Adipose Tissue Derivatives in Peripheral Nerve Regeneration after Transection: A Systematic Review
Abstract
1. Introduction
2. Materials and Methods
2.1. General Information
2.2. Data Selection and Extraction
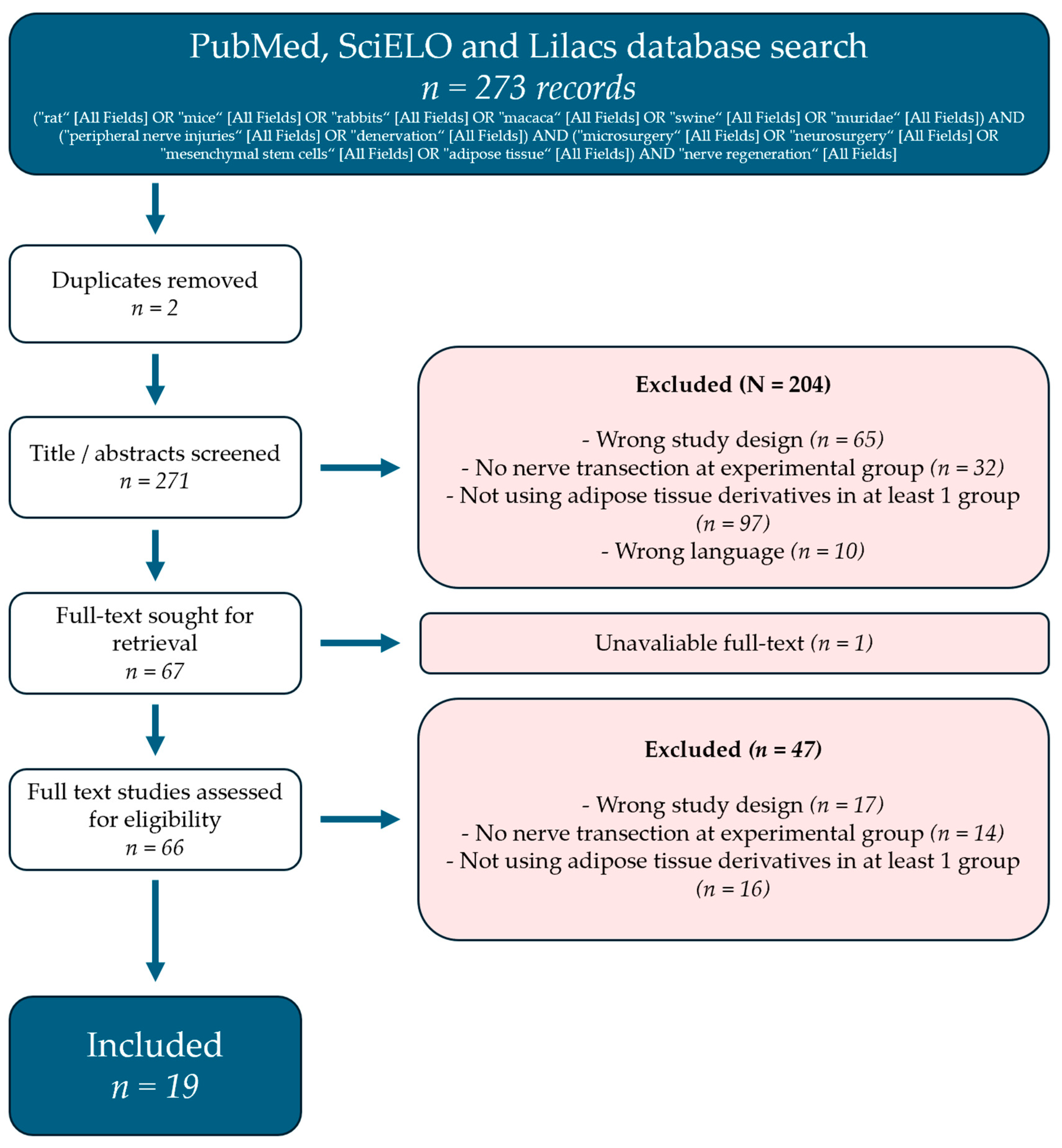
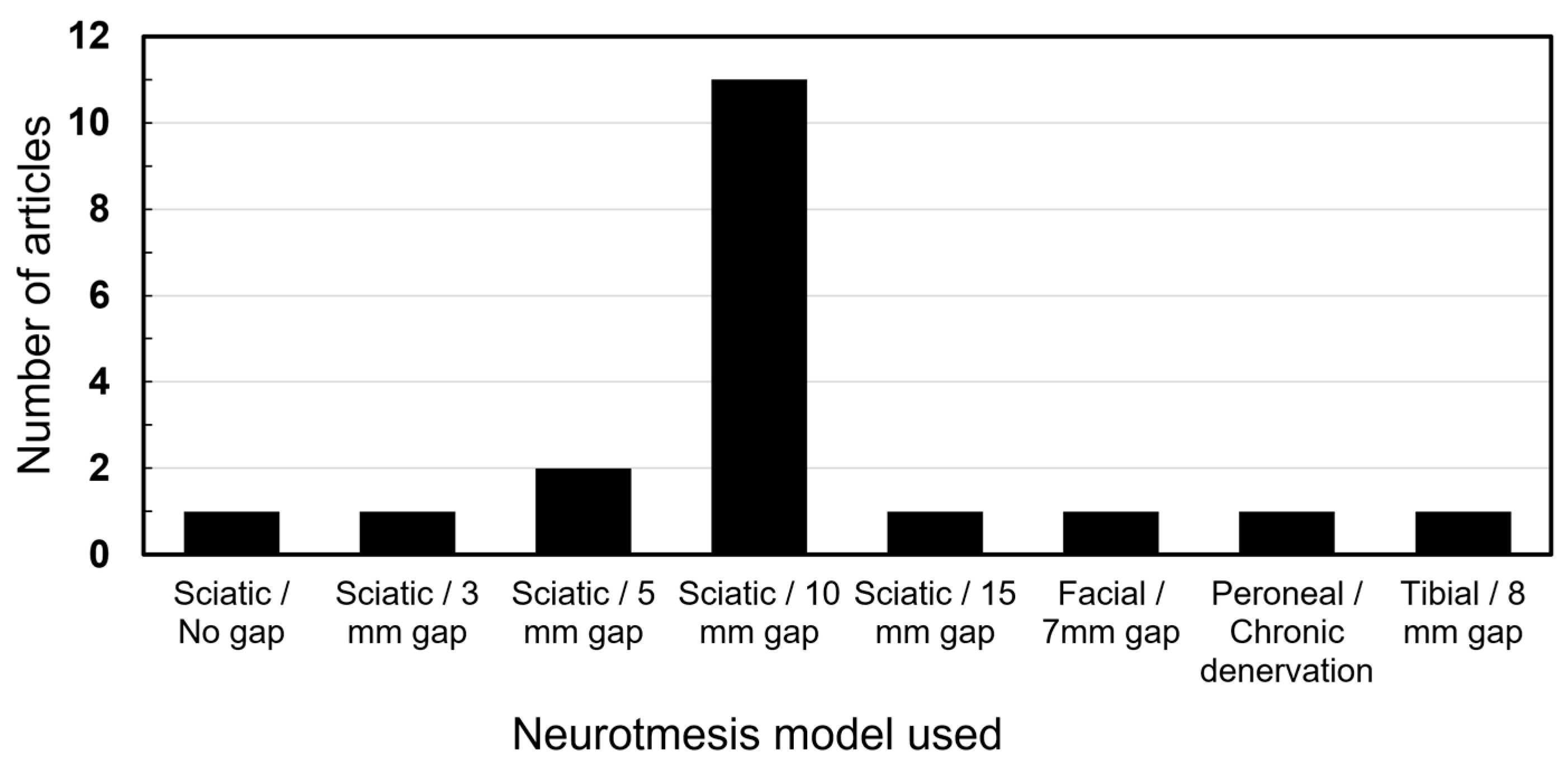
3. Results
4. Discussion
4.1. General Aspects
4.2. Adipose Tissue Derivatives
4.3. Trauma Mechanism
4.4. Functional Analysis
4.5. Histological Analysis
4.6. Other Analysis
4.7. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- England, J.D.; Asbury, A.K. Peripheral neuropathy. Lancet 2004, 363, 2151–2161. [Google Scholar] [CrossRef] [PubMed]
- Martyn, C.N.; Hughes, R.A. Epidemiology of peripheral neuropathy. J. Neurol. Neurosurg. Psychiatry 1997, 62, 310–318. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1074084/pdf/jnnpsyc00004-0006.pdf (accessed on 25 April 2024). [CrossRef] [PubMed]
- Robinson, L.R. Traumatic injury to peripheral nerves. Muscle Nerve 2022, 66, 661–670. [Google Scholar] [CrossRef] [PubMed]
- Scholz, T.D.; Krichevsky, A.; Sumarto, A.; Jaffurs, D.; Wirth, G.A.; Paydar, K.Z.; Evans, G.R.D. Peripheral Nerve Injuries: An International Survey of Current Treatments and Future Perspectives. J. Reconstr. Microsurg. 2009, 25, 339–344. [Google Scholar] [CrossRef] [PubMed]
- Neurapraxia; Axonotmesis; Neurotmesis. Nerve Injury: Classification, Clinical Assessment, Investigation, and Management. Semant. Sch. 2018. Available online: https://www.semanticscholar.org/paper/Nerve-injury%3A-Classification%2C-clinical-assessment%2C-Neurapraxia-Axonotmesis/fa2de78f0c685fa0d79b1f04632fc6f3524d3917 (accessed on 25 April 2024).
