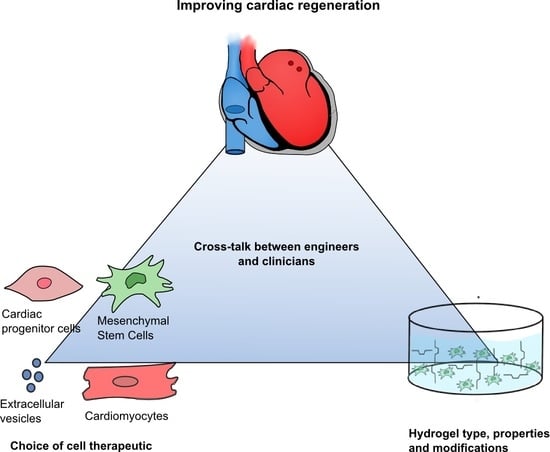
Injectable Hydrogels for Improving Cardiac Cell Therapy—In Vivo Evidence and Translational Challenges
Abstract
:1. Introduction
2. Injectable Hydrogels
2.1. Natural Hydrogels
2.2. Synthetic Hydrogels
3. Hydrogel Properties and Delivery Depends on Clinical Indication
3.1. Acute Myocardial Infarction
3.2. Chronic Ischemic Heart Failure and Non-Ischemic Dilated Cardiomyopathy
3.3. Coronary Artery By-Pass Graft
4. Cell Therapy Candidates and Hydrogel Requirements
4.1. Mesenchymal Stromal Cells and Endothelial Progenitor Cells
4.2. Cardiopoietic Cells and Cardiomyocytes
5. Current In Vivo Evidence
5.1. Clinical Studies
5.2. Preclinical Studies
6. Important Hydrogel Properties
6.1. Stiffness and Porosity
6.2. Functionalization
6.2.1. Adhesion Motifs
6.2.2. Angiogenesis
6.2.3. Graft Survival and Activity
6.3. Retention is Not Everything
7. Cell Delivery Strategies
7.1. Bulk Delivery
7.2. Microencapsulation
7.3. Single-Cell Coating
7.4. Delivery Route
8. Potential Roadblocks for Clinical Translation
8.1. Start with the End in Mind
8.2. Treatment Scalability and Logistics
8.3. Design and Production
9. Limitations
10. Perspectives
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Liao, X.; Yang, X.; Deng, H.; Hao, Y.; Mao, L.; Zhang, R.; Liao, W.; Yuan, M. Injectable Hydrogel-Based Nanocomposites for Cardiovascular Diseases. Front. Bioeng. Biotechnol. 2020, 8, 1–18. [Google Scholar] [CrossRef] [Green Version]
- Turner, D.; Rieger, A.C.; Balkan, W.; Hare, J.M. Clinical-Based Cell Therapies for Heart Disease-Current and Future State. Rambam Maimonides Med. J. 2020, 11, 1–20. [Google Scholar] [CrossRef]
- Malliaras, K.; Li, T.-S.; Luthringer, D.; Terrovitis, J.; Cheng, K.; Chakravarty, T.; Galang, G.; Zhang, Y.; Schoenhoff, F.; Van Eyk, J.; et al. Safety and Efficacy of Allogeneic Cell Therapy in Infarcted Rats Transplanted with Mismatched Cardiosphere-Derived Cells. Circulation 2013, 23, 1–7. [Google Scholar] [CrossRef] [Green Version]
- Mathieu, E.; Lamirault, G.; Toquet, C.; Lhommet, P.; Rederstorff, E.; Sourice, S.; Biteau, K.; Hulin, P.; Forest, V.; Weiss, P.; et al. Intramyocardial Delivery of Mesenchymal Stem Cell-Seeded Hydrogel Preserves Cardiac Function and Attenuates Ventricular Remodeling after Myocardial Infarction. PLoS ONE 2012, 7, e51991. [Google Scholar] [CrossRef]
- Madonna, R.; Van Laake, L.W.; Botker, H.E.; Davidson, S.M.; De Caterina, R.; Engel, F.B.; Eschenhagen, T.; Fernandez-Aviles, F.; Hausenloy, D.J.; Hulot, J.S.; et al. ESC Working Group on Cellular Biology of the Heart: Position Paper for Cardiovascular Research: Tissue Engineering Strategies Combined with Cell Therapies for Cardiac Repair in Ischaemic Heart Disease and Heart Failure. Cardiovasc. Res. 2019, 115, 488–500. [Google Scholar] [CrossRef] [Green Version]
- Malliaras, K.; Marbán, E. Cardiac Cell Therapy: Where Weve Been, Where We Are, and Where We Should Be Headed. Br. Med. Bull. 2011, 98, 161–185. [Google Scholar] [CrossRef] [Green Version]
- Vagnozzi, R.J.; Maillet, M.; Sargent, M.A.; Khalil, H.; Johansen, A.K.; Schwanekamp, J.A.; York, A.J.; Huang, V.; Nahrendorf, M.; Sadayappan, S.; et al. An Acute Immune Response Underlies the Benefit of Cardiac Stem Cell Therapy. Nature 2020, 176, 139–148. [Google Scholar] [CrossRef]
- He, X.; Wang, Q.; Zhao, Y.; Zhang, H.; Wang, B.; Pan, J.; Li, J.; Yu, H.; Wang, L.; Dai, J.; et al. Effect of Intramyocardial Grafting Collagen Scaffold With Mesenchymal Stromal Cells in Patients With Chronic Ischemic Heart Disease: A Randomized Clinical Trial. JAMA Netw. Open 2020, 3, e2016236. [Google Scholar] [CrossRef]
- De Vos, P.; Lazarjani, H.A.; Poncelet, D.; Faas, M.M. Polymers in Cell Encapsulation from an Enveloped Cell Perspective. Adv. Drug Deliv. Rev. 2014, 67–68, 15–34. [Google Scholar] [CrossRef]
