Research Engagement Changes Attitudes and Behaviours towards Agrichemical Safety in Australian Farmers
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design
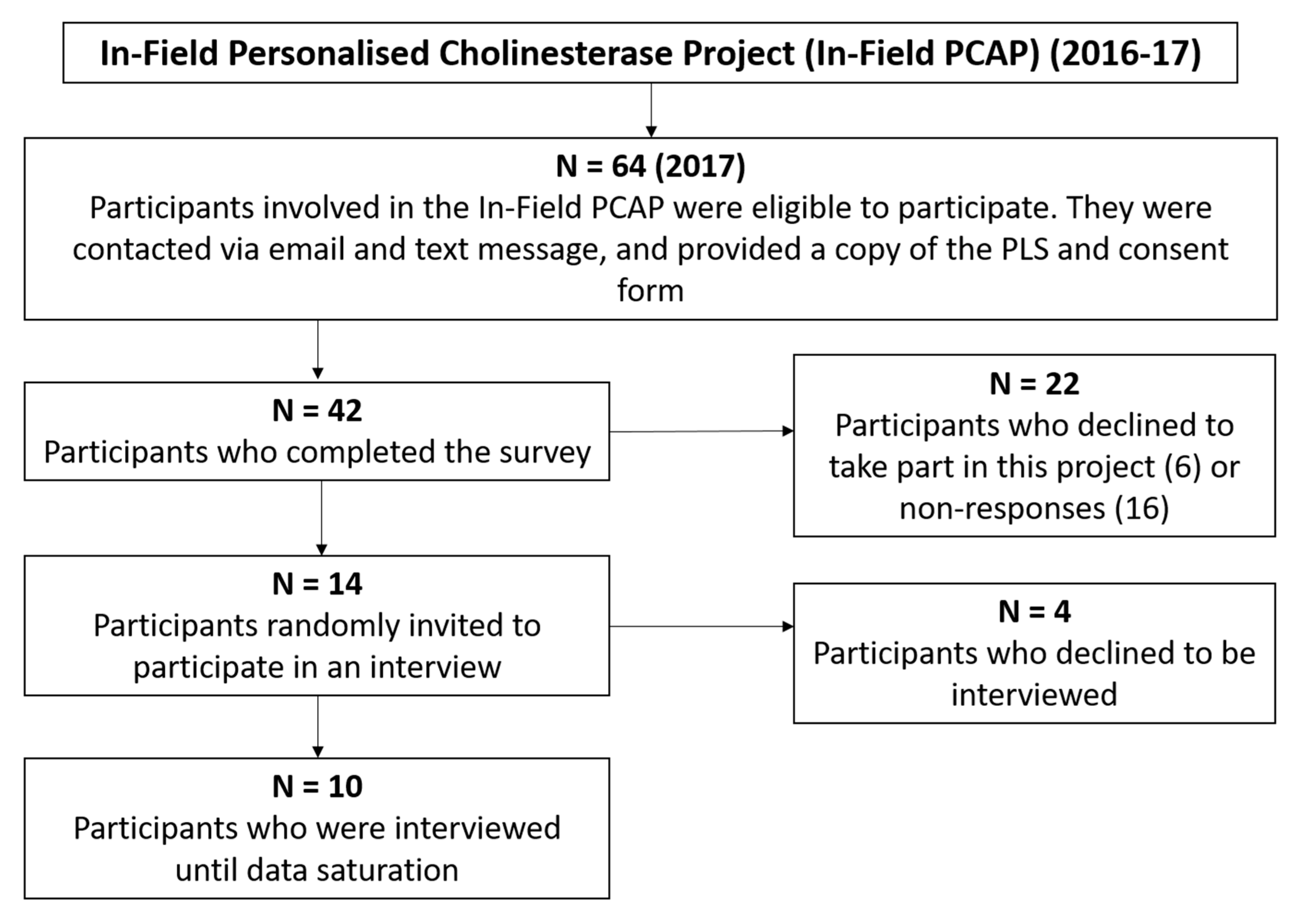
2.2. Participants
2.3. Sample
2.4. Ethics
2.5. Data Collection
2.6. Survey
2.7. Interview
2.8. Data Analyses
3. Results
3.1. Quantitative Results
3.1.1. Demographics
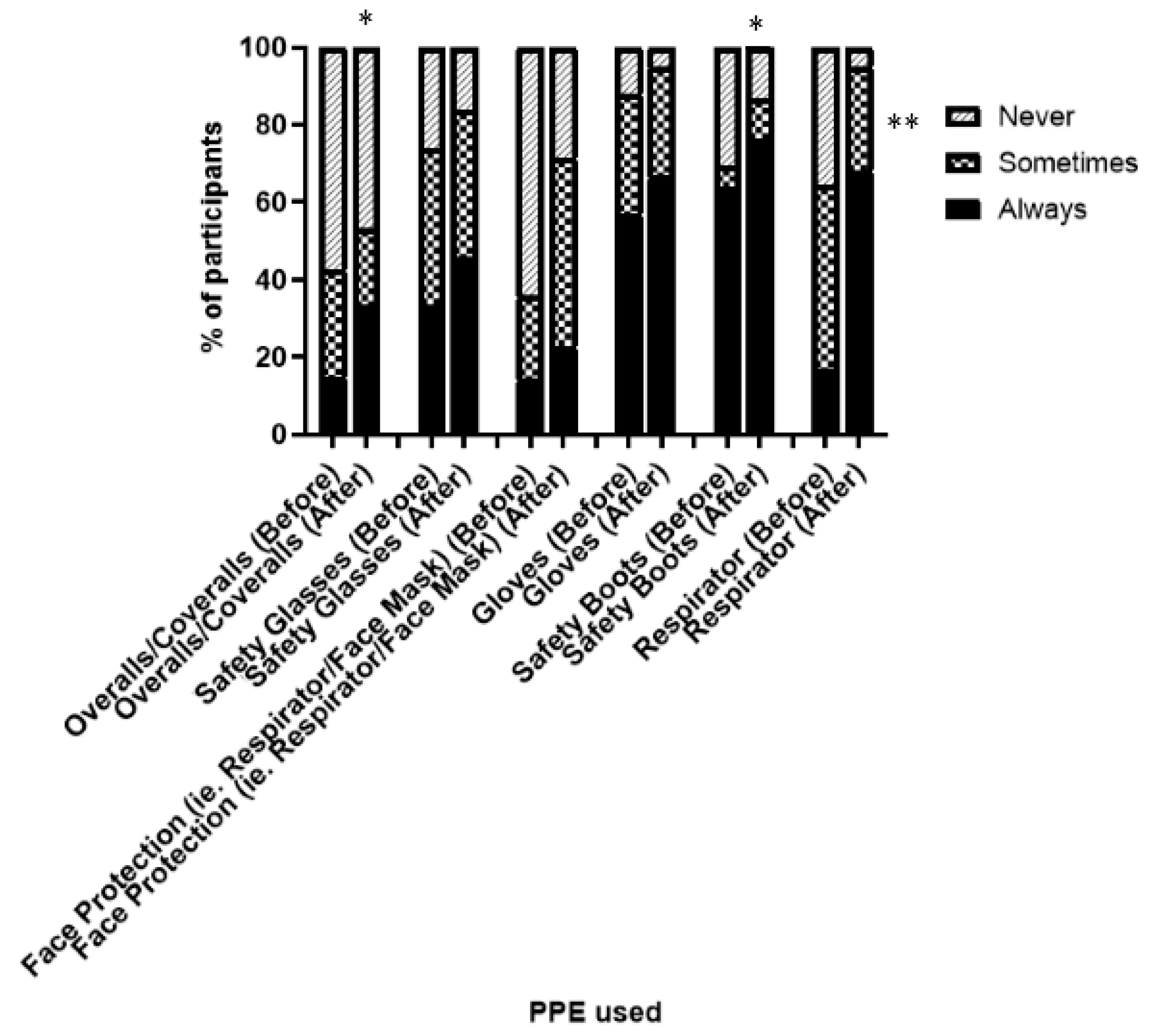
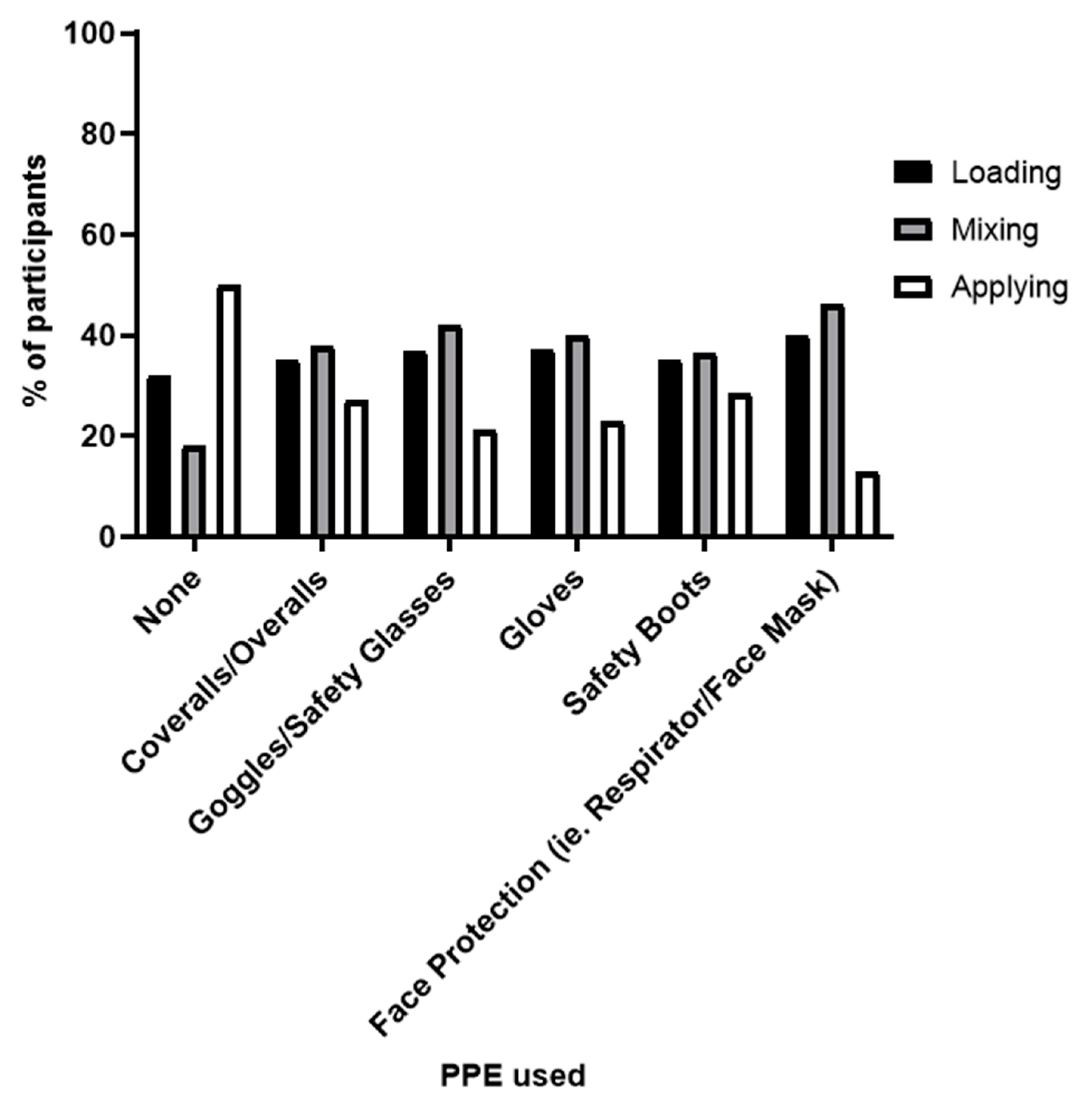
3.1.2. Use of Personal Protective Equipment (PPE)
3.2. Qualitative Results
“It was interesting to see how much chemical I was exposed to, and how my levels might peak and trough in relation to use of agrichemicals”.—John * (*name changed)
“There was initial skepticism when it first began, but when I started to see a correlation, my option changed. Visualising personal results was key in helping to change attitudes toward agrichemicals”.—(James*, Farmer)
‘I think the take home is that you can’t be safe enough.… you’ve just got to think it out and think what the consequences are of everything you do. Now having said that, I wish I knew that forty of fifty years ago’.—(Lou, Farmer)
4. Discussion
4.1. Principal Findings
4.2. Role of Training and Education
4.3. A Model for Engagement and Behaviour Change
4.4. Limitations
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Appendix A
| Question | |
|---|---|
