Green Tea Polyphenol Epigallocatechin-3-Gallate-Stearate Inhibits the Growth of Streptococcus mutans: A Promising New Approach in Caries Prevention
Abstract
1. Introduction
2. Materials and Methods
2.1. Culturing and Maintenance of Bacterial Cultures
2.2. Preparation of EGCG-S
2.3. Colony Forming Unit (CFU) Assay
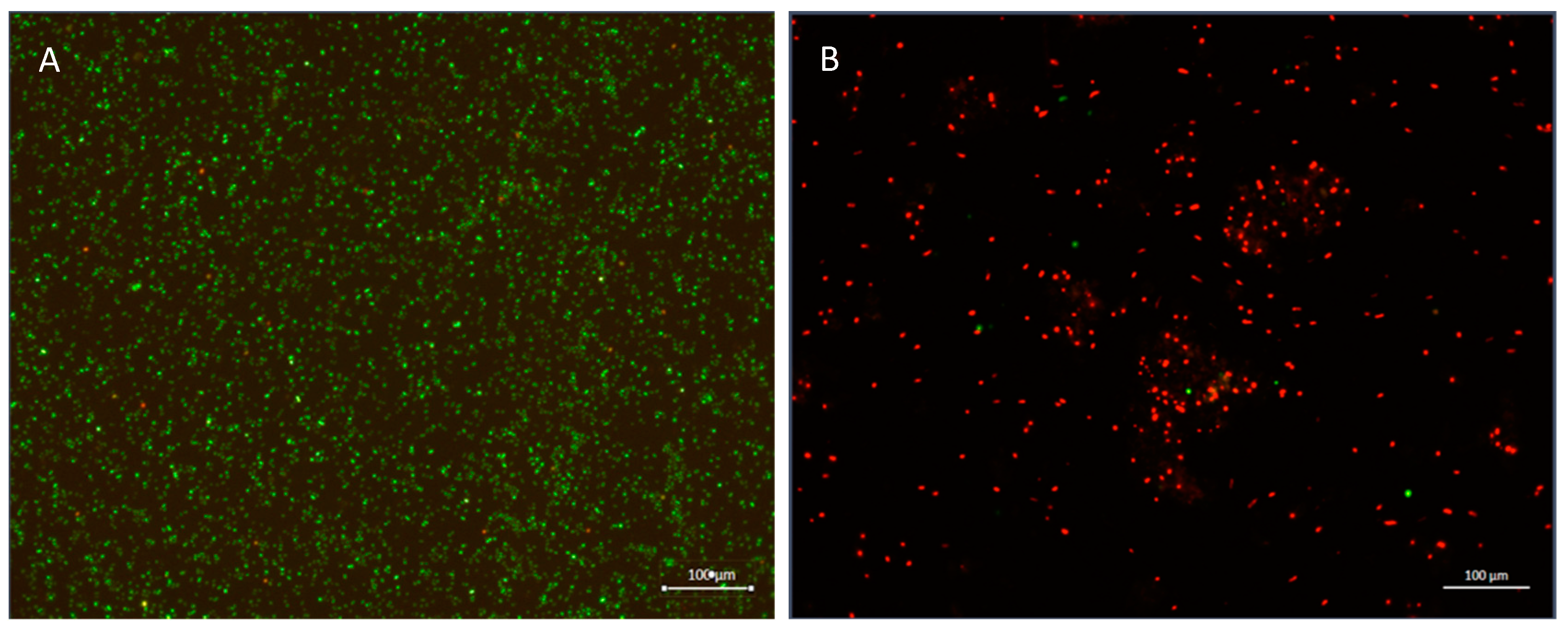
2.4. Viability Assay
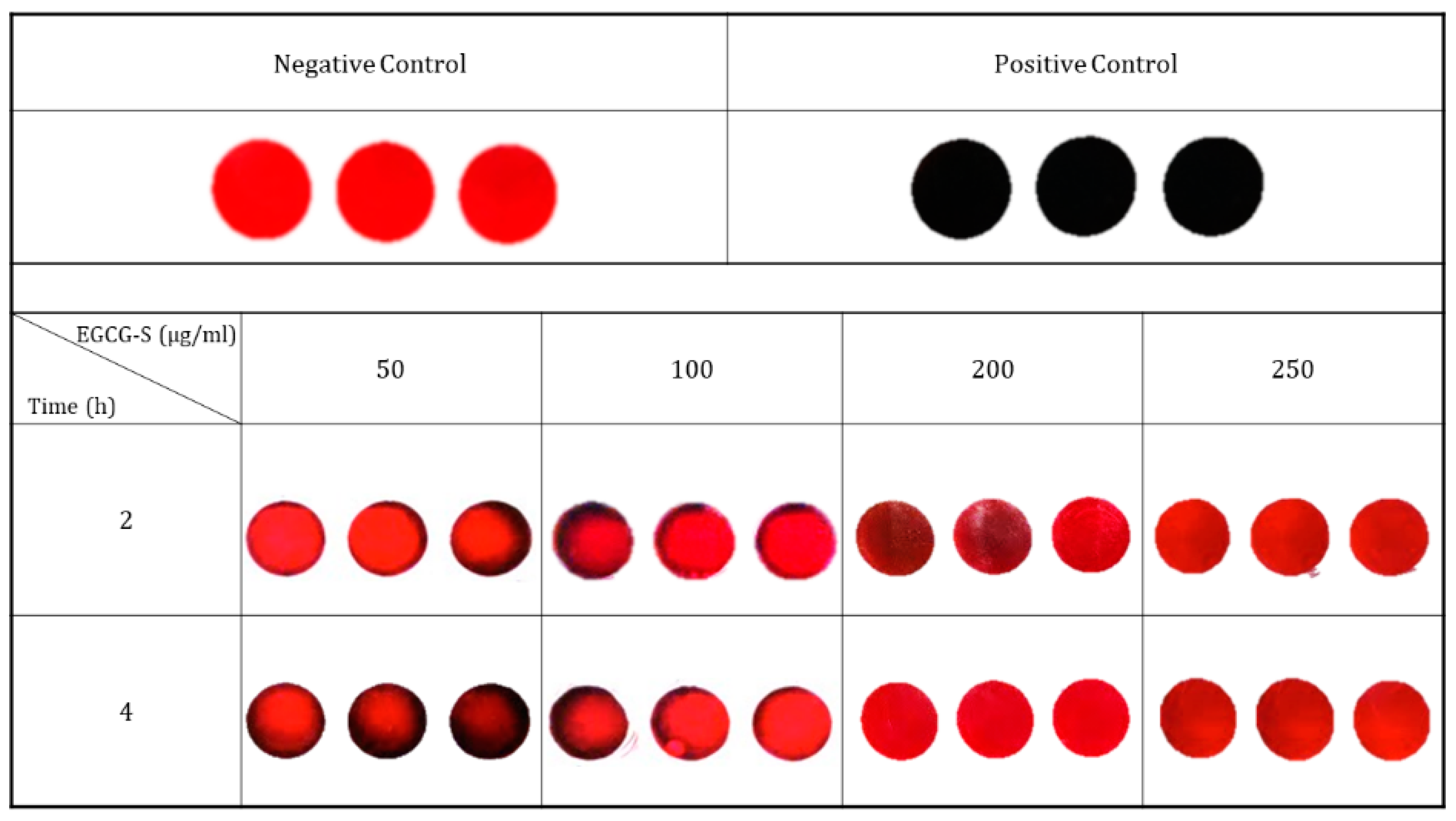
2.5. Congo Red Assay
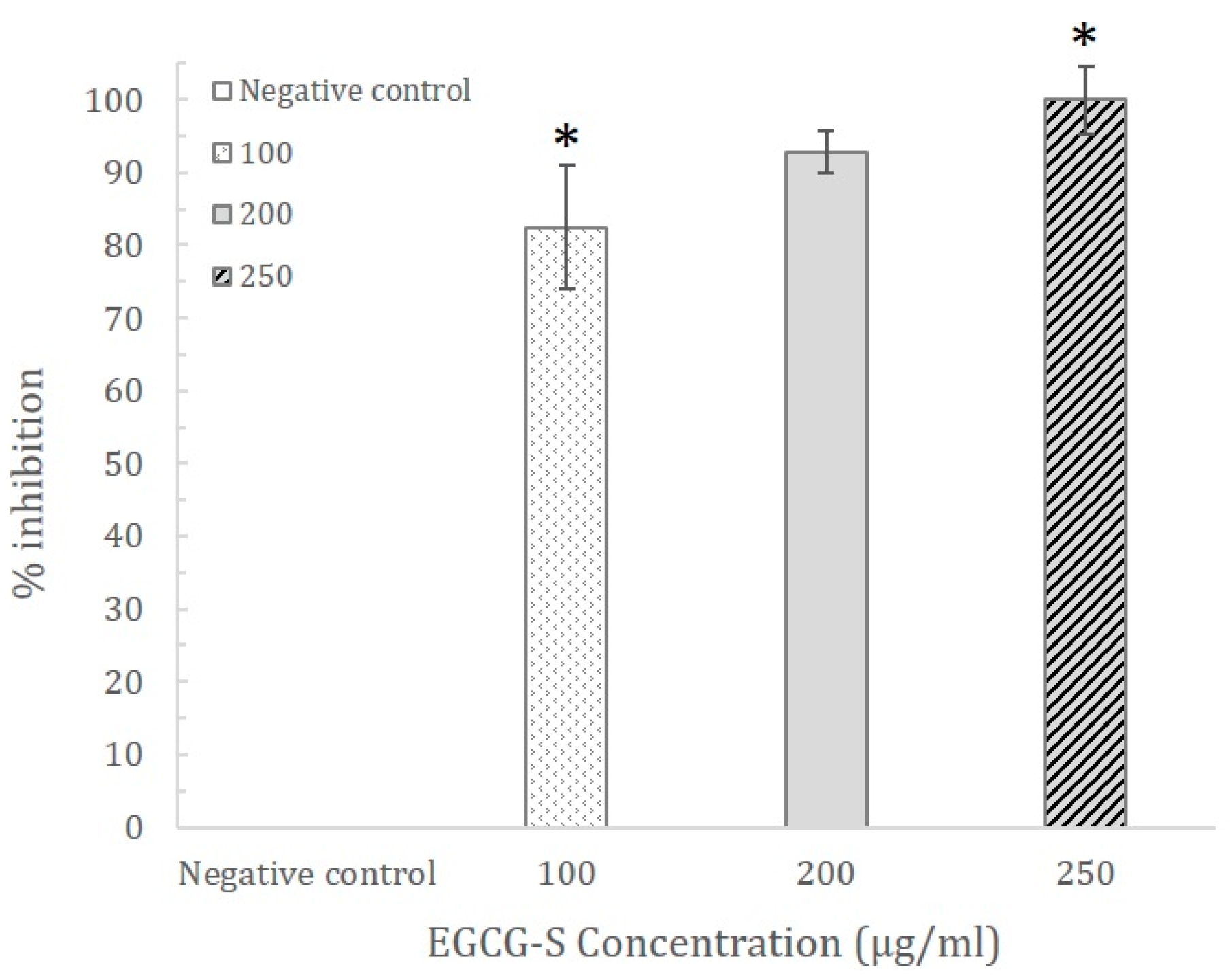
2.6. Crystal Violet Assay
2.7. Scanning Electron Microscopy (SEM)
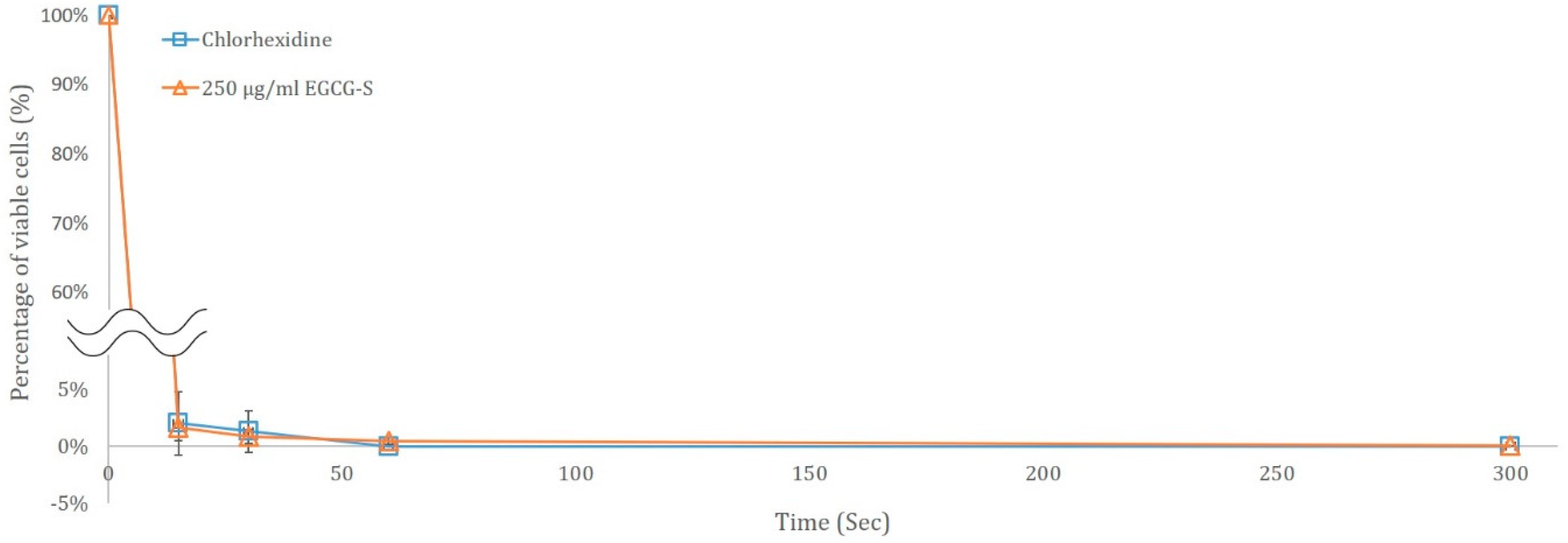
2.8. Time Course Study
2.9. Statistical Analysis
3. Results
3.1. The Effect of EGCG-S on S. mutans
3.2. The Effect of EGCG-S on Biofilm of S. mutans
3.3. Time Course Study of S. mutans treated with 250 µg/mL EGCG-S and Chlorhexidine Gluconate
4. Discussion
Author Contributions
Acknowledgments
Conflicts of Interest
References
- Aas, J.A.; Paster, B.J.; Stokes, L.N.; Olsen, I.; Dewhirst, F.E. Defining the normal bacterial flora of the oral cavity. J. Clin. Microbiol. 2005, 43, 5721–5732. [Google Scholar] [CrossRef] [PubMed]
- Gao, X.; Jiang, S.; Koh, D.; Hsu, C.-Y.S. Salivary biomarkers for dental caries. Periodontology 2000 2016, 70, 128–141. [Google Scholar] [CrossRef] [PubMed]
- Aframian, D.J.; Davidowitz, T.; Benoliel, R. The distribution of oral mucosal pH values in healthy saliva secretors. Oral Dis. 2006, 12, 420–423. [Google Scholar] [CrossRef] [PubMed]
- Downer, M.C.; Drugan, C.S.; Blinkhorn, A.S. Dental caries experience of British children in an international context. Community Dent. Health 2005, 22, 86–93. [Google Scholar] [PubMed]
