Human Papillomavirus (HPV) Vaccine Knowledge, Awareness and Acceptance among Dental Students and Post-Graduate Dental Residents
Abstract
1. Introduction
2. Methods
2.1. Study Approval
2.2. Questionnaire
- Vaccines are necessary to protect public health
- There are too many required vaccines
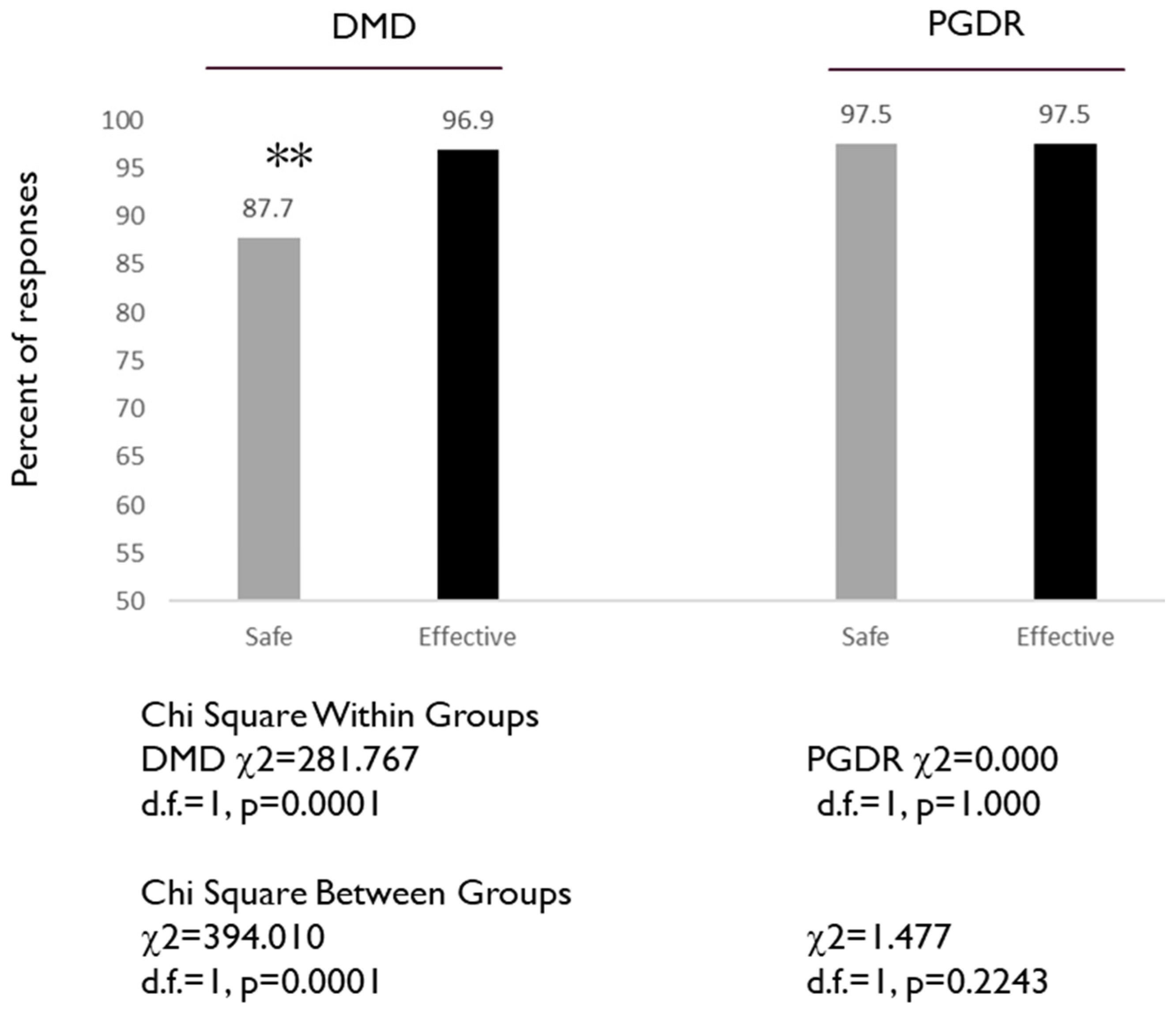
- Vaccines are generally safe
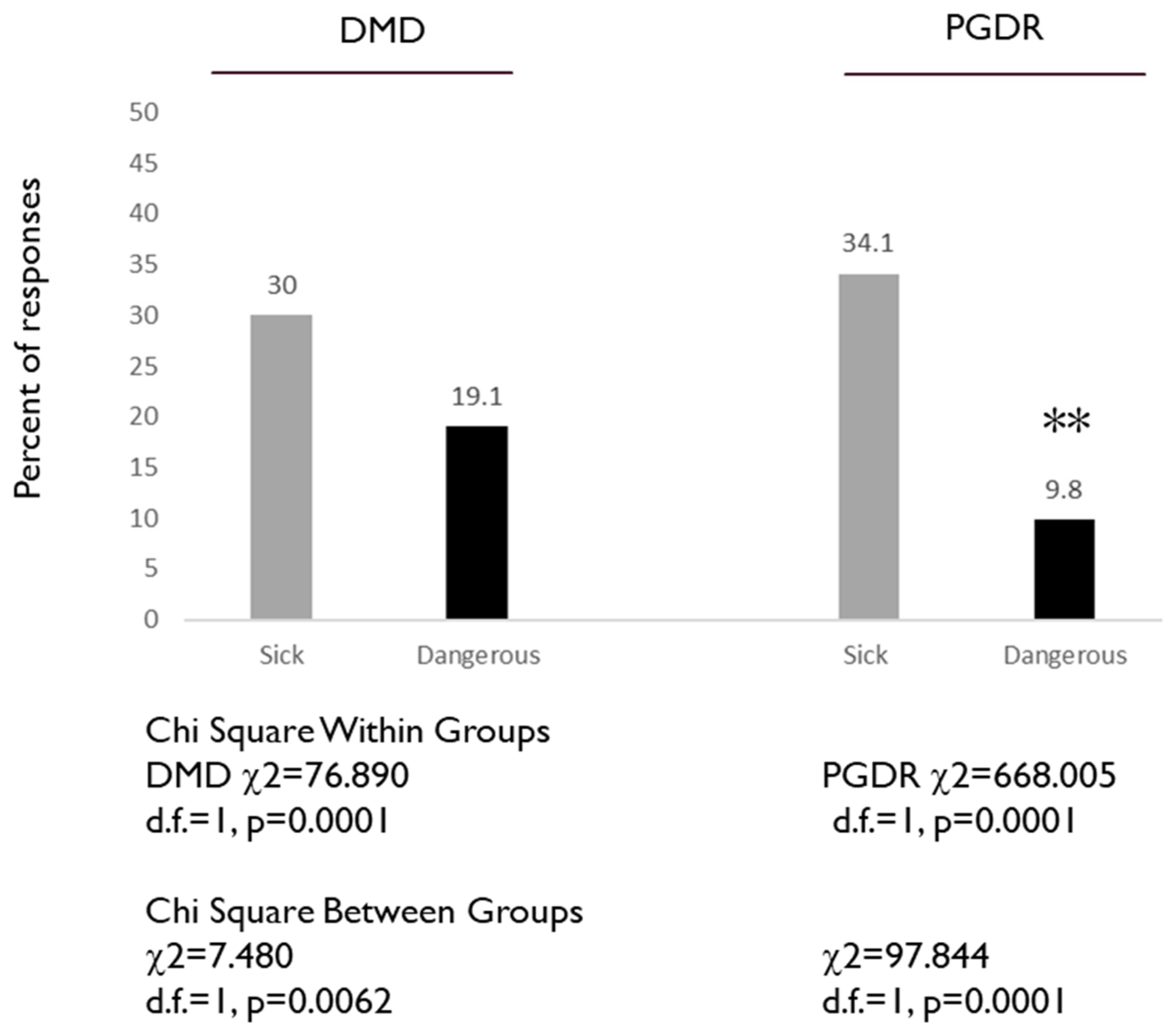
- Vaccination can make you sick
- Some vaccines are dangerous
- Vaccines are generally effective
- I follow the vaccine guidelines for myself
- I adhere to the vaccine guidelines for my family The second section was comprised of nine HPV-specific questions, which included:
- I am aware of a vaccine for human papillomavirus (HPV)
- HPV vaccination is important for me
- HPV vaccination is important for (my) spouse/partner
- HPV vaccination is important for (my) daughter(s)
- HPV vaccination is important for (my) son(s)
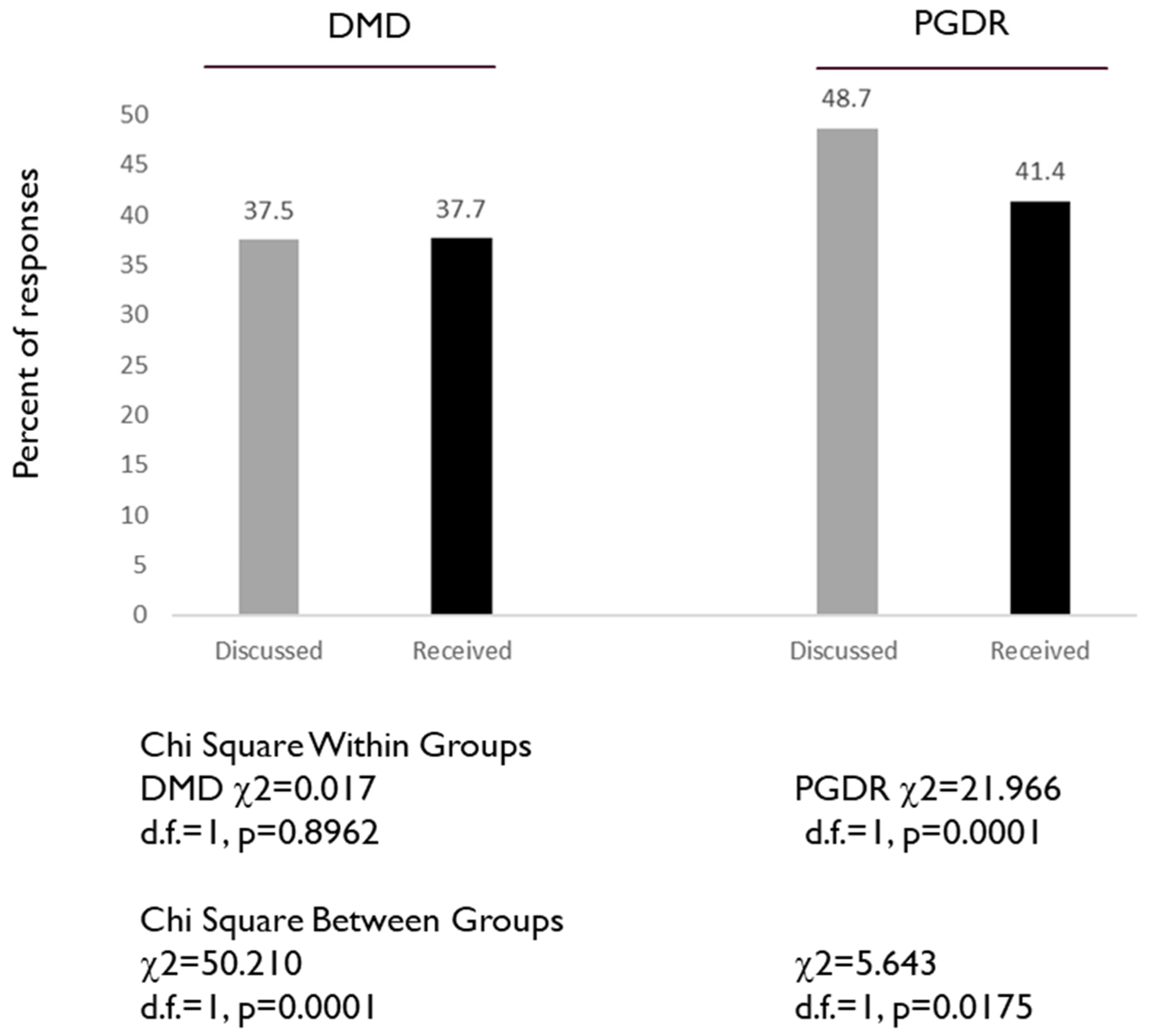
- I have discussed HPV vaccination with a doctor
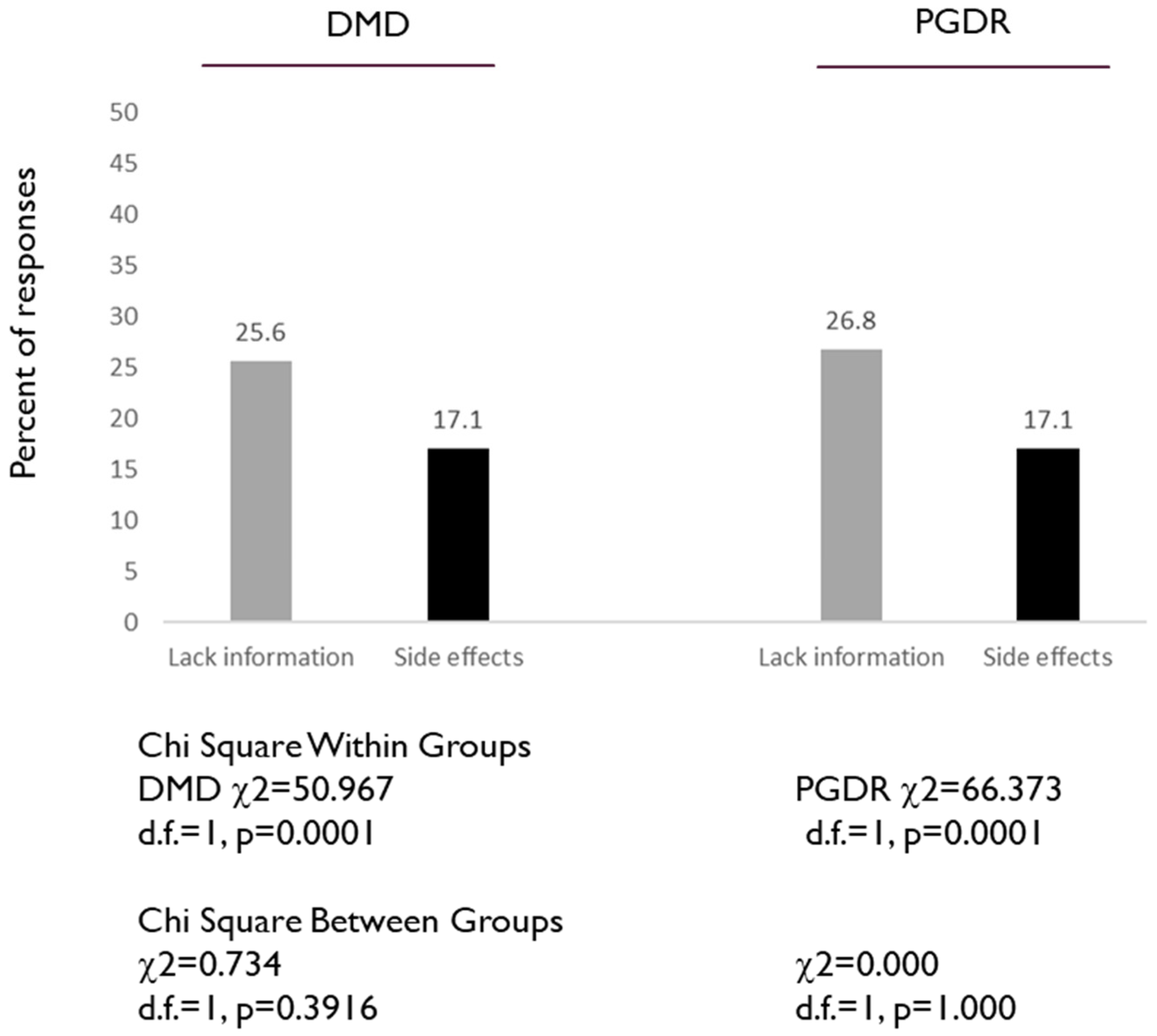
- I do not have enough information about the HPV vaccine
- I am concerned about possible HPV vaccine side effects
- I have already received the HPV vaccine
2.3. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Leidner, A.J.; Murthy, N.; Chesson, H.W.; Biggerstaff, M.; Stoecker, C.; Harris, A.M.; Acosta, A.; Dooling, K.; Bridges, C.B. Cost-effectiveness of adult vaccinations: A systematic review. Vaccine 2019, 37, 226–234. [Google Scholar] [CrossRef] [PubMed]
