Review of the Novel Echinocandin Antifungal Rezafungin: Animal Studies and Clinical Data
Abstract
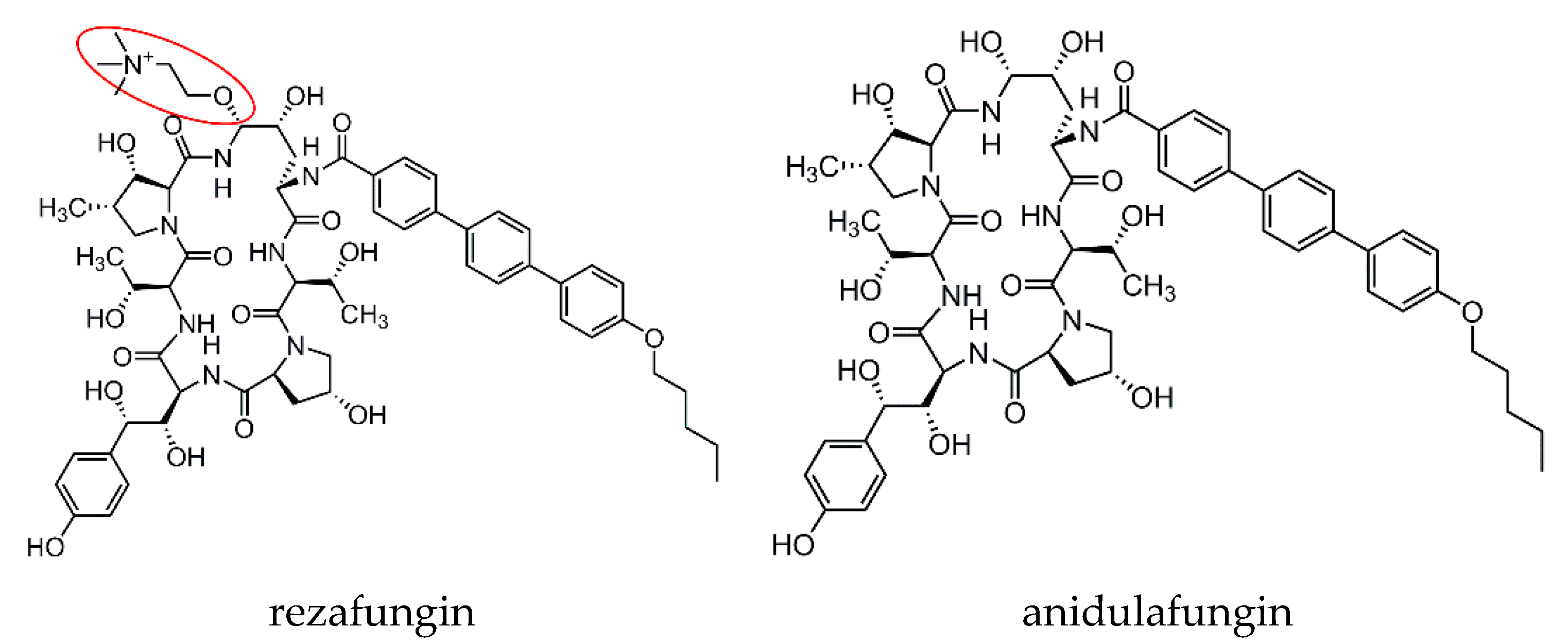
1. Introduction
2. Preclinical Pharmacokinetics
3. In Vivo Effectiveness
3.1. Animal Models
3.2. Efficacy/Pharmacodynamic Characterization in Invasive Candidiasis Model
3.3. In Vivo Efficacy against Other Fungal Pathogens
4. Clinical Development
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
References
- Hector, R.F. Compounds active against cell walls of medically important fungi. Clin. Microbiol. Rev. 1993, 6, 1–21. [Google Scholar] [CrossRef] [PubMed]
- Pappas, P.G.; Kauffman, C.A.; Andes, D.; Benjamin, D.K., Jr.; Calandra, T.F.; Edwards, J.E., Jr.; Filler, S.G.; Fisher, J.F.; Kullberg, B.J.; Ostrosky-Zeichner, L.; et al. Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2009, 48, 503–535. [Google Scholar] [CrossRef] [PubMed]
- Pappas, P.G.; Kauffman, C.A.; Andes, D.R.; Clancy, C.J.; Marr, K.A.; Ostrosky-Zeichner, L.; Reboli, A.C.; Schuster, M.G.; Vazquez, J.A.; Walsh, T.J.; et al. Executive Summary: Clinical Practice Guideline for the Management of Candidiasis: 2016 Update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2016, 62, 409–417. [Google Scholar] [CrossRef] [PubMed]
- Aruanno, M.; Glampedakis, E.; Lamoth, F. Echinocandins for the Treatment of Invasive Aspergillosis: From Laboratory to Bedside. Antimicrob. Agents Chemother. 2019, 63, e00399-19. [Google Scholar] [CrossRef] [PubMed]
- Patterson, T.F.; Thompson, G.R., 3rd; Denning, D.W.; Fishman, J.A.; Hadley, S.; Herbrecht, R.; Kontoyiannis, D.P.; Marr, K.A.; Morrison, V.A.; Nguyen, M.H.; et al. Practice Guidelines for the Diagnosis and Management of Aspergillosis: 2016 Update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2016, 63, e1–e60. [Google Scholar] [CrossRef]
- Krishnan, B.R.; James, K.D.; Polowy, K.; Bryant, B.J.; Vaidya, A.; Smith, S.; Laudeman, C.P. CD101, a novel echinocandin with exceptional stability properties and enhanced aqueous solubility. J. Antibiot. 2017, 70, 130–135. [Google Scholar] [CrossRef]
- Ong, V.; James, K.D.; Smith, S.; Krishnan, B.R. Pharmacokinetics of the Novel Echinocandin CD101 in Multiple Animal Species. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef]
- Sandison, T.; Ong, V.; Lee, J.; Thye, D. Safety and Pharmacokinetics of CD101 IV, a Novel Echinocandin, in Healthy Adults. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef] [PubMed]
- James, K.D.; Laudeman, C.P.; Malkar, N.B.; Krishnan, R.; Polowy, K. Structure-Activity Relationships of a Series of Echinocandins and the Discovery of CD101, a Highly Stable and Soluble Echinocandin with Distinctive Pharmacokinetic Properties. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Perez, W.B.; Jiménez-Ortigosa, C.; Hough, G.; Locke, J.B.; Ong, V.; Bartizal, K.; Perlin, D.S. CD101: A novel long-acting echinocandin. Cell. Microbiol. 2016, 18, 1308–1316. [Google Scholar] [CrossRef] [PubMed]
- Zhao, Y.; Prideaux, B.; Nagasaki, Y.; Lee, M.H.; Chen, P.Y.; Blanc, L.; Ho, H.; Clancy, C.J.; Nguyen, M.H.; Dartois, V.; et al. Unraveling Drug Penetration of Echinocandin Antifungals at the Site of Infection in an Intra-abdominal Abscess Model. Antimicrob. Agents Chemother. 2017, 61, e01009-17. [Google Scholar] [CrossRef]
