Impact of a Large Fire and Subsequent Pollution Control Failure at a Coke Works on Acute Asthma Exacerbations in Nearby Adult Residents
Abstract
1. Introduction
2. Literature Review
3. Materials and Methods
3.1. Acute Asthma Exacerbations
3.2. Other Data
3.3. Data Analysis
4. Results
4.1. Demographics
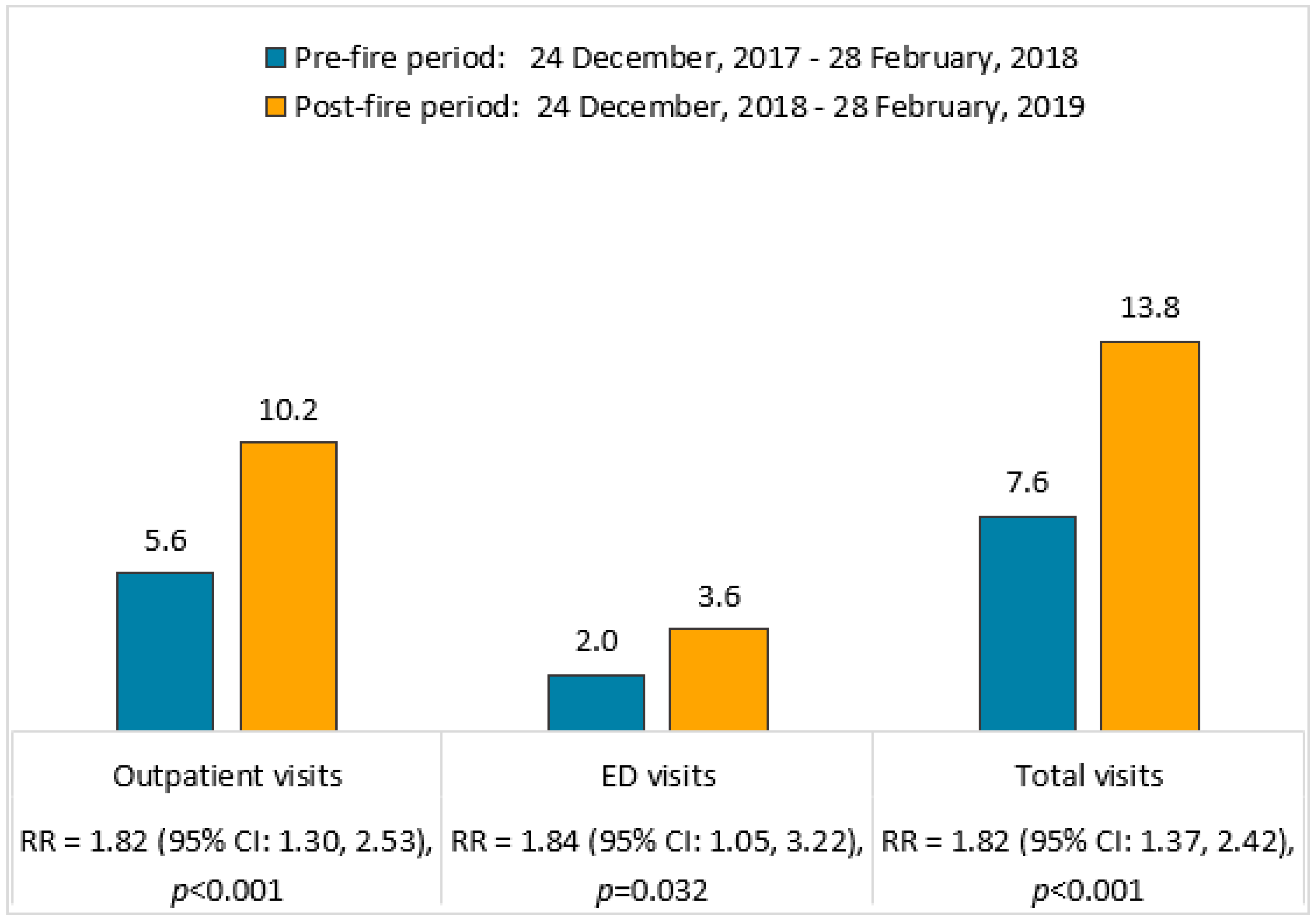
4.2. Visits for Acute Asthma
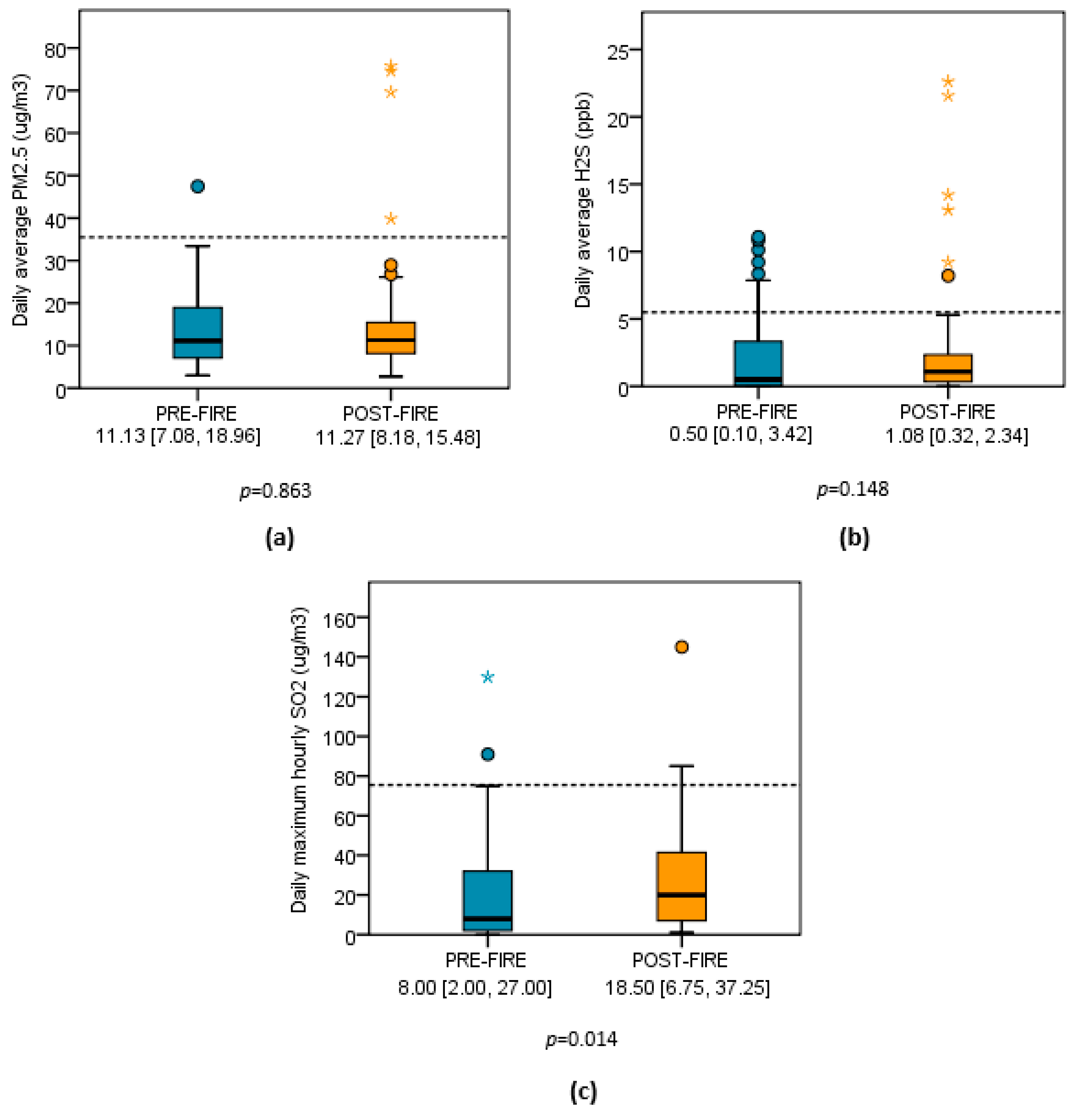
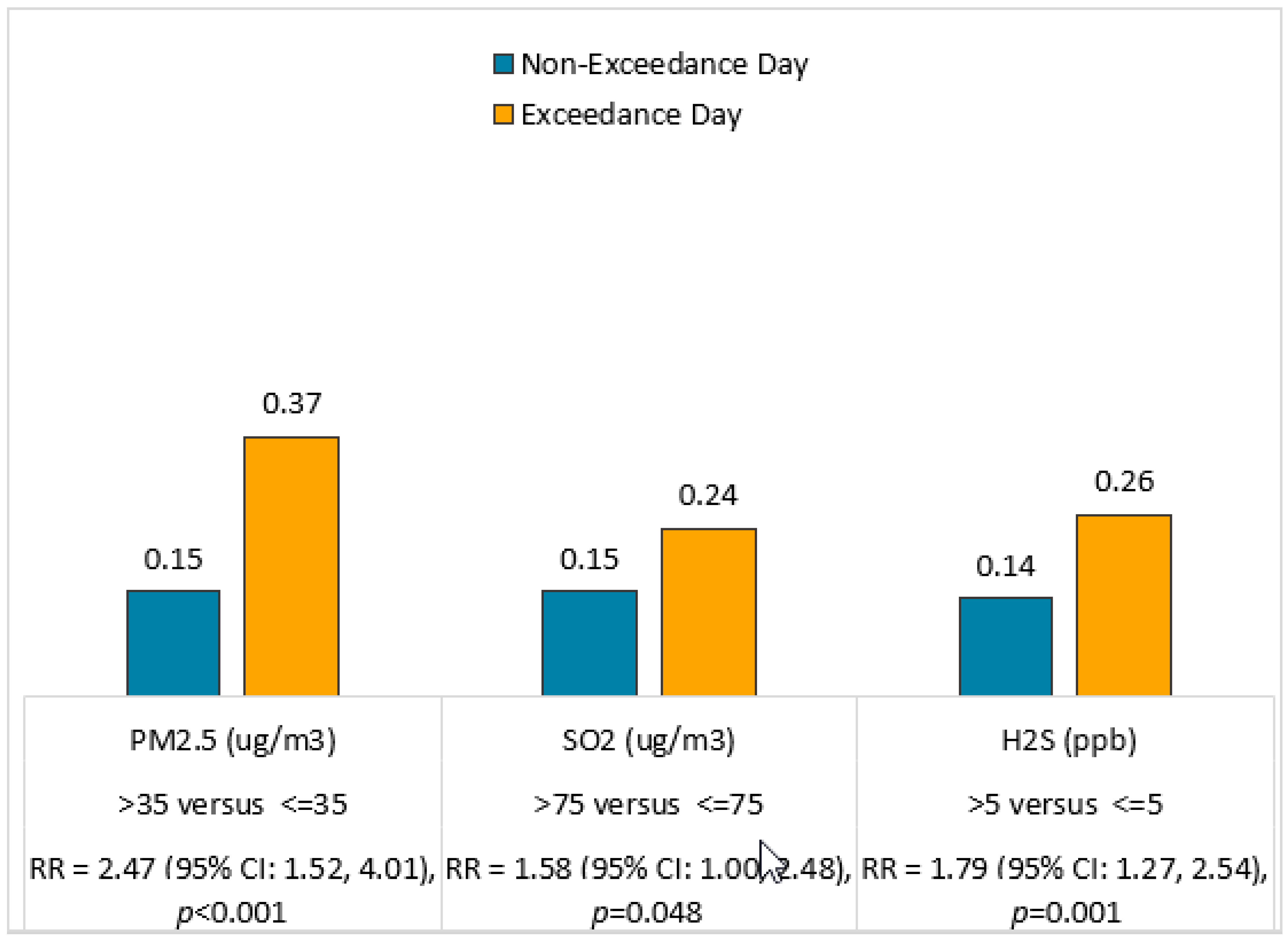
4.3. Outdoor Air Pollution
4.4. Weather Data
4.5. Influenza Rates
5. Discussion
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Allegheny County Health Department Air Quality Program 2019, 190202, 1–19. Enforcement-Order-190202-USS-Mon-Valley-Works.pdf. Available online: Pacokeovens.org (accessed on 14 March 2021).
- US Environmental Protection Agency. 2017 National Emissions Inventory (NEI) Data. Available online: https://www.epa.gov/air-emissions-inventories/2017-national-emissions-inventory-nei-data (accessed on 14 April 2021).
- US Environmental Protection Agency. Environmental Justice Screening Map and Tool. 2020 Version. Available online: https://ejscreen.epa.gov/mapper/ (accessed on 14 March 2021).
- Allegheny County Health Department. Mon Valley Air Quality. Available online: https://alleghenycounty.us.health/Health-Department/Programs/Air-Quality/Mon-Valley-Air-Quality.aspx (accessed on 5 June 2021).
- Allergy and Asthma Foundation of America. Asthma Facts. Available online: https://www.aafa.org/asthma-facts/ (accessed on 5 June 2021).