- Sheikh, S.; Biundo, E.; Courcier, S.; Damm, O.; Launay, O.; Maes, E.; Marcos, C.; Matthews, S.; Meijer, C.; Poscia, A.; et al. A report on the status of vaccination in Europe. Vaccine 2018, 36, 4979–4992. [Google Scholar] [CrossRef] [PubMed]
- Mrklas, K.J.; MacDonald, S.; Shea-Budgell, M.A.; Bedingfield, N.; Ganshorn, H.; Glaze, S.; Bill, L.; Healy, B.; Healy, C.; Guichon, J.; et al. Barriers, supports, and effective interventions for uptake of human papillomavirus- and other vaccines within global and Canadian Indigenous peoples: A systematic review protocol. Syst. Rev. 2018, 7, 40. [Google Scholar] [CrossRef] [PubMed]
- Rose, K.C. Adolescent Vaccines: Latest Recommendations, Addressing Barriers, and Improving Vaccine Rates. NASN Sch. Nurse 2017, 32, 217–222. [Google Scholar] [CrossRef]
- Bergman, H.; Buckley, B.S.; Villanueva, G.; Petkovic, J.; Garritty, C.; Lutje, V.; Riveros-Balta, A.X.; Low, N.; Henschke, N. Comparison of different human papillomavirus (HPV) vaccine types and dose schedules for prevention of HPV-related disease in females and males. Cochrane Database Syst. Rev. 2019, 2019, CD013479. [Google Scholar] [CrossRef] [PubMed]
- Murillo, R.; Ordóñez-Reyes, C. Human papillomavirus (HPV) vaccination: From clinical studies to immunization programs. Int. J. Gynecol. Cancer 2019, 29, 1317–1326. [Google Scholar] [CrossRef]
- Toh, Z.Q.; Kosasih, J.; Russell, F.M.; Garland, S.M.; Mulholland, E.K.; Licciardi, P.V. Recombinant human papillomavirus nonavalent vaccine in the prevention of cancers caused by human papillomavirus. Infect. Drug Resist. 2019, 12, 1951–1967. [Google Scholar] [CrossRef]