- Cushion, M.; Ashbaugh, A.; Lynch, K.; Linke, M.J.; Bartizal, K. Efficacy of CD101, a Novel Echinocandin, in Prevention of Pneumocystis Pneumonia (PCP): Thwarting the Biphasic Life Cycle of Pneumocystis. Blood 2016, 128, 3396-3396. [Google Scholar] [CrossRef]
- Ong, V.; Hough, G.; Schlosser, M.; Bartizal, K.; Balkovec, J.M.; James, K.D.; Krishnan, B.R. Preclinical Evaluation of the Stability, Safety, and Efficacy of CD101, a Novel Echinocandin. Antimicrob. Agents Chemother. 2016, 60, 6872–6879. [Google Scholar] [CrossRef] [PubMed]
- Miesel, L.; Lin, K.Y.; Ong, V. Rezafungin treatment in mouse models of invasive candidiasis and aspergillosis: Insights on the PK/PD pharmacometrics of rezafungin efficacy. Pharmacol. Res. Perspect. 2019, 7, e00546. [Google Scholar] [CrossRef] [PubMed]
- Wiederhold, N.P.; Najvar, L.K.; Jaramillo, R.; Olivo, M.; Wickes, B.L.; Catano, G.; Patterson, T.F. Extended-Interval Dosing of Rezafungin against Azole-Resistant Aspergillus fumigatus. Antimicrob. Agents Chemother. 2019, 63, e01165-19. [Google Scholar] [CrossRef] [PubMed]
- Lepak, A.J.; Zhao, M.; Andes, D.R. Pharmacodynamic Evaluation of Rezafungin (CD101) against Candida auris in the Neutropenic Mouse Invasive Candidiasis Model. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef]
- Lepak, A.J.; Zhao, M.; VanScoy, B.; Ambrose, P.G.; Andes, D.R. Pharmacodynamics of a Long-Acting Echinocandin, CD101, in a Neutropenic Invasive-Candidiasis Murine Model Using an Extended-Interval Dosing Design. Antimicrob. Agents Chemother. 2018, 62. [Google Scholar] [CrossRef]
- Lepak, A.J.; Zhao, M.; Andes, D.R. Determination of Pharmacodynamic Target Exposures for Rezafungin against Candida tropicalis and Candida dubliniensis in the Neutropenic Mouse Disseminated Candidiasis Model. Antimicrob. Agents Chemother. 2019, 63, e01556-19. [Google Scholar] [CrossRef]
- Hager, C.L.; Larkin, E.L.; Long, L.A.; Ghannoum, M.A. Evaluation of the efficacy of rezafungin, a novel echinocandin, in the treatment of disseminated Candida auris infection using an immunocompromised mouse model. J. Antimicrob. Chemother. 2018, 73, 2085–2088. [Google Scholar] [CrossRef]
- Ong, V.; Ashbaugh, A.; Cushion, M.T. Rezafungin Prevention of Pneumocystis Pneumonia and Pneumocystis Reactivation Using Different Doses and Durations of Prophylaxis in a Mouse Model. Biol. Blood Marrow Transplant. 2020, 26, S328–S329. [Google Scholar] [CrossRef]
- Long, L.; Herrada, J.; Caley, D.; Munguba, G.; Sherif, R.; Bartizal, K.; Ghannoum, M.A. Evaluation of the efficacy of rezafungin in the treatment of Candida albicans endophthalmitis using a rabbit model. In Proceedings of the European Congress of Clinical Microbiology & Infectious Diseases (ECCMID) 2020, Paris, France, 18–21 April 2020. [Google Scholar]
- Morales-López, S.E.; Parra-Giraldo, C.M.; Ceballos-Garzón, A.; Martínez, H.P.; Rodríguez, G.J.; Álvarez-Moreno, C.A.; Rodríguez, J.Y. Invasive Infections with Multidrug-Resistant Yeast Candida auris, Colombia. Emerg. Infect. Dis. 2017, 23, 162–164. [Google Scholar] [CrossRef] [PubMed]