- Bywra-Hill, B.; Presto, A.; Wenzel, S.E.; Fabisiak, J. Acute impact of a pollution control breach at a coke works on asthma control in nearby vulnerable adults. J. Allergy Clin. Immunol. 2021. [Google Scholar] [CrossRef]
- Linn, W.S. Respiratory effects of sulfur dioxide in heavily exercising asthmatics: A dose-response study. Am. Rev. Respir. Dis. 1983, 127, 278–283. [Google Scholar] [CrossRef]
- Balmes, J.R.; Fine, J.M.; Sheppard, D. Symptomatic Bronchoconstriction after Short-Term Inhalation of Sulfur Dioxide. Am. Rev. Respir. Dis. 1987, 136, 1117–1121. [Google Scholar] [CrossRef]
- Burra, T.A. Social disadvantage, air pollution, and asthma physician visits in Toronto, Canada. Environ. Res. 2009, 109, 567–574. [Google Scholar] [CrossRef]
- Alhanti, B.A.; Chang, H.H.; Winquist, A.; Mulholland, J.A.; Darrow, L.A.; Sarnat, S.E. Ambient air pollution and emergency department visits for asthma: A multi-city assessment of effect modification by age. J. Expo. Sci. Environ. Epidemiol. 2015, 26, 180–188. [Google Scholar] [CrossRef]
- Samoli, E. Acute effects of air pollution on pediatric asthma exacerbation: Evidence of association and effect modification. Environ. Res. 2011, 111, 418–424. [Google Scholar] [CrossRef]
- Malig, B.J.; Green, S.; Basu, R.; Broadwin, R. Coarse particles and respiratory emergency department visits in California. Am. J. Epidemiol. 2013, 178, 58–69. [Google Scholar] [CrossRef]
- Ostro, B. Associations of source-specific fine particulate matter with emergency department visits in California. Am. J. Epidemiol. 2016, 184, 450–459. [Google Scholar] [CrossRef] [PubMed]
- Krall, J.R. Associations between source-specific fine particulate matter and emergency department visits for respiratory disease in four US cities. Environ. Health Perspect. 2016, 1, 97–103. [Google Scholar] [CrossRef]
- Guo, Y.; Gao, C.X.; Dennekamp, M.; Dimitriadis, C.; Straney, L.; Ikin, J.; Abramson, M.J. The association of coal mine fire smoke with hospital emergency presentations and admissions: Time series analysis of Hazelwood Health Study. Chemosphere 2020, 253, 126667. [Google Scholar] [CrossRef] [PubMed]
- Johnson, A.L.; Dipnall, J.F.; Dennekamp, M.; Williamson, G.; Gao, C.X.; Carroll, M.T.; Dimitriadis, C.; Ikin, J.F.; Johnston, F.H.; McFarlane, A.C.; et al. Fine particulate matter exposure and medication dispensing during and after a coal mine fire: A time series analysis from the Hazelwood Health Study. Environ. Pollut. 2019, 246, 1027–1035. [Google Scholar] [CrossRef] [PubMed]
- Johnson, A.L.; Gao, C.X.; Dennekamp, M.; Williamson, G.J.; Brown, D.; Carroll, M.T.C.; Ikin, J.F.; Del Monaco, A.; Abramson, M.J.; Guo, Y. Associations between Respiratory Health Outcomes and Coal Mine Fire PM2.5 Smoke Exposure: A Cross-Sectional Study. Int. J. Environ. Res. Public Health 2019, 16, 4262. [Google Scholar] [CrossRef] [PubMed]
- Han, H.A.; Han, I.; McCurdy, S.; Whitworth, K.; Delclos, G.; Rammah, A.; Symanski, E. The Intercontinental Terminals Chemical Fire Study: A Rapid Response to an Industrial Disaster to Address Resident Concerns in Deer Park, Texas. Int. J. Environ. Res. Public Health 2020, 17, 986. [Google Scholar] [CrossRef]
- Kim, H.; Baidwan, N.K.; Kriebel, D.; Cifuentes, M.; Baron, S. Asthma among World Trade Center first responders: A qualitative synthesis and bias assessment. Int. J. Environ. Res. Public Health 2018, 15, 1053. [Google Scholar] [CrossRef]
- Borchers-Arriagada, N.; Palmer, A.J.; Bowman, D.M.J.S.; Williamson, G.J.; Johnston, F.H. Health impacts of ambient biomss smoke in Tasmania, Australia. Int. J. Environ. Res. Public Health 2020, 17, 3264. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.C.; Pereira, G.; Uhl, S.A.; Bravo, M.A.; Bell, M.L. A systemic review of the physical health impacts from non-occupational exposure to wildfire smoke. Environ. Res. 2015, 136, 120–132. [Google Scholar] [CrossRef]
