A Candida parapsilosis Overexpression Collection Reveals Genes Required for Pathogenesis
Abstract
1. Introduction
2. Materials and Methods
2.1. Strains and Growth Conditions
2.2. Construction of the Overexpression Cassettes
2.3. Generation of the Overexpression Mutants
2.4. Validation of the Mutant Strains
2.5. Characterization of the OE Mutant Strains
2.5.1. Growth Kinetics Measurements in Liquid Cultures
2.5.2. Viability Tests under Different Stress Conditions on Solid Media
2.5.3. Morphology Switch and Pseudohypha Forming Capacity
2.5.4. Biofilm Assay
2.5.5. Antifungal Susceptibility
2.5.6. Phagocytosis Assay
2.5.7. In Vivo Galleria mellonella Infection Model
2.5.8. Cell Wall Composition Assay
2.5.9. In Vivo Mouse Infection Model
2.6. Ethics Statement
2.7. Statistical Analysis
3. Results
3.1. Generation of an Overexpression Mutant Collection in C. parapsilosis
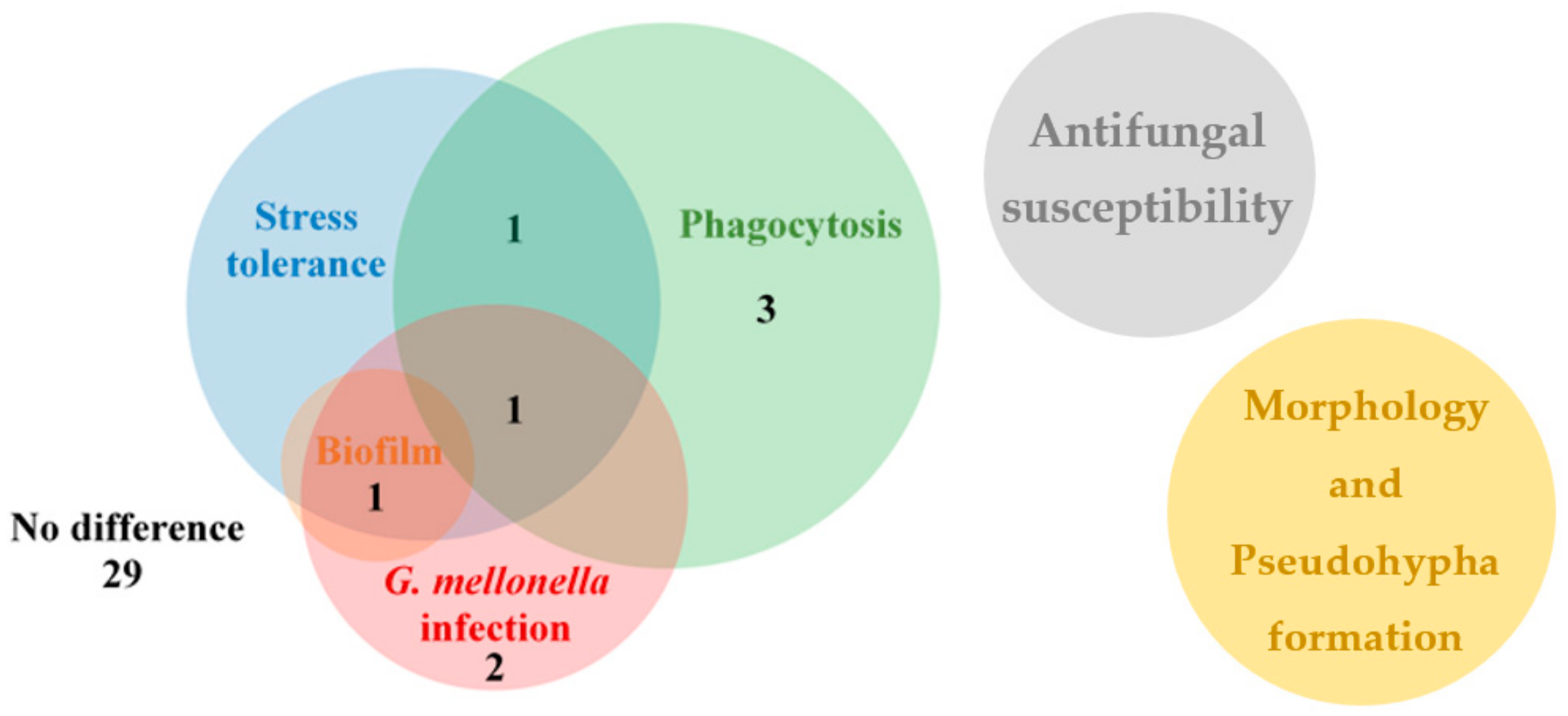
3.2. Characterization of the Generated OE Mutant Strains
3.2.1. Overexpression Does Not Affect Growth in either Complete or in Minimal Liquid Media
3.2.2. Overexpression of Certain Genes Affects Viability under Specific Stress Conditions
3.2.3. The Examined OE Mutants Did Not Display Any Alterations in Morphology or Pseudohypha Formation
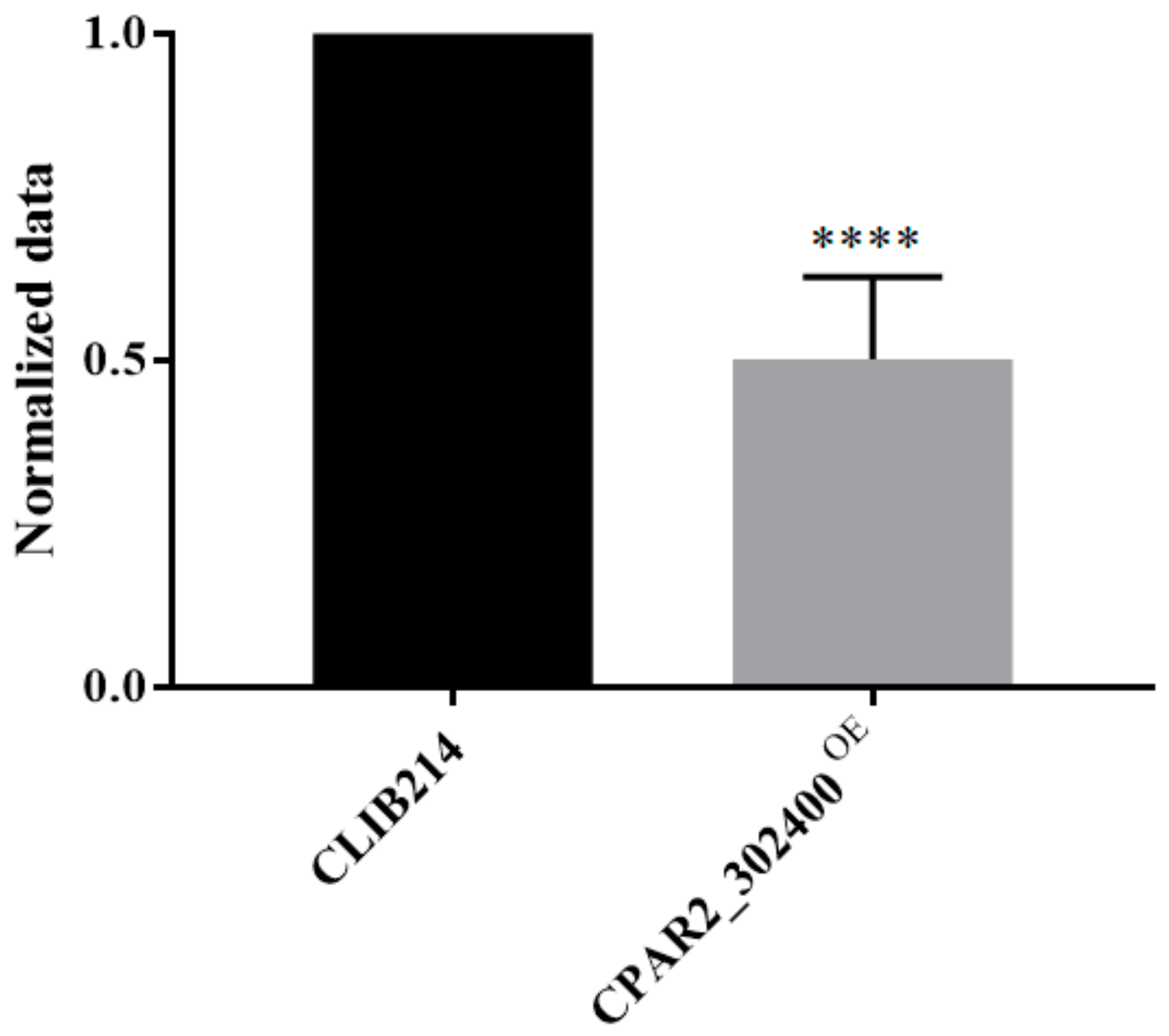
3.2.4. Overexpression of the CPAR2_302400 Gene Resulted in Attenuated Biofilm Formation
3.2.5. Overexpression of Selected Genes Did Not Affect Tolerance to Echinocandins
3.2.6. Overexpression of Certain Genes Interferes with Resistance to Phagocytosis by J774.2 Cells
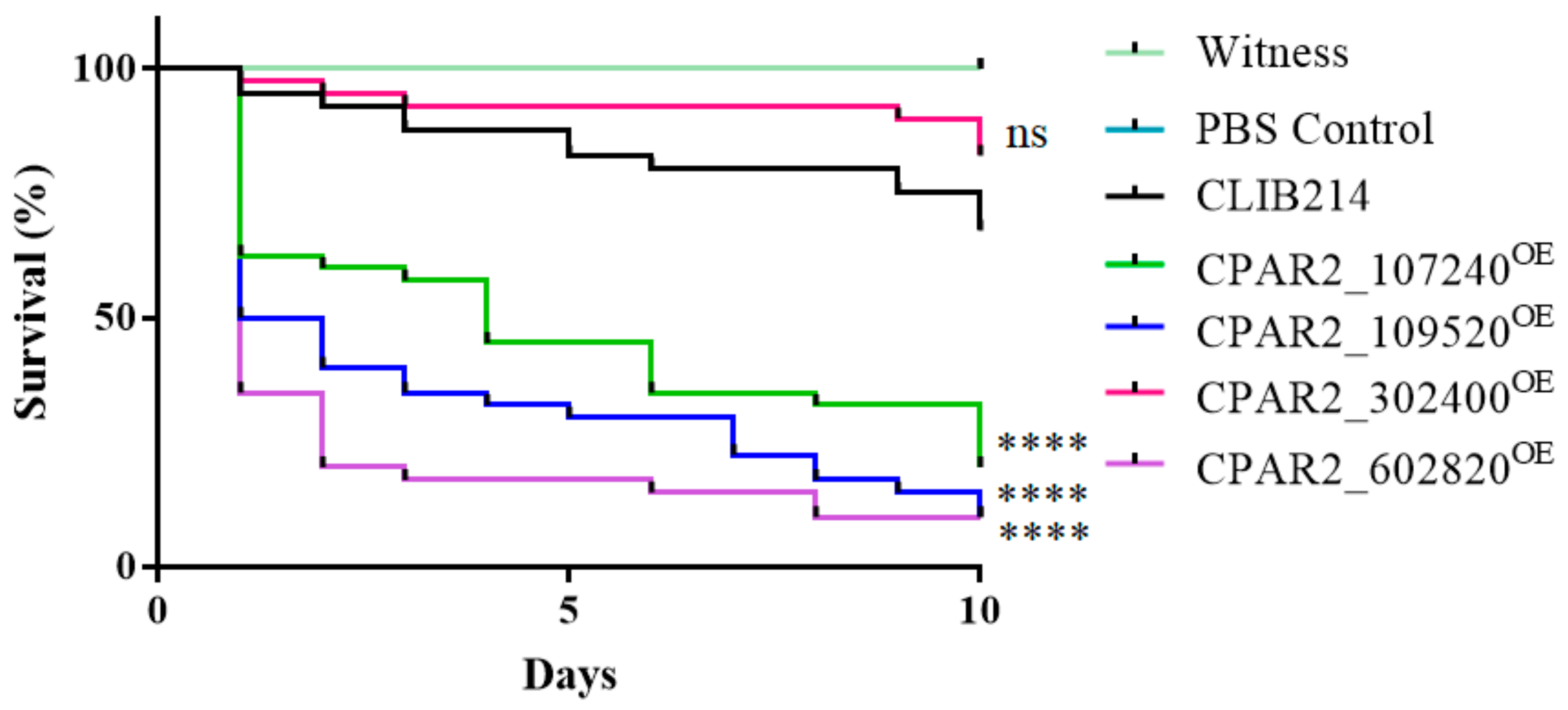
3.2.7. Overexpression of Certain Genes Regulate Virulence Related Processes in Galleria mellonella Larvae Model
3.2.8. Overexpression of the Selected Genes Does Not Affect Certain Components of the Cell Wall
3.2.9. CPAR2_109520 and CPAR2_302400 Differentially Alter Fungal Burden in Organs within Mus Musculus
4. Discussion
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Warnock, D.W. Trends in the epidemiology of invasive fungal infections. Nippon Ishinkin Gakkai Zasshi 2007, 48, 1–12. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Diekema, D.J. Epidemiology of invasive Candidiasis: A persistent public health problem. Clin. Microbiol. Rev. 2007, 20, 133–163. [Google Scholar] [CrossRef]
- Cleveland, A.A.; Farley, M.M.; Harrison, L.H.; Stein, B.; Hollick, R.; Lockhart, S.R.; Magill, S.S.; Derado, G.; Park, B.J.; Chiller, T.M.; et al. Changes in incidence and antifungal drug resistance in Candidemia: Results from population-based laboratory surveillance in Atlanta and Baltimore, 2008–2011. Clin. Infect. Dis. 2012, 55, 1352–1361. [Google Scholar] [CrossRef]
- Siopi, M.; Tarpatzi, A.; Kalogeropoulou, E.; Damianidou, S.; Vasilakopoulou, A.; Vourli, S.; Pournaras, S.; Meletiadis, J. Epidemiological trends of fungemia in greece with a focus on Candidemia during the recent financial crisis: A 10-Year survey in a tertiary care academic hospital and review of literature. Antimicrob. Agents Chemother. 2020, 64, e01516-19. [Google Scholar] [CrossRef]
- Fridkin, S.K.; Kaufman, D.; Edwards, J.R.; Shetty, S.; Horan, T. Changing incidence of Candida bloodstream infections among NICU patients in the United States: 1995–2004. Pediatrics 2006, 117, 1680–1687. [Google Scholar] [CrossRef]
- Juyal, D.; Sharma, M.; Pal, S.; Rathaur, V.K.; Sharma, N. Emergence of non-albicans Candida species in neonatal candidemia. N. Am. J. Med. Sci. 2013, 5, 541–545. [Google Scholar] [CrossRef]
- Yapar, N. Epidemiology and risk factors for invasive candidiasis. Ther. Clin. Risk Manag. 2014, 10, 95–105. [Google Scholar] [CrossRef]
- White, M.H. Editorial response: The contribution of fluconazole to the changing epidemiology of invasive Candidal infections. Clin. Infect. Dis. 1997, 24, 1129–1130. [Google Scholar] [CrossRef][Green Version]