- Chen, Y.; Li, C.; Li, C.; Chen, J.; Li, Y.; Xie, H.; Lin, C.; Fan, M.; Guo, Y.; Gao, E.; et al. Tailorable Hydrogel Improves Retention and Cardioprotection of Intramyocardial Transplanted Mesenchymal Stem Cells for the Treatment of Acute Myocardial Infarction in Mice. J. Am. Heart Assoc. 2020, 9. [Google Scholar] [CrossRef]
- Follin, B.; Ghotbi, A.A.; Clemmensen, A.E.; Bentsen, S.; Juhl, M.; Søndergaard, R.H.; Lund, L.D.; Haack-Sørensen, M.; Hasbak, P.; Cohen, S.; et al. Retention and Functional Effect of Adipose-Derived Stromal Cells Administered in Alginate Hydrogel in a Rat Model of Acute Myocardial Infarction. Stem Cells Int. 2018, 2018. [Google Scholar] [CrossRef] [PubMed]
- Ghanta, R.K.; Aghlara-Fotovat, S.; Pugazenthi, A.; Ryan, C.T.; Singh, V.P.; Mathison, M.; Jarvis, M.I.; Mukherjee, S.; Hernandez, A.; Veiseh, O. Immune-Modulatory Alginate Protects Mesenchymal Stem Cells for Sustained Delivery of Reparative Factors to Ischemic Myocardium. Biomater. Sci. 2020, 8, 5061–5070. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.; Li, P.; Qiao, C.; Wu, T.; Sun, X.; Wen, M.; Zhang, W. Chitosan Hydrogel Enhances the Therapeutic Efficacy of Bone Marrow-Derived Mesenchymal Stem Cells for Myocardial Infarction by Alleviating Vascular Endothelial Cell Pyroptosis. J. Cardiovasc. Pharm. 2020, 75, 75–83. [Google Scholar] [CrossRef]
- Yao, Y.; Yang, L.; Feng, L.F.; Yue, Z.W.; Zhao, N.H.; Li, Z.; He, Z.X. IGF-1C Domain-Modified Hydrogel Enhanced the Efficacy of Stem Cells in the Treatment of AMI. Stem Cell Res. 2020, 11, 1–14. [Google Scholar] [CrossRef]
- Xu, B.; Li, Y.; Deng, B.; Liu, X.; Wang, L.; Zhu, Q.L. Chitosan Hydrogel Improves Mesenchymal Stem Cell Transplant Survival and Cardiac Function Following Myocardial Infarction in Rats. Exp. Ther. Med. 2017, 13, 588–594. [Google Scholar] [CrossRef] [Green Version]
- Gerbin, K.A.; Mitzelfelt, K.A.; Guan, X.; Martinson, A.M.; Murry, C.E. Delta-1 Functionalized Hydrogel Promotes HESC-Cardiomyocyte Graft Proliferation and Maintains Heart Function Post-Injury. Mol. Ther. Methods Clin. Dev. 2020, 17, 986–998. [Google Scholar] [CrossRef]
- Lv, K.; Li, Q.; Zhang, L.; Wang, Y.; Zhong, Z.; Zhao, J.; Lin, X.; Wang, J.; Zhu, K.; Xiao, C.; et al. Incorporation of Small Extracellular Vesicles in Sodium Alginate Hydrogel as a Novel Therapeutic Strategy for Myocardial Infarction. Theranostics 2019, 9, 7403–7416. [Google Scholar] [CrossRef]
- Lee, K.Y.; Mooney, D.J. Hydrogels for Tissue Engineering. Chem. Rev. 2001, 101, 1869–1879. [Google Scholar] [CrossRef]
- Shachar, M.; Tsur-Gang, O.; Dvir, T.; Leor, J.; Cohen, S. The Effect of Immobilized RGD Peptide in Alginate Scaffolds on Cardiac Tissue Engineering. Acta Biomater. 2011, 7, 152–162. [Google Scholar] [CrossRef]
- Annabi, N.; Tamayol, A.; Uquillas, J.A.; Akbari, M.; Bertassoni, L.E.; Cha, C.; Camci-Unal, G.; Dokmeci, M.R.; Peppas, N.A.; Khademhosseini, A. 25th Anniversary Article: Rational Design and Applications of Hydrogels in Regenerative Medicine. Adv. Mater. 2014, 26, 85–124. [Google Scholar] [CrossRef]
- Zhou, A.; Chen, S.; He, B.; Zhao, W.; Chen, X.; Jiang, D. Controlled Release of TGF-Beta I from RADA Self-Assembling Peptide Hydrogel Scaffolds. Drug Des. Devel. Ther. 2016, 10, 3043–3051. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Chong, S.F.; Smith, A.A.A.; Zelikin, A.N. Microstructured, Functional PVA Hydrogels through Bioconjugation with Oligopeptides under Physiological Conditions. Small 2013, 9, 942–950. [Google Scholar] [CrossRef] [PubMed]
- Fisher, S.A.; Zhang, H.; Doree, C.; Mathur, A.; Martin-Rendon, E. Stem Cell Treatment for Acute Myocardial Infarction. Cochrane Database Syst. Rev. 2015, 2015. [Google Scholar] [CrossRef] [PubMed]