| 1. | I have read the Plain Language Statement & Consent Form, and by signing my name below, I agree to participate in this study |
| 2. | Including yourself, who currently lives in your home? |
| 3. | What is your current degree or level of education you have completed? If currently enrolled, what is your highest degree received? |
| 4. | In general, how would you describe your health? |
| 5. | How often do you consume alcohol? |
| 6. | How often do you have more than 4 standard drinks (if female) or 6 standard drinks (if male) in one day? |
| 7. | Which statement best describes your smoking behaviour? |
| 8. | Do you personally apply agrichemicals on your farm? |
| 9. | What method/s do you use to apply agrichemicals on your farm? Please select all that apply. |
| 10. | In the past year, which of the following agrichemicals were used on your farm? Were they self-applied? |
| 11. | In the past year, which of the following classes of agrichemicals were used on your farm? Were they self-applied? Insecticides, Herbicides, Fungicides, Fumigants, |
| 12. | Do you read the safety instructions on the label of agrichemicals used on your farm? Always, Sometimes, Never |
| 13 | What type of Personal Protective Equipment (PPE) do you usually wear when loading, mixing or applying agrichemicals? None, Overalls, Mask/Respirator, Googles/Safety glasses, Gloves, Face Protection, Safety Boots. (Loading, Mixing, Applying) |