- Robinson, L.R. Electrodiagnosis and Rehabilitation of Peripheral Nerve Injuries. Jpn. J. Rehabil. Med. 2004, 41, S71. [Google Scholar] [CrossRef]
- Walsh, S.; Midha, R. Practical considerations concerning the use of stem cells for peripheral nerve repair. Neurosurg. Focus 2009, 26, E2. [Google Scholar] [CrossRef]
- Leberfinger, A.N.; Ravnic, D.J.; Payne, R.; Rizk, E.; Koduru, S.V.; Hazard, S.W. Adipose-Derived Stem Cells in Peripheral Nerve Regeneration. Curr. Surg. Rep. 2017, 5, 5. [Google Scholar] [CrossRef]
- Nichols, C.M.; Myckatyn, T.M.; Rickman, S.R.; Fox, I.K.; Hadlock, T.; Mackinnon, S.E. Choosing the correct functional assay: A comprehensive assessment of functional tests in the rat. Behav. Brain Res. 2005, 163, 143–158. [Google Scholar] [CrossRef]
- Erba, P.; Mantovani, C.; Kalbermatten, D.F.; Pierer, G.; Terenghi, G.; Kingham, P.J. Regeneration potential and survival of transplanted undifferentiated adipose tissue-derived stem cells in peripheral nerve conduits. J. Plast. Reconstr. Aesthetic Surg. 2010, 63, e811–e817. [Google Scholar] [CrossRef]
- Gentile, P.; Calabrese, C.; De Angelis, B.; Pizzicannella, J.; Kothari, A.; Garcovich, S. Impact of the Different Preparation Methods to Obtain Human Adipose-Derived Stromal Vascular Fraction Cells (AD-SVFs) and Human Adipose-Derived Mesenchymal Stem Cells (AD-MSCs): Enzymatic Digestion Versus Mechanical Centrifugation. Int. J. Mol. Sci. 2019, 20, 5471. [Google Scholar] [CrossRef] [PubMed]
- Verpaele, A.; Tonnard, P. Discussion: Nanofat Cell Aggregates: A Nearly Constitutive Stromal Cell Inoculum for Regenerative Site-Specific Therapies. Plast. Reconstr. Surg./PSEF CD J. 2019, 144, 1089–1090. [Google Scholar] [CrossRef] [PubMed]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; et al. A Declaração PRISMA 2020: Diretriz Atualizada para Relatar Revisões Sistemáticas. Rev. Panam. De Salud Pública 2022, 46, 1. Available online: https://iris.paho.org/bitstream/handle/10665.2/56882/v46e1122022.pdf?sequence=5 (accessed on 25 April 2024). [CrossRef] [PubMed]
- Reid, A.J.; Sun, M.; Wiberg, M.; Downes, S.; Terenghi, G.; Kingham, P.J. Nerve repair with adipose-derived stem cells protects dorsal root ganglia neurons from apoptosis. Neuroscience 2011, 199, 515–522. [Google Scholar] [CrossRef] [PubMed]
- Summa, P.G.; Kalbermatten, D.F.; Pralong, E.; Raffoul, W.; Kingham, P.J.; Terenghi, G. Long-term in vivo regeneration of peripheral nerves through bioengineered nerve grafts. Neuroscience 2011, 181, 278–291. [Google Scholar] [CrossRef] [PubMed]
- Liu, G.; Cheng, Y.; Guo, S.; Feng, Y.; Li, Q.; Jia, H.; Wang, Y.; Tong, L.; Tong, X. Transplantation of adipose-derived stem cells for peripheral nerve repair. Int. J. Mol. Med. 2011, 28, 565–572. [Google Scholar]
- Tomita, K.; Madura, T.; Mantovani, C.; Terenghi, G. Differentiated adipose-derived stem cells promote myelination and enhance functional recovery in a rat model of chronic denervation. J. Neurosci. Res. 2012, 90, 1392–1402. [Google Scholar] [CrossRef] [PubMed]
- Hea Gu, J.; Hwa Ji, Y.; Dhong, E.S.; Hwee Kim, D.; Yoon, E.S. Transplantation of Adipose Derived Stem Cells for Peripheral Nerve Regeneration in Sciatic Nerve Defects of the Rat. Curr. Stem Cell Res. Ther. 2012, 7, 347–355. [Google Scholar] [CrossRef]
- Dai, L.G.; Huang, G.S.; Hsu, S.H. Sciatic Nerve Regeneration by Cocultured Schwann Cells and Stem Cells on Microporous Nerve Conduits. Cell Transplant. 2013, 22, 2029–2039. [Google Scholar] [CrossRef]
- Raisi, A.; Azizi, S.; Delirezh, N.; Heshmatian, B.; Farshid, A.A.; Amini, K. The mesenchymal stem cell–derived microvesicles enhance sciatic nerve regeneration in rat. J. Trauma Acute Care Surg. 2014, 76, 991–997. [Google Scholar] [CrossRef]