- Gyöngyösi, M.; Haller, P.M.; Blake, D.J.; Rendon, E.M. Meta-Analysis of Cell Therapy Studies in Heart Failure and Acute Myocardial Infarction. Circ. Res. 2018, 123, 301–308. [Google Scholar] [CrossRef] [PubMed]
- Mathur, A.; Fernandez-Aviles, F.; Bartunek, J.; Belmans, A.; Crea, F.; Dowlut, S.; Galinanes, M.; Good, M.C.; Hartikainen, J.; Hauskeller, C.; et al. The Effect of Intracoronary Infusion of Bone Marrow-Derivedmononuclear Cells on All-Cause Mortality in Acutemyocardial Infarction: The BAMI Trial. Eur. Heart J. 2020, 41, 3702–3710. [Google Scholar] [CrossRef]
- Pasotti, M.; Prati, F.; Arbustini, E. The Pathology of Myocardial Infarction in the Pre- and Post-Interventional Era. Heart 2006, 92, 1552–1556. [Google Scholar] [CrossRef] [Green Version]
- Vrtovec, B.; Poglajen, G.; Sever, M.; Lezaic, L.; Socan, A.; Haddad, F.; Wu, J.C. CD34+ Stem Cell Therapy in Nonischemic Dilated Cardiomyopathy Patients. Clin. Pharm. Ther. 2013, 94, 452–458. [Google Scholar] [CrossRef]
- Hare, J.M.; DiFede, D.L.; Rieger, A.C.; Florea, V.; Landin, A.M.; El-Khorazaty, J.; Khan, A.; Mushtaq, M.; Lowery, M.H.; Byrnes, J.J.; et al. Randomized Comparison of Allogeneic Versus Autologous Mesenchymal Stem Cells for Nonischemic Dilated Cardiomyopathy: POSEIDON-DCM Trial. J. Am. Coll. Cardiol. 2017, 69, 526–537. [Google Scholar] [CrossRef]
- Kanelidis, A.J.; Premer, C.; Lopez, J.; Balkan, W.; Hare, J.M. Route of Delivery Modulates the Efficacy of Mesenchymal Stem Cell Therapy for Myocardial Infarction: A Meta-Analysis of Preclinical Studies and Clinical Trials. Circ. Res. 2017, 176, 139–148. [Google Scholar] [CrossRef]
- Leor, J.; Tuvia, S.; Guetta, V.; Manczur, F.; Castel, D.; Willenz, U.; Petneházy, Ö.; Landa, N.; Feinberg, M.S.; Konen, E.; et al. Intracoronary Injection of In Situ Forming Alginate Hydrogel Reverses Left Ventricular Remodeling After Myocardial Infarction in Swine. J. Am. Coll. Cardiol. 2009, 54, 1014–1023. [Google Scholar] [CrossRef] [Green Version]
- Fu, H.; Chen, Q. Mesenchymal Stem Cell Therapy for Heart Failure: A Meta-Analysis. Herz 2020, 45, 557–563. [Google Scholar] [CrossRef]
- Golpanian, S.; Wolf, A.; Hatzistergos, K.E.; Hare, J.M. Rebuilding the Damaged Heart: Mesenchymal Stem Cells, Cell-Based Therapy, and Engineered Heart Tissue. Physiol. Rev. 2016, 96, 1127–1168. [Google Scholar] [CrossRef] [PubMed]
- Vrtovec, B. Cell Therapy for Nonischemic Cardiomyopathy. Circ. Res. 2018, 122, 28–30. [Google Scholar] [CrossRef]
- Hoeeg, C.; Frljak, S.; Qayyum, A.A.; Vrtovec, B.; Kastrup, J.; Ekblond, A.; Follin, B. Efficacy and Mode of Action of Mesenchymal Stem Cells in Non-Ischemic Dilated Cardiomyopathy: A Systematic Review. Biomedicines 2020, 8, 570. [Google Scholar] [CrossRef]
- Mathiasen, A.B.; Qayyum, A.A.; Jørgensen, E.; Helqvist, S.; Fischer-Nielsen, A.; Kofoed, K.F.; Haack-Sørensen, M.; Ekblond, A.; Kastrup, J. Bone Marrow-Derived Mesenchymal Stromal Cell Treatment in Patients with Severe Ischaemic Heart Failure: A Randomized Placebo-Controlled Trial (MSC-HF Trial). Eur. Heart J. 2015, 36, 1744–1753. [Google Scholar] [CrossRef] [Green Version]
- Kastrup, J.; Haack-Sørensen, M.; Juhl, M.; Harary Søndergaard, R.; Follin, B.; Drozd Lund, L.; Mønsted Johansen, E.; Ali Qayyum, A.; Bruun Mathiasen, A.; Jørgensen, E.; et al. Cryopreserved Off-the-Shelf Allogeneic Adipose-Derived Stromal Cells for Therapy in Patients with Ischemic Heart Disease and Heart Failure—A Safety Study. Stem Cells Transl. Med. 2017, 6, 1963–1971. [Google Scholar] [CrossRef]
- Grover, G.N.; Braden, R.L.; Christman, K.L. Oxime Cross-Linked Injectable Hydrogels for Catheter Delivery. Adv. Mater. 2013, 25, 2937–2942. [Google Scholar] [CrossRef] [Green Version]
