KLVFF Conjugated Curcumin Microemulsion-Based Hydrogel for Transnasal Route: Formulation Development, Optimization, Physicochemical Characterization, and Ex Vivo Evaluation
Abstract
1. Introduction
2. Results and Discussion
2.1. Physicochemical Characterization of ME and Microemulsion-Based Hydrogel
2.2. Fourier Transform Infrared (FTIR) Spectroscopy
2.3. Anticholinesterase Activity
2.4. Anti-Aggregation of Beta-Amyloid
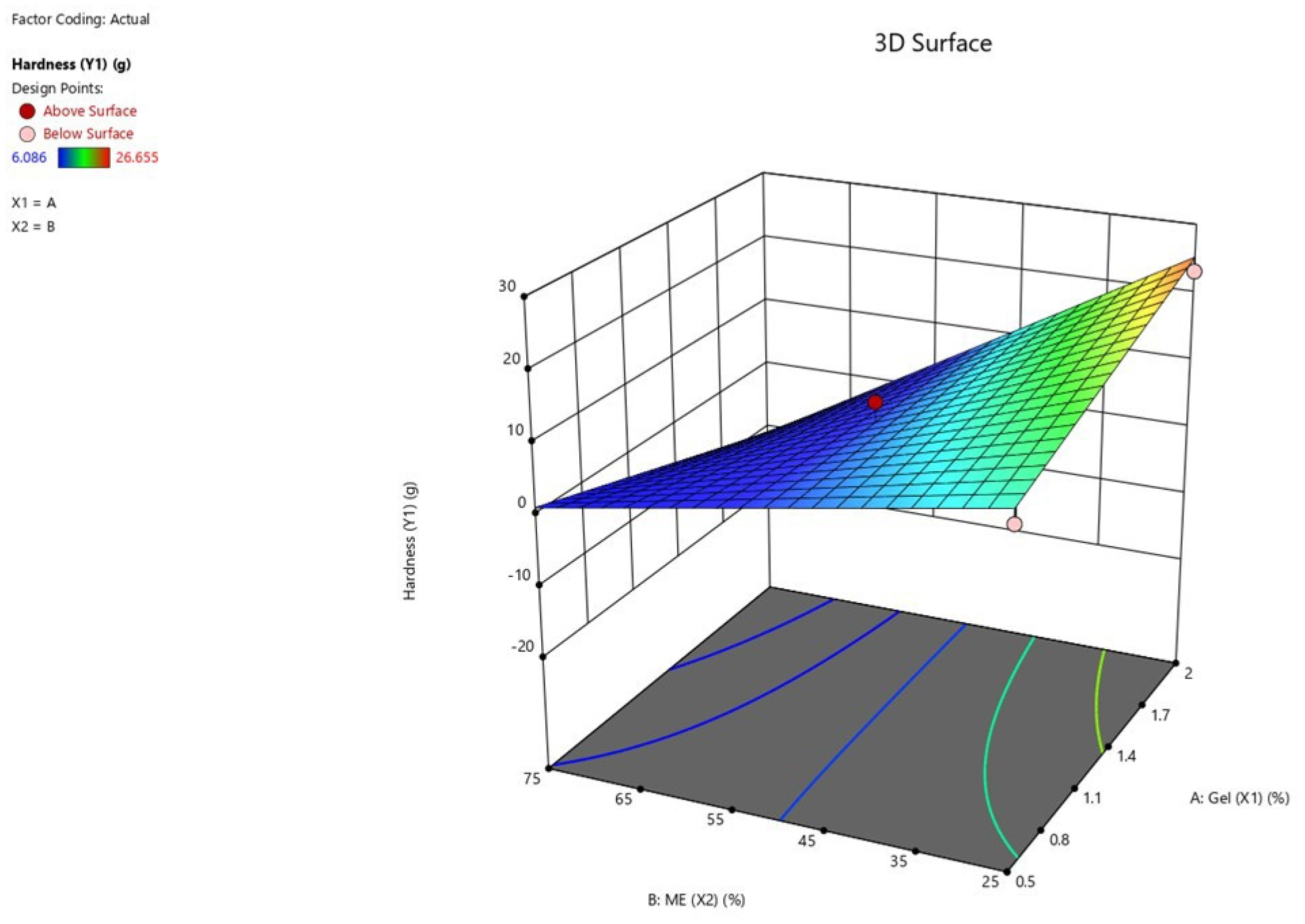
2.5. Formulation Optimization and Data Analysis
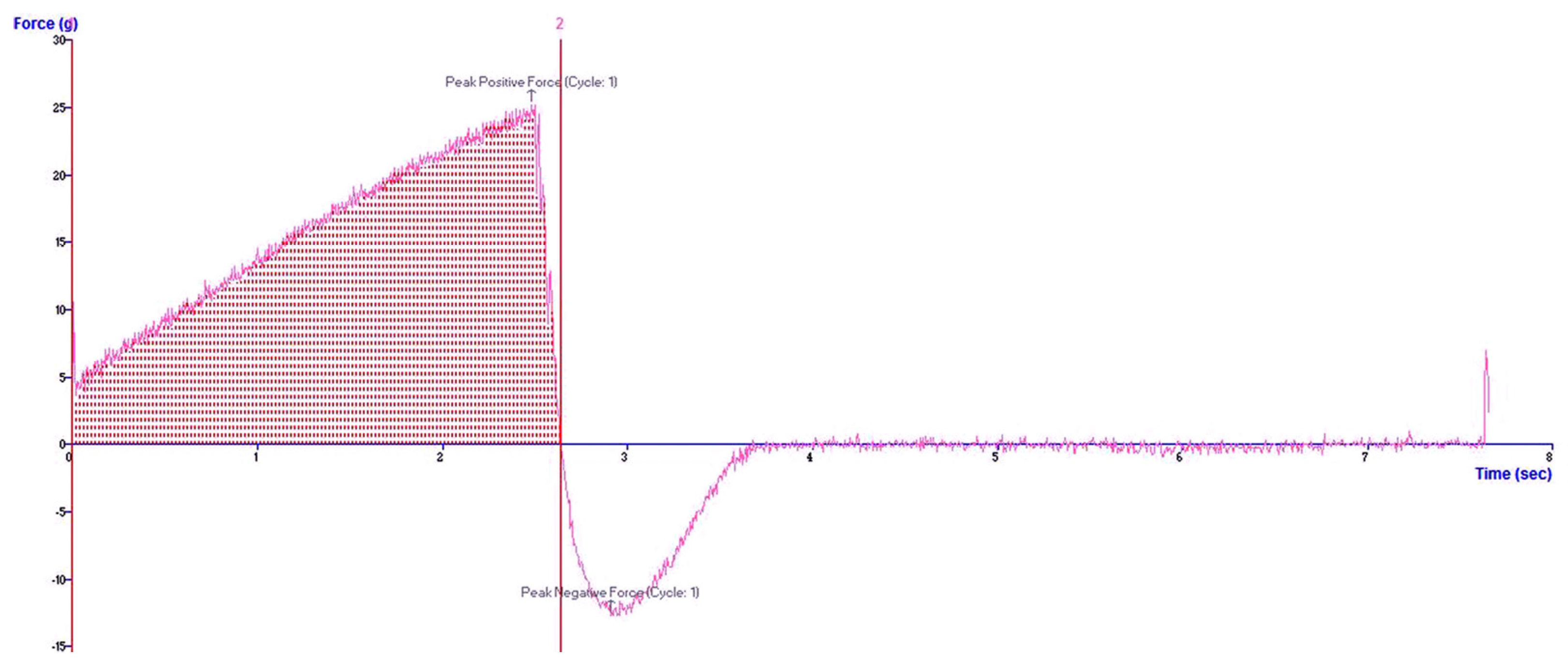
2.6. In Vitro Mucoadhesive Study
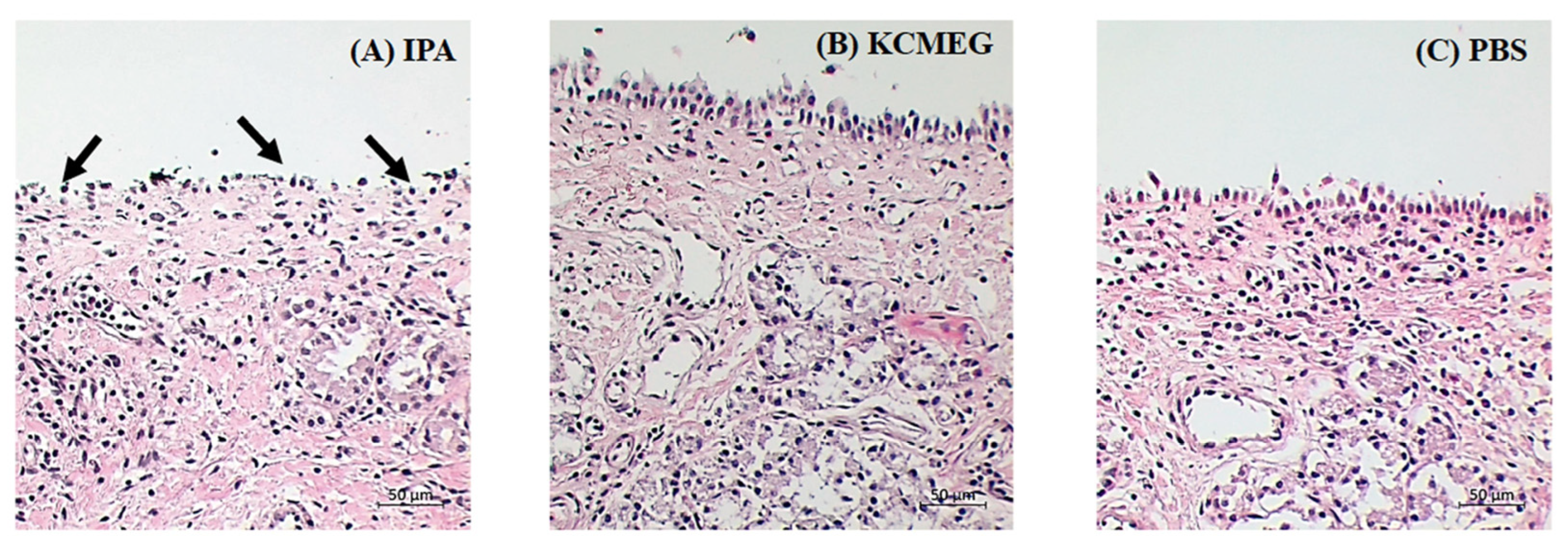
2.7. Nasal Cilio-Toxicity
3. Conclusions
4. Materials and Methods
4.1. Materials
4.2. Preparation of Curcumin-Loaded KLVFF-Pluronic F127 ME (KCME)
4.3. Physicochemical Characterization of ME and Microemulsion-Based Hydrogel
4.4. Fourier Transform Infrared Spectroscopy (FTIR)
4.5. Anticholinesterase Activity
4.6. Anti-Aggregation of Beta Amyloid
4.7. Optimization of Curcumin-Loaded KLVFF-Pluronic F127 ME-Based Hydrogel (KCMEG) by CCD
4.8. Optimization and Verification
4.9. In Vitro Mucoadhesion Study
4.10. Morphological Analysis (SEM)
4.11. Nasal Cilio-Toxicity Study
4.12. Statistical Analysis
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Breijyeh, Z.; Karaman, R. Comprehensive review on Alzheimer’s disease: Causes and treatment. Molecules 2020, 25, 5789. [Google Scholar] [CrossRef]
- Mira, A.; Gonçalves, R.; Rodrigues, I.T. Dysphagia in Alzheimer’s disease: A systematic review. Dement. Neuropsychol. 2022, 16, 261–269. [Google Scholar] [CrossRef]
- Fonseca, L.C.; Lopes, J.A.; Vieira, J.; Viegas, C.; Oliveira, C.S.; Hartmann, R.P.; Fonte, P. Intranasal drug delivery for treatment of Alzheimer’s disease. Drug Deliv. Transl. Res. 2021, 11, 411–425. [Google Scholar] [CrossRef] [PubMed]
- Taléns-Visconti, R.; de Julián-Ortiz, J.V.; Vila-Busó, O.; Diez-Sales, O.; Nácher, A. Intranasal Drug Administration in Alzheimer-Type Dementia: Towards Clinical Applications. Pharmaceutics 2023, 15, 1399. [Google Scholar] [CrossRef] [PubMed]
- Froelich, A.; Osmałek, T.; Jadach, B.; Puri, V.; Michniak-Kohn, B. Microemulsion-based media in nose-to-brain drug delivery. Pharmaceutics 2021, 13, 201. [Google Scholar] [CrossRef] [PubMed]
- Misra, A.; Kher, G. Drug delivery systems from nose to brain. Curr. Pharm. Biotechnol. 2012, 13, 2355–2379. [Google Scholar] [CrossRef]
- Acharya, S.P.; Pundarikakshudu, K.; Panchal, A.; Lalwani, A. Development of carbamazepine transnasal microemulsion for treatment of epilepsy. Drug Deliv. Transl. Res. 2013, 3, 252–259. [Google Scholar] [CrossRef]
- Xu, J.; Tao, J.; Wang, J. Design and application in delivery system of intranasal antidepressants. Front. Bioeng. Biotechnol. 2020, 8, 626882. [Google Scholar] [CrossRef]
- Alagusundaram, M.; Chengaiah, B.; Gnanaprakash, K.; Ramkanth, S.; Chetty, C.M.; Dhachinamoorthi, D. Nasal drug delivery system-an overview. Int. J. Res. Pharm. Sci. 2010, 1, 454–465. [Google Scholar]