- Marsh, P.D. Dental plaque as a microbial biofilm. Caries Res. 2004, 38, 204–211. [Google Scholar] [CrossRef] [PubMed]
- Blanco, A.R.; Sudano-Roccaro, A.; Spoto, G.C.; Nostro, A.; Rusciano, D. Epigallocatechin gallate inhibits biofilm formation by ocular staphylococcal isolates. Antimicrob. Agents Chemother. 2005, 49, 4339–4343. [Google Scholar] [CrossRef] [PubMed]
- Dunne, W.M. Bacterial adhesion: Seen any good biofilms lately? Clin. Microbiol. Rev. 2002, 15, 155–166. [Google Scholar] [CrossRef] [PubMed]
- Duchin, S.; van Houte, J. Colonization of teeth in humans by Streptococcus mutans as related to its concentration in saliva and host age. Infect. Immun. 1978, 20, 120–125. [Google Scholar] [PubMed]
- Kolenbrander, P.E.; Jakubovics, N.S.; Chalmers, N.I.; Palmer, R.J. Human Oral multispecies biofilms: Bacterial communities in health and disease. In The Biofilm Mode of Life: Mechanisms and Adaptations; Kjelleberg, S., Givskov, M., Eds.; Horizon Scientific Press: Poole, UK, 2007; pp. 175–190. [Google Scholar]
- Chu, T.-C.; Adams, S.D.; Lee, L.H. Tea polyphenolic compounds against herpes simplex viruses. In Cancer-Causing Viruses and Their Inhibitors; Gupta, S.P., Ed.; CRC Press, Taylor & Francis Group: Boca Raton, FL, USA, 2014. [Google Scholar]
- de Oliveira, A.; Adams, S.D.; Lee, L.H.; Murray, S.R.; Hsu, S.D.; Hammond, J.R.; Dickinson, D.; Chen, P.; Chu, T.C. Inhibition of herpes simplex virus type 1 with the modified green tea polyphenol palmitoyl-epigallocatechin gallate. Food Chem. Toxicol. 2013, 52, 207–215. [Google Scholar] [CrossRef] [PubMed]