- Nucci, M.; Marr, K.A. Emerging fungal diseases. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2005, 41, 521–526. [Google Scholar] [CrossRef]
- Cleveland, A.A.; Harrison, L.H.; Farley, M.M.; Hollick, R.; Stein, B.; Chiller, T.M.; Lockhart, S.R.; Park, B.J. Declining incidence of Candidemia and the shifting epidemiology of Candida resistance in two US Metropolitan Areas, 2008–2013: Results from population-based surveillance. PLoS ONE 2015, 10, e0120452. [Google Scholar] [CrossRef]
- Papon, N.; Courdavault, V.; Clastre, M.; Bennett, R.J. Emerging and emerged pathogenic Candida species: Beyond the Candida albicans paradigm. PLoS Pathog. 2013, 9, e1003550. [Google Scholar] [CrossRef] [PubMed]
- Clark, T.A.; Slavinski, S.A.; Morgan, J.; Lott, T.; Arthington-Skaggs, B.A.; Brandt, M.E.; Webb, R.M.; Currier, M.; Flowers, R.H.; Fridkin, S.K.; et al. Epidemiologic and molecular characterization of an outbreak of Candida parapsilosis bloodstream infections in a community hospital. J. Clin. Microbiol. 2004, 42, 4468–4472. [Google Scholar] [CrossRef] [PubMed]
- Kuhn, D.M.; Mikherjee, P.K.; Clark, T.A.; Pujol, C.; Chandra, J.; Hajjeh, R.A.; Warnock, D.W.; Soil, D.R.; Ghannoum, M.A. Candida parapsilosis characterization in an outbreak setting. Emerg. Infect. Dis. 2004, 10, 1074–1081. [Google Scholar] [CrossRef] [PubMed]
- Pammi, M.; Holland, L.; Butler, G.; Gacser, A.; Bliss, J.M. Candida parapsilosis is a significant neonatal pathogen: A systematic review and meta-analysis. Pediatr. Infect. Dis. J. 2013, 32, e206–e216. [Google Scholar] [CrossRef] [PubMed]
- Harrington, R.; Kindermann, S.L.; Hou, Q.; Taylor, R.J.; Azie, N.; Horn, D.L. Candidemia and invasive candidiasis among hospitalized neonates and pediatric patients. Curr. Med. Res. Opin. 2017, 33, 1803–1812. [Google Scholar] [CrossRef] [PubMed]
- Tóth, R.; Nosek, J.; Mora-Montes, H.M.; Gabaldon, T.; Bliss, J.M.; Nosanchuk, J.D.; Turner, S.A.; Butler, G.; Vágvölgyi, C.; Gácser, A.; et al. Candida parapsilosis: From genes to the bedside. Clin. Microbiol. Rev. 2019, 32, e00111-18. [Google Scholar] [CrossRef]
- Papp, C.; Kocsis, K.; Tóth, R.; Bodai, L.; Willis, J.R.; Ksiezopolska, E.; Lozoya-Pérez, N.E.; Vágvölgyi, C.; Mora Montes, H.; Gabaldón, T.; et al. Echinocandin-induced microevolution of Candida parapsilosis influences virulence and abiotic stress tolerance. mSphere 2018, 3. [Google Scholar] [CrossRef]
- Gácser, A.; Trofa, D.; Schäfer, W.; Nosanchuk, J.D. Targeted gene deletion in Candida parapsilosis demonstrates the role of secreted lipase in virulence. J. Clin. Investig. 2007, 117, 3049–3058. [Google Scholar] [CrossRef]
- Cillingová, A.; Zeman, I.; Tóth, R.; Neboháčová, M.; Dunčková, I.; Hölcová, M.; Jakúbková, M.; Gérecová, G.; Pryszcz, L.P.; Tomáška, Ľ.; et al. Eukaryotic transporters for hydroxyderivatives of benzoic acid. Sci. Rep. 2017, 7, 8998. [Google Scholar] [CrossRef]
- Zoppo, M.; Di Luca, M.; Franco, M.; Rizzato, C.; Lupetti, A.; Stringaro, A.; De Bernardis, F.; Schaudinn, C.; Barrasa, M.I.; Bottai, D.; et al. CpALS4770 and CpALS4780 contribution to the virulence of Candida parapsilosis. Microbiol. Res. 2020, 231, 126351. [Google Scholar] [CrossRef]
- Butler, G.; Rasmussen, M.D.; Lin, M.F.; Santos, M.A.S.; Sakthikumar, S.; Munro, C.A.; Rheinbay, E.; Grabherr, M.; Forche, A.; Reedy, J.L.; et al. Evolution of pathogenicity and sexual reproduction in eight Candida genomes. Nature 2009, 459, 657–662. [Google Scholar] [CrossRef] [PubMed]
- Pryszcz, L.P.; Németh, T.; Gácser, A.; Gabaldón, T. Unexpected genomic variability in clinical and environmental strains of the pathogenic yeast Candida parapsilosis. Genome Biol. Evol. 2013, 5, 2382–2392. [Google Scholar] [CrossRef] [PubMed]