- Jadhav, K.R.; Gambhire, M.N.; Shaikh, I.M.; Kadam, V.J.; Pisal, S.S. Nasal drug delivery system-factors affecting and applications. Curr. Drug Ther. 2007, 2, 27–38. [Google Scholar] [CrossRef]
- Patel, R.B.; Patel, M.R.; Bhatt, K.K.; Patel, B.G.; Gaikwad, R.V. Microemulsion-based drug delivery system for transnasal delivery of Carbamazepine: Preliminary brain-targeting study. Drug Deliv. 2016, 23, 207–213. [Google Scholar] [CrossRef]
- Keller, L.-A.; Merkel, O.; Popp, A. Intranasal drug delivery: Opportunities and toxicologic challenges during drug development. Drug Deliv. Transl. Res. 2021, 12, 735–757. [Google Scholar] [CrossRef]
- Erdő, F.; Bors, L.A.; Farkas, D.; Bajza, Á.; Gizurarson, S. Evaluation of intranasal delivery route of drug administration for brain targeting. Brain Res. Bull. 2018, 143, 155–170. [Google Scholar] [CrossRef] [PubMed]
- Espinoza, L.C.; Silva-Abreu, M.; Clares, B.; Rodríguez-Lagunas, M.J.; Halbaut, L.; Cañas, M.-A.; Calpena, A.C. Formulation strategies to improve nose-to-brain delivery of donepezil. Pharmaceutics 2019, 11, 64. [Google Scholar] [CrossRef]
- Francis, G.J.; Martinez, J.A.; Liu, W.Q.; Xu, K.; Ayer, A.; Fine, J.; Tuor, U.I.; Glazner, G.; Hanson, L.R.; Frey, W.H. Intranasal insulin prevents cognitive decline, cerebral atrophy and white matter changes in murine type I diabetic encephalopathy. Brain A J. Neurol. 2008, 131, 3311–3334. [Google Scholar]
- Zhang, J.C.; Zhang, F. Intranasal delivery of calcitonin gene-related peptide reduces cerebral vasospasm in rats. Front. Biosci. 2010, 2, 1502–1513. [Google Scholar]
- Jeong, S.-H.; Jang, J.-H.; Lee, Y.-B. Drug delivery to the brain via the nasal route of administration: Exploration of key targets and major consideration factors. J. Pharm. Investig. 2023, 53, 119–152. [Google Scholar] [CrossRef] [PubMed]
- Espinoza, L.C.; Vacacela, M.; Clares, B.; Garcia, M.L.; Fabrega, M.-J.; Calpena, A.C. Development of a Nasal Donepezil-loaded Microemulsion for the Treatment of Alzheimer’s Disease: In Vitro and ex vivo Characterization. CNS Neurol. Disord.-Drug Targets (Former. Curr. Drug Targets-CNS Neurol. Disord.) 2018, 17, 43–53. [Google Scholar] [CrossRef] [PubMed]
- Kulkarni, P.; Rawtani, D.; Barot, T. Design, development and In-Vitro/In-Vivo evaluation of intranasally delivered Rivastigmine and N-Acetyl Cysteine loaded bifunctional niosomes for applications in combinative treatment of Alzheimer’s disease. Eur. J. Pharm. Biopharm. 2021, 163, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Sood, S.; Jain, K.; Gowthamarajan, K. P1–382: Curcumin-donepezil–loaded nanostructured lipid carriers for intranasal delivery in an Alzheimer’s disease model. Alzheimer’s Dement. 2013, 9, 299. [Google Scholar] [CrossRef]
