Why We Need Minimum Basic Requirements in Science for Acupuncture Education
Abstract
:1. Introduction
2. Overview
2.1. Is There a Better Way?
2.2. Proposed Curricular Content
2.3. Encouraging Better-Designed Acupuncture Research
3. Conclusions
Conflicts of Interest
References
- Kalauokalani, D.; Cherkin, D.C.; Sherman, K.J. A comparison of physician and nonphysician acupuncture treatment for chronic low back pain. Clin. J. Pain. 2005, 21, 406–411. [Google Scholar] [CrossRef] [PubMed]
- American Board of Medical Acupuncture. ABMA Approved Training Programs. Available online: http://dabma.org/programs (accessed on 6 September 2016).
- Acupuncture Today. Acupuncture Schools. Available online: http://www.acupuncturetoday.com/schools/ (accessed on 6 September 2016).
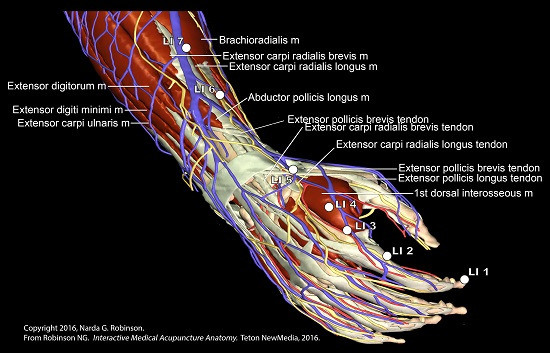
- Robinson, N.G. Interactive Medical Acupuncture Anatomy; Teton NewMedia: Jackson, WY, USA, 2016. [Google Scholar]
- Cheng, K.J. Neuroanatomical characteristics of acupuncture points: Relationship between their anatomical locations and traditional clinical indications. Acupunct. Med. 2011, 29, 289–294. [Google Scholar] [CrossRef] [PubMed]
- American Board of Medical Acupuncture Website. Recommended Readings for the ABMA Board Certification Examination. Available online: http://dabma.org/documents/EXAM_RECOMMENDED.pdf (accessed on 25 July 2016).
- Council of Colleges of Acupuncture and Oriental Medicine. Know Your Acupuncturist. Available online: http://www.ccaom.org/downloads/CCAOM_KnowYourAcu.pdf (accessed on 25 July 2016).
- NCCAOM® Study Guide for Diplomate in Acupuncture Certification, 2016. Available online: http://www.nccaom.org/forms-and-applications/ (accessed on 25 July 2016).
- O’Brien, K.A.; Abbas, E.; Zhang, J.; Guo, Z.-X.; Luo, R.; Bensoussan, A.; Komesaroff, P.A. Understanding the reliability of diagnostic variables in a Chinese Medicine examination. J. Altern. Complement. Med. 2009, 15, 727–734. [Google Scholar]
- Zhang, G.G.; Lee, W.L.; Lao, L.; Lee, W.L.; Handwerger, B.; Berman, B. The variability of TCM pattern diagnosis and herbal prescription on rheumatoid arthritis patients. Altern. Ther. Health Med. 2004, 10, 58–63. [Google Scholar] [PubMed]
- Gerwin, R.D. Diagnosis of myofascial pain syndrome. Phys. Med. Rehabil. Clin. N. Am. 2014, 25, 341–355. [Google Scholar] [CrossRef] [PubMed]
- Freeman, B.D. Is it time to rethink postgraduate training requirements for licensure? Acad. Med. 2016, 91, 20–22. [Google Scholar] [CrossRef] [PubMed]
- He, W.; Want, X.; Shi, H.; Shang, H.; Li, L.; Jing, X.; Zhu, B. Auricular acupuncture and vagal regulation. Evid.-Based Complement. Altern. Med. 2012. [Google Scholar] [CrossRef] [PubMed]
- Robinson, N.G. Personal communication with medical acupuncturists at the 2016 American Academy of Medical Acupuncture Annual Symposium during Dr. Robinson’s afternoon neuroanatomic acupuncture workshop presentation. Unpublished work. 2016. [Google Scholar]
- Litscher, G.; Rong, P.J. Auricular acupuncture. Evid.-Based Complement. Altern. Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Rong, P.J.; Zhao, J.J.; Wang, L.; Zhou, L.Q. Analysis of advantages and disadvantages of the location methods of international auricular acupuncture points. Evid.-Based Complement. Altern. Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Liu, Z.; Guan, L.; Wang, Y.; Xie, C.L.; Lin, X.M.; Zheng, G.Q. History and mechanism for treatment of intracerebral hemorrhage with scalp acupuncture. Evid.-Based Complement. Altern. Med. 2012. [Google Scholar] [CrossRef] [PubMed]
- Rezvani, M.; Yaraghi, A.; Mohseni, M.; Fathimoghadam, F. Efficacy of Yamamoto New Scalp Acupuncture versus Traditional Chinese acupuncture for migraine treatment. J. Altern. Complement. Med. 2014, 20, 371–374. [Google Scholar] [CrossRef] [PubMed]
- Zheng, G.Q.; Zhao, Z.M.; Wang, Y.; Gu, Y.; Li, Y.; Chen, X.M.; Fu, S.P.; Shen, J. Meta-analysis of scalp acupuncture for acute hypertensive intracerebral hemorrhage. J. Altern. Complement. Med. 2011, 17, 293–299. [Google Scholar] [CrossRef] [PubMed] [Green Version]
- Ochi, J.W. Korean hand therapy for tonsillectomy pain in children. Int. J. Pediatr. Otorhinolaryngol. 2015, 79, 1263–1267. [Google Scholar] [CrossRef] [PubMed]