- Logue, M.E.; Wong, S.; Wolfe, K.H.; Butler, G. A genome sequence survey shows that the pathogenic yeast Candida parapsilosis has a defective MTLa1 allele at its mating type locus. Eukaryot. Cell 2005, 4, 1009–1017. [Google Scholar] [CrossRef] [PubMed]
- Nosek, J.; Holesova, Z.; Kosa, P.; Gacser, A.; Tomaska, L. Biology and genetics of the pathogenic yeast Candida parapsilosis. Curr. Genet. 2009, 55, 497–509. [Google Scholar] [CrossRef] [PubMed]
- Candida Parapsilosis CDC317 Genome Snapshot/Overview. Available online: http://www.candidagenome.org/cache/C_parapsilosis_CDC317_genomeSnapshot.html (accessed on 16 November 2020).
- Candida albicans SC5314 Genome Snapshot/Overview. Available online: http://www.candidagenome.org/cache/C_albicans_SC5314_genomeSnapshot.html (accessed on 16 November 2020).
- Noble, S.M.; French, S.; Kohn, L.A.; Chen, V.; Johnson, A.D. Systematic screens of a Candida albicans homozygous deletion library decouple morphogenetic switching and pathogenicity. Nat. Genet. 2010, 42, 590–598. [Google Scholar] [CrossRef]
- Holland, L.M.; Schröder, M.S.; Turner, S.A.; Taff, H.; Andes, D.; Grózer, Z.; Gácser, A.; Ames, L.; Haynes, K.; Higgins, D.G.; et al. Comparative phenotypic analysis of the major fungal pathogens Candida parapsilosis and Candida albicans. PLOS Pathog. 2014, 10, e1004365. [Google Scholar] [CrossRef] [PubMed]
- Tóth, R.; Cabral, V.; Thuer, E.; Bohner, F.; Németh, T.; Papp, C.; Nimrichter, L.; Molnár, G.; Vágvölgyi, C.; Gabaldón, T.; et al. Investigation of Candida parapsilosis virulence regulatory factors during host-pathogen interaction. Sci. Rep. 2018, 8, 1346. [Google Scholar] [CrossRef]
- Breslow, D.K.; Cameron, D.M.; Collins, S.R.; Schuldiner, M.; Stewart-Ornstein, J.; Newman, H.W.; Braun, S.; Madhani, H.D.; Krogan, N.J.; Weissman, J.S.; et al. A comprehensive strategy enabling high-resolution functional analysis of the yeast genome. Nat. Methods 2008, 5, 711–718. [Google Scholar] [CrossRef]
- Verma, R.; Pradhan, D.; Maseet, M.; Singh, H.; Jain, A.K.; Khan, L.A. Genome-wide screening and in silico gene knockout to predict potential candidates for drug designing against Candida albicans. Infect. Genet. Evol. 2020, 80, 104196. [Google Scholar] [CrossRef]
- Noble, S.M.; Johnson, A.D. Strains and strategies for large-scale gene deletion studies of the diploid human fungal pathogen Candida albicans. Eukaryot. Cell 2005, 4, 298–309. [Google Scholar] [CrossRef]
- Reuss, O.; Vik, A.; Kolter, R.; Morschhäuser, J. The SAT1 flipper, an optimized tool for gene disruption in Candida albicans. Gene 2004, 341, 119–127. [Google Scholar] [CrossRef]
- Lombardi, L.; Salzberg, L.I.; Cinnéide, E.Ó.; O’Brien, C.; Butler, G. Large-scale generation of mutant strains in Candida parapsilosis using CRISPR-Cas9. Access Microbiol. 2019, 1, 695. [Google Scholar] [CrossRef]
- Vyas, V.K.; Barrasa, M.I.; Fink, G.R. A Candida albicans CRISPR system permits genetic engineering of essential genes and gene families. Sci. Adv. 2015, 1, e1500248. [Google Scholar] [CrossRef]
- Prelich, G. Gene overexpression: Uses, mechanisms, and interpretation. Genetics 2012, 190, 841–854. [Google Scholar] [CrossRef]
- Rorth, P.; Szabo, K.; Bailey, A.; Laverty, T.; Rehm, J.; Rubin, G.M.; Weigmann, K.; Milan, M.; Benes, V.; Ansorge, W.; et al. Systematic gain-of-function genetics in Drosophila. Development 1998, 125, 1049–1057. [Google Scholar]
- Palatnik, J.F.; Allen, E.; Wu, X.; Schommer, C.; Schwab, R.; Carrington, J.C.; Weigel, D. Control of leaf morphogenesis by microRNAs. Nature 2003, 425, 257–263. [Google Scholar] [CrossRef]
- Chua, G.; Morris, Q.D.; Sopko, R.; Robinson, M.D.; Ryan, O.; Chan, E.T.; Frey, B.J.; Andrews, B.J.; Boone, C.; Hughes, T.R.; et al. Identifying transcription factor functions and targets by phenotypic activation. Proc. Natl. Acad. Sci. USA 2006, 103, 12045–12050. [Google Scholar] [CrossRef]