- de Oliveira, A.; Prince, D.; Lo, C.Y.; Lee, L.H.; Chu, T.C. Antiviral activity of theaflavin digallate against herpes simplex virus type 1. Antivir. Res. 2015, 118, 56–67. [Google Scholar] [CrossRef] [PubMed]
- Elvinlewis, M.; Steelman, R. The anticariogenic effects of tea drinking among Dallas schoolchildren. J. Dent. Res. 1986, 65, 198. [Google Scholar]
- Haghjoo, B.; Lee, L.H.; Habiba, U.; Tahir, H.; Olabi, M.; Chu, T.-C. The synergistic effects of green tea polyphenols and antibiotics against potential pathogens. Adv. Biosci. Biotechnol. 2013, 4, 959. [Google Scholar] [CrossRef]
- Hamilton-Miller, J.M. Anti-cariogenic properties of tea (Camellia sinensis). J. Med. Microbiol. 2001, 50, 299–302. [Google Scholar] [CrossRef] [PubMed]
- Otake, S.; Makimura, M.; Kuroki, T.; Nishihara, Y.; Hirasawa, M. Anticaries effects of polyphenolic compounds from Japanese green tea. Caries Res. 1991, 25, 438–443. [Google Scholar] [CrossRef] [PubMed]
- Sakanaka, S.; Kim, M.; Taniguchi, M.; Yamamoto, T. Antibacterial substances in Japanese green tea extract against Streptococcus mutans, a cariogenic bacterium. Agric. Biol. Chem. 1989, 53, 2307–2311. [Google Scholar] [CrossRef]
- Xu, X.; Zhou, X.D.; Wu, C.D. Tea catechin epigallocatechin gallate inhibits Streptococcus mutans biofilm formation by suppressing gtf genes. Arch. Oral Biol. 2012, 57, 678–683. [Google Scholar] [CrossRef] [PubMed]
