Proof-of-Concept of IMU-Based Detection of ICU-Relevant Agitation Motion Patterns in Healthy Volunteers
Abstract
1. Introduction
2. Materials and Methods
2.1. Study Design and Ethics
2.2. Participant Demographics
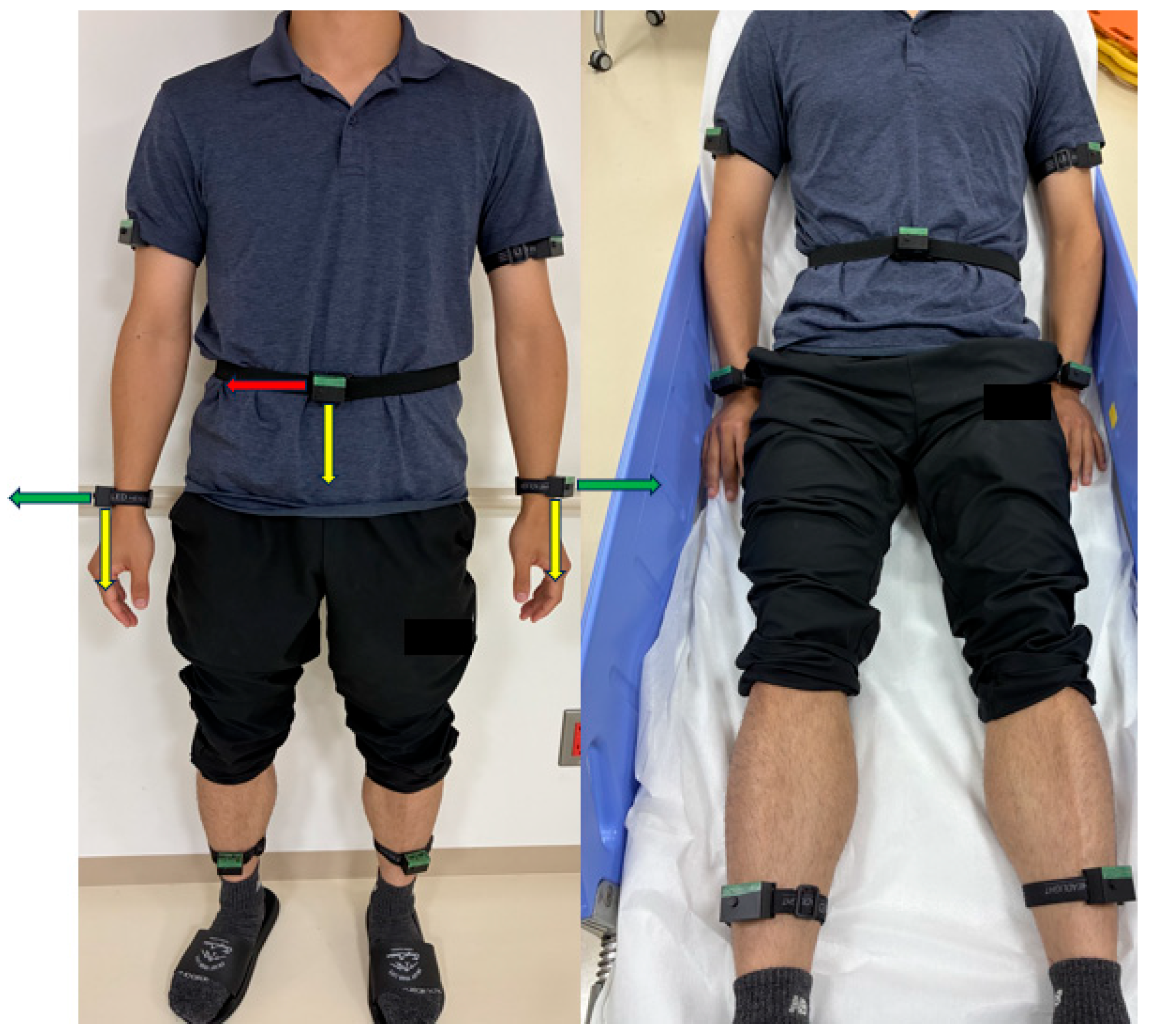
2.3. Overview of IMU Sensors
2.4. Data Collection
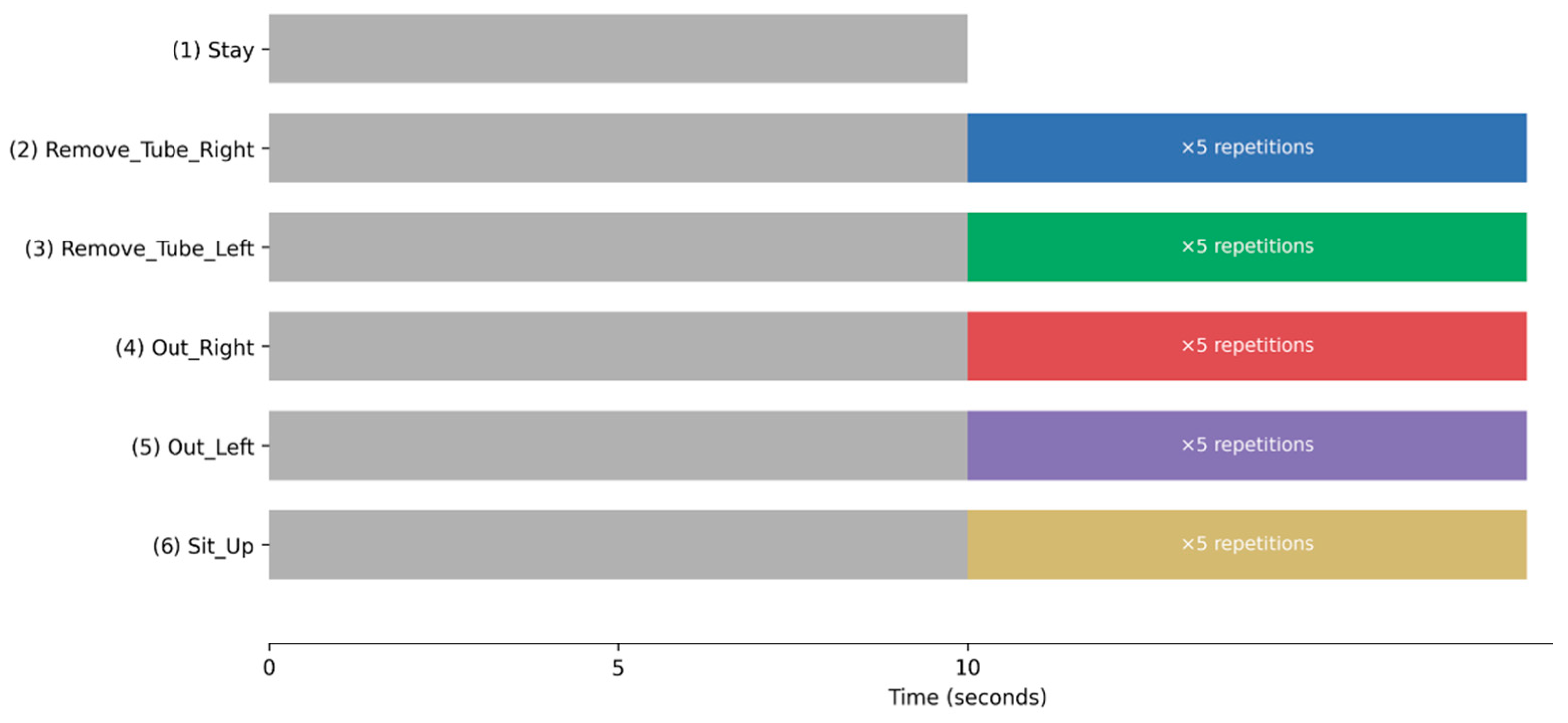
- Stay: lie still on the examination bed for 10 s;
- Remove_Tube_Right: move the right fingertip as close to the nose as possible;
- Remove_Tube_Left: move the left fingertip as close to the nose as possible;
- Out_Right: simultaneously extend the right arm and right leg beyond the side rail of the examination bed;
- Out_Left simultaneously extends the left arm and leg beyond the side rail of the examination bed;
- Sit_Up: transition from a supine to a sitting position.