| 14. | How frequently do you wear the following types of PPE when loading, mixing or applying agrichemicals? Always, Sometimes, Never, Not Applicable. |
| 15. | Do you wear respiratory protection? i.e. respirator, face mask. Yes, No. |
| 16. | Do you usually wear your respiratory protection when exposed to: Grain Dust, Sheep, Silo Dust, Treating and processing livestock, Feeding livestock, Washing and Disinfecting, Preparing spray equipment? |
| 17. | If you have a tractor with a cabin, do you use a carbon filter when applying agrichemicals? Yes, No, Not Applicable. |
| 18. | After use, do you take your PPE into the household? Yes, No, Not Applicable. |
| 19. | If you self-apply chemicals; I wear clean washed clothes everyday, I change my clothes immediately after a spill, I wash my clothes separately, I wash my hands before eating, I wash my hands before urinating. (Always, Sometimes, Never) |
| 20. | Do you clean your PPE regularly or when advised? Yes, No, I don’t know when is appropriate. |
| 21. | Do you check your PPE for wear and damage? Yes, No |
| 22. | In the past year, how have your work clothes usually been washed when you have been handling agrichemicals? Mix them with family wash, Soak them separately then wash in communal machine, Wash in machine only for this purpose, Wear disposable clothing. |
| 23. | In the past year, when you have been handling agrichemicals, how long would you usually work with the same pair of gloves before changing them for a new pair? Every time, At least once a month, 1–4 times per session, I do not change my gloves until they are visibly worn out, I wear disposable gloves, Do not wear gloves. |
| 24. | In the past year, how has agrichemical-applying equipment usually been washed at the end of application? Clean the nozzle, Rinse the tank, Hose down the sprayer, Hose down the tractor, Do not wash equipment, I don’t know, Other (specify) |
| 25. | Do you usually wear sunglasses as a form of PPE when loading, mixing agrichemicals? Yes, No |
| 26. | When you work directly in the sun, what type/s of sun protection do you usually use? Sunscreen, Sunglasses, Baseball cap, Another type of hat with a brim, long sleeved shirt, None of the above |
| 27. | Do you believe that your participation in the In-Field PCAP research has changed the way you handle organophosphates? Likert Scale of responses |
| 28. | Do you believe that your participation in the In-Field PCAP has been beneficial in any way? Likert Scale of responses |
Appendix B. Interview Questions
References
- National Institute of Environmental Health Sciences Pesticides. Available online: https://www.niehs.nih.gov/health/topics/agents/pesticides/index.cfm (accessed on 21 November 2018).