- Zhao, M.; Zheng, R.; Jiang, J.; Dickinson, D.; Fu, B.; Chu, T.-C.; Lee, L.H.; Pearl, H.; Hsu, S. Topical lipophilic epigallocatechin-3-gallate on herpes labialis: A phase II clinical trial of AverTeaX formula. Oral Surg. Oral Med. Oral Pathol. Oral Radiol. 2015, 120, 717–724. [Google Scholar] [CrossRef] [PubMed]
- Taylor, P.W.; Hamilton-Miller, J.M.; Stapleton, P.D. Antimicrobial properties of green tea catechins. Food Sci. Technol. Bull. 2005, 2, 71. [Google Scholar] [CrossRef] [PubMed]
- Hong, J.; Lu, H.; Meng, X.; Ryu, J.-H.; Hara, Y.; Yang, C.S. Stability, cellular uptake, biotransformation, and efflux of tea polyphenol (−)-epigallocatechin-3-gallate in HT-29 human colon adenocarcinoma cells. Cancer Res. 2002, 62, 7241–7246. [Google Scholar] [PubMed]
- Su, Y.L.; Leung, L.K.; Huang, Y.; Chen, Z.-Y. Stability of tea theaflavins and catechins. Food Chem. 2003, 83, 189–195. [Google Scholar]
- Venkateswara, B.; Sirisha, K.; Chava, V.K. Green tea extract for periodontal health. J. Indian Soc. Periodontol. 2011, 15, 18. [Google Scholar] [CrossRef] [PubMed]
- Chen, P.; Dickinson, D.; Hsu, S.D. Lipid-soluble green tea polyphenols: Stabilized for effective formulation. In Handbook of Green Tea and Health Research; McKinley, H., Jamieson, M., Eds.; Nova Science: New York, NY, USA, 2009; pp. 45–61. [Google Scholar]
- Xu, X.; Zhou, X.D.; Wu, C.D. The tea catechin epigallocatechin gallate suppresses cariogenic virulence factors of Streptococcus mutans. Antimicrob. Agents Chemother. 2011, 55, 1229–1236. [Google Scholar] [CrossRef] [PubMed]