- Patel, R.B.; Patel, M.R.; Bhatt, K.K.; Patel, B.G. Formulation consideration and characterization of microemulsion drug delivery system for transnasal administration of carbamazepine. Bull. Fac. Pharm. Cairo Univ. 2013, 51, 243–253. [Google Scholar] [CrossRef]
- Ugwoke, M.I.; Agu, R.U.; Verbeke, N.; Kinget, R. Nasal mucoadhesive drug delivery: Background, applications, trends and future perspectives. Adv. Drug Deliv. Rev. 2005, 57, 1640–1665. [Google Scholar] [CrossRef] [PubMed]
- Suzuki, Y.; Makino, Y. Mucosal drug delivery using cellulose derivatives as a functional polymer. J. Control. Release 1999, 62, 101–107. [Google Scholar] [CrossRef] [PubMed]
- Hewlings, S.J.; Kalman, D.S. Curcumin: A review of its effects on human health. Foods 2017, 6, 92. [Google Scholar] [CrossRef] [PubMed]
- Ege, D. Action mechanisms of curcumin in Alzheimer’s disease and its brain targeted delivery. Materials 2021, 14, 3332. [Google Scholar] [CrossRef] [PubMed]
- Bonaccorso, A.; Gigliobianco, M.R.; Pellitteri, R.; Santonocito, D.; Carbone, C.; Di Martino, P.; Puglisi, G.; Musumeci, T. Optimization of curcumin nanocrystals as promising strategy for nose-to-brain delivery application. Pharmaceutics 2020, 12, 476. [Google Scholar] [CrossRef] [PubMed]
- Vaz, G.; Clementino, A.; Mitsou, E.; Ferrari, E.; Buttini, F.; Sissa, C.; Xenakis, A.; Sonvico, F.; Dora, C.L. In Vitro Evaluation of Curcumin-and Quercetin-Loaded Nanoemulsions for Intranasal Administration: Effect of Surface Charge and Viscosity. Pharmaceutics 2022, 14, 194. [Google Scholar] [CrossRef] [PubMed]
- Mansour, M.; Nasr, M.; Ahmed-Farid, O.A.; Ahmed, R.F. Intranasal ondansetron microemulsion counteracting the adverse effects of cisplatin: Animal study. Pharmacol. Rep. 2023, 75, 199–210. [Google Scholar] [CrossRef]
- Pathak, R.; Dash, R.P.; Misra, M.; Nivsarkar, M. Role of mucoadhesive polymers in enhancing delivery of nimodipine microemulsion to brain via intranasal route. Acta Pharm. Sin. B 2014, 4, 151–160. [Google Scholar] [CrossRef]
- Shah, B.M.; Misra, M.; Shishoo, C.J.; Padh, H. Nose to brain microemulsion-based drug delivery system of rivastigmine: Formulation and ex-vivo characterization. Drug Deliv. 2015, 22, 918–930. [Google Scholar] [CrossRef]
- Jansson, B.; Hägerström, H.; Fransén, N.; Edsman, K.; Björk, E. The influence of gellan gum on the transfer of fluorescein dextran across rat nasal epithelium In Vivo. Eur. J. Pharm. Biopharm. 2005, 59, 557–564. [Google Scholar] [CrossRef]
- Illum, L. Nasal drug delivery—Possibilities, problems and solutions. J. Control. Release 2003, 87, 187–198. [Google Scholar] [CrossRef]
- Mandal, S.; Mandal, S.D.; Chuttani, K.; Sawant, K.K.; Subudhi, B.B. Preclinical study of ibuprofen loaded transnasal mucoadhesive microemulsion for neuroprotective effect in MPTP mice model. Iran. J. Pharm. Res. IJPR 2018, 17, 23. [Google Scholar]
- Barakat, N.; Omar, S.; Ahmed, A. Carbamazepine uptake into rat brain following intra-olfactory transport. J. Pharm. Pharmacol. 2006, 58, 63–72. [Google Scholar] [CrossRef]