- Australian Pesticides and Veterinary Medicines Authority Understanding Pesticide Labels. Available online: https://apvma.gov.au/node/11041 (accessed on 21 November 2018).
- De, A.; Bose, R.; Kumar, A.; Mozumdar, S. Worldwide Pesticide Use. In Targeted Delivery of Pesticides Using Biodegradable Polymeric Nanoparticles; Science, S.I.M., Ed.; Springer: Berlin/Heidelberg, Germany, 2013. [Google Scholar]
- Tabucanon, M.; Boonyatumanond, R. Pesticide Residues in Food and the Environment in Thailand; Seeking Agricultural Produce Free of Pesticide Residues, Canberra; Kennedy, I.R., Skerritt, J.H., Johnson, G.I., Highley, E., Eds.; Australian Centre for International Agricultural Research (ACIAR): Canberra, Australian, 1998; pp. 64–73.
- U.N Human Rights Council. Report of the Special Rapporteur on the Right to Food; (A/HRC/34/48); United Nations General Assembly, Human Rights Council: Hinebra, Switzerland, 2017. [Google Scholar]
- Konradsen, F. Acute pesticide poisoning—A global public health problem. Dan. Med. Bull. 2007, 54, 58–59. [Google Scholar]
- Pawlak, H.; Nowakowcz-Debek, B. Agriculture: Accident-prone Working Environment. Agric. Agric. Sci. Procedia 2015, 7, 209–214. [Google Scholar] [CrossRef]
- WorkSafe Victoria Farmers. Older Workers Dominate Workplace Death Toll. Available online: https://www.worksafe.vic.gov.au/news/2018-01/farmers-older-workers-dominate-workplace-death-toll (accessed on 17 December 2019).
- Cecchini, M.; Bedini, R.; Mosetti, D.; Marino, S.; Stasi, S. Safety Knowledge and Changing Behavior in Agricultural Workers: An Assessment Model Applied in Central Italy. Saf. Health Work 2018, 9, 164–171. [Google Scholar] [CrossRef] [PubMed]
- Hull, M.J.; Fennell, K.M.; Vallury, K.; Jones, M.; Ollman, J. A comparison of barriers to mental health support-seeking among farming and non-farming adults in rural South Australia. Aust. J. Rural Health 2018, 25, 347–353. [Google Scholar] [CrossRef] [PubMed]
- Marrs, T.C. Organophosphate poisoning. Pharmacol. Ther. 1993, 58, 15. [Google Scholar] [CrossRef]
- Robb, E.L.; Baker, M.B. Organophosphate Toxicity In Treasure Island (FL). Available online: https://www.ncbi.nlm.nih.gov/books/NBK470430 (accessed on 17 December 2019).
- Ellman, G.; Courtney, K.; Andres, V.; Featherstone, R. A new and rapid colorimetric determination of acetylcholinesterase activity. Biochem. Pharmacol. 1961, 7, 88–95. [Google Scholar] [CrossRef]
- English, K.; Jagals, P.; Ware, R.S.; Wylie, C.; Sly, P.D. Unintentional insecticide poisoning by age: An analysis of Queensland Poisons Information Centre calls. Aust. N. Z. J. Public Health 2016, 40, 457–461. [Google Scholar] [CrossRef]
- Perry, J.; Cotton, J.L.; Rahman, M.A.; Brumby, S.A. Organophosphate exposure and the chronic effects on farmers: A narrative review. Rural Remote Health 2020, 20, 39–55. [Google Scholar] [CrossRef]
- Khan, N.; Kennedy, A.; Cotton, J.; Brumby, S. A Pest to Mental Health? Exploring the link between exposure to agrichemicals in farmers and mental health. Int. J. Environ. Res. Public Health 2019, 16, 1327. [Google Scholar] [CrossRef]