- You, S.Q. Study on feasibility of Chinese green tea polyphenols (CTP) for preventing dental caries. Zhonghua Kou Qiang Yi Xue Za Zhi 1993, 28, 197–199, 254. [Google Scholar] [PubMed]
- Schwartz, K.; Syed, A.K.; Stephenson, R.E.; Rickard, A.H.; Boles, B.R. Functional amyloids composed of phenol soluble modulins stabilize Staphylococcus aureus biofilms. PLoS Pathog. 2012, 8, e1002744. [Google Scholar] [CrossRef] [PubMed]
- Nowak, J.; Cruz, C.D.; Palmer, J.; Fletcher, G.C.; Flint, S. Biofilm formation of the L. monocytogenes strain 15G01 is influenced by changes in environmental conditions. J. Microbiol. Methods 2015, 119, 189–195. [Google Scholar] [PubMed]
- Newby, J.R.; Lee, L.H.; Perez, J.L.; Tao, X.; Chu, T. Characterization of zinc stress response in Cyanobacterium Synechococcus sp. IU 625. Aquat. Toxicol. 2017, 186, 159–170. [Google Scholar] [CrossRef] [PubMed]
- Anita, P.; Sivasamy, S.; Madan Kumar, P.D.; Balan, I.N.; Ethiraj, S. In vitro antibacterial activity of Camellia sinensis extract against cariogenic microorganisms. J. Basic Clin. Pharm. 2015, 6, 35–39. [Google Scholar] [CrossRef] [PubMed]
- Caturla, N.; Vera-Samper, E.; Villalain, J.; Mateo, C.R.; Micol, V. The relationship between the antioxidant and the antibacterial properties of galloylated catechins and the structure of phospholipid model membranes. Free Radic. Biol. Med. 2003, 34, 648–662. [Google Scholar] [CrossRef]
- Gordon, N.C.; Wareham, D.W. Antimicrobial activity of the green tea polyphenol (−)-epigallocatechin-3-gallate (EGCG) against clinical isolates of Stenotrophomonas maltophilia. Int. J. Antimicrob. Agents 2010, 36, 129–131. [Google Scholar] [CrossRef] [PubMed]
