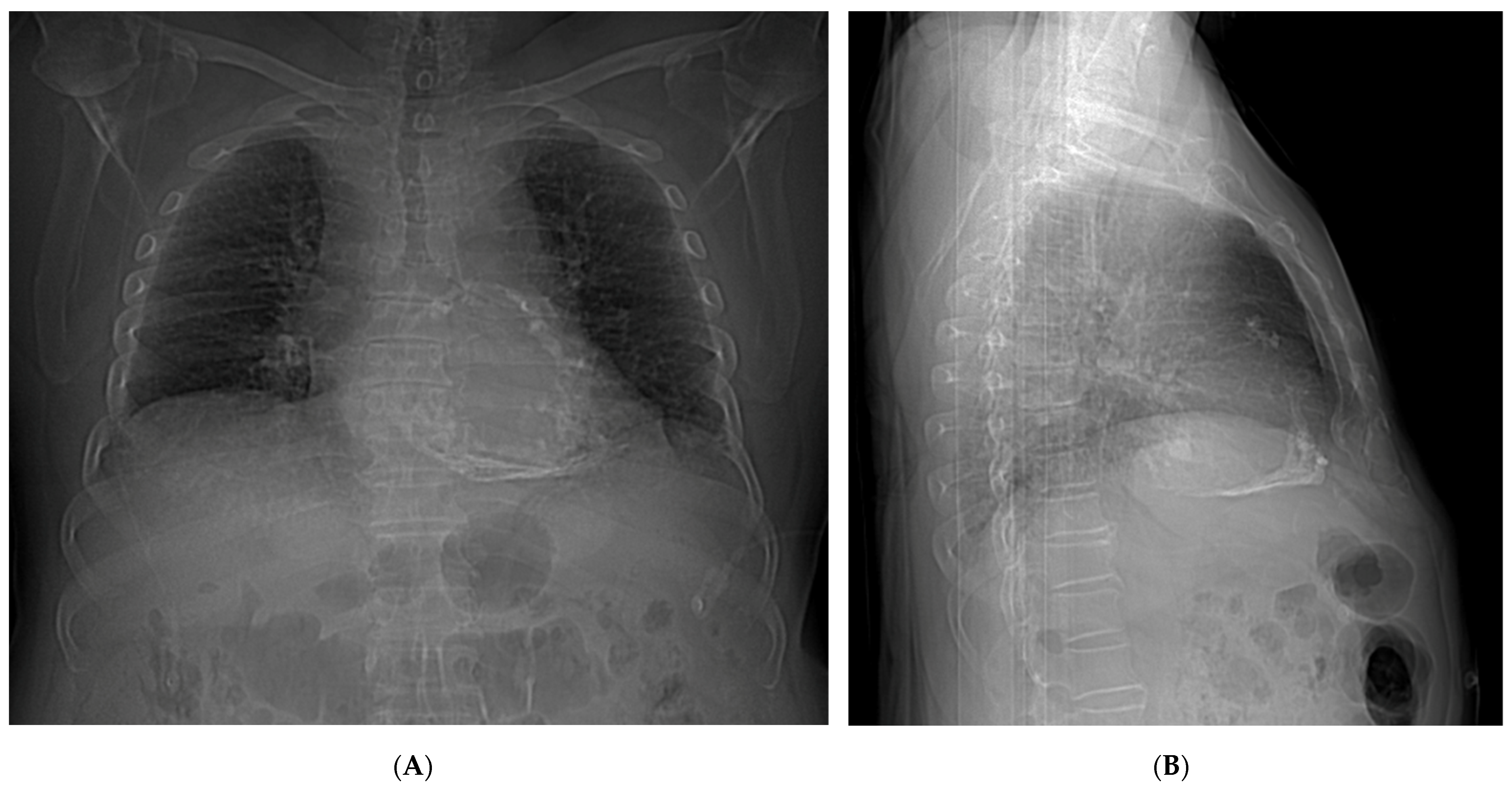
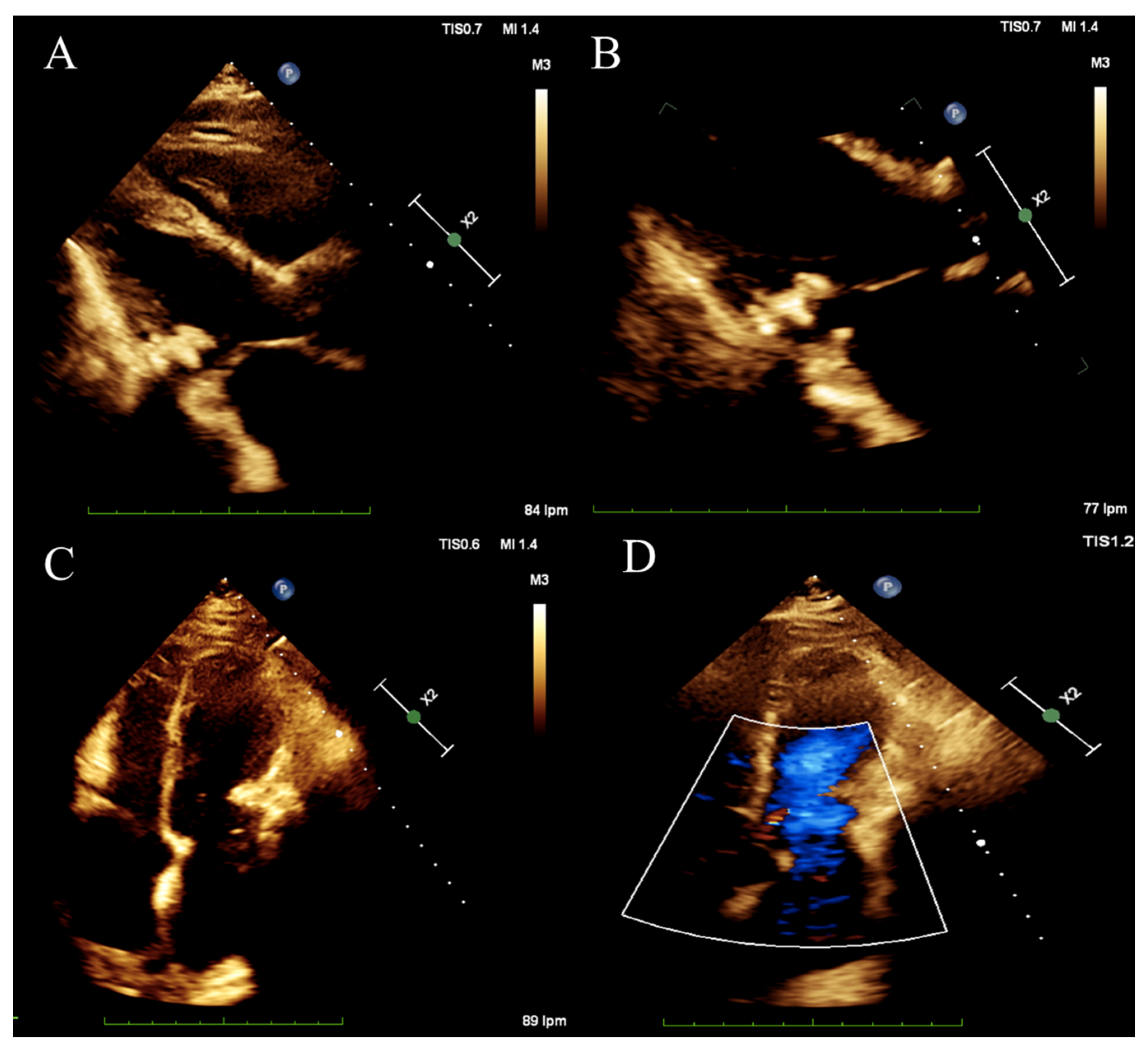
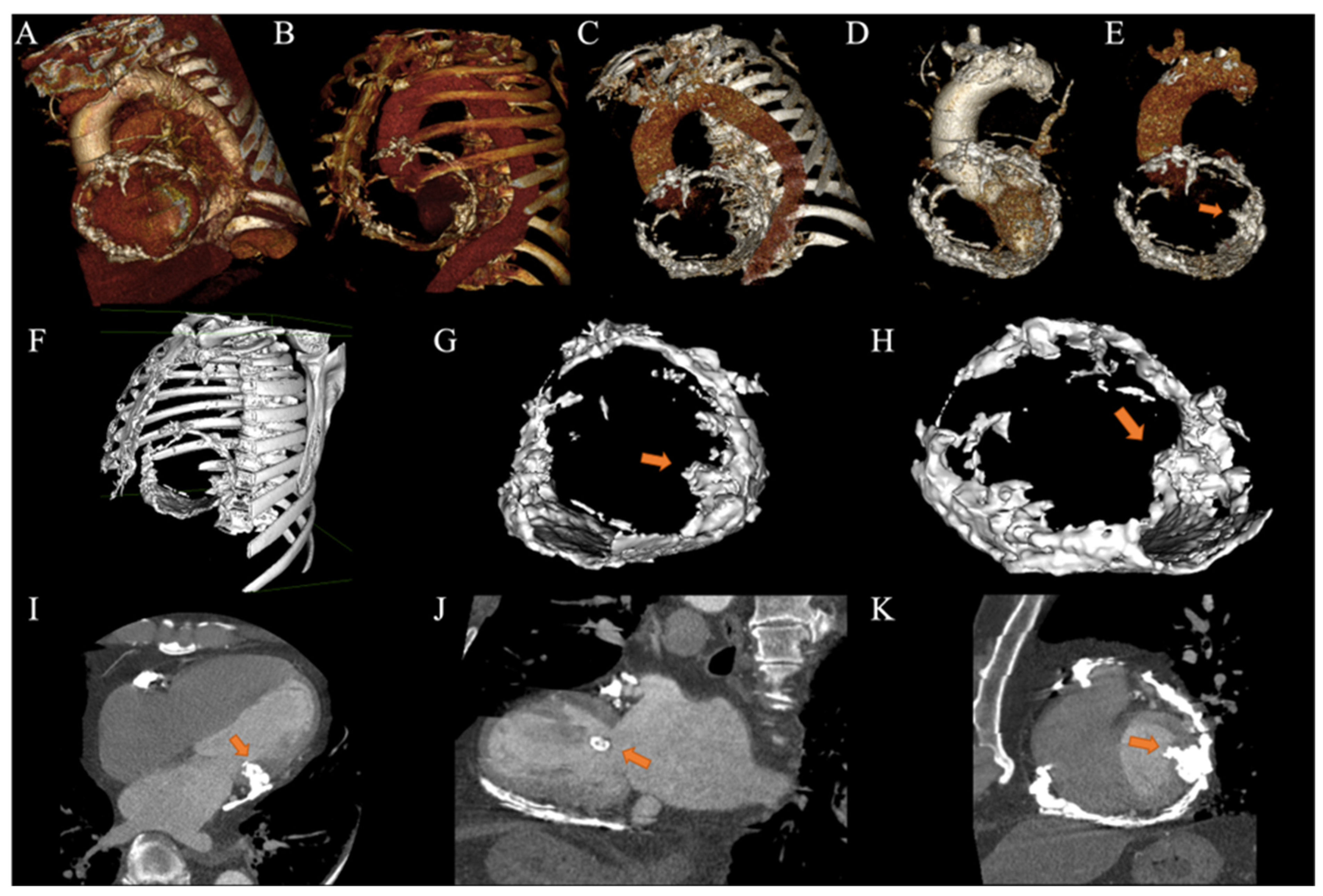
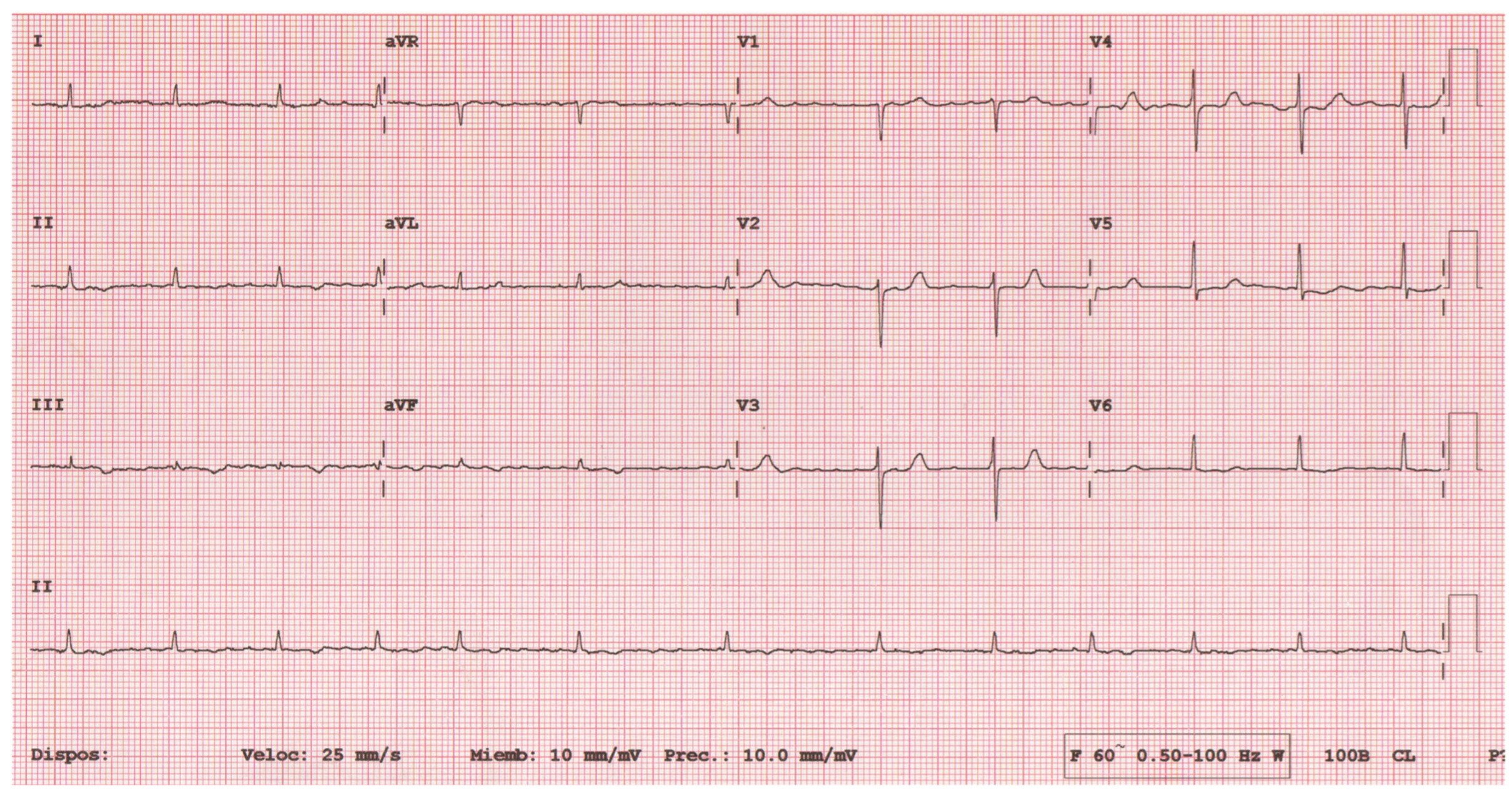
2.3. Clinical Findings
3. Discussion
4. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Mori, M.; Mullan, C.W.; Bin Mahmood, S.U.; Yousef, S.; Pelletier, K.J.; Mangi, A.A.; Geirsson, A. US national trends in the management and outcomes of constrictive pericarditis: 2005–2014. Can. J. Cardiol. 2019, 35, 1394–1399. [Google Scholar] [CrossRef] [PubMed]
- Khalid, N.; Hussain, K.; Shlofmitz, E. Pericardial Calcification. 2023 May 22. In StatPearls [Internet]; StatPearls Publishing: Treasure Island, FL, USA, 2024. [Google Scholar] [PubMed]
- Nguyen, T.; Phillips, C.; Movahed, A. Incidental findings of pericardial calcification. World J. Clin. Cases. 2014, 2, 455–458. [Google Scholar] [CrossRef] [PubMed]