- Rao, S.V.; Zeymer, U.; Douglas, P.S.; Al-Khalidi, H.; White, J.A.; Liu, J.; Levy, H.; Guetta, V.; Gibson, C.M.; Tanguay, J.F.; et al. Bioabsorbable Intracoronary Matrix for Prevention of Ventricular Remodeling After Myocardial Infarction. J. Am. Coll. Cardiol. 2016, 68, 715–723. [Google Scholar] [CrossRef]
- Dias, A.E.M.Á.S.; Melnikov, P.; Cônsolo, L.Z.Z. Oxidative Stress in Coronary Artery Bypass Surgery. Braz. J. Cardiovasc. Surg. 2015, 30, 417–424. [Google Scholar] [CrossRef]
- Cho, D.I.; Kim, M.R.; Jeong, H.Y.; Jeong, H.C.; Jeong, M.H.; Yoon, S.H.; Kim, Y.S.; Ahn, Y. Mesenchymal Stem Cells Reciprocally Regulate the M1/M2 Balance in Mouse Bone Marrow-Derived Macrophages. Exp. Mol. Med. 2014, 46, e70–e79. [Google Scholar] [CrossRef]
- Mao, C.; Hou, X.; Wang, B.; Chi, J.; Jiang, Y.; Zhang, C.; Li, Z. Intramuscular Injection of Human Umbilical Cord-Derived Mesenchymal Stem Cells Improves Cardiac Function in Dilated Cardiomyopathy Rats. Stem Cell Res. Ther. 2017, 8, 1–10. [Google Scholar] [CrossRef] [Green Version]
- Krampera, M. Mesenchymal Stromal Cell Licensing: A Multistep Process. Leukemia 2011, 25, 1408–1414. [Google Scholar] [CrossRef] [Green Version]
- Galleu, A.; Riffo-Vasquez, Y.; Trento, C.; Lomas, C.; Dolcetti, L.; Cheung, T.S.; Von Bonin, M.; Barbieri, L.; Halai, K.; Ward, S.; et al. Apoptosis in Mesenchymal Stromal Cells Induces In Vivo Recipient-Mediated Immunomodulation. Sci. Transl. Med. 2017, 9. [Google Scholar] [CrossRef] [Green Version]
- Follin, B.; Juhl, M.; Cohen, S.; Pedersen, A.E.; Gad, M.; Kastrup, J.; Ekblond, A. Human Adipose-Derived Stromal Cells in a Clinically Applicable Injectable Alginate Hydrogel: Phenotypic and Immunomodulatory Evaluation. Cytotherapy 2015, 17, 1104–1118. [Google Scholar] [CrossRef]
- Chow, A.; Stuckey, D.J.; Kidher, E.; Rocco, M.; Jabbour, R.J.; Mansfield, C.A.; Darzi, A.; Harding, S.E.; Stevens, M.M.; Athanasiou, T. Human Induced Pluripotent Stem Cell-Derived Cardiomyocyte Encapsulating Bioactive Hydrogels Improve Rat Heart Function Post Myocardial Infarction. Stem Cell Rep. 2017, 9, 1415–1422. [Google Scholar] [CrossRef] [Green Version]
- Pagano, F.; Picchio, V.; Angelini, F.; Iaccarino, A.; Peruzzi, M.; Cavarretta, E.; Biondi-Zoccai, G.; Sciarretta, S.; De Falco, E.; Chimenti, I.; et al. The Biological Mechanisms of Action of Cardiac Progenitor Cell Therapy. Curr. Cardiol. Rep. 2018, 20. [Google Scholar] [CrossRef]
- Le, T.; Chong, J. Cardiac Progenitor Cells for Heart Repair. Cell Death Discov. 2016, 2, 1–4. [Google Scholar] [CrossRef] [Green Version]
- Bhutani, S.; Nachlas, A.L.Y.; Brown, M.E.; Pete, T.; Johnson, C.T.; García, A.J.; Davis, M.E. Evaluation of Hydrogels Presenting Extracellular Matrix-Derived Adhesion Peptides and Encapsulating Cardiac Progenitor Cells for Cardiac Repair. ACS Biomater. Sci. Eng. 2019, 4, 200–210. [Google Scholar] [CrossRef]
- Chachques, J.C.; Trainini, J.C.; Lago, N.; Masoli, O.H.; Barisani, J.L.; Cortes-Morichetti, M.; Schussler, O.; Carpentier, A. Myocardial Assistance by Grafting a New Bioartificial Upgraded Myocardium (MAGNUM Clinical Trial): One Year Follow-Up. Cell Transpl. 2007, 16, 927–934. [Google Scholar] [CrossRef]
- Menasché, P.; Vanneaux, V.; Hagège, A.; Bel, A.; Cholley, B.; Parouchev, A.; Cacciapuoti, I.; Al-Daccak, R.; Benhamouda, N.; Blons, H.; et al. Transplantation of Human Embryonic Stem Cell–Derived Cardiovascular Progenitors for Severe Ischemic Left Ventricular Dysfunction. J. Am. Coll. Cardiol. 2018, 71, 429–438. [Google Scholar] [CrossRef]
- Wang, Q.; He, X.; Wang, B.; Pan, J.; Shi, C.; Li, J.; Wang, L.; Zhao, Y.; Dai, J.; Wang, D. Injectable Collagen Scaffold Promotes Swine Myocardial Infarction Recovery by Long-Term Local Retention of Transplanted Human Umbilical Cord Mesenchymal Stem Cells. Sci. China Life Sci. 2020. [Google Scholar] [CrossRef] [PubMed]