- Hamilton-Miller, J.M. Antimicrobial properties of tea (Camellia sinensis L.). Antimicrob. Agents Chemother. 1995, 39, 2375–2377. [Google Scholar] [CrossRef] [PubMed]
- Ikigai, H.; Nakae, T.; Hara, Y.; Shimamura, T. Bactericidal catechins damage the lipid bilayer. Biochim. Biophys. Acta 1993, 1147, 132–136. [Google Scholar] [CrossRef]
- Tamba, Y.; Ohba, S.; Kubota, M.; Yoshioka, H.; Yamazaki, M. Single GUV method reveals interaction of tea catechin (−)-epigallocatechin gallate with lipid membranes. Biophys. J. 2007, 92, 3178–3194. [Google Scholar] [CrossRef] [PubMed]
- Yanagawa, Y.; Yamamoto, Y.; Hara, Y.; Shimamura, T. A combination effect of epigallocatechin gallate, a major compound of green tea catechins, with antibiotics on Helicobacter pylori growth in vitro. Curr. Microbiol. 2003, 47, 244–249. [Google Scholar] [PubMed]
- Koech, K.R.; Wachira, F.N.; Ngure, R.M.; Wanyoko, J.K.; Bii, C.C.; Karori, S.M.; Kerio, L.C. Antioxidant, antimicrobial and synergistic activities of tea polyphenols. Afr. Crop Sci. J. 2014, 22, 837–846. [Google Scholar] [CrossRef]
- Osterburg, A.; Gardner, J.; Hyon, S.H.; Neely, A.; Babcock, G. Highly antibiotic-resistant Acinetobacter baumannii clinical isolates are killed by the green tea polyphenol (−)-epigallocatechin-3-gallate (EGCG). Clin. Microbiol. Infect. 2009, 15, 341–346. [Google Scholar] [CrossRef] [PubMed]
- Zhao, W.H.; Hu, Z.Q.; Okubo, S.; Hara, Y.; Shimamura, T. Mechanism of synergy between epigallocatechin gallate and beta-lactams against methicillin-resistant Staphylococcus aureus. Antimicrob. Agents Chemother. 2001, 45, 1737–1742. [Google Scholar] [CrossRef] [PubMed]