- Liu, Y.; Kern, J.T.; Walker, J.R.; Johnson, J.A.; Schultz, P.G.; Luesch, H. A genomic screen for activators of the antioxidant response element. Proc. Natl. Acad. Sci. USA 2007, 104, 5205–5210. [Google Scholar] [CrossRef]
- Schubert, S.; Barker, K.S.; Znaidi, S.; Schneider, S.; Dierolf, F.; Dunkel, N.; Aïd, M.; Boucher, G.; Rogers, P.D.; Raymond, M.; et al. Regulation of efflux pump expression and drug resistance by the transcription factors Mrr1, Upc2, and Cap1 in Candida albicans. Antimicrob. Agents Chemother. 2011, 55, 2212–2223. [Google Scholar] [CrossRef]
- Cabral, V.; Znaidi, S.; Walker, L.A.; Martin-Yken, H.; Dague, E.; Legrand, M.; Lee, K.; Chauvel, M.; Firon, A.; Rossignol, T.; et al. Targeted changes of the cell wall proteome influence Candida albicans ability to form single- and multi-strain biofilms. PLoS Pathog. 2014, 10, e1004542. [Google Scholar] [CrossRef]
- Schillig, R.; Morschhäuser, J. Analysis of a fungus-specific transcription factor family, the Candida albicans zinc cluster proteins, by artificial activation. Mol. Microbiol. 2013, 89, 1003–1017. [Google Scholar] [CrossRef]
- Schwarzmüller, T.; Ma, B.; Hiller, E.; Istel, F.; Tscherner, M.; Brunke, S.; Ames, L.; Firon, A.; Green, B.; Cabral, V.; et al. Systematic phenotyping of a large-scale Candida glabrata deletion collection reveals novel antifungal tolerance genes. PLoS Pathog. 2014, 10, e1004211. [Google Scholar] [CrossRef]
- Sopko, R.; Huang, D.; Preston, N.; Chua, G.; Papp, B.; Kafadar, K.; Snyder, M.; Oliver, S.G.; Cyert, M.; Hughes, T.R.; et al. Mapping pathways and phenotypes by systematic gene overexpression. Mol. Cell 2006, 21, 319–330. [Google Scholar] [CrossRef]
- Znaidi, S.; van Wijlick, L.; Hernández-Cervantes, A.; Sertour, N.; Desseyn, J.-L.; Vincent, F.; Atanassova, R.; Gouyer, V.; Munro, C.A.; Bachellier-Bassi, S.; et al. Systematic gene overexpression in Candida albicans identifies a regulator of early adaptation to the mammalian gut. Cell. Microbiol. 2018, 20, e12890. [Google Scholar] [CrossRef]
- Rine, J. Gene overexpression in studies of Saccharomyces cerevisiae. Methods Enzymol. 1991, 194, 239–251. [Google Scholar] [CrossRef]
- Zordan, R.E.; Galgoczy, D.J.; Johnson, A.D. Epigenetic properties of white–opaque switching in Candida albicans are based on a self-sustaining transcriptional feedback loop. Proc. Natl. Acad. Sci. USA 2006, 103, 12807–12812. [Google Scholar] [CrossRef]
- Fu, Y.; Luo, G.; Spellberg, B.J.; Edwards, J.E.; Ibrahim, A.S. Gene overexpression/suppression analysis of candidate virulence factors of Candida albicans. Eukaryot. Cell 2008, 7, 483–492. [Google Scholar] [CrossRef]
- Chauvel, M.; Nesseir, A.; Cabral, V.; Znaidi, S.; Goyard, S.; Bachellier-Bassi, S.; Firon, A.; Legrand, M.; Diogo, D.; Naulleau, C.; et al. A Versatile overexpression strategy in the pathogenic yeast Candida albicans: Identification of regulators of morphogenesis and fitness. PLoS ONE 2012, 7, e45912. [Google Scholar] [CrossRef]
- Magtanong, L.; Ho, C.H.; Barker, S.L.; Jiao, W.; Baryshnikova, A.; Bahr, S.; Smith, A.M.; Heisler, L.E.; Choy, J.S.; Kuzmin, E.; et al. Dosage suppression genetic interaction networks enhance functional wiring diagrams of the cell. Nat. Biotechnol. 2011, 29, 505–511. [Google Scholar] [CrossRef]
- Zhu, H.; Bilgin, M.; Bangham, R.; Hall, D.; Casamayor, A.; Bertone, P.; Lan, N.; Jansen, R.; Bidlingmaier, S.; Houfek, T.; et al. Global analysis of protein activities using proteome chips. Science 2001, 293, 2101–2105. [Google Scholar] [CrossRef]
- Németh, T.; Papp, C.; Vagvolgyi, C.; Chakraborty, T.; Gacser, A. Identification and characterization of a neutral locus for knock-in purposes in C. parapsilosis. Front. Microbiol. 2020, 11, 1194. [Google Scholar] [CrossRef] [PubMed]