- Bai, R.; Tian, L.; Li, Y.; Zhang, J.; Wei, Y.; Jin, Z.; Liu, Z.; Liu, H. Combining ECM Hydrogels of Cardiac Bioactivity with Stem Cells of High Cardiomyogenic Potential for Myocardial Repair. Stem Cells Int. 2019, 2019. [Google Scholar] [CrossRef] [PubMed]
- Firoozi, S.; Pahlavan, S.; Ghanian, M.H.; Rabbani, S.; Tavakol, S.; Barekat, M.; Yakhkeshi, S.; Mahmoudi, E.; Soleymani, M.; Baharvand, H. A Cell-Free SDKP-Conjugated Self-Assembling Peptide Hydrogel Sufficient for Improvement of Myocardial Infarction. Biomolecules 2020, 10, 205. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Gao, X.R.; Xu, H.J.; Wang, L.F.; Liu, C.B.; Yu, F. Mesenchymal Stem Cell Transplantation Carried in SVVYGLR Modified Self-Assembling Peptide Promoted Cardiac Repair and Angiogenesis after Myocardial Infarction. Biochem. Biophys. Res. Commun. 2017, 491, 112–118. [Google Scholar] [CrossRef] [PubMed]
- Rabbani, S.; Soleimani, M.; Imani, M.; Sahebjam, M.; Ghiaseddin, A.; Nassiri, S.M.; Majd Ardakani, J.; Tajik Rostami, M.; Jalali, A.; Mousanassab, B.; et al. Regenerating Heart Using a Novel Compound and Human Wharton Jelly Mesenchymal Stem Cells. Arch. Med. Res. 2017, 48, 228–237. [Google Scholar] [CrossRef] [PubMed]
- Han, C.; Zhou, J.; Liang, C.; Liu, B.; Pan, X.; Zhang, Y.; Wang, Y.; Yan, B.; Xie, W.; Liu, F.; et al. Human Umbilical Cord Mesenchymal Stem Cell Derived Exosomes Encapsulated in Functional Peptide Hydrogels Promote Cardiac Repair. Biomater. Sci. 2019, 7, 2920–2933. [Google Scholar] [CrossRef] [PubMed]
- Qiao, L.; Kong, Y.; Shi, Y.; Sun, A.; Ji, R.; Huang, C.; Li, Y.; Yang, X. Synergistic Effects of Adipose-Derived Stem Cells Combined with Decellularized Myocardial Matrix on the Treatment of Myocardial Infarction in Rats. Life Sci. 2019, 239, 116891. [Google Scholar] [CrossRef]
- Gaffey, A.C.; Chen, M.H.; Trubelja, A.; Venkataraman, C.M.; Chen, C.W.; Chung, J.J.; Schultz, S.; Sehgal, C.M.; Burdick, J.A.; Atluri, P. Delivery of Progenitor Cells with Injectable Shear-Thinning Hydrogel Maintains Geometry and Normalizes Strain to Stabilize Cardiac Function after Ischemia. J. Thorac. Cardiovasc. Surg. 2019, 157, 1479–1490. [Google Scholar] [CrossRef]
- Ciuffreda, M.C.; Malpasso, G.; Chokoza, C.; Bezuidenhout, D.; Goetsch, K.P.; Mura, M.; Pisano, F.; Davies, N.H.; Gnecchi, M. Synthetic Extracellular Matrix Mimic Hydrogel Improves Efficacy of Mesenchymal Stromal Cell Therapy for Ischemic Cardiomyopathy. Acta Biomater. 2018, 70, 71–83. [Google Scholar] [CrossRef]
- Wu, Z.; Chen, G.; Zhang, J.; Hua, Y.; Li, J.; Liu, B.; Huang, A.; Li, H.; Chen, M.; Ou, C. Treatment of Myocardial Infarction with Gene-Modified Mesenchymal Stem Cells in a Small Molecular Hydrogel. Sci. Rep. 2017, 7, 1–11. [Google Scholar] [CrossRef] [Green Version]
- Kanda, P.; Alarcon, E.I.; Yeuchyk, T.; Parent, S.; De Kemp, R.A.; Variola, F.; Courtman, D.; Stewart, D.J.; Davis, D.R. Deterministic Encapsulation of Human Cardiac Stem Cells in Variable Composition Nanoporous Gel Cocoons to Enhance Therapeutic Repair of Injured Myocardium. ACS Nano 2018, 12, 4338–4350. [Google Scholar] [CrossRef]
- Tang, J.; Cui, X.; Caranasos, T.G.; Hensley, M.T.; Vandergriff, A.C.; Hartanto, Y.; Shen, D.; Zhang, H.; Zhang, J.; Cheng, K. Heart Repair Using Nanogel-Encapsulated Human Cardiac Stem Cells in Mice and Pigs with Myocardial Infarction. ACS Nano 2017, 11, 9738–9749. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Gao, J.; Shang, Y.; Hua, Y.; Ye, M.; Yang, Z.; Ou, C.; Chen, M. Folic Acid Derived Hydrogel Enhances the Survival and Promotes Therapeutic Efficacy of IPS Cells for Acute Myocardial Infarction. ACS Appl. Mater. Interfaces 2018, 10, 24459–24468. [Google Scholar] [CrossRef]