- Yermak, I.M.; Davydova, V.N.; Volod’ko, A.V. Mucoadhesive Marine Polysaccharides. Mar. Drugs 2022, 20, 522. [Google Scholar] [CrossRef]
- de Lima, C.S.; Varca, J.P.; Alves, V.M.; Nogueira, K.M.; Cruz, C.P.; Rial-Hermida, M.I.; Kadłubowski, S.S.; Varca, G.H.; Lugão, A.B. Mucoadhesive Polymers and Their Applications in Drug Delivery Systems for the Treatment of Bladder Cancer. Gels 2022, 8, 587. [Google Scholar] [CrossRef]
- Shah, B.; Khunt, D.; Misra, M.; Padh, H. Formulation and in-vivo pharmacokinetic consideration of intranasal microemulsion and mucoadhesive microemulsion of rivastigmine for brain targeting. Pharm. Res. 2018, 35, 8. [Google Scholar] [CrossRef] [PubMed]
- Wen, M.M.; Ismail, N.I.K.; Nasra, M.M.; El-Kamel, A.H. Repurposing ibuprofen-loaded microemulsion for the management of Alzheimer’s disease: Evidence of potential intranasal brain targeting. Drug Deliv. 2021, 28, 1188–1203. [Google Scholar] [CrossRef] [PubMed]
- Jogani, V.V.; Shah, P.J.; Mishra, P.; Mishra, A.K.; Misra, A.R. Intranasal mucoadhesive microemulsion of tacrine to improve brain targeting. Alzheimer Dis. Assoc. Disord. 2008, 22, 116–124. [Google Scholar] [CrossRef] [PubMed]
- Mishra, V.; Thakur, S.; Patil, A.; Shukla, A. Quality by design (QbD) approaches in current pharmaceutical set-up. Expert. Opin. Drug Deliv. 2018, 15, 737–758. [Google Scholar] [CrossRef] [PubMed]
- Li, D.; Martini, N.; Wu, Z.; Chen, S.; Falconer, J.R.; Locke, M.; Zhang, Z.; Wen, J. Niosomal nanocarriers for enhanced dermal delivery of epigallocatechin gallate for protection against oxidative stress of the skin. Pharmaceutics 2022, 14, 726. [Google Scholar] [CrossRef]
- Acharya, S.P.; Pundarikakshudu, K.; Panchal, A.; Lalwani, A. Preparation and evaluation of transnasal microemulsion of carbamazepine. Asian J. Pharm. Sci. 2013, 8, 64–70. [Google Scholar] [CrossRef]
- Maqsood, I.; Masood, M.I.; Bashir, S.; Awais Nawaz, H.M.; Anjum, A.A.; Shahzadi, I.; Ahmad, M.; Masood, I. Preparation and In Vitro evaluation of Nystatin micro emulsion based gel. Pak. J. Pharm. Sci. 2015, 28, 1587–1593. [Google Scholar] [PubMed]
- Charan, T.R.; Bhutto, M.A.; Bhutto, M.A.; Tunio, A.A.; Murtaza, G.; Aftab, U.; Kandhro, F.; Khaskheli, S.A. Comparative analysis by total yield, antimicrobial and phytochemical evaluation of curcuminoid of district Kasur: With its potential use and characterization in electrospinning nanofibers. J. Ind. Text. 2022, 52, 15280837221111457. [Google Scholar] [CrossRef]
- Islam, M.T.; Rodríguez-Hornedo, N.; Ciotti, S.; Ackermann, C. Fourier transform infrared spectroscopy for the analysis of neutralizer-carbomer and surfactant-carbomer interactions in aqueous, hydroalcoholic, and anhydrous gel formulations. AAPS J. 2004, 6, 61–67. [Google Scholar] [CrossRef] [PubMed]