- Kappos, E.A.; Engels, P.E.; Tremp, M.; Meyer zu Schwabedissen, M.; di Summa, P.; Fischmann, A.; von Felten, S.; Scherberich, A.; Schaefer, D.J.; Kalbermatten, D.F. Peripheral Nerve Repair: Multimodal Comparison of the Long-Term Regenerative Potential of Adipose Tissue-Derived Cells in a Biodegradable Conduit. Stem Cells Dev. 2015, 24, 2127–2141. Available online: https://pubmed.ncbi.nlm.nih.gov/26134465/ (accessed on 22 April 2024). [CrossRef] [PubMed]
- Mohammadi, R.; Mehrtash, M.; Mehrtash, M.; Sajjadi, S.S. Nonexpanded Adipose Stromal Vascular Fraction Local Therapy on Peripheral Nerve Regeneration Using Allografts. J. Investig. Surg. 2015, 29, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Reichenberger, M.A.; Mueller, W.; Hartmann, J.; Diehm, Y.; Lass, U.; Koellensperger, E.; Leimer, U.; Germann, G.; Fischer, S. ADSCs in a fibrin matrix enhance nerve regeneration after epineural suturing in a rat model. Microsurgery 2015, 36, 491–500. [Google Scholar] [CrossRef]
- Tremp, M.; Meyer Zu Schwabedissen, M.; Kappos, E.A.; Engels, P.E.; Fischmann, A.; Scherberich, A.; Schaefer, D.J.; Kalbermatten, D.F. The Regeneration Potential after Human and Autologous Stem Cell Transplantation in a Rat Sciatic Nerve Injury Model Can Be Monitored by MRI. Cell Transplant. 2015, 24, 203–211. Available online: https://pubmed.ncbi.nlm.nih.gov/24380629/ (accessed on 22 April 2024). [CrossRef]
- He, X.; Ao, Q.; Wei, Y.; Song, J. Transplantation of miRNA-34a Overexpressing Adipose-Derived Stem Cell Enhances Rat Nerve Regeneration. Wound Repair Regen. Off. Publ. Wound Heal. Soc. Eur. Tissue Repair Soc. 2016, 24, 542–550. Available online: https://pubmed.ncbi.nlm.nih.gov/26899299/ (accessed on 22 April 2024). [CrossRef]
- Sowa, Y.; Kishida, T.; Imura, T.; Numajiri, T.; Nishino, K.; Tabata, Y.; Mazda, O.M. Adipose-Derived Stem Cells Promote Peripheral Nerve Regeneration In Vivo without Differentiation into Schwann-like Lineage. Plast. Reconstr. Surg. 2016, 137, 318e–330e. Available online: https://pubmed.ncbi.nlm.nih.gov/26818322/ (accessed on 22 April 2024). [CrossRef] [PubMed]
- Özkan, H.S.; Silistreli, Ö.K.; Ergür, B.; İrkören, S. Repairing peripheral nerve defects by vein grafts filled with adipose tissue derived stromal vascular fraction: An experimental study in rats. Turk. J. Trauma Emerg. Surg. 2016, 22, 7–11. [Google Scholar]
- Shimizu, M.; Matsumine, H.; Osaki, H.; Ueta, Y.; Tsunoda, S.; Kamei, W.; Hashimoto, K.; Niimi, Y.; Watanabe, Y.; Miyata, M.; et al. Adipose-derived stem cells and the stromal vascular fraction in polyglycolic acid-collagen nerve conduits promote rat facial nerve regeneration. Wound Repair Regen. 2018, 26, 446–455. [Google Scholar] [CrossRef]
- Chen, J.; Ren, S.; Duscher, D.; Kang, Y.; Liu, Y.; Wang, C.; Yuan, M.; Guo, G.; Xiong, H.; Zhan, P.; et al. Exosomes from human adipose-derived stem cells promote sciatic nerve regeneration via optimizing Schwann cell function. J. Cell. Physiol. 2019, 234, 23097–23110. [Google Scholar] [CrossRef]
- Durço, D.F.P.A.; Pestana, F.M.; Oliveira, J.T.; Ramalho, B.d.S.; Souza, L.M.; Cardoso, F.S.; da Silva, I.C.; Marques, S.A.; Domingues, R.C.; Pereira, C.C.; et al. Grafts of human adipose-derived stem cells into a biodegradable poly (acid lactic) conduit enhances sciatic nerve regeneration. Brain Res. 2020, 1747, 147026. [Google Scholar] [CrossRef]
- Schilling, B.K.; Baker, J.S.; Komatsu, C.; Turer, D.M.; Bengur, F.B.; Nerone, W.V.; Qin, F.; Cottrill, A.R.; Kokai, L.E.; Rubin, J.P.; et al. Intramuscular Nanofat Injection Promotes Inflammation-Induced Gastrocnemius Regeneration in a Syngeneic Rat Sciatic Nerve Injury Model. Plast. Reconstr. Surg. 2023, 151, 947e–958e. Available online: https://pubmed.ncbi.nlm.nih.gov/36728782/ (accessed on 22 April 2024). [CrossRef]
- Kastamoni, M.; Yavaş, S.E.; Ozgenel, G.Y.; Ersoy, S. The effects of fat graft and platelet-rich fibrin combination after epineurectomy in rats. Rev. Da Assoc. Médica Bras. 2023, 69, 272–278. Available online: https://www.scielo.br/j/ramb/a/qJvqDHfjC6vzNg3xKZryQNS/?lang=en# (accessed on 16 April 2024). [CrossRef] [PubMed]