- Forsberg, K.; Woodworth, K.; Walters, M.; Berkow, E.L.; Jackson, B.; Chiller, T.; Vallabhaneni, S. Candida auris: The recent emergence of a multidrug-resistant fungal pathogen. Med. Mycol. 2019, 57, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Vallabhaneni, S.; Kallen, A.; Tsay, S.; Chow, N.; Welsh, R.; Kerins, J.; Kemble, S.K.; Pacilli, M.; Black, S.R.; Landon, E.; et al. Investigation of the First Seven Reported Cases of Candida auris, a Globally Emerging Invasive, Multidrug-Resistant Fungus-United States, May 2013–August 2016. Am. J. Transplant. 2017, 17, 296–299. [Google Scholar] [CrossRef] [PubMed]
- Lakota, E.A.; Bader, J.C.; Ong, V.; Bartizal, K.; Miesel, L.; Andes, D.R.; Bhavnani, S.M.; Rubino, C.M.; Ambrose, P.G.; Lepak, A.J. Pharmacological Basis of CD101 Efficacy: Exposure Shape Matters. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef]
- Berkow, E.L.; Lockhart, S.R. Activity of CD101, a long-acting echinocandin, against clinical isolates of Candida auris. Diagn. Microbiol. Infect. Dis. 2018, 90, 196–197. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Messer, S.A.; Rhomberg, P.R.; Castanheira, M. CD101, a long-acting echinocandin, and comparator antifungal agents tested against a global collection of invasive fungal isolates in the SENTRY 2015 Antifungal Surveillance Program. Int. J. Antimicrob. Agents 2017, 50, 352–358. [Google Scholar] [CrossRef]
- Pfaller, M.A.; Messer, S.A.; Rhomberg, P.R.; Castanheira, M. Activity of a Long-Acting Echinocandin (CD101) and Seven Comparator Antifungal Agents Tested against a Global Collection of Contemporary Invasive Fungal Isolates in the SENTRY 2014 Antifungal Surveillance Program. Antimicrob. Agents Chemother. 2017, 61. [Google Scholar] [CrossRef]
- Cushion, M.T.; Linke, M.J.; Ashbaugh, A.; Sesterhenn, T.; Collins, M.S.; Lynch, K.; Brubaker, R.; Walzer, P.D. Echinocandin treatment of pneumocystis pneumonia in rodent models depletes cysts leaving trophic burdens that cannot transmit the infection. PLoS ONE 2010, 5, e8524. [Google Scholar] [CrossRef]
- Thompson, G.R.; Vazquez, J.; Soriano, A.; Skoutelis, A.; Ostrosky-Zeichner, L.; Mena, K.; Navalta, L.; Sandison, T.; Pappas, P. 1718. Rezafungin Clinical Safety and Efficacy in Patients With Candidemia and/or Invasive Candidiasis in the Randomized, Double-Blind, Multicenter, Phase 2 STRIVE Study. Open Forum Infect. Dis. 2018, 5, S52. [Google Scholar] [CrossRef][Green Version]
- Thompson, G.R.; Honore, P.M.; Horcajada, J.P.; Fortun, J.; Hites, M.; Bassetti, M.; Mena, K.; Navalta, L.; Viani, R.; Sandison, T.; et al. Rezafungin Clinical Safety and Efficacy in the Treatment of Candidaemia and/or Invasive Candidiasis: Combined Results from the STRIVE Phase 2 Trial Parts A and B. In Proceedings of the Trends in Medicial Mycology, Nice, France, 11–14 October 2019. [Google Scholar]
- Nyirjesy, P.; Alessio, C.; Jandourek, A.; Lee, J.D.; Sandison, T.; Sobel, J.D. CD101 Topical Compared With Oral Fluconazole for Acute Vulvovaginal Candidiasis: A Randomized Controlled Trial. J. Low. Genit. Tract Dis. 2019, 23, 226–229. [Google Scholar] [CrossRef]
| Aspect | Animal Model | Feature |
|---|---|---|