- Ross, S.J.M.; Brewin, C.R.; Curran, H.V.; Furlong, C.E.; Abraham-Smith, K.M.; Harrison, V. Neuropsychological and psychiatric functioning in sheep farmers exposed to low levels of organophosphate pesticides. Neurotoxicol. Teratol. 2011, 32, 7. [Google Scholar]
- Stephens, R.; Spurgeon, A.; Berry, H. Organophosphates; the relationship between chronic and acute exposure effects. Neurotoxicol. Teratol. 1996, 18, 449–453. [Google Scholar] [CrossRef]
- Rohlman, D.S.; Anger, W.K.; Lein, P.J. Correlating neurobehavioural performance with biomarkers of organophosphorous pesticide exposure. Neurotoxicology 2010, 32, 268–276. [Google Scholar] [CrossRef] [PubMed]
- Jones, A.; Gray, B.; Schaefer, M. Chemcert AgVet Chemical Users Course Resource Manual; ChemCert Australia (Vic) Incorporated: Warragul, Australia, 2011. [Google Scholar]
- Remoundou, K.; Brennan, M.; Frewer, L.J.; Hart, A. Pesticide Risk Perceptions, Knowledge, and Attitudes of Operators, Workers, and Residents: A Review of the Literature. Hum. Ecol. Risk Assess. 2014, 20, 1113–1138. [Google Scholar] [CrossRef]
- Franklin, R.C.; McBain-Rigg, K.E.; King, J.C.; Lower, T. Exploring the Barriers and Facilitators to Adoption of Improved Work Practices for Safety in the Primary Industries; Rural Industries Research and Development Coporation: Barton, ACT, Australia, 2015. [Google Scholar]
- Cotton, J.; Lewandowski, P.; Brumby, S. Cholinesterase Research Outreach Project (CROP): Measuring cholinesterase activity and pesticide use in an agricultural community. BMC Public Health 2015, 15, 748. [Google Scholar] [CrossRef]
- De Vaus, D. Structured questionnaires and interviews. In Handbook for Research Methods in Health Sciences; Minichiello, V., Sullivan, G., Greenwood, K., Axford, R., Eds.; Addison-Wesley: Sydney, Australia, 1999. [Google Scholar]
- Cotton, J.; Edwards, J.; Rahman, M.A.; Brumby, S. Cholinesterase research outreach project (CROP): Point of care cholinesterase measurement in an Australian agricultural community. Environ. Health 2018, 17, 31. [Google Scholar] [CrossRef]
- MacFarlane, E.; Carey, R.; Keegal, T.; El-Zaemay, S.; Fritschi, L. Dermal Exposure Associated with Occupational End Use of Pesticides and the Role of Protective Measures. Saf. Health Work 2013, 4, 6. [Google Scholar] [CrossRef]
- Baldi, I.; Lebailly, P.; Jean, S.; Rougetet, L.; Dulaurent, S.; Marquet, P. Pesticide contamination of workers in vineyards in France. J. Expo. Sci. Environ. Epidemiol. 2006, 6, 9. [Google Scholar] [CrossRef]
- Luong Thanh, B.Y.; Laopaiboon, M.; Koh, D.; Sakunkoo, P.; Moe, H. Behavioural interventions to promote workers’ use of respiratory protective equipment. Cochrane Database Syst. Rev. 2016, 12. [Google Scholar] [CrossRef]
- Australian Bureau of Statistics. Agricultural Commodities, Australia, 2016–2017; Commonwealth of Australia: Canberra, Australia, 2018.
- Safe Work Australia. Work Health and Safety in the Agricultural Industry; Safe Work Australa: Canberra, Australia, 2016.