- Clinical and Laboratory Standards Institute. Reference Method for Broth Dilution Antifungal Susceptibility Testing of Yeasts, 4th ed.; approved standard; CLSI document M27-S4; Clinical and Laboratory Standards Institute: Wayne, PA, USA, 2012. [Google Scholar]
- Clinical and Laboratory Standards Institute. Reference Method for Broth Dilution Antifungal Susceptibility Testing of Yeasts, 3rd ed.; approved standard; CLSI document M27-A3; Clinical and Laboratory Standards Institute: Wayne, PA, USA, 2008. [Google Scholar]
- Gerami-Nejad, M.; Zacchi, L.F.; McClellan, M.; Matter, K.; Berman, J. Shuttle vectors for facile gap repair cloning and integration into a neutral locus in Candida albicans. Microbiology 2013, 159, 565–579. [Google Scholar] [CrossRef] [PubMed]
- Igual, J.C.; Johnson, A.L.; Johnston, L.H. Coordinated regulation of gene expression by the cell cycle transcription factor Swi4 and the protein kinase C MAP kinase pathway for yeast cell integrity. EMBO J. 1996, 15, 5001–5013. [Google Scholar] [CrossRef] [PubMed]
- Thompson, D.S.; Carlisle, P.L.; Kadosh, D. Coevolution of morphology and virulence in Candida species. Eukaryot. Cell 2011, 10, 1173–1182. [Google Scholar] [CrossRef]
- Cleary, I.A.; Mulabagal, P.; Reinhard, S.M.; Yadev, N.P.; Murdoch, C.; Thornhill, M.H.; Lazzell, A.L.; Monteagudo, C.; Thomas, D.P.; Saville, S.P.; et al. Pseudohyphal regulation by the transcription factor Rfg1p in Candida albicans. Eukaryot. Cell 2010, 9, 1363–1373. [Google Scholar] [CrossRef][Green Version]
- Ryan, O.; Shapiro, R.S.; Kurat, C.F.; Mayhew, D.; Baryshnikova, A.; Chin, B.; Lin, Z.-Y.; Cox, M.J.; Vizeacoumar, F.; Cheung, D.; et al. Global gene deletion analysis exploring yeast filamentous growth. Science 2012, 337, 1353–1356. [Google Scholar] [CrossRef]
- Lackey, E.; Vipulanandan, G.; Childers, D.S.; Kadosh, D. Comparative evolution of morphological regulatory functions in Candida species. Eukaryot. Cell 2013, 12, 1356–1368. [Google Scholar] [CrossRef]
- Sudbery, P.; Gow, N.; Berman, J. The distinct morphogenic states of Candida albicans. Trends Microbiol. 2004, 12, 317–324. [Google Scholar] [CrossRef]
- Li, Z.; Nielsen, K. Morphology changes in human fungal pathogens upon interaction with the host. J. Fungi 2017, 3, 66. [Google Scholar] [CrossRef]
- O’Connor, L.; Caplice, N.; Coleman, D.C.; Sullivan, D.J.; Moran, G.P. Differential filamentation of Candida albicans and Candida dubliniensis Is governed by nutrient regulation of UME6 expression. Eukaryot. Cell 2010, 9, 1383–1397. [Google Scholar] [CrossRef]
- Trofa, D.; Gácser, A.; Nosanchuk, J.D. Candida parapsilosis, an emerging fungal pathogen. Clin. Microbiol. Rev. 2008, 21, 606–625. [Google Scholar] [CrossRef]
- Nobile, C.J.; Fox, E.P.; Nett, J.E.; Sorrells, T.R.; Mitrovich, Q.M.; Hernday, A.D.; Tuch, B.B.; Andes, D.R.; Johnson, A.D. A recently evolved transcriptional network controls biofilm development in Candida albicans. Cell 2012, 148, 126–138. [Google Scholar] [CrossRef] [PubMed]
- Barchiesi, F.; Spreghini, E.; Tomassetti, S.; Della Vittoria, A.; Arzeni, D.; Manso, E.; Scalise, G. Effects of caspofungin against Candida guilliermondii and Candida parapsilosis. Antimicrob. Agents Chemother. 2006, 50, 2719–2727. [Google Scholar] [CrossRef]
- Cappelletty, D.; Eiselstein-McKitrick, K. The echinocandins. Pharmacotherapy 2007, 27, 369–388. [Google Scholar] [CrossRef] [PubMed]
- Pfaller, M.A.; Boyken, L.; Hollis, R.J.; Kroeger, J.; Messer, S.A.; Tendolkar, S.; Diekema, D.J. In vitro susceptibility of invasive isolates of Candida spp. to anidulafungin, caspofungin, and micafungin: Six years of global surveillance. J. Clin. Microbiol. 2008, 46, 150–156. [Google Scholar] [CrossRef]