- Drolet, M.; Bénard, É.; Pérez, N.; Brisson, M. HPV Vaccination Impact Study Group. Population-level impact and herd effects following the introduction of human papillomavirus vaccination programmes: Updated systematic review and meta-analysis. Lancet 2019, 394, 497–509. [Google Scholar] [CrossRef]
- Chesson, H.W.; Meites, E.; Ekwueme, D.U.; Saraiya, M.; Markowitz, L.E. Updated medical care cost estimates for HPV-associated cancers: Implications for cost-effectiveness analyses of HPV vaccination in the United States. Hum. Vaccines Immunother. 2019, 15, 1942–1948. [Google Scholar] [CrossRef]
- Dilley, S.; Miller, K.M.; Huh, W.K. Human papillomavirus vaccination: Ongoing challenges and future directions. Gynecol. Oncol. 2020, 156, 498–502. [Google Scholar] [CrossRef]
- Halista, C.E.; Kline, R.J.; Bepko, J. Understanding Barriers to HPV Vaccination: Perspectives from Air Force Family Medicine Physicians and Active Duty Air Force Males. Mil. Med. 2019. [Google Scholar] [CrossRef] [PubMed]
- Guzman-Holst, A.; DeAntonio, R.; Prado-Cohrs, D.; Juliao, P. Barriers to vaccination in Latin America: A systematic literature review. Vaccine 2020, 38, 470–481. [Google Scholar] [CrossRef] [PubMed]
- Gidengil, C.; Chen, C.; Parker, A.M.; Nowak, S.; Matthews, L. Beliefs around childhood vaccines in the United States: A systematic review. Vaccine 2019, 37, 6793–6802. [Google Scholar] [CrossRef] [PubMed]
- Dibble, K.E.; Maksut, J.L.; Siembida, E.J.; Hutchison, M.; Bellizzi, K.M. A Systematic Literature Review of HPV Vaccination Barriers among Adolescent and Young Adult Males. J. Adolesc. Young Adult Oncol. 2019, 8, 495–511. [Google Scholar] [CrossRef] [PubMed]