- Choe, G.; Kim, S.W.; Park, J.; Park, J.; Kim, S.; Kim, Y.S.; Ahn, Y.; Jung, D.W.; Williams, D.R.; Lee, J.Y. Anti-Oxidant Activity Reinforced Reduced Graphene Oxide/Alginate Microgels: Mesenchymal Stem Cell Encapsulation and Regeneration of Infarcted Hearts. Biomaterials 2019, 225, 119513. [Google Scholar] [CrossRef]
- Tan, Y.; Wang, L.; Chen, G.; Liu, W.; Li, Z.; Wang, Y.; Wang, L.; Li, W.; Wu, J.; Hao, J. Hyaluronate Supports HESC-Cardiomyocyte Cell Therapy for Cardiac Regeneration after Acute Myocardial Infarction. Cell Prolif. 2020, 53, 1–10. [Google Scholar] [CrossRef]
- Engler, A.J.; Sen, S.; Sweeney, H.L.; Discher, D.E. Matrix Elasticity Directs Stem Cell Lineage Specification. Cell 2006, 126, 677–689. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Choe, G.; Park, J.; Park, H.; Lee, J.Y. Hydrogel Biomaterials for Stem Cell Microencapsulation. Polymers 2018, 10, 997. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Headen, D.M.; García, J.R.; García, A.J. Parallel Droplet Microfluidics for High Throughput Cell Encapsulation and Synthetic Microgel Generation. Microsyst. Nanoeng. 2018, 4, 1–9. [Google Scholar] [CrossRef]
- Gottipati, A.; Chelvarajan, L.; Peng, H.; Kong, R.; Cahall, C.F.; Li, C.; Tripathi, H.; Al-Darraji, A.; Ye, S.; Elsawalhy, E.; et al. Gelatin Based Polymer Cell Coating Improves Bone Marrow-Derived Cell Retention in the Heart after Myocardial Infarction. Stem Cell Rev. Rep. 2019, 15, 404–414. [Google Scholar] [CrossRef]
- Jamaiyar, A.; Wan, W.; Ohanyan, V.; Enrick, M.; Janota, D.; Cumpston, D.; Song, H.; Stevanov, K.; Kolz, C.L.; Hakobyan, T.; et al. Alignment of Inducible Vascular Progenitor Cells on a Micro-Bundle Scaffold Improves Cardiac Repair Following Myocardial Infarction. Basic Res. Cardiol. 2017, 112, 1–13. [Google Scholar] [CrossRef]
- Jabbari, E. Hydrogels for Cell Delivery. Gels 2018, 4, 58. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Youngblood, R.L.; Truong, N.F.; Segura, T.; Shea, L.D. It’s All in the Delivery: Designing Hydrogels for Cell and Non-Viral Gene Therapies. Mol. Ther. 2018, 26, 2087–2106. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Mehrali, M.; Thakur, A.; Pennisi, C.P.; Talebian, S.; Arpanaei, A.; Nikkhah, M.; Dolatshahi-Pirouz, A. Nanoreinforced Hydrogels for Tissue Engineering: Biomaterials That Are Compatible with Load-Bearing and Electroactive Tissues. Adv. Mater. 2017, 29. [Google Scholar] [CrossRef]
- Talebian, S.; Mehrali, M.; Taebnia, N.; Pennisi, C.P.; Kadumudi, F.B.; Foroughi, J.; Hasany, M.; Nikkhah, M.; Akbari, M.; Orive, G.; et al. Self-Healing Hydrogels: The Next Paradigm Shift in Tissue Engineering? Adv. Sci. 2019, 6. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Soares, G.C.; Learmonth, D.A.; Vallejo, M.C.; Davila, S.P.; González, P.; Sousa, R.A.; Oliveira, A.L. Supercritical CO2 Technology: The next Standard Sterilization Technique? Mater. Sci. Eng. C 2019, 99, 520–540. [Google Scholar] [CrossRef]
- Wang, H.; Heilshorn, S.C. Adaptable Hydrogel Networks with Reversible Linkages for Tissue Engineering. Adv. Mater. 2015, 176, 139–148. [Google Scholar] [CrossRef]


| Study | Indication | Cell Type | Hydrogel | Application | Trial Design | ClinicalTrials.gov Identifier |
|---|---|---|---|---|---|---|
| Menasché, 2018 (ESCORT) | CABG | hESC-derived CV progenitors | Fibrin patch | Patch placed over infarct area | Open label | NCT02057900 |
| Chachques, 2007 | CABG | BMMNCs | Collagen scaffold | Collagen scaffold to close injection sites | Open label | N/A |
| He, 2020 | CABG | UC-MSC | Collagen hydrogel | Injected cells/hydrogel co-therapy | RCT | NCT02635464 |
| Study | Indication | Cell Type | Hydrogel | Functionalization | Application | Functional Outcome Compared to Cells Only | Additional Effects |