- Damalas, C.A.; Abdollahzadeh, G. Farmers’ use of personal protective equipment during handling of plant protection products: Determinants of implementation. Sci. Total Environ. 2016, 571, 730–736. [Google Scholar] [CrossRef]
- Lichtenberg, E.; Zimmerman, R. Adverse Health Experiences, Environmental Attitudes, and Pesticide Usage Behavior of Farm Operators. Risk Anal. 1999, 19, 283–294. [Google Scholar] [CrossRef]
- Jing, F.; Yanfang, L. Pesticide-related Food Safety Risks: Farmers’ Self-protective Behavior and Food Safety Social Co-governance. J. Resour. Ecol. 2018, 9, 59–65. [Google Scholar] [CrossRef]
- Kang, J.; O’Donnell, J.M.; Colaianne, B.; Bircher, N.; Ren, D.; Smith, K.J. Use of personal protective equipment among health care personnel: Results of clinical observations and simulations. Am. J. Infect. Control 2017, 45, 17–23. [Google Scholar] [CrossRef] [PubMed]
- Slovic, P. The Perception of Risk; Taylor & Francis Ltd.: London, UK, 2011; p. 511. [Google Scholar]
- Ajzen, I. The theory of planned behavior. Organ. Behav. Hum. Decis. Process. 1991, 50, 33. [Google Scholar] [CrossRef]


| Participation in PCAP | Behaviour Changes | Point of Care: Measurement of AChE and PChE and Baseline Health and Lifestyle Assessment (HLA) | Changes in Behaviour and Practices | Benefits of These Changes |
|---|---|---|---|---|
| Self-report | Measured at 10 time points over 12 months. | Projected changes | Estimated benefits | |
Pre-clinic
| Pre and Post
|
|
|
| Variables | Participants, n (%) |
|---|---|
| Total participants | 42 |
| Age (years) | |
| Mean (± SD) | 48.8 (± 12.5) |
| Age groups | |
| 25–44 years | 17 (40.4) |
| 45–64 years | 20 (47.6) |
| 65+ years | 5 (12) |
| Gender | |
| Male | 40 (95.2) |
| Female | 2 (4.8) |
| Education | |
| Did not finish Year 12 | 10 (24) |
| Year 12 or High School equivalent | 6 (14.4) |
| Certificate I–IV | 10 (24) |
| Diploma or Associate Degree | 7 (15.6) |
| Bachelors or Honours | 9 (22) |
| Masters or PhD | 0 (0) |
| Farming Type | |
| Primary Farming Type | |
| Beef Cattle | 4 (9.5) |
| Sheep Farming | 11 (26.2) |
| Broad-acre Cropping | 26 (61.9) |
| Dairy Cattle | 1 (2.4) |
| Pig Farming | |
| Secondary Farming Type | |
| Beef Cattle | 7 (16.6) |
| Sheep Farming | 22.5 (52.4) |
| Broad-acre Cropping | 3 (7.1) |
| Dairy Farming | 0 (0) |
| Pig Farming | 1 (2.3) |
| Nil | 8.5 (20.2) |
| Measure | Number of Participants | Correlation Coefficient - Age | p |
|---|---|---|---|
| Respirator | 42 | −0.390 | 0.0010 |
| Safety Glasses | 37 | 0.430 | 0.010 |
| Gloves | 39 | 0.386 | 0.015 |
| Measure | Gloves | Safety Glasses | Safety Boots | Overalls |
|---|---|---|---|---|
| --- | rs(36) = 0.443 (p < 0.05) | rs(37) = 0.475 (p < 0.05) | |
| rs(36) = 0.443 (p <0.05) | --- | rs(36) = 0.409 (p < 0.05) | rs(30) = 0.423 (p < 0.05) |
| rs(37) = 0.475 (p <0.05) | rs(36) = 0.409 (p < 0.05) | --- | rs(28) = 0.443 (p < 0.05) |
| rs(30) = 0.423 (p < 0.05) | rs(28) = 0.443 (p < 0.05) | --- |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Russell-Green, S.; Cotton, J.; Brumby, S. Research Engagement Changes Attitudes and Behaviours towards Agrichemical Safety in Australian Farmers. Safety 2020, 6, 16. https://doi.org/10.3390/safety6010016
Russell-Green S, Cotton J, Brumby S. Research Engagement Changes Attitudes and Behaviours towards Agrichemical Safety in Australian Farmers. Safety. 2020; 6(1):16. https://doi.org/10.3390/safety6010016
Chicago/Turabian StyleRussell-Green, Sienna, Jacqueline Cotton, and Susan Brumby. 2020. "Research Engagement Changes Attitudes and Behaviours towards Agrichemical Safety in Australian Farmers" Safety 6, no. 1: 16. https://doi.org/10.3390/safety6010016
APA StyleRussell-Green, S., Cotton, J., & Brumby, S. (2020). Research Engagement Changes Attitudes and Behaviours towards Agrichemical Safety in Australian Farmers. Safety, 6(1), 16. https://doi.org/10.3390/safety6010016