- Patel, S.; Koskan, A.; Spolarich, A.; Perry, M.; Flood, T. Dental professionals’ knowledge, attitudes, and practice behaviors related to human papillomavirus vaccination. J. Public Health Dent. 2019. [Google Scholar] [CrossRef]
- Berenson, A.B.; Hirth, J.M.; Southerland, J.H. Knowledge of human papillomavirus among dental providers: A mixed methods study. Vaccine 2020, 38, 423–426. [Google Scholar] [CrossRef]
- Rutkoski, H.; Fowler, B.; Mooney, R.; Pappas, L.; Dixon, B.L.; Pinzon, L.M.; Winkler, J.; Kepka, D. Pilot Test of Survey to Assess Dental and Dental Hygiene Student Human Papillomavirus-Related Oropharyngeal Cancer Knowledge, Perceptions, and Clinical Practices. J. Cancer Educ. 2018, 33, 907–914. [Google Scholar] [CrossRef]
- Kepka, D.; Rutkoski, H.; Pappas, L.; Tay, D.L.; Winkler, J.R.; Dixon, B.; Velazquez, A.; Pinzon, L.M. US oral health students’ willingness to train and administer the HPV vaccine in dental practices. Prev. Med. Rep. 2019, 15, 100957. [Google Scholar] [CrossRef]
- Cotter, J.C.; Wilson, K.J.; Mallonee, L.F. Impact of HPV Immunization Training on Dental Hygiene Students’ Attitudes and Confidence Regarding HPV Preventive Education. J. Dent. Educ. 2019. [Google Scholar] [CrossRef]
- Gerend, M.A.; Magloire, Z.F. Awareness, knowledge, and beliefs about human papillomavirus in a racially diverse sample of young adults. J. Adolesc. Health 2008, 42, 237–242. [Google Scholar] [CrossRef]
- Arnell, T.L.; York, C.; Nadeau, A.; Donnelly, M.L.; Till, L.; Zargari, P.; Davis, W.; Finley, C.; Delaney, T.; Carney, J. The Role of the Dental Community in Oropharyngeal Cancer Prevention through HPV Vaccine Advocacy. J. Cancer Educ. 2019. [Google Scholar] [CrossRef] [PubMed]