- Brown, G.D. Innate antifungal immunity: The key role of phagocytes. Annu. Rev. Immunol. 2011, 29, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Höfs, S.; Mogavero, S.; Hube, B. Interaction of Candida albicans with host cells: Virulence factors, host defense, escape strategies, and the microbiota. J. Microbiol. 2016, 54, 149–169. [Google Scholar] [CrossRef]
- García-Rodas, R.; González-Camacho, F.; Rodríguez-Tudela, J.L.; Cuenca-Estrella, M.; Zaragoza, O. The interaction between Candida krusei and murine macrophages results in multiple outcomes, including intracellular survival and escape from killing. Infect. Immun. 2011, 79, 2136–2144. [Google Scholar] [CrossRef]
- Ellerbroek, P.M.; Walenkamp, A.M.E.; Hoepelman, A.I.M.; Coenjaerts, F.E.J. Effects of the capsular polysaccharides of Cryptococcus neoformans on phagocyte migration and inflammatory mediators. Curr. Med. Chem. 2004, 11, 253–266. [Google Scholar] [CrossRef]
- Pereira, T.; de Barros, P.; Fugisaki, L.; Rossoni, R.; Ribeiro, F.; de Menezes, R.; Junqueira, J.; Scorzoni, L. Recent advances in the use of Galleria mellonella model to study immune responses against human pathogens. J. Fungi 2018, 4, 128. [Google Scholar] [CrossRef]
- Braun, B.R.; Johnson, A.D. Control of filament formation in Candida albicans by the transcriptional repressor TUP1. Science 1997, 277, 105–109. [Google Scholar] [CrossRef] [PubMed]
- Zhao, R.; Lockhart, S.R.; Daniels, K.; Soll, D.R. Roles of TUP1 in switching, phase maintenance, and phase-specific gene expression in Candida albicans. Eukaryot. Cell 2002, 1, 353–365. [Google Scholar] [CrossRef] [PubMed][Green Version]
- Hu, C.-J.; Bai, C.; Zheng, X.-D.; Wang, Y.-M.; Wang, Y. Characterization and functional analysis of the siderophore-iron transporter CaArn1p in Candida albicans. J. Biol. Chem. 2002, 277, 30598–30605. [Google Scholar] [CrossRef]
- Murad, A.M.; Leng, P.; Straffon, M.; Wishart, J.; Macaskill, S.; MacCallum, D.; Schnell, N.; Talibi, D.; Marechal, D.; Tekaia, F.; et al. NRG1 represses yeast-hypha morphogenesis and hypha-specific gene expression in Candida albicans. EMBO J. 2001, 20, 4742–4752. [Google Scholar] [CrossRef] [PubMed]
- Wächtler, B.; Wilson, D.; Haedicke, K.; Dalle, F.; Hube, B. From attachment to damage: Defined genes of Candida albicans mediate adhesion, invasion and damage during interaction with oral epithelial cells. PLoS ONE 2011, 6, e17046. [Google Scholar] [CrossRef]
- Sassanfar, M.; Samson, L. Identification and preliminary characterization of an O6-methylguanine DNA repair methyltransferase in the yeast Saccharomyces cerevisiae. J. Biol. Chem. 1990, 265, 20–25. [Google Scholar]
- Xiao, W.; Derfler, B.; Chen, J.; Samson, L. Primary sequence and biological functions of a Saccharomyces cerevisiae O6-methylguanine/O4-methylthymine DNA repair methyltransferase gene. EMBO J. 1991, 10, 2179–2186. [Google Scholar] [CrossRef]
- Andersen, K.S.; Bojsen, R.; Sørensen, L.G.R.; Nielsen, M.W.; Lisby, M.; Folkesson, A.; Regenberg, B. Genetic basis for Saccharomyces cerevisiae biofilm in liquid medium. G3 Genes|Genomes|Genetics 2014, 4, 1671–1680. [Google Scholar] [CrossRef]
- Tóth, R.; Tóth, A.; Papp, C.; Jankovics, F.; Vágvölgyi, C.; Alonso, M.F.; Bain, J.M.; Erwig, L.-P.; Gácser, A. Kinetic studies of Candida parapsilosis phagocytosis by macrophages and detection of intracellular survival mechanisms. Front. Microbiol. 2014, 5, 633. [Google Scholar]
- Brennan, M.; Thomas, D.Y.; Whiteway, M.; Kavanagh, K. Correlation between virulence of Candida albicans mutants in mice and Galleria mellonella larvae. FEMS Immunol. Med. Microbiol. 2002, 34, 153–157. [Google Scholar] [CrossRef]
- Slater, J.L.; Gregson, L.; Denning, D.W.; Warn, P.A. Pathogenicity of Aspergillus fumigatus mutants assessed in Galleria mellonella matches that in mice. Med. Mycol. 2011, 49, S107–S113. [Google Scholar] [CrossRef] [PubMed]