- Umer, A.; Khalid, N.; Chhabra, L.; Memon, S.; Spodick, D.H. Constrictive pericarditis complicating cardiac transplantation. J. Cardiothorac. Surg. 2015, 10, 109. [Google Scholar] [CrossRef] [PubMed]
- Welch, T.D.; Oh, J.K. Constrictive Pericarditis. Cardiol. Clin. 2017, 35, 539–549. [Google Scholar] [CrossRef] [PubMed]
- Miranda, W.R.; Oh, J.K. Constrictive Pericarditis: A Practical Clinical Approach. Prog. Cardiovasc. Dis. 2017, 59, 369–379. [Google Scholar] [CrossRef] [PubMed]
- Syed, F.F.; Schaff, H.V.; Oh, J.K. Constrictive pericarditis—A curable diastolic heart failure. Nat. Rev. Cardiol. 2014, 11, 530–544, Erratum in Nat. Rev. Cardiol. 2015, 12, 682. [Google Scholar] [CrossRef] [PubMed]
- Ohri, R.; Salhiyyah, K.; Harding, S.; Ohri, S. Pericardial calcification: A case report of a three-dimensional disease. Int. J. Surg. Case Rep. 2019, 57, 152–154. [Google Scholar] [CrossRef] [PubMed]
- Oh, K.Y.; Shimizu, M.; Edwards, W.D.; Tazelaar, H.D.; Danielson, G.K. Surgical pathology of the parietal pericardium: A study of 344 cases (1993–1999). Cardiovasc Pathol. 2001, 10, 157–168. [Google Scholar] [CrossRef] [PubMed]
- Wang, L.; Cao, X.; Xue, J.; Li, H.; Shi, L.; Men, Y. Echocardiographic features of right ventricular diverticulum: A case report. J. Clin. Ultrasound. 2017, 45, 531–534. [Google Scholar] [CrossRef] [PubMed]
- Bouwman, R.A.; van Schijndel, R.J. Images in clinical medicine. Pericardial calcification noted long after Sydenham’s chorea. N. Engl. J. Med. 2009, 361, 1386. [Google Scholar] [CrossRef] [PubMed]