- Pramod, K.; Suneesh, C.V.; Shanavas, S.; Ansari, S.H.; Ali, J. Unveiling the compatibility of eugenol with formulation excipients by systematic drug-excipient compatibility studies. J. Anal. Sci. Technol. 2015, 6, 34. [Google Scholar] [CrossRef]
- Mazyed, E.A.; Zakaria, S. Enhancement of dissolution characteristics of clopidogrel bisulphate by proniosomes. Int. J. Appl. Pharm. 2019, 11, 77–85. [Google Scholar] [CrossRef]
- Afifi, S. Solid dispersion approach improving dissolution rate of stiripentol: A novel antiepileptic drug. Iran. J. Pharm. Res. IJPR 2015, 14, 1001. [Google Scholar]
- Marucci, G.; Buccioni, M.; Dal Ben, D.; Lambertucci, C.; Volpini, R.; Amenta, F. Efficacy of acetylcholinesterase inhibitors in Alzheimer’s disease. Neuropharmacology 2021, 190, 108352. [Google Scholar] [CrossRef] [PubMed]
- Jazayeri, S.B.; Amanlou, A.; Ghanadian, N.; Pasalar, P.; Amanlou, M. A preliminary investigation of anticholinesterase activity of some Iranian medicinal plants commonly used in traditional medicine. DARU J. Pharm. Sci. 2014, 22, 17. [Google Scholar] [CrossRef]
- Ali Reza, A.; Hossain, M.S.; Akhter, S.; Rahman, M.R.; Nasrin, M.; Uddin, M.J.; Sadik, G.; Khurshid Alam, A. In Vitro antioxidant and cholinesterase inhibitory activities of Elatostema papillosum leaves and correlation with their phytochemical profiles: A study relevant to the treatment of Alzheimer’s disease. BMC Complement. Altern. Med. 2018, 18, 123. [Google Scholar] [CrossRef] [PubMed]
- Ahmed, T.; Gilani, A.-H. Inhibitory effect of curcuminoids on acetylcholinesterase activity and attenuation of scopolamine-induced amnesia may explain medicinal use of turmeric in Alzheimer’s disease. Pharmacol. Biochem. Behav. 2009, 91, 554–559. [Google Scholar] [CrossRef]
- Hu, L.; Jia, Y.; Niu, F.; Jia, Z.; Yang, X.; Jiao, K. Preparation and enhancement of oral bioavailability of curcumin using microemulsions vehicle. J. Agric. Food Chem. 2012, 60, 7137–7141. [Google Scholar] [CrossRef] [PubMed]
- Bergonzi, M.; Hamdouch, R.; Mazzacuva, F.; Isacchi, B.; Bilia, A. Optimization, characterization and In Vitro evaluation of curcumin microemulsions. LWT-Food Sci. Technol. 2014, 59, 148–155. [Google Scholar] [CrossRef]
- Sohma, Y. Medicinal chemistry focusing on aggregation of amyloid-β. Chem. Pharm. Bull. 2016, 64, 1–7. [Google Scholar] [CrossRef]
- Huang, Q.; Zhao, Q.; Peng, J.; Yu, Y.; Wang, C.; Zou, Y.; Su, Y.; Zhu, L.; Wang, C.; Yang, Y. Peptide–polyphenol (KLVFF/EGCG) binary modulators for inhibiting aggregation and neurotoxicity of amyloid-β peptide. ACS Omega 2019, 4, 4233–4242. [Google Scholar] [CrossRef]
- Yang, F.; Lim, G.P.; Begum, A.N.; Ubeda, O.J.; Simmons, M.R.; Ambegaokar, S.S.; Chen, P.P.; Kayed, R.; Glabe, C.G.; Frautschy, S.A. Curcumin inhibits formation of amyloid β oligomers and fibrils, binds plaques, and reduces amyloid In Vivo. J. Biol. Chem. 2005, 280, 5892–5901. [Google Scholar] [CrossRef]
- Tang, M.; Taghibiglou, C. The mechanisms of action of curcumin in Alzheimer’s disease. J. Alzheimer’s Dis. 2017, 58, 1003–1016. [Google Scholar] [CrossRef]