- Huang, R.; Hu, Y.; Russell, A.G.; Mulholland, J.A.; Odman, M.T. The impacts of prescribed fire on PM2.5 air quality and human health: Applicaitgon to asthma-rleated emergency room visits in Georgia, USA. Int. J. Environ. Res. Public Health 2019, 16, 2312. [Google Scholar] [CrossRef]
- Shih, D.-H.; Wu, T.-W.; Liu, W.-X.; Shih, P.-Y. An azure ACES early warning system for air quality index deteriorating. Int. J. Environ. Res. Public Health 2019, 16, 4679. [Google Scholar] [CrossRef]
- Masselot, P.; Cheban, F.; Lavigne, E.; Campagna, C.; Gosselin, P.; Ouarda, T.B.M.J. Toward an improved air pollution warning system in Quebec. Int. J. Environ. Res. Public Health 2019, 16, 2095. [Google Scholar] [CrossRef]
- McClean, K.E.; Yao, J.; Henderson, S.B. An evaluation of the British Columbia ashtma monitoring system (BCAMS) and PM2.5 exposure metrics during the 2014 forest fire season. Int. J. Environ. Res. Public Health 2015, 12, 6710–6724. [Google Scholar] [CrossRef]
- Mirabelli, M.C.; Boehmer, T.K.; Damon, S.A.; Sircar, K.D.; Wall, H.K.; Yip, F.Y.; Zahran, H.S.; Garbe, P.L. Air Quality Awareness Among U.S. Adults With Respiratory and Heart Disease. Am. J. Prev. Med. 2018, 54, 679–687. [Google Scholar] [CrossRef] [PubMed]
- Mirabelli, M.C.; Ebelt, L.S.; Damon, S.A. Air quality index and air quality awareness amonng adults in the United States. Environ. Res. 2020, 183, 109185. [Google Scholar] [CrossRef] [PubMed]
- Lynch, K.M.; Mirabelli, M.C. Outdoor Air Quality Awareness, Perceptions, and Behaviors Among U.S. Children Aged 12–17 Years, 2015–2018. J. Adolesc. Heal. 2021, 68, 882–887. [Google Scholar] [CrossRef]
- D’Antoni, D.; Auyeung, V.; Walton, H.; Fuller, G.W.; Grieve, A.; Weinman, J. The effect of evidence and theory-based health advise accompanying smartphone air quality alerts on adherence to preventative recommenations during poor air quality days: A randomized controlled trial. Environ. Int. 2019, 124, 216–235. [Google Scholar] [CrossRef] [PubMed]
- Palmer, S.; Coleman, G. Building national public capacity for managing chemikcal events: A case study of the development of health protection services in the United Kingdom. J. Public Health Policy 2013, 34, 213–225. [Google Scholar] [CrossRef][Green Version]
- Chan, E.Y.Y.; Wang, Z.; Mark, C.K.M.; Liu, S.D. Industrial accidents in China: Risk reduction and response. Lancet 2015, 386, 1421–1422. [Google Scholar] [CrossRef]
- LaTourrette, T.; Davis, L.E.; Howell, D.R.; Sama, P.R.; Dausey, D.J. Public Health Preparedness and Response to Chemical and Radiological Incidents: Functions, Practices, and Areas for Future Work; RAND Corporation: Santa Monica, CA, USA, 2009. [Google Scholar]
- Centers for Disease Control and Prevention. Public Health Emergency Response Guide for State, Local and Tribal Public Health Directors; Version 2.0; US Department of Health and Human Services: Washington, DC, USA, 2011. Available online: https://emergency.cdc.gov/planning/responseguide.asp (accessed on 14 March 2021).
- US Census Bureau (2019). American Community Survey 5-Year Estimates. Retrieved from Census Reporter Profile Page for 15025. Available online: http://censusreporter.org/profiles/86000US15025-15025 (accessed on 14 March 2021).
- Allegheny County Health Department. Allegheny County Air Quality. Monitor Locations. Available online: https://www.alleghenycounty.us/Health-Department/Programs/Air-Quality/Air-Quality.aspx (accessed on 14 March 2021).
- US Environmental Protection Agency. NAAQS Table, Criteria Air Pollutants. Available online: https://www.epa.gov/criteria-air-pollutants/naaqs-table (accessed on 14 March 2021).
- Commonwealth of Pennsylvania (2021). 25 Pennsylvania Code Chapter 131. Ambient Air Quality Standards. Available online: https://www.pacodeandbulletin.gov (accessed on 14 March 2021).
- Sadar, A. Allegheny County Surface Temperature Inversion Analysis—2019. Allegheny County Health Department 2019. Available online: https://www.alleghenycounty.us/uploadedFiles/Allegheny_Home/Health_Department/Programs/Air_Quality/AnnualSfcTempInversionAnalysis-2019.pdf (accessed on 14 March 2021).