- Naleway, A.L.; Henninger, M.L.; Waiwaiole, L.A.; Mosen, D.M.; Leo, M.C.; Pihlstrom, D.J. Dental provider practices and perceptions regarding adolescent vaccination. J. Public Health Dent. 2018, 78, 159–164. [Google Scholar] [CrossRef] [PubMed]
- La Fauci, V.; Squeri, R.; Genovese, C.; Anzalone, C.; Fedele, F.; Squeri, A.; Alessi, V. An observational study of university students of healthcare area: Knowledge, attitudes and behaviour towards vaccinations. Clin. Ter. 2019, 170, e448–e453. [Google Scholar] [CrossRef] [PubMed]
- Shetty, S.; Prabhu, S.; Shetty, V.; Shetty, A.K. Knowledge, attitudes and factors associated with acceptability of human papillomavirus vaccination among undergraduate medical, dental and nursing students in South India. Hum. Vaccines Immunother. 2019, 15, 1656–1665. [Google Scholar] [CrossRef]
- Harris, K.L.; Tay, D.; Kaiser, D.; Praag, A.; Rutkoski, H.; Dixon, B.L.; Pinzon, L.M.; Winkler, J.R.; Kepka, D. The perspectives, barriers, and willingness of Utah dentists to engage in human papillomavirus (HPV) vaccine practices. Hum. Vaccines Immunother. 2020, 16, 436–444. [Google Scholar] [CrossRef]
- Grillo, A.C.; Ghoneima, A.A.M.; Garetto, L.P.; Bhamidipalli, S.S.; Stewart, K.T. Predictors of orthodontic residency performance: An assessment of scholastic and demographic selection parameters. Angle Orthod. 2019, 89, 488–494. [Google Scholar] [CrossRef]
- Yuan, J.C.; Lee, D.J.; Knoernschild, K.L.; Campbell, S.D.; Sukotjo, C. Resident selection criteria for advanced education in prosthodontic programs: Program directors’ perspective. J. Prosthodont. 2010, 19, 307–314. [Google Scholar] [CrossRef]