- Amorim-Vaz, S.; Delarze, E.; Ischer, F.; Sanglard, D.; Coste, A.T. Examining the virulence of Candida albicans transcription factor mutants using Galleria mellonella and mouse infection models. Front. Microbiol. 2015, 6, 367. [Google Scholar] [CrossRef] [PubMed]
- Jacobsen, I.D. Galleria mellonella as a model host to study virulence of Candida. Virulence 2014, 5, 237–239. [Google Scholar] [CrossRef] [PubMed]
- Bendel, C.M.; Hess, D.J.; Garni, R.M.; Henry-Stanley, M.; Wells, C.L. Comparative virulence of Candida albicans yeast and filamentous forms in orally and intravenously inoculated mice. Crit. Care Med. 2003, 31, 501–507. [Google Scholar] [CrossRef]
- Mora-Montes, H.M.; Bates, S.; Netea, M.G.; Castillo, L.; Brand, A.; Buurman, E.T.; Díaz-Jiménez, D.F.; Jan Kullberg, B.; Brown, A.J.P.; Odds, F.C.; et al. A multifunctional mannosyltransferase family in Candida albicans determines cell wall mannan structure and host-fungus interactions. J. Biol. Chem. 2010, 285, 12087–12095. [Google Scholar] [CrossRef]
- Erbs, P.; Exinger, F.; Jund, R. Characterization of the Saccharomyces cerevisiae FCY1 gene encoding cytosine deaminase and its homologue FCA1 of Candida albicans. Curr. Genet. 1997, 31, 1–6. [Google Scholar] [CrossRef]
- Harcus, D.; Nantel, A.; Marcil, A.; Rigby, T.; Whiteway, M. Transcription profiling of cyclic AMP signaling in Candida albicans. Mol. Biol. Cell 2004, 15, 4490–4499. [Google Scholar] [CrossRef]
- Xu, D.; Jiang, B.; Ketela, T.; Lemieux, S.; Veillette, K.; Martel, N.; Davison, J.; Sillaots, S.; Trosok, S.; Bachewich, C.; et al. Genome-wide fitness test and mechanism-of-action studies of inhibitory compounds in Candida albicans. PLOS Pathog. 2007, 3, e92. [Google Scholar] [CrossRef]
- Percival-Smith, A.; Segall, J. Characterization and mutational analysis of a cluster of three genes expressed preferentially during sporulation of Saccharomyces cerevisiae. Mol. Cell. Biol. 1986, 6, 2443–2451. [Google Scholar] [CrossRef]
- Nogi, Y.; Yano, R.; Dodd, J.; Carles, C.; Nomura, M. Gene RRN4 in Saccharomyces cerevisiae encodes the A12.2 subunit of RNA polymerase I and is essential only at high temperatures. Mol. Cell. Biol. 1993, 13, 114–122. [Google Scholar] [CrossRef]
- Chaillot, J.; Cook, M.A.; Corbeil, J.; Sellam, A. Genome-wide screen for haploinsufficient cell size genes in the opportunistic yeast Candida albicans. G3 Genes|Genomes|Genetics 2017, 7, 355–360. [Google Scholar] [CrossRef] [PubMed]
- Jones, D.G.L.; Rosamond, J. Isolation of a novel protein kinase-encoding gene from yeast by oligodeoxyribonucleotide probing. Gene 1990, 90, 87–92. [Google Scholar] [CrossRef]
- Moura, D.J.; Castilhos, B.; Immich, B.F.; Cañedo, A.D.; Henriques, J.A.P.; Lenz, G.; Saffi, J. Kin3 protein, a NIMA-related kinase of Saccharomyces cerevisiae, is involved in DNA adduct damage response. Cell Cycle 2010, 9, 2220–2229. [Google Scholar] [CrossRef] [PubMed]
- Pais, T.M.; Foulquié-Moreno, M.R.; Hubmann, G.; Duitama, J.; Swinnen, S.; Goovaerts, A.; Yang, Y.; Dumortier, F.; Thevelein, J.M. Comparative polygenic analysis of maximal ethanol accumulation capacity and tolerance to high ethanol levels of cell proliferation in yeast. PLoS Genet. 2013, 9, e1003548. [Google Scholar] [CrossRef]
- Sellam, A.; Chaillot, J.; Mallick, J.; Tebbji, F.; Richard Albert, J.; Cook, M.A.; Tyers, M. The p38/HOG stress-activated protein kinase network couples growth to division in Candida albicans. PLoS Genet. 2019, 15, e1008052. [Google Scholar] [CrossRef]
- Blankenship, J.R.; Fanning, S.; Hamaker, J.J.; Mitchell, A.P. An extensive circuitry for cell wall regulation in Candida albicans. PLOS Pathog. 2010, 6, e1000752. [Google Scholar] [CrossRef]