- Tang, S.Y.; Manickam, S.; Wei, T.K.; Nashiru, B. Formulation development and optimization of a novel Cremophore EL-based nanoemulsion using ultrasound cavitation. Ultrason. Sonochemistry 2012, 19, 330–345. [Google Scholar] [CrossRef]
- Cevher, E.; Taha, M.; Orlu, M.; Araman, A. Evaluation of mechanical and mucoadhesive properties of clomiphene citrate gel formulations containing carbomers and their thiolated derivatives. Drug Deliv. 2008, 15, 57–67. [Google Scholar] [CrossRef]
- Špaglová, M.; Papadakos, M.; Čuchorová, M.; Matušová, D. Release of Tretinoin Solubilized in Microemulsion from Carbopol and Xanthan Gel: In Vitro versus Ex Vivo Permeation Study. Polymers 2023, 15, 329. [Google Scholar] [CrossRef] [PubMed]
- Tan, Y.T.; Peh, K.K.; Al-Hanbali, O. Effect of Carbopol and polyvinylpyrrolidone on the mechanical, rheological, and release properties of bioadhesive polyethylene glycol gels. AAPS PharmSciTech 2000, 1, 69–78. [Google Scholar] [CrossRef] [PubMed]
- Basu, S.; Bandyopadhyay, A.K. Characterization of mucoadhesive nasal gels containing midazolam hydrochloride prepared from Linum usitatissimum L. mucilage. Braz. J. Pharm. Sci. 2011, 47, 817–823. [Google Scholar] [CrossRef][Green Version]
- Schipper, N.G.; Verhoef, J.C.; Merkus, F.W. The nasal mucociliary clearance: Relevance to nasal drug delivery. Pharm. Res. 1991, 8, 807–814. [Google Scholar] [CrossRef] [PubMed]
- Trenkel, M.; Scherließ, R. Nasal powder formulations: In-Vitro characterisation of the impact of powders on nasal residence time and sensory effects. Pharmaceutics 2021, 13, 385. [Google Scholar] [CrossRef]
- Graves, N.M.; Kriel, R.L.; Jones-Saete, C.; Cloyd, J.C. Relative bioavailability of rectally administered carbamazepine suspension in humans. Epilepsia 1985, 26, 429–433. [Google Scholar] [CrossRef]
- Quadir, M.; Zia, H.; Needham, T.E. Toxicological implications of nasal formulations. Drug Deliv. 1999, 6, 227–242. [Google Scholar] [CrossRef]
- Lv, H.; Wang, Y.; Yang, X.; Ling, G.; Zhang, P. Application of curcumin nanoformulations in Alzheimer’s disease: Prevention, diagnosis and treatment. Nutr. Neurosci. 2023, 26, 727–742. [Google Scholar] [CrossRef]
- Zhang, L.; Yang, S.; Wong, L.R.; Xie, H.; Ho, P.C.-L. In Vitro and In Vivo comparison of curcumin-encapsulated chitosan-coated poly (lactic-co-glycolic acid) nanoparticles and curcumin/hydroxypropyl-β-Cyclodextrin inclusion complexes administered intranasally as therapeutic strategies for Alzheimer’s Disease. Mol. Pharm. 2020, 17, 4256–4269. [Google Scholar] [CrossRef]
- Li, L.; Tan, L.; Zhang, Q.; Cheng, Y.; Liu, Y.; Li, R.; Hou, S. Nose-to-brain delivery of self-assembled curcumin-lactoferrin nanoparticles: Characterization, neuroprotective effect and In Vivo pharmacokinetic study. Front. Bioeng. Biotechnol. 2023, 11, 427. [Google Scholar] [CrossRef]