|---|---|---|---|---|---|---|---|
| Adult Stem Cells | |||||||
| Bai, 2019 | AMI in rats | Rat BADSC | Cardiac ECM in PBS | Bulk delivery IM | Greater improvement of LVEF than BADSCs | Improved cardiac differentiation of BADSCs | |
| Chen, 2020 | AMI in mice | Rat AT-MSC | Transglutaminase cross-linked gelatin | Bulk delivery IM | Only group which sig. improved LVEF | Improved retention and reduced fibrosis compared to ASC in PBS, improved MTT assay, decreased ANP and TNP mRNA | |
| Choe, 2019 | AMI in rats | Human UC-MSC | Alginate hydrogel | Graphene oxide +/– reduction | Microencapsulation IM | No sig. improvement | Decreased fibrotic area and increased infarct thickness |
| Ciuffreda, 2018 | Subacute MI in rats | Rat BM-MSC | PEG hydrogel | Heparinated | Bulk delivery IM | Only group which sig. improved LVEF | Improved retention |
| Firoozi, 2020 | AMI in rats | Human BM-MSC | RADA hydrogel | SDKP peptide integration | Bulk delivery IM | Greater improvement of LVEF than BM-MSCs | Improved retention; hydrogel effect in itself better than BMMSCs; decreased fibrosis |
| Follin, 2018 | AMI in immunodeficient rats | Human AT-MSC | Alginate cross-linked with calcium glucuronate | Bulk delivery IM | No difference in improvement | No difference in thickness, perfusion, or fibrosis | |
| Gaffey, 2018 | AMI in rats | Rat EPCs | Hyaluronate hydrogel | Adamantane and β-cyclodextrin | Bulk delivery IM | Only sig. LVEF improvement in gel + EPC group | Improved retention, myocardial velocity, and strain |
| Gao, 2017 | AMI in rats | Rat BM-MSC | RADA hydrogel | SVVYGLR peptide integration | Bulk delivery IM | Greater improvement of LVEF than BM-MSCs | Decreased collagen content, infarct size, number of vessels, and decreased number of apoptotic MSCs |
| Ghanta, 2020 | AMI in rats | Rat AT-MSC | TMTD alginate hydrogel | Capsules delivered epicardially | Greater improvement of LVEF than AT-MSCs | Only decreased fibrosis in the hydrogel group | |
| Gottipati, 2019 | AMI in mice | Mice BM-MSC | Photopolymerized gelatin methacrylamide and PEG diacrylate | Coated cells delivery IM | Improved retention by coating (double), similar macrophage density | Coating approach and no clumping tested | |
| Jamaiyar, 2017 | AMI in rats | Rat iVPC | PLGA microbundles | Bulk delivery IM | Only group with improved LVEF at four weeks, but no difference in improvement at eight weeks | No difference in infarct length or capillary-to-myocyte ratio | |
| Liu, 2017 | Acute I/R in rats | Rat BM-MSC | VEGF-gelatin-alginate-VEGF-gelatin | VEGF encapsulation | Coated cells delivered IV | Greater improvement of LVEF and perfusion than BM-MSC | Increased vascular density in peri-infarct and average area of myocardial islands in the infarct |
| Qiao, 2019 | Subacute AMI in rats | Rat AT-MSCs | Porcine cardiac ECM | Bulk delivery IM | Greater improvement in LVEF compared to AT-MSCs alone | Improved hemodynamic function; increased vessel density, expression of Ang-1, and VEGF; decreased fibrosis. | |
| Rabbani, 2017 | AMI in rabbits | Human WJ-MSC | PEG hyaluronic acid and chitosan hydrogel | Bulk delivery IM | Greater improvement of LVEF compared to WJ-MSC | Smaller infarct area (SPECT) and increased CD31 density | |
| Yao, 2020 | AMI in mice | Human P-MSC | Chitosan hydrogel | IGF-1 C domain | Bulk delivery IM | Only group with sig. improved LVEF | Increased angiogenesis, reduced collagen deposition, and inhibited inflammation |
| Yang, 2019 | AMI in mice | Mice BM-MSC | Chitosan thermosensitive hydrogel | Bulk delivery IM | Only group with sig. improved LVEF | Enhanced BM-MSC survival. inhibited inflammation, and alleviated pyroptosis of vascular endothelial cells | |