- Woolston, C. What China’s Leading Position in Natural Sciences Means for Global Research. Nature 2023, 620, S2–S5. Available online: https://www.nature.com/articles/d41586-023-02159-7#:~:text=China%20is%20already%20one%20of (accessed on 13 September 2023). [CrossRef] [PubMed]
- Zuk, P.A.; Zhu, M.; Ashjian, P.; De Ugarte, D.A.; Huang, J.I.; Mizuno, H.; Alfonso, Z.C.; Fraser, J.K.; Benhaim, P.; Hedrick, M.H. Human Adipose Tissue Is a Source of Multipotent Stem Cells. Mol. Biol. Cell 2002, 13, 4279–4295. [Google Scholar] [CrossRef] [PubMed]
- Si, Z.; Wang, X.; Sun, C.; Kang, Y.; Xu, J.; Wang, X.; Hui, Y. Adipose-derived stem cells: Sources, potency, and implications for regenerative therapies. Biomed. Pharmacother. 2019, 114, 108765. [Google Scholar] [CrossRef] [PubMed]
- Bacakova, L.; Zarubova, J.; Travnickova, M.; Musilkova, J.; Pajorova, J.; Slepicka, P.; Kasalkova, N.S.; Svorcik, V.; Kolska, Z.; Motarjem, H.I.; et al. Stem cells: Their source, potency and use in regenerative therapies with focus on adipose-derived stem cells—A review. Biotechnol. Adv. 2018, 36, 1111–1126. [Google Scholar] [CrossRef]
- Kokai, L.E.; Rubin, J.P.; Marra, K.G. The Potential of Adipose-Derived Adult Stem Cells as a Source of Neuronal Progenitor Cells. Plast. Reconstr. Surg. 2005, 116, 1453–1460. [Google Scholar] [CrossRef]
- Li, X.; Zhao, S.; Wang, L. Therapeutic effect of adipose-derived stem cell transplantation on optic nerve injury in rats. Mol. Med. Rep. 2018, 17, 2529–2534. [Google Scholar] [CrossRef]
- Gokce, A.; Peak, T.C.; Abdel-Mageed, A.B.; Hellstrom, W.J. Adipose Tissue-Derived Stem Cells for the Treatment of Erectile Dysfunction. Curr. Urol. Rep. 2016, 17, 14. [Google Scholar] [CrossRef]
- Kim, Y.J.; Jeong, J.H. Clinical Application of Adipose Stem Cells in Plastic Surgery. J. Korean Med. Sci. 2014, 29, 462. [Google Scholar] [CrossRef]
- Wang, B.B.; Guo, C.; Sun, S.Q.; Zhang, X.N.; Li, Z.; Li, W.J.; Li, Z.D.; Schumacher, M.; Liu, S. Comparison of the Nerve Regeneration Capacity and Characteristics between Sciatic Nerve Crush and Transection Injury Models in Rats. Biomed. Environ. Sci. 2023, 36, 160–173. [Google Scholar] [PubMed]
- Martins, R.S.; Siqueira, M.G.; da Silva, C.F.; Plese, J.P.P. Correlation between parameters of electrophysiological, histomorphometric and sciatic functional index evaluations after rat sciatic nerve repair. Arq. De Neuro-Psiquiatr. 2006, 64, 750–756. [Google Scholar] [CrossRef] [PubMed]
- de Medinaceli, L.; Freed, W.J.; Wyatt, R.J. An index of the functional condition of rat sciatic nerve based on measurements made from walking tracks. Exp. Neurol. 1982, 77, 634–643. [Google Scholar] [CrossRef] [PubMed]
- Orbay, H.; Uysal, A.C.; Hyakusoku, H.; Mizuno, H. Differentiated and Undifferentiated Adipose-Derived Stem Cells Improve Function in Rats with Peripheral Nerve Gaps. J. Plast. Reconstr. Aesthetic Surg. 2012, 65, 657–664. Available online: https://www.jprasurg.com/article/S1748-6815(11)00652-8/fulltext (accessed on 23 August 2022). [CrossRef]
- Shen, N.; Zhu, J. Application of sciatic functional index in nerve functional assessment. Microsurgery 1995, 16, 552–555. [Google Scholar] [CrossRef]
- Shenaq, J.M.; Shenaq, S.M.; Spira, M. Reliability of sciatic function index in assessing nerve regeneration across a 1 cm gap. Microsurgery 1989, 10, 214–219. [Google Scholar] [CrossRef]
- Moattari, M.; Kouchesfehani, H.M.; Kaka, G.; Sadraie, S.H.; Naghdi, M.; Mansouri, K. Chitosan-film associated with mesenchymal stem cells enhanced regeneration of peripheral nerves: A rat sciatic nerve model. J. Chem. Neuroanat. 2018, 88, 46–54. [Google Scholar] [CrossRef]
- Guo, Q.; Liu, C.; Hai, B.; Ma, T.; Zhang, W.; Tan, J.; Fu, X.; Wang, H.; Xu, Y.; Song, C. Chitosan conduits filled with simvastatin/Pluronic F-127 hydrogel promote peripheral nerve regeneration in rats. J. Biomed. Mater. Res. Part B Appl. Biomater. 2017, 106, 787–799. [Google Scholar] [CrossRef]