- von Erffa, J.; Daniel, W.G.; Achenbach, S. Three-dimensional visualization of severe pericardial calcification in constrictive pericarditis using multidetector-row computed tomography. Eur. Heart J. 2006, 27, 275. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Tugcu, A.; Yildirimturk, O.; Duran, C.; Aytekin, S. Constrictive pericarditis impressing and narrowing the ascending aorta. Echocardiography 2008, 25, 768–771. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Santaularia-Tomas, M.; Sanchez-Felix, E.; Santos-Zaldivar, K.; Grosjean-Alvarez, A.; Mendez-Dominguez, N. Pericardial Calcification: An Uncommon Case with Intraventricular Extension. Tomography 2024, 10, 1024-1030. https://doi.org/10.3390/tomography10070076
Santaularia-Tomas M, Sanchez-Felix E, Santos-Zaldivar K, Grosjean-Alvarez A, Mendez-Dominguez N. Pericardial Calcification: An Uncommon Case with Intraventricular Extension. Tomography. 2024; 10(7):1024-1030. https://doi.org/10.3390/tomography10070076
Chicago/Turabian StyleSantaularia-Tomas, Miguel, Ely Sanchez-Felix, Kassandra Santos-Zaldivar, Allison Grosjean-Alvarez, and Nina Mendez-Dominguez. 2024. "Pericardial Calcification: An Uncommon Case with Intraventricular Extension" Tomography 10, no. 7: 1024-1030. https://doi.org/10.3390/tomography10070076
APA StyleSantaularia-Tomas, M., Sanchez-Felix, E., Santos-Zaldivar, K., Grosjean-Alvarez, A., & Mendez-Dominguez, N. (2024). Pericardial Calcification: An Uncommon Case with Intraventricular Extension. Tomography, 10(7), 1024-1030. https://doi.org/10.3390/tomography10070076