- Centers for Disease Control and Prevention. US Influenza Surveillance System: Purpose and Methods. Available online: Htpps://www.cdc.gov/flu/weeklyoverview.htm (accessed on 6 March 2021).
- Allegheny County Health Department. Final 2018–2019 Seasonal flu Data. 2019, 1–4. Available online: https://www.alleghenycounty.us/uploadedFiles/Allegheny_Home/Health_Department/Health_Services/Immunization_Clinic/092819-final-18-19-flu-season-chart.pdf (accessed on 14 March 2021).
- US Census Bureau (2019). American Community Survey 5-Year Estimates. Retrieved from Census Reporter Profile Page for Allegehny County, PA. Available online: https://censusreporter.org/profiles/05000US42003-allegheny-county-pa (accessed on 14 March 2021).
- Kianifard, F.; Gallo, P.P. Poisson regression analysis in clinical research. J. Biopharm. Stat. 1995, 5, 115–129. [Google Scholar] [CrossRef]
- Campagna, D.; Kathman, S.J.; Pierson, R.; Inserra, S.G.; Phifer, B.L.; Middleton, D.C.; Zarus, G.M.; White, M.C. Ambient hydrogen sulfide, total reduced sulfur, and hospital visits for respiratory diseases in northeast Nebraska, 1998–2000. J. Expo. Sci. Environ. Epidemiol. 2004, 14, 180–187. [Google Scholar] [CrossRef]
- Durand, M.; Wilson, J.G. Spatial analysis of respiratory disease on an urbanized geothermal field. Environ. Res. 2006, 101, 238–245. [Google Scholar] [CrossRef]
- Carlsen, H.K.; Zoega, H.; Valdimarsdottir, U.; Gislason, T.; Hrafnkelsson, B. Hydrogen sulfide and particle matter levels associated with increased dispensing of anti-asthma drugs in Iceland’s capital. Environ. Res. 2012, 113, 33–39. [Google Scholar] [CrossRef] [PubMed]
- Bates, M.N.; Garrett, N.; Crane, J.; Balmes, J. Association of ambient hydrogen sulfide exposure with self-reported asthma and asthma symptoms. Environ. Res. 2013, 122, 81–87. [Google Scholar] [CrossRef]
- Pope, C.A. Respiratory disease associated with community air pollution and a steel mill, Utah Valley. Am. J. Public Health 1989, 79, 623–628. [Google Scholar] [CrossRef]
- Gentile, D.A.; Morphew, T.; Elliott, J.; Presto, A.A.; Skoner, D.P. Asthma Prevalence and Control among Schoolchildren Residing near Outdoor Air Pollution Sites. J. Asthma 2020, 5, 1–18. [Google Scholar] [CrossRef]
- Gauderman, W.J. Association of improved air quality with lung development in children. N. Engl. J. Med. 2015, 372, 905–913. [Google Scholar] [CrossRef]
- Gehring, U. Exposure to air pollution and development of asthma and rhinoconjunctivitis throughout childhood and adolescence: A population-based birth cohort study. Lancet Respir. Med. 2015, 3, 933–942. [Google Scholar] [CrossRef]
- Tétreault, L.F. Childhood exposure to ambient air pollutants and the onset of asthma: An administrative cohort study in Québec. Environ. Health Perspect. 2016, 124, 1276–1282. [Google Scholar] [CrossRef]
- Baatjies, R.; Adams, S.; Cairncross, E.; Omar, F.; Jeebhay, M. Factors associated with persistent lower respiratory symptoms or asthma among residents exposed to a sulfur stockpile fire incident. Int. J. Environ. Res. Public Health 2019, 16, 438. [Google Scholar] [CrossRef]
- Hansell, A.; Horwell, C.J.; Oppenheimer, C. The health hazards of volcanoes and geothermal areas. Occup. Environ. Med. 2006, 63, 149–156. [Google Scholar] [CrossRef]
- Amaral, A.F.S.; Rodrigues, A.S. Chronic exposure to volcanic environments and chronic bronchitis incidence in the Azores, Portugal. Environ. Res. 2007, 103, 419–423. [Google Scholar] [CrossRef]
- Piirla, P.L.; Nordam, H.; Korhonen, O.S.; Winblad, I. A thirteen-year follow-up of respiratory effects of acute exposure to sulfur dioxide. Scand J. Work Environ. Health 1996, 22, 191–196. [Google Scholar] [CrossRef]
- Beard, J.D.; Beck, C.; Graham, R.; Packham, S.C.; Traphagan, M.; Giles, R.T.; Morgan, J.G. Winter Temperature Inversions and Emergency Department Visits for Asthma in Salt Lake County, Utah, 2003–2008. Environ. Health Perspect. 2012, 120, 1385–1390. [Google Scholar] [CrossRef]
- US Environmental Protection Agency. Integrated Science Assessment for Particulate Matter. Integrated Synthesis. 2019, Pages 1–59 to 1–62. Available online: https://cfpub.epa.gov/ncea/isa/recordisplay.cfm?deid=347534#tab-3 (accessed on 14 March 2021).