- Tsai, S.L.; Fox, L.M.; Murakami, M.; Tsung, J.W. Auricular acupuncture in emergency department treatment of acute pain. Ann. Emerg. Med. 2016. [Google Scholar] [CrossRef] [PubMed]
- Ushinohama, A.; Cunha, B.P.; Costa, L.O.; Barela, A.M.; Freitas, P.B. Effect of a single session of ear acupuncture on pain intensity and postural control in individuals with chronic low back pain: A randomized controlled trial. Braz. J. Phys. Therapy 2016. [Google Scholar] [CrossRef] [PubMed]
- Wu, S.L.Y.; Leung, A.W.N.; Yew, D.T.W. Acupuncture for detoxification in treatment of opioid addiction. East Asian Arch. Psychiatry 2016, 26, 70–76. [Google Scholar] [PubMed]
- Ning, Z.; Lao, L. Acupuncture for pain management in evidence-based medicine. J. Acupunct. Meridian Stud. 2015, 8, 270–273. [Google Scholar] [CrossRef] [PubMed]
- Jiang, J.; Peng, W.; Gu, T.; King, C.; Yin, J.K. Critical review of data evaluation in teaching clinics of Traditional Chinese Medicine outside China: Implications for education. Explore 2016, 12, 188–195. [Google Scholar] [CrossRef] [PubMed]
- White, A.; Editorial board of acupuncture in medicine. Western medical acupuncture: A definition. Acupunct. Med. 2009, 27, 33–35. [Google Scholar] [PubMed]
- Hua, B.; Abbas, E.; Hayes, A.; Ryan, P.; Nelson, L.; O’Brien, K. Reliability of Chinese medicine diagnostic variables in the examination of patients with osteoarthritis of the knee. J. Altern. Complement. Med. 2012, 18, 1028–1037. [Google Scholar] [CrossRef] [PubMed]
- Da Silva, M.A.; Dorsher, P.T. Neuroanatomic and clinical correspondences: acupuncture and vagus nerve stimulation. J. Altern. Complement. Med. 2014, 20, 233–240. [Google Scholar] [CrossRef] [PubMed]
- Takahashi, T. Mechanism of acupuncture on neuromodulation in the gut—A review. Neuromodulation 2011, 14, 8–12. [Google Scholar] [CrossRef] [PubMed]
- Langevin, H.M.; Churchill, D.L.; Cipolla, M.J. Mechanical signaling through connective tissue: A mechanism for the therapeutic effect of acupuncture. FASEB J. 2001, 15, 2275–2282. [Google Scholar] [CrossRef] [PubMed]
- Zhang, F.; Kong, L.L.; Zhang, Y.Y.; Li, S.C. Evaluation of impact on health-related quality of life and cost effectiveness of Traditional Chinese Medicine: A systematic review of randomized clinical trials. J. Altern. Complement. Med. 2012, 18, 1108–1120. [Google Scholar] [CrossRef] [PubMed]
- STRICTA. Standards for Reporting Interventions in Controlled Trials of Acupuncture. Available online: http://www.stricta.info/ (accessed on 25 July 2016).
- DC’s Improbable Science Blog. Acupuncture Is a Theatrical Placebo: The End of a Myth. 30 May 2013. Available online: http://www.dcscience.net/2013/05/30/acupuncture-is-a-theatrical-placebo-the-end-of-a-myth/ (accessed on 17 June 2016).
- Want, S.M.; Harris, R.E.; Lin, Y.C.; Gan, T.J. Acupuncture in 21st century anesthesia: Is there a needle in the haystack? Anesth. Analg. 2013, 116, 1356–1359. [Google Scholar]
- Deng, S.; Zhao, X.; Du, R.; He, S.; Wen, Y.; Huang, L.; Tian, G.; Zhang, C.; Meng, Z.; Shi, X. Is acupuncture no more than a placebo? Extensive discussion required about possible bias. Exp. Ther. Med. 2015, 10, 1247–1252. [Google Scholar] [CrossRef] [PubMed]
- Lundeberg, T.; Lund, I.; Naslund, J.; Thomas, M. The Emperor’s sham—Wrong assumption that sham needling is sham. Acupunct. Med. 2008, 26, 239–242. [Google Scholar] [CrossRef] [PubMed]
© 2016 by the author; licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC-BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Robinson, N.G. Why We Need Minimum Basic Requirements in Science for Acupuncture Education. Medicines 2016, 3, 21. https://doi.org/10.3390/medicines3030021
Robinson NG. Why We Need Minimum Basic Requirements in Science for Acupuncture Education. Medicines. 2016; 3(3):21. https://doi.org/10.3390/medicines3030021
Chicago/Turabian StyleRobinson, Narda G. 2016. "Why We Need Minimum Basic Requirements in Science for Acupuncture Education" Medicines 3, no. 3: 21. https://doi.org/10.3390/medicines3030021
APA StyleRobinson, N. G. (2016). Why We Need Minimum Basic Requirements in Science for Acupuncture Education. Medicines, 3(3), 21. https://doi.org/10.3390/medicines3030021