- Phongpradist, R.; Thongchai, W.; Thongkorn, K.; Lekawanvijit, S.; Chittasupho, C. Surface Modification of Curcumin Microemulsions by Coupling of KLVFF Peptide: A Prototype for Targeted Bifunctional Microemulsions. Polymers 2022, 14, 443. [Google Scholar] [CrossRef] [PubMed]
- Patel, V.; Kukadiya, H.; Mashru, R.; Surti, N.; Mandal, S. Development of microemulsion for solubility enhancement of clopidogrel. Iran. J. Pharm. Res. IJPR 2010, 9, 327–334. [Google Scholar] [PubMed]
- Mandal, S.; Mandal, S.D.; Chuttani, K.; Subudhi, B.B. Mucoadhesive microemulsion of ibuprofen: Design and evaluation for brain targeting efficiency through intranasal route. Braz. J. Pharm. Sci. 2015, 51, 721–731. [Google Scholar] [CrossRef]
- Bachhav, Y.G.; Patravale, V.B. Microemulsion based vaginal gel of fluconazole: Formulation, In Vitro and In Vivo evaluation. Int. J. Pharm. 2009, 365, 175–179. [Google Scholar] [CrossRef] [PubMed]
- Hamed, R.; Abu Kwiak, A.D.; Al-Adhami, Y.; Hammad, A.M.; Obaidat, R.; Abusara, O.H.; Huwaij, R.A. Microemulsions as Lipid Nanosystems Loaded into Thermoresponsive In Situ Microgels for Local Ocular Delivery of Prednisolone. Pharmaceutics 2022, 14, 1975. [Google Scholar] [CrossRef]
- Chaiyana, W.; Saeio, K.; Hennink, W.E.; Okonogi, S. Characterization of potent anticholinesterase plant oil based microemulsion. Int. J. Pharm. 2010, 401, 32–40. [Google Scholar] [CrossRef]
- Lomarat, P.; Sripha, K.; Phanthong, P.; Kitphati, W.; Thirapanmethee, K.; Bunyapraphatsara, N. In Vitro biological activities of black pepper essential oil and its major components relevant to the prevention of Alzheimer’s disease. Thai J. Pharm. Sci. (TJPS) 2015, 39, 94–101. [Google Scholar]
- Reinke, A.A.; Gestwicki, J.E. Structure–activity Relationships of amyloid beta-aggregation inhibitors based on curcumin: Influence of linker length and flexibility. Chem. Biol. Drug Des. 2007, 70, 206–215. [Google Scholar] [CrossRef] [PubMed]
- Nakamura, F.; Ohta, R.; Machida, Y.; Nagai, T. In Vitro and In Vivo nasal mucoadhesion of some water-soluble polymers. Int. J. Pharm. 1996, 134, 173–181. [Google Scholar] [CrossRef]
- Yıldırım, Ö.A.; Durucan, C. Synthesis of zinc oxide nanoparticles elaborated by microemulsion method. J. Alloys Compd. 2010, 506, 944–949. [Google Scholar] [CrossRef]
- Pailla, S.R.; Sampathi, S.; Junnuthula, V.; Maddukuri, S.; Dodoala, S.; Dyawanapelly, S. Brain-Targeted Intranasal Delivery of Zotepine Microemulsion: Pharmacokinetics and Pharmacodynamics. Pharmaceutics 2022, 14, 978. [Google Scholar] [CrossRef] [PubMed]




| Formulation | Globule Size (nm) | PDI | Zeta Potential (mV) | %T | pH |
|---|---|---|---|---|---|
| KCME | 70.8 ± 3.4 | 0.409 ± 0.048 | −0.07 ± 0.74 | 97.03 ± 0.01 | 5.80 ± 0.02 |
| Formulation | Diameter of Spread Area (cm) | Retention Time (Min) |
|---|---|---|
| KCME | 3.22 ± 0.17 | 2.32 ± 0.08 |
| KCMEG | 0.90 ± 0.15 | 9.67 ± 0.13 |
| Variable | Hardness (Y1) | Adhesiveness (Y2) | |||
|---|---|---|---|---|---|