2.5. Standardization of Movement Duration and Temporal Segmentation Framework
2.6. Windowing Strategy and Phase-Rich Temporal Representation
- •
- Movement onset;
- •
- Peak execution;
- •
- Movement offset;
- •
- Transient micro-movements;
- •
- Static or near-static resting behavior.
2.7. Convolutional Neural Network
2.7.1. Model Structure
2.7.2. Training and Validation Protocol
2.7.3. Training Details and Reproducibility
2.7.4. Evaluation Metrics
3. Results
3.1. Missing Values
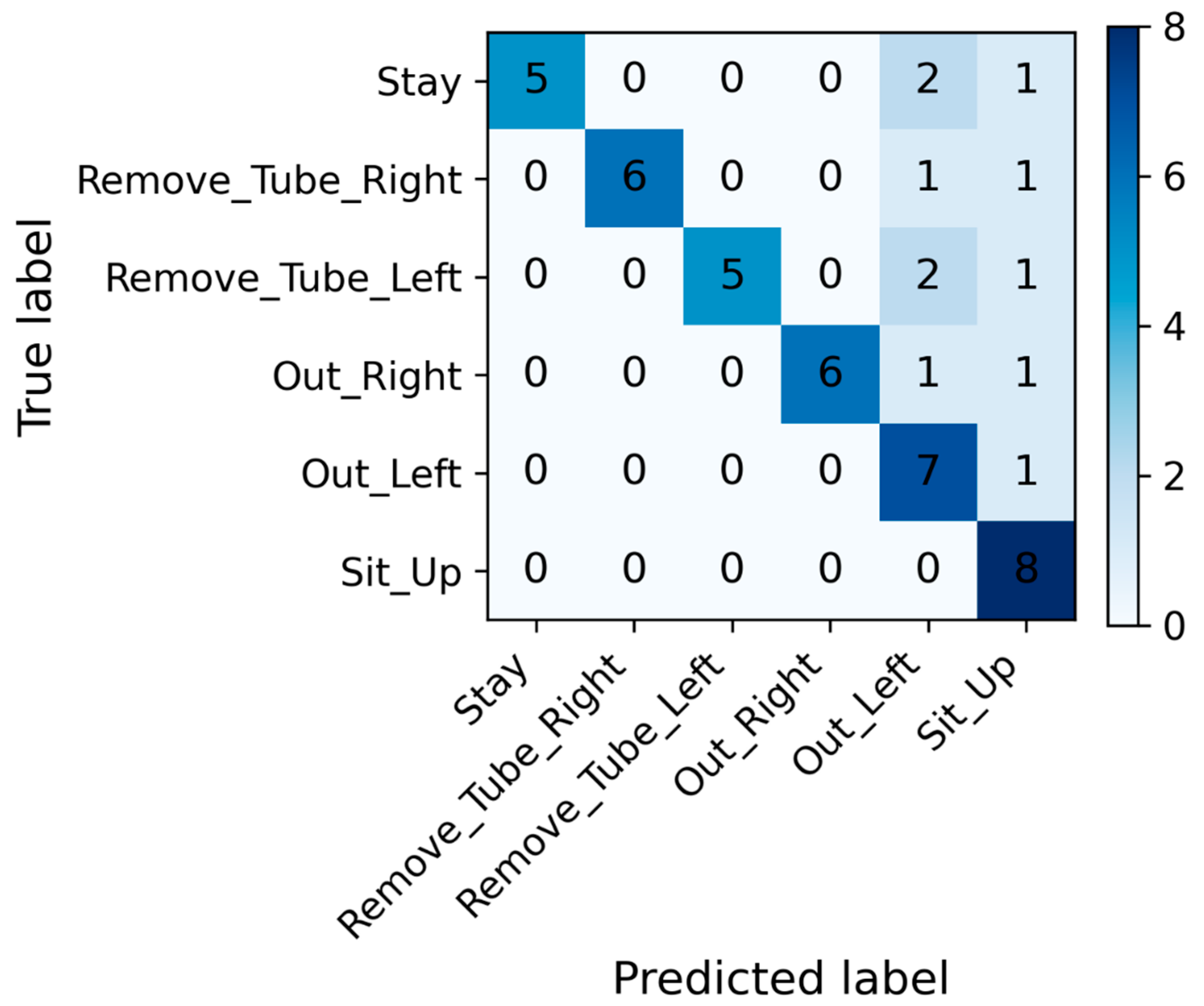
3.2. Primary Outcomes (Accuracy, Sensitivity, Specificity, Precision, and F1 Score)
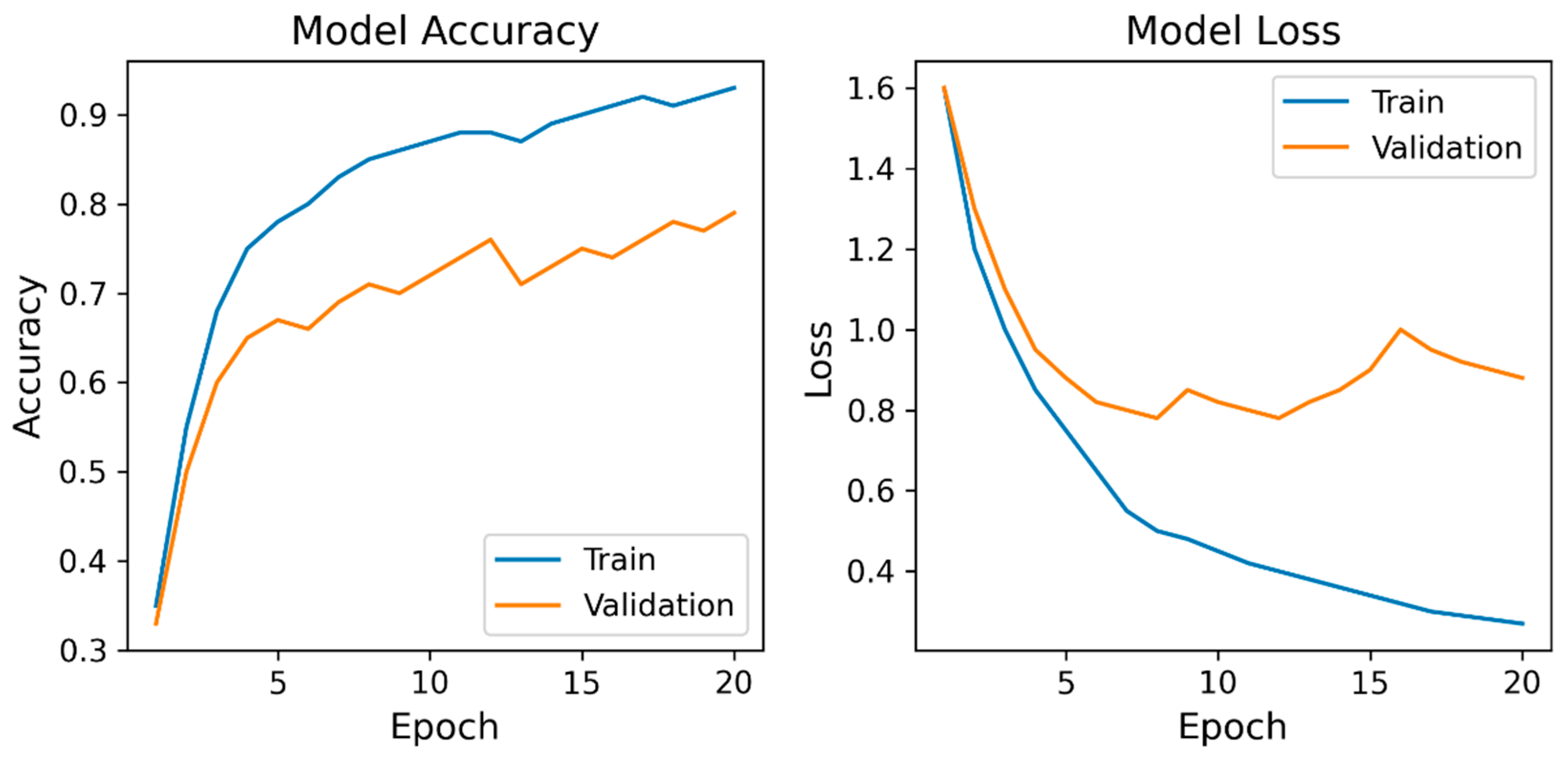
3.3. Secondary Outcome (Learning Curves)
4. Discussion
- Clinical validation in ICU settings: evaluate the IMU-based system in ICU patients with delirium or agitation to assess its performance under real-world conditions, including prolonged monitoring, sensor displacement, and environmental noise;
- Model and computational optimization: develop lightweight or hybrid architectures that maintain temporal feature extraction while enabling real-time inference on resource-constrained hardware;
- Sensor reduction and optimization: apply sensor selection and feature importance analyses to identify the minimal sensor configurations that preserve classification performance while improving clinical feasibility; and
- Extended and continuous monitoring analysis: investigate the robustness of the system using longer continuous recordings to capture dynamic transitions between resting and agitation-related movements.
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ICU | Intensive care unit |
| IMU | Inertial measurement unit |
| CNN | Convolutional neural network |
| BMI | Body mass index |
References
- Metheny, N.A.; Krieger, M.M.; Healey, F.; Meert, K.L. A review of guidelines to distinguish between gastric and pulmonary placement of nasogastric tubes. Heart Lung 2019, 48, 226–235. [Google Scholar] [CrossRef]