- US Environmental Protection Agency. Integrated Science Assessment for Sulfur Oxides—Health Criteria. December 2017. Available online: https://www.epa/gov/isa (accessed on 14 March 2021).
- PA Department of Environmental Protection. PA Environmental Justice Areas: Clairton, PA. Available online: https://padep1.maps.arcgis.com/apps/webappviewer/index.html?id=f31a188de122467691cae93c3339469c (accessed on 14 March 2021).
- Mikati, I.; Benson, A.; Luben, T.; Sacks, J.; Richmond-Bryant, J. Disparities in Distribution of Particulate Matter Emission Sources by Race and Poverty Status. Am. J. Public Health 2018, 108, 480–485. [Google Scholar] [CrossRef]
- Oyanna, T.J.; Podila, P.; Relyea, G.E. Effects of childhood exposure to PM2.5 in a Memphis pediatric chohort. Envrion. Monit. Assess 2019, 191, 330. [Google Scholar] [CrossRef]
- Tessum, C.W.; Apte, J.; Goodkind, A.L.; Muller, N.Z.; Mullins, K.A.; Paolella, D.A.; Polasky, S.; Springer, N.P.; Thakrar, S.K.; Marshall, J.D.; et al. Inequity in consumption of goods and services adds to racial–ethnic disparities in air pollution exposure. Proc. Natl. Acad. Sci. USA 2019, 116, 6001–6006. [Google Scholar] [CrossRef]
- Rodriguez-Villamizar, L.A.; Rosychuik, R.J.; Osornio-Vargas, A.; Villeneuve, P.J.; Rowe, B.H. Proximity to two main sources of industrial outdoor air pollution and emergency department visits for childhood asthma in Edmonton, Canada. Can. J. Public Health 2018, 108, e523–e529. [Google Scholar] [CrossRef]
- International Program on Chemical Safety and World Health Organization. Concise International Chemical Assessment Document 53—Hydrogen Sulfide: Human Health Aspects. 2003. Available online: https://www.who.int/ipcs/publications/cicad/en/cicad53.pdf (accessed on 14 March 2021).
- Nurmagambetov, T.; Kuwahara, R.; Garbe, P. The Economic Burden of Asthma in the United States, 2008–2013. Ann. Am. Thorac. Soc. 2017, 15, 348–356. Available online: https://www.atsjournals.org/doi/10.1513/AnnalsATS.201703-259OC (accessed on 14 March 2021). [CrossRef]
- Martenies, S.E.; Milando, C.W.; Williams, G.O.; Batterman, S.A. Disease and health inequalities attributable to air pollutant exposure in Detroit, Michigan. Int. J. Environ. Res. Public Health 2017, 14, 1243. [Google Scholar] [CrossRef]
- Rittner, R.; Flanagan, E.; Oudin, A.; Malmqvist, E. Health impacts from ambient particle exposure in Southern Sweden. Int. J. Environ. Res. Public Health 2020, 17, 5064. [Google Scholar] [CrossRef]
- Huang, Y.-T.; Chen, C.-C.; Ho, Y.-N.; Tsai, M.-T.; Tsai, C.-M.; Chuang, P.-C.; Cheng, F.-J. Short-Term Effects of Particulate Matter and Its Constituents on Emergency Room Visits for Chronic Obstructive Pulmonary Disease: A Time-Stratified Case-Crossover Study in an Urban Area. Int. J. Environ. Res. Public Health 2021, 18, 4400. [Google Scholar] [CrossRef]
- Shetty, B.S.P.; D’Souza, G.; Padukudru Anand, M. Effect of indoor air pollution on chronic obstructive pulmonary disease (COPD) deaths in Southern Asia—a systematic review and meta-analysis. Toxics 2021, 9, 85. [Google Scholar] [CrossRef]

| Demographic | Clairton, PA (Zip Code 15025) N = 16,298 | Allegheny County, PA N = 1,216,045 |
|---|---|---|
| Age, years: | ||
| <18 | 21% | 19% |
| 18–64 | 59% (N = 9616) | 62% (N = 753,948) |