| EGCG-S Concentration (µg/mL) | CFU (cells/mL) | Log Reduction |
|---|---|---|
| 0 | 1.01 × 1012 ± 9.24 × 1010 | 0 |
| 100 | 6.57 × 1010 ± 3.20 × 109 | 1.19 ± 0.02 |
| 200 | 9.20 × 109 ± 4.00 × 108 | 2.04 ± 0.02 |
| 250 | 2.30 × 109 ± 2.65 × 108 | 2.65 ± 0.01 |
© 2018 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).
Share and Cite
Melok, A.L.; Lee, L.H.; Mohamed Yussof, S.A.; Chu, T. Green Tea Polyphenol Epigallocatechin-3-Gallate-Stearate Inhibits the Growth of Streptococcus mutans: A Promising New Approach in Caries Prevention. Dent. J. 2018, 6, 38. https://doi.org/10.3390/dj6030038
Melok AL, Lee LH, Mohamed Yussof SA, Chu T. Green Tea Polyphenol Epigallocatechin-3-Gallate-Stearate Inhibits the Growth of Streptococcus mutans: A Promising New Approach in Caries Prevention. Dentistry Journal. 2018; 6(3):38. https://doi.org/10.3390/dj6030038
Chicago/Turabian StyleMelok, Amy Lynn, Lee H. Lee, Siti Ayuni Mohamed Yussof, and Tinchun Chu. 2018. "Green Tea Polyphenol Epigallocatechin-3-Gallate-Stearate Inhibits the Growth of Streptococcus mutans: A Promising New Approach in Caries Prevention" Dentistry Journal 6, no. 3: 38. https://doi.org/10.3390/dj6030038
APA StyleMelok, A. L., Lee, L. H., Mohamed Yussof, S. A., & Chu, T. (2018). Green Tea Polyphenol Epigallocatechin-3-Gallate-Stearate Inhibits the Growth of Streptococcus mutans: A Promising New Approach in Caries Prevention. Dentistry Journal, 6(3), 38. https://doi.org/10.3390/dj6030038