- Basso, D.M.; Beattie, M.S.; Bresnahan, J.C. A Sensitive and Reliable Locomotor Rating Scale for Open Field Testing in Rats. J. Neurotrauma 1995, 12, 1–21. Available online: https://pubmed.ncbi.nlm.nih.gov/7783230/ (accessed on 25 April 2024). [CrossRef]
- Bervar, M. An Alternative Video Footprint Analysis to Assess Functional Loss Following Injury to the Rat Sciatic Nerve. Acta Chir. Plast. 2002, 44, 86–89. Available online: https://pubmed.ncbi.nlm.nih.gov/12514995/ (accessed on 22 April 2024). [CrossRef]
- Bain, J.R.; Mackinnon, S.E.; Hunter, D.A. Functional Evaluation of Complete Sciatic, Peroneal, and Posterior Tibial Nerve Lesions in the Rat. Plast. Reconstr. Surg. 1989, 83, 129–136. [Google Scholar] [CrossRef] [PubMed]
- Pollari, E.; Prior, R.; Robberecht, W.; Van Damme, P.; Van Den Bosch, L. In Vivo Electrophysiological Measurement of Compound Muscle Action Potential from the Forelimbs in Mouse Models of Motor Neuron Degeneration. J. Vis. Exp. 2018, 136, e57741. [Google Scholar]
- Wang, Y.; Wang, H.; Mi, D.; Gu, X.; Hu, W. Periodical assessment of electrophysiological recovery following sciatic nerve crush via surface stimulation in rats. Neurological Sciences 2015, 36, 449–456. [Google Scholar] [CrossRef] [PubMed]
- Ao, Q.; Fung, C.-K.; Tsui, A.Y.-P.; Cai, S.; Zuo, H.-C.; Chan, Y.-S.; Shum, D.K.-Y. The regeneration of transected sciatic nerves of adult rats using chitosan nerve conduits seeded with bone marrow stromal cell-derived Schwann cells. Biomaterials 2011, 32, 787–796. [Google Scholar] [CrossRef] [PubMed]
- Matsumoto, K.; Ohnishi, K.; Kiyotani, T.; Sekine, T.; Ueda, H.; Nakamura, T.; Endo, K.; Shimizu, Y. Peripheral nerve regeneration across an 80-mm gap bridged by a polyglycolic acid (PGA)–collagen tube filled with laminin-coated collagen fibers: A histological and electrophysiological evaluation of regenerated nerves. Brain Res. 2000, 868, 315–328. [Google Scholar] [CrossRef] [PubMed]
- Wang, G.; Lu, G.; Ao, Q.; Gong, Y.; Zhang, X. Preparation of Cross-Linked Carboxymethyl Chitosan for Repairing Sciatic Nerve Injury in Rats. Biotechnol. Lett. 2010, 32, 59–66. Available online: https://pubmed.ncbi.nlm.nih.gov/19760120/ (accessed on 22 April 2024). [CrossRef] [PubMed]
- Ghnenis, A.B.; Czaikowski, R.E.; Zhang, Z.J.; Bushman, J.S. Toluidine Blue Staining of Resin-Embedded Sections for Evaluation of Peripheral Nerve Morphology. J. Vis. Exp. 2018, 137, e58031. [Google Scholar]
- Sridharan, G.; Shankar, A. Toluidine Blue: A Review of Its Chemistry and Clinical Utility. J. Oral Maxillofac. Pathol. 2012, 16, 251. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3424943/ (accessed on 25 April 2024). [CrossRef] [PubMed]
- Scipio, F.D.; Raimondo, S.; Tos, P.; Geuna, S. A simple protocol for paraffin-embedded myelin sheath staining with osmium tetroxide for light microscope observation. Microsc. Res. Tech. 2008, 71, 497–502. [Google Scholar] [CrossRef]
- Jessen, K.R.; Mirsky, R. The Origin and Development of Glial Cells in Peripheral Nerves. Nat. Rev. Neurosci. 2005, 6, 671–682. Available online: https://www.nature.com/articles/nrn1746 (accessed on 25 April 2024). [CrossRef]
- Jessen, K.R.; Mirsky, R. The Success and Failure of the Schwann Cell Response to Nerve Injury. Front. Cell. Neurosci. 2019, 13, 33. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6378273/ (accessed on 26 September 2019). [CrossRef]
- Harboe, M.; Torvund-Jensen, J.; Kjaer-Sorensen, K.; Laursen, L.S. Ephrin-A1-EphA4 signaling negatively regulates myelination in the central nervous system. Glia 2018, 66, 934–950. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Zheng, Z.; Hu, D. Inhibition of EphA4 expression promotes Schwann cell migration and peripheral nerve regeneration. Neurosci. Lett. 2013, 548, 201–205. [Google Scholar] [CrossRef] [PubMed]