| ≥65 | 20% | 19% |
| Gender: | ||
| Male | 48% | 48% |
| Female | 52% | 52% |
| Race: | ||
| African American | 16% | 13% |
| White | 80% | 78% |
| Other | 4% | 9% |
| Below federal poverty level | 11% | 11% |
| Median household income | USD 60,669 | USD 64,871 |
| Pollutant | Pre-Fire Daily Average Emissions | Post-Fire Daily Average Emissions |
|---|---|---|
| H2S (grains/100 dscf/day) | 10.91 | 262.25 |
| SO2 (lbs/day) | 2118.18 | 74,099.81 |
| Pollutant | Date | Monitor Location | Level |
|---|---|---|---|
| PM2.5 | 26 December 2018 | Liberty | 40 ug/m3 |
| 02 February 2019 | Liberty | 70 ug/m3 | |
| 03 February 2019 | Liberty | 76 ug/m3 | |
| 04 February 2019 | Liberty | 75 ug/m3 | |
| SO2 | 26 December 2018 | Liberty | 80 ppb |
| 28 December 2018 | Liberty | 145 ppb | |
| 02 January 2019 | Liberty | 81 ppb | |
| 03 January 2019 | Liberty | 85 ppb | |
| 07 January 2019 | North Braddock | 83 ppb | |
| 08 January 2019 | Liberty | 80 mppb | |
| 04 February 2019 | North Braddock | 82 ppb | |
| H2S | 26 December 2018 | Liberty | 14 ppb |
| 28 December 2018 | Liberty | 8 ppb | |
| 08 January 2019 | Liberty | 9 ppb | |
| 02 February 2019 | Liberty | 13 ppb | |
| 03 February 2019 | Liberty | 22 ppb | |
| 04 February 2019 | Liberty | 22 ppb |
| Parameter | Pre-Fire | Post-Fire | p-Value |
|---|---|---|---|
| N (% Days) | 24 days (35.8%) | 17 days (25.3%) | 0.317 |
| Strength (Daily AVG + STD) | 4.3 + 2.7 °C | 3.9 + 2.8 °C | 0.648 |
| Depth (Daily AVG + STD) | 339 + 272 m | 297 + 171 | 0.578 |
| Duration (Daily AVG + STD) | 5.3 + 2.7 h | 4.6 + 1.9 | 0.364 |
| Parameter | Pre-Fire | Post-Fire | Rate Ratio (95% CI) | p-Value |
|---|---|---|---|---|
| # Cases | 12,793 | 9856 | 1.30 (1.26, 1.33) | <0.001 |
| # Hospitalizations | 803 | 288 | 2.79 (2.44, 3.19) | <0.001 |
| # Deaths | 31 | 29 | 1.07 (0.64, 1.77) | 0.796 |
| Peak Week | 21–27 January 2018 | 17–23 January 2019 |
| Study Results |
|---|
|
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations. |
© 2021 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).
Share and Cite
Morphew, T.L.; Venkat, A.; Graham, J.; Mehalik, M.; Anderson, N.; Gentile, D. Impact of a Large Fire and Subsequent Pollution Control Failure at a Coke Works on Acute Asthma Exacerbations in Nearby Adult Residents. Toxics 2021, 9, 147. https://doi.org/10.3390/toxics9070147
Morphew TL, Venkat A, Graham J, Mehalik M, Anderson N, Gentile D. Impact of a Large Fire and Subsequent Pollution Control Failure at a Coke Works on Acute Asthma Exacerbations in Nearby Adult Residents. Toxics. 2021; 9(7):147. https://doi.org/10.3390/toxics9070147
Chicago/Turabian StyleMorphew, Tricia L., Arvind Venkat, John Graham, Matthew Mehalik, Norman Anderson, and Deborah Gentile. 2021. "Impact of a Large Fire and Subsequent Pollution Control Failure at a Coke Works on Acute Asthma Exacerbations in Nearby Adult Residents" Toxics 9, no. 7: 147. https://doi.org/10.3390/toxics9070147
APA StyleMorphew, T. L., Venkat, A., Graham, J., Mehalik, M., Anderson, N., & Gentile, D. (2021). Impact of a Large Fire and Subsequent Pollution Control Failure at a Coke Works on Acute Asthma Exacerbations in Nearby Adult Residents. Toxics, 9(7), 147. https://doi.org/10.3390/toxics9070147