- Yoshikawa, K.; Tanaka, T.; Ida, Y.; Furusawa, C.; Hirasawa, T.; Shimizu, H. Comprehensive phenotypic analysis of single-gene deletion and overexpression strains of Saccharomyces cerevisiae. Yeast 2011, 28, 349–361. [Google Scholar] [CrossRef]
- Swanson, M.S.; Malone, E.A.; Winston, F. SPT5, an essential gene important for normal transcription in Saccharomyces cerevisiae, encodes an acidic nuclear protein with a carboxy-terminal repeat. Mol. Cell. Biol. 1991, 11, 4286. [Google Scholar] [CrossRef]
- Hadwiger, J.A.; Wittenberg, C.; Richardson, H.E.; de Barros Lopes, M.; Reed, S.I. A family of cyclin homologs that control the G1 phase in yeast. Proc. Natl. Acad. Sci. USA 1989, 86, 6255–6259. [Google Scholar] [CrossRef]
- Wagner, A. Energy costs constrain the evolution of gene expression. J. Exp. Zool. Part. B Mol. Dev. Evol. 2007, 308B, 322–324. [Google Scholar] [CrossRef]



| Gene Name | Ortholog Name | RNE | Gene Name | Ortholog Name | RNE |
|---|---|---|---|---|---|
| CPAR2_100460 | CpHBT4 | 122.5 ± 17.7 | CPAR2_302400 | ScMGT1 | 424.4 ± 90.5 |
| CPAR2_100470 | CpHBT3 | 18.6 ± 0.9 | CPAR2_303240 | ScPFA5 | 44.7 ± 2.8 |
| CPAR2_100540 | CaHAP5 | 7.6 ± 0.9 | CPAR2_303730 | ScTHR1 | 66.1 ± 26 |
| CPAR2_104420 | ScLTE1 | 378.5 ± 22.1 | CPAR2_400270 | ScHIT1 | 31.6 ± 2.3 |
| CPAR2_105250 | CaPHO85 | 44.8 ± 3.5 | CPAR2_406400 | ScRPA12 | 41.7 ± 7.3 |
| CPAR2_107020 | CaHHF1 | 118.2 ± 11.0 | CPAR2_500180 | ScKIN3 | 675.7 ± 89.3 |
| CPAR2_107240 | CaKTR4/MNT4 | 70.4 ± 12.4 | CPAR2_500360 | ScAMS1 | 37.2 ± 2.6 |
| CPAR2_108840 | ScSPS1 | 50.5 ± 9.6 | CPAR2_501400 | CaCWH41 | 90.0 ± 11.2 |
| CPAR2_109520 | CaTUP1 | 19.1 ± 4.5 | CPAR2_503290 | CaRAD53 | 218.4 ± 25.9 |
| CPAR2_200040 | - | 212.2 ± 17.3 | CPAR2_503760 | ScTMA46 | 7.3 ± 0.7 |
| CPAR2_200390 | CaSPT3 | 9.0 ± 0.6 | CPAR2_602370 | ScRAD18 | 17.3 ± 2.1 |
| CPAR2_201920 | ScMNT2 | 7.3 ± 1.1 | CPAR2_602820 | CaFCA1 | 28.4 ± 8.4 |
| CPAR2_204840 | CpHBT2 | 8.9 ± 1.8 | CPAR2_602840 | ScTFB4 | 176.7 ± 30.6 |
| CPAR2_205060 | CaCDC28 | 30.6 ± 5.6 | CPAR2_700550 | ScRSC8 | 4.5 ± 0.5 |
| CPAR2_208600 | CaCPH1 | 44.5 ± 3.6 | CPAR2_703840 | ScSLM5 | 52.5 ± 8.4 |
| CPAR2_209240 | CaCDC19/PYK | 2.6 ± 0.0 | CPAR2_804030 | ScGSC2 | 134.6 ± 29.9 |
| CPAR2_209520 | CaMKK2 | 7.8 ± 1.3 | CPAR2_805930 | CaTEC1 | 34.5 ± 6.9 |
| CPAR2_300080 | ScADK2 | 134.8 ± 7.3 | CPAR2_806950 | ScNOB1 | 65.7 ± 9.9 |
| CPAR2_301360 | CaPMR1 | 38.9 ± 3.1 |
| Stressor | Caffeine (10 mM) | CFW (25 µg/mL) | CFW (50 µg/mL) | CR (10 µg/mL) | CR (25 µg/mL) | CR (50 µg/mL) | CR (75 µg/mL) | CR (100 µg/mL) | SDS (0.04% m/v) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| T (°C) | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 | 30 | 37 |
| CPAR2_109520OE (CpTUP1) | ||||||||||||||||||
| CPAR2_200040OE | ||||||||||||||||||
| CPAR2_302400OE (CpMGT1) | ||||||||||||||||||
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Pál, S.E.; Tóth, R.; Nosanchuk, J.D.; Vágvölgyi, C.; Németh, T.; Gácser, A. A Candida parapsilosis Overexpression Collection Reveals Genes Required for Pathogenesis. J. Fungi 2021, 7, 97. https://doi.org/10.3390/jof7020097
Pál SE, Tóth R, Nosanchuk JD, Vágvölgyi C, Németh T, Gácser A. A Candida parapsilosis Overexpression Collection Reveals Genes Required for Pathogenesis. Journal of Fungi. 2021; 7(2):97. https://doi.org/10.3390/jof7020097
Chicago/Turabian StylePál, Sára E., Renáta Tóth, Joshua D. Nosanchuk, Csaba Vágvölgyi, Tibor Németh, and Attila Gácser. 2021. "A Candida parapsilosis Overexpression Collection Reveals Genes Required for Pathogenesis" Journal of Fungi 7, no. 2: 97. https://doi.org/10.3390/jof7020097
APA StylePál, S. E., Tóth, R., Nosanchuk, J. D., Vágvölgyi, C., Németh, T., & Gácser, A. (2021). A Candida parapsilosis Overexpression Collection Reveals Genes Required for Pathogenesis. Journal of Fungi, 7(2), 97. https://doi.org/10.3390/jof7020097