- Alhajj, M.N.; Khader, Y.; Murad, A.H.; Celebic, A.; Halboub, E.; Márquez, J.R.; Macizo, C.C.; Khan, S.; Basnet, B.B.; Makzoumé, J.E.; et al. Perceived sources of stress amongst dental students: A multicountry study. Eur. J. Dent. Educ. 2018, 22, 258–271. [Google Scholar] [CrossRef]
- Andre, A.; Pierre, G.C.; McAndrew, M. Quality of Life among Dental Students: A Survey Study. J. Dent. Educ. 2017, 81, 1164–1170. [Google Scholar] [CrossRef]
- Guvenc, G.; Seven, M.; Akyuz, A. Health Belief Model Scale for Human Papilloma Virus and its Vaccination: Adaptation and Psychometric Testing. J. Pediatr. Adolesc. Gynecol. 2016, 29, 252–258. [Google Scholar] [CrossRef]
- Cunningham, J.; Wallston, K.A.; Wilkins, C.H.; Hull, P.C.; Miller, S.T. Development and Psychometric Evaluation of the HPV Clinical Trial Survey for Parents (CTSP-HPV) Using Traditional Survey Development Methods and Community Engagement Principles. Clin. Transl. Sci. 2015, 8, 702–709. [Google Scholar] [CrossRef] [PubMed]
- Perez, S.; Shapiro, G.K.; Tatar, O.; Joyal-Desmarais, K.; Rosberger, Z. Development and Validation of the Human Papillomavirus Attitudes and Beliefs Scale in a National Canadian Sample. Sex. Transm. Dis. 2016, 43, 626–632. [Google Scholar] [CrossRef] [PubMed]
| Demographics | DMD Student Population | DMD Survey Respondents | Statistical Analysis |
|---|---|---|---|
| Sex | |||
| Male | 55.4% (n = 173/312) | 54.9% (n = 161/293) | χ2 = 0.101, d.f. = 1 |
| Female | 44.6% (n = 139/312) | 45.1% (n = 132/293) | p = 0.7504 |
| Race/Ethnicity | |||
| White | 49.4% (n = 154) | 48.5% (n = 242/293) | χ2 = 0.324, d.f. = 1 |
| Non-White (Minority) | 50.6% (n = 158) | 51.5% (n = 151/293) | p = 0.5692 |