| F-Value | p-Value | F-Value | p-Value | ||
| Main effects | X1 | 0.0148 | 0.9072 | 9.93 | 0.0161 a |
| X2 | 87.91 | <0.0001 a | 53.78 | 0.0002 a | |
| Quadratic effects | X12 | - | - | - | - |
| X22 | - | - | - | - | |
| Interaction effects | X12 | 11.60 | 0.0144 a | - | - |
| R2 | 0.9464 | 0.9010 | |||
| Adjusted R2 | 0.9197 | 0.8727 | |||
| p-value of model | 0.0003 a | 0.0003 a | |||
| Response | Experimental Value | Predicted Value | Prediction Error (%) |
|---|---|---|---|
| Hardness (g) | 25.360 | 25.277 | 0.33% |
| Adhesiveness (g.s) | 38.98 | 33.874 | 15.07% |
| Factors | Code Levels and Actual Values | ||||
|---|---|---|---|---|---|
| Axial (−α) | Low (−1) | Center (0) | High (+1) | Axial (+α) | |
| X1 | 0.19 | 0.50 | 1.25 | 2.00 | 2.31 |
| X2 | 14.64 | 25 | 50 | 75 | 85.36 |
| Run | Independent Variable | Response Variable | ||
|---|---|---|---|---|
| X1 | X2 | Hardness (Y1: g) | Adhesiveness (Y2: g.s) | |
| 1 | 1.25 | 50 | 9.981 | 16.282 |
| 2 | 1.25 | 50 | 7.059 | 10.479 |
| 3 | 0.50 | 25 | 10.467 | 17.208 |
| 4 | 2.31 | 50 | 7.546 | 11.439 |
| 5 | 1.25 | 50 | 6.329 | 8.982 |
| 6 | 1.25 | 50 | 6.086 | 9.409 |
| 7 | 1.25 | 14.64 | 26.655 | 39.575 |
| 8 | 0.19 | 50 | 7.181 | 0.097 |
| 9 | 2.00 | 75 | N/A | N/A |
| 10 | 1.25 | 50 | 6.451 | 11.179 |
| 11 | 2.00 | 25 | 23.247 | 34.523 |
| 12 | 1.25 | 85.36 | N/A | N/A |
| 13 | 0.50 | 75 | N/A | N/A |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Phongpradist, R.; Jiaranaikulwanitch, J.; Thongkorn, K.; Lekawanvijit, S.; Sirilun, S.; Chittasupho, C.; Poomanee, W. KLVFF Conjugated Curcumin Microemulsion-Based Hydrogel for Transnasal Route: Formulation Development, Optimization, Physicochemical Characterization, and Ex Vivo Evaluation. Gels 2023, 9, 610. https://doi.org/10.3390/gels9080610
Phongpradist R, Jiaranaikulwanitch J, Thongkorn K, Lekawanvijit S, Sirilun S, Chittasupho C, Poomanee W. KLVFF Conjugated Curcumin Microemulsion-Based Hydrogel for Transnasal Route: Formulation Development, Optimization, Physicochemical Characterization, and Ex Vivo Evaluation. Gels. 2023; 9(8):610. https://doi.org/10.3390/gels9080610
Chicago/Turabian StylePhongpradist, Rungsinee, Jutamas Jiaranaikulwanitch, Kriangkrai Thongkorn, Suree Lekawanvijit, Sasithorn Sirilun, Chuda Chittasupho, and Worrapan Poomanee. 2023. "KLVFF Conjugated Curcumin Microemulsion-Based Hydrogel for Transnasal Route: Formulation Development, Optimization, Physicochemical Characterization, and Ex Vivo Evaluation" Gels 9, no. 8: 610. https://doi.org/10.3390/gels9080610
APA StylePhongpradist, R., Jiaranaikulwanitch, J., Thongkorn, K., Lekawanvijit, S., Sirilun, S., Chittasupho, C., & Poomanee, W. (2023). KLVFF Conjugated Curcumin Microemulsion-Based Hydrogel for Transnasal Route: Formulation Development, Optimization, Physicochemical Characterization, and Ex Vivo Evaluation. Gels, 9(8), 610. https://doi.org/10.3390/gels9080610