- Chen, R.; Yang, X.; Zhang, B.; Wang, S.; Bao, S.; Gu, Y.; Li, S. EphA4 Negatively Regulates Myelination by Inhibiting Schwann Cell Differentiation in the Peripheral Nervous System. Front. Neurosci. 2019, 13, 1191. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Sun, B.; Shibata, B.; Guo, F. Transmission electron microscopic analysis of myelination in the murine central nervous system. STAR Protoc. 2022, 3, 101304. [Google Scholar] [CrossRef] [PubMed]
- Nam, Y.H.; Park, S.; Yum, Y.; Jeong, S.; Park, H.E.; Kim, H.J.; Lim, J.; Choi, B.-O.; Jung, S.-C. Preclinical Efficacy of Peripheral Nerve Regeneration by Schwann Cell-like Cells Differentiated from Human Tonsil-Derived Mesenchymal Stem Cells in C22 Mice. Biomedicines 2023, 11, 3334. [Google Scholar] [CrossRef] [PubMed]
- Rui, B.; Guo, S.; Zeng, B.; Wang, J.; Chen, X. An implantable electrical stimulator used for peripheral nerve rehabilitation in rats. Exp. Ther. Med. 2013, 6, 22–28. [Google Scholar] [CrossRef] [PubMed]
- Ge, J.; Zhu, S.; Yang, Y.; Liu, Z.; Hu, X.; Huang, L.; Quan, X.; Wang, M.; Huang, J.; Li, Y.; et al. Experimental Immunological Demyelination Enhances Regeneration in Autograft-Repaired Long Peripheral Nerve Gaps. Sci. Rep. 2016, 6, 39828. Available online: https://www.nature.com/articles/srep39828 (accessed on 22 April 2024). [CrossRef] [PubMed]
- Sulong, A.; Hassan, N.; Hwei, N.; Lokanathan, Y.; Naicker, A.; Abdullah, S.; Yusof, M.; Htwe, O.; Idrus, R.; Haflah, N. Collagen-coated Polylactic-Glycolic Acid (PLGA) Seeded with Neural-Differentiated Human Mesenchymal Stem Cells as a Potential Nerve Conduit. Adv. Clin. Exp. Med. Off. Organ Wroc. Med. Univ. 2014, 23, 353–362. Available online: https://pubmed.ncbi.nlm.nih.gov/24979505/ (accessed on 22 April 2024). [CrossRef]
- Nadeau, S.; Filali, M.; Zhang, J.; Kerr, B.J.; Rivest, S.; Soulet, D.; Iwakura, Y.; Vaccari, J.P.d.R.; Keane, R.W.; Lacroix, S. Functional recovery after peripheral nerve injury is dependent on the pro-inflammatory cytokines IL-1β and TNF: Implications for neuropathic pain. J. Neurosci. Off. J. Soc. Neurosci. 2011, 31, 12533–12542. Available online: https://www.ncbi.nlm.nih.gov/pubmed/21880915 (accessed on 15 June 2020). [CrossRef]
- McKinnon, K.M. Flow Cytometry: An Overview. Curr. Protoc. Immunol. 2018, 120, 5.1.1–5.1.11. [Google Scholar] [CrossRef] [PubMed]
- Hayashi, A.; Moradzadeh, A.; Hunter, D.A.; Kawamura, D.H.; Puppala, V.K.; Tung, T.H.H.; Mackinnon, S.E.; Myckatyn, T.M. Retrograde Labeling in Peripheral Nerve Research: It Is Not All Black and White. J. Reconstr. Microsurg. 2007, 23, 381–389. [Google Scholar] [CrossRef]
- Catapano, J.; Willand, M.P.; Zhang, J.J.; Scholl, D.; Gordon, T.; Borschel, G.H. Retrograde labeling of regenerating motor and sensory neurons using silicone caps. J. Neurosci. Methods 2016, 259, 122–128. [Google Scholar] [CrossRef]
- Chen, L.; Leng, C.; Ru, Q.; Xiong, Q.; Zhou, M.; Wu, Y. Retrograde Labeling of Different Distribution Features of DRG P2X2 and P2X3 Receptors in a Neuropathic Pain Rat Model. BioMed Res. Int. 2020, 2020, 9861459. Available online: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7396081/ (accessed on 25 April 2024). [CrossRef] [PubMed]
- Pettersson, J.; Kalbermatten, D.F.; McGrath, A.; Novikova, L.N. Biodegradable fibrin conduit promotes long-term regeneration after peripheral nerve injury in adult rats. J. Plast. Reconstr. Aesthetic Surg. 2010, 63, 1893–1899. [Google Scholar] [CrossRef] [PubMed]
- Rodrίguez, F.J.; Verdú, E.; Ceballos, D.; Navarro, X. Nerve Guides Seeded with Autologous Schwann Cells Improve Nerve Regeneration. Exp. Neurol. 2000, 161, 571–584. [Google Scholar] [CrossRef]
- Vleggeert-Lankamp, C.L.A.M. The role of evaluation methods in the assessment of peripheral nerve regeneration through synthetic conduits: A systematic review. J. Neurosurg. 2007, 107, 1168–1189. [Google Scholar] [CrossRef]

| Author and Year | Sample | Study Groups | Functional Analysis | Histological Analysis | Other Analyses |
|---|---|---|---|---|---|
| Reid et al. (2011) [14] | 12 | Artificial CD; CD + ASCs; CD + SCs | - | LM; IAS; and Immunofluorescence | PCR; Western Blot; and ELISA |