| Xu, 2017 | AMI in rats | Rat BM-MSC | Chitosan hydrogel | Bulk delivery IM | Only group with sig. improved LVEF | Improved BM-MSC retention in the myocardium | |
| Wang, 2020 | Chronic MI in minipigs | Human UC-MSCs | Collagen hydrogel | Bulk delivery IM | Greater improvement in cardiac output compared to UC-MSCs alone | Increased retention and myocardial tissue islands in scar tissue; decreased scar area | |
| Wu, 2017 | AMI in rats | Rat BM-MSC | DFEFKDFEFKYRGD small molecule hydrogel | Bulk delivery IM | Only group with sig. improved LVEF | Small-molecule hydrogel BM-MSC improved retention compared to BM-MSC alone | |
| Extracellular vesicles | |||||||
| Chen, 2018 | AMI in rats | Rat EPC EVs | Hyaluronate hydrogel | Adamantane and β-cyclodextrin | Bulk delivery IM | Greater improvement in LVEF compared to EVs alone | Increased vessel density and scar thickness |
| Han, 2019 | AMI in rats | Human UCMSC exosome | PA-GHRPS NapFF hydrogel | PA-GHRPS peptide and NapFF integration | Bulk delivery | Greater improvement of LVEF than exosomes | Improved retention, decreased CD68 density and TGF-b |
| Lv, 2019 | AMI in rats | Rat BM-MSC derrived EV | Sodium alginate cross-linked with calcium chloride | Bulk delivery | Greater improvement of LVEF than EVs | Decreased infarct size, improved wall thickness, enhanced retention, angiogenesis, and macrophage polarization (CD206) and decreased apoptosis | |
| Cardiogenic cell types | |||||||
| Bhutani, 2018 | I/R in atymic rats | Human C-kit+ CPC | PEG crosslinked with VPM | RGD or GFOGER or RDG integration | Bulk delivery | Only group with sig. improved LVEEF was non-adhesive RDG | Improved retention at day 28, decreased scar tissue |
| Kanda, 2018 | Subacute MI in immunodeficient mice | Human EDC | Agarose with fibronectin and fibrinogen capsulated with PDMS | Coated cells | Greater improvement of LVEF with stiff version of gel | Improved retention. decreased scar size, and increased proliferative cardiomyocytes and non-cardiomyocytes; MMP-12, IL-6, and bFGF increased in cells in stiff gel compared to the other gel | |
| Tang, 2017 | AMI in mice and pigs | Human CSCs | Poly (NIPAM-AA) nanogel | Bulk delivery IM | Preserved LVEF compared to cells alone | Improved retention, prevented myocardial T cell inflammation, decreased scar size, amd increased viable myocardium and infarct thickness | |
| Cardiomyocytes | |||||||
| Gerbin, 2020 | AMI in atymic rats | Human ESC-CM | Collagen gel | Notch ligand delta 1 integraion | Bulk delivery IM | Only group with sig. improved LVEF | Improved graft size |
| Li, 2018 | AMI in mice | Mouse iPSC | Self-assembling folic acid modified peptide hydrogel | Bulk delivery IM | Greater improvement of LVEF than cardiac differentiated iPSC | Increased angiogenesis and decreased fibrosis | |
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Hoeeg, C.; Dolatshahi-Pirouz, A.; Follin, B. Injectable Hydrogels for Improving Cardiac Cell Therapy—In Vivo Evidence and Translational Challenges. Gels 2021, 7, 7. https://doi.org/10.3390/gels7010007
Hoeeg C, Dolatshahi-Pirouz A, Follin B. Injectable Hydrogels for Improving Cardiac Cell Therapy—In Vivo Evidence and Translational Challenges. Gels. 2021; 7(1):7. https://doi.org/10.3390/gels7010007
Chicago/Turabian StyleHoeeg, Cecilie, Alireza Dolatshahi-Pirouz, and Bjarke Follin. 2021. "Injectable Hydrogels for Improving Cardiac Cell Therapy—In Vivo Evidence and Translational Challenges" Gels 7, no. 1: 7. https://doi.org/10.3390/gels7010007
APA StyleHoeeg, C., Dolatshahi-Pirouz, A., & Follin, B. (2021). Injectable Hydrogels for Improving Cardiac Cell Therapy—In Vivo Evidence and Translational Challenges. Gels, 7(1), 7. https://doi.org/10.3390/gels7010007