- Motta, A.P.G.; Rigobello, M.C.G.; Silveira, R.C.C.P.; Gimenes, F.R.E. Nasogastric/nasoenteric tube-related adverse events: An integrative review. Rev. Lat. Am. De Enferm. 2021, 29, e3400. [Google Scholar] [CrossRef]
- Kang, J.; Yoo, Y.-S. Risk factors associated with unplanned removal of nasogastric tubes in neurocritical patients. Korean J. Adult Nurs. 2022, 34, 158–167. [Google Scholar] [CrossRef]
- Wu, G.; Soo, A.; Ronksley, P.; Holroyd-Leduc, J.; Bagshaw, S.M.; Wu, Q.; Quan, H.; Stelfox, H.T. A Multicenter cohort study of falls among patients admitted to the ICU. Crit. Care Med. 2022, 50, 810–818. [Google Scholar] [CrossRef]
- Lewis, K.; Balas, M.C.; Stollings, J.L.; McNett, M.; Girard, T.D.; Chanques, G.; Kho, M.E.; Pandharipande, P.P.; Weinhouse, G.L.; Brummel, N.E.; et al. A Focused Update to the Clinical Practice Guidelines for the Prevention and Management of Pain, Anxiety, Agitation/Sedation, Delirium, Immobility, and Sleep Disruption in Adult Patients in the ICU. Crit. Care Med. 2025, 53, e711–e727. [Google Scholar] [CrossRef]
- LacKamp, A.N.; Stevens, R.D. Neurologic Implications of Critical Illness and Organ Dysfunction. In Textbook of Neurointensive Care; Springer: London, UK, 2013; pp. 409–425. [Google Scholar] [CrossRef]
- Mellott, K.G.; Grap, M.J.; Munro, C.L.; Sessler, C.N.; Wetzel, P.A. Patient-Ventilator Dyssynchrony: Clinical Significance and Implications for Practice. Crit. Care Nurse 2009, 29, 41–55. [Google Scholar] [CrossRef] [PubMed]
- Almeida, T.M.L.; Azevedo, L.C.P.; Nosé, P.M.G.; Freitas, F.G.R.; Machado, F.R. Risk factors for agitation in critically ill patients. Rev. Bras. Ter. Intensiv. 2016, 28, 413–419. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.B.; Wu, H.Y.; Duan, M.L.; Yang, R.L.; Ji, C.H.; Liu, J.J.; Zhao, H. Delirium in the ICU: How much do we know? A narrative review. Ann. Med. 2024, 56, 2405072. [Google Scholar] [CrossRef]