| di Summa et al. (2011) [15] | 25 | Fibrin CD; Fibrin CD + ASCs; Fibrin CD + SC; Fibrin CD + BMSC; Autograft | CMAP | LM; IAS; and Immunofluorescence | RNL |
| Liu et al. (2011) [16] | 30 | Acellular nerve graft + DMEM; Acellular nerve graft + ASCs; Autograft | SFI and NCV | LM; IAS; TEM; and Immunofluorescence | PCR |
| Tomita et al. (2012) [17] | 18 | Vehicle; ASCs; SCs | PFI; CMAP; and MWR | LM; IAS; and Immunofluorescence | - |
| Gu et al. (2012) [18] | 30 | Silicone CD + fibrin glue; CD + Undifferentiated ASCs; CD + neurally differentiated ASCs | CMAP | LM; IAS; TEM; and Immunofluorescence | Western Blot |
| Dai et al. (2013) [19] | 30 | CD; CD + ASCs; CD + SCs; CD + DPSC; CD + ASCs + SCs; CD + DPSC + SCs | SFI; NCV; and MWR | LM and IAS | PCR |
| Raisi et al. (2014) [20] | 90 | CD; ASCs undifferentiated; ASCs microvesicles; ASCs Microvesicles + Pro-inflammatory; ASCs Microvesicles + anti-inflammatory | SFI and NCV | LM; IAS; and TEM | - |
| Kappos et al. (2015) [21] | 49 | CD + ASCs undifferentiated; CD + SCs; CD + autograft; CD + Human SVF; CD + Differentiated ASCs; CD + Human superficial ASCs; CD + Human Deep ASCs | SFI and MWR | LM and IAS | MRI scanning |
| Mohammadi et al. (2015) [22] | 30 | Sham; autograft; Allograft + SVF | BBB; SFI; SSI and MWR | LM; IAS; TBS; and Immunofluorescence | Biomechanical Stretch Testing |
| Reichenberger et al. (2015) [23] | 50 | Fibrin glue; Fibrin glue + ASCs | MWR | LM; IAS; TBS; and Immunofluorescence | - |
| Tremp et al. (2015) [24] | 49 | CD + DMEM; CD + ASCs; differentiated ASCs (SC-like); Human superficial ASCs; Human Deep ASCs; Human SVF; SCs | - | LM; IAS; and Immunofluorescence | MRI scanning |
| He et al. (2016) [25] | 16 | ASCs; ASCs with transduced vector control | SFI; CNAP; NCV; and MWR | LM; IAS; TBS; TEM; and Immunofluorescence | PCR |
| Sowa et al. (2016) [26] | 20 | CD; ASCs; SCs; Sham | SFI and MWR | LM; IAS; and Immunofluorescence | - |
| Özkan et al. (2016) [27] | 30 | Vein graft; Vein graft + SVF; Autograft | - | LM; IAS; and TBS | - |
| Shimizu et al. (2018) [28] | 24 | CD; CD + ASCs; CD + SVF | CMAP | LM; IAS; and TEM | RNL |
| Chen et al. (2019) [29] | 28 | Vehicle; ASCs | MWR | LM; TEM; IAS; TBS and Immunofluorescence | FC; PCR and Western Blot |
| Durço et al. (2020) [30] | 30 | CD + DMEM; CD + ASCs | CMAP | LM; TEM and IAS | Pinprick Test and RNL |
| Schilling et al. (2023) [31] | Unknown * | Control; Nanofat | SFI; MWR and TCF | LM and IAS | PCR; Cytokine Quantification |
| Kastamoni et al. (2023) [32] | 24 | Control: neurotomy of the left sciatic nerve; Intervention: fat graft at right nerve | - | LM; IAS; and Immunofluorescence | - |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Araújo, R.S.d.; Mussalem, M.G.V.B.; Carrijo, G.S.; Bani, J.V.d.F.; Ferreira, L.M. Adipose Tissue Derivatives in Peripheral Nerve Regeneration after Transection: A Systematic Review. Bioengineering 2024, 11, 697. https://doi.org/10.3390/bioengineering11070697
Araújo RSd, Mussalem MGVB, Carrijo GS, Bani JVdF, Ferreira LM. Adipose Tissue Derivatives in Peripheral Nerve Regeneration after Transection: A Systematic Review. Bioengineering. 2024; 11(7):697. https://doi.org/10.3390/bioengineering11070697
Chicago/Turabian StyleAraújo, Rafael Silva de, Matheus Galvão Valadares Bertolini Mussalem, Gabriel Sant’Ana Carrijo, João Victor de Figueiredo Bani, and Lydia Masako Ferreira. 2024. "Adipose Tissue Derivatives in Peripheral Nerve Regeneration after Transection: A Systematic Review" Bioengineering 11, no. 7: 697. https://doi.org/10.3390/bioengineering11070697
APA StyleAraújo, R. S. d., Mussalem, M. G. V. B., Carrijo, G. S., Bani, J. V. d. F., & Ferreira, L. M. (2024). Adipose Tissue Derivatives in Peripheral Nerve Regeneration after Transection: A Systematic Review. Bioengineering, 11(7), 697. https://doi.org/10.3390/bioengineering11070697