| Asian | 39.1% (n = 122) | ||
| Hispanic | 8.7% (n = 27) | ||
| Other | 2.9% (n = 9) |
| Demographics | Post-Graduate Resident Population | Post-Graduate Survey Respondents | Statistical Analysis |
|---|---|---|---|
| Sex | |||
| Male | 47.9% (n = 23/48) | 48.7% (n = 20/41) | χ2 = 0.256, d.f. = 1 |
| Female | 52.1% (n = 25/48) | 51.3% (n = 21/41) | p = 0.6128 |
| Race/Ethnicity | |||
| White | 45.8% (n = 22/48) | 46.3% (n = 19/41) | χ2 = 0.101, d.f. = 1 |
| Non-White (Minority) | 54.2% (n = 26/48) | 53.7% (n = 22/41) | p = 0.7512 |
| Asian | 54.2% (n = 26/48) | 53.7% (n = 22/41) | |
| Hispanic | N/A | N/A | |
| Other | N/A | N/A |
© 2020 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Mann, S.K.; Kingsley, K. Human Papillomavirus (HPV) Vaccine Knowledge, Awareness and Acceptance among Dental Students and Post-Graduate Dental Residents. Dent. J. 2020, 8, 45. https://doi.org/10.3390/dj8020045
Mann SK, Kingsley K. Human Papillomavirus (HPV) Vaccine Knowledge, Awareness and Acceptance among Dental Students and Post-Graduate Dental Residents. Dentistry Journal. 2020; 8(2):45. https://doi.org/10.3390/dj8020045
Chicago/Turabian StyleMann, Steven Kent, and Karl Kingsley. 2020. "Human Papillomavirus (HPV) Vaccine Knowledge, Awareness and Acceptance among Dental Students and Post-Graduate Dental Residents" Dentistry Journal 8, no. 2: 45. https://doi.org/10.3390/dj8020045
APA StyleMann, S. K., & Kingsley, K. (2020). Human Papillomavirus (HPV) Vaccine Knowledge, Awareness and Acceptance among Dental Students and Post-Graduate Dental Residents. Dentistry Journal, 8(2), 45. https://doi.org/10.3390/dj8020045