- Bonfiglio, A.; Farella, E.; Tacconi, D.; Bongers, R.M. Effects of different inertial measurement unit sensor-to-segment calibrations on clinical 3-dimensional humerothoracic joint angles estimation. J. Appl. Biomech. 2025, 41, 37–46. [Google Scholar] [CrossRef]
- Liengswangwong, W.; Lertviboonluk, N.; Yuksen, C.; Jamkrajang, P.; Limroongreungrat, W.; Mongkolpichayaruk, A.; Jenpanitpong, C.; Watcharakitpaisan, S.; Palee, C.; Reechaipichitkool, P.; et al. Validity of inertial measurement unit (IMU sensor) for measurement of cervical spine motion, compared with eight optoelectronic 3D cameras under spinal immobilization devices. Med. Devices 2024, 17, 261–269. [Google Scholar] [CrossRef]
- Jo, D.; Kim, H. Evaluating walkability across age groups and flooring materials using IMU sensors. Front. Public Health 2024, 12, 1509602. [Google Scholar] [CrossRef]
- Smits, S.R.; Hinterwimmer, F.; Burghart, R.; von Eisenhart-Rothe, R.; Rueckert, D. The use of artificial intelligence and wearable inertial measurement units in medicine: Systematic review. JMIR MHealth UHealth 2025, 13, e60521. [Google Scholar] [CrossRef]
- Wei, S.; Wu, Z. The application of wearable sensors and machine learning algorithms in rehabilitation training: A systematic review. Sensors 2023, 23, 7667. [Google Scholar] [CrossRef]
- Davoudi, A.; Manini, T.M.; Bihorac, A.; Rashidi, P. Role of wearable accelerometer devices in delirium studies: A systematic review. Crit. Care Explor. 2019, 1, e0027. [Google Scholar] [CrossRef] [PubMed]
- Angelucci, A.; Greco, M.; Cecconi, M.; Aliverti, A. Wearable devices for patient monitoring in the intensive care unit. Intensive Care Med. Exp. 2025, 13, 26. [Google Scholar] [CrossRef] [PubMed]
- Trevethan, R. Sensitivity, specificity, and predictive values: Foundations, pliabilities, and pitfalls in research and practice. Front. Public Health 2017, 5, 307. [Google Scholar] [CrossRef]
- Ely, E.W.; Inouye, S.K.; Bernard, G.R.; Gordon, S.; Francis, J.; May, L.; Truman, B.; Speroff, T.; Gautam, S.; Margolin, R.; et al. Delirium in mechanically ventilated patients: Validity and reliability of the Confusion Assessment Method for the Intensive Care Unit (CAM-ICU). J. Am. Med. Assoc. 2001, 286, 2703–2710. [Google Scholar] [CrossRef] [PubMed]