| PK/PD | Healthy mouse, rat, dog, cynomolgus monkey, chimpanzee; Immunocompetent mouse model of invasive candidiasis; Immunocompetent mouse model of intra-abdominal candidiasis; Neutropenic mouse model of invasive candidiasis | Dose proportional drug exposure (Cmax and AUC); Very long half-life (longer than any of currently approved echinocandin drug); Low clearance and wide tissue distribution; Quick and sustained penetration at infected tissue sites; AUC/MIC is the best index associated with efficacy; The shape of exposure curve also influences efficacy |
| Efficacy | Neutropenic mouse model of invasive candidiasis; Immunocompetent mouse model of intra-abdominal candidiasis; Immunocompetent rabbit model of invasive candidiasis; Neutropenic mouse model of disseminated invasive aspergillosis; Immunosuppressed mouse model of Pneumocystis pneumonia | Comparable or better efficacy than comparator drug (anidulafungin or micafungin) in Candida infection models, including those caused by echinocandin- and azole-resistant Candida strains; Effective in improving survival and reducing kidney burdens in both azole-sensitive and -resistant Aspergillus infections; Comparable efficacy to the standard of care (TMP/SMX) in prevention of Pneumocystis pneumonia |
| Clinical Status | Trial (ClinicalTrials.gov Identifier) | Objective | Key Finding |
|---|---|---|---|
| Phase 1 (completed) | Single-ascending-dose study (NCT02516904) | Safety, tolerability, and PK | No safety issues were noted; Dose-proportional plasma exposures (AUC and Cmax) and low clearance; Long half-life (~80 h after first dose and ~150 h following addition dose) |
| Multiple-ascending-dose study (NCT02551549) | |||
| Phase 2 (completed) | STRIVE (NCT02734862) | Efficacy to treat candidemia and invasive candidiasis | Rezafungin IV 400 mg first week followed by 200 mg once weekly regimen showed greater efficacy than caspofungin |
| RADIANT (NCT02733432) | Efficacy to treat vulvovaginitis | Topical formulations of rezafungin were safe and well tolerated; Cure rates of topical rezafungin were lower than those achieved with fluconazole | |
| Phase 3 (ongoing) | ReSTORE (NCT03667690) | Efficacy to treat candidemia and invasive candidiasis | To be determined |
| ReSPECT (NCT04368559) | Efficacy to prevent invasive fungal infections due to Candida, Aspergillus, and Pneumocystis | To be determined |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Zhao, Y.; Perlin, D.S. Review of the Novel Echinocandin Antifungal Rezafungin: Animal Studies and Clinical Data. J. Fungi 2020, 6, 192. https://doi.org/10.3390/jof6040192
Zhao Y, Perlin DS. Review of the Novel Echinocandin Antifungal Rezafungin: Animal Studies and Clinical Data. Journal of Fungi. 2020; 6(4):192. https://doi.org/10.3390/jof6040192
Chicago/Turabian StyleZhao, Yanan, and David S. Perlin. 2020. "Review of the Novel Echinocandin Antifungal Rezafungin: Animal Studies and Clinical Data" Journal of Fungi 6, no. 4: 192. https://doi.org/10.3390/jof6040192
APA StyleZhao, Y., & Perlin, D. S. (2020). Review of the Novel Echinocandin Antifungal Rezafungin: Animal Studies and Clinical Data. Journal of Fungi, 6(4), 192. https://doi.org/10.3390/jof6040192