- Devlin, J.W.; Skrobik, Y.; Gélinas, C.; Needham, D.M.; Slooter, A.J.C.; Pandharipande, P.P.; Watson, P.L.; Weinhouse, G.L.; Nunnally, M.E.; Rochwerg, B.; et al. Clinical practice guidelines for the prevention and management of pain, agitation/sedation, delirium, immobility, and sleep disruption in adult patients in the ICU. Crit. Care Med. 2018, 46, e825–e873. [Google Scholar] [CrossRef]
- Gusmao-Flores, D.; Salluh, J.I.F.; Chalhub, R.Á.; Quarantini, L.C. The confusion assessment method for the intensive care unit (CAM-ICU) and intensive care delirium screening checklist (ICDSC) for the diagnosis of delirium: A systematic review and meta-analysis of clinical studies. Crit. Care 2012, 16, R115. [Google Scholar] [CrossRef]
- Chen, T.-J.; Chung, Y.-W.; Chang, H.-C.R.; Chen, P.-Y.; Wu, C.-R.; Hsieh, S.-H.; Chiu, H.-Y. Diagnostic accuracy of the CAM-ICU and ICDSC in detecting intensive care unit delirium: A bivariate meta-analysis. Int. J. Nurs. Stud. 2021, 113, 103782. [Google Scholar] [CrossRef]
- Diao, Y.; Yu, X.; Zhang, Q.; Chen, X. The predictive value of confusion assessment method-intensive care unit and intensive care delirium screening checklist for delirium in critically ill patients in the intensive care unit: A systematic review and meta-analysis. Nurs. Crit. Care 2024, 29, 1224–1235. [Google Scholar] [CrossRef] [PubMed]
- Hanna, A.; Jirsch, J.; Alain, C.; Corvinelli, S.; Lee, J.S. Electroencephalogram Measured Functional Connectivity for Delirium Detection: A Systematic Review. Front. Neurosci. 2023, 17, 1274837. [Google Scholar] [CrossRef]
- Roberson, S.W.; Azeez, A.N.; Fulton, N.J.; Zhang, C.K.; Lee, X.T.A.; Ye, F.; Pandharipande, P.; Brummel, E.N.; Patel, B.M.; Ely, E.W. Quantitative EEG Signatures of Delirium and Coma in Mechanically Ventilated ICU Patients. Clin. Neurophysiol. 2023, 146, 40–48. [Google Scholar] [CrossRef]
- Huespe, I.; Giunta, D.; Acosta, K.; Avila, D.; Prado, E.; Sanghavi, D.; Carboni Bisso, I.; Giannasi, S.; Carini, F.C. Comparing Bispectral Index Monitoring vs Clinical Assessment for Deep Sedation in the ICU Effects on Delirium Reduction and Sedative Drug Doses—A Randomized Trial. Chest 2024, 166, 733–742. [Google Scholar] [CrossRef]
- Manning, J.; Chiasson, M. Does Bispectral Index Monitoring Belong in the Intensive Care Unit Setting?: A Narrative Review of Evidence. Dimens. Crit. Care Nurs. 2025, 44, 231–238. [Google Scholar] [CrossRef]
- Kamdar, B.B.; Kadden, D.J.; Vangala, S.; Elashoff, D.A.; Ong, M.K.; Martin, J.L.; Needham, D.M. Feasibility of Continuous Actigraphy in Patients in a Medical Intensive Care Unit. Am. J. Crit. Care 2017, 26, 329–335. [Google Scholar] [CrossRef]
- Ahmed, A.; Garcia-Agundez, A.; Petrovic, I.; Radaei, F.; Fife, J.; Zhou, J.; Karas, H.; Moody, S.; Drake, J.; Jones, R.N.; et al. Delirium detection using wearable sensors and machine learning in patients with intracerebral hemorrhage. Front. Neurol. 2023, 14, 1135472. [Google Scholar] [CrossRef] [PubMed]
- Schwab, K.E.; To, A.Q.; Chang, J.; Ronish, B.; Needham, D.M.; Martin, J.L.; Kamdar, B.B. Actigraphy to Measure Physical Activity in the Intensive Care Unit: A Systematic Review. J. Intensive Care Med. 2020, 35, 1323–1331. [Google Scholar] [CrossRef]
- Smith, J.; Parikh, D.; Tate, V.; Siddicky, S.F.; Hsiao, H.-Y. Validity of Valor inertial measurement unit for upper and lower extremity joint angles. Sensors 2024, 24, 5833. [Google Scholar] [CrossRef] [PubMed]

| Characteristics | Total (N = 15) |
|---|---|
| Sex [male], n (%) | 13.0 (86.7%) |
| Age [years], median (IQR) | 23.0 (21.0–24.5) |
| Weight [kg], median (IQR) | 66.0 (62.0–77.5) |
| Height [cm], median (IQR) | 172.0 (165.0–176.0) |
| BMI [kg/m2], median (IQR) | 23.8 (21.8–25.2) |
| Underlying disease, n (%) α | 4.0 (26.7%) |
| Movement Category | Accuracy (%) | Sensitivity (%) | Specificity (%) | Precision (%) | F1 Score (%) |
|---|---|---|---|---|---|
| Overall | 77.0 (70.0–85.4) | 77.0 (70.8–85.4) | 95.4 (94.1–97.0) | 84.5 (69.6–89.4) | 77.4 (66.4–85.6) |
| Stay | 100 (0–100) | 100 (0–100) | 95.0 (92.5–100) | 61.5 (0–77.7) | 72.7 (0–84.2) |
| Remove_Tube_Right | 75.0 (75.0–87.5) | 75.0 (75.0–87.5) | 100 (97.5–100) | 100 (80.0–100) | 85.7 (71.4–90.4) |
| Remove_Tube_Left | 87.5 (62.5–100) | 87.5 (62.5–100) | 100 (95.0–100) | 100 (76.3–100) | 84.2 (76.9–91.1) |
| Out_Right | 75.0 (62.5–87.5) | 75.0 (62.5–87.5) | 100 (97.5–100) | 100 (85.7–100) | 85.7 (71.4–93.3) |
| Out_Left | 87.5 (75.0–87.5) | 87.5 (75.0–87.5) | 100 (95.0–100) | 100 (77.7–100) | 82.3 (76.5–88.8) |
| Sit_Up | 87.5 (75.0–100) | 87.5 (75.0–100) | 95.0 (90.0–100) | 80.0 (61.5–100) | 77.7 (61.5–85.7) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.
Share and Cite
Yokoyama, R.; Hayasaka, T.; Harada, T.; Huang, S.; Yarimizu, K.; Yokoyama, M.; Kawamae, K. Proof-of-Concept of IMU-Based Detection of ICU-Relevant Agitation Motion Patterns in Healthy Volunteers. Bioengineering 2026, 13, 164. https://doi.org/10.3390/bioengineering13020164
Yokoyama R, Hayasaka T, Harada T, Huang S, Yarimizu K, Yokoyama M, Kawamae K. Proof-of-Concept of IMU-Based Detection of ICU-Relevant Agitation Motion Patterns in Healthy Volunteers. Bioengineering. 2026; 13(2):164. https://doi.org/10.3390/bioengineering13020164
Chicago/Turabian StyleYokoyama, Ryuto, Tatsuya Hayasaka, Tomochika Harada, Si’ao Huang, Kenya Yarimizu, Michio Yokoyama, and Kaneyuki Kawamae. 2026. "Proof-of-Concept of IMU-Based Detection of ICU-Relevant Agitation Motion Patterns in Healthy Volunteers" Bioengineering 13, no. 2: 164. https://doi.org/10.3390/bioengineering13020164
APA StyleYokoyama, R., Hayasaka, T., Harada, T., Huang, S., Yarimizu, K., Yokoyama, M., & Kawamae, K. (2026). Proof-of-Concept of IMU-Based Detection of ICU-Relevant Agitation Motion Patterns in Healthy Volunteers. Bioengineering, 13(2), 164. https://doi.org/10.3390/bioengineering13020164







